International Cartilage Repair Society
|
|
|
- Carol Ryan
- 6 years ago
- Views:
Transcription
1 OsteoArthritis and Cartilage (2004) 12, 586e596 Ó 2004 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi: /j.joca Active proliferation of mesenchymal cells prior to the chondrogenic repair response in rabbit full-thickness defects of articular cartilage 1 Hiroshi Mizuta M.D., Ph.D.y, Satoshi Kudo M.D., Ph.D.y, Eiichi Nakamura M.D., Ph.D.y, Yutaka Otsuka M.D., Ph.D.y, Katsumasa Takagi M.D., Ph.D.y and Yuji Hiraki Ph.D.zx* y Department of Orthopaedic and Neuro-Musculoskeletal Surgery, Faculty of Medical and Pharmaceutical Sciences, Kumamoto University, Kumamoto , Japan z Department of Cellular Differentiation, Institute for Frontier Medical Sciences, Kyoto University, Kyoto , Japan x CREST, Japan Science and Technology, Kawaguchi, Saitama , Japan Summary International Cartilage Repair Society Objectives: In full-thickness articular defects, fibroblast growth factor-2 (FGF-2) participates in the chondrogenic repair response which occurs in a defect-size dependent manner. Here we demonstrate that FGF-2 plays a critical role in the proliferation of pre-chondrogenic mesenchymal cells during chondrogenic induction. Methods: Three-millimeter- or 5-mm-diameter cylindrical defects were created in the femoral trochlea of the rabbit knee. The defects received sterile saline or FGF-2 (50 pg/h) via an osmotic pump for the initial 2 weeks. We assessed the proliferative capacity of undifferentiated mesenchymal cells in the reparative tissue with the anti-proliferating cell nuclear antigen (PCNA) monoclonal antibody. Using a total of 180 rabbits, we performed three sets of experiments. Results: In the 3-mm-diameter defects, undifferentiated mesenchymal cells spontaneously initiated chondrogenic differentiation within 2 weeks, resulting in the regeneration of surfacing articular cartilage concomitantly with the repair of subchondral bone. No evidence of chondrogenesis was seen in the 5-mm-diameter defects, whereas application of FGF-2 promoted successful regeneration of articular cartilage. In the 3-mm-diameter defects and in the FGF-2-treated 5-mm defects, PCNA immunoreactivity was widely detected in undifferentiated cells in the reparative tissue at 1 and 2 weeks after creation of the defects. In contrast, in the 5-mm-diameter defects without FGF-2 treatment, the PCNA-positive cells were found at a significantly lower incidence. Conclusions: Active expansion of undifferentiated cell population mediated by FGF-2 is required to initiate and support a chondrogenic repair response in full-thickness defects of articular cartilage. Endogenous FGF-2 could not meet the requirements of growth signaling in the center of larger sized defects. Ó 2004 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. Key words: Osteochondral defect, Chondrogenic repair, Fibroblast growth factor. Introduction Full-thickness defects that penetrate articular cartilage undergo repair to end up with either fibrous, or fibrocartilaginous tissue or, to a very limited extent, hyaline cartilage. Adult bone marrow contains mesenchymal cells that have the potential to differentiate into the adipogenic, chondrogenic, and osteogenic lineages 1. These cells can migrate from the underlying bone marrow into the defect cavities, and are thought to be responsible for the sequential reparative responses 2. In an adolescent rabbit model of defects created in the femoral trochlea, the regenerative 1 This work was partly supported by grants from the Ministry of Health, Labor and Welfare, and Grant-in Aid for Scientific Research from the Ministry of Education, Culture, Sports, Science and Technology of Japan. * Address correspondence and reprint requests to: Dr Yuji Hiraki, Department of Cellular Differentiation, Institute for Frontier Medical Sciences, Kyoto University, 53 Shogoin-Kawahara-cho, Sakyo-ku, Kyoto , Japan. Tel/Fax: ; hiraki@ frontier.kyoto-u.ac.jp Received 23 September 2003; revision accepted 9 April capacity largely depends on their size 2,3. Smaller cylindrical defects (%3 mm in diameter) spontaneously regenerate surfacing articular cartilage concomitantly with repair of the subchondral bone through differentiation of mesenchymal progenitor cells. In contrast, overt chondrogenesis does not occur in larger defects (R5 mm in diameter), but results in the formation of fibrous scar tissue. However, little is known about how the chondrogenic repair response occurs in a defect-size dependent manner. The sequence of events during chondrogenesis is regulated by various growth and differentiation factors such as fibroblast growth factor (FGF), insulin-like growth factor-l (IGF-I), transforming growth factor-b (TGF-b), and members of bone morphogenetic protein (BMP) family 4. Among them, FGF signaling has been suggested to play a role in support of the proliferation of mesenchymal progenitor cells 5e7.We previously reported that the local administration of FGF-2 facilitated the regenerative repair of articular cartilage to overcome the size-limitation of the regenerative capacity of cartilage in a 5-mm-diameter full-thickness articular cartilage defect of the rabbit knee 3,8. In 5-mm-diameter defects, the administration of FGF-2 (50 pg/h for 2 weeks) in the defect cavities induced the chondrogenic repair within 586
2 Osteoarthritis and Cartilage Vol. 12, No. 7 4 weeks to result in successful coverage of defects with articular cartilage. On the other hand, even in 3-mmdiameter smaller defects, spontaneous chondrogenic repair failed to occur when the action of endogenous FGF-2 was blocked by the administration of a neutralizing antibody against FGF-2 3. Thus we hypothesized that the role of FGF- 2 was to promote proliferation of prechondrogenic mesenchymal cells in the defects during cartilage induction. Here we extensively studied the proliferative response of undifferentiated mesenchymal cells during repair of fullthickness defects of articular cartilage using a monoclonal antibody against proliferating cell nuclear antigen (PCNA) for gaining insight into the role of FGF-2 actions for the defect-size dependent induction of chondrogenic repair. Materials and methods CREATION OF FULL-THICKNESS DEFECTS OF ARTICULAR CARTILAGE Small full-thickness defects (3 mm in diameter; 4 mm in depth) were created in the weight-bearing area of the femoral trochlea of 20 adolescent Japanese white rabbits (weighing kg; purchased from KBT Oriental Co., Ltd, Tosu, Japan) by an electric drill with a 3-mm-diameter drillbit under anesthetization by sodium pentobarbital (30 mg/ kg bodyweight intravenously), as described previously 3. Larger full-thickness defects (5 mm in diameter; 4 mm in depth) were similarly created with a 5-mm-diameter drill-bit in 40 rabbits. All animals were allowed to walk freely without any splintage. Animal care and experimental procedures were conducted in accordance with institutional guidelines ( kisoku.html). ADMINISTRATION OF FGF-2 The animals were fitted with an osmotic pump (model 2002; Alzet, Palo Alto, CA) connected to silastic medical grade tubing (0.75 mm internal-diameter/1.45 mm outerdiameter). A length of the tubing about 5 mm was introduced into the articular knee cavity through the articular capsule in order to administer agents in the defect cavity. The osmotic pump was placed subcutaneously in the hind region of the leg, and the articular capsule and skin were closed independently 3. For 20 animals that had a 5-mmdiameter defect, the osmotic pump had been previously filled with 200 ml of sterile saline containing human recombinant FGF-2 (Takeda Chemical Industries, Osaka, Japan; 0.1 mg/ml). The pump had a nominal pumping rate of 0.5 ml/h for a 2-week period. The other 20 animals that had a 5-mm-diameter defect and 20 animals that had a 3-mmdiameter defect received sterile saline alone with the same osmotic pump system. For the subsequent histochemical and immunohistochemical analyses, the animals were sacrificed at 1, 2, 4, or 8 weeks after creation of the defects. Three sets of experiments were performed by using a total of 180 rabbits, and reproducibly yielded the similar results. HISTOCHEMICAL ANALYSES Five animals in each group were sacrificed with an overdose of sodium pentobarbital at the indicated times. The distal portion of each femur was removed, fixed in 4% paraformaldehyde at room temperature for 1 h, decalcified with 10% ethylenediamine tetraacetic acid (EDTA) in 10 mm phosphate buffer ( ph 7.4) for 3 weeks, and then embedded in paraffin for subsequent histological analysis. Sections (5 mm thick) were cut in the transverse plane, and stained with hematoxylin and eosin or with safranin-o. IMMUNOHISTOCHEMICAL ANALYSES 587 The presence of type I and type II collagen in the reparative tissues was examined immunohistochemically using a mouse monoclonal antibody against human type I and type II collagen (Fuji Chemical, Takaoka, Japan) that specifically crossreact with rabbit type I and type II collagen, respectively 9. The paraffin sections were deparaffinized and hydrated. Endogenous peroxidase activity was blocked with 0.5% hydrogen peroxide in methanol and washed in 0.1% bovine serum albumin (BSA) in Tris-buffered saline (TBS). The sections were then treated with 500 U/ml testicular hyaluronidase (Sigma Chemical Co., St Louis, MO, USA). Non-specific staining was reduced by incubation with horse serum. The sections were incubated with the antibody against type I collagen (dilution 1:100) or with the antibody against type II collagen (dilution 1:100) overnight at 4(C. Antibody binding was visualized by using a Vectastain avidinebiotineperoxidase complex (ABC) kit (Vector Laboratories, Burlingame, CA) in combination with diaminobenzidine (DAB) solution according to the manufacturer s instructions. The sections were counterstained with hematoxylin. For proteoglycan immunostaining, the mouse monoclonal antibodies 2B6, 3B3, and 5D4 (Seikagaku Kogyo, Tokyo, Japan) were used to detect the localization of chondroitin-4- sulfate, chondroitin-6-sulfate, and keratan sulfate, respectively. Sections were deparaffinized and hydrated. The sections were treated with 5 U/ml chondroitinase ABC (Seikagaku Kogyo, Tokyo, Japan) in 0.1 M Triseacetate buffer ph 8.0 at 37(C for 60 min. Endogenous peroxidase activity was blocked by 0.5% hydrogen peroxidase in methanol. The sections were washed in 0.1% BSA in TBS and non-specific staining was reduced by incubation with 1.3% horse serum. The sections were incubated with a monoclonal antibody 2B6, 3B3, or 5D4 (diluted 1:50) overnight at 4(C. For visualization of antibody binding, a subsequent reaction was performed as described above. The sections were counterstained with hematoxylin. To assess the presence of macrophages, vascular endothelial cells, and osteoblasts in the reparative tissue, we first stained the sections of the femoral trochlea recovered at 1 and 2 weeks after the creation of the defects with antibodies against CD68 (EBM11; Dakopatts, Copenhagen, Denmark), CD31 (JC/70A; Dakopatts, Copenhagen, Denmark) or alkaline phosphatase (AP-59; Sigma Chemical, St Louis, MO), respectively. For the immunostaining, the sections were cut, deparaffinized, and hydrated. Endogenous peroxidase activity was blocked by 0.5% hydrogen peroxide in methanol. The sections were washed in 0.1% BSA in TBS. Non-specific staining was reduced by incubation with 1.3% horse serum. The sections were incubated with JC/70A monoclonal antibody (dilution 1:10) at room temperature for 30 min, with EBM11 (dilution 1:50) or AP-59 (dilution 1:100) monoclonal antibody at room temperature for 1 h. For visualization of antibody binding, a subsequent reaction was performed as described above. The sections were then counterstained with methyl green. The tissue of the femoral trochlea was included in the study as a positive control for identification of macrophages (osteoclasts), vascular endothelial cells, and osteoblasts.
