Management of Ductal Carcinoma In Situ
|
|
|
- Avice Harvey
- 5 years ago
- Views:
Transcription
1 Management of Ductal Carcinoma In Situ Stella Hetelekidis, MD Stuart J. Schnitt, MD Monica Morrow, MD Jay R. Harris, MD Introduction Ductal carcinoma in situ (DCIS), also known as intraductal carcinoma, is a proliferation of presumably malignant epithelial cells within the mammary ductal system. Because there is no light-microscopic evidence of invasion through the basement membrane into the surrounding tissue, DCIS is best viewed as a preinvasive lesion. The increased use of screening mammography over the past two decades has led to a marked increase in the number of patients diagnosed with DCIS, and today, in many centers, one DCIS lesion is diagnosed for every two to three mammographically detected invasive breast cancers. Although patients with DCIS have been traditionally treated with mastectomy, this treatment approach has recently Dr. Hetelekidis is a Radiation Oncologist at the Joint Center for Radiation Therapy and the Brigham and Women s Hospital and Clinical Instructor at Harvard Medical School in Boston, Massachusetts. Dr. Schnitt is the Associate Director of Surgical Pathology at the Beth Israel Hospital and Associate Professor of Pathology at Harvard Medical School in Boston, Massachusetts. Dr. Morrow is the Director of the Lynn Sage Comprehensive Breast Center and Associate Professor of Surgery in the Department of Surgery of Northwestern University Medical School in Chicago, Illinois. Dr. Harris is the Clinical and Educational Director at the Joint Center for Radiation Therapy and Professor of Radiation Oncology at Harvard Medical School in Boston, Massachusetts. come under scrutiny for several reasons. First, many patients with invasive breast cancer are currently treated with breastconserving therapy, making it difficult to justify the generalized use of mastectomy for patients with DCIS. In addition, the natural history of DCIS is only partially understood, particularly for small, mammographically detected lesions. In this article, we will review current concepts regarding the diagnosis, natural history, and treatment of DCIS. Presentation Prior to the era of mammographic screening, patients with DCIS most often presented with a palpable breast mass or with nipple discharge. Technical improvements in mammography and the widespread use of screening mammography have led to the increased detection of smaller, clinically occult DCIS lesions. Mammographically, DCIS usually appears as clustered microcalcifications without a soft tissue abnormality, although these findings are not specific for DCIS and may be seen with benign lesions as well as with invasive cancers. In fact, most calcifications are indeterminate mammographically, resulting in biopsy yields of only 20 to 25 percent. The microcalcifications in DCIS are most often secondary to the calcification of necrotic cellular debris within the involved ducts, and their extent and characteristics are better defined with magnification views. Suspicious mammographic 244 Ca A cancer Journal for Clinicians
2 microcalcifications are generally differentiated from benign calcium deposits by their number, distribution, and appearance. Coarse granular or linear calcifications or clusters of variably-shaped calcifications are regarded as most suspicious (Figs. 1 and 2). DCIS can also occasionally be an incidental finding in breast tissue removed for an unrelated abnormality, such as fibroadenoma. Finally, some patients with DCIS present with Paget s disease of the nipple-areolar complex. Pathology DCIS is comprised of a heterogeneous group of histopathologic lesions that have been classified into several subtypes based primarily on architectural pattern. The most frequent subtypes are comedo, cribriform, papillary, micropapillary, and solid (Figs. 3 and 4). Any given DCIS lesion may consist of one or more of these subtypes. Comedo-type DCIS consists of cells that are cytologically malignant, showing pleomorphism and high-grade nuclei. Central areas of necrosis are present in the involved spaces. These lesions have a high proliferative rate, and they often show aneuploidy, overexpression of the HER2/NEU (c-erbb-2) oncogene, accumulation of p53 tumor suppressor gene protein product, and angiogenesis in the surrounding stroma. 1-5 Using standard two-view mammography, there is a high correlation between the histologic extent of the lesion and the extent of the calcifications on mammogram. 6 Some investigators group the remaining subtypes of DCIS together as non-comedo lesions, based on the perception that these other types are often composed of cytologically bland cells with low-grade nuclei and a low proliferative rate. In fact, this dichotomous classification system is an oversimplification. Some DCIS lesions with low-grade nuclei may show necrosis, while others with cribriform, micropapillary, papillary, or solid architectural patterns may be composed of cytologically malignant cells with high-grade nuclei. In addition, some DCIS lesions have nuclei that are of intermediate grade. To overcome the limitations of traditional pathologic classification systems, which are based on architectural pattern, a number of alternative classification schemes have recently been proposed that emphasize nuclear grade as the most important histopathologic factor. 7-9 Estrogen- and progesterone-receptor proteins are seen in some cases of DCIS, more frequently in non-comedo types. 10 However, their importance in the management of patients with DCIS has not been established. In most cases, the diagnosis of DCIS is straightforward. However, in some cases, diagnostic problems do occur. At one end of the spectrum, it may be difficult to distinguish examples of low-grade DCIS from atypical ductal hyperplasia. At the other end, the distinction between pure DCIS and DCIS with microinvasion or even frankly invasive cancer may be problematic. Finally, the distinction between DCIS and lobular carcinoma in situ (LCIS) is sometimes difficult. The distribution of DCIS in the breast is of considerable interest. Several prior studies suggested that DCIS is frequently a multicentric disease. However, recent studies using more meticulous pathologic/mammographic correlative technique have shown that these additional foci are almost always present in relation to the index lesion (multifocal spread) and that true multicentricity is uncommon. 6 Most cases of DCIS show a segmental pattern of involvement in the breast. These observations have implications for the management of patients with DCIS and indicate that breast-preserving procedures may be feasible in many patients. About one percent of all patients with the diagnosis of DCIS are found to Vol. 45 No. 4 July/august
3 M a n a g e m e n t o f D u c t a l C a r c i n o m a i n s i t u have axillary lymph node involvement, a potential consequence of undetected stromal invasion. The frequencies of both microinvasion and axillary lymph node involvement are related to the extent of the DCIS lesion. Lagios 11 reviewed 111 cases of DCIS treated with mastectomy and found no evidence of occult invasion when the extent of DCIS was less than 2.5 cm, whereas 12 of 25 lesions (48 percent) larger than 5.5 cm were found to have microinvasion. Two instances of lymph node involvement occurred in association with microinvasion. Silverstein et al 12 have recently reviewed their experience with axillary dissection in 189 patients with DCIS, and no cases of lymph node involvement were found. Fig. 1. Craniocaudal-view mammogram shows numerous pleomorphic microcalcifications, many of which are arrayed along the course of ducts. The calcifications are varied in size and shape, but are predominantly rounded. Malignant Potential A critical but as yet unresolved issue concerning DCIS is its potential to progress to invasive breast cancer. Because DCIS was historically treated with mastectomy, little information on the risk of progression to invasive disease is available. In particular, the natural history of the Fig. 2. (A) Craniocaudal-view mammogram shows a focus of microcalcifications in the lateral aspect of the breast. (B) Magnification view better defines the extent of the microcalcifications and more clearly shows their linear characteristics. (C) Specimen mammogram shows removal of the microcalcifications seen in 2A and 2B. 246 Ca A cancer Journal for Clinicians
