Pigmented astrocytoma with suprasellar location: case report and literature review
|
|
|
- Calvin Ryan
- 5 years ago
- Views:
Transcription
1 Acta Neuropathol (2004) 108: DOI /s CASE REPORT Ba rd Kronen Krossnes Æ Olav Mella Æ Knut Wester Sverre Jarl Mørk Pigmented astrocytoma with suprasellar location: case report and literature review Received: 7 April 2004 / Revised: 14 June 2004 / Accepted: 18 June 2004 / Published online: 7 September 2004 Ó Springer-Verlag 2004 Abstract A large suprasellar, partly cystic, contrastenhancing tumor was resected from a 19-year-old woman who presented with bitemporal visual field defects and reduced visual acuity. Grossly, the tumor was brown and located in the subarachnoid space. Histologically, it was composed of spindle and pleomorphic cells, including giant tumor cells, with markedly pleomorphic nuclei. Reticulin fibers surrounded single cells and small groups of cells. Very few mitotic figures were found in the tumor, and no necrosis or microvascular proliferation was seen. The tumor thereby resembled a pleomorphic xanthoastrocytoma. Many of the tumor cells contained a dark-brown intracytoplasmic pigment, shown to be melanosomal melanin by ultrastructural examination. Immunohistochemical examination demonstrated that the pigment was present in glial tumor cells. Only four cases of pigmented astrocytic tumors have been published, none of these were suprasellar. Our patient received fractionated radiotherapy with a total dose of 48.6 Gy 14 months after gross total removal of the tumor. She is alive without relapse after 12-year follow-up. Keywords Astrocytoma Æ Melanin Æ Pleomorphic xanthoastrocytoma Æ Suprasellar tumor B. K. Krossnes (&) Æ S. J. Mørk The Gade Institute, Department of Pathology, Haukeland University Hospital, 5021 Bergen, Norway bkkr@haukeland.no Tel.: Fax: O. Mella Department of Oncology, Institute of Medicine, Haukeland University Hospital, 5021 Bergen, Norway K. Wester Department of Neurosurgery, Institute of Surgical Sciences, Haukeland University Hospital, 5021 Bergen, Norway Introduction Pigmented (melanotic) neoplasms have been reported at various sites in the central and peripheral nervous system. The non-neuroepithelial pigmented intracranial tumors reported in the literature are schwannoma [46], benign and malignant melanocytic lesions arising from the leptomeninges [17] and possibly meningioma [21]. Previous reports on pigmented neuroepithelial tumors include astrocytoma [19, 39, 43], ganglioglioma [41], ependymoma [8, 28, 34], subependymoma [34], choroid plexus papilloma [33, 38, 45], choroid plexus carcinoma [5, 27], primitive pineal tumor [4, 31, 32, 35], medulloblastoma [3, 6, 10, 18, 40], medulloepithelioma [37], and central neurocytoma [30]. Ultrastructurally, some of these tumors contained melanosomal melanin [6, 10, 19, 27, 39, 40], while others contained neuromelanin and/or lipofuscin [5, 8, 30, 33, 43]. There are only four previous reports of melanotic astrocytomas: one case of pigmented pilocytic astrocytoma [43], one case of astrocytoma which resembled a pleomorphic xanthoastrocytoma (PXA) [19], one case of PXA [39], and one cerebral ganglioglioma with PXA as the glioma component [41]. Except for the pilocytic astrocytoma, which contained neuromelanin, the pigment in these tumors was shown to be melanosomal melanin. Here we present a melanotic astrocytoma with remarkable morphology and location. Clinical history The patient developed normally until she was years old. Growth then stopped and she developed some adiposity. She had menarche at the age of 12 years, but developed secondary amenorrhea after her first menstruation. Gynecological examination did not show pathology, but endocrinological examination showed low s-estradiol levels. The patient was given medroksyprogesteronacetate for 5 days four times a year to induce menstruation. At the age of 18, she was submitted
2 462 to hospital after a trauma to her left eye. Half a year later she was referred to an ophthalmologist because of reduced visual acuity on the right eye. Bitemporal visual field defects were then found, most pronounced on the right eye. Further examination by CT revealed a suprasellar, well-circumscribed, partly cystic, contrast-enhancing tumor measuring cm in anteroposterior, mediolateral, and vertical directions, respectively (Fig. 1). There was a slight destruction of the dorsum sellae. The radiological diagnosis was craniopharyngeoma. The pituitary function was normal except for low s-levels of growth hormone. The visual field defects progressed over the next months and at the time of surgery the patient had developed bitemporal hemianopsia. Frontal craniotomy was performed when the patient was 19 years old, disclosing a brown suprasellar tumor located in the subarachnoid space. The tumor was found to grow along, and ventral to, both optic nerves and optic chiasma. Small pigmented spots presumed to represent tumor tissue, on the optic nerves near the entrance to the optic canals and on the anterior/inferior rim of the optic chiasma, were not resected to avoid damaging the optic nerves. The immediate peroperative impression was that the tumor might have originated in the leptomeninges at the diaphragma sellae or the optic nerves/ chiasma. The tumor seemed less likely to have originated from the infundibulum or the hypothalamus, as the tumor mass was easily advanced from under the chiasma, apparently not adherent to the anterior aspects of the hypothalamus/pituitary stalk. Postoperative cerebral magnetic resonance imaging (MRI) confirmed the presence of very small lesions with contrast enhancement along both optic nerves and in a small area in the floor of the third ventricle, regarded as probable residual tumor. The visual field defects continued to progress for 1 year after the operation; after that no further visual impairment was observed. However, MRI could not document further tumor growth. To reduce the danger of blindness, the patient was given radiotherapy to the original tumor area with margins including the posterior orbit, the optic chiasma and the hypophysis. Radiotherapy was started 14 months postoperatively, 27 fractions of 1.8 Gy were given to a total dose of 48.6 Gy. After radiotherapy she needed thyroxin medication and also developed diabetes insipidus, whereas the cortisol production remained normal. The radiological findings have been stable, and completely unchanged, during follow-up, and the visual defects also have stabilized. She was well and free of clinical and radiological signs of relapse at last follow-up 12 years after the operation. Materials and methods The surgical specimen was fixed in 10% buffered formalin, routinely processed, and embedded in paraffin. Five-micrometer-thick sections were cut and the following stains were performed: hematoxylin-eosin, Wilder s reticulin silver impregnation, Masson-Fontana s methenamine silver method, Schmorl s ferric-ferricyanide method for melanin, Perl s Prussian blue, periodic acid-schiff with and without prior treatment with diastase, and acid-fast stain (long Ziehl-Neelsen). For immunohistochemical study, paraffin-embedded sections were stained with primary antibodies against: glial fibrillary acidic protein (GFAP, polyclonal, 1:3,000) with and without prior bleaching (for 2 h) with 0.25% potassium permanganate, S-100 protein (polyclonal, 1:800) with and without prior bleaching with potassium permanganate, synaptophysin (polyclonal, 1:100), chromogranin-a (polyclonal, 1:1,600), neuron-specific enolase (monoclonal, 1:200), melanosome-associated antigen HMB-45 (monoclonal, 1:50), neurofilament protein (monoclonal, 1:400), vimentin (monoclonal, 1:100), desmin (monoclonal, 1:50), laminin (monoclonal, 1:25), epithelial membrane antigen (monoclonal, 1:200), cytokeratin (monoclonal, 1:25 DAKO code no. M0821), Ki-67 (MIB-1, monoclonal, 1:50), and p53 (monoclonal, 1:25). All primary antibodies were from DAKO. Immunohistochemical procedures were performed on the automatic immunostainer DAKO TechMate 500 with the DAKO ChemMate Detection Kit, peroxidase/ DAB (code no. K 5001), which is a detection system based on an indirect streptavidin-biotin method. The Ki- 67 labeling index was expressed as a percentage of the total number of cells after counting 1,000 cells in the area with highest number of stained nuclei. For electron microscopic examination, representative areas were excised from one of the paraffin blocks, washed with phosphate buffer, fixed in McDowell solution, postfixed with 1% osmium tetroxide and embedded in Epon 812. Ultrathin sections were cut and stained with uranyl acetate and lead citrate, and examined with a Philips TEM 410 electron microscope at 60 kv. Fig. 1 CT scans after contrast-injection showing a sharply demarcated, suprasellar, contrast-enhancing tumor. A Transverse section (maximal tumor diameter 3.2 cm). B Coronal section Results The formalin-fixed biopsy specimen showed a tumor composed of large pleomorphic cells with copious
3 463 eosinophilic cytoplasm. Spindle-shaped cells forming fascicles dominated, and larger, plumper, often multinucleated cells were interspersed between the spindlefig. 2 Histological features of the tumor. A Fascicles of pleomorphic, spindle-shaped cells with pigmented areas (hematoxylin and eosin). B Pleomorphic glial cells with highly atypical nuclei (hematoxylin and eosin). C Many tumor cells contain melanin pigment granules (green-blue) (Schmorl). D Reticulin fibers surround individual cells and small groups of cells (reticulin silver impregnation). E The tumor cells display GFAP immunoreactivity (red) (immunoperoxidase). F Co-localization of GFAP-immunoreactive fibrils (red) and melanin pigment granules (dark-brown) is seen in the cells in the center (immunoperoxidase). A, D 100; B, C, E 200; F 630 shaped cells. The tumor cells had large, pleomorphic, hyperchromatic nuclei. Coarse chromatin and prominent nucleoli were often seen and nuclear inclusions were common (Fig. 2A, B). Xanthomatous cells were not present. Mitoses were rare (less than 1 per 50 highpower fields). Dark-brown pigment granules were found in many tumor cells, particularly spindle-shaped cells. The pigment was colored green-blue by Schmorl (Fig. 2C), and black with Masson-Fontana. It was negative for Perl s Prussian blue, acid-fast stain, and periodic acid-schiff. The pigment was completely bleached with potassium permanganate. Staining with
4 464 Wilder s reticulin silver impregnation revealed reticulin fibers surrounding individual cells and small groups of cells (Fig. 2D). In one area a few eosinophilic granular bodies were found. The eosinophilic granular bodies were stained red with periodic acid-schiff both with and without prior treatment with diastase. Focally, a slight perivascular infiltration of small lymphocytes was seen. No necrosis or microvascular proliferation was found. Brain tissue was not found in any of the sections. Immunohistochemical examination showed strong positivity for GFAP (Fig. 2E), S-100 protein, and vimentin in the tumor cells. About half of the cells were also positive for neuron-specific enolase. Co-localization of GFAP and pigment granules was found in some tumor cells (Fig. 2F), but generally the GFAP staining was weaker in the pigmented than in the non-pigmented tumor cells. Co-localization of S-100 and pigment granules was also found. The tumor was negative for the following antibodies: synaptophysin, chromogranin-a, neurofilament protein, HMB-45, epithelial membrane antigen, cytokeratin, desmin, and p53. No basal lamina surrounding individual cells was found in sections stained for laminin. The MIB-1 labeling index was 3%. Ultrastructural examination revealed large numbers of mature melanosomes and also some stage II and III melanosomes in pigmented tumor cells (Fig. 3). Neuromelanin or lipofuscin granules were not found. Bundles of filaments, probably intermediate filaments, were found in many tumor cells, particularly in long, thin cytoplasmic processes. Condensed fibers were found around several cells, but typical basal lamina was not present. Discussion This tumor was difficult to classify when it was examined in 1991, and was diagnosed as a pleomorphic, possibly anaplastic, astrocytic tumor with melanin pigmentation. Using the current (2000) WHO classification [24] the tumor is probably best regarded as a PXA. This entity Fig. 3 Electron microscopical features of tumor cells. A A tumor cell containing mature melanosomes. B Less mature (stage II and III) melanosomes are found in some cells. A 32,000; B 60,000 was first described by Kepes et al. in 1979 [22], but was not included in the WHO classification of CNS tumors before 1993 [25]. The fascicular arrangement of neoplastic cells, great cellular pleomorphism, low mitotic activity, prominent pericellular reticulin network, perivascular lymphocytes, subarachnoidal location of the tumor (without brain invasion), and CT findings (a discrete, contrast-enhancing and cystic tumor), are consistent with the diagnosis PXA [23]. On the other hand, the tumor lacks xanthomatous cells typical for PXA and contains only scarce eosinopilic granular bodies. This diagnosis, however, does not depend on the presence of xanthomatous cells [7, 16]. The proliferation rate as evaluated by the MIB-1 labeling index (3%) is somewhat higher in the present case than generally reported in this entity (lower than 1%) [23]. However, it is well known that comparison of labeling indexes reported from different institutions using different Ki-67 antibodies must be done with caution [42]. PXA is most often located superficially in the cerebral hemispheres. The suprasellar location of the present case is therefore rare for PXA, but a case of PXA with a similar location (just above the sella turcica) has been reported by Heyerdal Strøm et al. [14]. This tumor entity has also been described in the thalamus [26], and even an intrasellar PXA is on record [1]. Our patient had growth arrest, adiposity, and secondary amenorrhea from the age of 12 years, symptoms that may have been caused by the suprasellar tumor, indicating a slow tumor growth over several years until she underwent surgery at the age of 19. The long postoperative survival in the present case also indicates that this tumor is a low-grade astrocytoma, as anaplastic astrocytomas, even after radiotherapy, rarely have this long survival. It is interesting to note that the four earlier reported pigmented astrocytomas were low-grade tumors (pilocytic astrocytoma, PXA and ganglioglioma with PXA as the glioma component). These cases were located in the temporal lobe and associated with long-standing epilepsy, as opposed to our patient, where the tumor was located to the suprasellar area, not associated with seizures. Recurrence of the tumor has not been reported in any of the earlier reported pigmented astrocytomas; however, only one report describes a follow-up of more than 2 years after
