Virology. Longitudinal study to assess the safety and efficacy of a live-attenuated SHIV vaccine in long term immunized rhesus macaques
|
|
|
- Naomi Lambert
- 6 years ago
- Views:
Transcription
1 Virology 383 (2009) Contents lists available at ScienceDirect Virology journal homepage: Longitudinal study to assess the safety and efficacy of a live-attenuated SHIV vaccine in long term immunized rhesus macaques Thomas M. Yankee a,, Darlene Sheffer a, Zhengian Liu a, Sukhbir Dhillon a, Fenglan Jia a, Yahia Chebloune a, Edward B. Stephens a,b, Opendra Narayan a, a Department of Microbiology, Molecular Genetics, and Immunology, University of Kansas Medical Center, 3025 WHW - MS 3029, 3901 Rainbow Boulevard, Kansas City, KS 66160, USA b Department of Anatomy and Cell Biology, University of Kansas Medical Center, Kansas City, KS 66160, USA article info abstract Article history: Received 7 July 2008 Returned to author for revision 6 August 2008 Accepted 26 September 2008 Available online 5 November 2008 Keywords: Live-attenuated vaccine SIV SHIV Safety Immune response Correlates of protection Live-attenuated viruses derived from SIV and SHIV have provided the most consistent protection against challenge with pathogenic viruses, but concerns regarding their long-term safety and efficacy have hampered their clinical usefulness. We report a longitudinal study in which we evaluated the long-term safety and efficacy of ΔvpuSHIV PPC, a live virus vaccine derived from SHIV PPC. Macaques were administered two inoculations of ΔvpuSHIV PPC, three years apart, and followed for eight years. None of the five vaccinated macaques developed an AIDS-like disease from the vaccine. At eight years, macaques were challenged with pathogenic SIV and SHIV. None of the four macaques with detectable cellular-mediated immunity prior to challenge had detectable viral RNA in the plasma. This study demonstrates that multiple inoculations of a live vaccine virus can be used safely and can significantly extend the efficacy of the vaccine, as compared to a single inoculation, which is efficacious for approximately three years Elsevier Inc. All rights reserved. Introduction The high capacity of human immunodeficiency virus (HIV-1) to mutate and escape immune responses has been a major obstacle to developing an effective vaccine against HIV-1. Despite this challenge, developing a vaccine against HIV-1 is of paramount importance to stem the global pandemic of HIV-1/AIDS. While numerous strategies for vaccines have been designed, none have been fully successful. To date, the most successful vaccines to date in protecting non-human primates against pathogenic SIV and SHIV have been live-attenuated vaccines based on SIV or SHIV (Whitney and Ruprecht, 2004; Robinson, 2007). These viruses were obtained by deleting one or more viral genes. The first such vaccine was SIV mac 239 in which nef was deleted. This vaccine was shown to induce protection of immunized macaques against the challenge with the highly pathogenic molecularly cloned SIV mac239 or the uncloned SIV mac 251 (Daniel et al., 1992). However, this liveattenuated vaccine virus was found to be pathogenic in infant macaques and some adult macaques (Baba et al., 1995, 1999). The results of these early studies raised a high level of skepticism that a live virus vaccine against HIV-1 could be developed that was safe enough to use in humans. Since these early studies, several laboratories have investigated other live virus vaccines in order to determine whether an attenuated vaccine Corresponding author. Fax: address: tyankee@kumc.edu (T.M. Yankee). Deceased. could be developed that is both safe and efficacious (Whitney and Ruprecht, 2004). Previously, we derived live-attenuated vaccines from the pathogenic SHIVs to evaluate whether they would protect monkeys from the highly pathogenic SHIVs and SIVs in primates. In earlier studies we described a live-attenuated SHIV-base vaccine ΔvpuΔnefSHIV PPC (Joag et al., 1998b) and showed it to be safe after serial passage (Mackay et al., 2002). However, it replicated poorly in vivo and offered little longterm protection against disease induced by challenge with pathogenic viruses (Joag et al., 1998b; Mackay et al., 2004a). To improve the immunogenicity of the SHIV-based vaccine, the vaccine was redesigned to generate ΔvpuSHIV PPC (Joag et al., 1998b), a vaccine that replicated much more robustly and was much more successful in conferring protection against disease caused by challenge viruses (Joag et al., 1998b; Silverstein et al., 2000; Mackay et al., 2004a). After challenge with pathogenic virus, vaccinated animals developed plasma virus levels during the acute phase that were at least two orders of magnitude lower than unvaccinated controls (Joag et al., 1998b). Despite the ability of ΔvpuSHIV PPC to reduce viremia, this vaccine did not prevent viremia and many vaccinated animals ultimately succumbed to AIDS. A recent study by Kumar et al. (2008) supported the finite nature of the protection by showing that the protection induced ΔvpuSHIV PPC vaccine against productive infection by a pathogenic virus only lasted approximately three years after vaccination. While previous studies established that ΔvpuSHIV PPC has the potential to be a highly effective vaccine, the long-term safety of this vaccine had not been evaluated. In addition, it is unknown whether /$ see front matter 2008 Elsevier Inc. All rights reserved. doi: /j.virol
2 104 T.M. Yankee et al. / Virology 383 (2009) multiple inoculations with ΔvpuSHIV PPC could extend the protection against disease caused by pathogenic virus. In this report we describe a longitudinal study using adult rhesus macaques immunized twice with ΔvpuSHIV PPC vaccine to evaluate the safety and efficacy of this vaccine virus. Results Viral load after immunization with ΔvpuSHIV PPC Five Indian rhesus macaques (RBq5, RCu5, RTp5, RUr5, and RVq5), were inoculated intradermally with the infectious DNA of the live vaccine virus ΔvpuSHIV PPC, which contains the X4 env gene from the HXB2 strain of HIV-1, and the gag, pol, and nef coding sequences from SIV mac 239. This DNA produces replication-competent virus with an average titer between 10 4 and 10 5 TCID 50 per ml in the culture supernatants of transfected HEK-293 T cells (data not shown). Consistent with previous experiments using ΔvpuSHIV PPC (Joag et al., 1998a), macaques inoculated with this DNA developed a productive infection that lasted four to eight weeks, as indicated by measuring viral RNA in plasma (Table 1). In addition, all animals seroconverted and remained seropositive during the entire study (data not shown). Circulating CD4 + and CD8 + T cell counts after the first inoculation The levels of circulating CD4 + and CD8 + T cells were calculated before and after each inoculation with ΔvpuSHIV PPC. After the first inoculation, the number of circulating CD4 + T cells at two weeks postinoculation averaged 52%±8.6% the number of CD4 + T cells prior to inoculation (Fig. 1A). The number of CD4 + T cells returned to at least 90% of pre-inoculation levels within an average of 12±7.1 weeks after vaccination. The circulating CD8 + T cell levels also declined sharply in four of five macaques in the first weeks post-inoculation (Fig. 1B). The four animals that developed a decline in circulating CD8 + T cell levels had an average of 42%±15% the number of CD8 + T cells prior to inoculation. Their CD8 + T cell levels returned to within 90% of preinoculation levels within 18±9.5 weeks. Animal RBq did not develop a decline in CD8 + T cells, suggesting that this animal may have had a potent immunologic response against the live virus that protected it from CD8 + T cell loss. These data indicated that, while ΔvpuSHIV PPC does not induce an AIDS-like syndrome, the vaccine can cause a transient depletion of CD4 + and CD8 + T cells. By contrast, the pathogenic form of SHIV typically causes severe atrophy of the thymus and ablates the CD4 + T cell compartment in secondary lymphoid tissues within six months of infection (Joag et al., 1996, 1997a, 1997b). Viral load and T cell levels following re-immunization with ΔvpuSHIV PPC Three years after the first inoculation (week 161), animals were inoculated orally with 1 ml of stock ΔvpuSHIV PPC virus containing TCID 50 per ml. Similar to the first inoculation, the second inoculation resulted in a transient productive infection followed by an extended period of latency (Table 2). In four out of the five animals, the peak plasma viral RNA levels after the second inoculation was considerably Table 1 Viral RNA in plasma (copies/ml) after first inoculation with ΔvpuSHIV PPC a RBq RCu RTp RUr RVq Week 2 16, ,000 37,000 73,000 Week ND 80,000 18,000 Week 8 ND b ND ND ND 650 Week 133 ND ND ND ND ND a Weeks indicate week after first inoculation with ΔvpuSHIV PPC. b ND = none detected. Fig. 1. Circulating CD4 + and CD8 + T cell levels decline after the first inoculation with ΔvpuSHIV PPC. The absolute numbers of CD4 + (Panel A) and CD8 + (Panel B) T cells were determined by staining whole blood with anti-cd3, anti-cd4, and anti-cd8. The numbers shown represent cells per μl blood. less than that caused by the first inoculation, suggesting that these animals had developed a degree of immunologic protection against ΔvpuSHIV PPC. Four to eight weeks after the second inoculation, viral RNA was undetectable in the plasma, although an occasional resurgence of viral RNA was detected (Table 2). These spikes suggested that the virus sporadically escaped and produced a low-grade productive infection. These bursts in viral replication were quickly suppressed as the viral RNA levels became undetectable at the next measurement. In four of five animals, CD4 + T cell counts dropped declined after the second inoculation with ΔvpuSHIV PPC (Fig. 2). Except for RBq5, the average circulating CD4 + T cell levels five weeks after the second inoculation (week 166) were 65%±16% of the number prior to reinoculation (week 159). Similarly, the number of CD8 + T cells in animals RCu5, RTp5, RUr5, and RVq5 averaged 56% ±8.8% the level prior to re-infection. RBq5 has no decrease in the number of CD4 + T cells and only a slight reduction in the number of CD8 + T cells after the second inoculation with ΔvpuSHIV PPC, further demonstrating that this animal had an unusual immunologic response to the vaccine. Transient depletion of CD8 + T cells Nearly two years after the second vaccination (week 254), we sought to determine which of the vaccinated animals still harbored Table 2 Viral RNA in plasma (copies/ml) after second inoculation with ΔvpuSHIV PPC a RBq RCu RTp RUr RVq Week 162 ND b ND 612 Week ,377 Week 164 ND ND Week Week 169 ND ND 414 ND ND Week 173 ND ND ND 1480 ND Week ND ND ND ND Week 186 ND ND ND ND 480 Week 195 ND ND ND ND ND Week 251 ND ND Week 253 ND ND ND ND ND a Weeks indicate week after first inoculation with ΔvpuSHIV PPC. b ND = none detected.
