Automated Ultrasound of the Breast for Diagnosis: Interobserver Agreement on Lesion Detection and Characterization
|
|
|
- Anissa Nicholson
- 6 years ago
- Views:
Transcription
1 Women s Imaging Original Research Shin et al. Automated Breast Ultrasound Women s Imaging Original Research Hee Jung Shin 1 Hak Hee Kim Joo Hee Cha Ju Hyun Park Kyoung Eun Lee Jeoung Hyun Kim Shin HJ, Kim HH, Cha JH, Park JH, Lee KE, Kim JH 1 All authors: Department of Radiology and Research Institute of Radiology, Asan Medical Center, University of Ulsan, College of Medicine, 86 Asanbyeongwon-gil, Songpa-gu, Seoul, , South Korea. Address correspondence to H. H. Kim (hhkim@amc.seoul.kr). AJR 2011; 197: WOMEN S IMAGING Keywords: automated ultrasound, breast, neoplasm DOI: /AJR Received September 24, 2010; accepted after revision March 7, X/11/ American Roentgen Ray Society Automated Ultrasound of the Breast for Diagnosis: Interobserver Agreement on Lesion Detection and Characterization OBJECTIVE. The purpose of this study was to prospectively evaluate interobserver agreement on lesion detection and characterization in the review of automated ultrasound images of the breast by five radiologists. SUBJECTS AND METHODS. From August to October 2009, bilateral whole-breast ultrasound examinations were performed with an automated technique and with a handheld device for 55 women consecutively scheduled to undergo diagnostic ultrasound. Three-dimensional volume data from automated ultrasound were reviewed by five radiologists, who were unaware of the results of ultrasound with a handheld device and mammography and of the clinical information. If a lesion was detected with automated ultrasound, clock-face position, distance from the nipple, largest diameter, and BI-RADS final assessment category were evaluated. If the lesion was a mass, shape, orientation, margin, echogenicity, and posterior feature were analyzed. Intraclass correlation coefficients and kappa statistics were used for statistical analysis. RESULTS. At least two observers identified 145 lesions with automated ultrasound. Among 725 possible detections, 587 (81%) detections were made. Individual investigators detected between 74% (107/145) and 88% (127/145) of the lesions. The rate of detection of lesions larger than 1.2 cm was 92%. Most lesions detected only with handheld ultrasound (11/12, 92%) or automated ultrasound (34/36, 94%) were cysts or probably benign masses. All intraclass correlation coefficients for lesion location and size exceeded 0.75, indicating high reliability. Substantial agreement was found for mass shape (κ = 0.71), orientation (κ = 0.72), margin (κ = 0.61), and BI-RADS final assessment category (κ = 0.63). CONCLUSION. Detection of lesions larger than 1.2 cm in greatest diameter was reliable. High reliability was obtained for reporting lesion size and location. Substantial agreement was obtained for description of key feature and final assessment category. B reast ultrasound has become accepted as a diagnostic tool to be used in conjunction with mammography for evaluating breast abnormalities [1]. The use of breast ultrasound preoperatively and in interventional procedures is well established [2, 3], and the use of mammography as the standard method for breast cancer screening has reduced breast cancer mortality [4]. Because mammograms are summation images, all breast tissue overlapping in each view, the value of mammography for cancer detection is reduced in the care of women with dense breast tissue, and mammographically missed cancer is a particular problem among these women [5, 6]. Boyd et al. [6] found that the odds of interval cancer among women with extremely dense breasts was 17.8 times that among women with fatty breasts. Ultrasound is an attractive supplement to mammography because it is widely available, relatively inexpensive, and well-tolerated by patients [7]. The combined diagnostic yield of mammography and breast ultrasound has been found to be greater than that of mammography alone [8] and is reported to be % among women with palpable masses [9]. Bilateral whole-breast ultrasound may also have value. Ultrasound can be used to identify additional invasive cancer and help assess the extent of disease in women with newly diagnosed cancer [2, 10 12]. Early results of single-center studies have been promising for cancer detection [13 17], but the time and skill necessary to detect small nonpalpable tumors with handheld ultrasound devices has discouraged widespread use [18, 19]. The results of a multicenter trial [20, 21] AJR:197, September
2 Shin et al. of supplemental screening breast ultrasound for women at high risk with dense breast tissue have been promising, but lack of uniformity and shortage of qualified personnel limit wide implementation of ultrasound with a handheld device. Using automated whole-breast ultrasound, personnel with lesser training can gather standardized uniform images, and physicians can interpret the image data sets efficiently in a short time. Several previous studies have shown that 3D automated breast ultrasound is feasible [22, 23] and that it facilitates detection and classification of solid and cystic lesions with high sensitivity in a selected patient group [24]. Kelly et al. [25, 26] found that using automated breast ultrasound in addition to mammography improved the accuracy of breast cancer detection, callback rates, and confidence in callbacks of women with dense breast tissue. Consistent recognition and characterization of lesions is critical in whole-breast ultrasound applications. They require consistent reporting of lesion location, size, and description and depiction of features. The purpose of our study was to prospectively evaluate interobserver agreement on lesion detection and characterization among five breast radiologists reviewing automated breast ultrasound images. Subjects and Methods Participants Our institutional review board approved this study. From August to October 2009, study participation was offered to patients who underwent consecutive diagnostic ultrasound examinations with handheld devices at our institution. Patients who agreed to participate in the study and signed an informed consent form were recruited for this study. Women with greater than 7-cm compressed breast thickness at mammography were specifically not recruited because of the limited effectiveness of ultrasound in identifying small masses at this depth and the resultant decreased reliability of automated ultrasound of the breast in examinations of these women [25]. A final sample of 55 patients (age range, years; mean, 48 years) underwent automated and handheld ultrasound in the supine position. The indications for ultrasound were preoperative staging of breast cancer for 20 patients, inconclusive mammographic findings for 10 patients, workup for abnormalities found at breast ultrasound at other hospitals for 10 patients, evaluation of palpable lump for six patients, follow-up of probably benign findings for six patients, nipple discharge for two patients, and follow-up after breast cancer surgery for one patient. Breast Ultrasound Handheld device Breast ultrasound with the handheld device (IU22, Philips Healthcare) equipped with a 50-mm linear-array transducer with a bandwidth of 5 12 MHz was performed by one of five radiologists with 1, 3, 6, and 9 years of experience according to a standardized scanning protocol. At our institution, the scanning technique for bilateral whole-breast ultrasound is standardized as follows: scanning of the right breast in the transverse and sagittal orientations, scanning of the inner aspect of the breast in a supine position, and scanning of the outer aspect of the breast in a supine oblique position with the woman s arm raised above her head. We documented each cystic and solid lesion with an image of its largest horizontal diameter (recording both horizontal and vertical diameters) and an image perpendicular to that with its respective diameter. For each lesion, we recorded the location according to breast, clock position to the nearest half hour, and estimated distance from the nipple in centimeters. The average time to perform a ultrasound examination with a handheld device was approximately 20 minutes. Automated system Automated ultrasound of the breast (Acuson S2000 automated breast volume scanner, Siemens Healthcare) was performed by two technologists, who had participated in 2 weeks of training in the technique. The device consisted of the automated breast volume scanner module with the core components of flexible arms, touchscreen monitor, and scanner (transducer, scan box, and screen membrane for contact). The large-footprint wide-frequency-bandwidth transducer (5 14 MHz with a 9-MHz center frequency) captures a volume of up to 15.4 cm 16.8 cm 6 cm maximum by acquisition of a series of 320 high-resolution axial 2D images at slice intervals of 0.5 mm. For scanning with the automated system, customized presets were used to optimize depth, gain, frequency, and view. A typical examination comprised three automated scans of each breast in the anteroposterior and both oblique positions. Occasional additional views were required for larger breasts, the scans being centered on a palpable abnormality or axillary lymph nodes. After acquisition, proprietary postprocessing algorithms were applied according to nipple location to maximize the quality of the diagnostic information. The proprietary postprocessing algorithms included a reverberation removal algorithm, an adaptive nipple shadow reduction tool, and a gain-correction algorithm provided and developed by the manufacturer. After acquisition, the series of axial images was automatically sent from the automated breast volume scanner to a dedicated breast ultrasound review workstation. The usual acquisition time for automated ultrasound of the breast was 60 seconds per scan. The total acquisition time per patient, including setup time, was 15 minutes. The system captured the volume data at slice intervals of 0.5 mm. After volume data acquisition, the data were automatically sent from the automated breast volume scanner to the workstation and reviewed in multiple orientations in a multiplanar reconstruction display. A total of 320 images were generated at 0.5-mm slice thickness and 160 images at 1-mm slice thickness. Therefore, at three scans per breast, 960 images were obtained for each breast at 0.5-mm intervals and 480 images at 1-mm intervals. Spatial compounding was applied during the scanning process, and harmonic imaging was feasible but not used for automated ultrasound. Features Recorded Five radiologists with 1, 3, 6, and 9 years of experience evaluated the 3D volume data at the automated breast ultrasound workstation. They had performed and interpreted images from at least 1500 breast ultrasound examinations in the previous year. They participated in a 3-hour tutorial explaining operation of the automated breast ultrasound review workstation, and all readers reviewed and discussed approximately 10 automated breast ultrasound examinations. The radiologists were blinded to the findings on the corresponding mammograms and handheld ultrasound images and to clinical information. Each reader evaluated automated ultrasound data according to the BI-RADS lexicon [27]. The BI-RADS ultrasound [27] features were recorded, beginning with whether the lesion was a special case. Special cases were defined as any of the following; cyst, complicated cyst, clustered microcysts, intraductal mass, lymph node, postsurgical scar, or calcifications. For each lesion, each reader was required to make a BI-RADS final assessment as one of the following: 1, negative; 2, benign; 3, probably benign (2% or lower probability of malignancy); 4A, low suspicion (risk of malignancy, 3 10%); 4B, intermediate suspicion (risk of malignancy, 11 49%); 4C, moderate suspicion (risk of malignancy, 50 94%); or 5, highly suggestive of malignancy (95% or greater likelihood of malignancy). For cases that were not deemed special, the following additional features were recorded: shape (oval, round, or irregular), orientation (parallel to the skin surface or not), margin (circumscribed, microlobulated, indistinct, spiculated, angular), boundary (abrupt or echogenic halo), echo pattern (anechoic, isoechoic, hyperechoic, hypoechoic, mixed hyperechoic-hypoechoic, complex cystic), and posterior feature (none, enhancement, shadowing, or combined enhancement and shadowing). Finally, each reader recorded lesion location (clock-face position, distance from the nipple in 748 AJR:197, September 2011
