Ultrasound Mapping of Lymph Node and Subcutaneous Metastases in Patients with Cutaneous Melanoma: Results of a Prospective Multicenter Study
|
|
|
- Donald Charles
- 6 years ago
- Views:
Transcription
1 Clinical and Laboratory Investigations DOI: / Received: November 29, 2004 Accepted: May 6, 2005 Ultrasound Mapping of Lymph Node and Subcutaneous Metastases in Patients with Cutaneous Melanoma: Results of a Prospective Multicenter Study a,b c d Andreas Blum Monika-Hildegard Schmid-Wendtner Vera Mauss-Kiefer c a d Julia Yvonne Eberle Christine Kuchelmeister Dorothee Dill-Müller a Department of Dermatology, University of Tübingen, Tübingen ; b Private and Teaching Practice of Dermatology, Konstanz ; c Department of Dermatology and Allergology, Ludwig-Maximilian-University, Munich, and d Department of Dermatology, University Hospital of the Saarland, Homburg/Saar, Germany Key Words Melanoma Sentinel lymph node biopsy Consecutive complete lymph node dissection Abstract Background: Ultrasound (sonography, B-mode sonography, ultrasonography) examination improves the sensitivity in more than 25% compared to the clinical palpation, especially after surgery on the regional lymph node area. Objective: To evaluate the distribution of metastases during follow-up in the draining lymph node areas from the scar of primary to regional lymph nodes (head and neck, supraclavicular, axilla, infraclavicular, groin) in patients with cutaneous melanoma with or without sentinel lymph node biopsy (SLNB) or former elective or consecutive complete lymph node dissection in case of positive sentinel lymph node (CLND). Methods: Prospective multicenter study of the Departments of Dermatology of the Universities of Homburg/Saar, Tübingen and Munich (Germany) in which the distribution of lymph node and subcutaneous metastases were mapped from the scar of primary to the lymphatic drainage region in Andreas Blum and Monika-Hildegard Schmid-Wendtner contributed equally to this work. 53 melanoma patients (23 women, 30 men; median age: 64 years; median tumor thickness: 1.99 mm) with known primary, visible lymph nodes or subcutaneous metastases proven by ultrasound and histopathology during the follow-up. Results: Especially in the axilla, infraclavicular region and groin the metastases were not limited to the anatomic lymph node regions. In 5 patients (9.4%) (4 of them were in stage IV) lymph node metastases were not located in the corresponding lymph node area. 32 patients without former SLNB had a time range between melanoma excision and lymph node metastases of 31 (median), 21 patients with SLNB had 18 (p! 0.005). In 11 patients with positive SLNB the time range was 17, in 10 patients with negative SLNB 21 (p! 0.005); in 32 patients with CLND the time range was 31 and in 21 patients without CLND 18 (p! 0.005). In thinner melanomas lymph node metastases occurred later (p! 0.05). Conclusions: After surgery of cutaneous melanoma, SLNB and CLND the lymphatic drainage can show significant changes which should be considered in clinical and ultrasound followup examinations. Especially for high-risk melanoma patients follow-up examinations should be performed at intervals of 3 in the first years. Patients at stage IV should be examined in all regional lymph node areas clinically and by ultrasound. Copyright 2006 S. Karger AG, Basel Fax karger@karger.ch S. Karger AG, Basel /06/ $23.50/0 Accessible online at: Andreas Blum, MD Private and Teaching Practice of Dermatology Seestrasse 3a DE Konstanz (Germany) Tel , Fax , a.blum@derma.de
2 Introduction Melanoma becomes a life-threatening malignancy with the developing of local, regional or distant metastases [1, 2]. Dissemination of metastases occurs in two thirds of these cases through the lymphatic system [3]. Mostly, the regional lymph node group associated to the primary melanoma is involved. A relevant prognostic parameter for further recurrences and survival is the number of affected lymph nodes [1, 4]. Therefore, especially high-risk melanoma patients should be examined in the draining lymphatic areas during the follow-up [5]. Hereby, the ultrasound (sonography, B-mode sonography, ultrasonography) examination improves the sensitivity in more than 25% compared to the clinical palpation, especially after surgery on the regional lymph node area [4, 6 9]. Ultrasound has a high diagnostic accuracy compared to the clinical examination and lower financial costs compared to computer tomography, magnetic resonance tomography or positron emission tomography [4, 5, 8, 9]. But, to guarantee the high diagnostic accuracy trained users and clear defined regional lymph node areas, which are associated to the primary, are demanded. Therefore, this prospective multicenter study was performed to evaluate the distribution of metastases in the draining lymph node areas in melanoma patients during the regular follow-up detected by ultrasound. Patients and Methods Patients Between September 2002 and August 2003, a total of 53 patients (23 women and 30 men) were included in this prospective study by the Departments of Dermatology of the Universities of Homburg/ Saar (22 patients), Tübingen (18 patients) and Munich (13 patients) during the follow-up of melanoma patients. Only patients with known primary, detected metastases of lymph nodes or intransit area in ultrasound and proven by histopathology were included. Metastases could be detected either at the first presentation of the patients or during the follow-up. Therefore, patients were included with or without sentinel lymph node biopsy (SLNB) or former elective or consecutive complete lymph node dissection in case of positive sentinel lymph node (CLND). In all centers patients with a positive SLNB received a CLND. Not included were patients with unknown primary melanomas of mucous membranes or organs other than the skin. Age range of the patients was years (mean, 60.6 years; median, 64 years). Tumor thickness range was mm (mean 3.22 mm; median 1.99 mm). Patients characteristics are listed in table 1. The regular follow-up of melanoma patients included history, physical examination, ultrasound of the scar, intransit and regional lymph node area(s) [5]. Structures suspicious for metastases on ultrasound were surgically removed for histopathologic examination. Table 1. Characteristics of 53 patients Characteristics Number of patients (%) Sex Female Male Tumor thickness, mm ^0.75 ^ ^ >4.00 Unknown Histologic subtypes SSM NM LMM ALM Unknown Site of the primary tumor Head and neck Trunk Arm Leg Sentinel lymph node biopsy Yes No Positiv sentinel lymph node biopsy Yes No CLND Yes No 23 (43.4) 30 (56.6) 5 (9.4) 25 (47.1) 1 (1.9) 21 (39.6) 20 (37.7) 4 (7.6) 6 (11.3) 2 (3.8) 7 (13.2) 17 (32.1) 1 (1.9) 28 (52.8) 21 (39.6) 32 (60.4) 11 (52.4) 10 (47.6) 32 (60.4) 21 (39.6) SSM = Superficial spreading melanoma; NM = nodular melanoma; LMM = lentiginous malignant melanoma; ALM = acrolentiginous melanoma; unknown = subtype not diagnosable in histopathology. Methods Ultrasound examinations were performed by all authors using real-time scanners (Homburg/Saar: Sonoline Elegra, Siemens Medical Solutions, Erlangen, Germany; Tübingen: AU4 Diagnostic Ultrasound System, Esaote Biomedica, Neufahrn-Munich, Germany; Munich: SSA-340 A, Toshiba Medical Systems, Neuss, Germany) with a MHz linear transducer. In all patients, the examination covered the scar of the primary, its 10-cm surrounding area and the regional lymphatic basin in longitudinal and transverse orientation. At the neck and extremities, this area corresponds to the large blood vessels whereas at the trunk about 30% of melanomas have two or more different lymphatic drainage areas [10 13]. At the proximal part of the extremities the tissue compartment on the lateral and medial region of the main vessels were also scanned. In case the melanoma was located at the head or neck, always both sides of the neck including the supraclavicular region were examined; in case the primary was located at one of the arms, hands or fingers, the axilla and infracla- 48 Blum /Schmid-Wendtner /Mauss-Kiefer / Eberle /Kuchelmeister /Dill-Müller
