Effect of aluminum on bone matrix inductive properties
|
|
|
- Beatrix Ellis
- 5 years ago
- Views:
Transcription
1 Kidney International, Vol. 38 (/990), PP Effect of aluminum on bone matrix inductive properties JIAN-MIN ZHU, WILLIAM HUFFER, and ALLEN C. ALFREY Departments of Medicine and Pathology, Denver V.A. Hospital, University of Colorado Medical Center, Denver, Colorado, USA, and Division of Endocrinology and Nephrology, Xian Medical University, Xian, People's Republic of China Effect of aluminum on bone matrix inductive properties. The effect of aluminum on the bone inductive properties of implanted bone matrix was studied in rats. After decalcification femur sections were placed in either 0.1 or 0.01 M AICI3 or a solution of similar ph without Al for 24 hours. Following 28 days of implantation in subcutaneous pouches the aluminum content was and 51 6 mg/kg in the matrix pretreated with 0.1 and 0.01 M AId3. At the same time period following implantation the matrix calcium content was and mmol/kg in the 0.1 and 0.01 M AId3 pretreated groups versus mmol/kg in the control group (P < 0.01). In the control group bone histology showed extensive osteoblastic and osteoclastic remodeling, tetracycline labeling and bone formation. In contrast all of these histological features were virtually absent in aluminum treated matrix. Aluminum-induced resistance of bone matrix to collagenase degradation and restoration of bone inductive properties with chelation suggests that aluminum forms intermolecular cross links between collagen fibrils. Aluminum-induced cross links of collagen fibrils and/or its effects on bone inductive proteins present in bone matrix could explain the mechanism by which aluminum induces osteomalacia. The association between aluminum and osteomalacia in humans with renal disease has been well established [IL In addition, aluminum causes osteomalacia in a number of different animal species including dogs, rats and pigs [2 4]. Aluminum has been shown to produce a number of effects which could alter bone formation. It has been shown in organ cultures that aluminum inhibits the synthesis of bone alkaline phosphatase and acid phosphatase, implying that aluminum may affect osteoblast and osteoclast function [5]. Furthermore, aluminum has been shown to cause a reduction in the number of osteoblasts and osteoclasts suggesting it could be directly toxic to these cells (6]. Other studies have found that aluminum has a direct effect on preventing the physical and chemical events leading to calcium-phosphate crystal formation [7]. Two features make aluminum associated osteomalacia unique. It is resistant to vitamin D treatment [8] and, unlike most other osteomalacic states, it occurs in the setting of hyperphosphatemia, mild hypercalcemia and an increased calcium X phosphate product [9]. These findings imply that the osteomalacia could result from an aluminum-induced alteration in bone matrix which renders it uncalcifiable. Consistent with this is histochemical staining which reveals that aluminum is Received for publication April 16, 1990 and in revised form July 23, 1990 Accepted for publication July 28, by the International Society of Nephrology 1141 present at the osteoid junction between calcified and noncalcified bone in aluminum-associated osteomalacia [10]. Historically aluminum has been used as a tanning agent because of its ability to cause intermolecular cross linkage of collagen fibrils [11]. Thus it would be expected that aluminum could also increase intermolecular cross linkage of bone collagen, bonding the aluminum to matrix, which could alter its ability to induce bone formation. The present study was undertaken to determine how pretreatment of decalcified bone matrix with aluminum would affect its bone inductive properties and its ability to calcify. Methods Preparation of bone matrix Bone matrix was prepared using a modification of the method described by Urist et al [121. Femurs were immediately removed from dead male Sprague-Dawley rats and sawed perpendicular to the shaft to obtain sections approximately 2.4 mm thick. The bone sections were cleaned of periosteal and endosteal tissues, washed several times in sterile distilled water and decalcified in 0.6 M HCI (I g tissue in 100 ml HCI) at 2 C for 48 hours. Under these conditions bone has been shown to be almost completly decalcified and to have minimal denaturation of bone matrix [12]. The bone was then removed from the acid and washed with sterile distilled water. After washing, the bone matrix was placed in 0.1 M or 0.01 M AId3 or M HCI for 24 hours at 2 C. The ph of the respective solutions was 3.6, 3.71 and 3.55 at the initiation of treatment and 3.67, 4.1 and 3.61 after the 24 hour incubation. In preparation for implantation the bone matrix was washed with sterile distilled water. Additional bone sections were decalcified and placed in either M HCI or 0.1 M AICI3 as described above. These sections were then placed in a solution containing either 20 moliml deferroxamine (DFO) or ethylenediamine tetracetic acid (EDTA) for an additional 24 hours. Implantation of bone matrix Male weanling Spraque-Dawley rats approximately four weeks old (weighing 80 to 100 g) were used for the recipients of the bone matrix. Two aluminum-treated matrix specimens and two control (HCI treated) specimens were implanted under sterile conditions into individual subcutaneous pouches (four) dissected into the ventral abdominal wall of each rat. The implants were removed at four and eight weeks following implantation. Matrix, untreated with aluminum, was implanted
2 1142 Zhu et a!: Aluminum effect on bone induction into four rats which received 1.5 mg/kg/day aluminum i.p. for 28 days following the implantation of matrix. Collagenase incubation Decalcified bone matrix was prepared as described above and placed in 0.1, 0.01, M Aid3 or M HCI at 2 C for 24 hours. The matrix was then washed, dried at room temperature and weighted. Each matrix specimen was placed in 4 ml of water containing 25 mg of collagenase (Worthington Biochemical Corporation, Freehodi, New Jersey, USA) for 15 hours at 37 C. The residual matrix was removed from the collagenase, air dried at room temperature for 48 hours and reweighed. In vitro nucleation of calcium-phosphate crystals A modification of the method described by Strates and Neuman [13] was used. The calcification solution consisted of 15 m barbital buffer, ph 7.4, 100 mm NaCI, 1.7 mm CaCl2 and 1.7 m potassium phosphate. Three to four mg samples of bone matrix pretreated with either 0.1 or 0.01 M Aid3 or M HCI were placed in the solution for 24 hours at 35 C. The specimens were then removed from the solution and analyzed for calcium as described below. Analytical procedures For aluminum and calcium determinations the bone matrix was dried to a constant weight at 105 C. The matrix was extracted with a saturated solution of EDTA at 25 C for three days. Calcium and aluminum determinations were performed by previously described methods [14, 15]. For histological studies rats with matrix implants were given tetracycline (16 mg/kg) five, three and one day(s) prior to removal of the implants. Following removal, the bone matrix was immediately placed into cold methanol. It was then embedded in glycol methacrylate for processing. The non-decalcified specimens were stained with either hematoxylin and eosin, acid fuschin or Von Kossa stain for routine histological studies or aurin tricarboxylic acid for aluminum. All results are given as mean I SD. Statistical comparisons were carried out with Student's f-test for two groups and analysis of variance for multiple group comparisons. Results The tissue aluminum in unimplanted matrix pretreated with 0.1 si Aid3 was , after 28 days of implantation and mg/kg after 56 days of implantation (Fig. 1). The tissue aluminum in unimplanted matrix pretreated with 0.01 M AICI3 was prior to implantation and 51 6 mg/kg after 28 days of implantation. In the matrix treated only with HCI aluminum was