American Cutaneous Leishmaniasis
|
|
|
- Jemimah Bradford
- 5 years ago
- Views:
Transcription
1 J R Army Med Corps, 1983; 129: Maj K Freeman MB, MRCP, RAMC Honorary Senior Registrar, Department of Dermatology Royal Devon and Exeter Hospital SUMMARY: This review outlines the present knowledge of American cutaneous leishmaniasis, a disease which, owing to the increase in international travel, is being seen with increasing frequency in Europe and North America. A knowledge of this disease is of particular importance to the military medical officer as in recent years approximately one-hundred and fifty cases of leishmaniasis have been seen in British troops who have served in Belize. Leishmania braziliensis sp. have been i.. olated from a number of these cases. Organisms of this complex had not previously been recorded in Belize and the Army Medical Services are therefore in a unique position to study this disease, as well as having a responsibility to ensure its correct management. Geography The disease is endemic in a large area of the Americas on either side of the equator, from approximately 25 N to approximately 30 0 S 1 It has been reported from Mexico, all of the Central American countries and every South American country with the exception of Chile. Autochthonous cases were thought not to occur in the United States, but in 1976, three such cases were reported 2 In man the incubation period for the disease is quite variable, usually between two and ten weeks, but occasionally several months. It is hence possible that individuals may present with the disease in countries where it is not endemic a considera ble time after leaving the area where they acquired their infection. Parasitology The disease is caused by a protozoa of the Leishmania genus, a member of the Trypanosomidae family, and is transmitted by the bite of an infected female phlebotomine sandily. In the gut of the insect vector the parasite is in the promastigote form, a motile spiral organism 15-40/L in length, with a single anterior flagellum. Multiplication is by binary fission. Promastigotes migrate from the gut of the sandfly to the buccal cavity and can subsequently be injected into the vertebrate host when the sandfly takes another blood meal. The organisms then invade local tissue histiocytes, where they change into non-flagellate amastigote forms. Multiplication within the vertebrate host is also by binary fission to give further amastigotes which are round or oval, measuring 2-5/L in length by 2-3/L in width. Sandflies feeding on an infected animal may acquire,infection with amastigotes which then develop into promastigotes in the gut and complete the parasite life cycle. The species of Leishmania responsible for cutaneous disease do not cause American viscenll. leishmaniasis, which is due to the related species L. chagasi and is less common than the cutaneous forms; numerous cases have been reported from Brazil and less from other American countries. Insect vectors and animals hosts Each species or sub species of Leishmania is transmitted between animals, and to man, by only a very limited number of phlebotomine sandfly species 3, despite numerous other species of sandfly feeding on both man and the relevant animal hosts 4 Sandflies usually bite between sunset and dawn 5, although they may bite at other times if disturbed from their resting sites amongst the forest litter on the ground". Sandflies have a limited flight range 7 and within their forest habitat the number of sandflies varies markedly from place to place. There are also marked variations in their populations with season 8 - in most areas the numbers are greatest during the rainy seasons although their numbers may decline with extremely high rainfall. Cutaneous leishmaniasis is a zoonosis, with the usual cycle being transmission of the disease from an infected animal to a healthy one by the sandfly. Man is only an 'accidental' host, when he is exposed to the bite of the infected sandfly and is usually the end of the transmission chain, playing no important part in the maintenance of the Leishmania species. Not all Leishmania can be transmitted to man. Small forest rodents such as the tree rat, white footed mouse and spiny pocket mouse 9 are the principal
2 161\ animal hosts for most species. Leishmania braziliensis infection of dogs has been described in Panama 10, but the sloths are the major hosts to Leishmania braziliensis panamensis. In both rodent and mammal hosts leishmanial infection may produce only a few indistinct skin lesions 1!, in rodents typically of the tail, and in other mammals around the ears or nose. Clinical features of human disease After an incubation period varying from two weeks to many months a small blue-red papule develops at the site of a sandfly bite. These lesions occur predominan.tly on exposed areas as the sandfly is unable to bite through clothing. Lesions of the head and neck, ears, arms and hands are therefore common, whilst lesions of the trunk are unusual. The initial lesions are single or few in number. The papule increases in size over ensuing weeks to form a nodule or plaque of between one half and twelve centimetres diameter. Superficial crusting may be present at the centre of relatively early lesions, but frank ulceration subsequently develops and a crust of dried exudate and pus, due to secondary bacterial infection,usually then forms over the granulomatous base. The ulcer has a raised, infiltrated blue-red border and is relatively painless. Not all lesions progress to ulceration, they may remain as papules, nodules, or plaques. Slight lymphangitis and lymphadenitis in the area draining the lesion is not uncommon. Some species of leishmania have a tendency to lymphatic or haematogenous spread to cause metastatic secondary lesions. In the majority of cases the natural course is for the skin lesion to eventually heal, leaving a characteristic scar which is slightly depressed, smooth, atrophic and dyschromic. Infections due to L. braziliensis braziliensis may lead to,the development of late nasopharyngeal lesions, espundia, as discussed below. Classification of Leishmania and features of the different species In the past various classifications 12 based on clinical features, geographic location and epidemiological findings have been employed. This has led to a proliferation of frequently overlapping and confusing terms which are all the more inappropriate as the disease is a zoononis with man only an 'accidental' host. Most workers now accept Lainson and Shaws 13 trinomial system of classification which divides the organisms into the mexicana complex and the braziliensis complex, each of which is then further divided into related species and sub species. Recent laboratory studies of the detailed morphology of the organisms 14, 15 of their DNA buoyant densities and electrophoresis of their enzymes 16, 17 support this classification and give more objective assessments of the parasites. The L mexicana complex The parasites of this complex multiply rapidly in the fore and mid gut of vector sandflies. On hamster inoculation they multiply rapidly1s to produce histiocytomata, with frequent metastatic spread. Growth on culture media is easy and rapid. Human disease due to members of this complex is frequently self-limiting. L mexicana Imexicana Infection with this organism occurs in Belize, Guatemala, parts of Mexico and probably other Central American countries. The principal insect vector is Lutzomyia olmeca olmeca. The rodent hosts and infected sandflies have a habitat confined to forest areas, hence human infection is confined almost exclusively to those who work and, or, live in the foresf9. Amongst native Belizians infection occurs mainly in mahogany cutters and chicleros. Chicleros tap the 'sapodilla' trees (Achras sapota) for the crude chewing gum latex 'chicle.' Both groups of workers spend many months of each year living and working in the forest. Clinically apparent infection is not common among women and children, even those living in villages adjacent to the forest. The reason for the high incidence of disease amongst the chicleros and its low incidence in the villagers is that the vector sandfly Lutzomyia olmeca olmeca does not readily bite man and prolonged exposure in the forest is therefore required for infection to occur. The classic lesions due to this species of Leishmania are the bay sore and the chiclero's ear20. The term bay sore was first used during the reign of Queen Elizabeth I to describe the ulcerated skin lesions which severely affected the early European colonists opening up the logging industry around the Bay of Honduras. Chicleros ear refers to the chronic cartilagenous destructive lesions which may develop when the infection involves the ear. Lainson and Strangways Dixon 21 report that 40% of the lesions they studied in Belize affected the ears, whilst 28 % involved the hands and arms. Lesions of the legs and torso are uncommon. The ear is an area which is seldom covered when other areas of the body are so protected, this will increase the risk of sandfly bites occurring on the ear rather than elsewhere, as the sandfly is unable to bite through clothing. Ear lesions may be diagnosed more frequently than lesions on other parts of the body as, unlike lesions of other areas, they do not tend to heal spontaneously, but rather progress to chronic destruction of the pinna causing considerable deformity. The
3 K Freeman relatively poor blood supply to the cartilage of the ear may facilitate the development of chronic lesions by leaving organisms here relatively inaccessible to the effects of cell mediated immunity. The lesions are usually single and in sites other than the ear are usually self limiting. An ulcer may develop to several centimetres in diameter before starting to resolve and although most lesions start to heal after a period of weeks, some persist for months or years. The author has seen one case in a former mahogany cutter where extensive ulceration of the arm had been present for seventeen years and showed no sign of healing. If more than one lesion is present they are usually few,in number and morphologically very similar, such multiple lesions are thought to be due to multiple bites within a short time causing separate primary lesions rather than to spread from a single primary lesion. Neither nasopharyngeal nor visceral lesions develop. L. mexicana amazonensis This species occurs in the Amazon basin, certain other parts of Brazil and in Trinidad. The vector Lutzomyia flaviscutellata seldom bites man 22, but when human infection does occur it usually follows a similar pattern to that due to L. mexicana mexicana with the exception that there is no prediliction for the ears. Diffuse cutaneous leishmaniasis developed ill six of twenty patients infected with this species who were studied in Brazil"". In this form of the disease numerous papules, nodules and plaques develop over the body surfaces, ulceration is uncommon. Parasites are exceedingly numerous within the lesions and there is specific anergy to the intradermal Montenegro test (vide infra). The multiple lesions are due to haematogeclous spread of the parasite which may be found in the blood. Internal organs are not involved and nasopharyngeal lesions do not occur. Response to therapy is poor, with frequent relapses 24 It has been suggested that the development of diffuse cutaneous leishmaniasis is due to a failure of the hosts cell mediated immunity to the parasite 25, 26, 27. This hypothesis does not however explain why internal organs are spared when the parasite is present in the blood stream. There is increasing evidence that the normal vertebrate host response to infection with Leishmania requires the participation of both cell mediated and humoral immunity28, and it is possible that failure of integrationof these responses within the dermis leads to diffuse" anergic disease. L. mexican'a venezuelensis L. mexicana venezuelelensis is the organism responsible for diffuse cutaneous leishmaniasis in 169 Venezuela. It is very similar to L. mexicana amazonensis and almost certainly causes simple cutaneous lesions as well as the diffuse disease. L. mexicana garnhami This species occurs in the humid zone of the Venezuelan Andes