3 588 H. Mizuta et al.: Cell Proliferation in Cartilage repair For the immunostaining of PCNA-positive cells, the sections were cut, deparaffinized, and dehydrated. Endogenous peroxidase activity was blocked by 0.5% hydrogen peroxide in methanol. The sections were washed in 0.1% BSA in TBS, and then treated with 500 U/ml testicular hyaluronidase (Sigma Chemical, St Louis, MO) 10. Nonspecific staining was reduced by incubation with 1.3% horse serum. The sections were incubated with a monoclonal antibody against PCNA (clone PC10; Dakopatts, Copenhagen, Denmark), diluted 1:400 with PBS, at room temperature for 2 h. For visualization of antibody binding, a subsequent reaction was performed as described above. The sections were then counterstained with methyl green. For the detection of PCNA, the growth plate of Japanese white rabbits was used as a positive control 11. Sections were incubated with either horse serum or purified non-immune mouse IgG (Sigma Chemical Co., St. Louise, MO) instead of specific primary antibodies, and stained as a negative control. ESTIMATION OF CELLULARITY AND CELL PROLIFERATION IN THE DEFECT CAVITIES The packing cell density of the reparative tissue in the defects was examined by the methods of Gallay et al. using the sections stained with hematoxylin and eosin 12. A section of the defects was divided into 12 square areas, 1 mm!1 mm, in the 3-mm-diameter defects and into 20 square areas of the same size in the 5-mm-diameter defects. We enrolled all the areas in the defects at 1 week, while the peripheral and deeper four areas that were completely filled with newly formed bone were excluded at 2 weeks (Fig. 1). Two fields were selected at a magnification of!200 in each of sampling areas, and all nuclei except those of endothelial cells in capillaries and inflammatory cells were counted. The cell density in the defects was calculated from the mean number of cell nuclei that was divided by the size of area. Three sections from each paraffin block were used to calculate the average cell density for one animal. The mean and standard deviation (SD) of cell densities were calculated for five animals in each experimental group. The PCNA-positive cells were counted according to the method of Aizawa et al. using the sections stained by PCNA antibodies 11. Sampling square areas (1 mm!1 mm) were determined similarly as described above. Five fields were selected at a magnification of!400 in each sampling area, and the positive and negative mesenchymal cells were counted in each field. The incidence of PCNA-positive cells was calculated for the peripheral and central region of the defect, respectively. The peripheral region of defects was defined as the areas that were adjacent to the persisting marrow trabeculae or that were partially invaded by newly formed woven bone. As shown in Fig. 1, at 1 week, the peripheral region contained nine areas in the 3-mm defects and 11 areas in the 5-mm defects. At 2 weeks, six areas of the 3-mm defects and nine areas of the 5-mm defects were regarded as the peripheral region. The other areas in each defect were defined as the central region. The measurements were carried out using three sections from each paraffin block for one animal. The results were expressed as the mean and SD for five animals in each experimental group. Sections were examined in a blinded manner by the evaluators not informed on the group assignment. For microscopic analysis, an Axioskop microscope equipped with MC10 photomicrographic attachment (Carl Zeiss, Germany) was used. Statistical significance was estimated using ManneWhitney s U test. A P value of!0.05 was considered significant. Results HISTOLOGICAL AND IMMUNOHISTOCHEMICAL OBSERVATIONS In rabbit, full-thickness defects of articular cartilage reproducibly take either chondrogenic or non-chondrogenic repair pathway primarily depending on the size of the defects 2,3. In the 3-mm-diameter small defects, the defect cavity was mostly filled with undifferentiated spindle-shaped cells by 1 week after creation of defects [Fig. 2(A)]. At 2 A B A 3-mm-diameter defect at 1 week A 5-mm-diameter defect at 1 week C D Articular Cartilage Subchondral Bone A 3-mm-diameter defect at 2 weeks A 5-mm-diameter defect at 2 weeks Fig. 1. Schematic illustration showing sampling fields used for determining the packing cell density of the undifferentiated mesenchymal cells and the incidence of PCNA-positive cells in the 3-mm-diameter (A, C) and 5-mm-diameter (B, D) defects. The defects at 1 week and 2 weeks are shown in panels A and B, and panels C and D, respectively. Open squares represent the peripheral region of the defects, and shaded squares represent the central region of the defects.
4 Osteoarthritis and Cartilage Vol. 12, No Fig. 2. Transverse sections of the reparative 3-mm-diameter defects treated with saline alone (A, D, G, J), 5-mm-diameter defects treated with saline alone (B, E, H, K), and 5-mm-diameter defects treated with FGF-2 (C, F, I, L). The sections were stained with safranin-o at (AeC) 1 week, (DeF) 2 weeks, (Gel) 4 weeks, and (JeL) 8 weeks after creating the defects. Bar: 500 mm. weeks, spherical chondrocytes surrounded by extracellular matrix stainable with safranin-o appeared in the central region of the defect cavity [Fig. 2(D)]. Appositional repair of subchondral bone had already been started. At 4 weeks, the defects were occupied by cartilaginous tissue with abundant cartilage matrix, which was actively replaced by subchondral bone from the depths of the defects [Fig. 2(G)]. The epiphyseal structure with the resurfacing hyaline-like cartilage was regenerated, and the original boneearticular cartilage junction was recovered by 8 weeks [Fig. 2(J)]. In the 5-mm-diameter larger defects, by contrast, undifferentiated spindle-shaped cells appeared at the periphery of the defect, and the center of the defect was filled with blood clot at 1 week, regardless of treatments with FGF-2 [Fig. 2(B, C)]. At 2 weeks, in the non-treated defects, osteoblastic differentiation of cells had taken place near the subchondral bone surface, but there was no evidence of cartilage formation [Fig. 2(E)]. The defects were almost filled with fibrous reparative tissue even at 4 weeks after defect creation [Fig. 2(H)]. At 8 weeks, the subchondral bone was almost reconstituted, but cells surfacing the defects were mostly non-chondrocytic and the matrix was not stained with safranin-o [Fig. 2(K)]. In the FGF-2-treated 5-mm-diameter defects, chondrogenic differentiation took place in the periphery of the subchondral bone surface within 2 weeks, as indicated by the appearance of spherical cells with the safranin-o positive extracellular matrix [Fig. 2(F)]. At 4 weeks, the defects were occupied by cartilaginous tissue, which was replaced gradually by the appositional growth of subchondral bone from the depth [Fig. 2(I)]. At 8 weeks, well-developed cartilage covered the defects, and the thickness of the safranin-o stained matrix had almost recovered that of the original articular cartilage [Fig. 2(L)]. In order to further assess the character of reparative tissue, the immunostaining for type I and type II collagens was performed (Figs. 3 and 4). In the 3-mm-diameterdefects, immunoreactivity to type I collagen was detected in
5 590 H. Mizuta et al.: Cell Proliferation in Cartilage repair Fig. 3. Immunohistochemistry of type I collagen in the reparative 3-mm-diameter defects treated with saline alone (A, D), 5-mm-diameter defects treated with saline alone (B, E), and 5-mm-diameter defects treated with FGF-2 (C, F) at 4 weeks (AeC) and at 8 weeks (DeF) after creation of the defects. Arrowheads indicate the boundary between the pre-existing articular cartilage (on the left side) and the reparative tissue (on the right side). The sections were counterstained with hematoxylin. Bar: 300 mm. Fig. 4. Immunohistochemistry of type II collagen in the reparative 3-mm-diameter defects treated with saline alone (A, D), 5-mm-diameter defects treated with saline alone (B, E), and 5-mm-diameter defects treated with FGF-2 (C, F) at 4 weeks (AeC) and at 8 weeks (DeF) after creation of the defects. Arrowheads indicate the boundary between the pre-existing articular cartilage (on the left side) and the reparative tissue (on the right side). The sections were counterstained with hematoxylin. Bar: 300 mm.
