Posttraumatic boutonnière and
|
|
|
- Madeline Stevenson
- 5 years ago
- Views:
Transcription
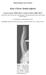
1 Review Article Posttraumatic Boutonnière and Swan Neck Deformities Kathleen E. McKeon, MD Donald H. Lee, MD Abstract Boutonnière and swan neck deformities of the finger can be the result of trauma. The complex anatomy of the extensor mechanism of the finger makes understanding the pathomechanics of these deformities challenging. These posttraumatic deformities should not be confused with those associated with inflammatory arthritis because the treatment options are often very different. An accurate clinical assessment is essential for selecting the appropriate treatment method. Physical examination, including Elson and intrinsic-plus tests, and plain radiography are important tools for diagnosis. A variety of nonsurgical and surgical treatment modalities can be used to restore the motion of the proximal and distal interphalangeal joints and rebalance the forces across these joints. An understanding of the anatomy, clinical presentation, treatment options, and expected outcomes is crucial for optimal treatment of posttraumatic boutonnière and swan neck deformities. From the Andrews Sports Medicine and Orthopaedic Center, Birmingham, AL (Dr. McKeon) and the Vanderbilt Orthopedic Institute, Nashville, TN (Dr. Lee). Dr. Lee or an immediate family member is a member of a speakers bureau or has made paid presentations on behalf of, serves as a paid consultant to, and has received research or institutional support from Biomet; and serves as a board member, owner, officer, or committee member of the American Academy of Orthopaedic Surgeons and the American Society for Surgery of the Hand. Neither Dr. McKeon nor any immediate family member has received anything of value from or has stock or stock options held in a commercial company or institution related directly or indirectly to the subject of this article. J Am Acad Orthop Surg 2015;23: JAAOS-D Copyright 2015 by the American Academy of Orthopaedic Surgeons. Posttraumatic boutonnière and swan neck deformities are complex clinical problems that are often poorly understood. A boutonnière deformity consists of flexion of the proximal interphalangeal (PIP) joint and hyperextension of the distal interphalangeal (DIP) joint. The anatomy and pathophysiology of this deformity was described by Hauck 1 in 1923, and is discussed in detail here. A swan neck deformity consists of hyperextension of the PIP joint and flexion of the DIP joint. Although swan neck deformity was first described in the setting of inflammatory arthritis, posttraumatic swan neck deformity has been recognized for nearly a century. Watson-Jones 2 described a swan neck deformity that resulted from a chronic disruption of the terminal tendon insertion at the distal phalanx (ie, mallet finger). Portis 3 described a swan neck deformity caused by a hyperextension injury of the PIP joint. Patients present to hand surgery clinics with a broad spectrum of acute, chronic, supple, and fixed boutonnière and swan neck deformities that requirearangeoftreatment. Anatomy An understanding of the anatomy and mechanics of the extensor mechanism of the finger is crucial to management of boutonnière and swan neck deformities 4-7 (Figure 1 and Table 1). The three muscles that contribute to the extensor mechanism of the finger are the extensor digitorum communis (EDC), the lumbrical, and the dorsal interosseous. The EDC is stabilized by the radial and ulnar sagittal bands as it crosses the metacarpophalangeal (MP) joint. The sagittal bands arise from the EDC tendon dorsally and travel transversely to insert on the October 2015, Vol 23, No
2 Posttraumatic Boutonnière and Swan Neck Deformities Figure 1 Illustrations of the radial (A) and dorsal (B) views of the finger demonstrating the anatomy of the extensor mechanism. A = common extensor tendon, B = sagittal band, C = transverse fibers, D = oblique fibers, E = conjoint lateral band, F = terminal tendon, G = flexor digitorum profundus tendon, H = dorsal interosseous muscle belly, I = lumbrical muscle belly, J = flexor digitorum superficialis tendon, K = medial tendon of the superficial head of the interosseous muscle, L = lateral tendon of the deep head of the interosseous muscle, M = flexor pulley, N = oblique retinacular ligament, O = transverse retinacular ligament, P = medial band of oblique fibers, Q = central slip, R = lateral slips, S = triangular ligament volar plate of the MP joint and the volar periosteum of the proximal phalanx (P1). In addition to stabilizing the EDC tendon, the sagittal bands help to extend the MP joint through a lasso effect. After crossing the MP joint, the EDC tendon trifurcates into a central slip and two lateral slips. The central slip inserts onto the dorsal base of the middle phalanx (P2) and extends the PIP joint. The two lateral slips travel radially and ulnarly to join their respective conjoint lateral bands. The lumbrical muscle originates on the flexor digitorum profundus tendon and is located on the radial aspect of the finger only. The lumbrical tendon passes volar to the deep intermetacarpal ligament at the level of the MP joint. Distally, the lumbrical tendon gives off contributions to the oblique fibers overlying the distal aspect of the P1. The oblique fibers join the medial bands of the interosseous and, with the central slip, extend the PIP joint. The lumbrical tendon terminates in the conjoint lateral band. The dorsal interosseous contribution to the extensor mechanism is arguably the most complex of the three muscles that contribute to the extensor mechanism. 4-7 The anatomy of first dorsal interosseous muscle varies slightly from that of other interosseous muscles 1 but, in general, the dorsal interosseous muscles are divided into two muscle bellies, the superficial and the deep heads. 8 The superficial head gives rises to the medial tendon, which passes deep to the sagittal band and inserts on the base of the P1. The medial tendon abducts the digit. The deep head gives rise to the lateral tendon, which passes superficial to the sagittal band. Distally, the lateral tendon gives off contributions to the transverse fibers over the middle aspect of P1, which flex the MP joint. Distal to the transverse fibers, the lateral tendon gives off contributions to the oblique fibers and the medial band of the interosseous, which extend the PIP joint. The lateral tendon then joins with the lateral slip of the EDC and the lumbrical tendon to form the conjoint lateral band. Distal to the PIP joint, the radial and ulnar conjoint lateral bands are anchored dorsally by the triangular ligament and volarly by the transverse retinacular ligament, preventing volar and dorsal subluxation of the conjoint lateral 624 Journal of the American Academy of Orthopaedic Surgeons
3 Kathleen E. McKeon, MD, and Donald H. Lee, MD Table 1 Extensor Mechanism Anatomy Structure Origin Insertion Action Common extensor tendon EDC muscle belly Central slip and lateral slip MP extension, PIP extension Sagittal band EDC tendon Volar plate of MP joint MP extension, stabilizes EDC tendon Transverse fibers Lateral tendon of deep head of interosseous EDC tendon MP flexion Oblique fibers Conjoint lateral band Lateral tendon of deep head of interosseous and lumbrical tendon Confluence of lateral tendon of deep head of the interosseous, lumbrical tendon, lateral slips Medial band of oblique fibers Terminal tendon PIP extension DIP extension Terminal tendon Conjoint lateral bands Distal phalanx DIP extension FDP tendon FDP muscle belly Distal phalanx DIP flexion Dorsal interosseous muscle Metacarpal Medial and lateral tendons MP flexion and abduction belly Lumbrical muscle belly FDP tendon Oblique fibers, radial lateral PIP and DIP extension band FDS tendon FDS muscle belly Middle phalanx PIP flexion Medial tendon of superficial head of interosseous Lateral tendon of deep head of interosseous Flexor pulley Superficial head of interosseous Lateral tubercle of base of proximal phalanx MP abduction Deep head of interosseous Transverse fibers MP flexion Volar metacarpal, phalanges, volar plates Volar metacarpal, phalanges, volar plates Prevents bowstringing, allows smooth gliding Oblique retinacular ligament Flexor sheath Terminal tendon Links PIP and DIP motion Transverse retinacular ligament Flexor sheath Conjoint lateral bands Prevents dorsal subluxation of conjoint lateral bands Medial band of oblique fibers Oblique fibers Dorsolateral tubercle of PIP extension middle phalanx Central slip EDC tendon Dorsal base of middle PIP extension phalanx Lateral slips EDC tendon Conjoint lateral bands DIP extension Triangular ligament Central slip (proximally), conjoint lateral bands (laterally) Terminal tendon (at apex) Prevents volar subluxation of lateral bands DIP = distal interphalangeal, EDC = extensor digitorum communis, FDP = flexor digitorum profundus, FDS = flexor digitorum superficialis, MP = metacarpophalangeal, PIP = proximal interphalangeal bands, respectively. Overlying the distal aspect of the P2, the radial and ulnar conjoint lateral bands come together to form the terminal tendon. The terminal tendon inserts into the base of the distal phalanx and extends the DIP joint. The oblique retinacular ligament is a controversial structure, but most studies report that it attaches to the flexor sheath proximally and the terminal tendon distally. 4-7 It passes dorsal to the axis of the DIP joint and volar to the axis of the PIP joint, linking the action of the DIP and PIP joints. As the PIP joint extends, the oblique retinacular ligament tightens and transmits force across the terminal tendon, resulting in DIP extension. Boutonnière Deformity Pathomechanics As mentioned earlier, a boutonnière deformity is a flexion deformity at the PIP joint and a hyperextension deformity at the DIP joint (Figure 2). It is the result of a disruption of the central slip and triangular ligament October 2015, Vol 23, No