3 T.M. Yankee et al. / Virology 383 (2009) Table 3 Viral RNA in plasma (copies/ml) after anti-cd8 treatment a RBq RCu RTp RUr RVq Week 254 Anti-CD8 ND b ND ND ND ND Week 255 ND , ,140 Week 256 ND 548, ,620 1,342, ,700 Week 257 ND 37,540 18,460 57,320 11,260 Week 258 ND 6860 ND ND 1760 Week 259 ND ND ND Week 263 ND ND ND ND ND Week 282 ND ND ND ND ND Week 361 ND ND ND ND ND a CD8 + cell immunodepletion led to a robust resurgence in viral load in four of the five animals. Animals were injected three times with anti-cd8 during week 254. b ND = none detected. Fig. 2. Circulating CD4 + and CD8 + T cell levels after the second inoculation with ΔvpuSHIV PPC. Macaques were re-inoculated at week 161 and the absolute numbers of CD4 + (Panel A) and CD8 + (Panel B) T cells were determined as described in the legend to Fig. 1. the vaccine virus. We administered a course of anti-cd8 antibodies using a procedure previously shown to be highly effective in reducing the level of CD8 + T cells and inducing the re-activation of latent viruses (Jin et al., 1999; Schmitz et al., 1999; Mackay et al., 2004b). In all five animals, the number of CD8 + T cells in the blood decreased to fewer than 10 cells/µl followed by complete recovery of CD8 + T cells within four weeks (Fig. 3B). Concomitant with the loss of CD8 + T cells was a high level of resurgence in the viral mrna levels in plasma of all animals except RBq5 (Table 3). These data indicate that all the animals (except RBq5) still harbored the vaccine virus at the time of anti-cd8 Fig. 3. Circulating CD4 + and CD8 + T cell levels after depletion of CD8 + cells. Macaques were injected intravenously three times with anti-cd8 antibodies during weeks 254 and 255. The absolute numbers of CD4 + (Panel A) and CD8 + (Panel B) T cells were determined as described in the legend of Fig. 1. treatment. Viral loads returned to undetectable levels upon the recovery of the CD8 + T cell population. Two animals (RTp5 and RVq5) had a significant loss of CD4 + T cells following the anti-cd8 treatment, but the levels returned to pre-anti- CD8 levels within one week (Fig. 3A). The other three animals developed an increase in CD4 + T cell counts that subsided upon the return on the CD8 + T cells. The five animals were followed for an additional three years after the anti-cd8 experiment. No viral RNA was detected in the plasma (Table 3) and the numbers of circulating CD4 + and CD8 + T cells remained stable during this period (data not shown). At week 400, blood cells were isolated to determine whether viral DNA could be detected. Viral DNA could be detected in two of the five animals (RCu5 and RVq5) (data not shown). These data suggested that the other animals may have eliminated the vaccine virus or the virus was present in hematopoietic cells in primary or secondary organs. Immune responses prior to challenge Prior to challenge, Gag-specific, Nef-specific, and Env-specific production of IFNγ by PBMCs was measured by ELISPOT (Fig. 4A) and antigen-specific proliferation (ASP) of PBMCs was measured by [ 3 H] thymidine incorporation (Fig. 4B). The four animals that had resurgence of virus following anti-cd8 treatment (RCu5, RTp5, RUr5, and RVq5) had Gag-specific ELISPOT and ASP responses. In addition, these four animals had Nef-specific ELISPOT responses and one animal (RUr5) had significant Nef-specific ASP. PBMCs from macaque RBq5 did not have any ELISPOT or ASP responses following incubation with peptides of the three viral proteins, SIV Gag, Nef, or Env. Similarly, the two unvaccinated control animals (animals 13Z and AL-95) also lacked ELISPOT and ASP responses against Gag, Nef, or Env. While the ASP assay showed that PBMCs proliferated in response to Gag and Nef, this assay did not indicate whether it was the CD4 + or CD8 + T cells that proliferated. To address this question, we measured proliferation by examining the dilution of 5-(and -6)-carboxyfluorescein diacetate, succinimidyl ester (CFSE) by flow cytometry. We electronically gated on CD4 + or CD8 + T cells and then analyzed proliferation. Nearly all of the proliferation detected was a result of proliferation of CD8 + T cells; there was minimal, if any, proliferation of CD4 + T cells (Fig. 4C). Next, we investigated whether T cells from vaccinated animals had a different surface phenotype than T cells from unvaccinated animals. The percentage of CD3 + PBMCs that were CD4 +, CD8 +, or CD4 + CD8 lo was indistinguishable among the seven animals (Fig. 5A). However, the CD8 + T cell population in the four animals with Gag-specific CMI responses had increased percentages of CD95 + cells, compared to RBq5 and the unvaccinated controls (88% ±9.4% versus 41% ±14%, p=0.010) (Fig. 5A). This suggested that the CD8 + T cells in the four successfully vaccinated animals had an activated or memory phenotype. Because these were outbred animals, it was not possible to
4 106 T.M. Yankee et al. / Virology 383 (2009) Fig. 4. Vaccinated animals have Gag-specific and Nef-specific CMI responses, but not Env-specific CMI responses, prior to challenge. Panel A. PBMCs were stimulated with overlapping peptides from Gag, Nef, or Env and IFNγ production was measured by ELISPOT. The numbers in each bar are the number of IFNγ producing cells/million total PBMCs. Panel B. PBMCs were stimulated with Gag, Nef, or Env peptides and proliferation was measured by [ 3 H]thymidine uptake. The stimulation index (SI) was calculated as the number of cpm induced by peptides divided by the cpm in unstimulated cells. Panel C. PBMCs were loaded with CFSE before stimulation with Gag, Nef, or Env peptides. After four days, cells were harvested labeled with anti-cd3, anti-cd4, and anti-cd8. The SI for CD3 + CD4 + and CD3 + CD8 + cells was calculated by dividing the percentage of CFSE lo cells in the peptide-stimulated samples by the percentage of CFSE lo cells in the unstimulated. define the phenotype of the antigen-specific T cells, although the persistence of the proliferation and IFNγ production suggested that the animals developed immunologic memory. We also tested whether sera from these animals developed neutralizing antibodies against pathogenic SHIV PPC, the parent virus of the vaccine. The sera were tested nearly eight years after the initial
5 T.M. Yankee et al. / Virology 383 (2009) Fig. 5. Macaques that were protected from challenge had an increase in the percentage of activated/memory CD8 + T cells prior to challenge and an expansion of CD4 + CD8 lo cells after challenge. Panel A. Prior to challenge, PBMCs were gated on CD3 + cells and analyzed for CD4 and CD8 expression (upper row). Cells were then gated on CD4 +, CD8 +, or CD4 + CD8 lo (DP) cells and analyzed for CD28 and CD95 expression (lower three rows). Panel B. Eight weeks after challenge, the experiment in Panel A was repeated. vaccination and prior to challenge. Macaques RBq5, RCu5, and RTp5 had neutralizing antibody titers less than 1:10 while RUr5 had a titer of 1:80 and RVq5 had a titer of 1:160. These data indicate that only two of the five animals developed and sustained detectable neutralizing antibodies. Protection against challenge Nearly eight years after the first inoculation with ΔvpuSHIV PPC, five years after the second inoculation with ΔvpuSHIV PPC, and nearly three years, after the anti-cd8 treatment (week 404), the five
6 108 T.M. Yankee et al. / Virology 383 (2009) Table 4 Viral RNA in plasma (copies/ml) after challenge a RBq RCu RTp RUr RVq 13Z AL-95 Week 404 challenge ND b ND ND ND ND ND ND Week 405 3,796,200 ND ND ND ND 894, ,988 Week ,136 ND ND ND ND 2,109,780 3,777,240 Week ,436 ND ND ND ND 258,108 88,812 Week ,200 ND ND ND ND 338, ,608 Week 412 ND ND ND ND ND 1,784, ,208 a Four of five vaccinated animals had no detectable SIV RNA during the eight week period after challenge. b ND = none detected. vaccinated animals and two unvaccinated control animals were challenged with a mixture of the pathogenic viruses SHIV KU2 and SIV mac 239. The four vaccinated animals that had detectable Gagspecific CMI responses prior to challenge had no detectable viremia following challenge with pathogenic virus (Table 4). The two unvaccinated animals and animal RBq5 developed viral RNA loads that exceeded 10 6 viral copies/ml plasma. Whereas RBq5 ultimately controlled viral replication, the detectable viral mrna levels persisted in the unvaccinated controls. These data suggested that RBq5 could not control the initial replication of the virus, but had an immune response that protected this animal from chronic viral infections. These data suggested that Gag-specific CMI responses may be predictive of successful vaccination. The four protected animals had greatly augmented Gag-specific and Nef-specific ELISPOT and ASP after challenge, compared to prior to challenge, indicating that infection with pathogenic virus triggered a robust immune response (Fig. 6). Only two animals (RTp5 and RVq5) developed Env-specific ELISPOT and one animal, RUr5, developed Envspecific ASP. These data suggested that Gag-specific and Nef-specific immune responses are more essential than Env-specific immune responses for the protection of animals against challenge with pathogenic SIV and SHIV. Finally, we analyzed the surface phenotype of T cell populations after challenge (Fig. 5B). The four vaccinated macaques that resisted challenge by pathogenic viruses had a four-fold increase in the percentage of CD3 + PBMC that were CD4 + CD8 lo,comparedtotheir respective pre-challenge phenotypes. On average, 2.6%±1.1% of CD3 + PBMCs were CD4 + CD8 lo prior to challenge and 10%±4.3% of CD3 + PBMCs were CD4 + CD8 lo post-challenge (p=0.040, paired t test). A statistically significant increase in the CD4 + CD8 lo population was not observed following challenge with pathogenic viruses in macaque RBq5 or the two control animals. In RBq5 and the control animals, an average of 4.0%±1.5% of CD3 + PBMCs were CD4 + CD8 lo prior to challenge and 3.3%± 1.1% of CD3 + PBMCs were CD4 + CD8 lo after challenge (p=0.11).thesedata suggested that the increase in CD4 + CD8 lo cells correlated with immunologic protection. Fig. 6. Vaccinated animals maintain SIV-specific CMI after challenge. Panel A. IFNγ production by PBMCs was calculated as described in the legend to Fig. 4. Panel B. Peptide-specific proliferation was analyzed by [ 3 H]thymidine uptake and the SI was calculated, as described in the legend of Fig. 4.