6 Osteoarthritis and Cartilage Vol. 12, No Fig. 5. Immunohistochemistry of chondroitin-4-sulfate (A, B), chondroitin-6-sulfate (C, D), and keratan sulfate (E, F) in the reparative 3-mmdiameter defects treated with saline alone (A, C, E), 5-mm-diameter defects treated with FGF-2 (B, D, F) at 8 weeks after creation of the defects. Arrowheads indicate the boundary between the pre-existing articular cartilage (on the left side) and the reparative tissue (on the right side). The sections were counterstained with hematoxylin. Bar: 300 mm. the immature reparative tissue around the differentiating cartilaginous tissues, as well as the pre-existing bony tissue at 2 weeks after creation of defects. At 4 weeks, as cartilaginous repair proceeded, the immunoreactivity was seen only at the surface of the reparative tissue [Fig. 3(A)]. At 8 weeks, there was no immunoreactivity to type I collagen in the most of the repaired articular cartilage, although the expression of type I collagen was persisted at the superficial layer [Fig. 3(D)]. In the FGF-2-treated 5-mm-diameter defects [Fig. 3(C, F)], a similar distribution of the type I collagen immunoreactivity was observed in the immature reparative tissue at superficial layer of cartilage. No apparent immunoreactivity was detected in either regenerated or pre-existing cartilaginous tissue. Marked induction of type I collagen was seen in the fibrous repair tissue formed in the 5-mm-diameter defects without the FGF-2 treatment [Fig. 3 (B, E)]. In clear contrast, the formation of type II collagen in cartilaginous tissues was detected by immunostaining at 2 weeks in the 3-mm-diameter defects. At 4 weeks, immunoreactive type II collagen was clearly detected in the regenerating cartilaginous tissue as well as pre-existing articular cartilage [Fig. 4(A)]. Surfacing immature reparative tissue, which was positive for type I collagen, was negative for type II collagen [Fig. 4]. At 8 weeks, reparative cartilaginous tissue was indistinguishable from pre-existing articular cartilage with regard to immunoreactivity to type II collagen [Fig. 4(D)]. In the 5-mm-diameter defects with the FGF-2 treatment, regenerated cartilaginous tissue markedly expressed type II collagen to the extent comparable with preexisting articular cartilage [Fig. 4(C, F)]. There was no immunoreactivity detected in fibrous reparative tissue formed in the 5-mm-diameter defects without the FGF-2 treatment [Fig. 4(B, E)]. To assess the character of extracellular matrix in the cartilaginous reparative tissue 9, immunohistochemical studies were carried out with monoclonal antibodies against
7 592 H. Mizuta et al.: Cell Proliferation in Cartilage repair Fig. 6. Immunohistochemistry of CD68 (A, B, G, H, M, N), CD31 (C, D, I, J, O, P), and alkaline phosphatase (E, F, K, L, Q, R) in the reparative tissues in the 3-mm-diameter defects treated with saline alone (AeF), 5-mm-diameter defects treated with saline alone (GeL), and 5-mmdiameter defects treated with FGF-2 (MeR) at 1 weeks after creation of the defects. Panels B, F, H, L, N, and R show osteoclasts (B, H, N) and osteoblasts (F, L, R) visualized (brown) by anti-cd68 and anti-alkaline phosphatase antibodies respectively, and used as positive controls for confirmation of the specific immunoreactivity of antibodies. Panels D, J, and P show vascular endothelial cells that were visualized by anti- CD31 antibody in the neighboring bony tissue. The sections were counterstained with methyl green. Bar: 50 mm. chondroitin-4-sulfate, chondroitin-6-sulfate, and keratan sulfate (Fig. 5). In the 3-mm-diameter defects at 4 and 8 weeks [Fig. 5(A, C, E)], immunoreactivities to chondroitin-4- sulfate, chondroitin-6-sulfate, and keratan sulfate were clearly detected in cartilaginous reparative tissues, at levels similar to those in the pre-existing articular cartilage. In the FGF-2-treated 5-mm-diameter defects, these glycosaminoglycans in cartilage proteoglycans were detected in regenerated chondrocytes and the surrounding matrix at 4 and 8 weeks [Fig. 5(B, D, F)]. LOCALIZATION OF PCNA-POSITIVE CELLS IN REPARATIVE TISSUE To assess the presence of macrophages, vascular endothelial cells, and osteoblasts in the reparative tissue, we first stained the sections of the femoral trochlea recovered at 1 week after the creation of the defects with antibodies against CD68, CD31 or alkaline phosphatase (Fig. 6). No positive staining above background was observed in either the 3-mm-diameter defects or the 5- mm-diameter defects irrespective of the FGF-2 treatment. Thus the reparative tissue is substantially composed of undifferentiated fibroblastic cells in agreement with histological observations mentioned above. Then, we assessed the packing cell density of the reparative tissue and the proliferative capacity of the undifferentiated fibroblastic cells that had filled the defect cavities by immunostaining PCNA 11,12. We stained the sections of the femoral trochlea recovered at 1 and 2 weeks after creation of the defects with hematoxylin and eosin, respectively. Then, semi-serial sections were stained with PCNA antibody. In the 3-mm-diameter defects, most of the undifferentiated cells were positively stained with PCNA antibody at 1 week [Fig. 7(A)]. At 2 weeks, the PCNA immunoreactivity persisted widely in mesenchymal cells beneath the surfacing area [Fig. 8(A)]. In the 5-mm-diameter defects without the FGF-2 treatment, by contrast, PCNA-positive cells were restricted only in the marginal areas of the defect cavities both at 1 week and at 2 weeks [Figs. 7(C) and 8(C)]. Most of the cells in the center of the defects did not express PCNA immunoreactivity [Figs. 7(B) and 8(B)]. However, administration of FGF-2 strikingly increased the PCNA immunoreactivity in undifferentiated mesenchymal cells in the 5-mm-diameter defects. Most of the undifferentiated cells were evidently stained with PCNA antibody at 1 week [Fig. 7(D)] and the immunoreactivity persisted in even at 2 weeks [Fig. 8(D)]. The pattern of immunostaining was accorded well with that in the 3-mm-diameter defects. PCNA immunoreactivity was barely detectable in chondrocytes of the pre-existing articular cartilage surrounding the defects. Application of FGF-2 exerted no apparent effect on proliferative activity in these chondrocytes (data not shown). Table I summarizes the packing cell density and the incidence of PCNA-positive cells in the reparative tissues. At 1 week, along with the packing cell density, the incidence of PCNA-positive cells for the whole defect and the packing
8 Osteoarthritis and Cartilage Vol. 12, No Fig. 7. Immunohistochemistry of PCNA in the reparative 3-mm-diameter defects treated with saline alone (A), 5-mm-diameter defects treated with saline alone (B, C), and 5-mm-diameter defects treated with FGF-2 (D) at 1 week after creation of the defects. Panels A, B, and D represent the PCNA-positive cells beneath the surfacing areas of the defects which correspond to the areas denoted by the asterisks in panels A, B, and C in Fig. 2, respectively. Panel C represents the PCNA-positive cells in the peripheral area of the defects which corresponds to the area denoted by the open circle in panel B of Fig. 2. The sections were counterstained with methyl green. Bar: 50 mm. cell density was significantly lower in the 5-mm-diameter defects than that in the 3-mm-diameter defects. The incidence of PCNA-positive cells in the 5-mm-diameter defects remained to a lower level even at 2 weeks in the 5- mm-diameter defects. By contrast, the incidence of PCNApositive cells in the FGF-2-treated 5-mm-diameter defects was as high as that in the 3-mm-diameter defects at 1 and 2 weeks, which was significantly higher than that in the nontreated 5-mm-diameter defects. The packing cell-density at 1 week was also significantly higher in the FGF-2-treated defects than that in the 5-mm-diameter defects without FGF-2 treatment. In the 3-mm-diameter defects and the FGF-2-treated 5-mm-diameter defects, no significant difference was found in the incidence of PCNA-positive cells between the peripheral and central region of the defects. Interestingly, in the 5-mm-diameter defects without FGF-2 treatment, the incidence of PCNA-positive cells for the peripheral region was 3- to 4-fold higher than that for the central region. Discussion Regeneration of cartilage occurs in a defect-size dependent manner during repair of full-thickness defect of articular cartilage (Fig. 2) 3,13. As demonstrated by immunohistochemistry, regenerated cartilaginous tissue expresses abundant cartilage-characteristic matrix components (Figs. 3e5). In the 3-mm-diameter cylindrical defects, cartilaginous tissue is spontaneously formed and the regenerated cartilage is then subsequently replaced by the accretionary growth of subchondral bone up to the original boneearticular cartilage junction. Thus the smaller defects are covered with surfacing articular cartilage. Although the accretionary growth of subchondral bone occurs, no cartilage formation takes place in the 5-mmdiameter larger defects. Local administration of FGF-2 within the defect cavities apparently overcomes this sizelimitation of cartilage repair. Treatment of 3-mm-diameter defects with neutralizing anit-fgf-2 monoclonal antibody markedly inhibited spontaneous cartilaginous repair to occur 3. As there was no evidence to indicate the proliferation of pre-existing articular chondrocytes 2,3, the growth of pre-existing chondrocytes is not involved in the actions of endogenous and/or exogenous FGF-2 during repair of defects. Obviously, undifferentiated mesenchymal progenitor cells that migrated from bone marrow were the likely targets of the FGF-2 actions (Fig. 6). Chondrogenic differentiation of mesenchymal cells proceeds through an ordered cascade of cellular events as demonstrated in vivo and in vitro: (1) the mobilization and migration of cells to the site of chondrogenesis, (2) prechondrogenic cellular interactions and condensation, and (3) the overt differentiation to chondrocytes 4. Cellular condensation is itself a multi-step process, which involves initiation, establishment of boundary conditions, cell adhesion, proliferation and growth. Although FGFs may act at more than one stage in this cascade of events, it is implicated that they play a central role in the active proliferation of progenitor cells and the maintenance of the
