NEUROMUSCULAR JUNCTION EFFECTS
|
|
|
- Opal Morris
- 6 years ago
- Views:
Transcription
1 Chapter Twelve NEUROMUSCULAR JUNCTION EFFECTS DOES PB PRODUCE NEUROMUSCULAR JUNCTION CHANGES? Acetylcholinesterase (AChE) inhibitors, including PB, produce acute destructive changes at the neuromuscular junction, the site of connection between nerve cells and muscle fibers, at which nerve cells signal muscles to contract. Because studies of the neuromuscular junction require microscopic inspection of muscle tissue and tests of electrical and chemical properties of the neuromuscular junction at a fine level, studies investigating these alterations have not been performed in living humans but primarily in muscle preparations from rats and frogs exposed to PB or other AChE inhibitors (also called anticholinesterases ). These studies have examined the effects of PB and other carbamate AChE inhibitors, sarin and other OP nerve-agent AChE inhibitors, and nonnerveagent OP (e.g., pesticide) AChE inhibitors on the muscle and neuromuscular junction. These observed alterations fall into several classes. Histopathological and ultrastructural changes are changes in structure and fine structure of the muscle and nerve muscle junction observed by light and electron microscopy. Some of the muscle changes are referred to as AChE inhibitor myopathy. Prejunctional changes refer to changes that occur on the nerve or signaling side of the neuromuscular junction. Prejunctional or presynaptic changes include changes in production and release of the neurotransmitter acetylcholine (ACh); or withdrawal of nerve branches from the motor endplate (muscle side). Postjunctional or postsynaptic changes refer to changes that occur on the muscle or signal-receiving side of the neuromuscular junction. Since the signal is received by binding of ACh to receptors on the postjunctional side, changes in receptor sensitivity or density are examples of postjunctional changes. These changes are reflected in alterations in currents and voltages produced, for 163
2 164 Pyridostigmine Bromide instance, by binding the ACh to the receptor; and changes in time constants of electrical response measured at the motor endplate. Clinical or behavioral changes are changes in muscle function or strength believed to result from alterations at the neuromuscular junction. Many of the alterations observed are similar regardless of which AChE inhibitor is used. However, specific drugs differ to some degree in their effect even within a class of anticholinesterase chemicals (for instance, different carbamates, or different organophosphorus nerve agents may produce effects that differ in detail) (Albuquerque, 1986). For example, differences may occur in how extensive certain changes are, in which specific muscles are affected and to what degree, in the time-course of the effect, and in the response to a change in dosage. Differences are not only quantitative but may also be qualitative, and a drug that produces a more profound change than another when examined by one technique (for instance, by examining receptor blocking) may produce a less pronounced change when viewed through the lens of another technique (for instance, AChE inhibition, or MEPP rise time ). The existence of marked, and in some instances long-lasting, changes at the neuromuscular junction is unequivocal. (These findings derive primarily from animal studies using high doses of AChE inhibitors.) The clinical significance these changes may have is less clear. Some have suggested that they may be responsible for a putative reduction in the rate of cure of myasthenics with thymectomy since the onset of treatment with PB (Rockefeller, 1997; Phillips and Torner, 1996). Others have suggested that these alterations may be responsible for symptoms in ill PGW veterans (Tiedt, 1994). In fact, current information is sufficient neither to confirm nor exclude long-lasting structural and/or functional effects at the motor endplate in humans with the doses and durations of PB treatment used in PGW veterans. Current information is also insufficient to confirm or exclude a role for changes in symptoms, such as fatigue or joint pain, reported by PGW veterans. ( Joint pain might or might not be produced by abnormal regulation of signals to opposing muscle groups during rest or activity. Abnormal strength or timing of signals could result in alterations in the pattern of highly coordinated contraction of some muscles with relaxation of others that occurs during normal activity and at rest.) Concomitant exposure to other AChE-inhibiting drugs, such as sarin or organophosphorus pesticides, could conceivably cause, modify, or amplify effects on the motor endplate. Again, while existing evidence does not exclude long-lasting biological and clinical effects on the motor endplate with PB use, neither is there persuasive evidence favoring such effects. Data to address the clinical significance and time-course of such changes as those seen in animal studies remain inadequate.
3 Neuromuscular Junction Effects 165 This chapter does not purport to contain a wholly comprehensive review of the literature regarding AChE inhibitors and motor endplate alterations. Rather, a sample of available information is provided to impart the nature of changes seen, the similarity and variation of alterations observed with different types of AChE inhibitors, and some of what is known regarding the time-course of these changes. Effects not only of PB but of other AChE inhibitors are reviewed. Because not all measures have been performed with PB, including assessments of long-term effects, it is useful to describe effects both for PB and for other AChE inhibitors. STUDIES WITH AChE INHIBITORS Animal Studies Animal studies (largely using muscle from rats given AChE inhibitors, such as PB; occasionally from frogs and other species treated with cholinesterase inhibitors) constitute the bulk of the evidence indicating changes in the neuromuscular junction that occur with use of PB and other anticholinesterases. Histopathological and Ultrastructural Changes: Postsynaptic and Myopathic Changes. PB has been shown to lead to light and electron microscopic changes in rats. These changes are primarily postsynaptic (causing alterations at the muscle side of the nerve-muscle junction), and myopathic (destructive to muscle tissue). Some investigators find the presynaptic region (the nerve side of the nerve-muscle junction) to be less affected. The nature of the changes in the muscle of rats given high-dose PB (98 mg/kg/day orally in feed 76 times the Gulf War daily dose and 228 times the per-dose Gulf War dose) include alteration in the striped appearance of muscle filaments and changes in the appearance of subcellular structures like mitochondria and sarcoplasmic reticulum. Some evidence of regeneration appears by 15 days, partially reversing the destructive changes. 1 1 In rats given high-dose PB (98 mg/kg/day administered orally in feed), unlike control animals, degenerative changes in muscle are seen with light and electron microscopy. Under the light microscope, approximately 1 percent of muscle fibers (or myofibers ) from the diaphragm were damaged. (Such damage is made evident by loss of striation or stripe pattern of myofilament architecture and presence of many centralized, highly convoluted cell nuclei in the muscle cells (Bowman, Schuschereba, et al., 1989).) On electron microscopy, myofibers were seen to contain swollen mitochondria (mitochondria are energy-producing organelles or subcellular structures) with accumulation of internal inclusions and numerous inflammatory cells (Bowman, Schuschereba, et al., 1989). By two days of PB administration, degenerative changes were seen in the postsynaptic region of the neuromuscular junction. By seven days, myofibers had additional changes. Myofibers were still damaged, with centralized nuclei, dilated sarcoplasmic reticulum, and disruption of Z bands ; and myofibers had increased glycogen. By 15 days, damaged fibers appeared to be in the process of regeneration, evidenced by large nuclei with dispersed chromatin and prominent nucleoli with
4 166 Pyridostigmine Bromide It has been suggested that some adaptive mechanism may be responsible for the partial reversal of early myopathy even in the presence of continued treatment. Seventy-four percent or more inhibition of AChE was observed throughout the study (Bowman, Schuschereba, et al., 1989), so that the reversal of myopathy cannot be the result of lessened cholinesterase inhibition, for instance from heightened metabolism of PB. A second study of rats with somewhat lower doses of PB (20 and 40 mg/kg 47 and 93 PGW dose-equivalents, respectively) but still greater than 50 percent AChE inhibition confirms the presence of changes on light microscopy. 2 Changes were unexpectedly more severe in the group with the lower dose of PB, for reasons that are unclear. The earliest changes could be detected immediately after the two-hour period required for complete inactivation (Gebbers, Lotscher, et al., 1986). In a third study on rat diaphragm, PB producing 78 percent reduction in AChE activity was again seen to induce marked changes, most directly adjacent to the synapse, with damage greatly reduced a few microns away and some normalappearing muscle filaments microns away. 3 Stimulated muscles (in which the nerve leading to the muscle was stimulated to produce a signal) showed the same pattern of organelle damage and myofibril disorganization, but the damage was more severe and the affected area more extensive. Damage was well developed 30 minutes after PB administration and was maximal at two hours. Myopathic or destructive changes can involve the endplate region of nearly all muscle fibers, but light microscopy revealed necrosis in only about 10 percent of fibers sampled, even after nearly complete ACh inhibition. It is unclear why some nerve fibers degenerate but most are preserved in spite of marked abnormalities in the fine structure of the fibers ( ultrastructural dense chromatin rims; sarcoplasmic reticulum in the postsynaptic region appeared less dilated. The presynaptic region appeared grossly normal at all times in this study. 2 Changes included acute focal necrosis (cell death) of disseminated single fibers and groups of fibers, mixed leukocyte infiltrates, and marked changes in motor endplates in skeletal muscle; changes were greater in diaphragm than in quadriceps muscle in this study (Gebbers, Lotscher, et al., 1986) (though another study found similar changes in three tested muscle types differing in the amount of fast- and slow-twitch muscle fibers, namely diaphragm, soleus, and extensor digitorum longus (Hudson, Foster, et al., 1985)). 3 Changes included supercontracted sarcomeres near the endplate region, subjunctional areas marked by disorganization of the myofibrillar apparatus, streaming of the Z-bands, and mitochondrial swelling. The most severely affected mitochondria were observed proximal to the junctional folds with progressively less severe alterations away from the junction. Regions closest to the synaptic cleft had the most severely damaged organelles. Essentially all mitochondria immediately adjacent to the neuromuscular junction exhibited marked intracristal swelling and some mitochondria showed an apparent absence of matrix. Contractile filaments were supercontracted with only remnants of Z-line material visible. The ultrastructural damage was greatly reduced within a few microns from this region, and by microns from the subjunctional membrane it was possible to detect precisely aligned sarcomeres and normal intracellular organelles (Adler, Hinman, et al., 1992).
