Early changes in gene expression that influence the course of primary glomerular disease
|
|
|
- Aubrey Blake
- 5 years ago
- Views:
Transcription
1 & 2007 International Society of Nephrology original article Early changes in gene expression that influence the course of primary glomerular disease LC Clement 1,4, G Liu 1,4, I Perez-Torres 3, YS Kanwar 2, C Avila-Casado 3 and SS Chugh 1 1 Department of Medicine, Northwestern University, Feinberg School of Medicine, Chicago, Illinois, USA; 2 Department of Pathology, Northwestern University, Feinberg School of Medicine, Chicago, Illinois, USA and 3 Department of Pathology, Instituto Nacional de Cardiologia, Mexico City, Mexico Serial changes in glomerular capillary loop gene expression were used to uncover mechanisms contributing to primary glomerular disease in rat models of passive Heymann nephritis and puromycin nephrosis. Before the onset of proteinuria, podocyte protein-tyrosine phosphatase (GLEPP1) expression was transiently decreased in the nephrosis model, whereas the immune costimulatory molecule B7.1 was stimulated in both models. To relate these changes to the development of proteinuria, the time of onset and intensity of proteinuria were altered. When the models were induced simultaneously, proteinuria and anasarca occurred earlier with the collapse of glomerular capillary loops. Upregulation of B7.1 with the downregulation of GLEPP1, Wilms tumor gene (WT1), megalin, and vascular endothelial growth factor started early and persisted through the course of disease. In the puromycin and the combined models, changes in GLEPP1 expression were corticosteroid-sensitive, whereas B7.1, WT1, vascular endothelial growth factor, and most slit diaphragm genes involved later in the combined model, except podocin, were corticosteroid-resistant. There was a very early increase in the nuclear expression of podocyte transcription factors ZHX2 and ZHX1 that may be linked to the changes in gene expression in the combined proteinuric model. Our studies suggest that an early and persistent change in mostly steroid-resistant glomerular gene expression is the hallmark of severe and progressive glomerular disease. Kidney International (2007) 72, ; doi: /sj.ki ; published online 25 April 2007 KEYWORDS: podocyte; minimal change disease; membranous nephropathy; ZHX proteins; WT1; glomerular collapse Correspondence: SS Chugh, Division of Nephrology, Tarry Northwestern University, Feinberg School of Medicine, 320 East Superior, Chicago, Illinois 60611, USA. s-chugh@northwestern.edu 4 These authors contributed equally to this work Received 21 November 2006; revised 12 March 2007; accepted 20 March 2007; published online 25 April 2007 Proteinuria and glomerular disease results from a myriad of structural and as yet inadequately defined functional changes in components of the glomerular capillary loop. In different models, these changes can be variously initiated by inflammatory cells, complement, cytokines, circulating factors, or antibody toxicity. Regardless of the initiating event, changes in one or more of several putative pathways initiate a sequence of events within the intrinsic components of the glomerular capillary loop that eventually result in the development of proteinuria and glomerular disease. There is a relative paucity of data on gene expression in experimental primary glomerular disease. 1 Most experimental studies, and all human kidney biopsy studies, have looked at time points coincident with, or after the onset of proteinuria. To understand the development of glomerular disease, it is important to study early changes, especially those just before the onset of proteinuria. Passive Heymann nephritis (PHN) and puromycin aminonucleoside nephrosis (PAN) are models of podocyte disease with a defined time point for the onset of proteinuria and a pre-proteinuric phase. Both models are suitable for the study of changes in gene expression before, and immediately after the onset of proteinuria. In this study, we induced both models in young rats, because they have very little baseline proteinuria, and onset of overt proteinuria is predictably on day 5 (occasionally on day 4). 1 Studies in these models indicate that transient changes in podocyte proteintyrosine phosphatase (GLEPP1) and B7.1 occur early, and that changes in GLEPP1 expression are partially corticosteroidsensitive. The potential importance of these gene changes in the development of proteinuria was assessed by changing the onset and intensity of proteinuria. Combining the two models results in the development of glomerular capillary loop collapse, which is associated with earlier onset of proteinuria, persistent changes in B7.1 and GLEPP1 expression, increased early podocyte nuclear expression of ZHX1 and ZHX2, additional downregulation of several mostly corticosteroidresistant genes, and early death from severe anasarca. RESULTS Induction of animal models of proteinuria Proteinuria data of a representative experiment for PAN, PHN, and PAN þ PHN combination is shown in Figure 1. In Kidney International (2007) 72,
