Wartenberg s migrant sensory neuritis: a prospective follow-up study
|
|
|
- Noel Chapman
- 5 years ago
- Views:
Transcription
1 J Neurol (2010) 257: DOI /s ORIGINAL COMMUNICATION Wartenberg s migrant sensory neuritis: a prospective follow-up study Abraham C. J. Stork Marjon F. G. van der Meulen W.-Ludo van der Pol Alexander F. J. E. Vrancken Hessel Franssen Nicolette C. Notermans Received: 27 October 2009 / Revised: 10 February 2010 / Accepted: 5 March 2010 / Published online: 31 March 2010 Ó The Author(s) This article is published with open access at Springerlink.com Abstract Migrant sensory neuropathy (Wartenberg s migrant sensory neuritis) is characterized by sudden numbness in the distribution of one or multiple cutaneous nerves. To study disease course and outcome, we prospectively followed 12 patients who presented to our tertiary referral neuromuscular outpatient clinic between January 2003 and January Medical history, neurological, laboratory and electrophysiological examinations were obtained from all patients. All patients were reviewed a second time in 2007, and five had a follow-up electrophysiological examination. At the first visit, 50% described an episode of stretching preceding the sensory complaints. All but three described pain in the affected area before or concomitant with sensory loss. At clinical examination a median of six skin areas were affected, and in 75% this could be confirmed by nerve conduction studies in at least one nerve. Forty-two percent had involvement of the trigeminal nerve. After a mean disease duration of 7.5 years, three patients reported a complete disappearance of sensory complaints and five that the pain had disappeared, but numbness remained. Three patients still had both painful and numb sensory deficits. One patient developed a distal symmetric sensory polyneuropathy. In conclusion, Wartenberg s sensory neuritis is a distinct, exclusively sensory, neuropathy, marked by pain preceding numbness in affected nerves. An episode of stretching preceding pain A. C. J. Stork (&) W.-Ludo van der Pol A. F. J. E. Vrancken H. Franssen N. C. Notermans UMC Utrecht, Utrecht, The Netherlands astork@umcutrecht.nl M. F. G. van der Meulen St. Antonius Hospital, Nieuwegein, The Netherlands is not necessary for the diagnosis. Wartenberg s sensory neuritis often retains its spotty, exclusively sensory characteristics after long term follow-up. Keywords Peripheral neuropathy Neuromuscular disease Diagnosis Wartenberg neuritis Migrant sensory neuritis Introduction Migrant sensory neuropathy (Wartenberg s migrant sensory neuritis) is characterized by sudden numbness in the distribution of one or multiple cutaneous nerves. The limited number of published clinical studies seems to suggest that it is a rare disorder. Most studies included few patients and were retrospective. They generally report a mild disease course, but follow-up data are scarce [1, 4, 6 8, 11, 13, 14]. In the absence of conclusive diagnostic tests, Wartenberg s migrant sensory neuritis remains a clinical diagnosis. The literature on Wartenberg s migrant sensory neuritis suggests that nerves can be affected sequentially or at the same time [7, 13]. Numbness can be preceded by painful sensations in the same area. Typically, stretching of the affected nerve, for example by kneeling down or abrupt dorsiflexion of the foot, sometimes precedes symptoms [7]. Nerves of the limbs are probably most commonly affected, but all cutaneous nerves (including trigeminal or truncal branches) can be affected. Function of motor nerves is normal [6]. Nerve conduction studies usually show decreased sensory nerve action potentials (SNAPs) of the involved nerves [8]. To document the clinical spectrum and outcome of Wartenberg s migrant sensory neuritis we conducted a prospective clinical and laboratory study with 5 years of follow-up.
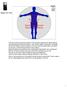
2 J Neurol (2010) 257: Patients and methods Patients who presented with isolated sensory deficits at our tertiary referral outpatient clinic for neuromuscular diseases at the University Medical Centre Utrecht (UMCU) between January 2003 and January 2004 were considered for inclusion. Exclusion criteria were a generalized polyneuropathy or a different explanation for the sensory deficits or painful skin, for example trauma. Patients who met these criteria and who gave their informed consent were included in the prospective cohort study. Medical history, time of onset, disease course, relation to stretching of nerves, pain, tingling or other sensory disorders, number of affected skin areas (defined as the area of skin surface with impaired sensation in the cutaneous distribution of one peripheral nerve), duration of symptoms were documented. Neurological examination was performed by one of the authors (MvdM) to exclude weakness or signs compatible with symmetric polyneuropathy, and to document sensory function of cutaneous nerves. Erythrocyte sedimentation rate, blood glucose and angiotensin converting enzyme (ACE) levels, presence of antinuclear antibodies, extractable nuclear antigen antibodies, and M-protein and anti-hu antibodies were determined. Electrophysiological studies included bilateral recording of sensory nerve action potentials (SNAPs) of the musculocutaneous, medial cutaneous antebrachii, median, ulnar, radial, saphenous, superficial peroneal, tibial, lateral femoral cutaneous and sural nerves. SNAPs were considered abnormal if the amplitude was below the lower limit of normal or if the amplitude on the affected side was less than 50% of the amplitude on the unaffected side [3, 5]. Motor nerve conduction and F-wave studies of the median, ulnar, tibial and deep peroneal nerves were also performed, as well as the H reflex of the m. soleus. Between June 2007 and January 2008, we interviewed all patients by telephone following a standardized questionnaire. If the interview raised the suspicion of progression of symptoms or the possibility of another diagnosis, neurological examination and electrophysiological studies were repeated. Results Twelve patients (six men) out of a total of 750 (1.6%) new patients presenting to our neuromuscular outpatient clinic met all inclusion criteria. All but three patients reported pain either preceding or concomitant with sensory deficits (Table 1). Six patients (50%) reported pain in the affected area in the weeks preceding numbness, one described pain lasting months before numbness set in. The quality of pain was variously described as stabbing, burning or tingling. Five (42%) patients reported hyperesthesia in the affected skin areas. Six (50%) patients reported stretching the affected skin area or nerve just before pain and numbness set in. Thus affected were the sural, peroneal, plantar, saphenal, radial and median nerves, by overextending the foot for the first three, and respectively everting the foot, flexing the wrist and extending the fingers for the other nerves. In all patients peripheral nerves of the limbs were affected, in five (42%) patients the trigeminal nerve was also involved and in four (33%) patients areas of the trunk were affected (Fig. 1). Physical examination yielded deficits in sensory function in a median of six nerves (range 3 8) per patient. Two patients had neither pain nor persistent sensory deficits, both reported that they considered their complaints to be light. One had no abnormalities at electrophysiological examination, the other had lowered and absent SNAPs of the relevant nerves for his remitting sensory deficits. Electrophysiological studies showed abnormal SNAPs of at least one of the clinically affected nerves in nine (75%) patients. Electrophysiological confirmation of sensory deficits was found in a median of two (range 0 3) nerves per patient (Table 2). Patient 7 had an asymmetric lowered SNAP of the peroneal nerve without sensory complaints in the distribution of the nerve, but all other lowered SNAPs were of clinically affected nerves. No conduction blocks were found. Motor nerve conduction studies were normal except for a lowered CMAP of the m. extensor digitorum brevis (deep peroneal nerve) of patient 11. Laboratory abnormalities included non-quantifiable IgG paraproteinemia in two patients and marginally elevated ACE levels in four patients. All patients were screened for the presence of anti-hu, ANA and ENA antibodies, none tested positive. Five years after the initial visit to the outpatient clinic the mean disease duration was 7.5 years (range 5 14 years). Clinical disease course showed considerable variation (Table 1). Three patients reported a complete disappearance of sensory complaints and five that the pain had disappeared, but numbness remained. Patient number 5, 6 and 9 still had both painful and numb sensory deficits. In all patients impact on daily life was limited, although two patients did describe problems in performing professional activities. One patient (patient 4 in Tables 1, 2) had hypoesthesia in a sock and glove pattern with generally lowered reflexes and absent knee and ankle jerks, consistent with distal symmetric sensory polyneuropathy. In the 5-year follow-up period six out of the remaining 11 patients developed new areas with sensory deficits, in these patients we regarded disease progression to be ongoing. Four patients reported a full recovery of sensory function in the newly affected areas, two developed persistent sensory deficits.
