Modification of thermoregulatory response to heat stress by body fluid regulation
|
|
|
- Antonia Gibson
- 5 years ago
- Views:
Transcription
1 J Phys Fitness Sports Med, 1(3): (212) JPFSM: Review Article Modification of thermoregulatory response to heat stress by body fluid regulation Akira Takamata Department of Environmental Health, Nara Women s University, Kitauoya Nishimachi, Nara , Japan Received: July 1, 212 / Accepted: September 5, 212 Abstract The thermoregulatory system interacts vitally with the body fluid regulatory system. Thermoregulatory response during heat stress, such as sweating and cutaneous vasodilation, stimulates body fluid regulatory response by elevating plasma osmolality and reducing central blood volume. Isotonic hypovolemia, or baroreceptor unloading, and plasma hyperosmolality, in turn, inhibit thermoregulatory response to heat stress, suggesting that body fluid regulation is given priority over thermoregulation. On the other hand, osmoregulatory vasopressin secretion and thirst are augmented by elevated body core temperature. Heat acclimation enhances thermoregulatory response to heat stress. Adaptation of the body fluid regulatory system, such as increased plasma volume and reduced osmotic inhibition of thermoregulatory response, is possibly involved in the mechanism for the enhancement of thermoregulatory response to heat stress by heat acclimation. In this review, we discuss the interaction between body fluid regulation, especially osmoregulation, and thermoregulation mainly in humans. Keywords : Osmoregulation, Volume Regulation, Sweating, Cutaneous Vasodilation, Heat Acclimation Introduction Preventing excessive heat accumulation, which causes hyperthermia, is critical for maintaining aerobic exercise performance, especially during high intensity exercise, because severe hyperthermia can be a critical factor of exhaustion during exercise 1). An increased body core temperature activates thermoregulatory response, such as sweating and cutaneous vasodilation 2), which stimulates body fluid regulatory and cardiovascular systems via hypovolemia, or baroreceptor unloading 3,4), and plasma hyperosmolality 4) ; activated body fluid regulatory and cardiovascular systems, in turn, inhibit thermoregulatory response to heat stress 4,5). Therefore, the thermoregulatory system vitally interacts with body fluid regulatory and cardiovascular systems, and maintenance of body fluid status possibly prevents progressive hyperthermia during exercise in a hot environment 4,5). The aim of this review is to discuss the interaction between body fluid regulatory and thermoregulatory systems, along with the effect of exercise training and heat acclimation on the interaction between these systems. Thermoregulation during heat stress In order to prevent excessive hyperthermia during heat stress, the thermoregulatory system increases heat Correspondence: takamata@cc.nara-wu.ac.jp loss from the body surface to the environment 2). Human autonomic thermoregulation during heat stress is accomplished by cutaneous vasodilation and sweating. Cutaneous vasodilation increases skin blood flow by reducing the vascular resistance of this region 3). Increased skin blood flow transfers heat from the body core to the surface, and increased skin temperature enhances heat dissipation from the body surface if skin temperature is higher than the atmospheric temperature. Evaporation of sweat enhances evaporative heat loss from the skin surface. Such thermoregulatory response is induced mainly by increased body core temperature, which is a signal for the negative feedback system, and by thermal input from the skin. The weight of thermal input for thermoregulatory response was estimated as for body core temperature and for mean skin temperature 6-8). Thermoregulatory response to increased body temperature can be quantified by the body temperature thresholds for the response, (represented as the body core temperature at the onset of thermoregulatory response), thermal responsiveness (represented as the increase in response per unit rise in body temperature above the threshold), and maximal response (represented as the leveling-off of a response resulting from increased body core temperature) 9). Thus, factors altering the body temperature thresholds, thermal responsiveness, and maximal response should have an impact on the regulated body core temperature during heat stress. There are several non-thermal factors which modify thermoregulatory response to heat
2 48 JPFSM: Takamata A stress 2,1,11). Among these factors, the body fluid regulatory system interacts most vitally with the thermoregulatory system 12-15). Body fluid change during heat stress and body fluid regulatory response Body fluid osmolality and volume are strictly controlled, within a very narrow range, by osmoregulatory and volume (ECF/plasma volume) regulatory systems 16). Plasma osmolality is one of the most tightly regulated homeostatic variables in mammals. A very small increase (3%) in plasma osmolality can elicit osmoregulatory vasopressin release and thirst 16-18). Vasopressin secretion and thirst are induced by increased plasma osmolality. Systemic vasopressin decreases urinary free water output by increasing free water reabsorption in the collecting duct; and water intake induced by thirst adds free water to the body. Extracellular fluid volume is regulated by the renin-angiotensin-aldosterone system (RAAS) and sodium appetite with a smaller contribution of vasopressin release and thirst 16). ECF volume is determined by sodium balance if the osmoregulatory system operates normally. RAAS decreases urinary sodium excretion by increasing sodium reabsorption, mainly in the distal tubule, and sodium appetite increases sodium content by increasing sodium intake. A relatively large decrease in plasma volume (~1 %) or blood pressure can stimulate vasopressin secretion and thirst 16). Sweating results in both hypovolemia and plasma hyperosmolality because of the hypotonic nature of sweat 19,2), and cutaneous vasodilation results in reduced central blood volume (baroreceptor unloading) by increasing blood pooling in the peripheral tissues 3,21). Therefore, the thermoregulatory response to heat stress, such as sweating and cutaneous vasodilation, stimulates both osmoregulatory and volume regulatory systems. This indicates there exists a strong interaction between thermoregulatory and body fluid regulatory systems. Effect of dehydration on thermoregulatory response to heat stress Since Adolph and associates reported that a water deficit, induced by profuse sweating during desert marching, increased the resting rectal temperature in the classic Man in the Desert in ), a number of studies have examined the effect of dehydration on thermoregulatory response. It is now well-established that dehydration attenuates thermoregulatory response, such as sweating and cutaneous vasodilation, to heat stress; and fluid replacement can reverse, at least partly, the dehydration-induced attenuation of thermoregulatory response to heat stress 4,5). However, Tokizawa et al. 23) recently reported that mild dehydration in humans attenuated autonomic thermoregulatory response and thermal sensation, but did not alter thermal pleasantness in a hot environment in human subjects, suggesting that behavioral thermoregulation will not be activated with mild dehydration. Further study is required to elucidate if hypohydration has no effect on thermal pleasantness or if severe hypohydration can attenuate thermal pleasantness. Dehydration induced by sweating, or thermal dehydration, results in extracellular fluid (ECF) sodium deficit, hypovolemia and ECF hyperosmolality. In this review, the effect of isotonic hypovolemia, or baroreceptor unloading, and plasma hyperosmolality on thermoregulatory response to heat stress are discussed separately. We also discuss the interactive effect of baroreceptor unloading and plasma hyperomolality on thermoregulatory response to heat stress. Hypovolemia and thermoregulation during heat stress To elucidate the effect of isotonic hypovolemia on thermoregulatory cutaneous vasodilation, Nadel et al. 24) examined forearm blood response to increased body temperature during exercise in diuretics-treated human subjects. They found that isotonic hypovolemia shifted the relationship between forearm blood flow/esophageal temperature response in a right/downward direction (Fig. 1), suggesting that isotonic hypovolemia inhibits thermoregulatory cutaneous vasodilation, while the effect of hyperhydration induced by antidiuretic hormon administration plus water ingestion (2 liters) was minimal. Although their data provided an insight into the inhibitory effect of isotonic hypovolemia on thermoregulatory cutaneous vasodilation, their data cannot provide us with enough information whether the inhibitory effect is caused by the increased body temperature threshold, reduced thermore Control Hypohydration Hyperhydration Fig. 1 The relationship between forearm blood flow and esophageal temperature during exercise in heat with 3 different hydration states: control, hypohydration and hyperhydration. Redrawn from Nadel, et al. (1981) 24).
