Derivation and Validation of a CT Scan Scoring System for Discriminating Malignant From Benign Pleural Effusions
|
|
|
- Ross Reynolds
- 6 years ago
- Views:
Transcription
1 [ Original Research Disorders of the Pleura ] Derivation and Validation of a CT Scan Scoring System for Discriminating Malignant From Benign Pleural Effusions José M. Porcel, MD, FCCP ; Marina Pardina, MD ; Silvia Bielsa, MD ; Antonio González, MD ; and Richard W. Light, MD, FCCP BACKGROUND: Chest CT scanning has become an integral part of the workup for undiagnosed pleural effusions. We aimed to develop a CT scan-based scoring system for differentiating between benign and malignant pleural effusions. METHODS: A number of chest CT scan abnormalities were compared between 228 patients with benign and 115 with malignant effusions (derivation cohort). A logistic regression analysis was used to identify the independent predictors of malignancy and generate CT scan scores, with more points assigned to those findings associated with higher b-coefficient values. The diagnostic accuracy of the CT scan scoring system was calculated for the derivation cohort and further evaluated in two independent populations (n 5 80 and 42, respectively) by two radiologists. RESULTS: CT scan scores predicting malignancy included any pleural lesion (ie, nodule, mass, or thickening) 1 cm (5 points); the presence of liver metastases, an abdominal mass, or a lung mass or nodule 1 cm (3 points each); and the absence of either pleural loculations, pericardial effusions, or cardiomegaly (2 points each). In the first validation cohort, a sum score of 7 yielded a sensitivity of 88% (95% CI, 73%-95%), specificity of 94% (95% CI, 83%-98%), likelihood ratio positive of 13.8 (95% CI, ), likelihood ratio negative of 0.13 (95% CI, ), and area under the receiver operating characteristics curve of (95% CI, ). Moreover, 69% of 42 patients with pathologically unconfirmed malignant effusions from a second independent cohort would have been correctly labeled by the predictive score. CONCLUSIONS: A simple CT scan-based scoring system can help physicians to separate malignant from benign pleural effusions. CHEST 2015; 147(2): Manuscript received January 3, 2014; revision accepted September 3, 2014; originally published Online First September 25, ABBREVIATIONS: AUC 5 area under the receiver operating characteristic curve; HU 5 Hounsfield units; LR 5 likelihood ratio; ROC 5 receiver operating characteristic AFFILIATIONS: From the Department of Internal Medicine (Drs Porcel and Bielsa) and the Department of Radiology (Drs Pardina and González), Pleural Diseases Unit, Arnau de Vilanova University Hospital, Biomedical Research Institute of Lleida, Lleida, Spain; and the Division of Allergy, Pulmonary, and Critical Care (Dr Light), Vanderbilt University Medical Center, Nashville, TN. FUNDING/SUPPORT: The authors have reported to CHEST that no funding was received for this study. CORRESPONDENCE TO: José M. Porcel, MD, FCCP, Department of Internal Medicine, Arnau de Vilanova University Hospital, Avda Alcalde Rovira Roure 80, Lleida, Spain; jporcelp@yahoo.es 2015 AMERICAN COLLEGE OF CHEST PHYSICIANS. Reproduction of this article is prohibited without written permission from the American College of Chest Physicians. See online for more details. DOI: /chest journal.publications.chestnet.org 513
2 Clinicians often encounter patients with pleural effusions that remain undiagnosed after the initial workup, which includes a thoracentesis. One of the main concerns is to rule out malignancy, since it is well known that pleural fluid cytology has a sensitivity of only 60%. 1 Another concern is to avoid subjecting frail patients to unnecessary invasive procedures and selecting just those who may benefit the most from such interventions. Chest CT scans furnish clues for a potentially underlying pathology in patients with pleural effusions (eg, pulmonary infiltrates, masses or emboli, mediastinal lymphadenopathies, or pericardial involvement). In addition, several CT scan features have been described in previous studies that may aid in the differentiation of malignant from benign pleural conditions. For example, images may reveal pleural nodularity and thickening, which are considered highly suggestive of a malignant cause. 1 However, the evidence supporting the discriminatory role of CT scanning relies upon just a few series in which the results were not validated in an independent population and often included a large percentage of mesotheliomas, which are more likely to exhibit abnormalities of the pleural surfaces. 2-8 In the present study, in addition to addressing the previous shortcomings we aimed to develop a simple CT scan scoring system, based on easily identifiable radiologic data, to be used by pulmonologists as a tool for separating malignant effusions from benign pleurisy. Materials and Methods Patient Selection From June 2008 to December 2011, all adult patients with pleural effusions who underwent both a diagnostic thoracentesis and a contrastenhanced chest CT scan at our institution, being determined as necessary by the attending physicians, were enrolled in this prospective study. Obtaining a definite cause of the pleural effusion was required for final inclusion. This population allowed for the generation of a pleural malignant-benign discriminating CT scan score, which was subsequently validated in a different set of patients recruited prospectively during Two different cohorts were further analyzed. One (ie, validation cohort) was composed of a stratified sample of consecutive patients with confirmed benign and malignant pleural effusions, to closely mirror the derivation cohort with respect to the distribution of causes. The other included patients with highly probable, but unconfirmed, malignant effusions based on the following criteria: demonstration of a primary tumor or clinical evidence of tumor dissemination (eg, liver metastases); exclusion of other potential causes for the effusion; and negative pleural fluid cytologic examination, which was considered to be a falsenegative result. In this subgroup of patients, a definitive diagnosis of malignancy through a pleural biopsy was not pursued, because the oncologist did not anticipate a change in treatment strategy in the event of a histopathologic confirmation of the pleural cancer, because of one of the following reasons: (1) the patient had a poor performance status, and, consequently, only palliative care was indicated; or (2) adjuvant chemotherapy and/or radiotherapy was already being considered as a beneficial treatment. The institutional ethics committee of our hospital (CEIC, University Hospital Arnau de Vilanova, ID 974/2011) approved the study protocol, and the participants signed written informed consent. Diagnostic Criteria An effusion was categorized as malignant if malignant cells were detected upon cytologic examination of the pleural fluid or biopsy specimens. Tuberculous pleuritis was diagnosed if Ziehl-Neelsen stains or Lowenstein-Jensen cultures of pleural fluid, sputum, or pleural biopsy specimens were positive or if granulomas were found in the parietal pleural biopsies. TB was considered probable in patients with lymphocytic exudates containing high pleural adenosine deaminase levels (. 35 U/L) that cleared in response to antituberculous therapy. A parapneumonic effusion was defined as any effusion associated with bacterial pneumonia, lung abscess, or bronchiectasis, and empyema described the presence of pus within the pleural space. The diagnosis of heart failure was based on history, physical examination, chest radiographs, ECG, echocardiogram (if available), and response to diuretics. Other causes of pleural effusions followed well-established clinical criteria. All patients with benign conditions were followed up by means of clinical examination and imaging until the complete resolution of the pleural effusion. CT Scan Examination All CT imaging studies were performed with a 16-multiple detector CT scanner (Brilliance 16; Koninklijke Philips N.V.), using the following scan parameters: collimation mm, tube rotation time 0.75 s, pitch 0.938, 120 kv, and section thickness of 3 mm with a 1.5-mm reconstruction interval. Patients were given 120 ml of nonionic contrast material (iobitridol, Xenetic 300; Guerbet Group; or iopromide, Ultravist 300; Bayer AG) at 3 ml/s injected through an IV cannula (Abbocath 20G) with a mechanical automated injector (Med-tron). Images, which were acquired after a 60-s delay from the start of injection, extended from the lung apices to the level of the adrenals and were viewed with a picture archiving and communication system with standard lung (level, 2450 Hounsfield units [HU]; width, 1,600 HU) and mediastinal (level, 40 HU; width, 400 HU) windows. The CT scan features evaluated for the discriminating analysis were: (1) focal pleural thickening (ie, a visible pleural line of 3 mm, limited to a single lobe); (2) diffuse pleural thickening, which was further characterized by whether it enveloped the entire perimeter of the hemithorax at any CT scan slice (circumferential thickening); (3) pleural nodules (ie, focal pleural thickening with a nodular contour and, 3 cm in length); both nodules and thickening were assessed in terms of their precise size and anatomic location (eg, parietal, visceral, mediastinal, or diaphragmatic); (4) pleural-based masses ( 3 cm); (5) pleural contrast enhancement, including the split pleural sign, whereby enhanced visceral and parietal pleural surfaces are seen separated by pleural fluid; (6) increase in attenuation of extrapleural fat; (7) pleural calcifications; (8) pleural fluid attenuation values expressed in HU; (9) pleural loculations (ie, an effusion that is compartmentalized, or has septations or a convex shape facing the lung parenchyma, or is accumulated in a nondependent portion); (10) effusion s side (bilaterality); (11) volume of pleural effusions using a previously reported formula 9 ; (12) thoracic lymph node enlargement. 