5 Neuromuscular Junction Effects 167 abnormalities). The incidence of necrotic fibers is dose-dependent, suggesting that some muscle fibers may be especially sensitive to AChE inhibitors, perhaps related to the threshold or firing pattern of the muscle cell (or motor unit ) (Adler, Hinman, et al., 1992). Importantly, PB administration in rats produced marked postsynaptic ultrastructural changes, 4 even when no animals displayed outward signs of anticholinesterase intoxication (Hudson, Foster, et al., 1985). Presynaptic Changes. Some neuromuscular junctions of all three muscles tested in rats underwent partial denervation (withdrawal of nerve terminal branches from the muscle) following either acute injection of PB (1 mg/kg or 2.3 times the Gulf War dose by single injection) or subchronic delivery of PB by osmotic minipump (with constant 70 percent inhibition throughout a 14-day period) (Hudson, Foster, et al., 1985). The three tested muscles were the diaphragm, the soleus (a posterior lower leg muscle), and the extensor digitorum longus (which extends the toes). Together these muscles include fast-twitch and slow-twitch fiber types. Withdrawal of nerve branches constitutes a presynaptic change, because the nerve branches are from the signaling side. Although recovery was in process and in some cases reportedly complete at the termination of the follow-up 60 days after cessation of treatment, some changes were still present at this time (Hudson, 1985), primarily histological changes in muscle. (This is the longest identified period of follow-up after cessation of PB treatment in these studies. A related study using PB (0.36 mg/kg by single subcutaneous injection, or subacute PB by osmotic minipump 0.84 of a Gulf War dose) noted that intrusion of processes from non nerve supporting or glial cells termed Schwann cells in the synaptic region (the synaptic cleft ) and partial withdrawal of nerve terminals acted as a type of denervation, effectively reducing the amount of synapse surface available for optimal functioning (Hudson, Foster, et al., 1985). 5 4 Postsynaptic changes with acute PB treatment (0.36 mg/kg by single subcutaneous injection) included rarefied areas in mitochondria, and occasional mitochondria were associated with membranous lamellar structures. Subjunctional myofibrillar structure was disorganized in occasional neuromuscular junctions. Subacute treatment with PB (for two days) led to highly variable changes, with swelling or rarefaction of the mitochondrial matrix, some grossly altered mitochondria with multilayered membrane structures in subjunctional regions, and similar variability within each of three tested muscle types. There was loss of myofibrillar organization in some neuromuscular junctions, with more subtle changes in Z-lines, myosin, and actin filament organization in others. 5 Synaptic vesicles (vesicles or inpouchings of membrane that contain neurotransmitters) were so densely packed that there was no space to accommodate cytoplasm in the nerve terminal. With acute treatment, mitochondria presynaptically were either similar to the controls or were characterized by swollen regions in neuromuscular junctions of all three muscles (Hudson, Foster, et al., 1985). With subacute treatment, there was local separation of pre- and postsynaptic components. In some regions, crests of several junctional folds lacked the typical apposing nerve terminal, and
6 168 Pyridostigmine Bromide Studies in rats, using neostigmine (a carbamate compound related to pyridostigmine), have also noted significant presynaptic alterations 6 including depletion of neurotransmitter-containing vesicles (Hudson, Rash, et al., 1978). It has been shown that destructive ultrastructural changes such as those described require that ACh interact with its receptor. These changes were eliminated if the nerve synapsing on the neuromuscular junction was cut, if ACh receptors at the endplate were chemically inactivated (by the agent alpha bungarotoxin ), if oxime treatment was administered promptly to pull the AChE inhibitor off the AChE, or if a receptor blocker (namely d-tubocurarine, a paralytic agent) was simultaneously administered, thus preventing spontaneous fasciculations of the muscle (Salpeter, Kasprzak, et al., 1979; Gebbers, Lotscher, et al., 1986; Adler, Hinman, et al., 1992; Hudson, Rash, et al., 1978). Moreover, damage is promoted by nerve stimulation (Adler, Hinman, et al., 1992). These findings indicate that the destructive changes may result from increased synaptic activity because of heightened availability of ACh and that they depend on successful interaction of ACh with its receptor. It has been suggested that the diaphragm may be particularly vulnerable because of its constant activity (Gebbers, Lotscher, et al., 1986; Dettbarn, 1984). The condition may be more pronounced in slow-twitch rather than fast-twitch muscle (Wecker and Dettbarn, 1976), or this finding may simply reflect differences in muscle activity. Myopathy in in vitro muscles occurs both in the absence and presence of nerve stimulation. Although nerve stimulation facilitates this effect, so evidently does spontaneous muscle twitching or fasciculation (Adler, Hinman, et al., 1992), which may result when spontaneously released or leaked neurotransmitter binds to the receptor. While the detailed mechanism of the muscle damage or myopathy that results when AChE inhibitors (such as PB) are given is not well understood, this damage is known to be mediated through calcium (Yamaguchi, Robson, et al., 1983; Toth, Karscu, et al., 1983; Dettbarn, 1984; Kawabuchi, 1982; Salpeter, Kaszprzak, et al., 1979; Leonard and Salpeter, 1979). Several possible mechanisms have been postulated. 7 Schwann cells frequently occupied the position normally occupied by the nerve terminal (Hudson, Foster, et al., 1985). 6 Presynaptic changes, in addition to synaptic vesicle depletion, included appearance of numerous coated vesicles and membrane cisternae indicating continued nerve terminal hyperactivity (Hudson, Rash, et al., 1978); degeneration and partial recovery of the nerve axon were observed with chronic treatment (Hudson, Rash, et al., 1978). 7 For instance, membrane phospholipase may be activated by calcium, directly or through calmodulin or phosphatidylinositol; the latter is split into diacylglycerol and inositol triphosphate, with the latter activating calcium, and calcium in turn activating protein kinases. Calcium in muscle fibers may activate an endogenous neutral protease that can catalyze degradation of myofibrils and Z-lines. Excess depolarization of endplate receptors may enhance calcium influx. PB may also directly influence neuromuscular transmission, acting as a weak agonist, thus further increasing
7 Neuromuscular Junction Effects 169 Other AChE Inhibitors. Similar patterns of damage to skeletal muscle have been reported in experiments with other carbamates (e.g., neostigmine) (Osame, Kawabuchi, 1975; Kawabuchi, Osame, et al., 1976; Kawabuchi, 1982; Engel, Lambert, and Santa, 1973), with OPs (Gebbers, Lotscher, et al., 1986; Salpeter, Kasprzak, et al., 1979; Preusser, 1967; Laskowski, Olson, et al., 1975; Laskowski, Olson, et al., 1977; Fischer, 1968; Gebbers, Lotscher, et al., 1986; Dettbarn, 1984; Feng, Rogers, et al., 1973; Fenichel, Kibler, et al., 1972; Fenichel, Kibler, et al., 1974; Ariens, Meeter, et al., 1969) like paraoxon (Laskowski, Olson, et al., 1975; Laskowski, Olson, et al., 1977; Fenichel, Kibler, et al., 1974); DFP (Feng, Rogers, et al., 1973), and with the nerve agents tabun and soman (Gebbers, Lotscher, et al., 1986; Preusser, 1967). For example, one study found that paraoxon, as well as OP cholinesterase inhibitors, produced progressive myopathy in skeletal muscle (Wecker and Dettbarn, 1976). 8 Partial reversibility of these muscle damaging effects has been commonly reported. For instance, in rats exposed to DFP for two weeks, by day 14 there was loss of sensitivity to the necrotizing actions in all the muscles tested (diaphragm, soleus, extensor digitorum longus) (Gupta, Patterson, et al., 1986). Typically, some reversal of the damage occurs even when AChE-inhibiting agents continue to be given. As noted previously, AChE-inhibiting agents that differ substantially from one another chemically produce similar effects, supporting presence of a mechanism involving heightened acetylcholinergic activity. Moreover, direct ACh enhancement produces the same effect (Fenichel, Kibler, et al., 1974). Nonetheless, neostigmine was shown to have direct action on motor nerve endings 9 in addition to inhibiting AChE, suggesting that some mechanisms idiosyncratic to individual chemicals may also be operative (Braga, Rowan, et al., 1993). Variability of the Effect. Some studies report differences from one muscle type to another in the ultrastructural (pertaining to the fine structure of tissue, seen with an electron microscope) pre- and postsynaptic alterations of the neuromuscular junction. These differences have been attributed to different amounts of fast- versus slow-twitch (red versus white) muscle fibers or to differences in muscle activity that occur with the different types of muscles. intracellular calcium concentration (Gebbers, Lotscher, et al., 1986; Chang and Neumann, 1976; Yamaguchi, Robson, et al., 1983; Toth, Karscu, et al., 1983; Akaike, Ikeda, et al., 1984). 8 Myopathic changes included presence of splitting fibers, then enlargement of central nuclei, more-intense splitting and breakdown of fiber architecture, and finally total fiber necrosis and phagocytosis (Wecker and Dettbarn, 1976). There was significant recovery of enzyme activity within 24 hours. It was suggested that there may be a critical period of cholinesterase activity to initiate the myopathic process. 9 Direct actions included blocking delayed rectifier potassium channels and enhancing transmitter release (Braga, Rowan, et al., 1993).
8 170 Pyridostigmine Bromide In one study, alterations of the neuromuscular junction occurred in diaphragm, soleus, and extensor digitorum longus with acute PB (0.36 mg/kg sc or 0.84 Gulf War doses) or subacute PB (two days, 10 mg/ml PB by subcutaneously implanted osmotic minipump); both doses produced percent whole blood cholinesterase depression). Changes occurred in each muscle of every animal examined, but there was considerable variation in the extent of damage even within individual fibers. The severity varied from fiber to fiber, but variability appeared random and not strongly related to the specific fiber type or to the dosage regimen (though effects in diaphragm muscle may have been greater) (Hudson, Foster, et al., 1985). No information was given to allow determination of the effect of muscle fiber activity on these changes. Mitochondrial Effects. Increased cholinergic activity induced by PB (perhaps through increased intracellular free calcium) has been reported to cause deterioration in mitochondrial function resulting in heart and muscle damage. One report suggests that this may be mediated by reductions in the mitochondrialbound enzyme hexokinase, which is closely linked to oxidative metabolism in the mitochondria. PB led to a reduction in mitochondrial hexokinase in rats tibialis anterior muscle (a muscle in the anterior lower leg) but not in heart muscle. (30 PGW doses led to 60 percent reduction of hexokinase in tibialis anterior muscle, a reduction that was statistically significant (p <.005). Hexokinase was reduced by only 10 percent in the heart, a difference that was not significant (Glass-Marmor and Beitner, 1996).) Prejunctional Effects: Changes in Neurotransmitter Production. Choline acetyltransferase is the enzyme that catalyzes or facilitates the final step in ACh production (Albuquerque, Boyne, et al., 1983). Choline acetyltransferase activity was increased in muscle (in intramuscular nerves) following administration of the OP DFP (Gupta, Patterson, et al., 1986) and following nerve agent administration (Albuquerque, Boyne, et al., 1983); this increased activity should lead to increased production of ACh, an effect that could potentiate the AChE-inhibiting effects of these agents. No data were supplied on the effect of PB on choline acetyltransferase activity. The relative timecourse of this effect, and the relation to the time-course of multiple potentially downregulatory effects, was not elucidated. Prejunctional Effects: Changes in Neurotransmitter Release. Most studies evaluating changes at the motor endplate employ high doses of PB, leading to at least 50 percent AChE inhibition. Data are limited on effects of lower doses of PB, doses more comparable to those employed with PGW veterans. Studies have found marked but reversible reduction in the amount of ACh released by each nerve impulse with five to seven days of (1 mg/kg) neostigmine given to rats (Roberts and Thesleff, 1969). Also, reduction in quantal