2 young rats, PAN and PHN cause proteinuria on day 5, whereas in the PAN þ PHN combination, proteinuria develops on day 2. Lack of proteinuria on day 3 of the individual models and day 1.5 of the combination model was confirmed both by protein assay and confocal imaging of proximal tubules for rat albumin. Because there is a shift to the left in terms of the onset of proteinuria (i.e., day 2, compared to days 4 5 in the original models), day 1.5 is taken as a preproteinuric time point, and day 3 as the immediate postproteinuric time point. Histological characterization of the animal models Histological assessment of each group confirmed the induction of disease (Figures 2 and 3). PAN and PHN were histologically similar to previous descriptions extensively published in the literature. Evidence of significant foot process effacement was present in the proteinuric PHN, PAN, and combination rats. This PAN þ PHN combination model has features of both PAN and PHN, for example extensive foot process effacement as typical of PAN, and subepithelial deposits as seen in PHN. In the day 6 combination rats, about a third of the glomeruli had collapsed capillary loops (see detailed analysis later). Day 1.5 and 3 combination rats had no evidence of capillary loop collapse. Most PAN þ PHN combination rats develop progressive anasarca early, and die by days 7 8. The expression of several podocyte markers was studied in various study groups by immunostaining. Only results for selected proteins are presented (Figure 4, Figure S6). As is also noted in human collapsing glomerulopathy, 2 Wilms tumor gene (WT1), a podocyte-specific transcriptional factor in the adult kidney, was significantly decreased in glomeruli with collapsed loops, and only mildly decreased in glomeruli with normal appearing capillary loops in the combination day 6 rats. WT1 staining was unchanged in PAN and marginally decreased in PHN at later time points. Expression of GLEPP1 was moderately decreased even in glomeruli with noncollapsed loops in the combination day 6 group and severely depleted in those with collapsed loops. In a b Proteinuria (mg/18 h) Proteinuria (mg/18 h) Control Day 3 0 Day 6 Day 10 Control Day 3 Day 6 Day 10 c Proteinuria (mg/18 h) PAN PHN PAN+PHN Control sheep serum/pbs 50 0 Day 1 Day 2 Day 3 Day 5 Day 6 Day 10 d Proteinuria (mg/18 h) PAN PAN-S Control Day 1.5 Day 3 Day 5 Day 6 X XX Day 10 e Proteinuria (mg/18 h) PAN+PHN Control Control+steroids Day 1.5 Day 3 Day 6 Figure 1 Induction of proteinuria in the PAN, PHN, and PAN þ PHN combination models. (a) PAN and (b) PHN rats develop proteinuria on day 5 (occasionally on day 4), whereas (c) PAN þ PHN combination rats become proteinuric on day 2. Po0.001 for all proteinuric time points vs controls in a c. (d, e) Effect of corticosteroids therapy on proteinuria in (d) PAN and (e) PAN þ PHN combination rats is shown. Rats were treated on alternate days with corticosteroids (see text), resulting in mild decrease in proteinuria. (n ¼ 4 rats/group in all experiments). x indicates Po0.001; xx indicates Po0.01. X 338 Kidney International (2007) 72,
3 a c b d addition, several tubules contained evidence of laminin and neph1 staining in the luminal protein casts in the day 6 combination group (staining with control IgG-negative), further supporting shedding of components from the collapsed glomerular capillary loops. Some proliferating cell nuclear antigen (PCNA, marker of cell proliferation)-positive cells are noted to be tethered to the glomerular tuft, whereas others are noted in the urinary space. Immunostains with preimmune sera or normal IgG of the same species as the primary antibody were conducted in each experiment and were uniformly negative. Figure 2 Morphological changes in glomeruli in the PAN þ PHN combination study on day 6. (a) A control group rat with normal glomerular morphology on periodic acid-schiff staining is shown. (b) A periodic acid-schiff-stained glomerulus from the study group with segmental collapse of the capillary loops and some nucleated cells that are either adherent to the glomerular tuft (arrow) or free in the urinary space (arrowhead) are shown. (c) A confocal image showing global collapse of glomerular capillary loops stained with anti-laminin antibody (red). Nuclei are