7 T.M. Yankee et al. / Virology 383 (2009) Discussion The data presented here represent the longest assessment of the safety and efficacy of a live vaccine virus against SIV in macaques. Animals were inoculated with ΔvpuSHIV PPC twice in order to determine if this vaccine strategy could protect animals from productive infection induced by pathogenic virus. Prior experiments used a single inoculation of ΔvpuSHIV PPC followed three years later by challenge with a cocktail of pathogenic viruses (Kumar et al., 2008). Under these conditions, the vaccine virus was unable to prevent viremia. However, in the current study, animals were vaccinated, revaccinated three years later, and then challenged five years after the second inoculation. Four of five animals were aviremic following infection with challenge viruses. These data demonstrate that multiple inoculations with a live virus vaccine can extend the efficacy of the vaccine. Despite transient declines in circulating CD4 + and CD8 + T cell levels, no sustained loss of CD4 + or CD8 + T cells was observed in any of the five vaccinated animals, indicating that ΔvpuSHIV PPC was safe for use in the context of repeated inoculations over time. A possible explanation for these transient decreases in the number of circulating T cells is that the virus may infect and kill thymocytes. When replication of ΔvpuSHIV PPC is controlled, the thymus may be restored and T cell counts recover. Alternatively, the depletion of circulating T cells could be attributed to re-localization of cells from the blood into lymphoid tissues. Further studies are required to determine the mechanism. Previous studies demonstrated that the vaccine virus must persist in order for protection against disease induced by pathogenic virus to be sustained (Kumar et al., 2008). In the current study, we treated macaques with anti-cd8 antibodies to transiently deplete the animals of CD8 + T cells to determine if a resurgence in viremia would occur from undetectable reservoirs of the vaccine virus (Table 3). While this treatment demonstrated that four of five vaccinated animals still harbored virus, it also led to a third bolus of vaccine virus. This extra bolus may have boosted the immune responses against Gag and Nef, adding to the efficacy of the vaccine. The animals that had three boluses of viral replication did not develop high viral loads and AIDS, despite having an average of 34-fold increase in viral burdens after the anti-cd8 treatment than after either immunization. These data clearly demonstrate that the virus remained viable, but had not reverted to a pathogenic phenotype. A striking feature of the protective immunity observed in this study was the complete lack of viremia in successfully vaccinated animals (Table 4). This remarkable suppression of viral replication was likely due to Gag-specific and Nef-specific CD8 + T cells that could recognize and become activated by MHC class I-expressing cells that presented Gag or Nef peptides because no Env-specific immune responses could be detected in most animals. The importance of Gag-specific immune responses was highlighted in a recent paper by Kiepela et al. (2007), who showed in HIV-infected individuals that Gag-specific immune responses were associated with lower levels of viremia and Env-specific responses were associated with higher levels of viremia. In addition, it was recently reported that the Gag liberated during the virus-uncoating stage can be processed and presented on MHC class I prior to viral integration (Sacha et al., 2007). In the case of an intravenous injection of challenge virus, it is likely that virus infected the macrophages in the blood and spleen and then Gag-specific CD8 + T cells targeted and killed the infected cells before the virus could complete its life cycle. Of note, little or no Env-specific cellular-mediated immune responses were detected prior to challenge in any of the animals and only two animals had detectable anti-shiv PPC neutralizing antibody titers prior to challenge. In addition, the animals were vaccinated with a derivative of SHIV that contains a macaque-adapted HXB2 envelope glycoprotein, which is CXCR4-tropic. The animals were challenged with a mixture of CXCR4-tropic SHIV KU2 and CCR5- tropic SIV mac 239. If there were undetectable Env-specific immune responses in the vaccinated animals, these responses would likely be directed against the challenge SHIV, not SIV. However, our data demonstrated that ΔvpuSHIV PPC protected against productive infection by both SHIV KU2 and SIV mac 239, suggesting that Envspecific immune responses were not critical for immunological protection of the challenge viruses. This observation is highly significant for vaccine design because Env is not well conserved across HIV-1 strains and subtypes while Gag is more conserved. Thus, it is likely that a single vaccine could be effective against multiple strains of HIV-1 and perhaps multiple subtypes of the virus. It is unlikely that the mechanism of protection conferred by ΔvpuSHIV PPC is viral interference because ΔvpuSHIV PPC and SIV mac 239 have different tropisms. ΔvpuSHIV PPC targets CXCR4-expressing CD4 + T cells, which are primarily naïve peripheral T cells and T cell precursors in the thymus. SIV mac 239 targets CCR5-expressing cells, which are primarily memory T cells. Another reason that viral interference is unlikely is that, at the time of challenge, there was no detectable vaccine virus in the plasma. It is difficult to conceive that an undetectable viral load could interfere with a high intravenous dose of challenge virus. Macaque RBq5 was the outlier in this study. This animal did not develop a resurgence of virus after treatment with the anti-cd8 antibodies (Table 3), suggesting that the animal had eliminated the vaccine virus. The lack of CMI responses against Gag and Nef together with failure of the vaccine virus to persist supported our previous work showing that maintenance of vaccine-induced CMI responses required persistence of the virus (Joag et al., 1998b; Silverstein et al., 2000; Mackay et al., 2004a). More importantly, however, the data from RBq5 reinforced the conclusion from the present study that CMI responses against Gag and Nef correlated with protection from productive infection by the challenge virus. The fact that this animal developed control of the challenge virus, similar to the manner in which it controlled the vaccine virus, suggested that it had mounted a strong innate immune response that did not develop into an adaptive immune response. This conclusion was also supported by the fact that RBq5 did not develop the transient loss of T cells following inoculation with the vaccine see in the other animals. Coinciding with control of replication of the challenge virus, CD4 + CD8 lo T cells underwent substantial expansion in the successfully vaccinated animals (Fig. 2). CD4 + CD8 lo T cells were first described in humans by Blue et al. (1985) and have since been found in healthy individuals as well as in patients with viral infections, tumors, and autoimmune diseases. In healthy individuals, the majority of CD4 + CD8 lo T cells have a memory phenotype and can be readily activated by virally infected cells in vitro (Nascimbeni et al., 2004; Pahar et al., 2006). This has led to the speculation that peripheral CD4 + CD8 lo T cells are terminally differentiated memory T cells. In further support of this model, CD4 + CD8 lo T cells have been shown to be expanded preferentially in an individual infected with HIV for eight years (Weiss et al., 1998). CD4 + CD8 lo T cells are a target for SIV infection in macaques (Akari et al., 1999). The expansion of this population of cells in the animals resisting productive infection by pathogenic virus suggested that these cells are an important component of the immune response needed to control viral replication. In conclusion, the results presented here describe a longitudinal study in which macaques were inoculated twice over the course of an eight-year study. Whereas previous studies using a single inoculation demonstrated that ΔvpuSHIV PPC could not protect animals from productive infection by a pathogenic virus beyond three years, this study shows that a second inoculation extended the duration of protection beyond eight years.
8 110 T.M. Yankee et al. / Virology 383 (2009) Materials and methods Animals and vaccination Indian rhesus macaques were housed individually in the Laboratory Animal Resources building of the University of Kansas Medical Center (Kansas City, KS) under conditions approved by the Association for the Assessment and Accreditation of Laboratory Animal Care. These studies were begun when the animals were five years old. All experiments were performed in compliance with the University of Kansas Medical Center Institutional Animal Care and Use Committee. Infectious DNA of ΔvpuSHIV KU1 was prepared as described earlier (Joag et al., 1998a). A virus stock was prepared from this DNA by transfecting CEM174 cells with the DNA followed by harvest of supernatant fluid several days later. Animals were inoculated intradermally with 200 μg of the infectious DNA suspended in 2 ml of PBS. The animals were injected at four sites with 0.5 ml of the DNA suspension. Three years later, animals were revaccinated orally with the vaccine virus. Each animal was tranquilized and 1 ml of the viral suspension was placed at the back of the mouth using a 1 ml syringe. Stocks of SIV mac 239 and SHIV KU2 were prepared by inoculating CD8-depleted PBMCs from a rhesus macaque. The supernatant fluid from this culture was collected, aliquoted, and frozen at 80 C, similar to the vaccine virus. Infectivity of both viruses was assessed in CEM174 cells and showed a titer of approximately 10 5 TCID/ml. Processing of blood samples Peripheral venous blood collected in EDTA was centrifuged to separate plasma and buffy coats. Plasma was frozen for determination of plasma viral RNA concentrations. PBMC were separated from buffy coats by centrifugation through Ficoll-Paque density gradients and portions used for virus isolation, flow cytometry, antigen-specific proliferation (ASP), and ELISPOT assays. Determining plasma viral RNA using quantitative real-time RT-PCR analysis Plasma viral RNA loads were measured in RNA extracted from μl of EDTA anticoagulated plasma samples as previously described (Mackay et al., 2002, 2004a). Briefly, RNA samples were subjected to real-time RT-PCR using gag specific primers (forward GCAGAGGAGGAAATTACCCAGTAC, reverse CAATTTTACCCAGGCATT- TAATGTT), 5 -FAM- and 3 -TAMRA-labeled TaqMan probe (TGTCCA- CCTGCCATTAAGCCCGA), and the Taqman Universal PCR Mastermix (Applied Biosystems) in duplicate reactions in the ABI PRISM 7700 Sequence Detection System (Hofmann-Lehmann et al., 2000). These primers and probes detect all SHIVs and SIVs in this study. Viral RNA copy numbers were calculated per milliliter of plasma. The minimal level of detection was 360 copies/ml. Flow cytometry and determination of CD4/CD8 levels Anti-CD3-FITC, anti-cd4-pe, anti-cd8-apc-cy7, anti-cd28-apc, and anti-cd95-pe were purchased from BD Bioscience, San Jose, CA. Flow cytometry studies were performed using a BD LSR II (BD Immunocytometry Systems, San Jose, CA). Data were analyzed using BD FACSDiva software (BD Biosciences, San Jose, CA). The absolute numbers of CD4 + and CD8 + T cells were calculated by multiplying the percentage of CD4 + CD3 + and CD8 + CD3 + cells by the lymphocytes/μl from a complete blood count. Antigen-specific proliferation (ASP) assays The ASP assays were performed as previously described (Mackay et al., 2004a). Briefly, triplicate cultures of PBMC were incubated with overlapping peptides derived from Gag, Nef, or Env for four days at 37 C. The peptides were 15-mers based on the sequence of the SIV mac 239 and spanned the entire length of the proteins. Peptides were kindly provided by the National Institutes of Health AIDS Research and Reference Reagent Program (McKesson Bio-Services, Germantown, MD). [ 3 H]Thymidine was added to the culture h before harvesting. [ 3 H]Thymidine incorporation was measured by liquid scintillation counting (Packard Instrument, Meriden, CT). Stimulation indices (SI) were calculated as mean cpm, divided by the mean cpm in control wells. SI values greater than three were considered significant because