9 Neuromuscular Junction Effects 171 content of nerve-stimulated endplate potentials has been shown (endplate potentials are changes in voltage on the postjunctional side produced by release of multiple quanta, or vesicles of ACh, at the presynaptic side following a signal by the postsynaptic neuron) in rat extensor digitorum muscle (Tiedt, Albuquerque, et al., 1978). It has been suggested that chronic use of carbamates in myasthenia gravis patients may depress neuromuscular transmission in part because of a low endplate potential quantal content (Roberts and Thesleff, 1969), a form of downregulation of the acetylcholine system in response to excessive ACh activity; however, reduced transmitter release in one study had returned almost to normal after days of continued treatment (Tiedt, Albuquerque, et al., 1978). Postjunctional Effects: Electrophysiological and in Receptor Changes. ACh binds to receptors at the postjunctional side of the neuromuscular junction, inducing electrical currents and changes in voltage in the motor endplate (postjunctional membrane). If these changes are adequate, they result in contraction of the muscle fiber. A single vesicle of ACh may be randomly released; one vesicle contains one quantum of ACh, which comprises several thousand ACh molecules, representing the smallest amount of ACh released (Kuffler and Yoshikami, 1975). If a nerve cell is excited and fires, producing an action potential to signal to the muscle, about 200 quanta are released into the synapse or neuromuscular junction (Kuffler, Nicholls, et al., 1984). Release of a single quantum by the prejunctional nerve leads to relatively small changes in current at the motor endplate. (The current is produced when ACh binds to receptors at the motor endplate, leading ions to traverse specialized ion channels in the membrane.) This change is termed a miniature endplate current (MEPC), and the size of the current is determined by fixing the voltage at the endplate. Alternatively, the endplate current can be held constant to determine the change in voltage, or miniature endplate potential (MEPP). If a nerve cell fires (generates an action potential), the complement of about 200 quanta produces larger changes in current and voltage termed the endplate current and endplate potential, respectively. Nerves that signal muscle cells may be artificially stimulated to fire, and endplate currents and potentials can then be measured. MEPCs and MEPPs may be measured when random quanta are released. Moreover, ACh or other cholinergic agonists can be directly applied to the endplate to determine receptor sensitivity, by measuring changes in currents or voltages. Information from MEPCs and from endplate currents differs slightly; for instance, a MEPC may be reduced if there are fewer ACh molecules in a quantum, or if there is reduced sensitivity of the receptor to ACh. An endplate current may be reduced
10 172 Pyridostigmine Bromide if there are fewer ACh molecules in a quantum, fewer quanta for each action potential, or reduced receptor sensitivity. Moreover, amplitude is not the only property of currents and potentials they also have temporal properties. Studies have looked both at the electrophysiological measures with spontaneous or induced signaling of nerve to muscle and at receptor sensitivity. In several studies of rat diaphragm, soleus, and extensor digitorum muscle, PB led to prolongation of MEPC decay (threefold to fourfold slowing), with small (23 percent) increases in MEPC amplitude (Adler, Hinman, et al., 1992); and MEPP with a slow rise-time (> 1 ms) and low frequency (Meshul, Boyne, et al., 1985). Levels of AChE inhibition were higher than in PB-treated PGW veterans, e.g., 78 percent reduction in AChE activity (Adler, Hinman, et al., 1992). This effect was seen not only with PB but with other cholinesterase inhibitors, including sarin and soman; the effect was more pronounced with sarin and PB than with soman (Meshul, Boyne, et al., 1985). Moreover, PB affected both the extensor muscle and the soleus, whereas sarin affected endplates primarily of the soleus, and soman affected neither (Meshul, Boyne, et al., 1985). (This suggests that testing of only one or two muscle groups may be inadequate to exclude an effect, and effects identified may not generalize with fidelity to other muscle groups.) In rat extensor digitorum longus muscle, treatment with neostigmine produced decreased MEPP amplitude and frequency and decreased endplate potential amplitude (accompanied by decreased junctional ACh sensitivity and decreased quantal content of nerve-evoked endplate potentials). Although by days of continued treatment the reduced rate of transmitter release had returned almost to normal, the alterations in the postsynaptic membrane lasted for the full 106 days of continued treatment (Tiedt, Albuquerque, et al., 1978). In rat diaphragm muscle in vitro, low concentrations of neostigmine (.0001 mmol/l) led to decrement then full recuperation of compound muscle action potential (CMAP) amplitudes on repetitive stimulation of the phrenic nerve (the nerve that supplies the diaphragm), increased MEPP amplitudes, and prolonged decay time for the MEPC. Higher concentrations led to unimodal reduction in the CMAP, endplate potential, and MEPP amplitudes and a double exponential time-course of MEPC decay (Maselli and Leung, 1993a and 1993b). It was concluded that low concentrations impair neuromuscular transmission by transient depolarization of the endplate, while higher concentrations induce desensitization and direct blockade of the endplate receptor channel, probably in its open configuration. Studies with nerve agents have actually shown opposite effects on endplate currents with low- and high-dose treatment. Except for tabun, the other OP nerve agents (soman, sarin, and VX) at low concentrations (< 1 µm) facilitated, while high doses (> 10 µm) of all four depressed, the endplate current peak ampli-
11 Neuromuscular Junction Effects 173 tude, with VX producing the greatest depression (Albuquerque, 1986). Moreover, the time constant of endplate current decay t EPC was prolonged, and a maximum increase was achieved with 1 µm in the case of VX, sarin, and tabun, whereas soman produced a maximal increase at 0.1µM concentration. Doses of > 1µM of all OPs shortened t EPC from an enhanced level achieved by a low dose. At the 1µM concentration, all four OPs produced near-maximal enhancement (approximately three times greater than control) of t EPc, while at doses of 10 µm or greater, the t EPC values appeared lower than with the 1µM dose; a greater reduction was observed with VX (Albuquerque, 1986). The enhancement of t EPC can be attributed to inhibition of AChE, while reduction with higher doses appears to be due to their action on the ACh receptor ion channel complex, or on the associated ionic channels (Albuquerque, 1986). PB also facilitates receptor desensitization (a functional form of downregulation) (Meshul, Boyne, et al., 1985); indeed, it has been suggested that PB may have its therapeutic effects against OP compounds partly because it produces a desensitized state of the ACh receptor (Albuquerque, Boyne, et al., 1983). Receptors desensitized by PB would be insensitive to the anticholinesterase effects of the OP compounds. Desensitizing effects of PB on the nicotinic ACh receptor have been shown in investigations of macroscopic as well as the microscopic events. Using fluctuation analysis as well as the patch clamp technique (in which the voltage of the membrane is held constant and electrical currents, resulting from movement of ions across channels, are measured), the agent has been shown to decrease single-channel conductance (conductance of ions across a single ACh receptor following binding of two molecules). PB decreases the endplate current and MEPC peak amplitudes, and, after an initial prolongation of these events presumably due to anticholinesterase effects (that is, due to increased availability of ACh), brings the time-constant of decay back to control levels (Albuquerque, Boyne, et al., 1983). The desensitization of the ACh receptor induced by PB has been demonstrated by ACh iontophoresis experiments (direct application of ACh onto receptors) but can also be demonstrated by a patch clamp technique By patch clamp one can measure the characteristics only of open channels. There are multiple closed states with different receptor configuration; specific sequences of closed states must be gone through prior to a channel s opening, but this technique does not allow distinction among them. It has been possible to demonstrate the existence of an intermediate state of channel behavior by such agents as PB that enhance desensitization. The channels in the presence of PB, for example, reveal intense flickering, and the channel openings appear in a bursting pattern, uncharacteristic of the channels in control condition. These are the channels that are presumably about to become desensitized and fail to open at all or open with a markedly decreased conductance. Following the appearance of many channels with much flickering and successive waves of bursting activity,
12 174 Pyridostigmine Bromide Receptor desensitization produced by PB may contribute to reduction in benefit of PB to myasthenics over time. (Throughout this section, other mechanisms are identified that may potentially be involved in functional cholinergic downregulation and could also contribute to reduction in the benefit of PB to myasthenics with continued treatment.) Neuromuscular adaptation has also been demonstrated following administration of the OP DFP in the rat; this adaptation was found to be caused by the recovery of AChE activity due to de novo synthesis of AChE, and reduction in the number of nicotinic ACh receptors (Gupta, Patterson, et al., 1986). PB s ability to facilitate receptor desensitization does not prevent the development of endplate myopathy (Meshul, Boyne, et al., 1985), though one could speculate that it may contribute to the failure of endplate myopathy to progress, and the eventual partial regression of this process. More careful characterization of the time-course of the two is needed. Desensitization rates vary for different carbamate anticholinesterases acting on the ACh receptor ion channel complex, at least in rats. The effect of neostigmine exceeds that of physostigmine, which in turn exceeds pyridostigmine (Meshul, Boyne, et al., 1985). These effects differ from certain other downregulating effects, which require continued AChE inhibition and therefore are weaker (or absent) for physostigmine than for PB, since physostigmine has a shorter time-course. Failure of neuromuscular transmission loss of ability of a signal from a nerve cell to produce contraction in the muscle fiber to which it connects has been reported with anticholinesterases, but the reasons for this failure are incompletely understood. When a nerve signals to a muscle, the membrane voltage becomes less negative, a process called depolarization, which occurs as ions (such as sodium or potassium) move through channels in the membrane. Adequate depolarization leads the muscle fiber to generate an action potential (a self-propagating electrochemical signal that produces contraction of the fiber). However, prolonged depolarization inactivates the sodium channels so that effective signaling cannot take place. According to a study using DFP in rat diaphragm muscle, two patterns of stimulation-induced endplate depolarization have been described that may account for the impairment in neuromuscular transmission reported with anticholinesterases. One pattern exhibited progressive staircase summation of long decay endplate potentials resulting in maximal depolarization at the end of the stimulation period. The other had maximal endplate depolarization at the start of the stimulation period followed by progressive return to the prestimulation levels (Maselli and Leung, 1993a). Transient endplate depolar- channel opening frequency drops drastically and channel conductance decreases (Albuquerque, Boyne, et al., 1983).
13 Neuromuscular Junction Effects 175 ization was proposed to underlie the decremental response followed by recuperation of CMAP amplitudes in humans at early stages of toxicity with OP compounds (Maselli and Leung, 1993a). Transient endplate depolarization was suggested to account for failure of neuromuscular transmission induced by low concentrations of anticholinesterases; while high concentrations induce additional desensitization and direct blockade of the endplate receptor, which becomes the dominant mechanism for failure of neuromuscular transmission (Maselli and Leung, 1993a and 1993b). (These are mechanisms of possible cholinergic downregulation with AChE inhibitors.) With 14 days of DFP administration in rats, postsynaptic nicotinic receptor density (Bmax) was reduced to 44 percent without a change in the affinity constant (Gupta, Patterson, et al., 1986), another potential mechanism for at least temporary downregulation. Changes in AChE. With DFP administration in rats, though AChE activity was initially reduced to 20 to 24 percent of control, no further inhibition of AChE occurred with continued DFP for 14 days, but there was recovery of enzyme activity, especially certain forms (the 4SD and 10S forms) (Gupta, Patterson, et al., 1986). Whether this recovery results from increased AChE production, reduced sensitivity of AChE to DFP, or other effects was not elucidated. Depending on the mechanism involved, this recovery could conceivably produce another form of downregulation. However, other studies employing PB have found persistent inhibition of AChE with continued treatment. The effect on AChE inhibition and on ACh release following discontinuation of PB has not been well defined, and the relative contributions and time-courses of agonism and downregulation remain to be determined. Clinical Changes. Despite marked ultrastructural damage to muscle fibers, postsynaptic elements, and perhaps presynaptic elements, some reports indicate that muscle function (in in vitro tests) is not compromised, at least according to certain tests. Diaphragm muscles underwent no significant reduction in twitch or tetanic tension during or after a two-week exposure to PB, which was proposed to be due to the confined area of ultrastructural damage. Synaptic transmission and action potential generation, based on in vitro findings, were expected to remain functional, with decrements in tension due to abnormal properties of the myopathic regions presumably too small to detect (Adler, Hinman, et al., 1992). Other studies (using neostigmine) have shown a reduction in indirectly and directly elicited muscle contraction with three days of treatment (Tiedt, Albuquerque, et al., 1978). In another study of rats exposed to DFP for 14 days, there was initial appearance followed by disappearance of fasciculations in all muscles tested (diaphragm, soleus, extensor digitorum longus) (Gupta, Patterson, et al., 1986).