1 cm in the short-axis diameter; (13) parenchymal lung lesions (ie, nodules, masses, atelectasis, alveolar or interstitial patterns); (14) pericardial effusion; (15) cardiomegaly (cardiothoracic ratio. 0.5 in axial images); (16) liver metastases; (17) abdominal masses displayed at the upper abdominal slices from chest CT scan; (18) hepatomegaly (craniocaudal liver span cm in the midclavicular line); and (19) dilation of the inferior vena cava (diameter. 1.7 cm) measured just above the entrance of the suprahepatic veins. Interpretation of chest CT imaging in the derivation cohort was done by a thoracic radiologist blinded to the final diagnosis. The same 514 Original Research [ 147 # 2 CHEST FEBRUARY 2015 ]
3 investigator, together with a general radiologist, both with 20 years of experience, applied the resulting CT scan scoring system to the validation cohorts, also in blinded fashion, with disagreements resolved by consensus. For bilateral pleural effusions, the CT scan findings were recorded from the side of diagnostic thoracentesis or biopsy. Statistical Analysis Categorical and continuous data are expressed as numbers (percentages) and medians (25th and 75th percentiles), respectively. Between-group comparisons were performed with the x 2, Fisher exact, Kruskal-Wallis, and Mann-Whitney U tests, as appropriate. Receiver operating characteristic (ROC) curve analysis helped to decide the optimal cutoff points for continuous variables based on their highest diagnostic accuracy. A logistic regression analysis with backward conditional method served to select those radiologic variables entering the scoring system. Weight values to each variable were assigned proportionally to the magnitude of the logistic equation s coefficients. The diagnostic performance of the derived score for labeling malignant pleural effusions in both the derivation and validation cohorts was calculated through contingency tables (sensitivity, specificity, likelihood ratios [LRs]) and the area under ROC curve (AUC). Interobserver agreement about radiologic signs was expressed using the k statistic. The statistical significance level was set at 0.05 (two-tailed). All analyses were conducted with the SPSS version 18.0 statistical software (IBM). Results Study Population Baseline characteristics of the 343 patients who composed the derivation cohort are shown in Table 1. Patients were aged 69 (53-80) years, 59% were men, and 34% had malignant effusions, which were metastatic in 94% of the cases. Lung cancer was the leading cause (36.5%) of pleural malignancies. The validation cohort consisted of 80 patients, with a median age of 71 (55-83) years, of whom 41% had pleural malignancy, mostly (97%) of metastatic origin. The generated CT scan score was also applied to an additional sample of 42 patients (median age, 73 [58-85] years, 52% men) TABLE 1 ] Baseline Characteristics of the Derivation and Validation Cohort Characteristic Derivation Cohort (n 5 343) Validation Cohort (n 5 80) P Value Age, y 69 (53-80) 71 (55-83).24 Male 201 (59) 51 (64).25 Malignant effusions 115 (34) 33 (41).92 Lung Unknown origin 15 5 Breast 14 4 Lymphoma 14 4 Ovary 8 3 Mesothelioma 6 1 Miscellaneous 15 5 Benign effusions 228 (66) 47 (59).72 Parapneumonics Heart failure TB 22 5 Pericardial diseases 9 4 Pulmonary emboli 9 2 Miscellaneous 30 5 Data are expressed as No. (%), No., or median (quartiles) as appropriate. with probable malignant effusions from the following tumor primaries: 21 lung; six breast; two each of lymphoma, kidney, melanoma, pancreas, colon, and stomach; and one each of sarcoma, unknown primary, and GI stromal tumor. CT Scan Data From the Derivation Cohort Most of the evaluated radiologic variables were found to be significantly different between malignant and benign pleural effusions in the bivariate analysis, with the exception of bilateral effusions, circumferential pleural thickening, pleural calcifications, pleural enhancement after contrast infusion, CT scan attenuation values of the pleural fluid, and hepatomegaly ( Table 2 ). Pleural nodularity or thickening 1 cm (cutoff established by ROC analysis) was the most consistent feature arguing for malignant effusions (Figs 1, 2 ). Three patients with benign conditions (two TB and one sarcoidosis) exhibited pleural nodules, 1 cm. Two of those three patients (one TB and one sarcoidosis) also had focal pleural thickening, 1 cm. Diffuse pleural thickening was present in 11 parapneumonics/empyemas, which was circumferential for seven, and measured. 1 cm in one. The presence of any pleural lesion 1 cm, either nodules, masses, or thickening, had a sensitivity of 43% (95% CI, 34%-52%), specificity of 99.6% (95% CI, 98%-100%), LR positive of 97.2 (95% CI, ), and LR negative of 0.58 (95% CI, ) for identifying malignant effusions. Of interest, CT scan showed pleural loculations in 78 (76%) parapneumonics/empyemas and 13 (59%) tuberculous, 40 (35%) malignant, and 16 (29%) heart failure-related effusions. Thoracic lymphadenopathies were seen in 35%, 41%, 50%, and 15% of these respective causes. As expected, cardiomegaly and dilation of the inferior vena cava were prevalent (55% and 100%, respectively) in heart failure, also being characterized by a low attenuation coefficient (decreased density) of the pleural fluid ( 2 4 HU; quartiles, 2 7 to 1). journal.publications.chestnet.org 515
4 TABLE 2 ] Chest CT Scan Findings in the Derivation Cohort Chest CT Scan Characteristics Benign Effusions (n 5 228) Malignant Effusions (n 5 115) P Value Pleural nodules 3 (1.3) 44 (38),.01 Pleural nodules 1 cm 0 (0) 40 (35),.01 Pleural masses 0 (0) 11 (9.5),.01 Focal pleural thickening 2 (0.9) 23 (20),.01 Focal pleural thickening 1 cm 0 (0) 14 (12),.01 Diffuse pleural thickening 11 (5) 15 (13),.01 Diffuse pleural thickening 1 cm 1 (0.4) 13 (11),.01 Focal or diffuse pleural thickening 1 cm 1 (0.4) 24 (21),.01 Circumferential pleural thickening 7 (3) 5 (4).54 Pleural nodules or thickening 1 cm 1 (0.4) 49 (43),.01 Mediastinal pleural involvement 10 (4) 36 (31),.01 Bilateral pleural effusions 68 (30) 24 (21).08 Pleural contrast enhancement 119 (52) 50 (43).14 Split pleural sign 10 (4) 4 (3).71 Increased attenuation of extrapleural fat 9 (4) 16 (14),.01 Pleural calcifications 1 (0.4) 0 (0).47 Pleural fluid attenuation values, Hounsfield units 4 ( 2 3 to 9.5) 5 (1 to 10).23 Pleural loculations 129 (57) 40 (35),.01 Pleural effusion s size, a ml 400 (200 to 988) 800 (350 to 1,800),.01 Thoracic lymph nodes. 1 cm 56 (25) 57 (50),.01 Lung mass 4 (2) 32 (28),.01 Lung nodule/s 13 (6) 34 (30),.01 Lung nodule 1-3 cm 11 (5) 24 (21),.01 Obstructive atelectasis 4 (2) 43 (37),.01 Pericardial effusion 28 (12) 2 (2),.01 Cardiomegaly 41 (18) 4 (3),.01 Liver metastases 2 (0.9) 21 (18),.01 Abdominal mass (scan extended to the adrenals) 2 (0.9) b 17 (15) b,.01 Hepatomegaly 10 (4) 2 (2).19 Inferior vena cava. 1.7 cm 205 (90) 68 (59),.01 Data are expressed as No. (%) or median (quartiles) as appropriate. a Pleural fl uid volume was calculated by a formula from Reference 9. b Abdominal masses were located in the peritoneum (7), suprarenal glands (4), pancreas (2), kidney (2), lymph nodes (2), spleen (1), and stomach (1). Generation of a CT Scan Score All radiologic findings that displayed statistical significance in the bivariate analysis were processed using a multivariable logistic regression model. The model selected nine as being predictive of malignancy. However, two of them, namely obstructive atelectasis and the volume of pleural effusion, were then excluded because they are not readily recognizable by an inexperienced pulmonologist. The remaining seven parameters helped to establish weight scores ( Table 3 ) as follows: any pleural lesion 1 cm (5 points), liver metastases (3 points), abdominal mass (3 points), lung mass or lung nodule 1 cm (3 points), absence of pleural loculations (2 points), no pericardial effusion (2 points), and nonenlarged cardiac silhouette (2 points). Thus, CT scan scores ranged from 0 to 20. Table 4 shows the performance of predictive scores in the derivation group. As the cutoff value was raised, the specificity of the rule increased, whereas the sensitivity concurrently decreased. At the best cutoff of 7 points, the scoring system yielded 74% sensitivity (95% CI, 65%-81%), 92% specificity (95% CI, 88%-95%), LR positive 9.4 (95% CI, ), LR negative 0.28 (95% CI, ), and AUC (95% CI, ) 516 Original Research [ 147 # 2 CHEST FEBRUARY 2015 ]