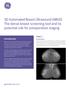
3 Automated Breast Ultrasound centimeters), largest diameter in centimeters, BI- RADS features [27], and BI-RADS final assessment category. Ultrasound findings of benign lesions included cyst, fat lobule, fibrous ridge, ductal ectasia, and hyperechoic lesion. Probably benign lesions were defined as circumscribed, oval, or gently lobulated nonpalpable hypoechoic masses and had no suspicious findings. Suspicious lesions were defined as noncircumscribed hypoechoic masses with a nonparallel orientation, microcalcifications, posterior shadowing, echogenic halo, or ductal extension. HHUS: 121 lesions ABUS only: 36 lesions Exclusion: 12 lesions detected by only one reader on ABUS 145 lesions in 55 patients detected by at least two readers Malignant: 28 lesions High-risk: 3 lesions Benign or probably benign: 114 lesions Data Review and Statistical Analysis The primary aim of this study was to estimate the reproducibility of assessment of various lesion characteristics across multiple readers using automated breast ultrasound for diagnostic purposes. The assessments included measurement of size, identification of lesions, and recording of lesion location. Initially, summary tables and simple frequencies were used to explore the data and check for outliers. Intraclass correlation coefficient was calculated for continuous variables, such as number of lesions detected, lesion size, clock position, and distance from the nipple, compared with the findings with handheld ultrasound. Kappa statistics were used to measure agreement on lesion features and final assessments compared with the consensus finding. Missing values were excluded. A kappa value of 1.0 denoted perfect agreement; , almost perfect agreement; , substantial agreement; , moderate agreement; , fair agreement; and 0.20 or less, slight agreement [28]. Two-sided 95% CI was used to estimate the intraclass correlation coefficient. Agreement values were estimated for different subgroups according to various parameters (e.g., size, benign vs malignant histopathologic outcome). For size, we arbitrarily determined a cutoff point of 0.7 cm, which was the median value of the longest diameter. For categoric variables, we pooled data from all five readers to obtain overall percentages. For data analysis, the findings at automated ultrasound and handheld ultrasound were compared by one radiologist (6 years of experience in breast ultrasound), and lesions were matched and assigned lesion numbers across five readers. To reduce the effect of false-positive detection, for reproducibility and kappa statistics, we considered only lesions seen by at least two readers. The consensus description across all readers identifying any given lesion was considered the reference standard for that lesion. Consensus was defined as detection of a lesion by at least two readers. Fig. 1 Flow chart summarizes study sample in terms of numbers of lesions. ABUS = automated breast ultrasound, HHUS = handheld ultrasound. Results Participants A total of 121 lesions in 55 patients (age range, years; mean, 48 years) were identified with conventional handheld ultrasound. Thirty-six lesions were additionally identified with automated breast ultrasound. Four of the 157 lesions were detected by no reader, and eight lesions were detected by only one reader using automated ultrasound. Therefore, 145 lesions were identified by at least two observers using automated ultrasound, and these 145 lesions comprised the study sample (Fig. 1). The largest diameter of the 145 lesions ranged from 0.2 to 11.0 cm (mean, 1.1 ± 1.4 [SD] cm; median, 0.7 cm). The largest diameter of the 28 malignant lesions ranged from 0.6 to 9.3 cm (mean, 2.4 ± 1.7 cm; median, 2.1 cm). Twenty patients had 28 malignant lesions and underwent 22 ultrasound-guided biopsies. Seventeen patients had invasive ductal carcinoma, one patient had ductal carcinoma in situ, one patient had invasive lobular carcinoma, and one patient had metaplastic carcinoma. Three patients had high-risk lesions diagnosed at subsequent percutaneous biopsy, all of which were papilloma. All papillomas were excised. The other 32 patients had benign or probably benign lesions according to the review of mammograms and handheld ultrasound images. Lesion Detection With Automated Whole-Breast Ultrasound Of 725 potential detections, 587 (81%) detections were made. Individual investigators detected between 107 (74%) and 127 (88%) of the 145 lesions in the sample. Twentythree (16%) were detected by only two investigators; 22 (15%) were detected by three investigators; 25 (17%) were detected by four investigators; and 75 (52%) were detected by five investigators. Among a total of 138 detections of 70 lesions missed by fewer than three readers, 70 (51%) were simple (n = 45) or complicated cysts (n = 25) with an average size of 0.5 cm; seven (5%) were ductal ectasia; 50 (36%) were probably benign masses with an average size of 0.7 cm; six (4%) were indeterminate masses with no proven malignancy; and five (4%) were malignant lesions proved pathologically that were missed by one reader (one lesion) or two readers (two lesions) at automated ultrasound. With respect to the 12 lesions identified with handheld ultrasound and not detected with automated ultrasound (four by none of the five radiologists, eight by only one radiologist), five corresponded to cysts, four to probably benign masses (diameter, 0.7 cm or less), two to ductal ectasia, and one to biopsyproven ductal carcinoma in situ (Fig. 2). This lesion was very subtle even on ultrasound images obtained with the handheld device. The radiologist who performed handheld ultrasound reviewed mammograms at the time and detected this subtle lesion, which corresponded to pleomorphic calcifications on mammograms. However, none of the five readers detected this subtle lesion with automated ultrasound (Fig. 2). The other three lesions not detected by any of the five readers were one cyst and two probably benign masses. Pathologic examination showed 20 patients had 28 biopsy-proven malignant lesions. Twenty-four of the 28 malignant lesions were detected by all five readers, and three lesions were detected by three or four readers (Fig. 3). The single remaining lesion was not detected by any of the five readers, as mentioned earlier (Fig. 2). Among 36 lesions detected only with automated ultrasound, 20 lesions were considered consensus masses and 16 lesions were AJR:197, September
4 Shin et al. considered consensus cysts. Eighteen consensus masses were interpreted as probably benign, and the other two were interpreted as indeterminate. After automated ultrasound, these two patients underwent second-look ultrasound. One lesion was not reproducible at handheld ultrasound and was misinterpreted by two readers at automated ultrasound owing to the presence of Cooper ligament shadowing (Fig. 4). The other lesion was considered probably benign at handheld ultrasound. The lesion detection rate increased as lesion size increased, as follows: 107 of 155 (69%) potential detections were made at a lesion size of 0.4 cm or smaller, 243 of 310 (78%) at cm, 66 of 75 (88%) at 0.9 A 1.2 cm, and 171 of 185 (92%) at more than 1.2 cm in diameter. The sensitivity and specificity of handheld ultrasound were 100% and 93%. The sensitivity of automated ultrasound for the five readers was 100%, 90%, 100%, 93%, and 97%, and the specificity was 92%, 91%, 86%, 96%, and 94%. The area under the curve was for handheld ultrasound: for reader 1, for reader 2, for reader 3, for reader 4, and for reader 5. Agreement The intraclass correlation coefficients for number of detected lesions, clock position, distance from the nipple, and largest diameter were 0.83 (95% CI, ), 0.77 (95% CI, ), 0.89 (95% CI, ), and 0.92 (95% CI, ). All exceeded 0.75, which indicated very high reliability. In terms of comparison of the findings with handheld ultrasound and automated ultrasound, intraclass correlation coefficients for clock position, distance from the nipple, and largest diameter were 0.75, 0.89, and Sixty-five of the 145 lesions were considered special cases. For special cases (cyst, complicated cyst, ductal ectasia, calcifications, lymph node, or not a special case), the overall kappa value was 0.63 (Table 1). Specific designation of a lesion as a cyst or complicated cyst had kappa values of 0.65 and Special cases were excluded from subsequent feature analysis, which left 80 solid masses to be described by consensus. For mass, the overall kappa value was 0.75 (Table 1). Substantial agreement was found for assessment of lesion shape (κ = 0.71) and mass orientation (κ = 0.72). Reader agreement was greatest for irregular shape (κ = 0.76) and lowest for round shape (κ = 0.25) (Table 2). Substantial agreement was found for margin assessment (κ = 0.61). Almost perfect agreement was found when margins were grouped into circumscribed or not (κ = 0.808). Moderate agreement was found between readers in echogenicity assessment (κ = 0.45). The lowest agreement was noted for complex cystic masses (κ = 0.33). Fig year-old woman with biopsy-proven cancer of right breast. A, Mammogram of left breast shows pleomorphic calcifications with segmental distribution in upper outer quadrant. B, Handheld ultrasound image of left breast shows subtle mixed hyperechoic-hypoechoic lesions with suspicious echogenic foci (arrows). C, Automated ultrasound image of left breast shows subtle localized areas of heterogeneous echogenicity (arrows) without definite associated mass in upper outer quadrant that were not detected by any of five readers. Surgery confirmed presence of 3.0-cm ductal carcinoma in situ, micropapillary pattern. B A C B Fig year-old woman with breast cancer. A, Handheld ultrasound image shows irregularly shaped hypoechoic mass with microlobulated margin (arrows) adjacent to biopsy-proven malignant mass (circle) in upper outer quadrant of left breast. B, Automated ultrasound image shows malignant-looking mass (arrows) adjacent to biopsy-proven malignant mass (circle), which was not detected by one reader. Surgery confirmed two foci of invasive ductal carcinoma. 750 AJR:197, September 2011
