Diagnosis and treatment of vascular brain-stem malformations
|
|
|
- Annis Tamsin Allen
- 5 years ago
- Views:
Transcription
1 J Neurosurg 72:27-34, 1990 Diagnosis and treatment of vascular brain-stem malformations SHIRO KASHIWAGI, M.D., HARRY R. VAN LOVEREN, M.D., JOHN M. TEW, JR., M.D., J. GEOFFREY WIOT, M.D., STUART n. WELL, M.D., AND ROBERT A. LUKIN, M.D. Departments of Neurosurgery and Radiology, University of Cincinnati College of Medicine, and the Mayfield Neurological Institute, Cincinnati, Ohio Vascular malformations are a common cause of spontaneous brain-stem hemorrhage in young normotensive individuals. These lesions are no longer cryptic. Magnetic resonance (MR) imaging has renewed interest in the treatment of this disorder because of the precise accuracy in diagnosis and localization of these lesions that it affords. The MR image demonstrates characteristic findings of multiple hemorrhages of varying ages surrounded by a hypointense peripheral zone of hemosiderin. Five cases of vascular brain-stem malformation diagnosed with MR imaging are described. The vascular malformations could be demonstrated as "flow void" areas in three cases. Three patients were treated surgically and vascular malformations were confirmed; all three patients improved postoperatively. Two patients were treated nonsurgically; one of these recovered from a second hemorrhage and the other experienced neurological deterioration after a single hemorrhage. Highenergy radiotherapy was not effective for the one vascular malformation treated by this method. This experience suggests that surgical exploration should be considered for vascular brain-stem malformations when the diagnosis is confirmed by MR criteria and the clinical course and lesion are both progressive in character. KEY WORDS " vascular malformation 9 pontine hematoma brain stem 9 magnetic resonance imaging T HE recent development of magnetic resonance (MR) imaging has renewed interest in vascular malformations of the brain stem. 13,14,21,36 Pathological studies indicate that the pons is one of the most common sites of these malformations. 26'27'48 Their association with primary pontine hemorrhage in young, normotensive individuals makes premorbid recognition vitally important. Vascular malformations have been confirmed histologically in autopsy cases of pontine hematoma 23'38,43 and in several cases of surgically evacuated pontine hematoma. 7,I2,33"34"4~ Preoperative diagnosis has been difficult due to poor resolution of computerized tomography (CT) scans in the retroclival region. 3-5'29 Total surgical removal has not been documented prior to this report. The clinical diagnosis is frequently obscure. These malformations may present a course that mimics neoplastic disease, 1~ demyelinating disease, ~'2'7'2~ 23,42 and acute and subacute cerebral infarction) 6"9'3~ The natural history of these lesions is poorly documented. Most reported cases present with signs and symptoms of progressive brain-stem deterioration characterized by recurring hemorrhage. The end-point of the follow-up period for patients in these series is major disability, 24.26,43 surgical treatment, 4' ~ 1,15, i s, 19,2s,28,30-34,40,41, 44,50,51 or death. We present five cases of pontine hematoma due to vascular malformations which were not visualized by angiography but were diagnosed by MR imaging. The patients ranged in age from 22 to 36 years. There were three females and two males. The multiplanar imaging capability of the MR technology provides accurate localization of brain-stem lesions and documents a surgical corridor to the lesion which minimizes operative trauma. Case 1 Case Reports This 25-year-old left-handed man had been well until 1 month prior to admission, when he noted the sudden onset of paresthesias and incoordination of the left hand. These symptoms progressed over several days with development of diplopia on right gaze and weakness of the left upper extremity. J. Neurosurg. / Volume 72/January,
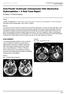
2 S. Kashiwagi, et al. FIG. 1. Case 1. Magnetic resonance images, sagittal Trweighted (spin-echo, TR 500/TE 20 msec) image (left) and axial T2-weighted (spin-echo, TR 2000/TE 80 msec) image (right), showing signal changes of acute hemorrhage (deoxyhemoglobin) and subacute hemorrhage (intracellular and free methemoglobin) within the pons. Hypointense nodule (arrow, left) anterior to the pontine mass probably represents hemosiderin from a remote hemorrhage. Curvilinear hypointensity (arrow, right) is believed to represent a "flow void" area within a vessel. Examination. Pertinent findings on neurological examination consisted of fight abducens nerve palsy, hypesthesia and hypalgesia over the left side of the face, bilaterally diminished gag reflex, mild weakness of the left upper extremity, diminished fine motor skills, and a left Babinski reflex. Contrast-enhanced CT showed multiple abnormal vessels in the lateral walls of the fourth ventricle. Angiography demonstrated abnormal vessels in the venous phase representing a venous angioma. An MR study showed a 1.5-cm pontomedullary mass with signal changes characteristic of subacute and acute hemorrhage. Adjacent to the mass were multiple serpiginous signal-void areas, indicating flowing blood in aberrant vessels (Fig. 1). Operation. Surgical exploration was performed with the patient in the lateral-oblique position. A midline suboccipital craniotomy was created with section of the inferior cerebellar vermis. Two large veins were identified to the right of midline on the floor of the fourth ventricle at the level of the facial colliculi. The vein entered the floor of the fourth ventricle lateral to the median raphe. These large veins were coagulated with bipolar cautery and the brain stem was entered between them. A hematoma was evacuated and several smaller veins were coagulated. No attempt was made to totally excise the hematoma en mass, but all microscopic vessels were obliterated with bipolar coagulation. Postoperative Course. The postoperative neurological examination documented the addition of fight facial paralysis and gait ataxia to the preoperative deficit. Neurological function improved to allow the patient to return to his employment as a computer technician. A hypoglossal-facial nerve anastomosis was performed to reanimate the face. The patient has been followed for 24 months. There has been no evidence of recurrent hemorrhage and a recent MR image demonstrated no evidence of residual malformation. Case 2 This 22-year-old right-handed woman developed paroxysmal right frontal headache on August 23, 1987, followed by paresthesias of the right side of the face and body and horizontal diptopia on right gaze. Examination. Pertinent findings on neurological examination consisted of horizontal nystagmus on right gaze, hypesthesia and hypalgesia over the fight side of the face and body, dysmetria in the right upper extremity, and a wide-based unsteady gait. ACT scan demonstrated a 2.0-cm pontine hematoma which was associated with displacement of the floor of the fourth ventricle. Angiography was normal. Magnetic resonance imaging demonstrated a mass in the pons with signal changes characteristic of mixed acute, subacute, and chronic hemorrhage. A halo of low signal consistent with the presence of hemosiderin surrounded the hematoma (Fig. 2 left and center). The patient's symptoms resolved almost completely over several days. She continued to do well until 2 months later, when she suffered another episode of frontal headache, followed by increasing sensory deficit 28 J. Neurosurg. / Volume 72/January, 1990