5 465 surgery [41]. Our case is thus the first published case where long-term postoperative course without relapse has been documented, indicating that pigmented PXA do not differ from ordinary PXA concerning prognosis. Melanocytes, derived from the neural crest, are normally present in the pia mater of adult human subjects, although they are seldom recognized, except over the ventrolateral surface of the medulla oblongata and upper spinal cord [13]. These cells are the presumed origin of melanotic lesions in the meninges such as melanocytoma and malignant melanoma [17]. Melanin is normally produced in a specialized organelle called the melanosome. This organelle contains the enzyme tyrosinase, which is involved in the oxidation of tyrosine to the pigmented polymers we call melanin [36]. Production of melanosomal melanin in tissues of central neuroepithelial origin is developmentally restricted in humans to the fetal pineal gland [11] and to the pigmented layer of the retina [29]. Astrocytes are not involved in either of these synthetic modalities. Experiments in the OTT-6050 mouse teratoma model have shown that melanosomal melanin may be produced in primitive central neuroepithelial cells [12, 44]. Neuromelanin, which is believed to be a product of auto-oxidation of precursors in catecholamine synthesis, is normally found in certain groups of neurons such as substantia nigra and locus ceruleus. Ultrastructurally, neuromelanin is similar to lipofuscin [15]. Neuromelanin and melanosomal melanin have similar staining qualities in that they both are Schmorl and Masson-Fontana positive, with positivity disappearing after potassium permanganate bleaching [8]. In the present case lack of staining with periodic acid-schiff and acid-fast stain excludes the possibility that the pigment is lipofuscin [2, 8]. Ultrastructurally, the pigment was shown to be melanin by the finding of stage II and III melanosomes (premelanosomes) [9], and no neuromelanin was found. The pigmented cells tended to be spindle shaped, and generally had smaller nuclei than the large plumper tumor cells. Theoretically, the pigmented cells could be entrapped leptomeningeal melanocytes, proliferating in response to the astrocytic tumor. It was difficult to demonstrate positive reaction for GFAP in the pigmented cells by immunohistochemistry, but this may have been related to the intense pigmentation in most of the cells. A few pigmented cells were, however, positive for GFAP (Fig. 2F). Three of the four reported pigmented astrocytomas contained melanosomal melanin, and it was concluded that the pigment was present in neoplastic glia cells [19, 39, 41]. The pigmented cells were negative for HMB-45, which is a monoclonal antibody that detects a glycoconjugate present in immature melanosomes [20]. Negativity for HMB-45 was also found in the three earlier described pigmented astrocytomas with ultrastructurally documented premelanosomes [19, 39, 41]. One pigmented medulloblastoma has been reported to be negative for HMB-45 [3], whereas some of the pigmented cells were positive for HMB-45 in another case [40]. Pigmented schwannomas and the melanocytic lesions of the leptomeninges are most often positive for HMB-45 [24]. These findings indicate that HMB-45 should not be expected to be demonstrable by immunohistochemistry in pigmented gliomas even if melanosomal melanin is found ultrastructurally. We have here presented the fifth published example of a pigmented astrocytoma. This case provides further evidence that not only tumors derived from the neural crest, but also neuroepithelial tumors originating from cells derived from the primitive neural tube, may produce melanosomal melanin. The long postoperative survival indicates that pigmented PXA have a good prognosis. References 1. Arita K, Kurisu K, Tominaga A, Sugiyama K, Sumida M, Hirose T (2002) Intrasellar pleomorphic xanthoastrocytoma: case report. Neurosurgery 51: Barden H (1979) Acid fast staining of oxidized neuromelanin and lipofuscin in the human brain. J Neuropathol Exp Neurol 38: Baylac F, Martinoli A, Marie B, Bracard S, Marchal JC, Sommelet D, Hassoun J, Plenat F (1997) Une variete exceptionelle de medulloblastome: le medulloblastome melanotique. Ann Pathol 17: Best PV (1973) A medulloblastoma-like tumour with melanin formation. J Pathol 110: Boesel CP, Suhan JP (1979) A pigmented choroid plexus carcinoma: histochemical and ultrastructural studies. J Neuropathol Exp Neurol 38: Boesel CP, Suhan JP, Sayers MP (1978) Melanotic medulloblastoma. Report of a case with ultrastructural findings. J Neuropathol Exp Neurol 37: Burger PC, Scheithauer BW (1994) Atlas of tumor pathology. Tumors of the central nervous system. Armed Forces Institute of Pathology, Washington 8. Chan ACL, Ho LC, Yip WWL, Cheung FC (2003) Pigmented ependymoma with lipofuscin and neuromelanin production. Arch Pathol Lab Med 127: Dickersin GR (2000) Diagnostic electron microscopy. A text/ atlas, 2nd edn. Springer, New York Berlin Heidelberg 10. Dolman CL (1988) Melanotic medulloblastoma. Acta Neuropathol 76: Dooling EC, Chi JG, Gilles FH (1977) Melanotic neuroectodermal tumor of infancy: its histological similarities to fetal pineal gland. Cancer 39: Erdelyi E, VandenBerg SR, Raese J, Barchas JD, Rubinstein LJ, Herman MM (1981) Neural differentiation in the OTT6050 mouse teratoma: enzymatic and immunofluorescence characterization of a tumor fraction showing melanogenesis in neuroepithelial cells. Virchows Arch 393: Gibson JB, Burrows D, Weir WP (1957) Primary melanoma of the meninges. J Pathol Bacteriol 74: Heyerdahl Strøm E, Skullerud K (1983) Pleomorphic xanthoastrocytoma: report of 5 cases. Clin Neuropathol 2: Hirano A (1997) Neurons and astrocytes. In: Davis RL, Robertson DM (eds) Textbook of neuropathology, 3rd edn. Williams and Wilkins, Baltimore, pp Ironside JW, Moss TH, Louis DN, Lowe JS, Weller RO (2002) Diagnostic patology of nervous system tumours. Churchill Livingstone, Edinburgh 17. Jellinger K, Chou P, Paulus W (2000) Melanocytic lesions. In: Kleihues P, Cavenee WK (eds) World Health Organization classification of tumours. Pathology and genetics of tumours of the nervous system. IARC Press, Lyon, pp
6 Kalimo H, Haapasalo H (2000) Melanotic medulloblastoma. In: Kleihues P, Cavenee WK (eds) Pathology and genetics of tumours of the nervous system. IARC Press, Lyon, p Kanzawa T, Takahashi H, Hayano M, Mori S, Shimbo Y, Kitazawa T (1997) Melanotic cerebral astrocytoma: case report and literature review. Acta Neuropathol 93: Kapur RP, Bigler SA, Skelly M, Gown AM (1992) Anti-melanoma monoclonal antibody HMB45 identified an oncofetal glycoconjugate associated with immature melanosomes. J Histochem Cytochem 40: Kepes JJ (1982) Meningiomas: biology, pathology and differential diagnosis. Masson, New York 22. Kepes JJ, Rubinstein LJ, Eng LF (1979) Pleomorphic xanthoastrocytoma: a distinctive meningocerebral glioma of young subjects with a relatively favourable prognosis. Cancer 44: Kepes JJ, Louis DN, Giannini C, Paulus W (2000) Pleomorphic xanthoastrocytoma. In: Kleinhues P, Cavenee WK (eds) World Health Organization classification of tumours. Pathology and genetics of tumours of the nervous system. IARC Press, Lyon, pp Kleihues P, Cavenee WK (eds) (2000) World Health Organization classification of tumours. Pathology and genetics of tumours of the nervous system. IARC Press, Lyon 25. Kleihues P, Burger PC, Scheithauer BW (1993) World Health Organization International Classification of tumours. Histological typing of tumours of the central nervous system, 2nd edn. Springer, Berlin Heidelberg New York 26. Kros JM, Vecht CJ, Stefanko SZ (1991) The pleomorphic xanthoastrocytoma and its differential diagnosis: A study of five cases. Hum Pathol 22: Lana-Peixoto MA, Lagos J, Silbert SW (1977) Primary pigmented carcinoma of the choroid plexus. A light and electron microscopic study. J Neurosurg 47: McCloskey JJ, Parker JC Jr, Brooks WH, Blacker HM (1976) Melanin as a component of cerebral gliomas: the melanotic cerebral ependymoma. Cancer 37: Mund