QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19
|
|
|
- Anne Charles
- 6 years ago
- Views:
Transcription
1 1 QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion, excretion Explain how the structure of the glomerulus promotes and limits filtration Describe the factors that influence GFR and the processes involved in its regulation Explain how creatinine clearance is determined and describe its clinical significance I. REABSROPTION OVERVIEW a. More then 99% of the fluid entering the tubules must be reabsorbed into the blood as filtrate moved through the nephrons b. Most reabsorption takes place in the proximal tubule, with smaller amounts in the distal segments i. Regulated reabsorption by hormones in the distal nephron allows kidneys to return ions and water to the plasma selectively as needed to maintain homeostasis c. Reabsorption may be a Active or Passive i. Water and ions in the proximal tubule have the same solute concentrations as the extracellular fluid, so to move out of tubule cells must use active transport to create concentration or electrochemical gradients ii. DIAGRAM: General Overview of Tubular Reabsorption Active transport of Na + from tubule men to ECF creates transepithelial electrical gradient in which lumen is more negative than the ECF Anions then follow the positively charged Na + out of the lumen Net movement of Na + and anions from lumen to ECF causes water to follow by osmosis Loss of volume from lumen increases the concentration of solutes (K +, Ca 2+, Urea) left behind in the filtrate o Unchanged amount of solute in a smaller volume produces an increase concentration Once luminal solute concentrations are higher than solute concentrations in the ECF, the solutes are free to diffuse out of the lumen if the epithelium of the tubule is permeable to them II. PASSIVE FOLLOWED BY ACTIVE; TRANSPORT OF SODIUM a. Active transport of Na + is the primary driving force for most renal reabsorption b. Filtrate entering proximal tubules has a similar ion composition with plasma c. Filtrate has higher Na + concentration then proximal tubule cells that separate tubule lumen and interstitial fluid of the peritubular capillaries
2 2 i. Na + can thus enter tubule cells passively by moving down its electrochemical gradient ii. In proximal tubule Na + -H + Antiporter players major role in Na + reabsorption d. One inside tubule cell Na + is actively transported out across basolateral membrane by Na + -K + -ATPase III. SECONDARY ACTIVE TRANSPORT: Symport with Sodium a. Sodium-linked secondary active transport i. Sodium binds with other organic metabolite to help transport across tubule into interstitial fluid ii. Responsible for glucose, amino acid, ion, and various organic metabolite reabsorption iii. DIAGRAM: Sodium-linked glucose reabsorption in proximal tubule Na + -dependent glucose reabsorption across proximal tubule epithelium Proximal tubule cell apical membrane contains (SGLT) Na + -glucose co-transporter that harnesses the energy of Na + for use by Glucose to diffuse Na + is then pumped from proximal tubule cell to interstitial fluid by Na + -K + -ATPase Glucose is then pumped from proximal tubule cell to interstitial fluid by GLUT transporters
3 3 IV. UREA: PASSIVE REABSORPTION a. Urea: nitrogenous waste product b. No active transporters in proximal tubule but will move across epithelium by diffusion if there is a urea concentration gradient [gradient usually created by active transport of Na + and other solutes] c. Process: i. When Na + and other solutes are reabsorbed from the proximal tubule the transfer of osmotically active particles makes the ECF more concentrated than the filtrate remaining in the lumen ii. As a response to the osmotic gradient, water moves by osmosis from tubule lumen to ECF iii. When H 2 O leaves lumen for ECF the filtrate concentration of urea increases because the same amount of urea is contained in a smaller volume iv. Once concentration gradient for urea exists, urea diffuses out of lumen in to ECF V. SATURATION a. Saturation of Renal Transport Plays an Important Role in Kidney Function i. Saturation refers to maximum rate of transport that occurs when all available carriers are occupied by a substrate ii. The transport rate at saturation is the transport maximum (T M ) [mg/min] 1. Transport maximum is the maximum rate at which 100% of a substance