less than 2 mg/kg both before and after implantation. The tissue calcium content in unimplanted bone matrix treated with AId3 or HCI was less than I mmol/kg dry weight. Following 28 days of implantation the tissue calcium content was in the control tissue, in the tissue pretreated with 0.01 M AId3 and mmol/kg in the tissue pretreated with 0.1 M AId3 (P < 0.01 between all groups). Following 56 days of implantation the calcium was in the control tissue and in the tissue pretreated wth 0.1 M AICI3 as compared to mmol/kg in undecalcified normal rat bone < Time, days Fig. 1. Aluminum concentration in matrix exposed to 0.1 M AId3 before implantation (N = 4), and 28 (N 8) and 56 (N = 6) days following implantation. FIg. 2. Tetracycline labels (2 light lines on surface, arrows) in untreated matrix after 28-days of implantation. Histological examination of the control tissue following 28 and 56 days of implantation revealed extensive tetracycline labeling, bone formation and remodeling with numerous osteoblasts and osteoclasts (Figs. 2, 3). In contrast in the matrix pretreated with 0.1 M AId3 following both 28 and 56 days of implantation, there was almost total absence of bone formation as shown by no tetracycline labeling and little evidence of cellular activity (Fig. 4). Of further interest was the fact that the implanted matrix pretreated with 0.1 M AICI3 was virtually unchanged from its pre-implanted appearance. It had incited little if any tissue reaction and had undergone virtually no degradation. In contrast the untreated matrix had assumed the appearance of the implanted femur section prior to decalcification (Fig. 4). In the matrix pretreated with 0.01 M AICI3 and removed 28 days following implantation, there were islands of bone formation within the matrix but much less bone than in the control tissue. The control group showed no staining with the
3 Zhu et a!: Aluminum effect on bone induction g S I S. a Pt' 2 'I p 4'- ½ Fig. 4. Matrix treated with 0.1 si Aid3 (left) and control (right) after 28 days of implantation. There is no cellular activity or bone formation in the treated matrix Fig. 3. Osteoblastic and osteoclastic activity with bone formation and osteoid deposition in untreated matrix implanted for 28 days. Abbreviations are: Ost, osteoid; Osb, osteoblast; Cb, calcified bone; Oci, osteoclast; M, marrow. aluminum stain, whereas, the aluminum group showed diffuse staining of the entire matrix. Following chelation with DFO and EDTA the bone matrix aluminum was less than 3 mg/kg in both control and aluminum pre-treated matrix before and after implantation. In the DFO groups, calcium content of the implant was versus mmollkg in the aluminum pre-treated and control tissues (P = NS). Similarly in the EDTA groups there was no difference between calcium content of aluminum pre-treated and control matrix ( vs mmollkg, P = NS). Bone matrix aluminum prior to collagenase treatment was , and mg/kg in the three groups pretreated with aluminum (0.1, 0.01 and M AId3). The percent of bone matrix which had not undergone degradation after collagenase treatment was 93 4, 70 18, 33 22% in the three aluminum groups (Fig. 5) as compared to 15 8% in the controls (P < 0.05 between all groups). In contrast to the in vivo results, pretreatment of bone matrix with aluminum enhanced the calcification resulting in vitro from I ilii A Fig. 5. Percent of matrix remaining after 15 hours of incubation with collagenase in control matrix treated with HCI and matrix treated with M, 0.01 M and 0.1 MAId3 (each group N = 4). a metastable solution. The tissue calcium content was and 34 5 mmol/kg in matrix pretreated with 0.1 and 0.01 M AId3, respectively (P < 0.01) as compared to 14 2 mmol/kg in the control matrix (P <0.01). To determine the effect of extracellular aluminum on bone induction, bone matrix was implanted into four rats which received i.p. aluminum injections daily over a 28 day period following implantation. Plasma aluminum levels were pg/liter six hours after aluminum injections as compared to 5 1 tgiliter in controls. At the end of the study matrix calcium was mmol/kg in the aluminum treated group as compared to mmollkg in the controls (P = NS). Discussion These studies show that aluminum treatment of decalcified bone matrix markedly inhibits its bone inductive properties. In addition, aluminum treatment was found to increase bone
4 1144 Zhu et a!: Aluminum effect on bone induction matrix resistance to degradation by collagenase and enhance its in vitro calcification from a metastable solution. An increased resistance of collagen to collagenase degradation has been attributed to increased maturity and cross linking [16]. In this case it seems highly likely that this resulted from increased cross linkage caused by the aluminum. Additional support for aluminum cross linkage of collagen is the finding that the aluminum pre-treated bone matrix was virtually total intact after 56 days of implantation. It has previously been shown that cross linked collagen is not only resistant to collagenase degradation in vitro but it is also resistant in vivo to degradation [17]. Mineral tannage has been extensively used in the tanning industry. While chrome has been the most widely used element, aluminum and zirconium have also been employed [17]. In this form of tannage cross links are through chrome or aluminum coordination complexes containing hydroxol, oxo, phosphate or sulfate bridges into which carboxyl groups on collagen enter forming the cross links. This provides the most hydrothermally stable and commercially important tannages [18]. In further support for aluminum-inhibiting bone matrix inductive properties by cross linkage of collagen fibrils is the fact that this inhibitory property is completely reversed by the removal of aluminum from the matrix by chelation. This is a well known method of detanning metal tannages [11]. Additional evidence for the chemical bonding of aluminum in bone matrix is the rather constant uptake of aluminum by matrix from solutions containing various concentrations of aluminum. Further support comes from the finding that at least one compartment of aluminum in matrix is very stable as supported by the minimal change in matrix aluminum concentration which occurred between 28 and 56 days of implantation. The fact that aluminum was found to enhance the calcifiability of matrix from an in vitro metastable solution is additional evidence that aluminum alters the structure of bone collagen probably through increasing cross linkage. Increased cross linking may predispose collagen to develop dystrophic or metastatic calcification. This is suggested by the fact that cross linking collagen with glutaraldehyde predisposes pericardial bioprosthetic heart valves to calcify [19]. Bovine pericardium does not have bone inductive properties; therefore, its calcification would appear to be of the dystrophic or metastic type. However, aldehyde cross links are different from those formed by minerals. Aldehyde cross linking results from the formation of stable covalent cross links associated with a relatively limited number of amine groups available on collagen [17]. Irrespective of aluminum's effect on promoting dystrophic calcification of collagen, which might account for most of the calcium present in matrix treated with 0.1 M AId3, it would appear that its major effect on bone matrix was the eradication of its bone inductive capabilities. Reddi, Wientroub and Muthukumaran have extensively studied the bone inductive properties of decalcified bone matrix [20]. Normally within the first week following implantation there is vascular invasion and the appearance of chrondroblasts and chrondrocytes with cartilage formation in the implant and subsequent calcification of the cartilage. In a matter of days this is followed by the presences of osteoblasts and osteoclasts with extensive bone formation, remodeling and dissolution of the implanted matrix. In the control implants the expected extensive bone formation and