3 JPFSM: Interaction between thermoregulation and body fluid regulation 481 sponsiveness, or both, because the number of data points is not enough to characterize the response. A recent study reported that isotonic hypohydration increased the body core temperature threshold for both cutaneous vasodilation during moderate exercise, but not for sweating; and isotonic hypohydration did not alter the thermal responsiveness for both cutaneous vasodilation and sweating 25). Baroreceptor unloading with use of lower body negative pressure (LBNP), which decreases central blood volume (CBV) without any change in total body fluid volume, also inhibited thermoregulatory cutaneous vasodilation during exercise 26-29) and passive body heating 28), indicating that the effect of hypovolemia is possibly mediated by the unloading of volume receptors in the cardiopulmonary region. However, Ryan and Proppe 3) reported that repletion of whole ECF volume, by isotonic saline, eliminated attenuation of the increase in iliac blood flow in dehydrated baboons; whereas the selective repletion of plasma volume by infusion of an isotonic 6% dextran solution only partly reversed attenuation. From the results, they concluded that the effect of dehydration on a thermally-induced increase in iliac vascular conductance was not due to reduced plasma volume, but rather to reduced interstitial volume 3). It is not clear if involvement of this mechanism in the hypovolemia-induced inhibition of cutaneous blood flow is specific for baboons. Although the mechanism of attenuated thermoregulatory cutaneous vasodilation by a reduced ECF volume remains controversial, involvement of cardiopulmonary baroreflex is likely involved in the inhibition of thermoregulatory cutaneous vasodilation. Kamijo et al. 31) recently examined the efferent mechanism for hypovolemia-induced inhibition of thermal cutaneous vasodilation, and they demonstrated that inhibition of cutaneous vasodilatation, induced by hypovolemia during hyperthermia, might be caused by a reduction in the skin sympathetic nerve activity component synchronized with the cardiac cycle. Their data further support the involvement of cardiopulmonary baroreflex in the hypovolemic inhibition of thermal cutaneous vasodilation. Baroreceptor unloading is likely to inhibit thermal cutaneous vasodilation, during exercise, by increasing the body core temperature threshold and decreasing both thermal responsiveness and maximal response 27). The hypovolemic effect on thermal sweating is controversial. Studies show changes in blood volume do not influence thermoregulatory sweating in exercising humans 25,32). Although Mack et al. 27) reported that baroreceptor unloading with use of LBNP inhibits thermal sweating during exercise, isotonic hypovolemia seems to inhibit thermoregulatory cutaneous vasodilation more selectively than sweating. Plasma hyperosmolality and thermoregulatory response to heat stress The effect of plasma hyperosmolality, without hypo- volemia, on thermoregulatory evaporative heat loss, including sweating and panting, has been intensively studied 12,15). Increased ECF/plasma osmolality (cell dehydration) attenuates thermal sweating in exercising humans 33,34), and goats 35), as well as respiratory evaporative heat loss in other animal species in response to passive heating 36,37). Fortney et al. 33) compared the effect of dehydration and plasma hyperosmolality on forearm blood flow, and sweating response to an increased esophageal temperature induced by moderate exercise. They found that dehydration increased the body temperature threshold for sweating and cutaneous vasodilation, and also reduced thermoresponsiveness above the threshold; whereas hyperosmolality, without hypovolemia, elevated the body temperature threshold with unchanged thermoresponsiveness. From these observations, they concluded that plasma hyperosmolality increases the body temperature threshold for thermoregulatory responses, such as sweating and cutaneous vasodilation; and hypovolemia reduces thermoresponsiveness above the threshold. Takamata et al. 38,39) reported that increased plasma osmolality elevates the esophageal temperature thresholds for both sweating and cutaneous vasodilation with thermoresponsiveness above the threshold unchanged in passively heated humans (Fig. 2). Thus, plasma hyperosmolality increases the body temperature threshold for sweating, but does not alter thermoresponsiveness during heat stress. The delayed onset of sweating and cutaneous vasodilation during heat stress, i.e. the increased esophageal temperature threshold for sweating, was the major factor resulting in greater heat storage during passive heating in a condition of cell dehydration 38,39). Animal studies have demonstrated that intracerebroventricular (ICV) 4,41) or intra-arterial 42) infusion of hypertonic solution inhibits thermoregulatory evaporative heat loss without any changes in systemic osmolality. In addition, the activity of the hypothalamic thermosensitive neurons, of slice preparations, was inhibited with a hypertonic medium 43). Thus, the mechanism of ECF/plasma hyperosmolality-induced inhibition of thermoregulatory evaporative heat loss has been considered a central effect. Cell dehydration, induced by increased ECF/plasma osmolality, stimulates thirst and vasopressin secretion 16,18). Drinking causes a rapid reduction of osmoregulatory response, such as thirst and plasma vasopressin release, before any changes in plasma osmolality or plasma volume occur. This response has been demonstrated in dogs 44), and also in humans following 24 h water deprivation 45) and hypertonic saline infusion 46). It has been hypothesized that the rapid effect of drinking is mainly mediated by mechanical stimulation of the oropharyngeal receptors; and this reflex has been called the oropharyngeal reflex. Takamata, et al. 38) examined the effect of drinking on osmotically-inhibited sweating in passively heated humans, and found that osmotic inhibition of thermal sweating was reversed immediately after drinking a small amount
4 482 JPFSM: Takamata A Fig. 2 The chenges in local chest sweating rate ( SR ch; left) and cutaneous vascular conductance ( CVC; right) as a function of the change in esophageal temperature ( T es) during passive body heating after hypertonic or isotonic saline infusion. Values are the means ± SE of 11 subjects. Modified from Takamata et al. (21) 39). because an inhibitory effect of plasma hyperosmolality on thermoregulation occurred without a reduction in plasma osmolality. While the effect of hyperosmolality on thermoregulatory evaporative heat loss has been intensively studied 12,15), the effect of increased plasma osmolality on thermoregulatory cutaneous vasodilatory response to increased body temperature has received much less attention than the effect of hypovolemia or baroreceptor unloading 21). Fortney et al. 33) compared the effects of dehydration and hyperosmolality on thermoregulatory response, such as forearm blood flow and sweating, to increased body core temperature during exercise. They reported that the esophageal temperature threshold for the increase in forearm blood flow, presumably cutaneous blood flow, was elevated in exercising human subjects by plasma hyperosmolality induced by hypertonic saline infusion following water deprivation. In contrast, Proppe 53) reported that hypovolemia, induced by diuretics treatment, attenuated the increase in iliac blood flow (iliac vascular conductance) as much as dehydration, during passive body heating in baboons; but hyperosmolality did not have such an effect. From these results, he concluded that the dehydrationinduced reduction in limb blood flow, presumably skin blood flow, is mainly caused by hypovolemia or reduced interstitial fluid volume; and that the effect of hyperosmolality is negligible. Takamata et al. 39,54) examined the effect of plasma hyperosmolality on thermoregulatory cutaneous vascular and sweating responses in humans during passive body heating. They found that the increase in esophageal temperature, required to elicit both cutaneous vasodilation and sweating ( Tes threshold for cutaneous vasodilation and sweating), increased linearly with the increase in plasma osmolality. Thus, a larger increase in Tes was required to elicit a response with the increase in plasma osmolality; and the equilibrated temperature during pasof water (Fig. 3). Several studies in humans 47,48), goats 35) and sheep 49) showed similar results, although plasma osmolality or osmoregulatory response before and after drinking were not measured in most of the studies. The recovery of sweating occurred immediately after drinking, without any change in plasma osmolality or plasma volume (Fig. 3), suggesting that this response is mediated by the receptors in the early alimentary tract, probably the oropharyngeal receptor 38,49). Because plasma osmolality remained high after drinking in a hyperosmotic condition, and drinking reversed the osmotic inhibition of thermal sweating to almost the level seen in the euhydrated condition, the local or direct effect of hyperosmolality on the sweat glands was not the main cause of the osmotic inhibition of thermal sweating in humans. Further, drinking did not have a direct effect on thermal sweating, because the sweating rate did not increase in response to drinking in the euhydrated condition. Taken together, these results suggest that the osmotic inhibitory effect on thermal sweating in humans is mainly a central effect, and drinking itself can remove this osmotic inhibition of the thermoregulatory center. The acute recovery of thermal sweating by drinking water was associated with reduced thirst ratings and reduced AVP secretion; and oropharyngeal stimulation is known to suppress osmoregulatory response, such as thirst and AVP secretion. It is postulated that drinking eliminates the osmotic inhibitory input to the thermoregulatory center 38). It hase been reported that drinking may well attenuate osmosensitive neuron activity 5,51). It is unlikely that changes in plasma AVP have a direct influence on the thermoregulatory center 52) and/or the sweat glands 19). These data allow us to speculate that the osmoreceptors or central osmoregulatory pathways, which induce both thirst and AVP secretion, are involved in the osmotic inhibition of thermoregulatory sweating. It is unlikely that thermosensitive neurons are directly inhibited by osmotic stimulus,
5 JPFSM: Interaction between thermoregulation and body fluid regulation Fig. 4 Tes thresholds for cutaneous vasodilation ( Tes for CVD), for sweating ( Tes for sweating), and Tes during thermal equilibrium as functions of plasma osmolality (Posm) during passive body heating after isotonic or hypertonic saline infusion. All data points determined for each subject, in each condition, are shown as small gray circles, and mean and SE (n=6) in each condition, as black circles. Modified from Takamata et al. (1997) 54). Fig. 3 Effect of drinking water on local chest sweating (SR ch), esophageal temperature (T es), plasma osmolality (P osm), change in plasma volume ( PV), plasma arginine vasopressin concentration ([AVP] p), and subjective thirst rating. Subjects were infused with either hypertonic saline (3 % NaCl; black circles) or isotonic saline (.9 % NaCl; gray circles) before passive body heating. Subjects drank 2-ml water at 6 min after the onset of heating (indicated by shaded column). Data are shown as mean and SE of 7 subjects. Values significantly different from values of the predrinking period are indicated by an. Modified from Takamata et al. (1995) 38). sive body heating also increased linearly with the increase in plasma osmolality. They proposed that the rise in the Tes threshold per unit increase in plasma osmolality was.44 C for cutaneous vasodilation,.34 C for sweating, and.35 C for equilibrated body core temperature increase during passive body heating (Fig. 4). The thermoresponsiveness (defined by the slope of the Tes-response relationship above the threshold) of cutaneous vasodilation was likely to be unchanged. Thus, in humans, the inhibitory effect of plasma hyperosmolality is not specific for sweating, but also for cutaneous vasodilation, and plasma hyperosmolality increases the body core temperature thresholds for both sweating and cutaneous vasodilation without a change in thermal responsiveness of these responses above the threshold. In contrast, hyperosmolality did not influence the thermally-induced increase in iliac blood flow 53). The thermally-induced increase in hind limb vascular conductance in baboons was nearly completely mimicked by an a-adrenergic receptor blockade, suggesting that there is no human-like active vasodilatory system, and that skin blood flow is controlled mainly by the reduction in vasoconstrictor tone in baboons 55). To elucidate the efferent mechanism for osmotic inhibition of thermal cutaneous vasodilation, Shibasaki et al. 56) examined the effect of plasma hyperosmolality on the cutaneous vascular response to increased body core temperature on the sites with or without treatment of bretylium, which inhibits the vasoconstrictor system. They found that bretylium treatment did not alter the osmoti-