3 Fig. 1. Lymph node areas at the head. a Dorsal right side. b Dorsal left side. c Ventral right side. d Ventral left side. Grey squares indicates melanoma metastases from a primary of the head. Fig. 3. Lymph node areas at the groin and thigh. a Dorsal left side. b Dorsal right side. c Ventral right side. d Ventral left side. Grey squares indicate melanoma metastases from a primary of the thigh, calf, feet or toes and black circles from a primary of the lower belly or back or buttocks. Fig. 2. Lymph node areas at the axilla. a Dorsal left side. b Dorsal right side. c Ventral right side. d Ventral left side. Grey squares indicate melanoma metastases from a primary of the lower belly or back and black circles from a primary of the upper thorax or back, shoulder, arm, hand or fingers. vicular region were examined; with a melanoma at the trunk, both axillas, infraclavicular regions and both groins and in case the melanoma was located at the thigh, calf, foot or toes, the ipsilateral groin was examined. In every patient this procedure was performed and documented in horizontal and vertical planes. Ultrasound assessment of visible lymph nodes was first based on morphologic criteria (size, shape, echogenicity of the center and cortex of the lymph node). The index according to Solbiati (ratio of maximal and minimal diameters in transversal and longitudinal sonographic sections) was calculated for every lymph node [14]. Lymph nodes were considered as malignant at ultrasound if the following criteria were found [15] : Solbiati index less than two and/or predominance of low echogenicity of the whole lymph node structure and/or lymph node center with low echogenicity and/or asymmetric regions with low echogenicity in the lymph node margin. In the case of malignant lymph node or subcutaneous metastasis in ultrasound, the exact anatomic position was indicated in a figure ( fig. 1 3 ) for every patient. The evaluation of data was performed using the statistical package SPSS (SPSS, Chicago, Ill., USA) for Windows. Statistical testing was performed using Wilcoxon signed ranks test or Mann- Whitney U test. In each statistical analysis, p! 0.05 was regarded as statistically significant. Ultrasound Mapping of Lymph Node Metastases 49
4 Results The results of the location of primary and lymph node metastases are given in table 2. In 5 of 53 patients (9.4%) the lymph node metastases were not found in the corresponding lymph node area of the primary melanoma. Patient 11 had her primary at her right foot, followed by metastases in her right groins; during this study a metastasis at her right axilla was detected. Patient 17 had his melanoma at his upper right back with metastases at his right axilla, followed with hepatic and pulmonal metastases; a metastasis was now found in his left axilla. Patient 19 had his melanoma at his right foot, followed by pulmonal metastases; now a metastasis was detected at his right groin. Patient 36 had his melanoma at his ventral right thigh, followed by inguinal metastases; now a metastasis was found in his left axilla. In patient 44, a metastasis was detected about 10 cm above the left groin whereas she had a melanoma at her dorsal left calf. The distribution of the metastases to the head and neck is presented in figure 1, to the axillas and infraclavicular regions in figure 2, and to the groins and thighs in figure 3. In 6 patients (11.3%) metastases were found at their neck, in 17 patients (32.1%) at the axilla, in 23 patients (43.4%) at the groin, and in 7 patients (13.2%) local subcutaneous metastases (thorax, back, thigh and calf) were diagnosed. In the patients (n = 32), in which a sentinel lymph node biopsy (SLNB) was not performed, the time range between surgery of the primary and lymph node metastases was (mean, 38.9 ; median, 31 ); in patients with performed SLNB (n = 21) the time range was (mean, 23.1 ; median, 18 ) (p! 0.005). A significant difference in the time range was also found in the group of metastatic (n = 11; ; mean, 19.0 ; median, 17 ) and nonmetastatic (n = 10; ; mean, 27.5 ; median, 21 ) SLNB (p! 0.005). Finally, a significant difference was found between the groups with (n = 32; ; mean, 32.3 ; median, 31 ) and without (n = 21; ; mean, 33.1 ; median, 18 ) consecutive complete lymph node dissection (CNLD) (p! 0.005). The time differences between the surgery of the primary and lymph node metastases are given in table 3. If the melanomas were classified into only two groups (thinner or thicker than 1.50 mm), a significant difference was calculated (p! 0.05). Table 2. Location of primary and lymph node metastases Patient No. Location of primary Location of metastasis 1 upper left back left axilla 2 forehead left left cheek 3 ventral left thigh left groin 4 upper right shoulder right axilla 5 left foot left groin 6 right buttock right groin 7 upper left shoulder left axilla 8 left shoulder left axilla 9 left big toe left groin 10 right proximal arm right axilla 11 right foot right axilla 12 ventral left thigh left groin 13 dorsal left calf left groin 14 dorsal left head left neck 15 ventral left calf left groin 16 ventral left thigh left groin 17 upper right back left axilla 18 dorsal right head right neck 19 left foot right groin 20 upper left back left axilla 21 ventral left thigh left groin 22 ventral right thigh right groin 23 ventral left calf left groin 24 dorsal central head left groin 25 big left toe left groin 26 dorsal left calf left calf 27 left foot left groin 28 dorsal right calf right groin 29 upper left thorax left thorax 30 ventral right calf right groin 31 big right toe right groin 32 ventral left calf left groin 33 ventral left thigh left thigh 34 middle left back left back 35 ventral left thigh left thigh 36 ventral right thigh left axilla 37 ventral right thorax right axilla 38 middle right belly right axilla 39 middle right belly right axilla 40 ventral left thigh left thigh 41 ventral left thigh left groin 42 right cheek right cheek 43 dorsal left calf left groin 44 dorsal left calf left groin 45 dorsal left calf left groin 46 ventral left thigh left groin 47 upper thorax right right axilla 48 right neck right neck 49 right shoulder right axilla 50 dorsal right head right neck 51 upper right thorax right axilla 52 upper right back right back 53 upper middle thorax right axilla 50 Blum /Schmid-Wendtner /Mauss-Kiefer / Eberle /Kuchelmeister /Dill-Müller
5 Table 3. Time differences depending on thickness of tumor Tumor thickness Number of patients (%) Minimum Maximum Mean Median ^0.75 mm ^ mm ^ mm >4.00 mm Unknown 5 (9.4) 25 (47.1) 1 (1.9) Discussion As far as we know, this was the first prospective study using ultrasound for mapping the distribution of melanoma metastases in regional lymph node areas with or without former surgery. We found a wide distribution in the different areas of proven metastases in histopathology ( fig. 1 3 ). In 8 of 53 patients (15.1%) metastases were found in and around the scar in the subcutaneous tissue. In the head and neck region metastases were found at the glandula parotis, on the cheek and more or less at the area of the great vessels. In the axillary region metastases were found in the axilla and in its wide surrounding. At the back this included the latissimus dorsi muscle and, ventrally, metastases were found in the pectoral muscles and the region of the upper lateral belly. In the groin, a wide distribution of metastases was worked out from the region above the ligamentum inguinale to the distal area of the thigh. Also, metastases were detected medially and laterally to the main blood vessels. Several studies worked out that more than 25% of the lymph node metastases cannot be detected by palpation [4, 8, 9]. One special explanation for this difference between clinical and ultrasound examination could be that the clinical examination is less extensive than the wide area in which metastases could be found. In 5 of 53 patients (9.4%), metastases were detected in other lymph node regions by using ultrasound. Four of the 5 patients had previous metastases in the regional lymph nodes or even in the organs. So these patients were in stage IV of their disease which could explain the spread of metastases in further regional lymph node areas. The present data could not be compared with the data about the distribution of sentinel lymph node biopsy (SLNB) [10 13]. Normally, lymphoscintigraphy is performed before surgery of the primary or at least after a small excision biopsy that leads to no or little change in lymphatic drainage. But surgery with recommended safety margins, a SLNB or even a CNLD after positive SLNB have a significant impact on lymphatic drainage. Physicians should be aware of this when they are running clinical and ultrasound follow-up examinations. Significant differences in the time range to progression were found in the groups with or without sentinel lymph node biopsy and with positive or negative sentinel lymph nodes. In the case of metastatic lymph node(s), an earlier recurrence in the lymph node area was worked out in patients with performed SLNB and patients with positive SLNB. This could also be confirmed that thicker melanomas had earlier lymph node metastases than thinner which has also been reported in the literature [1 5]. However, our data showed that patients with CLND developed lymph node metastases significantly later than patients without CLND. One explanation could be that our collective was too small for analyzing this question. Another explanation could be that due to the CLND micrometastases are not distinguishable by ultrasound. This hypothesis could be supported that the most of high risk melanoma patients had a positive SLNB and underwent a CLND. Probably, this collective might have a benefit of the CLND [16]. In the present study, patients with CLND had longer disease free time concerning lymph or subcutaneous metastatic nodes than patients with positive or negative SLNB (31, 17 and 21, respectively). Also here we have to consider that our collective, especially regarding the correlation of affected nodes in CLND or SLNB and tumor thickness, was too small for analyzing this question. In addition, one possible explanation could be that by CLND micrometastases were removed which remained still present in patients with positive or negative SLNB. Studies with a larger data base could be able to answer this question of distribution in the subgroups. The early detection of subcutaneous and regional lymph node metastases in patients with melanoma is critical for their prognosis [1 4]. Therefore, intensive clinical and ultrasound examination could improve the benefit for patients in the follow-up, especially for high-risk mel- Ultrasound Mapping of Lymph Node Metastases 51