14 176 Pyridostigmine Bromide It is not known whether ultrastructural changes such as those observed in animal studies could produce apparently normal function in selected muscle function challenge tests but also lead to symptoms of subjective fatigue (perhaps corresponding to abnormalities that these particular tests do not capture). In studies of rats demonstrating ultrastructural and electrophysiological changes, animals expressing these changes demonstrated behavior varying from no identified findings to death, with fasciculations, prostration, salivation, urination, defecation, and rhinorrhea seen (Adler, Hinman, et al., 1992). Many of these changes represent activation of the muscarinic system. Of greater interest would be careful studies of muscle function and animal activity during and after acute and chronic cessation of the agent. Human Studies with PB: Comparison of Myasthenic Changes in Humans to PB-Induced Changes in Animals Ultrastructural and Electrophysiological. It has been speculated that carbamates used to treat myasthenia gravis, such as PB and neostigmine, may contribute in part to the neuromuscular alterations observed in myasthenia gravis. The changes produced by PB are similar to but not identical with those seen in rabbit and human myasthenia (Tiedt, Albuquerque, et al., 1978). Similarities with myasthenia gravis include reduced MEPP amplitude and frequency, reduced junctional ACh sensitivity (see Downregulation ), alterations in neuromuscular geometry, and disruption of synaptic folds. Dissimilarities include the frequency distribution of MEPP amplitude, variation of neuromuscular junction ACh receptor sensitivity and ACh potential time-course, muscle membrane cable properties, and state of contraction of the endplate sarcoplasm (a membrane within the neuron that contains calcium) (Tiedt, Albuquerque, et al., 1978). One study concluded that it appears likely that neostigmine treatment in patients with myasthenia gravis does not have an important role in the pathogenesis of the disease, but that it may contribute to the observed alterations. (Tiedt, Albuquerque, et al., 1978.) Others voice concern that the ultrastructural appearance of myasthenic endplates is similar to the ion accumulation myopathy caused by PB (Meshul, Boyne, et al., 1985); they note that administration of a therapeutic agent that increases the desensitizing effects of ACh and can still lead to excess ion accumulation (with ion leak into muscle cytoplasm as a possible proximal cause of myasthenic myopathy) may have complex and possibly counterproductive consequences that have not been anticipated. (Meshul, Boyne, et al., 1985.) Clinical. Some studies suggest that clinical effects on muscle function do not occur subacutely with PB use, while others have shown modest effects. For
15 Neuromuscular Junction Effects 177 example, muscle strength and endurance were not significantly affected by eight days of PB treatment leading to percent cholinesterase inhibition in a group of 35 healthy male year-old volunteers in a double-blind placebo controlled trial that tested isometric handgrip, isokinetic elbow flexor and extensor strength, and knee flexor and extensor strength (Glickson, Achiron, et al., 1991). Other studies in smaller samples failed to find differences in grip strength after one or several 30 mg tablets of PB (n = 7 and n = 5; Levine, Kolka, et al., 1991; Forster, Barber, et al., 1994) (one or several Gulf War doses). Of these, one also examined and failed to show a difference in 60 percent peak hand-grip endurance time, or peak torque for leg extension (Levine, Kolka, et al., 1991). In contrast, one small (n = 7) double-blind, placebo-controlled crossover study did demonstrate a modest (~3 percent, p <.05) reduction in grip strength in those receiving pyridostigmine (Cook, Kolka, et al., 1992). (Subjects received PB for one week and placebo for one week and received daily focused examinations.) The possibility cannot be excluded that modest effects, delayed effects, or effects with different motor measures occurred. One study performed evaluations of neuromuscular function in 20 PGW veterans with severe muscle fatigue, weakness, or myalgias (muscular pain) interfering with their daily activities (Amato, McVey, et al., 1997). Tests included nerve conduction, effects of repetitive nerve stimulation, quantitative single fiber electromyography, and muscle biopsies. Mild increases in CK (an enzyme released by the muscle with acute muscle damage) were seen in six of 20 patients (range IU/l); one patient who reportedly had not received PB had mildly increased jitter on single-fiber EMG, and muscle biopsies showed abnormalities in 5 of 20 patients. Both patients with tubular aggregates reported having received PB. The abnormal findings were not believed to be clinically significant. However this conclusion is at best problematic in the face of marked clinical symptoms in these subjects, because no testing was performed in matched controls to determine the frequencies of these abnormalities in asymptomatic individuals of similar age and training. (The authors performed no power calculations; neither did they define at the outset how many abnormal biopsies or CKs would be expected if the group were normal. ) Manually tested muscle strength was measured and was reportedly normal in all instances. Unfortunately, this is an extremely crude measure (it may supply the same score for a world champion weight lifter and a non-physically-active grandmother; it is not sensitive to even substantial differences within this normal range). No sensitive quantitative measures of muscle strength, and comparisons to healthy non-pgw deployed individuals of similar age and training, were performed. In summary, clinical findings with PB on motor outcomes have used short-term trials evaluating acute effects, without long-term follow-up after discontin-
16 178 Pyridostigmine Bromide uation, in small samples, using limited tests of motor function. Some studies but not others have shown significant but subtle effects on measured functions. One study performed biopsies, muscle enzyme testing, and limited neuromuscular testing in symptomatic PGW veterans with muscular complaints but failed to employ a control group. A set of observed abnormalities was construed as not clinically significant and unrelated to possible toxin exposures, although no cogent justification for this position was provided. Duration of Changes The changes that take place pre- and postsynaptically appear to be partially or mostly reversible, even with continued treatment with anticholinesterases, including PB, with much of the reversal occurring early. However there are provisos to this reversibility. First, the reversal may not be altogether complete. One study stated that recovery of twitch tensions following cessation of PB was essentially complete by one day after cessation (Adler, Maxwell, et al., 1984), but in fact although the value was indeed stable from one to 15 days following cessation, recovery to the original baseline never occurred. Second, at least some changes appear to be long-lasting. Studies in rats (extensor digitorum longus muscle) have shown that some changes at the neuromuscular junction (alterations of the postsynaptic membrane) persisted for as long as 106 days, the duration of continued treatment (with neostigmine) (Tiedt, Albuquerque, et al., 1978). More directly relevant to the issue of PGW veterans is the question of whether changes persist beyond the cessation of treatment. The study with the longest identified follow-up after cessation of PB delivery 60 days found that while recovery was reportedly complete 60 days after cessation of PB treatment in some rats (following a single injection of PB or 14 days of PB delivery by osmotic minipump), in other animals changes were still present 60 days after discontinuing PB, perhaps more so in specific muscles such as the soleus. Sixty days is relatively chronic in the life of a rat. (One rat week is said for some purposes to correspond to one human year. Using this crude guide, extrapolation to humans of data from the rat study would suggest continued tissue damage in some individuals extending to roughly eight years, with no further testing thereafter.) Thus, current data do not exclude the possibility that some animals never fully recover the pre-pb appearance of their muscle tissue. The clinical correlation of this finding, if any, remains to be defined. In general, each of the changes histological and ultrastructural, electrical and chemical, and presynaptic and postsynaptic; changes in receptor density and sensitivity, withdrawal of nerve terminals, reductions in quantal content and quantal release, alterations in AChE production, or susceptibility to inhibition needs to be evaluated more carefully for time-course of reversal following PB
17 Neuromuscular Junction Effects 179 discontinuation, for interactions with other changes, and for individual differences in extent and in time-course. CONCLUSIONS Current evidence from studies in animals suggests that toxic effects result from cholinergic excitation at the neuromuscular junction in reaction to high doses of AChE inhibitors including PB. PB and other AChE inhibitors lead to alterations in function of the neuromuscular junction as well as physical destruction. These effects are partially reversible even with continued PB administration, but they may not be completely reversed even long after PB discontinuation. AChE inhibitors lead to changes in ACh production, ACh release, receptor response to ACh administration, muscle fiber organization, and clinical symptoms. These effects appear to result at least in part from excitation at the neuromuscular junction and the interaction of ACh with its receptor (with a concomitant influx of calcium). For this reason, tonically, persistently, or highly active muscles or muscle sites may be more affected. Some effects vary with the individual AChE inhibitor chosen or the dose employed (effects may even be opposite in direction with low and high dose of cholinesterase-inhibiting agents) (Albuquerque, Boyne, et al., 1983; Albuquerque, 1986), although the effects of dose for the many reported changes in receptor function, ultrastructure, and electrophysiological properties have not been well characterized. Many changes in quantal release of ACh, in current and voltage changes in response to ACh at the motor endplate, and in the sensitivity to postjunctional ACh receptors appear to reduce cholinergic function. This reduction in function may occur in response to, and may partially offset, the heightened ACh delivery at the synapse during the period of pharmacological AChE inhibition. Although the duration of most effects (on ACh production and release, receptor sensitivity, myopathic changes, etc.) have not been well characterized, some effects have been shown to be quite long-lasting following discontinuation of the AChE inhibitor. It is not known whether all effects eventually reverse in all or most cases. The time-course of different effects has not been well characterized, neither have the doses at which the several effects are first seen. The effects have not been well studied across species or in primates. Moreover, the clinical sequelae of these changes, if any, are not well understood. It could be postulated that one consequence of these changes namely functional cholinergic downregulation attended by reduced cholinergic activity may lead to subjective fatigability in humans (conceivably leading to symptoms suggestive of chronic fatigue ), but no data directly support or refute this proposition. This hypothesis would be weakly supported if treatment with cholinergic drugs led to subjective improvement in PGW veterans who report fatigue. However,
What effect would an AChE inhibitor have at the neuromuscular junction?
 CASE 4 A 32-year-old woman presents to her primary care physician s office with difficulty chewing food. She states that when she eats certain foods that require a significant amount of chewing (meat),
CASE 4 A 32-year-old woman presents to her primary care physician s office with difficulty chewing food. She states that when she eats certain foods that require a significant amount of chewing (meat),
PSK4U THE NEUROMUSCULAR SYSTEM
 PSK4U THE NEUROMUSCULAR SYSTEM REVIEW Review of muscle so we can see how the neuromuscular system works This is not on today's note Skeletal Muscle Cell: Cellular System A) Excitation System Electrical
PSK4U THE NEUROMUSCULAR SYSTEM REVIEW Review of muscle so we can see how the neuromuscular system works This is not on today's note Skeletal Muscle Cell: Cellular System A) Excitation System Electrical
Quantal Analysis Problems
 Quantal Analysis Problems 1. Imagine you had performed an experiment on a muscle preparation from a Drosophila larva. In this experiment, intracellular recordings were made from an identified muscle fibre,
Quantal Analysis Problems 1. Imagine you had performed an experiment on a muscle preparation from a Drosophila larva. In this experiment, intracellular recordings were made from an identified muscle fibre,
Muscle Tissue- 3 Types
 AN INTRODUCTION TO MUSCLE TISSUE Muscle Tissue- 3 Types Skeletal muscle (focus on these) Cardiac muscle Smooth muscle FUNCTIONS OF SKELETAL MUSCLES Produce movement of the skeleton Maintain posture and
AN INTRODUCTION TO MUSCLE TISSUE Muscle Tissue- 3 Types Skeletal muscle (focus on these) Cardiac muscle Smooth muscle FUNCTIONS OF SKELETAL MUSCLES Produce movement of the skeleton Maintain posture and
Muscle Physiology. Introduction. Four Characteristics of Muscle tissue. Skeletal Muscle
 Muscle Physiology Introduction Muscle = tissue capable of forceful shortening or contraction Converts chemical energy (ATP) into mechanical energy Important in: Respiration Urine collection & flow Gastrointestinal
Muscle Physiology Introduction Muscle = tissue capable of forceful shortening or contraction Converts chemical energy (ATP) into mechanical energy Important in: Respiration Urine collection & flow Gastrointestinal
Neuromuscular Junction Testing ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER
 Neuromuscular Junction Testing ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Neurophysiology Electrodiagnostic Evaluation Clinical Application
Neuromuscular Junction Testing ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Neurophysiology Electrodiagnostic Evaluation Clinical Application
Muscle and Muscle Tissue
 Muscle and Muscle Tissue Make up about half of total body mass Exerts force by converting chemical energy, ATP, to mechanical energy Muscle tissue is classified based on Shape Number and position of nuclei
Muscle and Muscle Tissue Make up about half of total body mass Exerts force by converting chemical energy, ATP, to mechanical energy Muscle tissue is classified based on Shape Number and position of nuclei
Medicine, University of Lund, Sweden
 336 J. Phy8iol. (1961), 156, pp. 336-343 With 6 text-ftgures Printed in Great Britain AN ELECTROPHYSIOLOGIC STUDY OF THE NEURO- MUSCULAR JUNCTION IN MYASTHENIA GRAVIS BY 0. DAHLBACK, D. ELMQVIST, T. R.