4 small, mammographically detected lesions seen with increasing frequency today is largely unknown. There have been three studies in which retrospective reviews of benign breast biopsies have identified small numbers of patients with DCIS who received no treatment beyond diagnostic biopsy Page et al 13 found progression to invasive disease in seven (28 percent) of 25 patients at intervals from three to 10 years (mean, 6.1 years). Rosen et al 14 noted progression in eight of 15 patients; however, an additional 15 patients had been lost to follow-up. Eusebi et al 15 noted that two of 28 patients with DCIS developed ipsilateral invasive breast carcinoma (mean follow-up, 16.7 years). In addition, Alpers and Wellings 16 reported that of 44 patients with invasive carcinoma of the breast undergoing bilateral mastectomy, 21 (48 percent) were found to have DCIS of the contralateral breast. This is in contrast to the rate of development of contralateral invasive breast cancer, which is about 10 to 15 percent over 20 years. Therefore, it appears that some, but not all, DCIS lesions will progress to invasive carcinoma. Options for Treatment The treatment of patients with DCIS with mastectomy is associated with cure rates approaching 100 percent However, mastectomy has been viewed by some clinicians as a prophylactic treatment because it is used to prevent the development of an invasive breast cancer. With the increasing use of breast-conserving treatment for patients with invasive breast carcinoma, the routine use of mastectomy for patients with DCIS has been questioned, particularly for small, lowgrade lesions. Several investigators have examined the results of breast-conserving treatment of DCIS using surgical resection alone (Table 1). 2,7,20-24 Lagios et al 7 reported the results in 79 women with DCIS measuring 25 mm or less (mean size, 6.8 mm) treated with wide excision alone. With a mean of 124 months of follow-up, 13 local recurrences (16 percent) have been noted (personal communication, March 1995). Six of these recurrences were invasive carcinomas, and seven were DCIS. The recurrence rate was 33 percent (12/36) in patients with high-grade DCIS containing comedo-type necrosis versus two percent (1/43) in patients with intermediate- or low-grade DCIS. Schwartz et al 20 similarly examined the treatment results for 70 patients with DCIS lesions measuring 2.5 cm or less. All patients underwent re-excision of the surgical bed, achieving negative margins of resection. Eleven patients (15 percent) experienced local recurrence (mean follow-up, 49 months). Here, too, the risk of local recurrence varied greatly with histologic subtype: 12 (32 percent) of 38 patients with comedo histology experienced local recurrence while only one (three percent) of 32 patients with non-comedo histology had a recurrence. In both of these series, careful histopathologic and mammographic techniques were used to assess the adequacy of the resection. Other investigators have reported on the use of excision and radiation therapy for DCIS (Table 2) ,25-29 Hiramatsu et al 25 recently reviewed the outcome of 76 patients treated with excision and radiation therapy (median follow-up, 74 months). The five- and 10-year local recurrence rates were four percent and 15 percent, respectively. Four of the seven recurrences were invasive, and three were DCIS. Solin et al 26 reported the results of 172 patients treated at multiple institutions. With a mean follow-up period of 84 months, 16 recurrences (nine percent) were found, and almost half of these were invasive. The presence of comedo-type DCIS plus nuclear grade 3 was a significant predictor for local recurrence, but not for overall survival. The median time to recurrence was 62 months, with a Vol. 45 No. 4 July/august
5 M a n a g e m e n t o f D u c t a l C a r c i n o m a i n s i t u A Fig. 3. Cribriform-type (low-grade) ductal carcinoma in situ. (A) Low-power photomicrograph demonstrates several spaces involved with a fenestrated proliferation of ductal carcinoma in situ cells. Rare psammoma-type calcifications are present (arrows). (B) High-power view demonstrates cytologic detail. The intraductal carcinoma cell nuclei are small and relatively uniform in appearance. There is no evidence of mitotic activity. A psammoma-type calcification is present in the center of the field. B A B Fig. 4. Comedo-type (high-grade) ductal carcinoma in situ. (A) Low-power photomicrograph of an involved space shows in situ carcinoma cells at the periphery and large central area of necrosis (N) which is focally calcified (arrow). (B) High-power view shows cytologically malignant cells with nuclear pleomorphism and variably prominent nucleoli. A mitotic figure is evident (arrow). range of 19 to 119 months. Silverstein et al 30 initially found that among patients treated with excision and radiation therapy, a higher local recurrence rate was observed for patients with the comedo subtype (11 percent) compared with the non-comedo subtypes (two percent) (median follow-up, 45 months). However, an update of this study revealed that this difference was no 248 Ca A cancer Journal for Clinicians
6 longer apparent with longer follow-up. 21 Others have also found no effect of the histologic subtype alone on the recurrence rates after irradiation. 26 Two studies from the National Surgical Adjuvant Breast and Bowel Project (NSABP) have been reported on treatment outcome in patients with DCIS. Protocol B-06 was a prospective, randomized study designed to examine the outcome in patients with invasive breast carcinoma treated with mastectomy, lumpectomy alone, or lumpectomy and irradiation. 31 Upon retrospective review of pathologic materials, 78 patients were found to have had DCIS alone. 32 Only one of these patients presented with a mammographically detected lesion, and the mean size for the 71 lesions in which pathologic dimensions were available was 2.2±1.3 cm. Updated results on 76 patients are available. 22 With a follow-up of 83 months, two (seven percent) of 27 patients treated with irradiation experienced local recurrence, while none of the 28 patients treated with mastectomy recurred locally (one patient died of metastatic disease without a local recurrence). In contrast, nine (43 percent) of the 21 patients treated with lumpectomy alone had local failures. Although analysis was limited by the small number of patients, no difference in overall survival was observed among the three groups. The results of the first prospective, randomized study examining the role of radiation therapy in breast-conserving treatment of DCIS were recently reported by the NSABP (Protocol B-17). 23 In this study, 818 women with DCIS were randomly assigned to either lumpectomy alone or lumpectomy followed by breast irradiation. Histologically negative surgical margins were a study requirement. With a median follow-up of 43 months, event-free survival was found to be higher in women treated with breast irradiation (84 percent versus 74 percent), and this was primarily due to fewer ipsilateral breast recurrences developing in the irradiated group. Sixty-four ipsilateral breast recurrences (16 percent) occurred in the group treated with lumpectomy alone, while 28 (seven percent) developed in the patients treated with lumpectomy and irradiation. The greatest reduction was seen in the subsequent development of ipsilateral invasive carcinoma. The fiveyear cumulative incidence of invasive breast cancers was 10.5 percent with lumpectomy alone, compared with 2.9 percent with the addition of radiation therapy. The reduction in the recurrence of DCIS was also statistically significant, but not as striking, with a cumulative incidence of 10.4 percent at five years with lumpectomy alone and 7.5 percent with lumpectomy and irradiation. Most of the recurrences were seen at or near the primary site. Other events, such as the development of contralateral breast cancer, were similar in the two groups. A recent analysis of the significance of pathologic findings of the NSABP B- 17 protocol showed the only statistically significant independent predictors for ipsilateral breast recurrence to be the presence of comedo-type necrosis and involved/uncertain margins. 33 Although the addition of radiation therapy reduced the risk of recurrence in all subgroups, the difference was greatest in those patients whose DCIS lesions showed moderate to marked comedo necrosis. Nonetheless, several questions remain unanswered from this single, randomized study. Accurate determination of the extent of DCIS lesions is often difficult, and the sizes of the lesions from Protocol B-17 were not systematically recorded in all patients. Another limitation is the relatively short follow-up period (mean, 43 months). Increasing recurrence rates are observed with follow-up beyond five years. 21,25 Whether the rates of local recurrence for the two groups will continue to diverge over time remains to be seen. The most recent NSABP study investigated the potential role of tamoxifen in patients with DCIS treated with exci- Vol. 45 No. 4 July/august
7 M a n a g e m e n t o f D u c t a l C a r c i n o m a i n s i t u Table 1 Studies of Ductal Carcinoma In Situ Treated with Wide Excision Alone Mean Number of Follow-up Recurrence Invasive Reference Patients (months) No. (percent) (percent) Arnesson et al (13) 40 Carpenter et al (18) 20 Lagios et al (16) 46 Schwartz et al (15) 27 Silverstein et al (8) 50 Fisher et al 22 (B-06) (43) 56 Fisher et al 23 (B-17) (16) 50 sion and breast irradiation (Protocol B- 24). In an attempt to further reduce the local recurrence rate and possibly decrease the rate of contralateral breast cancer development, patients were randomized to treatment for five years with tamoxifen or with placebo. This study had no specific limits on the size of the intraductal lesion, and negative resection margins were not mandatory for entry. Additionally, postsurgical mammograms were not required, and women with additional areas of microcalcifications were not excluded. A number of European trials are also investigating the roles of radiation therapy and tamoxifen in combination with limited surgery. Approach to Management Given the heterogeneous nature of these lesions, the uncertainty about natural history, and the paucity of long-term results with breast-conserving therapy, the treatment of DCIS has become one of the most controversial areas in the field of breast disease. Some clinicians believe mastectomy should be offered to all patients with DCIS because of its high degree of effectiveness. Other clinicians believe the small, mammographically detected tumors commonly diagnosed today do not require mastectomy given the uncertain risk of progression and the effectiveness of breast-conserving therapy. The NSABP B-17 results suggest that many patients with DCIS may be treated with excision and irradiation, but it is unclear, at present, how this treatment compares to mastectomy. In addition, it is likely that some patients with DCIS may be treated by excision alone, but it is unclear how to best identify them. In the absence of prospective, randomized trials comparing mastectomy and breast-conserving treatment, several outcomes of treatment should be considered in assessing the available data. These outcomes include the risk of recurrence, the risk of invasive breast cancer, the risk of dying of breast cancer, and the psychologic and physical implications of mastectomy. Current data on breast-conserving treatment with radiation therapy 250 Ca A cancer Journal for Clinicians