SIs greater than two were never obtained with PBMCs from non-immunized animals. ELISPOT assays ELSIPOT assays were performed as described previously (Mackay et al., 2004b). Briefly, IFNγ production was measured by incubating PBMC with the same peptides used for ASP analyses. Millipore multiscreen Immobilon-P opaque hydrophobic high-protein binding 96-well plates (0.45 μm; Billerica, MA) were coated with anti-monkey IFNγ (Mabtech, Stockholm, Sweden). Cells were incubated with media alone, media containing peptides, or media containing Con A. After incubation and washing, Vectastain AB kit (Vector Laboratories, Burlingame, CA) was added. Color development was performed using Nova-Red. Spots were counted with a stereomicroscope and reported as number of sports/10 6 PBMC. CD8 + T cell depletion On day 0 of treatment, animals were given 10 mg/kg anti-cd8 antibodies subcutaneously. On days 3 and 7, animals were injected intravenously with 5 mg/kg anti-cd8 antibodies. The anti-cd8 antibodies were kindly provided by Dr. Keith Reimann, Beth Israel Deaconess Medical Center, Harvard Medical School. Blood samples were obtained at the indicated time points for analysis. Neutralizing antibody assay Two-fold dilutions of sera were mixed with 100 TCID 50 and CEMX174 cells. Virus-sera mixtures were incubated at 37 C for 30 min and then inoculated into respective indicator cell cultures. Inoculated cells were examined for development of fusion cytopathic effects everyday for one week. Acknowledgments The anti-cd8 mabs were kindly provided by the National Cell Culture Center (BioVest International, Minneapolis, MN), and produced by Keith Reimann and Joern Schmitz. We especially thank Dr. Reimann for helpful suggestions. We thank Istvan Adany, Zhuang Li, and Ramakrishna Hedge for technical assistance. This publication was made supported by NIH Grant Number P20 RR from the COBRE Program of the National Center for Research Resource, AI051220, AI References Akari, H., Nam, K.H., Mori, K., Otani, I., Shibata, H., Adachi, A., Terao, K., Yoshikawa, Y., Effects of SIVmac infection on peripheral blood CD4+CD8+ T lymphocytes in cynomolgus macaques. Clin. Immunol. 91, Baba, T.W., Jeong, Y.S., Pennick, D., Bronson, R., Greene, M.F., Ruprecht, R.M., Pathogenicity of live, attenuated SIV after mucosal infection of neonatal macaques. Science 267, Baba, T.W., Liska, V., Khimani, A.H., Ray, N.B., Dailey, P.J., Penninck, D., Bronson, R., Greene, M.F., McClure, H.M., Martin, L.N., Ruprecht, R.M., Live attenuated, multiply deleted simian immunodeficiency virus causes AIDS in infant and adult macaques. Nat. Med. 5, Blue, M.L., Daley, J.F., Levine, H., Schlossman, S.F., Coexpression of T4 and T8 on peripheral blood T cells demonstrated by two-color fluorescence flow cytometry. J. Immunol. 134,
9 T.M. Yankee et al. / Virology 383 (2009) Daniel, M.D., Kirchhoff, F., Czajak, S.C., Sehgal, P.K., Desrosiers, R.C., Protective effects of a live attenuated SIV vaccine with a deletion in the nef gene. Science 258, Hofmann-Lehmann, R., Swenerton, R.K., Liska, V., Leutenegger, C.M., Lutz, H., McClure, H.M., Ruprecht, R.M., Sensitive and robust one-tube real-time reverse transcriptase-polymerase chain reaction to quantify SIV RNA load: comparison of one- versus two-enzyme systems. AIDS Res. Hum. Retrovir. 16, Jin, X., Bauer, D.E., Tuttleton, S.E., Lewin, S., Gettie, A., Blanchard, J., Irwin, C.E., Safrit, J.T., Mittler, J., Weinberger, L., Kostrikis, L.G., Zhang, L., Perelson, A.S., Ho, D.D., Dramatic rise in plasma viremia after CD8(+) T cell depletion in simian immunodeficiency virus-infected macaques. J. Exp. Med. 189, Joag, S.V., Li, Z., Foresman, L., Stephens, E.B., Zhao, L.J., Adany, I., Pinson, D.M., McClure, H.M., Narayan, O., Chimeric simian/human immunodeficiency virus that causes progressive loss of CD4+ T cells and AIDS in pig-tailed macaques. J. Virol. 70, Joag, S.V., Adany, I., Li, Z., Foresman, L., Pinson, D.M., Wang, C., Stephens, E.B., Raghavan, R., Narayan, O., 1997a. Animal model of mucosally transmitted human immunodeficiency virus type 1 disease: intravaginal and oral deposition of simian/human immunodeficiency virus in macaques results in systemic infection, elimination of CD4+ T cells, and AIDS. J. Virol. 71, Joag, S.V., Li, Z., Foresman, L., Pinson, D.M., Raghavan, R., Zhuge, W., Adany, I., Wang, C., Jia, F., Sheffer, D., Ranchalis, J., Watson, A., Narayan, O., 1997b. Characterization of the pathogenic KU-SHIV model of acquired immunodeficiency syndrome in macaques. AIDS Res. Hum. Retrovir. 13, Joag, S.V., Liu, Z.Q., Stephens, E.B., Smith, M.S., Kumar, A., Li, Z., Wang, C., Sheffer, D., Jia, F., Foresman, L., Adany, I., Lifson, J., McClure, H.M., Narayan, O.,1998a. Oral immunization of macaques with attenuated vaccine virus induces protection against vaginally transmitted AIDS. J. Virol. 72, Joag, S.V., Liu, Z.Q., Stephens, E.B., Smith, M.S., Kumar, A., Li, Z., Wang, C., Sheffer, D., Jia, F., Foresman, L., Adany, I., Lifson, J., McClure, H.M., Narayan, O., 1998b. Oral immunization of macaques with attenuated vaccine virus induces protection against vaginally transmitted AIDS. J. Virol. 72, Kiepiela, P., Ngumbela, K., Thobakgale, C., Ramduth, D., Honeyborne, I., Moodley, E., Reddy, S., de Pierres, C., Mncube, Z., Mkhwanazi, N., Bishop, K., van der Stok, M., Nair, K., Khan, N., Crawford, H., Payne, R., Leslie, A., Prado, J., Prendergast, A., Frater, J., McCarthy, N., Brander, C., Learn, G.H., Nickle, D., Rousseau, C., Coovadia, H., Mullins, J.I., Heckerman, D., Walker, B.D., Goulder, P., CD8+ T-cell responses to different HIV proteins have discordant associations with viral load. Nat. Med. 13, Kumar, A., Liu, Z., Sheffer, D., Smith, M., Singh, D.K., Buch, S., Narayan, O., Protection of macaques against AIDS with a live attenuated SHIV vaccine is of finite duration. Virology 371, Mackay, G.A., Niu, Y., Liu, Z.Q., Mukherjee, S., Li, Z., Adany, I., Buch, S., Zhuge, W., McClure, H.M., Narayan, O., Smith, M.S., Presence of Intact vpu and nef genes in nonpathogenic SHIV is essential for acquisition of pathogenicity of this virus by serial passage in macaques. Virology 295, Mackay, G.A., Liu, Z., Singh, D.K., Smith, M.S., Mukherjee, S., Sheffer, D., Jia, F., Adany, I., Sun, K.H., Dhillon, S., Zhuge, W., Narayan, O., 2004a. Protection against lateonset AIDS in macaques prophylactically immunized with a live simian HIV vaccine was dependent on persistence of the vaccine virus. J. Immunol. 173, Mackay, G.A., Liu, Z., Singh, D.K., Smith, M.S., Mukherjee, S., Sheffer, D., Jia, F., Adany, I., Sun, K.H., Dhillon, S., Zhuge, W., Narayan, O., 2004b. Protection against lateonset AIDS in macaques prophylactically immunized with a live simian HIV vaccine was dependent on persistence of the vaccine virus. J. Immunol. 173, Nascimbeni, M., Shin, E.C., Chiriboga, L., Kleiner, D.E., Rehermann, B., Peripheral CD4(+)CD8(+) T cells are differentiated effector memory cells with antiviral functions. Blood 104, Pahar, B., Lackner, A.A., Veazey, R.S., Intestinal double-positive CD4+CD8+ T cells are highly activated memory cells with an increased capacity to produce cytokines. Eur. J. Immunol. 36, Robinson, H.L., HIV/AIDS vaccines: Clin. Pharmacol. Ther. 82, Sacha, J.B., Chung, C., Rakasz, E.G., Spencer, S.P., Jonas, A.K., Bean, A.T., Lee, W., Burwitz, B.J., Stephany, J.J., Loffredo, J.T., Allison, D.B., Adnan, S., Hoji, A., Wilson, N.A., Friedrich, T.C., Lifson, J.D., Yang, O.O., Watkins, D.I., Gag-specific CD8+T lymphocytes recognize infected cells before AIDS-virus integration and viral protein expression. J. Immunol. 178, Schmitz, J.E., Simon, M.A., Kuroda, M.J., Lifton, M.A., Ollert, M.W., Vogel, C.W., Racz, P., Tenner-Racz, K., Scallon, B.J., Dalesandro, M., Ghrayeb, J., Rieber, E.P., Sasseville, V.G., Reimann, K.A., A nonhuman primate model for the selective elimination of CD8+ lymphocytes using a mouse-human chimeric monoclonal antibody. Am. J. Pathol. 154, Silverstein, P.S., Mackay, G.A., Mukherjee, S., Li, Z., Piatak Jr., M., Lifson, J.D., Narayan, O., Kumar, A., Pathogenic simian/human immunodeficiency virus SHIV(KU) inoculated into immunized macaques caused infection, but virus burdens progressively declined with time. J. Virol. 74, Weiss, L., Roux, A., Garcia, S., Demouchy, C., Haeffner-Cavaillon, N., Kazatchkine, M.D., Gougeon, M.L., Persistent expansion, in a human immunodeficiency virusinfected person, of V beta-restricted CD4+CD8+ T lymphocytes that express cytotoxicity-associated molecules and are committed to produce interferongamma and tumor necrosis factor-alpha. J. Infect. Dis. 178, Whitney, J.B., Ruprecht, R.M., Live attenuated HIV vaccines: pitfalls and prospects. Curr. Opin. Infect. Dis. 17,
on January 7, 2019 by guest
 JOURNAL OF VIROLOGY, Nov. 2000, p. 10489 10497 Vol. 74, No. 22 0022-538X/00/$04.00 0 Copyright 2000, American Society for Microbiology. All Rights Reserved. Pathogenic Simian/Human Immunodeficiency Virus
JOURNAL OF VIROLOGY, Nov. 2000, p. 10489 10497 Vol. 74, No. 22 0022-538X/00/$04.00 0 Copyright 2000, American Society for Microbiology. All Rights Reserved. Pathogenic Simian/Human Immunodeficiency Virus
Received 29 August 2002/Accepted 3 December 2002
 JOURNAL OF VIROLOGY, Mar. 2003, p. 3099 3118 Vol. 77, No. 5 0022-538X/03/$08.00 0 DOI: 10.1128/JVI.77.5.3099 3118.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved. Simian-Human
JOURNAL OF VIROLOGY, Mar. 2003, p. 3099 3118 Vol. 77, No. 5 0022-538X/03/$08.00 0 DOI: 10.1128/JVI.77.5.3099 3118.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved. Simian-Human
Antibody Dependent Cellular Cytotxic activity: Past and Future. Guido Ferrari, M.D. Duke University Medical Center
 Antibody Dependent Cellular Cytotxic activity: Past and Future Guido Ferrari, M.D. Duke University Medical Center Mechanism of Antibody Dependent Cellular Cytotoxicity (ADCC) ADCC Effector Cells (NK, monocytes/macrophages,
Antibody Dependent Cellular Cytotxic activity: Past and Future Guido Ferrari, M.D. Duke University Medical Center Mechanism of Antibody Dependent Cellular Cytotoxicity (ADCC) ADCC Effector Cells (NK, monocytes/macrophages,
How HIV Causes Disease Prof. Bruce D. Walker
 How HIV Causes Disease Howard Hughes Medical Institute Massachusetts General Hospital Harvard Medical School 1 The global AIDS crisis 60 million infections 20 million deaths 2 3 The screen versions of
How HIV Causes Disease Howard Hughes Medical Institute Massachusetts General Hospital Harvard Medical School 1 The global AIDS crisis 60 million infections 20 million deaths 2 3 The screen versions of
Immunoprophylaxis against AIDS in macaques with a lentiviral DNA vaccine
 Virology 351 (2006) 444 454 www.elsevier.com/locate/yviro Immunoprophylaxis against AIDS in macaques with a lentiviral DNA vaccine ZhenQian Liu a, Dinesh K. Singh a,1, Darlene Sheffer a, Marilyn S. Smith
Virology 351 (2006) 444 454 www.elsevier.com/locate/yviro Immunoprophylaxis against AIDS in macaques with a lentiviral DNA vaccine ZhenQian Liu a, Dinesh K. Singh a,1, Darlene Sheffer a, Marilyn S. Smith
HIV Anti-HIV Neutralizing Antibodies
 ,**/ The Japanese Society for AIDS Research The Journal of AIDS Research : HIV HIV Anti-HIV Neutralizing Antibodies * Junji SHIBATA and Shuzo MATSUSHITA * Division of Clinical Retrovirology and Infectious
,**/ The Japanese Society for AIDS Research The Journal of AIDS Research : HIV HIV Anti-HIV Neutralizing Antibodies * Junji SHIBATA and Shuzo MATSUSHITA * Division of Clinical Retrovirology and Infectious
Received 4 December 2001/Accepted 29 April 2002
 JOURNAL OF VIROLOGY, Aug. 2002, p. 8433 8445 Vol. 76, No. 16 0022-538X/02/$04.00 0 DOI: 10.1128/JVI.76.16.8433 8445.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved. The Relationship
JOURNAL OF VIROLOGY, Aug. 2002, p. 8433 8445 Vol. 76, No. 16 0022-538X/02/$04.00 0 DOI: 10.1128/JVI.76.16.8433 8445.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved. The Relationship
Immunization with single-cycle SIV significantly reduces viral loads after an intravenous challenge with SIV(mac)239
 University of Massachusetts Medical School escholarship@umms Preventive and Behavioral Medicine Publications and Presentations Preventive and Behavioral Medicine 1-23-2009 Immunization with single-cycle
University of Massachusetts Medical School escholarship@umms Preventive and Behavioral Medicine Publications and Presentations Preventive and Behavioral Medicine 1-23-2009 Immunization with single-cycle