stained with Sytox green. (d) PCNA staining (brown) with hematoxylin counterstain in the PAN þ PHN group is shown. The glomerulus has segmental collapse and PCNApositive cells adherent to the glomerular tuft (arrow) and free in the urinary space (arrowhead). The asterisk indicates a dividing podocyte nucleus, or two very closely placed PCNA-positive cells. Some PCNApositive cells are also noted in the parietal capsule and the interstitium. Control immunostains were negative and are not shown. Original magnification (for additional images, see Figure S7). Changes in gene expression in PAN, PHN, and PAN þ PHN combination The major reason for inducing the combination model was to change the onset of proteinuria and study if genes altered before the onset of proteinuria in the individual models also moved with the onset of proteinuria. A representative summary of significant changes in gene expression is listed in Table 1. Because all the experiments were repeated several times with multiple measurements for each gene in each study, the results from a representative study of each kind are presented. Slit diaphragm genes No significant changes in the expression of slit diaphragm (SD) genes were noted before the onset of proteinuria in either PAN or PHN, indicating that they cannot be primarily implicated in the pathogenesis of proteinuria in these models. Decrease in nephrin and FAT1 expression developed on days 6 and 10 of PHN, respectively, whereas marginal decrease in nephrin expression was noted on day 6 in some PAN studies. SD-related genes are, however, the major new a b c Day 3 Day 3 Day 1.5 d e f Day 6 PAN Day 6 PHN Day 3 PAN+PHN Figure 3 Electron microscopy of PAN, PHN, and PAN þ PHN combination injected rats. Podocyte foot processes were preserved on day 3 (a) PAN and (b) PHN, and day 1.5 of (c) the PAN þ PHN combination. Effacement of foot processes was noted on day 6 (d) PAN and (e) PHN, and on day 3 (f) PAN þ PHN combination. Subepithelial electron-dense deposits (see arrows), a classic feature of PHN, were also noted in the PAN þ PHN combination. Original magnification Kidney International (2007) 72,
4 a b c Control group Red stain : albumin PAN + PHN group Red stain : albumin PAN + PHN group Red stain : neph1 d e f g h i j k l Red stain: laminin Blue stain: WT1 Red stain: GLEPP1 Control PAN + PHN group Capillary loops preserved PAN + PHN group Capillary loops collapsed Figure 4 Confocal assessment of changes in glomerular protein expression in the PAN þ PHN study on day 6. (a c) Low power images showing absence of albumin staining in the control group, and the presence of albumin (red in B) and neph1 (red in C, arrow) in tubular casts in the study group. In (d l), green color identifies nuclei. (d f) Decrease in b2g1-laminim staining (red) in the (e) noncollapsed and (f) collapsed glomerular capillary loops is shown. Some laminin is also present in the tubular luminal casts (arrow in f), suggesting breakdown of the glomerular capillary loop in the study group. (g l) Severe depletion of WT1 (blue) and GLEPP1 (red) in glomeruli with collapsed loops, and mild (for WT1) and moderate (for GLEPP1) decrease in glomeruli with preserved capillary loops in the study group, is shown. Green color identifies all nuclei. Control immunostains using preimmune serum or normal IgG were negative and are not shown. Original magnification genes that were downregulated in the combination model vs the individual models. Podocyte cell surface protein genes Transient decrease in the GLEPP1 expression (Figure S6) and increase in B7.1 developed on PAN day 3, both of which subsided after the onset of proteinuria. In PHN, increase in B7.1 expression was contributed to both by the podocyte and infiltrating cells, because CD45 expression was also increased. In the combination model, the expression of GLEPP1 was persistently decreased, and that of B7.1 persistently increased through all time points in the absence of any changes in CD45 expression. Decrease in megalin expression developed after the onset of proteinuria in PAN and PHN, and before the onset of proteinuria in the combination model. A prominent new feature of the combination model was the decrease in aminopeptidase A expression late in the combination group. Matrix genes Decrease in COL4A3 and COL4A4 was noted after the onset of proteinuria in all models. No distinctive features were noted in this group of genes. 340 Kidney International (2007) 72,