9 594 H. Mizuta et al.: Cell Proliferation in Cartilage repair Fig. 8. Immunohistochemistry of PCNA in the reparative 3-mm-diameter defects treated with saline alone (A), 5-mm-diameter defects treated with saline alone (B, C), and 5-mm-diameter defects treated with FGF-2 (D) at 2 weeks after creation of the defects. Panels A, B, and D represent the PCNA-positive cells beneath the surfacing areas of the defects which correspond to the areas denoted by asterisks in panels D, E, and F in Fig. 2, respectively. Panel C represents the PCNA-positive cells in the peripheral area of the defects which corresponds to the area denoted by the open circle in panel E of Fig. 2. The sections were counterstained with methyl green. Bar: 50 mm. progenitor cell population at the site of cartilage formation 5,7,14,15. Tsutsumi and coworkers reported that FGF-2 potently stimulated self-renewal of mesenchymal stem cells or mesenchymal progenitor cells without loss of differentiation potentials 16. In agreement with this notion and our preliminary experiments 8, the FGF-2 (50 pg/h for 2 weeks) treatment of 5-mm-diameter defects resulted in the marked increase of PCNA-positive undifferentiated cells prior to overt chondrogenesis in the reparative tissue, as compared to that in the untreated 5-mm-diameter defects (Table I). Average incidence of PCNA-positive cells dramatically increased by FGF-2 from 16.5% to 57.8% at 1 week after creation of defects and from 19.4% to 40.1% at 2 weeks. The increased level of PCNA-positive cells was comparable to that of cells in the 3-mm-diameter smaller defects (56.1% at 1 week and 42.9% at 2 weeks), where overt chondrogenesis was spontaneously induced. The resultant cartilaginous tissue occupied the defect cavities from 2 to 4 weeks after creation of defects 2,3. Thus, as indexed by a high incidence of PCNA-positive cells, active expansion and maintenance of progenitor cell populations were well correlated with the capacity of subsequent overt chondrogenesis to occur (Figs. 7 and 8). The 3-mm-diameter smaller defects were fully covered with the proliferating cell population from the periphery of subchondral bone to the center (Fig. 1). By the FGF-2 administration, the defect cavities were similarly covered with the proliferating progenitor cell population (Figs. 7 and 8). Endogenous FGF-2 signaling is also implicated in the spontaneous chondrogenic repair response in the 3-mm-diameter smaller defects, since a neutralizing monoclonal antibody against FGF-2 completely blocked overt chondrogenesis in these smaller defects 3,8. As trabecular bone surface is one of major storage sites of FGF-2 in the body 8,17, a flux of FGF-2 liberated from subchondral bone surface during creation of defects by drilling and the initial hematoma formation can be a candidate of endogenous source of FGF-2. In addition, as previously demonstrated by in situ hybridization and immunohistochemistry, mesenchymal cells that strongly express FGF-2 accumulated from the periphery of subchondral bone in the defect cavities 3. These cells can also serve as a source of endogenous FGF-2 signaling. The flux of FGF-2 may be supplied in a manner proportional to the surface area (square of a defect size) of subchondral bone facing a defect cavity, while the volume of a defect cavity increases with cubic of a defect size. Thus it is reasonably assumed that the supply of endogenous FGF-2 signaling cannot catch up with the increasing demand of FGF-2 signaling required for the maintenance of an expanding progenitor cell population in larger defects. As shown in Table I, without administration of exogenous FGF-2, a gradient of PCNA-positive cells was formed in 5-mm-diameter defects. At the central region [hatched area shown in Fig. 1(B, D)], the population of proliferating cells must be reduced below a critical threshold (4.8% at 1 week and 5.7% at 2 weeks) for induction of overt chondrogenesis, as compared to that (28.2% at 1 week and 31.0% at 2 weeks) in the peripheral region of subchondral bone surface. Therefore, even though cartilaginous induction took place occasionally at the periphery of bone, regenerating cartilage failed to
10 Osteoarthritis and Cartilage Vol. 12, No Table I Cellularity and incidence of PCNA-positive cells in the reparative tissue in the defects Cell density (cells x 10-3 /µm 2 ) Whole defect PCNA-positive cells (% of total) Central region Peripheral region At 1 week 3-mm diameter defect 1.86 ± ± ± ± 16.1 Control 5-mm diameter defect FGF-treated 5-mm diameter defect 0.66 ± ± ± ± ± ± ± ± 17.9 * * At 2 week 3-mm diameter defect 1.93 ± ± ± ± 14.9 * Control 5-mm diameter defect FGF-treated 5-mm diameter defect 2.01 ± ± ± ± 22.1 * 5.7 ± ± ± ± 19.5 Values are meansgsd for five animals. *P!0:05, P!0:01. y All nuclei were counted in a total of 72 fields in the 3-mm-diameter defects at 1 week, 120 in the 5-mm-diameter defects at 1 week, 48 in the 3-mm-diameter defects at 2 weeks, and 96 in the 5-mm-diameter defects at 2 weeks using three sections for each animal at a magnification of!200, as described in Materials and methods. z The PCNA-positive and -negative mesenchymal cells also were counted in a total of 180 fields in the 3-mm-diameter defects at 1 week, 300 in the 5-mm defects at 1 week, 120 in the 3-mm-diameter at 2 weeks, and 240 in the 5-mm-diameter defects at 2 weeks using three sections for each animal at a magnification of!400. cover the entire surface of the 5-mm-diameter defect cavities. In the present study, we demonstrated that the successful cartilaginous resurfacing of full-thickness defects required the initiation and maintenance of expanding chondroprogenitor cell population prior to overt chondrogenesis in the defect cavities. The data suggest that FGF-2 signaling plays a role in this process as a regulatory mechanism for a defect-size dependent regeneration of articular cartilage. Further understanding of regulatory mechanism of cartilage regeneration may provide clues for new therapeutic strategy of regenerative medicine. Acknowledgements Recombinant human FGF-2 was a generous gift from Dr T. Kurokawa (Takeda Chemical Industries, Osaka, Japan). This work was partly supported by grants from the Ministry of Health, Labor and Welfare, and Grant-in Aid for Scientific Research from the Ministry of Education, Culture, Sports, Science and Technology of Japan. This work has been supported in part by CREST of JST (Japan Science and Technology Corporation). References 1. Pittenger MF, Mackay AM, Beck SC, Jaiswal RK, Douglas R, Mosca JD, et al. Multilineage potential of adult human mesenchymal stem cells. Science 1999; 284:143e7. 2. Shapiro F, Koide S, Glimcher MJ. Cell origin and differentiation in the repair of full-thickness defects of articular cartilage. J Bone Joint Surg Am 1993;75: 532e Otsuka Y, Mizuta H, Takagi K, Iyama K, Yoshitake Y, Nishikawa K, et al. Requirement of fibroblast growth factor signaling for regeneration of epiphyseal morphology in rabbit full-thickness defects of articular cartilage. Dev Growth Differ 1997;39:143e Hall BK, Miyake T. All for one and one for all: condensations and the initiation of skeletal development. Bioessays 2000;22:138e Niswander L, Tickle C, Vogel A, Booth I, Martin GR. FGF-4 replaces the apical ectodermal ridge and directs outgrowth and patterning of the limb. Cell 1993;75:579e Rousseau F, Bonaventure J, Legeai-Mallet L, Pelet A, Rozet JM, Maroteaux P, et al. Mutations in the gene encoding fibroblast growth factor receptor-3 in achondroplasia. Nature 1994;371:252e4. 7. Cohn MJ, Izpisua-Belmonte JC, Abud H, Heath JK, Tickle C. Fibroblast growth factors induce additional limb development from the flank of chick embryos. Cell 1995;80:739e Hiraki Y, Shukunami C, Iyama K, Mizuta H. Differentiation of chondrogenic precursor cells during the regeneration of articular cartilage. Osteoarthritis Cartilage 2001;9:S102e8.