4 Posttraumatic Boutonnière and Swan Neck Deformities Figure 2 Photograph of the fingers demonstrating a boutonnière deformity of the long finger. on the dorsum of the finger. Common mechanisms of injury include blunt trauma, an open laceration, or a volar dislocation of the PIP joint. 9,10 An injury to the central slip and triangular ligament allows the conjoint lateral bands to subluxate volarly with PIP flexion. Over time, a PIP joint extension lag develops. Without prompt treatment, the PIP extension lag becomes a fixed flexion deformity, causing the lateral bands to become permanently subluxated volarly. The injury to the central slip and triangular ligament also allows the lateral bands to migrate proximally because of the loss of the tethering effect of the central slip. As the lateral bands subluxate volarly, they migrate further proximally secondary to the pull of the lumbrical and interosseous muscles. This leads to increased tension on the terminal tendon and hyperextension at the DIP joint. A true boutonnière deformity should not be confused with a pseudo deformity, in which a hyperextension injury to the PIP joint leads to a PIP flexion contracture In a pseudo deformity, the central slip and triangular ligament remain competent, and the DIP joint retains full mobility. The flexion contracture is caused by scarring of the volar plate and joint capsule rather than by a derangement of the Figure 3 Photograph of the hand demonstrating the Elson test. The clinician holds the proximal interphalangeal joint in 90 of flexion as the patient tries to extend the distal interphalangeal joint. extensor mechanism. Although they both have a similar clinical presentation, distinguishing between these two entities by using clinical examination tests, including the Elson and Boyes tests, is important because the appropriate treatment options are different for a pseudo deformity. Treatment of a pseudo deformity involves early, aggressive motion, whereas treatment of a true boutonnière deformity involves a period of immobilization. Clinical Evaluation and Classification Several signs can lead the examiner to suspect an injury to the extensor mechanism in a patient with an injury to the PIP joint. The Elson test is the most reliable maneuver for diagnosis of an acute boutonnière injury. 15,16 The examiner holds the PIP joint in 90 of flexion and instructs the patient to actively extend the DIP joint. With an intact extensor mechanism, holding the PIP joint in 90 of flexion causes slack in the lateral bands as they are held distally by their attachments to the central slip. The patient is unable to generate any extension power at the DIP joint. With a boutonnière injury, flexion of the PIP joint does not advance the lateral bands distally secondary to disruption of the central slip. Tension is generated in the terminal tendon because of the disrupted central slip. Therefore, the patient is able to generate an abnormal amount of active extension at the DIP joint with the PIP joint held in flexion (Figure 3). It may be necessary to perform a digital block before the Elson test is done to allow an accurate assessment. Another useful clinical maneuver is the Boyes test, which is used to assess the patient s ability to actively flex the DIP joint with the PIP joint held in extension. Patients with an intact extensor mechanism should be able to fully and actively flex the DIP joint. Patients with contracted lateral bands will have decreased active flexion at the DIP joint when the PIP joint is held in extension. This test may not be positive in an acute setting. 17 Plain radiographs of the finger should be obtained in patients with an injury to the PIP joint. Radiography may demonstrate subtle DIP hyperextension that can be difficult to detect with a clinical examination alone. Central slip avulsions may involve a bony fragment, which can alter treatment. In general, advanced imaging modalities are not needed for diagnosis of boutonnière deformity. Chronic boutonnière deformities are categorized using the Burton classification (Table 2). 18 This classification system is based on clinical examination findings and the radiographic appearance of the PIP joint. Nonsurgical Management For patients who present with an acute, closed boutonnière injury 626 Journal of the American Academy of Orthopaedic Surgeons
5 Kathleen E. McKeon, MD, and Donald H. Lee, MD (Burton stage I), nonsurgical management is generally recommended; this consists of splinting the PIP joint in extension for 4 to 8 weeks to allow the central slip to heal. Active DIP flexion exercises are performed multiple times daily to pull the lateral bands dorsally and to counteract the proximal migration of the lateral bands. After 4 to 8 weeks of full-time splinting, PIP flexion exercises are introduced, but the PIP extension splint is worn at night for an additional 4 to 6 weeks. 10 Chronic, fixed boutonnière deformities (Burton stage II) are often amenable to nonsurgical management, as long as full passive PIP extension can be achieved with a therapy protocol. Full passive PIP extension is achieved with serial casting or dynamic splinting over a period of 6 to 12 weeks. Active DIP flexion exercises are a critical part of the therapy protocol in this situation, as well. Once full passive PIP extension is achieved, it is maintained with extension splinting for 6 to 12 weeks, followed by a protocol to gradually resume PIP flexion. Table 2 Burton Classification of Boutonnière Deformity 18 Stage I II III IV Description Supple, passively correctable deformity Fixed contracture, contracted lateral bands, no joint involvement Volar plate and collateral ligament contractures, intra-articular fibrosis Volar plate and collateral ligament contractures, intra-articular fibrosis plus proximal interphalangeal joint arthritis Table 3 Burton s Principles for Treatment of Chronic Boutonnière Deformity 18 Surgical treatment of boutonnière deformities should be done only by experienced hand surgeons. Surgical treatment is rarely necessary for supple boutonnière deformities. Preoperative and postoperative therapy programs are an essential part of surgical treatment. Tendon procedures should be done after full passive PIP joint extension has been achieved. Procedures may need to be staged, with tendon rebalancing following a PIP contracture release. If arthritic change is present, tendon rebalancing should be combined with implant arthroplasty or arthrodesis. Flexor function should not be jeopardized in an attempt to achieve full extension. All procedures involve rebalancing the extensor mechanism to divert force from the DIP joint to the PIP joint. DIP = distal interphalangeal, PIP = proximal interphalangeal Surgical Management Acute Boutonnière Deformity Surgical intervention is occasionally necessary for boutonnière deformities. In patients with acute, closed injuries (Burton stage I) that are not amenable to full-time PIP extension splinting, pinning of the PIP joint may be beneficial. The PIP joint is extended, effectively reducing the lateral bands, and a inch Kirschner wire is placed across the joint. The wire is left in place for 4 to 6 weeks and then removed, followed by initiation of PIP flexion exercises. 10 Patients with acute, open boutonnière injuries often have joint involvement and may benefit from irrigation and débridement in the operating room. At the time of débridement, a primary repair of the central slip can be performed or the slip can be reattached to the base of the P2 with a bone anchor or through bone tunnels. After repair of the central slip, the PIP joint is pinned in extension for 6 weeks to protect the repair. Bony avulsions of the central slip may also warrant surgical management in the acute setting. Although patients with small bony fragments may be managed nonsurgically as described earlier, larger bony fragments require fixation to the base of the P2 with Kirschner wires or screws. Other factors, such as chronicity, displacement, and patient compliance, should also be considered. The decision to treat a bony boutonnière injury surgically or nonsurgically is best left to an experienced hand surgeon. Chronic Boutonnière Deformity Surgical management of chronic boutonnière deformities should be approached with caution. Seven principles for management of a chronic boutonnière deformity described by Burton 18 are outlined in Table 3. Patients with a boutonnière deformity generally retain full flexion and grip strength and have few functional limitations. Surgical intervention may lead to extension contractures of the PIP joint and poor functional outcomes. Prior to undertaking any surgical reconstruction, it is imperative to thoroughly discuss the risks and expected outcomes with the patient. October 2015, Vol 23, No
6 Posttraumatic Boutonnière and Swan Neck Deformities Table 4 Etiology of Posttraumatic Boutonnière and Swan Neck Deformities Figure 4 Deformity Boutonnière Swan neck Etiology Disruption of central slip and triangular ligament Extrinsic Disruption of terminal tendon (mallet) Wrist or MP joint flexion contracture Intrinsic Chronic MP volar subluxation Ischemic contracture Tendon adhesion Articular Volar plate/capsule injury (hyperextension) Disruption of FDS Photograph of the ring finger demonstrating a swan neck deformity in the setting of a chronic mallet deformity. FDS = flexor digitorum superficialis, MP = metacarpophalangeal If a patient wishes to proceed with surgical correction of a chronic boutonnière deformity, the first step is to achieve full passive PIP joint extension with a preoperative therapy program that includes splinting or casting, a dynamic external fixator, or an open joint contracture release. Once full passive PIP joint extension has been achieved, several tendon rebalancing procedures can be used. The simplest tendon rebalancing procedure is a terminal tendon tenotomy (ie, distal Fowler or Dolphin tenotomy). 19,20 By dividing the terminal tendon, the hyperextension force on the DIP joint is removed. The extensor mechanism retracts, allowing for more force to be transmitted to the PIP joint and decreasing the PIP extensor lag. Postoperatively, a DIP extension splint is worn at all times for 6 to 8 weeks, except during range-ofmotion (ROM) exercises. The tendon rebalancing technique developed by Littler and Eaton 21 can also be used. Through a dorsal incision, the lateral bands are sharply released from the lumbrical muscle contribution and the oblique retinacular ligament. The lateral bands are then mobilized dorsally and sutured together in the midline, distal to the PIP joint. This effectively diverts all active extension power (extrinsic and intrinsic) to the PIP joint, while maintaining DIP extension through the action of the preserved oblique retinacular ligament. Curtis et al 22 described a staged reconstruction performed with local anesthesia to allow accurate assessment of active motion intraoperatively. In the first stage, an extensor tenolysis is performed through a dorsal incision. If full active extension is present at this point, the procedure is complete. If an extensor lag remains, then the transverse retinacular ligaments are transected, allowing the lateral bands to swing dorsally. Active extension is reassessed. If full active extension is present, then the procedure is complete. If an extensor lag,20 remains, then a Fowler tenotomy is performed. If an extensor lag.20 remains after the transverse retinacular ligaments are transected, then the central tendon is dissected free and advanced 4 to 6 mm into a drill hole at the base of the P2. 23 The slackened lateral bands can then be loosely sutured dorsally to the central tendon to augment the tendon advancement. Occasionally, the central slip is attenuated and a reconstructive procedure, such as a turndown procedure, is required. Finally, for patients with arthritic change and pain at the PIP joint associated with a long-standing boutonnière deformity, an arthrodesis is the procedure of choice. Swan Neck Deformity Etiology Unlike a boutonnière deformity, which is the result of an injury to the central slip and triangular ligament, a posttraumatic swan neck deformity can result from a variety of initial injuries Zancolli 26 classified these injuries into three categories: extrinsic, intrinsic, and articular (Table 4). Extrinsic causes of swan neck deformities are the result of excessive extension force on the P2. In the setting of a flexible PIP joint, hyperextension develops over time, with chronic extension force. For example, disruption of the terminal tendon (eg, a mallet finger injury) allows the lateral bands to migrate proximally, increasing the extension force on the P2 (Figure 4). Posttraumatic wrist or MP joint flexion contractures also increase the tension on the EDC tendon, increasing the extensor force on the P2 and leading to deformity over time. 628 Journal of the American Academy of Orthopaedic Surgeons