3 Vascular brain-stem malformations FIG. 2. Case 2. Left: Preoperative sagittal T~-weighted (spin-echo, TR 500/TE 20 msec) magnetic resonance (MR) image demonstrating a signal characteristic of subacute hemorrhage (arrow) within the pons. Center: Preoperative axial T2-weighted (spin-edho, TR 2000/TE 80 msec) MR image revealing an increased signal characteristic of subacute hemorrhage (free methemoglobin). A thin rim (arrow) of hypointensity represents hemosiderin-laden macrophages. Right: Postoperative axial Tl-weighted (spin-echo, TR 500/TE 20 msec) MR image demonstrating complete resection of malformation and hematoma. of the right side of the face and body, diplopia, and incoordination of the right hand. Her gait became unsteady, and she required support. Neurological examination documented horizontal nystagmus, partial right abducens nerve palsy, mild fight pronator muscle drift, hypesthesia and hypalgesia over the right side of the face and body, dysmetria and incoordination of the right upper and lower extremities, and a wide-based unsteady gait with falling to the right. Mild hyperreflexia was noted in all extremities. An MR study showed an increase in the size of the pontine hematoma with new signal characteristics consistent with acute hemorrhage. Operation. Surgery was performed with the patient in a lateral-oblique position. A midline suboccipital craniotomy was carried out with section of the inferior cerebellar vermis (Fig. 3). The lateral aspect of the floor of the fourth ventricle was bulging posteriorly beneath an area of bluish discoloration. The hematoma cavity was opened and dark-brown fluid was evacuated. A mass consisting of hematoma and small blood vessels was totally excised with bipolar cautery and laser. Postoperative Course. The postoperative neurological examination showed partial internuclear ophthalmoplegia and increased gait ataxia. Histological evaluation of the excised specimen demonstrated a venous angioma (Fig. 4). Postoperative MR imaging confirmed that the lesion was totally removed (Fig. 2 right). The patient recovered neurological function and has subsequently returned to her previous employment as a primary-school teacher. FIG. 3. The patient is operated on in a lateral oblique position as demonstrated in the drawing (lower). A midline incision and suboccipital craniotomy are performed to provide access to the cerebellar vermis. Under the operating microscope the vermis is divided and self-retaining retractor blades are placed to provide access to the floor of the fourth ventricle. The malformation and hematoma are resected with impedence-monitored bipolar coagulation and the neodymium: yttrium-aluminum-garnet (Nd:YAG) laser. J. Neurosurg. / Volume 72~January,
4 S. Kashiwagi, et al. Case 3 This 36-year-old man developed the sudden onset of severe headache. Examination. Neurological examination revealed right facial palsy, right abducens nerve palsy, anesthesia of the left side of the body, decreased coordination of the left extremities, left hyperreflexia, and left Babinski reflex. ACT scan demonstrated a pontine mass which was surgically explored through a suboccipital craniectomy at another institution. Subsequently, MR imaging revealed a 2.0-cm pontine mass with a signal characteristic of acute hemorrhage surrounded by a thin rim of low signal due to hemosiderin (Fig. 5 left). Angiography was normal. The patient received high-energy proton-beam radiotherapy for a presumptive diagnosis of cavernous angioma. Subsequent to this treatment, he was observed closely for 2 years. He continued to demonstrate sequences of deterioration of cranial nerve, cerebellar, and left pyramidal function. An MR image demonstrated an expanding mass lesion consisting of hematomas of varying ages. Operation. Surgery was performed with the patient in the lateral-oblique position. A midline suboccipital craniotomy was made with section of the inferior cerebellar vermis. The right lateral aspect of the floor of the fourth ventricle was replaced by a grape-like mass in the region of the facial colliculus (Fig. 6). The cavity was opened and the malformation and hematoma were extirpated from the brain stem. Postoperative Course. The patient's neurological examination demonstrated a left partial sixth nerve palsy and left peripheral facial palsy in addition to the preoperative neurological findings. He continues to improve to a condition considerably better than his preoperative status. Histological examination of the surgical specimen demonstrated a venous angioma. Postoperative MR imaging demonstrated complete resection of the malformation and hematoma (Fig. 5 right). Case 4 This 34-year-old right-handed woman had been well until 10 days prior to admission, when she developed bitemporal headache. The following morning she continued to have bitemporal and occipital headache, and developed a fluctuating horizontal diplopia on right gaze. Over several days she developed motion sickness, patchy paresthesias of the left upper and lower extremities, clumsiness of the left hand, dysarthria, and dysphagia. Examination. Pertinent findings on neurological examination consisted of right abducens nerve palsy, right lower facial weakness, decreased right auditory acuity, left hemiparesis, and left Babinski reflex. Computerized tomography demonstrated a 2.0-cm pontine hematoma (Fig. 7 lower right). Angiography did not FIG. 4. Photomicrograph of the surgical specimen from Case 2 showing a section of abnormal vascular tissue consisting of thin- and thick-walled vascular channels. H & E, x 27. FIG. 5. Case 3. Left: Preoperative axial Tt-weighted (spin-echo, TR 850/TE 26 msec) magnetic resonance (MR) image showing the increased signal of subacute hemorrhage (intracellular and free methemoglobin) within the pons. Right: Postoperative axial T~-weighted (spin-echo, TR 500/ TE 20 msec) MR image demonstrating complete resection of the malformation and hematoma. 30 J. Neurosurg. / Volume 72/January, 1990
5 Vascular brain-stem malformations demonstrate any abnormal vessels. An MR study showed a pontomedullary mass with the signal characteristics of mixed acute and subacute hemorrhage. The mass was surrounded by an increased signal characteristic of edema (Fig. 7 upper). No abnormal vessels were visible in the brain stem; however, incidental findings of multiple focal areas of hypointensity in the cerebral white matter were thought to represent small vascular malformations containing chronic hemorrhage (Fig. 7 lower left). Course. The patient's symptoms gradually improved over the following month. A moderate degree of incoordination of the left upper extremity and left abducens nerve palsy persisted. Three months later, she suffered a repeat bout of headache and worsening of her neurological condition. A C T scan showed recurrent pontine hemorrhage. She recovered and has returned to her position as an executive secretary. Surgical treatment is not planned unless progressive deterioration is demonstrated. FIG. 6. Case 3. Operative photograph showing the presence of a cavernous angioma arising from the right side of the floor of the fourth ventricle. The medium raphe (small arrow) and left facial colliculus (large arrow) are clearly seen, as well as discoloration of the floor consistent with prior hemorrhage. J. Neurosurg. / Volume 72/January, 1990 Case 5 This 36-year-old right-handed man abrupt onset of dizziness, nausea and vertigo 3 days prior to admission. On admission, he experienced right facial difficulty in swallowing. developed the vomiting, and the day before numbness and E x a m i n a t i o n a n d Course. The neurological findings included nystagmus on right lateral gaze, decreased facial sensation and corneal reflex on the right, and an ataxic gait. A C T scan demonstrated a 1.0-cm pontine hematoma. An M R study showed a pontomedullary mass with the signal characteristics of acute hemorrhage (Fig. 8). The mass was surrounded by an increased signal characteristic of edema. A signal flow-void area consistent with vascular malformation was present within the hematoma. Angiography was normal. Over FIG. 7. Case 4. Upper: Axial Tl-weighted (spin-echo, TR 500/TE 20 msec) magnetic resonance (MR) image (left) and axial T2-weighted (spin-echo, TR 2000/TE 80 msec) MR image (righo demonstrating multiple hemorrhages of different ages within the pons. The T2-weighted image reveals the increased signal of edema adjacent to the mass. Lower Left." Axial T2-weighted MR image (spin-echo, TR 2000/TE 80 msec) showing multiple focal areas of hypointensity (arrowheads) without mass effect. These were not seen on contrastenhanced computerized tomography (CT) scans (not shown) and were thought to represent additional vascular malformations with remote hemorrhage. Lower Right: Non-contrast CT scan showing high density in the pons consistent with hemorrhage. A contrast-enhanced CT scan (not shown) demonstrated minimum enhancement of the pontine mass. 31
