Effect of salbutamol nebulization in transient tachypnea of newborn
|
|
|
- Anthony Hoover
- 6 years ago
- Views:
Transcription
1 International Journal of Current Research in Medical Sciences ISSN: P-ISJN: A , E -ISJN: A Original Research Article Volume 3, Issue Effect of salbutamol nebulization in transient tachypnea of newborn *Amanpreet Kaur, **Pardeep Singh Kahlon, ***Karnail Singh, ***MS Pannu *Junior Resident, **Assistant Professor, ***Professor, Department of Paediatrics, Govt. Medical College, Amritsar, India, Corresponding Author: Dr. Pardeep Singh Kahlon, Assistant Professor, Department of Paediatrics, Govt. Medical College, Amritsar, India, E- mail:docpsk@yahoo.com Abstract Background: Transient tachypnea of newborn (TTN) is a parenchymal lung disease present in neontes usually within 6 hours of life. Signs of TTN usually persist for hours in mild disease but can last upto 72 hours in more severe cases. In severe cases of TTN, complications such as pneumothorax, need for extracorporeal membrane oxygenation, and death have been reported. Objective: To study the effect of single dose of salbutamol nebulization in TTN administered at diagnosis and assess its efficacy at 30minutes, 1hour and 4 hours post nebulization and the side effects if any at 4 hours Materials and methods: Study design: Double blind prospective placebo controlled study, one dose of inhaled salbutamol or normal saline solution was administered to 50 newborns each with gestational age of 35 to 41 weeks and diagnosed as TTN according to clinical and radiological features. Setting: Pediatrics Department, Bebe Nanki Mother and Child Care Centre, Government Medical College, Amritsar. Participants:100 newborns. Outcome variables: TTN score, oxygen saturation, respiratory rate and average duration of hospital stay. Results: After one dose of salbutamol nebulization, the TTN score, respiratory rate, oxygen saturation and duration of hospitalization did not decrease significantly when compared with the normal saline group (p value >0.05). No side effects like tachycardia, hypokalemia and hyperglycemia were noted in salbutamol group when compared to normal saline group. Conclusion: Inhaled salbutamol treatment did not show any effect on early resolution of symptoms and early discharge of babies. Keywords: TTN, Salbutamol nebulization. DOI: 1
2 Introduction Transient tachypnea of newborn (TTN) is parenchymal lung disease. It is the benign selflimited condition resulting from delayed resorption of foetal lung fluid 1.This condition is characterised by:- Tachypnea with signs of mild respiratory distress including retractions, grunting, nasal flaring and mild cyanosis. Decreased oxygen saturation alleviated by supplemental oxygen with FiO 2 less than 40% 2. It is the common cause of respiratory distress in the immediate new born period. In a review of 33,289 term deliveries (37 to 42 weeks), the incidence of TTN was 5.7 per 1000 births 3. Infants with TTN present within the first 6 hours of life. Signs of TTN usually persist for hours in mild disease but can last up to 72 hours in more severe cases 2. Although it is self limited condition, there is an increase data to suggest that TTN increases risk for developing a wheezing syndrome early in the life 4. During late gestation, in response to increased concentrations of catecholamines and other hormones, the mature lung epithelium switches from actively secreting chloride and liquid into the air spaces to actively reabsorbing sodium and liquid 5-6. Increased oxygen tension at birth enhances the capacity of the epithelium to transport sodium and increases gene expression of the epithelial sodium channel (ENaC) followed by transport into the interstitum via basolateral na+/k+-atpase and passive movement of chloride and water through the par cellular and intracellular pathways 6.Epithelial sodium channels play a crucial role in lung liquid clearance at birth. In fact, the first evidence of involvement of these receptors came from measurements of an amiloride-induced drop in potential difference between the nasal epithelium and subcutaneous space in newborns. Gowen et al 7 demonstrated that this potential difference was reduced in infants with TTN (suggesting a defect in sodium trans-port), and recovery from TTN in 1 to 3 days was associated with an increase in potential difference to normal level. Passive resorption of liquid also occurs after birth because 2 of differences among the oncotic pressure of air spaces, interstitium, and blood vessels. The majority of water transport across the apical membrane is thought to occur through aquaporin 5 (AQP5) water channels 8. Materials and Methods This prospective study was conducted on 100 new borns diagnosed with TTN admitted in the Paediatrics Department of Bebe Nanki Mother and Child Care Centre attached to Government Medical College and Hospital, Amritsar. The study criteria of patients are described as follows- Selection of cases Inclusion criteria 1. Neonates (35 to 41 weeks of gestation) diagnosed as TTN (according to Rawling and Smith Criteria) Exclusion criteria 1. Premature neonates [<35 weeks] 2. Neonates requiring respiratory support in form of CPAP and mechanical ventilation. 3. Exclusion of other known respiratory disorders like: Meconium Aspiration- irregular pattern of increased density throughout lung, no meconium staining of skin Respiratory Distress Syndrome- having reticulo-granular pattern in x-rays picture, premature neonates, no surfactant therapy. Congenital heart disease-having murmur, signs of heart failure. Birth asphyxia-history suggestive of intrauterine asphyxia, delayed cry at birth. TTN was diagnosed according to Rawlings and smith 9 which is based on the radiologic and clinical findings- 1] Early(within 6 hours of birth) onset of tachypnea [in uneventful late preterm(35-36weeks)or term newborn]
3 2] Persistence of tachypnea sometimes with retaractions, or expiratory grunting and, occasionally, cyanosis that is relieved by minimal oxygen supplementation. 3] Chest generally sounds clear without rales or rhonchi. Chest radiograph shows: Prominent pulmonary vascular markings. Fluid in the interlobar fissure. Flat diaphragms and rarely pleural effusion. Hyperaeration Blood sugar and electrolytes (serum sodium and potassium levels) were also determined as the base line recording. Two solutions, of which one containing salbutamol and another containing normal saline were prepared.there was no detectable difference in colour, smell, or other physical properties between these two solutions. After diagnosing a patient of TTN, candidates were allotted with a study number and his/her TTN score. Respiratory rate, heart rate and oxygen saturation were recorded. These study numbers corresponded to the order of the patient entering the study. Simple random sampling was done according to a computer generated random number table on a master list to one of the two solutions i.e. salbutamol solution and normal saline solution. Then neonate was nebulised with either of the solution. Both the caregiver and the subject were blinded regarding the drug used for nebulization. sample was collected again at 4 hours after nebulization for serum potassium and glucose levels. Patients received one nebulized dose of either 3ml 0.9% normal saline solution(placebo) or the solution of salbutamol 3 ml (asthalin solution is 5mg/ml) in a normal saline 0.9% solution. The standard dose of salbutamol was calculated according to the weight of the baby i.e. 0.15mg/kg. Solution was given with jet type nebulizer along with continuous flow of oxygen at 5 to 6 litres/min. Administration of the solution was performed by nurse on duty. The dose was administered over 15 minutes, and vital signs were monitored at 30minutes,1 hour and 4 hours 3 after nebulization. Intravenous fluids were given as 60ml/kg in enrolled babies and additional oxygen inhalation was given at 2 litres/min through nasal prongs after the nebulization in both cases and control group. 30minutes, 1 hour and 4 hours after nebulization, following parameters were noted like : Respiratory rate Heart rate Oxygen saturation TTN score 4 hours after nebulization blood sample collected for- Results Serum potassium Blood Glucose levels In the present study 65% of the patients were males and 35% were females( figure 1).The mean age of presentation in hours was 3.80±1.77 hours. We also analysed the patient characteristics like gender distribution, age at which the neonate presented to hospital and gestational age (in weeks) at birth. There were no significant differences between the treatment and control groups with regard to any of the following: gestational age (38.35±1.22 vs 38.52±1.26), birth weight, age at admission to hospital (3.80±1.77 in cases and 3.50±1.77 in control group), initial respiratory rate (73.4±4.5 vs 72.2±4.8) and oxygen saturation on admission (94.7±1.6 vs 94.82±1.76). Figure and table 2 shows the result of nebulization in salbutamol and normal saline group in TTN score. There was no significant difference in between two group statistically. Figure and table 3 shows the respiratory rate between two groups after nebulization, statistically it is not significant difference.