6 484 JPFSM: Takamata A cally-inhibited cutaneous vascular response to heat stress. Thus, the osmotically-induced elevation of the internal temperature threshold for cutaneous vasodilation is due primarily to an elevation in the body core temperature threshold for the onset of active vasodilation, and not to enhancement of vasoconstrictor activity. Plasma hyperosmolality attenuates the active vasodilatory system, as well as sweating, by elevation of the body core temperature thresholds 21,56,57). Kamijo et al. 58) reported that oropharyngeal stimulation can reverse dehydration-induced inhibition of thermoregulatory cutaneous vasodilation in exercising humans, suggesting that the mechanism for osmotic inhibition of cutaneous vasodilation is the same as the mechanism for osmotic inhibition of sweating. The central osmoreceptor or osmoregluratory pathway, involved in thirst and vasopressin secretion, might be involved in the osmotic inhibition of thermal cutaneous vasodilation 38,58). In contrast to the effect on autonomic thermoregulatory response, plasma hyperosmolality augmented heatescape and cold-seeking behavior in rats 59,6), suggesting that behavioral thermoregulation is enhanced by plasma hyperosmolality. It was also reported that dehydrated sheep, exposed to heat, exhibit selective brain cooling up to threefold greater than when euhydrated 61). These responses might contribute to preventing excessive water loss and hyperthermia by compensating osmotic inhibition of an autonomic thermoregulatory response. Interactive effect of plasma hyperosmolality and baroreceptor unloading on thermoregulatory response to heat stress There are a few studies examining the interactive effect of hypovolemia, or baroreceptor unloading, and plasma hyperosmolality on thermoregulatory response. Nakajima, et al. 62) examined the effect of isotonic hypovolemia, induced by diuretic treatment, and hyperosmolality induced by subcutaneous injection of hypertonic saline in rats, and they found that hypovolemia attenuated a maximal tail vasodilatory response to hyperthermia; and plasma hyperosmolality, with hypovolemia, increased the body core temperature threshold for tail vasodilation without further reduction in tail vascular conductance. The effect of hypovolemia and plasma hyperosmolality seemed to have an additive effect in their study. However, the mode of interactive action of hypovolemia and hyperosmolality remains unknown from their study, because the effect of hyperosmolality without hypovolemia was not examined. Further, regulation of tail vascular response to increased temperature is different from human cutaneous vascular response because the tail is rich in arteriovenous anastomoses (AVAs) 63). It is hard to compare the regulation of cutaneous blood flow in rats with such regulation in humans. In humans, Ito, et al. 64) found that the decrease in peripheral vascular conductance, in response to baroreceptor unloading, became larger during hyperthermia. They concluded that an interactive effect exists of plasma osmolality and central hypovolemia on peripheral vascular response during heat stress, but not in normothermia. Thus, plasma osmolality and baroreceptor unloading have a synergistic effect on thermoregulatory active vasodilation. On the other hand, Lynn et al. 65) reported an additive effect of hyperosmolality and baroreceptor unloading on the onset threshold for increases in CVC during whole body heat stress, while the onset threshold for sweating during heat stress was only elevated by hyperosmolality, with no effect of the baroreflex. Further study is required to fully elucidate the interactive effect of plasma osmolality and baroreceptor unloading on thermoregulatory response to heat stress. Thermal modification of osmoregulation Body fluid volume and its osmolality are controlled within a very narrow range by the osmoregulatory and volume (ECF volume) regulatory systems 16). Fluid regulatory hormone vasopressin secretion and thirst are stimulated by extracellular fluid hyperosmolality, i.e., cell dehydration, and are also stimulated, to a lesser extent, by hypovolemia including reduced atrial or arterial blood pressure 18). There are several factors, other than plasma hyperosmolality and/or hypovolemia, which stimulate vasopressin secretion, such as nausea, pain, hypoxia, and hypoglycemia, etc. 18,66). In addition to these influences, several studies have revealed that heat exposure elevates plasma vasopressin concentration and reduces the urinary excretion rate 67-69), suggesting that an increased body temperature is a potential factor for vasopressin secretion. Thermal dehydration induces both ECF hyperosmolality (cell dehydration) and ECF sodium deficit (hypovolemia), and thermoregulatory cutaneous vasodilation reduces central blood volume (central hypovolemia). Forsling et al. 67) reported that whole body passive heating increased plasma vasopressin concentration in pigs, and hypothalamic cooling reduced this response; but they found inconsistent changes in plasma vasopressin concentration with hypothalamic or spinal cord heating and cooling in cold, thermoneutral and warm conditions. Szczepanska-Sadowska 7) reported that hypothalamic heating augmented AVP secretion in dogs. Takamata et al. 71) examined the effect of passive body heating on osmoregulatory responses in humans, such as vasopressin secretion and subjective thirst. They reported that passive body heating, without changing plasma osmolality, did not increase plasma vasopressin concentration. They also reported thatwhile the hypertonic saline infusion increased vasopressin secretion in both hyperthermic and normothermic conditions, the increase in plasma vasopressin concentration was much higher during hyperthermia than normothermia, and fluid intake following infusion was
7 JPFSM: Interaction between thermoregulation and body fluid regulation 485 also larger under hyperthermia; although the increase in plasma osmolality during and after infusion was similar (Fig. 5). Thus, the effect of hyperthermia was dependent on the level of plasma osmolality. From these results, Takamata et al. 71) concluded that the effect of the increase in body temperature on vasopressin secretion is plasma osmolality dependent; and the contradictory literature concerning the effects of increased body temperature may be due to a lack of strict control of plasma osmolality. The augmented osmosensitivity for vasopressin secretion and thirst, caused by increased body temperature, would contribute to body fluid restoration and conservation during progressive thermal dehydration. A recent study demonstrated that the trpv1 gene is required in the AVP neurons Lower leg immersion 3 % NaCl infusion Thermoneutral Passive heating Cutaneous circulation is controlled primarily by thermal drive or body temperature, and a couple of nonthermal factors are known to modify this thermoregulatory cutaneous vascular response 21,29). It has been reported that exercise inhibits thermoregulatory cutaneous vasodilation in an exercise intensity-dependent manner. Light exercise does not alter thermoregulatory cutaneous vasodilation, while moderate to heavy exercise inhibits cutaneous vascular response by elevating the body temperature threshold 74-76). An increase in plasma osmolality occurs in response to exercise intensity in a fashion similar to the elevation of the body core temperature threshold for cutaneous vasodilation 77-79). Takamata et al. 8) examined the relationship between the increase in body temperature, required to elicit cutaneous vasodilation ( Tes threshold for cutaneous vasodilation), and plasma osmolality during light/moderate exercise (~3 and 55 % of peak V O 2 ) and passive body heating. Then they compared that relationship with data obtained in their previous study, of the same subjects, in which they determined the relationships during passive body heating following isotonic (.9% NaCl) or hypertonic (2 to 3% NaCl) saline infusion 54). The results showed that the relationship between the Tes threshold for cutaneous vasodilation and plasma osmolality was shown to be on the same regression line, both during exercise and during passive body heating, with or without infusions (Fig. 6). Those data suggest that the elevation of the body core temperature threshold for cutaneous vasodilation could be the result of increased plasma osmolality induced by exercise, and not due to reduced plasma volume or the intensity of exercise itself. Mitono et al. 81) examined further to elucidate the involvement of increased plasma osmolality during exercise in the elevation of the body core temperature threshold for cutaneous vasodilation. They infused hypotonic saline to prevent exercise-induced hyperosmolality, and determined the body core temperature threshold for cutaneous vasodilation. They found that elevation of the body core temperature threshold, for forearm vascular conductance, was attenuated by an acute hypotonic saline infusion, suggesting that the exercise-induced increase in the body core temperature threshold for forearm vascular conductance is at least partially attributed to the increased plasma osmolality induced by exercise 8,81). Both exercise-induced inhibition and osmotic inhibi- Rehydration Fig. 5 Plasma osmolality, subjective thirst rating, plasma arginine vasopressin concentration ([AVP]p), and cumulative water intake (CWI), before, during, and after hypertonic saline infusion. Values are mean and SE of seven subjects. Significant differences between thermoneutral and passive heating are indicated by an. Modified from Takamata et al. (1995) 71). for thermally-induced vaspressin secretion. Thus, the AVP neurons are likely to be thermosensitive 72). The interactive effect of body temperature and osmolality on AVP secretion remains unkinown. However, a similar interaction has been provided by the demonstration that TRPV4- expressing cells show a noticeably greater response to hypotonicity at 37 C than at room temperature 73). Thermoregulatory cutaneous vasodilation during exercise: Involvement of osmoregulation
8 486 JPFSM: Takamata A tion of cutaneous vasodilation, by the increased body core temperature threshold, are not due to increased sympathetic vasoconstrictor tone, but rather to attenuated active vasodilator outflow 56,82). Therefore, the mechanism for exercise-induced elevation of the core temperature threshold for cutaneous vasodilation can be mediated by increased plasma osmolality; and, thus, the hypothesis can be supported that hyperosmolality, induced by exercise, is involved in the elevation of the body core temperature threshold for cutaneous vasodilation during intense exercise. Fig. 6 Relationship between Tes threshold for cutaneous vasodilation ( T es for CVD) and plasma osmolality (P osm) during light (black circles) and moderate exercise (black triangles) and passive heating (white circle), and passive body heating with isotonic or hypertonic saline infusion (gray circles). Mean and SE values for each condition are shown as large symbols. Modified from Takamata et al. (1998) 8). Heat acclimation and osmoregulatory adaptation Due to the hypotonic nature of sweat 19), profuse sweating during prolonged heat exposure and/or exercise results in hyperosmotic hypovolemia. Heat acclimation reduces sweat sodium concentration 83-85), and therefore, the increase in plasma osmolality at a given sweat output should be larger in heat-acclimated people, which would be beneficial to maintain ECF/plasma volume during prolonged sweating because a larger increase in ECF/plasma osmolality draws more free water from the intracellular to the extracellular space 86). Thus, hypovolemic inhibition of thermoregulatory response, mainly cutaneous vascular response, is expected to become smaller with heat acclimation, by preventing excessive ECF loss 87). Heat acclimation improves thermal endurance 1,83), and shifts the body temperature threshold for sweating and cutaneous vasodilation to a lower body core temperature 88), although the sweat sodium concentration is decreased. Takamata et al. 39) determined the relationship between osmotic inhibition of thermoregulatory response and sweat sodium concentration in 11 subjects. The osmotic inhibition was quantified as an increase in Tes threshold for sweating and cutaneous vasodilation per unit rise in plasma osmolality. As shown in Fig. 7, osmotic inhibition of thermoregulatory sweating and cutaneous vasodilation were linearly correlated with sweat sodium concentration. These results suggest that heat acclimation could attenuate the osmotic inhibitory effect on thermoregulation. The effect of heat acclimation is likely to be specific to the osmotic inhibition of thermoregulation, but not to osmoregulation in general, because osmosensitivity for vasopressin secretion is not related to sweat sodium concentration. Ichinose et al. 89) examined the effect of heat acclimation on osmotic inhibition of thermoregulatory response (longitudinal study). They found that osmotic elevation of the body core temperature threshold for cu- Fig. 7 Relationship between the shift in Tes threshold for sweating per unit rise in plasma osmolality (Osmotic shift in Tes for sweating) and sweat sodium concentration (left), and between osmotic shift in Tes for cutaneous vasodiltion (CVD) and sweat sodium concentration. Modified from Takamata et al. (21) 39).