remodeling was observed. However, in the aluminum treated matrix there was virtually no cellular activity and very little bone formation in the implant. This would suggest that aluminum treatment of matrix prevented calcification by suppressing matrix bone inductive ability and cellular involvement in this process. This is also supported by the vitro data showing that aluminum enhances the ability of collagen to calcify which tends to exclude a basic alteration in collagen which prevents its calcification. This loss of inductive ability of bone matrix could also explain why there is a decrease number and function of osteoblasts and osteoclasts in organ cultures which have been treated with aluminum. The presence of aluminum in the matrix is required for this inhibitory effect since chelation of aluminum restores the bone inductive properties. This inhibitory effect could result from aluminum cross links of the collagen fibrils. However, it has been suggested that collagen is not necessary for the bone inductive properties of matrix [21]. Somewhat against this is the fact that the osteo-inductive components of bone have been shown to be ineffective in causing bone formation in tendons, also type I collagen [22]. Because of this, it has been suggested that bone collagen might be a more suitable substratum for anchorage-dependent proliferation and differentiation of cells capable of bone formation [221. This would be consistent with the finding in this study showing that bone formation in the implanted matrix resembled the implant prior to being decalcifled. It is possible that aluminum-induced cross links of collagen could either immobilize the bone inductive proteins or simply the presence of aluminum in matrix could somehow have a direct effect on inhibiting bone induction. In further support that aluminum bound in matrix is responsible for inhibiting bone induction is the fact that i.p. injected aluminum, which increased plasma aluminum and presumably extracellular fluid aluminum, had no effect on the bone inductive property of matrix. Irrespective of the mechanism by which aluminum inhibits bone induction it requires only a small amount, less than 50 mg aluminumlkg matrix, to suppress bone formation. Whole bone aluminum obtained from uremic patients with osteomalacia typically have much higher bone aluminum levels than this [23]. In addition, the bone aluminum in osteomalacic bone tends to be concentrated in the osteoid, making it even more likely that it could alter the osteoid structure and its ability to promote bone formation. Acknowledgments This study was supported by V.A. research funding. Dr. Zhu was partially supported by a grant from Xian Medical University, Xian, PRC. This work was presented in part at the American Society of Nephrology annual meeting in 1989, and published in Kidney mt 37:1990. Reprint requests to Allen C. Alfrey, M.D., Denver V.A. Hospital, 1055 Clerpnont Street, Denver, Colorado 80220, USA. References I. WARD MK, FEEST TO, ELLIS HA, PARKINSON IS, Kniut DNS: Osteomalacia dialysis osteodystrophy: Evidence for a water borne aetiological agent; probably aluminum. Lancet i: , CHAN YL, ALFREY AC, POSEN S. LIs5NER D, HILLS E, DUNSTAN CR, EVANS RA: The effect of aluminum on normal and uremic rats:
5 Zhu et a!: Aluminum effect on bone induction 1145 Tissue distribution, vitamin D metabolites and quantitative bone histology. CaIcif Tiss mt 35: , GOODMAN WG, HENRY DA, H0R5T R, NUDELMAN RK, ALFREY AC, COBURN JW: Parenteral aluminum administration in the dog. II. Induction of osteomalacia and effect on vitamin D metabolites. Kidney mt 25: , SEDMAN AB, ALFREY AC, MILLER NL, GOODMAN WG: Tissue and cellular basis for impaired bone formation in aluminum-related osteomalacia in the pig. J Gun Invest 79:86 92, DRUEKE T, LIEBERHERR M, COURNOT G: Pathophysiology of aluminum induced bone disease. Contr Nephrol 64: , LIEBERHERR M, GROSSE B, COURNOT 0, THIL CL, BALSAN S: In vitro effects of aluminum on bone phosphatases: A possible interaction with bpth and vitamin D3 metabolites. Calcif Tiss In! 34: , MEYER JL, THOMAS WC: Aluminum and aluminum complexes. Effect on calcium phosphate precipitation. Kidney mt 29:S20 S23, HODSMAN AB, SHERRARD Di, WONG EGC, BRICKMAN AS, LEE DBN, ALFREY AC, SINGER FR, NORMAN AW, COBURN JW: Vitamin D resistant osteomalacia in hemodialysis patients lacking secondary hyperparathyroidism. Ann Intern Med 94: , HODSMAN AB, SHERRARD Di, ALFREY AC, OTT 5, BRICKMAN AS, MILLER N, MALONEY N, COBURN JW: Bone aluminum and histomorphometric features of renal osteodystrophy. J C/in Endocrinol Metab 54: , MALONEY NA, OTT SM, ALFREY AC, MILLER NL, SHERRARD Di: Histological quanitation of aluminum in iliac bone from patients with renal failure. J Lab C/in Med 99: , HARLAN iw, FEAIRHELLER SH: Chemistry of cross-linking of collagen during tanning, in Protein Cross/inking Biochemical and Molecular Aspects, edited by M. FRIEDMAN, New York, Plenum Press, 1977, p URIST MR. DOWELL TA, HAY PH, STRATES BS: Inductive substrates for bone formation. C/in Orthopaedics Related Res 59:59 96, STRATES BS, NEUMAN WF: On the mechanism of calcification. Proc Soc Exp Biol Med 97: , ALFREY AC, MILLER NL: Bone magnesium pools in uremia. J C/in Invest 52: , LEGENDRE GR, ALFREY AC: Measuring picogram amounts of aluminum in biological tissue by flameless atomic absorption analysis of a chelate. C/in Chem 22:53 56, HARRIS ED, FARRELL ME: Resistance to collagenase: A characteristic of collagen fibrils cross-linked by formaldehyde. Biochimica et Biophysica ACTA 278: , YANNAS JR. BURKE if, HUANG C, GORDON PL: Correlation of in vivo collagen degradation rate with in vitro measurements. J Biomed Mater Res 9: , HEIDEMANN E: The chemistry of tanning, in Collagen, (vol III, Biotechnology), edited by ME NIMNI, Boca Raton, CRC Press, Inc., 1988, p GOLOMB 0, SCHOEN Fi, SMITH MS. LINDEN i, DixoN, M, LEVY, Ri: The role of glutaraldehyde-induced cross-links in calcification of bovine pericardium used in cardiac valve bioprostheses. Am J Pathol 127: , REDDI AH, WIENTROUB S, MUTHUKUMARAN i: Biological principles of bone induction. Orthopedic C/in N Am 18: , URIST MR. DELANGE Ri, FINERMAN GAM: Bone cell differentiation and growth factors. Science 220: , SAMPATH TK, REDDI AH: Dissociative extraction and reconstitution of extracellular matrix components involved in local bone differentiation. Proc NatI Acad Sci USA 78: , ALFREY AC, HEGG A, CRASWELL P: Metabolism and toxicity of aluminum in renal failure. Am J C/in Nutr 33: , 1980
Bone histologic response to deferoxamine in aluminum related bone disease
 Kidney International, Vol. 31 (1987), pp. 1344 135 CLINICAL INVESTIGATION Bone histologic response to deferoxamine in aluminum related bone disease DENNIS L. ANDRESS, HENRY G. NEBEKER, SUSAN M. OTT, DAVID
Kidney International, Vol. 31 (1987), pp. 1344 135 CLINICAL INVESTIGATION Bone histologic response to deferoxamine in aluminum related bone disease DENNIS L. ANDRESS, HENRY G. NEBEKER, SUSAN M. OTT, DAVID
Frequency of Metabolic Bone Disease in Haemodialysis Patients
 Frequency of Metabolic Bone Disease in Haemodialysis Patients Pages with reference to book, From 83 To 86 Rizwan Hussain, Arshad Ahmed, Abdul Salam Soomro, Saeed Hassan Chishty, Syed Ali Jaffar Naqvi (
Frequency of Metabolic Bone Disease in Haemodialysis Patients Pages with reference to book, From 83 To 86 Rizwan Hussain, Arshad Ahmed, Abdul Salam Soomro, Saeed Hassan Chishty, Syed Ali Jaffar Naqvi (
Kobe University Repository : Kernel
 Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
Case 4 Generalised bone pain
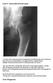 Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
BONE TISSUE. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
CKD-Mineral Bone Disorder (MBD) Pathogenesis of Metabolic Bone Disease. Grants: NIH, Abbott, Amgen, OPKO, Shire
 Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Module 2:! Functional Musculoskeletal Anatomy A! Semester 1! !!! !!!! Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb!
 Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience
 Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience Michael Chan, Renal Dietitian Regina Qu Appelle Health Region BC Nephrology Days There is a strong association among
Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience Michael Chan, Renal Dietitian Regina Qu Appelle Health Region BC Nephrology Days There is a strong association among
Secondary Hyperparathyroidism: Where are we now?
 Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
Metabolic Bone Disease (Past, Present and Future Challenges in the Management)
 Metabolic Bone Disease 871 151 Metabolic Bone Disease (Past, Present and Future Challenges in the Management) SNA RIZVI INTRODUCTION The past 40 years have seen some important historical events leading
Metabolic Bone Disease 871 151 Metabolic Bone Disease (Past, Present and Future Challenges in the Management) SNA RIZVI INTRODUCTION The past 40 years have seen some important historical events leading
Biology. Dr. Khalida Ibrahim
 Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
TRACP & ALP double-stain Kit
 Table of Content I. Description... 2 II. Introduction... 2 III. Principles... 2 IV. Kit components... 3 V. Storage... 3 VI. Preparation of reagents... 3 VII. Methods... 4-7 Cell fixation... 4 Activity
Table of Content I. Description... 2 II. Introduction... 2 III. Principles... 2 IV. Kit components... 3 V. Storage... 3 VI. Preparation of reagents... 3 VII. Methods... 4-7 Cell fixation... 4 Activity
For more information about how to cite these materials visit
 Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
BONE HISTOLOGY SLIDE PRESENTATION
 BONE HISTOLOGY SLIDE PRESENTATION PRESENTED BY: SKELETECH, INC. Clients and Friends: SkeleTech invites you to use these complimentary images for your own presentations or as teaching slides for bone biology.
BONE HISTOLOGY SLIDE PRESENTATION PRESENTED BY: SKELETECH, INC. Clients and Friends: SkeleTech invites you to use these complimentary images for your own presentations or as teaching slides for bone biology.
The relief of bone pain in primary biliary cirrhosis with calcium infusions
 Gut, 1974, 15, 788-793 The relief of bone pain in primary biliary cirrhosis with calcium infusions A. B. AJDUKIEWICZ, J. E. AGNEW, P. D. BYERS, M. R. WILLS1, AND SHEILA SHERLOCK From the Departments of
Gut, 1974, 15, 788-793 The relief of bone pain in primary biliary cirrhosis with calcium infusions A. B. AJDUKIEWICZ, J. E. AGNEW, P. D. BYERS, M. R. WILLS1, AND SHEILA SHERLOCK From the Departments of
Bone Disorders in CKD
 Osteoporosis in Dialysis Patients Challenges in Management David M. Klachko MD FACP Professor Emeritus of Medicine University of Missouri-Columbia Bone Disorders in CKD PTH-mediated high-turnover (osteitis
Osteoporosis in Dialysis Patients Challenges in Management David M. Klachko MD FACP Professor Emeritus of Medicine University of Missouri-Columbia Bone Disorders in CKD PTH-mediated high-turnover (osteitis
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
Brief Communication. Alkaline Phosphatase Activity of Glutaraldehyde-Treated Bovine Pericardium Used in Bioprosthetic Cardiac Valves
 844 Brief Communication Alkaline Phosphatase Activity of Glutaraldehyde-Treated Bovine Pericardium Used in Bioprosthetic Cardiac Valves Anthony R. Maranto and Frederick J. Schoen Bioprosthetic valves fail
844 Brief Communication Alkaline Phosphatase Activity of Glutaraldehyde-Treated Bovine Pericardium Used in Bioprosthetic Cardiac Valves Anthony R. Maranto and Frederick J. Schoen Bioprosthetic valves fail
Synergistic Inhibition of Calcification of Porcine Aortic Root with Preincubation in FeCl 3 and a-amino Oleic Acid in a Rat Subdermal Model
 Synergistic Inhibition of Calcification of Porcine Aortic Root with Preincubation in FeCl 3 and a-amino Oleic Acid in a Rat Subdermal Model Weiliam Chen, 1 Frederick J. Schoen, 2 David J. Myers, 3 Robert
Synergistic Inhibition of Calcification of Porcine Aortic Root with Preincubation in FeCl 3 and a-amino Oleic Acid in a Rat Subdermal Model Weiliam Chen, 1 Frederick J. Schoen, 2 David J. Myers, 3 Robert
Decalcification and Clearing of Bone eg. Fibula. Salem Kharwa Clinical Anatomy Medical School
 Decalcification and Clearing of Bone eg. Fibula Salem Kharwa Clinical Anatomy Medical School Bone composition Bone consists of cells (osteocytes) surrounded by a calcified matrix containing collagen fibres.
Decalcification and Clearing of Bone eg. Fibula Salem Kharwa Clinical Anatomy Medical School Bone composition Bone consists of cells (osteocytes) surrounded by a calcified matrix containing collagen fibres.
The Skeletal System:Bone Tissue
 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH
 PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
Renal Osteodystrophy. Chapter 6. I. Introduction. Classification of Bone Disease. Eric W. Young
 Chapter 6 Renal Osteodystrophy Eric W. Young I. Introduction Renal osteodystrophy refers to bone disease that occurs in patients with kidney disease. Bone disease occurs across the full spectrum of kidney
Chapter 6 Renal Osteodystrophy Eric W. Young I. Introduction Renal osteodystrophy refers to bone disease that occurs in patients with kidney disease. Bone disease occurs across the full spectrum of kidney
A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication
 Kidney International, Vol. 53 (1998), pp. 223 227 A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication JOHN E. ANTONSEN, DONALD
Kidney International, Vol. 53 (1998), pp. 223 227 A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication JOHN E. ANTONSEN, DONALD
Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients. Int.J.Curr.Res.Aca.Rev.2016; 4(11):
 Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients Seyed Seifollah Beladi Mousavi 1, Arman Shahriari 2 and Fatemeh Roumi 3 * 1 Department of Nephrology,
Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients Seyed Seifollah Beladi Mousavi 1, Arman Shahriari 2 and Fatemeh Roumi 3 * 1 Department of Nephrology,
Normal kidneys filter large amounts of organic
 ORIGINAL ARTICLE - NEPHROLOGY Effect Of Lanthanum Carbonate vs Calcium Acetate As A Phosphate Binder In Stage 3-4 CKD- Treat To Goal Study K.S. Sajeev Kumar (1), M K Mohandas (1), Ramdas Pisharody (1),
ORIGINAL ARTICLE - NEPHROLOGY Effect Of Lanthanum Carbonate vs Calcium Acetate As A Phosphate Binder In Stage 3-4 CKD- Treat To Goal Study K.S. Sajeev Kumar (1), M K Mohandas (1), Ramdas Pisharody (1),
Evidence for a Serum Factor That Initiates the Re-calcification of Demineralized Bone* S
 THE JOURNAL OF BIOLOGICAL CHEMISTRY Vol. 279, No. 18, Issue of April 30, pp. 19169 19180, 2004 2004 by The American Society for Biochemistry and Molecular Biology, Inc. Printed in U.S.A. Evidence for a
THE JOURNAL OF BIOLOGICAL CHEMISTRY Vol. 279, No. 18, Issue of April 30, pp. 19169 19180, 2004 2004 by The American Society for Biochemistry and Molecular Biology, Inc. Printed in U.S.A. Evidence for a