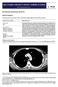
5 TABLE 3 ] CT Scan Scoring System for Predicting Malignant Pleural Effusions Parameters OR (95% CI) Score Any pleural lesion a 1 cm 250 (24-2,650) 5 Liver metastases 30.7 (6-156) 3 Abdominal mass 15.3 (4-65) 3 Lung mass or lung nodule/s 1 cm Absence of pleural loculations 12.2 (5-29) (2-9) 2 No pericardial effusion 23.5 (1-626) 2 Nonenlarged cardiac silhouette 9.3 (2-48) 2 a Nodule, mass, or thickening. Figure 1 CT scan showing a malignant pleural nodule (arrowhead). for discriminating malignant and benign pleural effusions. The respective median CT scan scores in patients with heart failure, parapneumonics, TB, and malignancy were 4 (2-6), 4 (4-6), 6 (4-7), and 9 (6-11). If we had only considered patients with exudative effusions and a negative first cytologic fluid analysis, which reflects a more typical scenario in which CT scan is ordered, a CT scan score 7 would have had 74% sensitivity (95% CI, 55%-87%), 91% specificity (95% CI, 85%-95%), LR positive 8.44 (95% CI, ), and LR negative 0.28 (95% CI, ) for labeling malignant pleurisy. Validation of the CT Scan Scoring System The operating characteristics of a CT scan score 7 in the validation cohort (33 malignant and 47 benign new effusions) were: sensitivity 88% (95% CI, 73%-95%), specificity 94% (95% CI, 83%-98%), LR positive 13.8 (95% CI, ), LR negative 0.13 (95% CI, ), Figure 2 Radiologic appearance of malignant pleural thickening (arrowheads). and AUC (95% CI, ). The predictive model was then evaluated in 42 patients with a clinical diagnosis of malignant effusions whose pleural fluid cytology was considered to be falsely negative. Ten (24%) exhibited pleural lesions 1 cm, 22 (52%) lung masses or nodules 1 cm, eight (19%) abdominal masses, and six (14%) liver metastases, whereas the absence of pleural loculations, pericardial effusions, and cardiomegaly characterized 24 (57%), 40 (95%), and 36 (86%) cases, respectively. Overall, 29 (69%) patients scored 7, a figure that did not differ significantly from that of the confirmed malignant effusions from the derivation cohort (74%, P 5.54). For most of the parameters composing the CT scan score, the interobserver agreement was substantial, as indicated by a k statistic. 0.6 (Table 5 ). Discussion We have developed and validated a CT scan scoring system to assess the probability of malignancy in patients with pleural effusions. The proposed method not only appears to be simple and feasible but also has high interobserver reliability and accurately distinguishes between benign and malignant pleural effusions, as reflected by an AUC of From a maximum sum of 20 points, a score 7 would prompt consideration of a malignant process, whereas a score of, 5 would mitigate against it. Of note, the discriminative properties of the CT scan scoring system remained unchanged for the subgroup of patients in whom no diagnosis had been obtained after an initial thoracentesis (ie, exudative effusion and a first negative pleural fluid cytologic result), the population for which CT scan is most commonly ordered in routine clinical practice. Although the CT scan findings of pleural effusions secondary to malignancy, 10 empyema, 11 or TB 12 have been journal.publications.chestnet.org 517
6 TABLE 4 ] Operating Characteristics of the CT Scan Scoring System for Identifying Malignant Effusions (Derivation Cohort) Score Sensitivity, % (95% CI) Specificity, % (95% CI) LR Positive (95% CI) LR Negative (95% CI) 5 or 6 93 (87-96) 68 (61-73) 2.9 ( ) 0.10 ( ) 7 74 (65-81) 92 (88-95) 9.4 ( ) 0.28 ( ) 8 or 9 59 (50-68) 97 (94-99) 22.5 ( ) 0.42 ( ) (21-38) 100 (98-100) 65.4 ( ) 0.72 ( ) LR 5 likelihood ratio. described individually, few previous studies have analyzed the value of CT scan for the differential diagnosis of benign and malignant causes of pleural effusions. 2-8 Unfortunately, most were retrospective, 2-4,6-8 did not perform a multivariate analysis to select the relevant CT scan discriminative data, 2-5,7,8 and, most importantly, did not validate their findings using an independent population. 2-8 Some CT scan features, namely pleural nodularity, pleural thickening 1 cm, circumferential thickening (pleural rind) and mediastinal pleural involvement have been consistently reported as highly suggestive of a malignant process. The sum of seven series, totaling 457 patients with malignant pleural effusions (35% mesotheliomas) and 475 with benign pleural conditions (50% TB), 2-8 yields respective mean sensitivities and specificities for the preceding CT scan data as follows: pleural nodules, 39% (range, 18%-53%) and 95% (range, 87%-100%) 2-8 ; pleural thickening 1 cm, 34% (range, 7%-47%) and 87% (range, 64%-98%) 2,6-8 ; mediastinal pleural involvement, 46.5% (range, 14%-74%) and 84% (range, 68%-97%) 2-4,6-8 ; and pleural rind, 32% (range, 7%-54%) and 88.5% (range, 63%-100%). 2-8 The operating characteristics of pleural nodules and thickening in our large prospective series compared similarly with these figures. Nevertheless, our findings showed a trend toward a lower proportion of pleural rind (4%) in malignant effusions, probably due to the low number of mesothelioma cases TABLE 5 ] Interobserver Agreement for CT Scan Variables (Validation Cohort) CT Scan Findings k Coefficient (95% CI) Any pleural lesion 1 cm 0.81 ( ) Liver metastases 0.94 (0.84-1) Abdominal mass 0.88 (0.73-1) Lung mass or lung nodule/s 1 cm 0.86 ( ) Absence of pleural loculations 0.55 ( ) No pericardial effusion 0.84 (0.63-1) Nonenlarged cardiac silhouette 0.65 ( ) included. Furthermore, some classic malignant-related radiologic data, such as pleural mediastinal involvement, lost significance as predictors of malignancy due to the strong influence of pleural nodularity or thickening in the logistic regression model. It was found that benign conditions, such as TB and parapneumonic effusions, rarely demonstrated some features typically associated with metastases to the pleura, that is, pleural nodularity and thickening. These particular CT scan findings are also helpful in guiding pleural biopsies to the sites more likely to yield a positive diagnosis, in cases where pleural fluid analyses are not contributory. 13 In this sense, pleural lesions easily amenable to biopsy occurred in 43% of confirmed and 24% of cytologically negative malignant effusions. The generated scoring system outperformed the predictive capability of any individual parameter. Its diagnostic threshold (7 points) was exceeded by about threefourths of patients with malignant pleurisy, regardless of the results of pleural fluid cytology. Th is study is subject to limitations. It can be argued that the applicability of the scoring system may depend on the prevalence of specific causes of pleural effusions in the population in which it is to be implemented. Our derivation and validation cohorts accurately reflected the relative proportion of pleural effusion causes in our country. 14 For example, lung cancer and mesothelioma accounted for 37% and 3% of 840 malignant effusions, respectively, whereas TB was the cause of 9% of 3,077 pleural effusions in a recent series from our hospital. 14 In the derivation cohort, these percentages were 36.5%, 5%, and 6.5%, respectively. However, in other geographic areas, the incidence of mesothelioma or TB may substantially change and so too may the accuracy of the CT scan score. In most of the previous benignmalignant CT scan discrimination studies, there was indeed an overrepresentation of mesotheliomas 2,3,5-7 and TB 6-8 in the comparison groups, pointing to a selection bias. A second potential limitation relates to radiologic interpretation. Although the radiologist was 518 Original Research [ 147 # 2 CHEST FEBRUARY 2015 ]