6 S. Kashiwagi, et al. several days, the patient's neurological examination returned to normal. He has returned to his employment as a newspaper editor and is being observed for evidence of recurrent hemorrhage. Discussion The term "cryptic" vascular malformation was introduced in 1956 by Crawford and Russell 9 to designate small vascular malformations which escaped angiographic detection but were identified histologically in cases of spontaneous cerebral hemorrhage. Cryptic malformations represent a heterogeneous group of vascular malformations with variable histological characteristics, and include cavernous angiomas, venous angiomas, telangiectasias, and totally thrombosed arteriovenous malformations. Computerized tomography has improved detection of brain-stem lesions but lacks the specificity to differentiate vascular malformations from other lesions such as tumors and granulomas. 29 Magnetic resonance imaging has increased sensitivity and specificity in the diagnosis of these lesions and can differentiate between acute hemorrhage (intracellular deoxyhemoglobin), subacute hemorrhage (intracellular and free methemoglobin), and chronic hemorrhage (hemosiderin); evaluation by MR imaging of such vascular malformations demonstrates a relatively uniform and characteristic morphology, so it is difficult to call them "cryptic." The typical findings are a central focus of abnormal signal indicating acute hemorrhage associated FIG. 8. Case 5. Sagittal Tt-weighted magnetic resonance image (spin-echo, TR 500/TE 20 msec) showing signal characteristics consistent with acute and subacute hemorrhage. with intracellular deoxyhemoglobin (hypointense to isodense with brain on T~-weighted images, hypointense on Tz-weighted images), subacute hemorrhage with intracellular and free methemoglobin (hyperintense on Trweighted images, hyperintense on T2-weighted images), or chronic hemorrhage with hemosiderin (extremely hypointense on both TI- and Tz-weighted images). Multiple hemorrhages of varying ages are common in occult malformations and the aging quality of hemoglobin permits accurate differentiation by MR imaging. Occasionally a signal-void area caused by blood flowing in vessels can be detected inside or adjacent to the hemorrhage. I3,~4,2~,36 In the patients reported here, central foci consisted of subacute hemorrhage (Cases 1 and 3) and multiple hemorrhages of different ages (Cases 2 and 4). Acute hemorrhage was seen in Case 5. All patients showed peripheral hypointense rims indicating the presence of (chronic) hemosiderin. Vascular malformations were demonstrated as "flow void" areas in Cases 2, 3, and 4. The age of the hemorrhages shown on MR imaging correlated well with the timing of the clinical signs of hemorrhage in most patients. In two patients who underwent surgery, a venous angioma was proven histologically. In the two nonsurgical patients, histological confirmation has not been obtained. In contrast to the acute serious course of hypertensive pontine hemorrhage, pontine hematoma due to rupture of a vascular malformation presents a relatively milder onset and variable clinical course. The most common presentations are: progressive neurological deterioration over days or weeks mimicking pontine glioma, 1~ relapsing and remitting course lasting over a period of weeks, months, or even years suggesting demyelination, 1.2.7,20.23,42 or subacute onset suggesting an infectious process or stroke of the brain stem. ~6'19'3~ There are numerous isolated reports of successful evacuation of a pontine hematoma in the literature. 4,11,15,18,19,25,28,30-34,39-41,44,45,47,50,51 The most com- monly utilized surgical procedure is a posterior approach through the inferior vermis, exposure of the lesion in the floor of the fourth ventricle, and drainage of the hematoma. Supracerebellar approach to the upper ports, subtonsillar approach to the lower pons, 5~ and subtemporal approach with pedunculotomy ~5 have also been reported. Stereotactic evacuation of a brainstem hematoma is an accepted method of treatment; 3,6 however, vascular malformations may not be adequately treated or diagnosed by this procedure. Total removal of the hematoma and malformation is the preferred form of treatment. The outcome after surgical evacuation of pontine hematomas has been generally good. 4'11'15'18'19'25'28' ,41 In most cases, neurological deficits were reported to be improved or stabilized. There were only a few cases in which patients suffered severe or progressive neurological deterioration. 19'46 The natural history of pontine hematoma due to rupture of vascular malfor- 32,I. Neurosurg. / Volume 72/January, 1990
7 Vascular brain-stem malformations mations is not known. In most cases, signs and symptoms showed progressive or fluctuating deterioration over weeks, months, or years until either surgery or death intervenes. Recurrent hemorrhage with neurological deterioration is documented clinically. 8,19,22'35 Pathological examination of autopsy cases and MR imaging documents multiple hemorrhages of different ages in most cases. 14'37 External irradiation has been proposed for treatment of cavernous angioma of the brain; 42,49 however, its efficacy has not been proven in other types of cryptic vascular malformations ~7 (L Steiner: personal communication, 1989). We have observed a patient with brain-stem vascular malformation who developed slowly progressive neurological deterioration after radiation therapy. Sano and Ochiai 4~ compared surgical treatment with medical treatment, and concluded that pontine hematomas in nonhypertensive patients under 40 years of age should be explored in an effort to extirpate the suspected cryptic vascular malformation and prevent rebleeding. The present experience documents the ability of MR imaging to diagnose heretofore "cryptic" vascular malformations of the brain stem. In view of this greater diagnostic accuracy, the precise anatomical localization, and the acceptable surgical morbidity compared with the morbidity associated with nonsurgical therapy, surgical extirpation for lesions associated with progressive or recurrent neurological deterioration is clearly recommended. The location of the lesion in surgically accessible sites may mandate surgical treatment in patients who have not suffered major disability. Careful evaluation of the natural history and the course of results following surgical and radiation therapy is needed to determine the ultimate choice of treatment for early detected lesions. Addendum Since submission of this manuscript, the authors have evaluated and treated six additional patients with vascular brain-stem malformations. Two patients remain neurologically intact after a single hemorrhage. Four more patients presented with progressive neurological deficits secondary to multiple hemorrhages. These were three women and one man, ranging in age from 23 to 43 years. These four patients underwent complete surgical extirpation of a vascular malformation and hematoma; histological evaluation demonstrated cavernous angioma in all cases. Only one patient exhibited additional morbidity related to hydrocephalus after removal of a malformation from the mesencephalon. The other three patients have returned to gainful employment. This additional experience further documents the necessity of surgical treatment for vascular brain-stem malformations. References 1. Abroms IF, Yessayan L, Shillito J, et al: Spontaneous intracerebral haemorrhage in patients suspected of mal- tiple sclerosis. J Neurol Neurosurg Psychiatry 34: , Arseni C, Stanciu M: Primary haematomas of the brain stem. Acta Neurochir 28: , Beatty RM, Zervas NT: Stereotactic aspiration of a brain stem hematoma. Neurosurgery 13: , Becker DH, Silverberg GD: Successful evacuation of an acute pontine hematoma. Surg Neurol 10: , Becker DH, Townsend J J, Kramer RA, et al: Occult cerebrovascular malformations. A series of 18 histologically verified cases with negative angiography. Brain 102: , Bosch DA, Beute GN: Successful stereotaxic evacuation of an acute pontomedullary hematoma. Case report. J Neurosurg 62: , Britt RH, Conner WS, Enzmann DR: Occult arteriovenous malformation of the brainstem simulating multiple sclerosis. Neurology 31: , Burns J, Lisak R, Schut L, et al: Recovery following brainstem hemorrhage. Ann Neurol 7: , Crawford JV, Russell DS: Cryptic arteriovenous and venous hamartomas of the brain. J Neurol Neurosurg Psychiatry 19:1-11, Dandy WE: The Brain. New York: Harper & Row, 1969, pp Doczi T, Thomas DGT: Successful removal of an intrapontine haematoma. J Neurol Neurosurg Psychiatry 42: , Durwood Q J, Barnett HJM, Ban- HWK: Presentation and management of mesencephalic hematoma. Report of two cases. J Neurosurg 56: , Gomori JM, Grossman RI, Goldberg HI, et al: Occult cerebral vascular malformations: high-field MRI imaging. Radiology 158: , Griffin C, DeLaPaz R, Enzmann D: Magnetic resonance appearance of slow flow vascular malformations of the brainstem. Neuroradiology 29: , Humphreys RP: Computerized tomographic definition of mesencephalic hematoma with evacuation through pedunculotomy. Case report. J Neurosurg 49: , Kempe LG: Surgical removal of an intramedullary haematoma simulating Wallenberg's syndrome. J Neurol Neurosurg Psychiatry 27:78-80, Kjellberg RN, Davis KR, Lyons S, et al: Bragg peak proton beam therapy for arteriovenous malformation of the brain. Clin Neurosurg 31: , Koos WT, Sunder-Plassmann M, Salah S: Successful removal of a large intrapontine hematoma. Case report. J Neurosurg 31: , Kowada M, lto Z, Matsuoka S, et al: Primary pontine haemorrhage revealed by pneumoencephalo-roulette tomography, and a report on surgically treated cases. Acta Neurochir 25: , Kushner M J, Bressman SB: The clinical manifestations of pontine hemorrhage. Neurology 35: , Lemme-Plaghos L, Kucharczyk W, Brant-Zawadzki M, et al: MRI of angiographically occult vascular malformations. AJNR 1: , Lindheimer JH, Barrows HS: Recurrent pontine hemorrhage incident to venous angioma of the pons: report of a case. Bull LA Neurol Soc 27: , Logue V, Monckton G: Posterior fossa angiomas. A clinical presentation of nine cases. Brain 77: , Margolis G, Odom GL, Woodhall B, et al: The role of small angiomatous malformations in the production of intracerebral hematomas. J Neurosurg 8: , 1951 J. Neurosurg. / Volume 72/January,