can be reabsorbed iii. Ex: Glucose Reabsorption 1. Normal plasma glucose concentrations, all glucose that enters the nephron is reabsorbed before it reaches end of proximal tubule 2. If person has diabetes mellitus, or excessive blood glucose concentrations, glucose is filtered faster than the carriers of the peritubular capillaries can reabsorb it a. Result: Glucose escapes reabsorption and is excreted in the urine b. The plasma concentration at which glucose first appears in the urine is called the renal threshold [mg/min] for glucose Calculations a) GFR x plasma concentration = filtration rate b) GFR x renal threshold = T M Transport rate of a substance is proportional to the plasma concentration of the substance up to the point at which transporters become saturated Once saturation occurs transport rate reaches a maximum (T M ) The plasma concentration of substrate at which the (T M ) occurs is called the renal threshold Excretion = Filtration (increasing) Reabsorption (constant) VI. PERITUBULAR CAPILLARY PRESSURES FAVORS REABSORPTION a. Drive force for reabsorption from the interstitial fluid into the capillaries is the low hydrostatic pressure that exists along the entire length of the peritubular capillaries i. Peritubular capillaries have hydrostatic pressure [blood pressure; opposes movement of fluid into peritubular capillaries] of 10 mm Hg (in contrast to glomerular capillary hydrostatic pressure which is 55 mm Hg) ii. Colloid osmotic pressure (favors movement of fluid into peritubular capillaries) is 30 mm Hg 1. RESULT: Pressure gradient is 20 mm Hg in favor of absorption of fluid into capillaries a. Fluid that is reabsorbed then passes from capillaries to venous circulation and returns to the heart
4 4 VII. FLUID/ELECTROLYTE HOMEOSTATIC BALANCE a. In the coarse of a day we consume roughly 2 liters of food and 6-15 grams of NaCl i. Also bring in various electrolytes including K +, H +, Ca 2+, HCO - 3 and phosphate (HPO 2-4) b. THIRST: critical because drinking is only normal way to replace lost water c. SALT APPETITE: critical behavior that leads people to seek and ingest salt (sodium chloride NaCl) d. Importance of i. H 2 O and Na + : Associated with ECF volume and osmolarity ii. K + : Inbalances can cause serious problems with cardiac and muscle function iii. Ca 2+ : Variety of body processes, from Exocytosis and muscle contraction to bone formation and blood clotting iv. H + and HCO - 3: Ions whose balance determines body ph e. ECF Osmolarity Affects Cell Volume i. If osmolarity of ECF changes water moves into or out of cells and changes intercellular volume ii. If ECF osmolarity decreases (result of excess water intake) water moves into cells and they swell iii. If ECF osmolarity increases (result of salt intake) water moves into cells and they shrink 1. Shrinking or swelling (changes in cell volume) can impair cell function 2. Ex: Swelling cells ion channels in membrane open disrupts membrane potential and cell signaling f. Fluid and Electrolyte Balance Requires Integration of Multiple Systems i. Fluid and electrolyte balances is integrative because it involves cardiovascular and respiratory systems, and renal and behavioral responses 1. Rapid Responses performed by: a. Lungs b. Cardiovascular system 2. Slow Responses performed by: a. Kidneys Under Neural Control Under Endocrine and neuroendocrine control CAPATION: The Body s Integrated Responses to Changes in Blood Volume and Blood Pressure
5 5 WATER BALANCE OSMOSIS EXPLAINED a. Water Distribution a. Plasma: 8% b. Interstitial Tissue: 25% [tissue fluid/external fluid/3 rd space] c. Intracellular Fluid: 67% b. Tonicity and Cell Volume a. Effect of cell in isotonic environment: No Change b. Effect of cell in hypertonic environment: Cell shrinks/dehydrates c. Effect of cell in hypotonic environment: Cell swells/rehydrates c. IV Fluid Therapy a. Blood volume/pressure therapy i. Isotonic solution b. Rehydration therapy i. Hypotonic solution c. Tonicity d. Salt content determines water movement d. Volume-Osmolarity Challenges a. Sensors i. Volume receptors = Atria of heart ii. Baroreceptors = Carotid arteries and aortic arch iii. Osmoreceptors = Hypothalamus b. Effectors i. Glomerulus = GFR ii. Hypothalamus = Thirst iii. Heart = C.O. (cardiac output) iv. Vasculature = P.R. (peripheral resistance) v. DCT = Na Reabsorption vi. Collecting Duct = Water Reabsorption c. Rules Plasma (effects) 3 rd space (effects) intracellular space Osmosis: Water movement from low gradient to high gradient Fig on back of page/overview of system physiology for dehydration compensation i. Body responds to changes in osmolarity before it responds to changes in blood volume/pressure ii. If two efferent pathways have opposite effects on the same effector, assume that negative feedback is dominant; that is, the one that opposes the initial stimulus