8 Table 2 Studies of Ductal Carcinoma In Situ Treated with Excision and Radiation Therapy Mean Number of Follow-up Recurrence Invasive Reference Patients (months) No. (percent) (percent) Hiramatsu et al (9) 57 McCormick et al (18) 30 Ray et al (9) 20 Silverstein et al (10) 50 Solin et al (9) 44 Stotter et al (9) 100 Fisher et al 22 (B-06) (7) 50 Fisher et al 23 (B-17) (7) 40 show recurrence rates of 10 to 15 percent at 10 years. Because about half of these recurrences are invasive, the risk of invasive breast cancer is about five to seven percent. Assuming that with close follow-up after treatment of DCIS, these invasive lesions would be detected early, then the risk of ultimately dying of breast cancer can be estimated to be about two to three percent. This compares with a risk of about one to two percent after mastectomy. If we consider that women with LCIS, who develop invasive breast cancer at a rate of about one percent per year (or 10 percent at 10 years), are typically managed with observation alone, then breast-conserving therapy for patients with DCIS seems a reasonable option. Is there a subset of patients that can be treated with excision alone? Retrospective data indicate that patients with small DCIS lesions, particularly of the non-comedo subtypes, may be adequately treated with lumpectomy alone if attention is given to the histologic resection margins and there is verification of complete tumor removal by postoperative mammogram. The only results available from a prospective study at this time are those from the NSABP Protocol B Additional prospective studies looking at excision alone for selected patients with DCIS are still needed. Treatment Recommendations Most patients with DCIS have nonpalpable, mammographically detected lesions, and careful mammographic and pathologic evaluation is necessary for formulating treatment recommendations. Patients who are found to have suspicious calcifications on screening mammography should have magnification views performed to clearly define the full extent of the calcifications. Needle localization should be used to guide the biopsy, and if the calcifications are extensive, bracketing wires are often used to aid in complete excision. Specimen mammography and postexcision mammograms are useful to confirm the removal of all suspicious calcifications. On pathologic evaluation, the speci- Vol. 45 No. 4 July/august
9 M a n a g e m e n t o f D u c t a l C a r c i n o m a i n s i t u men should be carefully oriented and inked, with particular attention given to the nuclear grade, the architectural subtype, the correlation of microcalcifications with DCIS, the extent of disease, and the distance between the DCIS and the resection margins. Evidence of microinvasion should be noted. It is recommended that biopsy tissue without a discernible mass not be sent for biochemical analysis of estrogen-receptor proteins as small areas of invasion may be inadvertently missed. Once DCIS is diagnosed, treatment options should be discussed with the patient, considering the various outcomes and risks described above. Breast-conserving treatment should require removal of all microcalcifications (as seen on specimen mammography or magnification views) and negative microscopic margins of resection; re-excision is often necessary to achieve this. If a patient wishes to have breast-conserving therapy and is an appropriate candidate, entry onto a protocol should be encouraged. Not every patient with DCIS who desires breast-conserving treatment will be an appropriate candidate. In general, simple mastectomy is recommended for women in whom the DCIS is too extensive to be adequately removed. This in turn may be determined not only by the extent of the disease, but also by the size of the breast, the histopathology (e.g., margins), and the cosmetic result that is acceptable to each patient. Axillary dissection is not routinely performed; however, a limited dissection is commonly performed in patients with extensive lesions, particularly if these are high-grade. In patients treated with mastectomy, reconstruction using tissue flaps or implants is done based on each patient s desires. Hormonal therapy for DCIS is currently not indicated except on study protocols. Future Studies Additional information is needed from clinical trials and laboratory studies to improve the management of patients with DCIS. The results of the NSABP B-24 trial and others will provide important information about the utility of tamoxifen. The optimal histologic classification of DCIS is still in evolution, and further work is needed in correlating histology with clinical outcome. Whether new classification systems that emphasize nuclear grade of DCIS will be of prognostic significance and aid in the selection of patients for various treatments remains to be seen. Research is needed to identify factors associated with the development of invasive disease. Work is currently under way examining genetic changes, angiogenesis, and cellular growth factors as prognostic markers. 4,5,34,35 Finally, long-term results from clinical trials are needed to provide patients more accurate estimates of outcome based on treatment choice. CA References 1. Meyer JS: Cell kinetics of histologic variants of in situ breast carcinoma. Breast Cancer Res Treat 1986;7: Carpenter R, Boulter PS, Cooke T, Gibbs NM: Management of screen detected ductal carcinoma in situ of the female breast. Br J Surg 1989;76: van de Vijver MJ, Peterse JL, Mooi WJ, et al: Neu-protein overexpression in breast cancer: Association with comedo-type ductal carcinoma in situ and limited prognostic value in stage II breast cancer. N Engl J Med 1988;319: Poller DN, Roberts EC, Bell JA, et al: p53 protein expression in mammary ductal carcinoma in situ: Relationship to immunohistochemical expression of estrogen receptor and c-erbb-2 protein. Hum Pathol 1993;24: Guidi AJ, Fischer L, Harris JR, Schnitt SJ: Microvessel density and distribution in ductal carcinoma in situ of the breast. J Natl Cancer Inst 1994; 86: Holland R, Hendriks JH, Vebeek AL, et al: Extent, distribution, and mammographic/histological correlations of breast ductal carcinoma in situ. Lancet 1990;335: Ca A cancer Journal for Clinicians
10 7. Lagios MD, Margolin FR, Westdahl PR, Rose MR: Mammographically detected duct carcinoma in situ: Frequency of local recurrence following tylectomy and prognostic effect of nuclear grade on local recurrence. Cancer 1989;63: Holland R, Peterse JL, Millis RR, et al: Ductal carcinoma in situ: A proposal for a new classification. Semin Diagn Pathol 1994;11: Poller DN, Silverstein MJ, Galea M, et al: Ductal carcinoma in situ of the breast: A proposal for a new simplified histological classification association between cellular proliferation and c-erbb-2 protein expression. Mod Pathol 1994;7: Bur ME, Zimarowski MJ, Schnitt SJ, et al: Estrogen receptor immunohistochemistry in carcinoma in situ of the breast. Cancer 1992;69: Lagios MD: Ductal carcinoma in situ: Pathology and treatment. Surg Clin North Am 1990;70: Silverstein MJ, Gierson ED, Waisman JR, et al: Axillary lymph node dissection for T1a breast carcinoma: Is it indicated. Cancer 1994;73: Page DL, Dupont WD, Rogers LW, Landenberger M: Intraductal carcinoma of the breast: Follow-up after biopsy only. Cancer 1982;49: Rosen PP, Braun DW Jr, Kinne DE: The clinical significance of preinvasive breast carcinoma. Cancer 1980;46(suppl 4): Eusebi V, Foschini MP, Cook MG, et al: Longterm follow-up of in situ carcinoma of the breast with special emphasis on clinging carcinoma. Semin Diagn Pathol 1989;6: Alpers CE, Wellings SR: The prevalence of carcinoma in situ in normal and cancer-associated breasts. Hum Pathol 1985;16: Ashikari R, Huvos AG, Snyder RE: Prospective study of non-infiltrating carcinoma of the breast. Cancer 1977;39: Sunshine JA, Moseley HS, Fletcher WS, Krippaehe WW: Breast carcinoma in situ: A retrospective review of 112 cases with a minimum 10 year follow-up. Am J Surg 1985;150: Farrow JH: Current concepts in the detection and treatment of the earliest of the early breast cancers. Cancer 1970;25: Schwartz GF, Finkel GC, Garcia JC, Patchefsky AS: Subclinical ductal carcinoma in situ of the breast: Treatment by local excision and surveillance alone. Cancer 1992;70: Silverstein MJ, Cohlan BF, Gierson ED, et al: Duct carcinoma in situ: 227 cases without microinvasion. Eur J Cancer 1992;28: Fisher ER, Leeming R, Anderson S, et al: Conservative management of intraductal carcinoma (DCIS) of the breast. J Surg Oncol 1991;47: Fisher B, Costantino J, Redmond C, et al: Lumpectomy compared with lumpectomy and radiation therapy for the treatment of intraductal breast cancer. N Engl J Med 1993;328: Arnesson LG, Smeds S, Fagerberg G, Grontolt O: Follow-up of two treatment modalities for ductal cancer in situ of the breast. Br J Surg 1989;76: Hiramatsu H, Bornstein BA, Recht A, et al: Outcome and risk factors for local failure after conservative surgery and radiotherapy for ductal carcinoma in situ, The Cancer Journal from Scientific American in press. 