Nature Medicine: doi: /nm.2109
 HIV 1 Infects Multipotent Progenitor Cells Causing Cell Death and Establishing Latent Cellular Reservoirs Christoph C. Carter, Adewunmi Onafuwa Nuga, Lucy A. M c Namara, James Riddell IV, Dale Bixby, Michael
HIV 1 Infects Multipotent Progenitor Cells Causing Cell Death and Establishing Latent Cellular Reservoirs Christoph C. Carter, Adewunmi Onafuwa Nuga, Lucy A. M c Namara, James Riddell IV, Dale Bixby, Michael
DEBATE ON HIV ENVELOPE AS A T CELL IMMUNOGEN HAS BEEN GAG-GED
 DEBATE ON HIV ENVELOPE AS A T CELL IMMUNOGEN HAS BEEN GAG-GED Viv Peut Kent Laboratory, University of Melbourne, Australia WHY ENVELOPE? Env subject to both humoral and cellular immune responses Perhaps
DEBATE ON HIV ENVELOPE AS A T CELL IMMUNOGEN HAS BEEN GAG-GED Viv Peut Kent Laboratory, University of Melbourne, Australia WHY ENVELOPE? Env subject to both humoral and cellular immune responses Perhaps
Rapid perforin upregulation directly ex vivo by CD8 + T cells is a defining characteristic of HIV elite controllers
 Rapid perforin upregulation directly ex vivo by CD8 + T cells is a defining characteristic of HIV elite controllers Adam R. Hersperger Department of Microbiology University of Pennsylvania Evidence for
Rapid perforin upregulation directly ex vivo by CD8 + T cells is a defining characteristic of HIV elite controllers Adam R. Hersperger Department of Microbiology University of Pennsylvania Evidence for
A VACCINE FOR HIV BIOE 301 LECTURE 10 MITALI BANERJEE HAART
 BIOE 301 LECTURE 10 MITALI BANERJEE A VACCINE FOR HIV HIV HAART Visit wikipedia.org and learn the mechanism of action of the five classes of antiretroviral drugs. (1) Reverse transcriptase inhibitors (RTIs)
BIOE 301 LECTURE 10 MITALI BANERJEE A VACCINE FOR HIV HIV HAART Visit wikipedia.org and learn the mechanism of action of the five classes of antiretroviral drugs. (1) Reverse transcriptase inhibitors (RTIs)
Supplemental Materials and Methods Plasmids and viruses Quantitative Reverse Transcription PCR Generation of molecular standard for quantitative PCR
 Supplemental Materials and Methods Plasmids and viruses To generate pseudotyped viruses, the previously described recombinant plasmids pnl4-3-δnef-gfp or pnl4-3-δ6-drgfp and a vector expressing HIV-1 X4
Supplemental Materials and Methods Plasmids and viruses To generate pseudotyped viruses, the previously described recombinant plasmids pnl4-3-δnef-gfp or pnl4-3-δ6-drgfp and a vector expressing HIV-1 X4
Innate and Cellular Immunology Control of Infection by Cell-mediated Immunity
 Innate & adaptive Immunity Innate and Cellular Immunology Control of Infection by Cell-mediated Immunity Helen Horton PhD Seattle Biomedical Research Institute Depts of Global Health & Medicine, UW Cellular
Innate & adaptive Immunity Innate and Cellular Immunology Control of Infection by Cell-mediated Immunity Helen Horton PhD Seattle Biomedical Research Institute Depts of Global Health & Medicine, UW Cellular
Supporting Information
 Supporting Information Sui et al..7/pnas.997 Pre-CLP CM9 LA9 SL Tat# Pol Vif % Tetramer + CD + CD + Vac+IL- +IL- Vac Fig. S. Frequencies of six different CD + CD + Mamu-A*-tetramer + cells were measured
Supporting Information Sui et al..7/pnas.997 Pre-CLP CM9 LA9 SL Tat# Pol Vif % Tetramer + CD + CD + Vac+IL- +IL- Vac Fig. S. Frequencies of six different CD + CD + Mamu-A*-tetramer + cells were measured
Immunization with Single-Cycle SIV Significantly Reduces Viral Loads After an Intravenous Challenge with SIV mac 239
 Immunization with Single-Cycle SIV Significantly Reduces Viral Loads After an Intravenous Challenge with SIV mac 239 Bin Jia 1, Sharon K. Ng 1, M. Quinn DeGottardi 1, Michael Piatak Jr. 2, Eloísa Yuste
Immunization with Single-Cycle SIV Significantly Reduces Viral Loads After an Intravenous Challenge with SIV mac 239 Bin Jia 1, Sharon K. Ng 1, M. Quinn DeGottardi 1, Michael Piatak Jr. 2, Eloísa Yuste
Alternate Antibody-Based Therapeutic Strategies To Purge the HIV Cell Reservoir
 Alternate Antibody-Based Therapeutic Strategies To Purge the HIV Cell Reservoir Giuseppe Pantaleo, M.D. Professor of Medicine Head, Division of Immunology and Allergy Executive Director, Swiss Vaccine
Alternate Antibody-Based Therapeutic Strategies To Purge the HIV Cell Reservoir Giuseppe Pantaleo, M.D. Professor of Medicine Head, Division of Immunology and Allergy Executive Director, Swiss Vaccine
Characterization of T-Cell Responses in Macaques Immunized with a Single Dose of HIV DNA Vaccine
 JOURNAL OF VIROLOGY, Feb. 2010, p. 1243 1253 Vol. 84, No. 3 0022-538X/10/$12.00 doi:10.1128/jvi.01846-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Characterization of T-Cell
JOURNAL OF VIROLOGY, Feb. 2010, p. 1243 1253 Vol. 84, No. 3 0022-538X/10/$12.00 doi:10.1128/jvi.01846-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Characterization of T-Cell
Original Article. Kwofie TB, Miura T 1. Abstract. Introduction
 Original Article Increased Virus Replication and Cytotoxicity of Non pathogenic Simian Human Immuno Deficiency Viruses NM 3rN After Serial Passage in a Monkey Derived Cell Line Kwofie TB, Miura T 1 Departments
Original Article Increased Virus Replication and Cytotoxicity of Non pathogenic Simian Human Immuno Deficiency Viruses NM 3rN After Serial Passage in a Monkey Derived Cell Line Kwofie TB, Miura T 1 Departments
staining and flow cytometry
 Detection of influenza virus-specific T cell responses by intracellular by cytokine intracellular staining cytokine staining and flow cytometry Detection of influenza virus-specific T cell responses and
Detection of influenza virus-specific T cell responses by intracellular by cytokine intracellular staining cytokine staining and flow cytometry Detection of influenza virus-specific T cell responses and
NK mediated Antibody Dependent Cellular Cytotoxicity in HIV infections
 NK mediated Antibody Dependent Cellular Cytotoxicity in HIV infections Amy Chung Dr. Ivan Stratov Prof. Stephen Kent ADCC process consists of Target cell QuickTime and a TIFF (Uncompressed) FcγR decompressor
NK mediated Antibody Dependent Cellular Cytotoxicity in HIV infections Amy Chung Dr. Ivan Stratov Prof. Stephen Kent ADCC process consists of Target cell QuickTime and a TIFF (Uncompressed) FcγR decompressor
Fayth K. Yoshimura, Ph.D. September 7, of 7 HIV - BASIC PROPERTIES
 1 of 7 I. Viral Origin. A. Retrovirus - animal lentiviruses. HIV - BASIC PROPERTIES 1. HIV is a member of the Retrovirus family and more specifically it is a member of the Lentivirus genus of this family.
1 of 7 I. Viral Origin. A. Retrovirus - animal lentiviruses. HIV - BASIC PROPERTIES 1. HIV is a member of the Retrovirus family and more specifically it is a member of the Lentivirus genus of this family.
ADCC Develops Over Time during Persistent Infection with Live-Attenuated SIV and Is Associated with Complete Protection against SIV(mac)251 Challenge
 University of Massachusetts Medical School escholarship@umms Preventive and Behavioral Medicine Publications and Presentations Preventive and Behavioral Medicine 8-2012 ADCC Develops Over Time during Persistent
University of Massachusetts Medical School escholarship@umms Preventive and Behavioral Medicine Publications and Presentations Preventive and Behavioral Medicine 8-2012 ADCC Develops Over Time during Persistent
Received 8 October 1997/Accepted 5 January 1998
 JOURNAL OF VIROLOGY, Apr. 1998, p. 3248 3258 Vol. 72, No. 4 0022-538X/98/$04.00 0 Copyright 1998, American Society for Microbiology In Vivo Replication Capacity Rather Than In Vitro Macrophage Tropism
JOURNAL OF VIROLOGY, Apr. 1998, p. 3248 3258 Vol. 72, No. 4 0022-538X/98/$04.00 0 Copyright 1998, American Society for Microbiology In Vivo Replication Capacity Rather Than In Vitro Macrophage Tropism
Supporting Information
 Supporting Information Walker et al. 1.173/pnas.111753118 - JR-CSF 1 3 1 4 1 5 1 6 1 7 1 8 blank beads protein A beads JR-FL - 1 3 1 4 1 5 1 6 1 7 1 8 - MGRM-C26 1 3 1 4 1 5 1 6 1 7 1 8 reciprocal serum
Supporting Information Walker et al. 1.173/pnas.111753118 - JR-CSF 1 3 1 4 1 5 1 6 1 7 1 8 blank beads protein A beads JR-FL - 1 3 1 4 1 5 1 6 1 7 1 8 - MGRM-C26 1 3 1 4 1 5 1 6 1 7 1 8 reciprocal serum
Establishment and Targeting of the Viral Reservoir in Rhesus Monkeys
 Establishment and Targeting of the Viral Reservoir in Rhesus Monkeys Dan H. Barouch, M.D., Ph.D. Center for Virology and Vaccine Research Beth Israel Deaconess Medical Center Ragon Institute of MGH, MIT,
Establishment and Targeting of the Viral Reservoir in Rhesus Monkeys Dan H. Barouch, M.D., Ph.D. Center for Virology and Vaccine Research Beth Israel Deaconess Medical Center Ragon Institute of MGH, MIT,
Massive infection and loss of memory CD4 + T cells in multiple tissues during acute SIV infection
 Massive infection and loss of memory CD4 + T cells in multiple tissues during acute SIV infection Joseph J. Mattapallil 1, Daniel C. Douek 2, Brenna Hill 2, Yoshiaki Nishimura 3, Malcolm Martin 3 & Mario
Massive infection and loss of memory CD4 + T cells in multiple tissues during acute SIV infection Joseph J. Mattapallil 1, Daniel C. Douek 2, Brenna Hill 2, Yoshiaki Nishimura 3, Malcolm Martin 3 & Mario
Human Immunodeficiency Virus Type-1 Myeloid Derived Suppressor Cells Inhibit Cytomegalovirus Inflammation through Interleukin-27 and B7-H4
 Human Immunodeficiency Virus Type-1 Myeloid Derived Suppressor Cells Inhibit Cytomegalovirus Inflammation through Interleukin-27 and B7-H4 Ankita Garg, Rodney Trout and Stephen A. Spector,,* Department
Human Immunodeficiency Virus Type-1 Myeloid Derived Suppressor Cells Inhibit Cytomegalovirus Inflammation through Interleukin-27 and B7-H4 Ankita Garg, Rodney Trout and Stephen A. Spector,,* Department
Ex vivo Human Antigen-specific T Cell Proliferation and Degranulation Willemijn Hobo 1, Wieger Norde 1 and Harry Dolstra 2*
 Ex vivo Human Antigen-specific T Cell Proliferation and Degranulation Willemijn Hobo 1, Wieger Norde 1 and Harry Dolstra 2* 1 Department of Laboratory Medicine - Laboratory of Hematology, Radboud University
Ex vivo Human Antigen-specific T Cell Proliferation and Degranulation Willemijn Hobo 1, Wieger Norde 1 and Harry Dolstra 2* 1 Department of Laboratory Medicine - Laboratory of Hematology, Radboud University
Rapid antigen-specific T cell enrichment (Rapid ARTE)
 Direct ex vivo characterization of human antigen-specific CD154+CD4+ T cell Rapid antigen-specific T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central role
Direct ex vivo characterization of human antigen-specific CD154+CD4+ T cell Rapid antigen-specific T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central role
Understanding HIV. Transmitted/Founder Viruses. Brandon Keele SAIC-Frederick National Cancer Institute
 Understanding HIV Transmission Utilizing Transmitted/Founder Viruses Brandon Keele SAIC-Frederick National Cancer Institute AIDS Vaccine 2011 15 September 2011 Overview Several years ago, the CHAVI sought
Understanding HIV Transmission Utilizing Transmitted/Founder Viruses Brandon Keele SAIC-Frederick National Cancer Institute AIDS Vaccine 2011 15 September 2011 Overview Several years ago, the CHAVI sought
Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD-
 Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
VIRAL TITER COUNTS. The best methods of measuring infectious lentiviral titer
 VIRAL TITER COUNTS The best methods of measuring infectious lentiviral titer FLUORESCENCE CYCLES qpcr of Viral RNA SUMMARY Viral vectors are now routinely used for gene transduction in a wide variety of
VIRAL TITER COUNTS The best methods of measuring infectious lentiviral titer FLUORESCENCE CYCLES qpcr of Viral RNA SUMMARY Viral vectors are now routinely used for gene transduction in a wide variety of
GOVX-B11: A Clade B HIV Vaccine for the Developed World
 GeoVax Labs, Inc. 19 Lake Park Drive Suite 3 Atlanta, GA 3 (678) 384-72 GOVX-B11: A Clade B HIV Vaccine for the Developed World Executive summary: GOVX-B11 is a Clade B HIV vaccine targeted for use in
GeoVax Labs, Inc. 19 Lake Park Drive Suite 3 Atlanta, GA 3 (678) 384-72 GOVX-B11: A Clade B HIV Vaccine for the Developed World Executive summary: GOVX-B11 is a Clade B HIV vaccine targeted for use in
Replicating measles-shiv vaccine induces long term preservation of central memory CD4 cells in the gut of macaques challenged with SHIV89.