ML, Rodrigues MM (1979) Embryology of the human retinal pigment epithelium. In: Zinn KM, Marmor MF (eds) The retinal pigment epithelium. Harvard University Press, Cambridge, pp Ng TH, Wong AY, Boadle R, Compton JS (1999) Pigmented central neurocytoma. Am J Surg Pathol 23: Ogata A, Fujioka Y, Nagashima K, Tashiro K, Aida T, Abe H (1989) Malignant melanotic neuroectodermal tumor arising from the pineal body. Acta Neuropathol 77: Raisanen J, Vogel H, Horoupian DS (1990) Primitive pineal tumor with retinoblastomatous and retinal/ciliary epithelial differentiation: an immunohistochemical study. J Neurooncol 9: Reimund EL, Sitton JE, Harkin JC (1990) Pigmented choroid plexus papilloma. Arch Pathol Lab Med 114: Rosenblum MK, Erlandson RA, Aleksic SN, Budzilovich GN (1990) Melanotic ependymoma and subependymoma. Am J Surg Pathol 14: Schmidbauer M, Budka H, Pilz P (1989) Neuroepithelial and ectomesenchymal differentiation in a primitive pineal tumor ( pineal anlage tumor ). Clin Neuropathol 8:7 10 Seiji M, Fitzpatrick TB, Birbeck MSC (1961) The melanosome: a distinctive subcellular particle of mammalian melanocytes and the site of melanogenesis. J Invest Dermatol 36:243 Sharma MC, Gaikwad S, Mahapatra AK, Jain AK, Sarkar C (1998) Pigmented medulloepithelioma: case report and review of literature. Childs Nerv Syst 14:74 78 Sharma MC, Sarkar C, Gaikwad S, Sharma C, Singh VP (1999) Choroid plexus papilloma: a clinicopathological study of 23 cases. Surg Neurol 52:37 39 Sharma MC, Arora R, Khanna N, Singh VP, Sarkar C (2001) Pigmented pleomorphic xanthoastrocytoma. Report of a rare case with review of the literature. Arch Pathol Lab Med 125: Sharma MC, Agarwal M, Suri A, Gaikwad S, Mukhopadhyay P, Sarkar C (2002) A melanotic desmoplastic medulloblastoma: report of a rare case and review of the literature. Brain Tumor Pathol 19:93 96 Soffer D, Lach B, Constantini S (1992) Melanotic cerebral ganglioglioma: evidence for melanogenesis in neoplastic astrocytes. Acta Neuropathol 83: Torp SH, Granli US (2001) Proliferative activity in human glioblastomas assessed by various techniques. APMIS 109: Vajtai I, Yonekawa Y, Scha uble B, Paulus W (1996) Melanotic astrocytoma. Acta Neuropathol 91: Van den Berg SR, Hess JR, Herman MM, DeArmond SJ, Halks-Miller M, Rubinstein LJ (1981) Neural differentiation in the OTT-6050 mouse teratoma. Virchows Arch 392: Watanabe K, Ando Y, Iwanaga H, Ochiai C, Nagai M, Okada K, Watanabe N (1995) Choroid plexus papilloma containing melanin pigment. Clin Neuropathol 14: Woodruff JM, Kourea HP, Louis DN, Scheithauer BW (2000) Schwannoma. In: Kleihues P, Cavenee WK (eds) World Health Organization classification of tumours. Pathology and genetics of tumours of the nervous system. IARC Press, Lyon, pp
monotonous, stippled, round, smoothcontoured nuclei and scanty acidophilic or
 monotonous, stippled, round, smoothcontoured nuclei and scanty acidophilic or vacuolated cytoplasm. The cells are surrounded by a loose fibrillary stroma that is traversed by delicate capillaries. Ill
monotonous, stippled, round, smoothcontoured nuclei and scanty acidophilic or vacuolated cytoplasm. The cells are surrounded by a loose fibrillary stroma that is traversed by delicate capillaries. Ill
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad
 Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Hemosiderin pigmentation of tumour cells in cerebellar pilocytic astrocytoma associated with post-traumatic hemorrhage in adults
 Case report Hemosiderin pigmentation of tumour cells in cerebellar pilocytic astrocytoma associated with post-traumatic hemorrhage in adults Anna Taraszewska 1, Zbigniew Czernicki 2, Jaros³aw Andrychowski
Case report Hemosiderin pigmentation of tumour cells in cerebellar pilocytic astrocytoma associated with post-traumatic hemorrhage in adults Anna Taraszewska 1, Zbigniew Czernicki 2, Jaros³aw Andrychowski
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
Pleomorphic Xanthoastrocytoma
 Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
MR Imaging of Pial Melanosis Secondary to a Posterior Fossa Melanotic Ependymoma
 AJNR Am J Neuroradiol 26:804 808, April 2005 Case Report MR Imaging of Pial Melanosis Secondary to a Posterior Fossa Melanotic Ependymoma Sait Albayram, Efsun Urger, Buge Oz, Ali Kafadar, Civan Islak,
AJNR Am J Neuroradiol 26:804 808, April 2005 Case Report MR Imaging of Pial Melanosis Secondary to a Posterior Fossa Melanotic Ependymoma Sait Albayram, Efsun Urger, Buge Oz, Ali Kafadar, Civan Islak,
Histopathological Study and Categorisation of Brain Tumors
 Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Pathologic Analysis of CNS Surgical Specimens
 2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
Neurocytoma a Rare Intraventricular Tumor
 Neurocytoma a Rare Intraventricular Tumor J. A. Mallick,S. A. Ali ( Department of Oncology, Liaquat National Postgraduate Medical Centre, Karachi. ) Introduction Central neurocytoma was first recognized
Neurocytoma a Rare Intraventricular Tumor J. A. Mallick,S. A. Ali ( Department of Oncology, Liaquat National Postgraduate Medical Centre, Karachi. ) Introduction Central neurocytoma was first recognized
Anna Maria Buccoliero Department of Biomedicine, Careggi Hospital Florence
 PEDIATRIC RHABDOID MENINGIOMA Anna Maria Buccoliero Department of Biomedicine, Careggi Hospital Florence CLINICAL HISTORY A 3-year-old boy, with a recent history of seizures, was admitted to the Neurosurgery
PEDIATRIC RHABDOID MENINGIOMA Anna Maria Buccoliero Department of Biomedicine, Careggi Hospital Florence CLINICAL HISTORY A 3-year-old boy, with a recent history of seizures, was admitted to the Neurosurgery
Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS
 Multiple Primary and Histology Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS 1 Prerequisites 2 Completion of Multiple Primary and Histology General Coding Rules 3 There are many ways
Multiple Primary and Histology Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS 1 Prerequisites 2 Completion of Multiple Primary and Histology General Coding Rules 3 There are many ways
American Journal of. Medical Case Reports. CAM5.2 Expression in Metastatic Tumours of CNS: A Diagnostic Tool
 American Journal of American Journals of Medical Case Reports http://ivyunion.org/index.php/ajmcr/index Medical Case Reports Mathur SK et al. American Journal of Medical Case Reports 2014, 2:1-8 Vol 2,
American Journal of American Journals of Medical Case Reports http://ivyunion.org/index.php/ajmcr/index Medical Case Reports Mathur SK et al. American Journal of Medical Case Reports 2014, 2:1-8 Vol 2,
Intramedullary melanocytoma of thoracic spine: A rare case report
 1 di 12 16/07/2014 11.16 Asian J Neurosurg. 2014 Jan-Mar; 9(1): 36 39. doi: 10.4103/1793-5482.131068 PMCID: PMC4038865 Intramedullary melanocytoma of thoracic spine: A rare case report 1 Pranav Dorwal,
1 di 12 16/07/2014 11.16 Asian J Neurosurg. 2014 Jan-Mar; 9(1): 36 39. doi: 10.4103/1793-5482.131068 PMCID: PMC4038865 Intramedullary melanocytoma of thoracic spine: A rare case report 1 Pranav Dorwal,
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
Five Most Common Problems in Surgical Neuropathology
 Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Gangliogliomas: A Report of Five Cases
 Case Report Gangliogliomas: A Report of Five Cases Nair V, Suri VS, Tatke M, Saran RK, Malhotra V, Singh D* Departments of Pathology and *Neurosurgery, G. B. Pant Hospital, New Delhi, India. Correspondence
Case Report Gangliogliomas: A Report of Five Cases Nair V, Suri VS, Tatke M, Saran RK, Malhotra V, Singh D* Departments of Pathology and *Neurosurgery, G. B. Pant Hospital, New Delhi, India. Correspondence