3 1346 J Neurol (2010) 257: Table 1 Patient characteristics at study entry and follow-up Patient Age at study entry Duration of disease at initial evaluation Sex Presence of pain Stretch Number of affected areas at study entry Number of newly affected areas during follow-up Number of persistent sensory deficits Disease duration at last follow-up Period of progressive disease F? M? M? F?? 5 Progression to sensory polyneuropathy F?? [ F?? [ M? F F?? [ M? M [ F?? Fig. 1 Localization and frequency of sensory deficits in all patients at initial visit either by history taking or neurological examination. Colors indicate the number of times deficits were observed: green 1, yellow 2, blue 3, purple 4, red 5 Electrophysiological examinations were repeated in five patients. In patient 1 no abnormalities in SNAP amplitudes were found, consistent with the disappearance of persistent, spotty sensory complaints since her inclusion in this study. An additional abnormally low SNAP of the superficial peroneal nerve was found in one patient (patient 5),
4 J Neurol (2010) 257: Table 2 Sensory deficits found by neurological examination and nerve conduction study at study entry and follow-up Patient Radial Median Ulnar Peroneal Sural Saphenous Tibial Trigeminal Trunk Lat cut high Digital foot 1???*???*? 2?*?*?*?? 3?# #?#? 4???*?*? 5?#???*??*? 6?#??*#?? 7??*?*?*??? 8????? 9??* #??*?* 10??*??*? 11?*?*?*?#???? 12?#??? denotes affected nerves at initial examination # at follow-up, uni- or bilaterally * denotes affected nerves with both clinical and electrophysiological (low SNAP amplitude) sensory dysfunction at initial presentation at follow-up consistent with history taking and physical examination. In two other patients (patients 7 and 11) there was a decrease of SNAP amplitudes of the affected nerves that still showed sensory deficits at follow-up. The patient that had progressed to polyneuropathy had generally lowered SNAPs. A cause for the axonal neuropathy could not be uncovered. Discussion After 5-year follow-up all but one patient still had exclusively sensory, spotty complaints. In most patients the symptoms were remitting and their severity and impact on daily life were limited, both at initial presentation and after 5 years follow-up. The sensation of stretching preceding sensory complaints was not very helpful for establishing the diagnosis as only half of the patients remembered either physical stretching or a feeling of overstretching preceding the other symptoms. The presence or absence of stretching did not lead to a difference in progression or persistence of sensory complaints. In most patients at least one of the sensory deficits revealed by history taking or neurological examination could be confirmed with an abnormal SNAP of the affected sensory nerve, making small fiber neuropathy by definition an unlikely explanation. Only one patient developed distal symmetrical sensory deficits that eventually lead to a diagnosis of chronic idiopathic axonal polyneuropathy [12]. Whether the spotty sensory complaints at the initial examination were a rare first manifestation of the polyneuropathy, or if this patient coincidentally developed two distinct neuropathies, could not be established, because of the idiopathic nature of both neuropathies. In all other patients repeated history taking, neurological examination and ancillary evaluations show no sensory polyneuropathy or small fiber neuropathy (although no techniques were available to assess function of small sensory nerve fibers) [2]. The highly variable distribution of affected nerves in individual patients, and the absence of a progression from distal to proximal nerves do not point to a length-dependent etiology. The pattern is more reminiscent of immunemediated neuropathies like multifocal motor neuropathy [9]. In most patients the first sensory loss was distally in the legs or arms. Only two patients had their first sensory abnormalities in the legs, proximally of the knees. Although we found involvement of the trigeminal nerve and thoracic nerves in a remarkably high number of patients, none of them originally presented with sensory loss in just these areas. The absence of any underlying cause, the lack of continuous pain and absence of motor involvement in our patients during follow up also made mononeuritis multiplex associated with an autoimmune disease unlikely [10]. For this reason, we refrained from further investigating the etiology of Wartenberg s sensory neuritis by nerve biopsy. Nerve biopsy studies in Wartenberg patients show variable and aspecific changes ranging from perineural inflammatory changes, changes more suggestive of nonsystemic vasculitic neuropathy to axonal degeneration as seen in ischemic neuronal lesions [1, 6 8, 11, 14]. The absence of histopathological data in our study precludes inferring a possible immune-mediated etiology of Wartenberg s sensory neuritis. However, our follow-up
5 1348 J Neurol (2010) 257: data do show that in typical cases with a clinical history and neurological and electrophysiological findings consistent with Wartenberg s sensory neuritis, a nerve biopsy can reasonably be omitted from the diagnostic work-up. Given the mild and often remitting course of the disease in our patient group, the adverse sequelae that may result from nerve biopsies do seem disproportionate when considering possible therapeutical benefits and risks of the procedure for individual patients. In conclusion, Wartenberg s sensory neuritis is a clearly distinct syndrome, leading to relatively mild but persistent sensory deficits. In this study, laboratory tests in the absence of positive signs of systemic disease did not yield any clinically relevant results. Nerve conduction studies can support the diagnosis. Mainstay for the diagnosis is exclusion of motor deficits by history taking, neurological and electrophysiological examination in combination with the typical complaints of numbness in multiple skin areas with a sudden onset, after or during painful sensations in the same area. In these cases, patients can be reassured about the disease course, as it can be expected to remain relatively benign, without motor involvement or serious functional disability. Open Access This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited. References 1. Asbury AK, Picard EH, Baringer JR (1972) Sensory perineuritis. Arch Neurol 26: Devigili G, Tugnoli V, Penza P, Camozzi F, Lombardi R, Melli G, Broglio L, Granieri E, Lauria G (2008) The diagnostic criteria for small fibre neuropathy: from symptoms to neuropathology. Brain 131: Franssen H, Notermans NC (2006) Length dependence in polyneuropathy associated with IgM gammopathy. Ann Neurol 59: Keunen RWM, ten Bruggen JP, Mauser HW, Ackerstaff RGA (1988) Migrant sensory neuritis of Wartenberg. Clin Neurol Neurosurg 90(1): Kimura J (2001) Electrodiagnosis in diseases of nerve and muscle. Oxford University Press, New York 6. Laterre C, Ghilain S, Tassin S, Guerit JM (1988) La neuropathie sensitive disseminée de Wartenberg. Rev Neurol (Paris) 144: Matthews WB, Eseri M (1983) Migrant sensory neuritis of Wartenberg. J Neurol Neurosurg Psychiatry 46: Nicolle MW, Barron JR, Watson BV, Hammond RR, Miller TA (2001) Wartenberg s migrant sensory neuritis. Muscle Nerve 24(3): Nobile-Orazio E, Cappellari A, Priori A (2005) Multifocal motor neuropathy: current concepts and controversies. Muscle Nerve 31: Servioli L, Pérez C, Consani S, Suárez A, Sehabiaga G, Collazo C, Catalá G (2007) Prevalence and characteristics of immunomediated neuropathies in a group of patients with autoimmune diseases. J Clin Neuromuscul Dis 9(2): Sobue G, Nakao N, Kumazawa K, Mitsuma T (1989) Migrating multiple mononeuritis and nonsystemic angitis. Rinsho Shinkeigaku 29(10): Vrancken AF, Franssen H, Wokke JH, Teunissen LH, Notermans NC (2002) Chronic Idiopathic Axonal Polyneuropathy and succesful aging of the peripheral nervous system. Arch Neur 59: Wartenberg R (1958) Migrant sensory neuritis, a clinical study with review of literature. Oxford University Press, New York, pp Zifko UA, Hahn AF (1997) Migrant sensory neuropathy; report of 5 cases and review of literature. J Periph Nerv System 2(3):
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment
 Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment 7 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, HW Van Es, LH Van den Berg Annals of Neurology 2000;
Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment 7 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, HW Van Es, LH Van den Berg Annals of Neurology 2000;
A/Professor Arun Aggarwal Balmain Hospital
 A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
Differential Diagnosis of Neuropathies and Compression. Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre
 Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Index. Note: Page numbers of article titles are in boldface type.
 Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
Making sense of Nerve conduction & EMG
 Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment
 Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment 11 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, LH Van den Berg
Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment 11 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, LH Van den Berg
Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes
 Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes 1 This lab involves the second section of the exercise Spinal Cord, Spinal Nerves, and the Autonomic Nervous System,
Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes 1 This lab involves the second section of the exercise Spinal Cord, Spinal Nerves, and the Autonomic Nervous System,
Diagnostic investigation of patients with chronic polyneuropathy: evaluation of a clinical guideline
 J Neurol Neurosurg Psychiatry 2001;71:205 209 205 Department of Neurology, Academic Medical Centre, University of Amsterdam, PO Box 22700, 1100 DE Amsterdam, The Netherlands N R Rosenberg P Portegies M
J Neurol Neurosurg Psychiatry 2001;71:205 209 205 Department of Neurology, Academic Medical Centre, University of Amsterdam, PO Box 22700, 1100 DE Amsterdam, The Netherlands N R Rosenberg P Portegies M
Sensory mononeuritis: differentiating pure neural leprosy from non-systemic vasculitic neuropathy
 Lepr Rev (2017) 88, 274 279 CASE REPORT Sensory mononeuritis: differentiating pure neural leprosy from non-systemic vasculitic neuropathy PINELOPI TSOUNI*, JOHANNES ALEXANDER LOBRINUS**, ANDREAS J. STECK*
Lepr Rev (2017) 88, 274 279 CASE REPORT Sensory mononeuritis: differentiating pure neural leprosy from non-systemic vasculitic neuropathy PINELOPI TSOUNI*, JOHANNES ALEXANDER LOBRINUS**, ANDREAS J. STECK*
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists
 Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
For convenience values outside the normal range are bolded. Normal values for the specified patient are stated below the tables.
 Case tudy 8 or convenience values outside the normal range are bolded. Normal values for the specified patient are stated below the tables. History: 60 year-ol man with a history of left hand weakness
Case tudy 8 or convenience values outside the normal range are bolded. Normal values for the specified patient are stated below the tables. History: 60 year-ol man with a history of left hand weakness
Motor and sensory nerve conduction studies
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
Treatment of multifocal motor neuropathy with interferon-β1a
 Treatment of multifocal motor neuropathy with interferon-β1a 12 MMN RM Van den Berg-Vos, LH Van den Berg, H Franssen, PA Van Doorn, ISJ Martina, JHJ Wokke Adapted from Neurology 2000; 54: 1518-1521. Chapter
Treatment of multifocal motor neuropathy with interferon-β1a 12 MMN RM Van den Berg-Vos, LH Van den Berg, H Franssen, PA Van Doorn, ISJ Martina, JHJ Wokke Adapted from Neurology 2000; 54: 1518-1521. Chapter
Electrodiagnostics for Back & Neck Pain. Steven Andersen, MD Providence Physiatry Clinic
 Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
Comparison of Sudomotor and Sensory Nerve Testing in Painful Sensory Neuropathies
 138 Original Article Comparison of Sudomotor and Sensory Nerve Testing in Painful Sensory Neuropathies James M. Killian, MD,* Shane Smyth, MD,* Rudy Guerra, PhD, Ishan Adhikari, MD,* and Yadollah Harati,
138 Original Article Comparison of Sudomotor and Sensory Nerve Testing in Painful Sensory Neuropathies James M. Killian, MD,* Shane Smyth, MD,* Rudy Guerra, PhD, Ishan Adhikari, MD,* and Yadollah Harati,
Left peroneal neuropathy icd 10 code
 Cari untuk: Cari Cari Left peroneal neuropathy icd 10 code 2018 ICD-10 code for Injury of deep peroneal nerve at ankle and foot level, left leg is S94.22. Lookup the complete ICD 10 Code details for S94.22.
Cari untuk: Cari Cari Left peroneal neuropathy icd 10 code 2018 ICD-10 code for Injury of deep peroneal nerve at ankle and foot level, left leg is S94.22. Lookup the complete ICD 10 Code details for S94.22.
DIAGNOSIS OF DIABETIC NEUROPATHY
 DIAGNOSIS OF DIABETIC NEUROPATHY Dept of PM&R, College of Medicine, Korea University Dong Hwee Kim Electrodiagnosis ANS Clinical Measures QST DIAGRAM OF CASUAL PATHWAYS TO FOOT ULCERATION Rathur & Boulton.
DIAGNOSIS OF DIABETIC NEUROPATHY Dept of PM&R, College of Medicine, Korea University Dong Hwee Kim Electrodiagnosis ANS Clinical Measures QST DIAGRAM OF CASUAL PATHWAYS TO FOOT ULCERATION Rathur & Boulton.