8 S. Kashiwagi, et al. 25. Martin PM: L'h6matome bulbotub6rantiel op6rable. Acta Neurol Belg 71: , McCormick WF, Hardman JM, Boulter TR: Vascular malformations ("angiomas') of the brain, with special reference to those occurring in the posterior fossa. J Neurosurg 28: , McCormick WF, Nofzinger JD: "Cryptic" vascular malformations of the central nervous system. J Neurosurg 24: , Murphy MG: Successful evacuation of acute pontine hematoma. Case report. J Neurosurg 37: , Norman D: Computerized tomography of cerebrovascular malformations, in Wilson CB, Stein BM (eds): Intracranial Arteriovenous Malformations. Baltimore: Williams & Wilkins, 1984, pp Obrador S, Dierssen G, Ordoriz B J: Surgical evacuation of a pontine-medullary hematoma. Case report. J Neurosurg 33:82-84, I. O'Laoire SA, Crockard HA, Thomas DGT, et al: Brainstem hematoma. A report of six surgically treated cases. J Neurosurg 56: , Pak H, Patel SC, Malik GM, et al: Successful evacuation of a pontine hematoma secondary to rupture of a venous angioma. Surg Neurol 15: , Pau A, Viale ES, Turtas S: Surgical removal of a pontine haematoma associated with a cryptic angioma. Case report. Acta Neurochir 50: , Pouyanne H, Got M, Julien J, et al: Deux cases d'h6matomes intraprotub~rantiels op6refi, l~tude critique. Neurochirurgie 13: , Richardson JG, Bagnall AW: Recurrent subarachnoid hemorrhage due to arterio angioma of cerebellum and brainstem. Can Med Assoc 3 43: , Rigamonti D, Drayer BP, Johnson PC, et al: The MRI appearance of cerebral cavernous malformations (angiomas). J Neurosurg 67: , Rigamonti D, Spetzler RF, Johnson PC, et al: Cerebral vascular malformations. Barrow Neurol Inst Q 3:18-27, Roberson GH, Kase CS, Wolpow ER: Telangiectases and cavernous angiomas of the brainstem: "cryptic" vascular malformations. Report of a case. Neuroradiology 8: 83-89, Russell B, Rengachary SS, McGregor D: Primary pontine hematoma presenting as a cerebellopontine angle mass. Neurosurgery 19: , Sano K, Ochiai C: Brain stem haematomas. Clinical aspects with reference to indications for treatment, in Pia HW, Langmaid C, Zierski J (eds): Spontaneous tntracerebral Haematomas. Advances in Diagnosis and Therapy. New York: Springer-Verlag, 1980, pp Scott BB, Seeger JF, Schneider RC: Successful evacuation of a pontine hematoma secondary to rupture of a pathologically diagnosed "cryptic" vascular malformation. Case report. J Neurosurg 39: , Stahl SM, Johnson KP, Malamud N: The clinical and pathological spectrum of brain-stem vascular malformations. Long-term course stimulates multiple sclerosis. Arch Neurol 37:25-29, Teilmann K: Hemangiomas of the pons. Arch Neurol Psychiatry 69: , Umansky F, Toledo E, Cohen M, et al: Successful removal of an acute brain stem hematoma in a young child. Childs Brain 10: , Vaquero J, Areitio E, Leunda G, et al: Hematoma of the pons. Surg Neurol 14: , Vaquero J, Salazar J, Martinez P, et al: Cavernomas of the central nervous system: clinical syndromes, CT scan diagnosis, and prognosis after surgical treatment. Acta Neurochir 85:29-33, Veerapen RJ, Sbieh IA, O'Laoire SA: Surgical treatment of cryptic AVM's and associated hematoma in the brain stem and spinal cord. J Neurosurg 65: , White RJ, Kernohan JW, Wood MW: A study of fifty intracranial vascular tumors found incidentally at necropsy. J Neuropathol Exp Neurol 17: , Yamasaki T, Handa H, Yamashita J, et ah Intracranial and orbital cavernous angiomas. A review of 30 cases. 3 Neurosurg 64: , Ya~argil MG: Microneurosurgery, Vol IIIb. New York: Thieme, 1987, pp Yoshimoto T, Suzuki J: Radical surgery on cavernous angioma of the brainstem. Surg Neurol 26:72-78, 1986 Manuscript received January 25, Accepted in final form June 26, Address reprint requests to: John M. Tew, Jr., M.D., Department of Neurosurgery, University of Cincinnati College of Medicine, 231 Bethesda Avenue, Cincinnati, Ohio J. Neurosurg. / Volume 72/January, 1990
A LTHOUGH the first operation for brain-stem
 J Neurosurg 56".222-227, 1982 Brain-stem hematoma A report of six surgically treated cases SEAN A. O'LAOIRE, M.D., F.R.C.S.I., F.R.C.S., H. ALAN CROCKARD, F.R.C.S., DAVID G. T. THOMAS, M.R.C.P., F.R.C.S.,
J Neurosurg 56".222-227, 1982 Brain-stem hematoma A report of six surgically treated cases SEAN A. O'LAOIRE, M.D., F.R.C.S.I., F.R.C.S., H. ALAN CROCKARD, F.R.C.S., DAVID G. T. THOMAS, M.R.C.P., F.R.C.S.,
Surgery of Angiomas in the Brainstem With a Stress on the Presence of Telangiectasia
 II-4. Spinal and Vascular Malformation Other than AVM Surgery of Angiomas in the Brainstem With a Stress on the Presence of Telangiectasia Masashi FUKUI, Toshio MATSUSHIMA, Kiyonobu IKEZAKI, Yoshihiro
II-4. Spinal and Vascular Malformation Other than AVM Surgery of Angiomas in the Brainstem With a Stress on the Presence of Telangiectasia Masashi FUKUI, Toshio MATSUSHIMA, Kiyonobu IKEZAKI, Yoshihiro
DIRECT SURGERY FOR INTRA-AXIAL
 Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
Surgical management of hematomas of the brain stem
 J Neurosurg 73:181-186, 1990 Surgical management of hematomas of the brain stem ALEXANDER N. KONOVALOV, DR.M.S., M.D., ALDO SPALLONE, M.D., UVAIS B. MAKHMUDOV, M.D., JELENA A. KUKHLAJEVA, M.D., AND VALENTINA
J Neurosurg 73:181-186, 1990 Surgical management of hematomas of the brain stem ALEXANDER N. KONOVALOV, DR.M.S., M.D., ALDO SPALLONE, M.D., UVAIS B. MAKHMUDOV, M.D., JELENA A. KUKHLAJEVA, M.D., AND VALENTINA
Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case
 Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case Soo-Bin Yim, M.D., Jong-Sung Kim, M.D., Yang Kwon,M.D.*, Choong-Gon
Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case Soo-Bin Yim, M.D., Jong-Sung Kim, M.D., Yang Kwon,M.D.*, Choong-Gon
Vascular Malformations of the Brain: A Review of Imaging Features and Risks
 Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
V ASCULAR malformations of the brain stem are
 J Neurosurg 70:847-852, 1989 Vascular malformations of the brain stem DOUGLAS CHYATTE, M.D. Section of Neurological Surgery, Subsection of Cerebrovascular Diseases, Yale University School of Medicine,
J Neurosurg 70:847-852, 1989 Vascular malformations of the brain stem DOUGLAS CHYATTE, M.D. Section of Neurological Surgery, Subsection of Cerebrovascular Diseases, Yale University School of Medicine,
MR Flow Imaging in Vascular Malformations Using Gradient Recalled Acquisition
 637 MR Flow Imaging in Vascular Malformations Using Gradient Recalled Acquisition William M. Needell 1 Kenneth R. Maravilla Twenty patients with known or suspected intracranial vascular lesions were evaluated
637 MR Flow Imaging in Vascular Malformations Using Gradient Recalled Acquisition William M. Needell 1 Kenneth R. Maravilla Twenty patients with known or suspected intracranial vascular lesions were evaluated
Radiological Appearance of Extra-axial CNS Hemangioma
 Chin J Radiol 2002; 27: 183-190 183 Radiological Appearance of Extra-axial CNS Hemangioma MING-SHIANG YANG CLAYTON CHI-CHANG CHEN WEN-HSIEN CHEN HAO-CHUN HUNG SAN-KAN LEE Department of Radiology, Taichung
Chin J Radiol 2002; 27: 183-190 183 Radiological Appearance of Extra-axial CNS Hemangioma MING-SHIANG YANG CLAYTON CHI-CHANG CHEN WEN-HSIEN CHEN HAO-CHUN HUNG SAN-KAN LEE Department of Radiology, Taichung
External carotid blood supply to acoustic neurinomas
 External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Year 2003 Paper two: Questions supplied by Tricia
 question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
The MRI appearance of cavernous malformations (angiomas)
 J Neurosnrg 67:518-524, 1987 The MRI appearance of cavernous malformations (angiomas) DANIELE RIGAMONTI, M.D., BURTON P. DRAYEI~ M.D., PETER C. JOHNSON, M.D., MARK N. HADLEY, M.D., JOSEPH ZABRAMSKI, M.D.,
J Neurosnrg 67:518-524, 1987 The MRI appearance of cavernous malformations (angiomas) DANIELE RIGAMONTI, M.D., BURTON P. DRAYEI~ M.D., PETER C. JOHNSON, M.D., MARK N. HADLEY, M.D., JOSEPH ZABRAMSKI, M.D.,
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al.
 ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
Approach to a Neurologic Diagnosis
 Approach to a Neurologic Diagnosis Neurologic Diagnosis History Physical & Neurological Examination Ancillary Procedures 3 Questions Asked Focal neurologic deficits Increased intracranial pressure Signs
Approach to a Neurologic Diagnosis Neurologic Diagnosis History Physical & Neurological Examination Ancillary Procedures 3 Questions Asked Focal neurologic deficits Increased intracranial pressure Signs
RESEARCH HUMAN CLINICAL STUDIES
 TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Cavernous Malformation of Brainstem, Thalamus, and Basal Ganglia: A Series of 176 Patients Paritosh Pandey, MD Erick M. Westbroek,
TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Cavernous Malformation of Brainstem, Thalamus, and Basal Ganglia: A Series of 176 Patients Paritosh Pandey, MD Erick M. Westbroek,
VASCULAR MALFORMATIONS. Owen Samuels, MD Adam Webb, MD Emory University
 VASCULAR MALFORMATIONS Owen Samuels, MD Adam Webb, MD Emory University Introduction Brain and spinal cord vascular malformations can be separated into five main categories: 1) Arteriovenous malformation,
VASCULAR MALFORMATIONS Owen Samuels, MD Adam Webb, MD Emory University Introduction Brain and spinal cord vascular malformations can be separated into five main categories: 1) Arteriovenous malformation,
Pontine haemorrhage: a clinical analysis of 26 cases
 Journal of Neurology, Neurosurgery, and Psychiatry 1985;48:658-662 Pontine haemorrhage: a clinical analysis of 26 cases SHOJI MASIYAMA, HIROSHI NIIZUMA, JIRO SUZUKI From the Division ofneurosurgery, Institute
Journal of Neurology, Neurosurgery, and Psychiatry 1985;48:658-662 Pontine haemorrhage: a clinical analysis of 26 cases SHOJI MASIYAMA, HIROSHI NIIZUMA, JIRO SUZUKI From the Division ofneurosurgery, Institute
Chiari Malformations. Google. Objectives Seventh Annual NKY TBI Conference 3/22/13. Kerry R. Crone, M.D.
 Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
MR Imaging of Spinal Cord Arteriovenous Malformations at 0.5 T: Study of 34 Cases
 833 MR Imaging of Spinal Cord Arteriovenous Malformations at 0.5 T: Study of 34 Cases D. Dormont 1 F. Gelbert 2 E. Assouline 2 D. Reizine 2 A. Helias 2 M. C. Riche 2 J. Chiras 1 J. Sories 1 J. J. Merland
833 MR Imaging of Spinal Cord Arteriovenous Malformations at 0.5 T: Study of 34 Cases D. Dormont 1 F. Gelbert 2 E. Assouline 2 D. Reizine 2 A. Helias 2 M. C. Riche 2 J. Chiras 1 J. Sories 1 J. J. Merland
Uncommon Symptomatic Cerebral Vascular Malformations
 Uncommon Symptomatic Cerebral Vascular Malformations Mauro Bergui and Gianni Boris Bradac Summary: We describe three cases of unusual vascular malformations in which the most relevant angiographic findings
Uncommon Symptomatic Cerebral Vascular Malformations Mauro Bergui and Gianni Boris Bradac Summary: We describe three cases of unusual vascular malformations in which the most relevant angiographic findings
Magnetic resonance imaging (MR!) provides
 0 Wallerian Degeneration of the Pyramidal Tract in Capsular Infarction Studied by Magnetic Resonance Imaging Jesiis Pujol, MD, Josep L. Marti-Vilalta, MD, Carme Junqu6, PhD, Pere Vendrell, PhD, Juan Fernandez,
0 Wallerian Degeneration of the Pyramidal Tract in Capsular Infarction Studied by Magnetic Resonance Imaging Jesiis Pujol, MD, Josep L. Marti-Vilalta, MD, Carme Junqu6, PhD, Pere Vendrell, PhD, Juan Fernandez,
A mong intracranial vascular malformations the cavernous
 PAPER Surgical removal of brain stem cavernous malformations: surgical indications, technical considerations, and results I E Sandalcioglu, H Wiedemayer, S Secer, S Asgari, D Stolke... See end of article
PAPER Surgical removal of brain stem cavernous malformations: surgical indications, technical considerations, and results I E Sandalcioglu, H Wiedemayer, S Secer, S Asgari, D Stolke... See end of article
Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report
 Neurosurg Focus 5 (3):Article 9, 1998 Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report Dean Chou, M.D., Prakash Sampath, M.D., and Henry Brem, M.D. Departments of Neurological
Neurosurg Focus 5 (3):Article 9, 1998 Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report Dean Chou, M.D., Prakash Sampath, M.D., and Henry Brem, M.D. Departments of Neurological
Neuroanatomy of a Stroke. Joni Clark, MD Professor of Neurology Barrow Neurologic Institute
 Neuroanatomy of a Stroke Joni Clark, MD Professor of Neurology Barrow Neurologic Institute No disclosures Stroke case presentations Review signs and symptoms Review pertinent exam findings Identify the
Neuroanatomy of a Stroke Joni Clark, MD Professor of Neurology Barrow Neurologic Institute No disclosures Stroke case presentations Review signs and symptoms Review pertinent exam findings Identify the
Overview of Stroke: Etiologies, Demographics, Syndromes, and Outcomes. Alex Abou-Chebl, MD, FSVIN Medical Director, Stroke Baptist Health Louisville
 Overview of Stroke: Etiologies, Demographics, Syndromes, and Outcomes Alex Abou-Chebl, MD, FSVIN Medical Director, Stroke Baptist Health Louisville Disclosure Statement of Financial Interest Within the
Overview of Stroke: Etiologies, Demographics, Syndromes, and Outcomes Alex Abou-Chebl, MD, FSVIN Medical Director, Stroke Baptist Health Louisville Disclosure Statement of Financial Interest Within the
Application of three-dimensional angiography in elderly patients with meningioma
 Application of three-dimensional angiography in elderly patients with meningioma Poster No.: C-0123 Congress: ECR 2012 Type: Scientific Paper Authors: X. Han, J. Chen, K. Shi; Haikou/CN Keywords: Neuroradiology
Application of three-dimensional angiography in elderly patients with meningioma Poster No.: C-0123 Congress: ECR 2012 Type: Scientific Paper Authors: X. Han, J. Chen, K. Shi; Haikou/CN Keywords: Neuroradiology
TUMOURS IN THE REGION OF FORAMEN MAGNUM
 TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male
 Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Neurosurg Focus 3 (3):Clinical Pearl, 1997
 Neurosurg Focus 3 (3):Clinical Pearl, 1997 De novo formation of a central nervous system cavernous malformation: implications for predicting risk of hemorrhage Case report and review of the literature
Neurosurg Focus 3 (3):Clinical Pearl, 1997 De novo formation of a central nervous system cavernous malformation: implications for predicting risk of hemorrhage Case report and review of the literature
University Journal of Medicine and Medical Sciences
 ISSN 2455-2852 Volume 2 Issue 5 2016 Case report -Opalski's syndrome A rare variant of lateral medullary syndrome in TAKAYASUS ARTERITIS SHANKAR GANESH N NAINAR Department of Neurology, MADRAS MEDICAL