Department of Anatomy, Glasgow University
 THE UPTAKE OF LABELLED SULPHATE INJECTED INTO THE HOST ANIMAL BY CARTILAGE HOMOGRAFTS By G. M. WYBURN, D.Sc., F.R.F.P.S.G., and P. BACSICH, D.Sc., M.D. Department of Anatomy, Glasgow University INTRODUCTION
THE UPTAKE OF LABELLED SULPHATE INJECTED INTO THE HOST ANIMAL BY CARTILAGE HOMOGRAFTS By G. M. WYBURN, D.Sc., F.R.F.P.S.G., and P. BACSICH, D.Sc., M.D. Department of Anatomy, Glasgow University INTRODUCTION
MEDICAL JOURNAL ORIGINAL ARTICLE INTRODUCTION
 1790 SÃO PAULO MEDICAL JOURNAL ORIGINAL ARTICLE Maria Eugênia Leite Duarte, Ana Lúcia Passos Peixoto, Andréa da Silva Pacheco, Angela Vieira Peixoto, Rodrigo Dezerto Rodriguez, Jocemir Ronaldo Lugon, Elisa
1790 SÃO PAULO MEDICAL JOURNAL ORIGINAL ARTICLE Maria Eugênia Leite Duarte, Ana Lúcia Passos Peixoto, Andréa da Silva Pacheco, Angela Vieira Peixoto, Rodrigo Dezerto Rodriguez, Jocemir Ronaldo Lugon, Elisa
Reversal of adynamic bone disease by lowering of dialysate calcium
 http://www.kidney-international.org & 26 International Society of Nephrology original article Reversal of adynamic bone disease by lowering of dialysate calcium A Haris 1, DJ Sherrard 2 and G Hercz 3 1
http://www.kidney-international.org & 26 International Society of Nephrology original article Reversal of adynamic bone disease by lowering of dialysate calcium A Haris 1, DJ Sherrard 2 and G Hercz 3 1
Comparative Animal Study of OssiMend and Healos 13,14
 Comparative Animal Study of OssiMend and Healos 13,14 Objective This study was conducted to evaluate the use of OssiMend as compared with Healos in combination with autologous bone marrow as a bone grafting
Comparative Animal Study of OssiMend and Healos 13,14 Objective This study was conducted to evaluate the use of OssiMend as compared with Healos in combination with autologous bone marrow as a bone grafting
Regulation of the skeletal mass through the life span
 Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
17. CALCIUM AND PHOSPHOROUS METABOLISM. Calcium. Role of calcium ROLE OF CALCIUM STORAGE. Calcium movement
 17. CALCIUM AND PHOSPHOROUS METABOLISM Many physiological processes are regulated directly or indirectly by calcium. Furthermore, the main physical structure of vertebrates and other species depend on
17. CALCIUM AND PHOSPHOROUS METABOLISM Many physiological processes are regulated directly or indirectly by calcium. Furthermore, the main physical structure of vertebrates and other species depend on
The impact of improved phosphorus control: use of sevelamer hydrochloride in patients with chronic renal failure
 Nephrol Dial Transplant (2002) 17: 340 345 The impact of improved phosphorus control: use of sevelamer hydrochloride in patients with chronic renal failure Naseem Amin Genzyme Corporation, Cambridge, MA,
Nephrol Dial Transplant (2002) 17: 340 345 The impact of improved phosphorus control: use of sevelamer hydrochloride in patients with chronic renal failure Naseem Amin Genzyme Corporation, Cambridge, MA,
Therapeutic golas in the treatment of CKD-MBD
 Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
20. CALCIUM AND PHOSPHOROUS METABOLISM
 20. CALCIUM AND PHOSPHOROUS METABOLISM Many physiological processes are regulated directly or indirectly by calcium. Furthermore, the main physical structure of vertebrates and other species depend on
20. CALCIUM AND PHOSPHOROUS METABOLISM Many physiological processes are regulated directly or indirectly by calcium. Furthermore, the main physical structure of vertebrates and other species depend on
Induction of De Novo Bone Formation in the Beagle A Novel Effect of Aluminum
 Induction of De Novo Bone Formation in the Beagle A Novel Effect of Aluminum L. D. Quarles, H. J. Gitelman,* and M. K. Drezner Departments ofmedicine, Physiology, and Pathology, Duke University Medical
Induction of De Novo Bone Formation in the Beagle A Novel Effect of Aluminum L. D. Quarles, H. J. Gitelman,* and M. K. Drezner Departments ofmedicine, Physiology, and Pathology, Duke University Medical
Ca, Mg metabolism, bone diseases. Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary
 Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues
 An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
OSTEOMALACIA UPDATE. Nothing to Disclose. Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco
 OSTEOMALACIA UPDATE Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco Nothing to Disclose 1 Case History 59 YO WM referred for evaluation of diffuse
OSTEOMALACIA UPDATE Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco Nothing to Disclose 1 Case History 59 YO WM referred for evaluation of diffuse
FORMATION OF BONE. Intramembranous Ossification. Bone-Lec-10-Prof.Dr.Adnan Albideri
 FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
Determination of Calcium in Milk
 Determination of Calcium in Milk Calcium an important mineral for the body Calcium is an important component of a healthy diet and a mineral necessary for life. Calcium is a mineral that people need to
Determination of Calcium in Milk Calcium an important mineral for the body Calcium is an important component of a healthy diet and a mineral necessary for life. Calcium is a mineral that people need to
Bone Markers and Vascular Calcification in CKD-MBD
 Bone Markers and Vascular Calcification in CKD-MBD Pierre Delanaye, MD, PhD Department of Nephrology, Dialysis, Transplantation CHU Sart Tilman University of Liège BELGIUM Bone Markers and Vascular Calcification
Bone Markers and Vascular Calcification in CKD-MBD Pierre Delanaye, MD, PhD Department of Nephrology, Dialysis, Transplantation CHU Sart Tilman University of Liège BELGIUM Bone Markers and Vascular Calcification
A Novel Murine Model Of Adynamic Bone Disease (ABD)
 A Novel Murine Model Of Adynamic Bone Disease (ABD) Adeline H. Ng 1,2, Thomas L. Willett, PhD 2,1, Benjamin A. Alman 3,1, Marc D. Grynpas 1,2. 1 University of Toronto, Toronto, ON, Canada, 2 Samuel Lunenfeld
A Novel Murine Model Of Adynamic Bone Disease (ABD) Adeline H. Ng 1,2, Thomas L. Willett, PhD 2,1, Benjamin A. Alman 3,1, Marc D. Grynpas 1,2. 1 University of Toronto, Toronto, ON, Canada, 2 Samuel Lunenfeld
Biochemistry #01 Bone Formation Dr. Nabil Bashir Farah Banyhany
 Biochemistry #01 Bone Formation Dr. Nabil Bashir Farah Banyhany Greetings This lecture is quite detailed, but I promise you will make it through, it just requires your 100% FOCUS! Let s begin. Today s
Biochemistry #01 Bone Formation Dr. Nabil Bashir Farah Banyhany Greetings This lecture is quite detailed, but I promise you will make it through, it just requires your 100% FOCUS! Let s begin. Today s
Aldehyde reduction in a novel pericardial tissue reduces calcification using rabbit intramuscular model