9 JPFSM: Interaction between thermoregulation and body fluid regulation 487 taneous vasodilation was attenuated by ten-day exercise training, but not for sweating. They also found that attenuation of osmotic elevation of the body core temperature threshold for cutaneous vasodilation was correlated with plasma volume expansion by exercise training. Taken together, osmoregulatory adaptation is possibly involved in the mechanism of heat acclimation, in addition to the involvement of plasma volume expansion 4,9). This osmoregulatory adaptation contributes to maintaining a lower body temperature during progressive heat exposure or during exercise accompanied by profuse sweating. Conclusions The maintenance of body fluid volume and osmolality, as an internal environment, is essential to maintaining the physiological functions of organisms. In this review, the authorrs have shown that thermoregulatory function was inhibited by plasma hyperosmolality, and that hyperthermia augments osmoregulatory vasopressin secretion and thirst. It was also demonstrated that osmoregulatory adaptation is possibly involved in the mechanism of heat acclimation. Although accumulated data suggest that the interaction between osmoregulation and thermoregulation occurs in the central nervous system, the central mechanism of this interaction still remains unknown. It is expected that future studies will investigate the mechanisms for the interaction between body fluid regulation and thermoregulation. References 1) Nielsen B, Hales JR, Strange S, Christensen NJ, Warberg J, Saltin B Human circulatory and thermoregulatory adaptations with heat acclimation and exercise in a hot, dry environment. J Physiol (Lond). 46: ) Nadel ER Recent advances in temperature regulation during exercise in humans. Fed Proc. 44: ) Rowell LB Cardiovascular adjustments to thermal stress. In: Handbook of Physiology. Peripheral Circulation and Organ Blood Flow. (Shepherd JT, Abboud FM, eds.), pp , American Physiological Society, Bethesda, MD. 4) Sawka MN, Montain SJ. 2. Fluid and electrolyte supplementation for exercise heat stress. Am J Clin Nutr. 72: 564S- 572S. 5) Takamata A, Morimoto T, Nose H. 21. Interrelationship between osmoregulation and thermoregulation in a hot environment and during exercise. In: Exercise, Nutrition, and Environmental Stress (Nose H, Gisolfi CV, Imaizumi K, eds.), 1: , Cooper Publishing Group, LLC., MI, USA. 6) Nadel ER, Bullard RW, Stolwijk JAJ Importance of skin temperature in the regulation of sweating. J Appl Physiol. 31: ) Nadel ER, Mitchell JW, Saltin B, Stolwijk JAJ Peripheral modifications to the central drive for sweating. J Appl Physiol. 31: ) Wenger CB, Roberts MF, Stolwijk JAJ, Nadel ER Forearm blood flow during body temperature transients produced by leg exercise. J Appl Physiol. 38: ) Werner J Temperature regulation during exercise: an overview. In Perspectives in Exercise Science and Sports Medicine Volume 6: Exercise, Heat and Thermoregulation. (Gisolfi CV, Lamb DR, Nadel ER, eds.), pp , Brown & Benchmark, Dubuque, IA. 1) Shibasaki M, Kondo N, Crandall CG. 23. Non-thermoregulatory modulation of sweating in humans. Exerc Sport Sci Rev. 31: ) Kondo N, Nishiyasu T, Inoue Y, Koga S. 21. Non-thermal modification of heat-loss responses during exercise in humans. Eur J Appl Physiol. 11: ) Baker MA Thermoregulation in dehydrated vertebrates. In: Milestones in Environmental Physiology: Progress in Biometeorology, Vol. 7. pp , SPB Academic Publishing, The Hague, The Netherlands. 13) Morimoto T Thermoregulation and body fluids: Role of blood volume and central venous pressure. Jpn J Physiol. 4: ) Nose H, Takamata A Integrative regulation of body temperature and body fluid in humans exercising in a hot environment. Int J Biometeorol. 4: ) Morimoto T, Itoh T, Takamata A Thermoregulation and body fluid in hot environment. Prog Brain Res. 115: ) Verbalis JG Clinical aspects of body fluid homeostasis in humans. In Handbook of Behavioral Neurobiology 1, Neurobiology of Food and Fluid Intake. (Stricker EM eds.), pp , Plenum Press. New York. 17) Robertson GL, Shelton RS, Athar S The osmoregulation of vasopressin. Kidney Int. 1: ) Robertson GL, Athar S The interaction of blood osmolality and blood volume in regulating plasma vasopressin in man. J Clin Endocrinol Metab. 42: ) Sato K The physiology, pharmacology, and biochemistry of eccrine sweat gland. Rev Physiol Biochem Pharmacol. 79: ) Nose H, Mack GW, Shi X, Nadel ER Shift in body fluid compartments after dehydration in humans. J Appl Physiol. 65: ) Johnson JM, Proppe DW Cardiovascular adjustments to heat stress. In Handbook of Physiology Section 4: Environmental Physiology, Vol. 1. (Fregly MJ, Blatteis CM, eds.), pp , Oxford University Press, New York. 22) Adolf EF Physiology of Man in Desert. pp , Interscience, New York. 23) Tokizawa K, Yasuhara S, Nakamura M, Uchida Y, Crawshaw LI, Nagashima K. 21. Mild hypohydration induced by exercise in the heat attenuates autonomic thermoregulatory responses to the heat, but not thermal pleasantness in humans. Physiol Behav. 1: ) Nadel ER, Fortoney SM, Wenger CB Effect of hydration state on circulatory and thermal regulation. J Appl Physiol. 49: ) Ikegawa S, Kamijo Y, Okazaki K, Masuki S, Okada Y, Nose H Effects of hypohydration on thermoregulation during exercise before and after 5-day aerobic training in a warm environment in young men. J Appl Physiol. 11: ) Mack GW, Nose H, Nadel ER Role of cardiopulmonary baroreflexes during dynamic exercise. J Appl Physiol. 65:
10 488 JPFSM: Takamata A 27) Mack G, Nishiyasu T, Shi X Baroreceptor modulation of cutaneous vasodilator and sudomotor responses to thermal stress in humans. J Physiol (Lond.). 483: ) Kellogg DL Jr, Johnson JM, Kosiba, WA Baroreflex control of cutaneous active vasodilator system in humans. Circ Res. 66: ) Kenney WL, Johnson JM Control of skin blood flow during exercise. Med Sci Sports Exerc. 24: ) Ryan K L, Proppe DW Effects of compartmental fluid repletion on heaat-induced limb vasodilation in dehydrated baboons. Am J Physiol. 259 (Regulatory Integrative Comp Physiol 28): R1139-R ) Kamijo Y-I, Okada Y, Ikegawa S, Okazaki K, Goto M, Nose H Skin sympathetic nerve activity component synchronizing with cardiac cycle is involved in hypovolaemic suppression of cutaneous vasodilatation in hyperthermia. J Physiol (Lond). 589: ) Fortney SM, Nadel ER, Wenger CB, Bove JR Effect of blood volume on sweating rate and body fluids in exercising humans. J. Appl. Physiol. 51: ) Fortney SM, Wenger CB, Bove JR, Nadel E.R Effect of hyperosmolality on control of blood flow and sweating. J Appl Physiol. 57: ) Nielsen B Effects of changes in plasma volume and osmolality on thermoregulation during exercise. Acta Physiol Scand. 9: ) Baker MA Effects of dehydration and rehydration on thermoregulatory sweating in goats. J Physiol (Lond.): 417: ) Baker M, Doris PA Control of evaporative heat loss during changes in plasma osmolality in the cat. J Physiol. (Lond.), 328: ) Kozlowski S, Greenleaf JE, Turlejska E, Nazar, K Extracellular hyperosmolality and body temperature during physical exercise in dogs. Am J Physiol. 239 (Regulatory Integrative Comp Physiol. 8), R18-R ) Takamata A, Mack GW, Gillen CM, Jozsi AC, Nadel ER Osmoregulatory modulation of thermal sweating in humans: reflex effects of drinking. Am J Physiol. 268 (Regulatory Integrative Comp Physiol. 37): R414-R ) Takamata A, Yoshida T, Nishida N, Morimoto T. 21. Relationship of osmotic inhibition in thermoregulatory responses and sweat sodium concentration in humans. Am J Physiol Regul Integr Comp Physiol. 28: R623-R629. 4) Turlejska E, Baker MA Elevated CSF osmolality inhibits thermoregulatory heat loss responses. Am J Physiol. 251 (Regulatory Integrative Comp Physiol. 2): R749-R ) Owen MD, Matthes RD, Gisolfi CV Effect of cerebrospinal fluid hyperosmolality on sweating in the heat-stressed patas monkey. J Appl Physiol. 67: ) Baker MA, Dawson DD Inhibition of thermal panting by intracarotid infusion of hypertonic saline in dogs. Am J Physiol. 249 (Regulatory Integrative Comp Physiol. 18): R787-R ) Nakashima T, Hori T, Kiyohara T, Shibata M Osmosensitivity of preoptic thermosensitive neurons in hypothalamic slices in vitro. Pflügers Arch. 45: ) Thrasher TN, Keil, LC, Ramsay D.J Drinking, oropharyngeal signals, and inhibition of vasopressin secretion in dogs. Am J Physiol. 253 (Regulatory Integrative Comp Physiol. 