5 Automated Breast Ultrasound TABLE 1: Interobserver Agreement on BI-RADS Descriptors BI-RADS Descriptor No. of Lesions k Subgroup k Special case (0.040) Cyst (0.05) Complicated cyst (0.07) Duct ectasia 3 NA Calcifications 1 NA Lymph node 1 NA Mass (0.04) Note Data in parentheses are standard error. NA = not applicable (no entries). TABLE 2: Interobserver Agreement on BI-RADS Features of 80 Masses A B Fig year-old woman with indeterminate breast mass. A, Automated ultrasound image of left breast shows irregularly shaped hypoechoic mass (arrow) with posterior shadowing that was interpreted as indeterminate by two readers. B, Second-look handheld ultrasound image shows lesion (arrow) was not reproducible. Finding was considered shadowing due to Cooper ligament. Moderate agreement was achieved in description of posterior acoustic features (κ = 0.42). BI-RADS final assessment categories of the 145 lesions were reported as 1 or 2 (40%, 240 of 603), 3 (31%, 184 of 603), 4A (11%, 68 of 603), 4B (3%, 19 of 603), 4C (2%, 12 of 603), and 5 (13%, 80 of 603) by five readers (Table 3). Examination of all categories together showed substantial agreement (κ = 0.63). Substantial agreement was found when final assessment was grouped into three categories: 1 and 2, 3, and 4A 4C and 5 (κ = 0.712). In terms BI-RADS Descriptor No. of Interpretations (n = 358) a k b Subgroup k b Mass shape 0.71 (0.06) Round 12 (3) 0.25 (0.11) Oval 211 (59) 0.74 (0.05) Irregular 135 (38) 0.76 (0.06) Mass orientation 0.72 (0.08) Mass margins 0.61 (0.04) Circumscribed 195 (54) 0.81 (0.05) Microlobulated 38 (11) 0.20 (0.06) Indistinct 75 (21) 0.68 (0.08) Spiculated 24 (7) 0.52 (0.15) Angular 26 (7) 0.11 (0.06) Lesion boundary 0.43 (0.07) Echogenicity relative to fat 0.45 (0.05) Isoechoic 107 (30) 0.42 (0.05) Hypoechoic 227 (63) 0.48 (0.06) Mixed hyperechoic-hypoechoic 10 (3) 0.49 (0.20) Complex cystic 14 (4) 0.33 (0.05) Posterior features 0.42 (0.07) None 276 (77) 0.59 (0.07) Shadowing 52 (15) 0.47 (0.09) Enhancement 30 (8) 0.28 (0.06) Note 358 interpretations of 80 masses. Data are from automated ultrasound across five observers. NA = not applicable (no entries). a Data in parentheses are percentages. b Data in parentheses are standard error. AJR:197, September
6 Shin et al. TABLE 3: Percentage of Lesions in Each BI-RADS Category and Interobserver Agreement BI-RADS Final Assessment Category or Subdivision Percentage of Interpretations (n = 603) k a Subgroup k 0.63 (0.04) 1 or (0.07) (0.05) 4A (0.07) 4B (0.03) 4C (0.05) (0.07) Note 603 interpretations of 145 lesions based on automated ultrasound findings. Data are for five observers. Data in parentheses are standard error. a For grouped final assessments (1 or 2, 3, and 4A C or 5), k = of comparison of the findings at handheld and automated ultrasound, substantial agreement also was found for final assessment (κ = 0.64). Subgroup Findings With respect to malignant versus benign masses, reader agreement was lower regarding malignant lesions in the assessment of mass orientation and posterior acoustic feature (Table 4). Agreement on other features, such as mass shape, margin, lesion boundary, and echogenicity, was greater for malignant lesions than for benign lesions. With respect to grouping of the lesions on the basis of size, reader agreement was generally less for lesions 0.7 cm and smaller. This difference between size groups was more pronounced for mass shape, margin, echogenicity, and posterior acoustic feature. Similarly, worse concordance on assessment of BI-RADS category was noted for masses measuring 0.7 cm and smaller (κ = 0.37) than for masses larger than 0.7 cm (κ = 0.67). Discussion Breast ultrasound is considered an invaluable tool in breast imaging and a first-line examination with a role in both detection and characterization of breast lesions [14]. As TABLE 4: Interobserver Agreement on BI-RADS Descriptors According to Size and Nature of Mass are other breast imaging techniques, breast ultrasound is affected by a lack of reproducibility in lesion characterization, particularly of small lesions [28 34]. Unlike lesions detected at most other radiologic examinations, a lesion not detected during breast ultrasound generally is not documented. Automated whole-breast ultrasound has potential for complete documentation. It is well known that compared with use of mammography alone, the use of breast ultrasound improves breast cancer detection [19, 25, 35]. However, the operator dependence of handheld ultrasound is a major concern with respect to the widespread use of whole-breast ultrasound. Automated ultrasound has several advantages over handheld ultrasound: The technique is more readily reproducible, has 3D capability through multiplanar reconstruction, and allows delayed interpretation outside of real time, optimizing the radiologist s reading environment. When we interpret automated ultrasound images in routine clinical practice, consistent recognition of lesions, especially breast cancer, across multiple readers is an important issue. In our study, we found high reliability in the recording of lesion location, which was described as lesion size, clock position, and distance from the nipple in centimeters. Previous studies showed that 6.6% of women needed short-interval follow-up of probably benign findings seen only at ultrasound [35]. Our results suggest that such follow-up with automated ultrasound is feasible because lesion size and location are consistently recorded. The primary goal of our study was assessment of the reliability of automated ultrasound for lesion detection, description, and interpretation in the diagnostic setting. We found the rate of lesion detection increased as lesion size increased; detection was reliable (92%) only when mean lesion diameter was greater than 1.2 cm. In terms of lesion detection, 12 of 121 lesions detected with handheld ultrasound were not detected by all five readers (four lesions) or were detected by only one reader (eight lesions). Only one of these 12 cases was biopsy-proven ductal carcinoma in situ (Fig. 2), which was a very subtle lesion even at handheld ultrasound. In routine practice, radiologists review mammographic and clinical findings before interpreting automated ultrasound images. The problem of missing small subtle lesions in routine practice can be avoided when automated ultrasound findings are interpreted along with the clinical and mammographic findings. In addition, all but one of the Size Nature Descriptor Overall (n = 80) 0.7 cm (n = 18) > 0.7 cm (n = 62) Benign (n = 50) Malignant (n = 30) Mass shape 0.71 (0.06) 0.35 (0.16) 0.75 (0.06) 0.40 (0.12) 0.64 (0.12) Mass orientation 0.72 (0.08) 0.68 (0.10) 0.72 (0.09) 0.71 (0.09) 0.69 (0.19) Mass margin 0.61 (0.04) 0.40 (0.14) 0.67 (0.05) 0.40 (0.06) 0.65 (0.08) Lesion boundary 0.43 (0.07) 0.32 (0.07) 0.54 (0.07) 0.45 (0.07) 0.52 (0.13) Echogenicity 0.45 (0.05) 0.31 (0.11) 0.55 (0.05) 0.42 (0.09) 0.47 (0.07) Posterior acoustic feature 0.42 (0.07) 0.30 (0.12) 0.52 (0.07) 0.45 (0.09) 0.41 (0.08) BI-RADS final assessment category 0.63 (0.04) 0.37 (0.16) 0.67 (0.05) 0.55 (0.07) 0.65 (0.09) Note Data in parentheses are standard error. 752 AJR:197, September 2011
7 Automated Breast Ultrasound 28 biopsy-proven malignant lesions (the exception was the aforementioned carcinoma in situ) were detected by more than three readers, which showed high reliability of cancer detection with automated ultrasound. Falsepositive detection is also an issue with respect to incorporating automated ultrasound in routine practice. In this study, 34 of 36 (94%) lesions detected only with automated ultrasound were small probably benign masses or cysts, and only two (6%) lesions were interpreted as consensus indeterminate masses. These findings were not reproducible at handheld ultrasound. The false-positive detection rate (6%) leading to possible recommendation of biopsy based on automated ultrasound findings was sufficiently low. In diagnostic applications, it is critical to minimize the rate of performance of unnecessary biopsy. Accurate lesion characterization is critical to successful use of automated ultrasound. We found substantial agreement on description of special cases (κ = 0.63) and masses (κ = 0.75) and relatively inconsistent characterization of complicated cysts. Berg et al. [33] reported that detection and characterization of cysts varied with lesion size and that characterization of lesions as simple cyst equivalents was unreliable for lesions 0.3 cm in diameter or smaller. At least some of the variability in differentiating simple cysts from complicated cysts and solid lesions likely relates to variable user-defined gain and possibly difference in scanning pressure. However, because we are familiar with automated ultrasound images and can change the contrast, this problem can be ameliorated. In terms of mass shape and margin, we found a higher rate of agreement on circumscribed margin but a lower rate on angular margin and round shape compared with results of a previous study [34]. This difference can be explained by the small number of lesions with angular margins (seven lesions) and a round shape (three lesions). On the other hand, the proportion of probably benign masses in our study was larger than that in the previous study, which might have contributed to the higher rate of agreement on circumscribed margins. The differences from findings in other studies also might have been related to the small sample size and the differences between the 3D volume data acquired with automated ultrasound and the 2D data acquired with handheld ultrasound. In other words, we reviewed 3D volume data using multiplanar images, whereas in previous studies of handheld ultrasound, the investigators reviewed representative 2D captured images. Several previous studies [29, 31, 32, 34] have shown substantial agreement on key features of lesion description at handheld ultrasound. We found moderate agreement on lesion boundary, echogenicity, and posterior acoustic features. In subgroup analysis, a higher rate of agreement was found for lesions with a diameter greater than 0.7 cm than for the smaller lesions. A higher rate of agreement also was found for malignant than for benign lesions with respect to key features such as mass shape, margin, and echogenicity. Management according to BI-RADS final assessment is important and should be reproducible across readers. We found substantial agreement with a kappa value of 0.63 for BI-RADS final assessment, which is better than the results of previous studies [30 32, 34]. Skaane et al. [29] reported slightly lower interobserver agreement on management based on ultrasound than mammographic or combined readings with a mean kappa value of 0.48 for hard-copy ultrasound images in comparison with kappa values of 0.58 for mammography and 0.71 for combined readings. Baker et al. [31] reported a kappa value of 0.51 for management based on ultrasound findings. Berg et al. [32] also reported a kappa value of 0.52 for BI-RADS final assessment. In our study, categories 4B and 4C had the lowest kappa values, 0.32 and This finding can be explained by the small number of lesions in these categories and the lack of known factors clearly and objectively defining each subdivision, leading to variable and subjective conceptions of categories 4A, 4B, and 4C among radiologists [34]. In daily practice, automated ultrasound of the breast may have benefit over handheld ultrasound in several respects. First, patients with multiple masses might benefit from faster examination times. Second, patients with malignant breast tumors larger than 5 cm who undergo neoadjuvant chemotherapy may benefit from the automated technique because the handheld device has a smaller footprint (5 cm) and therefore is limited in the evaluation of extent of disease. Third, for patients with dense breast tissue impeding mammography, screening automated ultrasound may be beneficial because of improved workflow efficiency and lack of operator dependence. Fourth, for surgical planning, surgeons who are familiar with the coronal plane may appreciate the multiplanar images obtained with automated ultrasound. Last, second-look ultrasound after breast MRI can be avoided because the 3D volume data on the whole-breast parenchyma can be reviewed after breast MRI. Our study had several weaknesses. First, the readers were blinded to the mammographic and clinical findings, and BI-RADS categorization established only with the ultrasound features does not always reflect actual practice. For example, some lesions might have been classified as category 4 at mammography but as category 3 at ultrasound, and biopsy would have been recommended on the basis of the mammographic finding despite the ultrasound evaluation. Second, our study included a relatively small number of patients. In addition, the number of special cases, such as calcifications and lymph nodes, was relatively small, and there was a lack of clustered microcysts. Third, some descriptors, such as intraductal mass and clustered microcyst, were not assessed. These descriptors should be prospectively evaluated for correlation with the mammographic and clinical findings. Allowing the readers to choose more than one descriptor for the margins, because more than one contour characteristic can be present in the same mass, would have been more realistic. Fourth, none of the 36 lesions detected only with automated ultrasound was biopsied or followed long enough to confirm the benign histologic finding. Further study is needed to confirm our results. Fifth, we did not compare all findings of handheld and automated ultrasound. We compared the findings of the two techniques only for lesion location and final assessment because not all readers reevaluated the captured handheld ultrasound image. Instead, one radiologist matched the findings of handheld ultrasound and automated ultrasound across five readers. Conclusion With a standardized scanning protocol and interpretation criteria for automated ultrasound, we found that detection of lesions larger than 1.2 cm in largest diameter was reliable. High reliability was obtained for reporting lesion size and location, but there was a relatively small number of special cases such as calcifications and lymph nodes and a lack of clustered microcysts. Further studies with a larger number of patients are needed to confirm these results. References 1. Bassett LW. Imaging of breast masses. Radiol Clin North Am 2000; 38: AJR:197, September