4 Table 1 -TTN SCORE- 10 SCORE 0 POINT 1 POINT 2 POINT 3 POINT Expiratory grunt None Intermittent Continuous - Subcostal retractions None Mild Moderate Severe Cyanosis None At extremities Central - Nasal flaring None Mild Moderate Severe Supraclavicular retractions None Mild Moderate Severe Figure 1 shows the distribution of neonates according to gender 0 Newborns Male % Female % Figure 2: shows the TTN score after nebulization On admission 4hours after nebulization Group S Group NS Table 2: Different values of TTN score in groups at different time interval 4
5 TTN SCORE Group S Group NS p-value Mean SD Mean SD On admission min after nebulization hour after nebulization hours after nebulization Figure 3 shows the respiratory rate in different groups Table 3: Different values of mean (with standard deviation) of respiratory rate in groups at different time interval Respiratory rate Group S Group NS p-value Mean ±SD Mean ±SD On admission min after nebulization hour after nebulization hours after nebulization Discussion 5
6 Present study was undertaken to see the effect of salbutamol nebulization in transient tachypnea of newborn in the following parameters. Clinical characteristics Respiratory rate: In our study the mean respiratory rate of Salbutamol Group (cases) before nebulization was ± 4.5 and it did not decrease significantly 4 hours after nebulization (72.2±5.1). P value was 0.866,which was statistically not significant when we compared it with the respiratory rate of neonates in the control group. This is in contrast to results observed by Armangil D et al 10 which showed significant decrease in respiratory rate (70±19 vs 62±14) and by Venkatamurthy et al 11 respiratory rate was (75.74±5.93 and 66.31±7.41) before and after nebulization respectively. Myo Jing Kim et al 12 showed that there was decrease in the duration of tachypnea after treatment with salbutamol nebulization than in the control group (31.3±23.7 h vs. 53.5±56.8 h, respectively); but this difference was not significant ( P=0.37). However, no differences in the maximum respiratory rates during the acute period after inhalation treatment were observed between the salbutamol inhalation group and the control group. TTN score: In our study the mean TTN score before and after 4 hours nebulization in salbutamol group was (5.7±1.0 and 5.40±1.41) and in control group (5.66±1.12 and 5.76±1.15) and it did not decrease significantly with p-value of The mean TTN score observed before and after salbutamol nebulization in other studies like Armangil D et al is (8 vs. 2.5) and Venkatamurthy et al(8.26±0.44 vs. 5.77±2.07) showed a decrease in TTN score after nebulization. Oxygen Saturation: There was no significant difference with the resultant p-value of 0.32 in the oxygen saturation between the salbutamol (94.78±1.64 on admission and after nebulization) and normal saline group (94.82±1.76 on admission and 95.9±1.88). Int. J. Curr. Res. Med. Sci. (2017). 3(8): Average duration of the hospital stay (in days): Our analysis showed that patients treated with either solution had no significant difference in terms of the duration of hospitalization with p value of >0.05, these results were in accordance with the study done by Myo Jing Kim et al which also showed that the duration of hospitalization was similar between the 2 groups (8.5±3.9 days vs. 8.8±3.2 days in treatment and control group respectively). Short term/immediate adverse effects: Our analysis showed no incidence tachycardia (>180/min) after salbutamol nebulization when compared with normal saline group with p value Heart rate evaluated after salbutamol nebulization (137±7.8) showed no significant increase when compared with normal baseline evaluation at the time of admission (135±9.3). Similar results in heart in both treatment and control group after nebulization were shown by the studies done by the Armangil D et aland Venkatamurthy et al. Specific adverse effect: Our study showed no significant change in the serum potassium levels and blood glucose levels after salbutamol nebulization when they were compared with the normal saline group. Studies done by Armangil et al also showed that after nebulization there was no significant change in serum potassium levels in salbutamol and normal saline group respectively. Conclusion Thus it can be concluded from the present study that 65% of the patients were males and 35% were females. Group which was nebulized with salbutamol did not show statistically significant improvement in the respiratory rate, TTN score and oxygen saturation when compared with the control group (>0.05). T here were no immediate as well as specific side effects observed in the
7 salbutamol group. Average duration of hospital stay (in days) was almost similar between two groups. Thus, we conclude that our results did not show any significant effect of salbutamol nebulization (single dose) in early resolution of symptoms and early discharge of the baby. There is a need to explore the subject further taking larger sample size with change of dosing schedule to show the efficacy of salbutamol, if any, in treatment of the TTN. Source of funding: Nil Conflict of interest: None declared References 1. Avery ME, Gatewood OB, Brumley GE. Transient tachypnea of newborn. Possible delayed resorption of fluid at birth. Am J Dis Child Apr; 111(4): Kienstra KA. Transient tachypnea of the newborn. In: Cloherty JP, Eichenwald EC, Hansen AR, Stark AR. Manual of neonatal care. 7 th ed. New Delhi. Wolters Kluwer, 2011, p Morrison JJ, Resnnie JM, Milton PJ. Neonatal respiratory morbidity and mode of delivery at term: influence of timing of elective caesarean section. Br J Obstet Gynaecol 1995 Feb; 102(2): Liem JJ, Huq SI, Ekuma O,Becker AB, Kozyrskyj AL. Transient tachypnea of newborn may be an early manifestation of wheezing syndrome. J Paediatr 2007 Jul; 15(1): Int. J. Curr. Res. Med. Sci. (2017). 3(8): Aslan E, Tutdibi E, Martens S, Han Y, Monz D, Gortner L. Transient tachypnea of the newborn (TTN): a role for polymorphisms in the beta-adrenergic receptor (ADRB) encoding genes. Acta Paediatr Oct; 97(10): Birnkrant DJ, Picone C, Markowitz W, El khwad M, Shen WJ, Tafari N. Association of the transient tachypnea of newborn and childhood asthma. Pediatr Pulmonol Oct;41(10): Ramachandrappa A, Jain L. Elective cesarean section: its impact on neonatal respiratory outcome. Clin Perinatol. 2006; 35(2): Miller LK, Calenoff L, Boehm JJ, Riedy MJ. Respiratory distress in the newborn. JAMA 1980;243(11): Ambalavan N, Carlo WA. Transient tachypnea of newborn. In: Kliegman RM, Stanton BF, St. Geme JW, Schor NF, Behrman RE. Nelson Textbook of Pediatrics. 19th ed. New Delhi: Elsevier: 2012, p Armangil D, Yurdakok M, Korkmaz A, Yigit S. Tekinalp G. Inhaled salbutamol for the treatment of transient tachypnea of newborn. J Paeditr 2011 Sep; 159(3): Venktamurthy M, Hemachandra Reddy K, Murali SM. Salbutamol nebulization, a Cost- Effective method in treating wetlung. International Journal of Health Information and Medical Research 2014; 1(1): Kim MJ, Yoo JH, Jung JA, Byun SY. The effect of inhaled albuterol in transient tachynea of newborn. Allergy Asthma Immunol Res 2014Mar; 6(2): How to cite this article: Amanpreet Kaur, Pardeep Singh Kahlon, Karnail Singh, MS Pannu. (2017). Effect of salbutamol nebulization in transient tachypnea of newborn. Int. J. Curr. Res. Med. Sci. 3(8): 1-7. DOI: Access this Article in Online Quick Response Code Website: Subject: Medical Sciences 7