26. Solin LJ, Yeh IT, Kurtz J, et al: Ductal carcinoma in situ (intraductal carcinoma) of the breast treated with breast-conserving surgery and definitive irradiation. Cancer 1993;71: McCormick B, Rosen P, Kinne D, et al: Duct carcinoma in situ of the breast: An analysis of local control after conservation surgery and radiotherapy. Int J Radiat Oncol Biol Phys 1991;21: Ray GR, Adelson J, Hayhurst E, et al: Ductal carcinoma in situ of the breast: Results of treatment by conservative surgery and definitive irradiation. Int J Radiat Oncol Biol Phys 1994;28: Stotter AT, McNeese M, Oswald MJ, et al: The role of limited surgery with irradiation in primary treatment of ductal in situ breast cancer. Int J Radiat Oncol Biol Phys 1990;18: Silverstein MJ, Waisman JR, Gamagami P, et al: Intraductal carcinoma of the breast (208 cases): Clinical factors influencing treatment choice. Cancer 1990;66: Fisher B, Redmond C, Poisson R, et al: Eightyear results of a randomized clinical trial comparing total mastectomy and lumpectomy with or without irradiation in the treatment of breast cancer. N Engl J Med 1989;320: Fisher ER, Sass R, Fisher B, et al: Pathologic findings from the National Surgical Adjuvant Breast Project (Protocol 6): I. Intraductal carcinoma (DCIS). Cancer 1986;57: Fisher ER, Costantino J, Fisher B, et al: Pathologic findings from the National Surgical Adjuvant Breast Project (NSABP) Protocol B-17: Intraductal carcinoma. Cancer 1995;75: Simpson JF, O Malley F, Dupont WD, Page DL: Heterogeneous expression of nm23 gene product in noninvasive breast carcinoma. Cancer 1994;73: Normanno N, Giordino T, Smith K, et al: Expression of amphiregulin, cripto-1 and heregulin alpha in primary human breast carcinomas. Proc Annu Meet Am Assoc Cancer Res 1994;35:A76. Abstract. Vol. 45 No. 4 July/august
Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction
 Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction Aldona J. Spiegel, M.D., and Charles E. Butler, M.D. Houston, Texas Skin-sparing
Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction Aldona J. Spiegel, M.D., and Charles E. Butler, M.D. Houston, Texas Skin-sparing
ANATOMIC PATHOLOGY. Original Article
 ANATOMIC PATHOLOGY Original Article Intraductal Carcinoma Associated With Invasive Carcinoma of the Breast A Comparison of the Two Lesions With Implications for Intraductal Carcinoma Classification Systems
ANATOMIC PATHOLOGY Original Article Intraductal Carcinoma Associated With Invasive Carcinoma of the Breast A Comparison of the Two Lesions With Implications for Intraductal Carcinoma Classification Systems
Ductal carcinoma in situ
 Breast series CLINICAL PRACTICE Ductal carcinoma in situ Management update Kirsty Stuart, BSc (Med), MBBS, FRANZCR, is a radiation oncologist, NSW Breast Cancer Institute, Westmead Hospital, New South
Breast series CLINICAL PRACTICE Ductal carcinoma in situ Management update Kirsty Stuart, BSc (Med), MBBS, FRANZCR, is a radiation oncologist, NSW Breast Cancer Institute, Westmead Hospital, New South
Radiation and DCIS. The 16 th Annual Conference on A Multidisciplinary Approach to Comprehensive Breast Care and Imaging
 Radiation and DCIS The 16 th Annual Conference on A Multidisciplinary Approach to Comprehensive Breast Care and Imaging Einsley-Marie Janowski, MD, PhD Assistant Professor Department of Radiation Oncology
Radiation and DCIS The 16 th Annual Conference on A Multidisciplinary Approach to Comprehensive Breast Care and Imaging Einsley-Marie Janowski, MD, PhD Assistant Professor Department of Radiation Oncology
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer. Saima Saeed MD
 Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
In Situ Breast Carcinoma. James L. Connolly, M.D Beth Israel Deaconess Medical Center Professor of Pathology Harvard Medical School Boston, MA
 In Situ Breast Carcinoma James L. Connolly, M.D Beth Israel Deaconess Medical Center Professor of Pathology Harvard Medical School Boston, MA Content In Situ Ductal Carcinoma In Situ Lobular Carcinoma
In Situ Breast Carcinoma James L. Connolly, M.D Beth Israel Deaconess Medical Center Professor of Pathology Harvard Medical School Boston, MA Content In Situ Ductal Carcinoma In Situ Lobular Carcinoma
Ductal Carcinoma-in-Situ: New Concepts and Controversies
 Ductal Carcinoma-in-Situ: New Concepts and Controversies James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS Case Presentation
Ductal Carcinoma-in-Situ: New Concepts and Controversies James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS Case Presentation
Case Scenario 1. 2/15/2011 The patient received IMRT 45 Gy at 1.8 Gy per fraction for 25 fractions.
 Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Balancing Evidence and Clinical Practice in the Treatment of Localized Breast Cancer May 5, 2006
 Balancing Evidence and Clinical Practice in the Treatment of Localized Breast Cancer May 5, 2006 Deborah Hamolsky MS, RN : DCIS Carol Franc Buck Breast Care Center UCSF Comprehensive Cancer Center Jane
Balancing Evidence and Clinical Practice in the Treatment of Localized Breast Cancer May 5, 2006 Deborah Hamolsky MS, RN : DCIS Carol Franc Buck Breast Care Center UCSF Comprehensive Cancer Center Jane
Ductal Carcinoma in Situ. Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA
 Ductal Carcinoma in Situ Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Definition of DCIS WHO 2012 A neoplastic proliferation
Ductal Carcinoma in Situ Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Definition of DCIS WHO 2012 A neoplastic proliferation
Basement membrane in lobule.
 Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Epithelial Columnar Breast Lesions: Histopathology and Molecular Markers
 29th Annual International Conference Advances in the Application of Monoclonal Antibodies in Clinical Oncology and Symposium on Cancer Stem Cells 25 th -27t h June, 2012, Mykonos, Greece Epithelial Columnar
29th Annual International Conference Advances in the Application of Monoclonal Antibodies in Clinical Oncology and Symposium on Cancer Stem Cells 25 th -27t h June, 2012, Mykonos, Greece Epithelial Columnar
Ductal Carcinoma In Situ of the Breast: Controversial Issues
 Ductal Carcinoma In Situ of the Breast: Controversial Issues MELVIN J. SILVERSTEIN The Breast Center*, Van Nuys, California, USA Key Words. DCIS Ductal carcinoma in situ Noninvasive breast cancer Intraductal
Ductal Carcinoma In Situ of the Breast: Controversial Issues MELVIN J. SILVERSTEIN The Breast Center*, Van Nuys, California, USA Key Words. DCIS Ductal carcinoma in situ Noninvasive breast cancer Intraductal
CLINICAL SIGNIFICANCE OF BENIGN EPITHELIAL CHANGES
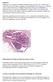 Papillomas. Papillomas are composed of multiple branching fibrovascular cores, each having a connective tissue axis lined by luminal and myoepithelial cells ( Fig. 23-11 ). Growth occurs within a dilated
Papillomas. Papillomas are composed of multiple branching fibrovascular cores, each having a connective tissue axis lined by luminal and myoepithelial cells ( Fig. 23-11 ). Growth occurs within a dilated
Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node
 Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node Oil Cyst Mass, Intermediate Concern Microlobulated Margins Obscured Margins Mass, Favoring Malignant Indistinct
Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node Oil Cyst Mass, Intermediate Concern Microlobulated Margins Obscured Margins Mass, Favoring Malignant Indistinct
Treatment options for the precancerous Atypical Breast lesions. Prof. YOUNG-JIN SUH The Catholic University of Korea
 Treatment options for the precancerous Atypical Breast lesions Prof. YOUNG-JIN SUH The Catholic University of Korea Not so benign lesions? Imaging abnormalities(10% recall) lead to diagnostic evaluation,
Treatment options for the precancerous Atypical Breast lesions Prof. YOUNG-JIN SUH The Catholic University of Korea Not so benign lesions? Imaging abnormalities(10% recall) lead to diagnostic evaluation,
LOBULAR CARCINOMA IN SITU: WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE
 : WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE Benjamin O. Anderson, M.D. Director, Breast Health Clinic Professor of Surgery and Global Health, University of Washington Joint Member, Fred Hutchinson Cancer
: WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE Benjamin O. Anderson, M.D. Director, Breast Health Clinic Professor of Surgery and Global Health, University of Washington Joint Member, Fred Hutchinson Cancer
Evaluation of Breast Specimens Removed by Needle Localization Technique
 Evaluation of Breast Specimens Removed by Needle Localization Technique Specimen Handling: The breast specimen when received should be measured and grossly inspected for any orientation designated by the
Evaluation of Breast Specimens Removed by Needle Localization Technique Specimen Handling: The breast specimen when received should be measured and grossly inspected for any orientation designated by the
A712(18)- Test slide, Breast cancer tissues with corresponding normal tissues
 A712(18)- Test slide, Breast cancer tissues with corresponding normal tissues (formalin fixed) For research use only Specifications: No. of cases: 12 Tissue type: Breast cancer tissues with corresponding
A712(18)- Test slide, Breast cancer tissues with corresponding normal tissues (formalin fixed) For research use only Specifications: No. of cases: 12 Tissue type: Breast cancer tissues with corresponding
Disclosures. Premalignant Lesions of the Breast: What Clinicians Want and Why. NY Times: Prone to Error: Earliest Steps to Find Cancer.