peripheral neuropathy peripheral neuropathy neuropathy peripheral neuropathy neuropathic foot heel Bilateral foot pain Bilateral heel pain bilateral
 Peripheral neuropathy (PN) is damage to or disease affecting nerves, which may impair sensation, movement, gland or organ function, or other aspects of health. The 2018 edition of ICD-10-CM G62.9. Auditory
Peripheral neuropathy (PN) is damage to or disease affecting nerves, which may impair sensation, movement, gland or organ function, or other aspects of health. The 2018 edition of ICD-10-CM G62.9. Auditory
Table 1: Nerve Conduction Studies (summarised)
 Table 1: Nerve Conduction Studies (summarised) Sensory nerve conduction 1 week* 3 months Superficial radial sensory Normal, symmetric SNAP and CV No change Median to digit II Normal, symmetric SNAP and
Table 1: Nerve Conduction Studies (summarised) Sensory nerve conduction 1 week* 3 months Superficial radial sensory Normal, symmetric SNAP and CV No change Median to digit II Normal, symmetric SNAP and
ACUTE SYMMETRICAL MOTOR NEUROPATHY IN DIABETES MELLITUS
 Prize-Winning Paper Summary ACUTE SYMMETRICAL MOTOR NEUROPATHY IN DIABETES MELLITUS A distinct clinical entity M. Gourie Devi* The main clinical features in 12 patients with acute motor neuropathy associated
Prize-Winning Paper Summary ACUTE SYMMETRICAL MOTOR NEUROPATHY IN DIABETES MELLITUS A distinct clinical entity M. Gourie Devi* The main clinical features in 12 patients with acute motor neuropathy associated
Clinical and Electrophysiological Abnormalities amongst the Patients of Diabetic Truncal Polyneuropathy
 Original Article GCSMC J Med Sci Vol (VI) No (II) July-December 2017 Clinical and Electrophysiological Abnormalities amongst the Patients of Diabetic Truncal Polyneuropathy Chilvana Patel*, Surya Murthy
Original Article GCSMC J Med Sci Vol (VI) No (II) July-December 2017 Clinical and Electrophysiological Abnormalities amongst the Patients of Diabetic Truncal Polyneuropathy Chilvana Patel*, Surya Murthy
A STUDY OF ASSESSMENT IN PERIPHERAL NEUROPATHY IN PATIENTS WITH NEWLY DETECTED THYROID DISORDERS IN A TERTIARY CARE TEACHING INSTITUTE
 A STUDY OF ASSESSMENT IN PERIPHERAL NEUROPATHY IN PATIENTS WITH NEWLY DETECTED THYROID DISORDERS IN A TERTIARY CARE TEACHING INSTITUTE Rajan Ganesan 1, Marimuthu Arumugam 2, Arungandhi Pachaiappan 3, Thilakavathi
A STUDY OF ASSESSMENT IN PERIPHERAL NEUROPATHY IN PATIENTS WITH NEWLY DETECTED THYROID DISORDERS IN A TERTIARY CARE TEACHING INSTITUTE Rajan Ganesan 1, Marimuthu Arumugam 2, Arungandhi Pachaiappan 3, Thilakavathi
Pediatric Aspects of EDX
 Pediatric Aspects of EDX Albert C. Clairmont, MD Associate Professor-Clinical The Ohio State University February 25, 2013 Objectives Overview of Pediatric Electrodiagnosis (EDX) Understand the different
Pediatric Aspects of EDX Albert C. Clairmont, MD Associate Professor-Clinical The Ohio State University February 25, 2013 Objectives Overview of Pediatric Electrodiagnosis (EDX) Understand the different
Lower Limb Nerves. Clinical Anatomy
 Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Comparison of diabetes patients with demyelinating diabetic sensorimotor polyneuropathy to those diagnosed with CIDP
 Comparison of diabetes patients with demyelinating diabetic sensorimotor polyneuropathy to those diagnosed with CIDP Samantha K. Dunnigan 1, Hamid Ebadi 1, Ari Breiner 1, Hans D. Katzberg 1, Leif E. Lovblom
Comparison of diabetes patients with demyelinating diabetic sensorimotor polyneuropathy to those diagnosed with CIDP Samantha K. Dunnigan 1, Hamid Ebadi 1, Ari Breiner 1, Hans D. Katzberg 1, Leif E. Lovblom
Electrodiagnostic Measures
 Electrodiagnostic Measures E lectrodiagnostic assessments are sensitive, specific, and reproducible measures of the presence and severity of peripheral nerve involvement in patients with diabetes (1).
Electrodiagnostic Measures E lectrodiagnostic assessments are sensitive, specific, and reproducible measures of the presence and severity of peripheral nerve involvement in patients with diabetes (1).
Nerve Conduction Studies and EMG
 Nerve Conduction Studies and EMG Limitations of other methods of investigations of the neuromuscular system - Dr Rob Henderson, Neurologist Assessment of Weakness Thanks Peter Silburn PERIPHERAL NEUROPATHY
Nerve Conduction Studies and EMG Limitations of other methods of investigations of the neuromuscular system - Dr Rob Henderson, Neurologist Assessment of Weakness Thanks Peter Silburn PERIPHERAL NEUROPATHY
NEUROPATHY IN PERIPHERAL VASCULAR DISEASE 1
 267 616.833-02:616.13-005 NEUROPATHY IN PERIPHERAL VASCULAR DISEASE 1 Its Bearing on Diabetic Neuropathy BY E. C. HUTCHINSON AND L. A. LIVERSKDGE (From the Department of Neurology, Manchester Royal Infirmary)
267 616.833-02:616.13-005 NEUROPATHY IN PERIPHERAL VASCULAR DISEASE 1 Its Bearing on Diabetic Neuropathy BY E. C. HUTCHINSON AND L. A. LIVERSKDGE (From the Department of Neurology, Manchester Royal Infirmary)
Case Example. Nerve Entrapments in the Lower limb
 Nerve Entrapments in the Lower limb February, 2013 William S. Pease, M.D. Ernest W. Johnson Professor of PM&R Case Example CC: Right ankle dorsiflexion weakness with minimal paresthesias HPI: 87 year-old
Nerve Entrapments in the Lower limb February, 2013 William S. Pease, M.D. Ernest W. Johnson Professor of PM&R Case Example CC: Right ankle dorsiflexion weakness with minimal paresthesias HPI: 87 year-old
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM. Andrzej Sladkowski
 Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
CIDP + MMN - how to diagnose and treat. Dr Hadi Manji
 CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
Kim Chong Hwa MD,PhD Sejong general hospital, Division of endocrine & metabolism
 Kim Chong Hwa MD,PhD Sejong general hospital, Division of endocrine & metabolism st1 Classification and definition of diabetic neuropathies Painful diabetic peripheral neuropathy Diabetic autonomic neuropathy
Kim Chong Hwa MD,PhD Sejong general hospital, Division of endocrine & metabolism st1 Classification and definition of diabetic neuropathies Painful diabetic peripheral neuropathy Diabetic autonomic neuropathy
Nerve Site Latency ms Amplitude mv Distance mm Conduction Velocity m/s
 Clinical Electrophysiology Instructions and Sample Reports NCS/EMG REPORT Date: August 2007 Reason for Electrophysiologic Referral: Bilateral upper extremity pain and numbness. History: 59 year-old female
Clinical Electrophysiology Instructions and Sample Reports NCS/EMG REPORT Date: August 2007 Reason for Electrophysiologic Referral: Bilateral upper extremity pain and numbness. History: 59 year-old female
The Role of Hyperlipidemia on Nerve Conduction. Abdul Raheem H Dawoud, MB,ChB, Board* Shaymaa J Al Shareefi, MB,ChB, MSc* Hedef D El Yassin, PhD, **
 Bahrain Medical Bulletin, Vol. ٣٠, No. ٢, June ٢٠٠٨ The Role of Hyperlipidemia on Nerve Conduction Abdul Raheem H Dawoud, MB,ChB, Board* Shaymaa J Al Shareefi, MB,ChB, MSc* Hedef D El Yassin, PhD, ** Background:
Bahrain Medical Bulletin, Vol. ٣٠, No. ٢, June ٢٠٠٨ The Role of Hyperlipidemia on Nerve Conduction Abdul Raheem H Dawoud, MB,ChB, Board* Shaymaa J Al Shareefi, MB,ChB, MSc* Hedef D El Yassin, PhD, ** Background:
Clinical and electrophysiologic features of childhood Guillain-Barré syndrome in Northeast China
 Journal of the Formosan Medical Association (2014) 113, 634e639 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical and electrophysiologic features
Journal of the Formosan Medical Association (2014) 113, 634e639 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical and electrophysiologic features
Anatomy MCQs Week 13
 Anatomy MCQs Week 13 1. Posterior to the medial malleolus of the ankle: The neurovascular bundle lies between Tibialis Posterior and Flexor Digitorum Longus The tendon of Tibialis Posterior inserts into
Anatomy MCQs Week 13 1. Posterior to the medial malleolus of the ankle: The neurovascular bundle lies between Tibialis Posterior and Flexor Digitorum Longus The tendon of Tibialis Posterior inserts into
ORIGINAL ARTICLE. STUDY OF CLINICO ELECTROPHYSIOLOGICAL PROFILE OF DIABETIC NEUROPATHY Sachin. G. J, Ravi Vaswani, Shilpa. B.