ISSN 2455-2852 Volume 2 Issue 5 2016 Case report -Opalski's syndrome A rare variant of lateral medullary syndrome in TAKAYASUS ARTERITIS SHANKAR GANESH N NAINAR Department of Neurology, MADRAS MEDICAL
Microsurgery for ruptured cerebellar arteriovenous malformations
 European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT
 Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage
 Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
/ / / / / / Hospital Abstraction: Stroke/TIA. Participant ID: Hospital Code: Multi-Ethnic Study of Atherosclerosis
 Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
The Use of Early Postoperative MR in Detecting Residual Juvenile Cerebellar Pilocytic Astrocytoma
 AJNR Am J Neuroradiol 19:151 156, January 1998 The Use of Early Postoperative MR in Detecting Residual Juvenile Cerebellar Pilocytic Astrocytoma Nancy K. Rollins, Perry Nisen, and Kenneth N. Shapiro PURPOSE:
AJNR Am J Neuroradiol 19:151 156, January 1998 The Use of Early Postoperative MR in Detecting Residual Juvenile Cerebellar Pilocytic Astrocytoma Nancy K. Rollins, Perry Nisen, and Kenneth N. Shapiro PURPOSE:
Marc Norman, Ph.D. - Do Not Use without Permission 1. Cerebrovascular Accidents. Marc Norman, Ph.D. Department of Psychiatry
 Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
Department of Radiology University of California San Diego. MR Angiography. Techniques & Applications. John R. Hesselink, M.D.
 Department of Radiology University of California San Diego MR Angiography Techniques & Applications John R. Hesselink, M.D. Vascular Imaging Arterial flow void Flow enhancement Gadolinium enhancement Vascular
Department of Radiology University of California San Diego MR Angiography Techniques & Applications John R. Hesselink, M.D. Vascular Imaging Arterial flow void Flow enhancement Gadolinium enhancement Vascular
2. Subarachnoid Hemorrhage
 Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Organized Intracerebral Hematoma with Acute Hemorrhage: CT Patterns and
 409 Organized Intracerebral Hematoma with Acute Hemorrhage: CT Patterns and Pathologic Correlations Ya-Yen Lee' Richard Moser 2 Janet M. Bruner Pamela Van Tassel' Five cases of pathologically proven organized
409 Organized Intracerebral Hematoma with Acute Hemorrhage: CT Patterns and Pathologic Correlations Ya-Yen Lee' Richard Moser 2 Janet M. Bruner Pamela Van Tassel' Five cases of pathologically proven organized
Meningioma tumor. Meningiomas are named according to their location (Fig. 1) and cause various symptoms: > 1
 Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
It s Always a Stroke; Except For When It s Not..
 It s Always a Stroke; Except For When It s Not.. TREVOR PHINNEY, D.O. Disclosures No Relevant Disclosures 1 Objectives Discuss variables of differential diagnosis for stroke Review when to TPA and when
It s Always a Stroke; Except For When It s Not.. TREVOR PHINNEY, D.O. Disclosures No Relevant Disclosures 1 Objectives Discuss variables of differential diagnosis for stroke Review when to TPA and when
the face department, Geneva University Hospitals and University of Geneva, Rue Micheli-du-Crest
 Final article published in Journal of Neurology 2009 Jun;256(6):1017-8. http://dx.doi.org/10.1007/s00415-009-5041-6. Sixth cranial nerve palsy and contralateral hemiparesis (Raymond s syndrome) sparing
Final article published in Journal of Neurology 2009 Jun;256(6):1017-8. http://dx.doi.org/10.1007/s00415-009-5041-6. Sixth cranial nerve palsy and contralateral hemiparesis (Raymond s syndrome) sparing
MR Imaging of Intracranial Fluid Levels
 695 MR Imaging of Intracranial Fluid Levels James J. Abrahams 1 Mika Lidov Carlos Artiles Six patients with seven intracranial fluid levels were evaluated with both CT and MR at 1.5 T. A surgical diagnosis
695 MR Imaging of Intracranial Fluid Levels James J. Abrahams 1 Mika Lidov Carlos Artiles Six patients with seven intracranial fluid levels were evaluated with both CT and MR at 1.5 T. A surgical diagnosis
Primary pontine haemorrhage: clinical and computed tomographic correlations
 Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:346-352 Primary pontine haemorrhage: clinical and computed tomographic correlations LEON A WESBERG From the Department of Neurology and Psychiatry
Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:346-352 Primary pontine haemorrhage: clinical and computed tomographic correlations LEON A WESBERG From the Department of Neurology and Psychiatry
THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE
 THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE * Dr. Sumendra Raj Pandey, Prof. Dr. Liu Pei WU, Dr. Sohan Kumar Sah, Dr. Lalu Yadav, Md. Sadam Husen Haque and Rajan KR. Chaurasiya
THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE * Dr. Sumendra Raj Pandey, Prof. Dr. Liu Pei WU, Dr. Sohan Kumar Sah, Dr. Lalu Yadav, Md. Sadam Husen Haque and Rajan KR. Chaurasiya
A characteristic feature of acute haematomas in the brain on echo-planar diffusion-weighted imaging
 Neuroradiology (2002) 44: 907 911 DOI 10.1007/s00234-002-0860-5 DIAGNOSTIC NEURORADIOLOGY N. Morita M. Harada K. Yoneda H. Nishitani M. Uno A characteristic feature of acute haematomas in the brain on
Neuroradiology (2002) 44: 907 911 DOI 10.1007/s00234-002-0860-5 DIAGNOSTIC NEURORADIOLOGY N. Morita M. Harada K. Yoneda H. Nishitani M. Uno A characteristic feature of acute haematomas in the brain on
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease
 AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
Adult intramedullary astrocytomas of the spinal cord
 J Neurosurg 77:355-359, 1992 Adult intramedullary astrocytomas of the spinal cord FRED J. EPSTEIN, M.D., JEAN-PIERRE FARMER, M.D., F.R.C.S., AND DIANA FREED Division of Pediatric Neurosurgery, Department
J Neurosurg 77:355-359, 1992 Adult intramedullary astrocytomas of the spinal cord FRED J. EPSTEIN, M.D., JEAN-PIERRE FARMER, M.D., F.R.C.S., AND DIANA FREED Division of Pediatric Neurosurgery, Department
Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury
 Chin J Radiol 2005; 30: 173-177 173 Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury HUI-YI CHEN 1 YING-SHYUAN LI 1 CHUNG-HO CHEN 1
Chin J Radiol 2005; 30: 173-177 173 Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury HUI-YI CHEN 1 YING-SHYUAN LI 1 CHUNG-HO CHEN 1
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
Key Clinical Concepts
 Cerebrovascular Review and General Vascular Syndromes, Including Those That Impact Dizziness Key Clinical Concepts Basic Review of Cerebrovascular Circulation Circulation to the brain is divided into anterior
Cerebrovascular Review and General Vascular Syndromes, Including Those That Impact Dizziness Key Clinical Concepts Basic Review of Cerebrovascular Circulation Circulation to the brain is divided into anterior