7 blinded to the clinical diagnosis, the assessment of the pleural surfaces may have been biased in those patients having additional CT scan features that suggested malignancy (eg, liver metastases, lung masses or nodules). Moreover, the requirement for both CT scan and pleural fluid data among the inclusion criteria might appear to introduce a potential selection bias. However, knowledge of pleural fluid analyses is essential for definitively classifying patients who undergo a CT scan examination as having a definite malignant or benign effusion. Finally, the scoring system should be viewed as an aid for constructing a differential diagnosis of pleural effusions, which does not preclude obtaining a cytohistologic confirmation of malignancy. It may be considered a diagnostic weight to estimate the probability of malignancy, in combination with other clinical findings. A prospective validation of this CT scan score in large cohorts is warranted. To conclude, a simple chest CT scan scoring system, which includes the evaluation of pleural nodularity or thickening, liver metastases, abdominal masses, lung nodules or masses, pleural loculations, pericardial effusions, and cardiomegaly, may be reliably used for the differential diagnosis of pleural effusions. Acknowledgments Author contributions: J. M. P. is the guarantor of this study. J. M. P. contributed to conception and design, acquisition of data, drafting the manuscript, and approving the final version; M. P. contributed to acquisition of data, analysis and interpretation of data, and approving the final version; S. B. contributed to research design, analysis and interpretation of data, and approving the final version; A. G. contributed to analysis and interpretation of data and approving the final version; and R. W. L. contributed to critical revision of the manuscript for important intellectual content and approving the final version. Financial/nonfinancial disclosures: The authors have reported to CHEST that no potential conflicts of interest exist with any companies/organizations whose products or services may be discussed in this article. References 1. Porcel JM, Light RW. Pleural effusions. Dis Mon ;59(2): Leung AN, Müller NL, Miller RR. CT in differential diagnosis of diffuse pleural disease. AJR Am J Roentgenol ;154(3): Hierholzer J, Luo L, Bittner RC, et al. MRI and CT in the differential diagnosis of pleural disease. Chest ;118(3): Arenas-Jiménez J, Alonso-Charterina S, Sánchez-Payá J, Fernández-Latorre F, Gil-Sánchez S, Lloret-Llorens M. Evaluation of CT findings for diagnosis of pleural effusions. Eur Radiol ; 10 (4): Traill ZC, Davies RJ, Gleeson FV. Thoracic computed tomography in patients with suspected malignant pleural effusions. Clin Radiol ;56(3): Metintas M, Ucgun I, Elbek O, et al. Computed tomography features in malignant pleural mesothelioma and other commonly seen pleural diseases. Eur J Radiol ;41(1): Yilmaz U, Polat G, Sahin N, Soy O, Gülay U. CT in differential diagnosis of benign and malignant pleural disease. Monaldi Arch Chest Dis ;63(1): Kim JS, Shim SS, Kim Y, Ryu YJ, Lee JH. Chest CT findings of pleural tuberculosis: differential diagnosis of pleural tuberculosis and malignant pleural dissemination. Acta Radiol ;55(9): Mergo PJ, Helmberger T, Didovic J, Cernigliaro J, Ros PR, Staab EV. New formula for quantification of pleural effusions from computed tomography. J Thorac Imaging ;14(2): O Donovan PB, Eng P. Pleural changes in malignant pleural effusions: appearance on computed tomography. Cleve Clin J Med ;61(2): Waite RJ, Carbonneau RJ, Balikian JP, Umali CB, Pezzella AT, Nash G. Parietal pleural changes in empyema: appearances at CT. Radiology ; 175 ( 1 ): Yilmaz MU, Kumcuoglu Z, Utkaner G, Yalniz O, Erkmen G. Computed tomography findings of tuberculous pleurisy. Int J Tuberc Lung Dis ; 2 ( 2 ): Maskell NA, Gleeson FV, Davies RJ. Standard pleural biopsy versus CT-guided cutting-needle biopsy for diagnosis of malignant disease in pleural effusions: a randomised controlled trial. Lancet ;361(9366): Porcel JM, Esquerda A, Vives M, Bielsa S. Etiology of pleural effusions: analysis of more than 3,000 consecutive thoracenteses. Arch Bronconeumol ;50(5): journal.publications.chestnet.org 519
JMSCR Vol 04 Issue 10 Page October 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i10.08 Ultrasound and CT Evaluation of Pleural
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i10.08 Ultrasound and CT Evaluation of Pleural
Chest Radiology Interpretation: Findings of Tuberculosis
 Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
Diffuse high-attenuation within mediastinal lymph nodes on non-enhanced CT scan: Usefulness in the prediction of benignancy
 Diffuse high-attenuation within mediastinal lymph nodes on non-enhanced CT scan: Usefulness in the prediction of benignancy Poster No.: C-1785 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific
Diffuse high-attenuation within mediastinal lymph nodes on non-enhanced CT scan: Usefulness in the prediction of benignancy Poster No.: C-1785 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific
Malignant Effusions. Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital
 Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
Atypical Pleural Fluid Profiles in Tuberculous Pleural Effusion: Sequential Changes Compared with Parapneumonic and Malignant Pleural Effusions
 ORIGINAL ARTICLE Atypical Pleural Fluid Profiles in Tuberculous Pleural Effusion: Sequential Changes Compared with Parapneumonic and Malignant Pleural Effusions Chang Ho Kim, So Yeon Lee, Yong Dae Lee,
ORIGINAL ARTICLE Atypical Pleural Fluid Profiles in Tuberculous Pleural Effusion: Sequential Changes Compared with Parapneumonic and Malignant Pleural Effusions Chang Ho Kim, So Yeon Lee, Yong Dae Lee,
TB Intensive Houston, Texas
 TB Intensive Houston, Texas October 15-17, 17 2013 Diagnosis of TB: Radiology Rosa M Estrada-Y-Martin, MD MSc FCCP October 16, 2013 Rosa M Estrada-Y-Martin, MD MSc FCCP, has the following disclosures to
TB Intensive Houston, Texas October 15-17, 17 2013 Diagnosis of TB: Radiology Rosa M Estrada-Y-Martin, MD MSc FCCP October 16, 2013 Rosa M Estrada-Y-Martin, MD MSc FCCP, has the following disclosures to
Imaging Decisions Start Here SM
 Owing to its high resolution and wide anatomic coverage, dynamic first-pass perfusion 320-detector-row CT outperforms PET/CT for distinguishing benign from malignant lung nodules, researchers from Japan
Owing to its high resolution and wide anatomic coverage, dynamic first-pass perfusion 320-detector-row CT outperforms PET/CT for distinguishing benign from malignant lung nodules, researchers from Japan
Radiological staging of lung cancer. Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh
 Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
PULMONARY TUBERCULOSIS RADIOLOGY
 PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions
 ORIGINAL ARTICLE Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions Silvia Bielsa, MD,* José Martín-Juan, MD, José M. Porcel, MD,* and Francisco Rodríguez-Panadero, MD Background
ORIGINAL ARTICLE Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions Silvia Bielsa, MD,* José Martín-Juan, MD, José M. Porcel, MD,* and Francisco Rodríguez-Panadero, MD Background
Computed tomography features in malignant pleural mesothelioma and other commonly seen pleural diseases
 European Journal of Radiology 41 (2002) 1 9 www.elsevier.com/locate/ejrad Computed tomography features in malignant pleural mesothelioma and other commonly seen pleural diseases Muzaffer Metintas a, *,
European Journal of Radiology 41 (2002) 1 9 www.elsevier.com/locate/ejrad Computed tomography features in malignant pleural mesothelioma and other commonly seen pleural diseases Muzaffer Metintas a, *,
MRI and CT in the Differential Diagnosis of Pleural Disease*
 MRI and CT in the Differential Diagnosis of Pleural Disease* Johannes Hierholzer, MD; Liangping Luo, MD; Roland C. Bittner, MD; Christian Stroszczynski, MD; Ralf-Jürgen Schröder, MD; Nicolas Schoenfeld,
MRI and CT in the Differential Diagnosis of Pleural Disease* Johannes Hierholzer, MD; Liangping Luo, MD; Roland C. Bittner, MD; Christian Stroszczynski, MD; Ralf-Jürgen Schröder, MD; Nicolas Schoenfeld,
Epithelial mesotheliomas can be extremely difficult to distinguish
 ORIGINAL ARTICLE The Use of Pleural Fluid scd44v6/std Ratio for Distinguishing Mesothelioma from Other Pleural Malignancies José M. Porcel, MD,* Aureli Esquerda, PharmD, Francisco Rodriguez-Panadero, MD,
ORIGINAL ARTICLE The Use of Pleural Fluid scd44v6/std Ratio for Distinguishing Mesothelioma from Other Pleural Malignancies José M. Porcel, MD,* Aureli Esquerda, PharmD, Francisco Rodriguez-Panadero, MD,
The Imaging Journey of Patients with Malignant Pleural Mesothelioma: Experience of a Tertiary Mesothelioma MDT
 The Imaging Journey of Patients with Malignant Pleural Mesothelioma: Experience of a Tertiary Mesothelioma MDT V. Lam, J. Brozik, A. J. Sharkey, A. Bajaj, D. T. Barnes Glenfield Hospital, Leicester, United
The Imaging Journey of Patients with Malignant Pleural Mesothelioma: Experience of a Tertiary Mesothelioma MDT V. Lam, J. Brozik, A. J. Sharkey, A. Bajaj, D. T. Barnes Glenfield Hospital, Leicester, United
Biomarkers of infection for the differential diagnosis of pleural effusions
 Eur Respir J 2009; 34: 1383 1389 DOI: 10.1183/09031936.00197208 CopyrightßERS Journals Ltd 2009 Biomarkers of infection for the differential diagnosis of pleural effusions J.M. Porcel*, M. Vives #, G.