up to a height of 1,800" metres. It produces spontaneously healing cutaneou$lesions which are usually single. Late nasopharyngeal involvement does not occur. The vector is thought to be Lutzomyia townsendi. The L. braziliensis complex Parasites of this complex develop in the fore, mid and hind gut of the vector sandflies. Growth on hamster inoculation is slow, producing small swellings with few detectable parasites and no metastatic spread. Growth on culture media is slow and difficult. Human disease due to this group may present with single or multiple skin lesions which may be very destructive, nasopharyngeal involvement may develop subsequently. L. braziliensis braziliensis Most cases due to this organism occur in Brazil. The principal vector Psychodopygus wellcomei bites man during the daylight hours as well as at night. The primary lesions are usually few in number but they are frequently large, chronic and destructive ulcers. Tt is usually possible to demonstrate only a few parasites in the lesion and there is a very vigorous tisue reaction. Late metastasis to nasopharyngeal tissues, espundia, is common; the incidence varying from one region to another. In Venezuela it is said to occur in between twelve and thirty-four per cent of cases whilst in Brazil an incidence of eighty per cent has been reported. The mechanism of development of these late lesions is not established - it presumably reflects haematogenous or lymphatic dissemination of the parasites but the reason for the localization of the lesions remains unclear. Leishmania are present in the nasopharyngeal lesions in their early stages but become progressively more difficult to demonstrate as the condition progresses. There is usually an asymptomatic period of three to ten years between the primary skin lesion and the late nasopharyngeal lesions developing. The reason for this delay is unknown. In Brazil some patients develop the nasopharyngeal lesions within one year of their primary lesion developing, but only some 10% of cases of espundia have an active primary lesion at the time of presentation with nasopharyngeal disease. The mucosa overlying the anterior cartilagenous part of the nasal septum becomes inflamed. The patient usually notices some nasal dis-
4 170 charge and small nose-bleeds may occur on blowing the nose. Ulceration usually follows within a short time, destroying mucosa, cartilage and soft tissues but initially leaving bone intact. The lesion then extends progressively more deeply into surrounding tissues causing massive destruction of the nasal fossae, palate, fauces, pharynx tongue, gums and floor of mouth. Further spread may involve the trachea, bronchi and larynx, involvement of which causes marked change in the voice. Secondary bacterial infection occurs almost invariably. Gross disfigurement develops and severely compromises normal speech, feeding and breathing. Wasting and malnutrition due to feeding difficulties develop and death due to respiratory infection may ensue. Late lesions of the genitalia and rectum occur, but less frequently than do nasopharyngeal lesions. These late lesions may prove very difficult to treat. L. braziliensis guyanensis This species occurs in Guyana, Surinam and Brazil. The principal vector is Lutzomyia umbratalis. There is a tendency for Leishmania from the pr,imary ulcer to metastasise along the lymphatics draining that area to give lymphadenitis, nodules or further ulcers. Metastasies to give numerous ulcers widely distributed over the body, 'pian-bois', is not uncommon. Only a few parasites can be isolated from lesions. The species does not cause nasopharyngeal disease. L. braziliensis panamensis Causes simple cutaneous leishmaniasis in Panama; sloths are the major animal host. L. peruviana Differs markedly from other forms of American cutaneous leishmaniasis in that it occurs on the barren western slopes of the Andes in Peru up to a height of 2800 m, whilst all other forms are confined to lower, humid, forested areas. The domestic dogis the only known animal reservoir and transmission seems to be essentially domiciliary. It causes a single or limited number of self-healing lesions called 'uta', with no nasopharyngeal involvement. Diagnosis A history of having visited the relevant geographic area together with the clinical appearance should suggest the diagnosis. Differential diagnosis may include pyogenic infections, basal cell epithelioma, keratoacanthoma, phagedenic and 'tropical' ulcers, atypical mycobacterial infection, lymphoma, sporotrichosis, tungiasis and cysticercosis. Lepromatous leprosy closely resembles the angergic form and nasopharyngeal disease must. be differentiated from South American blastomycosis, lethal mid-line granuloma and rhinoscleroma. Definitive diagnosis requires demonstration of the parasites microscopically. Superficial smears may be negative in the presence of secondary bacterial infection; it is therefore preferable to make a linear scalqel incision along the edge of a lesion and take the ~mears from the cut edge; a bloody smear is of no Use. A fine bore pipette or needle may be used to obtain tissue fluid from the edge of a lesion or samples may be taken from the cleaned base of an ulcer. The ease with which Leishmania are isolated varies from spec.ies to species. Early lesions are more likely to yield a positive result than are late lesions, particularly if secondary bacterial infection has developed. In addition to the examination of smears stained with Giemsa's or Leishman's stains, culture of the specimens should also be carried out. Leishmania may sometimes be detected only by culture and this is also necessary to identify the species. The use of both artificial culture media and inocu lation route into hamsters is recommended. Novy, MacNeill and Nicholles (NNN) medium is one of the oldest and most frequently used media, often with the addition of an antibiotic to inhibi1 bacterial growth. Initial culture may however be more successful on a semi solid blood agar medium. with subsequent inoculation onto NNN medium which has a solid phase with liquid overlay. Microscopic examination of a biopsy from the lesion is a less reliable means of diagnosis than the above methods. If a biopsy is taken an impression smear of the tissue should be taken prior to fixing, and a part of the tissue cultured for Leishmania. Histologically early lesions frequently show hyperkeratosis and acanthosis. Liquefactive degeneration of the basal cell layer of the epidermis may develop in the presence of a continguous dermal infiltrate. The dermal infiltrate is granulomatous with large numbers of epithelioid histiocytes, lymphocytes, plasma cells, polymorphonuclear leucocytes and Langhans' giant cells in varying proportions. Amastigotes may be seen within macrophages and are more easily visualised with Giemsa or Leishman stain than with haematoxylin and eosin. There is usually dilatation and reactive growth of dermal blood vessels in the affected areas and occasional extravascular erythrocytes may be seen. Chronic ulcerated lesions usually have an infiltrate consisting mainly of polymorphonuclear leucocytes. Montenegro's intradermal leishmanin test may be used to give further evidence to support the diagnosis. The test consists of the intradermal injection of cultured, heat killed Leishmania. The standard dose is 0.1 ml, containing at least 100,000 promastigotes and with a nitrogen concentration of at
5 t K Freeman least 30 ILg!ml. The injection site is marked and examined at 48 and 72 hours. A positive reaction is an indurated papule of 5 mm. or greater diameter, surrounded by erythema. A positive result indicates present or previous leishmanial infection. The rates of positive delayed hypersensitivity are higher than the rates of past or present clinical disease, as the test is specific and reproducible this suggests that subclinical cases of leishmaniasis occur 29. In residents of areas endemic for leishmaniasis this is not a defimtive test as positive reactions may reflect previous infection and any current skin lesion could be of unrelated aetiology. In individuals who have not previously visited endemic areas the test,is more reliable as previous leishmanial infection is unlikely. The test becomes positive within a few weeks of infection and remains so for many years, possibly for life. A positive reaction indicates the ability to mount a localised immune response at the site of injected anigen and does not indicate complete immunity to infection with the various species of Leishmania. There are several modifications of this test using different antigens 30 American cutaneous leishmaniasis does not lead to the massive increase in circulating gamma globulins seen in kala azar. Specific circulating antibodies,are formed however and techniques are being developed to identify these in a reliable diagnostic test. At present these tests are available in only a few specialist centres and require further refinement, before becoming available for general use. Immunofluorescence 31, 32, radio-immunoassay, enzyme profiles 33 and enzyme linked immunosorbent assay34 are among the techniques in use. Treatment The tendency to spontaneous healing of some forms of leishmaniasis has led to claims for the therapeutic efficacy of a wide variety of drugs, which subsequent investigations have shown to have no effect on the natural course of the disease. The drugs which have been proven to be effective are potentially toxic and therefore it is important to ~stablish the diagnosis prior to commencing therapy In order that these substances are not given unnecessarily. It is also of use to establish the species of leishmania responsible for the infection. Cases due to L. braziliensis braziliensis all need to have a full course of treatment with an effective drug in order to prevent subsequent mucocutaneous lesions whilst lesions due to L. mexicana mexicana ma; re.solve completely, and lead to no late sequelae, Without any specific drug therapy. Extensive lesions and lesions involving the cartilage of the ear or nose ~equi~e. ef!ective treatment. If facilities for species IdentIficatIOn are not available a decision on whether 171 to employ drug therapy should be based on knowledge of the pattern of disease previously experienced in the area where the disease was contracted. Although late mucocutaneous lesions have been reported from every endemic country south of Mexico the incidence is much higher in the southern areas than the more northerly ones. Pentavalent antimony (Sb) compounds are the most widely used drugs, either sodium stibogluconate (Pentostam) or antimony-n-methyl glutamine (Glucantime). There is no evidence that either drug has advantages over the other in efficacy or toxicity. Sodium stibogluconate is more readily available in the UK, in the United States it is obtainable only from the National Communicable Diseases Centres, Atlanta, Georgia. Although intramuscular administration is possible a prolonged course of treatment is necessary and slow intravenous injection is therefore preferred. Therapy should be as a hospital in-patient whenever possible. The dose of pentostam is mg. Sb / kg body weight with a maximum daily dose of 850 mg. Sb. This dose is given daily for at least three weeks. With daily injections antimonyaccumulates in the body35. Toxic effects 36 include nausea, vomiting, anorexia, fever, joint pains, transient changes in the ST and T37, 38 segments of the ECG and bradycardia 39. Lesions which have not responded to adequate antimony therapy may respond to a diamidine drug such as pentamidine 40 The drug is given by slow intravenous injection in intermittent seven to twelve day courses and may cause pruritus, exfoliative dermatitis, impaired glucose tolerance' and neuropathies; too rapid injection can cause hypotension and collapse 41 This drug should be used only in patients with normal hepatic and renal function. Severe mucous membrane lesions unresponsive to the above agents may be treated with amphotericin B42 in a dose of 0.5 to 1.00 mg/kg body weight (maximum dose 50 mg) by slow intravenous.infusion diluted in 5 % dextrose solution to a concentration of drug of 100 mg/l or less. The drug should be given on alternate days over a three to seven week period. It is very toxic and treatment often has to be discontinued for this reason. Fever, nausea, and anorexia develop commonly, venous thrombosis may occur at infusion sites. Renal damage is not unusual and the dosage should be reduced if the blood creatinine rises.. Ther.e. are several reports of the efficacy of nfamplcm 43, 44 but further controlled trials are required as treatment failures are also reported45. Ketoconazole has been reported to be effective in a limited number of cases 46 Early reports of the efficacy of trimethoprim-sulfmethoxazole 47 or metro ~idaz~le48 have not been borne out by subsequent mvestigators 49, 50. Intralesional injections of anti-