6 anoma. The following recommendations are proposed for the ultrasound examination: Examination from the Scar of Primary to the Regional Lymph Node Area(s). The ultrasound examination should start at the site of the scar of the primary melanoma, followed by the lymphatic drainage area(s). After examination of an area of 10 cm around the scar, the transducer should be moved along the lymphatic vessels to the regional lymphatic region in transversal orientation. Examination of the Cervical Region(s). The head of the patient should be turned to the opposite site. First, the glandula parotis will be examined in two planes. Then the transducer will be moved to the retroauricular area. The cervical vessels including the surrounding tissue will be examined in a horizontal and a vertical plane from the insertion of the sternocleidomastoidal muscle to the upper thoracic aperture. The evaluation of the submandibular and, finally, the supraclavicular region follows. Examination of the Axillary and the Infraclavicular Region(s). Patients will be examined in a position with a 120 abduction of the arm. The examination will be performed in a horizontal pattern in cross-sections along the axillary artery, starting from lower axillary region towards the brachial artery and the proximal third of the upper arm, and to the opposite towards the subclavian artery. Finally, the area between the latissimus dorsi (posterior axillary line), the pectoral muscles (anterior axillary line) and the beginning of the upper arm (upper limitation) will be completely evaluated. Examination of the Groins. The inguinal ligament, inguinal and femoral vessels are the leading anatomic structures for examination of this area. Following the inguinal ligament from the anterior superior iliac spine to the symphysis, the vessels will be crossed. Now the transducer follows the vessels in a horizontal plane 5 10 cm cranial of the inguinal ligament. Caudal of the inguinal ligament, the adductor canal will be completely examined by ultrasound. Lateral and medial of the femoral vessels, the upper third of the thigh will be scanned in two planes. For patients with high-risk melanoma, clinical and ultrasound examination should be recommended at intervals of 3 in the first 3 5 years [5]. Weekly selfexamination should be demonstrated to the patient which can also lead to an earlier detection of a metastasis. Patients at stage IV should be examined in all regional lymph node areas clinically and with ultrasound. Although the nodal metastases have no significant impact on overall patient survival in stage IV, the ultrasound could be used for monitoring therapies, for providing tumor material for vaccination in clinical studies or for planning surgical intervention to minimize tumor load. References 1 Balch CM: Cutaneous melanoma: prognosis and treatment results. Semin Surg Oncol 1992; 8: Schmid-Wendtner M, Baumert J, Schmidt M, Plewig G, Volkenandt M, Hölzel D: Prognostic index for cutaneous melanoma: an analysis after follow-up of 2,715 patients. Melanoma Res 2001; 11: Balch CM, Soong SJ, Murad TM, Smith JW, Maddox WA, Durant JR: A multifactorial analysis of melanoma. IV. Prognostic factors in 200 melanoma patients with distant metastases (stage III). J Clin Oncol 1983; 1: Voit C, Mayer T, Kron M, Schoengen A, Sterry W, Weber L, Proebstle TM: Efficacy of ultrasound B-scan compared with physical examination in follow-up of melanoma patients. Cancer 2001; 91: Garbe C, Paul A, Kohler-Späth H, et al: Prospective evaluation of a follow-up schedule in 2,008 patients with cutaneous melanoma: recommendations for an improved follow-up strategy. J Clin Oncol 2003; 21: Nazarian LN, Alexander AA, Rawool NM, Kurtz AB, Maguire HC, Mastrangelo MJ: Malignant melanoma: impact of superficial US on management. Radiology 1996; 199: Rossi CR, Seno A, Vecchiato A, et al: The impact of ultrasound scanning in the staging and follow-up of patients with clinical stage I cutaneous melanoma. Eur J Cancer 1997; 33: Blum A, Schlagenhauff B, Stroebel W, Breuninger H, Rassner G, Garbe C: Ultrasound examination of regional lymph nodes significantly improves early detection of locoregional metastases during the follow-up of cutaneous melanoma. Results of a prospective study in 1,288 Patients. Cancer 2000; 88: Schmid-Wendtner MH, Paerschke G, Baumert J, Plewig G, Volkenandt M: Value of ultrasonography compared with physical examination for the detection of locoregional metastases in patients with cutaneous melanoma. Melanoma Res 2003; 13: Uren RF, Howman-Giles R, Thompson JF, et al: Lymphoscintigraphy to identify sentinel lymph nodes in patients with melanoma. Melanoma Res 1994; 4: Rees WV, Robinson DS, Holmes EC, Morton DL: Altered lymphatic drainage following lymphadenectomy. Cancer 1980; 45: Morton DL: Sentinel lymphadenectomy for patients with clinical stage I melanoma. J Surg Oncol 1997; 66: Porter GA, Ross MI, Berman RS, Lee JE, Mansfield PF, Gershenwald JE: Significance of multiple nodal basin drainage in truncal melanoma patients undergoing sentinel lymph node biopsy. Ann Surg Oncol 2000; 7: Solbiati L, Rizzatto G, Belotti E: High resolution sonography of cervical lymph nodes in head and neck cancer: criteria for differentiation of reactive versus malignant lymph nodes. Proceedings of the 74th Meeting of the Radiologic Society of North America. Chicago, Radiologic Society of North America, 1988, abstr 113ff. 15 Vassallo P, Wernecke K, Roos N, Peters PE: Differentiation of benign from malignant superficial lymphadenopathy: the role of highresolution US. Radiology 1992; 183: Cascinelli N, Morabito A, Santinami M, MacKie RM, Belli F: Immediate or delayed dissection of regional nodes in patients with melanoma of the trunk: a randomised trial. WHO Melanoma Programme. Lancet ; 351: Blum /Schmid-Wendtner /Mauss-Kiefer / Eberle /Kuchelmeister /Dill-Müller
Critical meta-analysis of the diagnostic criteria employed for the sonography (US) diagnosis of lymph node metastasis in the melanoma patient
 Critical meta-analysis of the diagnostic criteria employed for the sonography (US) diagnosis of lymph node metastasis in the melanoma patient Poster No.: C-0992 Congress: ECR 2011 Type: Scientific Exhibit
Critical meta-analysis of the diagnostic criteria employed for the sonography (US) diagnosis of lymph node metastasis in the melanoma patient Poster No.: C-0992 Congress: ECR 2011 Type: Scientific Exhibit
You Are Going to Cut How Much Skin? Locoregional Surgical Treatment. Justin Rivard MD, MSc, FRCSC September 21, 2018
 You Are Going to Cut How Much Skin? Locoregional Surgical Treatment Justin Rivard MD, MSc, FRCSC September 21, 2018 Presenter Disclosure Faculty/Speaker: Justin Rivard Relationships with financial sponsors:
You Are Going to Cut How Much Skin? Locoregional Surgical Treatment Justin Rivard MD, MSc, FRCSC September 21, 2018 Presenter Disclosure Faculty/Speaker: Justin Rivard Relationships with financial sponsors:
LYMPHATIC DRAINAGE PATTERNS OF HEAD AND NECK CUTANEOUS MELANOMA OBSERVED ON LYMPHOSCINTIGRAPHY AND SENTINEL LYMPH NODE BIOPSY
 LYMPHATIC DRAINAGE PATTERNS OF HEAD AND NECK CUTANEOUS MELANOMA OBSERVED ON LYMPHOSCINTIGRAPHY AND SENTINEL LYMPH NODE BIOPSY Doris Lin, MD, 1 Benjamin L. Franc, MD, 2 Mohammed Kashani-Sabet, MD, 3 Mark
LYMPHATIC DRAINAGE PATTERNS OF HEAD AND NECK CUTANEOUS MELANOMA OBSERVED ON LYMPHOSCINTIGRAPHY AND SENTINEL LYMPH NODE BIOPSY Doris Lin, MD, 1 Benjamin L. Franc, MD, 2 Mohammed Kashani-Sabet, MD, 3 Mark
Improved Differentiation of Benign and Malignant Lymphadenopathy in Patients With Cutaneous Melanoma by Contrast-Enhanced Color Doppler Sonography
 STUDY Improved Differentiation of Benign and Malignant Lymphadenopathy in Patients With Cutaneous Melanoma by Contrast-Enhanced Color Doppler Sonography Monika-Hildegard Schmid-Wendtner, MD; Karin Partscht,
STUDY Improved Differentiation of Benign and Malignant Lymphadenopathy in Patients With Cutaneous Melanoma by Contrast-Enhanced Color Doppler Sonography Monika-Hildegard Schmid-Wendtner, MD; Karin Partscht,
Rebecca Vogel, PGY-4 March 5, 2012
 Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
Therapeutic Lymph Node Dissection in Melanoma: Different Prognosis for Different Macrometastasis Sites?