5 Table 1 List of positive fold-changes in rat glomerular gene expression (mean7s.e.) in the various study groups relative to the corresponding control at the same time point as measured by real-time PCR in PAN, PHN, and PAN+PHN combination experiments PAN day 3 PAN day 6 PAN day 10 Podocyte surface proteins Podocyte surface proteins Podocyte surface proteins kglepp kpodocalyxin kpodocalyxin mb kmegalin kmegalin kb1-integrin Angiogenesis-related Angiogenesis-related kvegfa kangiopoietin kangiopoietin GBM/matrix proteins kangiopoietin kcol4a GBM/matrix proteins kcol4a kcol4a kcol4a PHN day 3 PHN day 6 PHN day 10 Podocyte surface proteins Podocyte surface proteins Podocyte surface proteins mb mb mb Infiltrating leukocyte marker Angiogenesis-related kglepp mcd kvegfa kmegalin kangiopoietin kpodocalyxin SD-related kdystroglycan knephrin kb1-integrin Angiogenesis-related kvegfa kangiopoietin GBM/matrix proteins kcol4a kcol4a kagrin SD-related kfat Transcriptional factors klmx1b kwt Infiltrating leukocyte marker mcd PAN+PHN day 1.5 PAN+PHN day 3 PAN+PHN day 6 Podocyte surface proteins Podocyte surface proteins Podocyte surface proteins mb mb mb kglepp kglepp kglepp kmegalin kmegalin kmegalin Angiogenesis-related Angiogenesis-related kpodocalyxin kvegfa kvegfa kdystroglycan Transcriptional factors kangiopoietin kaminopeptidase A kwt SD-related Angiogenesis-related kpodocin kvegfa kangiopoietin kangiopoietin GBM/matrix proteins kcol4a kcol4a SD-related kpodocin kcd2ap knephrin knephl kzo Transcriptional factors kwt kpod klmxib Intracellular proteins ka-actinin GBM, glomerular basement membrane; PAN, puromycin aminonucleoside nephrosis; PHN, passive Heymann nephritis; SD, slit diaphragm; VEGFA, vascular endothelial growth factor A; WT1, Wilms tumor gene. Gene changes before the onset of proteinuria in various models are shaded. Kidney International (2007) 72,
6 Intracellular proteins No major changes in cathepsin expression were noted in any of the models. Downregulation of a-actinin 4 was a new change noted only on day 6 of the combination model. Transcriptional factors Mild decrease in WT1 and Lmx1b expression were noted on day 10 of PHN, whereas early and progressively increasing downregulation of WT1 and late involvement of Lmx1b were prominent in the combination model. Late decrease in Pod1 expression is a new feature of the combination model. Angiogenesis-related genes Whereas changes in the expression of vascular endothelial growth factor occurred after the onset of proteinuria in PAN and PHN, early onset of downregulation was a prominent feature of the combination model. Effect of corticosteroids on proteinuria and gene expression patterns As has been described previously, 3 corticosteroids decrease, but do not abolish, proteinuria in PAN. Proteinuria in the PAN-steroids and PAN þ PHN combination steroids study is shown in Figure 1. Light and electron microscopies of corticosteroid-treated and untreated rats at each time point were indistinguishable. Statistically significant decrease in proteinuria was noted in the corticosteroid-treated rats on day 5 (Po0.001) and day 6 (Po0.01) in the PANcorticosteroids (PAN-S) group, and day 6 of the PAN PHN combination group (Po0.01), thereby confirming previous observations that PAN is a partially corticosteroid-responsive disease model. Proteinuria on day 10 in PAN-S tended to be less than PAN, but the changes were not statistically significant. Because changes in expression of genes altered on day 3 are likely to influence the course of proteinuria as measured on days 6 and 10, we studied the expression of GLEPP1 and B7.1 in the corticosteroid-treated and untreated rats on day 3 (Table 2). Changes in GLEPP1 expression were corticosteroid-responsive and B7.1 corticosteroid-resistant. In the combination study, proteinuria was significantly decreased in the corticosteroid-treated group on day 6 (Figure 1). Treatment with corticosteroids does not otherwise influence the disease course. Of the genes studied in the corticosteroid-treated rats on day 1.5 before the onset of proteinuria, GLEPP1 and megalin were corticosteroidsensitive. Most genes that were unique to the combination model and were altered after the onset of proteinuria were corticosteroid-resistant, with the notable exception of podocin (Table 2). Assessment for glomerular capillary loop collapse was conducted by an experienced pathologist using sections stained for laminin and nonspecific nuclear stain Sytox green (Figures 2 and 4, Figure S7). Significant changes were noted exclusively in the PAN þ PHN combination day 6 and PAN þ PHN combination day 6 steroid-treated groups. Of 253 glomeruli analyzed in the PAN þ PHN combination group day 6, 23% had segmental collapse, 15% had global collapse, and 62% appeared normal. Of 271 glomeruli analyzed in the PAN þ PHN combination corticosteroid group day 6, 20% had segmental collapse, 15% had