6 172 leishmanial agents are used in a few centres, they are often painful and may increase subsequent scarring and are not therefore recommended 51 Amastigotes are only able to multiply within a narrow temperature range and locally applied heat appears to speed the resolution of lesions 52 Cryotherapy is also reported to be effective 53, H whilst cautery may result in unsightly scars~5. Disease Control Eradication of the animal hosts or insects vectors at present seems to be impractical. There are reports from other parts of the world that anti-malal'ial insect spraying reduces the incidence of leishmaniasis; the extent of the jungle habitat of the vectors in America would make such an insecticidal policy impossible to implement effectively. Of the insect repellents at present available N N-diethyl-m-toluamide is the most effective against sandflies, but the climate of Central and South America necessitate frequent applications. There is at present no effective, safe, way to immunize people living in endemic areas. 'Immunization' against L tropicainfections has been carried out in several countries by intradermal injection of live parasites into a cosmetically unimportant area 56, 57, os, 59, producing clinical lesions at the injection site and subsequently immunity to reinfection. Such.immunity can at present only be achieved with live organisms and requires careful control of the injected parasite to ensure that it is sufficiently immunogenic 6D, but does not lead to severe disease. The several different species of Leishmania responsible for disease in the Americas makes the problem of immunization more difficult. It is essential that any induced infection will not lead to espundia, and detailed knowledge of the type of disease present in a locality is required before contemplating immunization. Induced or naturally acquired infection with Leishmania usually leaves the subject immune to re-infection with that particular species and there is evidence of some cross immunity between species 61 Organisms of the mexicana complex appear to be poor immunizing agents against both other species of the same complex and against members of the braziliensis complex. This suggests that these species which usually produce self limiting disease, grow rapidly in culture and are easily maintained are unlikely to be of use for immunization against potentially more serious L braziliensis braziliensis infections. Species of the braziliensis complex appear to be more effective immunizing agents, but are more likely to cause serious disease. There therefore remains a great deal of work to be done before routine human immunization is an acceptable procedure 62 Long term chemoprophylaxis is not feasible for residents of endemic areas, but if a suitable orally administered drug were found this would have potential use for visitors to endemic areas. KERDEL VEGAS F. American Leishmaniasis-in Clinical Tropical Dermatology. London. Blackwell Scientific Publications, SHAW P K. Autochthonous dermal leishmaniasis in Texas. Am ] Trop Med Hyg 1976; 25: ARIAS J R, de FREITAS R A. On the vectors of cutaneous leishmaniasis in the Central Amazon of Brazil. Acta Amazonica 1977; 7: KILLICK KENDRICK R. Recent advances and outstanding problems in the biology of phlebotomi ne sandflies. Acta Tropica (Switz) 1978; 35: STRANGWAYS DIXON J, LAINSON R. Dermal leishmaniasis in British Honduras. Brit Med] 1962; 1: WILLIAMS P. Phlebotomus sandflies and leishmaniasis in British Honduras (Belize). Trans R Soc Trop Med Hyg 1970; 64: PERFIT'ER P P. Phlebotomidae-in Fauna of the USSR, Vol Ill, Diptera. No. 2 Academy of Sciences of the USSR. New Serial No SHAW J J, LAINSON R. Leishmaniasis in Brazil VI. Trans R Soc Trop Med Hyg 1972; 66: LAINSON R, STRANGWAYS DIXON J. Dermal leishmaniasis in British Honduras. Brit Med] 1962; 1: HERRER A, CHRISTENSEN H A, BEUMER R J. Epidemiological patterns of cutaneous leishmaniasis in Panama 11. Ann Trop Med Parasitol 1976; 70: HERRER A, CHRISTENSEN H A. Infrequency of gross skin lesions among Panamanian forest mammals with cutaneous leishmaniasis. Parasitology 1975; 71: GARDENER P J. Taxonomy of the genus Leishmania. A review of the nomenclature and classification. Trop Dis Bull 1977; 74: LAINSON R, SHAW J J. Leishmaniasis of the New World: Taxonomic problems. Brit Med Bull; 1972: SHAW J J, LAINSON R. Leishmaniasi~ in Brazil XI. Observations on the morphology of. Leishmania of the braziliensis and mexicana complexes. ] Trop Med Hyg 1976; 79: qardenj?r. P ~, SHCHORY L, CHANCE M L. Species differentiation III the genus Leishmania by morphometric studies with the electron microscope. Ann Trop Med Parasitol 1977; 71: CHANCE M L, PETERS W, SHCHORY L. Biochemical taxonomy of Leishmania I. Ann Trop Med Parasilo I 1974; 68: GARDENER P J, QiANCE M L, PETERS W. Biochemical taxonomy of Leishmania 11. Ann Trop Med Parasitol 1974; 68: LAINSON R, SHAW J J. Leishmaniasis in Brazil V. Trans R Soc Trop Med Hyg 1970; 64: GARNHAM P C C, LEWIS D J. Parasites of British Honduras with special references to leishmaniasis. Trans R Soc Trop Med Hyg 1959; 53:
7 K Freeman 20 NovALEs J. Cutaneous leishmaniasis in Mexico. 21 1nl I Dermatol 1974; 13: LAINSON R, STRANGWAYS DIXON J. ~eishmf!ni.a mexicana: the epidemiology of dermal lelshmamasls in British Honduras. Trans R Soc Trop Med Hyg 1963; 57: SHAW J J, LAINSON R. Leishmaniasis in Brazil H. Trans R Sac Trop Med Hyg 1968; 62: LAINSON R, SHAW J J. Epidemiology and ecology of leishmaniasis in Latin America. Nature 1978; 273: CONVIT J, KERDAL VEGAS F. Disseminated cutaneous leishmaniasis. Archs Dermatol 1965; 91: BRAY R S. Epidemiology of leishmaniasis. Ciba Foundation Symposium No. 20 (new series) Trypanosomiasis and leishmaniasis pp Amsterdam. North Holland Publishing Company CoNVIT J, PINARDI M E, RONDON A J. Diffuse cutaneous leishmaniasis: a disease due to an immunological defect of the host. Trans R Soc Trop Med Hyg 1972; 66: CONVIT J, PINARDI M E. Cutaneous leishmaniasis: the clinical and immunopathological spectrum in South America. Ciba Foundation Symposium No 20 (new series) Trypanosomiasis and leishmaniasis pp Amsterdam. North Holland Publishing Company MAUEL J, BEHlN R. Cell mediated and humoral immunity to protozeal infections. Transplant Rev 1974; 19: PIFANIA F. La evaluacion de la leishmaniasis tegumentaria americana en el Valle de Aroa, Estado Yaracuy, Venezuela. Arch Venezol Med Trop Parasitol Med 1962; 4: PELLEGRINO J, PEREIVA L H, FURTADO T A. Mucocutaneous leishmaniasis, intradermal test with a promastigote suspension and a crude extract from Leishmania braziliensis. Rev lnst Trop Sao Paulo 1977; 19: BRAY R S, LAINSON R. The immunology and serology of leishmaniasis I; the fluorescent antibody staining technique. Trans R Soc Trap Med Hyg 1965; 59: GUIMARAES M C S, GIOVANNINI V L, CAMARGO M E. Antigenic standardisation for mucocutaneous leishmaniasis immunofluorescence test. Rev lnst Med Trop Sao Paulo 1974; 16: MILES M A et al. Leishmaniasis in Brazil XV. Biochemical distinction of Leishmania mexicana amazonensis L braziliensis braziliensis and L braziliensis guyanensis. TraIlS R Soc Trop Med Hyg 1981; 75(4): ROFFI J et al. Detection of circulating antibodies in cutaneous leishmaniasis by enzyme-linked immunosorbent assay (ELISA). Am I Trop Med Hyg 1980; 29(2): STEMMER K L. Pharmacology and toxicology of heavy metals: antimony. Pharmacology and Therapeutics Series A 1976; 1: HARVEY S C. Heavy metals; antimony. In the Pharmacological basis of Therapeutics. London: Macmillan Pnblishing Co Inc, 1975: DEMPSEY J J. Leishmaniasis in the Sudan Republic XXVI. Electrocardiographic findings in Sudanese Kala-azar. East Afr Med J 1965; 42: SAPIRE D W, SULVERMAN N H. Myocardial involvement in antimony therapy. South Atr Med J 1970; 44: COLTEN M de V LoGAN M. Effects of antimony on the cardiovascuiar system and intestinal smooth muscle. I Pharmac expo Ther. 1966; 151: NIEMEL M P L A. Traitment de la leishman!asis braziliensis cutanee par la lomidine (pentamidme). Bordeaux medical 1977; 10/11: BRYCESON A D M. Diffuse cutaneous leishmaniasis in Ethiopia H - treatment. Trans R Sac Trap Med Hyg 1970; 64: MARSDEN P D et al. Mucocutaneous leishmaniasis _ an unsolved clinical problem. Tropical Doctor 1977; 7: SELIM M M, KANDIL E. Rifampicin in the treatment of cutaneous leishmaniasis. J. Kuwait Med Assoc 1972; 6: DOURADO H V et al. Leishmanione tegumentar americana: tratments corn rifampicina. Rev Bras Clin Ter (Brazil) 1975; 4: WHITE S W HENDRICKS L D, CHULAY J D. Leishmaniasis: a' case history and treatment failure with rifampicin. Arch Dermatol 1980; 116(6): URCUYO, F G, ZAIAS, N. Oral ketoconazole in the treatment of leishmaniasis. Int J Dermatol 1982; 21(7): KANDIL E. Treatment of cutaneous leishmaniasis with trimethoprim-sulfamethoazole combination. Dermatologica 1973; 146: BELTRAN, H F, GUTIERREZ, M, BIAGGI, F F. Utile du metronidazole dans le traitement de la leishmaniose cutanee Mexicaine. Bull Soc Pathol Escot 1967; 60: SMIT, A M, VAN DER KAAG, H J. Cutaneous leish maniasis. Dermatologica 1977; 154: BRYCE, C et al. American cutaneous leishmaniasis, inefficacy of metronidazole in treatment. I.A.M.A. 1974; 228: BRYCESON, A D M. Cutaneous leishmaniasis. Brit J Derm 1976; 94: MUTINGA, M J, MNGOLA, E N. Alternate treatment of cutaneous leishmaniasis. East Afr Med J 1974; 51: DORMAN, G D. Treatment of cutaneous leishman iasis by freezing. J Am Med Assac 1974; 227: , 54 BASSIOUNY, A et al. Cryosurgery in cutaneous leishmaniasis. Brit J Dermatol 1982; 107(4): 467~ SAGHER, F. Cutaneous Leishmaniasis. In Clinical Tropical Dermatology. London. Blackwell Scientific Publications 1975: , 56 BERBERIAN, D A. Vaccination and immunity against oriental sore. Trans R Sac Trop Med Hyg 1939; 33: GUNDERS, A E, NAGAN, L, MICHAELl, D. Follow up study of a vaccination programme against leishmaniasis I and n. Trans R Soc Trop Med Hyg 1972; 66: KATZENNELLENBOGEN, I, LEVY, I. Prevention of leishmaniasis in a Kibbutz by inoculation. Harefuah 1968; 75: SENEKJI, HA, BEATTIE, C P. Artificial infection and immunisation of man with cultures of L tropica. Trans R Sac Trop Med Hyg 1941; 34: KOUFMAN, Z et al. Observation on immunisation against cutaneous leishmaniasis in Jsrael. Israel J Med Sci 1978; 14: LAINSON, R, SHAW, J J. Studies on the immunology and serology of leishmaniasis Ill. Trans R Soc Trop Med Hyg 1966; 60: LAINSON, R, SHAW, J J. Leishmaniasis in Brazil XII. I Trop Med Hyg 1977; 80:
The Most Common Parasitic Infections In Yemen. Medical Parasitology
 The Most Common Parasitic Infections In Yemen Medical Parasitology ﻓﺎﯾز اﻟﺧوﻻﻧﻲ / د 2 : is a vector-borne disease that transmitted by sandflies and caused by obligate intracellular protozoa of the genus
The Most Common Parasitic Infections In Yemen Medical Parasitology ﻓﺎﯾز اﻟﺧوﻻﻧﻲ / د 2 : is a vector-borne disease that transmitted by sandflies and caused by obligate intracellular protozoa of the genus
Welcome to the Jungle! Dr Aileen Oon, 2017 Microbiology Registrar
 Welcome to the Jungle! Dr Aileen Oon, 2017 Microbiology Registrar AA 55M presented with sores on left olecranon and umbilical area Umbilical sores present for 3 weeks Left olecranon lesions for 1 week
Welcome to the Jungle! Dr Aileen Oon, 2017 Microbiology Registrar AA 55M presented with sores on left olecranon and umbilical area Umbilical sores present for 3 weeks Left olecranon lesions for 1 week
2.Trichomonas vaginalis
 2.Trichomonas vaginalis 1. Pathogenic to human &causes vaginitis (trichomoniasis). 2. troph. Is round or pear like in shape, contains 4-6 flagella, all originating from anterior end & only one extend posteriorly.