7 Kathleen E. McKeon, MD, and Donald H. Lee, MD The intrinsic causes of swan neck deformities are related to tightness of the intrinsic muscles, or an intrinsicplus finger. Chronic volar subluxation of the MP joint (either posttraumatic or the result of inflammatory arthritis) can lead to tightening of the intrinsic muscles over time. Other mechanisms include ischemic contractures that develop after compartment syndrome of the hand and intrinsic tendon adhesions. Articular causes of swan neck deformity include injury to or degeneration of the volar structures of the PIP joint. This can be the result of a posttraumatic injury, inflammatory arthritis, or generalized hyperlaxity. Hyperextension injury to the PIP joint can lead to disruption of the volar plate and volar capsule, which can lead to chronic insufficiency of the volar structures if not appropriately treated. The flexor digitorum superficialis (FDS) tendon also serves as a palmar stabilizer of the PIP joint; therefore FDS disruptions can also lead to PIP hyperextension deformity over time. Clinical Evaluation and Classification A careful history and physical examination can help the clinician determine the etiology of the swan neck deformity. A history of prior injuries (eg, mallet injury, FDS tendon laceration, PIP joint hyperextension injury) makes determining the etiology straightforward. In the absence of a known injury, physical examination and imaging can aid in diagnosis. Some persons with ligamentous laxity are able to hold their fingers in a swan neck posture naturally, but they rarely have any functional limitations. The physical examination should start by assessing the patient for signs of inflammatory arthritis, such as the involvement of multiple joints in the hands and wrists because the treatment Table 5 Classification System for Swan Neck Deformity Type Characteristics I II III IV Full range of motion, no intrinsic tightness, no functional limitations Intrinsic tightness Stiff PIP in all positions of the MP joint, joint space preserved Severe arthritic change MP = metacarpophalangeal, PIP = proximal interphalangeal recommendations for a posttraumatic swan neck deformity are significantly different than those for a swan neck deformity associated with autoimmune synovitis. If signs of inflammatory arthritis are present, a referral to a rheumatologist is indicated. The flexibility of the DIP, PIP, and MP joints should be assessed with active and passive motion. The integrity of the FDS tendon should be assessed, as well. The Bunnell test can be used to assess the flexibility and tightness of the intrinsic muscles. 27 Because the intrinsic tendons pass volar to the MP joint axis of rotation, they are relaxed and tensioned with MP joint flexion and extension, respectively. Conversely, because the intrinsic tendons pass dorsal to the PIP joint axis of rotation, they are relaxed with PIP joint extension and tensioned with PIP joint flexion. If the intrinsic muscles are excessively tight, holding the MP joint in extension will tighten the intrinsic tendons even further and increase the extension force across the PIP joint. Therefore, a patient with intrinsic muscle tightness will have a decrease in passive and active flexion of the PIP joint with the MP joint held in extension. Radiography is an important part of the clinical assessment of swan neck deformity. The presence of fractures (eg, bony mallet, avulsion fracture of the PIP volar plate) may change the treatment plan, particularly if the fragment is large enough to undergo open reduction and internal fixation. The presence of arthritis will change the treatment recommendations, as well. Advanced imaging (eg, MRI, CT) is rarely indicated. The classification of swan neck deformities is based on the ROM of the PIP joint and radiographic findings. This classification system can serve as the basis for treatment recommendations 10 (Tables 5 and 6). Nonsurgical Management For patients with mild swan neck deformities and full active flexion of the PIP joint, nonsurgical management is often indicated. These patients often report difficulty initiating flexion from the hyperextended posture. They may also report snapping of the lateral bands, which occurs when the dorsally subluxated lateral bands reduce volarly as the finger moves from hyperextension to flexion. A silver ring splint or other functional splint that limits PIP hyperextension while allowing full flexion can limit these symptoms. These splints are low profile, easy to wear, and aesthetically pleasing 28 (Figure 5). Surgical Management For patients with mild deformity who do not wish to wear a splint or those with more severe deformity, surgery is indicated. The choice of procedure is based on the severity of the October 2015, Vol 23, No
8 Posttraumatic Boutonnière and Swan Neck Deformities Table 6 Management Options for Swan Neck Deformity Type Metacarpophalangeal Joint Proximal Interphalangeal Joint Distal Interphalangeal Joint I None Splint, a procedure to limit hyperextension, including FDS tenodesis, oblique retinacular ligament reconstruction, lateral band translocation, dermadesis, volar plate repair (if the etiology is a volar plate injury) II III IV Intrinsic release, reconstruction as needed Intrinsic release, reconstruction as needed Intrinsic release, reconstruction as needed Procedure to limit hyperextension (see type I) Stepwise approach beginning with PIP joint manipulation and then a skin release or lateral band mobilization, if needed. At the conclusion of procedure, flexor tendon gliding is checked. Once full PIP motion present, a procedure to limit hyperextension (see type I) can be performed. Arthroplasty combined with procedure to limit hyperextension (see type I), arthrodesis Nonsurgical management, arthrodesis Nonsurgical management, arthrodesis Nonsurgical management, arthrodesis Nonsurgical management, arthrodesis FDS = flexor digitorum superficialis, PIP = proximal interphalangeal Figure 5 Photograph of a silver ring splint used for management of swan neck deformity. deformity. For patients with type I deformities and full ROM of the PIP joint, soft-tissue procedures are indicated to limit hyperextension of the PIP joint. These procedures can be combined with an arthrodesis of the DIP joint if the flexion contracture of the DIP joint is severe. Several soft-tissue procedures have been used to limit hyperextension of the PIP joint. The most widely used technique is the FDS tenodesis, or FDS sling technique. 29 Through a volar zig-zag incision, a window is made in the flexor sheath on either side of the A3 pulley. One slip of FDS is incised approximately 1.5 cm from its insertion, leaving the distal attachment intact. The PIP joint is flexed 20 to 30, and the detached FDS slip is fixed proximally to the bone with an anchor, or it is sutured to the distal edge of the A2 pulley, forming a static tether to PIP hyperextension. Postoperatively, the joint is splinted in 30 of flexion for 3 weeks. At 3 weeks, active flexion is initiated, but extension block splinting is continued to prevent hyperextension for at least an additional 3 weeks. Oblique retinacular ligament reconstruction is another technique used to address hyperextension of the PIP joint The ulnar lateral band is freed from the extensor mechanism and incised proximally, leaving the distal insertion intact. The lateral band is then transposed volar to the Cleland ligaments to bring it volar to the axis of rotation of the PIP joint. The lateral band is passed to the opposite side of the finger and sutured to the flexor tendon sheath, with the PIP joint held in 30 of flexion. In theory, this reconstruction should correct the PIP hyperextension by providing a static tether as well as increasing the extension force on the DIP joint to correct the DIP flexion deformity. In practice, however, the terminal tendon is often attenuated and incompetent, so the DIP joint deformity is rarely completely corrected with this method. Alternatively, the oblique retinacular ligament can be reconstructed using an autologous tendon graft. 33 When a disruption of the volar plate was the initial injury that led to the swan neck deformity, a direct repair of the volar plate is indicated Volar plate repair can be done through a volar incision, using bone anchors or drill holes in the base of the P2. Lateral band translocation and dermadesis have also been used to manage mild swan neck deformities. 26,37 These procedures can be 630 Journal of the American Academy of Orthopaedic Surgeons
9 Kathleen E. McKeon, MD, and Donald H. Lee, MD done alone or in conjunction with one of the procedures described earlier. For patients with a type II swan neck deformity with intrinsic tightness, an intrinsic release should be combined with one of the procedures described earlier to address PIP hyperextension. An intrinsic release is performed through a dorsoulnar longitudinal incision over the P1. The structures of the extensor mechanism are identified. The lateral band and oblique fibers are incised at the level of the distal half of the P1, with care taken to leave intact the central slip, the lateral slips of the extensor tendon, and the transverse fibers. 38,39 For patients with a type III swan neck deformity, full passive ROM of the PIP joint must be restored before addressing the deformity. This can be done with a stepwise approach, starting with a closed gentle manipulation of the PIP joint, with the goal of achieving 80 to 90 of flexion. If motion is restored, but the dorsal skin is blanched and at risk of necrosis, a skin release can be done. The skin release is performed distal to the joint, with an oblique incision made over the P2. The skin is allowed to heal by secondary intention. If a closed manipulation does not restore adequate motion, an open release of the lateral bands is performed by making two parallel incisions on either side of the central slip, allowing the lateral bands to move volarly. 24 After passive PIP flexion is restored with any of these methods, flexor tendon gliding should be assessed to ensure that no secondary adhesions of the flexor tendons are present. This can be done by assessing active motion if the surgery is performed under local anesthesia or by making an incision in the palm and pulling direct traction on the flexor tendons. Once adequate PIP joint motion has been achieved and smooth flexor tendon gliding has been ensured, any of the previously described procedures to address PIP hyperextension can be performed. Typically, an intrinsic release is necessary. For patients with a type IV swan neck deformity, the PIP joint should be addressed with arthroplasty or arthrodesis. If arthroplasty is performed, it is necessary to address the soft-tissue balancing around the joint with a procedure to limit PIP hyperextension. The decision between arthroplasty and arthrodesis depends on many variables and should be made on a case-by-case basis for each patient. Summary Determining the appropriate course of treatment for each patient with a posttraumatic boutonnière or swan neck deformity requires the clinician to have a thorough understanding of the anatomy of the extensor mechanism, the etiology of the deformity, the available nonsurgical management modalities, and the techniques for surgical correction. The clinician should work with the patient to elucidate any functional limitations and to ensure that he or she maintains realistic expectations. References Evidence-based Medicine: Levels of evidence are described in the table of contents. In this article, reference 28 is a level II study. References 11, 13, 14, 16, 19, 20, 22, 23, 29-33, and are level IV studies. References 3, 8, 12, 16, 21, 27, 30, and 34 are level V expert opinion. References printed in bold type are those published within the past 5 years. 