11 596 H. Mizuta et al.: Cell Proliferation in Cartilage repair 9. Takeuchi N, Suzuki Y, Sagehashi Y, Yamaguchi T, Itoh H, Iwata H. Histologic examination of meniscal repair in rabbits. Clin Orthop 1997; 253e Iyama K, Ninomiya Y, Olsen BR, Linsenmayer TF, Trelstad RL, Hayashi M. Spatiotemporal pattern of type X collagen gene expression and collagen deposition in embryonic chick vertebrae undergoing endochondral ossification. Anat Rec 1991;229: 462e Aizawa T, Kokubun S, Tanaka Y. Apoptosis and proliferation of growth plate chondrocytes in rabbits. J Bone Joint Surg Br 1997;79:483e Gallay SH, Miura Y, Commisso CN, Fitzsimmons JS, O Driscoll SW. Relationship of donor site to chondrogenic potential of periosteum in vitro. J Orthop Res 1994;12:515e Convery F, Akeson W, Koewn G. The repair of osteochondral defects: an experimental study in horses. Clin Orthop 1972;82:253e Shukunami C, Ohta Y, Sakuda M, Hiraki Y. Sequential progression of the differentiation program by bone morphogenetic protein-2 in chondrogenic cell line ATDC5. Exp Cell Res 1998;241:1e Shimizu A, Tada K, Shukunami C, Hiraki Y, Kurokawa T, Magane N, et al. A novel alternatively spliced fibroblast growth factor receptor 3 isoform lacking the acid box domain is expressed during chondrogenic differentiation of ATDC5 cells. J Biol Chem 2001;276: 11031e Tsutsumi S, Shimazu A, Miyazaki K, Pan H, Koike C, Yoshida E, et al. Retention of multilineage differentiation potential of mesenchymal cells during proliferation in response to FGF. Biochem Biophys Res Commun 2001;288:413e Hauschka PV, Mavrakos AE, Iafrati MD, Doleman SE, Klagsbrun M. Growth factors in bone matrix. Isolation of multiple types by affinity chromatography on heparine Sepharose. J Biol Chem 1986;261:12665e74.
o~ r;'c' - OSTEOARTHRITIS
 Osteoarthritis and Cartilage (2001) 9, Supplement A, S102-S108 2001 OsteoArthritis Research Society International doi:10.1053/joca.2001.0451, available online at http://www.idealibrary.com on IDE~l Osteoarthritis
Osteoarthritis and Cartilage (2001) 9, Supplement A, S102-S108 2001 OsteoArthritis Research Society International doi:10.1053/joca.2001.0451, available online at http://www.idealibrary.com on IDE~l Osteoarthritis
Cartilaginous repair of full-thickness articular cartilage defects is induced by the intermittent activation of PTH/PTHrP signaling
 Osteoarthritis and Cartilage 19 (2011) 886e894 Cartilaginous repair of full-thickness articular cartilage defects is induced by the intermittent activation of PTH/PTHrP signaling S. Kudo y, H. Mizuta y,
Osteoarthritis and Cartilage 19 (2011) 886e894 Cartilaginous repair of full-thickness articular cartilage defects is induced by the intermittent activation of PTH/PTHrP signaling S. Kudo y, H. Mizuta y,
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2004) 12, 834e842 ª 2004 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2004.07.003 One day exposure to
OsteoArthritis and Cartilage (2004) 12, 834e842 ª 2004 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2004.07.003 One day exposure to
BONE TISSUE. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
Supplemental Data. Wnt/β-Catenin Signaling in Mesenchymal Progenitors. Controls Osteoblast and Chondrocyte
 Supplemental Data Wnt/β-Catenin Signaling in Mesenchymal Progenitors Controls Osteoblast and Chondrocyte Differentiation during Vertebrate Skeletogenesis Timothy F. Day, Xizhi Guo, Lisa Garrett-Beal, and
Supplemental Data Wnt/β-Catenin Signaling in Mesenchymal Progenitors Controls Osteoblast and Chondrocyte Differentiation during Vertebrate Skeletogenesis Timothy F. Day, Xizhi Guo, Lisa Garrett-Beal, and
Growth and repair: Cartilage is a vascular tissues that receives nutrients by diffusion through its matrix, cartilage grow by 2 mechanisms:
 Skeletal connective tissues: (cartilage and bone): Cartilage and bone are specialized connective tissues both adapted to serve as skeletal framework in most vertebrates the presence of solid inter cellular
Skeletal connective tissues: (cartilage and bone): Cartilage and bone are specialized connective tissues both adapted to serve as skeletal framework in most vertebrates the presence of solid inter cellular
CARTILAGE. Dr. Emad I Shaqoura M.D, M.Sc. Anatomy Faculty of Medicine, Islamic University-Gaza October, 2015
 CARTILAGE Dr. Emad I Shaqoura M.D, M.Sc. Anatomy Faculty of Medicine, Islamic University-Gaza October, 2015 Introduction Hyaline Cartilage Elastic Cartilage Fibrocartilage Cartilage Formation, Growth,
CARTILAGE Dr. Emad I Shaqoura M.D, M.Sc. Anatomy Faculty of Medicine, Islamic University-Gaza October, 2015 Introduction Hyaline Cartilage Elastic Cartilage Fibrocartilage Cartilage Formation, Growth,
Cartilage. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Cartilage Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology 1 Cartilage is a specialized type of connective tissue designed to give support, bear weight and withstand tension, torsion and
Cartilage Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology 1 Cartilage is a specialized type of connective tissue designed to give support, bear weight and withstand tension, torsion and
Biology. Dr. Khalida Ibrahim
 Biology Dr. Khalida Ibrahim The cartilage General characteristics: 1. Cartilage is a specialized type of connective tissue (supporting connective tissue). 2. Consists, like other connective tissues, of
Biology Dr. Khalida Ibrahim The cartilage General characteristics: 1. Cartilage is a specialized type of connective tissue (supporting connective tissue). 2. Consists, like other connective tissues, of
Bone. Development. Tim Arnett. University College London. Department of Anatomy and Developmental Biology
 Bone Development Tim Arnett Department of Anatomy and Developmental Biology University College London Bone development Outline Bone composition matrix + mineral Bone formation - intramembranous & endochondral
Bone Development Tim Arnett Department of Anatomy and Developmental Biology University College London Bone development Outline Bone composition matrix + mineral Bone formation - intramembranous & endochondral
Chapter 6: Skeletal System: Bones and Bone Tissue
 Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Blood. Hematopoietic Tissue
 Blood Hematopoietic Tissue Is a type of connective tissue in which its cells are suspended in a circulating fluid. Erythrocytes+ leukocytes + platelets (thrombocytes) =formed elements of blood. These formed
Blood Hematopoietic Tissue Is a type of connective tissue in which its cells are suspended in a circulating fluid. Erythrocytes+ leukocytes + platelets (thrombocytes) =formed elements of blood. These formed
The Skeletal System:Bone Tissue
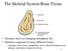 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue
 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
What are the parts of the skeletal system? Chapter 6- Part I Bones and Skeletal Tissues. Growth of Cartilage. Bones come in many shapes
 Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
PROCHONDRIX CARTILAGE RESTORATION MATRIX CONTAINS GROWTH FACTORS NECESSARY FOR HYALINE CARTILAGE REGENERATION
 A L L O S O U R C E PROCHONDRIX CARTILAGE RESTORATION MATRIX CONTAINS GROWTH FACTORS NECESSARY FOR HYALINE CARTILAGE REGENERATION Ryan Delaney MS; Carolyn Barrett BS, MBA; Peter Stevens PhD, MBA AlloSource,
A L L O S O U R C E PROCHONDRIX CARTILAGE RESTORATION MATRIX CONTAINS GROWTH FACTORS NECESSARY FOR HYALINE CARTILAGE REGENERATION Ryan Delaney MS; Carolyn Barrett BS, MBA; Peter Stevens PhD, MBA AlloSource,
Regulation of the IGF axis by TGF-b during periosteal chondrogenesis: implications for articular cartilage repair
 Regulation of the IGF axis by TGF-b during periosteal chondrogenesis: implications for articular cartilage repair Chapter 04 Boek 1_Gie.indb 55 21-05-2007 12:27:33 Chapter 04 Abstract Goal: TGF-b and IGF-I
Regulation of the IGF axis by TGF-b during periosteal chondrogenesis: implications for articular cartilage repair Chapter 04 Boek 1_Gie.indb 55 21-05-2007 12:27:33 Chapter 04 Abstract Goal: TGF-b and IGF-I
Skeletal System. The skeletal System... Components
 Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
SKELETAL TISSUES CHAPTER 7 INTRODUCTION TO THE SKELETAL SYSTEM TYPES OF BONES
 SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
Quiz 6. Cartilage and Bone
 Quiz 6 Cartilage and Bone MCQs X type (true or false): 1. Cartilage tissue: a. Has a rich blood supply. b. Develops from mesenchyme. c. Has ability for a quick regeneration. d. Has chondrocytes as precursor
Quiz 6 Cartilage and Bone MCQs X type (true or false): 1. Cartilage tissue: a. Has a rich blood supply. b. Develops from mesenchyme. c. Has ability for a quick regeneration. d. Has chondrocytes as precursor
2 PROCESSES OF BONE OSSIFICATION
 2 PROCESSES OF BONE OSSIFICATION ENDOCHONDRAL OSSIFICATION 6 STEPS 1. CARTILAGE ENLARGES, BY APPOSITIONAL GROWTH; CHONDROCYTES AT CENTER OF CARTILAGE GROW IN SIZE; MATRIX REDUCES IN SIZE & SPICULES CALCIFY;
2 PROCESSES OF BONE OSSIFICATION ENDOCHONDRAL OSSIFICATION 6 STEPS 1. CARTILAGE ENLARGES, BY APPOSITIONAL GROWTH; CHONDROCYTES AT CENTER OF CARTILAGE GROW IN SIZE; MATRIX REDUCES IN SIZE & SPICULES CALCIFY;
Dr. Heba Kalbouneh. Saba Alfayoumi. Heba Kalbouneh
 11 Dr. Heba Kalbouneh Saba Alfayoumi Heba Kalbouneh 2- Bone Bone tissue is also classified into primary bone and secondary bone. In the beginning, the first bone that is deposited by the osteoblasts is
11 Dr. Heba Kalbouneh Saba Alfayoumi Heba Kalbouneh 2- Bone Bone tissue is also classified into primary bone and secondary bone. In the beginning, the first bone that is deposited by the osteoblasts is
FORMATION OF BONE. Intramembranous Ossification. Bone-Lec-10-Prof.Dr.Adnan Albideri
 FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice
 Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice Basak Doyran 1, Wei Tong 2, Qing Li 1, Haoruo Jia 2, Xianrong Zhang 3,
Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice Basak Doyran 1, Wei Tong 2, Qing Li 1, Haoruo Jia 2, Xianrong Zhang 3,
contains an antiangiogenesis factor
 CARTILAGE & BONE Cartilage and Bone objectives Student must learn :. What is the meaning of cartilage, and their function, location in human body.. To distinguish the 3 types of cartilage. And their cells,
CARTILAGE & BONE Cartilage and Bone objectives Student must learn :. What is the meaning of cartilage, and their function, location in human body.. To distinguish the 3 types of cartilage. And their cells,
Cartilage. - Cartilage together with long bone form the skeleton and support the body.