22): R59-R ) Geelen G, Keil LC, Kravik SE, Wade CE, Thrasher TN, Barnes PR, Pyka G, Nesvig C, Greenleaf JE Inhibition of plasma vasopressin after drinking in dehydrated humans. Am J Physiol. 247 (Regulatory Integrative Comp Physiol. 16): R968-R ) Thompson CJ, Burd JM, Baylis PH Acute suppression of plasma vasopressin and thirst after drinking in hypernatremic humans. Am J Physiol. 252 (Regulatory Integrative Comp Physiol. 21): R1138-R ) Nicolaïdis S Early systemic responses to orogastric stimulation in the regulation of food and water balance: Functional and electrophysiological data. Ann NY Acad Sci. 157: ) Senay LCJ, Christensen ML Cardiovascular and sweating responses to water ingestion during dehydration. J Appl Physiol. 2: ) McKinley MJ, McAllen RM, Whyte D, Mathai ML. 28. Central osmoregulatory influences on thermoregulation. Clin Exp Pharmacol Physiol. 35: ) Arnauld E, DuPont J Vasopressin release and firing of supraoptic neurosecretory neurones during drinking in the dehydrated monkey. Pflügers Arch. 394: ) Vincent JD, Arnauld E, Bioulac B Activity of osmosensitive single cells in the hypothalamus of the behaving monkey during drinking. Brain Res. 44: ) Owen MD, Matthes RD, Gisolfi CV Effect of CSF ANG II and AVP on sweating in the heat-stressed patas monkey. J Appl Physiol. 67: ) Proppe DW Effects of hyperosmolality and diuretics on heat-induced limb vasodilation in baboons. Am J Physiol. 258 (Regulatory Integrative Comp Physiol. 27): R39-R ) Takamata A, Nagashima K, Nose H, Morimoto T Osmoregulatory inhibition of thermally induced cutaneous vasodilation in passively heated humans. Am J Physiol. 273 (Regulatory Integrative Comp Physiol. 42): R197-R24. 55) Wyss CR, Rowell LB Lack of humanlike active vasodilation in skin of heat-stressed baboons. J Appl Physiol. 41: ) Shibasaki M, Aoki K, Morimoto K, Johnson JM, Takamata A. 29. Plasma hyperosmolality elevates the internal temperature threshold for active thermoregulatory vasodilation during heat stress in humans. AJP: Regulatory, Integrative and Comparative Physiology. 297: R ) Kellogg DL Jr, Johnson JM, Kosiba WA Selective abolition of adrenergic vasoconstrictor responses in skin by local iontophoresis of bretylium. Am J Physiol. 257 (Heart Circ. Physiol. 26): H1599-H ) Kamijo Y-I, Okumoto T, Takeno Y, Okazaki K, Inaki M, Masuki S, Nose H. 25. Transient cutaneous vasodilatation and hypotension after drinking in dehydrated and exercising men. J Physiol (Lond). 568: ) Nagashima K, Nakai S, Konishi M, Su L, Kanosue K. 21. Increased heat-escape/cold-seeking behavior following hypertonic saline injection in rats. Am J Physiol Regul Integr Comp Physiol. 28: R131-R136. 6) Konishi M, Nagashima K, Kanosue K. 22. Systemic salt loading decreases body temperature and increases heat-escape/cold-seeking behaviour via the central AT 1 and V 1 receptors in rats. J Physiol (Lond). 545: ) Fuller A, Meyer LCR, Mitchell D, Maloney SK. 27. Dehydration increases the magnitude of selective brain cooling
11 JPFSM: Interaction between thermoregulation and body fluid regulation 489 independently of core temperature in sheep. Am J Physiol Regul Integr Comp Physiol. 293: R438-R ) Nakajima Y, Nose H, Takamata A Plasma hyperosmolality and arterial pressure regulation during heating in dehydrated and awake rats. Am J Physiol. 275: R173-R ) Hales JR, Iriki M, Tsuchiya K, Kozawa E Thermallyinduced cutaneous sympathetic activity related to blood flow through capillaries and arteriovenous anastomoses. Pflügers Arch. 375: ) Ito T, Itoh T, Hayano T, Yamauchi K, Takamata A. 25. Plasma hyperosmolality augments peripheral vascular response to baroreceptor unloading during heat stress. Am J Physiol Regul Integr Comp Physiol. 289: R432-R44. 65) Lynn AG, Gagnon D, Binder K, Boushel RC, Kenny GP Divergent roles of plasma osmolality and the baroreflex on sweating and skin blood flow. Am J Physiol Regul Integr Comp Physiol. 32: R634-R ) Baylis PH Osmoregulation and control of vasopressin secretion in healthy humans. Am J Physiol., 253 (Regulatory Integrative Comp. Physiol. 22): R671-R ) Forslin ML, Ingram DL, Stanier MW Effects of various ambient temperature and of heating and cooling the hypothalamus and cervical spinal cord on antidiuretic hormone secretion and urinary osmolality in pigs. J Physiol. (Lond.) 257: ) Itoh S The release of antidiuretic hormone from the posterior pituitary body on exposure to heat. Jpn J Physiol. 4: ) Segar WE, Moore WW The regulation of antidiuretic hormone release in man: I. Effect of change in position and ambient temperature on blood ADH levels. J Clin Invest. 47: ) Szczepanska-Sadowska E Plasma ADH increase and thirst suppression elicited by preoptic heating in the dog. Am J Physiol. 226: ) Takamata A, Mack GW, Stachenfeld NS, Nadel ER Body temperature modification of osmotically induced vasopressin secretion and thirst in humans. Am J Physiol. 269 (Regulatory Integrative Comp Physiol. 38): R874-R88. 72) Sharif-Naeini R, Ciura S, Bourque CW. 28. TRPV1 gene required for thermosensory transduction and anticipatory secretion from vasopressin neurons during hyperthermia. Neuron. 58: ) Liedtke, Y. Choe, M.A. Martí-Renom, A.M. Bell, C.S. Denis, A. Sali, A.J. Hudspeth, J.M. Friedman, S. Heller. 2. Vanilloid receptor-related osmotically activated channel (VR-OAC), a candidate vertebrate osmoreceptor. Cell 13: ) Mack GW, Nose H, Takamata A, Okuno T, Morimoto T Influence of exercise intensity and plasma volume on active cutaneous vasodilation in humans. Med Sci Sports Exer. 26: ) Smolander J, Saalo J, Korhonen O Effect of work load on cutaneous vascular response to exercise. J Appl Physiol. 71: ) Taylor, W. F., Johnson, J. M., Kosiba, W. A., & Kwan, C. M Graded cutaneous vascular responses to dynamic leg exercise. J. Appl. Physiol. 64: ) Convertino VA, Keil LC, Bernauer EM, Greenleaf JE Plasma volume, osmolality, vasopressin, and renin activity during graded exercise in man. J. Appl. Physiol. 5: ) Nose H, Takamata A, Mack GW, Oda Y, Okuno T, Kang D-H, Morimoto T Water and electrolyte balance in the vascular space during graded exercise in humans. J. Appl. Physiol., 7: ) Takamata A, Nose H, Kinoshita T, Hirose M, Itoh T, Morimoto T. 2. Effect of acute hypoxia on vasopressin release and intravascular fluid during dynamic exercise in humans. Am J Physiol Regul Integr Comp Physiol. 279: R161-R168. 8) Takamata A, Nagashima K, Nose H, Morimoto T Role of plasma osmolality in the delayed onset of thermal cutaneous vasodilation during exercise in humans. Am J Physiol. 275 (Regulatory Integrative Comp Physiol. 44): R286-R29. 81) Mitono H, Endoh H, Okazaki K, Ichinose T, Masuki S, Takamata A, Nose H. 25. Acute hypoosmolality attenuates the suppression of cutaneous vasodilation with increased exercise intensity. J Appl Physiol. 99: ) Kellogg DL Jr, Johnson JM, Kosiba WA Control of internal temperature threshold for active cutaneous vasodilation by dynamic exercise. J Appl Physiol. 71: ) Nielsen B, Strange S, Christensen NJ, Warberg J, Saltin B Acute and adaptive responses in humans to exercise in a warm, humid environment. Pflügers Arch. 434: ) Kirby CR, Convertino VA Plasma aldosterone and sweat sodium concentrations after exercise and heat acclimation. J Appl Physiol. 61: ) Buono MJ, Ball KD, Kolkhorst FW. 27. Sodium ion concentration vs. sweat rate relationship in humans. J Appl Physiol. 13: ) Nose H, Mack GW, Shi X, Nadel ER Shift in body fluid compartments after dehydration in humans. J Appl Physiol. 65: ) Nose H, Mack GW, Shi X, Morimoto K, Nadel ER Effect of saline infusion during exercise on themal and circulatory regulations. J Appl Physiol. 69: ) Roberts MF, Wenger CB, Stolwijk JA, Nadel ER Skin blood flow and sweating changes following exercise training and heat acclimation. J Appl Physiol. 43: ) Ichinose T, Okazaki K, Masuki S, Mitono H, Chen M, Endoh H, Nose H. 25. Ten-day endurance training attenuates the hyperosmotic suppression of cutaneous vasodilation during exercise but not sweating. J Appl Physiol. 99: ) Okazaki K, Kamijo Y, Takeno Y, Okumoto T, Masuki S, Nose H. 22. Effects of exercise training on thermoregulatory responses and blood volume in older men. J Appl Physiol. 93:
Monday, 17 April 2017 BODY FLUID HOMEOSTASIS
 Monday, 17 April 2017 BODY FLUID HOMEOSTASIS Phenomenon: shipwrecked sailor on raft in ocean ("water, water everywhere but not a drop to drink") Why are the sailors thirsty? (What stimulated thirst?) Why