1. Hauck G: Die Ruptur der Dorsalaponeurose am ersten Interphalangealgelenk, zugleich ein Beitrag zur Anatomic und Physiologie der Dorsalaponeurose. Arch Klin Chirurgie 1923;123: Watson-Jones R: Fractures and Joint Injuries, ed 3. Baltimore, MD, Williams and Wilkins Co, 1943, p Portis RB: Hyperextensibility of the proximal interphalangeal joint of the finger following trauma. J Bone Joint Surg Am 1954;36(6): Smith RJ: Balance and kinetics of the fingers under normal and pathological conditions. Clin Orthop Relat Res 1974;104: Smith RJ: Intrinsic muscles of the fingers: Function, dysfunction, and surgical reconstruction. AAOS Instructional Course Lectures Volume 26, Rosemont, IL, American Academy of Orthopaedic Surgeons, 1975, pp Landsmeer JM: The anatomy of the dorsal aponeurosis of the human finger and its functional significance. Anat Rec 1949;104 (1): Tubiana R, Valentin P: The physiology of the extension of the fingers. Surg Clin North Am 1964;44: Masquelet AC, Salama J, Outrequin G, Serrault M, Chevrel JP: Morphology and functional anatomy of the first dorsal interosseous muscle of the hand. Surg Radiol Anat 1986;8(1): Souter WA: The problem of boutonniere deformity. Clin Orthop Relat Res 1974; 104: Strauch RJ: Extensor tendon injury, in Wolfe SW, Hotchkiss RN, Pederson WC, Kozin SH, eds: Green s Operative Hand Surgery, ed 6. Philadelphia, PA, Elsevier, 2011, vol 1, pp McCue FC, Honner R, Gieck JH, Andrews J, Hakala M: A pseudoboutonniere deformity. Hand 1975;7(2): Rothwell AG: The pseudo-boutonniere deformity. NZMedJ1979;89(628): McCue FC, Honner R, Johnson MC, Gieck JH: Athletic injuries of the proximal interphalangeal joint requiring surgical treatment. J Bone Joint Surg Am 1970;52 (5): Bowers WH: The proximal interphalangeal joint volar plate: II. A clinical study of hyperextension injury. J Hand Surg Am 1981;6(1): Rubin J, Bozentka DJ, Bora FW: Diagnosis of closed central slip injuries: A cadaveric analysis of non-invasive tests. J Hand Surg Br 1996;21(5): Elson RA: Rupture of the central slip of the extensor hood of the finger: A test for early diagnosis. J Bone Joint Surg Br 1986;68(2): Boyes JH: Bunnell s Surgery of the Hand, ed 5. Philadelphia, PA, Lippincott, 1970, p 393. October 2015, Vol 23, No
10 Posttraumatic Boutonnière and Swan Neck Deformities 18. Burton RI: Extensor tendons-late reconstruction, in Green DP, ed: Operative Hand Surgery. New York, NY, ChurchillLivingstone,1988,pp Meadows SE, Schneider LH, Sherwyn JH: Treatment of the chronic boutonniere deformity by extensor tenotomy. Hand Clin 1995;11(3): Stern PJ: Extensor tenotomy: A technique for correction of posttraumatic distal interphalangeal joint hyperextension deformity. J Hand Surg Am 1989;14(3): Littler JW, Eaton RG: Redistribution of forces in the correction of Boutonniere deformity. J Bone Joint Surg Am 1967;49 (7): Curtis RM, Reid RL, Provost JM: A staged technique for the repair of the traumatic boutonniere deformity. J Hand Surg Am 1983;8(2): Caroli A, Zanasi S, Squarzina PB, Guerra M, Pancaldi G: Operative treatment of the post-traumatic boutonnière deformity: A modification of the direct anatomical repair technique. J Hand Surg Br 1990;15(4): Feldon P, Terrono AL, Nalebuff EA, Millender LH: Rheumatoid arthritis and other connective tissue disease, in Wolfe SW, Hotchkiss RN, Pederson WC, Kozin SH, eds: Green s Operative Hand Surgery, ed 6. Philadelphia, PA, Elsevier, 2011, vol 2, pp Dreyfus JN, Schnitzer TJ: Pathogenesis and differential diagnosis of the swan-neck deformity. Semin Arthritis Rheum 1983;13 (2): Zancolli E: Structural and Dynamic Bases of Hand Surgery, ed 2. Philadelphia, PA, Lippincott, 1979, pp 64-79, Bunnell S: Ischaemic contracture, local, in the hand. J Bone Joint Surg Am 1953;35(1): van der Giesen FJ, Nelissen RG, van Lankveld WJ, et al: Swan neck deformities in rheumatoid arthritis: A qualitative study on the patients perspectives on hand function problems and finger splints. Musculoskeletal Care 2010;8(4): Catalano LW III, Skarparis AC, Glickel SZ, et al: Treatment of chronic, traumatic hyperextension deformities of the proximal interphalangeal joint with flexor digitorum superficialis tenodesis. J Hand Surg Am 2003;28(3): Ahmed HA, Goldie BS: Proximal interphalangeal joint instability: A dynamic technique for stabilization. J Hand Surg Br 2002;27(4): Ko JH, Kalainov DM, Hsu LP, Fang RC, Mastey RD: Double lateral band transfer for treatment of traumatic hyperextension instability of the proximal interphalangeal joint: A report of two cases. Hand (N Y) 2012;7(1): Kleinman WB, Petersen DP: Oblique retinacular ligament reconstruction for chronic mallet finger deformity. J Hand Surg Am 1984;9(3): Thompson JS, Littler JW, Upton J: The spiral oblique retinacular ligament (SORL). J Hand Surg Am 1978;3(5): Onishi Y, Fujioka H, Doita M: Treatment of chronic post-traumatic hyperextension deformity of proximal interphalangeal joint using the suture anchor: A case report. Hand Surg 2007;12(1): Wollstein R, Watson HK, Carlson L: A technique for the repair of chronic volar plate avulsion of the proximal interphalangeal joint: A review of 54 cases. Plast Reconstr Surg 2006;117(4): Melone CP Jr, Polatsch DB, Beldner S, Khorsandi M: Volar plate repair for posttraumatic hyperextension deformity of the proximal interphalangeal joint. Am J Orthop (Belle Mead NJ) 2010;39(4): Tonkin MA, Hughes J, Smith KL: Lateral band translocation for swan-neck deformity. JHandSurgAm1992;17(2): Harris C Jr, Riordan DC: Intrinsic contracture in the hand and its surgical treatment. J Bone Joint Surg Am 1954;36 (1): Shin AY, Amadio PC: The stiff finger, in Wolfe SW, Hotchkiss RN, Pederson WC, Kozin SH, eds: Green s Operative Hand Surgery, ed 6. Philadelphia, PA, Elsevier, 2011, vol 1, pp Journal of the American Academy of Orthopaedic Surgeons
Revisiting the Curtis Procedure for Boutonniere Deformity Correction
 180 Letter to Editor Revisiting the Curtis Procedure for Boutonniere Deformity Correction Lee Seng Khoo*, Vasco Senna-Fernandes Ivo Pitanguy Institute, Rua Dona Mariana 65, Botafogo, Rio De Janeiro, Brazil
180 Letter to Editor Revisiting the Curtis Procedure for Boutonniere Deformity Correction Lee Seng Khoo*, Vasco Senna-Fernandes Ivo Pitanguy Institute, Rua Dona Mariana 65, Botafogo, Rio De Janeiro, Brazil
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 The Stiff Hand: Boutonniere & Sylvia Dávila, PT, CHT San Antonio, Texas Extensor Mechanism Central slip inserts into base of the middle phalanx Lateral bands lie dorsal to the PIP joint center of rotation
The Stiff Hand: Boutonniere & Sylvia Dávila, PT, CHT San Antonio, Texas Extensor Mechanism Central slip inserts into base of the middle phalanx Lateral bands lie dorsal to the PIP joint center of rotation
Interesting Case Series. Swan-Neck Deformity in Cerebral Palsy
 Interesting Case Series Swan-Neck Deformity in Cerebral Palsy Leyu Chiu, BA, a Nicholas S. Adams, MD, a,b and Paul A. Luce, MD, a,b,c a Michigan State University College of Human Medicine, Grand Rapids,
Interesting Case Series Swan-Neck Deformity in Cerebral Palsy Leyu Chiu, BA, a Nicholas S. Adams, MD, a,b and Paul A. Luce, MD, a,b,c a Michigan State University College of Human Medicine, Grand Rapids,
Reversing PIP Joint Contractures:
 Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System John M. Agee M.D. Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System
Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System John M. Agee M.D. Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System
The Rheumatoid Hand Deformities & Management. Dr. Anirudh Sharma Resident Department of Orthopedics
 + The Rheumatoid Hand Deformities & Management Dr. Anirudh Sharma Resident Department of Orthopedics + Why is Rheumatoid Arthritis important? + RA is a very debilitating disease median life expectancy
+ The Rheumatoid Hand Deformities & Management Dr. Anirudh Sharma Resident Department of Orthopedics + Why is Rheumatoid Arthritis important? + RA is a very debilitating disease median life expectancy
FINGER INJURIES. Chapter 24, pgs ,
 FINGER INJURIES Chapter 24, pgs 727 730, 741 743 1. Demonstrate mastery of anatomical references to the hand and fingers. 2. Compare and contrast Mallet Finger, Swan Neck Deformity and Boutonnière Deformity.
FINGER INJURIES Chapter 24, pgs 727 730, 741 743 1. Demonstrate mastery of anatomical references to the hand and fingers. 2. Compare and contrast Mallet Finger, Swan Neck Deformity and Boutonnière Deformity.
Swan-Neck Deformity. Introduction. Anatomy
 Swan-Neck Deformity Introduction Normal finger position and movement occur from the balanced actions of many important structures. Ligaments support the finger joints. Muscles hold and move the fingers.
Swan-Neck Deformity Introduction Normal finger position and movement occur from the balanced actions of many important structures. Ligaments support the finger joints. Muscles hold and move the fingers.
5/8/2017. Finger Injuries in Football. Tendon Injuries of the Hand and Wrist in Football Steve Kronlage, MD Andrews Institute Gulf Breeze, Florida
 Finger Injuries in Football Tendon Injuries of the Hand and Wrist in Football Steve Kronlage, MD Andrews Institute Gulf Breeze, Florida A jammed finger is an injury (at very least a torn ligament) A swollen
Finger Injuries in Football Tendon Injuries of the Hand and Wrist in Football Steve Kronlage, MD Andrews Institute Gulf Breeze, Florida A jammed finger is an injury (at very least a torn ligament) A swollen
MR: Finger and Thumb Injuries
 MR: Finger and Thumb Injuries Laura W. Bancroft, M.D. Professor of Radiology University of Central Florida Florida State University Outline Normal anatomy of the fingers and thumb MR imaging protocols
MR: Finger and Thumb Injuries Laura W. Bancroft, M.D. Professor of Radiology University of Central Florida Florida State University Outline Normal anatomy of the fingers and thumb MR imaging protocols
Institute of Reconstructive Surgery, Sofia, Bulgaria
 TRANSPOSITION OF THE LATERAL SLIPS OF THE APONEUROSIS IN TREATMENT OF LONG-STANDING " BOUTONNIERE DEFORMITY " OF THE FINGERS By IVAN MATEV Institute of Reconstructive Surgery, Sofia, Bulgaria RUPTURE of
TRANSPOSITION OF THE LATERAL SLIPS OF THE APONEUROSIS IN TREATMENT OF LONG-STANDING " BOUTONNIERE DEFORMITY " OF THE FINGERS By IVAN MATEV Institute of Reconstructive Surgery, Sofia, Bulgaria RUPTURE of
RHEUMATOID HAND. History Pain Loss of function Neck pain. Diminished ADL assessment:
 RHEUMATOID HAND History Pain Loss of function Neck pain Diminished ADL assessment: Using toothbrush, hairbrush, knife, fork Dressing bra, Pulling up trousers / stockings Operating remote control Hobbies
RHEUMATOID HAND History Pain Loss of function Neck pain Diminished ADL assessment: Using toothbrush, hairbrush, knife, fork Dressing bra, Pulling up trousers / stockings Operating remote control Hobbies
Fractures of the Hand in Children Which are simple? And Which have pitfalls??