 Ann Surg Oncol (01) 19:91 91 DOI.14/s44-01-401- ORIGINAL ARTICLE MELANOMAS Therapeutic Lymph Node Dissection in Melanoma: Different Prognosis for Different Macrometastasis Sites? K. P. Wevers, MD, E. Bastiaannet,
Ann Surg Oncol (01) 19:91 91 DOI.14/s44-01-401- ORIGINAL ARTICLE MELANOMAS Therapeutic Lymph Node Dissection in Melanoma: Different Prognosis for Different Macrometastasis Sites? K. P. Wevers, MD, E. Bastiaannet,
Melanoma Quality Reporting
 Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Talk to Your Doctor. Fact Sheet
 Talk to Your Doctor Hearing the words you have skin cancer is overwhelming and would leave anyone with a lot of questions. If you have been diagnosed with Stage I or II cutaneous melanoma with no apparent
Talk to Your Doctor Hearing the words you have skin cancer is overwhelming and would leave anyone with a lot of questions. If you have been diagnosed with Stage I or II cutaneous melanoma with no apparent
ORIGINAL ARTICLE. Clinical Node-Negative Thick Melanoma
 ORIGINAL ARTICLE Clinical Node-Negative Thick Melanoma George I. Salti, MD; Ashwin Kansagra, MD; Michael A. Warso, MD; Salve G. Ronan, MD ; Tapas K. Das Gupta, MD, PhD, DSc Background: Patients with T4
ORIGINAL ARTICLE Clinical Node-Negative Thick Melanoma George I. Salti, MD; Ashwin Kansagra, MD; Michael A. Warso, MD; Salve G. Ronan, MD ; Tapas K. Das Gupta, MD, PhD, DSc Background: Patients with T4
Results, morbidity, and quality of life of melanoma patients undergoing sentinel lymph node staging Vries, Mattijs de
 University of Groningen Results, morbidity, and quality of life of melanoma patients undergoing sentinel lymph node staging Vries, Mattijs de IMPORTANT NOTE: You are advised to consult the publisher's
University of Groningen Results, morbidity, and quality of life of melanoma patients undergoing sentinel lymph node staging Vries, Mattijs de IMPORTANT NOTE: You are advised to consult the publisher's
Translating Evidence into Practice: Primary Cutaneous Melanoma Guidelines. Sentinel Lymph Node Biopsy
 American Academy of Dermatology 2018 Annual Meeting San Diego, CA, February 17, 2018 Translating Evidence into Practice: Primary Cutaneous Melanoma Guidelines. Sentinel Lymph Node Biopsy Christopher Bichakjian,
American Academy of Dermatology 2018 Annual Meeting San Diego, CA, February 17, 2018 Translating Evidence into Practice: Primary Cutaneous Melanoma Guidelines. Sentinel Lymph Node Biopsy Christopher Bichakjian,
Radionuclide detection of sentinel lymph node
 Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival
 MOLECULAR AND CLINICAL ONCOLOGY 7: 1083-1088, 2017 Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival FARUK TAS
MOLECULAR AND CLINICAL ONCOLOGY 7: 1083-1088, 2017 Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival FARUK TAS
Lab no 1 Structural organization of the human body
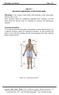 Physiology Lab Manual Page 1 of 6 Lab no 1 Structural organization of the human body Physiology is the science which deals with functions of the body parts, and how they work. Since function cannot be
Physiology Lab Manual Page 1 of 6 Lab no 1 Structural organization of the human body Physiology is the science which deals with functions of the body parts, and how they work. Since function cannot be
Kentaro Tanaka, 1 Hiroki Mori, 1 Mutsumi Okazaki, 1 Aya Nishizawa, 2 and Hiroo Yokozeki Introduction. 2. Case Presentation
 Case Reports in Oncological Medicine Volume 2013, Article ID 259326, 4 pages http://dx.doi.org/10.1155/2013/259326 Case Report Long-Term Treatment Outcome after Only Popliteal Lymph Node Dissection for
Case Reports in Oncological Medicine Volume 2013, Article ID 259326, 4 pages http://dx.doi.org/10.1155/2013/259326 Case Report Long-Term Treatment Outcome after Only Popliteal Lymph Node Dissection for
1
 www.clinicaloncology.com.ua 1 Prognostic factors of appearing micrometastases in sentinel lymph nodes in skin melanoma M.N.Kukushkina, S.I.Korovin, O.I.Solodyannikova, G.G.Sukach, A.Yu.Palivets, A.N.Potorocha,
www.clinicaloncology.com.ua 1 Prognostic factors of appearing micrometastases in sentinel lymph nodes in skin melanoma M.N.Kukushkina, S.I.Korovin, O.I.Solodyannikova, G.G.Sukach, A.Yu.Palivets, A.N.Potorocha,
Nodal staging in localized melanoma. The experience of the Brescia Melanoma Unit
 The British Association of Plastic Surgeons (2003) 56, 534 539 Nodal staging in localized melanoma. The experience of the Brescia Melanoma Unit Giorgio Manca a, *, Fabio Facchetti b, Claudio Pizzocaro
The British Association of Plastic Surgeons (2003) 56, 534 539 Nodal staging in localized melanoma. The experience of the Brescia Melanoma Unit Giorgio Manca a, *, Fabio Facchetti b, Claudio Pizzocaro
PAPER. Prognostic Information From Sentinel Lymph Node Biopsy in Patients With Thick Melanoma
 PAPER Prognostic Information From Sentinel Lymph Node Biopsy in Patients With Thick Melanoma Charles R. Scoggins, MD, MBA; Adrianne L. Bowen, MD; Robert C. Martin II, MD, PhD; Michael J. Edwards, MD; Douglas
PAPER Prognostic Information From Sentinel Lymph Node Biopsy in Patients With Thick Melanoma Charles R. Scoggins, MD, MBA; Adrianne L. Bowen, MD; Robert C. Martin II, MD, PhD; Michael J. Edwards, MD; Douglas
Nodal Treatment in Melanoma: Snow to MSLT-II
 Nodal Treatment in Melanoma: Snow to MSLT-II Mark B. Faries, MD, FACS Director, Donald L. Morton Melanoma Research Program Program Director, JWCI Complex General Surgical Oncology Fellowship Director,
Nodal Treatment in Melanoma: Snow to MSLT-II Mark B. Faries, MD, FACS Director, Donald L. Morton Melanoma Research Program Program Director, JWCI Complex General Surgical Oncology Fellowship Director,
Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy
 Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy Dale Han, MD Assistant Professor Department of Surgery Section of Surgical Oncology No disclosures Background Desmoplastic melanoma (DM)
Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy Dale Han, MD Assistant Professor Department of Surgery Section of Surgical Oncology No disclosures Background Desmoplastic melanoma (DM)
NEW SURGICAL APPROACHES TO MELANOMA THERAPY
 NEW SURGICAL APPROACHES TO MELANOMA THERAPY Melanoma 2003: New Insights Into Therapy & Treatment Douglas L. Fraker, M.D. University of Pennsylvania Surgical Treatment of Melanoma Primary resection margins
NEW SURGICAL APPROACHES TO MELANOMA THERAPY Melanoma 2003: New Insights Into Therapy & Treatment Douglas L. Fraker, M.D. University of Pennsylvania Surgical Treatment of Melanoma Primary resection margins
SENTINEL LYMPH node (SLN) biopsy has become
 COMMENTARY Sentinel Lymph Node Biopsy for Melanoma: Controversy Despite Widespread Agreement By Kelly M. McMasters, Douglas S. Reintgen, Merrick I. Ross, Jeffrey E. Gershenwald, Michael J. Edwards, Arthur
COMMENTARY Sentinel Lymph Node Biopsy for Melanoma: Controversy Despite Widespread Agreement By Kelly M. McMasters, Douglas S. Reintgen, Merrick I. Ross, Jeffrey E. Gershenwald, Michael J. Edwards, Arthur
Prognosis of Sentinel Node Staged Patients with Primary Cutaneous Melanoma
 Prognosis of Sentinel Node Staged Patients with Primary Cutaneous Melanoma Otmar Elsaeßer 1., Ulrike Leiter 1 *., Petra G. Buettner 2, Thomas K. Eigentler 1, Friedegund Meier 1, Benjamin Weide 1, Gisela
Prognosis of Sentinel Node Staged Patients with Primary Cutaneous Melanoma Otmar Elsaeßer 1., Ulrike Leiter 1 *., Petra G. Buettner 2, Thomas K. Eigentler 1, Friedegund Meier 1, Benjamin Weide 1, Gisela