 Cartilage - Cartilage is a special type of CT has a firm pliable matrix that can resist mechanical stress, act as a shock absorber. - Cartilage together with long bone form the skeleton and support the
Cartilage - Cartilage is a special type of CT has a firm pliable matrix that can resist mechanical stress, act as a shock absorber. - Cartilage together with long bone form the skeleton and support the
Functions of the Skeletal System. Chapter 6: Osseous Tissue and Bone Structure. Classification of Bones. Bone Shapes
 Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
For more information about how to cite these materials visit
 Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
Why the dog? Analogy of the anatomy
 Why the dog? Analogy of the anatomy Surgically Induced canine OA models: Anterior (cranial) cruciate ligament transection model Pond MJ, Nuki G. Ann Rheum Dis 1973 (and > 100 others) Meniscal disruption
Why the dog? Analogy of the anatomy Surgically Induced canine OA models: Anterior (cranial) cruciate ligament transection model Pond MJ, Nuki G. Ann Rheum Dis 1973 (and > 100 others) Meniscal disruption
Chapter 7. Skeletal System
 Chapter 7 Skeletal System 1 Introduction: A. Bones are very active, living tissues B. Each bone is made up of several types of tissues and so is an organ. C. Bone functions include: muscle attachment,
Chapter 7 Skeletal System 1 Introduction: A. Bones are very active, living tissues B. Each bone is made up of several types of tissues and so is an organ. C. Bone functions include: muscle attachment,
Sheets 16&17. Dr. Heba Kalbouneh. Dr. Heba Kalbouneh. Dr. Heba Kalbouneh
 Sheets 16&17 Dr. Heba Kalbouneh Dr. Heba Kalbouneh Dr. Heba Kalbouneh Ossification (formation of bone) - Osteoblasts are responsible for producing the extracellular matrix of the bone and these osteoblasts
Sheets 16&17 Dr. Heba Kalbouneh Dr. Heba Kalbouneh Dr. Heba Kalbouneh Ossification (formation of bone) - Osteoblasts are responsible for producing the extracellular matrix of the bone and these osteoblasts
Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury
 Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury Bastian OW, Koenderman L, Alblas J, Leenen LPH, Blokhuis TJ. Neutrophils contribute to
Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury Bastian OW, Koenderman L, Alblas J, Leenen LPH, Blokhuis TJ. Neutrophils contribute to
BIOH111. o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system
 BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
Pathophysiology of fracture healing
 Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
Deleterious Effects of Intermittent Recombinant Parathyroid. hormone on cartilage formation in a rabbit microfracture
 HSSJ (2010) 6: 79 84 DOI 10.1007/s11420-009-9134-7 ORIGINAL ARTICLE Deleterious Effects of Intermittent Recombinant Parathyroid Hormone on Cartilage Formation in a Rabbit Microfracture Model: a Preliminary
HSSJ (2010) 6: 79 84 DOI 10.1007/s11420-009-9134-7 ORIGINAL ARTICLE Deleterious Effects of Intermittent Recombinant Parathyroid Hormone on Cartilage Formation in a Rabbit Microfracture Model: a Preliminary
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS
 OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
NOTES: Skeletal System (Ch 5, part 1)
 NOTES: Skeletal System (Ch 5, part 1) Individual bones are the organs of the skeletal system. A bone contains very active tissues. BONE STRUCTURE: *Bone structure reflects its function. Parts of a long
NOTES: Skeletal System (Ch 5, part 1) Individual bones are the organs of the skeletal system. A bone contains very active tissues. BONE STRUCTURE: *Bone structure reflects its function. Parts of a long
Bones. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
 Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
Lecture Overview. Connective Tissues. Marieb s Human Anatomy and Physiology. Chapter 4 Tissues: The Living Fabric Connective Tissues Lecture 10
 Marieb s Human Anatomy and Physiology Marieb Hoehn Chapter 4 Tissues: The Living Fabric Connective Tissues Lecture 10 Lecture Overview General composition and function of connective tissue Components of
Marieb s Human Anatomy and Physiology Marieb Hoehn Chapter 4 Tissues: The Living Fabric Connective Tissues Lecture 10 Lecture Overview General composition and function of connective tissue Components of
Compact bone; Many parallel Haversian canals contain: small blood vessels. very small nerve. Interconnected by Volkmann s canals.
 Special characteristics of COMPACT BONE (dense bone) Thick; well vascularized Osteocytes and lamellae Concentric rings around blood vessels Most bones: outer compact bone inner spongy bone Marrow cavity
Special characteristics of COMPACT BONE (dense bone) Thick; well vascularized Osteocytes and lamellae Concentric rings around blood vessels Most bones: outer compact bone inner spongy bone Marrow cavity
Biology. Dr. Khalida Ibrahim
 Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
Skeletal Tissues Dr. Ali Ebneshahidi
 Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection: Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection: Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
stem cell products Basement Membrane Matrix Products Rat Mesenchymal Stem Cell Growth and Differentiation Products
 stem cell products Basement Membrane Matrix Products Rat Mesenchymal Stem Cell Growth and Differentiation Products Stem Cell Qualified Extracellular Matrix Proteins Stem cell research requires the finest
stem cell products Basement Membrane Matrix Products Rat Mesenchymal Stem Cell Growth and Differentiation Products Stem Cell Qualified Extracellular Matrix Proteins Stem cell research requires the finest
Fig Articular cartilage. Epiphysis. Red bone marrow Epiphyseal line. Marrow cavity. Yellow bone marrow. Periosteum. Nutrient foramen Diaphysis
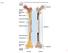 Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Chapter 5 The Skeletal System:Bone Tissue. Functions of Bone. Bones
 Chapter 5 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose,
Chapter 5 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose,
Cartilage-Specific Matrix Protein Chondromodulin-I Is Associated with Chondroid Formation in Salivary Pleomorphic Adenomas
 American Journal of Pathology, Vol. 158, No. 4, April 2001 Copyright American Society for Investigative Pathology Cartilage-Specific Matrix Protein Chondromodulin-I Is Associated with Chondroid Formation
American Journal of Pathology, Vol. 158, No. 4, April 2001 Copyright American Society for Investigative Pathology Cartilage-Specific Matrix Protein Chondromodulin-I Is Associated with Chondroid Formation
Skeletal Tissues. Skeletal tissues. Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs.
 Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
Ultrastructure and Immunolocalization of Transforming Growth Factor-Beta in Chondrification of Murine Ligamentous Fibroblasts and Endochondral
 Aeta Histochem, Cytochena. Vol. 30 No, 4 371-379 (1997) Ultrastructure and Immunolocalization of Transforming Growth Factor-Beta in Chondrification of Murine Ligamentous Fibroblasts and Endochondral Calcification
Aeta Histochem, Cytochena. Vol. 30 No, 4 371-379 (1997) Ultrastructure and Immunolocalization of Transforming Growth Factor-Beta in Chondrification of Murine Ligamentous Fibroblasts and Endochondral Calcification
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
The Skeletal System. Chapter 7a. Skeletal System Introduction Functions of the skeleton Framework of bones The skeleton through life
 The Skeletal System Skeletal System Introduction Functions of the skeleton Framework of bones The skeleton through life Chapter 7a Support Protection Movement Storage areas Minerals Lipids Hemopoiesis
The Skeletal System Skeletal System Introduction Functions of the skeleton Framework of bones The skeleton through life Chapter 7a Support Protection Movement Storage areas Minerals Lipids Hemopoiesis
Osteochondral regeneration. Getting to the core of the problem.
 Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
doi: /jor.20426
 doi: 10.1002/jor.20426 Title Repair of large osteochondral defects with allogeneic cartilaginous aggregates formed from bone marrow-derived cells using RWV bioreactor Tomokazu Yoshioka 1,MD, Hajime Mishima
doi: 10.1002/jor.20426 Title Repair of large osteochondral defects with allogeneic cartilaginous aggregates formed from bone marrow-derived cells using RWV bioreactor Tomokazu Yoshioka 1,MD, Hajime Mishima
CHAPTER 6 LECTURE OUTLINE
 CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
ANATOMY & PHYSIOLOGY - CLUTCH CH. 8 - BONE AND CARTILAGE.
 !! www.clutchprep.com CONCEPT: BONE CLASSIFICATIONS There are four classifications of bones based on their 1. Long bones are greater in length than in width - Found in the upper and lower limbs (ex: arm,
!! www.clutchprep.com CONCEPT: BONE CLASSIFICATIONS There are four classifications of bones based on their 1. Long bones are greater in length than in width - Found in the upper and lower limbs (ex: arm,
Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration.
 Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration. By Linero I., Chaparro O., 2014 Suzana Tufegdzic 1 Background 2 Background Stem Cells: undifferentiated
Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration. By Linero I., Chaparro O., 2014 Suzana Tufegdzic 1 Background 2 Background Stem Cells: undifferentiated
Title. CitationJournal of Bioscience and Bioengineering, 100(1): 12. Issue Date Doc URL. Type. File Information
 Title Effect of chondroitin sulfate and hyaluronic acid on Author(s)Nishimoto, Shohei; Takagi, Mutsumi; Wakitani, Shigey CitationJournal of Bioscience and Bioengineering, 100(1): 12 Issue Date 2005-07
Title Effect of chondroitin sulfate and hyaluronic acid on Author(s)Nishimoto, Shohei; Takagi, Mutsumi; Wakitani, Shigey CitationJournal of Bioscience and Bioengineering, 100(1): 12 Issue Date 2005-07
Bone Tissue- Chapter 5 5-1
 Bone Tissue- Chapter 5 5-1 Bone Functions Support Protection Assistance in movement Mineral storage and release Blood cell production Triglyceride storage 5-2 Bone Chemistry Water (25%) Organic Constituent
Bone Tissue- Chapter 5 5-1 Bone Functions Support Protection Assistance in movement Mineral storage and release Blood cell production Triglyceride storage 5-2 Bone Chemistry Water (25%) Organic Constituent
Skeletal Tissues. Dr. Ali Ebneshahidi
 Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection : Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection : Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Module 2:! Functional Musculoskeletal Anatomy A! Semester 1! !!! !!!! Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb!
 Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Rama Nada. - Mousa Al-Abbadi. 1 P a g e
 - 1 - Rama Nada - - Mousa Al-Abbadi 1 P a g e Bones, Joints and Soft tissue tumors Before we start: the first 8 minutes was recalling to Dr.Mousa s duties, go over them in the slides. Wherever you see
- 1 - Rama Nada - - Mousa Al-Abbadi 1 P a g e Bones, Joints and Soft tissue tumors Before we start: the first 8 minutes was recalling to Dr.Mousa s duties, go over them in the slides. Wherever you see
Osteology. Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College
 Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
LIST OF ORGANS FOR HISTOPATHOLOGICAL ANALYSIS:!! Neural!!!!!!Respiratory:! Brain : Cerebrum,!!! Lungs and trachea! Olfactory, Cerebellum!!!!Other:!
 LIST OF ORGANS FOR HISTOPATHOLOGICAL ANALYSIS:!! Neural!!!!!!Respiratory:! Brain : Cerebrum,!!! Lungs and trachea! Olfactory, Cerebellum!!!!Other:! Spinal cord and peripheral nerves! Eyes, Inner ear, nasal
LIST OF ORGANS FOR HISTOPATHOLOGICAL ANALYSIS:!! Neural!!!!!!Respiratory:! Brain : Cerebrum,!!! Lungs and trachea! Olfactory, Cerebellum!!!!Other:! Spinal cord and peripheral nerves! Eyes, Inner ear, nasal
Development of Bone Canaliculi During Bone Repair
 Development of Bone Canaliculi During Bone Repair K. KUSUZAKI, 1 N. KAGEYAMA, 1 H. SHINJO, 1 H. TAKESHITA, 1 H. MURATA, 1 S. HASHIGUCHI, 1 T. ASHIHARA, 2 and Y. HIRASAWA 1 Departments of 1 Orthopaedic
Development of Bone Canaliculi During Bone Repair K. KUSUZAKI, 1 N. KAGEYAMA, 1 H. SHINJO, 1 H. TAKESHITA, 1 H. MURATA, 1 S. HASHIGUCHI, 1 T. ASHIHARA, 2 and Y. HIRASAWA 1 Departments of 1 Orthopaedic
SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over 3 Weeks. A SEPARATE WORKSHEET WILL BE PROVIDED.
 BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
Anatomy & Physiology Skeletal System
 I. Functions of the Skeletal System A. the body Anatomy & Physiology Skeletal System B. of vital organs C. Provide for movement D. storage (calcium & phosphate) E. cell formation II. Bone Structure A.
I. Functions of the Skeletal System A. the body Anatomy & Physiology Skeletal System B. of vital organs C. Provide for movement D. storage (calcium & phosphate) E. cell formation II. Bone Structure A.
Supplementary Figure 1 The ability to regenerate an ear hole is discontinuous with wound healing. Ear-hole closure at D85 for each sex within each
 Supplementary Figure 1 The ability to regenerate an ear hole is discontinuous with wound healing. Ear-hole closure at D85 for each sex within each species observed. Data show a binary response to a 4 mm
Supplementary Figure 1 The ability to regenerate an ear hole is discontinuous with wound healing. Ear-hole closure at D85 for each sex within each species observed. Data show a binary response to a 4 mm
Most abundant and widely distributed tissues in the body Binds, support, and strengthen body tissues, protect and insulate internal organ, serve as
 Connective tissue Most abundant and widely distributed tissues in the body Binds, support, and strengthen body tissues, protect and insulate internal organ, serve as major transport system, compartmentalizes
Connective tissue Most abundant and widely distributed tissues in the body Binds, support, and strengthen body tissues, protect and insulate internal organ, serve as major transport system, compartmentalizes
physical properties depend on: electrostatic bonds between collagen/elastic fibers and GAGs water bound to negatively charged sulfated GAG chains
 connective/supporting tissue bears mechanical stress without distortion -> shock absorption smooth surface -> facilitates movements of joints guides development of bones chondrocytes extracellular matrix
connective/supporting tissue bears mechanical stress without distortion -> shock absorption smooth surface -> facilitates movements of joints guides development of bones chondrocytes extracellular matrix
Sheet #9. Dr. Heba Kalbouneh. Dr. Heba Kalbouneh. Dr. Heba Kalbouneh
 Sheet #9 Dr. Heba Kalbouneh Dr. Heba Kalbouneh Dr. Heba Kalbouneh Elastic fibers The main function of elastic fibers is to provide elasticity. In other words these fibers are able to restore the original
Sheet #9 Dr. Heba Kalbouneh Dr. Heba Kalbouneh Dr. Heba Kalbouneh Elastic fibers The main function of elastic fibers is to provide elasticity. In other words these fibers are able to restore the original
Spontaneous Repair of Full- Thickness Defects of Articular Cartilage in a Goat Model A PRELIMINARY STUDY
 53 Spontaneous Repair of Full- Thickness Defects of Articular Cartilage in a Goat Model A PRELIMINARY STUDY BY DOUGLAS W. JACKSON, MD, PEGGY A. LALOR, PHD, HAROLD M. ABERMAN, DVM, AND TIMOTHY M. SIMON,
53 Spontaneous Repair of Full- Thickness Defects of Articular Cartilage in a Goat Model A PRELIMINARY STUDY BY DOUGLAS W. JACKSON, MD, PEGGY A. LALOR, PHD, HAROLD M. ABERMAN, DVM, AND TIMOTHY M. SIMON,
CHONDROTOXICITY OF LOCAL ANESTHETIC
 CHONDROTOXICITY OF LOCAL ANESTHETIC Sport Med 2017 Jas Chahal MD FRCSC MSc MBA University of Toronto NO DISCLOSURES Objectives To understand the clinical presentation and pathogenesis of chondrolysis Differentiate
CHONDROTOXICITY OF LOCAL ANESTHETIC Sport Med 2017 Jas Chahal MD FRCSC MSc MBA University of Toronto NO DISCLOSURES Objectives To understand the clinical presentation and pathogenesis of chondrolysis Differentiate
Figure 1. Morphology of a normal furcation area (hematoxylin and eosin [H&E] staining), a Low magnification view of a furcation area.