6 6 Osmolarity excess electrolyte solutes such as Na, K, Cl, phosphates Osmolarity decrease of electrolyte solutes Loop Diuretics 1) Furosemide (Lasix) 2) Bumetanide (Bumex) a. Both work on loop of Henle b. Block Na-K-Cl (sodium potassium chloride pumps) c. Block reabsorption of sodium (which thus blocks H 2O reabsorption to peritubular capillaries/interstitial tissue and space) d. Used to lower fluid volumes (increase excretion) e. Given to patients with CHF, edema, high blood volume, heart failure VIII. URINE CONCENTRATION IS DETERMINED IN THE LOOP OF HENLE AND COLLETING DUCTS a. Osmolarity (urine concentration) is a measure of how much water is excreted by the kidneys b. (excess) water kidneys excrete copious amounts of dilute urine with osmolarity as low as 50 mosm i. Removal of excess water in urine is known as dieresis c. (low) water kidneys conserve water and urine becomes highly concentrated, as high as 1200 mosm [1200 mosm is four times as concentrated as blood which is 300 mosm] d. Kidneys alter urine concentration by varying the amount of 1) water and 2) Na + reabsorbed in distal nephron ((specifically the DCT)) CAPTION: REFERENCE i. Produce Dilute Urine: Non-permeable water membrane (no H 2 O reabsorption) that allows solute to pass ii. Produce Concentrated Urine: Nephron reabsorbs H 2 O while leaving solute in tubule lumen e. Osmosis (diffusion of water from to areas) will not take place unless concentration gradient exists i. Renal medulla maintains high osmotic concentration in interstitial fluid ii. High Medullary interstitial osmolarity allows urine to be concentrated f. Fluid Movement through the Loop of Henle i. Reabsorption in the proximal tubule is isomotic ii. Filtrate entering loop of Henle (descending tubule) has osmolarity of 300 mosm (isomotic to blood) iii. Filtrate leaving loop of Henle (ascending tubule) has osmolarity of 100 mosm (hyposmotic to blood) 1. Hyposmotic fluid created by thick portion of ascending limb where Na 2+, K +, and Cl - are transported out of the tubule lumen 2. These cells apical surface is impermeable to water thus when cells transport solute out of lumen water cannot follow, creating a hyposmotic solution iv. Hyposmotic fluid leaving the loop of Henle then passing through the distal tubule and into the collecting duct, its final concentration is determined by the epithelia cells permeability to water in the distal nephron 1. Cells not water permeable water remains in tubule and filtrate remains dilute 2. Cells water permeable water diffuses out of tubule and into the interstitial fluid making filtrate becomes concentrated v. Kidney s homeostatic mechanisms can do nothing to restore lost fluid volume; one ingestion or infusion of water (through IV) can replace water that has been lost Loop of Henle Volume Concentration Descending Loop Decreases Increases Ascending Loop Unchanged Decreases
7 7 CAPTION: OSMOLARITY CHANGES AS FILTRATE FLOWS THROUGH THE NEPHRON g. The Loop of Henle Is a Countercurrent Multiplier i. The Renal Countercurrent Multiplier 1. Transfers solutes instead of heat as in a typical countercurrent exchange system 2. Filtrate enters descending limb which is permeable to water and impermeable to ions a. Decreasing Volume b. Increasing Concentration i. Water moving by osmosis into more highly concentrated (bigger gradient) of interstitial fluid of vasa recta 3. Ascending Loop of Henle a. Impermeable to water b. Permeable to ions (Na, K, and Cl) i. Loss of solute (ions) causes filtrate osmolarity to decrease c. 25% of Na and K reabsorption takes place in ascending limb d. NKCC symporter (Na/K/Cl/Cl) uses energy stored in Na + concentration gradient to transport Na +, K +, and 2Cl - from lumen of Henle into interstitial fluid i. NKCC symporter inhibited by loop diuretic drugs (Lasix)