Monday, 17 April 2017 BODY FLUID HOMEOSTASIS Phenomenon: shipwrecked sailor on raft in ocean ("water, water everywhere but not a drop to drink") Why are the sailors thirsty? (What stimulated thirst?) Why
Effect of Activated Sweat Glands on the Intensity-Dependent Sweating Response to Sustained Static Exercise in Mildly Heated Humans
 Short Communication Japanese Journal of Physiology, 52, 229 233, 2002 Effect of Activated Sweat Glands on the Intensity-Dependent Sweating Response to Sustained Static Exercise in Mildly Heated Humans
Short Communication Japanese Journal of Physiology, 52, 229 233, 2002 Effect of Activated Sweat Glands on the Intensity-Dependent Sweating Response to Sustained Static Exercise in Mildly Heated Humans
Plasma hyperosmolality and arterial pressure regulation during heating in dehydrated and awake rats
 Plasma hyperosmolality and arterial pressure regulation during heating in dehydrated and awake rats YASUFUMI NAKAJIMA, HIROSHI NOSE, AND AKIRA TAKAMATA Departments of Anesthesiology and Physiology, Kyoto
Plasma hyperosmolality and arterial pressure regulation during heating in dehydrated and awake rats YASUFUMI NAKAJIMA, HIROSHI NOSE, AND AKIRA TAKAMATA Departments of Anesthesiology and Physiology, Kyoto
Drinking Strategies: Planned Drinking Versus Drinking to Thirst
 Sports Med (2018) 48 (Suppl 1):S31 S37 https://doi.org/10.1007/s40279-017-0844-6 REVIEW ARTICLE Drinking Strategies: Planned Drinking Versus Drinking to Thirst Robert W. Kenefick 1 Published online: 24
Sports Med (2018) 48 (Suppl 1):S31 S37 https://doi.org/10.1007/s40279-017-0844-6 REVIEW ARTICLE Drinking Strategies: Planned Drinking Versus Drinking to Thirst Robert W. Kenefick 1 Published online: 24
Blood Pressure Fox Chapter 14 part 2
 Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
The Journal of Physiology
 J Physiol 594.2 (2016) pp 497 506 497 Plasma hyperosmolality attenuates skin sympathetic nerve activity during passive heat stress in humans Daniel Gagnon, Steven A. Romero, Hai Ngo, Paula Y. S. Poh and
J Physiol 594.2 (2016) pp 497 506 497 Plasma hyperosmolality attenuates skin sympathetic nerve activity during passive heat stress in humans Daniel Gagnon, Steven A. Romero, Hai Ngo, Paula Y. S. Poh and
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Extracellular fluid (ECF) compartment volume control
 Water Balance Made Easier Joon K. Choi, DO. Extracellular fluid (ECF) compartment volume control Humans regulate ECF volume mainly by regulating body sodium content. Several major systems work together
Water Balance Made Easier Joon K. Choi, DO. Extracellular fluid (ECF) compartment volume control Humans regulate ECF volume mainly by regulating body sodium content. Several major systems work together
Body fluids. Lecture 13:
 Lecture 13: Body fluids Body fluids are distributed in compartments: A. Intracellular compartment: inside the cells of the body (two thirds) B. Extracellular compartment: (one third) it is divided into
Lecture 13: Body fluids Body fluids are distributed in compartments: A. Intracellular compartment: inside the cells of the body (two thirds) B. Extracellular compartment: (one third) it is divided into
SODIUM INGESTION, THIRST AND DRINKING DURING ENDURANCE EXERCISE
 SSE #122 Sports Science Exchange (2014) Vol. 27, No. 122, 1-5 SODIUM INGESTION, THIRST AND DRINKING DURING ENDURANCE EXERCISE Nina S. Stachenfeld The John B. Pierce Laboratory Department of Obstetrics,
SSE #122 Sports Science Exchange (2014) Vol. 27, No. 122, 1-5 SODIUM INGESTION, THIRST AND DRINKING DURING ENDURANCE EXERCISE Nina S. Stachenfeld The John B. Pierce Laboratory Department of Obstetrics,
The role of oropharnygeal receptors in thirst perception after dehydration and rehydration
 Niger. J. Physiol. Sci. 29(June 2014) 037 042 www.njps.com.ng The role of oropharnygeal receptors in thirst perception after dehydration and rehydration * Obika, LFO., Okpere, S.O., Ozoene, J.O. and Amabebe,
Niger. J. Physiol. Sci. 29(June 2014) 037 042 www.njps.com.ng The role of oropharnygeal receptors in thirst perception after dehydration and rehydration * Obika, LFO., Okpere, S.O., Ozoene, J.O. and Amabebe,
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D.
 Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Physiology of osmo- and volume regulation, LOs #78 & #79
 Physiology of osmo- and volume regulation, LOs #78 & #79 Gyöngyi Karcsúné Kis, MSc, PhD 2 nd March 2018 Characteristic Osmoregulation Volume regulation What is being sensed Plasma osmolality Effective
Physiology of osmo- and volume regulation, LOs #78 & #79 Gyöngyi Karcsúné Kis, MSc, PhD 2 nd March 2018 Characteristic Osmoregulation Volume regulation What is being sensed Plasma osmolality Effective
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance
 Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Mechanisms underlying the postexercise attenuation of skin blood flow and sweating. Ryan McGinn B.Sc., University of Ottawa, 2013
 Mechanisms underlying the postexercise attenuation of skin blood flow and sweating Ryan McGinn B.Sc., University of Ottawa, 2013 Thesis submitted to the Faculty of Graduate and Postdoctoral Studies In
Mechanisms underlying the postexercise attenuation of skin blood flow and sweating Ryan McGinn B.Sc., University of Ottawa, 2013 Thesis submitted to the Faculty of Graduate and Postdoctoral Studies In
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are
 Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
 Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Chapter 12. Temperature Regulation
 Chapter 12 Temperature Regulation Temperature Regulation Body core temperature regulation Critical for: Cellular structures Metabolic pathways Too high Protein structure of cells destroyed Too low Slowed
Chapter 12 Temperature Regulation Temperature Regulation Body core temperature regulation Critical for: Cellular structures Metabolic pathways Too high Protein structure of cells destroyed Too low Slowed
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Diurnal variation in cutaneous vasodilator and vasoconstrictor systems during heat stress
 Am J Physiol Regulatory Integrative Comp Physiol 281: R591 R595, 2001. Diurnal variation in cutaneous vasodilator and vasoconstrictor systems during heat stress KEN AOKI, 1,2 DAN P. STEPHENS, 1 AND JOHN
Am J Physiol Regulatory Integrative Comp Physiol 281: R591 R595, 2001. Diurnal variation in cutaneous vasodilator and vasoconstrictor systems during heat stress KEN AOKI, 1,2 DAN P. STEPHENS, 1 AND JOHN
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Pathophysiology: Regulation of Water Intake and Excretion, Ghent 03/2013. Outline: Regulation of water intake and excretion
 Pathophysiology: Regulation of Water Intake and Excretion, Ghent 03/2013 Daniel G. Bichet, M.D. Université de Montréal Groupe des Protéines Membranaires; Service de néphrologie, Hôpital du Sacré- Cœur
Pathophysiology: Regulation of Water Intake and Excretion, Ghent 03/2013 Daniel G. Bichet, M.D. Université de Montréal Groupe des Protéines Membranaires; Service de néphrologie, Hôpital du Sacré- Cœur
8. URINE CONCENTRATION
 8. URINE CONCENTRATION The final concentration of the urine is very dependent on the amount of liquid ingested, the losses through respiration, faeces and skin, including sweating. When the intake far
8. URINE CONCENTRATION The final concentration of the urine is very dependent on the amount of liquid ingested, the losses through respiration, faeces and skin, including sweating. When the intake far
Fal Fal P h y s i o l o g y 6 1 1, S a n F r a n c i s c o S t a t e U n i v e r s i t y
 Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
Chapter Nine. Temperature Regulation, Thirst, and Hunger
 Chapter Nine Temperature Regulation, Thirst, and Hunger Regulating Systems Homeostasis: Physiological equilibrium Epic FAIL with weight? Obesity rates 1980-2000 Motivation: Activating and directing behavior
Chapter Nine Temperature Regulation, Thirst, and Hunger Regulating Systems Homeostasis: Physiological equilibrium Epic FAIL with weight? Obesity rates 1980-2000 Motivation: Activating and directing behavior
Fluids and electrolytes
 Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Fluid and electrolyte balance, imbalance
 Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
The Urinary System 15PART B. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
9/20/2010. Exercise Science: Theory: Hydration KEY POINTS. 1. Water is weird stuff. That s why it s so important.