8 Shin et al. 2. Berg WA, Gutierrez L, NessAiver MS, et al. Diagnostic accuracy of mammography, clinical examination, US, and MR imaging in preoperative assessment of breast cancer. Radiology 2004; 233: Helbich TH, Matzek W, Fuchsjäger MH. Stereotactic and ultrasound-guided breast biopsy. Eur Radiol 2004; 14: Shapiro S, Venet W, Strax P, Venet L, Roeser R. Tento fourteen-year effect of screening on breast cancer mortality. J Natl Cancer Inst 1982; 69: Mandelson MT, Oestreicher N, Porter PL, et al. Breast density as a predictor of mammographic detection: comparison of interval- and screen-detected cancers. J Natl Cancer Inst 2000; 92: Boyd NF, Guo H, Martin LJ, et al. Mammographic density and the risk and detection of breast cancer. N Engl J Med 2007; 356: Mendelson EB, Tobin CE. Critical pathways in using breast US. RadioGraphics 1995; 15: Flobbe K, Bosch AM, Kessels AG, et al. The additional diagnostic value of ultrasonography in the diagnosis of breast cancer. Arch Intern Med 2003; 163: Houssami N, Irwig L, Simpson JM, McKessar M, Blome S, Noakes J. Sydney Breast Imaging Accuracy Study: comparative sensitivity and specificity of mammography and sonography in young women with symptoms. AJR 2003; 180: Berg WA, Gilbreath PL. Multicentric and multifocal cancer: whole-breast US in preoperative evaluation. Radiology 2000; 214: Hlawatsch A, Teifke A, Schmidt M, Thelen M. Preoperative assessment of breast cancer: sonography versus MR imaging. AJR 2002; 179: Moon WK, Noh DY, Im JG. Multifocal, multicentric, and contralateral breast cancers: bilateral whole-breast US in the preoperative evaluation of patients. Radiology 2002; 224: Gordon PB, Goldenberg SL. Malignant breast masses detected only by ultrasound: a retrospective review. Cancer 1995; 76: Kaplan SS. Clinical utility of bilateral wholebreast US in the evaluation of women with dense breast tissue. Radiology 2001; 221: Kolb TM, Lichy J, Newhouse JH. Comparison of the performance of screening mammography, physical examination, and breast US and evaluation of factors that influence them: an analysis of 27,825 patient evaluations. Radiology 2002; 225: Crystal P, Strano SD, Shcharynski S, Koretz MJ. Using sonography to screen women with mammographically dense breasts. AJR 2003; 181: Leconte I, Feger C, Galant C, et al. Mammography and subsequent whole-breast sonography of nonpalpable breast cancers: the importance of radiologic breast density. AJR 2003; 180: Buchberger W, Niehoff A, Obrist P, DeKoekkoek- Doll P, Dünser M. Clinically and mammographically occult breast lesions: detection and classification with high-resolution sonography. Semin Ultrasound CT MR 2000; 21: Kopans DB. Breast-cancer screening with ultrasonography. Lancet 1999; 354: Berg WA, Blume JD, Cormack JB, et al. Combined screening with ultrasound and mammography vs mammography alone in women at elevated risk of breast cancer. JAMA 2008; 299: Corsetti V, Ferrari A, Ghirardi M, et al. Role of ultrasonography in detecting mammographically occult breast carcinoma in women with dense breasts. Radiol Med 2006; 111: Chou YH, Tiu CM, Chiang HR, et al. Ultrasound BI-RADS categories applied in an automated breast ultrasound system: diagnostic reliability (abstr). RSNA Oak Brook, IL: Radiological Society of North America, rsna.org/index.cfm?em_id= &event=1. Accessed May 17, Destounis S, Young W, Murphy P, et al. Initial experience of automated breast ultrasound screening trial in the setting of a community based private practice (abstr). RSNA Oak Brook, IL: Radiological Society of North America, id= &event=1. Accessed May 17, Wenkel E, Heckmann M, Heinrich M, et al. Automated breast ultrasound: lesion detection and BI- RADS classification a pilot study. Rofo 2008; 180: Kelly KM, Dean J, Comulada WS, Lee SJ. Breast cancer detection using automated whole breast ultrasound and mammography in radiographically dense breasts. Eur Radiol 2010; 20: Kelly KM, Dean J, Lee SJ, Comulada WS. Breast cancer detection: radiologists performance using mammography with and without automated wholebreast ultrasound. Eur Radiol 2010; 20: Mendelson EB, Baum JK, Berg WA, et al. BI- RADS: ultrasound, 1st ed. In: D Orsi CJ, Mendelson EB, Ikeda DM, et al. Breast Imaging Reporting and Data System: ACR BI-RADS breast imaging atlas. Reston, VA: American College of Radiology, Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics 1977; 33: Skaane P, Engedal K, Skjennald A. Interobserver variation in the interpretation of breast imaging: comparison of mammography, ultrasonography, and both combined in the interpretation of palpable noncalcified breast masses. Acta Radiol 1997; 38: Berg WA, Campassi C, Langenberg P, Sexton MJ. Breast Imaging Reporting and Data System: interand intraobserver variability in feature analysis and final assessment. AJR 2000; 174: Baker JA, Kornguth PJ, Soo MS, Walsh R, Mengoni P. Sonography of solid breast lesions: observer variability of lesion description and assessment. AJR 1999; 172: Berg WA, Blume JD, Cormack JB, Mendelson EB. Operator dependence of physician-performed whole-breast US: lesion detection and characterization. Radiology 2006; 241: Berg WA, Blume JD, Cormack JB, Mendelson EB, Madsen EL; ACRIN 6666 Investigators. Lesion detection and characterization in a breast US phantom: results of the ACRIN 6666 investigators. Radiology 2006; 239: Abdullah N, Mesurolle B, El-Khoury M, Kao E. Breast imaging reporting and data system lexicon for US: interobserver agreement for assessment of breast masses. Radiology 2009; 252: Berg WA. Supplemental screening sonography in dense breasts. Radiol Clin North Am 2004; 42: AJR:197, September 2011
RESEARCH ARTICLE. Woo Jung Choi, Joo Hee Cha*, Hak Hee Kim, Hee Jung Shin, Hyunji Kim, Eun Young Chae, Min Ji Hong. Abstract.
 DOI:http://dx.doi.org/10.7314/APJCP.2014.15.21.9101 RESEARCH ARTICLE Comparison of Automated Breast Volume Scanning and Hand- Held Ultrasound in the Detection of Breast Cancer: an Analysis of 5,566 Patient
DOI:http://dx.doi.org/10.7314/APJCP.2014.15.21.9101 RESEARCH ARTICLE Comparison of Automated Breast Volume Scanning and Hand- Held Ultrasound in the Detection of Breast Cancer: an Analysis of 5,566 Patient
ACRIN 6666 IM Additional Evaluation: Additional Views/Targeted US
 Additional Evaluation: Additional Views/Targeted US For revised or corrected form check box and fax to 215-717-0936. Instructions: The form is completed based on recommendations (from ID form) for additional
Additional Evaluation: Additional Views/Targeted US For revised or corrected form check box and fax to 215-717-0936. Instructions: The form is completed based on recommendations (from ID form) for additional
Breast cancer is the leading site of new cancer patients in Thai
 Original Article Can Automated Breast Volume Scanning be an Alternative Tool to Handheld Ultrasonography for Breast Cancer Screening? attawach Ariyaratrangsee, MD 1 ; Worachart Saksirinukul, MD 1 ; Thanyalak
Original Article Can Automated Breast Volume Scanning be an Alternative Tool to Handheld Ultrasonography for Breast Cancer Screening? attawach Ariyaratrangsee, MD 1 ; Worachart Saksirinukul, MD 1 ; Thanyalak
Observer Agreement Using the ACR Breast Imaging Reporting and Data System (BI-RADS)-Ultrasound, First Edition (2003)
 Observer Agreement Using the ACR Breast Imaging Reporting and Data System (BI-RADS)-Ultrasound, First Edition (2003) Chang Suk Park, MD 1 Jae Hee Lee, MD 2 Hyeon Woo Yim, MD 3 Bong Joo Kang, MD 4 Hyeon
Observer Agreement Using the ACR Breast Imaging Reporting and Data System (BI-RADS)-Ultrasound, First Edition (2003) Chang Suk Park, MD 1 Jae Hee Lee, MD 2 Hyeon Woo Yim, MD 3 Bong Joo Kang, MD 4 Hyeon
Aims and objectives. Page 2 of 10
 Diagnostic performance of automated breast volume scanner (ABVS) versus hand-held ultrasound (HHUS) as second look for breast lesions detected only on magnetic resonance imaging. Poster No.: C-1701 Congress:
Diagnostic performance of automated breast volume scanner (ABVS) versus hand-held ultrasound (HHUS) as second look for breast lesions detected only on magnetic resonance imaging. Poster No.: C-1701 Congress:
Table 1. Classification of US Features Based on BI-RADS for US in Benign and Malignant Breast Lesions US Features Benign n(%) Malignant n(%) Odds
 215 Table 1. Classification of US Features Based on BI-RADS for US in Benign and Malignant Breast Lesions US Features Benign n(%) Malignant n(%) Odds ratio 719 (100) 305(100) Shape Oval 445 (61.9) 019
215 Table 1. Classification of US Features Based on BI-RADS for US in Benign and Malignant Breast Lesions US Features Benign n(%) Malignant n(%) Odds ratio 719 (100) 305(100) Shape Oval 445 (61.9) 019
Over the recent decades, breast ultrasonography (US) has
 ORIGINAL RESEARCH Application of Computer-Aided Diagnosis on Breast Ultrasonography Evaluation of Diagnostic Performances and Agreement of Radiologists According to Different Levels of Experience Eun Cho,
ORIGINAL RESEARCH Application of Computer-Aided Diagnosis on Breast Ultrasonography Evaluation of Diagnostic Performances and Agreement of Radiologists According to Different Levels of Experience Eun Cho,
Leonard M. Glassman MD
 BI-RADS The New BI-RADS Leonard M. Glassman MD FACR Former Chief of Breast Imaging American Institute for Radiologic Pathology Washington Radiology Associates, PC Breast Imaging Reporting and Data System
BI-RADS The New BI-RADS Leonard M. Glassman MD FACR Former Chief of Breast Imaging American Institute for Radiologic Pathology Washington Radiology Associates, PC Breast Imaging Reporting and Data System
Mammography and Subsequent Whole-Breast Sonography of Nonpalpable Breast Cancers: The Importance of Radiologic Breast Density
 Isabelle Leconte 1 Chantal Feger 1 Christine Galant 2 Martine Berlière 3 Bruno Vande Berg 1 William D Hoore 4 Baudouin Maldague 1 Received July 11, 2002; accepted after revision October 28, 2002. 1 Department
Isabelle Leconte 1 Chantal Feger 1 Christine Galant 2 Martine Berlière 3 Bruno Vande Berg 1 William D Hoore 4 Baudouin Maldague 1 Received July 11, 2002; accepted after revision October 28, 2002. 1 Department
Mammographically non-calcified ductal carcinoma in situ: sonographic features with pathological correlation in 35 patients
 Clinical Radiology (2009) 64, 628e636 ORIGINAL PAPER Mammographically non-calcified ductal carcinoma in situ: sonographic features with pathological correlation in 35 patients B. Mesurolle a, *, M. El-Khoury