8 8 h. The Vasa Recta Removes Water i. Water or solutes that leave the tubule move into the vasa recta if an osmotic or concentration gradient exists between medullary interstitium and blood in vasa recta ii. Blood flowing through the vasa recta removes the water reabsorbed from the loop of Henle i. Urea Increases the Osmolarity of the Medullary Interstitium IX. HORMONES OF THE FLUID/ELECTROLYTE BALANCE Classification Excrete/Retain Water/Salt Blood Effects Hormones Involved Diuretic Excrete Water volume osmolarity Anti-Diuretic Retain Water Conserve volume Maintain osmolarity Natriuetic Excrete Salt volume osmolarity Anti-Natriuetic Retain Salt Conserve volume Maintain osmolarity Atrial Natriuretic Peptide (ANP) Vasopressin (ADH) Angiotensin II Atrial Natriuretic Peptide Angiotensin II Aldosterone a. Diuretics i. Promote Excretion of or Water ii. Cause decrease in blood volume iii. Cause increase in osmolarity iv. Hormone: 1. Atrial Natriuretic Peptide a. Atrial Natriuretic Peptide (ANP; also known as atriopeptin) b. Peptide hormone produced in specialized myocardial cells in the atria of the heart i. Related hormone [BNP] Brain Natriuretic Peptide is synthesized by ventricular myocardial cells and certain brain neurons c. Released by the heart when myocardial cells stretch more than normal [as would occur with increased blood volume] d. Enhance Na + and H 2 O excretion e. Inhibit the release of renin, aldosterone, and vasopressin f. Effects of ANP Inhibits (-) Aldosterone Decreases Na 2+ reabsorption Inhibits (-) Angiotensin Prevents thirst and vasoconstriction Inhibits (-) Vasopressin (ADH) Decreases water reabsorption Promotes (+) GFR Increases urine output Caption: Actions of Natriuretic Peptides
9 9 b. Anti-Diuretics i. Promote Retention of Water ii. Conserve volume iii. Main osmolarity iv. Hormones: 1. Vasopressin (ADH) a. When acting on target cells water pores are present in the apical membrane that allow water to move out of the lumen (by osmosis) and into interstitial fluid of the renal medulla b. Posterior Pituitary hormone c. Adds water pores (aquaporins) in the apical membrane of the collecting ducts i. Aquaporins activated by arrival of ADH from posterior pituitary gland and bind to designated cells, activating G-protein/cAMP second messenger system ii. Phosphorylation of intracellular proteins causes aquaporin-2 (AQP2) vesicle to move to apical membrane and fuse with it, making the wall permeable to water iii. This process is imitated by Exocytosis and ended by endocytosis is known as membrane recycling
10 10 STIMULI ABBREVIATED Blood osmolarity Blood volume Blood pressure d. Stimuli for Vasopressin secretion i. Plasma Osmolarity 1. Monitored by Osmoreceptors, which are stretch sensitive cells that active sensory neurons when osmolarity increase above threshold 2. Osmoreceptors found in hypothalamus 3. When plasma osmolarity rises above 280 mosm Osmoreceptors fire [releasing vasopressin] 4. When plasma osmolarity is below 280 mosm Osmoreceptors do not fire [no release of vasopressin] ii. Blood volume 1. Stretch sensitive receptors found in the Atria 2. When blood volume is low the receptors signal hypothalamus to secrete vasopressin iii. Blood pressure 1. Monitored by carotid and aortic baroreceptors 2. When blood pressure is low the receptors signal hypothalamus to secrete vasopressin 2. Angiotensin II a. (ANG II) signals aldosterone release from the adrenal cortex b. Tropic hormone; stimulates aldosterone secretion in most situations c. Most potent vasoconstrictor; constricts systemic arteries BP without changing blood volume
11 11 d. Stimulates i. Thirst ii. Aldosterone iii. ADH e. Is component of the RAAS [Renin-Angiotensin-Aldosterone System] i. A multistep pathway for maintain blood pressure 1. RAAS stimulated by BP and Blood Volume 2. Juxtaglomerular Granular cells in afferent arterioles of nephron secrete enzyme called renin 3. Renin activates angiotensinogen into angiotensin I 4. Angiotensin I encounters enzyme angiotensin converting enzyme (ACE) and converts ANG I ANG II CAPTION: This map outline the control of aldosterone secretion as well as the blood pressure raising effects of ANG II f. Inhibited by pharmacological drug called ACE Inhibitors i. Antihypertensive drug ii. Drug blocks ACE-mediated conversion of ANG I ANG II; thereby helping to relax blood vessels and lower blood pressure iii. Less ANG II less aldosterone decrease in Na + reabsorption decrease ECF volume