 Replicating measles-shiv vaccine induces long term preservation of central memory CD4 cells in the gut of macaques challenged with SHIV89.6P Frédéric Tangy Viral Genomics and Vaccination Laboratory Measles
Replicating measles-shiv vaccine induces long term preservation of central memory CD4 cells in the gut of macaques challenged with SHIV89.6P Frédéric Tangy Viral Genomics and Vaccination Laboratory Measles
Optimizing Intracellular Flow Cytometry:
 Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors An encore presentation by Jurg Rohrer, PhD, BD Biosciences 10.26.10 Outline Introduction Cytokines
Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors An encore presentation by Jurg Rohrer, PhD, BD Biosciences 10.26.10 Outline Introduction Cytokines
In vitro human regulatory T cell suppression assay
 Human CD4 + CD25 + regulatory T cell isolation, in vitro suppression assay and analysis In vitro human regulatory T cell suppression assay Introduction Regulatory T (Treg) cells are a subpopulation of
Human CD4 + CD25 + regulatory T cell isolation, in vitro suppression assay and analysis In vitro human regulatory T cell suppression assay Introduction Regulatory T (Treg) cells are a subpopulation of
Why are validated immunogenicity assays important for HIV vaccine development?
 Why are validated immunogenicity assays important for HIV vaccine development? There is a need to compare immunogenicity of products in the pipeline, when similar or different in class when developed by
Why are validated immunogenicity assays important for HIV vaccine development? There is a need to compare immunogenicity of products in the pipeline, when similar or different in class when developed by
Received 19 September 2007/Accepted 21 November 2007
 JOURNAL OF VIROLOGY, Feb. 2008, p. 1723 1738 Vol. 82, No. 4 0022-538X/08/$08.00 0 doi:10.1128/jvi.02084-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Patterns of CD8 Immunodominance
JOURNAL OF VIROLOGY, Feb. 2008, p. 1723 1738 Vol. 82, No. 4 0022-538X/08/$08.00 0 doi:10.1128/jvi.02084-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Patterns of CD8 Immunodominance
Human Immunodeficiency Virus
 Human Immunodeficiency Virus Virion Genome Genes and proteins Viruses and hosts Diseases Distinctive characteristics Viruses and hosts Lentivirus from Latin lentis (slow), for slow progression of disease
Human Immunodeficiency Virus Virion Genome Genes and proteins Viruses and hosts Diseases Distinctive characteristics Viruses and hosts Lentivirus from Latin lentis (slow), for slow progression of disease
X/01/$ DOI: /JVI Copyright 2001, American Society for Microbiology. All Rights Reserved.
 JOURNAL OF VIROLOGY, Apr. 2001, p. 3753 3765 Vol. 75, No. 8 0022-538X/01/$04.00 0 DOI: 10.1128/JVI.75.8.3753 3765.2001 Copyright 2001, American Society for Microbiology. All Rights Reserved. Route of Simian
JOURNAL OF VIROLOGY, Apr. 2001, p. 3753 3765 Vol. 75, No. 8 0022-538X/01/$04.00 0 DOI: 10.1128/JVI.75.8.3753 3765.2001 Copyright 2001, American Society for Microbiology. All Rights Reserved. Route of Simian
DATA SHEET. Provided: 500 µl of 5.6 mm Tris HCl, 4.4 mm Tris base, 0.05% sodium azide 0.1 mm EDTA, 5 mg/liter calf thymus DNA.
 Viral Load DNA >> Standard PCR standard 0 Copies Catalog Number: 1122 Lot Number: 150298 Release Category: A Provided: 500 µl of 5.6 mm Tris HCl, 4.4 mm Tris base, 0.05% sodium azide 0.1 mm EDTA, 5 mg/liter
Viral Load DNA >> Standard PCR standard 0 Copies Catalog Number: 1122 Lot Number: 150298 Release Category: A Provided: 500 µl of 5.6 mm Tris HCl, 4.4 mm Tris base, 0.05% sodium azide 0.1 mm EDTA, 5 mg/liter
Imaging B Cell Follicles to Investigate HIV/SIV Persistence. Elizabeth Connick, M.D. University of Arizona May 8, 2017
 Imaging B Cell ollicles to Investigate HIV/SIV Persistence Elizabeth Connick, M.D. University of Arizona May 8, 2017 Most HIV Replication Occurs In Secondary Lymphoid Tissues Tenner-Racz K et al. Am J
Imaging B Cell ollicles to Investigate HIV/SIV Persistence Elizabeth Connick, M.D. University of Arizona May 8, 2017 Most HIV Replication Occurs In Secondary Lymphoid Tissues Tenner-Racz K et al. Am J
MedChem 401~ Retroviridae. Retroviridae
 MedChem 401~ Retroviridae Retroviruses plus-sense RNA genome (!8-10 kb) protein capsid lipid envelop envelope glycoproteins reverse transcriptase enzyme integrase enzyme protease enzyme Retroviridae The
MedChem 401~ Retroviridae Retroviruses plus-sense RNA genome (!8-10 kb) protein capsid lipid envelop envelope glycoproteins reverse transcriptase enzyme integrase enzyme protease enzyme Retroviridae The
Treatment with IL-7 Prevents the Decline of Circulating CD4 + T Cells during the Acute Phase of SIV Infection in Rhesus Macaques
 SUPPORTING INFORMATION FOR: Treatment with IL-7 Prevents the Decline of Circulating CD4 + T Cells during the Acute Phase of SIV Infection in Rhesus Macaques Lia Vassena, 1,2 Huiyi Miao, 1 Raffaello Cimbro,
SUPPORTING INFORMATION FOR: Treatment with IL-7 Prevents the Decline of Circulating CD4 + T Cells during the Acute Phase of SIV Infection in Rhesus Macaques Lia Vassena, 1,2 Huiyi Miao, 1 Raffaello Cimbro,
HIV 101: Fundamentals of HIV Infection
 HIV 101: Fundamentals of HIV Infection David H. Spach, MD Professor of Medicine University of Washington Seattle, Washington Learning Objectives After attending this presentation, learners will be able
HIV 101: Fundamentals of HIV Infection David H. Spach, MD Professor of Medicine University of Washington Seattle, Washington Learning Objectives After attending this presentation, learners will be able
SUPPLEMENTARY INFORMATION
 Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Low immune activation despite high levels of pathogenic HIV-1 results in long-term asymptomatic disease
 Low immune activation despite high levels of pathogenic HIV-1 results in long-term asymptomatic disease Shailesh K. Choudhary 1 *, Nienke Vrisekoop 2 *, Christine A. Jansen 2, Sigrid A. Otto 2, Hanneke
Low immune activation despite high levels of pathogenic HIV-1 results in long-term asymptomatic disease Shailesh K. Choudhary 1 *, Nienke Vrisekoop 2 *, Christine A. Jansen 2, Sigrid A. Otto 2, Hanneke
Supporting Information
 Supporting Information Hatziioannou et al. 10.1073/pnas.0812587106 SI Text Viral Constructs and Viral Stock Generation. To generate the HIV-1 constructs used throughout these studies, the env gene in an
Supporting Information Hatziioannou et al. 10.1073/pnas.0812587106 SI Text Viral Constructs and Viral Stock Generation. To generate the HIV-1 constructs used throughout these studies, the env gene in an
Optimizing Intracellular Flow Cytometry:
 Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors Presented by Jurg Rohrer, PhD, BD Biosciences 23-10780-00 Outline Introduction Cytokines Transcription
Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors Presented by Jurg Rohrer, PhD, BD Biosciences 23-10780-00 Outline Introduction Cytokines Transcription
A PROJECT ON HIV INTRODUCED BY. Abdul Wahab Ali Gabeen Mahmoud Kamal Singer
 A PROJECT ON HIV INTRODUCED BY Abdul Wahab Ali Gabeen Mahmoud Kamal Singer Introduction: Three groups of nations have been identified in which the epidemiology of HIV(Human Immunodeficiency Virus) varies:
A PROJECT ON HIV INTRODUCED BY Abdul Wahab Ali Gabeen Mahmoud Kamal Singer Introduction: Three groups of nations have been identified in which the epidemiology of HIV(Human Immunodeficiency Virus) varies:
Micropathology Ltd. University of Warwick Science Park, Venture Centre, Sir William Lyons Road, Coventry CV4 7EZ
 www.micropathology.com info@micropathology.com Micropathology Ltd Tel 24hrs: +44 (0) 24-76 323222 Fax / Ans: +44 (0) 24-76 - 323333 University of Warwick Science Park, Venture Centre, Sir William Lyons
www.micropathology.com info@micropathology.com Micropathology Ltd Tel 24hrs: +44 (0) 24-76 323222 Fax / Ans: +44 (0) 24-76 - 323333 University of Warwick Science Park, Venture Centre, Sir William Lyons
SUPPLEMENTARY INFORMATION
 ` SUPPLEMENTAL FIGURES doi:10.1038/nature10003 Supplemental Figure 1: RhCMV/SIV vectors establish and indefinitely maintain high frequency SIV-specific T cell responses in diverse tissues: The figure shows
` SUPPLEMENTAL FIGURES doi:10.1038/nature10003 Supplemental Figure 1: RhCMV/SIV vectors establish and indefinitely maintain high frequency SIV-specific T cell responses in diverse tissues: The figure shows
JAK3 inhibitor administration in vivo in chronically SIV Infected Rhesus Macaques
 JAK3 inhibitor administration in vivo in chronically SIV Infected Rhesus Macaques preferentially depletes NK Cells Ladawan Kowawisatsut 1 Kovit Pattanapanyasat 1 Aftab A. Ansari 2 1 Department of Immunology
JAK3 inhibitor administration in vivo in chronically SIV Infected Rhesus Macaques preferentially depletes NK Cells Ladawan Kowawisatsut 1 Kovit Pattanapanyasat 1 Aftab A. Ansari 2 1 Department of Immunology
Viral Reservoirs and anti-latency interventions in nonhuman primate models of SIV/SHIV infection
 Viral Reservoirs and anti-latency interventions in nonhuman primate models of SIV/SHIV infection Koen Van Rompay California National Primate Research Center University of California Davis Outline Introduction
Viral Reservoirs and anti-latency interventions in nonhuman primate models of SIV/SHIV infection Koen Van Rompay California National Primate Research Center University of California Davis Outline Introduction
The humoral immune responses to IBV proteins.