 Disclosures Premalignant Lesions of the Breast: What Clinicians Want and Why I have nothing to disclose Rick Baehner, MD Assistant Professor, UCSF Pathology NY Times: Prone to Error: Earliest Steps to
Disclosures Premalignant Lesions of the Breast: What Clinicians Want and Why I have nothing to disclose Rick Baehner, MD Assistant Professor, UCSF Pathology NY Times: Prone to Error: Earliest Steps to
Surgical Pathology Issues of Practical Importance
 Surgical Pathology Issues of Practical Importance Anne Moore, MD Medical Oncology Syed Hoda, MD Surgical Pathology The pathologist is central to the team approach needed to manage the patient with breast
Surgical Pathology Issues of Practical Importance Anne Moore, MD Medical Oncology Syed Hoda, MD Surgical Pathology The pathologist is central to the team approach needed to manage the patient with breast
Promise of a beautiful day
 Promise of a beautiful day Ductal carcinoma in Situ Lobular Carcinoma in Situ Natural History Manosmed Tartous Oct 2009 Gérard ABADJIAN MD Pathology Department Hôtel-Dieu de France. Associate Professor
Promise of a beautiful day Ductal carcinoma in Situ Lobular Carcinoma in Situ Natural History Manosmed Tartous Oct 2009 Gérard ABADJIAN MD Pathology Department Hôtel-Dieu de France. Associate Professor
Case Scenario 1 History and Physical 3/15/13 Imaging Pathology
 Case Scenario 1 History and Physical 3/15/13 The patient is an 84 year old white female who presented with an abnormal mammogram. The patient has a five year history of refractory anemia with ringed sideroblasts
Case Scenario 1 History and Physical 3/15/13 The patient is an 84 year old white female who presented with an abnormal mammogram. The patient has a five year history of refractory anemia with ringed sideroblasts
Invasive Papillary Breast Carcinoma
 410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
THE INFLUENCE OF MARGIN WIDTH ON LOCAL CONTROL OF DUCTAL CARCINOMA IN SITU OF THE BREAST
 THE INFLUENCE OF MARGIN WIDTH ON LOCAL CONTROL OF DUCTAL CARCINOMA IN SITU OF THE BREAST MELVIN J. SILVERSTEIN, M.D., MICHAEL D. LAGIOS, M.D., SUSAN GROSHEN, H.D., JAMES R. WAISMAN, M.D., BERNARD S. LEWINSKY,
THE INFLUENCE OF MARGIN WIDTH ON LOCAL CONTROL OF DUCTAL CARCINOMA IN SITU OF THE BREAST MELVIN J. SILVERSTEIN, M.D., MICHAEL D. LAGIOS, M.D., SUSAN GROSHEN, H.D., JAMES R. WAISMAN, M.D., BERNARD S. LEWINSKY,
Papillary Lesions of the Breast A Practical Approach to Diagnosis. (Arch Pathol Lab Med. 2016;140: ; doi: /arpa.
 Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Breast pathology. 2nd Department of Pathology Semmelweis University
 Breast pathology 2nd Department of Pathology Semmelweis University Breast pathology - Summary - Benign lesions - Acute mastitis - Plasma cell mastitis / duct ectasia - Fat necrosis - Fibrocystic change/
Breast pathology 2nd Department of Pathology Semmelweis University Breast pathology - Summary - Benign lesions - Acute mastitis - Plasma cell mastitis / duct ectasia - Fat necrosis - Fibrocystic change/
Mammographic imaging of nonpalpable breast lesions. Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand
 Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Standards for Diagnosis and Management of Ductal Carcinoma in Situ (DCIS) of the Breast
 d i a g n o s i s a n d m a n a g e m e n t s t a n d a r d s f o r d c i s Standards for Diagnosis and Management of Ductal Carcinoma in Situ (DCIS) of the Breast American College of Radiology American
d i a g n o s i s a n d m a n a g e m e n t s t a n d a r d s f o r d c i s Standards for Diagnosis and Management of Ductal Carcinoma in Situ (DCIS) of the Breast American College of Radiology American
Cytyc Corporation - Case Presentation Archive - March 2002
 FirstCyte Ductal Lavage History: 68 Year Old Female Gail Index: Unknown Clinical History: Negative Mammogram in 1995 6 yrs. later presents with bloody nipple discharge Subsequent suspicious mammogram Suspicious
FirstCyte Ductal Lavage History: 68 Year Old Female Gail Index: Unknown Clinical History: Negative Mammogram in 1995 6 yrs. later presents with bloody nipple discharge Subsequent suspicious mammogram Suspicious
Interpretation of Breast Pathology in the Era of Minimally Invasive Procedures
 Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine Jacksonville Medical Director, UF Health Breast Center Chief of Pathology
Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine Jacksonville Medical Director, UF Health Breast Center Chief of Pathology
ACRIN 6666 Therapeutic Surgery Form
 S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
Management of Ductal Carcinoma in Situ of the Breast: A Clinical Practice Guideline
 Evidence-based Series #1-10 Version 2.2006: Section 1 Management of Ductal Carcinoma in Situ of the Breast: A Clinical Practice Guideline W. Shelley, D. McCready, C. Holloway, M. Trudeau, S. Sinclair,
Evidence-based Series #1-10 Version 2.2006: Section 1 Management of Ductal Carcinoma in Situ of the Breast: A Clinical Practice Guideline W. Shelley, D. McCready, C. Holloway, M. Trudeau, S. Sinclair,
Columnar Cell Lesions
 Columnar Cell Lesions Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Question? Columnar cell lesions are: a) Annoying lesions
Columnar Cell Lesions Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Question? Columnar cell lesions are: a) Annoying lesions
Columnar Cell Lesions. Columnar Cell Lesions and Flat Epithelial Atypia
 Columnar Cell Lesions and Stuart J. Schnitt, M.D. Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Columnar Cell Lesions Lesions characterized by columnar epithelial cells
Columnar Cell Lesions and Stuart J. Schnitt, M.D. Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Columnar Cell Lesions Lesions characterized by columnar epithelial cells
Image guided core biopsies:
 Recommendations on the Surgical, Radiologic and Pathologic Approaches to Breast Disease: Using best practices based on multidisciplinary methodologies developed through the Allina Breast Committee. Image
Recommendations on the Surgical, Radiologic and Pathologic Approaches to Breast Disease: Using best practices based on multidisciplinary methodologies developed through the Allina Breast Committee. Image
A712(19)- Test slide, Breast cancer tissues with corresponding normal tissues
 A712(19)- Test slide, Breast cancer tissues with corresponding normal tissues (formalin fixed) For research use only Specifications: No. of cases: 12 Tissue type: Breast cancer tissues with corresponding
A712(19)- Test slide, Breast cancer tissues with corresponding normal tissues (formalin fixed) For research use only Specifications: No. of cases: 12 Tissue type: Breast cancer tissues with corresponding
Ductal Carcinoma in Situ (DCIS)
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Ductal Carcinoma in Situ (DCIS) Ductal Carcinoma in Situ DCIS Versions 2002 2017: Audretsch / Blohmer / Brunnert / Budach /
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Ductal Carcinoma in Situ (DCIS) Ductal Carcinoma in Situ DCIS Versions 2002 2017: Audretsch / Blohmer / Brunnert / Budach /
Papillary Lesions of the breast
 Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
BREAST MRI. Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School
 BREAST MRI Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School BREAST MRI Any assessment of the breast parenchyma requires the administration
BREAST MRI Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School BREAST MRI Any assessment of the breast parenchyma requires the administration
Papillary Lesions of the Breast: WHO Update
 Papillary Lesions of the Breast: WHO Update Stuart J. Schnitt, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Papillary Lesions of the Breast
Papillary Lesions of the Breast: WHO Update Stuart J. Schnitt, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Papillary Lesions of the Breast
04/10/2018 HIGH RISK BREAST LESIONS. Pathology Perspectives of High Risk Breast Lesions ELEVATED RISK OF BREAST CANCER HISTORICAL PERSPECTIVES
 Pathology Perspectives of High Risk Breast Lesions Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head Director of Clinical Trials, Research and Development The University of Texas MD