The Effects of Inhaled β-adrenergic Agonists in Transient Tachypnea of the Newborn
 645258GPHXXX10.1177/2333794X16645258Global Pediatric HealthKeleş et al research-article2016 Original Article The Effects of Inhaled β-adrenergic Agonists in Transient Tachypnea of the Newborn Global Pediatric
645258GPHXXX10.1177/2333794X16645258Global Pediatric HealthKeleş et al research-article2016 Original Article The Effects of Inhaled β-adrenergic Agonists in Transient Tachypnea of the Newborn Global Pediatric
In the neonatal period, transient tachypnea of the newborn (TTN) is the most frequent cause of early respiratory distress
 Inhaled Beta-2 Agonist Salbutamol for the Treatment of Transient Tachypnea of the Newborn Didem Armangil, MD, Murat Yurdak ok, MD, Ayşe Korkmaz, MD, Şule Yigit, MD, and G ulsevin Tekinalp, MD Objective
Inhaled Beta-2 Agonist Salbutamol for the Treatment of Transient Tachypnea of the Newborn Didem Armangil, MD, Murat Yurdak ok, MD, Ayşe Korkmaz, MD, Şule Yigit, MD, and G ulsevin Tekinalp, MD Objective
A radiological perspective of assessing neonatal respiratory distress syndrome
 Original Research Article A radiological perspective of assessing neonatal respiratory distress syndrome Jayesh Shah 1, Nikhil Parvatkar 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident,
Original Research Article A radiological perspective of assessing neonatal respiratory distress syndrome Jayesh Shah 1, Nikhil Parvatkar 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident,
Review of Neonatal Respiratory Problems
 Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Hyaline membrane disease. By : Dr. Ch Sarishma Peadiatric Pg
 Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Clinicoetiological profile and risk assessment of newborn with respiratory distress in a tertiary care centre in South India
 International Journal of Contemporary Pediatrics Sahoo MR et al. Int J Contemp Pediatr. 2015 Nov;2(4):433-439 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Research Article DOI: http://dx.doi.org/10.18203/2349-3291.ijcp20150990
International Journal of Contemporary Pediatrics Sahoo MR et al. Int J Contemp Pediatr. 2015 Nov;2(4):433-439 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Research Article DOI: http://dx.doi.org/10.18203/2349-3291.ijcp20150990
Presented By : Kamlah Olaimat
 Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME
 INDIAN PEDIATRICS VOLUME 35-FEBRUAKY 1998 ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME Kanya Mukhopadhyay, Praveen Kumar and Anil Narang From the Division of Neonatology, Department
INDIAN PEDIATRICS VOLUME 35-FEBRUAKY 1998 ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME Kanya Mukhopadhyay, Praveen Kumar and Anil Narang From the Division of Neonatology, Department
Furosemide for transient tachypnoea of the newborn (Review)
 Kassab M, Khriesat WM, Bawadi H, Anabrees J This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in The Cochrane Library 2013, Issue 6 http://www.thecochranelibrary.com
Kassab M, Khriesat WM, Bawadi H, Anabrees J This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in The Cochrane Library 2013, Issue 6 http://www.thecochranelibrary.com
SUMPh N. Testemitanu Radiology and Medical imaging department PEDIATRIC IMAGING. M. Crivceanschii, assistant professor
 SUMPh N. Testemitanu Radiology and Medical imaging department PEDIATRIC IMAGING M. Crivceanschii, assistant professor GOALS AND OBJECTIVES to be aware of the role of modern diagnostic imaging modalities
SUMPh N. Testemitanu Radiology and Medical imaging department PEDIATRIC IMAGING M. Crivceanschii, assistant professor GOALS AND OBJECTIVES to be aware of the role of modern diagnostic imaging modalities
MFMU - Background. MFMU - Background MFMU GOALS
 MFMU - Background Highlights From The MFM Units Network Ronald Wapner, MD Modern OB management (especially high risk pregnancies) has adopted principles of care, employed pharmaceuticals, applied methodologies
MFMU - Background Highlights From The MFM Units Network Ronald Wapner, MD Modern OB management (especially high risk pregnancies) has adopted principles of care, employed pharmaceuticals, applied methodologies
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Bronchiolitis: diagnosis and management of bronchiolitis in children. 1.1 Short title Bronchiolitis in children 2 The remit The
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Bronchiolitis: diagnosis and management of bronchiolitis in children. 1.1 Short title Bronchiolitis in children 2 The remit The
Objectives. Case Presentation. Respiratory Emergencies
 Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Infection. Risk factor for infection ACoRN alerting sign with * Clinical deterioration. Problem List. Respiratory. Cardiovascular
 The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) NICU POCKET GUIDE
 Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) TM NICU POCKET GUIDE Patient Selection Diagnoses Patient presents with one or more of the following symptoms: These
Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) TM NICU POCKET GUIDE Patient Selection Diagnoses Patient presents with one or more of the following symptoms: These
Etiological Study of Respiratory Distress in Newborn
 ORIGINAL RESEARCH www.ijcmr.com Etiological Study of P. Brahmaiah 1, K. Rami Reddy 2 ABSTRACT Introduction: Respiratory distress is one of the commonest disorder encountered within the first 48-72 hours
ORIGINAL RESEARCH www.ijcmr.com Etiological Study of P. Brahmaiah 1, K. Rami Reddy 2 ABSTRACT Introduction: Respiratory distress is one of the commonest disorder encountered within the first 48-72 hours
PFIZER INC. THERAPEUTIC AREA AND FDA APPROVED INDICATIONS: See USPI.