![Figure 1. Morphology of a normal furcation area (hematoxylin and eosin [H&E] staining), a Low magnification view of a furcation area. Figure 1. Morphology of a normal furcation area (hematoxylin and eosin [H&E] staining), a Low magnification view of a furcation area.](/thumbs/94/120315208.jpg) 905 Errata that were The following figures are four-color representations of figures incorrectly published in black and white in the July and August issues. Immunohistochemical Expression of Extracellular
905 Errata that were The following figures are four-color representations of figures incorrectly published in black and white in the July and August issues. Immunohistochemical Expression of Extracellular
Introduction. Acute sodium overload produces renal tubulointerstitial inflammation in normal rats
 Acute sodium overload produces renal tubulointerstitial inflammation in normal rats MI Roson, et al. Kidney International (2006) Introduction Present by Kanya Bunnan and Wiraporn paebua Tubular sodium
Acute sodium overload produces renal tubulointerstitial inflammation in normal rats MI Roson, et al. Kidney International (2006) Introduction Present by Kanya Bunnan and Wiraporn paebua Tubular sodium
What is bone? Specialized form of connective tissue: mineralized collagen matrix, therefore very rigid and strong while still retaining some degree of
 Bone What is bone? Specialized form of connective tissue: mineralized collagen matrix, therefore very rigid and strong while still retaining some degree of flexibility Other types of connective tissue:
Bone What is bone? Specialized form of connective tissue: mineralized collagen matrix, therefore very rigid and strong while still retaining some degree of flexibility Other types of connective tissue:
Supplementary Material for
 Supplementary Material for Parathyroid Hormone Signaling through Low-density-lipoprotein-related Protein 6 Mei Wan, Chaozhe Yang, Jun Li, Xiangwei Wu, Hongling Yuan, Hairong Ma, Xi He, Shuyi Nie, Chenbei
Supplementary Material for Parathyroid Hormone Signaling through Low-density-lipoprotein-related Protein 6 Mei Wan, Chaozhe Yang, Jun Li, Xiangwei Wu, Hongling Yuan, Hairong Ma, Xi He, Shuyi Nie, Chenbei
Peggers Super Summaries Basic Sciences Bone
 Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
Supplementary Data. Supplementary Methods:
 Supplementary Data Supplementary Methods: Release kinetics of from collagen sponges in vivo. 2μg of human recombinant 165 was labeled with lexafluor 555 (Microscale Protein Labeling Kit; Invitrogen) as
Supplementary Data Supplementary Methods: Release kinetics of from collagen sponges in vivo. 2μg of human recombinant 165 was labeled with lexafluor 555 (Microscale Protein Labeling Kit; Invitrogen) as
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung
 IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
Ossification = Osteogenesis
 Ossification = Osteogenesis Ossification = Osteogenesis Parts of the fetal skeleton form during the first few weeks after conception By the end of the 8 th week, the skeletal pattern is formed : cartilage
Ossification = Osteogenesis Ossification = Osteogenesis Parts of the fetal skeleton form during the first few weeks after conception By the end of the 8 th week, the skeletal pattern is formed : cartilage
Assay Kit for Measurement of Proteoglycan. (Sulfated Glycosaminoglycan Quantification Kit)
 Assay Kit for Measurement of Proteoglycan. (Sulfated Glycosaminoglycan Quantification Kit) Cat. No. 280560-N INTRODUCTION Glycosaminoglycans (GAGs) are a major component of the extracellular matrix (ECM)
Assay Kit for Measurement of Proteoglycan. (Sulfated Glycosaminoglycan Quantification Kit) Cat. No. 280560-N INTRODUCTION Glycosaminoglycans (GAGs) are a major component of the extracellular matrix (ECM)
Mouse C-peptide EIA. Cat. No. YII-YK013-EX FOR LABORATORY USE ONLY
 Mouse C-peptide EIA Cat. No. YII-YK013-EX FOR LABORATORY USE ONLY TOYO 2CHOME, KOTO-KU, TOKYO, 135-0016, JAPAN http://www.cosmobio.co.jp e-mail : export@cosmobio.co.jp Phone : +81-3-5632-9617 FAX : +81-3-5632-9618
Mouse C-peptide EIA Cat. No. YII-YK013-EX FOR LABORATORY USE ONLY TOYO 2CHOME, KOTO-KU, TOKYO, 135-0016, JAPAN http://www.cosmobio.co.jp e-mail : export@cosmobio.co.jp Phone : +81-3-5632-9617 FAX : +81-3-5632-9618
Spontaneous Regression Mechanisms of Lumbar Disc Herniation Role of apoptosis and macrophages during disc tissue resorption
 Spontaneous Regression Mechanisms of Lumbar Disc Herniation Role of apoptosis and macrophages during disc tissue resorption Shigeru Kobayashi, MD,PhD, 1 Riya Kosaka MD,PhD 2, Adam Meir, FRCS, 2 1 Dept.
Spontaneous Regression Mechanisms of Lumbar Disc Herniation Role of apoptosis and macrophages during disc tissue resorption Shigeru Kobayashi, MD,PhD, 1 Riya Kosaka MD,PhD 2, Adam Meir, FRCS, 2 1 Dept.
Introduction and Terminology
 Introduction and Terminology Histology - study of tissues (histo = tissues). Tissue Epithelial Tissue Covers and protects exposed surfaces. Muscle Tissue Skeletal muscle, smooth muscle and cardiac muscle.
Introduction and Terminology Histology - study of tissues (histo = tissues). Tissue Epithelial Tissue Covers and protects exposed surfaces. Muscle Tissue Skeletal muscle, smooth muscle and cardiac muscle.
HISTOLOGY Lecture TWO DR. ASHRAF SAID
 HISTOLOGY Lecture TWO DR. ASHRAF SAID Start Of this lecture TISSUES TISSUE: A DEFINITION A group of connected and interdependent cells that cooperate to perform a specific function CONNECTIVE TISSUE The
HISTOLOGY Lecture TWO DR. ASHRAF SAID Start Of this lecture TISSUES TISSUE: A DEFINITION A group of connected and interdependent cells that cooperate to perform a specific function CONNECTIVE TISSUE The
Basics of Cartilage Restoration Introduction of TruFit
 Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
A. cells that perform related functions and are similar in structure. B. extracellular material - made by cells and secreted into interstitial space
 I. tissue components A. cells that perform related functions and are similar in structure B. extracellular material - made by cells and secreted into interstitial space II. tissue types A. epithelium (e.)
I. tissue components A. cells that perform related functions and are similar in structure B. extracellular material - made by cells and secreted into interstitial space II. tissue types A. epithelium (e.)
Histopathology: healing
 Histopathology: healing These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information that
Histopathology: healing These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information that
Stem Cells and Sport Medicine
 Stem Cells and Sport Medicine Rehal Abbas Bhojani, MD CAQSM Memorial Hermann Medical Group 2014 Sports Medicine Symposium of the Americas Stem cell biology Overview Potential applications of stem cells
Stem Cells and Sport Medicine Rehal Abbas Bhojani, MD CAQSM Memorial Hermann Medical Group 2014 Sports Medicine Symposium of the Americas Stem cell biology Overview Potential applications of stem cells
Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of the Tibia
 Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM
 ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
Dr. Heba Kalbouneh. Dr. Heba Kalbouneh. Dr. Heba Kalbouneh
 Dr. Heba Kalbouneh Dr. Heba Kalbouneh Dr. Heba Kalbouneh Cartilage Cartilage is a special form of connective tissue; it has the same origin of connective tissue (embryonic mesenchyme). It contains cells
Dr. Heba Kalbouneh Dr. Heba Kalbouneh Dr. Heba Kalbouneh Cartilage Cartilage is a special form of connective tissue; it has the same origin of connective tissue (embryonic mesenchyme). It contains cells
Which compound is reponsible for the viscous character of the ground substance?
 1 2 Which type of collagen forms the coarse collagen fibres in dense regular and irregular connective tissues? Which compound is reponsible for the viscous character of the ground substance? 3 Which class
1 2 Which type of collagen forms the coarse collagen fibres in dense regular and irregular connective tissues? Which compound is reponsible for the viscous character of the ground substance? 3 Which class
(A) PCR primers (arrows) designed to distinguish wild type (P1+P2), targeted (P1+P2) and excised (P1+P3)14-
 1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: van Seters M, van Beurden M, ten Kate FJW, et al. Treatment
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: van Seters M, van Beurden M, ten Kate FJW, et al. Treatment
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 6 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 6 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
SKELETAL SYSTEM. Introduction Notes (pt 1)
 SKELETAL SYSTEM Introduction Notes (pt 1) I. INTRODUCTION 1. Bones include active, living tissues: bone tissue, cartilage, dense connective tissue, blood, and nervous tissue. 2. Bones: support and protect
SKELETAL SYSTEM Introduction Notes (pt 1) I. INTRODUCTION 1. Bones include active, living tissues: bone tissue, cartilage, dense connective tissue, blood, and nervous tissue. 2. Bones: support and protect
Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis
 Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis Andreas Panagopoulos MD, PhD Upper Limb & Sports Medicine Orthopaedic Surgeon Assistant Professor, University of Patras Outline Teriparatide
Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis Andreas Panagopoulos MD, PhD Upper Limb & Sports Medicine Orthopaedic Surgeon Assistant Professor, University of Patras Outline Teriparatide
Derived copy of Bone *
 OpenStax-CNX module: m57739 1 Derived copy of Bone * Shannon McDermott Based on Bone by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
OpenStax-CNX module: m57739 1 Derived copy of Bone * Shannon McDermott Based on Bone by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
Tissue renewal and Repair. Nisamanee Charoenchon, PhD Department of Pathobiology, Faculty of Science
 Tissue renewal and Repair Nisamanee Charoenchon, PhD Email: nisamanee.cha@mahidol.ac.th Department of Pathobiology, Faculty of Science Topic Objectives 1. Describe processes of tissue repair, regeneration
Tissue renewal and Repair Nisamanee Charoenchon, PhD Email: nisamanee.cha@mahidol.ac.th Department of Pathobiology, Faculty of Science Topic Objectives 1. Describe processes of tissue repair, regeneration