Pathology Perspectives of High Risk Breast Lesions Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head Director of Clinical Trials, Research and Development The University of Texas MD
Papillary Lesions of the Breast
 Papillary Lesions of the Breast Laura C. Collins, M.D. Associate Professor of Pathology Associate Director, Division of Anatomic Pathology Beth Israel Deaconess Medical Center and Harvard Medical School
Papillary Lesions of the Breast Laura C. Collins, M.D. Associate Professor of Pathology Associate Director, Division of Anatomic Pathology Beth Israel Deaconess Medical Center and Harvard Medical School
BREAST PATHOLOGY. Fibrocystic Changes
 BREAST PATHOLOGY Lesions of the breast are very common, and they present as palpable, sometimes painful, nodules or masses. Most of these lesions are benign. Breast cancer is the 2 nd most common cause
BREAST PATHOLOGY Lesions of the breast are very common, and they present as palpable, sometimes painful, nodules or masses. Most of these lesions are benign. Breast cancer is the 2 nd most common cause
Diseases of the breast (2 of 2) Breast cancer
 Diseases of the breast (2 of 2) Breast cancer Epidemiology & etiology The most common type of cancer & the 2 nd most common cause of cancer death in women 1 of 8 women in USA Affects 7% of women Peak at
Diseases of the breast (2 of 2) Breast cancer Epidemiology & etiology The most common type of cancer & the 2 nd most common cause of cancer death in women 1 of 8 women in USA Affects 7% of women Peak at
Breast Surgery: Yesterday, Today and Tomorrow
 Breast Surgery: Yesterday, Today and Tomorrow Baptist Hospital Gladys L. Giron, MD, FACS October 11,2014 Homestead Hospital Baptist Children s Hospital Doctors Hospital Baptist Cardiac & Vascular Institute
Breast Surgery: Yesterday, Today and Tomorrow Baptist Hospital Gladys L. Giron, MD, FACS October 11,2014 Homestead Hospital Baptist Children s Hospital Doctors Hospital Baptist Cardiac & Vascular Institute
Breast Pathology. Breast Development
 Breast Pathology Lecturer: Hanina Hibshoosh, M.D. Reading: Kumar, Cotran, Robbins, Basic Pathology, 6th Edition, pages 623-635 Breast Development 5th week - thickening of the epidermis - milk line 5th
Breast Pathology Lecturer: Hanina Hibshoosh, M.D. Reading: Kumar, Cotran, Robbins, Basic Pathology, 6th Edition, pages 623-635 Breast Development 5th week - thickening of the epidermis - milk line 5th
Maram Abdaljaleel, MD Dermatopathologist and Neuropathologist University of Jordan, School of Medicine
 Maram Abdaljaleel, MD Dermatopathologist and Neuropathologist University of Jordan, School of Medicine The most common non-skin malignancy of women 2 nd most common cause of cancer deaths in women, following
Maram Abdaljaleel, MD Dermatopathologist and Neuropathologist University of Jordan, School of Medicine The most common non-skin malignancy of women 2 nd most common cause of cancer deaths in women, following
Protocol for the Examination of Biopsy Specimens From Patients With Invasive Carcinoma of the Breast
 Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: BreastInvasive 1.0.0.0 Protocol Posting Date: February 2019 Accreditation Requirements The use of
Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: BreastInvasive 1.0.0.0 Protocol Posting Date: February 2019 Accreditation Requirements The use of
Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity.
 Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity. Background: 46 year old married premenopausal female with dense breasts has noticed
Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity. Background: 46 year old married premenopausal female with dense breasts has noticed
Proliferative Epithelial lesions of the Breast. Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London
 Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
Original Report. Mucocele-Like Tumors of the Breast: Mammographic and Sonographic Appearances. Katrina Glazebrook 1 Carol Reynolds 2
 Katrina Glazebrook 1 Carol Reynolds 2 Received January 2, 2002; accepted after revision August 28, 2002. 1 Department of Radiology, Mayo Clinic, 200 First St. S.W., Rochester, MN 55905. Address correspondence
Katrina Glazebrook 1 Carol Reynolds 2 Received January 2, 2002; accepted after revision August 28, 2002. 1 Department of Radiology, Mayo Clinic, 200 First St. S.W., Rochester, MN 55905. Address correspondence
Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity.
 Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity. Background: 46 year old married premenopausal female with dense breasts has noticed
Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity. Background: 46 year old married premenopausal female with dense breasts has noticed
Diseases of the breast (1 of 2)
 Diseases of the breast (1 of 2) Introduction A histology introduction Normal ducts and lobules of the breast are lined by two layers of cells a layer of luminal cells overlying a second layer of myoepithelial
Diseases of the breast (1 of 2) Introduction A histology introduction Normal ducts and lobules of the breast are lined by two layers of cells a layer of luminal cells overlying a second layer of myoepithelial
Int. J. Curr. Res. Med. Sci. (2018). 4(7): 1-7. International Journal of Current Research in Medical Sciences
 International Journal of Current Research in Medical Sciences ISSN: 2454-5716 P-ISJN: A4372-3064, E -ISJN: A4372-3061 www.ijcrims.com Original Research Article Volume 4, Issue 7-2018 DOI: http://dx.doi.org/10.22192/ijcrms.2018.04.07.001
International Journal of Current Research in Medical Sciences ISSN: 2454-5716 P-ISJN: A4372-3064, E -ISJN: A4372-3061 www.ijcrims.com Original Research Article Volume 4, Issue 7-2018 DOI: http://dx.doi.org/10.22192/ijcrms.2018.04.07.001
Breast Cancer. Dr. Andres Wiernik 2017
 Breast Cancer Dr. Andres Wiernik 2017 Agenda: The Facts! (Epidemiology/Risk Factors) Biological Classification/Phenotypes of Breast Cancer Treatment approach Local Systemic Agenda: The Facts! (Epidemiology/Risk
Breast Cancer Dr. Andres Wiernik 2017 Agenda: The Facts! (Epidemiology/Risk Factors) Biological Classification/Phenotypes of Breast Cancer Treatment approach Local Systemic Agenda: The Facts! (Epidemiology/Risk
Original Article. Spontaneous Healing of Breast Cancer
 Breast Cancer Vol. 12 No. 2 April 2005 Original Article Rie Horii 1, 3, Futoshi Akiyama 1, Fujio Kasumi 2, Morio Koike 3, and Goi Sakamoto 1 1 Department of Breast Pathology, the Cancer Institute of the
Breast Cancer Vol. 12 No. 2 April 2005 Original Article Rie Horii 1, 3, Futoshi Akiyama 1, Fujio Kasumi 2, Morio Koike 3, and Goi Sakamoto 1 1 Department of Breast Pathology, the Cancer Institute of the
Citation Hong Kong Practitioner, 1996, v. 18 n. 2, p
 Title Conservative surgery for breast cancer Author(s) Poon, RTP; Chow, LWC; Au, GKH Citation Hong Kong Practitioner, 1996, v. 18 n. 2, p. 68-72 Issued Date 1996 URL http://hdl.handle.net/722/45367 Rights
Title Conservative surgery for breast cancer Author(s) Poon, RTP; Chow, LWC; Au, GKH Citation Hong Kong Practitioner, 1996, v. 18 n. 2, p. 68-72 Issued Date 1996 URL http://hdl.handle.net/722/45367 Rights
Access and take the CME test online and receive 1 AMA PRA Category 1 Credit at CME.TheOncologist.com
 The Oncologist Breast Cancer Current Treatment and Clinical Trial Developments for Ductal Carcinoma In Situ of the Breast JUDY C. BOUGHEY, a RICARDO J. GONZALEZ, b EVERETT BONNER, c HENRY M. KUERER b a
The Oncologist Breast Cancer Current Treatment and Clinical Trial Developments for Ductal Carcinoma In Situ of the Breast JUDY C. BOUGHEY, a RICARDO J. GONZALEZ, b EVERETT BONNER, c HENRY M. KUERER b a
BREAST MRI. Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School
 BREAST MRI Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School BREAST MRI Any assessment of the breast parenchyma requires the administration
BREAST MRI Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School BREAST MRI Any assessment of the breast parenchyma requires the administration
Breast Cancer Diagnosis, Treatment and Follow-up
 Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ).