336 J. Phy8iol. (1961), 156, pp. 336-343 With 6 text-ftgures Printed in Great Britain AN ELECTROPHYSIOLOGIC STUDY OF THE NEURO- MUSCULAR JUNCTION IN MYASTHENIA GRAVIS BY 0. DAHLBACK, D. ELMQVIST, T. R.
ANSC (FSTC) 607 Physiology and Biochemistry of Muscle as a Food MOTOR INNERVATION AND MUSCLE CONTRACTION
 ANSC (FSTC) 607 Physiology and Biochemistry of Muscle as a Food MOTOR INNERVATION AND MUSCLE CONTRACTION I. Motor innervation of muscle A. Motor neuron 1. Branched (can innervate many myofibers) à terminal
ANSC (FSTC) 607 Physiology and Biochemistry of Muscle as a Food MOTOR INNERVATION AND MUSCLE CONTRACTION I. Motor innervation of muscle A. Motor neuron 1. Branched (can innervate many myofibers) à terminal
CHAPTER 44: Neurons and Nervous Systems
 CHAPTER 44: Neurons and Nervous Systems 1. What are the three different types of neurons and what are their functions? a. b. c. 2. Label and list the function of each part of the neuron. 3. How does the
CHAPTER 44: Neurons and Nervous Systems 1. What are the three different types of neurons and what are their functions? a. b. c. 2. Label and list the function of each part of the neuron. 3. How does the
Muscle Physiology. Dr. Ebneshahidi Ebneshahidi
 Muscle Physiology Dr. Ebneshahidi Skeletal Muscle Figure 9.2 (a) Functions of the muscular system 1. Locomotion body movements are due to skeletal muscle contraction. 2. Vasoconstriction and vasodilatation
Muscle Physiology Dr. Ebneshahidi Skeletal Muscle Figure 9.2 (a) Functions of the muscular system 1. Locomotion body movements are due to skeletal muscle contraction. 2. Vasoconstriction and vasodilatation
Chapter 9 Muscle. Types of muscle Skeletal muscle Cardiac muscle Smooth muscle. Striated muscle
 Chapter 9 Muscle Types of muscle Skeletal muscle Cardiac muscle Smooth muscle Striated muscle Chapter 9 Muscle (cont.) The sliding filament mechanism, in which myosin filaments bind to and move actin
Chapter 9 Muscle Types of muscle Skeletal muscle Cardiac muscle Smooth muscle Striated muscle Chapter 9 Muscle (cont.) The sliding filament mechanism, in which myosin filaments bind to and move actin
Skeletal Muscle and the Molecular Basis of Contraction. Lanny Shulman, O.D., Ph.D. University of Houston College of Optometry
 Skeletal Muscle and the Molecular Basis of Contraction Lanny Shulman, O.D., Ph.D. University of Houston College of Optometry Like neurons, all muscle cells can be excited chemically, electrically, and
Skeletal Muscle and the Molecular Basis of Contraction Lanny Shulman, O.D., Ph.D. University of Houston College of Optometry Like neurons, all muscle cells can be excited chemically, electrically, and
Skeletal Muscle. Connective tissue: Binding, support and insulation. Blood vessels
 Chapter 12 Muscle Physiology Outline o Skeletal Muscle Structure o The mechanism of Force Generation in Muscle o The mechanics of Skeletal Muscle Contraction o Skeletal Muscle Metabolism o Control of Skeletal
Chapter 12 Muscle Physiology Outline o Skeletal Muscle Structure o The mechanism of Force Generation in Muscle o The mechanics of Skeletal Muscle Contraction o Skeletal Muscle Metabolism o Control of Skeletal
Baraa Ayed. Mohammad khatatbeh. 1 P a g e
 4 Baraa Ayed أسامة الخض Mohammad khatatbeh 1 P a g e Today we want to talk about these concepts: Excitation-Contraction coupling Smooth muscles (Generally speaking) Excitation-Contraction coupling Excitation-Contraction
4 Baraa Ayed أسامة الخض Mohammad khatatbeh 1 P a g e Today we want to talk about these concepts: Excitation-Contraction coupling Smooth muscles (Generally speaking) Excitation-Contraction coupling Excitation-Contraction
Cellular Bioelectricity
 ELEC ENG 3BB3: Cellular Bioelectricity Notes for Lecture 22 Friday, February 28, 2014 10. THE NEUROMUSCULAR JUNCTION We will look at: Structure of the neuromuscular junction Evidence for the quantal nature
ELEC ENG 3BB3: Cellular Bioelectricity Notes for Lecture 22 Friday, February 28, 2014 10. THE NEUROMUSCULAR JUNCTION We will look at: Structure of the neuromuscular junction Evidence for the quantal nature
Organismic Biology Bio 207. Lecture 6. Muscle and movement; sliding filaments; E-C coupling; length-tension relationships; biomechanics. Prof.
 Organismic Biology Bio 207 Lecture 6 Muscle and movement; sliding filaments; E-C coupling; length-tension relationships; biomechanics Prof. Simchon Today s Agenda Skeletal muscle Neuro Muscular Junction
Organismic Biology Bio 207 Lecture 6 Muscle and movement; sliding filaments; E-C coupling; length-tension relationships; biomechanics Prof. Simchon Today s Agenda Skeletal muscle Neuro Muscular Junction
Muscle and Neuromuscular Junction. Peter Takizawa Department of Cell Biology
 Muscle and Neuromuscular Junction Peter Takizawa Department of Cell Biology Types and structure of muscle cells Structural basis of contraction Triggering muscle contraction Skeletal muscle consists of
Muscle and Neuromuscular Junction Peter Takizawa Department of Cell Biology Types and structure of muscle cells Structural basis of contraction Triggering muscle contraction Skeletal muscle consists of
MUSCLE TISSUE (MUSCLE PHYSIOLOGY) PART I: MUSCLE STRUCTURE
 PART I: MUSCLE STRUCTURE Muscle Tissue A primary tissue type, divided into: skeletal muscle cardiac muscle smooth muscle Functions of Skeletal Muscles Produce skeletal movement Maintain body position Support
PART I: MUSCLE STRUCTURE Muscle Tissue A primary tissue type, divided into: skeletal muscle cardiac muscle smooth muscle Functions of Skeletal Muscles Produce skeletal movement Maintain body position Support
Chapter 10: Muscles. Vocabulary: aponeurosis, fatigue
 Chapter 10: Muscles 37. Describe the structural components of skeletal muscle tissue from the molecular to the organ level. 38. Describe the structure, function, and importance of sarcomeres. 39. Identify
Chapter 10: Muscles 37. Describe the structural components of skeletal muscle tissue from the molecular to the organ level. 38. Describe the structure, function, and importance of sarcomeres. 39. Identify
Skeletal Muscle Contraction 4/11/2018 Dr. Hiwa Shafiq
 Skeletal Muscle Contraction 4/11/2018 Dr. Hiwa Shafiq Skeletal Muscle Fiber About 40 per cent of the body is skeletal muscle, and 10 per cent is smooth and cardiac muscle. Skeletal muscles are composed
Skeletal Muscle Contraction 4/11/2018 Dr. Hiwa Shafiq Skeletal Muscle Fiber About 40 per cent of the body is skeletal muscle, and 10 per cent is smooth and cardiac muscle. Skeletal muscles are composed
Chapter 9 - Muscle and Muscle Tissue
 Chapter 9 - Muscle and Muscle Tissue I. Overview of muscle tissue A. Three muscle types in the body: B. Special characteristics 1. Excitability: able to receive and respond to a stimulus 2. Contractility:
Chapter 9 - Muscle and Muscle Tissue I. Overview of muscle tissue A. Three muscle types in the body: B. Special characteristics 1. Excitability: able to receive and respond to a stimulus 2. Contractility:
SYNAPTIC TRANSMISSION 1
 SYNAPTIC TRANSMISSION 1 I. OVERVIEW A. In order to pass and process information and mediate responses cells communicate with other cells. These notes examine the two means whereby excitable cells can rapidly
SYNAPTIC TRANSMISSION 1 I. OVERVIEW A. In order to pass and process information and mediate responses cells communicate with other cells. These notes examine the two means whereby excitable cells can rapidly
Skeletal Muscle Qiang XIA (
 Skeletal Muscle Qiang XIA ( 夏强 ), PhD Department of Physiology Rm C518, Block C, Research Building, School of Medicine Tel: 88208252 Email: xiaqiang@zju.edu.cn Course website: http://10.71.121.151/physiology
Skeletal Muscle Qiang XIA ( 夏强 ), PhD Department of Physiology Rm C518, Block C, Research Building, School of Medicine Tel: 88208252 Email: xiaqiang@zju.edu.cn Course website: http://10.71.121.151/physiology
Anatomy and Physiology 1 Chapter 10 self quiz Pro, Dima Darwish,MD.
 Anatomy and Physiology 1 Chapter 10 self quiz Pro, Dima Darwish,MD. 1) Which of the following is a recognized function of skeletal muscle? A) produce movement B) maintain posture C) maintain body temperature
Anatomy and Physiology 1 Chapter 10 self quiz Pro, Dima Darwish,MD. 1) Which of the following is a recognized function of skeletal muscle? A) produce movement B) maintain posture C) maintain body temperature
About This Chapter. Skeletal muscle Mechanics of body movement Smooth muscle Cardiac muscle Pearson Education, Inc.
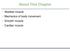 About This Chapter Skeletal muscle Mechanics of body movement Smooth muscle Cardiac muscle Skeletal Muscle Usually attached to bones by tendons Origin: closest to the trunk or to more stationary bone Insertion:
About This Chapter Skeletal muscle Mechanics of body movement Smooth muscle Cardiac muscle Skeletal Muscle Usually attached to bones by tendons Origin: closest to the trunk or to more stationary bone Insertion:
Chapter 10 Muscle Tissue Lecture Outline
 Chapter 10 Muscle Tissue Lecture Outline Muscle tissue types 1. Skeletal muscle = voluntary striated 2. Cardiac muscle = involuntary striated 3. Smooth muscle = involuntary nonstriated Characteristics
Chapter 10 Muscle Tissue Lecture Outline Muscle tissue types 1. Skeletal muscle = voluntary striated 2. Cardiac muscle = involuntary striated 3. Smooth muscle = involuntary nonstriated Characteristics
Fig Copyright McGraw-Hill Education. Permission required for reproduction or display. Nucleus. Muscle fiber. Endomysium. Striations.