global collapse, and 65% appeared normal. Difference between the two groups was not statistically significant. Assessment of distribution of ZHX proteins in the PAN þ PHN combination model A recent publication from our laboratory 1 shows that the three members of the ZHX transcriptional factor family, ZHX1, ZHX2, and ZHX3, are major regulators of podocyte gene expression in glomerular disease. These proteins are predominantly sequestered in the nonnuclear compartment (90 95% for ZHX2 and ZHX3, 80% for ZHX1) in the normal in vivo podocyte. As shown in that study, the predominant ZHX protein-related event in puromycin nephrosis is the transient downregulation, followed by recovery of ZHX3 Table 2 Effect of corticosteroids treatment on changes in gene expression before the onset of proteinuria (PAN, PAN PHN combination), and genes newly altered in the PAN PHN combination model after the onset of proteinuria Gene studied PAN day 3 PAN day 3-S P-value Interpretation GLEPP1 k k Steroid-sensitive B7.1 m m Steroid-resistant PAN+PHN day 1.5 PAN+PHN day 1.5-S GLEPP1 k k Steroid-sensitive B7.1 m m Steroid-resistant Megalin k k Steroid-sensitive VEGF k k Steroid-resistant WT1 k k Steroid-resistant PAN+PHN day 6 PAN+PHN day 6-S Podocin k k Steroid-sensitive CD2AP k k Steroid-resistant Neph 1 k k Steroid-resistant ZO-1 k k Steroid-resistant a-cactinin 4 k k Steroid-resistant Aminopeptidase A k k Steroid-resistant Pod1 k k Steroid-resistant PAN, puromycin aminonucleoside nephrosis; PHN, passive Heymann nephritis; VEGF, vascular endothelial growth factor A. Values represent fold change (mean7s.e.) in expression relative to the corresponding control group at the same time point. 342 Kidney International (2007) 72,
7 expression. This is associated with loss of heterodimerization of ZHX proteins, and entry of ZHX3 into the nucleus coinciding with the development of proteinuria. Assessment of staining for ZHX proteins in the combination model revealed that ZHX1 and ZHX2 were redistributed to the podocyte nucleus as early as day 1.5, even though decreased amounts of both proteins were present in the podocyte (Figure 5). Overall ZHX3 expression was increased, but redistribution to the nucleus was not prominent. Keeping in mind that a large number of the genes studied by us are regulated by ZHX proteins, their increased nuclear presence suggests that early migration of ZHX2 and ZHX1 are likely to mediate some of the gene expression changes in the combination model, for example downregulation of WT1 expression. By contrast, in PHN, changes in the expression of ZHX proteins were noted after the onset of proteinuria (Figure S8). By day 10, expression of ZHX1 (nuclear and nonnuclear) was decreased, and increased podocyte nuclear expression of ZHX2 and ZHX3 was noted, despite marginal decrease in expression in the nonnuclear compartment. DISCUSSION This paper offers new insight into several aspects of the pathogenesis of glomerular disease. In PAN and PHN, the mrna expression of the podocyte cell cell proteins (SD proteins) and the podocyte cell matrix interaction proteins (integrins, dystroglycans) did not change before the onset of proteinuria, indicating that these two important groups of genes are not directly involved in the pathogenesis of proteinuria in the models studied. Changes in SD gene expression are not a prominent feature of PAN, although marginal changes in nephrin gene expression were noted on day 6 (after the onset of proteinuria) in one of three PAN experiments. In PHN, only the expression of nephrin and FAT1 are significantly decreased after the onset of proteinuria. In the combination model, very early and prominent involvement of podocin is noted. The SD genes are the major group of genes that are altered in the combination model and not in the individual models. Interestingly, some of the genes altered only in the combination model have been implicated in the development of focal segmental glomerulosclerosis (aactinin 4, 4 podocin, 5 CD2AP, 6 and WT1 7,8 ). Other genes that are new to the combination model include pod1 and aminopeptidase A. Whereas the decrease in expression of GLEPP1 9 after the onset of proteinuria has been reported previously, 10 its marginal decrease on day 3 of PAN, as observed by us, is even more meaningful. Downregulation before the onset of proteinuria migrates to day 1.5 in the combination model, and is also corticosteroid-sensitive, suggesting a likely role in the pathogenesis of proteinuria. Even though GLEPP1 / and þ / mice are not proteinuric, 11 this does not contradict our findings. It is quite likely that that other genes with similar function may compensate for the lack of GLEPP1 in a b