 Fractures of the Hand in Children Which are simple? And Which have pitfalls?? Kaye E Wilkins DVM, MD Professor of Orthopedics and Pediatrics Departments of Orthopedics and Pediatrics University of Texas
Fractures of the Hand in Children Which are simple? And Which have pitfalls?? Kaye E Wilkins DVM, MD Professor of Orthopedics and Pediatrics Departments of Orthopedics and Pediatrics University of Texas
Hand Fractures: When is closed treatment OK? Epidemiology in USA: Metacarpal fractures: Page 1
 Hand Fractures: When is closed treatment OK? Robert J Strauch MD Professor of Orthopaedic Surgery Columbia University New York City Epidemiology in USA: 2009 Distal radius fx s: 16/10,000 Phalangeal fx
Hand Fractures: When is closed treatment OK? Robert J Strauch MD Professor of Orthopaedic Surgery Columbia University New York City Epidemiology in USA: 2009 Distal radius fx s: 16/10,000 Phalangeal fx
Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL
 Andrew McNamara, MD The Orthopaedic and Fracture Clinic 1431 Premier Drive Mankato, MN 56001 507-386-6600 Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL Patient Name: Date: Diagnosis:
Andrew McNamara, MD The Orthopaedic and Fracture Clinic 1431 Premier Drive Mankato, MN 56001 507-386-6600 Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL Patient Name: Date: Diagnosis:
Hand injuries. The metacarpal bones may fracture through the base, shaft or the neck.
 Hand injuries Metacarpal injuries The metacarpal bones may fracture through the base, shaft or the neck. Shaft fractures; these are caused by direct trauma which may cause transverse # of one or more metacarpal
Hand injuries Metacarpal injuries The metacarpal bones may fracture through the base, shaft or the neck. Shaft fractures; these are caused by direct trauma which may cause transverse # of one or more metacarpal
Clinical Orthopaedic Rehabilitation Volume 1 and 2
 Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Ascension. Silicone MCP surgical technique. surgical technique Ascension Silicone MCP
 Ascension Silicone MCP surgical technique WW 2 Introduction This manual describes the sequence of techniques and instruments used to implant the Ascension Silicone MCP (FIGURE 1A). Successful use of this
Ascension Silicone MCP surgical technique WW 2 Introduction This manual describes the sequence of techniques and instruments used to implant the Ascension Silicone MCP (FIGURE 1A). Successful use of this
A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report
 CASE REPORT 41 OPEN ACCESS A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report Aysha Rajeev, John Harrison ABSTRACT Introduction: The phalangeal
CASE REPORT 41 OPEN ACCESS A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report Aysha Rajeev, John Harrison ABSTRACT Introduction: The phalangeal
Physical therapy of the wrist and hand
 Physical therapy of the wrist and hand Functional anatomy wrist and hand The wrist includes distal radius, scaphoid, lunate, triquetrum, pisiform, trapezium, trapezoid, capitate, and hamate. The hand includes
Physical therapy of the wrist and hand Functional anatomy wrist and hand The wrist includes distal radius, scaphoid, lunate, triquetrum, pisiform, trapezium, trapezoid, capitate, and hamate. The hand includes
Interesting Case Series. Zone I Flexor Tendon Injuries
 Interesting Case Series Zone I Flexor Tendon Injuries Evgenios Evgeniou, MBBS, MRCS, a and Harriet Walker, MBBS, MRCS b a North Bristol NHS Trust, Bristol, United Kingdom, b Plymouth Hospitals NHS Trust,
Interesting Case Series Zone I Flexor Tendon Injuries Evgenios Evgeniou, MBBS, MRCS, a and Harriet Walker, MBBS, MRCS b a North Bristol NHS Trust, Bristol, United Kingdom, b Plymouth Hospitals NHS Trust,
AROM of DIP flex/ext, 10 reps hourly.
 BRIGHAM AND WOMEN S HOSPITAL A Teaching Affiliate of Harvard Medical School 75 Francis St. Boston, Massachusetts 02115 Department of Rehabilitation Services Physical Therapy The intent of this protocol
BRIGHAM AND WOMEN S HOSPITAL A Teaching Affiliate of Harvard Medical School 75 Francis St. Boston, Massachusetts 02115 Department of Rehabilitation Services Physical Therapy The intent of this protocol
Andrew B. Stein, MD Boston University Medical Center May 2 & 3, 2016
 Andrew B. Stein, MD Boston University Medical Center andrew.stein@bmc.org Work Related Workshop WorkInjuries Related Injuries Workshop Tendon injuries may be obvious or subtle History (mechanism of injury)
Andrew B. Stein, MD Boston University Medical Center andrew.stein@bmc.org Work Related Workshop WorkInjuries Related Injuries Workshop Tendon injuries may be obvious or subtle History (mechanism of injury)
Fractures and dislocations of the fingers
 Chapter 1 Fractures and dislocations of the fingers Felix S. Chew, M.D., and Catherine Maldjian, M.D. Case 1 1 Phalangeal tuft avulsion fracture 31-year-old woman injured in a ground-level fall. Lateral
Chapter 1 Fractures and dislocations of the fingers Felix S. Chew, M.D., and Catherine Maldjian, M.D. Case 1 1 Phalangeal tuft avulsion fracture 31-year-old woman injured in a ground-level fall. Lateral
Closed Proximal Phalangeal Fracture Management in Hand: An Outcome Analysis
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/577 Closed Proximal Phalangeal Fracture Management in Hand: An Outcome Analysis R Senthilkumar 1, E Kovarthini 2, Heber
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/577 Closed Proximal Phalangeal Fracture Management in Hand: An Outcome Analysis R Senthilkumar 1, E Kovarthini 2, Heber
Finger fractures and dislocations may
 Common Finger Fractures and Dislocations JAMES R. BORCHERS, MD, MPH, and THOMAS M. BEST, MD, PhD, The Ohio State University, Columbus, Ohio Finger fractures and dislocations are common injuries that are
Common Finger Fractures and Dislocations JAMES R. BORCHERS, MD, MPH, and THOMAS M. BEST, MD, PhD, The Ohio State University, Columbus, Ohio Finger fractures and dislocations are common injuries that are
Wrist and Hand Anatomy
 Wrist and Hand Anatomy Bone Anatomy Scapoid Lunate Triquetrium Pisiform Trapeziod Trapezium Capitate Hamate Wrist Articulations Radiocarpal Joint Proximal portion Distal portion Most surface contact found
Wrist and Hand Anatomy Bone Anatomy Scapoid Lunate Triquetrium Pisiform Trapeziod Trapezium Capitate Hamate Wrist Articulations Radiocarpal Joint Proximal portion Distal portion Most surface contact found
Extensor Tendon Repair Zones II, III, IV
 Zones II, III, IV D. WATTS, MD Indications Lacerations to the central slip, lateral bends and/or triangular ligament Rupture of the central slip in association with a PIP joint volar dislocation Avulsion
Zones II, III, IV D. WATTS, MD Indications Lacerations to the central slip, lateral bends and/or triangular ligament Rupture of the central slip in association with a PIP joint volar dislocation Avulsion
Silicone PIP, MCP & MCP-X (PreFlex)
 Silicone PIP, MCP & MCP-X (PreFlex) Finger Joint Arthroplasty Operative Technique Silicone PIP Silicone MCP Silicone PreFlex (MCP-X) Stryker Disclaimer This publication sets forth detailed recommended
Silicone PIP, MCP & MCP-X (PreFlex) Finger Joint Arthroplasty Operative Technique Silicone PIP Silicone MCP Silicone PreFlex (MCP-X) Stryker Disclaimer This publication sets forth detailed recommended
Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure
 Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure TRUONG LE DAO, MD, IFAAD 1 Burkhalter W.E, Cristhensen R.C, Brown P.W, Extensor Indicis Proprius opponensplasty
Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure TRUONG LE DAO, MD, IFAAD 1 Burkhalter W.E, Cristhensen R.C, Brown P.W, Extensor Indicis Proprius opponensplasty
Trigger Digits, Mallet Finger & Metacarpal Injuries. Joseph P. McCormick, M.D. Affinity Orthopaedics & Sports Medicine 2013
 Trigger Digits, Mallet Finger & Metacarpal Injuries Joseph P. McCormick, M.D. Affinity Orthopaedics & Sports Medicine 2013 Overview Trigger Digits: diagnosis and treatment Bonus: approach in children Mallet
Trigger Digits, Mallet Finger & Metacarpal Injuries Joseph P. McCormick, M.D. Affinity Orthopaedics & Sports Medicine 2013 Overview Trigger Digits: diagnosis and treatment Bonus: approach in children Mallet
BASIC PRINCIPLES OF HAND TRAUMA: ARE CHILDREN DIFFERENT? SUSAN THOMPSON, MD, FRCSC
 BASIC PRINCIPLES OF HAND TRAUMA: ARE CHILDREN DIFFERENT? SUSAN THOMPSON, MD, FRCSC EPIDEMIOLOGY HAND FRACTURES MAKE UP 2.3% OF ER VISITS INCIDENCE VARIES WITH AGE LOW IN TODDLERS INCREASES WITH AGE (20
BASIC PRINCIPLES OF HAND TRAUMA: ARE CHILDREN DIFFERENT? SUSAN THOMPSON, MD, FRCSC EPIDEMIOLOGY HAND FRACTURES MAKE UP 2.3% OF ER VISITS INCIDENCE VARIES WITH AGE LOW IN TODDLERS INCREASES WITH AGE (20
Mallet Baseball Finger
 Mallet Baseball Finger Introduction When you think about how much we use our hands, it's not hard to understand why injuries to the fingers are common. Most of these injuries heal without significant problems.
Mallet Baseball Finger Introduction When you think about how much we use our hands, it's not hard to understand why injuries to the fingers are common. Most of these injuries heal without significant problems.