 Fig. 11.1 Nucleus Muscle fiber Endomysium Striations Ed Reschke 1 Fig. 11.2 Muscle fiber Nucleus I band A band Z disc Mitochondria Openings into transverse tubules Sarcoplasmic reticulum Triad: Terminal
Fig. 11.1 Nucleus Muscle fiber Endomysium Striations Ed Reschke 1 Fig. 11.2 Muscle fiber Nucleus I band A band Z disc Mitochondria Openings into transverse tubules Sarcoplasmic reticulum Triad: Terminal
Portions from Chapter 6 CHAPTER 7. The Nervous System: Neurons and Synapses. Chapter 7 Outline. and Supporting Cells
 CHAPTER 7 The Nervous System: Neurons and Synapses Chapter 7 Outline Neurons and Supporting Cells Activity in Axons The Synapse Acetylcholine as a Neurotransmitter Monoamines as Neurotransmitters Other
CHAPTER 7 The Nervous System: Neurons and Synapses Chapter 7 Outline Neurons and Supporting Cells Activity in Axons The Synapse Acetylcholine as a Neurotransmitter Monoamines as Neurotransmitters Other
Human Anatomy. Muscle Tissue and Organization. DR.SADIQ ALI (K.E Medalist) 10-1
 Human Anatomy Muscle Tissue and Organization DR.SADIQ ALI (K.E Medalist) 10-1 Tissue and Organization Over 700 skeletal muscles have been named. Form the muscular system. Muscle tissue is distributed almost
Human Anatomy Muscle Tissue and Organization DR.SADIQ ALI (K.E Medalist) 10-1 Tissue and Organization Over 700 skeletal muscles have been named. Form the muscular system. Muscle tissue is distributed almost
Chapter 8 Notes. Muscles
 Chapter 8 Notes Muscles 8.1 Intro Three muscle types Skeletal Smooth cardiac 8.2 Structure of Skeletal Muscle Composition Skeletal muscle tissue Nervous tissue Blood Connective tissue Connective tissue
Chapter 8 Notes Muscles 8.1 Intro Three muscle types Skeletal Smooth cardiac 8.2 Structure of Skeletal Muscle Composition Skeletal muscle tissue Nervous tissue Blood Connective tissue Connective tissue
MUSCULAR TISSUE. Dr. Gary Mumaugh
 MUSCULAR TISSUE Dr. Gary Mumaugh MUSCLE OVERVIEW The three types of muscle tissue are skeletal, cardiac, and smooth These types differ in structure, location, function, and means of activation FUNCTIONAL
MUSCULAR TISSUE Dr. Gary Mumaugh MUSCLE OVERVIEW The three types of muscle tissue are skeletal, cardiac, and smooth These types differ in structure, location, function, and means of activation FUNCTIONAL
Muscle Tissue. Alternating contraction and relaxation of cells. Chemical energy changed into mechanical energy
 Know these muscles Muscle Tissue Alternating contraction and relaxation of cells Chemical energy changed into mechanical energy 3 Types of Muscle Tissue Skeletal muscle attaches to bone, skin or fascia
Know these muscles Muscle Tissue Alternating contraction and relaxation of cells Chemical energy changed into mechanical energy 3 Types of Muscle Tissue Skeletal muscle attaches to bone, skin or fascia
2/19/2018. Learn and Understand:
 Muscular System with Special Emphasis on Skeletal Muscle Anatomy and Physiology Learn and Understand: The definition of cell changes again The contractile unit of muscle is the sarcomere. ATP and Ca 2+
Muscular System with Special Emphasis on Skeletal Muscle Anatomy and Physiology Learn and Understand: The definition of cell changes again The contractile unit of muscle is the sarcomere. ATP and Ca 2+
Alterations in Synaptic Strength Preceding Axon Withdrawal
 Alterations in Synaptic Strength Preceding Axon Withdrawal H. Colman, J. Nabekura, J.W. Lichtman presented by Ana Fiallos Synaptic Transmission at the Neuromuscular Junction Motor neurons with cell bodies
Alterations in Synaptic Strength Preceding Axon Withdrawal H. Colman, J. Nabekura, J.W. Lichtman presented by Ana Fiallos Synaptic Transmission at the Neuromuscular Junction Motor neurons with cell bodies
Nerve Cell (aka neuron)
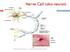 Nerve Cell (aka neuron) Neuromuscular Junction Nerve cell Muscle fiber (cell) The Nerve Stimulus and Action Potential The Nerve Stimulus and Action Potential Skeletal muscles must be stimulated by a motor
Nerve Cell (aka neuron) Neuromuscular Junction Nerve cell Muscle fiber (cell) The Nerve Stimulus and Action Potential The Nerve Stimulus and Action Potential Skeletal muscles must be stimulated by a motor
Concept 50.5: The physical interaction of protein filaments is required for muscle function
 Concept 50.5: The physical interaction of protein filaments is required for muscle function Muscle activity is a response to input from the nervous system The action of a muscle is always to contract Vertebrate
Concept 50.5: The physical interaction of protein filaments is required for muscle function Muscle activity is a response to input from the nervous system The action of a muscle is always to contract Vertebrate
Muscle Tissue. PowerPoint Lecture Presentations prepared by Jason LaPres. Lone Star College North Harris Pearson Education, Inc.
 10 Muscle Tissue PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to Muscle Tissue Muscle Tissue A primary tissue type, divided into: Skeletal muscle
10 Muscle Tissue PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to Muscle Tissue Muscle Tissue A primary tissue type, divided into: Skeletal muscle
Chapter 45: Synapses Transmission of Nerve Impulses Between Neurons. Chad Smurthwaite & Jordan Shellmire
 Chapter 45: Synapses Transmission of Nerve Impulses Between Neurons Chad Smurthwaite & Jordan Shellmire The Chemical Synapse The most common type of synapse used for signal transmission in the central
Chapter 45: Synapses Transmission of Nerve Impulses Between Neurons Chad Smurthwaite & Jordan Shellmire The Chemical Synapse The most common type of synapse used for signal transmission in the central
Muscles and Muscle Tissue
 1 Muscles and Muscle Tissue Chapter 9 2 Overview of Muscle Tissues Compare and Contrast the three basic types of muscle tissue List four important functions of muscle tissue 3 Muscle Terminology Muscle
1 Muscles and Muscle Tissue Chapter 9 2 Overview of Muscle Tissues Compare and Contrast the three basic types of muscle tissue List four important functions of muscle tissue 3 Muscle Terminology Muscle
Functions of Muscle Tissue
 The Muscular System Functions of Muscle Tissue Movement Facilitation Thermogenesis Postural Support Regulation of Organ Volume Protects Internal Organs Pumps Blood (HEART) Characteristics of Muscle Tissue
The Muscular System Functions of Muscle Tissue Movement Facilitation Thermogenesis Postural Support Regulation of Organ Volume Protects Internal Organs Pumps Blood (HEART) Characteristics of Muscle Tissue
1/4/2017. Introduction. Connective Tissue Coverings. 9.1: Structure of a Skeletal Muscle. Skeletal Muscle Fibers. Connective Tissue Coverings
 Introduction Chapter 09 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright McGraw-Hill Education. Permission required for reproduction
Introduction Chapter 09 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright McGraw-Hill Education. Permission required for reproduction
MUSCULAR SYSTEM CHAPTER 09 BIO 211: ANATOMY & PHYSIOLOGY I
 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 09 MUSCULAR SYSTEM Part 2 of 2 Dr. Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy
1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 09 MUSCULAR SYSTEM Part 2 of 2 Dr. Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy
CLASS SET Unit 4: The Muscular System STUDY GUIDE
 NPHS Anatomy & Physiology Questions to answer: 1) List three functions of the muscular system. 1) movement 2) thermogenesis (generates heat) 3) posture & body/joint support CLASS SET Unit 4: The Muscular
NPHS Anatomy & Physiology Questions to answer: 1) List three functions of the muscular system. 1) movement 2) thermogenesis (generates heat) 3) posture & body/joint support CLASS SET Unit 4: The Muscular
Introduction to Neurobiology
 Biology 240 General Zoology Introduction to Neurobiology Nervous System functions: communication of information via nerve signals integration and processing of information control of physiological and
Biology 240 General Zoology Introduction to Neurobiology Nervous System functions: communication of information via nerve signals integration and processing of information control of physiological and
BIPN100 F15 Human Physiology 1 Lecture 3. Synaptic Transmission p. 1
 BIPN100 F15 Human Physiology 1 Lecture 3. Synaptic Transmission p. 1 Terms you should know: synapse, neuromuscular junction (NMJ), pre-synaptic, post-synaptic, synaptic cleft, acetylcholine (ACh), acetylcholine
BIPN100 F15 Human Physiology 1 Lecture 3. Synaptic Transmission p. 1 Terms you should know: synapse, neuromuscular junction (NMJ), pre-synaptic, post-synaptic, synaptic cleft, acetylcholine (ACh), acetylcholine
Chapter 10 -Muscle Tissue
 Chapter 10 -Muscle Tissue Muscles: 1. Overview of Muscle Tissue A. Review 5 functions of muscle tissue. B. Review the 5 properties of muscle tissue. WHICH do they share with nervous tissue? (2, plus the
Chapter 10 -Muscle Tissue Muscles: 1. Overview of Muscle Tissue A. Review 5 functions of muscle tissue. B. Review the 5 properties of muscle tissue. WHICH do they share with nervous tissue? (2, plus the
Chapter 10 Muscle Tissue and Physiology Chapter Outline
 Chapter 10 Muscle Tissue and Physiology Chapter Outline Module 10.1 Overview of muscle tissue (Figures 10.1 10.2) A. Types of Muscle Tissue (Figure 10.1) 1. The three types of cells in muscle tissue are,,
Chapter 10 Muscle Tissue and Physiology Chapter Outline Module 10.1 Overview of muscle tissue (Figures 10.1 10.2) A. Types of Muscle Tissue (Figure 10.1) 1. The three types of cells in muscle tissue are,,
Hole s Human Anatomy and Physiology Eleventh Edition. Mrs. Hummer. Chapter 9 Muscular System
 Hole s Human Anatomy and Physiology Eleventh Edition Mrs. Hummer Chapter 9 Muscular System 1 Chapter 9 Muscular System Skeletal Muscle usually attached to bones under conscious control striated Three Types
Hole s Human Anatomy and Physiology Eleventh Edition Mrs. Hummer Chapter 9 Muscular System 1 Chapter 9 Muscular System Skeletal Muscle usually attached to bones under conscious control striated Three Types
Microanatomy of Muscles. Anatomy & Physiology Class
 Microanatomy of Muscles Anatomy & Physiology Class Three Main Muscle Types Objectives: By the end of this presentation you will have the information to: 1. 2. 3. 4. 5. 6. Describe the 3 main types of muscles.
Microanatomy of Muscles Anatomy & Physiology Class Three Main Muscle Types Objectives: By the end of this presentation you will have the information to: 1. 2. 3. 4. 5. 6. Describe the 3 main types of muscles.
Muscular Tissue. Functions of Muscular Tissue. Types of Muscular Tissue. Skeletal Muscular Tissue. Properties of Muscular Tissue
 Muscular Tissue Functions of Muscular Tissue Muscle makes up a large percentage of the body s weight (40-50%) Their main functions are to: Create motion muscles work with nerves, bones, and joints to produce
Muscular Tissue Functions of Muscular Tissue Muscle makes up a large percentage of the body s weight (40-50%) Their main functions are to: Create motion muscles work with nerves, bones, and joints to produce
Ch 10: Skeletal Muscle Tissue (Myology)
 Ch 10: Skeletal Muscle Tissue (Myology) main objectives: Describe the distinguishing characteristics of the different muscle tissues Discuss the organization of skeletal muscle Explain the micro-anatomy
Ch 10: Skeletal Muscle Tissue (Myology) main objectives: Describe the distinguishing characteristics of the different muscle tissues Discuss the organization of skeletal muscle Explain the micro-anatomy
Neuromuscular Transmission Diomedes E. Logothetis, Ph.D. (Dr. DeSimone s lecture notes revised) Learning Objectives:
 Neuromuscular Transmission Diomedes E. Logothetis, Ph.D. (Dr. DeSimone s lecture notes revised) Learning Objectives: 1. Know the subunit composition of nicotinic ACh channels, general topology of the α
Neuromuscular Transmission Diomedes E. Logothetis, Ph.D. (Dr. DeSimone s lecture notes revised) Learning Objectives: 1. Know the subunit composition of nicotinic ACh channels, general topology of the α
Ch.10 Muscle Tissue. Copyright 2009, John Wiley & Sons, Inc.