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
** SURFACTANT THERAPY**
 ** SURFACTANT THERAPY** Full Title of Guideline: Surfactant Therapy Author (include email and role): Stephen Wardle (V4) Reviewed by Dushyant Batra Consultant Neonatologist Division & Speciality: Division:
** SURFACTANT THERAPY** Full Title of Guideline: Surfactant Therapy Author (include email and role): Stephen Wardle (V4) Reviewed by Dushyant Batra Consultant Neonatologist Division & Speciality: Division:
Radiological evaluation of neonatal lesions in 118 neonates
 Original Research Article ISSN: 394-006 (P) Radiological evaluation of neonatal thoracic lesions in 8 neonates Konark Sarvaiya *, Himanshu Singla, Nirav Patel, Jai Inder Dhillon, Babubhai Patel 3 nd year
Original Research Article ISSN: 394-006 (P) Radiological evaluation of neonatal thoracic lesions in 8 neonates Konark Sarvaiya *, Himanshu Singla, Nirav Patel, Jai Inder Dhillon, Babubhai Patel 3 nd year
Risk of Wheezing Attacks in Infants With Transient Tachypnea Newborns
 Iran J Pediatr. 2016 February; 26(1): e2295. Published online 2016 January 30. doi: 10.5812/ijp.2295 Research Article Risk of Wheezing Attacks in Infants With Transient Tachypnea Newborns Mohammad Golshantafti,
Iran J Pediatr. 2016 February; 26(1): e2295. Published online 2016 January 30. doi: 10.5812/ijp.2295 Research Article Risk of Wheezing Attacks in Infants With Transient Tachypnea Newborns Mohammad Golshantafti,
COMPLICATED STAPHYLOCOCCAL INFECTION IN A NEONATE. A. Ansary*, D. Varghese, L. Jackson ROYAL HOSPITAL FOR CHILDREN, GLASGOW,UK
 COMPLICATED STAPHYLOCOCCAL INFECTION IN A NEONATE A. Ansary*, D. Varghese, L. Jackson ROYAL HOSPITAL FOR CHILDREN, GLASGOW,UK Complicated staphylococcal infection in a neonate Overview Case Radiology/biochemistry/microbiology
COMPLICATED STAPHYLOCOCCAL INFECTION IN A NEONATE A. Ansary*, D. Varghese, L. Jackson ROYAL HOSPITAL FOR CHILDREN, GLASGOW,UK Complicated staphylococcal infection in a neonate Overview Case Radiology/biochemistry/microbiology
Respiratory Disorders in the Newborn: Identification and Diagnosis Hany Aly. DOI: /pir
 Respiratory Disorders in the Newborn: Identification and Diagnosis Hany Aly Pediatr. Rev. 2004;25;201-208 DOI: 10.1542/pir.25-6-201 The online version of this article, along with updated information and
Respiratory Disorders in the Newborn: Identification and Diagnosis Hany Aly Pediatr. Rev. 2004;25;201-208 DOI: 10.1542/pir.25-6-201 The online version of this article, along with updated information and
Asthma Care in the Emergency Department Clinical Practice Guideline
 Asthma Care in the Emergency Department Clinical Practice Guideline Inclusion: 1) Children 2 years of age or older with a prior history of wheezing, and 2) Children less than 2 years of age with likely
Asthma Care in the Emergency Department Clinical Practice Guideline Inclusion: 1) Children 2 years of age or older with a prior history of wheezing, and 2) Children less than 2 years of age with likely
BRONCHIOLITIS. See also the PSNZ guideline - Wheeze & Chest Infections in infants under 1 year (www.paediatrics.org.nz)
 Definition What is Bronchiolitis? Assessment Management Flow Chart Admission Guidelines Investigations Management Use of Bronchodilators Other treatments Discharge Planning Bronchiolitis & Asthma References
Definition What is Bronchiolitis? Assessment Management Flow Chart Admission Guidelines Investigations Management Use of Bronchodilators Other treatments Discharge Planning Bronchiolitis & Asthma References
Simulation 08: Cyanotic Preterm Infant in Respiratory Distress
 Flow Chart Simulation 08: Cyanotic Preterm Infant in Respiratory Distress Opening Scenario Section 1 Type: DM As staff therapist assigned to a Level 2 NICU in a 250 bed rural medical center you are called
Flow Chart Simulation 08: Cyanotic Preterm Infant in Respiratory Distress Opening Scenario Section 1 Type: DM As staff therapist assigned to a Level 2 NICU in a 250 bed rural medical center you are called
Chest X rays and Case Studies. No disclosures. Outline 5/31/2018. Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital
 Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
The Early use of CPAP in Neonatal Pneumonia: Randomized Control Trial.
 DOI: 1.176/aimdr.18...PE Original Article ISSN (O):395-8; ISSN (P):395-81 The Early use of CPAP in Neonatal Pneumonia: Randomized Control Trial. Dinesh Munian 1, Ratan Kumar Biswas, Ranajit Mukherjee 3
DOI: 1.176/aimdr.18...PE Original Article ISSN (O):395-8; ISSN (P):395-81 The Early use of CPAP in Neonatal Pneumonia: Randomized Control Trial. Dinesh Munian 1, Ratan Kumar Biswas, Ranajit Mukherjee 3
1st Annual Clinical Simulation Conference
 1st Annual Clinical Simulation Conference Newborns with Acute Respiratory Distress: Diagnosis and Management Ma Teresa C. Ambat, MD Assistant Professor Division of Neonatology, Department of Pediatrics
1st Annual Clinical Simulation Conference Newborns with Acute Respiratory Distress: Diagnosis and Management Ma Teresa C. Ambat, MD Assistant Professor Division of Neonatology, Department of Pediatrics
Approach to Bronchiolitis
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Approach to Bronchiolitis. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Approach to Bronchiolitis. These podcasts are designed to give medical students an overview of key topics in pediatrics.