 STUDY OF CLINICO ELECTROPHYSIOLOGICAL PROFILE OF DIABETIC NEUROPATHY Sachin. G. J, Ravi Vaswani, Shilpa. B. 1. Assistant Professor, Department of Medicine, Vijayanagara Institute of Medical Sciences. Bellary.
STUDY OF CLINICO ELECTROPHYSIOLOGICAL PROFILE OF DIABETIC NEUROPATHY Sachin. G. J, Ravi Vaswani, Shilpa. B. 1. Assistant Professor, Department of Medicine, Vijayanagara Institute of Medical Sciences. Bellary.
Electrophysiology of Brachial and Lumbosacral Plexopathies
 18 Electrophysiology of Brachial and Lumbosacral Plexopathies Juan A. Acosta and Elizabeth M. Raynor Summary Brachial and lumbosacral plexopathies represent a heterogeneous group of disorders including
18 Electrophysiology of Brachial and Lumbosacral Plexopathies Juan A. Acosta and Elizabeth M. Raynor Summary Brachial and lumbosacral plexopathies represent a heterogeneous group of disorders including
Distal chronic spinal muscular atrophy involving the hands
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Histological Spectrum of Pure Neuritic Leprosy:
 Department of Histopathology Postgraduate Institute of Medical Education & Research Chandigarh,India Histological Spectrum of Pure Neuritic Leprosy: Experience at Tertiary Care Centre Dr Uma Nahar INTRODUCTION
Department of Histopathology Postgraduate Institute of Medical Education & Research Chandigarh,India Histological Spectrum of Pure Neuritic Leprosy: Experience at Tertiary Care Centre Dr Uma Nahar INTRODUCTION
Evaluation of Peripheral Neuropathy. Evaluation of Peripheral Neuropathy - Introduction
 Evaluation of Peripheral Neuropathy Chris Edwards, MD Ochsner Neurology, Main Campus Evaluation of Peripheral Neuropathy - Introduction A very common complaint in the clinic Presentation is variable Multiple
Evaluation of Peripheral Neuropathy Chris Edwards, MD Ochsner Neurology, Main Campus Evaluation of Peripheral Neuropathy - Introduction A very common complaint in the clinic Presentation is variable Multiple
Tibial and Common Peroneal Nerve Compression in The Popliteal Fossa: A Case Report and Literature Review
 ISPUB.COM The Internet Journal of Plastic Surgery Volume 2 Number 1 Tibial and Common Peroneal Nerve Compression in The Popliteal Fossa: A Case Report and Literature D Reichner, G Evans Citation D Reichner,
ISPUB.COM The Internet Journal of Plastic Surgery Volume 2 Number 1 Tibial and Common Peroneal Nerve Compression in The Popliteal Fossa: A Case Report and Literature D Reichner, G Evans Citation D Reichner,
ACUTE AND CHRONIC NEUROPATHIES
 ACUTE AND CHRONIC NEUROPATHIES American College of Osteopathic Internists Internal Medicine Board Review Course 2018 April 25-29, 2018 Marriott Chicago Downtown Chicago, Illinois Scott Spradlin D.O.,FACP,FACOI
ACUTE AND CHRONIC NEUROPATHIES American College of Osteopathic Internists Internal Medicine Board Review Course 2018 April 25-29, 2018 Marriott Chicago Downtown Chicago, Illinois Scott Spradlin D.O.,FACP,FACOI
Comparison of Somatic and Sudomotor Nerve Fibers in Type 2 Diabetes Mellitus
 JCN Open Access pissn 1738-6586 / eissn 2005-5013 / J Clin Neurol 2017;13(4):366-370 / https://doi.org/10.3988/jcn.2017.13.4.366 ORIGINAL ARTICLE Comparison of Somatic and Sudomotor Nerve Fibers in Type
JCN Open Access pissn 1738-6586 / eissn 2005-5013 / J Clin Neurol 2017;13(4):366-370 / https://doi.org/10.3988/jcn.2017.13.4.366 ORIGINAL ARTICLE Comparison of Somatic and Sudomotor Nerve Fibers in Type
Numbness in right leg icd 10
 Search Search Numbness in right leg icd 10 A list of the most commonly used ICD -9 codes in Physical Medicine & Rehabilitation and Pain Management clinics. ICD - 10 codes will be slowly added over time.
Search Search Numbness in right leg icd 10 A list of the most commonly used ICD -9 codes in Physical Medicine & Rehabilitation and Pain Management clinics. ICD - 10 codes will be slowly added over time.
Chapter 13: The Spinal Cord and Spinal Nerves
 Chapter 13: The Spinal Cord and Spinal Nerves Spinal Cord Anatomy Protective structures: Vertebral column and the meninges protect the spinal cord and provide physical stability. a. Dura mater, b. Arachnoid,
Chapter 13: The Spinal Cord and Spinal Nerves Spinal Cord Anatomy Protective structures: Vertebral column and the meninges protect the spinal cord and provide physical stability. a. Dura mater, b. Arachnoid,
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases
 Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Assessment of the Brachial Plexus EMG Course CNSF Halifax Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University
 Assessment of the Brachial Plexus EMG Course CNSF Halifax 2018 Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University Angela Scott, Association of Electromyography Technologists of
Assessment of the Brachial Plexus EMG Course CNSF Halifax 2018 Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University Angela Scott, Association of Electromyography Technologists of
How to Think like a Neurologist Review of Exam Process and Assessment Findings
 Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
ORIGINAL COMMUNICATION. IVIg dose increase
 J Neurol (2009) 256:608 614 DOI 10.1007/s00415-009-0130-0 ORIGINAL COMMUNICATION Andreas Baumann Christian W. Hess Matthias Sturzenegger IVIg dose increase in multifocal motor neuropathy A prospective
J Neurol (2009) 256:608 614 DOI 10.1007/s00415-009-0130-0 ORIGINAL COMMUNICATION Andreas Baumann Christian W. Hess Matthias Sturzenegger IVIg dose increase in multifocal motor neuropathy A prospective
The Lower Limb VI: The Leg. Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa
 The Lower Limb VI: The Leg Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa Muscles of the leg Posterior compartment (superficial & deep): primary plantar flexors of the foot flexors of the toes Anterior compartment:
The Lower Limb VI: The Leg Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa Muscles of the leg Posterior compartment (superficial & deep): primary plantar flexors of the foot flexors of the toes Anterior compartment:
The Leg. Prof. Oluwadiya KS
 The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
Patogenesi e terapia della Neuropatia Motoria Multifocale
 26 Settembre 2014 Patogenesi e terapia della Neuropatia Motoria Multifocale Francesca Gallia Neurologia 2, Ist. Clin. Humanitas Rozzano, Milano Multifocal Motor Neuropathy Rare disorder characterized by:
26 Settembre 2014 Patogenesi e terapia della Neuropatia Motoria Multifocale Francesca Gallia Neurologia 2, Ist. Clin. Humanitas Rozzano, Milano Multifocal Motor Neuropathy Rare disorder characterized by:
Where should you palpate the pulse of different arteries in the lower limb?
 Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
Vasculitis of the peripheral nervous system
 4 rd Congress of the European Academy of Neurology Lisbon, Portugal, June 16-19, 2018 Teaching Course 5 Acute emergencies in neuromuscular disease - Level 2 Vasculitis of the peripheral nervous system
4 rd Congress of the European Academy of Neurology Lisbon, Portugal, June 16-19, 2018 Teaching Course 5 Acute emergencies in neuromuscular disease - Level 2 Vasculitis of the peripheral nervous system
Some observations we are making
 Some observations we are making The audience is very smart and they know how to diagnose a neuropathy. There is a standard workup that all patients seem to get: B12, folate, RPR, TSH prior to them being
Some observations we are making The audience is very smart and they know how to diagnose a neuropathy. There is a standard workup that all patients seem to get: B12, folate, RPR, TSH prior to them being
Compound Nerve Action Potential of Common Peroneal Nerve and Sural Nerve Action Potential in Common Peroneal Neuropathy
 J Korean Med Sci 2008; 23: 117-21 ISSN 1011-8934 DOI: 10.3346/jkms.2008.23.1.117 Copyright The Korean Academy of Medical Sciences Compound Nerve Action Potential of Common Peroneal Nerve and Sural Nerve
J Korean Med Sci 2008; 23: 117-21 ISSN 1011-8934 DOI: 10.3346/jkms.2008.23.1.117 Copyright The Korean Academy of Medical Sciences Compound Nerve Action Potential of Common Peroneal Nerve and Sural Nerve
A family study of Charcot-Marie-Tooth disease
 Joturnal of Medical Genetics, 1982, 19, 88-93 A family study of Charcot-Marie-Tooth disease A P BROOKS* AND A E H EMERY From the University Department of Human Genetics, Western General Hospital, Edinburgh
Joturnal of Medical Genetics, 1982, 19, 88-93 A family study of Charcot-Marie-Tooth disease A P BROOKS* AND A E H EMERY From the University Department of Human Genetics, Western General Hospital, Edinburgh
Nerve Conduction Study in Healthy Individuals: a Gender Based Study
 Original Article Nerve Conduction Study in Healthy Individuals: a Gender Based Study Dilip Thakur 1, BH Paudel 1, BK Bajaj 2, CB Jha 3 Department of Physiology 1 Internal Medicine 2 and Anatomy 3, BPKIHS
Original Article Nerve Conduction Study in Healthy Individuals: a Gender Based Study Dilip Thakur 1, BH Paudel 1, BK Bajaj 2, CB Jha 3 Department of Physiology 1 Internal Medicine 2 and Anatomy 3, BPKIHS
Disclosure. Entrapment Neuropathies - Overview. Common mononeuropathy sites. Definitions. Common mononeuropathy sites. Common mononeuropathy sites
 Disclosure Entrapment Neuropathies - Overview I receive compensation from Wiley- Blackwell publishers for my work as Editor-in-Chief of Muscle & Nerve Lawrence H. Phillips, II, MD Definitions Mononeuropathy:
Disclosure Entrapment Neuropathies - Overview I receive compensation from Wiley- Blackwell publishers for my work as Editor-in-Chief of Muscle & Nerve Lawrence H. Phillips, II, MD Definitions Mononeuropathy:
PNS and ANS Flashcards
 1. Name several SOMATIC SENSES Light touch (being touched by a feather), heat, cold, vibration, pressure, pain are SOMATIC SENSES. 2. What are proprioceptors; and how is proprioception tested? PROPRIOCEPTORS
1. Name several SOMATIC SENSES Light touch (being touched by a feather), heat, cold, vibration, pressure, pain are SOMATIC SENSES. 2. What are proprioceptors; and how is proprioception tested? PROPRIOCEPTORS
Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome
 Iranian Journal of Neurology Original Paper Iran J Neurol 2014; 13(3): 138-143 Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome Received: 9 Mar 2014 Accepted:
Iranian Journal of Neurology Original Paper Iran J Neurol 2014; 13(3): 138-143 Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome Received: 9 Mar 2014 Accepted:
Electrodiagnostic Variations in Guillain-Barré Syndrome - Retrospective Analysis of 95 Patients
 Original Article GCSMC J Med Sci Vol (VI) No (II) July-December 2017 Electrodiagnostic Variations in Guillain-Barré Syndrome - Retrospective Analysis of 95 Patients Chilvana Patel*, Surya Murthy Vishnubhakat**
Original Article GCSMC J Med Sci Vol (VI) No (II) July-December 2017 Electrodiagnostic Variations in Guillain-Barré Syndrome - Retrospective Analysis of 95 Patients Chilvana Patel*, Surya Murthy Vishnubhakat**
The Internist s Approach to Neuropathy
 The Internist s Approach to Neuropathy VOLKAN GRANIT, MD, MSC ASSISTANT PROFESSOR OF NEUROLOGY NEUROMUSCU LAR DIVISION UNIVERSITY OF MIAMI, MILLER SCHOOL OF MEDICINE RELEVANT DECLARATIONS Financial disclosures:
The Internist s Approach to Neuropathy VOLKAN GRANIT, MD, MSC ASSISTANT PROFESSOR OF NEUROLOGY NEUROMUSCU LAR DIVISION UNIVERSITY OF MIAMI, MILLER SCHOOL OF MEDICINE RELEVANT DECLARATIONS Financial disclosures:
Case 3. Your Diagnosis?