Hand Anatomy A Patient's Guide to Hand Anatomy
 Hand Anatomy A Patient's Guide to Hand Anatomy Introduction Few structures of the human anatomy are as unique as the hand. The hand needs to be mobile in order to position the fingers and thumb. Adequate
Hand Anatomy A Patient's Guide to Hand Anatomy Introduction Few structures of the human anatomy are as unique as the hand. The hand needs to be mobile in order to position the fingers and thumb. Adequate
Finger Mobility Deficits Fracture of metacarpal Fracture of phalanx of phalanges
 1 Finger Mobility Deficits ICD-9-CM codes: 715.4 Osteoarthrosis of the hand 815.0 Fracture of metacarpal 816.0 Fracture of phalanx of phalanges ICF codes: Activities and Participation code: d4301 Carrying
1 Finger Mobility Deficits ICD-9-CM codes: 715.4 Osteoarthrosis of the hand 815.0 Fracture of metacarpal 816.0 Fracture of phalanx of phalanges ICF codes: Activities and Participation code: d4301 Carrying
11/13/2017. Complications of Flexor Tendon Repair. Brandon E. Earp, M.D. How do we best get there?
 Complications of Flexor Tendon Repair Brandon E. Earp, M.D. Chief of Orthopaedic Surgery Brigham and Women s Faulkner Hospital Vice-Chair of Clinical Operations Brigham and Women s Hospital Frontiers in
Complications of Flexor Tendon Repair Brandon E. Earp, M.D. Chief of Orthopaedic Surgery Brigham and Women s Faulkner Hospital Vice-Chair of Clinical Operations Brigham and Women s Hospital Frontiers in
Study of clinical problems: Mallet injuries
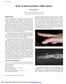 Review Article Study of clinical problems: Mallet injuries Hin-Keung WONG Department of Orthopaedics & Traumatology, Princess Margaret Hospital, Hong Kong SAR INTRODUCTION The extensor mechanism of the
Review Article Study of clinical problems: Mallet injuries Hin-Keung WONG Department of Orthopaedics & Traumatology, Princess Margaret Hospital, Hong Kong SAR INTRODUCTION The extensor mechanism of the
SPECIAL ARTICLE. Missed tendon injuries INTRODUCTION
 Archives of Emergency Medicine, 1991, 8, 87-91 SPECIAL ARTICLE Missed tendon injuries H. R. GULY Consultant in A & E, Derriford Hospital, Plymouth INTRODUCTION The timing of the repair of divided tendons
Archives of Emergency Medicine, 1991, 8, 87-91 SPECIAL ARTICLE Missed tendon injuries H. R. GULY Consultant in A & E, Derriford Hospital, Plymouth INTRODUCTION The timing of the repair of divided tendons
PIP Joint Injuries of the Finger A Patient's Guide to PIP Joint Injuries of the Finger
 PIP Joint Injuries of the Finger A Patient's Guide to PIP Joint Injuries of the Finger Introduction We use our hands constantly, placing them in harm's way continuously. Injuries to the finger joints are
PIP Joint Injuries of the Finger A Patient's Guide to PIP Joint Injuries of the Finger Introduction We use our hands constantly, placing them in harm's way continuously. Injuries to the finger joints are
Ligaments of Elbow hinge: sagittal plane so need lateral and medial ligaments
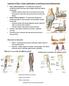 Ligaments of Elbow hinge: sagittal plane so need lateral and medial ligaments Ulnar Collateral ligament on medial side; arising from medial epicondyle and stops excess valgus movement (lateral movement)
Ligaments of Elbow hinge: sagittal plane so need lateral and medial ligaments Ulnar Collateral ligament on medial side; arising from medial epicondyle and stops excess valgus movement (lateral movement)
Wrist & Hand Assessment and General View
 Wrist & Hand Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The hand can be divided
Wrist & Hand Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The hand can be divided
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Common. Common Hand Problems in Elite Athletes
 Common Hand Problems in Elite Athletes Fred Corley M.D. Dept. of Orthopaedic Surgery UTHSCSA I have no disclosures concerning this talk. The University of Texas Health Science Center @ San Antonio - Orthopaedics
Common Hand Problems in Elite Athletes Fred Corley M.D. Dept. of Orthopaedic Surgery UTHSCSA I have no disclosures concerning this talk. The University of Texas Health Science Center @ San Antonio - Orthopaedics
Poliomyelitis: Splints for the Upper Extremity
 Poliomyelitis: Splints for the Upper Extremity By C.E. IRWIN, M.D. Atlanta, Ga. The splints to be discussed in this presentation are designed and used for therapeutic reasons only. They are in no sense
Poliomyelitis: Splints for the Upper Extremity By C.E. IRWIN, M.D. Atlanta, Ga. The splints to be discussed in this presentation are designed and used for therapeutic reasons only. They are in no sense
Muscle/Tendon Functions: Thumb. Extensor Tendon Healing. Digital Extension. Digital Extension. Supporting Ligaments: ORL. Supporting Ligaments
 Extensor Tendon Anatomy, Common Injury and Treatment Christina Schmidt, OTR/L, CHT University of California, Irvine Irvine, CA February 9-11, 2018 2 How Extensor Tendons Differ from Flexor Tendons Dorsum
Extensor Tendon Anatomy, Common Injury and Treatment Christina Schmidt, OTR/L, CHT University of California, Irvine Irvine, CA February 9-11, 2018 2 How Extensor Tendons Differ from Flexor Tendons Dorsum
What you don t want to miss
 March 25, 2009 Vishal Michael Shah, M.D. What you don t want to miss Spectrum of Injuries Contusions Sprains Dislocations Fractures Lacerations Tendon Avulsions Ligament Tears Overuse Injuries FINGER
March 25, 2009 Vishal Michael Shah, M.D. What you don t want to miss Spectrum of Injuries Contusions Sprains Dislocations Fractures Lacerations Tendon Avulsions Ligament Tears Overuse Injuries FINGER
The Birmingham Hook Plate Treatment Of Irreduceable Displaced Mallet Avulsion Fractures: A Technical Note
 ISPUB.COM The Internet Journal of Hand Surgery Volume 1 Number 1 The Birmingham Hook Plate Treatment Of Irreduceable Displaced Mallet Avulsion Fractures: A Technical S Tan, D Power Citation S Tan, D Power..
ISPUB.COM The Internet Journal of Hand Surgery Volume 1 Number 1 The Birmingham Hook Plate Treatment Of Irreduceable Displaced Mallet Avulsion Fractures: A Technical S Tan, D Power Citation S Tan, D Power..
Ascension. MCP surgical technique. surgical technique Ascension MCP PyroCarbon Total Joint
 Ascension MCP surgical technique PyroCarbon Total Joint WW 1.0 Table of Contents 2.0 Introduction............................ 2 3.0 Ascension MCP Implants................ 2 4.0 Instrumentation for MCP
Ascension MCP surgical technique PyroCarbon Total Joint WW 1.0 Table of Contents 2.0 Introduction............................ 2 3.0 Ascension MCP Implants................ 2 4.0 Instrumentation for MCP
Wrist and Hand Complaints
 Wrist and Hand Complaints Charles S. Day, M.D., M.B.A. Chief, Hand & Upper Extremity Surgery St. Elizabeth s Medical Center Tufts University School of Medicine Primary Care Internal Medicine 2018 Outline
Wrist and Hand Complaints Charles S. Day, M.D., M.B.A. Chief, Hand & Upper Extremity Surgery St. Elizabeth s Medical Center Tufts University School of Medicine Primary Care Internal Medicine 2018 Outline
Integra. Silicone PIP Implant SURGICAL TECHNIQUE
 Integra Silicone PIP Implant SURGICAL TECHNIQUE Table of Contents Indications For Use...2 Contraindications...2 Warnings and Precautions...2 Surgical Technique Preoperative Assessment... 3 Step 1: Initial
Integra Silicone PIP Implant SURGICAL TECHNIQUE Table of Contents Indications For Use...2 Contraindications...2 Warnings and Precautions...2 Surgical Technique Preoperative Assessment... 3 Step 1: Initial
Closed Injuries: Bone, Ligament, and Tendon
 Closed Injuries: Bone, Ligament, and Tendon 2 Leo M. Rozmaryn Mallet Deformity Introduction L. M. Rozmaryn ( ) Division of Uniformed Services, University Health Sciences Center, Washington, D.C, 9420 Key
Closed Injuries: Bone, Ligament, and Tendon 2 Leo M. Rozmaryn Mallet Deformity Introduction L. M. Rozmaryn ( ) Division of Uniformed Services, University Health Sciences Center, Washington, D.C, 9420 Key
IC 30: Tips and Tricks for Management of Hand Fractures-Simple to Complex
 IC 30: Tips and Tricks for Management of Hand Fractures-Simple to Complex Moderator(s): Randip R. Bindra, FRCS, MCh Orth Faculty: Andrea Atzei, MD, Donald H. Lalonde, MD, David S. Ruch, MD Session Handouts
IC 30: Tips and Tricks for Management of Hand Fractures-Simple to Complex Moderator(s): Randip R. Bindra, FRCS, MCh Orth Faculty: Andrea Atzei, MD, Donald H. Lalonde, MD, David S. Ruch, MD Session Handouts
Volar Plate Avulsion Fractures
 Journal of the Accident and Medical Practitioners Association (JAMPA) 2006; Vol. 3 (No. 1) Accident and Medical Practitioners Association, New Zealand Volar Plate Avulsion Fractures Sarah Cooper, MBChB
Journal of the Accident and Medical Practitioners Association (JAMPA) 2006; Vol. 3 (No. 1) Accident and Medical Practitioners Association, New Zealand Volar Plate Avulsion Fractures Sarah Cooper, MBChB
Trapezium is by the thumb, Trapezoid is inside
 Trapezium is by the thumb, Trapezoid is inside Intercarpal Jt Radiocarpal Jt Distal Middle Proximal DIP PIP Interphalangeal Jts Metacarpalphalangeal (MCP) Jt Metacarpal Carpometacarpal (CMC) Jt Trapezium
Trapezium is by the thumb, Trapezoid is inside Intercarpal Jt Radiocarpal Jt Distal Middle Proximal DIP PIP Interphalangeal Jts Metacarpalphalangeal (MCP) Jt Metacarpal Carpometacarpal (CMC) Jt Trapezium
Research Article How Early Can We Mobilise 4 th And 5 th Metacarpal Shaft Fractures? A Retrospective Study
 Cronicon OPEN ACCESS ORTHOPAEDICS Research Article How Early Can We Mobilise 4 th And 5 th Metacarpal Shaft Fractures? A Retrospective Study Mohammed KM Ali 1, Abid Hussain 1, CA Mbah 1, Alaa Mustafa 1,
Cronicon OPEN ACCESS ORTHOPAEDICS Research Article How Early Can We Mobilise 4 th And 5 th Metacarpal Shaft Fractures? A Retrospective Study Mohammed KM Ali 1, Abid Hussain 1, CA Mbah 1, Alaa Mustafa 1,
CAUSES OF PROLAPSE AND COLLAPSE OF THE PROXIMAl" INTERPHALANGEAL JOINT J. C. VAN DER MEULEN. Rotterdam
 Causes of Prolapse and Collapse of the Proximal Interphalangeal Joint-f. C. Vander Meu{en CAUSES OF PROLAPSE AND COLLAPSE OF THE PROXIMAl" INTERPHALANGEAL JOINT J. C. VAN DER MEULEN. Rotterdam INTRODUCTION