 J Mater Sci: Mater Med (2017) 28:16 DOI 10.1007/s10856-016-5829-8 CLINICAL APPLICATIONS OF BIOMATERIALS Original Research Aldehyde reduction in a novel pericardial tissue reduces calcification using rabbit
J Mater Sci: Mater Med (2017) 28:16 DOI 10.1007/s10856-016-5829-8 CLINICAL APPLICATIONS OF BIOMATERIALS Original Research Aldehyde reduction in a novel pericardial tissue reduces calcification using rabbit
Effect of lanthanum carbonate and calcium acetate in the treatment of hyperphosphatemia in patients of chronic kidney disease
 Research Article Effect of lanthanum and calcium acetate in the treatment of hyperphosphatemia in patients of chronic kidney disease P. Thomas Scaria, Reneega Gangadhar 1, Ramdas Pisharody 2 ABSTRACT Departments
Research Article Effect of lanthanum and calcium acetate in the treatment of hyperphosphatemia in patients of chronic kidney disease P. Thomas Scaria, Reneega Gangadhar 1, Ramdas Pisharody 2 ABSTRACT Departments
Osseous Tissue and Bone Structure
 C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
Tissue Reaction to Root Canal Filling Material Embedded Subcutaneously in Rats
 11 Chapter 2 Tissue Reaction to Root Canal Filling Material Embedded Subcutaneously in Rats Takanaga Ochiai Keisuke Nakano Hiromasa Hasegawa Toshiyuki Kawakami Abstract The reaction of subcutaneous connective
11 Chapter 2 Tissue Reaction to Root Canal Filling Material Embedded Subcutaneously in Rats Takanaga Ochiai Keisuke Nakano Hiromasa Hasegawa Toshiyuki Kawakami Abstract The reaction of subcutaneous connective
CHAPTER 6 LECTURE OUTLINE
 CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
Functions of the Skeletal System. Chapter 6: Osseous Tissue and Bone Structure. Classification of Bones. Bone Shapes
 Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Secondary hyperparathyroidism an Update on Pathophysiology and Treatment
 Secondary hyperparathyroidism an Update on Pathophysiology and Treatment Klaus Olgaard Copenhagen Budapest Nephrology School August 2007 HPT IN CRF Renal mass Ca 2+ 1,25(OH) 2 D 3 CaR Hyperparathyroidism
Secondary hyperparathyroidism an Update on Pathophysiology and Treatment Klaus Olgaard Copenhagen Budapest Nephrology School August 2007 HPT IN CRF Renal mass Ca 2+ 1,25(OH) 2 D 3 CaR Hyperparathyroidism
Motility and eosin uptake of formaldehyde-treated ram
 Motility and eosin uptake of formaldehyde-treated ram spermatozoa O. A. Osinowo, J. O. Bale, E. O. Oyedipe and L. O. Eduvie Department ofanimal Reproduction, National Animal Production Research Institute,
Motility and eosin uptake of formaldehyde-treated ram spermatozoa O. A. Osinowo, J. O. Bale, E. O. Oyedipe and L. O. Eduvie Department ofanimal Reproduction, National Animal Production Research Institute,
SKELETAL SYSTEM CHAPTER 07. Bone Function BIO 211: ANATOMY & PHYSIOLOGY I. Body Movement interacts with muscles bones act as rigid bar of a lever
 Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
SKELETAL SYSTEM CHAPTER 07 BIO 211: ANATOMY & PHYSIOLOGY I
 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury
 Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury Bastian OW, Koenderman L, Alblas J, Leenen LPH, Blokhuis TJ. Neutrophils contribute to
Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury Bastian OW, Koenderman L, Alblas J, Leenen LPH, Blokhuis TJ. Neutrophils contribute to
K/DOQI-recommended intact PTH levels do not prevent low-turnover bone disease in hemodialysis patients
 http://www.kidney-international.org & 2008 International Society of Nephrology original article see commentary on page 674 K/DOQI-recommended intact PTH levels do not prevent low-turnover bone disease
http://www.kidney-international.org & 2008 International Society of Nephrology original article see commentary on page 674 K/DOQI-recommended intact PTH levels do not prevent low-turnover bone disease
A Tale of Four Traumas. Understanding how bones break
 A Tale of Four Traumas Understanding how bones break Bone Break Classifications First Classification Based on whether the break is open to the environment or not. CLOSED- not an open wound. Broken but
A Tale of Four Traumas Understanding how bones break Bone Break Classifications First Classification Based on whether the break is open to the environment or not. CLOSED- not an open wound. Broken but
Significance of minimodeling in dialysis patients with adynamic bone disease
 Kidney International, Vol. (5), pp. 33 39 DIALYSIS TRANSPLANTATION Significance of minimodeling in dialysis patients with adynamic bone disease YOSHIFUMI UBARA,TETSUO TAGAMI,SYOHEI NAKANISHI, NAOKI SAWA,
Kidney International, Vol. (5), pp. 33 39 DIALYSIS TRANSPLANTATION Significance of minimodeling in dialysis patients with adynamic bone disease YOSHIFUMI UBARA,TETSUO TAGAMI,SYOHEI NAKANISHI, NAOKI SAWA,
ISPUB.COM. O Egbuna, A Bose INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Nephrology Volume 2 Number 2 Acute Aluminum Neurotoxicity Secondary To Treatment Of Severe Hyperphosphatemia Of Acute Renal Failure And The K/DOQI Guidelines: A Case Report
ISPUB.COM The Internet Journal of Nephrology Volume 2 Number 2 Acute Aluminum Neurotoxicity Secondary To Treatment Of Severe Hyperphosphatemia Of Acute Renal Failure And The K/DOQI Guidelines: A Case Report
INDUCED CORNEAL OPACITIES IN THE RAT*t
 Brit. J. Ophthal. (1967) 51, 124 INDUCED CORNEAL OPACITIES IN THE RAT*t BY R. J. FABIAN, J. M. BOND, AND H. P. DROBECK Experimental Pathology and Toxicology, Sterling- Winthrop Research Institute, Rensselaer,
Brit. J. Ophthal. (1967) 51, 124 INDUCED CORNEAL OPACITIES IN THE RAT*t BY R. J. FABIAN, J. M. BOND, AND H. P. DROBECK Experimental Pathology and Toxicology, Sterling- Winthrop Research Institute, Rensselaer,
Bone Remodeling & Repair Pathologies
 Bone Remodeling & Repair Pathologies Skeletal system remodels itself to maintain homeostasis Remodeling Maintainence replaces mineral reserves (osteocytes) of the matrix Remodelling recycles (osteoclasts)
Bone Remodeling & Repair Pathologies Skeletal system remodels itself to maintain homeostasis Remodeling Maintainence replaces mineral reserves (osteocytes) of the matrix Remodelling recycles (osteoclasts)
Fig Articular cartilage. Epiphysis. Red bone marrow Epiphyseal line. Marrow cavity. Yellow bone marrow. Periosteum. Nutrient foramen Diaphysis
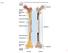 Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Elution of Tumoricidal Doses of Bortezomib from a Resorbable Cement Carrier
 Elution of Tumoricidal Doses of Bortezomib from a Resorbable Cement Carrier Matthew Allen, Vet MB, PhD, Brittani Jones, BS. The Ohio State University, Columbus, OH, USA. Disclosures: M. Allen: 5; Johnson
Elution of Tumoricidal Doses of Bortezomib from a Resorbable Cement Carrier Matthew Allen, Vet MB, PhD, Brittani Jones, BS. The Ohio State University, Columbus, OH, USA. Disclosures: M. Allen: 5; Johnson
SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over 3 Weeks. A SEPARATE WORKSHEET WILL BE PROVIDED.
 BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration.
 Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration. By Linero I., Chaparro O., 2014 Suzana Tufegdzic 1 Background 2 Background Stem Cells: undifferentiated
Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration. By Linero I., Chaparro O., 2014 Suzana Tufegdzic 1 Background 2 Background Stem Cells: undifferentiated
BONE REMODELLING. Tim Arnett. University College London. Department of Anatomy and Developmental Biology
 BONE REMODELLING Tim Arnett Department of Anatomy and Developmental Biology University College London The skeleton, out of sight and often out of mind, is a formidable mass of tissue occupying about 9%
BONE REMODELLING Tim Arnett Department of Anatomy and Developmental Biology University College London The skeleton, out of sight and often out of mind, is a formidable mass of tissue occupying about 9%
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary
 SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
Ability of Hydroxyapatite-Bone Morphologenetic Protein (BMP) Complex to Induce Dentin Formation in Dogs
 Okajimas Folia Anat. Jpn., 70(5): 195-202, December, 1993 Ability of Hydroxyapatite-Bone Morphologenetic Protein (BMP) Complex to Induce Dentin Formation in Dogs By Fumihiko SUWA, Lianjia Yang, Yoshikuni
Okajimas Folia Anat. Jpn., 70(5): 195-202, December, 1993 Ability of Hydroxyapatite-Bone Morphologenetic Protein (BMP) Complex to Induce Dentin Formation in Dogs By Fumihiko SUWA, Lianjia Yang, Yoshikuni
Bone disease in pediatric patients undergoing dialysis with CAPD or CCPD
 Kidney International, Vol. 33 (/988), pp. 975 982 Bone disease in pediatric patients undergoing dialysis with CAPD or CCPD ISIDRO B. SALUSKY, JACK W. COBURN, JUDITH BRILL, JOANNE FOLEY, EDUARDO SLATOPOLSKY,
Kidney International, Vol. 33 (/988), pp. 975 982 Bone disease in pediatric patients undergoing dialysis with CAPD or CCPD ISIDRO B. SALUSKY, JACK W. COBURN, JUDITH BRILL, JOANNE FOLEY, EDUARDO SLATOPOLSKY,
Biochemical markers of renal osteodystrophy in pediatric
 Kidney International, Vol. 45 (1994), pp. 253 258 Biochemical markers of renal osteodystrophy in pediatric patients undergoing CAPD/CCPD ISIDRO B. SALUSKY, JORGE A. RAMIREZ, WILLIAM OPPENHEIM, BARBARA
Kidney International, Vol. 45 (1994), pp. 253 258 Biochemical markers of renal osteodystrophy in pediatric patients undergoing CAPD/CCPD ISIDRO B. SALUSKY, JORGE A. RAMIREZ, WILLIAM OPPENHEIM, BARBARA
Advances in Peritoneal Dialysis, Vol. 29, 2013
 Advances in Peritoneal Dialysis, Vol. 29, 2013 Takeyuki Hiramatsu, 1 Takahiro Hayasaki, 1 Akinori Hobo, 1 Shinji Furuta, 1 Koki Kabu, 2 Yukio Tonozuka, 2 Yoshiyasu Iida 1 Icodextrin Eliminates Phosphate
Advances in Peritoneal Dialysis, Vol. 29, 2013 Takeyuki Hiramatsu, 1 Takahiro Hayasaki, 1 Akinori Hobo, 1 Shinji Furuta, 1 Koki Kabu, 2 Yukio Tonozuka, 2 Yoshiyasu Iida 1 Icodextrin Eliminates Phosphate
PART FOUR. Metabolism and Nutrition
 PART FOUR Metabolism and Nutrition Advances in Peritoneal Dialysis, Vol. 21, 2005 Maria Mesquita, 1 Eric Wittersheim, 2 Anne Demulder, 2 Max Dratwa, 1 Pierre Bergmann 3 Bone Cytokines and Renal Osteodystrophy
PART FOUR Metabolism and Nutrition Advances in Peritoneal Dialysis, Vol. 21, 2005 Maria Mesquita, 1 Eric Wittersheim, 2 Anne Demulder, 2 Max Dratwa, 1 Pierre Bergmann 3 Bone Cytokines and Renal Osteodystrophy
Assessment of magnesium status for diagnosis and therapy
 Magnesium Research 2010; 23 (4): S194-8 SHORT REPORT Assessment of magnesium status for diagnosis and therapy Ronald J. Elin Department of Pathology and Laboratory Medicine, School of Medicine, University
Magnesium Research 2010; 23 (4): S194-8 SHORT REPORT Assessment of magnesium status for diagnosis and therapy Ronald J. Elin Department of Pathology and Laboratory Medicine, School of Medicine, University
Elecsys bone marker panel. Optimal patient management starts in the laboratory
 bone marker panel Optimal patient management starts in the laboratory Complete solution for osteoporosis The most complete bone metabolism panel on a single platform bone marker assays are important diagnostic
bone marker panel Optimal patient management starts in the laboratory Complete solution for osteoporosis The most complete bone metabolism panel on a single platform bone marker assays are important diagnostic
Jemds.com. Original Article STUDY OF RENAL OSTEODYSTROPHY IN CHRONIC RENAL FAILURE
 STUDY OF RENAL OSTEODYSTROPHY IN CHRONIC RENAL FAILURE Nalina Thimmappa 1, Giriraja Kanakapura Vrushabaih 2, Pula Laxmi Bindumathi 3, Pooja Pillai 4, Bhaskar Balasundaram 5 1Associate Professor, Department
STUDY OF RENAL OSTEODYSTROPHY IN CHRONIC RENAL FAILURE Nalina Thimmappa 1, Giriraja Kanakapura Vrushabaih 2, Pula Laxmi Bindumathi 3, Pooja Pillai 4, Bhaskar Balasundaram 5 1Associate Professor, Department
Calcium, phosphate & magnesium regulation
 Calcium, phosphate & magnesium regulation Tim Arnett Department of Cell and Developmental Biology University College London Bone composition Treated with hydrochloric acid to dissolve mineral leaves organic
Calcium, phosphate & magnesium regulation Tim Arnett Department of Cell and Developmental Biology University College London Bone composition Treated with hydrochloric acid to dissolve mineral leaves organic
Skeletal Tissues. Skeletal tissues. Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs.
 Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
Inion BioRestore. Bone Graft Substitute. Product Overview
 Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Osteochondral regeneration. Getting to the core of the problem.
 Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
Renal bone disease 1990: An unmet challenge for the nephrologist
 Kidney International, Vol. 38 (1990), pp. 193 2 11 Renal bone disease 1990: An unmet challenge for the nephrologist EDITORIAL REVIEW The replacement of excretory kidney function by dialysis or by renal
Kidney International, Vol. 38 (1990), pp. 193 2 11 Renal bone disease 1990: An unmet challenge for the nephrologist EDITORIAL REVIEW The replacement of excretory kidney function by dialysis or by renal
Two major types of arterial calcification have been observed
 The Elastic Lamellae of Devitalized Arteries Calcify When Incubated in Serum Evidence for a Serum Calcification Factor Paul A. Price, Wai Si Chan, Dawn M. Jolson, Matthew K. Williamson Downloaded from
The Elastic Lamellae of Devitalized Arteries Calcify When Incubated in Serum Evidence for a Serum Calcification Factor Paul A. Price, Wai Si Chan, Dawn M. Jolson, Matthew K. Williamson Downloaded from
Metabolic Bone Disease Related to Chronic Kidney Disease
 Metabolic Bone Disease Related to Chronic Kidney Disease Deborah Sellmeyer, MD Director, Johns Hopkins Metabolic Bone Center Dept of Medicine, Division of Endocrinology Disclosure DSMB member for denosumab
Metabolic Bone Disease Related to Chronic Kidney Disease Deborah Sellmeyer, MD Director, Johns Hopkins Metabolic Bone Center Dept of Medicine, Division of Endocrinology Disclosure DSMB member for denosumab
Calcification of Bovine Pericardium: Glutaraldehyde Versus No-React Biomodification
 Calcification of Bovine Pericardium: Glutaraldehyde Versus No-React Biomodification Amir Abolhoda, MD, Sumei Yu, MS, J. Rodrigo Oyarzun, MD, John R. McCormick, MD, John D. Bogden, PhD, and Shlomo Gabbay,
Calcification of Bovine Pericardium: Glutaraldehyde Versus No-React Biomodification Amir Abolhoda, MD, Sumei Yu, MS, J. Rodrigo Oyarzun, MD, John R. McCormick, MD, John D. Bogden, PhD, and Shlomo Gabbay,
Chapter 6: Osseous Tissue and Bone Structure
 Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
The Role of the Laboratory in Metabolic Bone Disease
 The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
Original epidemiologic studies 1 have suggested that approximately
 Factors for Increased Morbidity and Mortality in Uremia: Hyperphosphatemia Nathan W. Levin, Frank A. Gotch, and Martin K. Kuhlmann Hyperphosphatemia is a metabolic abnormality present in the majority of
Factors for Increased Morbidity and Mortality in Uremia: Hyperphosphatemia Nathan W. Levin, Frank A. Gotch, and Martin K. Kuhlmann Hyperphosphatemia is a metabolic abnormality present in the majority of
Invited Re vie W. Cellular and molecular alterations of osteoblasts in human disorders of bone formation. Histology and H istopat hology
 Histol Histopathol (1999) 14: 525-538 http://www.ehu.es/histol-histopathol Histology and H istopat hology Invited Re vie W Cellular and molecular alterations of osteoblasts in human disorders of bone formation
Histol Histopathol (1999) 14: 525-538 http://www.ehu.es/histol-histopathol Histology and H istopat hology Invited Re vie W Cellular and molecular alterations of osteoblasts in human disorders of bone formation
Differences in bone turnover and intact PTH levels between African American and Caucasian patients with end-stage renal disease
 Kidney International, Vol. 64 (2003), pp. 737 742 Differences in bone turnover and intact PTH levels between African American and Caucasian patients with end-stage renal disease B. PETER SAWAYA, REZKALLA
Kidney International, Vol. 64 (2003), pp. 737 742 Differences in bone turnover and intact PTH levels between African American and Caucasian patients with end-stage renal disease B. PETER SAWAYA, REZKALLA
Using the Ch6diak-Higashi Marker
 A Study of the Origin of Pulmonary Macrophages Using the Ch6diak-Higashi Marker Kent J. Johnson, MD, Peter A. Ward, MD, Gary Striker, MD, and Robin Kunkel, MS Using bone marrow reconstitution techniques
A Study of the Origin of Pulmonary Macrophages Using the Ch6diak-Higashi Marker Kent J. Johnson, MD, Peter A. Ward, MD, Gary Striker, MD, and Robin Kunkel, MS Using bone marrow reconstitution techniques
The Distribution of Collagenous Connective Tissue in Rat Ovarian Follicles
 BIOLOGY OF REPRODUCTION 14, 502-506 (1976). The Distribution of Collagenous Connective Tissue in Rat Ovarian Follicles LAWRENCE L ESPEY Reproductive Physiology Laboratory, Trinity University, San Antonio,
BIOLOGY OF REPRODUCTION 14, 502-506 (1976). The Distribution of Collagenous Connective Tissue in Rat Ovarian Follicles LAWRENCE L ESPEY Reproductive Physiology Laboratory, Trinity University, San Antonio,
, P <0.01, after Al. Bone Al rose from to mg/kg
 Kidney International, Vol. 25 (1984), pp. 37 3 75 Parenteral aluminum administration in the dog: II. Induction of osteomalacia and effect on vitamin D metabolism WILLIAM G. GOODMAN, DAN A. HENRY, RONALD
Kidney International, Vol. 25 (1984), pp. 37 3 75 Parenteral aluminum administration in the dog: II. Induction of osteomalacia and effect on vitamin D metabolism WILLIAM G. GOODMAN, DAN A. HENRY, RONALD
The hart and bone in concert
 The hart and bone in concert Piotr Rozentryt III Department of Cardiology, Silesian Centre for Heart Disease, Silesian Medical University, Zabrze, Poland Disclosure Research grant, speaker`s fee, travel
The hart and bone in concert Piotr Rozentryt III Department of Cardiology, Silesian Centre for Heart Disease, Silesian Medical University, Zabrze, Poland Disclosure Research grant, speaker`s fee, travel
Anti-calcifying Treatment of Glutaraldehyde Fixed Bovine Pericardium: Comparisons and Evaluation of Possible Synergic Effects
 QCVC Committees Scientific Activities Central Hall General Information FAC Thematic Units Arrhythmias and Electrophysiology Basic Research Bioengineering and Medical Informatics Cardiac Surgical Intensive
QCVC Committees Scientific Activities Central Hall General Information FAC Thematic Units Arrhythmias and Electrophysiology Basic Research Bioengineering and Medical Informatics Cardiac Surgical Intensive
Experiments were carried out then with the object of producing complete disappearance of the A
 Relation of Glucagon to A Cells of the Pancreas*. (22339) SERGIO A. BENCOSME AND J. FREI. (Introduced by J.S.L. Browne Departament of pathology, Queen`s University, Kingston, Ontario, Canada. In spite
Relation of Glucagon to A Cells of the Pancreas*. (22339) SERGIO A. BENCOSME AND J. FREI. (Introduced by J.S.L. Browne Departament of pathology, Queen`s University, Kingston, Ontario, Canada. In spite
Pediatric metabolic bone diseases
 Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
(From The Ben May Laboratory for Cancer Research, The University of Chicago, Chicago, Illinois 60637)
 TRANSFORMATION OF FIBROBLASTS BY ALLOGENEIC AND XENOGENEIC TRANSPLANTS OF DEMINERALIZED TOOTH AND BONE* BY CHARLES HUGGINS, M.D., SOL WISEMAN, AND A. H. REDDI, PH.D. (From The Ben May Laboratory for Cancer
TRANSFORMATION OF FIBROBLASTS BY ALLOGENEIC AND XENOGENEIC TRANSPLANTS OF DEMINERALIZED TOOTH AND BONE* BY CHARLES HUGGINS, M.D., SOL WISEMAN, AND A. H. REDDI, PH.D. (From The Ben May Laboratory for Cancer
Extraosseous Calcification
 Extraosseous Calcification EVIDENCE FOR ABNORMAL PYROPHOSPHATE METABOLISM IN UREMIA ALLEN C. ALFREY, CLIVE C. SOLOMONS, JENNY CiRciuLLo, and NANCY L. MILLER From the Renal Section, Denver Veterans Administration
Extraosseous Calcification EVIDENCE FOR ABNORMAL PYROPHOSPHATE METABOLISM IN UREMIA ALLEN C. ALFREY, CLIVE C. SOLOMONS, JENNY CiRciuLLo, and NANCY L. MILLER From the Renal Section, Denver Veterans Administration