Wheezy? Easy Peasy! The Emergent Management of Asthma & Bronchiolitis. Maneesha Agarwal MD Assistant Professor of Pediatrics & Emergency Medicine
 Wheezy? Easy Peasy! The Emergent Management of Asthma & Bronchiolitis Maneesha Agarwal MD Assistant Professor of Pediatrics & Emergency Medicine Asthma Defined National Asthma Education and Prevention
Wheezy? Easy Peasy! The Emergent Management of Asthma & Bronchiolitis Maneesha Agarwal MD Assistant Professor of Pediatrics & Emergency Medicine Asthma Defined National Asthma Education and Prevention
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Surfactant Administration
 Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Pediatric Bronchiolitis. Janie Robles, PharmD, AE-C Assistant Professor of Pharmacy Practice Pediatrics School of Pharmacy TTUHSC Lubbock, Texas
 This PowerPoint file is a supplement to the video presentation. Some of the educational content of this program is not available solely through the PowerPoint file. Participants should use all materials
This PowerPoint file is a supplement to the video presentation. Some of the educational content of this program is not available solely through the PowerPoint file. Participants should use all materials
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
CLINICAL MEETING CASE PRESENTATION : by DR.K.ADITYA 1 ST yr PG DEPARTMENT OF PEDIATRICS
 CLINICAL MEETING 14-9-2017 CASE PRESENTATION : by DR.K.ADITYA 1 ST yr PG DEPARTMENT OF PEDIATRICS Case History Baby A Age: 7 months Male Baby Residence: Miryalguda, Nalgonda DOA : 17-8-17 around 5 PM Chief
CLINICAL MEETING 14-9-2017 CASE PRESENTATION : by DR.K.ADITYA 1 ST yr PG DEPARTMENT OF PEDIATRICS Case History Baby A Age: 7 months Male Baby Residence: Miryalguda, Nalgonda DOA : 17-8-17 around 5 PM Chief
Low dose versus standard dose Insulin infusion therapy in Pediatric Diabetic Ketoacidosis - A Randomized Clinical Trial
 INTERNATIONAL JOURNAL OF CURRENT RESEARCH IN BIOLOGY AND MEDICINE ISSN: 2455-944X www.darshanpublishers.com DOI:10.22192/ijcrbm Volume 3, Issue 3-2018 Original Research Article DOI: http://dx.doi.org/10.22192/ijcrbm.2018.03.03.006
INTERNATIONAL JOURNAL OF CURRENT RESEARCH IN BIOLOGY AND MEDICINE ISSN: 2455-944X www.darshanpublishers.com DOI:10.22192/ijcrbm Volume 3, Issue 3-2018 Original Research Article DOI: http://dx.doi.org/10.22192/ijcrbm.2018.03.03.006
AEROSURF Phase 2 Program Update Investor Conference Call
 AEROSURF Phase 2 Program Update Investor Conference Call November 12, 2015 Forward Looking Statement To the extent that statements in this presentation are not strictly historical, including statements
AEROSURF Phase 2 Program Update Investor Conference Call November 12, 2015 Forward Looking Statement To the extent that statements in this presentation are not strictly historical, including statements
Dr. (Kate) Katherine Miller GUELPH ON 121 RESPIRATORY DISTRESS IN THE NEWBORN
 Society of Rural Physicians of Canada 26TH ANNUAL RURAL AND REMOTE MEDICINE COURSE ST. JOHN'S NEWFOUNDLAND AND LABRADOR APRIL 12-14, 2018 Dr. (Kate) Katherine Miller GUELPH ON 121 RESPIRATORY DISTRESS
Society of Rural Physicians of Canada 26TH ANNUAL RURAL AND REMOTE MEDICINE COURSE ST. JOHN'S NEWFOUNDLAND AND LABRADOR APRIL 12-14, 2018 Dr. (Kate) Katherine Miller GUELPH ON 121 RESPIRATORY DISTRESS
Epidemiology of admissions with respiratory illnesses: a single tertiary centre experience
 International Journal of Contemporary Pediatrics Das S et al. Int J Contemp Pediatr. 2017 Mar;4(2):378-382 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3291.ijcp20170005
International Journal of Contemporary Pediatrics Das S et al. Int J Contemp Pediatr. 2017 Mar;4(2):378-382 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3291.ijcp20170005
BRONCHIOLITIS PEDIATRIC
 DEFINITION Bronchiolitis is typically defined as the first episode of wheezing in infants < 24 months of age. It is a viral illness of the lower respiratory tract that causes tachypnea, bronchospasm, and
DEFINITION Bronchiolitis is typically defined as the first episode of wheezing in infants < 24 months of age. It is a viral illness of the lower respiratory tract that causes tachypnea, bronchospasm, and
PAEDIATRIC ACUTE CARE GUIDELINE. Croup. This document should be read in conjunction with this DISCLAIMER
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Croup Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Croup Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia
 Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Neonatal Resuscitation in What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011
 Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
A study of clinico-biochemical profile of neonatal seizure: A tertiary care hospital study
 Original Research Article A study of clinico-biochemical profile of neonatal seizure: A tertiary care hospital study Wakil Paswan 1*, Bankey Behari Singh 2 1 Assistant Professor, 2 Associate Professor
Original Research Article A study of clinico-biochemical profile of neonatal seizure: A tertiary care hospital study Wakil Paswan 1*, Bankey Behari Singh 2 1 Assistant Professor, 2 Associate Professor
Home-Made Continuous Positive Airways Pressure Device may Reduce Mortality in Neonates with Respiratory Distress in Low-Resource Setting
 JOURNAL OF TROPICAL PEDIATRICS, VOL. 60, NO. 5, 2014 Home-Made Continuous Positive Airways Pressure Device may Reduce Mortality in Neonates with Respiratory Distress in Low-Resource Setting by Subhashchandra
JOURNAL OF TROPICAL PEDIATRICS, VOL. 60, NO. 5, 2014 Home-Made Continuous Positive Airways Pressure Device may Reduce Mortality in Neonates with Respiratory Distress in Low-Resource Setting by Subhashchandra
PRACTICE GUIDELINES WOMEN S HEALTH PROGRAM
 C Title: NEWBORN: HYPOGLYCEMIA IN NEONATES BORN AT 35+0 WEEKS GESTATION AND GREATER: DIAGNOSIS AND MANAGEMENT IN THE FIRST 72 HOURS Authorization Section Head, Neonatology, Program Director, Women s Health
C Title: NEWBORN: HYPOGLYCEMIA IN NEONATES BORN AT 35+0 WEEKS GESTATION AND GREATER: DIAGNOSIS AND MANAGEMENT IN THE FIRST 72 HOURS Authorization Section Head, Neonatology, Program Director, Women s Health
Practical Application of CPAP
 CHAPTER 3 Practical Application of CPAP Dr. Srinivas Murki Neonatologist Fernadez Hospital, Hyderabad. A.P. Practical Application of CPAP Continuous positive airway pressure (CPAP) applied to premature
CHAPTER 3 Practical Application of CPAP Dr. Srinivas Murki Neonatologist Fernadez Hospital, Hyderabad. A.P. Practical Application of CPAP Continuous positive airway pressure (CPAP) applied to premature
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
PUMANI bcpap GUIDELINES FOR CLINICIANS. An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use
 An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use What is bcpap? bcpap stands for bubble Continuous Positive Airway Pressure. Sometimes called Continuous Distending Pressure,
An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use What is bcpap? bcpap stands for bubble Continuous Positive Airway Pressure. Sometimes called Continuous Distending Pressure,
Neurodevelopmental Risk?