2.Trichomonas vaginalis 1. Pathogenic to human &causes vaginitis (trichomoniasis). 2. troph. Is round or pear like in shape, contains 4-6 flagella, all originating from anterior end & only one extend posteriorly.
Leishmaniasis, Kala Azar(The Black Fever)
 Leishmaniasis, Kala Azar(The Black Fever) By Lawrence Hall Etiologic agent Protist obligate intracellular parasite, Transmission Vectors Phylum: Euglenozoa (genus Leishmania) Over 21 species that infect
Leishmaniasis, Kala Azar(The Black Fever) By Lawrence Hall Etiologic agent Protist obligate intracellular parasite, Transmission Vectors Phylum: Euglenozoa (genus Leishmania) Over 21 species that infect
HAEMOFLAGELLATES. Dr. Anuluck Junkum Department of Parasitology Faculty of Medicine
 HAEMOFLAGELLATES Dr. Anuluck Junkum Department of Parasitology Faculty of Medicine Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of Leishmania spp. and Trypanosoma
HAEMOFLAGELLATES Dr. Anuluck Junkum Department of Parasitology Faculty of Medicine Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of Leishmania spp. and Trypanosoma
Acta Dermatovenerol Croat 2008;16(2):60-64 CLINICAL ARTICLE
 2008;16(2):60-64 CLINICAL ARTICLE Clinical Efficacy of Intramuscular Meglumine Antimoniate Alone and in Combination with Intralesional Meglumine Antimoniate in the Treatment of Old World Cutaneous Leishmaniasis
2008;16(2):60-64 CLINICAL ARTICLE Clinical Efficacy of Intramuscular Meglumine Antimoniate Alone and in Combination with Intralesional Meglumine Antimoniate in the Treatment of Old World Cutaneous Leishmaniasis
Leishmaniasis. CDR R.L. Gutierrez Oct 2014
 Leishmaniasis CDR R.L. Gutierrez Oct 2014 Overview Protozoan parasite(s) of tissue and WBCs Many species / Many Syndromes (Cutaneous / Visceral) Pathogen: Location - Old World vs. New World Host: Immune
Leishmaniasis CDR R.L. Gutierrez Oct 2014 Overview Protozoan parasite(s) of tissue and WBCs Many species / Many Syndromes (Cutaneous / Visceral) Pathogen: Location - Old World vs. New World Host: Immune
BIO Parasitology Spring 2009
 BIO 475 - Parasitology Spring 2009 Stephen M. Shuster Northern Arizona University http://www4.nau.edu/isopod Lecture 5 Discovery of the Disease In 1924 the Kala-Azar Commission noted that the distribution
BIO 475 - Parasitology Spring 2009 Stephen M. Shuster Northern Arizona University http://www4.nau.edu/isopod Lecture 5 Discovery of the Disease In 1924 the Kala-Azar Commission noted that the distribution
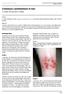
SUMMARY. Cutaneous leishmaniasis with only skin involvement: single to multiple skin ulcers, satellite lesions and nodular lymphangitis.
 SUMMARY Leishmaniasis is a disease affecting predominantly people in the developing countries; 350 million people worldwide are at risk and yearly more than 2 million new cases occur. Leishmaniasis is
SUMMARY Leishmaniasis is a disease affecting predominantly people in the developing countries; 350 million people worldwide are at risk and yearly more than 2 million new cases occur. Leishmaniasis is
Morphological forms of hemoflagellates
 Parasitology Lecture: 1 Hemoflagellates (blood and tissue flagellates) *Classification: - Sub-kingdom: Protozoa -Phylum: Sarcomastigophora -Sub-phylum: Mastigiphora -Class: Zoomastigophora د. رائد *Flagellates
Parasitology Lecture: 1 Hemoflagellates (blood and tissue flagellates) *Classification: - Sub-kingdom: Protozoa -Phylum: Sarcomastigophora -Sub-phylum: Mastigiphora -Class: Zoomastigophora د. رائد *Flagellates
World Health Organization Department of Communicable Disease Surveillance and Response
 WHO Report on Global Surveillance of Epidemic-prone Infectious Diseases World Health Organization Department of Communicable Disease Surveillance and Response This document has been downloaded from the
WHO Report on Global Surveillance of Epidemic-prone Infectious Diseases World Health Organization Department of Communicable Disease Surveillance and Response This document has been downloaded from the
Laboratory diagnosis of Blood and tissue flagellates
 Laboratory diagnosis of Blood and tissue flagellates (Leishmania and trypanosma) Sarah Alharbi Clinical Laboratory department Collage of Applied Medical Sciences King Saud University Leishmania and trypanosma:
Laboratory diagnosis of Blood and tissue flagellates (Leishmania and trypanosma) Sarah Alharbi Clinical Laboratory department Collage of Applied Medical Sciences King Saud University Leishmania and trypanosma:
Laboratory investigation of Cutaneous Leishmaniasis in Karachi
 Laboratory investigation of Cutaneous Leishmaniasis in Karachi Pages with reference to book, From 248 To 250 G.M. Rajpar, M.A. Khan, A. Hafiz ( Department of Microbiology, Jinnah Postgraduate Medical Centre,
Laboratory investigation of Cutaneous Leishmaniasis in Karachi Pages with reference to book, From 248 To 250 G.M. Rajpar, M.A. Khan, A. Hafiz ( Department of Microbiology, Jinnah Postgraduate Medical Centre,
Leishmaniasis. MAJ Kris Paolino September 2014
 Leishmaniasis MAJ Kris Paolino September 2014 Thanks to COL (Ret) Kent Kester MAJ Leyi Lin http://www.niaid.nih.gov/topics/leishmaniasis History Sir William Boog Leishman (1865-1926) Matriculated at the
Leishmaniasis MAJ Kris Paolino September 2014 Thanks to COL (Ret) Kent Kester MAJ Leyi Lin http://www.niaid.nih.gov/topics/leishmaniasis History Sir William Boog Leishman (1865-1926) Matriculated at the
Sodium Stibogluconate treatment for cutaneous leishmaniasis: A clinical study of 43 cases from the north of Jordan
 Sodium Stibogluconate treatment for cutaneous leishmaniasis: A clinical study of 43 cases from the north of Jordan Mamoun Mohammad Al-Athamneh Hiathem Qasem Abu Al-haija Ra ed Smadi Ayman S. Qaqaa Heba
Sodium Stibogluconate treatment for cutaneous leishmaniasis: A clinical study of 43 cases from the north of Jordan Mamoun Mohammad Al-Athamneh Hiathem Qasem Abu Al-haija Ra ed Smadi Ayman S. Qaqaa Heba
WMLN Case Study. Necrotizing Palate Biopsy Specimen. Youngmi Kim Sr. Microbiologist TB Lab & Parasitology Lab MS, M(ASCP)
 WMLN Case Study Necrotizing Palate Biopsy Specimen Youngmi Kim Sr. Microbiologist TB Lab & Parasitology Lab MS, M(ASCP) 44 year old male from Honduras Immigrated to US 12 years ago to WI 4 years ago Seen
WMLN Case Study Necrotizing Palate Biopsy Specimen Youngmi Kim Sr. Microbiologist TB Lab & Parasitology Lab MS, M(ASCP) 44 year old male from Honduras Immigrated to US 12 years ago to WI 4 years ago Seen
~Trichinella Spiralis:
 Musculoskeletal System **Today we are going to talk about the parasites that affect the musculoskeletal system ~Trichinella Spiralis: It s a small nematode that measures to about 2-3mm in length. In general
Musculoskeletal System **Today we are going to talk about the parasites that affect the musculoskeletal system ~Trichinella Spiralis: It s a small nematode that measures to about 2-3mm in length. In general
THE LEISHMANIA TEST IN EXPERIMENTAL LEISHMANIASIS (ORIENTAL SORE) IN HUMAN SUBJECTS
 THE IN EXPERIMENTAL SIS (ORIENTAL SORE) IN HUMAN SUBJECTS A. DOSTROVSKY, M.D. The reaction of the skin to the intracutaneous injection of leishmania vaccine has been studied and established as a diagnostic
THE IN EXPERIMENTAL SIS (ORIENTAL SORE) IN HUMAN SUBJECTS A. DOSTROVSKY, M.D. The reaction of the skin to the intracutaneous injection of leishmania vaccine has been studied and established as a diagnostic
Fact sheet. Yellow fever
 Fact sheet Key facts is an acute viral haemorrhagic disease transmitted by infected mosquitoes. The yellow in the name refers to the jaundice that affects some patients. Up to 50% of severely affected
Fact sheet Key facts is an acute viral haemorrhagic disease transmitted by infected mosquitoes. The yellow in the name refers to the jaundice that affects some patients. Up to 50% of severely affected
(From the Department of Medicine, the Peiping Union Medical College, Peiping, China)
 Published Online: 1 April, 1934 Supp Info: http://doi.org/10.1084/jem.59.4.491 Downloaded from jem.rupress.org on October 9, 2018 VIABLE LEISHMANIA DONOVANI IN NASAL AND ORAL SECRETIONS OF PATIENTS WITH
Published Online: 1 April, 1934 Supp Info: http://doi.org/10.1084/jem.59.4.491 Downloaded from jem.rupress.org on October 9, 2018 VIABLE LEISHMANIA DONOVANI IN NASAL AND ORAL SECRETIONS OF PATIENTS WITH
What is Kala-azar? What are Signs & Symptoms of Kala-Azar?