 SOLID TUMORS WORKSHOP Cases for review Prostate Cancer Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ). January 2009 PSA 4.4, 20% free; August 2009 PSA 5.2; Sept 2009
SOLID TUMORS WORKSHOP Cases for review Prostate Cancer Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ). January 2009 PSA 4.4, 20% free; August 2009 PSA 5.2; Sept 2009
A DEEPER DIVE INTO DUCTAL CARCINOMA IN SITU: CLINICAL AND PATHOLOGIC CONSIDERATIONS IN 2015
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 A DEEPER DIVE INTO DUCTAL CARCINOMA IN SITU: CLINICAL AND PATHOLOGIC CONSIDERATIONS IN 2015
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 A DEEPER DIVE INTO DUCTAL CARCINOMA IN SITU: CLINICAL AND PATHOLOGIC CONSIDERATIONS IN 2015
Benign, Reactive and Inflammatory Lesions of the Breast
 Benign, Reactive and Inflammatory Lesions of the Breast Marilin Rosa, MD Associate Member Section Head of Breast Pathology Department of Anatomic Pathology Program Director, Breast Pathology Fellowship
Benign, Reactive and Inflammatory Lesions of the Breast Marilin Rosa, MD Associate Member Section Head of Breast Pathology Department of Anatomic Pathology Program Director, Breast Pathology Fellowship
Imaging in breast cancer. Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since
 Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
1 NORMAL HISTOLOGY AND METAPLASIAS
 1 NORMAL HISTOLOGY AND METAPLASIAS, MD Anatomy and Histology 1 Metaplasias 2 ANATOMY AND HISTOLOGY The female breast is composed of a branching duct system, which begins at the nipple with the major lactiferous
1 NORMAL HISTOLOGY AND METAPLASIAS, MD Anatomy and Histology 1 Metaplasias 2 ANATOMY AND HISTOLOGY The female breast is composed of a branching duct system, which begins at the nipple with the major lactiferous
National Diagnostic Imaging Symposium 2013 SAM - Breast MRI 1
 National Diagnostic Imaging Symposium 2013 December 8-12, 2013 Disney s Yacht Club Resort Lake Buena Vista, Florida Self Assessment Module Questions, Answers and References Day SAM Title - Each SAM title
National Diagnostic Imaging Symposium 2013 December 8-12, 2013 Disney s Yacht Club Resort Lake Buena Vista, Florida Self Assessment Module Questions, Answers and References Day SAM Title - Each SAM title
Women s Imaging Original Research
 Mammography of Recurrent Breast Cancer Women s Imaging Original Research WOMEN S IMAGING Renee W. Pinsky 1 Murray Rebner 2 Lori J. Pierce 3 Merav A. Ben-David 3,4 Frank Vicini 5 Karen A. Hunt 1,6 Mark
Mammography of Recurrent Breast Cancer Women s Imaging Original Research WOMEN S IMAGING Renee W. Pinsky 1 Murray Rebner 2 Lori J. Pierce 3 Merav A. Ben-David 3,4 Frank Vicini 5 Karen A. Hunt 1,6 Mark
ANNEX 1 OBJECTIVES. At the completion of the training period, the fellow should be able to:
 1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
ROLE OF MRI IN SCREENING, DIAGNOSIS AND MANAGEMENT OF BREAST CANCER. B.Zandi Professor of Radiology
 ROLE OF MRI IN SCREENING, DIAGNOSIS AND MANAGEMENT OF BREAST CANCER B.Zandi Professor of Radiology Introduction In the USA, Breast Cancer is : The Most Common Non-Skin Cancer The Second Leading cause of
ROLE OF MRI IN SCREENING, DIAGNOSIS AND MANAGEMENT OF BREAST CANCER B.Zandi Professor of Radiology Introduction In the USA, Breast Cancer is : The Most Common Non-Skin Cancer The Second Leading cause of
Accuracy of Specimen Radiography in Assessing Complete Local Excision with Breast-Conservation Surgery
 RESEARCH ARTICLE Editorial Process: Submission:09/22/2017 Acceptance:01/21/2018 Accuracy of Specimen Radiography in Assessing Complete Local Excision with Breast-Conservation Surgery Saira Naz, Imrana
RESEARCH ARTICLE Editorial Process: Submission:09/22/2017 Acceptance:01/21/2018 Accuracy of Specimen Radiography in Assessing Complete Local Excision with Breast-Conservation Surgery Saira Naz, Imrana
Good afternoon everyone. First of all many thanks to Dr. Bonaventura and Dr. Arn for inviting
 PATHOLOGY IN-SITU CARCINOMA, ROHIT BHARGAVA, MD 1 Good afternoon everyone. First of all many thanks to Dr. Bonaventura and Dr. Arn for inviting me here, it s great to be here and I m going to talk about
PATHOLOGY IN-SITU CARCINOMA, ROHIT BHARGAVA, MD 1 Good afternoon everyone. First of all many thanks to Dr. Bonaventura and Dr. Arn for inviting me here, it s great to be here and I m going to talk about
Prophylactic Mastectomy
 Prophylactic Mastectomy Policy Number: Original Effective Date: MM.06.010 01/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO 08/24/2012 Section: Surgery Place(s) of Service: Inpatient I.
Prophylactic Mastectomy Policy Number: Original Effective Date: MM.06.010 01/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO 08/24/2012 Section: Surgery Place(s) of Service: Inpatient I.
Ana Sofia Preto 19/06/2013
 Ana Sofia Preto 19/06/2013 Understanding the underlying pathophysiologic processes leading to the various types of calcifications Description and illustration of the several types of calcifications, according
Ana Sofia Preto 19/06/2013 Understanding the underlying pathophysiologic processes leading to the various types of calcifications Description and illustration of the several types of calcifications, according
Case study 1. Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research
 NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
Ductal Carcinoma in Situ: The Mammographer s Perspective
 585 Ductal Carcinoma in Situ: The Mammographer s Perspective Paul C. Stomper1 and Frederick R. Margolin2 Ductal carcinoma in situ represents a heterogeneous group of lesions now most commonly discovered
585 Ductal Carcinoma in Situ: The Mammographer s Perspective Paul C. Stomper1 and Frederick R. Margolin2 Ductal carcinoma in situ represents a heterogeneous group of lesions now most commonly discovered
AMSER Case of the Month: November 2018
 AMSER Case of the Month: November 2018 42 year old with right breast mass Rina Kiyota Petek Lake Erie College of Osteopathic Medicine, OMS-III Kossivi Dantey, MD Bibianna Klepchick, MD Matthew Hartman,
AMSER Case of the Month: November 2018 42 year old with right breast mass Rina Kiyota Petek Lake Erie College of Osteopathic Medicine, OMS-III Kossivi Dantey, MD Bibianna Klepchick, MD Matthew Hartman,
Resection Margins in Breast Conserving Surgery. Alberto Costa, MD Canton Ticino Breast Unit Lugano, Switzerland
 Resection Margins in Breast Conserving Surgery Alberto Costa, MD Canton Ticino Breast Unit Lugano, Switzerland Breast Conserving Surgery 1 Probably one of the most important innovation in cancer surgery
Resection Margins in Breast Conserving Surgery Alberto Costa, MD Canton Ticino Breast Unit Lugano, Switzerland Breast Conserving Surgery 1 Probably one of the most important innovation in cancer surgery
6/3/2010. Outline of Talk. Lobular Breast Cancer: Definition of lobular differentiation. Common Problems in Diagnosing LCIS in Core Biopsies
 Outline of Talk Lobular Breast Cancer: Common Problems in Diagnosing LCIS in Core Biopsies Definition of lobular differentiation Variants of LCIS that: carry risk for unsampled invasive cancer mimic DCIS
Outline of Talk Lobular Breast Cancer: Common Problems in Diagnosing LCIS in Core Biopsies Definition of lobular differentiation Variants of LCIS that: carry risk for unsampled invasive cancer mimic DCIS
Histological Type. Morphological and Molecular Typing of breast Cancer. Nottingham Tenovus Primary Breast Cancer Study. Survival (%) Ian Ellis
 Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological Type
Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological Type
COPE Library Sample
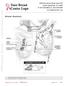 Breast Anatomy LOBULE LOBE ACINI (MILK PRODUCING UNITS) NIPPLE AREOLA COMPLEX ENLARGEMENT OF DUCT AND LOBE LOBULE SUPRACLAVICULAR NODES INFRACLAVICULAR NODES DUCT DUCT ACINI (MILK PRODUCING UNITS) 8420
Breast Anatomy LOBULE LOBE ACINI (MILK PRODUCING UNITS) NIPPLE AREOLA COMPLEX ENLARGEMENT OF DUCT AND LOBE LOBULE SUPRACLAVICULAR NODES INFRACLAVICULAR NODES DUCT DUCT ACINI (MILK PRODUCING UNITS) 8420
Lobular Carcinoma In Situ Variants in Breast Cores
 Lobular Carcinoma In Situ Variants in Breast Cores Potential for Misdiagnosis, Upgrade Rates at Surgical Excision, and Practical Implications Megan E. Sullivan, MD; Seema A. Khan, MD; Yurdanur Sullu, MD;
Lobular Carcinoma In Situ Variants in Breast Cores Potential for Misdiagnosis, Upgrade Rates at Surgical Excision, and Practical Implications Megan E. Sullivan, MD; Seema A. Khan, MD; Yurdanur Sullu, MD;
Carcinoma mammario: le istologie non frequenti. Valentina Guarneri Università di Padova IOV-IRCCS
 Carcinoma mammario: le istologie non frequenti Valentina Guarneri Università di Padova IOV-IRCCS Histological diversity of breast adenocarcinomas Different histological types are defined according to specific
Carcinoma mammario: le istologie non frequenti Valentina Guarneri Università di Padova IOV-IRCCS Histological diversity of breast adenocarcinomas Different histological types are defined according to specific
AMSER Case of the Month: November 2018
 AMSER Case of the Month: November 2018 52 year old female with an abnormal screening mammogram Areeg Rehman, MS 4 Nova Southeastern University Rebecca T. Sivarajah, MD Penn State University College of
AMSER Case of the Month: November 2018 52 year old female with an abnormal screening mammogram Areeg Rehman, MS 4 Nova Southeastern University Rebecca T. Sivarajah, MD Penn State University College of
Ultrastructure of the Periductal Area of Comedo Carcinoma in situ of the Breast
 284 Annals of Clinical & Laboratory Science, vol. 31, no. 3, 2001 Ultrastructure of the Periductal Area of Comedo Carcinoma in situ of the Breast Ping Tang, Saul Teichberg, Beth Roberts, and Steven I.