 Ch.10 Muscle Tissue Preview Chapter 10 In groups we will define the following terms 1. Skeletal muscle 2. Smooth muscle 3. Cardiac muscle 4. Sarcomere 5. Myofibril 6. Myofilament 7. Sarcoplasmic reticulum
Ch.10 Muscle Tissue Preview Chapter 10 In groups we will define the following terms 1. Skeletal muscle 2. Smooth muscle 3. Cardiac muscle 4. Sarcomere 5. Myofibril 6. Myofilament 7. Sarcoplasmic reticulum
Activity Dependent Changes At the Developing Neuromuscular Junction
 Activity Dependent Changes At the Developing Neuromuscular Junction (slides 16, 17 and 18 have been slightly modified for clarity) MCP Lecture 2-3 9.013/7.68 04 Neuromuscular Junction Development 1. Muscle
Activity Dependent Changes At the Developing Neuromuscular Junction (slides 16, 17 and 18 have been slightly modified for clarity) MCP Lecture 2-3 9.013/7.68 04 Neuromuscular Junction Development 1. Muscle
Neuromuscular Junction
 Muscle Relaxants Neuromuscular Junction Cholinergic antagonists Neuromuscular-blocking agents (mostly nicotinic antagonists): interfere with transmission of efferent impulses to skeletal muscles. These
Muscle Relaxants Neuromuscular Junction Cholinergic antagonists Neuromuscular-blocking agents (mostly nicotinic antagonists): interfere with transmission of efferent impulses to skeletal muscles. These
Neurons Chapter 7 2/19/2016. Learning Objectives. Cells of the Nervous System. Cells of the Nervous System. Cells of the Nervous System
 Learning Objectives Neurons Chapter 7 Identify and describe the functions of the two main divisions of the nervous system. Differentiate between a neuron and neuroglial cells in terms of structure and
Learning Objectives Neurons Chapter 7 Identify and describe the functions of the two main divisions of the nervous system. Differentiate between a neuron and neuroglial cells in terms of structure and
Nerve regeneration. Somatic nervous system
 Somatic nervous system Signals from CNS are sent to skeletal muscles. Final result is a muscle contraction. Motor neuron starts in CNS and its axon ends at a muscle cell. Alpha motor neuron Alpha motor
Somatic nervous system Signals from CNS are sent to skeletal muscles. Final result is a muscle contraction. Motor neuron starts in CNS and its axon ends at a muscle cell. Alpha motor neuron Alpha motor
Nerve meets muscle. Nerve regeneration. Somatic nervous system
 Somatic nervous system Signals from CNS are sent to skeletal muscles. Final result is a muscle contraction. Alpha motor neurons branch into several terminals (can be over 1000), each contacting a separate
Somatic nervous system Signals from CNS are sent to skeletal muscles. Final result is a muscle contraction. Alpha motor neurons branch into several terminals (can be over 1000), each contacting a separate
The Musculoskeletal System. Chapter 46
 The Musculoskeletal System Chapter 46 Types of Skeletal Systems Changes in movement occur because muscles pull against a support structure Zoologists recognize three types: 1. Hydrostatic skeletons a fluid
The Musculoskeletal System Chapter 46 Types of Skeletal Systems Changes in movement occur because muscles pull against a support structure Zoologists recognize three types: 1. Hydrostatic skeletons a fluid
Skeletal Muscle Contraction 5/11/2017 Dr. Hiwa Shafiq
 Skeletal Muscle Contraction 5/11/2017 Dr. Hiwa Shafiq Skeletal Muscle Fiber About 40 per cent of the body is skeletal muscle, and 10 per cent is smooth and cardiac muscle. Skeletal muscles are composed
Skeletal Muscle Contraction 5/11/2017 Dr. Hiwa Shafiq Skeletal Muscle Fiber About 40 per cent of the body is skeletal muscle, and 10 per cent is smooth and cardiac muscle. Skeletal muscles are composed
Section: Chapter 5: Multiple Choice. 1. The structure of synapses is best viewed with a(n):
 Section: Chapter 5: Multiple Choice 1. The structure of synapses is best viewed with a(n): p.155 electron microscope. light microscope. confocal microscope. nissle-stained microscopic procedure. 2. Electron
Section: Chapter 5: Multiple Choice 1. The structure of synapses is best viewed with a(n): p.155 electron microscope. light microscope. confocal microscope. nissle-stained microscopic procedure. 2. Electron
Skeletal Muscle. Cardiac Muscle. Smooth Muscle. II. Muscular System. The Muscular System
 Chapter CHAPTER 8 8 The Muscular System College Prep NOTES Smooth Muscle Found in body organs,vessels, respiratory passages Not striated, tapered, single cell nucleus involuntary, peristaltic contractions
Chapter CHAPTER 8 8 The Muscular System College Prep NOTES Smooth Muscle Found in body organs,vessels, respiratory passages Not striated, tapered, single cell nucleus involuntary, peristaltic contractions
Chapter 8: Skeletal Muscle: Structure and Function
 Chapter 8: Skeletal Muscle: Structure and Function Objectives Draw & label the microstructure of skeletal muscle Outline the steps leading to muscle shortening Define the concentric and isometric Discuss:
Chapter 8: Skeletal Muscle: Structure and Function Objectives Draw & label the microstructure of skeletal muscle Outline the steps leading to muscle shortening Define the concentric and isometric Discuss:
Biology 201-Worksheet on Muscle System (Answers are in your power point outlines-there is no key!)
 Bio 201 Tissues and Skin 1 February 23, 2011 Biology 201-Worksheet on Muscle System (Answers are in your power point outlines-there is no key!) 1. Name and define 5 characteristics of the muscle system.
Bio 201 Tissues and Skin 1 February 23, 2011 Biology 201-Worksheet on Muscle System (Answers are in your power point outlines-there is no key!) 1. Name and define 5 characteristics of the muscle system.
NEUROMUSCULAR BLOCKING AGENTS
 NEUROMUSCULAR BLOCKING AGENTS Edward JN Ishac, Ph.D. Associate Professor, Pharmacology and Toxicology Smith 742, 828-2127, Email: eishac@vcu.edu Learning Objectives: 1. Understand the physiology of the
NEUROMUSCULAR BLOCKING AGENTS Edward JN Ishac, Ph.D. Associate Professor, Pharmacology and Toxicology Smith 742, 828-2127, Email: eishac@vcu.edu Learning Objectives: 1. Understand the physiology of the
Synaptic Transmission
 Synaptic Transmission Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Synaptic transmission involves the release
Synaptic Transmission Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Synaptic transmission involves the release
NERVOUS SYSTEM NERVOUS SYSTEM. Somatic nervous system. Brain Spinal Cord Autonomic nervous system. Sympathetic nervous system
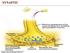 SYNAPTIC NERVOUS SYSTEM NERVOUS SYSTEM CENTRAL NERVOUS SYSTEM PERIPHERAL NERVOUS SYSTEM Brain Spinal Cord Autonomic nervous system Somatic nervous system Sympathetic nervous system Parasympathetic nervous
SYNAPTIC NERVOUS SYSTEM NERVOUS SYSTEM CENTRAL NERVOUS SYSTEM PERIPHERAL NERVOUS SYSTEM Brain Spinal Cord Autonomic nervous system Somatic nervous system Sympathetic nervous system Parasympathetic nervous
Skeletal Muscle Tissue
 Functions of Skeletal Muscle Skeletal Muscle Tissue Keri Muma Bio 6 Movement muscles attach directly or indirectly to bone, pull on bone or tissue when they contract Maintain posture / body position muscles
Functions of Skeletal Muscle Skeletal Muscle Tissue Keri Muma Bio 6 Movement muscles attach directly or indirectly to bone, pull on bone or tissue when they contract Maintain posture / body position muscles
Successive magnifications
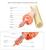 Successive magnifications Skeletal ("striated" = striped) muscle cell ("fiber" = cell) 10-100 microns (huge) and long (tendon to tendon) There are smaller units within fiber called "myofibrils" (1-2 microns
Successive magnifications Skeletal ("striated" = striped) muscle cell ("fiber" = cell) 10-100 microns (huge) and long (tendon to tendon) There are smaller units within fiber called "myofibrils" (1-2 microns
Musculoskeletal Systems. Anatomy: Arrangement of Cells Physiology: Contractions
 Musculoskeletal Systems Anatomy: Arrangement of Cells Physiology: Contractions Characteristics of all muscle Contractile: it shortens Excitable: receives & responds to electrical signals Extensible: stretches
Musculoskeletal Systems Anatomy: Arrangement of Cells Physiology: Contractions Characteristics of all muscle Contractile: it shortens Excitable: receives & responds to electrical signals Extensible: stretches
Stanley Iyadurai, PhD MD. Assistant Professor of Neurology/Neuromuscular Medicine Nationwide Children s Hospital Myology Course 2015
 1 Stanley Iyadurai, PhD MD Assistant Professor of Neurology/Neuromuscular Medicine Nationwide Children s Hospital Myology Course 2015 Motor unit motor neuron, its axon, and nerve terminals, and muscle
1 Stanley Iyadurai, PhD MD Assistant Professor of Neurology/Neuromuscular Medicine Nationwide Children s Hospital Myology Course 2015 Motor unit motor neuron, its axon, and nerve terminals, and muscle
Neuromuscular Blockers
 Neuromuscular Blockers Joanne Leung joanneleung22@hotmail.com Oct 14, 2014 Objectives After this lecture, you should be able to: Describe the physiology of the neuromuscular junction Differentiate the
Neuromuscular Blockers Joanne Leung joanneleung22@hotmail.com Oct 14, 2014 Objectives After this lecture, you should be able to: Describe the physiology of the neuromuscular junction Differentiate the
Neuromuscular Physiology. Skeletal muscle & Neuromuscular junction
 Neuromuscular Physiology. Skeletal muscle & Neuromuscular junction Dr. Ana-Maria Zagrean Discipline of Physiology and Fundamental Neuroscience, Carol Davila University of Medicine and Pharmacy Muscles:
Neuromuscular Physiology. Skeletal muscle & Neuromuscular junction Dr. Ana-Maria Zagrean Discipline of Physiology and Fundamental Neuroscience, Carol Davila University of Medicine and Pharmacy Muscles:
Honors Muscular System Notes CHAPTER 8
 Honors Muscular System Notes CHAPTER 8 I. Types of Muscle Tissue Fill in the chart with the correct information (p.162) Type of muscle Location Characteristics Control Action 1. 2. 3. II. The Muscular
Honors Muscular System Notes CHAPTER 8 I. Types of Muscle Tissue Fill in the chart with the correct information (p.162) Type of muscle Location Characteristics Control Action 1. 2. 3. II. The Muscular
SYNAPTIC COMMUNICATION
 BASICS OF NEUROBIOLOGY SYNAPTIC COMMUNICATION ZSOLT LIPOSITS 1 NERVE ENDINGS II. Interneuronal communication 2 INTERNEURONAL COMMUNICATION I. ELECTRONIC SYNAPSE GAP JUNCTION II. CHEMICAL SYNAPSE SYNAPSES
BASICS OF NEUROBIOLOGY SYNAPTIC COMMUNICATION ZSOLT LIPOSITS 1 NERVE ENDINGS II. Interneuronal communication 2 INTERNEURONAL COMMUNICATION I. ELECTRONIC SYNAPSE GAP JUNCTION II. CHEMICAL SYNAPSE SYNAPSES
The Muscular System. Objective: The student will become familiar with the structure and function of the muscular system
 The Muscular System Objective: The student will become familiar with the structure and function of the muscular system 1 Question of the day: What moves you? Composition: The musclar system makes up 40-50%
The Muscular System Objective: The student will become familiar with the structure and function of the muscular system 1 Question of the day: What moves you? Composition: The musclar system makes up 40-50%
Energy for Muscle Contractions: Direct phosphorylation. Creatine phosphate loses a phosphate to ADP to create ATP
 Energy for Muscle Contractions: Direct phosphorylation Aerobic respiration Anaerobic respiration (lactic acid fermentation) Creatine phosphate loses a phosphate to ADP to create ATP Requires oxygen to
Energy for Muscle Contractions: Direct phosphorylation Aerobic respiration Anaerobic respiration (lactic acid fermentation) Creatine phosphate loses a phosphate to ADP to create ATP Requires oxygen to
Session 3-Part 2: Skeletal Muscle
 Session 3-Part 2: Skeletal Muscle Course: Introduction to Exercise Science-Level 2 (Exercise Physiology) Presentation Created by Ken Baldwin, M.ED, ACSM-H/FI Copyright EFS Inc. All Rights Reserved. Skeletal
Session 3-Part 2: Skeletal Muscle Course: Introduction to Exercise Science-Level 2 (Exercise Physiology) Presentation Created by Ken Baldwin, M.ED, ACSM-H/FI Copyright EFS Inc. All Rights Reserved. Skeletal
BIOH111. o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system
 BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 10 Muscular Tissue Introduction The purpose of the chapter is to: 1. Learn about the structure and function of the 3 types of muscular tissue
Principles of Anatomy and Physiology 14 th Edition CHAPTER 10 Muscular Tissue Introduction The purpose of the chapter is to: 1. Learn about the structure and function of the 3 types of muscular tissue
3) Most of the organelles in a neuron are located in the A) dendritic region. B) axon hillock. C) axon. D) cell body. E) axon terminals.