A case of multinodular high-grade neuroepithelial tumor
 Brain Tumor Pathol (2011) 28:253 257 DOI 10.1007/s10014-011-0032-6 CASE REPORT A case of multinodular high-grade neuroepithelial tumor with ependymal differentiation Kensaku Kamada Yuko Tanaka Takayuki
Brain Tumor Pathol (2011) 28:253 257 DOI 10.1007/s10014-011-0032-6 CASE REPORT A case of multinodular high-grade neuroepithelial tumor with ependymal differentiation Kensaku Kamada Yuko Tanaka Takayuki
Brain Tumors. Medulloblastoma. Pilocytic astrocytoma: Ahmed Koriesh, MD. Pathological finding
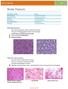 NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
Astroblastoma : A Case Report
 J Korean Med Sci 2004; 19: 772-6 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Astroblastoma : A Case Report Astroblastoma is one of the very unusual type of tumors, whose histogenesis
J Korean Med Sci 2004; 19: 772-6 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Astroblastoma : A Case Report Astroblastoma is one of the very unusual type of tumors, whose histogenesis
Tumors of the Central Nervous System
 Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Pleomorphic Xanthoastrocytoma
 Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 Overview Pleomorphic xanthoastrocytoma (PXA) is an uncommon
Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 Overview Pleomorphic xanthoastrocytoma (PXA) is an uncommon
CHINESE MEDICAL ASSOCIATION
 Zhu et al. Chinese Neurosurgical Journal (2017) 3:22 DOI 10.1186/s41016-017-0087-2 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Anaplastic pleomorphic xanthoastrocytoma with disseminated
Zhu et al. Chinese Neurosurgical Journal (2017) 3:22 DOI 10.1186/s41016-017-0087-2 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Anaplastic pleomorphic xanthoastrocytoma with disseminated
Special slide seminar
 Special slide seminar Tomáš Rozkoš The Fingerland Department of Pathology Charles University Medical Faculty and Faculty Hospital in Hradec Králové Czech Republic Case history, 33 years old resistance
Special slide seminar Tomáš Rozkoš The Fingerland Department of Pathology Charles University Medical Faculty and Faculty Hospital in Hradec Králové Czech Republic Case history, 33 years old resistance
Decreased Vision and Junctional Scotoma from Pituicytoma
 Decreased Vision and Junctional Scotoma from Pituicytoma The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published
Decreased Vision and Junctional Scotoma from Pituicytoma The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published
SPECIAL SLIDE SEMINAR CASE 3
 SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
Rapid recurrence of a malignant meningioma: case report
 Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
HAEMANGIOBLASTOMA CASE REPORT
 HAEMANGIOBLASTOMA Pages with reference to book, From 113 To 115 Saleem Sadiq, K.C. Kyriacou ( Department of Pathology, College of Medicine, King Saud University, Riyadh, Saudi Arabia. ) Z.B. Jamjoom (
HAEMANGIOBLASTOMA Pages with reference to book, From 113 To 115 Saleem Sadiq, K.C. Kyriacou ( Department of Pathology, College of Medicine, King Saud University, Riyadh, Saudi Arabia. ) Z.B. Jamjoom (
I have no conflicts of interest in relation to this presentation. Vogel FS & Burger PC 3/28/2016
 IF THIS IS NOT GLIOBLASTOMA, THEN WHAT IS IT? Murat Gokden, MD Department of Pathology/Neuropathology University of Arkansas for Medical Sciences Little Rock, AR mgokden@uams.edu I have no conflicts of
IF THIS IS NOT GLIOBLASTOMA, THEN WHAT IS IT? Murat Gokden, MD Department of Pathology/Neuropathology University of Arkansas for Medical Sciences Little Rock, AR mgokden@uams.edu I have no conflicts of
AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017
 AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017 SYLLABUS Papillary Tumor of the Pineal Region and the Differential
AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017 SYLLABUS Papillary Tumor of the Pineal Region and the Differential
Classification of spontaneous brain tumors in rats
 Classification of spontaneous brain tumors in rats Central Nervous System Neoplasms in the Rat (Solleveld HA, et al., 1991) 1. Tumors of Neuroepithelial Tissue A. Astrocytic and oligodendroglial tumors
Classification of spontaneous brain tumors in rats Central Nervous System Neoplasms in the Rat (Solleveld HA, et al., 1991) 1. Tumors of Neuroepithelial Tissue A. Astrocytic and oligodendroglial tumors
Case #3. USCAP Neuropathology Evening Seminar/Companion Meeting
 Case #3 USCAP Neuropathology Evening Seminar/Companion Meeting Clinical History A 71-year year-old man presented with a 4-4 week history of word finding difficulty. An initial screening head CT followed
Case #3 USCAP Neuropathology Evening Seminar/Companion Meeting Clinical History A 71-year year-old man presented with a 4-4 week history of word finding difficulty. An initial screening head CT followed
Case Report Xanthomatous meningioma: a case report with review of the literature
 Int J Clin Exp Pathol 2013;6(10):2242-2246 www.ijcep.com /ISSN:1936-2625/IJCEP1308033 Case Report Xanthomatous meningioma: a case report with review of the literature Mitsuaki Ishida 1, Tadateru Fukami
Int J Clin Exp Pathol 2013;6(10):2242-2246 www.ijcep.com /ISSN:1936-2625/IJCEP1308033 Case Report Xanthomatous meningioma: a case report with review of the literature Mitsuaki Ishida 1, Tadateru Fukami
Supra- and infratentorial brain tumors from childhood to maternity
 Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Imaging of Normal Leptomeningeal Melanin
 Imaging of Normal Leptomeningeal Melanin Stephen S. Gebarski and Mila A. Blaivas PURPOSE: To find the CT and MR characteristics of normal leptomeningeal melanin, which can be macroscopically visible at
Imaging of Normal Leptomeningeal Melanin Stephen S. Gebarski and Mila A. Blaivas PURPOSE: To find the CT and MR characteristics of normal leptomeningeal melanin, which can be macroscopically visible at
Cerebral Parenchymal Lesions: I. Metastatic Neoplasms
 Chapter 4 Cerebral Parenchymal Lesions: I. Metastatic Neoplasms After one has reasonably ruled out the possibility of a nonneoplastic diagnosis (see Chap. 3), one is left with considering a diagnosis of
Chapter 4 Cerebral Parenchymal Lesions: I. Metastatic Neoplasms After one has reasonably ruled out the possibility of a nonneoplastic diagnosis (see Chap. 3), one is left with considering a diagnosis of
Case Report Spinal pleomorphic xanthoastrocytoma companied with periventricular tumor
 Int J Clin Exp Pathol 2015;8(1):1036-1040 www.ijcep.com /ISSN:1936-2625/IJCEP0003595 Case Report Spinal pleomorphic xanthoastrocytoma companied with periventricular tumor Xintong Zhao 1, Xiaochun Jiang
Int J Clin Exp Pathol 2015;8(1):1036-1040 www.ijcep.com /ISSN:1936-2625/IJCEP0003595 Case Report Spinal pleomorphic xanthoastrocytoma companied with periventricular tumor Xintong Zhao 1, Xiaochun Jiang
Case Report A case report on intermediate-grade malignant meningeal melanocytoma with elevated cell proliferation index
 Int J Clin Exp Pathol 2015;8(9):11698-11703 www.ijcep.com /ISSN:1936-2625/IJCEP0012900 Case Report A case report on intermediate-grade malignant meningeal melanocytoma with elevated cell proliferation
Int J Clin Exp Pathol 2015;8(9):11698-11703 www.ijcep.com /ISSN:1936-2625/IJCEP0012900 Case Report A case report on intermediate-grade malignant meningeal melanocytoma with elevated cell proliferation
Characterization of morphologically benign biologically aggressive meningiomas
 Characterization of morphologically benign biologically aggressive meningiomas Original Article Shalinee Rao, N. Sadiya, Saraswathi Doraiswami, D. Prathiba Department of Pathology, Sri Ramachandra Medical