Clinical Radiology (2009) 64, 628e636 ORIGINAL PAPER Mammographically non-calcified ductal carcinoma in situ: sonographic features with pathological correlation in 35 patients B. Mesurolle a, *, M. El-Khoury
Introduction ORIGINAL ARTICLE. 170 Ultrasonography 33(3), July 2014 e-ultrasonography.org
 Positive predictive value of additional synchronous breast lesions in wholebreast ultrasonography at the diagnosis of breast cancer: clinical and imaging factors Ah Hyun Kim 1 *, Min Jung Kim 1, Eun-Kyung
Positive predictive value of additional synchronous breast lesions in wholebreast ultrasonography at the diagnosis of breast cancer: clinical and imaging factors Ah Hyun Kim 1 *, Min Jung Kim 1, Eun-Kyung
Diagnostic benefits of ultrasound-guided. CNB) versus mammograph-guided biopsy for suspicious microcalcifications. without definite breast mass
 Volume 118 No. 19 2018, 531-543 ISSN: 1311-8080 (printed version); ISSN: 1314-3395 (on-line version) url: http://www.ijpam.eu ijpam.eu Diagnostic benefits of ultrasound-guided biopsy versus mammography-guided
Volume 118 No. 19 2018, 531-543 ISSN: 1311-8080 (printed version); ISSN: 1314-3395 (on-line version) url: http://www.ijpam.eu ijpam.eu Diagnostic benefits of ultrasound-guided biopsy versus mammography-guided
ISSN X (Print) Research Article. *Corresponding author Dr. Amlendu Nagar
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(3A):1069-1073 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(3A):1069-1073 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Yonsei University, College of Medicine, 5 Department of Radiology, Soonchunhyang University Bucheon Hospital,
 Original Article Interobserver Variability and Diagnostic Performance with the Fifth Edition of the ACR BI-RADS Lexicon for Ultrasound; Validation from Multi-institutions Sung Hun Kim 1, Dong Wook Kim
Original Article Interobserver Variability and Diagnostic Performance with the Fifth Edition of the ACR BI-RADS Lexicon for Ultrasound; Validation from Multi-institutions Sung Hun Kim 1, Dong Wook Kim
Ductal carcinoma in situ, underestimation, ultrasound-guided core needle biopsy
 Ductal carcinoma in situ diagnosed after an ultrasoundguided 14-gauge core needle biopsy of breast masses: Can underestimation be predicted preoperatively? Poster No.: C-0442 Congress: ECR 2010 Type: Scientific
Ductal carcinoma in situ diagnosed after an ultrasoundguided 14-gauge core needle biopsy of breast masses: Can underestimation be predicted preoperatively? Poster No.: C-0442 Congress: ECR 2010 Type: Scientific
Triple Receptor Negative Breast Cancer: Imaging and Clinical Characteristics
 Women s Imaging Original Research Krizmanich-Conniff et al. Triple Receptor Negative Breast Cancer Women s Imaging Original Research Kristin M. Krizmanich-Conniff 1 Chintana Paramagul 2 Stephanie K. Patterson
Women s Imaging Original Research Krizmanich-Conniff et al. Triple Receptor Negative Breast Cancer Women s Imaging Original Research Kristin M. Krizmanich-Conniff 1 Chintana Paramagul 2 Stephanie K. Patterson
Validation of the fifth edition BI-RADS ultrasound lexicon with comparison of fourth and fifth edition diagnostic performance using video clips
 Validation of the fifth edition BI-RADS ultrasound lexicon with comparison of fourth and fifth edition diagnostic performance using video clips Jung Hyun Yoon 1, Min Jung Kim 1, Hye Sun Lee 2, Sung Hun
Validation of the fifth edition BI-RADS ultrasound lexicon with comparison of fourth and fifth edition diagnostic performance using video clips Jung Hyun Yoon 1, Min Jung Kim 1, Hye Sun Lee 2, Sung Hun
Reassessment and Follow-Up Results of BI-RADS Category 3 Lesions Detected on Screening Breast Ultrasound
 Women s Imaging Original Research Chae et al. I-RDS Category 3 Lesions Found on Screening Ultrasound Women s Imaging Original Research Eun Young Chae 1 Joo Hee Cha Hee Jung Shin Woo Jung Choi Hak Hee Kim
Women s Imaging Original Research Chae et al. I-RDS Category 3 Lesions Found on Screening Ultrasound Women s Imaging Original Research Eun Young Chae 1 Joo Hee Cha Hee Jung Shin Woo Jung Choi Hak Hee Kim
Mammographic imaging of nonpalpable breast lesions. Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand
 Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Amammography report is a key component of the breast
 Review Article Writing a Mammography Report Amammography report is a key component of the breast cancer diagnostic process. Although mammographic findings were not clearly differentiated between benign
Review Article Writing a Mammography Report Amammography report is a key component of the breast cancer diagnostic process. Although mammographic findings were not clearly differentiated between benign
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY
 EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
Imaging in breast cancer. Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since
 Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
The latest developments - Automated Breast Volume Scanning. Dr. med. M. Golatta
 The latest developments - Automated Breast Volume Scanning Dr. med. M. Golatta Automated Breast Volume US: Why? o Mammography is limited in dense breasts: high false negative rate o Many of these tumors
The latest developments - Automated Breast Volume Scanning Dr. med. M. Golatta Automated Breast Volume US: Why? o Mammography is limited in dense breasts: high false negative rate o Many of these tumors
BI-RADS Update. Martha B. Mainiero, MD, FACR, FSBI Brown University Rhode Island Hospital
 BI-RADS Update Martha B. Mainiero, MD, FACR, FSBI Brown University Rhode Island Hospital No Disclosures BI-RADS History 1980s Quality Issues ACR Accreditation BI-RADS 1994 2003 4 th Edition MRI, US January
BI-RADS Update Martha B. Mainiero, MD, FACR, FSBI Brown University Rhode Island Hospital No Disclosures BI-RADS History 1980s Quality Issues ACR Accreditation BI-RADS 1994 2003 4 th Edition MRI, US January
Ultrasonography. Methods. Brief Description. Indications. Device-related Prerequisites. Technical Requirements. Evaluation Criteria
 1 Ultrasonography Brief Description Imaging modality using sound waves Tissue-specific wave reflection. Indications Evaluation of palpable breast nodules Evaluation of clinically occult mammographic findings
1 Ultrasonography Brief Description Imaging modality using sound waves Tissue-specific wave reflection. Indications Evaluation of palpable breast nodules Evaluation of clinically occult mammographic findings
Current Status of Supplementary Screening With Breast Ultrasound
 Current Status of Supplementary Screening With Breast Ultrasound Stephen A. Feig, M.D., FACR Fong and Jean Tsai Professor of Women s Imaging Department of Radiologic Sciences University of California,
Current Status of Supplementary Screening With Breast Ultrasound Stephen A. Feig, M.D., FACR Fong and Jean Tsai Professor of Women s Imaging Department of Radiologic Sciences University of California,
Ultrasound Assessment of Invasive Breast Cancer:
 Ultrasound Assessment of Invasive Breast Cancer: Correlation with Histologic Grade 1 Joo Hee Cha, M.D., Woo Kyung Moon, M.D. 2, Nariya Cho, M.D. 2, Sun Mi Kim, M.D. 2, Seung Ja Kim, M.D. 2, Seong Ho Park,
Ultrasound Assessment of Invasive Breast Cancer: Correlation with Histologic Grade 1 Joo Hee Cha, M.D., Woo Kyung Moon, M.D. 2, Nariya Cho, M.D. 2, Sun Mi Kim, M.D. 2, Seung Ja Kim, M.D. 2, Seong Ho Park,
Breast Ultrasound: Improving Your Skills & Patient Care
 Breast Ultrasound: Improving Your Skills & Patient Care Objectives Discuss US techniques available for image optimization. Review & compare the US appearances of benign & malignant masses. Cherie M. Kuzmiak,
Breast Ultrasound: Improving Your Skills & Patient Care Objectives Discuss US techniques available for image optimization. Review & compare the US appearances of benign & malignant masses. Cherie M. Kuzmiak,
Mucocele-Like Tumors of the Breast as Cystic Lesions: Sonographic-Pathologic Correlation
 Women s Imaging Original Research Kim et al. Breast Tumors as Cystic Lesions Women s Imaging Original Research WOMEN S IMGING Sun Mi Kim 1,2 Hak Hee Kim 1 Doo Kyung Kang 3 Hee Jung Shin 1 Nariya Cho 4
Women s Imaging Original Research Kim et al. Breast Tumors as Cystic Lesions Women s Imaging Original Research WOMEN S IMGING Sun Mi Kim 1,2 Hak Hee Kim 1 Doo Kyung Kang 3 Hee Jung Shin 1 Nariya Cho 4
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY
 EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
Screening Breast Ultrasound: Past, Present, and Future
 Women s Imaging Review Brem et al. Breast Cancer Screening Ultrasound Women s Imaging Review FOCUS ON: Rachel F. Brem 1 Megan J. Lenihan Jennifer Lieberman Jessica Torrente Brem RF, Lenihan MJ, Lieberman
Women s Imaging Review Brem et al. Breast Cancer Screening Ultrasound Women s Imaging Review FOCUS ON: Rachel F. Brem 1 Megan J. Lenihan Jennifer Lieberman Jessica Torrente Brem RF, Lenihan MJ, Lieberman
3D Automated breast ultrasound (ABUS): pictorial review of applications and clinical utility.
 3D Automated breast ultrasound (ABUS): pictorial review of applications and clinical utility. Poster No.: C-1182 Congress: ECR 2013 Type: Educational Exhibit Authors: A. Domingo, C. Cusido, F. V. Gras,
3D Automated breast ultrasound (ABUS): pictorial review of applications and clinical utility. Poster No.: C-1182 Congress: ECR 2013 Type: Educational Exhibit Authors: A. Domingo, C. Cusido, F. V. Gras,
Radiologic Findings of Mucocele-like Tumors of the breast: Can we differentiate pure benign from associated with high risk lesions?
 Radiologic Findings of Mucocele-like Tumors of the breast: Can we differentiate pure benign from associated with high risk lesions? Poster No.: C-0332 Congress: ECR 2014 Type: Educational Exhibit Authors:
Radiologic Findings of Mucocele-like Tumors of the breast: Can we differentiate pure benign from associated with high risk lesions? Poster No.: C-0332 Congress: ECR 2014 Type: Educational Exhibit Authors:
Pitfalls and Limitations of Breast MRI. Susan Orel Roth, MD Professor of Radiology University of Pennsylvania
 Pitfalls and Limitations of Breast MRI Susan Orel Roth, MD Professor of Radiology University of Pennsylvania Objectives Review the etiologies of false negative breast MRI examinations Discuss the limitations
Pitfalls and Limitations of Breast MRI Susan Orel Roth, MD Professor of Radiology University of Pennsylvania Objectives Review the etiologies of false negative breast MRI examinations Discuss the limitations
Contrast-enhanced Breast MRI RSSA 2013
 Contrast-enhanced Breast MRI RSSA 2013 Prof. dr. Maurice van den Bosch University Medical Center Utrecht, the Netherlands Index 1) Breast cancer 2) Why MRI of the breast 3) Technique 4) Interpretation
Contrast-enhanced Breast MRI RSSA 2013 Prof. dr. Maurice van den Bosch University Medical Center Utrecht, the Netherlands Index 1) Breast cancer 2) Why MRI of the breast 3) Technique 4) Interpretation
Pictorial Review of the Ultrasound Appearances of Ductal Carcinoma in Situ
 Pictorial Review of the Ultrasound Appearances of Ductal Carcinoma in Situ Poster No.: R-0079 Congress: 2016 ASM Type: Educational Exhibit Authors: W. G. D. U. M. Wijesinghe, D. Gunawardena, D. B. Taylor
Pictorial Review of the Ultrasound Appearances of Ductal Carcinoma in Situ Poster No.: R-0079 Congress: 2016 ASM Type: Educational Exhibit Authors: W. G. D. U. M. Wijesinghe, D. Gunawardena, D. B. Taylor
Atypical ductal hyperplasia diagnosed at ultrasound guided biopsy of breast mass
 Atypical ductal hyperplasia diagnosed at ultrasound guided biopsy of breast mass Poster No.: C-1483 Congress: ECR 2014 Type: Authors: Keywords: DOI: Scientific Exhibit J. Cho, J. Chung, E. S. Cha, J. E.
Atypical ductal hyperplasia diagnosed at ultrasound guided biopsy of breast mass Poster No.: C-1483 Congress: ECR 2014 Type: Authors: Keywords: DOI: Scientific Exhibit J. Cho, J. Chung, E. S. Cha, J. E.