Eur Respir J 2009; 34: 1383 1389 DOI: 10.1183/09031936.00197208 CopyrightßERS Journals Ltd 2009 Biomarkers of infection for the differential diagnosis of pleural effusions J.M. Porcel*, M. Vives #, G.
Respiratory Interactive Session. Elaine Borg
 Respiratory Interactive Session Elaine Borg Case 1 Respiratory Cytology 55 year old gentleman Anterior mediastinal mass EBUS FNA Case 1 Respiratory Cytology 55 year old gentleman with anterior mediastinal
Respiratory Interactive Session Elaine Borg Case 1 Respiratory Cytology 55 year old gentleman Anterior mediastinal mass EBUS FNA Case 1 Respiratory Cytology 55 year old gentleman with anterior mediastinal
Radiologic assessment of response of tumors to treatment. Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1
 Radiologic assessment of response of tumors to treatment Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1 Objective response assessment is important to describe the treatment effect of
Radiologic assessment of response of tumors to treatment Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1 Objective response assessment is important to describe the treatment effect of
FDG PET/CT STAGING OF LUNG CANCER. Dr Shakher Ramdave
 FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
What to Do with Small Lung Nodules Hanh Vu Nghiem, MD William Beaumont Hospital Royal Oak, Michigan
 What to Do with Small Lung Nodules Hanh Vu Nghiem, MD William Beaumont Hospital Royal Oak, Michigan Small Lung Nodules What to do with small lung nodules? We biopsy them when requested What are our accuracy
What to Do with Small Lung Nodules Hanh Vu Nghiem, MD William Beaumont Hospital Royal Oak, Michigan Small Lung Nodules What to do with small lung nodules? We biopsy them when requested What are our accuracy
May-Lin Wilgus. A. Study Purpose and Rationale
 Utility of a Computer-Aided Diagnosis Program in the Evaluation of Solitary Pulmonary Nodules Detected on Computed Tomography Scans: A Prospective Observational Study May-Lin Wilgus A. Study Purpose and
Utility of a Computer-Aided Diagnosis Program in the Evaluation of Solitary Pulmonary Nodules Detected on Computed Tomography Scans: A Prospective Observational Study May-Lin Wilgus A. Study Purpose and
An Introduction to Radiology for TB Nurses
 An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
A New, Simple Method for Estimating Pleural Effusion Size on CT Scans
 CHEST A New, Simple Method for Estimating Pleural Effusion Size on CT Scans Matthew P. Moy, MD ; Jeffrey M. Levsky, MD, PhD ; Netanel S. Berko, MD ; Alla Godelman, MD ; Vineet R. Jain, MD ; and Linda B.
CHEST A New, Simple Method for Estimating Pleural Effusion Size on CT Scans Matthew P. Moy, MD ; Jeffrey M. Levsky, MD, PhD ; Netanel S. Berko, MD ; Alla Godelman, MD ; Vineet R. Jain, MD ; and Linda B.
Thoracic Ultrasound in the diagnosis of Malignant Pleural Effusion
 Thorax Online First, published on October 13, 2008 as 10.1136/thx.2008.100545 Thoracic Ultrasound in the diagnosis of Malignant Pleural Effusion Authors: Nagmi R Qureshi FRCR 1* Najib M Rahman MRCP 2*
Thorax Online First, published on October 13, 2008 as 10.1136/thx.2008.100545 Thoracic Ultrasound in the diagnosis of Malignant Pleural Effusion Authors: Nagmi R Qureshi FRCR 1* Najib M Rahman MRCP 2*
Utility of 18 F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer
 Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Efficacy of ultrasonography and computed tomography in differentiating transudate from exudate in patients with pleural effusion
 Efficacy of ultrasonography and computed tomography in differentiating transudate from exudate in patients with pleural effusion Purpose: To evaluate USG and CT imaging findings in differentiating transudative
Efficacy of ultrasonography and computed tomography in differentiating transudate from exudate in patients with pleural effusion Purpose: To evaluate USG and CT imaging findings in differentiating transudative
Efficacy of Computed Tomography (CT) Attenuation Values and CT Findings in the Differentiation of Pleural Effusion
 Signature: Pol J Radiol, 2017; 82: 100-105 DOI: 10.12659/PJR.898963 ORIGINAL ARTICLE Received: 2016.04.10 Accepted: 2016.05.31 Published: 2017.02.19 Authors Contribution: A Study Design B Data Collection
Signature: Pol J Radiol, 2017; 82: 100-105 DOI: 10.12659/PJR.898963 ORIGINAL ARTICLE Received: 2016.04.10 Accepted: 2016.05.31 Published: 2017.02.19 Authors Contribution: A Study Design B Data Collection
Pulmonary Embolism. Thoracic radiologist Helena Lauri
 Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Computed Tomography (CT) Scan Features of Pulmonary Drug-Resistant Tuberculosis in Non-HIV-Infected Patients
 Cronicon OPEN ACCESS EC BACTERIOLOGY AND VIROLOGY Research Article Computed Tomography (CT) Scan Features of Pulmonary Drug-Resistant Tuberculosis in Non-HIV-Infected Patients Ehsan Shahverdi 1 *, Ashkan
Cronicon OPEN ACCESS EC BACTERIOLOGY AND VIROLOGY Research Article Computed Tomography (CT) Scan Features of Pulmonary Drug-Resistant Tuberculosis in Non-HIV-Infected Patients Ehsan Shahverdi 1 *, Ashkan
Management of Pleural Effusion
 Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
10/17/2016. Nuts and Bolts of Thoracic Radiology. Objectives. Techniques
 Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Role of imaging (images) in my practice. Dr P Senthur Nambi Consultant Infectious Diseases
 Role of imaging (images) in my practice Dr P Senthur Nambi Consultant Infectious Diseases Medical images: My thoughts Images are just images Subject to the intellect of the interpreter View it in conjuction
Role of imaging (images) in my practice Dr P Senthur Nambi Consultant Infectious Diseases Medical images: My thoughts Images are just images Subject to the intellect of the interpreter View it in conjuction
TB Radiology for Nurses Garold O. Minns, MD
 TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
Different characteristics of tuberculous pleural effusion according to pleural fluid cellular predominance and loculation
 Original Article Different characteristics of tuberculous pleural effusion according to pleural fluid cellular predominance and loculation Jaehee Lee 1, Jae Kwang Lim 2, Seung Soo Yoo 1, Shin Yup Lee 1,
Original Article Different characteristics of tuberculous pleural effusion according to pleural fluid cellular predominance and loculation Jaehee Lee 1, Jae Kwang Lim 2, Seung Soo Yoo 1, Shin Yup Lee 1,
PLEURAL EFFUSION. Prof. G. Zuliani
 PLEURAL EFFUSION Prof. G. Zuliani Anatomy of pleural membrane and pleural space Pleural membrane consists of parietal pleura and visceral pleura A space situated between parietal and visceral pleura is
PLEURAL EFFUSION Prof. G. Zuliani Anatomy of pleural membrane and pleural space Pleural membrane consists of parietal pleura and visceral pleura A space situated between parietal and visceral pleura is
Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule
 Original Article Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule Xuan Zhang*, Hong-Hong Yan, Jun-Tao Lin, Ze-Hua Wu, Jia Liu, Xu-Wei Cao, Xue-Ning Yang From
Original Article Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule Xuan Zhang*, Hong-Hong Yan, Jun-Tao Lin, Ze-Hua Wu, Jia Liu, Xu-Wei Cao, Xue-Ning Yang From
Lung. 10/24/13 Chest X-ray: 2.9 cm mass like density in the inferior lingular segment worrisome for neoplasm. Malignancy cannot be excluded.