 What is Kala-azar? Kala-azar is a slow progressing indigenous disease caused by a protozoan parasite of genus Leishmania In India Leishmania donovani is the only parasite causing this disease The parasite
What is Kala-azar? Kala-azar is a slow progressing indigenous disease caused by a protozoan parasite of genus Leishmania In India Leishmania donovani is the only parasite causing this disease The parasite
Leishmaniasis WRAIR- GEIS 'Operational Clinical Infectious Disease' Course
 Leishmaniasis WRAIR- GEIS 'Operational Clinical Infectious Disease' Course UNCLASSIFIED Acknowledgments LTC James E. Moon, MD Chief, Sleep Trials Branch Walter Reed Army Institute of Research CDR Ramiro
Leishmaniasis WRAIR- GEIS 'Operational Clinical Infectious Disease' Course UNCLASSIFIED Acknowledgments LTC James E. Moon, MD Chief, Sleep Trials Branch Walter Reed Army Institute of Research CDR Ramiro
Cutaneous Leishmaniasis : Global overview
 Cutaneous Leishmaniasis : Global overview Meeting of stakeholders for selected Health R&D Demostration Projects, 7-10 May 2014, WHO, Geneva Dr. Daniel Argaw Dagne, NTD/WHO CSR - DDC AFRO Leishmaniasis
Cutaneous Leishmaniasis : Global overview Meeting of stakeholders for selected Health R&D Demostration Projects, 7-10 May 2014, WHO, Geneva Dr. Daniel Argaw Dagne, NTD/WHO CSR - DDC AFRO Leishmaniasis
Leishmaniasis. caused by Leishmania spp. 利什曼原蟲 transmitted by Phlebotomine flies (Sandflies 白蛉 )
 Leishmaniasis caused by Leishmania spp. 利什曼原蟲 transmitted by Phlebotomine flies (Sandflies 白蛉 ) Cutaneous Leishmaniasis Mucocutaneous Leishmaniasis Visceral Leishmaniasis About 12 million people are currently
Leishmaniasis caused by Leishmania spp. 利什曼原蟲 transmitted by Phlebotomine flies (Sandflies 白蛉 ) Cutaneous Leishmaniasis Mucocutaneous Leishmaniasis Visceral Leishmaniasis About 12 million people are currently
Leishmaniasis. caused by Leishmania spp. 利什曼原蟲 transmitted by Phlebotomine flies (Sandflies 白蛉 ) 皮膚型黏膜型內臟型. Cutaneous Leishmaniasis
 Leishmaniasis caused by Leishmania spp. 利什曼原蟲 transmitted by Phlebotomine flies (Sandflies 白蛉 ) 皮膚型黏膜型內臟型 Cutaneous Leishmaniasis Mucocutaneous Leishmaniasis Visceral Leishmaniasis About 12 million people
Leishmaniasis caused by Leishmania spp. 利什曼原蟲 transmitted by Phlebotomine flies (Sandflies 白蛉 ) 皮膚型黏膜型內臟型 Cutaneous Leishmaniasis Mucocutaneous Leishmaniasis Visceral Leishmaniasis About 12 million people
TOWARD AN APPROACH FOR CUTANEOUS LEISHMANIA TREATMENT. Mohammed Wael Daboul
 Original Articles DOI: 10.7241/ourd.20131.09 Source of Support: Nil Competing Interests: None TOWARD AN APPROACH FOR CUTANEOUS LEISHMANIA TREATMENT Mohammed Wael Daboul Laboratory Medicine Specialist,
Original Articles DOI: 10.7241/ourd.20131.09 Source of Support: Nil Competing Interests: None TOWARD AN APPROACH FOR CUTANEOUS LEISHMANIA TREATMENT Mohammed Wael Daboul Laboratory Medicine Specialist,
CASE OF CUTANEOUS LEISHMANIASIS OF THE LID*
 Brit. J. Ophthal. (1965) 49, 542 CASE OF CUTANEOUS LEISHMANIASIS OF THE LID* BY GWYN MORGAN Department ofpathology, Institute of Ophthalmology, University of London THE lid is involved only in about 2
Brit. J. Ophthal. (1965) 49, 542 CASE OF CUTANEOUS LEISHMANIASIS OF THE LID* BY GWYN MORGAN Department ofpathology, Institute of Ophthalmology, University of London THE lid is involved only in about 2
Blood Smears Only 6 October Sample Preparation and Quality Control 15B-K
 NEW YORK STATE Parasitology Proficiency Testing Program Blood Smears Only 6 October 5 The purpose of the New York State Proficiency Testing Program in the category of Parasitology - Blood Smears Only is
NEW YORK STATE Parasitology Proficiency Testing Program Blood Smears Only 6 October 5 The purpose of the New York State Proficiency Testing Program in the category of Parasitology - Blood Smears Only is
Necrotizing and suppurative lymphadenitis in Leishmania
 Tropical Medicine and International Health VOLUME I NO. 2 PP 243-250 APRIL 1996 Necrotizing and suppurative lymphadenitis in Leishmania major infections A. Gaafar r, A. Ismai13, A. Y. El Kadaro4, Elsir
Tropical Medicine and International Health VOLUME I NO. 2 PP 243-250 APRIL 1996 Necrotizing and suppurative lymphadenitis in Leishmania major infections A. Gaafar r, A. Ismai13, A. Y. El Kadaro4, Elsir
Leishmaniaand Leishmaniasis
 Leishmaniaand Leishmaniasis Methodenseminar SS2014 IRMA SCHABUSSOVA, PhD Institute of Specific Prophylaxis and Tropical Medicine; Medical University Vienna Kinderspitalgasse 15, A-1090 Vienna, Austria
Leishmaniaand Leishmaniasis Methodenseminar SS2014 IRMA SCHABUSSOVA, PhD Institute of Specific Prophylaxis and Tropical Medicine; Medical University Vienna Kinderspitalgasse 15, A-1090 Vienna, Austria
Leishmaniasis. By Joseph Knight, PA-C. 2. Explain the differences in the reasons leishmaniasis is spreading in Afghanistan and India.
 Leishmaniasis By Joseph Knight, PA-C Objectives 1. Identify the two types of leishmaniasis. 2. Explain the differences in the reasons leishmaniasis is spreading in Afghanistan and India. 3. Discuss how
Leishmaniasis By Joseph Knight, PA-C Objectives 1. Identify the two types of leishmaniasis. 2. Explain the differences in the reasons leishmaniasis is spreading in Afghanistan and India. 3. Discuss how
CHRONIC INFLAMMATION
 CHRONIC INFLAMMATION Chronic inflammation is an inflammatory response of prolonged duration often for months, years or even indefinitely. Its prolonged course is proved by persistence of the causative
CHRONIC INFLAMMATION Chronic inflammation is an inflammatory response of prolonged duration often for months, years or even indefinitely. Its prolonged course is proved by persistence of the causative
Kinetoplastids Handout
 Kinetoplastids Handout 1 Kinetoplastids widespread group of flagellated protozoa parasitize virtually all animal groups as well as plants and insects 3 distinct kinetoplastid species cause human disease
Kinetoplastids Handout 1 Kinetoplastids widespread group of flagellated protozoa parasitize virtually all animal groups as well as plants and insects 3 distinct kinetoplastid species cause human disease
Cutaneous Leishmaniasis in a Chinese man returning from the Amazon forest in Brazil
 Hong Kong J. Dermatol. Venereol. (2013) 21, 79-83 Case Report Cutaneous Leishmaniasis in a Chinese man returning from the Amazon forest in Brazil JTHT Yu and SY Wong A 60-year-old man presented with ulcerated
Hong Kong J. Dermatol. Venereol. (2013) 21, 79-83 Case Report Cutaneous Leishmaniasis in a Chinese man returning from the Amazon forest in Brazil JTHT Yu and SY Wong A 60-year-old man presented with ulcerated
Post Kala-azar Dermal Leishmaniasis (PKDL) from the field to the cellular and the subcellular levels
 Post Kala-azar Dermal Leishmaniasis (PKDL) from the field to the cellular and the subcellular levels A M EL Hassan Institute of Endemic Diseases University of Khartoum Introduction PKDL is a VL related
Post Kala-azar Dermal Leishmaniasis (PKDL) from the field to the cellular and the subcellular levels A M EL Hassan Institute of Endemic Diseases University of Khartoum Introduction PKDL is a VL related
Uncommon clinical presentations of leprosy: apropos of three cases
 Lepr Rev (2016) 87, 246 251 CASE REPORT Uncommon clinical presentations of leprosy: apropos of three cases RASHMI JINDAL* & NADIA SHIRAZI** *Department of Dermatology, Venereology & Leprosy, Himalayan
Lepr Rev (2016) 87, 246 251 CASE REPORT Uncommon clinical presentations of leprosy: apropos of three cases RASHMI JINDAL* & NADIA SHIRAZI** *Department of Dermatology, Venereology & Leprosy, Himalayan
VISERAL LEISHMANIASI S (KALA-AZAR)
 VISERAL LEISHMANIASI S (KALA-AZAR) :OUTLINES DEFINITION. EPIDEMIOLOGY. PARASITE & VECTOR. PATHOLOGY CLINICAL & LIFE CYCLE. PICTURE. COMPLICATIONS. DIAGNOSIS. INVESTIGATIONS. MANAGEMENT TREATMENT S CONTROL.