Characterization of morphologically benign biologically aggressive meningiomas Original Article Shalinee Rao, N. Sadiya, Saraswathi Doraiswami, D. Prathiba Department of Pathology, Sri Ramachandra Medical
Supratentorial Gangliocytoma Mimicking Extra-axial Tumor: A Report of Two Cases
 Supratentorial Gangliocytoma Mimicking Extra-axial Tumor: A Report of Two Cases Ho Sung Kim, MD 1 Ho Kyu Lee, MD 1 Ae Kyung Jeong, MD 1 Ji Hoon Shin, MD 1 Choong Gon Choi, MD 1 Shin Kwang Khang, MD 2 We
Supratentorial Gangliocytoma Mimicking Extra-axial Tumor: A Report of Two Cases Ho Sung Kim, MD 1 Ho Kyu Lee, MD 1 Ae Kyung Jeong, MD 1 Ji Hoon Shin, MD 1 Choong Gon Choi, MD 1 Shin Kwang Khang, MD 2 We
Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child
 Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
Diplomate of the American Board of Pathology in Anatomic and Clinical Pathology
 A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
Immunohistochemical Staining for Claudin-1 Can Help Distinguish Meningiomas From Histologic Mimics
 Anatomic Pathology / CLAUDIN-1 IN MENINGIOMAS Immunohistochemical Staining for Claudin-1 Can Help Distinguish Meningiomas From Histologic Mimics Hejin P. Hahn, MD, PhD, Elizabeth A. Bundock, MD, PhD, and
Anatomic Pathology / CLAUDIN-1 IN MENINGIOMAS Immunohistochemical Staining for Claudin-1 Can Help Distinguish Meningiomas From Histologic Mimics Hejin P. Hahn, MD, PhD, Elizabeth A. Bundock, MD, PhD, and
Histological pattern of central nervous system neoplasms
 ecommons@aku Department of Pathology and Laboratory Medicine Medical College, Pakistan April 2001 Histological pattern of central nervous system neoplasms Z. Ahmed Aga Khan University S. Muzaffar Aga Khan
ecommons@aku Department of Pathology and Laboratory Medicine Medical College, Pakistan April 2001 Histological pattern of central nervous system neoplasms Z. Ahmed Aga Khan University S. Muzaffar Aga Khan
Understanding general brain tumor pathology, Part I: The basics. Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky
 Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Advances In Orbital Neuropathology
 Advances In Orbital Neuropathology Charles G. Eberhart, MD PhD Associate Professor of Pathology, Ophthalmology and Oncology Johns Hopkins University School of Medicine Overview Non-neoplastic lesions Microphthalmos/pseudoglioma
Advances In Orbital Neuropathology Charles G. Eberhart, MD PhD Associate Professor of Pathology, Ophthalmology and Oncology Johns Hopkins University School of Medicine Overview Non-neoplastic lesions Microphthalmos/pseudoglioma
Financial disclosures
 Mesenchymal Neoplasms with Melanocytic Differentiation By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchcock Medical Center Geisel
Mesenchymal Neoplasms with Melanocytic Differentiation By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchcock Medical Center Geisel
Rhabdoid Meningioma In A Background Of Atypical Meningioma With Lipomatous Metaplasia: Case Report And Review Of Literature
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Rhabdoid Meningioma In A Background Of Atypical Meningioma With Lipomatous Metaplasia: Case Report And Review Of Literature S Shuja, T Lucey,
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Rhabdoid Meningioma In A Background Of Atypical Meningioma With Lipomatous Metaplasia: Case Report And Review Of Literature S Shuja, T Lucey,
No financial or other disclosures
 Case 2014-5 Esther N. Bit-Ivan, DO Northwestern University Jason Wang, MD Jason Park, MD Korgun Koral, MD Children s Medical Center Charles Timmons, MD Veena Rajaram, MD No financial or other disclosures
Case 2014-5 Esther N. Bit-Ivan, DO Northwestern University Jason Wang, MD Jason Park, MD Korgun Koral, MD Children s Medical Center Charles Timmons, MD Veena Rajaram, MD No financial or other disclosures
Desmoplastic Melanoma R/O BCC. Clinical Information. 74 y.o. man with lesion on left side of neck r/o BCC
 R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
USCAP Neuropathology. Case No. 3 Elisabeth J. Rushing, MD Armed Forces Institute of Pathology Washington, DC
 USCAP Neuropathology Case No. 3 Elisabeth J. Rushing, MD Armed Forces Institute of Pathology Washington, DC Clinical history The patient is a 9 year-old boy who has had seizures since age 2, at which time
USCAP Neuropathology Case No. 3 Elisabeth J. Rushing, MD Armed Forces Institute of Pathology Washington, DC Clinical history The patient is a 9 year-old boy who has had seizures since age 2, at which time
Non-hematogenous endogenous pigments
 Non-hematogenous endogenous pigments 0 This group contains the following : 1. Melanins. 2. Lipofuscins. 3. Chromaffin. 4. Pseudomelanosis. 5. Dubin-Johnson pigments. 6. Ceroid-type lipofuscins. 7. Hamazaki-Weisenberg
Non-hematogenous endogenous pigments 0 This group contains the following : 1. Melanins. 2. Lipofuscins. 3. Chromaffin. 4. Pseudomelanosis. 5. Dubin-Johnson pigments. 6. Ceroid-type lipofuscins. 7. Hamazaki-Weisenberg
Frontal intraparenchymal schwannoma: a case report
 Case Report Medical Journal of the Islamic Republic of Iran.Vol. 23, No. 2, August, 2009. pp. 112-116 Frontal intraparenchymal schwannoma: a case report Mansour Parvaresh-Rizi 1,MD., Seyed Ebrahim Hejazian
Case Report Medical Journal of the Islamic Republic of Iran.Vol. 23, No. 2, August, 2009. pp. 112-116 Frontal intraparenchymal schwannoma: a case report Mansour Parvaresh-Rizi 1,MD., Seyed Ebrahim Hejazian
2017 Diagnostic Slide Session Case 3
 2017 Diagnostic Slide Session Case 3 Andrew Gao, MD Lili-Naz Hazrati, MD, PhD Cynthia Hawkins, MD, PhD Hospital for Sick Children and University of Toronto, Toronto, Canada Disclosures: none Clinical History
2017 Diagnostic Slide Session Case 3 Andrew Gao, MD Lili-Naz Hazrati, MD, PhD Cynthia Hawkins, MD, PhD Hospital for Sick Children and University of Toronto, Toronto, Canada Disclosures: none Clinical History
Intramedullary Clear Cell Ependymoma in the Thoracic Spinal Cord: A Case with Its Crush Smear and Ultrastructural Findings
 J Korean Med Sci 2007; 22 (Suppl): S149-53 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Intramedullary Clear Cell Ependymoma in the Thoracic Spinal Cord: A Case with Its Crush Smear
J Korean Med Sci 2007; 22 (Suppl): S149-53 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Intramedullary Clear Cell Ependymoma in the Thoracic Spinal Cord: A Case with Its Crush Smear
1/10/2018. Soft Tissue Tumors Showing Melanocytic Differentiation. Overview. Desmoplastic/ Spindle Cell Melanoma
 2016 MFMER slide-1 2016 MFMER slide-2 2016 MFMER slide-3 Soft Tissue Tumors Showing Melanocytic Differentiation Andrew L. Folpe, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic, Rochester,
2016 MFMER slide-1 2016 MFMER slide-2 2016 MFMER slide-3 Soft Tissue Tumors Showing Melanocytic Differentiation Andrew L. Folpe, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic, Rochester,
number Done by Corrected by Doctor Maha Shomaf
 number 16 Done by Waseem Abo-Obeida Corrected by Zeina Assaf Doctor Maha Shomaf MALIGNANT NEOPLASMS The four fundamental features by which benign and malignant tumors can be distinguished are: 1- differentiation
number 16 Done by Waseem Abo-Obeida Corrected by Zeina Assaf Doctor Maha Shomaf MALIGNANT NEOPLASMS The four fundamental features by which benign and malignant tumors can be distinguished are: 1- differentiation
Case Presentation. Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD. Department of Pathology Jordan University Hospital Amman, Jordan
 Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