3D Automated Breast Ultrasound (ABUS): The dense breast screening tool and its potential role for preoperative staging
 3D Automated Breast Ultrasound (ABUS): The dense breast screening tool and its potential role for preoperative staging Introduction Breast cancer is by far the most common cancer amongst women across Europe,
3D Automated Breast Ultrasound (ABUS): The dense breast screening tool and its potential role for preoperative staging Introduction Breast cancer is by far the most common cancer amongst women across Europe,
Index words: Breast US Breast neoplasm Breast cancer
 Index words: Breast US Breast neoplasm Breast cancer 125 47.. 53. (),, taller than wide. 50.. 126 Table 1. + 34 24-106 145,, + 139 167-1 2 + 65 37-75 132 47. duct extension. 127 taller than wide + 62 95-78
Index words: Breast US Breast neoplasm Breast cancer 125 47.. 53. (),, taller than wide. 50.. 126 Table 1. + 34 24-106 145,, + 139 167-1 2 + 65 37-75 132 47. duct extension. 127 taller than wide + 62 95-78
Sonographically-Guided 14-Gauge Core Needle Biopsy for Papillary Lesions of the Breast
 Sonographically-Guided 14-Gauge Core Needle Biopsy for Papillary Lesions of the Breast Eun Sook Ko, MD Nariya Cho, MD Joo Hee Cha, MD Jeong Seon Park, MD Sun Mi Kim, MD Woo Kyung Moon, MD Index terms:
Sonographically-Guided 14-Gauge Core Needle Biopsy for Papillary Lesions of the Breast Eun Sook Ko, MD Nariya Cho, MD Joo Hee Cha, MD Jeong Seon Park, MD Sun Mi Kim, MD Woo Kyung Moon, MD Index terms:
BI-RADS Categorization As a Predictor of Malignancy 1
 Susan G. Orel, MD Nicole Kay, BA Carol Reynolds, MD Daniel C. Sullivan, MD BI-RADS Categorization As a Predictor of Malignancy 1 Index terms: Breast, biopsy, 00.1261 Breast neoplasms, localization, 00.125,
Susan G. Orel, MD Nicole Kay, BA Carol Reynolds, MD Daniel C. Sullivan, MD BI-RADS Categorization As a Predictor of Malignancy 1 Index terms: Breast, biopsy, 00.1261 Breast neoplasms, localization, 00.125,
Using Automated Breast Sonography as Part of a Multimodality Approach to Dense Breast Screening
 447993JDM28410.1177/8756479312447993Giulia no and GiulianoJournal of Diagnostic Medical Sonography Original Article Using Automated Breast Sonography as Part of a Multimodality Approach to Dense Breast
447993JDM28410.1177/8756479312447993Giulia no and GiulianoJournal of Diagnostic Medical Sonography Original Article Using Automated Breast Sonography as Part of a Multimodality Approach to Dense Breast
Pure and Mixed Tubular Carcinoma of the Breast: Mammographic and Sonographic Differential Features
 Pure and Mixed Tubular Carcinoma of the Breast: Mammographic and Sonographic Differential Features Hee Jung Shin, MD 1 Hak Hee Kim, MD 1 Sun Mi Kim, MD 1 Dae Bong Kim, MD 1 Ye Ri Lee, MD 1 Mi-Jung Kim,
Pure and Mixed Tubular Carcinoma of the Breast: Mammographic and Sonographic Differential Features Hee Jung Shin, MD 1 Hak Hee Kim, MD 1 Sun Mi Kim, MD 1 Dae Bong Kim, MD 1 Ye Ri Lee, MD 1 Mi-Jung Kim,
Here are examples of bilateral analog mammograms from the same patient including CC and MLO projections.
 Good afternoon. It s my pleasure to be discussing Diagnostic Breast Imaging over the next half hour. I m Wei Yang, Professor of Diagnostic Radiology and Chief, the Section of Breast Imaging as well as
Good afternoon. It s my pleasure to be discussing Diagnostic Breast Imaging over the next half hour. I m Wei Yang, Professor of Diagnostic Radiology and Chief, the Section of Breast Imaging as well as
Is Probably Benign Really Just Benign? Peter R Eby, MD, FSBI Virginia Mason Medical Center Seattle, WA
 Is Probably Benign Really Just Benign? Peter R Eby, MD, FSBI Virginia Mason Medical Center Seattle, WA Disclosures: CONSULTANT FOR DEVICOR MEDICAL ARS Question 1 Is probably benign really just benign?
Is Probably Benign Really Just Benign? Peter R Eby, MD, FSBI Virginia Mason Medical Center Seattle, WA Disclosures: CONSULTANT FOR DEVICOR MEDICAL ARS Question 1 Is probably benign really just benign?
Multiple Bilateral Circumscribed Masses at Screening Breast US: Consider Annual Follow-up 1
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Wendie A. Berg, MD,
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Wendie A. Berg, MD,
Look differently. Invenia ABUS. Automated Breast Ultrasound
 Look differently. Invenia ABUS Automated Breast Ultrasound InveniaTM ABUS from GE Healthcare offers a view beyond mammography, with breast screening technology that looks differently. 40 % The unseen risk.
Look differently. Invenia ABUS Automated Breast Ultrasound InveniaTM ABUS from GE Healthcare offers a view beyond mammography, with breast screening technology that looks differently. 40 % The unseen risk.
ORIGINAL ARTICLE EVALUATION OF BREAST LESIONS USING X-RAY MAMMOGRAM WITH HISTOPATHOLOGICAL CORRELATION
 Available online at www.journalijmrr.com INTERNATIONAL JOURNAL OF MODERN RESEARCH AND REVIEWS IJMRR ISSN: 2347-8314 Int. J. Modn. Res. Revs. Volume 3, Issue 10, pp 807-814, October, 2015 ORIGINAL ARTICLE
Available online at www.journalijmrr.com INTERNATIONAL JOURNAL OF MODERN RESEARCH AND REVIEWS IJMRR ISSN: 2347-8314 Int. J. Modn. Res. Revs. Volume 3, Issue 10, pp 807-814, October, 2015 ORIGINAL ARTICLE
Clinical Utility of Bilateral Whole-Breast US in the Evaluation of Women with Dense Breast Tissue 1
 Stuart S. Kaplan, MD Index terms: Breast, parenchymal pattern Breast, US, 00.129, 00.12989 Breast neoplasms, diagnosis, 00.32 Breast neoplasms, US, 00.129, 00.12989 Breast radiography, quality assurance,
Stuart S. Kaplan, MD Index terms: Breast, parenchymal pattern Breast, US, 00.129, 00.12989 Breast neoplasms, diagnosis, 00.32 Breast neoplasms, US, 00.129, 00.12989 Breast radiography, quality assurance,
Original Report. Mucocele-Like Tumors of the Breast: Mammographic and Sonographic Appearances. Katrina Glazebrook 1 Carol Reynolds 2
 Katrina Glazebrook 1 Carol Reynolds 2 Received January 2, 2002; accepted after revision August 28, 2002. 1 Department of Radiology, Mayo Clinic, 200 First St. S.W., Rochester, MN 55905. Address correspondence
Katrina Glazebrook 1 Carol Reynolds 2 Received January 2, 2002; accepted after revision August 28, 2002. 1 Department of Radiology, Mayo Clinic, 200 First St. S.W., Rochester, MN 55905. Address correspondence
Since its introduction in 2000, digital mammography has become
 Review Article Smith A, PhD email : Andrew.smith@hologic.com Since its introduction in 2000, digital mammography has become an accepted standard of care in breast cancer screening and has paved the way
Review Article Smith A, PhD email : Andrew.smith@hologic.com Since its introduction in 2000, digital mammography has become an accepted standard of care in breast cancer screening and has paved the way
Retrospective Analysis on Malignant Calcification Previously Misdiagnosed as Benign on Screening Mammography 스크리닝유방촬영술에서양성으로진단되었던악성석회화에대한후향적분석
 Original Article pissn 1738-2637 / eissn 2288-2928 https://doi.org/10.3348/jksr.2017.76.4.251 Retrospective Analysis on Malignant Calcification Previously Misdiagnosed as Benign on Screening 스크리닝유방촬영술에서양성으로진단되었던악성석회화에대한후향적분석
Original Article pissn 1738-2637 / eissn 2288-2928 https://doi.org/10.3348/jksr.2017.76.4.251 Retrospective Analysis on Malignant Calcification Previously Misdiagnosed as Benign on Screening 스크리닝유방촬영술에서양성으로진단되었던악성석회화에대한후향적분석
Sonographic Differentiation of Benign and Malignant Cystic Lesions of the Breast
 Article Sonographic Differentiation of Benign and Malignant Cystic Lesions of the Breast Yun-Woo Chang, MD, PhD, Kwi Hyang Kwon, MD, Dong Erk Goo, MD, Deuk Lin Choi, MD, Hye Kyung Lee, MD, Seung Boo Yang,
Article Sonographic Differentiation of Benign and Malignant Cystic Lesions of the Breast Yun-Woo Chang, MD, PhD, Kwi Hyang Kwon, MD, Dong Erk Goo, MD, Deuk Lin Choi, MD, Hye Kyung Lee, MD, Seung Boo Yang,
Policies, Standards, and Guidelines. Guidelines on Breast Ultrasound Examination and Reporting
 Policies, Standards, and Guidelines Guidelines on Breast Ultrasound Examination and Reporting Approved by Council June 2018 Approved: June 2018 Guidelines on Breast Ultrasound Examination and Reporting
Policies, Standards, and Guidelines Guidelines on Breast Ultrasound Examination and Reporting Approved by Council June 2018 Approved: June 2018 Guidelines on Breast Ultrasound Examination and Reporting
The radiologic workup of a palpable breast mass
 Imaging in Practice CME CREDIT EDUCTIONL OJECTIVE: The reader will consider which breast masses require further workup and which imaging study is most appropriate Lauren Stein, MD Imaging Institute, Cleveland
Imaging in Practice CME CREDIT EDUCTIONL OJECTIVE: The reader will consider which breast masses require further workup and which imaging study is most appropriate Lauren Stein, MD Imaging Institute, Cleveland
Ultrasound of the Breast BASICS FOR THE ORDERING CLINICIAN
 Ultrasound of the Breast BASICS FOR THE ORDERING CLINICIAN Breast Ultrasound Anatomy Skin Breast Parenchyma Pectoralis Fascia Pectoralis Breast Ultrasound Anatomy Indications for Breast Ultrasound Palpable
Ultrasound of the Breast BASICS FOR THE ORDERING CLINICIAN Breast Ultrasound Anatomy Skin Breast Parenchyma Pectoralis Fascia Pectoralis Breast Ultrasound Anatomy Indications for Breast Ultrasound Palpable
Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node
 Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node Oil Cyst Mass, Intermediate Concern Microlobulated Margins Obscured Margins Mass, Favoring Malignant Indistinct
Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node Oil Cyst Mass, Intermediate Concern Microlobulated Margins Obscured Margins Mass, Favoring Malignant Indistinct
RSNA, /radiol Appendix E1. Methods
 RSNA, 2016 10.1148/radiol.2016151097 Appendix E1 Methods US and Near-infrared Data Acquisition Four optical wavelengths (740 nm, 780 nm, 808 nm, and 830 nm) were used to sequentially deliver the light
RSNA, 2016 10.1148/radiol.2016151097 Appendix E1 Methods US and Near-infrared Data Acquisition Four optical wavelengths (740 nm, 780 nm, 808 nm, and 830 nm) were used to sequentially deliver the light
Management of Palpable Abnormalities in the Breast Katerina Dodelzon, MD July 31, 2018, 7:00pm ET
 Management of Palpable Abnormalities in the Breast Katerina Dodelzon, MD July 31, 2018, 7:00pm ET SAM Questions 1. 21 year old female presenting with left breast palpable mass, what is the most appropriate