VISERAL LEISHMANIASI S (KALA-AZAR) :OUTLINES DEFINITION. EPIDEMIOLOGY. PARASITE & VECTOR. PATHOLOGY CLINICAL & LIFE CYCLE. PICTURE. COMPLICATIONS. DIAGNOSIS. INVESTIGATIONS. MANAGEMENT TREATMENT S CONTROL.
Recommendations for Coping with Leishmaniasis: A Review of Control Strategies. Centro de Convenções de Reboças Red Room 17: 00h
 Recommendations for Coping with Leishmaniasis: A Review of Control Strategies Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000
Recommendations for Coping with Leishmaniasis: A Review of Control Strategies Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000
Trypanosomiasis. Introduction. Epidemiology. Global Epidemiology. Trypanosomiasis Risk in UK Travellers
 Trypanosomiasis Introduction Epidemiology Risk for travellers Transmission Signs and symptoms Treatment Prevention References Reading list Links Introduction Trypanosomiasis is caused by parasitic protozoa
Trypanosomiasis Introduction Epidemiology Risk for travellers Transmission Signs and symptoms Treatment Prevention References Reading list Links Introduction Trypanosomiasis is caused by parasitic protozoa
CONTROLE DAS LEISHMANIOSES O QUE FALTA FAZER? Centro de Convenções de Reboças Red Room 17: 00h
 CONTROLE DAS LEISHMANIOSES O QUE FALTA FAZER? Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000 deaths (6.7%) 310 million at
CONTROLE DAS LEISHMANIOSES O QUE FALTA FAZER? Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000 deaths (6.7%) 310 million at
CLINCOPATHOLOGICAL CASE
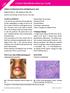 CLINCOPATHOLOGICAL CASE Solitary erythematous firm noduloplaque on nose Hassab El-Naby H., MD, Mosbeh Al Sadat, MD Department of Dermatology, Al-Azhar University, Cairo, Egypt. CLINICAL FINDINGS A 36-year-old
CLINCOPATHOLOGICAL CASE Solitary erythematous firm noduloplaque on nose Hassab El-Naby H., MD, Mosbeh Al Sadat, MD Department of Dermatology, Al-Azhar University, Cairo, Egypt. CLINICAL FINDINGS A 36-year-old
Cutaneous leishmaniasis in an overseas Filipino worker who responded favorably to oral itraconazole
 CSE REPORT Cutaneous leishmaniasis in an overseas Filipino worker who responded favorably to oral itraconazole udi, MD 1, ilza ellamy R. Limcangco, MD, FPDS 2, Johannes F, Dayrit, MD, FPDS 2,3 Introduction:
CSE REPORT Cutaneous leishmaniasis in an overseas Filipino worker who responded favorably to oral itraconazole udi, MD 1, ilza ellamy R. Limcangco, MD, FPDS 2, Johannes F, Dayrit, MD, FPDS 2,3 Introduction:
Cutaneous Leishmaniasis in an Immigrant Saudi Worker: A Case Report
 J HEALTH POPUL NUTR 2014 Jun;32(2):372-376 ISSN 1606-0997 $ 5.00+0.20 INTERNATIONAL CENTRE FOR DIARRHOEAL DISEASE RESEARCH, BANGLADESH CASE STUDY Cutaneous Leishmaniasis in an Immigrant Saudi Worker: A
J HEALTH POPUL NUTR 2014 Jun;32(2):372-376 ISSN 1606-0997 $ 5.00+0.20 INTERNATIONAL CENTRE FOR DIARRHOEAL DISEASE RESEARCH, BANGLADESH CASE STUDY Cutaneous Leishmaniasis in an Immigrant Saudi Worker: A
Cutaneous leishmaniasis: advances in disease pathogenesis, diagnostics and therapeutics
 Clinical dermatology Review article CED Clinical and Experimental Dermatology Cutaneous leishmaniasis: advances in disease pathogenesis, diagnostics and therapeutics M. Ameen Royal Free Hospital, Royal
Clinical dermatology Review article CED Clinical and Experimental Dermatology Cutaneous leishmaniasis: advances in disease pathogenesis, diagnostics and therapeutics M. Ameen Royal Free Hospital, Royal
Original Article Comparison of fine needle aspiration with biopsy in the diagnosis of cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin
 Original Article Comparison of fine needle aspiration with biopsy in the diagnosis of cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin Department of Dermatology, Pakistan Institute of Medical Sciences,
Original Article Comparison of fine needle aspiration with biopsy in the diagnosis of cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin Department of Dermatology, Pakistan Institute of Medical Sciences,
Flagellates. Dr. Anuluck Junkum PARA
 Flagellates Dr. Anuluck Junkum PARA 317242 Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of pathogenic flagellates Classification of Protozoa Based on locomotive
Flagellates Dr. Anuluck Junkum PARA 317242 Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of pathogenic flagellates Classification of Protozoa Based on locomotive
Treatment of Cutaneous Leishmaniasis with Allopurinol and Stibogluconate
 165 Treatment of Cutaneous Leishmaniasis with Allopurinol and S. Martinez, M. Gonzalez, and M. E. Vernaza From the Department of Internal Medicine, University of Cauca, Popayan, and the University Hospital
165 Treatment of Cutaneous Leishmaniasis with Allopurinol and S. Martinez, M. Gonzalez, and M. E. Vernaza From the Department of Internal Medicine, University of Cauca, Popayan, and the University Hospital
Summary of Cases & Epidemiology Aspects of Leishmaniasis in Thailand
 Summary of Cases & Epidemiology Aspects of Leishmaniasis in Thailand Sukmee T. 1, Mungthin M. 2, Apiwathanasorn C. 3, Leelayoova S. 2 1 Department of Microbiology, Phramongkutklao College of Medicine 2
Summary of Cases & Epidemiology Aspects of Leishmaniasis in Thailand Sukmee T. 1, Mungthin M. 2, Apiwathanasorn C. 3, Leelayoova S. 2 1 Department of Microbiology, Phramongkutklao College of Medicine 2
Protozoa from tissues. Leishmania spp. Naegleria fowleri Toxoplasma gondii Trichomonas vaginalis Trypanosoma spp.
 Protozoa from tissues Leishmania spp. Naegleria fowleri Toxoplasma gondii Trichomonas vaginalis Trypanosoma spp. Leishmaniasis Leishmania infantum, Leishmania donovani, in macrophages of man. Female sandflies:
Protozoa from tissues Leishmania spp. Naegleria fowleri Toxoplasma gondii Trichomonas vaginalis Trypanosoma spp. Leishmaniasis Leishmania infantum, Leishmania donovani, in macrophages of man. Female sandflies:
Leishmaniasis: A forgotten disease among neglected people
 ISPUB.COM The Internet Journal of Health Volume 11 Number 2 Leishmaniasis: A forgotten disease among neglected people Y Homsi, G Makdisi Citation Y Homsi, G Makdisi. Leishmaniasis: A forgotten disease
ISPUB.COM The Internet Journal of Health Volume 11 Number 2 Leishmaniasis: A forgotten disease among neglected people Y Homsi, G Makdisi Citation Y Homsi, G Makdisi. Leishmaniasis: A forgotten disease
Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive)
 Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) July 2012 May 2018 December 2005 Case Definition Confirmed Case Clinical
Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) July 2012 May 2018 December 2005 Case Definition Confirmed Case Clinical
Cutaneous Leishmania
 DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Cutaneous Leishmania Ibrahim Khalifeh, MD I do not have any relevant relationships with industry. Cutaneous Leishmania: Is it a Legend? Ibrahim Khalifeh,
DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Cutaneous Leishmania Ibrahim Khalifeh, MD I do not have any relevant relationships with industry. Cutaneous Leishmania: Is it a Legend? Ibrahim Khalifeh,
AEDES AEGYFTI AS A FACTOR IN THE INTERNATIONAL SPREAD OF YELLOW FEVER. Statement presented by the Delegations of Brazil, Cuba and Panama
 UNITED NATIONS NATIONS UNIES WORLD HEALTH ORGANIZATION SEVENTH WORLD HEALTH ASSEMBLY ORGANISATION MONDIALE DE LA SANTÉ A7/IQ/WP/4 8 May 1954 ORIGINA. Lî ENGLISH AEDES AEGYFTI AS A FACTOR IN THE INTERNATIONAL
UNITED NATIONS NATIONS UNIES WORLD HEALTH ORGANIZATION SEVENTH WORLD HEALTH ASSEMBLY ORGANISATION MONDIALE DE LA SANTÉ A7/IQ/WP/4 8 May 1954 ORIGINA. Lî ENGLISH AEDES AEGYFTI AS A FACTOR IN THE INTERNATIONAL
المركب النموذج--- سبيتز وحمة = Type Spitz's Nevus, Compound SPITZ NEVUS 1 / 7
 SPITZ NEVUS 1 / 7 Epidemiology An annual incidence rate of 1.4 cases of Spitz nevus per 100,000 individuals has been estimated in Australia, compared with 25.4 per 100,000 individuals for cutaneous melanoma
SPITZ NEVUS 1 / 7 Epidemiology An annual incidence rate of 1.4 cases of Spitz nevus per 100,000 individuals has been estimated in Australia, compared with 25.4 per 100,000 individuals for cutaneous melanoma
DOI /j x
 THERAPEUTICS DOI 10.1111/j.1365-2133.2007.07872.x Diffuse cutaneous leishmaniasis responds to miltefosine but then relapses O. Zerpa, M. Ulrich, B. Blanco, M. Polegre, A. Avila, N. Matos,* I. Mendoza,
THERAPEUTICS DOI 10.1111/j.1365-2133.2007.07872.x Diffuse cutaneous leishmaniasis responds to miltefosine but then relapses O. Zerpa, M. Ulrich, B. Blanco, M. Polegre, A. Avila, N. Matos,* I. Mendoza,
Leishmaniasis in the WhO european region
 Leishmaniasis in the WhO european region This information leaflet contains six sections and is intended for a generic and public health audience: 1.Leishmaniasis is present in europe. What are the risks
Leishmaniasis in the WhO european region This information leaflet contains six sections and is intended for a generic and public health audience: 1.Leishmaniasis is present in europe. What are the risks
WRAIR- GEIS 'OPERATIONAL CLINICAL INFECTIOUS DISEASE' COURSE
 Leishmaniasis WRAIR- GEIS 'OPERATIONAL CLINICAL INFECTIOUS DISEASE' COURSE The opinions or assertions contained herein are the private views of the author, and are not to be construed as official, or as
Leishmaniasis WRAIR- GEIS 'OPERATIONAL CLINICAL INFECTIOUS DISEASE' COURSE The opinions or assertions contained herein are the private views of the author, and are not to be construed as official, or as
New insights on leishmaniasis in immunosuppressive conditions
 New insights on leishmaniasis in immunosuppressive conditions Javier Moreno Immunoparasitology Unit WHO Collaborative Center for Leishmaniasis Centro Nacional de Microbiología INSTITUTO DE SALUD CARLOS