Index. Note: Page numbers of article titles are in boldface type. A Age as factor in melanoma, Anorectal melanoma RT for, 1035
 Index Note: Page numbers of article titles are in boldface type. A Age as factor in melanoma, 947 948 Anorectal melanoma RT for, 1035 B Bacille Calmette-Guerin (BCG) in melanoma, 1008 BCG. See Bacille
Index Note: Page numbers of article titles are in boldface type. A Age as factor in melanoma, 947 948 Anorectal melanoma RT for, 1035 B Bacille Calmette-Guerin (BCG) in melanoma, 1008 BCG. See Bacille
Review Article Lymphoscintigraphy Defines New Lymphatic Pathways from Cutaneous Melanoma Site: Clinical Implications and Surgical Management
 Radiology Research and Practice Volume 2011, Article ID 817043, 5 pages doi:10.1155/2011/817043 Review Article Lymphoscintigraphy Defines New Lymphatic Pathways from Cutaneous Melanoma Site: Clinical Implications
Radiology Research and Practice Volume 2011, Article ID 817043, 5 pages doi:10.1155/2011/817043 Review Article Lymphoscintigraphy Defines New Lymphatic Pathways from Cutaneous Melanoma Site: Clinical Implications
Sonography for Locoregional Staging and Follow-up of Cutaneous Melanoma
 Technical Advance Sonography for Locoregional Staging and Follow-up of Cutaneous Melanoma How We Do It Orlando Catalano, MD, Sergio Venanzio Setola, MD, Paolo Vallone, MD, Mauro Mattace Raso, MD, Adolfo
Technical Advance Sonography for Locoregional Staging and Follow-up of Cutaneous Melanoma How We Do It Orlando Catalano, MD, Sergio Venanzio Setola, MD, Paolo Vallone, MD, Mauro Mattace Raso, MD, Adolfo
Anatomical Terminology
 Anatomical Terminology Dr. A. Ebneshahidi Anatomy Anatomy : is the study of structures or body parts and their relationships to on another. Anatomy : Gross anatomy - macroscopic. Histology - microscopic.
Anatomical Terminology Dr. A. Ebneshahidi Anatomy Anatomy : is the study of structures or body parts and their relationships to on another. Anatomy : Gross anatomy - macroscopic. Histology - microscopic.
Sentinel Node Localisation of Melanoma
 Sentinel Node Localisation of Melanoma V Bongers, Diakonessenhuis, Utrecht 1. Introduction A melanoma is mostly a malignancy of the skin. The sentinel lymph node (SLN) concept of sequential progression
Sentinel Node Localisation of Melanoma V Bongers, Diakonessenhuis, Utrecht 1. Introduction A melanoma is mostly a malignancy of the skin. The sentinel lymph node (SLN) concept of sequential progression
ANATYOMY OF The thigh
 ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
Directly Coded Summary Stage Melanoma
 Directly Coded Summary Stage Melanoma National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention and Control, National Program of Cancer Registries Directly Coded
Directly Coded Summary Stage Melanoma National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention and Control, National Program of Cancer Registries Directly Coded
No Benefit to Routine Completion Lymphadenectomy for Sentinel Lymph Node Positive Melanoma
 No Benefit to Routine Completion Lymphadenectomy for Sentinel Lymph Node Positive Melanoma Michael Lowe, MD Assistant Professor of Surgery Winship Cancer Institute Emory University School of Medicine July
No Benefit to Routine Completion Lymphadenectomy for Sentinel Lymph Node Positive Melanoma Michael Lowe, MD Assistant Professor of Surgery Winship Cancer Institute Emory University School of Medicine July
Chapter 1: Introduction to the Human Body Test Bank
 Chapter 1: Introduction to the Human Body Test Bank MULTIPLE CHOICE 1. What is the branch of science that studies how the body functions? a. Anatomy b. Histology c. Pathology d. Physiology 2. Which word
Chapter 1: Introduction to the Human Body Test Bank MULTIPLE CHOICE 1. What is the branch of science that studies how the body functions? a. Anatomy b. Histology c. Pathology d. Physiology 2. Which word
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Topics for Discussion. Malignant Melanoma. Surgical Treatment. Current Treatment of Cutaneous Melanoma 5/17/2013. Lymph Regional nodes:
 Topics for Discussion What is a sentinel lymph node (SLN)? Utility of sentinel lymph biopsies: therapeutic or staging? Current Treatment of Cutaneous Melanoma Carlos Corvera, M.D. Associate Professor of
Topics for Discussion What is a sentinel lymph node (SLN)? Utility of sentinel lymph biopsies: therapeutic or staging? Current Treatment of Cutaneous Melanoma Carlos Corvera, M.D. Associate Professor of
Melanoma Surgery Update James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division
 Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Sentinel Lymph Node Biopsy Is Valuable For All Cancer. Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner
 Sentinel Lymph Node Biopsy Is Valuable For All Cancer Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner History Lymphatics first described by Rasmus Bartholin in 1653 Rudolf Virchow postulated
Sentinel Lymph Node Biopsy Is Valuable For All Cancer Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner History Lymphatics first described by Rasmus Bartholin in 1653 Rudolf Virchow postulated
Malignant Melanoma in Turkey: A Single Institution s Experience on 475 Cases
 Malignant Melanoma in Turkey: A Single Institution s Experience on 475 Cases Faruk Tas, Sidika Kurul, Hakan Camlica and Erkan Topuz Institute of Oncology, Istanbul University, Istanbul, Turkey Received
Malignant Melanoma in Turkey: A Single Institution s Experience on 475 Cases Faruk Tas, Sidika Kurul, Hakan Camlica and Erkan Topuz Institute of Oncology, Istanbul University, Istanbul, Turkey Received
Anatomy The study of the body's structure.
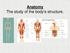 Anatomy The study of the body's structure. * 1. Systemic- Study of each of the body's systems. 2. Regional- Study of a specific area of the body 3. Surface- Study of external features. Physiology The study
Anatomy The study of the body's structure. * 1. Systemic- Study of each of the body's systems. 2. Regional- Study of a specific area of the body 3. Surface- Study of external features. Physiology The study
Katsuhiro Yamada, Natsuko Noguti, Masaaki Tsuda, Hazime Nagato, Naoko Hasunuma, Yoshihiro Umebayashi and Motomu Manabe
 Akita J Med 36 : 45-52, 2009 45 Katsuhiro Yamada, Natsuko Noguti, Masaaki Tsuda, Hazime Nagato, Naoko Hasunuma, Yoshihiro Umebayashi and Motomu Manabe (Received 22 December 2008, Accepted 15 January 2009)
Akita J Med 36 : 45-52, 2009 45 Katsuhiro Yamada, Natsuko Noguti, Masaaki Tsuda, Hazime Nagato, Naoko Hasunuma, Yoshihiro Umebayashi and Motomu Manabe (Received 22 December 2008, Accepted 15 January 2009)
Practice of Axilla Surgery
 Summer School of Breast Disease 2016 Practice of Axilla Surgery Axillary Lymph Node Dissection & Sentinel Lymph Node Biopsy 연세의대외과 박세호 Contents Anatomy of the axilla Axillary lymph node dissection (ALND)
Summer School of Breast Disease 2016 Practice of Axilla Surgery Axillary Lymph Node Dissection & Sentinel Lymph Node Biopsy 연세의대외과 박세호 Contents Anatomy of the axilla Axillary lymph node dissection (ALND)
Morphological characteristics of the primary tumor and micrometastases in sentinel lymph nodes as a predictor of melanoma progression
 Morphological characteristics of the primary tumor and micrometastases in sentinel lymph nodes as a predictor of melanoma progression M.N. Kukushkina, S.I. Korovin, O.I. Solodyannikova, G.G. Sukach, A.Yu.
Morphological characteristics of the primary tumor and micrometastases in sentinel lymph nodes as a predictor of melanoma progression M.N. Kukushkina, S.I. Korovin, O.I. Solodyannikova, G.G. Sukach, A.Yu.