CT Patterns in Histopathologically Complex Cavernous Hemangiomas
 389 CT Patterns in Histopathologically Complex Cavernous Hemangiomas Jamshid Ahmadi1 Carol Ann Miller 2 Hervey D. Segall 1 Sun-Hyung Park 1.3 Chi-Shing Zee 1 Ronald L. Becker 4 Computed tomographic (CT)
389 CT Patterns in Histopathologically Complex Cavernous Hemangiomas Jamshid Ahmadi1 Carol Ann Miller 2 Hervey D. Segall 1 Sun-Hyung Park 1.3 Chi-Shing Zee 1 Ronald L. Becker 4 Computed tomographic (CT)
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
A Rare Cause of Cerebellar Ataxia Syndrome: Superficial Siderosis of Central Nervous System
 257 Rare Cause of Cerebellar taxia Syndrome: Superficial Siderosis of Central Nervous System Simon Kang Seng Ting, MRCP, Kumar M Prakash, FRCP bstract- Purpose: To describe and emphasize importance of
257 Rare Cause of Cerebellar taxia Syndrome: Superficial Siderosis of Central Nervous System Simon Kang Seng Ting, MRCP, Kumar M Prakash, FRCP bstract- Purpose: To describe and emphasize importance of
Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature
 Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
MR and CT of Occult Vascular Malformations of the Brain
 771 MR and CT of Occult Vascular Malformations of the Brain Paul F. J. New' Robert G. Ojemann' Kenneth R. Davis 1 Bruce R. Rosen 1 Roberto Heros' Raymond N. Kjellberg' Raymond D. Adams 2 E. P. Richardson
771 MR and CT of Occult Vascular Malformations of the Brain Paul F. J. New' Robert G. Ojemann' Kenneth R. Davis 1 Bruce R. Rosen 1 Roberto Heros' Raymond N. Kjellberg' Raymond D. Adams 2 E. P. Richardson
Update on Pediatric Brain Tumors
 Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Common Pitfalls in Multiple Sclerosis and CNS Demyelinating Diseases
 Common Pitfalls in Multiple Sclerosis and CNS Demyelinating Diseases Case-Based Learning Common Pitfalls in Multiple Sclerosis and CNS Demyelinating Diseases Case-Based Learning Mayo Clinic College of
Common Pitfalls in Multiple Sclerosis and CNS Demyelinating Diseases Case-Based Learning Common Pitfalls in Multiple Sclerosis and CNS Demyelinating Diseases Case-Based Learning Mayo Clinic College of
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord
 The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
MR Characteristics of Subdural Hematomas and Hygromas at 1.5 T
 687 MR Characteristics of Subdural Hematomas and Hygromas at 1.5 T Edward S. Fobben 1 Robert I. Grossman Scott W. tlas David B. Hackney Herbert I. Goldberg Robert. Zimmerman Larissa T. Bilaniuk MR images
687 MR Characteristics of Subdural Hematomas and Hygromas at 1.5 T Edward S. Fobben 1 Robert I. Grossman Scott W. tlas David B. Hackney Herbert I. Goldberg Robert. Zimmerman Larissa T. Bilaniuk MR images
Stroke - Intracranial hemorrhage. Dr. Amitesh Aggarwal Associate Professor Department of Medicine
 Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Magnetic resonance imaging (MRI) appears to
 297 Early Diagnosis of Basilar Artery Occlusion Using Magnetic Resonance Imaging Jos6 Biller, MD, William T.C. Yuh, MD, Galen W. Mitchell, MD, Askiel Bruno, MD, and Harold P. Adams Jr., MD Three patients
297 Early Diagnosis of Basilar Artery Occlusion Using Magnetic Resonance Imaging Jos6 Biller, MD, William T.C. Yuh, MD, Galen W. Mitchell, MD, Askiel Bruno, MD, and Harold P. Adams Jr., MD Three patients
NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE
 THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Effect of clot removal on cerebral vasospasm TETSUJI INAGAWA, M.D., MITSUO YAMAMOTO, M.D., AND KAZUKO KAMIYA, M.D.
 J Neurosurg 72:224-230, 1990 Effect of clot removal on cerebral vasospasm TETSUJI INAGAWA, M.D., MITSUO YAMAMOTO, M.D., AND KAZUKO KAMIYA, M.D. Department of Neurosurgery, Shimane Prefectural Central Hospital,
J Neurosurg 72:224-230, 1990 Effect of clot removal on cerebral vasospasm TETSUJI INAGAWA, M.D., MITSUO YAMAMOTO, M.D., AND KAZUKO KAMIYA, M.D. Department of Neurosurgery, Shimane Prefectural Central Hospital,
Cranial Postoperative Site: MR Imaging Appearance
 27 Cranial Postoperative Site: MR Imaging Appearance Charles F. Lanzieri1 Mark Larkins2 Andrew Mancall 1 Ronald Lorig 1 Paul M. Duchesneau 1 Scott A. Rosenbloom 1 Meredith A. Weinstein 1 The ability to
27 Cranial Postoperative Site: MR Imaging Appearance Charles F. Lanzieri1 Mark Larkins2 Andrew Mancall 1 Ronald Lorig 1 Paul M. Duchesneau 1 Scott A. Rosenbloom 1 Meredith A. Weinstein 1 The ability to
Neuroradiology MR Protocols
 Neuroradiology MR Protocols Brain protocols N 1: Brain MRI without contrast N 2: Pre- and post-contrast brain MRI N 3 is deleted N 4: Brain MRI without or pre-/post-contrast (seizure protocol) N 5: Pre-
Neuroradiology MR Protocols Brain protocols N 1: Brain MRI without contrast N 2: Pre- and post-contrast brain MRI N 3 is deleted N 4: Brain MRI without or pre-/post-contrast (seizure protocol) N 5: Pre-
Attenuation value in HU From -500 To HU From -10 To HU From 60 To 90 HU. From 200 HU and above
 Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Variable Appearances of Subacute Intracranial Hematomas on High-Field Spin-Echo MR
 1019 Variable Appearances of Subacute Intracranial Hematomas on High-Field Spin-Echo MR John M. Gomori' 2 Robert I. Grossman' David B. Hackney' Herbert I. Goldberg' Robert A. Zimmerman' Larissa T. Bilaniuk'
1019 Variable Appearances of Subacute Intracranial Hematomas on High-Field Spin-Echo MR John M. Gomori' 2 Robert I. Grossman' David B. Hackney' Herbert I. Goldberg' Robert A. Zimmerman' Larissa T. Bilaniuk'
Neurosurgery. Neurosurgery
 Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
ARTERIOVENOUS MALFORMATION OR CONTUSION : A DIAGNOSTIC DILEMMA. Yong Pei Yee, Ibrahim Lutfi Shuaib, Jafri Malin Abdullah*
 Malaysian Journal of Medical Sciences, Vol. 8, No. 2, July 2001 (47-51) CASE REPORT ARTERIOVENOUS MALFORMATION OR CONTUSION : A DIAGNOSTIC DILEMMA Yong Pei Yee, Ibrahim Lutfi Shuaib, Jafri Malin Abdullah*
Malaysian Journal of Medical Sciences, Vol. 8, No. 2, July 2001 (47-51) CASE REPORT ARTERIOVENOUS MALFORMATION OR CONTUSION : A DIAGNOSTIC DILEMMA Yong Pei Yee, Ibrahim Lutfi Shuaib, Jafri Malin Abdullah*
Vascular Malformations of the Brain. William A. Cox, M.D. Forensic Pathologist/Neuropathologist. September 8, 2014
 Vascular Malformations of the Brain William A. Cox, M.D. Forensic Pathologist/Neuropathologist September 8, 2014 Vascular malformations of the brain are classified into four principal groups: arteriovenous
Vascular Malformations of the Brain William A. Cox, M.D. Forensic Pathologist/Neuropathologist September 8, 2014 Vascular malformations of the brain are classified into four principal groups: arteriovenous
Title. Author(s) Takahashi, Haruo. Issue Date Right.