 Exercise Science: Theory: Hydration Bob Murray, PhD, FACSM Founder & Principal, Sports Science Insights, LLC www.sportsscienceinsights.com bob@sportsscienceinsights.com 7 5 3 6 2 Boise State University
Exercise Science: Theory: Hydration Bob Murray, PhD, FACSM Founder & Principal, Sports Science Insights, LLC www.sportsscienceinsights.com bob@sportsscienceinsights.com 7 5 3 6 2 Boise State University
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
HOMEOSTASIS 37 C. ph of % blood sugar
 HOMEOSTASIS ph of 7.35 37 C 0.1% blood sugar Homeostasis an equilibrium (steady state) between an organism s various physiological functions, and between the organism and the environment. This is a balance
HOMEOSTASIS ph of 7.35 37 C 0.1% blood sugar Homeostasis an equilibrium (steady state) between an organism s various physiological functions, and between the organism and the environment. This is a balance
BODY FLUID. Outline. Functions of body fluid Water distribution in the body Maintenance of body fluid. Regulation of fluid homeostasis
 BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
Body Water ANS 215 Physiology and Anatomy of Domesticated Animals
 Body Water ANS 215 Physiology and Anatomy of Domesticated Animals I. Body Water A. Water is the most abundant constituent comprising 60% of total body weight. 1. Solvent for many chemicals of the body
Body Water ANS 215 Physiology and Anatomy of Domesticated Animals I. Body Water A. Water is the most abundant constituent comprising 60% of total body weight. 1. Solvent for many chemicals of the body
significant increases in e.h.l. ( W/kg, P < 0-001) and reductions in Tb ( OC,
 J. Phy8iol. (1982), 328, pp. 535-545 535 With 2 text-figure8 Printed in Gireat Britain CONTROL OF EVAPORATIVE HEAT LOSS DURING CHANGES IN PLASMA OSMOLALITY IN THE CAT BY M. A. BAKER AND P. A. DORIS* From
J. Phy8iol. (1982), 328, pp. 535-545 535 With 2 text-figure8 Printed in Gireat Britain CONTROL OF EVAPORATIVE HEAT LOSS DURING CHANGES IN PLASMA OSMOLALITY IN THE CAT BY M. A. BAKER AND P. A. DORIS* From
Blood pressure control Contin. Reflex Mechanisms. Dr. Hiwa Shafiq
 Blood pressure control Contin. Reflex Mechanisms Dr. Hiwa Shafiq 17-12-2018 A. Baroreceptor reflexes Baroreceptors (stretch receptors) located in the walls of several large systemic arteries( specially
Blood pressure control Contin. Reflex Mechanisms Dr. Hiwa Shafiq 17-12-2018 A. Baroreceptor reflexes Baroreceptors (stretch receptors) located in the walls of several large systemic arteries( specially
Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi
 Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi At the end of this lecture student should be able to describe: The loop of Henle is referred to as countercurrent
Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi At the end of this lecture student should be able to describe: The loop of Henle is referred to as countercurrent
Cardiovascular System B L O O D V E S S E L S 2
 Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Chapter 24 Water, Electrolyte and Acid-Base Balance
 Chapter 24 Water, Electrolyte and Acid-Base Balance Total body water for 150 lb. male = 40L 65% ICF 35% ECF 25% tissue fluid 8% blood plasma, lymph 2% transcellular fluid (CSF, synovial fluid) Water Movement
Chapter 24 Water, Electrolyte and Acid-Base Balance Total body water for 150 lb. male = 40L 65% ICF 35% ECF 25% tissue fluid 8% blood plasma, lymph 2% transcellular fluid (CSF, synovial fluid) Water Movement
DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI Page 1 Page 2 syndrome of inappropriate secretion of antidiuretic hormone in malignancy
DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI Page 1 Page 2 syndrome of inappropriate secretion of antidiuretic hormone in malignancy
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
I. Metabolic Wastes Metabolic Waste:
 I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
(WBGT) AND BODY WEIGHT LOSS, FLUID INTAKE AND SWEAT LOSS DURING PHYSICAL EXERCISE
 RELATIONSHIPS BETWEEN ENVIRONMENTAL TEMPERATURE (WBGT) AND BODY WEIGHT LOSS, FLUID INTAKE AND SWEAT LOSS DURING PHYSICAL EXERCISE SEIICHI NAKAI, TETSUYA YOSHIDA, AKIRA Y0RIM0T0, NAOKI OKAMOTO and TAKETOSHI
RELATIONSHIPS BETWEEN ENVIRONMENTAL TEMPERATURE (WBGT) AND BODY WEIGHT LOSS, FLUID INTAKE AND SWEAT LOSS DURING PHYSICAL EXERCISE SEIICHI NAKAI, TETSUYA YOSHIDA, AKIRA Y0RIM0T0, NAOKI OKAMOTO and TAKETOSHI
body temperature was consistently and completely suppressed by simultaneous cooling of the thermode in the pre-optic region to 5 or 10 C.
 J. Phygiol. (1976), 257, pp. 673-686 673 With 4 text-figurem Printed in Great Britain EFFECTS OF VARIOUS AMBIENT TEMPERATURES AND OF HEATING AND COOLING THE HYPOTHALAMUS AND CERVICAL SPINAL CORD ON ANTIDIURETIC
J. Phygiol. (1976), 257, pp. 673-686 673 With 4 text-figurem Printed in Great Britain EFFECTS OF VARIOUS AMBIENT TEMPERATURES AND OF HEATING AND COOLING THE HYPOTHALAMUS AND CERVICAL SPINAL CORD ON ANTIDIURETIC
Neural control and mechanisms of eccrine sweating during heat stress and exercise
 Invited Review J Appl Physiol 100: 1692 1701, 2006; doi:10.1152/japplphysiol.01124.2005. HIGHLIGHTED TOPIC and Mammalian Thermoregulation A Physiological Systems Approach to Human Neural control and mechanisms
Invited Review J Appl Physiol 100: 1692 1701, 2006; doi:10.1152/japplphysiol.01124.2005. HIGHLIGHTED TOPIC and Mammalian Thermoregulation A Physiological Systems Approach to Human Neural control and mechanisms
Effects of Hydration on Mental and Cognitive Processes in Children and Adults
 Effects of Hydration on Mental and Cognitive Processes in Children and Adults Matthew S. Ganio, Ph.D. Assistant Professor of Exercise Science Director, Human Performance Laboratory Department of Health,
Effects of Hydration on Mental and Cognitive Processes in Children and Adults Matthew S. Ganio, Ph.D. Assistant Professor of Exercise Science Director, Human Performance Laboratory Department of Health,
Chapter 15 Fluid and Acid-Base Balance
 Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
CHAPTER 27 LECTURE OUTLINE
 CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
FLUID THERAPY: IT S MORE THAN JUST LACTATED RINGERS
 FLUID THERAPY: IT S MORE THAN JUST LACTATED RINGERS Elisa M. Mazzaferro, MS, DVM, PhD, DACVECC Cornell University Veterinary Specialists, Stamford, CT, USA Total body water constitutes approximately 60%
FLUID THERAPY: IT S MORE THAN JUST LACTATED RINGERS Elisa M. Mazzaferro, MS, DVM, PhD, DACVECC Cornell University Veterinary Specialists, Stamford, CT, USA Total body water constitutes approximately 60%
Hitoshi Wakabayashi 1,2*, Titis Wijayanto 1, Joo-Young Lee 1,3, Nobuko Hashiguchi 4, Mohamed Saat 5 and Yutaka Tochihara 1,6
 Wakabayashi et al. Journal of Physiological Anthropology 2014, 33:5 ORIGINAL ARTICLE Open Access A comparison of hydration effect on body fluid and temperature regulation between Malaysian and Japanese
Wakabayashi et al. Journal of Physiological Anthropology 2014, 33:5 ORIGINAL ARTICLE Open Access A comparison of hydration effect on body fluid and temperature regulation between Malaysian and Japanese
WOMEN ARE NOT SMALL MEN: SEX DIFFERENCES AND PERFORMANCE. Stacy T Sims, PhD
 WOMEN ARE NOT SMALL MEN: SEX DIFFERENCES AND PERFORMANCE Stacy T Sims, PhD OUTLINE Overview The Science: design and general assumptions The Menstrual Cycle: Fluid Balance Thermoregulation Metabolism: Fuel
WOMEN ARE NOT SMALL MEN: SEX DIFFERENCES AND PERFORMANCE Stacy T Sims, PhD OUTLINE Overview The Science: design and general assumptions The Menstrual Cycle: Fluid Balance Thermoregulation Metabolism: Fuel
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Fluid, Electrolyte, and Acid-Base Balance. Maintaining Water and Electrolyte Balance of Blood
 514 Essentials of Human Anatomy and Physiology Intracellular fluid volume = 25 L, 40% body weight Total body water volume = 40 L, 60% body weight Extracellular fluid (ECF) volume =15 L, 20% body weight
514 Essentials of Human Anatomy and Physiology Intracellular fluid volume = 25 L, 40% body weight Total body water volume = 40 L, 60% body weight Extracellular fluid (ECF) volume =15 L, 20% body weight
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE
 Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
Regulating the Internal Environment. AP Biology
 Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform to external
Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform to external
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Water, Electrolytes, and Acid-Base Balance
 Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
(Received 11 June 1979)
 J. Phymol. (1980), 304, pp. 389-396 389 With 2 text-fiure8 Printed in Great Britain TH FFCTS OF AMBINT TMPRATUR ON URINARY FLOW AND COMPOSITION IN TH FOWL BY. AZAHAN AND A. H. SYKS From Wye College, University
J. Phymol. (1980), 304, pp. 389-396 389 With 2 text-fiure8 Printed in Great Britain TH FFCTS OF AMBINT TMPRATUR ON URINARY FLOW AND COMPOSITION IN TH FOWL BY. AZAHAN AND A. H. SYKS From Wye College, University
Hyponatremia. Mis-named talk? Basic Pathophysiology
 Hyponatremia Great Lakes Hospital Medicine Symposium by Brian Wolfe, MD Assistant Professor of Internal Medicine University of Colorado Denver Mis-named talk? Why do we care about Hyponatremia? concentration
Hyponatremia Great Lakes Hospital Medicine Symposium by Brian Wolfe, MD Assistant Professor of Internal Medicine University of Colorado Denver Mis-named talk? Why do we care about Hyponatremia? concentration
BIOH122 Session 6 Vascular Regulation
 BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
The kidneys are excretory and regulatory organs. By
 exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
Ch. 44 Regulating the Internal Environment
 Ch. 44 Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform
Ch. 44 Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform
3. The following diagram is a summary of a homeostatic mechanism for compound X.
 VCAA EXAM QUESTIONS MULTIPLE CHOICE QUESTIONS 1. Homeostasis is the condition of a relatively stable internal environment. The internal environment of a multicellular organism includes A. tissue fluid.