 Normal Newborn During transitional hypoglycemia normal newborns have an enhanced ketogenic response to fasting. Newborn brains have enhanced capability to use ketone bodies for fuel Allows newborns to
Normal Newborn During transitional hypoglycemia normal newborns have an enhanced ketogenic response to fasting. Newborn brains have enhanced capability to use ketone bodies for fuel Allows newborns to
Subject: Inhaled Nitric Oxide
 07-00007-12 Original Effective Date: 04/15/01 Reviewed: 09/27/18 Revised: 10/15/18 Subject: Inhaled Nitric Oxide THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION, EXPLANATION OF BENEFITS,
07-00007-12 Original Effective Date: 04/15/01 Reviewed: 09/27/18 Revised: 10/15/18 Subject: Inhaled Nitric Oxide THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION, EXPLANATION OF BENEFITS,
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION
 CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL
 AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL A. Definition of Therapy: 1. Cough machine: 4 sets of 5 breaths with a goal of I:E pressures approximately the same of 30-40. Inhale time = 1 second, exhale
AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL A. Definition of Therapy: 1. Cough machine: 4 sets of 5 breaths with a goal of I:E pressures approximately the same of 30-40. Inhale time = 1 second, exhale
A study of neonatal and maternal outcomes of asthma during pregnancy
 International Journal of Research in Medical Sciences Meena BL et al. Int J Res Med Sci. 2013 Feb;1(1):23-27 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: 10.5455/2320-6012.ijrms20130206
International Journal of Research in Medical Sciences Meena BL et al. Int J Res Med Sci. 2013 Feb;1(1):23-27 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: 10.5455/2320-6012.ijrms20130206
Infant Of Diabetic Mother(IDM)
 Infant Of Diabetic Mother(IDM) Sangram Satish Magar 1, Sanskriti Mirashi 2 1. M.D. Sch.(Kaumarbhrutya-Balrog) 2.Guide (Kaumarbhrutya-Balrog), L.R.P.Medical college,islampur,tal- Walwa, dist- Sangli, Maharashtra,
Infant Of Diabetic Mother(IDM) Sangram Satish Magar 1, Sanskriti Mirashi 2 1. M.D. Sch.(Kaumarbhrutya-Balrog) 2.Guide (Kaumarbhrutya-Balrog), L.R.P.Medical college,islampur,tal- Walwa, dist- Sangli, Maharashtra,
-Tamara Wahbeh. -Razan Abu Rumman. Dr. Mohammed Al-Muhtaseb
 -2 -Tamara Wahbeh -Razan Abu Rumman Dr. Mohammed Al-Muhtaseb I tried to include everything the doctor mentioned in both the lecture and his slides in the simplest way possible, so hopefully there would
-2 -Tamara Wahbeh -Razan Abu Rumman Dr. Mohammed Al-Muhtaseb I tried to include everything the doctor mentioned in both the lecture and his slides in the simplest way possible, so hopefully there would
NRP Raising the Bar for Providers and Instructors
 NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy
 An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
BPD. Neonatal/Pediatric Cardiopulmonary Care. Disease. Bronchopulmonary Dysplasia. Baby Jane
 1 Neonatal/Pediatric Cardiopulmonary Care Disease 2 Bronchopulmonary Dysplasia 3 is a 33-day-old prematurely born girl who weighs 1420 g. At birth, her estimated gestational age was 28 weeks. Her initial
1 Neonatal/Pediatric Cardiopulmonary Care Disease 2 Bronchopulmonary Dysplasia 3 is a 33-day-old prematurely born girl who weighs 1420 g. At birth, her estimated gestational age was 28 weeks. Her initial
Respiratory Management in Pediatrics
 Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
5 Million neonatal deaths each year worldwide. 20% caused by neonatal asphyxia. Improvement of the outcome of 1 million newborns every year
 1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
Fluid & Electrolyte Balances in Term & Preterm Infants. Carolyn Abitbol, M.D. University of Miami/ Holtz Children s Hospital
 Fluid & Electrolyte Balances in Term & Preterm Infants Carolyn Abitbol, M.D. University of Miami/ Holtz Children s Hospital Objectives Review maintenance fluid & electrolyte requirements in neonates Discuss
Fluid & Electrolyte Balances in Term & Preterm Infants Carolyn Abitbol, M.D. University of Miami/ Holtz Children s Hospital Objectives Review maintenance fluid & electrolyte requirements in neonates Discuss
Provide guidelines for the management of mechanical ventilation in infants <34 weeks gestation.
 Page 1 of 5 PURPOSE: Provide guidelines for the management of mechanical ventilation in infants
Page 1 of 5 PURPOSE: Provide guidelines for the management of mechanical ventilation in infants
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 3 rd Week Discussion with Dr. Muna Al-Jufairi (Part 2)
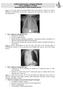 Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 3 rd Week Discussion with Dr. Muna Al-Jufairi (Part 2) - Case 1: a 32 weeks preterm developed RDS 4 hours after delivery. Chest X-ray shows:
Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 3 rd Week Discussion with Dr. Muna Al-Jufairi (Part 2) - Case 1: a 32 weeks preterm developed RDS 4 hours after delivery. Chest X-ray shows:
Pediatric Assessment Triangle
 Pediatric Assessment Triangle Katherine Remick, MD, FAAP Associate Medical Director Austin Travis County EMS Pediatric Emergency Medicine Dell Children s Medical Center Objectives 1. Discuss why the Pediatric
Pediatric Assessment Triangle Katherine Remick, MD, FAAP Associate Medical Director Austin Travis County EMS Pediatric Emergency Medicine Dell Children s Medical Center Objectives 1. Discuss why the Pediatric
PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني
 Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
Usefulness of DuoPAP in the treatment of very low birth weight preterm infants with neonatal respiratory distress syndrome
 European Review for Medical and Pharmacological Sciences 2015; 19: 573-577 Usefulness of DuoPAP in the treatment of very low birth weight preterm infants with neonatal respiratory distress syndrome B.