 Lung Case Scenario 1 A 54 year white male presents with a recent abnormal CT of the chest. The patient has a history of melanoma, kidney, and prostate cancers. 10/24/13 Chest X-ray: 2.9 cm mass like density
Lung Case Scenario 1 A 54 year white male presents with a recent abnormal CT of the chest. The patient has a history of melanoma, kidney, and prostate cancers. 10/24/13 Chest X-ray: 2.9 cm mass like density
objectives Pitfalls and Pearls in PET/CT imaging Kevin Robinson, DO Assistant Professor Department of Radiology Michigan State University
 objectives Pitfalls and Pearls in PET/CT imaging Kevin Robinson, DO Assistant Professor Department of Radiology Michigan State University To determine the regions of physiologic activity To understand
objectives Pitfalls and Pearls in PET/CT imaging Kevin Robinson, DO Assistant Professor Department of Radiology Michigan State University To determine the regions of physiologic activity To understand
Tuberculosis in Patients with End-Stage Renal Disease 1
 Tuberculosis in Patients with End-Stage Renal Disease 1 Hyo-Cheol Kim, M.D., Jin Mo Goo, M.D., Myung Jin Chung, M.D., Min Hoan Moon, M.D., Young Hwan Koh, M.D., and Jung-Gi Im, M.D. Purpose: The purpose
Tuberculosis in Patients with End-Stage Renal Disease 1 Hyo-Cheol Kim, M.D., Jin Mo Goo, M.D., Myung Jin Chung, M.D., Min Hoan Moon, M.D., Young Hwan Koh, M.D., and Jung-Gi Im, M.D. Purpose: The purpose
Imaging of pleural masses: Which to choose? Republished article $
 Respiratory Medicine CME (2008) 1, 10 14 respiratory MEDICINE CME CME ARTICLE Imaging of pleural masses: Which to choose? Republished article $ Aaron S. Bruns, John G. Mastronarde Division of Pulmonary
Respiratory Medicine CME (2008) 1, 10 14 respiratory MEDICINE CME CME ARTICLE Imaging of pleural masses: Which to choose? Republished article $ Aaron S. Bruns, John G. Mastronarde Division of Pulmonary
A Practical Approach to Ultrasound Assessment of Respiratory Distress
 A Practical Approach to Ultrasound Assessment of Respiratory Distress Yanick Beaulieu, MD, FRCPC Director, Bedside Ultrasound Curriculum Division of Cardiology and Critical Care Hôpital du Sacré-Coeur
A Practical Approach to Ultrasound Assessment of Respiratory Distress Yanick Beaulieu, MD, FRCPC Director, Bedside Ultrasound Curriculum Division of Cardiology and Critical Care Hôpital du Sacré-Coeur
Extraosseous myeloma: imaging features
 Extraosseous myeloma: imaging features C. Santos Montón, R. Corrales, J. M. Bastida Bermejo, M. Villanueva Delgado, R. E. Correa Soto, J. M. Alonso Sánchez; Salamanca/ES Learning objectives -To review
Extraosseous myeloma: imaging features C. Santos Montón, R. Corrales, J. M. Bastida Bermejo, M. Villanueva Delgado, R. E. Correa Soto, J. M. Alonso Sánchez; Salamanca/ES Learning objectives -To review
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page
 The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
CT in Differential Diagnosis of Diffuse Pleural Disease
 487 0361-803x/9o/1 543-0487 American Roentgen Ray Society Ann N. Leung1 Nestor L. MUller1 Roberta R. Miller2 Received August 31, 1989; accepted after revision October 16, 1989. Department of Radiology,
487 0361-803x/9o/1 543-0487 American Roentgen Ray Society Ann N. Leung1 Nestor L. MUller1 Roberta R. Miller2 Received August 31, 1989; accepted after revision October 16, 1989. Department of Radiology,
PET CT for Staging Lung Cancer
 PET CT for Staging Lung Cancer Rohit Kochhar Consultant Radiologist Disclosures Neither I nor my immediate family members have financial relationships with commercial organizations that may have a direct
PET CT for Staging Lung Cancer Rohit Kochhar Consultant Radiologist Disclosures Neither I nor my immediate family members have financial relationships with commercial organizations that may have a direct
Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings
 Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings Poster No.: C-2067 Congress: ECR 2017 Type: Educational Exhibit Authors: J. M. Almeida, N. Antunes, C. Leal, L. Figueiredo ; Lisboa/PT,
Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings Poster No.: C-2067 Congress: ECR 2017 Type: Educational Exhibit Authors: J. M. Almeida, N. Antunes, C. Leal, L. Figueiredo ; Lisboa/PT,
The solitary pulmonary nodule: Assessing the success of predicting malignancy
 The solitary pulmonary nodule: Assessing the success of predicting malignancy Poster No.: C-0829 Congress: ECR 2010 Type: Scientific Exhibit Topic: Chest Authors: R. W. K. Lindsay, J. Foster, K. McManus;
The solitary pulmonary nodule: Assessing the success of predicting malignancy Poster No.: C-0829 Congress: ECR 2010 Type: Scientific Exhibit Topic: Chest Authors: R. W. K. Lindsay, J. Foster, K. McManus;
available at journal homepage:
 Respiratory Medicine (2010) 104, 1211e1217 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Diagnosing tuberculous pleural effusion using clinical data and pleural fluid
Respiratory Medicine (2010) 104, 1211e1217 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Diagnosing tuberculous pleural effusion using clinical data and pleural fluid
Mediastinal Staging. Samer Kanaan, M.D.
 Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Comparison of RECIST version 1.0 and 1.1 in assessment of tumor response by computed tomography in advanced gastric cancer
 Original Article Comparison of RECIST version 1.0 and 1.1 in assessment of tumor response by computed tomography in advanced gastric cancer Gil-Su Jang 1 *, Min-Jeong Kim 2 *, Hong-Il Ha 2, Jung Han Kim
Original Article Comparison of RECIST version 1.0 and 1.1 in assessment of tumor response by computed tomography in advanced gastric cancer Gil-Su Jang 1 *, Min-Jeong Kim 2 *, Hong-Il Ha 2, Jung Han Kim
Pleural effusion in patients with extrapleural primary malignancies
 ORIGINAL ARTICLE Differentiation Between Malignant and Benign Pleural Effusion in Patients With Extra-Pleural Primary Malignancies Assessment With Positron Emission Tomography-Computed Tomography Jacob
ORIGINAL ARTICLE Differentiation Between Malignant and Benign Pleural Effusion in Patients With Extra-Pleural Primary Malignancies Assessment With Positron Emission Tomography-Computed Tomography Jacob
Differentiation of Pleural Effusions From Parenchymal Opacities: Accuracy of Bedside Chest Radiography
 Cardiopulmonary Imaging Original Research Kitazono et al. Chest Radiography of Pleural Effusions Cardiopulmonary Imaging Original Research Mary T. Kitazono 1 Charles T. Lau Andrea N. Parada Pooja Renjen
Cardiopulmonary Imaging Original Research Kitazono et al. Chest Radiography of Pleural Effusions Cardiopulmonary Imaging Original Research Mary T. Kitazono 1 Charles T. Lau Andrea N. Parada Pooja Renjen
Sectional Anatomy Quiz II
 Sectional Anatomy II Rashid Hashmi Rural Clinical School, University of New South Wales, Wagga Wagga, New South Wales, Australia A R T I C L E I N F O Article type: Article history: Received: 3 Aug 2017
Sectional Anatomy II Rashid Hashmi Rural Clinical School, University of New South Wales, Wagga Wagga, New South Wales, Australia A R T I C L E I N F O Article type: Article history: Received: 3 Aug 2017
Pleural Space Infections: Microbiologic And Fluid Characteristics In 84 Patients. J Porcel, P Vázquez, M Vives, A Nogués, M Falguera, A Manonelles
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 3 Number 1 Pleural Space Infections: Microbiologic And Fluid Characteristics In 84 Patients J Porcel, P Vázquez, M Vives, A Nogués, M Falguera,
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 3 Number 1 Pleural Space Infections: Microbiologic And Fluid Characteristics In 84 Patients J Porcel, P Vázquez, M Vives, A Nogués, M Falguera,
Case 5 15-year-old male
 Case 5 15-year-old male Present illness: Six months ago, abnormality of ECG was incidentally detected by annual health check. His blood level of γ-gtp, HbA1c and norepinephrine were elevated; however,
Case 5 15-year-old male Present illness: Six months ago, abnormality of ECG was incidentally detected by annual health check. His blood level of γ-gtp, HbA1c and norepinephrine were elevated; however,
Comparison of High-resolution CT Findings between Miliary Metastases and Miliary Tuberculosis 1
 Comparison of High-resolution CT Findings between Miliary Metastases and Miliary Tuberculosis 1 Chan Sung Kim, M.D., Ki-Nam Lee, M.D., Jin Hwa Lee, M.D. Purpose: To compare the findings of high-resolution
Comparison of High-resolution CT Findings between Miliary Metastases and Miliary Tuberculosis 1 Chan Sung Kim, M.D., Ki-Nam Lee, M.D., Jin Hwa Lee, M.D. Purpose: To compare the findings of high-resolution
THE BENEFITS OF BIG DATA
 THE BENEFITS OF BIG DATA Disclosures I am a named inventor on a number of patents and patent applications relating to the evaluation of pulmonary nodules on CT scans of the chest which are owned by Cornell
THE BENEFITS OF BIG DATA Disclosures I am a named inventor on a number of patents and patent applications relating to the evaluation of pulmonary nodules on CT scans of the chest which are owned by Cornell
Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases
 Pleural effusions Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases A pleural effusion is an abnormal collection of fluid in the pleural space resulting from excess fluid production or decreased
Pleural effusions Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases A pleural effusion is an abnormal collection of fluid in the pleural space resulting from excess fluid production or decreased
Scientific Exhibit. Authors: D. Takenaka, Y. Ohno, Y. Onishi, K. Matsumoto, T.