Causes of Prolapse and Collapse of the Proximal Interphalangeal Joint-f. C. Vander Meu{en CAUSES OF PROLAPSE AND COLLAPSE OF THE PROXIMAl" INTERPHALANGEAL JOINT J. C. VAN DER MEULEN. Rotterdam INTRODUCTION
Fracture and Dislocation of the Carpus ( 1-Jan-1985 )
 In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
Fracture and Dislocation of Metacarpal Bones, Metacarpophalangeal Joints, Phalanges, and Interphalangeal Joints ( 1-Jan-1985 )
 In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
8 Recovering From HAND FRACTURE SURGERY
 8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
Classification of Established Volkmann s Ischemic Contracture and the Program for Its Treatment
 10 Classification of Established Volkmann s Ischemic Contracture and the Program for Its Treatment In spite of the advances made in preventive treatment of muscular ischemia at the forearm and hand, there
10 Classification of Established Volkmann s Ischemic Contracture and the Program for Its Treatment In spite of the advances made in preventive treatment of muscular ischemia at the forearm and hand, there
Dynamic treatment for proximal phalangeal fracture of the hand
 Journal of Orthopaedic Surgery 2007;15(2):211-5 Dynamic treatment for proximal phalangeal fracture of the hand G Rajesh, WY Ip, SP Chow, BKK Fung Department of Orthopaedics and Traumatology, University
Journal of Orthopaedic Surgery 2007;15(2):211-5 Dynamic treatment for proximal phalangeal fracture of the hand G Rajesh, WY Ip, SP Chow, BKK Fung Department of Orthopaedics and Traumatology, University
Introduction to Ultrasound Examination of the Hand and upper
 Introduction to Ultrasound Examination of the Hand and upper Emil Dionysian, M.D. Ultrasound of upper ext. Upside Convenient Opens another exam dimension Can be like a stethoscope Helps 3-D D visualization
Introduction to Ultrasound Examination of the Hand and upper Emil Dionysian, M.D. Ultrasound of upper ext. Upside Convenient Opens another exam dimension Can be like a stethoscope Helps 3-D D visualization
Client centered approach to distal radius fracture management. Jared Rasmussen OTR
 Client centered approach to distal radius fracture management Jared Rasmussen OTR Disclosures Sadly, no financial disclosures Objectives Review of anatomy, common fractures of the distal radius, fixation
Client centered approach to distal radius fracture management Jared Rasmussen OTR Disclosures Sadly, no financial disclosures Objectives Review of anatomy, common fractures of the distal radius, fixation
Anatomy of the Hand and Nomenclature. R K Kankate Specialist Registrar St.George s Hospital
 Anatomy of the Hand and Nomenclature R K Kankate Specialist Registrar St.George s Hospital Bony skeleton muscles and ligaments nervous, arterial and venous system Ossification of bones: carpus Most carpal
Anatomy of the Hand and Nomenclature R K Kankate Specialist Registrar St.George s Hospital Bony skeleton muscles and ligaments nervous, arterial and venous system Ossification of bones: carpus Most carpal
An anatomic. deformity. onic boutonniere :onstruction. "he Journal. ne Joint. urgery in :o. p 115, evolution~ alis muscle [:396-7, earra flex~
 "he Journal ne Joint urgery in :o. p 115, evolution~ alis muscle [:396-7, earra flex~ earm flexon: it 70:281.9L Philadelphia, tot dieitoru~ lie. Br J Pla~.or d io~ito~-a~ Dis 36:524. to an imbalance of
"he Journal ne Joint urgery in :o. p 115, evolution~ alis muscle [:396-7, earra flex~ earm flexon: it 70:281.9L Philadelphia, tot dieitoru~ lie. Br J Pla~.or d io~ito~-a~ Dis 36:524. to an imbalance of
eplasty: Vol. 8 Assessment of the Distal Extent of the A1 Pulley Release: A New Technique
 eplasty: Vol. 8 Assessment of the Distal Extent of the A1 Pulley Release: A New Technique Ron Hazani, MD, Nitin J. Engineer, MD, Linda L Division of Plastic Surgery, School of Medicine, University of Louisville,
eplasty: Vol. 8 Assessment of the Distal Extent of the A1 Pulley Release: A New Technique Ron Hazani, MD, Nitin J. Engineer, MD, Linda L Division of Plastic Surgery, School of Medicine, University of Louisville,
Integra. Silicone MCP Joint Prosthesis SURGICAL TECHNIQUE
 Integra Silicone MCP Joint Prosthesis SURGICAL TECHNIQUE Table of Contents Introduction Indications For Use...2 Contraindications...2 Warnings and Precautions... 2 System Overview... 3 Surgical Technique
Integra Silicone MCP Joint Prosthesis SURGICAL TECHNIQUE Table of Contents Introduction Indications For Use...2 Contraindications...2 Warnings and Precautions... 2 System Overview... 3 Surgical Technique
Assessing hand ligaments and tendons lesions using MRI
 Assessing hand ligaments and tendons lesions using MRI Award: Certificate of Merit Poster No.: C-0691 Congress: ECR 2017 Type: Educational Exhibit Authors: A. M. Benitez Vazquez, M. I. Rossi Prieto, C.
Assessing hand ligaments and tendons lesions using MRI Award: Certificate of Merit Poster No.: C-0691 Congress: ECR 2017 Type: Educational Exhibit Authors: A. M. Benitez Vazquez, M. I. Rossi Prieto, C.
Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley.
 TRIGGER DIGITS Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley. Abstract Primary stenosing tenosynovitis is usually idiopathic
TRIGGER DIGITS Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley. Abstract Primary stenosing tenosynovitis is usually idiopathic
Index. Note: Page numbers of article titles are in boldface type. Hand Clin 21 (2005)
 Hand Clin 21 (2005) 501 505 Index Note: Page numbers of article titles are in boldface type. A Antibiotics, following distal radius fracture treatment, 295, 296 Arthritis, following malunion of distal
Hand Clin 21 (2005) 501 505 Index Note: Page numbers of article titles are in boldface type. A Antibiotics, following distal radius fracture treatment, 295, 296 Arthritis, following malunion of distal
Acknowledgements. Methods of Learning. The Dorsal Interossei 11/2/17. Special thanks to:
 The Dorsal Interossei Mike Cricchio, MBA, OT/L, CHT Site Manager UFHealth Hand and Upper Extremity criccm@gmail.com Acknowledgements Special thanks to: Michelle Darnell, DPT, PT Kimberly Hellriegel, OTR/L
The Dorsal Interossei Mike Cricchio, MBA, OT/L, CHT Site Manager UFHealth Hand and Upper Extremity criccm@gmail.com Acknowledgements Special thanks to: Michelle Darnell, DPT, PT Kimberly Hellriegel, OTR/L
Assessment of the Distal Extent of the A1 Pulley Release: A New Technique
 Assessment of the Distal Extent of the A1 Pulley Release: A New Technique Ron Hazani, MD, Nitin J. Engineer, MD, Linda L. Zeineh, MD, and Bradon J. Wilhelmi, MD Division of Plastic Surgery, School of Medicine,
Assessment of the Distal Extent of the A1 Pulley Release: A New Technique Ron Hazani, MD, Nitin J. Engineer, MD, Linda L. Zeineh, MD, and Bradon J. Wilhelmi, MD Division of Plastic Surgery, School of Medicine,
MEDIAL EPICONDYLE FRACTURES
 MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
Mallet Finger Injuries
 A Patient s Guide to Mallet Finger Injuries 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Mallet Finger Injuries 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER: The information in this booklet is compiled
HAND SURGERY- GUIDELINES for POST-OP TREATMENT and REFERRAL to HAND THERAPY
 HAND SURGERY- GUIDELINES for POST-OP TREATMENT and REFERRAL to HAND THERAPY Please use the specific hand therapy referral form. Always give at least one telephone number for the patient so that there is
HAND SURGERY- GUIDELINES for POST-OP TREATMENT and REFERRAL to HAND THERAPY Please use the specific hand therapy referral form. Always give at least one telephone number for the patient so that there is
SWAN'S NECK DEFORMITY OF THE FINGERS
 SWAN'S NECK DEFORMITY OF THE FINGERS By STEWART H. HARRISON, F.R.C.S., L.D.S.R.C.S.(Edin.) The Mount Vernon Centre of Plastic Surgery, Northwood, Middlesex, and the Windsor Group of Hospitals HYPEREXTENSION
SWAN'S NECK DEFORMITY OF THE FINGERS By STEWART H. HARRISON, F.R.C.S., L.D.S.R.C.S.(Edin.) The Mount Vernon Centre of Plastic Surgery, Northwood, Middlesex, and the Windsor Group of Hospitals HYPEREXTENSION
Management of Mallet Fracture by Closed Extension-Block Pinning A case based review of a novel technique
 Management of Mallet Fracture by Closed Extension-Block Pinning A case based review of a novel technique Sharat Agarwal 1, Mohammad Nasim Akhtar 2 1. Assistant Professor, Department of Orthopedics & Trauma,
Management of Mallet Fracture by Closed Extension-Block Pinning A case based review of a novel technique Sharat Agarwal 1, Mohammad Nasim Akhtar 2 1. Assistant Professor, Department of Orthopedics & Trauma,
PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE
 C H A P T E R 5 PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE Raymond G. Cavaliere, DPM INTRODUCTION Hammertoes can be classified as simple, moderate, and severe. The deformities
C H A P T E R 5 PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE Raymond G. Cavaliere, DPM INTRODUCTION Hammertoes can be classified as simple, moderate, and severe. The deformities
Carpal Instability: Clarification of the Most Common Etiologies and Imaging Findings
 Carpal Instability: Clarification of the Most Common Etiologies and Imaging Findings Corey Matthews DO, Nicholas Strle DO, Donald von Borstel DO Oklahoma State University Medical Center, Department of
Carpal Instability: Clarification of the Most Common Etiologies and Imaging Findings Corey Matthews DO, Nicholas Strle DO, Donald von Borstel DO Oklahoma State University Medical Center, Department of
Comparison of Miniplate and K-wire in Treatment of Metacarpal and Phalangeal Fractures
 The THAI Journal of SURGERY 2009; 30:5-10. Official Publication of the Royal College of Surgeons of Thailand Comparison of Miniplate and K-wire in Treatment of Metacarpal and Phalangeal Fractures Somboon
The THAI Journal of SURGERY 2009; 30:5-10. Official Publication of the Royal College of Surgeons of Thailand Comparison of Miniplate and K-wire in Treatment of Metacarpal and Phalangeal Fractures Somboon
NEUFLEX MCP/PIP FINGER JOINT IMPLANT SYSTEMS SURGICAL TECHNIQUE. This publication is not intended for distribution in the USA.