European Review for Medical and Pharmacological Sciences 2015; 19: 573-577 Usefulness of DuoPAP in the treatment of very low birth weight preterm infants with neonatal respiratory distress syndrome B.
SWISS SOCIETY OF NEONATOLOGY. Supercarbia in an infant with meconium aspiration syndrome
 SWISS SOCIETY OF NEONATOLOGY Supercarbia in an infant with meconium aspiration syndrome January 2006 2 Wilhelm C, Frey B, Department of Intensive Care and Neonatology, University Children s Hospital Zurich,
SWISS SOCIETY OF NEONATOLOGY Supercarbia in an infant with meconium aspiration syndrome January 2006 2 Wilhelm C, Frey B, Department of Intensive Care and Neonatology, University Children s Hospital Zurich,
Received: Jun 15, 2013; Accepted: Nov 08, 2013; First Online Available: Jan 24, 2014
 Original Article Iran J Pediatr Feb 2014; Vol 24 (No 1), Pp: 57-63 Management of Neonatal Respiratory Distress Syndrome Employing ACoRN Respiratory Sequence Protocol versus Early Nasal Continuous Positive
Original Article Iran J Pediatr Feb 2014; Vol 24 (No 1), Pp: 57-63 Management of Neonatal Respiratory Distress Syndrome Employing ACoRN Respiratory Sequence Protocol versus Early Nasal Continuous Positive
The Turkish Journal of Pediatrics 2014; 56:
 The Turkish Journal of Pediatrics 2014; 56: 232-237 Original INSURE method (INtubation-SURfactant-Extubation) in early and late premature neonates with respiratory distress: factors affecting the outcome
The Turkish Journal of Pediatrics 2014; 56: 232-237 Original INSURE method (INtubation-SURfactant-Extubation) in early and late premature neonates with respiratory distress: factors affecting the outcome
Under-five and infant mortality constitutes. Validation of IMNCI Algorithm for Young Infants (0-2 months) in India
 R E S E A R C H P A P E R Validation of IMNCI Algorithm for Young Infants (0-2 months) in India SATNAM KAUR, V SINGH, AK DUTTA AND J CHANDRA From the Department of Pediatrics, Kalawati Saran Children s
R E S E A R C H P A P E R Validation of IMNCI Algorithm for Young Infants (0-2 months) in India SATNAM KAUR, V SINGH, AK DUTTA AND J CHANDRA From the Department of Pediatrics, Kalawati Saran Children s
Nguyen Tien Dung A/Prof. PhD. MD Head of Pediatric Department - Bach Mai Hospital
 Nguyen Tien Dung A/Prof. PhD. MD Head of Pediatric Department - Bach Mai Hospital A girl patient 11 years old admitted to Bach mai Hospital at 4h15, 12nd November because of difficult breathing She has
Nguyen Tien Dung A/Prof. PhD. MD Head of Pediatric Department - Bach Mai Hospital A girl patient 11 years old admitted to Bach mai Hospital at 4h15, 12nd November because of difficult breathing She has
SCVMC RESPIRATORY CARE PROCEDURE
 Page 1 of 8 Rev. - 11/99, 11/05, 4/11 R-NC - 08/99,08/00, 04/03,10/08,04/09, 07/11, 6/12 B7180-43 OBJECTIVE Continuous Nebulization allows for continuous, controlled drug delivery to the lung, avoiding
Page 1 of 8 Rev. - 11/99, 11/05, 4/11 R-NC - 08/99,08/00, 04/03,10/08,04/09, 07/11, 6/12 B7180-43 OBJECTIVE Continuous Nebulization allows for continuous, controlled drug delivery to the lung, avoiding
Simulation 1: Two Year-Old Child in Respiratory Distress
 Simulation 1: Two Year-Old Child in Respiratory Distress Opening Scenario (Links to Section 1) You are the respiratory therapist in a 300 bed community hospital working the evening shift. At 8:30 PM you
Simulation 1: Two Year-Old Child in Respiratory Distress Opening Scenario (Links to Section 1) You are the respiratory therapist in a 300 bed community hospital working the evening shift. At 8:30 PM you
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Admission/Discharge Form for Infants Born in Please DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Appendix 1. Causes of Neonatal Deaths. Interval between. Gestation at birth. birth and death. Allocation. (weeks +days ) Cause of death.