Management of Palpable Abnormalities in the Breast Katerina Dodelzon, MD July 31, 2018, 7:00pm ET SAM Questions 1. 21 year old female presenting with left breast palpable mass, what is the most appropriate
Sonographic Detection and Sonographically Guided Biopsy of Breast Microcalcifications
 Sonographic Detection and Sonographically Guided Biopsy of Breast Microcalcifications Mary Scott Soo 1 Jay A. Baker Eric L. Rosen OBJECTIVE. The purpose of this study was to evaluate the ability of sonography
Sonographic Detection and Sonographically Guided Biopsy of Breast Microcalcifications Mary Scott Soo 1 Jay A. Baker Eric L. Rosen OBJECTIVE. The purpose of this study was to evaluate the ability of sonography
Ductal carcinoma in situ: ultrasound, mammography and MRI features with pathologic correlation
 Ductal carcinoma in situ: ultrasound, mammography and MRI features with pathologic correlation Poster No.: C-2252 Congress: ECR 2013 Type: Educational Exhibit Authors: L. Fernandes, H. A. M. R. Tinto,
Ductal carcinoma in situ: ultrasound, mammography and MRI features with pathologic correlation Poster No.: C-2252 Congress: ECR 2013 Type: Educational Exhibit Authors: L. Fernandes, H. A. M. R. Tinto,
Mammographic evaluation of palpable breast masses with pathological correlation: a tertiary care centre study in Nepal
 Original article 21 Mammographic evaluation of palpable breast masses with pathological correlation: a tertiary care centre study in Nepal G. Gurung, R. K. Ghimire, B. Lohani Department of Radiology and
Original article 21 Mammographic evaluation of palpable breast masses with pathological correlation: a tertiary care centre study in Nepal G. Gurung, R. K. Ghimire, B. Lohani Department of Radiology and
OPTO-ACOUSTIC BREAST IMAGING
 OPTO-ACOUSTIC BREAST IMAGING A Novel Fusion of Functional and Morphologic Imaging Reni S. Butler, MD A. Thomas Stavros, MD F. Lee Tucker, MD Michael J. Ulissey, MD PURPOSE 1. Explain opto-acoustic (OA)
OPTO-ACOUSTIC BREAST IMAGING A Novel Fusion of Functional and Morphologic Imaging Reni S. Butler, MD A. Thomas Stavros, MD F. Lee Tucker, MD Michael J. Ulissey, MD PURPOSE 1. Explain opto-acoustic (OA)
S. Murgo, MD. Chr St-Joseph, Mons Erasme Hospital, Brussels
 S. Murgo, MD Chr St-Joseph, Mons Erasme Hospital, Brussels? Introduction Mammography reports are sometimes ambiguous and indecisive. ACR has developped the BIRADS. BIRADS consists of a lexicon in order
S. Murgo, MD Chr St-Joseph, Mons Erasme Hospital, Brussels? Introduction Mammography reports are sometimes ambiguous and indecisive. ACR has developped the BIRADS. BIRADS consists of a lexicon in order
Assessment of extent of disease: digital breast tomosynthesis (DBT) versus full-field digital mammography (FFDM)
 Assessment of extent of disease: digital breast tomosynthesis (DBT) versus full-field digital mammography (FFDM) Poster No.: C-1237 Congress: ECR 2012 Type: Scientific Paper Authors: N. Seo 1, H. H. Kim
Assessment of extent of disease: digital breast tomosynthesis (DBT) versus full-field digital mammography (FFDM) Poster No.: C-1237 Congress: ECR 2012 Type: Scientific Paper Authors: N. Seo 1, H. H. Kim
Sonographic Appearance of Invasive Ductal Carcinoma of the Breast According to Histologic Grade
 Women s Imaging Original Research Blaichman et al. Efficacy of Sonographic Features in BI-RADS Lexicon Women s Imaging Original Research Jason Blaichman 1 James C. Marcus Tahra Alsaadi Mona El-Khoury Sarkis
Women s Imaging Original Research Blaichman et al. Efficacy of Sonographic Features in BI-RADS Lexicon Women s Imaging Original Research Jason Blaichman 1 James C. Marcus Tahra Alsaadi Mona El-Khoury Sarkis
THYROID NODULES: THE ROLE OF ULTRASOUND
 THYROID NODULES: THE ROLE OF ULTRASOUND NOVEMBER 2017 DR. DEAN DURANT DEFINITION Thyroid nodule: Focal area within the thyroid gland with echogenicity different from surrounding parenchyma. THYROID NODULES
THYROID NODULES: THE ROLE OF ULTRASOUND NOVEMBER 2017 DR. DEAN DURANT DEFINITION Thyroid nodule: Focal area within the thyroid gland with echogenicity different from surrounding parenchyma. THYROID NODULES
Dense Breasts, Get Educated
 Dense Breasts, Get Educated What are Dense Breasts? The normal appearances to breasts, both visually and on mammography, varies greatly. On mammography, one of the important ways breasts differ is breast
Dense Breasts, Get Educated What are Dense Breasts? The normal appearances to breasts, both visually and on mammography, varies greatly. On mammography, one of the important ways breasts differ is breast
Updates in Mammography. Dr. Yang Faridah A. Aziz Department of Biomedical Imaging University Malaya Medical Centre
 Updates in Mammography Dr. Yang Faridah A. Aziz Department of Biomedical Imaging University Malaya Medical Centre Updates in Mammography Breast Imaging Dr. Yang Faridah A. Aziz Department of Biomedical
Updates in Mammography Dr. Yang Faridah A. Aziz Department of Biomedical Imaging University Malaya Medical Centre Updates in Mammography Breast Imaging Dr. Yang Faridah A. Aziz Department of Biomedical
New Palpable Breast Lump With Recent Negative Mammogram: Is Repeat Mammography Necessary?
 Women s Imaging Original Research Leung et al. Repeat Mammogram for Breast Lump Found After Negative Mammogram Women s Imaging Original Research Stephanie E. Leung 1 Ilanit Ben-Nachum Anat Kornecki Leung
Women s Imaging Original Research Leung et al. Repeat Mammogram for Breast Lump Found After Negative Mammogram Women s Imaging Original Research Stephanie E. Leung 1 Ilanit Ben-Nachum Anat Kornecki Leung
Atypical Ductal Hyperplasia of the Breast:
 Atypical Ductal Hyperplasia of the Breast: Radiologic and Histopathologic Correlation 1 Ji Young Lee, M.D., Bo Kyoung Seo, M.D. 2, Jung Hyck Kim, M.D., Yu Whan Oh, M.D., Kyu Ran Cho, M.D., Eun Jeong Choi,
Atypical Ductal Hyperplasia of the Breast: Radiologic and Histopathologic Correlation 1 Ji Young Lee, M.D., Bo Kyoung Seo, M.D. 2, Jung Hyck Kim, M.D., Yu Whan Oh, M.D., Kyu Ran Cho, M.D., Eun Jeong Choi,
Practical and illustrated summary of updated BI-RADS for ultrasonography
 Practical and illustrated summary of updated I-RS for ultrasonography Jiyon Lee epartment of Radiology, NYU School of Medicine, NYU ancer Institute, reast Imaging enter, New York, NY, US The merican ollege
Practical and illustrated summary of updated I-RS for ultrasonography Jiyon Lee epartment of Radiology, NYU School of Medicine, NYU ancer Institute, reast Imaging enter, New York, NY, US The merican ollege
Short-Term Follow-Up of Palpable Breast Lesions With Benign Imaging Features: Evaluation of 375 Lesions in 320 Women
 Women s Imaging Original Research Follow-Up Imaging of Palpable Breast Lesions Women s Imaging Original Research WOMEN S IMAGING Jennifer A. Harvey 1 Brandi T. Nicholson 1 Alexander P. LoRusso 1,2 Michael
Women s Imaging Original Research Follow-Up Imaging of Palpable Breast Lesions Women s Imaging Original Research WOMEN S IMAGING Jennifer A. Harvey 1 Brandi T. Nicholson 1 Alexander P. LoRusso 1,2 Michael
Standard Breast Imaging Modalities. Lilian Wang, M.D. Breast Imaging Section Department of Radiology Northwestern Medicine
 Standard Breast Imaging Modalities Lilian Wang, M.D. Breast Imaging Section Department of Radiology Northwestern Medicine Overview Standard breast imaging modalities Mammography Ultrasound MRI Imaging
Standard Breast Imaging Modalities Lilian Wang, M.D. Breast Imaging Section Department of Radiology Northwestern Medicine Overview Standard breast imaging modalities Mammography Ultrasound MRI Imaging
Screening with New Modalities: Breast Ultrasound
 Screening with New Modalities: Breast Ultrasound Wendie A. Berg, MD, PhD Professor of Radiology Magee-Womens Hospital of UPMC University of Pittsburgh School of Medicine Disclosures No personal financial
Screening with New Modalities: Breast Ultrasound Wendie A. Berg, MD, PhD Professor of Radiology Magee-Womens Hospital of UPMC University of Pittsburgh School of Medicine Disclosures No personal financial
Invasive lobular carcinoma of the breast; spectrum of imaging findings.
 Invasive lobular carcinoma of the breast; spectrum of imaging findings. Poster No.: C-0847 Congress: ECR 2014 Type: Educational Exhibit Authors: D. Mandich, T. Diaz de Bustamante, L. Koren, M. Arroyo,
Invasive lobular carcinoma of the breast; spectrum of imaging findings. Poster No.: C-0847 Congress: ECR 2014 Type: Educational Exhibit Authors: D. Mandich, T. Diaz de Bustamante, L. Koren, M. Arroyo,
A-005 US DIAGNOSIS OF NONPALPABLE BREAST LESIONS
 A-005 US DIAGNOSIS OF NONPALPABLE BREAST LESIONS Hideaki Shirai M.D., M. Sakurai M.D., K. Yoshida M.D., N. Usuda M.D., H. Masuoka M.D., I. Shimokawara M.D, K. Asaishi M.D. Sapporo Kotoni Breast Clinic,
A-005 US DIAGNOSIS OF NONPALPABLE BREAST LESIONS Hideaki Shirai M.D., M. Sakurai M.D., K. Yoshida M.D., N. Usuda M.D., H. Masuoka M.D., I. Shimokawara M.D, K. Asaishi M.D. Sapporo Kotoni Breast Clinic,
Non-mass Enhancement on Breast MRI. Aditi A. Desai, MD Margaret Ann Mays, MD
 Non-mass Enhancement on Breast MRI Aditi A. Desai, MD Margaret Ann Mays, MD Breast MRI Important screening and diagnostic tool, given its high sensitivity for breast cancer detection Breast MRI - Indications
Non-mass Enhancement on Breast MRI Aditi A. Desai, MD Margaret Ann Mays, MD Breast MRI Important screening and diagnostic tool, given its high sensitivity for breast cancer detection Breast MRI - Indications
Breast Imaging Lexicon
 9//201 200 BI RADS th Edition 201 BI RADS th Edition Breast Imaging Lexicon Mammographic Pathology and Assessment Categories Deborah Thames, R.T.(R)(M)(QM) The Advanced Health Education Center Nonmember:
9//201 200 BI RADS th Edition 201 BI RADS th Edition Breast Imaging Lexicon Mammographic Pathology and Assessment Categories Deborah Thames, R.T.(R)(M)(QM) The Advanced Health Education Center Nonmember:
Non-Calcified Ductal Carcinoma in Situ: Ultrasound and Mammographic Findings Correlated with Histological Findings
 Yonsei Med J 49(1):103-110, 2008 DOI 10.3349/ymj.2008.49.1.103 Non-Calcified Ductal Carcinoma in Situ: Ultrasound and Mammographic Findings Correlated with Histological Findings Kyu Ran Cho, 1 Bo Kyoung
Yonsei Med J 49(1):103-110, 2008 DOI 10.3349/ymj.2008.49.1.103 Non-Calcified Ductal Carcinoma in Situ: Ultrasound and Mammographic Findings Correlated with Histological Findings Kyu Ran Cho, 1 Bo Kyoung
Armed Forces Institute of Pathology.