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation A case with posterior fossa epiderm symptoms caused by insufficiency of usefulness of free DICOM image view Takasaki, Kenji; Kumagami, Hidetaka
NAOSITE: Nagasaki University's Ac Title Author(s) Citation A case with posterior fossa epiderm symptoms caused by insufficiency of usefulness of free DICOM image view Takasaki, Kenji; Kumagami, Hidetaka
Occlusive hyperemia: a theory for the hemodynamic complications following resection of intracerebral arteriovenous malformations
 J Neurosurg 78: 167-175, 1993 Occlusive hyperemia: a theory for the hemodynamic complications following resection of intracerebral arteriovenous malformations NAYEF R. F. AL-RODHAN, M.D., PH.D., THORALF
J Neurosurg 78: 167-175, 1993 Occlusive hyperemia: a theory for the hemodynamic complications following resection of intracerebral arteriovenous malformations NAYEF R. F. AL-RODHAN, M.D., PH.D., THORALF
SHORTLY AFTER ITS FIRST DEpiction
 OBSERVATION Seven-Tesla Magnetic Resonance Imaging New Vision of Microvascular Abnormalities in Multiple Sclerosis Yulin Ge, MD; Vahe M. Zohrabian, MD; Robert I. Grossman, MD Background: Although the role
OBSERVATION Seven-Tesla Magnetic Resonance Imaging New Vision of Microvascular Abnormalities in Multiple Sclerosis Yulin Ge, MD; Vahe M. Zohrabian, MD; Robert I. Grossman, MD Background: Although the role
Case 9511 Hypertensive microangiopathy
 Case 9511 Hypertensive microangiopathy Schepers S, Barthels C Section: Neuroradiology Published: 2011, Nov. 3 Patient: 67 year(s), male Authors' Institution Department of Radiology, Jessa ziekenhuis campus
Case 9511 Hypertensive microangiopathy Schepers S, Barthels C Section: Neuroradiology Published: 2011, Nov. 3 Patient: 67 year(s), male Authors' Institution Department of Radiology, Jessa ziekenhuis campus
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
Clinical presentations of vascular malformations of the brain stem: comparison of angiographically positive and negative types
 Journal ofneurology, Neurosurgery, and Psychiatry 1989;52:167-175 Clinical presentations of vascular malformations of the brain stem: comparison of angiographically positive and negative types MASAMITSU
Journal ofneurology, Neurosurgery, and Psychiatry 1989;52:167-175 Clinical presentations of vascular malformations of the brain stem: comparison of angiographically positive and negative types MASAMITSU
multiple sclerosis by magnetic resonance imaging
 Index terms: Computed tomography Magnetic resonance sequence optimization Multiple sclerosis The evaluation of multiple sclerosis by magnetic resonance imaging Val M. Runge, M.D.*1 4, Ann C. Price, M.D.*
Index terms: Computed tomography Magnetic resonance sequence optimization Multiple sclerosis The evaluation of multiple sclerosis by magnetic resonance imaging Val M. Runge, M.D.*1 4, Ann C. Price, M.D.*
Accepted Manuscript. Comparison of costs and outcomes of patients presenting with a rare brainstem syndrome. Devin E. Prior, Vijay Renga
 Accepted Manuscript Comparison of costs and outcomes of patients presenting with a rare brainstem syndrome Devin E. Prior, Vijay Renga PII: S2405-6502(18)30036-4 DOI: https://doi.org/10.1016/j.ensci.2018.11.004
Accepted Manuscript Comparison of costs and outcomes of patients presenting with a rare brainstem syndrome Devin E. Prior, Vijay Renga PII: S2405-6502(18)30036-4 DOI: https://doi.org/10.1016/j.ensci.2018.11.004
Microsurgical Resection of Incompletely Obliterated Intracranial Arteriovenous Malformations Following Stereotactic Radiosurgery
 II-2. Selection of Treatment Microsurgical Resection of Incompletely Obliterated Intracranial Arteriovenous Malformations Following Stereotactic Radiosurgery Steven D. CHANG*, Gary K. STEINBERG*, Richard
II-2. Selection of Treatment Microsurgical Resection of Incompletely Obliterated Intracranial Arteriovenous Malformations Following Stereotactic Radiosurgery Steven D. CHANG*, Gary K. STEINBERG*, Richard
Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report
 ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report A Babbu, R Katheerayson Citation A Babbu, R Katheerayson..
ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report A Babbu, R Katheerayson Citation A Babbu, R Katheerayson..
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cavernous Malformations at Optic Apparatus: Three Cases
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, https//doi.org/10.7461/jcen.2018.20.3.176 Case Report Cavernous Malformations at Optic Apparatus: Three Cases
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, https//doi.org/10.7461/jcen.2018.20.3.176 Case Report Cavernous Malformations at Optic Apparatus: Three Cases
Radiographic and statistical analysis of Brain Arteriovenous Malformations.
 Radiographic and statistical analysis of Brain Arteriovenous Malformations. Poster No.: C-0996 Congress: ECR 2017 Type: Educational Exhibit Authors: C. E. Rodriguez 1, A. Lopez Moreno 1, D. Sánchez Paré
Radiographic and statistical analysis of Brain Arteriovenous Malformations. Poster No.: C-0996 Congress: ECR 2017 Type: Educational Exhibit Authors: C. E. Rodriguez 1, A. Lopez Moreno 1, D. Sánchez Paré
UPSTATE Comprehensive Stroke Center. Neurosurgical Interventions Satish Krishnamurthy MD, MCh
 UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
 www.yassermetwally.com MANAGEMENT OF CEREBRAL HAEMORRHAGE (ICH): A QUICK GUIDE Overview 10% of strokes is caused by ICH. Main Causes: Less than 40 years old: vascular malformations and illicit drug use.
www.yassermetwally.com MANAGEMENT OF CEREBRAL HAEMORRHAGE (ICH): A QUICK GUIDE Overview 10% of strokes is caused by ICH. Main Causes: Less than 40 years old: vascular malformations and illicit drug use.
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports-
 Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
Fig. 1. A 58-year-old woman with severe lower extremity pain and weakness
 3 7 A B Fig. 1. A 58-year-old woman with severe lower extremity pain and weakness (case 1). MR sagittal image shows a posterior epidural mass (solid black arrows) showing iso intensity on T1-weighted image
3 7 A B Fig. 1. A 58-year-old woman with severe lower extremity pain and weakness (case 1). MR sagittal image shows a posterior epidural mass (solid black arrows) showing iso intensity on T1-weighted image
Magnetic Resonance Imaging Findings of Eosinophilic Meningoencephalitis Caused by Angiostrongyliasis
 Chin J Radiol 2001; 26: 45-49 45 CASE REPORT Magnetic Resonance Imaging Findings of Eosinophilic Meningoencephalitis Caused by Angiostrongyliasis TSYH-JYI HSIEH 1 GIN-CHUNG LIU 1 CHUAN-MIN YEN 2 YU-TING
Chin J Radiol 2001; 26: 45-49 45 CASE REPORT Magnetic Resonance Imaging Findings of Eosinophilic Meningoencephalitis Caused by Angiostrongyliasis TSYH-JYI HSIEH 1 GIN-CHUNG LIU 1 CHUAN-MIN YEN 2 YU-TING
A.J. Hauer Intracranial dural arteriovenous fistulae
 A.J. Hauer 27-06-2018 Intracranial dural arteriovenous fistulae Dural arteriovenous fistulae (davfs) epidemiology Pathological anastomoses (within the dural leaflets) between meningeal arteries and dural
A.J. Hauer 27-06-2018 Intracranial dural arteriovenous fistulae Dural arteriovenous fistulae (davfs) epidemiology Pathological anastomoses (within the dural leaflets) between meningeal arteries and dural