 The humoral immune responses to IBV proteins. E. Dan Heller and Rosa Meir The Hebrew University of Jerusalem, Israel COST FA1207 meeting WG2 + WG3, Budapest, Jan. 2015 1 IBV encodes four major structural
The humoral immune responses to IBV proteins. E. Dan Heller and Rosa Meir The Hebrew University of Jerusalem, Israel COST FA1207 meeting WG2 + WG3, Budapest, Jan. 2015 1 IBV encodes four major structural
MID-TERM EXAMINATION
 Epidemiology 227 May 2, 2007 MID-TERM EXAMINATION Select the best answer for the multiple choice questions. There are 75 questions and 11 pages on the examination. Each question will count one point. Notify
Epidemiology 227 May 2, 2007 MID-TERM EXAMINATION Select the best answer for the multiple choice questions. There are 75 questions and 11 pages on the examination. Each question will count one point. Notify
A Noninfectious Simian/Human Immunodeficiency Virus DNA Vaccine That Protects Macaques against AIDS
 JOURNAL OF VIROLOGY, Mar. 2005, p. 3419 3428 Vol. 79, No. 6 0022-538X/05/$08.00 0 doi:10.1128/jvi.79.6.3419 3428.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved. A Noninfectious
JOURNAL OF VIROLOGY, Mar. 2005, p. 3419 3428 Vol. 79, No. 6 0022-538X/05/$08.00 0 doi:10.1128/jvi.79.6.3419 3428.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved. A Noninfectious
PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human
 Anti-CD19-CAR transduced T-cell preparation PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human AB serum (Gemini) and 300 international units/ml IL-2 (Novartis). T cell proliferation
Anti-CD19-CAR transduced T-cell preparation PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human AB serum (Gemini) and 300 international units/ml IL-2 (Novartis). T cell proliferation
Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE)
 Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central
Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central
Sysmex Educational Enhancement and Development No
 SEED Haematology No 1 2015 Introduction to the basics of CD4 and HIV Viral Load Testing The purpose of this newsletter is to provide an introduction to the basics of the specific laboratory tests that
SEED Haematology No 1 2015 Introduction to the basics of CD4 and HIV Viral Load Testing The purpose of this newsletter is to provide an introduction to the basics of the specific laboratory tests that
Therapeutic strategies for immune reconstitution in acquired immunodeficiency syndrome
 30 1, 1, 2, 3 1. ( ), 201508; 2., 200040; 3., 200032 : ( AIDS) ( HIV) 20 90,,,,,, AIDS, CD4 + T ( CTL), HIV, : ; ; Therapeutic strategies for immune reconstitution in acquired immunodeficiency syndrome
30 1, 1, 2, 3 1. ( ), 201508; 2., 200040; 3., 200032 : ( AIDS) ( HIV) 20 90,,,,,, AIDS, CD4 + T ( CTL), HIV, : ; ; Therapeutic strategies for immune reconstitution in acquired immunodeficiency syndrome
Are we targeting the right HIV determinants?
 QuickTime et un décompresseur TIFF (non compressé) sont requis pour visionner cette image. AIDS Vaccine 2009 October 22 nd 2009 - Paris Are we targeting the right HIV determinants? Françoise BARRÉ-SINOUSSI
QuickTime et un décompresseur TIFF (non compressé) sont requis pour visionner cette image. AIDS Vaccine 2009 October 22 nd 2009 - Paris Are we targeting the right HIV determinants? Françoise BARRÉ-SINOUSSI
The Role of B Cell Follicles in HIV Replication and Persistence
 The Role of B Cell ollicles in HIV Replication and Persistence Elizabeth Connick, M.D. Professor of Medicine Chief, Division of Infectious Diseases University of Arizona July 17, 2016 IAS 2016 Towards
The Role of B Cell ollicles in HIV Replication and Persistence Elizabeth Connick, M.D. Professor of Medicine Chief, Division of Infectious Diseases University of Arizona July 17, 2016 IAS 2016 Towards
Application Information Bulletin: Human NK Cells Phenotypic characterizing of human Natural Killer (NK) cell populations in peripheral blood
 Application Information Bulletin: Human NK Cells Phenotypic characterizing of human Natural Killer (NK) cell populations in peripheral blood Christopher A Fraker, Ph.D., University of Miami - Miami, Florida
Application Information Bulletin: Human NK Cells Phenotypic characterizing of human Natural Killer (NK) cell populations in peripheral blood Christopher A Fraker, Ph.D., University of Miami - Miami, Florida
On an individual level. Time since infection. NEJM, April HIV-1 evolution in response to immune selection pressures
 HIV-1 evolution in response to immune selection pressures BISC 441 guest lecture Zabrina Brumme, Ph.D. Assistant Professor, Faculty of Health Sciences Simon Fraser University http://www3.niaid.nih.gov/topics/hivaids/understanding/biology/structure.htm
HIV-1 evolution in response to immune selection pressures BISC 441 guest lecture Zabrina Brumme, Ph.D. Assistant Professor, Faculty of Health Sciences Simon Fraser University http://www3.niaid.nih.gov/topics/hivaids/understanding/biology/structure.htm
HIV INFECTION: An Overview
 HIV INFECTION: An Overview UNIVERSITY OF PAPUA NEW GUINEA SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ
HIV INFECTION: An Overview UNIVERSITY OF PAPUA NEW GUINEA SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ
In vitro human regulatory T cell expansion
 - 1 - Human CD4 + CD25 + regulatory T cell isolation, Workflow in vitro expansion and analysis In vitro human regulatory T cell expansion Introduction Regulatory T (Treg) cells are a subpopulation of T
- 1 - Human CD4 + CD25 + regulatory T cell isolation, Workflow in vitro expansion and analysis In vitro human regulatory T cell expansion Introduction Regulatory T (Treg) cells are a subpopulation of T
Vaccination with Attenuated Simian Immunodeficiency Virus by DNA Inoculation
 JOURNAL OF VIROLOGY, Dec. 2001, p. 11930 11934 Vol. 75, No. 23 0022-538X/01/$04.00 0 DOI: 10.1128/JVI.75.23.11930 11934.2001 Copyright 2001, American Society for Microbiology. All Rights Reserved. Vaccination
JOURNAL OF VIROLOGY, Dec. 2001, p. 11930 11934 Vol. 75, No. 23 0022-538X/01/$04.00 0 DOI: 10.1128/JVI.75.23.11930 11934.2001 Copyright 2001, American Society for Microbiology. All Rights Reserved. Vaccination
5. Over the last ten years, the proportion of HIV-infected persons who are women has: a. Increased b. Decreased c. Remained about the same 1
 Epidemiology 227 April 24, 2009 MID-TERM EXAMINATION Select the best answer for the multiple choice questions. There are 60 questions and 9 pages on the examination. Each question will count one point.
Epidemiology 227 April 24, 2009 MID-TERM EXAMINATION Select the best answer for the multiple choice questions. There are 60 questions and 9 pages on the examination. Each question will count one point.
In vitro human regulatory T cell expansion
 - 1 - Human CD4 + CD25 + CD127 dim/- regulatory T cell Workflow isolation, in vitro expansion and analysis In vitro human regulatory T cell expansion Introduction Regulatory T (Treg) cells are a subpopulation
- 1 - Human CD4 + CD25 + CD127 dim/- regulatory T cell Workflow isolation, in vitro expansion and analysis In vitro human regulatory T cell expansion Introduction Regulatory T (Treg) cells are a subpopulation
Commercially available HLA Class II tetramers (Beckman Coulter) conjugated to
 Class II tetramer staining Commercially available HLA Class II tetramers (Beckman Coulter) conjugated to PE were combined with dominant HIV epitopes (DRB1*0101-DRFYKTLRAEQASQEV, DRB1*0301- PEKEVLVWKFDSRLAFHH,
Class II tetramer staining Commercially available HLA Class II tetramers (Beckman Coulter) conjugated to PE were combined with dominant HIV epitopes (DRB1*0101-DRFYKTLRAEQASQEV, DRB1*0301- PEKEVLVWKFDSRLAFHH,
Strategies for an HIV vaccine
 Strategies for an HIV vaccine Norman L. Letvin J Clin Invest. 2002;110(1):15-27. https://doi.org/10.1172/jci15985. Perspective The development of an HIV vaccine poses an unprecedented challenge to the
Strategies for an HIV vaccine Norman L. Letvin J Clin Invest. 2002;110(1):15-27. https://doi.org/10.1172/jci15985. Perspective The development of an HIV vaccine poses an unprecedented challenge to the
Micro 301 HIV/AIDS. Since its discovery 31 years ago 12/3/ Acquired Immunodeficiency Syndrome (AIDS) has killed >32 million people
 Micro 301 HIV/AIDS Shiu-Lok Hu hus@uw.edu December 3, 2012 Since its discovery 31 years ago Acquired Immunodeficiency Syndrome (AIDS) has killed >32 million people In 2011 34.0 million [31.4 35.9 million]
Micro 301 HIV/AIDS Shiu-Lok Hu hus@uw.edu December 3, 2012 Since its discovery 31 years ago Acquired Immunodeficiency Syndrome (AIDS) has killed >32 million people In 2011 34.0 million [31.4 35.9 million]
Cellular Immunity in Aging and HIV: Correlates of Protection. Immune Senescence
 Cellular Immunity in Aging and HIV: Correlates of Protection Janet E. McElhaney, MD Professor of Medicine Allan M. McGavin Chair in Research Geriatrics University of British Columbia Vancouver, BC and
Cellular Immunity in Aging and HIV: Correlates of Protection Janet E. McElhaney, MD Professor of Medicine Allan M. McGavin Chair in Research Geriatrics University of British Columbia Vancouver, BC and
HIV Immunopathogenesis. Modeling the Immune System May 2, 2007
 HIV Immunopathogenesis Modeling the Immune System May 2, 2007 Question 1 : Explain how HIV infects the host Zafer Iscan Yuanjian Wang Zufferey Abhishek Garg How does HIV infect the host? HIV infection
HIV Immunopathogenesis Modeling the Immune System May 2, 2007 Question 1 : Explain how HIV infects the host Zafer Iscan Yuanjian Wang Zufferey Abhishek Garg How does HIV infect the host? HIV infection
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
NIH Public Access Author Manuscript Nature. Author manuscript; available in PMC 2009 July 1.