c Control d e f PAN+ PHN Day 1.5 g h i PAN+ PHN Day 6 ZHX1 ZHX2 ZHX3 Figure 5 Confocal assessment of expression of ZHX proteins in the PAN þ PHN combination model. Overall expression of podocyte ZHX1 (green in d, g) and ZHX2 (green in e, h) appears to be decreased in the study group compared to controls (a, b). However, prominent redistribution of ZHX1 and ZHX2 into the nucleus (arrows in d, e, g, h) is noted as early as day 1.5. Because nuclear ZHX proteins are transcriptionally active, it is possible that some of the gene expression changes noted in the combination model, including downregulation of WT1, may be mediated by this early nuclear redistribution of ZHX proteins. The overall expression of ZHX3 appears to be marginally increased (f, i), but prominent redistribution into the nucleus, as published previously in PAN (c), is not obvious. Blue stain identifies all nuclei. Control immunostains using preimmune serum or normal IgG were negative and are not shown. Original magnification 400. Kidney International (2007) 72,
8 these mice during development. The notable feature of GLEPP1 in PAN is the transient nature of the change. Interestingly, we observed persistent downregulation of GLEPP1 in the combination model. Whether this relates directly to the rapid downhill course in these rats is not clear. Changes in B7.1 expression are also revealing. Unlike the persistent upregulation noted after incubation of cultured GECs with puromycin aminonucleoside, 12 in vivo PAN is associated with transient upregulation of B7.1 before the onset of proteinuria. This upregulation occurs in podocytes and is not related to inflammatory cells, because CD45 expression, a surrogate marker of leukocyte infiltration, is unchanged. These finding were confirmed by immunostaining day 3 PAN kidney with anti-cd45 antibodies. Upregulation of B7.1 also shifts to day 1.5 in the combination model, is persistent throughout the time course (in the absence of CD45 changes, which contrasts it from the PHN pattern), but, in contrast to GLEPP1, is corticosteroid unresponsive. None of the genes in our panel were altered on day 1.5 of the individual models. In terms of the gene expression profile, with small exceptions, PAN and PHN alter different genes on day 6. This is logical, because the known basic mechanisms of injury are different (e.g. xanthine oxidase stress vs complementmediated injury and mitogen-activated protein kinase pathway activation). When the two models are induced together, the same early day 3 changes that are noted in the individual model are also noted on day 1.5 of the combination model, and because these changes migrate with the onset of proteinuria, they are also likely to be causally involved in its development. In the combination model, however, there are additional changes in gene expression on day 1.5 that would otherwise occur much later in the individual models. Moreover, these changes are more severe and persistent in the combination model. Why does this happen? These models of podocyte disease are best viewed as a combination of different pathways, some distinct to each model, and some shared among these models. The representative genes studied by us likely belong to at least some of these pathways, but there are likely to be many other pathways that contain genes not studied by us. Combining the two models likely exaggerates the pathways that are common between the two models, and this may result in the early and persistent changes in WT1, vascular endothelial growth factor, and megalin (late day 10 changes in one or both individual models) noted on day 1.5 of the combination model. Changes in these pathways, as well as others not studied by us, are likely to result in the development of a more severe phenotype in the combination model. The development of collapse of the glomerular capillary loops after simultaneous induction of PAN and PHN is an interesting and novel finding. Whereas there was a major element of serendipity in this observation, it is interesting that this approach has never been used previously to vary the onset of proteinuria, largely because most studies in the past have focused on the proteinuric phase of glomerular disease, rather than its pre-proteinuric phase. These observations are made with unperfused kidneys and with kidneys that were perfused before killing. Whereas some cells are noted in the urinary space on day 6 of the combination model, it is not as prominent as in HIVAN or other forms of human collapsing glomerulopathy. Therefore, despite the presence of prominent glomerular capillary loop collapse in the day 6 combination rats, we are unable to label this as collapsing