 Case 3 45 year-old presenting with a history of injury to the right shoulder whilst working in the freezing work. He was loading a sheep over an incline with his arm around the sheep. He felt pain in the
Case 3 45 year-old presenting with a history of injury to the right shoulder whilst working in the freezing work. He was loading a sheep over an incline with his arm around the sheep. He felt pain in the
Nerve Conduction Studies NCS
 Nerve Conduction Studies NCS Nerve conduction studies are an essential part of an EMG examination. The clinical usefulness of NCS in the diagnosis of diffuse and local neuropathies has been thoroughly
Nerve Conduction Studies NCS Nerve conduction studies are an essential part of an EMG examination. The clinical usefulness of NCS in the diagnosis of diffuse and local neuropathies has been thoroughly
The clinical spectrum of Malaysian patients with. Chronic inflammatory demyelinating polyneuropathy
 Neurology Asia 2004; 9 : 39 45 The clinical spectrum of Malaysian patients with chronic inflammatory demyelinating polyneuropathy Khean Jin GOH, Wai Keong NG, Nee Kong CHEW, Chong Tin TAN Division of Neurology,
Neurology Asia 2004; 9 : 39 45 The clinical spectrum of Malaysian patients with chronic inflammatory demyelinating polyneuropathy Khean Jin GOH, Wai Keong NG, Nee Kong CHEW, Chong Tin TAN Division of Neurology,
Nerve Conduction Studies NCS
 Nerve Conduction Studies NCS Nerve conduction studies are an essential part of an EMG examination. The clinical usefulness of NCS in the diagnosis of diffuse and local neuropathies has been thoroughly
Nerve Conduction Studies NCS Nerve conduction studies are an essential part of an EMG examination. The clinical usefulness of NCS in the diagnosis of diffuse and local neuropathies has been thoroughly
International Journal of Basic & Applied Physiology
 ELECTRODIAGNOSTIC FEATURES IN CLINICALLY SUSPECTED GUILLAIN BARRE SYNDROME Asha Shrivastava*, Rashmi Dave**, Sanjeev Shrivastava ***, Brajesh Sharma **** *Professor, ** JR III, *** Assistant Professor,
ELECTRODIAGNOSTIC FEATURES IN CLINICALLY SUSPECTED GUILLAIN BARRE SYNDROME Asha Shrivastava*, Rashmi Dave**, Sanjeev Shrivastava ***, Brajesh Sharma **** *Professor, ** JR III, *** Assistant Professor,
November 16-18, 2017 Hotel Monteleone New Orleans, LA. Provided by
 November 16-18, 2017 Hotel Monteleone New Orleans, LA Provided by Diabetic Neuropathy: A Global and Growing Problem John D. England, MD Louisiana State University Health Sciences Center School of Medicine
November 16-18, 2017 Hotel Monteleone New Orleans, LA Provided by Diabetic Neuropathy: A Global and Growing Problem John D. England, MD Louisiana State University Health Sciences Center School of Medicine
Zahid H. Bajwa, MD. Boston Headache Institute Boston PainCare HMS 2018
 Zahid H. Bajwa, MD Boston Headache Institute Boston PainCare HMS 2018 Zahid H. Bajwa, M.D. Director, Boston Headache Institute Director, Clinical Research, Boston PainCare ZBAJWA@BOSTONPAINCARE.COM BOARD
Zahid H. Bajwa, MD Boston Headache Institute Boston PainCare HMS 2018 Zahid H. Bajwa, M.D. Director, Boston Headache Institute Director, Clinical Research, Boston PainCare ZBAJWA@BOSTONPAINCARE.COM BOARD
A Tale of Five Demyelinating Neuropathies
 Objectives A Tale of Five Demyelinating Neuropathies Tahseen Mozaffar, MD FAAN Professor and Vice Chair of Neurology Director, UC Irvine-MDA ALS and Neuromuscular Center Director, Neurology Residency Training
Objectives A Tale of Five Demyelinating Neuropathies Tahseen Mozaffar, MD FAAN Professor and Vice Chair of Neurology Director, UC Irvine-MDA ALS and Neuromuscular Center Director, Neurology Residency Training
Case Report. Annals of Rehabilitation Medicine INTRODUCTION
 Case Report Ann Rehabil Med 2018;42(3):483-487 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2018.42.3.483 Annals of Rehabilitation Medicine Diagnosis of Pure Ulnar Sensory Neuropathy Around
Case Report Ann Rehabil Med 2018;42(3):483-487 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2018.42.3.483 Annals of Rehabilitation Medicine Diagnosis of Pure Ulnar Sensory Neuropathy Around
Motor, Reflex, Coordination and Sensory Screening Examination
 Motor, Reflex, Coordination and Sensory Screening Examination K. Jeffrey Miller, DC, DABCO Miller 2002 2002-2012 K Jeffrey Miller DC DABCO Motor Function Neurological Testing Handedness Right or Left Handed
Motor, Reflex, Coordination and Sensory Screening Examination K. Jeffrey Miller, DC, DABCO Miller 2002 2002-2012 K Jeffrey Miller DC DABCO Motor Function Neurological Testing Handedness Right or Left Handed
Bilateral nerve damage icd 10
 Bilateral nerve damage icd 10 The Borg System is 100 % Bilateral nerve damage icd 10 Anterior interosseous nerve syndrome; Neuropathy (nerve damage), suprascapular; Paralysis of phrenic nerve; Posterior
Bilateral nerve damage icd 10 The Borg System is 100 % Bilateral nerve damage icd 10 Anterior interosseous nerve syndrome; Neuropathy (nerve damage), suprascapular; Paralysis of phrenic nerve; Posterior
Jonathan Katz, MD CPMC
 Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC First, a bit of background Classic CIDP--TREATABLE MADSAM/Asymmetric Neuropathy Chronic Length Dependent Neuropathy-
Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC First, a bit of background Classic CIDP--TREATABLE MADSAM/Asymmetric Neuropathy Chronic Length Dependent Neuropathy-
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
Synapse Homework. Back page last question not counted. 4 pts total, each question worth 0.18pts. 26/34 students answered correctly!
 Synapse Homework Back page last question not counted 26/34 students answered correctly! 4 pts total, each question worth 0.18pts Business TASS hours extended! MWF 1-2pm, Willamette 204 T and Th 9:30-10:30am,
Synapse Homework Back page last question not counted 26/34 students answered correctly! 4 pts total, each question worth 0.18pts Business TASS hours extended! MWF 1-2pm, Willamette 204 T and Th 9:30-10:30am,
Epidermal Nerve Fiber and Schwann cell densities in the distal leg of Nine-banded Armadillos with Experimental Leprosy neuropathy
 Epidermal Nerve Fiber and Schwann cell densities in the distal leg of Nine-banded Armadillos with Experimental Leprosy neuropathy Gigi J Ebenezer 1 Richard Truman 2 David Scollard 2 Michael Polydefkis
Epidermal Nerve Fiber and Schwann cell densities in the distal leg of Nine-banded Armadillos with Experimental Leprosy neuropathy Gigi J Ebenezer 1 Richard Truman 2 David Scollard 2 Michael Polydefkis
Jose Santiago Campos, MD and Eric L. Altschuler, MD, PhD
 Numb Toes Jose Santiago Campos, MD and Eric L. Altschuler, MD, PhD No one involved in the planning of this CME activity have anyy relevant financial relationships to disclose. Authors/faculty have nothingg
Numb Toes Jose Santiago Campos, MD and Eric L. Altschuler, MD, PhD No one involved in the planning of this CME activity have anyy relevant financial relationships to disclose. Authors/faculty have nothingg
Ahmed Abbas, Mark Cook, Liong Hiew Fu, Alistair Lewthwaite, Colin Shirley, Yusuf A. Rajabally
 2016, Elsevier. Licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International http://creativecommons.org/licenses/by-nc-nd/4.0/ Accepted Manuscript A case of POEMS mimicking
2016, Elsevier. Licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International http://creativecommons.org/licenses/by-nc-nd/4.0/ Accepted Manuscript A case of POEMS mimicking
Located Deep to Flexor Retinaculum on medial aspect of ankle. Posterior to Posterior Tibial Artery. Tom, Dick, and Very Nervous Harry
 ANKLE BLOCK ANESTHESIA GREGORY CLARK D.P.M. HEAD, SECTION OF PODIATRY SCRIPPS CLINIC LA JOLLA, CALIFORNIA A METHOD BY WHICH ONE MAY PROVIDE AN ANESTHETIC BLOCK TO THE FOOT OR ANKLE WITH A MINIMUM OF PATIENT
ANKLE BLOCK ANESTHESIA GREGORY CLARK D.P.M. HEAD, SECTION OF PODIATRY SCRIPPS CLINIC LA JOLLA, CALIFORNIA A METHOD BY WHICH ONE MAY PROVIDE AN ANESTHETIC BLOCK TO THE FOOT OR ANKLE WITH A MINIMUM OF PATIENT
Diabetic Neuropathy. Nicholas J. Silvestri, M.D.