284 Annals of Clinical & Laboratory Science, vol. 31, no. 3, 2001 Ultrastructure of the Periductal Area of Comedo Carcinoma in situ of the Breast Ping Tang, Saul Teichberg, Beth Roberts, and Steven I.
04/10/2018. Intraductal Papillary Neoplasms Of Breast INTRADUCTAL PAPILLOMA
 Intraductal Papillary Neoplasms Of Breast Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head The University of Texas MD Anderson Cancer Center 25 th Annual Seminar in Pathology Pittsburgh,
Intraductal Papillary Neoplasms Of Breast Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head The University of Texas MD Anderson Cancer Center 25 th Annual Seminar in Pathology Pittsburgh,
Columnar Cell Lesions and Flat Epithelial Atypia
 Columnar Cell Lesions and Flat Epithelial Atypia Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School, Boston, MA Terminology for Columnar Cell
Columnar Cell Lesions and Flat Epithelial Atypia Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School, Boston, MA Terminology for Columnar Cell
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Non-Calcified Ductal Carcinoma in Situ: Ultrasound and Mammographic Findings Correlated with Histological Findings
 Yonsei Med J 49(1):103-110, 2008 DOI 10.3349/ymj.2008.49.1.103 Non-Calcified Ductal Carcinoma in Situ: Ultrasound and Mammographic Findings Correlated with Histological Findings Kyu Ran Cho, 1 Bo Kyoung
Yonsei Med J 49(1):103-110, 2008 DOI 10.3349/ymj.2008.49.1.103 Non-Calcified Ductal Carcinoma in Situ: Ultrasound and Mammographic Findings Correlated with Histological Findings Kyu Ran Cho, 1 Bo Kyoung
Speaker s Bureau. Travel expenses. Advisory Boards. Stock. Genentech Invuity Medtronic Pacira. Faxitron. Dune TransMed7 Genomic Health.
 Management of DCIS Shawna C. Willey, MD, FACS Professor of Surgery, Georgetown University Director, Medstar Regional Breast Health Program Chief, Department of Surgery Medstar Georgetown University Hospital
Management of DCIS Shawna C. Willey, MD, FACS Professor of Surgery, Georgetown University Director, Medstar Regional Breast Health Program Chief, Department of Surgery Medstar Georgetown University Hospital
Surgical Therapy: Sentinel Node Biopsy and Breast Conservation
 Surgical Therapy: Sentinel Node Biopsy and Breast Conservation Stephen B. Edge, MD Professor of Surgery and Oncology Roswell Park Cancer Institute University at Buffalo Dr. Roswell Park: Tradition in Cancer
Surgical Therapy: Sentinel Node Biopsy and Breast Conservation Stephen B. Edge, MD Professor of Surgery and Oncology Roswell Park Cancer Institute University at Buffalo Dr. Roswell Park: Tradition in Cancer
259 Patients with DCIS of the breast applying USC/Van Nuys prognostic index: a retrospective review with long term follow up
 Breast Cancer Res Treat (2008) 109:405 416 DOI 10.1007/s10549-007-9668-7 REVIEW 259 Patients with DCIS of the breast applying USC/Van Nuys prognostic index: a retrospective review with long term follow
Breast Cancer Res Treat (2008) 109:405 416 DOI 10.1007/s10549-007-9668-7 REVIEW 259 Patients with DCIS of the breast applying USC/Van Nuys prognostic index: a retrospective review with long term follow
Bruno CUTULI Policlinico Courlancy REIMS. WORKSHOP SULL IRRADIAZIONE MAMMARIA IPOFRAZIONATA Il carcinoma duttale in situ
 Bruno CUTULI Policlinico Courlancy REIMS WORKSHOP SULL IRRADIAZIONE MAMMARIA IPOFRAZIONATA Il carcinoma duttale in situ XXI CONGRESSO AIRO GENOVA 22.11.2011 INTRODUCTION Due to wide diffusion of mammography,
Bruno CUTULI Policlinico Courlancy REIMS WORKSHOP SULL IRRADIAZIONE MAMMARIA IPOFRAZIONATA Il carcinoma duttale in situ XXI CONGRESSO AIRO GENOVA 22.11.2011 INTRODUCTION Due to wide diffusion of mammography,
Ahmad Elahi*, Gholamreza Toogeh,Habibollah Mahmoodzadeh, Behnaz Jahanbin, Farhad Shahi,
 Clinical Experience Open Access DOI: 10.1187/abc.20185258-62 Ductal Carcinoma In Situ Close to the Inked Margin: A Case Presented in Multidisciplinary Session With Clinical Discussion and Decision Making
Clinical Experience Open Access DOI: 10.1187/abc.20185258-62 Ductal Carcinoma In Situ Close to the Inked Margin: A Case Presented in Multidisciplinary Session With Clinical Discussion and Decision Making
BREAST CONSERVATION TREATMENT IN EARLY STAGE DISEASE AND DCIS LAWRENCE J. SOLIN, MD, FACR, FASTRO
 BREAST CONSERVATION TREATMENT IN EARLY STAGE DISEASE AND DCIS LAWRENCE J. SOLIN, MD, FACR, FASTRO Chairman Department of Radiation Oncology Albert Einstein Medical Center Philadelphia, PA Professor (Adjunct)
BREAST CONSERVATION TREATMENT IN EARLY STAGE DISEASE AND DCIS LAWRENCE J. SOLIN, MD, FACR, FASTRO Chairman Department of Radiation Oncology Albert Einstein Medical Center Philadelphia, PA Professor (Adjunct)
Breast Cancer FAQ. How does Breast Cancer spread? Breast cancer spreads by invading into
 FAQ Breast Cancer What is Breast Cancer? Breast Cancer is the second leading cause of cancer deaths in women today (second to lung cancer) and is the most common cancer among women excluding non-melanoma
FAQ Breast Cancer What is Breast Cancer? Breast Cancer is the second leading cause of cancer deaths in women today (second to lung cancer) and is the most common cancer among women excluding non-melanoma
The management of ductal carcinoma in situ of the breast
 The management of ductal carcinoma in situ of the breast K A Skinner and M J Silverstein Keck School of Medicine, University of Southern California, USC/Norris Comprehensive Cancer Center, 1441 Eastlake
The management of ductal carcinoma in situ of the breast K A Skinner and M J Silverstein Keck School of Medicine, University of Southern California, USC/Norris Comprehensive Cancer Center, 1441 Eastlake
Proliferative Breast Disease: implications of core biopsy diagnosis. Proliferative Breast Disease
 Proliferative Breast Disease: implications of core biopsy diagnosis Jean F. Simpson, M.D. Breast Pathology Consultants, Inc. Nashville, TN Proliferative Breast Disease Must be interpreted in clinical and
Proliferative Breast Disease: implications of core biopsy diagnosis Jean F. Simpson, M.D. Breast Pathology Consultants, Inc. Nashville, TN Proliferative Breast Disease Must be interpreted in clinical and
How to Use MRI Following Neoadjuvant Chemotherapy (NAC) in Locally Advanced Breast Cancer
 Global Breast Cancer Conference 2016 & 5 th International Breast Cancer Symposium April 29 th 2016, 09:40-10:50 How to Use MRI Following Neoadjuvant Chemotherapy (NAC) in Locally Advanced Breast Cancer
Global Breast Cancer Conference 2016 & 5 th International Breast Cancer Symposium April 29 th 2016, 09:40-10:50 How to Use MRI Following Neoadjuvant Chemotherapy (NAC) in Locally Advanced Breast Cancer