 The feasibility of biphasic contrast-media-injection-protocol for chest imaging on 320-slice volume MDCT: Direct comparison of biphasic and bolus contrast-media injection protocols on 320-slice volume
The feasibility of biphasic contrast-media-injection-protocol for chest imaging on 320-slice volume MDCT: Direct comparison of biphasic and bolus contrast-media injection protocols on 320-slice volume
PET IMAGING (POSITRON EMISSION TOMOGRAPY) FACT SHEET
 Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Lung Cancer - Suspected
 Lung Cancer - Suspected Shared Decision Making Lung Cancer: http://www.enhertsccg.nhs.uk/ Patient presents with abnormal CXR Lung cancer - clinical presentation History and Examination Incidental finding
Lung Cancer - Suspected Shared Decision Making Lung Cancer: http://www.enhertsccg.nhs.uk/ Patient presents with abnormal CXR Lung cancer - clinical presentation History and Examination Incidental finding
Ultrasound-guided pleural cutting needle biopsy: accuracy and factors influencing diagnostic yield
 Original Article Ultrasound-guided pleural cutting needle biopsy: accuracy and factors influencing diagnostic yield Yuxin Zhang 1#, Jiaxin Tang 2#, Xinghua Zhou 1, Dazhi Zhou 1, Jinlin Wang 2, Qing Tang
Original Article Ultrasound-guided pleural cutting needle biopsy: accuracy and factors influencing diagnostic yield Yuxin Zhang 1#, Jiaxin Tang 2#, Xinghua Zhou 1, Dazhi Zhou 1, Jinlin Wang 2, Qing Tang
GUIDELINES FOR CANCER IMAGING Lung Cancer
 GUIDELINES FOR CANCER IMAGING Lung Cancer Greater Manchester and Cheshire Cancer Network Cancer Imaging Cross-Cutting Group April 2010 1 INTRODUCTION This document is intended as a ready reference for
GUIDELINES FOR CANCER IMAGING Lung Cancer Greater Manchester and Cheshire Cancer Network Cancer Imaging Cross-Cutting Group April 2010 1 INTRODUCTION This document is intended as a ready reference for
North of Scotland Cancer Network Clinical Management Guideline for Mesothelioma
 THIS DOCUMENT IS North of Scotland Cancer Network Clinical Management Guideline for Mesothelioma [Based on WOSCAN SCLC CMG with further extensive consultation within NOSCAN] UNCONTROLLED WHEN PRINTED Document
THIS DOCUMENT IS North of Scotland Cancer Network Clinical Management Guideline for Mesothelioma [Based on WOSCAN SCLC CMG with further extensive consultation within NOSCAN] UNCONTROLLED WHEN PRINTED Document
Collaborative Stage. Site-Specific Instructions - LUNG
 Slide 1 Collaborative Stage Site-Specific Instructions - LUNG In this presentation, we are going to review the AJCC Cancer Staging criteria for the lung primary site. Slide 2 Reading Assignments As each
Slide 1 Collaborative Stage Site-Specific Instructions - LUNG In this presentation, we are going to review the AJCC Cancer Staging criteria for the lung primary site. Slide 2 Reading Assignments As each
Guidelines for the Management of Pulmonary Nodules Detected by Low-dose CT Lung Cancer Screening
 Guidelines for the Management of Pulmonary Nodules Detected by Low-dose CT Lung Cancer Screening 1. Introduction In January 2005, the Committee for Preparation of Clinical Practice Guidelines for the Management
Guidelines for the Management of Pulmonary Nodules Detected by Low-dose CT Lung Cancer Screening 1. Introduction In January 2005, the Committee for Preparation of Clinical Practice Guidelines for the Management
Comparison of CT findings between MDR-TB and XDR-TB
 Comparison of CT findings between MDR-TB and XDR-TB Poster No.: C-0757 Congress: ECR 2017 Type: Authors: Keywords: DOI: Scientific Exhibit K. Yoon, H. Soohee; Changwon-si/KR Thorax, Lung, Respiratory system,
Comparison of CT findings between MDR-TB and XDR-TB Poster No.: C-0757 Congress: ECR 2017 Type: Authors: Keywords: DOI: Scientific Exhibit K. Yoon, H. Soohee; Changwon-si/KR Thorax, Lung, Respiratory system,
Comparison of CT findings of between MDR-TB and XDR-TB: A propensity score matching study
 Comparison of CT findings of between MDR-TB and XDR-TB: A propensity score matching study Purpose: The purpose of this study was to compare the CT findings between MDR-TB and XDR-TB groups using by propensity
Comparison of CT findings of between MDR-TB and XDR-TB: A propensity score matching study Purpose: The purpose of this study was to compare the CT findings between MDR-TB and XDR-TB groups using by propensity
Case of the Day Chest
 Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer
 Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Intrathoracic extrapleural lesions: MDCT
 Intrathoracic extrapleural lesions: MDCT Poster No.: C-0994 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: S. S. Kim, Y. T. Kim, S. S. Jou, J. K. Han; Cheonan/KR Keywords: Thoracic
Intrathoracic extrapleural lesions: MDCT Poster No.: C-0994 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: S. S. Kim, Y. T. Kim, S. S. Jou, J. K. Han; Cheonan/KR Keywords: Thoracic
Approach to Pulmonary Nodules
 Approach to Pulmonary Nodules Edwin Jackson, Jr., DO Assistant Professor-Clinical Director, James Early Detection Clinic Department of Internal Medicine Division of Pulmonary, Allergy, Critical Care and
Approach to Pulmonary Nodules Edwin Jackson, Jr., DO Assistant Professor-Clinical Director, James Early Detection Clinic Department of Internal Medicine Division of Pulmonary, Allergy, Critical Care and
Diagnosis of TB: Radiology David Finlay, MD
 TB Intensive Tyler, Texas June 2-4, 2010 Diagnosis of TB: Radiology David Finlay, MD June 3, 2010 2stages stages- Tuberculosis 1. primary infection 2. reactivation, or post primary disease 2 1 Primary
TB Intensive Tyler, Texas June 2-4, 2010 Diagnosis of TB: Radiology David Finlay, MD June 3, 2010 2stages stages- Tuberculosis 1. primary infection 2. reactivation, or post primary disease 2 1 Primary
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
The distinction between transudates and exudates
 Journal of Biomedical Science (2005) 12:985 990 985 DOI 10.1007/s11373-005-9014-1 The distinction between transudates and exudates Ugur Gonlugur 1, * & Tanseli Efeoglu Gonlugur 2 1 Department of Chest
Journal of Biomedical Science (2005) 12:985 990 985 DOI 10.1007/s11373-005-9014-1 The distinction between transudates and exudates Ugur Gonlugur 1, * & Tanseli Efeoglu Gonlugur 2 1 Department of Chest
American College of Radiology ACR Appropriateness Criteria
 American College of Radiology ACR Criteria Radiologic Management of Thoracic Nodules and Masses Variant 1: Middle-aged patient (35 60 years old) with an incidental 1.5-cm lung nodule. The lesion was smooth.
American College of Radiology ACR Criteria Radiologic Management of Thoracic Nodules and Masses Variant 1: Middle-aged patient (35 60 years old) with an incidental 1.5-cm lung nodule. The lesion was smooth.