Schedule of Accreditation issued by United Kingdom Accreditation Service 2 Pine Trees, Chertsey Lane, Staines-upon-Thames, TW18 3HR, UK
 Schedule of Accreditation 2 Pine Trees, Chertsey Lane, Staines-upon-Thames, TW18 3HR, UK Department of Eye Pathology 1 st Floor, Cayton Street Building UCL Institute of Ophthalmology 11-43 Bath Street
Schedule of Accreditation 2 Pine Trees, Chertsey Lane, Staines-upon-Thames, TW18 3HR, UK Department of Eye Pathology 1 st Floor, Cayton Street Building UCL Institute of Ophthalmology 11-43 Bath Street
Among the benign intraepithelial melanocytic proliferations, Inflamed Conjunctival Nevi. Histopathological Criteria. Resident Short Reviews
 Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Symtomatic Subependymoma Of The Lateral Ventricle: A Rare Entity A Case report and review of literature
 ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Symtomatic Subependymoma Of The Lateral Ventricle: A Rare Entity A Case report and review of M Sharma, V Velho, P Ghodgaonkar, D Palande
ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Symtomatic Subependymoma Of The Lateral Ventricle: A Rare Entity A Case report and review of M Sharma, V Velho, P Ghodgaonkar, D Palande
2018 Diagnostic Slide Session Case #8
 2018 Diagnostic Slide Session Case #8 Angela N. Viaene, MacLean P. Nasrallah, and Zissimos Mourelatos Hospital of the University of Pennsylvania AANP June 9, 2018 Disclosures: none Clinical History Healthy,
2018 Diagnostic Slide Session Case #8 Angela N. Viaene, MacLean P. Nasrallah, and Zissimos Mourelatos Hospital of the University of Pennsylvania AANP June 9, 2018 Disclosures: none Clinical History Healthy,
Neuropathology Evening Session: Case 3
 Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT
 Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT Two different neoplasia in the same biopsy material called
Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT Two different neoplasia in the same biopsy material called
In 2005, Wang and coworkers 1 described a report of 8
 Angiocentric Glioma A Clinicopathologic Review of 5 Tumors With Identification of Associated Cortical Dysplasia Trent Marburger, MD; Richard Prayson, MD N Context. Angiocentric glioma is a rare, epilepsy-associated,
Angiocentric Glioma A Clinicopathologic Review of 5 Tumors With Identification of Associated Cortical Dysplasia Trent Marburger, MD; Richard Prayson, MD N Context. Angiocentric glioma is a rare, epilepsy-associated,
2. Subependymal giant cell astrocytoma:
 I. Astrocytomas: A. Diffusely infiltrating ( astrocytoma, anaplastic astrocytoma, GBM) B. Localised (pilocytic astrocytoma, pleomorphic xanthoastrocytoma, SGCA) *Grading: Diffuse: 1. Astrocytoma WHO grade
I. Astrocytomas: A. Diffusely infiltrating ( astrocytoma, anaplastic astrocytoma, GBM) B. Localised (pilocytic astrocytoma, pleomorphic xanthoastrocytoma, SGCA) *Grading: Diffuse: 1. Astrocytoma WHO grade
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
Patients Treated with Leksell Gamma Knife
 Patients Treated with Leksell Gamma Knife 1968-2016 TREATMENTS REPORTED 2016 BY REGION AND INDICATION INDICATION Asia excl. Europe Latin Middle East & Africa North Grand Total Benign Tumors 12283 9778
Patients Treated with Leksell Gamma Knife 1968-2016 TREATMENTS REPORTED 2016 BY REGION AND INDICATION INDICATION Asia excl. Europe Latin Middle East & Africa North Grand Total Benign Tumors 12283 9778
Histopathology: skin pathology
 Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
Interesting Case Series. Desmoplastic Melanoma
 Interesting Case Series Desmoplastic Melanoma Anthony Maurice Kordahi, MD, Joshua B. Elston, MD, Ellen M. Robertson, MD, and C. Wayne Cruse, MD Division of Plastic Surgery, Department of Surgery, University
Interesting Case Series Desmoplastic Melanoma Anthony Maurice Kordahi, MD, Joshua B. Elston, MD, Ellen M. Robertson, MD, and C. Wayne Cruse, MD Division of Plastic Surgery, Department of Surgery, University
Disclosures. The Thin Red Line Between Neuropathology and Head & Neck Pathology. Introduction CASE 1. Current Issues Tihan
 Disclosures I have nothing to disclose The Thin Red Line Between Neuropathology and Head & Neck Pathology Tarik Tihan, MD, PhD UCSF, Department of Pathology Neuropathology Division Introduction Three cases
Disclosures I have nothing to disclose The Thin Red Line Between Neuropathology and Head & Neck Pathology Tarik Tihan, MD, PhD UCSF, Department of Pathology Neuropathology Division Introduction Three cases
University Journal of Pre and Para Clinical Sciences
 ISSN 2455 2879 Volume 2 Issue 1 2016 Metaplastic carcinoma breast a rare case report Abstract : Metaplastic carcinoma of the breast is a rare malignancy with two distinct cell lines described as a breast
ISSN 2455 2879 Volume 2 Issue 1 2016 Metaplastic carcinoma breast a rare case report Abstract : Metaplastic carcinoma of the breast is a rare malignancy with two distinct cell lines described as a breast
Multicompartmental congenital intracranial immature teratoma
 Neurology Asia 2013; 18(1) : 117 121 Multicompartmental congenital intracranial immature teratoma 1 Dharmendra Ganesan MS FRCS(SN), 1 Sheau Fung Sia MS MRCS, 1 Vairavan Narayanan MS, 2 Gnana Kumar FRCR,
Neurology Asia 2013; 18(1) : 117 121 Multicompartmental congenital intracranial immature teratoma 1 Dharmendra Ganesan MS FRCS(SN), 1 Sheau Fung Sia MS MRCS, 1 Vairavan Narayanan MS, 2 Gnana Kumar FRCR,
From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma
 From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma Marcus C de Jong, Annette C Moll, Sophia Göricke, Paul van der Valk, Wijnanda A Kors, Jonas A
From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma Marcus C de Jong, Annette C Moll, Sophia Göricke, Paul van der Valk, Wijnanda A Kors, Jonas A
OMICS PUBLISHING GROUP/Clinical Meningioma with remarkable multiple rosette formation: A diagnostically difficult case
 OMICS PUBLISHING GROUP/Clinical Meningioma with remarkable multiple rosette formation: A diagnostically difficult case --Manuscript Draft-- Manuscript Number: Full Title: Short Title: Article Type: Section/Category:
OMICS PUBLISHING GROUP/Clinical Meningioma with remarkable multiple rosette formation: A diagnostically difficult case --Manuscript Draft-- Manuscript Number: Full Title: Short Title: Article Type: Section/Category:
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
In 1988 Dumas-Duport et al. first used
 Copyright 2009, Barrow Neurological Institute Dysembryoplastic Neuroepithelial Tumor: A Review Mark Garrett, MD Jennifer Eschbacher, MD Peter Nakaji, MD Most DNETs are benign, low-grade lesions. However,
Copyright 2009, Barrow Neurological Institute Dysembryoplastic Neuroepithelial Tumor: A Review Mark Garrett, MD Jennifer Eschbacher, MD Peter Nakaji, MD Most DNETs are benign, low-grade lesions. However,
Division of Pathology
 Case 38 Adult woman with a 35mm right breast lump at the 10 o clock position. Excision performed. (Case contributed by Dr Mihir Gudi, KKH) Division of Pathology Merlion, One Fullerton Singapore Diagnosis
Case 38 Adult woman with a 35mm right breast lump at the 10 o clock position. Excision performed. (Case contributed by Dr Mihir Gudi, KKH) Division of Pathology Merlion, One Fullerton Singapore Diagnosis
Neoplasia 2018 Lecture 2. Dr Heyam Awad MD, FRCPath
 Neoplasia 2018 Lecture 2 Dr Heyam Awad MD, FRCPath ILOS 1. List the differences between benign and malignant tumors. 2. Recognize the histological features of malignancy. 3. Define dysplasia and understand
Neoplasia 2018 Lecture 2 Dr Heyam Awad MD, FRCPath ILOS 1. List the differences between benign and malignant tumors. 2. Recognize the histological features of malignancy. 3. Define dysplasia and understand