12 12 c. Natriuetic i. Cause Na + (sodium) loss/excretion ii. Cause H 2 O loss/excretion iii. Used to lower blood pressure and blood volume iv. Hormone: 1. Atrial Natriuretic Peptide (ANP; also known as atriopeptin) 2. Peptide hormone produced in specialized myocardial cells in the atria of the heart a. Related hormone [BNP] Brain Natriuretic Peptide is synthesized by ventricular myocardial cells and certain brain neurons 3. Released by the heart when myocardial cells stretch more than normal [as would occur with increased blood volume] 4. Enhance Na + and H 2 O excretion 5. Inhibit the release of renin, aldosterone, and vasopressin 6. Effects of ANP Inhibits (-) Aldosterone Decreases Na 2+ reabsorption Inhibits (-) Angiotensin Prevents thirst and vasoconstriction Inhibits (-) Vasopressin (ADH) Decreases water reabsorption Promotes (+) GFR Increases urine output d. Anti-Natriuetic i. Promotes Retention of salt ii. Conserves volume iii. Maintains osmolarity iv. Hormones: 1. Angiotensin II 2. Aldosterone a. Steroid hormone synthesized in the adrenal cortex b. Increases activity of Na + -K + -ATPase c. Causes Na + reabsorption and K + secretion d. Maintains blood volume e. Stimulated by i. Low osmolarity ii. Low blood volume
13 13 CAPTION: Aldosterone action in principal cells iii. Hyponatremia ( Na 2+ ) iv. Hyperkalemia ( K) v. Angiotensin II f. Inhibited by i. High osmolarity LOW BLOOD VOLUME/PRESSURE AND WATER CONSERVATION a. Low Blood volume activates RAAS b. Low blood volume stimulates vasopressin (ADH) secretion HIGH BLOOD VOLUME/PRESSURE AND WATER EXCRETION a. Atrial baroreceptors respond to high pressure by releasing ANP b. Pharmacological intervention: ACE inhibitors X. THE DCT REGULATES THE FINAL SODIUM CONTENT OF URINE a. Effects/mechanism of Na + reabsorption i. Effect on Water 1. Drives water reabsorption ii. Effect on Potassium 1. Drives potassium reabsorption and secretion iii. Is enhanced by aldosterone NOTE: Na reabsorption generally linked to K secretion [Na-K exchange] NOTE: Na-K exchange can be blocked by aldosterone antagonist Amiloride 1. Aldosterone = Function in Na reabsorption/k secretion [released by adrenal cortex]
14 14 b. Diuretics K Depleting (strong) Loop Diuretics [Na-K-2Cl in ascending limb] Thiazide Diuretics [TSCL in DCT] Diuretics K Sparing (weak) Amiloride [ENaC in DCT] ARB [Aldosterone Receptor Blocker] ACE inhibitor Thizaides Act on ascending loop of Henle (DCT) Block Na reabsorption blocking water reabsorption increasing urine dilution Block K reabsorption excrete excessive amounts of potassium Giving to people with C.H.F, high BP, edema XI. Acid-Base Balance (ph Homeostasis) a. Normal ph of body is 7.40 (slightly alkaline) b. Normal ph range of plasma is i. Acidosis 1. ph is to low 2. Neurons become less excitable and CNS depression results ii. Alkalosis 1. ph is to high 2. Neurons become hyperexcitable firing action potentials at the slightest signal c. Disturbances of acid-base balance are associated with disturbances in K + balance d. Potassium (K + ) and (H + ) exchangers e. Compensation of ph leads to K + imbalances f. Loop of Henle i. Proximal Tubule 1. Secretes Hydrogen 2. - Reabsorbs HCO 3 ii. Distal Nephron 1. Controls Acid excretion 2. Intercalated cells (I cells) responsible for acid-base regulation
15 15
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX
 One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BIOLOGY - CLUTCH CH.44 - OSMOREGULATION AND EXCRETION.
 !! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
!! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
Fluid and electrolyte balance, imbalance
 Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
Urine Formation. Urinary Physiology Urinary Section pages Urine Formation. Glomerular Filtration 4/24/2016
 Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance
 Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Functions of Proximal Convoluted Tubules
 1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
Chapter 15 Fluid and Acid-Base Balance
 Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
I. Metabolic Wastes Metabolic Waste:
 I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
Other Factors Affecting GFR. Chapter 25. After Filtration. Reabsorption and Secretion. 5 Functions of the PCT
 Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D.
 Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Hill et al. 2004, Fig. 27.6
 Lecture 25, 15 November 2005 Osmoregulation (Chapters 25-28) Vertebrate Physiology ECOL 437 (aka MCB 437, VetSci 437) University of Arizona Fall 2005 1. Osmoregulation 2. Kidney Function Text: Chapters
Lecture 25, 15 November 2005 Osmoregulation (Chapters 25-28) Vertebrate Physiology ECOL 437 (aka MCB 437, VetSci 437) University of Arizona Fall 2005 1. Osmoregulation 2. Kidney Function Text: Chapters
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Na + Transport 1 and 2 Linda Costanzo, Ph.D.
 Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
November 30, 2016 & URINE FORMATION
 & URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
& URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are
 Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
osmoregulation mechanisms in gills, salt glands, and kidneys
 Ionic & Osmotic Homeostasis osmoregulation mechanisms in gills, salt glands, and kidneys extracellular intracellular 22 23 Salt Secretion: recycle Figure in Box 26.2 Hill et al. 2004 active Down electrochemical
Ionic & Osmotic Homeostasis osmoregulation mechanisms in gills, salt glands, and kidneys extracellular intracellular 22 23 Salt Secretion: recycle Figure in Box 26.2 Hill et al. 2004 active Down electrochemical
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Ch 17 Physiology of the Kidneys
 Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Counter-Current System Regulation of Renal Functions
 Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
1.&Glomerular/Pressure&Filtration&
 Urine&Formation& Overall&Process&! Urine gets rid of wastes (NH 3, urea, uric acid, creatinine) and other substances (vitamins, penicillin, histamines) found in excess in the blood!! blood is filtered
Urine&Formation& Overall&Process&! Urine gets rid of wastes (NH 3, urea, uric acid, creatinine) and other substances (vitamins, penicillin, histamines) found in excess in the blood!! blood is filtered
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Potassium secretion. E k = -61 log ([k] inside / [k] outside).
![Potassium secretion. E k = -61 log ([k] inside / [k] outside). Potassium secretion. E k = -61 log ([k] inside / [k] outside).](/thumbs/80/80478709.jpg) 1 Potassium secretion In this sheet, we will continue talking about ultrafiltration in kidney but with different substance which is K+. Here are some informations that you should know about potassium;
1 Potassium secretion In this sheet, we will continue talking about ultrafiltration in kidney but with different substance which is K+. Here are some informations that you should know about potassium;
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Renal Physiology. April, J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine.
 Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Fluids and electrolytes
 Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Physiology (6) 2/4/2018. Rahmeh Alsukkar
 Physiology (6) 2/4/2018 Rahmeh Alsukkar **unfortunately the sheet does not involve the slides. ** the doctor repeat a lot of things from the previous lecture so this sheet will begin from slide 139 to
Physiology (6) 2/4/2018 Rahmeh Alsukkar **unfortunately the sheet does not involve the slides. ** the doctor repeat a lot of things from the previous lecture so this sheet will begin from slide 139 to
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
8. URINE CONCENTRATION
 8. URINE CONCENTRATION The final concentration of the urine is very dependent on the amount of liquid ingested, the losses through respiration, faeces and skin, including sweating. When the intake far
8. URINE CONCENTRATION The final concentration of the urine is very dependent on the amount of liquid ingested, the losses through respiration, faeces and skin, including sweating. When the intake far
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018
 RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018 Intercalated cells Intercalated cells secrete either H + (Typ A) or HCO 3- (Typ B). In intercalated cells Typ A can be observed
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018 Intercalated cells Intercalated cells secrete either H + (Typ A) or HCO 3- (Typ B). In intercalated cells Typ A can be observed
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
CHAPTER 27 LECTURE OUTLINE
 CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
From Blood Filtrate to Urine: A Closer Look
 Blood Vessels Associated with the Nephrons Each nephron supplied with blood by an afferent arteriole branch of renal artery divides into glomerular capillaries capillaries converge as they leave glomerulus
Blood Vessels Associated with the Nephrons Each nephron supplied with blood by an afferent arteriole branch of renal artery divides into glomerular capillaries capillaries converge as they leave glomerulus
Fal Fal P h y s i o l o g y 6 1 1, S a n F r a n c i s c o S t a t e U n i v e r s i t y
 Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
11/05/1431. Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate
 Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
Diuretics having the quality of exciting excessive excretion of urine. OED. Inhibitors of Sodium Reabsorption Saluretics not Aquaretics
 Diuretics having the quality of exciting excessive excretion of urine. OED Inhibitors of Sodium Reabsorption Saluretics not Aquaretics 1 Sodium Absorption Na Entry into the Cell down an electrochemical