 NEUFLEX MCP/PIP FINGER JOINT IMPLANT SYSTEMS This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE MCP SURGICAL TECHNIQUE Summary provided by designing surgeon Arnold-Peter C.
NEUFLEX MCP/PIP FINGER JOINT IMPLANT SYSTEMS This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE MCP SURGICAL TECHNIQUE Summary provided by designing surgeon Arnold-Peter C.
SWANSON. Flexible Finger Joint Implant SURGIC AL TECHNIQUE
 SWANSON Flexible Finger Joint Implant SURGIC AL TECHNIQUE Contents Preface 4 Chapter 1 5 5 6 7 7 7 8 Chapter 2 9 9 15 15 16 19 19 Appendix A 20 Appendix B 22 Design Surgeon Introduction Device Description
SWANSON Flexible Finger Joint Implant SURGIC AL TECHNIQUE Contents Preface 4 Chapter 1 5 5 6 7 7 7 8 Chapter 2 9 9 15 15 16 19 19 Appendix A 20 Appendix B 22 Design Surgeon Introduction Device Description
A Patient s Guide to Adult Finger Fractures
 A Patient s Guide to Adult Finger Fractures 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 1 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Adult Finger Fractures 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 1 DISCLAIMER: The information in this booklet is compiled from a variety
Tendon transfers for ulnar nerve palsy
 Tendon transfers for ulnar nerve palsy Caroline LECLERCQ, de la main Paris, France Gruppo MANUS Etiology - Distal palsy - Nerve laceration at forearm & wrist - Neuromuscular diseases CMT, leprosy - Lower
Tendon transfers for ulnar nerve palsy Caroline LECLERCQ, de la main Paris, France Gruppo MANUS Etiology - Distal palsy - Nerve laceration at forearm & wrist - Neuromuscular diseases CMT, leprosy - Lower
A Patient s Guide to Elbow Dislocation
 A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
Kinesiology of The Wrist and Hand. Cuneyt Mirzanli Istanbul Gelisim University
 Kinesiology of The Wrist and Hand Cuneyt Mirzanli Istanbul Gelisim University Bones The wrist and hand contain 29 bones including the radius and ulna. There are eight carpal bones in two rows of four to
Kinesiology of The Wrist and Hand Cuneyt Mirzanli Istanbul Gelisim University Bones The wrist and hand contain 29 bones including the radius and ulna. There are eight carpal bones in two rows of four to
Wrist and Hand Anatomy/Biomechanics
 Wrist and Hand Anatomy/Biomechanics Kristin Kelley, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Orthopaedic Manual Physical Therapy Series 2017-2018 Anatomy -
Wrist and Hand Anatomy/Biomechanics Kristin Kelley, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Orthopaedic Manual Physical Therapy Series 2017-2018 Anatomy -
10/10/2014. Structure and Function of the Hand. The Hand. Osteology of the Hand
 Structure and Function of the Hand 19 bones and 19 joints are necessary to produce all the motions of the hand The Hand Dorsal aspect Palmar aspect The digits are numbered 1-5 Thumb = #1 Little finger
Structure and Function of the Hand 19 bones and 19 joints are necessary to produce all the motions of the hand The Hand Dorsal aspect Palmar aspect The digits are numbered 1-5 Thumb = #1 Little finger
Anatomy - Hand. Wrist and Hand Anatomy/Biomechanics. Osteology. Carpal Arch. Property of VOMPTI, LLC
 Wrist and Hand Anatomy/Biomechanics Kristin Kelley, DPT, OCS, FAAOMPT The wrist The metacarpals The Phalanges Digit 1 thumb Digit 5 digiti minimi Anatomy - Hand Orthopaedic Manual Physical Therapy Series
Wrist and Hand Anatomy/Biomechanics Kristin Kelley, DPT, OCS, FAAOMPT The wrist The metacarpals The Phalanges Digit 1 thumb Digit 5 digiti minimi Anatomy - Hand Orthopaedic Manual Physical Therapy Series
Stenosing flexor tenosynovitis (trigger finger) is
 An Original Study Recalcitrant Trigger Finger Managed With Flexor Digitorum Superficialis Resection Sohail N. Husain, MD, Sylvan E. Clarke, MD, Glenn A. Buterbaugh, MD, and Joseph E. Imbriglia, MD Abstract
An Original Study Recalcitrant Trigger Finger Managed With Flexor Digitorum Superficialis Resection Sohail N. Husain, MD, Sylvan E. Clarke, MD, Glenn A. Buterbaugh, MD, and Joseph E. Imbriglia, MD Abstract
FACTORS INFLUENCING THE MANAGEMENT OF THE FLEXOR TENDON INJURIES IN THE HAND
 Basrah Journal of Surgery FACTORS INFLUENCING THE MANAGEMENT OF THE FLEXOR TENDON INJURIES IN THE HAND Avadis F.I.C.M.S. Lecturer in Orthopaedic, Department of Surgery, College of Medicine, and specialist
Basrah Journal of Surgery FACTORS INFLUENCING THE MANAGEMENT OF THE FLEXOR TENDON INJURIES IN THE HAND Avadis F.I.C.M.S. Lecturer in Orthopaedic, Department of Surgery, College of Medicine, and specialist
Open irreducible fracture/dislocation of the four ulnar metacarpals at the metacarpophalangeal joints: case report
 Open irreducible fracture/dislocation of the four ulnar metacarpals at the metacarpophalangeal joints: case report Eurico Monteiro, Pedro Negrão, Vitor Vidinha, Manuel Gutierres & Rui Pinto European Orthopaedics
Open irreducible fracture/dislocation of the four ulnar metacarpals at the metacarpophalangeal joints: case report Eurico Monteiro, Pedro Negrão, Vitor Vidinha, Manuel Gutierres & Rui Pinto European Orthopaedics
JuggerKnot Soft Anchor 1.0 mm Mini. Scapholunate Ligament Repair/Reconstruction. Brochure and Surgical Technique
 JuggerKnot Soft Anchor 1.0 mm Mini Scapholunate Ligament Repair/Reconstruction Brochure and Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide
JuggerKnot Soft Anchor 1.0 mm Mini Scapholunate Ligament Repair/Reconstruction Brochure and Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide
FOOSH It sounded like a fun thing at the time!
 FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
Jacqueline C. Vanderzanden, Brian D. Adams & Justin J. Guan
 MCP arthrodesis using an intramedullary interlocking device Jacqueline C. Vanderzanden, Brian D. Adams & Justin J. Guan HAND ISSN 1558-9447 HAND DOI 10.1007/s11552-013-9579-5 1 23 Your article is published
MCP arthrodesis using an intramedullary interlocking device Jacqueline C. Vanderzanden, Brian D. Adams & Justin J. Guan HAND ISSN 1558-9447 HAND DOI 10.1007/s11552-013-9579-5 1 23 Your article is published
Open Reduction of Proximal Interphalangeal Fracture-Dislocation through a Midlateral Incision Using Absorbable Suture Materials
 Open Reduction of Proximal Interphalangeal Fracture-Dislocation through a Midlateral Incision Using Absorbable Suture Materials Jae Jun Lee, Hyoung Joon Park, Hyun Gon Choi, Dong Hyeok Shin, Ki Il Uhm
Open Reduction of Proximal Interphalangeal Fracture-Dislocation through a Midlateral Incision Using Absorbable Suture Materials Jae Jun Lee, Hyoung Joon Park, Hyun Gon Choi, Dong Hyeok Shin, Ki Il Uhm
1 Comprehensive Orthopaedic Review Hand and Wrist Tendinopathies Bernard F. Hearon, MD September 2, de Quervain Disorder Fritz de Quervain,
 1 Comprehensive Orthopaedic Review Hand and Wrist Tendinopathies Bernard F. Hearon, MD September 2, 2016 2 de Quervain Disorder Fritz de Quervain, Swiss surgeon, 1895 Stenosing tendinosis, 1st dorsal compartment
1 Comprehensive Orthopaedic Review Hand and Wrist Tendinopathies Bernard F. Hearon, MD September 2, 2016 2 de Quervain Disorder Fritz de Quervain, Swiss surgeon, 1895 Stenosing tendinosis, 1st dorsal compartment
MODIFIED EXTENSION BLOCK PINNING FOR LARGE MALLET FRACTURES
 Benha M. J.. Vol. 26 No 1 Jan. 2009 MODIFIED EXTENSION BLOCK PINNING FOR LARGE MALLET FRACTURES Abdel-Salam A. Ahmed MD and Islam H. Hegazy MD Department oj Orthopedic Surgery. BenhaJaculty ojmedicine.
Benha M. J.. Vol. 26 No 1 Jan. 2009 MODIFIED EXTENSION BLOCK PINNING FOR LARGE MALLET FRACTURES Abdel-Salam A. Ahmed MD and Islam H. Hegazy MD Department oj Orthopedic Surgery. BenhaJaculty ojmedicine.
SR MCP System Metacarpophalangeal Arthroplasty. Operative technique
 SR MCP System Metacarpophalangeal Arthroplasty Operative technique SR MCP System Metacarpophalangeal Arthroplasty Operative technique SR MCP System Metacarpophalangeal Arthroplasty Contents 1. Pre-operative
SR MCP System Metacarpophalangeal Arthroplasty Operative technique SR MCP System Metacarpophalangeal Arthroplasty Operative technique SR MCP System Metacarpophalangeal Arthroplasty Contents 1. Pre-operative
The Forearm, Wrist, Hand and Fingers. Contusion Injuries to the Forearm. Forearm Fractures 12/11/2017. Oak Ridge High School Conroe, Texas
 The Forearm, Wrist, Hand and Fingers Oak Ridge High School Conroe, Texas Contusion Injuries to the Forearm The forearm is constantly exposed to bruising and contusions in contact sports. The ulna receives
The Forearm, Wrist, Hand and Fingers Oak Ridge High School Conroe, Texas Contusion Injuries to the Forearm The forearm is constantly exposed to bruising and contusions in contact sports. The ulna receives