Meningiomas account for approximately 4% of all
 Intraorbital Meningiomas A Pathologic Review Using Current World Health Organization Criteria Deepali Jain, MD; Katayoon B. Ebrahimi, MD; Neil R. Miller, MD; Charles G. Eberhart, MD, PhD N Context. Meningiomas
Intraorbital Meningiomas A Pathologic Review Using Current World Health Organization Criteria Deepali Jain, MD; Katayoon B. Ebrahimi, MD; Neil R. Miller, MD; Charles G. Eberhart, MD, PhD N Context. Meningiomas
Ocular Neoplasia CL Davis 9/08. Richard R Dubielzig
 Ocular Neoplasia CL Davis 9/08 Richard R Dubielzig 2135/5722 Canine Melanocytic Tumors Outside the Globe: 264 Conjunctival: 159 Eye Lid: 72 Skin: 33 Affecting the Globe: 1871 Anterior Uveal Melanocytoma:
Ocular Neoplasia CL Davis 9/08 Richard R Dubielzig 2135/5722 Canine Melanocytic Tumors Outside the Globe: 264 Conjunctival: 159 Eye Lid: 72 Skin: 33 Affecting the Globe: 1871 Anterior Uveal Melanocytoma:
The recently updated World Health Organization (WHO)
 REVIEW ARTICLE The Expanding Family of Glioneuronal Tumors Daniela S. Allende, MD and Richard A. Prayson, MD Abstract: Three new entities have been recently added to the group of glioneuronal tumors in
REVIEW ARTICLE The Expanding Family of Glioneuronal Tumors Daniela S. Allende, MD and Richard A. Prayson, MD Abstract: Three new entities have been recently added to the group of glioneuronal tumors in
SUPPLEMENTARY INFORMATION
 VOLUME: 1 ARTICLE NUMBER: 0027 In the format provided by the authors and unedited. Rapid intraoperative histology of unprocessed surgical specimens via fibre-laser-based stimulated Raman scattering microscopy
VOLUME: 1 ARTICLE NUMBER: 0027 In the format provided by the authors and unedited. Rapid intraoperative histology of unprocessed surgical specimens via fibre-laser-based stimulated Raman scattering microscopy
CASE REPORT Malignant transformation of breast ductal adenoma: a diagnostic pitfall
 Malaysian J Pathol 2015; 37(3) : 281 285 CASE REPORT Malignant transformation of breast ductal adenoma: a diagnostic pitfall Hiroko HAYASHI, Hiroshi OHTANI,* Junzo YAMAGUCHI,** and Isao SHIMOKAWA Department
Malaysian J Pathol 2015; 37(3) : 281 285 CASE REPORT Malignant transformation of breast ductal adenoma: a diagnostic pitfall Hiroko HAYASHI, Hiroshi OHTANI,* Junzo YAMAGUCHI,** and Isao SHIMOKAWA Department
Case 1. Maysa Al-Hussaini MD FRCPath
 Case 1 Maysa Al-Hussaini MD FRCPath MAYSA King AL-HUSSAINI Hussein Cancer MD Center MRCPATH KING HUSSEIN Amman CANCER Jordan CENTER Clinical history 4 year old boy History of frontal headache, sleepiness.
Case 1 Maysa Al-Hussaini MD FRCPath MAYSA King AL-HUSSAINI Hussein Cancer MD Center MRCPATH KING HUSSEIN Amman CANCER Jordan CENTER Clinical history 4 year old boy History of frontal headache, sleepiness.
Pituitary Gland (Hypophysis)
 Endocrine Organs Pituitary Gland (Hypophysis) Function o Production of hormones Location o Connected to the hypothalamus via an infundibulum situated within the sella turcica of the sphenoid bone Structure
Endocrine Organs Pituitary Gland (Hypophysis) Function o Production of hormones Location o Connected to the hypothalamus via an infundibulum situated within the sella turcica of the sphenoid bone Structure
FORELIMB SWEAT GLAND ADENOCARCINOMA IN A CAT
 I: 2047-2051 ISSN: 2277 4998 FORELIMB SWEAT GLAND ADENOCARCINOMA IN A CAT ABEDI G 1, HESARAKI S 2, ASGHARI A 1* 1: Department of Clinical Science, Science and Research branch, Islamic Azad University,
I: 2047-2051 ISSN: 2277 4998 FORELIMB SWEAT GLAND ADENOCARCINOMA IN A CAT ABEDI G 1, HESARAKI S 2, ASGHARI A 1* 1: Department of Clinical Science, Science and Research branch, Islamic Azad University,
Recurrence of astrocytoma of optic nerve after 48 years
 Brit. J. Ophthal. (1976) 6o, 539 Recurrence of astrocytoma of optic nerve after 48 years JOAN MULLANEY, J. WALSH, W. R. LEE, AND J. H. ADAMS From the National Ophthalmic Pathology Laboratory of Ireland,
Brit. J. Ophthal. (1976) 6o, 539 Recurrence of astrocytoma of optic nerve after 48 years JOAN MULLANEY, J. WALSH, W. R. LEE, AND J. H. ADAMS From the National Ophthalmic Pathology Laboratory of Ireland,
Malignant Transformation of Craniopharyngioma without Radiation Therapy: Case Report and Review of the Literature
 Case Report J Korean Neurosurg Soc 60 (1) : 108-113, 2017 https://doi.org/10.3340/jkns.2015.0707.022 pissn 2005-3711 eissn 1598-7876 Malignant Transformation of Craniopharyngioma without Radiation Therapy:
Case Report J Korean Neurosurg Soc 60 (1) : 108-113, 2017 https://doi.org/10.3340/jkns.2015.0707.022 pissn 2005-3711 eissn 1598-7876 Malignant Transformation of Craniopharyngioma without Radiation Therapy:
Myoepithelial carcinoma (malignant myoepithelioma) of the parotid gland arising in a pleomorphic adenoma
 552 Royal Group of Hospitals Trust, Belfast, UK Department of Pathology W G McCluggage P G Toner Department of Otorhinolaryngology W J Primrose Correspondence to: Dr W G McCluggage, Department of Pathology,
552 Royal Group of Hospitals Trust, Belfast, UK Department of Pathology W G McCluggage P G Toner Department of Otorhinolaryngology W J Primrose Correspondence to: Dr W G McCluggage, Department of Pathology,
Note: The cause of testicular neoplasms remains unknown
 - In the 15- to 34-year-old age group, they are the most common tumors of men. - Tumors of the testis are a heterogeneous group of neoplasms that include: I. Germ cell tumors : 95%; all are malignant.
- In the 15- to 34-year-old age group, they are the most common tumors of men. - Tumors of the testis are a heterogeneous group of neoplasms that include: I. Germ cell tumors : 95%; all are malignant.
Synchronous squamous cell carcinoma of the breast. and invasive lobular carcinoma
 Sentani K et al. 1 Letter to the editor Synchronous squamous cell carcinoma of the breast and invasive lobular carcinoma Kazuhiro Sentani, 1 Takashi Tashiro, 2 Naohide Oue, 1 Wataru Yasui 1 1 Department
Sentani K et al. 1 Letter to the editor Synchronous squamous cell carcinoma of the breast and invasive lobular carcinoma Kazuhiro Sentani, 1 Takashi Tashiro, 2 Naohide Oue, 1 Wataru Yasui 1 1 Department
Case 2. Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset
 Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
CASE year old male with a PET avid nodule in the left adrenal gland
 CASE 1 55 year old male with a PET avid nodule in the left adrenal gland Case 1 Adrenal gland parenchyma partly replaced by a spindle cell tumour with mild nuclear pleomorphism Atypical mitoses present
CASE 1 55 year old male with a PET avid nodule in the left adrenal gland Case 1 Adrenal gland parenchyma partly replaced by a spindle cell tumour with mild nuclear pleomorphism Atypical mitoses present
Chapter 1 Introduction
 Chapter 1 Introduction Men think epilepsy divine, merely because they do not understand it. But if they called everything divine which they do not understand, why, there would be no end to divine things.
Chapter 1 Introduction Men think epilepsy divine, merely because they do not understand it. But if they called everything divine which they do not understand, why, there would be no end to divine things.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
A 25 year old female with a palpable mass in the right lower quadrant of her abdomen
 May 2016 A 25 year old female with a palpable mass in the right lower quadrant of her abdomen Contributed by: Paul Ndekwe, MD, Resident Physician, Indiana University School of Department of Pathology and
May 2016 A 25 year old female with a palpable mass in the right lower quadrant of her abdomen Contributed by: Paul Ndekwe, MD, Resident Physician, Indiana University School of Department of Pathology and