New insights on leishmaniasis in immunosuppressive conditions Javier Moreno Immunoparasitology Unit WHO Collaborative Center for Leishmaniasis Centro Nacional de Microbiología INSTITUTO DE SALUD CARLOS
(NATO STANAG 2122, CENTO STANAG 2122, SEATO STANAG 2122)
 (NATO STANAG 2122, CENTO STANAG 2122, SEATO STANAG 2122) Bacteria Bacteria are microscopic, single-celled forms of plant life, containing no chlorophyll. They live on the skin, on the surface of the stratum
(NATO STANAG 2122, CENTO STANAG 2122, SEATO STANAG 2122) Bacteria Bacteria are microscopic, single-celled forms of plant life, containing no chlorophyll. They live on the skin, on the surface of the stratum
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW
 MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
Frequently Asked Questions on Visceral Leishmaniasis (Kala-azar)
 SEA-CD-274 Frequently Asked Questions on Visceral Leishmaniasis (Kala-azar) World Health Organization 2013 All rights reserved. Requests for publications, or for permission to reproduce or translate WHO
SEA-CD-274 Frequently Asked Questions on Visceral Leishmaniasis (Kala-azar) World Health Organization 2013 All rights reserved. Requests for publications, or for permission to reproduce or translate WHO
Neglected Diseases (NDs) Landscape in Brazil and South America
 Frontiers in Science on Neglected Diseases 13 th November 2014 Neglected Diseases (NDs) Landscape in Brazil and South America Jeffrey Shaw São Paulo University Biomedical Sciences Institute jeffreyj@usp.br
Frontiers in Science on Neglected Diseases 13 th November 2014 Neglected Diseases (NDs) Landscape in Brazil and South America Jeffrey Shaw São Paulo University Biomedical Sciences Institute jeffreyj@usp.br
Lecture 5: Dr. Jabar Etaby
 Lecture 5: Dr. Jabar Etaby 1 2 Onchocerca volvulus (Blinding filariasis; river blindness) Microfilaria of Onchocerca volvulus, from skin snip from a patient seen in Guatemala. Wet preparation 3 Some important
Lecture 5: Dr. Jabar Etaby 1 2 Onchocerca volvulus (Blinding filariasis; river blindness) Microfilaria of Onchocerca volvulus, from skin snip from a patient seen in Guatemala. Wet preparation 3 Some important
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
New Insights into Diagnosing Leishmaniasis
 New Insights into Diagnosing Leishmaniasis Eric Zini Snow meeting, 13 March 2009 Climate Variability and Visceral Leishmaniasis in Europe WHO/TDR, Jan. 2008 Late Eighties Maroli et al., Trop Med Int Health
New Insights into Diagnosing Leishmaniasis Eric Zini Snow meeting, 13 March 2009 Climate Variability and Visceral Leishmaniasis in Europe WHO/TDR, Jan. 2008 Late Eighties Maroli et al., Trop Med Int Health
Skin Cancer - Non-Melanoma
 Skin Cancer - Non-Melanoma Introduction Each year, millions of people find out that they have skin cancer. Skin cancer is almost 100% curable if found early and treated right away. It is possible to prevent
Skin Cancer - Non-Melanoma Introduction Each year, millions of people find out that they have skin cancer. Skin cancer is almost 100% curable if found early and treated right away. It is possible to prevent
History of Leishmaniasis (from Wikipedia)
 History of Leishmaniasis (from Wikipedia) Descriptions of conspicuous lesions similar to cutaneous leishmaniasis (CL) has been discovered on tablets from King Ashurbanipal from the 7th century BC, some
History of Leishmaniasis (from Wikipedia) Descriptions of conspicuous lesions similar to cutaneous leishmaniasis (CL) has been discovered on tablets from King Ashurbanipal from the 7th century BC, some
INHIBITION OF INTRACUTANEOUS LEISHMANIN REACTION BY HYDROCORTISONE ACETATE
 INHIBITION OF INTRACUTANEOUS LEISHMANIN REACTION BY HYDROCORTISONE ACETATE COMPARISON WITH CoRTIsoNE, ACTH, AND HYALURONIDASE* A. DOSTROVSKY, M.D. AND H. A. COHEN, M.D. The inhibitory effect of cortisone
INHIBITION OF INTRACUTANEOUS LEISHMANIN REACTION BY HYDROCORTISONE ACETATE COMPARISON WITH CoRTIsoNE, ACTH, AND HYALURONIDASE* A. DOSTROVSKY, M.D. AND H. A. COHEN, M.D. The inhibitory effect of cortisone
KINETOPLASTIDS. Kinetoplast. Nucleus
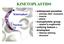 KINETOPLASTIDS Kinetoplast Nucleus widespread parasites animals (fish humans) insects plants monophyletic group related to euglenoids unifying feature = kinetoplast Giemsa staining structure KINETOPLAST
KINETOPLASTIDS Kinetoplast Nucleus widespread parasites animals (fish humans) insects plants monophyletic group related to euglenoids unifying feature = kinetoplast Giemsa staining structure KINETOPLAST
A histopathological study of cutaneous leishmaniasis in Sri Lanka
 A histopathological study of cutaneous leishmaniasis in Sri Lanka C H P Herath 1, N V I Ratnatunga 2, R Waduge 3, P Ratnayake 3, C N Ratnatunga 4, S Ramadasa 2 (Index words: cutaneous leishmaniasis, histopathology,
A histopathological study of cutaneous leishmaniasis in Sri Lanka C H P Herath 1, N V I Ratnatunga 2, R Waduge 3, P Ratnayake 3, C N Ratnatunga 4, S Ramadasa 2 (Index words: cutaneous leishmaniasis, histopathology,
Departments of Dermatology, Venereology and Leprosy and *Microbiology, Indira Gandhi Medical College, Shimla, India.
 Net Study Comparative efþ cacy of intralesional sodium stibogluconate (SSG) alone and its combination with intramuscular SSG to treat localized cutaneous leishmaniasis: Results of a pilot study Ajeet K.
Net Study Comparative efþ cacy of intralesional sodium stibogluconate (SSG) alone and its combination with intramuscular SSG to treat localized cutaneous leishmaniasis: Results of a pilot study Ajeet K.
Periocular skin cancer
 Periocular skin cancer Information for patients Skin cancer involving the skin of the eyelid or around the eye is called a periocular skin cancer. Eyelid skin cancers occur most often on the lower eyelid,
Periocular skin cancer Information for patients Skin cancer involving the skin of the eyelid or around the eye is called a periocular skin cancer. Eyelid skin cancers occur most often on the lower eyelid,
Yellow fever. Key facts
 From: http://www.who.int/en/news-room/fact-sheets/detail/yellow-fever WHO/E. Soteras Jalil Yellow fever 14 March 2018 Key facts Yellow fever is an acute viral haemorrhagic disease transmitted by infected
From: http://www.who.int/en/news-room/fact-sheets/detail/yellow-fever WHO/E. Soteras Jalil Yellow fever 14 March 2018 Key facts Yellow fever is an acute viral haemorrhagic disease transmitted by infected
GENUS: LEISHMANIA. Under the genus Leishmania, there are 2 subgenus: SPECIES PARASITIC IN MEN. Under subgenus Leishmania, there are following species:
 GENUS: LEISHMANIA Species parasitic in man: Under the genus Leishmania, there are 2 subgenus: 1. Leishmania 2. Viannia SPECIES PARASITIC IN MEN Under subgenus Leishmania, there are following species: LEISHMANIA
GENUS: LEISHMANIA Species parasitic in man: Under the genus Leishmania, there are 2 subgenus: 1. Leishmania 2. Viannia SPECIES PARASITIC IN MEN Under subgenus Leishmania, there are following species: LEISHMANIA
manifestations are uncommon. Initial descriptions of the disease (Rosai and Dorfman, 1969) specifically
 Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
Visceral leishmaniasis: an endemic disease with global impact
 Visceral leishmaniasis: an endemic disease with global impact Professor Olivier Lortholary, MD, PhD Department of Infectious and Tropical diseases Hôpital Necker-Enfants Malades Université Paris Descartes
Visceral leishmaniasis: an endemic disease with global impact Professor Olivier Lortholary, MD, PhD Department of Infectious and Tropical diseases Hôpital Necker-Enfants Malades Université Paris Descartes
Everything you ever wanted to know about Zika Virus Disease
 Everything you ever wanted to know about Zika Virus Disease (in 14 slides) Jon Temte, MD/PhD University of Wisconsin School of Medicine and Public Health 28 January 2016 Zika Virus mosquito-borne flavivirus
Everything you ever wanted to know about Zika Virus Disease (in 14 slides) Jon Temte, MD/PhD University of Wisconsin School of Medicine and Public Health 28 January 2016 Zika Virus mosquito-borne flavivirus
 Malaria parasites Malaria parasites are micro-organisms that belong to the genus Plasmodium. There are more than 100 species of Plasmodium, which can infect many animal species such as reptiles, birds,
Malaria parasites Malaria parasites are micro-organisms that belong to the genus Plasmodium. There are more than 100 species of Plasmodium, which can infect many animal species such as reptiles, birds,
Alberta Health Public Health Notifiable Disease Management Guidelines January 2013
 January 2013 Rickettsial Infections Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) January 2013 January 2013 December
January 2013 Rickettsial Infections Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) January 2013 January 2013 December
Animal Models of Leishmaniasis Relevant to Vaccine Development. David Sacks Laboratory of Parasitic Diseases NIAID, NIH
 Animal Models of Leishmaniasis Relevant to Vaccine Development David Sacks Laboratory of Parasitic Diseases NIAID, NIH Leishmaniasis: A spectrum of diseases associated with a diversity of parasite species,
Animal Models of Leishmaniasis Relevant to Vaccine Development David Sacks Laboratory of Parasitic Diseases NIAID, NIH Leishmaniasis: A spectrum of diseases associated with a diversity of parasite species,
ISPUB.COM. Cutaneous Leishmaniasis in Iran. C Yazdi, M Narmani, B Sadri INTRODUCTION CASE 1 CASE 2
 ISPUB.COM The Internet Journal of Infectious Diseases Volume 3 Number 1 Cutaneous Leishmaniasis in Iran C Yazdi, M Narmani, B Sadri Citation C Yazdi, M Narmani, B Sadri. Cutaneous Leishmaniasis in Iran.