 Armed Forces Institute of Pathology www.radpath.com Armed Forces Institute of Pathology Breast Disease www.radpath.org Armed Forces Institute of Pathology Interpretation of Breast MRI Leonard M. Glassman
Armed Forces Institute of Pathology www.radpath.com Armed Forces Institute of Pathology Breast Disease www.radpath.org Armed Forces Institute of Pathology Interpretation of Breast MRI Leonard M. Glassman
Imaging-Guided Core Needle Biopsy of Papillary Lesions of the Breast
 Eric L. Rosen 1 Rex C. Bentley 2 Jay A. Baker 1 Mary Scott Soo 1 Received January 30, 2002; accepted after revision April 12, 2002. 1 Department of Radiology, Breast Imaging Division, Duke University Medical
Eric L. Rosen 1 Rex C. Bentley 2 Jay A. Baker 1 Mary Scott Soo 1 Received January 30, 2002; accepted after revision April 12, 2002. 1 Department of Radiology, Breast Imaging Division, Duke University Medical
BI-RADS and Breast MRI. Kathy Borovicka, M.D. Thursday February 15, 2018
 BI-RADS and Breast MRI Kathy Borovicka, M.D. Thursday February 15, 2018 Learning Objectives Be familiar with the Breast Imaging Reporting and Data System (BI-RADS) Understand the components of a breast
BI-RADS and Breast MRI Kathy Borovicka, M.D. Thursday February 15, 2018 Learning Objectives Be familiar with the Breast Imaging Reporting and Data System (BI-RADS) Understand the components of a breast
Evolution of diagnostic ultrasound systems Current achievements in breast ultrasound
 Evolution of diagnostic ultrasound systems Current achievements in breast ultrasound Dr. Ayumi Izumori, M. D. Department of Breast Surgery, Takamatsu Heiwa Hospital Tokushima Breast Care Clinic, Japan
Evolution of diagnostic ultrasound systems Current achievements in breast ultrasound Dr. Ayumi Izumori, M. D. Department of Breast Surgery, Takamatsu Heiwa Hospital Tokushima Breast Care Clinic, Japan
ORIGINAL INVESTIGATION. The Additional Diagnostic Value of Ultrasonography in the Diagnosis of Breast Cancer
 ORIGINAL INVESTIGATION The Additional Diagnostic Value of Ultrasonography in the Diagnosis of Breast Cancer Karin Flobbe, PhD; Anne Marie Bosch, MD; Alfons G. H. Kessels, MD, MSc; Geerard L. Beets, MD,
ORIGINAL INVESTIGATION The Additional Diagnostic Value of Ultrasonography in the Diagnosis of Breast Cancer Karin Flobbe, PhD; Anne Marie Bosch, MD; Alfons G. H. Kessels, MD, MSc; Geerard L. Beets, MD,
Interobserver Variability of Ultrasound Elastography: How It Affects the Diagnosis of Breast Lesions
 Women s Imaging Original Research Yoon et al. Elastography of Breast Lesions Women s Imaging Original Research Downloaded from www.ajronline.org by 46.3.21.182 on 1/24/18 from IP address 46.3.21.182. Copyright
Women s Imaging Original Research Yoon et al. Elastography of Breast Lesions Women s Imaging Original Research Downloaded from www.ajronline.org by 46.3.21.182 on 1/24/18 from IP address 46.3.21.182. Copyright
Breast Tomosynthesis. What is breast tomosynthesis?
 Scan for mobile link. Breast Tomosynthesis Breast tomosynthesis is an advanced form of mammography, a specific type of breast imaging that uses low-dose x-rays to detect cancer early when it is most treatable.
Scan for mobile link. Breast Tomosynthesis Breast tomosynthesis is an advanced form of mammography, a specific type of breast imaging that uses low-dose x-rays to detect cancer early when it is most treatable.
Breast-Specific Gamma Imaging for the Detection of Breast Cancer in Dense Versus Nondense Breasts
 Women s Imaging Original Research Rechtman et al. BSGI in Dense Versus Nondense Breasts Women s Imaging Original Research FOCUS ON: Lauren R. Rechtman 1 Megan J. Lenihan 1 Jennifer H. Lieberman 1 Christine
Women s Imaging Original Research Rechtman et al. BSGI in Dense Versus Nondense Breasts Women s Imaging Original Research FOCUS ON: Lauren R. Rechtman 1 Megan J. Lenihan 1 Jennifer H. Lieberman 1 Christine
Interpretation of automated breast ultrasound (ABUS) with and without knowledge of mammography: a reader performance study
 Original Article Interpretation of automated breast ultrasound (ABUS) with and without knowledge of mammography: a reader performance study Acta Radiologica 2015, Vol. 56(4) 404 412! The Foundation Acta
Original Article Interpretation of automated breast ultrasound (ABUS) with and without knowledge of mammography: a reader performance study Acta Radiologica 2015, Vol. 56(4) 404 412! The Foundation Acta
Intracystic papillary carcinoma of the breast
 Intracystic papillary carcinoma of the breast Poster No.: C-1932 Congress: ECR 2011 Type: Educational Exhibit Authors: V. Dimarelos, F. TZIKOS, N. Kotziamani, G. Rodokalakis, 1 2 3 1 1 1 2 T. MALKOTSI
Intracystic papillary carcinoma of the breast Poster No.: C-1932 Congress: ECR 2011 Type: Educational Exhibit Authors: V. Dimarelos, F. TZIKOS, N. Kotziamani, G. Rodokalakis, 1 2 3 1 1 1 2 T. MALKOTSI
Criteria of Malignancy. Evaluation Score
 30 5 Diagnostic Criteria Criteria of Malignancy Table 5.2 lists criteria in contrast-enhancing MR mammography that strongly indicate the presence of malignancy or are unspecific. Unifactorial evaluation
30 5 Diagnostic Criteria Criteria of Malignancy Table 5.2 lists criteria in contrast-enhancing MR mammography that strongly indicate the presence of malignancy or are unspecific. Unifactorial evaluation
Cystic Hypersecretory Carcinoma of the Breast:
 J Korean Soc Radiol 2010;62:287-294 Cystic Hypersecretory Carcinoma of the Breast: Sonographic Features with a Histological Correlation 1 Sang Yu Nam, M.D., Boo-Kyung Han, M.D., Jung Hee Shin, M.D., Eun
J Korean Soc Radiol 2010;62:287-294 Cystic Hypersecretory Carcinoma of the Breast: Sonographic Features with a Histological Correlation 1 Sang Yu Nam, M.D., Boo-Kyung Han, M.D., Jung Hee Shin, M.D., Eun
Bilateral breast cancer: the role of mammography and ultrasonography in early detection
 Original article Bilateral breast cancer: the role of mammography and ultrasonography in early detection Onthira Lekamnuaypon, M.D., 1 Pailin Kongmebhol, M.D., 1 Malai Muttarak, M.D. 1 Neelaya Sukhamwang,
Original article Bilateral breast cancer: the role of mammography and ultrasonography in early detection Onthira Lekamnuaypon, M.D., 1 Pailin Kongmebhol, M.D., 1 Malai Muttarak, M.D. 1 Neelaya Sukhamwang,
Financial Disclosures
 Financial Disclosures 3D Mammography: The Latest Developments in the Breast Imaging Arena I have no financial disclosures Dr. Katharine Lampen-Sachar Breast and Body Radiologist Radiology Associates of
Financial Disclosures 3D Mammography: The Latest Developments in the Breast Imaging Arena I have no financial disclosures Dr. Katharine Lampen-Sachar Breast and Body Radiologist Radiology Associates of
ORIGINAL ARTICLE. *Author affiliations appear at the end of this article.
 Interobserver agreement in breast ultrasound categorization in the Mammography and Ultrasonography Study for Breast Cancer Screening Effectiveness (MUST-BE) trial: results of a preliminary study Eun Jung
Interobserver agreement in breast ultrasound categorization in the Mammography and Ultrasonography Study for Breast Cancer Screening Effectiveness (MUST-BE) trial: results of a preliminary study Eun Jung
Emerging Techniques in Breast Imaging: Contrast-Enhanced Mammography and Fast MRI
 Emerging Techniques in Breast Imaging: Contrast-Enhanced Mammography and Fast MRI Lilian Wang, M.D. Breast Imaging Section Department of Radiology Northwestern Medicine Overview Rationale for new imaging
Emerging Techniques in Breast Imaging: Contrast-Enhanced Mammography and Fast MRI Lilian Wang, M.D. Breast Imaging Section Department of Radiology Northwestern Medicine Overview Rationale for new imaging
Athina Vourtsis & Aspasia Kachulis
 The performance of 3D ABUS versus HHUS in the visualisation and BI-RADS characterisation of breast lesions in a large cohort of 1,886 women Athina Vourtsis & Aspasia Kachulis European Radiology ISSN 0938-7994
The performance of 3D ABUS versus HHUS in the visualisation and BI-RADS characterisation of breast lesions in a large cohort of 1,886 women Athina Vourtsis & Aspasia Kachulis European Radiology ISSN 0938-7994
Thyroid Nodules: US Risk Stratification. Alex Tessnow, MD, FACE, ECNU University of Texas Southwestern Associate Professor of Medicine Dallas, Texas
 Thyroid Nodules: US Risk Stratification Alex Tessnow, MD, FACE, ECNU University of Texas Southwestern Associate Professor of Medicine Dallas, Texas Which of the following is true? A. All echogenic foci
Thyroid Nodules: US Risk Stratification Alex Tessnow, MD, FACE, ECNU University of Texas Southwestern Associate Professor of Medicine Dallas, Texas Which of the following is true? A. All echogenic foci
Breast imaging in general practice
 Breast series CLINICAL PRACTICE Breast imaging in general practice Nehmat Houssami, MBBS, FAFPHM, FASBP, PhD, is Associate Clinical Director, NSW Breast Cancer Institute, Westmead Hospital, Honorary Senior
Breast series CLINICAL PRACTICE Breast imaging in general practice Nehmat Houssami, MBBS, FAFPHM, FASBP, PhD, is Associate Clinical Director, NSW Breast Cancer Institute, Westmead Hospital, Honorary Senior
UW Radiology Review Course Breast Calcifications. BI-RADS 5 th Edition
 UW Radiology Review Course Breast Calcifications Grace Kalish, MD Vantage Radiology BI-RADS 5 th Edition Benign Skin Vascular Large rod like Coarse popcorn Suspicious Amorphous Coarse heterogenous Fine
UW Radiology Review Course Breast Calcifications Grace Kalish, MD Vantage Radiology BI-RADS 5 th Edition Benign Skin Vascular Large rod like Coarse popcorn Suspicious Amorphous Coarse heterogenous Fine