VCAA EXAM QUESTIONS MULTIPLE CHOICE QUESTIONS 1. Homeostasis is the condition of a relatively stable internal environment. The internal environment of a multicellular organism includes A. tissue fluid.
University of Bristol - Explore Bristol Research
 Charkoudian, N., Hart, E. C. J., Barnes, J. N., & Joyner, M. J. (2017). Autonomic control of body temperature and blood pressure: influences of female sex hormones. Clinical Autonomic Research, 27(3),
Charkoudian, N., Hart, E. C. J., Barnes, J. N., & Joyner, M. J. (2017). Autonomic control of body temperature and blood pressure: influences of female sex hormones. Clinical Autonomic Research, 27(3),
Worksheet No. FA-1705A Page 1 of 7
 Worksheet No. FA-1705A Page 1 of 7 WORKSHEET for Evidence-Based Review of Science for First Aid Worksheet author(s) Susan W. Yeargin, PhD, ATC Date Submitted for review: Initial: 11/30/09 Clinical question.
Worksheet No. FA-1705A Page 1 of 7 WORKSHEET for Evidence-Based Review of Science for First Aid Worksheet author(s) Susan W. Yeargin, PhD, ATC Date Submitted for review: Initial: 11/30/09 Clinical question.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
HYDRATION & AEROBIC PERFORMANCE: IMPACT OF ENVIRONMENT
 SSE #152 Sports Science Exchange (2015) Vol. 28, No. 152, 1-5 HYDRATION & AEROBIC PERFORMANCE: IMPACT OF ENVIRONMENT Michael N. Sawka, PhD School of Applied Physiology Georgia Institute of Technology United
SSE #152 Sports Science Exchange (2015) Vol. 28, No. 152, 1-5 HYDRATION & AEROBIC PERFORMANCE: IMPACT OF ENVIRONMENT Michael N. Sawka, PhD School of Applied Physiology Georgia Institute of Technology United
For more information about how to cite these materials visit
 Author(s): Michael Heung, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Michael Heung, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Body water content. Fluid compartments. Regulation of water output. Water balance and ECF osmolallty. Regulation of water intake
 Body water content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; females 50% This difference reflects
Body water content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; females 50% This difference reflects
The roles of hands and feet in temperature regulation in hot and cold environments
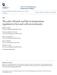 University of Wollongong Research Online Faculty of Health and Behavioural Sciences - Papers (Archive) Faculty of Science, Medicine and Health 2009 The roles of hands and feet in temperature regulation
University of Wollongong Research Online Faculty of Health and Behavioural Sciences - Papers (Archive) Faculty of Science, Medicine and Health 2009 The roles of hands and feet in temperature regulation
H 2 O, Electrolytes and Acid-Base Balance
 H 2 O, Electrolytes and Acid-Base Balance Body Fluids Intracellular Fluid Compartment All fluid inside the cells 40% of body weight Extracellular Fluid Compartment All fluid outside of cells 20% of body
H 2 O, Electrolytes and Acid-Base Balance Body Fluids Intracellular Fluid Compartment All fluid inside the cells 40% of body weight Extracellular Fluid Compartment All fluid outside of cells 20% of body
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
The effect of heat acclimation on body-fluid regulation
 University of Wollongong Research Online University of Wollongong Thesis Collection University of Wollongong Thesis Collections 1999 The effect of heat acclimation on body-fluid regulation Mark J. Patterson
University of Wollongong Research Online University of Wollongong Thesis Collection University of Wollongong Thesis Collections 1999 The effect of heat acclimation on body-fluid regulation Mark J. Patterson
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINE CONCENTRATION AND REGULATION OF ECF OSMOLARITY
 URINE CONCENTRATION AND REGULATION OF ECF OSMOLARITY Dilute and concentrated urine 1-Dilute urine : Nephron function continuous reabsorption. Solutes while failing to reabsorbe water in distal tubule and
URINE CONCENTRATION AND REGULATION OF ECF OSMOLARITY Dilute and concentrated urine 1-Dilute urine : Nephron function continuous reabsorption. Solutes while failing to reabsorbe water in distal tubule and
People maintain normal body temperature despite variations in both their metabolic activity and Ambient temperature Homeothermic animals (hot blooded)
 People maintain normal body temperature despite variations in both their metabolic activity and Ambient temperature Homeothermic animals (hot blooded) Animals with body temperature changes with environmental
People maintain normal body temperature despite variations in both their metabolic activity and Ambient temperature Homeothermic animals (hot blooded) Animals with body temperature changes with environmental
CASE 13. What neural and humoral pathways regulate arterial pressure? What are two effects of angiotensin II?
 CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
Metabolism ANS 215 Physiology and Anatomy of Domesticated Animals
 Metabolism ANS 215 Physiology and Anatomy of Domesticated Animals I. Body Temperature A. Chemical reaction of the body and therefore body functions are affected by body temperature 1. Each species has
Metabolism ANS 215 Physiology and Anatomy of Domesticated Animals I. Body Temperature A. Chemical reaction of the body and therefore body functions are affected by body temperature 1. Each species has
Ventilatory response to increasing body temperature: Characteristics and effect on central fatigue
 J Phys Fitness Sports Med, 4(2): 143-149 (2015) DOI: 10.7600/jpfsm.4.143 JPFSM: Review Article Ventilatory response to increasing body temperature: Characteristics and effect on central fatigue Keiji Hayashi
J Phys Fitness Sports Med, 4(2): 143-149 (2015) DOI: 10.7600/jpfsm.4.143 JPFSM: Review Article Ventilatory response to increasing body temperature: Characteristics and effect on central fatigue Keiji Hayashi
QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19
![QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19](/thumbs/80/80449526.jpg) 1 QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion, excretion
1 QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion, excretion
Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua
 Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua Assistant Professor Nephrology Unit, Department of Medicine College of Medicine,
Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua Assistant Professor Nephrology Unit, Department of Medicine College of Medicine,
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
CIE Biology A-level Topic 14: Homeostasis
 CIE Biology A-level Topic 14: Homeostasis Notes Communication is essential for the survival of organism as all living organisms must be able to detect and respond to changes in both their internal and
CIE Biology A-level Topic 14: Homeostasis Notes Communication is essential for the survival of organism as all living organisms must be able to detect and respond to changes in both their internal and
Chapter 44. Regulating the Internal Environment. AP Biology
 Chapter 44. Regulating the Internal Environment Homeostasis Living in the world organisms had a choice: regulate their internal environment maintain relatively constant internal conditions conform to the
Chapter 44. Regulating the Internal Environment Homeostasis Living in the world organisms had a choice: regulate their internal environment maintain relatively constant internal conditions conform to the
November 30, 2016 & URINE FORMATION
 & URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
& URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
THERMOREGULATION PHARMACOLOGY 6/21/2017 MATERI AJAR FISIOLOGI VETERINER II (TERMOREGULASI) 1
 THERMOREGULATION DIVISION OF PHYSIOLOGY DEPARTMENT OF ANATOMY, PHYSIOLOGY AND PHARMACOLOGY FACULTY OF VETERINARY MEDICINE IPB 2017 6/21/2017 MATERI AJAR FISIOLOGI VETERINER II (TERMOREGULASI) 1 Regulation
THERMOREGULATION DIVISION OF PHYSIOLOGY DEPARTMENT OF ANATOMY, PHYSIOLOGY AND PHARMACOLOGY FACULTY OF VETERINARY MEDICINE IPB 2017 6/21/2017 MATERI AJAR FISIOLOGI VETERINER II (TERMOREGULASI) 1 Regulation
Cooling Effect of Fluid Replacement During
 Cooling Effect of Fluid Replacement During Heavy Sweating Seiji YAMADA*, Chikanobu MATSUBARA*, Hiroshi NOSE*, Kenju MIKI*, Toshiyuki ITOH*, Yoshiteru SEO*, Kazufumi HIRAKAWA* and Taketoshi MORIMOTO* *
Cooling Effect of Fluid Replacement During Heavy Sweating Seiji YAMADA*, Chikanobu MATSUBARA*, Hiroshi NOSE*, Kenju MIKI*, Toshiyuki ITOH*, Yoshiteru SEO*, Kazufumi HIRAKAWA* and Taketoshi MORIMOTO* *
Chapter 1 Introduction to Physiology and Homeostasis
 Chapter 1 Introduction to Physiology and Homeostasis MULTIPLE CHOICE 1. Select the incorrect association. a. anatomy/function b. human body/multicellular. c. carbon dioxide/cell waste product. d. physiology/body
Chapter 1 Introduction to Physiology and Homeostasis MULTIPLE CHOICE 1. Select the incorrect association. a. anatomy/function b. human body/multicellular. c. carbon dioxide/cell waste product. d. physiology/body
Chapter 12. Ingestive Behavior
 Chapter 12 Ingestive Behavior Drinking a. fluid compartments b. osmometric thirst c. volumetric thirst Eating a. energy sources b. starting a meal c. stopping a meal d. eating disordersd Drinking a. fluid
Chapter 12 Ingestive Behavior Drinking a. fluid compartments b. osmometric thirst c. volumetric thirst Eating a. energy sources b. starting a meal c. stopping a meal d. eating disordersd Drinking a. fluid
iworx Physiology Lab Experiment Experiment HK-1 Human Kidney
 iworx Physiology Lab Experiment Experiment HK-1 Human Kidney Note: The lab presented here is intended for evaluation purposes only. iworx users should refer to the User Area on www.iworx.com for the most
iworx Physiology Lab Experiment Experiment HK-1 Human Kidney Note: The lab presented here is intended for evaluation purposes only. iworx users should refer to the User Area on www.iworx.com for the most
The ability of the kidneys to regulate extracellular fluid volume by altering sodium
 REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