Key messages. CXR interpretation in TB/HIV setting. Training course
 Key messages CXR interpretation in TB/HIV setting Training course Normal CXR Front view and lateral view Good notions of technical conditions to obtain a good CXR Good knowledge of criteria for quality
Key messages CXR interpretation in TB/HIV setting Training course Normal CXR Front view and lateral view Good notions of technical conditions to obtain a good CXR Good knowledge of criteria for quality
Multicentre analysis of incidental findings on low resolution CT attenuation correction images : an extended study
 Multicentre analysis of incidental findings on low resolution CT attenuation correction images : an extended study Coward, J, Lawson, R, Kane, T, Elias, M, Howes, A, Birchall, J and Hogg, P http://dx.doi.org/10.1259/bjr.20150555
Multicentre analysis of incidental findings on low resolution CT attenuation correction images : an extended study Coward, J, Lawson, R, Kane, T, Elias, M, Howes, A, Birchall, J and Hogg, P http://dx.doi.org/10.1259/bjr.20150555
Peritoneal tuberculosis: retrospective analysis of clinical and radiologic findings in our institution from 2003 to 2013
 Peritoneal tuberculosis: retrospective analysis of clinical and radiologic findings in our institution from 2003 to 2013 Poster No.: C-2332 Congress: ECR 2015 Type: Scientific Exhibit Authors: A. Viteri,
Peritoneal tuberculosis: retrospective analysis of clinical and radiologic findings in our institution from 2003 to 2013 Poster No.: C-2332 Congress: ECR 2015 Type: Scientific Exhibit Authors: A. Viteri,
Primary multidrug-resistant tuberculosis versus drug-sensitive tuberculosis in non-hivinfected patients: Comparisons of CT findings
 RESEARCH ARTICLE Primary multidrug-resistant tuberculosis versus drug-sensitive tuberculosis in non-hivinfected patients: Comparisons of CT findings Duo Li, Wei He, Budong Chen, Pingxin Lv* Department
RESEARCH ARTICLE Primary multidrug-resistant tuberculosis versus drug-sensitive tuberculosis in non-hivinfected patients: Comparisons of CT findings Duo Li, Wei He, Budong Chen, Pingxin Lv* Department
The Frequency and Significance of Small (15 mm) Hepatic Lesions Detected by CT
 535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
Combined efficacy of pleural fluid lymphocyte neutrophil ratio and pleural fluid adenosine deaminase for the diagnosis of tubercular pleural effusion
 Original article: Combined efficacy of pleural fluid lymphocyte neutrophil ratio and pleural fluid adenosine deaminase for the diagnosis of tubercular pleural effusion Kavita S Kore, Guruprasad Antin,
Original article: Combined efficacy of pleural fluid lymphocyte neutrophil ratio and pleural fluid adenosine deaminase for the diagnosis of tubercular pleural effusion Kavita S Kore, Guruprasad Antin,
Pleural Plaques: Appearances, Mimics and Clinical implications
 Pleural Plaques: Appearances, Mimics and Clinical implications Poster No.: P-0108 Congress: ESTI 2014 Type: Educational Poster Authors: D. J. Martin, K. J. Litton, H. Adams; Cardiff/UK Keywords: Occupational
Pleural Plaques: Appearances, Mimics and Clinical implications Poster No.: P-0108 Congress: ESTI 2014 Type: Educational Poster Authors: D. J. Martin, K. J. Litton, H. Adams; Cardiff/UK Keywords: Occupational
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis)
 Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Quantification of pleural effusion on CT by simple measurement
 Quantification of pleural effusion on CT by simple measurement Martin Hazlinger a, Filip Ctvrtlik a, Katerina Langova b, Miroslav Herman a Aims. To find the simplest method for quantifying pleural effusion
Quantification of pleural effusion on CT by simple measurement Martin Hazlinger a, Filip Ctvrtlik a, Katerina Langova b, Miroslav Herman a Aims. To find the simplest method for quantifying pleural effusion
Diagnostic accuracy of tumor markers for malignant pleural effusion: a derivation and validation study
 Original Article Diagnostic accuracy of tumor markers for malignant pleural effusion: a derivation and validation study Kan Zhai 1,2, Wen Wang 1, Yao Wang 1, Jing-Yuan Liu 3, Qiong Zhou 3, Huan-Zhong Shi
Original Article Diagnostic accuracy of tumor markers for malignant pleural effusion: a derivation and validation study Kan Zhai 1,2, Wen Wang 1, Yao Wang 1, Jing-Yuan Liu 3, Qiong Zhou 3, Huan-Zhong Shi
Radiographic Assessment of Response An Overview of RECIST v1.1
 Radiographic Assessment of Response An Overview of RECIST v1.1 Stephen Liu, MD Georgetown University May 15 th, 2015 Presentation Objectives To understand the purpose of RECIST guidelines To describe the
Radiographic Assessment of Response An Overview of RECIST v1.1 Stephen Liu, MD Georgetown University May 15 th, 2015 Presentation Objectives To understand the purpose of RECIST guidelines To describe the
Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations
 Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations TECHNICAL EVALUATION 1. Projection: AP/PA view To differentiate between AP & PA films,
Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations TECHNICAL EVALUATION 1. Projection: AP/PA view To differentiate between AP & PA films,
A 50-year-old male with fever, cough, dyspnoea, chest pain, weight loss and night sweats
 Petru Emil Muntean muntean.petruemil@yahoo.com Pulmonology, Spitalul Clinic Judetean Mures, Targu Mures, Romania. A 50-year-old male with fever, cough, dyspnoea, chest pain, weight loss and night sweats
Petru Emil Muntean muntean.petruemil@yahoo.com Pulmonology, Spitalul Clinic Judetean Mures, Targu Mures, Romania. A 50-year-old male with fever, cough, dyspnoea, chest pain, weight loss and night sweats
ARDS - a must know. Page 1 of 14
 ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
Computed tomography of the chest: I. Basic principles
 BJA Education, 15 (6): 299 304 (2015) doi: 10.1093/bjaceaccp/mku063 Advance Access Publication Date: 2 February 2015 Matrix reference 1A03, 2A12 Computed tomography of the chest: I. Basic principles P
BJA Education, 15 (6): 299 304 (2015) doi: 10.1093/bjaceaccp/mku063 Advance Access Publication Date: 2 February 2015 Matrix reference 1A03, 2A12 Computed tomography of the chest: I. Basic principles P
September 2014 Imaging Case of the Month. Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
The Imaging Analysis of Pulmonary Sarcodiosis
 www.cancercellresearch.org ISSN: 2161-2609 Article The Imaging Analysis of Pulmonary Sarcodiosis Xin He, Chuanyu Zhang* Department of Radiology, Affiliated Hospital of Qingdao University, Qingdao, China
www.cancercellresearch.org ISSN: 2161-2609 Article The Imaging Analysis of Pulmonary Sarcodiosis Xin He, Chuanyu Zhang* Department of Radiology, Affiliated Hospital of Qingdao University, Qingdao, China
Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2
 Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2 The Committee for Management of CT-screening-detected Pulmonary Nodules 2009-2011 The Japanese Society of CT Screening
Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2 The Committee for Management of CT-screening-detected Pulmonary Nodules 2009-2011 The Japanese Society of CT Screening
and localized ground glass opacities, or bronchiolar focal or multifocal micronodules;
 E1 Chest CT scan and Pneumoniae_YE Claessens et al- Supplementary methods Level of CAP probability according to CT scan - definite CAP: systematic alveolar condensation, or alveolar condensation with peripheral
E1 Chest CT scan and Pneumoniae_YE Claessens et al- Supplementary methods Level of CAP probability according to CT scan - definite CAP: systematic alveolar condensation, or alveolar condensation with peripheral
Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms
 Original Research Article Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms Anand Vachhani 1, Shashvat Modia 1*, Varun Garasia 1, Deepak Bhimani 1, C. Raychaudhuri
Original Research Article Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms Anand Vachhani 1, Shashvat Modia 1*, Varun Garasia 1, Deepak Bhimani 1, C. Raychaudhuri
1/25/13 Right partial nephrectomy followed by completion right radical nephrectomy.
 History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
Diagnostic Approach to Pleural Effusion
 Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Lung cancer in patients with chronic empyema
 Lung cancer in patients with chronic empyema Poster No.: P-0025 Congress: ESTI 2015 Type: Scientific Poster Authors: Y. Lee, C.-K. Park; Guri/KR Keywords: Neoplasia, Biopsy, PET-CT, CT, Thorax, Lung DOI:
Lung cancer in patients with chronic empyema Poster No.: P-0025 Congress: ESTI 2015 Type: Scientific Poster Authors: Y. Lee, C.-K. Park; Guri/KR Keywords: Neoplasia, Biopsy, PET-CT, CT, Thorax, Lung DOI:
Principal Investigator. General Information. Certification Published on The YODA Project (http://yoda.yale.
 Principal Investigator First Name: Nicola Last Name: Schieda Degree: MD FRCP(C) Primary Affiliation: The Ottawa Hospital - The University of Ottawa E-mail: nschieda@toh.on.ca Phone number: 613-798-5555
Principal Investigator First Name: Nicola Last Name: Schieda Degree: MD FRCP(C) Primary Affiliation: The Ottawa Hospital - The University of Ottawa E-mail: nschieda@toh.on.ca Phone number: 613-798-5555