 Diabetic Neuropathy Nicholas J. Silvestri, M.D. Types of Neuropathies Associated with Diabetes Mellitus p Chronic distal sensorimotor polyneuropathy p Focal compression neuropathies p Autonomic neuropathy
Diabetic Neuropathy Nicholas J. Silvestri, M.D. Types of Neuropathies Associated with Diabetes Mellitus p Chronic distal sensorimotor polyneuropathy p Focal compression neuropathies p Autonomic neuropathy
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
ORIGINAL CONTRIBUTION. Efficacy of Intravenous Immunoglobulin in Patients With IgG Monoclonal Gammopathy and Polyneuropathy
 ORIGINAL CONTRIBUTION Efficacy of Intravenous Immunoglobulin in Patients With IgG Monoclonal Gammopathy and Polyneuropathy Kenneth C. Gorson, MD; Allan H. Ropper, MD; David H. Weinberg, MD; Robert Weinstein,
ORIGINAL CONTRIBUTION Efficacy of Intravenous Immunoglobulin in Patients With IgG Monoclonal Gammopathy and Polyneuropathy Kenneth C. Gorson, MD; Allan H. Ropper, MD; David H. Weinberg, MD; Robert Weinstein,
Compound Action Potential, CAP
 Stimulus Strength UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PHYSIOLOGY & BIOCHEMISTRY INTRODUCTION TO NEUROPHYSIOLOGY Spring, 2013 Textbook of Medical Physiology by: Guyton & Hall, 12 th edition
Stimulus Strength UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PHYSIOLOGY & BIOCHEMISTRY INTRODUCTION TO NEUROPHYSIOLOGY Spring, 2013 Textbook of Medical Physiology by: Guyton & Hall, 12 th edition
This is a repository copy of Anti-MAG negative distal acquired demyelinating symmetric neuropathy in association with a neuroendocrine tumor..
 This is a repository copy of Anti-MAG negative distal acquired demyelinating symmetric neuropathy in association with a neuroendocrine tumor.. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk//
This is a repository copy of Anti-MAG negative distal acquired demyelinating symmetric neuropathy in association with a neuroendocrine tumor.. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk//
Icd 10 code neuropathy
 Icd 10 code neuropathy Hereditary and idiopathic neuropathy, unspecified. 2016 2017 2018 Billable/Specific Code. G60.9 is a billable/specific ICD - 10 -CM code that can be used to indicate a. ICD-10 Online
Icd 10 code neuropathy Hereditary and idiopathic neuropathy, unspecified. 2016 2017 2018 Billable/Specific Code. G60.9 is a billable/specific ICD - 10 -CM code that can be used to indicate a. ICD-10 Online
Evaluation of Tingling and Numbness in the Upper Extremities
 Evaluation of Tingling and Numbness in the Upper Extremities DR. W. ANTHONY FRISELLA M.D. ADVANCED BONE & JOINT, ST CHARLES MO MONA 2018 Overview Polyneuropathy Compressive nerve lesions Carpal tunnel
Evaluation of Tingling and Numbness in the Upper Extremities DR. W. ANTHONY FRISELLA M.D. ADVANCED BONE & JOINT, ST CHARLES MO MONA 2018 Overview Polyneuropathy Compressive nerve lesions Carpal tunnel
Nerves of Upper limb. Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh
 Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
ORIGINAL CONTRIBUTION. Small-Fiber Neuropathy/Neuronopathy Associated With Celiac Disease
 ORIGINAL CONTRIBUTION Small-Fiber Neuropathy/Neuronopathy Associated With Celiac Disease Skin Biopsy Findings Thomas H. Brannagan III, MD; Arthur P. Hays, MD; Steven S. Chin, MD, PhD; Howard W. Sander,
ORIGINAL CONTRIBUTION Small-Fiber Neuropathy/Neuronopathy Associated With Celiac Disease Skin Biopsy Findings Thomas H. Brannagan III, MD; Arthur P. Hays, MD; Steven S. Chin, MD, PhD; Howard W. Sander,
Median-ulnar nerve communications and carpal tunnel syndrome
 Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 982-986 Median-ulnar nerve communications and carpal tunnel syndrome LUDWIG GUTMANN From the Department of Neurology, West Virginia University,
Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 982-986 Median-ulnar nerve communications and carpal tunnel syndrome LUDWIG GUTMANN From the Department of Neurology, West Virginia University,
Peripheral Nerve Problems
 UW MEDICINE PATIENT EDUCATION Peripheral Nerve Problems How they develop and ways to treat them This handout explains how nerves work, what happens when they are injured, and how peripheral nerve problems
UW MEDICINE PATIENT EDUCATION Peripheral Nerve Problems How they develop and ways to treat them This handout explains how nerves work, what happens when they are injured, and how peripheral nerve problems
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS
 HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
 doi: 10.2169/internalmedicine.1723-18 http://internmed.jp CASE REPORT Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
doi: 10.2169/internalmedicine.1723-18 http://internmed.jp CASE REPORT Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
CAPTURING CASES OF DISTAL SYMMETRIC POLYNEUROPATHY IN A COMMUNITY
 CAPTURING CASES OF DISTAL SYMMETRIC POLYNEUROPATHY IN A COMMUNITY BRIAN CALLAGHAN, MD, 1 KEVIN KERBER, MD, 1 RUTH LONGORIA, AA, 1 EVA FELDMAN, MD, PhD, 1 and LYNDA LISABETH, PhD 2 1 Department of Neurology,
CAPTURING CASES OF DISTAL SYMMETRIC POLYNEUROPATHY IN A COMMUNITY BRIAN CALLAGHAN, MD, 1 KEVIN KERBER, MD, 1 RUTH LONGORIA, AA, 1 EVA FELDMAN, MD, PhD, 1 and LYNDA LISABETH, PhD 2 1 Department of Neurology,
Leg. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
Peripheral Nerve Problems
 Patient Education Peripheral Nerve Problems How they develop and ways to treat them This handout provides general information about how nerves work, what happens when they are injured, and how peripheral
Patient Education Peripheral Nerve Problems How they develop and ways to treat them This handout provides general information about how nerves work, what happens when they are injured, and how peripheral
~, /' ~::'~ EXTENSOR HALLUCIS LONGUS. Leg-anterolateral :.:~ / ~\,
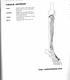 TIBIALIS ANTERIOR Lateral condyle of tibia, upper half of lateral surface of tibia, interosseous membrane Medial side and plantar surface of medial cuneiform bone, and base of first metatarsal bone Dorsiflexes
TIBIALIS ANTERIOR Lateral condyle of tibia, upper half of lateral surface of tibia, interosseous membrane Medial side and plantar surface of medial cuneiform bone, and base of first metatarsal bone Dorsiflexes