Work-up/Follow-up: Baseline and Surveillance Studies for Cutaneous Melanoma Patients
 2018 AAD Annual Meeting, San Diego, CA Work-up/Follow-up: Baseline and Surveillance Studies for Cutaneous Melanoma Patients Susan M. Swetter, MD, FAAD Professor of Dermatology Director, Pigmented Lesion
2018 AAD Annual Meeting, San Diego, CA Work-up/Follow-up: Baseline and Surveillance Studies for Cutaneous Melanoma Patients Susan M. Swetter, MD, FAAD Professor of Dermatology Director, Pigmented Lesion
Radiology- Pathology Conference 4/29/2012. Lymph Nodes. John McGrath
 Radiology- Pathology Conference 4/29/2012 Lymph Nodes John McGrath 1 Presentation material is for education purposes only. All rights reserved. 2012 URMC Radiology Page 1 of 24 Case 1: 51 year-old male
Radiology- Pathology Conference 4/29/2012 Lymph Nodes John McGrath 1 Presentation material is for education purposes only. All rights reserved. 2012 URMC Radiology Page 1 of 24 Case 1: 51 year-old male
Cutaneous Melanoma: Epidemiology (USA) The Sentinel Node in Head and Neck Melanoma. Cutaneous Melanoma: Epidemiology (USA)
 The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
ORIGINAL ARTICLE PROGNOSTIC IMPLICATION OF SENTINEL LYMPH NODE BIOPSY IN CUTANEOUS HEAD AND NECK MELANOMA
 ORIGINAL ARTICLE PROGNOSTIC IMPLICATION OF SENTINEL LYMPH NODE BIOPSY IN CUTANEOUS HEAD AND NECK MELANOMA Benjamin E. Saltman, MD, 1 Ian Ganly, MD, 2 Snehal G. Patel, MD, 2 Daniel G. Coit, MD, 3 Mary Sue
ORIGINAL ARTICLE PROGNOSTIC IMPLICATION OF SENTINEL LYMPH NODE BIOPSY IN CUTANEOUS HEAD AND NECK MELANOMA Benjamin E. Saltman, MD, 1 Ian Ganly, MD, 2 Snehal G. Patel, MD, 2 Daniel G. Coit, MD, 3 Mary Sue
Clinical Practice Guidelines
 Clinical Practice Guidelines Clinical Practice Guidelines for Melanoma Douglas Reintgen, MD, et al H. Lee Moffitt Cancer Center & Research Institute These clinical practice guidelines for melanoma have
Clinical Practice Guidelines Clinical Practice Guidelines for Melanoma Douglas Reintgen, MD, et al H. Lee Moffitt Cancer Center & Research Institute These clinical practice guidelines for melanoma have
Patent Blue Dye (P.B.D) tums.ac.ir
 80-84 1387 2 66 80 : 30 :.. 1385 1382.. Patent Blue Dye (P.B.D). 48 :. - (%47)13 19 195 17.. :.. : * * 88723410 : email: omranipour@ tums.ac.ir. 4 5. Patent Blue Dye (P.B.D) 6-8 %13. %20 1 2. 3 1992 Morton.
80-84 1387 2 66 80 : 30 :.. 1385 1382.. Patent Blue Dye (P.B.D). 48 :. - (%47)13 19 195 17.. :.. : * * 88723410 : email: omranipour@ tums.ac.ir. 4 5. Patent Blue Dye (P.B.D) 6-8 %13. %20 1 2. 3 1992 Morton.
The Language of Anatomy. (Anatomical Terminology)
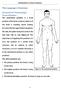 The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Citation for published version (APA): Francken, A. B. (2007). Primary and metastatic melanoma: aspects of follow-up and staging s.n.
 University of Groningen Primary and metastatic melanoma Francken, Anne Brecht IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen Primary and metastatic melanoma Francken, Anne Brecht IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
Predictive Factors for the Positivity of the Sentinel Lymph Node in Malignant Melanoma
 ORIGINAL RESEARCH SURGERY // ANATOMO-PATHOLOGY Predictive Factors for the Positivity of the Sentinel Lymph Node in Malignant Melanoma Călin Crăciun, Orsolya Hankó- Bauer, Zalán Benedek, Sorin Sorlea, Marius
ORIGINAL RESEARCH SURGERY // ANATOMO-PATHOLOGY Predictive Factors for the Positivity of the Sentinel Lymph Node in Malignant Melanoma Călin Crăciun, Orsolya Hankó- Bauer, Zalán Benedek, Sorin Sorlea, Marius
ORIGINAL ARTICLE. Reliability of Sentinel Lymph Node Mapping With Biopsy for Head and Neck Cutaneous Melanoma
 ORIGINAL ARTICLE Reliability of Sentinel Lymph Node Mapping With Biopsy for Head and Neck Cutaneous Melanoma Cecelia E. Schmalbach, MD; Brian Nussenbaum, MD; Riley S. Rees, MD; Jennifer Schwartz, MD; Timothy
ORIGINAL ARTICLE Reliability of Sentinel Lymph Node Mapping With Biopsy for Head and Neck Cutaneous Melanoma Cecelia E. Schmalbach, MD; Brian Nussenbaum, MD; Riley S. Rees, MD; Jennifer Schwartz, MD; Timothy
Surgical Issues in Melanoma
 Surgical Issues in Melanoma Mark B. Faries, MD, FACS Director, Donald L. Morton Melanoma Research Program Director, Surgical Oncology Training Program Professor of Surgery John Wayne Cancer Institute Surgical
Surgical Issues in Melanoma Mark B. Faries, MD, FACS Director, Donald L. Morton Melanoma Research Program Director, Surgical Oncology Training Program Professor of Surgery John Wayne Cancer Institute Surgical
Update on SLN and Melanoma: DECOG and MSLT-II. Gordon H. Hafner, MD, FACS
 Update on SLN and Melanoma: DECOG and MSLT-II Gordon H. Hafner, MD, FACS No disclosures The surgery of malignant disease is not the surgery of organs, it is of the lymphatic system. Lord Moynihan Lymph
Update on SLN and Melanoma: DECOG and MSLT-II Gordon H. Hafner, MD, FACS No disclosures The surgery of malignant disease is not the surgery of organs, it is of the lymphatic system. Lord Moynihan Lymph
Epithelial Cancer- NMSC & Melanoma
 Epithelial Cancer- NMSC & Melanoma David Chin MB, BCh, BAO, LRCP, LRCS (Ireland) MCh(MD), PhD (UQ), FRCS, FRACS (Plast) Plastic & Reconstructive Surgeon Visiting Scientist Melanoma Genomic Group & Drug
Epithelial Cancer- NMSC & Melanoma David Chin MB, BCh, BAO, LRCP, LRCS (Ireland) MCh(MD), PhD (UQ), FRCS, FRACS (Plast) Plastic & Reconstructive Surgeon Visiting Scientist Melanoma Genomic Group & Drug
Clinico-pathological Features of Patients with Melanoma and Positive Sentinel Lymph Node Biopsy: A Single Institution Experience
 2015;23(2):122-129 CLINICAL ARTICLE Clinico-pathological Features of Patients with Melanoma and Positive Sentinel Lymph Node Biopsy: A Single Institution Experience Damir Homolak 1, Mirna Šitum 2,3, Hrvoje
2015;23(2):122-129 CLINICAL ARTICLE Clinico-pathological Features of Patients with Melanoma and Positive Sentinel Lymph Node Biopsy: A Single Institution Experience Damir Homolak 1, Mirna Šitum 2,3, Hrvoje
The tail sign and the string sign: a new sonography (US) finding in patients with superficial melanoma metastasis
 The tail sign and the string sign: a new sonography (US) finding in patients with superficial melanoma metastasis Poster No.: C-1088 Congress: ECR 2012 Type: Scientific Exhibit Authors: A. Nunziata, O.
The tail sign and the string sign: a new sonography (US) finding in patients with superficial melanoma metastasis Poster No.: C-1088 Congress: ECR 2012 Type: Scientific Exhibit Authors: A. Nunziata, O.
1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter.
 Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
PAPER. Effect of Multiple Nodal Basin Drainage on Cutaneous Melanoma
 PAPER Effect of Multiple Nodal Basin Drainage on Cutaneous Melanoma Andrea C. Federico, BA; Anees B. Chagpar, MD; Merrick I. Ross, MD; Robert C. G. Martin, MD; R. Dirk Noyes, MD; James S. Goydos, MD; Peter
PAPER Effect of Multiple Nodal Basin Drainage on Cutaneous Melanoma Andrea C. Federico, BA; Anees B. Chagpar, MD; Merrick I. Ross, MD; Robert C. G. Martin, MD; R. Dirk Noyes, MD; James S. Goydos, MD; Peter
VENOUS DRAINAGE O US F UPPER UPPER LIM B BY dr.fahad Ullah
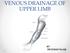 VENOUS DRAINAGE OF UPPER LIMB BY dr.fahad Ullah Venous drainage of the supper limb The venous system of the upper limb drains deoxygenated blood from the arm, forearm and hand It can anatomically be divided
VENOUS DRAINAGE OF UPPER LIMB BY dr.fahad Ullah Venous drainage of the supper limb The venous system of the upper limb drains deoxygenated blood from the arm, forearm and hand It can anatomically be divided
THE ROLE OF CONTEMPORARY IMAGING AND HYBRID METHODS IN THE DIAGNOSIS OF CUTANEOUS MALIGNANT MELANOMA(CMM) AND MERKEL CELL CARCINOMA (MCC)
 THE ROLE OF CONTEMPORARY IMAGING AND HYBRID METHODS IN THE DIAGNOSIS OF CUTANEOUS MALIGNANT MELANOMA(CMM) AND MERKEL CELL CARCINOMA (MCC) I.Kostadinova, Sofia, Bulgaria CMM some clinical facts The incidence
THE ROLE OF CONTEMPORARY IMAGING AND HYBRID METHODS IN THE DIAGNOSIS OF CUTANEOUS MALIGNANT MELANOMA(CMM) AND MERKEL CELL CARCINOMA (MCC) I.Kostadinova, Sofia, Bulgaria CMM some clinical facts The incidence
Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ]
![Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ] Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ]](/thumbs/82/86783199.jpg) CS Tumor Size Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ] Note: the specific tumor size as documented in the medical record. If the ONLY information regarding tumor size is the physician's
CS Tumor Size Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ] Note: the specific tumor size as documented in the medical record. If the ONLY information regarding tumor size is the physician's
3. A plane is an imaginary line dividing the body into.
 CHAPTER 2 Multiple Choice Choose the one alternative that best completes the statement or answers the question. 1. Knowing the exact body region where pain is located can help a physician determine the.
CHAPTER 2 Multiple Choice Choose the one alternative that best completes the statement or answers the question. 1. Knowing the exact body region where pain is located can help a physician determine the.
Canadian Scientific Journal. Intraoperative color detection of lymph nodes metastases in thyroid cancer
 Canadian Scientific Journal 2 (2014) Contents lists available at Canadian Scientific Journal Canadian Scientific Journal journal homepage: Intraoperative color detection of lymph nodes metastases in thyroid
Canadian Scientific Journal 2 (2014) Contents lists available at Canadian Scientific Journal Canadian Scientific Journal journal homepage: Intraoperative color detection of lymph nodes metastases in thyroid
IAEA Pediatric Radiation Oncology Training Dr Laskar Version 1 June SOFT TISSUE SARCOMA (Non Rhabdomyosarcoma)
 SOFT TISSUE SARCOMA (Non Rhabdomyosarcoma) Soft Tissue structures Fat, Muscles, Fibrous tissue, Blood vessels, Supporting cells of peripheral nervous system Soft Tissue Sarcomas:- embryologically arise
SOFT TISSUE SARCOMA (Non Rhabdomyosarcoma) Soft Tissue structures Fat, Muscles, Fibrous tissue, Blood vessels, Supporting cells of peripheral nervous system Soft Tissue Sarcomas:- embryologically arise
University of Groningen
 University of Groningen Nodular Histologic Subtype and Ulceration are Tumor Factors Associated with High Risk of Recurrence in Sentinel Node-Negative Melanoma Patients Faut, Marloes; Wevers, Kevin; van
University of Groningen Nodular Histologic Subtype and Ulceration are Tumor Factors Associated with High Risk of Recurrence in Sentinel Node-Negative Melanoma Patients Faut, Marloes; Wevers, Kevin; van
Sentinel lymph node (SLN) biopsy is a wellestablished
 ORIGINAL ARTICLE DISCORDANT LYMPHATIC DRAINAGE PATTERNS REVEALED BY SERIAL LYMPHOSCINTIGRAPHY IN CUTANEOUS HEAD AND NECK MALIGNANCIES Alliric I. Willis, MD, John A. Ridge, MD, PhD Department of Surgical
ORIGINAL ARTICLE DISCORDANT LYMPHATIC DRAINAGE PATTERNS REVEALED BY SERIAL LYMPHOSCINTIGRAPHY IN CUTANEOUS HEAD AND NECK MALIGNANCIES Alliric I. Willis, MD, John A. Ridge, MD, PhD Department of Surgical
YOU MUST BRING GLOVES FOR THIS ACTIVITY
 ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. 2) Observe and sketch histology slide
ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. 2) Observe and sketch histology slide
Day 5 Respiratory & Cardiovascular: Respiratory System
 Day 5 Respiratory & Cardiovascular: Respiratory System Be very careful not to damage the heart and lungs while separating the ribs! Analysis Questions-Respiratory & Cardiovascular Log into QUIA using your
Day 5 Respiratory & Cardiovascular: Respiratory System Be very careful not to damage the heart and lungs while separating the ribs! Analysis Questions-Respiratory & Cardiovascular Log into QUIA using your
VESSELS: GROSS ANATOMY
 ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. 2) Observe and sketch histology slide
ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. 2) Observe and sketch histology slide
ORIGINAL ARTICLE. Patterns of Recurrence in Patients With Melanoma After Radical Lymph Node Dissection
 ORIGINAL ARTICLE Patterns of Recurrence in Patients With Melanoma After Radical Lymph Node Dissection Nir Nathansohn, MD, MHA; Jacob Schachter, MD; Haim Gutman, MD Hypothesis: Previous interventions (excisional
ORIGINAL ARTICLE Patterns of Recurrence in Patients With Melanoma After Radical Lymph Node Dissection Nir Nathansohn, MD, MHA; Jacob Schachter, MD; Haim Gutman, MD Hypothesis: Previous interventions (excisional
ANATYOMY OF The thigh
 ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
Time Course and Pattern of Metastasis of Cutaneous Melanoma Differ between Men and Women
 Time Course and Pattern of Metastasis of Cutaneous Melanoma Differ between Men and Women Liljana Mervic 1,2 * 1 Department of Dermatology, Center of Dermatooncology, University of Tüebingen, Germany, 2
Time Course and Pattern of Metastasis of Cutaneous Melanoma Differ between Men and Women Liljana Mervic 1,2 * 1 Department of Dermatology, Center of Dermatooncology, University of Tüebingen, Germany, 2
ORIGINAL ARTICLE. (SLN) biopsy is revolutionizing
 ORIGINAL ARTICLE Management of Malignant Melanoma of the Head and Neck Using Dynamic Lymphoscintigraphy and Gamma Probe Guided Sentinel Lymph Node Biopsy Grant W. Carlson, MD; Douglas R. Murray, MD; Robert
ORIGINAL ARTICLE Management of Malignant Melanoma of the Head and Neck Using Dynamic Lymphoscintigraphy and Gamma Probe Guided Sentinel Lymph Node Biopsy Grant W. Carlson, MD; Douglas R. Murray, MD; Robert
Melanoma. Kaushik Mukherjee MD A. Scott Pearson MD
 Melanoma Kaushik Mukherjee MD A. Scott Pearson MD Disclosures You still have to study Not all inclusive No Western blots Extensive use of Google Image Search and Sabiston Melanoma Basics 8 th most common
Melanoma Kaushik Mukherjee MD A. Scott Pearson MD Disclosures You still have to study Not all inclusive No Western blots Extensive use of Google Image Search and Sabiston Melanoma Basics 8 th most common
Gateway to the upper limb. An area of transition between the neck and the arm.
 Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Study on Efficacy of Preoperative Ultrasonography for Axillary Lymph Node Involvement In Breast Carcinoma
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 4 Ver. II. (Apr. 2014), PP 01-05 Study on Efficacy of Preoperative Ultrasonography for Axillary
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 4 Ver. II. (Apr. 2014), PP 01-05 Study on Efficacy of Preoperative Ultrasonography for Axillary
Prognostic Variables and Surgical Management of Foot Melanoma: Review of a 25-Year Institutional Experience
 Virginia Commonwealth University VCU Scholars Compass Surgery Publications Dept. of Surgery 11 Prognostic Variables and Surgical Management of Foot Melanoma: Review of a 5-Year Institutional Experience
Virginia Commonwealth University VCU Scholars Compass Surgery Publications Dept. of Surgery 11 Prognostic Variables and Surgical Management of Foot Melanoma: Review of a 5-Year Institutional Experience
Anatomy and Physiology Unit 1 Review Sheet
 Anatomy and Physiology Unit 1 Review Sheet Chapter 1 Name Date Hour 1. investigates the body's structure, whereas investigates the processes or functions of living things. A. Physiology, cytology B. Physiology,
Anatomy and Physiology Unit 1 Review Sheet Chapter 1 Name Date Hour 1. investigates the body's structure, whereas investigates the processes or functions of living things. A. Physiology, cytology B. Physiology,
Surgery for Melanoma and What s on the Horizon
 and What s on the Horizon Giorgos C. Karakousis, M.D. Assistant Professor of Surgery Perelman School of Medicine at the University of Pennsylvania Background/Overview 76,870 cases of melanoma estimated
and What s on the Horizon Giorgos C. Karakousis, M.D. Assistant Professor of Surgery Perelman School of Medicine at the University of Pennsylvania Background/Overview 76,870 cases of melanoma estimated
Disclosures. SLNB for Melanoma 25/02/2014 SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION
 8 th Canadian Melanoma Conference February 22, 2014 Rimrock Resort Hotel, Banff, Alberta SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION Christopher Bichakjian,
8 th Canadian Melanoma Conference February 22, 2014 Rimrock Resort Hotel, Banff, Alberta SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION Christopher Bichakjian,
PAPER. Is Completion Lymphadenectomy After a Positive Sentinel Lymph Node Biopsy for Cutaneous Melanoma Always Necessary?
 PAPER Is Completion Lymphadenectomy After a Positive Sentinel Lymph Node Biopsy for Cutaneous Melanoma Always Necessary? Nahel Elias, MD; Kenneth K. Tanabe, MD; Arthur J. Sober, MD; Michele A. Gadd, MD;
PAPER Is Completion Lymphadenectomy After a Positive Sentinel Lymph Node Biopsy for Cutaneous Melanoma Always Necessary? Nahel Elias, MD; Kenneth K. Tanabe, MD; Arthur J. Sober, MD; Michele A. Gadd, MD;
Sentinel Lymph Node Biopsy for the T1 (Thin) Melanoma: Is It Necessary?
 Sentinel Lymph Node Biopsy for the T1 (Thin) Melanoma: Is It Necessary? Maurice Y. Nahabedian, MD Anthony P. Tufaro, MD Paul N. Manson, MD The use of sentinel lymph node biopsy for the T1 melanoma is controversial.
Sentinel Lymph Node Biopsy for the T1 (Thin) Melanoma: Is It Necessary? Maurice Y. Nahabedian, MD Anthony P. Tufaro, MD Paul N. Manson, MD The use of sentinel lymph node biopsy for the T1 melanoma is controversial.
Muscle Action Origin Insertion Nerve Innervation Chapter Page. Deltoid. Trapezius. Latissimus Dorsi
 Muscle Action Origin Insertion Nerve Innervation Chapter Page All Fibers Abduct the shoulder (glenohumeral joint) Deltoid Anterior Fibers Flex the shoulder (G/H joint) Horizontally adduct the shoulder
Muscle Action Origin Insertion Nerve Innervation Chapter Page All Fibers Abduct the shoulder (glenohumeral joint) Deltoid Anterior Fibers Flex the shoulder (G/H joint) Horizontally adduct the shoulder
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Melanoma Case Scenario 1
 Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Dr Rosalie Stephens. Mr Richard Martin. Medical Oncologist Auckland City Hospital Auckland
 Dr Rosalie Stephens Medical Oncologist Auckland City Hospital Auckland Mr Richard Martin General Surgeon Melanoma Unit Team Waitemata District Health Board Auckland 8:30-9:25 WS #99: Interactive Case Studies
Dr Rosalie Stephens Medical Oncologist Auckland City Hospital Auckland Mr Richard Martin General Surgeon Melanoma Unit Team Waitemata District Health Board Auckland 8:30-9:25 WS #99: Interactive Case Studies
ANATYOMY OF The thigh
 ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 1, 2 and 3 are From the lumber plexus 5- Intermediate cutaneous
ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 1, 2 and 3 are From the lumber plexus 5- Intermediate cutaneous
Clinical and Pathological Features of Cutaneous Malignant Melanoma: A Retrospective Analysis of 124 Japanese Patients
 Clinical and Pathological Features of Cutaneous Malignant Melanoma: A Retrospective Analysis of 24 Japanese Patients Yoshie Kuno, Kazuyuki Ishihara, Naoya Yamazaki and Kiyoshi Mukai 2 'Dermatology Division
Clinical and Pathological Features of Cutaneous Malignant Melanoma: A Retrospective Analysis of 24 Japanese Patients Yoshie Kuno, Kazuyuki Ishihara, Naoya Yamazaki and Kiyoshi Mukai 2 'Dermatology Division
Melanoma Case Scenario 1
 Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Sentinel Lymph Node Biopsy for Breast Cancer
 Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
Clinical Pathological Conference. Malignant Melanoma of the Vulva
 Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Contradiction of Clinical Expectations in Lymphoscintigraphy Sentinel Node Mapping in Detecting Microscopic Melanoma Metastasis
 Case Report 474 Contradiction of Clinical Expectations in Lymphoscintigraphy Sentinel Node Mapping in Detecting Microscopic Melanoma Metastasis John WC Chang, MD; Hsui-Fong Chiang, RN; Yung-Feng Lo 1,
Case Report 474 Contradiction of Clinical Expectations in Lymphoscintigraphy Sentinel Node Mapping in Detecting Microscopic Melanoma Metastasis John WC Chang, MD; Hsui-Fong Chiang, RN; Yung-Feng Lo 1,
Anatomical Language. Human Anatomy & Physiology Honors Ms. Chase
 Anatomical Language Human Anatomy & Physiology Honors 2014 2015 Ms. Chase Anatomical Position Body erect, feet slightly apart, palms facing forward, thumbs point away from the body DIRECTIONAL TERMS Allow
Anatomical Language Human Anatomy & Physiology Honors 2014 2015 Ms. Chase Anatomical Position Body erect, feet slightly apart, palms facing forward, thumbs point away from the body DIRECTIONAL TERMS Allow
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 1: Proximal bones, plexuses and patterns
 213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 1: Proximal bones, plexuses and patterns CLAVICLE Examine an isolated clavicle and compare it with a clavicle on an articulated skeleton. Viewed from above,
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 1: Proximal bones, plexuses and patterns CLAVICLE Examine an isolated clavicle and compare it with a clavicle on an articulated skeleton. Viewed from above,
9. Which term refers to the back? A. Inferior B. Lateral C. Posterior D. Peripheral 10. The heart is to the lungs. A. dorsal B. superior C.
 1 Student: 1. Which term refers to the study of how an organ functions? A. Anatomy B. Physiology C. Ecology D. Homeostasis 2. Observing the parts of the brain would be part of the study of A. homeostasis.
1 Student: 1. Which term refers to the study of how an organ functions? A. Anatomy B. Physiology C. Ecology D. Homeostasis 2. Observing the parts of the brain would be part of the study of A. homeostasis.
category cm0. Category will ensure it T1 melanoma. 68 Retinoblastoma
 AJCC 8 th Edition Chapter 1 Principles of Cancer Staging: Node Status Not Required in Rare Circumstances Clinical Staging, cn Category For some cancer sites in which lymph node involvement is rare, patients
AJCC 8 th Edition Chapter 1 Principles of Cancer Staging: Node Status Not Required in Rare Circumstances Clinical Staging, cn Category For some cancer sites in which lymph node involvement is rare, patients
Surgical Margins in Cutaneous Melanoma (2 cm Versus 5 cm for Lesions Measuring Less Than 2.1-mm Thick)
 1941 Surgical Margins in Cutaneous Melanoma (2 cm Versus 5 cm for Lesions Measuring Less Than 2.1-mm Thick) Long-Term Results of a Large European Multicentric Phase III Study David Khayat, M.D., Ph.D.
1941 Surgical Margins in Cutaneous Melanoma (2 cm Versus 5 cm for Lesions Measuring Less Than 2.1-mm Thick) Long-Term Results of a Large European Multicentric Phase III Study David Khayat, M.D., Ph.D.
3 Mohammad Al-Mohtasib Areej Mosleh
 3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