 NIH Public Access Author Manuscript Published in final edited form as: Nature. 2009 January 1; 457(7225): 87 91. doi:10.1038/nature07469. Immune Control of an SIV Challenge by a T Cell-Based Vaccine in
NIH Public Access Author Manuscript Published in final edited form as: Nature. 2009 January 1; 457(7225): 87 91. doi:10.1038/nature07469. Immune Control of an SIV Challenge by a T Cell-Based Vaccine in
cure research HIV & AIDS
 Glossary of terms HIV & AIDS cure research Antiretroviral Therapy (ART) ART involves the use of several (usually a cocktail of three or more) antiretroviral drugs to halt HIV replication. ART drugs may
Glossary of terms HIV & AIDS cure research Antiretroviral Therapy (ART) ART involves the use of several (usually a cocktail of three or more) antiretroviral drugs to halt HIV replication. ART drugs may
Supplementary Data Table of Contents:
 Supplementary Data Table of Contents: - Supplementary Methods - Supplementary Figures S1(A-B) - Supplementary Figures S2 (A-B) - Supplementary Figures S3 - Supplementary Figures S4(A-B) - Supplementary
Supplementary Data Table of Contents: - Supplementary Methods - Supplementary Figures S1(A-B) - Supplementary Figures S2 (A-B) - Supplementary Figures S3 - Supplementary Figures S4(A-B) - Supplementary
David Verhoeven, Sumathi Sankaran, Melanie Silvey, and Satya Dandekar*
 JOURNAL OF VIROLOGY, Apr. 2008, p. 4016 4027 Vol. 82, No. 8 0022-538X/08/$08.00 0 doi:10.1128/jvi.02164-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Antiviral Therapy during
JOURNAL OF VIROLOGY, Apr. 2008, p. 4016 4027 Vol. 82, No. 8 0022-538X/08/$08.00 0 doi:10.1128/jvi.02164-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Antiviral Therapy during
Antibody-Dependent Cell-Mediated Cytotoxicity in Simian Immunodeficiency Virus-Infected Rhesus Monkeys
 JOURNAL OF VIROLOGY, July 2011, p. 6906 6912 Vol. 85, No. 14 0022-538X/11/$12.00 doi:10.1128/jvi.00326-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Antibody-Dependent Cell-Mediated
JOURNAL OF VIROLOGY, July 2011, p. 6906 6912 Vol. 85, No. 14 0022-538X/11/$12.00 doi:10.1128/jvi.00326-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Antibody-Dependent Cell-Mediated
3. Lymphocyte proliferation (fig. 15.4): Clones of responder cells and memory cells are derived from B cells and T cells.
 Chapter 15 Adaptive, Specific Immunity and Immunization* *Lecture notes are to be used as a study guide only and do not represent the comprehensive information you will need to know for the exams. Specific
Chapter 15 Adaptive, Specific Immunity and Immunization* *Lecture notes are to be used as a study guide only and do not represent the comprehensive information you will need to know for the exams. Specific
T Memory Stem Cells: A Long-term Reservoir for HIV-1
 Towards an HIV Cure Pre-Conference Symposium 20 & 21 July 2012 T Memory Stem Cells: A Long-term Reservoir for HIV-1 Maria J Buzon, PhD Ragon Institute of MGH, MIT and Harvard, Massachussetts General Hospital,
Towards an HIV Cure Pre-Conference Symposium 20 & 21 July 2012 T Memory Stem Cells: A Long-term Reservoir for HIV-1 Maria J Buzon, PhD Ragon Institute of MGH, MIT and Harvard, Massachussetts General Hospital,
Application of μmacs Streptavidin MicroBeads for the analysis of HIV-1 directly from patient plasma
 Excerpt from MACS&more Vol 8 1/2004 Application of μmacs Streptavidin MicroBeads for the analysis of HIV-1 directly from patient plasma L. Davis Lupo and Salvatore T. Butera HIV and Retrovirology Branch,
Excerpt from MACS&more Vol 8 1/2004 Application of μmacs Streptavidin MicroBeads for the analysis of HIV-1 directly from patient plasma L. Davis Lupo and Salvatore T. Butera HIV and Retrovirology Branch,
RAISON D ETRE OF THE IMMUNE SYSTEM:
 RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Acquired Immunity Innate immunity: (Antigen nonspecific) defense
RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Acquired Immunity Innate immunity: (Antigen nonspecific) defense
Supplementary Figures
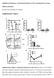 Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Activation of NK Cells by ADCC Antibodies and HIV Disease Progression
 RAPID COMMUNICATION Activation of NK Cells by ADCC Antibodies and HIV Disease Progression Amy W. Chung, BSc, PhD,* Marjon Navis, PhD,* Gamze Isitman, BSc,* Leia Wren, BSc,* Julie Silvers, RN, Janaki Amin,
RAPID COMMUNICATION Activation of NK Cells by ADCC Antibodies and HIV Disease Progression Amy W. Chung, BSc, PhD,* Marjon Navis, PhD,* Gamze Isitman, BSc,* Leia Wren, BSc,* Julie Silvers, RN, Janaki Amin,
DNA and Protein Vaccination Confers Protection Upon Mucosal Challenge with Heterologous SIVsmE660 (OA 10.04)
 DNA and Protein Vaccination Confers Protection Upon Mucosal Challenge with Heterologous SIVsmE660 (OA 10.04) Rashmi Jalah Human Retrovirus Pathogenesis Section, Vaccine Branch, CCR, National Cancer Institute
DNA and Protein Vaccination Confers Protection Upon Mucosal Challenge with Heterologous SIVsmE660 (OA 10.04) Rashmi Jalah Human Retrovirus Pathogenesis Section, Vaccine Branch, CCR, National Cancer Institute
Supplementary Figure 1. Gating strategy and quantification of integrated HIV DNA in sorted CD4 + T-cell subsets.
 Supplementary information HIV reservoir size and persistence are driven by T-cell survival and homeostatic proliferation. Chomont, N., M. El Far, P. Ancuta, L. Trautmann, F. A. Procopio, B. Yassine-Diab,
Supplementary information HIV reservoir size and persistence are driven by T-cell survival and homeostatic proliferation. Chomont, N., M. El Far, P. Ancuta, L. Trautmann, F. A. Procopio, B. Yassine-Diab,
MATERIALS AND METHODS. Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All
 MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
Supplementary Figure 1
 Supplementary Figure 1 Supplementary Figure 1: Cryopreservation alters CD62L expression by CD4 T cells. Freshly isolated (left) or cryopreserved PBMCs (right) were stained with the mix of antibodies described
Supplementary Figure 1 Supplementary Figure 1: Cryopreservation alters CD62L expression by CD4 T cells. Freshly isolated (left) or cryopreserved PBMCs (right) were stained with the mix of antibodies described
Supplementary Figure 1. ALVAC-protein vaccines and macaque immunization. (A) Maximum likelihood
 Supplementary Figure 1. ALVAC-protein vaccines and macaque immunization. (A) Maximum likelihood tree illustrating CRF01_AE gp120 protein sequence relationships between 107 Envs sampled in the RV144 trial
Supplementary Figure 1. ALVAC-protein vaccines and macaque immunization. (A) Maximum likelihood tree illustrating CRF01_AE gp120 protein sequence relationships between 107 Envs sampled in the RV144 trial
Zheng, BJ; Du, LY; Zhao, GY; Lin, YP; Sui, HY; Chan, C; Ma, S; Guan, Y; Yuen, KY. Citation Hong Kong Medical Journal, 2008, v. 14 suppl. 4, p.
 Title Studies of SARS virus vaccines Author(s) Zheng, BJ; Du, LY; Zhao, GY; Lin, YP; Sui, HY; Chan, C; Ma, S; Guan, Y; Yuen, KY Citation Hong Kong Medical Journal, 2008, v. 14 suppl. 4, p. 39-43 Issued
Title Studies of SARS virus vaccines Author(s) Zheng, BJ; Du, LY; Zhao, GY; Lin, YP; Sui, HY; Chan, C; Ma, S; Guan, Y; Yuen, KY Citation Hong Kong Medical Journal, 2008, v. 14 suppl. 4, p. 39-43 Issued
NOTES. Michael D. George,* David Verhoeven, Sumathi Sankaran, Tiffany Glavan, Elizabeth Reay, and Satya Dandekar
 CLINICAL AND VACCINE IMMUNOLOGY, Feb. 2009, p. 277 281 Vol. 16, No. 2 1556-6811/09/$08.00 0 doi:10.1128/cvi.00265-08 Copyright 2009, American Society for Microbiology. All Rights Reserved. NOTES Heightened
CLINICAL AND VACCINE IMMUNOLOGY, Feb. 2009, p. 277 281 Vol. 16, No. 2 1556-6811/09/$08.00 0 doi:10.1128/cvi.00265-08 Copyright 2009, American Society for Microbiology. All Rights Reserved. NOTES Heightened
IMMUNOLOGICAL MEMORY. CD4 T Follicular Helper Cells. Memory CD8 T Cell Differentiation
 IMMUNOLOGICAL MEMORY CD4 T Follicular Helper Cells Memory CD8 T Cell Differentiation CD4 T Cell Differentiation Bcl-6 T-bet GATA-3 ROR t Foxp3 CD4 T follicular helper (Tfh) cells FUNCTION Provide essential
IMMUNOLOGICAL MEMORY CD4 T Follicular Helper Cells Memory CD8 T Cell Differentiation CD4 T Cell Differentiation Bcl-6 T-bet GATA-3 ROR t Foxp3 CD4 T follicular helper (Tfh) cells FUNCTION Provide essential
Nef functions in BLT mice to enhance HIV-1 replication and deplete CD4 + CD8 + thymocytes
 Zou et al. Retrovirology 12, 9:44 RESEARCH Open Access Nef functions in BLT mice to enhance HIV-1 replication and deplete CD4 + CD8 + thymocytes Wei Zou 1, Paul W Denton 1, Richard L Watkins 1, John F
Zou et al. Retrovirology 12, 9:44 RESEARCH Open Access Nef functions in BLT mice to enhance HIV-1 replication and deplete CD4 + CD8 + thymocytes Wei Zou 1, Paul W Denton 1, Richard L Watkins 1, John F
Nature Medicine: doi: /nm.4322
 1 2 3 4 5 6 7 8 9 10 11 Supplementary Figure 1. Predicted RNA structure of 3 UTR and sequence alignment of deleted nucleotides. (a) Predicted RNA secondary structure of ZIKV 3 UTR. The stem-loop structure
1 2 3 4 5 6 7 8 9 10 11 Supplementary Figure 1. Predicted RNA structure of 3 UTR and sequence alignment of deleted nucleotides. (a) Predicted RNA secondary structure of ZIKV 3 UTR. The stem-loop structure
pplementary Figur Supplementary Figure 1. a.
 pplementary Figur Supplementary Figure 1. a. Quantification by RT-qPCR of YFV-17D and YFV-17D pol- (+) RNA in the supernatant of cultured Huh7.5 cells following viral RNA electroporation of respective
pplementary Figur Supplementary Figure 1. a. Quantification by RT-qPCR of YFV-17D and YFV-17D pol- (+) RNA in the supernatant of cultured Huh7.5 cells following viral RNA electroporation of respective
Feb 11, Gene Therapy. Sam K.P. Kung Immunology Rm 417 Apotex Center
 Gene Therapy Sam K.P. Kung Immunology Rm 417 Apotex Center Objectives: The concept of gene therapy, and an introduction of some of the currently used gene therapy vector Undesirable immune responses to
Gene Therapy Sam K.P. Kung Immunology Rm 417 Apotex Center Objectives: The concept of gene therapy, and an introduction of some of the currently used gene therapy vector Undesirable immune responses to