ISPUB.COM The Internet Journal of Infectious Diseases Volume 3 Number 1 Cutaneous Leishmaniasis in Iran C Yazdi, M Narmani, B Sadri Citation C Yazdi, M Narmani, B Sadri. Cutaneous Leishmaniasis in Iran.
Viral Hemorrhagic Fevers
 Viral Hemorrhagic Fevers (VHFs) http://www.ncrr.nih.gov/publications/ncrr_reporter/summer-fall2009/images/essential_2.jpg Definition Viral hemorrhagic fevers (VHFs) refer to a group of illnesses that are
Viral Hemorrhagic Fevers (VHFs) http://www.ncrr.nih.gov/publications/ncrr_reporter/summer-fall2009/images/essential_2.jpg Definition Viral hemorrhagic fevers (VHFs) refer to a group of illnesses that are
Introduction to Lesson 4 - The Lymphatic System
 Introduction to Lesson 4 - The Lymphatic System Your circulatory system is not your body s only vascular transport system. Closely associated with the blood vessels of the circulatory system is the lymphatic
Introduction to Lesson 4 - The Lymphatic System Your circulatory system is not your body s only vascular transport system. Closely associated with the blood vessels of the circulatory system is the lymphatic
Epidemiological Study of Cutaneous Leishmaniasis in Tuz
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 477-483 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.056
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 477-483 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.056
Invest in the future, defeat malaria
 Invest in the future, defeat malaria Malaria is caused by parasites from the genus Plasmodium, which are spread to people by infected mosquitoes. There are five species of Plasmodium that can infect humans.
Invest in the future, defeat malaria Malaria is caused by parasites from the genus Plasmodium, which are spread to people by infected mosquitoes. There are five species of Plasmodium that can infect humans.
Control of leishmaniasis
 SIXTIETH WORLD HEALTH ASSEMBLY A60/10 Provisional agenda item 12.3 22 March 2007 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
SIXTIETH WORLD HEALTH ASSEMBLY A60/10 Provisional agenda item 12.3 22 March 2007 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
0 BSERVATIONS ON THE PARASITE LEIiSHMANIA MEXICANA AMAZONENSIS AND ITS NATURAL INFECTION OF THE SAND FLY LUTZOMYIA OLMECA NOCIW
 0 BSERVATIONS ON THE PARASITE LEIiSHMANIA MEXICANA AMAZONENSIS AND ITS NATURAL INFECTION OF THE SAND FLY LUTZOMYIA OLMECA NOCIW Jorge R. Arzi~s,~ Rzli A. de Freitas, 3 Roberto D. Nazx4 and Toby K Barre&
0 BSERVATIONS ON THE PARASITE LEIiSHMANIA MEXICANA AMAZONENSIS AND ITS NATURAL INFECTION OF THE SAND FLY LUTZOMYIA OLMECA NOCIW Jorge R. Arzi~s,~ Rzli A. de Freitas, 3 Roberto D. Nazx4 and Toby K Barre&
Dual Wavelength Phototherapy System
 Dual Wavelength Phototherapy System The AKLARUS Blue and Red Combination System is an effective, drugfree alternative for treating acne & photodamaged skin. The non-invasive Aklarus treatment has been
Dual Wavelength Phototherapy System The AKLARUS Blue and Red Combination System is an effective, drugfree alternative for treating acne & photodamaged skin. The non-invasive Aklarus treatment has been
Elimination of VL in the Indian subcontinent is it achievable?
 Elimination of VL in the Indian subcontinent is it achievable? P Das Rajendra Memorial Research Institute, Patna Jorge Alvar DNDi, Geneva Bhawna Sharma DNDi, India Leishmaniasis 350 million at risk worldwide
Elimination of VL in the Indian subcontinent is it achievable? P Das Rajendra Memorial Research Institute, Patna Jorge Alvar DNDi, Geneva Bhawna Sharma DNDi, India Leishmaniasis 350 million at risk worldwide
Prevalence of Cutaneous Leishmaniasis among HIV and Non-HIV Patients attending some Selected Hospitals in Jos Plateau State
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 06 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.706.307
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 06 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.706.307
African Trypanosomes
 African Trypanosomes Giemsa-stained blood smear of African trypanosomes viewed under the 100X objective lens. The block arrows denote trypomastigote forms of the African trypanosomes found within the blood
African Trypanosomes Giemsa-stained blood smear of African trypanosomes viewed under the 100X objective lens. The block arrows denote trypomastigote forms of the African trypanosomes found within the blood
LESIONS OF THE ORAL CAVITY ORAL CAVITY. Oral Cavity Subsites 4/10/2013 LIPS TEETH GINGIVA ORAL MUCOUS MEMBRANES PALATE TONGUE ORAL LYMPHOID TISSUES
 LESIONS OF THE ORAL CAVITY David I. Kutler, MD, FACS Associate Professor Division of Head and Neck Surgery Department of Otolaryngology HNS Weill Cornell Medical Center ORAL CAVITY LIPS TEETH GINGIVA ORAL
LESIONS OF THE ORAL CAVITY David I. Kutler, MD, FACS Associate Professor Division of Head and Neck Surgery Department of Otolaryngology HNS Weill Cornell Medical Center ORAL CAVITY LIPS TEETH GINGIVA ORAL
Analysis of Enhancing Effect of Sand Fly Saliva on Leishmania Infection in Mice
 INFCTION AND IMMUNITY, May 1991, p. 1592-1598 19-9567/91/51592-7$2./ Copyright X) 1991, American Society for Microbiology Vol. 59, No. 5 Analysis of nhancing ffect of Sand Fly Saliva on Leishmania Infection
INFCTION AND IMMUNITY, May 1991, p. 1592-1598 19-9567/91/51592-7$2./ Copyright X) 1991, American Society for Microbiology Vol. 59, No. 5 Analysis of nhancing ffect of Sand Fly Saliva on Leishmania Infection
BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY
 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Cancer is a group of more than 100 different diseases that are characterized by uncontrolled cellular growth,
BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Cancer is a group of more than 100 different diseases that are characterized by uncontrolled cellular growth,
Evaluation of Thermotherapy for the Treatment of Cutaneous Leishmaniasis in Kabul, Afghanistan: A Randomized Controlled Trial
 MILITARY MEDICINE, 177, 3:345, 2012 Evaluation of Thermotherapy for the Treatment of Cutaneous Leishmaniasis in Kabul, Afghanistan: A Randomized Controlled Trial Najibullah Safi, MD*; COL Gary D. Davis,
MILITARY MEDICINE, 177, 3:345, 2012 Evaluation of Thermotherapy for the Treatment of Cutaneous Leishmaniasis in Kabul, Afghanistan: A Randomized Controlled Trial Najibullah Safi, MD*; COL Gary D. Davis,
Blood Smears Only 07 February Sample Preparation and Quality Control 12B A
 NEW YORK STATE Parasitology Proficiency Testing Program Blood Smears Only 07 February 2012 The purpose of the New York State Proficiency Testing Program in the category of Parasitology Blood Smears Only
NEW YORK STATE Parasitology Proficiency Testing Program Blood Smears Only 07 February 2012 The purpose of the New York State Proficiency Testing Program in the category of Parasitology Blood Smears Only
Mechanistic Studies of Pentamidine Analogs on Leishmania donovani Promastigotes
 Mechanistic Studies of Pentamidine Analogs on Leishmania donovani Promastigotes Undergraduate Honors Thesis The Ohio State University, College of Pharmacy Division of Medicinal Chemistry and Pharmacognosy
Mechanistic Studies of Pentamidine Analogs on Leishmania donovani Promastigotes Undergraduate Honors Thesis The Ohio State University, College of Pharmacy Division of Medicinal Chemistry and Pharmacognosy
Recognizing African swine fever 13. Post mortem findings
 Recognizing African swine fever 13 Post mortem findings Carcasses of pigs that die in the acute stage of the disease are often in good condition. In white-skinned pigs, bluish-purple discolouration of
Recognizing African swine fever 13 Post mortem findings Carcasses of pigs that die in the acute stage of the disease are often in good condition. In white-skinned pigs, bluish-purple discolouration of
Laboratory Diagnosis of Endemic
 Laboratory Diagnosis of Endemic Typhus and Rocky Mountain Spotted Fever* L. F. BADGER, M.D. P. A. Surgeon, U. S. Public Health Service, Washington, D. C. THERE is widely scattered throughout the world
Laboratory Diagnosis of Endemic Typhus and Rocky Mountain Spotted Fever* L. F. BADGER, M.D. P. A. Surgeon, U. S. Public Health Service, Washington, D. C. THERE is widely scattered throughout the world