Diuretics having the quality of exciting excessive excretion of urine. OED Inhibitors of Sodium Reabsorption Saluretics not Aquaretics 1 Sodium Absorption Na Entry into the Cell down an electrochemical
BIOL 221 Chapter 26 Fluids & Electrolytes. 35 slides
 BIOL 221 Chapter 26 Fluids & Electrolytes 35 slides 1 Body Water Content Total Body Water is the percentage of a person s weight that is water. TBW can easily vary due to: gender males have higher TBW
BIOL 221 Chapter 26 Fluids & Electrolytes 35 slides 1 Body Water Content Total Body Water is the percentage of a person s weight that is water. TBW can easily vary due to: gender males have higher TBW
Body Water Content Total Body Water is the percentage of a person s weight that is water. TBW can easily vary due to: gender
 BIOL 221 Chapter 26 Fluids & Electrolytes 35 slides 1 Body Water Content Total Body Water is the percentage of a person s weight that is water. TBW can easily vary due to: gender males have higher TBW
BIOL 221 Chapter 26 Fluids & Electrolytes 35 slides 1 Body Water Content Total Body Water is the percentage of a person s weight that is water. TBW can easily vary due to: gender males have higher TBW
Renal Physiology - Lectures
 Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE
 Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Normal Renal Function
 Normal Renal Function Functions of the Kidney: balances solute and water transport excretes metabolic waste products conserves nutrient regulates acid-base balance secretes hormones that help regulate
Normal Renal Function Functions of the Kidney: balances solute and water transport excretes metabolic waste products conserves nutrient regulates acid-base balance secretes hormones that help regulate
Renal Functions: Renal Functions: Renal Function: Produce Urine
 Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Chapter 17. Lecture Outline. See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes.
 Chapter 17 Lecture Outline See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Chapter 17 Lecture Outline See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Identify and describe. mechanism involved in Glucose reabsorption
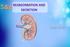 Define tubular reabsorption, tubular secretion, transcellular and paracellular transport. Identify and describe mechanism involved in Glucose reabsorption Describe tubular secretion with PAH transport
Define tubular reabsorption, tubular secretion, transcellular and paracellular transport. Identify and describe mechanism involved in Glucose reabsorption Describe tubular secretion with PAH transport
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Body Fluid Dynamics. I. Body fluids - Must remain constant - Intake = output. Insensible H 2 0 loss Capillary Membrane
 I. Body fluids - Must remain constant - Intake = output Body Fluid Dynamics Metabolic H 2 0 Preformed Free H 2 0 in Urine Feces Sweat H 2 0 Food - Body fluid distribution: Insensible H 2 0 loss Capillary
I. Body fluids - Must remain constant - Intake = output Body Fluid Dynamics Metabolic H 2 0 Preformed Free H 2 0 in Urine Feces Sweat H 2 0 Food - Body fluid distribution: Insensible H 2 0 loss Capillary
Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi
 Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi At the end of this lecture student should be able to describe: The loop of Henle is referred to as countercurrent
Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi At the end of this lecture student should be able to describe: The loop of Henle is referred to as countercurrent
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
organs of the urinary system
 organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 18 Urinary System 3 Tubular Reabsorption and Secretion Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Principles of
BIOH122 Human Biological Science 2 Session 18 Urinary System 3 Tubular Reabsorption and Secretion Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Principles of
Lecture 16: The Nephron
 Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
Renal Physiology II Tubular functions
 Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
Renal System Physiology
 M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
Functional morphology of kidneys Clearance
 Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Chapter 26 The Urinary System
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
mid ihsan (Physiology ) GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B **
 (Physiology ) mid ihsan GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B ** Colloid pressure in the efferent arteriole is: A- More than that leaving
(Physiology ) mid ihsan GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B ** Colloid pressure in the efferent arteriole is: A- More than that leaving
Kidney Physiology. Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed
 Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Water, Electrolytes, and Acid-Base Balance
 Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
Kidney Structure. Renal Lobe = renal pyramid & overlying cortex. Renal Lobule = medullary ray & surrounding cortical labryinth.
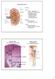 Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Regulating the Internal Environment. AP Biology
 Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform to external
Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform to external