 Chapter 48 Neurons, Synapses, and Signaling Multiple-Choice Questions 1) A simple nervous system A) must include chemical senses, mechanoreception, and vision. B) includes a minimum of 12 ganglia. C) has
Chapter 48 Neurons, Synapses, and Signaling Multiple-Choice Questions 1) A simple nervous system A) must include chemical senses, mechanoreception, and vision. B) includes a minimum of 12 ganglia. C) has
Bio 103 Muscular System 61
 61 Lecture Outline: MUSCULAR SYSTEM [Chapter 9] A. Functions of Skeletal Muscle 1. Movement 2. Maintain posture 3. Support 4. Guard openings 5. Maintain body temperature (thermogenesis) B. Muscle Tissue
61 Lecture Outline: MUSCULAR SYSTEM [Chapter 9] A. Functions of Skeletal Muscle 1. Movement 2. Maintain posture 3. Support 4. Guard openings 5. Maintain body temperature (thermogenesis) B. Muscle Tissue
Ch 12: Muscles sarcolemma, t-tubules, sarcoplasmic reticulum, myofibrils, myofilaments, sarcomere...
 Ch 12: Muscles Review micro-anatomy of muscle tissue Terminology examples: sarcolemma, t-tubules, sarcoplasmic reticulum, myofibrils, myofilaments, sarcomere... SLOs Differentiate levels of muscle structure:
Ch 12: Muscles Review micro-anatomy of muscle tissue Terminology examples: sarcolemma, t-tubules, sarcoplasmic reticulum, myofibrils, myofilaments, sarcomere... SLOs Differentiate levels of muscle structure:
Muscle Physiology. Bio 219 Dr. Adam Ross Napa Valley College
 Muscle Physiology Bio 219 Dr. Adam Ross Napa Valley College Muscle tissue Muscle is an excitable tissue capable of force production Three types Skeletal- striated, voluntary Cardiac- non-striated, involuntary
Muscle Physiology Bio 219 Dr. Adam Ross Napa Valley College Muscle tissue Muscle is an excitable tissue capable of force production Three types Skeletal- striated, voluntary Cardiac- non-striated, involuntary
AP Biology. Animal Locomotion. Muscles & Motor Locomotion. Why Do We Need All That ATP? Lots of ways to get around. Muscle
 Muscles & Motor Locomotion Animal Locomotion What are the advantages of locomotion? sessile motile Why Do We Need All That? 2006-2007 Lots of ways to get around Lots of ways to get around mollusk mammal
Muscles & Motor Locomotion Animal Locomotion What are the advantages of locomotion? sessile motile Why Do We Need All That? 2006-2007 Lots of ways to get around Lots of ways to get around mollusk mammal
MODULE 6 MUSCLE PHYSIOLOGY
 MODULE 6 MUSCLE PHYSIOLOGY III SEMESTER BOTANY Syllabi: Striated, Non striated and Cardiac muscle, Ultra structure of striated muscle fibre, Mechanism of muscle contraction, Threshold and spike potential,
MODULE 6 MUSCLE PHYSIOLOGY III SEMESTER BOTANY Syllabi: Striated, Non striated and Cardiac muscle, Ultra structure of striated muscle fibre, Mechanism of muscle contraction, Threshold and spike potential,
Nerve Muscle Relationship and Neural Muscular Junction Quiz. Remember, you need to know the structure and the function!
 Nerve Muscle Relationship and Neural Muscular Junction Quiz Remember, you need to know the structure and the function! What is this called? What is this? Schwann cell What is this called? Basal lamina
Nerve Muscle Relationship and Neural Muscular Junction Quiz Remember, you need to know the structure and the function! What is this called? What is this? Schwann cell What is this called? Basal lamina
Muscle Tissue. General concepts. Classification of muscle. I. Functional classification is based on the type of neural control.
 Muscle Tissue LEARNING OBJECTIVES 1. Identify the three types of muscle tissue at the light microscopic level. 2. List and compare the structural and functional features of each of the three muscle fiber
Muscle Tissue LEARNING OBJECTIVES 1. Identify the three types of muscle tissue at the light microscopic level. 2. List and compare the structural and functional features of each of the three muscle fiber
1. Differences in function of the 3 muscle types: a) Skeletal Muscle b) Cardiac Muscle c) Smooth Muscle
 Ch 9: Muscle Physiology Objectives: 1. Review 3 muscle types and how they are regulated. 2. Review muscle anatomy. 3. Sliding filament theory of how muscles contract and relax. 4. Energetics of muscle
Ch 9: Muscle Physiology Objectives: 1. Review 3 muscle types and how they are regulated. 2. Review muscle anatomy. 3. Sliding filament theory of how muscles contract and relax. 4. Energetics of muscle
EVIDENCE FOR NEUROTRANSMITTER DYSREGULATION IDENTIFIED OR PUBLISHED SINCE THE REVIEW PROCESS
 Addendum EVIDENCE FOR NEUROTRANSMITTER DYSREGULATION IDENTIFIED OR PUBLISHED SINCE THE REVIEW PROCESS Information not included in the original discussion of neurotransmitter dysregulation is provided here.
Addendum EVIDENCE FOR NEUROTRANSMITTER DYSREGULATION IDENTIFIED OR PUBLISHED SINCE THE REVIEW PROCESS Information not included in the original discussion of neurotransmitter dysregulation is provided here.
Connective tissue MUSCLE TISSUE
 Connective tissue MUSCLE TISSUE Part 1 General features of MT Develop from mesoderm Many cells, less intercellular matrix Function contraction (shortening) Skeletal (striated, voluntary) Types of MT Cardiac
Connective tissue MUSCLE TISSUE Part 1 General features of MT Develop from mesoderm Many cells, less intercellular matrix Function contraction (shortening) Skeletal (striated, voluntary) Types of MT Cardiac
Muscles & Motor Locomotion Why Do We Need All That ATP?
 Muscles & Motor Locomotion Why Do We Need All That ATP? 2006-2007 Animal Locomotion What are the advantages of locomotion? sessile motile Lots of ways to get around Lots of ways to get around mollusk mammal
Muscles & Motor Locomotion Why Do We Need All That ATP? 2006-2007 Animal Locomotion What are the advantages of locomotion? sessile motile Lots of ways to get around Lots of ways to get around mollusk mammal
The Muscular System. Specialized tissue that enable the body and its parts to move.
 The Muscular System Specialized tissue that enable the body and its parts to move. Anterior View Posterior View TRIVIA! How many muscles are there in the human body? Answer: 640 Muscles The muscles make
The Muscular System Specialized tissue that enable the body and its parts to move. Anterior View Posterior View TRIVIA! How many muscles are there in the human body? Answer: 640 Muscles The muscles make
Ch 12 can be done in one lecture
 Ch 12 can be done in one lecture Developed by John Gallagher, MS, DVM Chapter 12: Muscles Review muscle anatomy (esp. microanatomy of skeletal muscle) Terminology: sarcolemma t-tubules sarcoplasmic reticulum
Ch 12 can be done in one lecture Developed by John Gallagher, MS, DVM Chapter 12: Muscles Review muscle anatomy (esp. microanatomy of skeletal muscle) Terminology: sarcolemma t-tubules sarcoplasmic reticulum
Muscle Tissue. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Muscle Tissue Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Functions of muscle tissue Movement Maintenance of posture Joint stabilization Heat generation Tendon Belly Tendon Types of
Muscle Tissue Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Functions of muscle tissue Movement Maintenance of posture Joint stabilization Heat generation Tendon Belly Tendon Types of
Lecture Overview. Muscular System. Marieb s Human Anatomy and Physiology. Chapter 9 Muscles and Muscle Tissue Lecture 16
 Marieb s Human Anatomy and Physiology Marieb Hoehn Chapter 9 Muscles and Muscle Tissue Lecture 16 1 Lecture Overview Types, characteristics, functions of muscle Structure of skeletal muscle Mechanism of
Marieb s Human Anatomy and Physiology Marieb Hoehn Chapter 9 Muscles and Muscle Tissue Lecture 16 1 Lecture Overview Types, characteristics, functions of muscle Structure of skeletal muscle Mechanism of
Essentials of Human Anatomy & Physiology. The Muscular System
 Essentials of Human Anatomy & Physiology The Muscular System The Muscular System Muscles are responsible for all types of body movement they contract or shorten and are the machine of the body Three basic
Essentials of Human Anatomy & Physiology The Muscular System The Muscular System Muscles are responsible for all types of body movement they contract or shorten and are the machine of the body Three basic
Contrac7on. Ch. 9 A- 2 Notes 11/30/14. Sliding Filament Model of Contrac7on. Requirements for Skeletal Muscle Contrac7on
 Contrac7on Ch. 9 A- 2 Notes The genera7on of Does not necessarily cause shortening of the fiber Shortening occurs when tension generated by cross bridges on the thin filaments forces opposing shortening
Contrac7on Ch. 9 A- 2 Notes The genera7on of Does not necessarily cause shortening of the fiber Shortening occurs when tension generated by cross bridges on the thin filaments forces opposing shortening
NEURONS COMMUNICATE WITH OTHER CELLS AT SYNAPSES 34.3
 NEURONS COMMUNICATE WITH OTHER CELLS AT SYNAPSES 34.3 NEURONS COMMUNICATE WITH OTHER CELLS AT SYNAPSES Neurons communicate with other neurons or target cells at synapses. Chemical synapse: a very narrow
NEURONS COMMUNICATE WITH OTHER CELLS AT SYNAPSES 34.3 NEURONS COMMUNICATE WITH OTHER CELLS AT SYNAPSES Neurons communicate with other neurons or target cells at synapses. Chemical synapse: a very narrow