 Appendix 1. Causes of Neonatal Deaths Interval between Gestation at birth birth and death Allocation (weeks +days ) (days) Cause of death Amnioinfusion 25 +1/7 20 Respiratory and circulatory insufficiency
Appendix 1. Causes of Neonatal Deaths Interval between Gestation at birth birth and death Allocation (weeks +days ) (days) Cause of death Amnioinfusion 25 +1/7 20 Respiratory and circulatory insufficiency
Respiratory Distress Syndrome
 Respiratory Distress Syndrome -Introduction: Generally speaking, there s an overlap between the presentations of cardiac and respiratory illnesses in neonates. Also there s a considerable overlap between
Respiratory Distress Syndrome -Introduction: Generally speaking, there s an overlap between the presentations of cardiac and respiratory illnesses in neonates. Also there s a considerable overlap between
ORIGINAL ARTICLE. DD Woodhead, DK Lambert, JM Clark and RD Christensen. Intermountain Healthcare, McKay-Dee Hospital, Ogden, UT, USA
 ORIGINAL ARTICLE Comparing two methods of delivering high-flow gas therapy by nasal cannula following endotracheal extubation: a prospective, randomized, masked, crossover trial DD Woodhead, DK Lambert,
ORIGINAL ARTICLE Comparing two methods of delivering high-flow gas therapy by nasal cannula following endotracheal extubation: a prospective, randomized, masked, crossover trial DD Woodhead, DK Lambert,
Efficacy of Nebulised Ipratropium in Acute Bronchial Asthma
 ORIGINAL ARTICLE JIACM 2002; 3(4): 353-59 Efficacy of Nebulised Ipratropium in Acute Bronchial Asthma Praveen Aggarwal*, Onkar Singh**, Jyoti P Wali***, Rohini Handa*, Sada N Dwivedi****, Ashutosh Biswas*****,
ORIGINAL ARTICLE JIACM 2002; 3(4): 353-59 Efficacy of Nebulised Ipratropium in Acute Bronchial Asthma Praveen Aggarwal*, Onkar Singh**, Jyoti P Wali***, Rohini Handa*, Sada N Dwivedi****, Ashutosh Biswas*****,
Bubble CPAP for Respiratory Distress Syndrome in Preterm Infants
 R E S E A R C H P A P E R Bubble CPAP for Respiratory Distress Syndrome in Preterm Infants JAGDISH KOTI*, SRINIVAS MURKI, PRAMOD GADDAM, ANUPAMA REDDY AND M DASARADHA RAMI REDDY From Fernandez Hospital
R E S E A R C H P A P E R Bubble CPAP for Respiratory Distress Syndrome in Preterm Infants JAGDISH KOTI*, SRINIVAS MURKI, PRAMOD GADDAM, ANUPAMA REDDY AND M DASARADHA RAMI REDDY From Fernandez Hospital
When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영
 When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영 The Korean Society of Cardiology COI Disclosure Eun-Young Choi The author have no financial conflicts of interest to disclose
When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영 The Korean Society of Cardiology COI Disclosure Eun-Young Choi The author have no financial conflicts of interest to disclose
SWISS SOCIETY OF NEONATOLOGY. Pulmonary complications of congenital listeriosis in a preterm infant
 SWISS SOCIETY OF NEONATOLOGY Pulmonary complications of congenital listeriosis in a preterm infant April 2009 2 Mészàros A, el Helou S, Zimmermann U, Berger TM, Neonatal and Pediatric Intensive Care Unit
SWISS SOCIETY OF NEONATOLOGY Pulmonary complications of congenital listeriosis in a preterm infant April 2009 2 Mészàros A, el Helou S, Zimmermann U, Berger TM, Neonatal and Pediatric Intensive Care Unit
PAEDIATRIC ACUTE CARE GUIDELINE. Bronchiolitis
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Bronchiolitis Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Bronchiolitis Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read
Learning Objectives. At the conclusion of this module, participants should be better able to:
 Learning Objectives At the conclusion of this module, participants should be better able to: Treat asymptomatic neonatal hypoglycemia with buccal dextrose gel Develop patient-specific approaches to intravenous
Learning Objectives At the conclusion of this module, participants should be better able to: Treat asymptomatic neonatal hypoglycemia with buccal dextrose gel Develop patient-specific approaches to intravenous
Kugelman A, Riskin A, Said W, Shoris I, Mor F, Bader D.
 Heated, Humidified High-Flow Nasal Cannula (HHHFNC) vs. Nasal Intermittent Positive Pressure Ventilation (NIPPV) for the Primary Treatment of RDS, A Randomized, Controlled, Prospective, Pilot Study Kugelman
Heated, Humidified High-Flow Nasal Cannula (HHHFNC) vs. Nasal Intermittent Positive Pressure Ventilation (NIPPV) for the Primary Treatment of RDS, A Randomized, Controlled, Prospective, Pilot Study Kugelman
PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1
 PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1 Module A1 In-patient management of acute respiratory illness 1. Record of a total of 50 cases in 24 36 months to reflect competencies outlined in curriculum Bronchiolitis
PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1 Module A1 In-patient management of acute respiratory illness 1. Record of a total of 50 cases in 24 36 months to reflect competencies outlined in curriculum Bronchiolitis
Management of Common Respiratory Disorders in Children. Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016
 Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
Management of Common Respiratory Disorders in Children. Disclosures. Roadmap 6/10/2016
 Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
PAEDIATRIC RESPIRATORY FAILURE. Tang Swee Fong Department of Paediatrics University Kebangsaan Malaysia Medical Centre
 PAEDIATRIC RESPIRATORY FAILURE Tang Swee Fong Department of Paediatrics University Kebangsaan Malaysia Medical Centre Outline of lecture Bronchiolitis Bronchopulmonary dysplasia Asthma ARDS Bronchiolitis
PAEDIATRIC RESPIRATORY FAILURE Tang Swee Fong Department of Paediatrics University Kebangsaan Malaysia Medical Centre Outline of lecture Bronchiolitis Bronchopulmonary dysplasia Asthma ARDS Bronchiolitis
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
Morbidity profile of infants of mothers with gestational diabetes admitted to a tertiary care centre
 International Journal of Contemporary Pediatrics Devi Meenakshi K. BB et al. Int J Contemp Pediatr. 2017 May;4(3):960-965 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article
International Journal of Contemporary Pediatrics Devi Meenakshi K. BB et al. Int J Contemp Pediatr. 2017 May;4(3):960-965 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article
 NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
Sample. Affix patient label within this box.
 Instructions for completing orders Complete pages 1-3 for General Inpatient Orders. All pathway compatible orders (indicated by ) within the General Inpatient Orders will be followed automatically. Optional
Instructions for completing orders Complete pages 1-3 for General Inpatient Orders. All pathway compatible orders (indicated by ) within the General Inpatient Orders will be followed automatically. Optional
PEDIATRIC ASTHMA INPATIENT CARE MAP
 DATE PATIENT PEDIATRIC ASTHMA INPATIENT CARE MAP DOB HSC NO. PHIN Approved by the Winnipeg Regional Health Authority This Care Map is to be used as a guideline and in no way replaces sound clinical judgment
DATE PATIENT PEDIATRIC ASTHMA INPATIENT CARE MAP DOB HSC NO. PHIN Approved by the Winnipeg Regional Health Authority This Care Map is to be used as a guideline and in no way replaces sound clinical judgment
OBSERVATION UNIT ASTHMA PATHWAY OUTLINE Westmoreland Hospital PAGE 1 OF 5
 PAGE 1 OF 5 Exclusion Criteria: (Reason to admit to hospital) A. New EKG changes except sinus tachycardia B. Respiratory Rate > 40 C. Signs/symptoms of Heart Failure D. Impending respiratory failure or
PAGE 1 OF 5 Exclusion Criteria: (Reason to admit to hospital) A. New EKG changes except sinus tachycardia B. Respiratory Rate > 40 C. Signs/symptoms of Heart Failure D. Impending respiratory failure or
Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis
 Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis Gal S, Riskin A, Chistyakov I, Shifman N, Srugo I, and Kugelman A Pediatric Department and Pediatric Pulmonary Unit Bnai Zion
Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis Gal S, Riskin A, Chistyakov I, Shifman N, Srugo I, and Kugelman A Pediatric Department and Pediatric Pulmonary Unit Bnai Zion