glomerulopathy, which, according to current histological criteria, required both capillary loop collapse and extensive epithelial cell proliferation. The lack of extensive epithelial cell proliferation may be related to the rapid development of changes in the combination model, and the early death of these rats from severe anasarca. Alternatively, distinct pathways may be involved in the development of capillary loop collapse, and in epithelial cell proliferation, and that only the capillary loop collapse-related pathways may be prominently involved in the combination model. Evidence of shedding of glomerular basement membrane and podocytes is often noted in the day 6 PAN þ PHN sections as positive staining for laminin and neph1 in the tubular lumen. In addition, downregulation of WT1 mrna and protein expression, a feature of collapsing glomerulopathy, is noted clearly in the combination model. The prominent redistribution of ZHX1 and ZHX2 proteins into the podocyte nucleus in the combination model, which contrasts with the prominent redistribution of ZHX3 in PAN recently published by us, is likely to explain some of the differences in the gene expression profile noted between the two models, for example presence of WT1 downregulation. Because these changes occur early in the course of the combination model, they are likely to be at least partially responsible for the progressive downhill course of the combination model. In summary, this paper describes early changes in gene expression in primary glomerular disease. It also suggests that simultaneous activation of pathways from two different disorders can result in the redistribution to the nucleus of critical transcriptional factors that result in the development of more severe and rapidly progressive glomerular disease. Further study will be required to link these changes and identify additional pathways that may be involved. MATERIALS AND METHODS Identification of candidate genes Candidate genes were selected if they met two or more of the following criteria: (1) they are critical for maintaining the structure and function of the glomerular capillary loop; (2) within the glomerulus, they are relatively specific to the glomerular capillary loop; and (3) they have been associated with, or have a possibility of being associated with proteinuria. After classifying these genes into structural/functional groups, Taqman probes and primer pairs for each of these genes were developed and tested (Table 3). Real-time polymerase chain reaction Real-time polymerase chain reaction (PCR) primers and probes (FAM-MGB combination) were designed for each gene of interest 344 Kidney International (2007) 72,
9 using Primer Express 2.0 software (Applied Biosystems, Foster City, CA, USA) as described previously. 13 All custom designed probes and control 18S (VIC-MGB) probes were obtained from Applied Biosystems. Details of real-time PCR and establishment of cutoff of significance of a threefold change are described in a recent study. 1 Each value for change in expression in a study group is relative to the expression of a control group at the same time point. Induction of proteinuria PAN and PHN, both models of podocyte injury, were initially studied. Glomerular injury was confirmed by measuring proteinuria, and by light microscopy, immunofluorescence microscopy, and electron microscopy. Glomeruli were extracted using different sets of autoclaved sieves of similar age. To ensure uniformity of technique, all key procedures were performed by the same individual throughout the study. All models were induced at least three times to ensure the validity of the data. Data from a representative study of each kind is presented. All animal studies were approved by the Animal Care and Use Committee at Northwestern University. Induction of PAN Puromycin aminonucleoside (15 mg/100 g) or an equivalent volume of sterile filtered phosphate-buffered saline (PBS) were injected intravenously once into different groups of g male Wistar rats (n ¼ 4 rats/group, baseline proteinuria o1 mg/18 h), and rats euthanized on days 3, 6, and 10 after injection. Rats develop Table 3 Primers and Taqman real-time PCR probes developed for rat glomerular capillary loop genes studied Gene Forward primer Reverse primer Probe SD genes Neph1* TTGCTGCCTTAGTGTTCTTTCTCTAC CCTCAACGTCACATCCTTTCG ACGTCGCAAAGGCAGT Nephrin* TTCAGCAAGGAGACCTTCAAGAA GCCCCTCAATCCACAGCTT TCACTCACCTTGAATGTGA ZO-1* GAGCTACGCTTGCCACACTGT TCGGATCTCCAGGAAGACACTT ACCCTAAAACTTGGCAAAA Podocin TGGAAGCTGAGGCACAAAGA TCCCCTTCGGCAGCAA AGGCCAAAGTGCGGG CD2AP TCAGTAGACCTTGATGCCTTGGT GGAAGCTATGTCATCAAAATTTACATTATC CAGGAACTCAAAAGAAA FAT1 TCAGAGTCCTGTGATGACAATGG GAGGAACACTGGGCATCCA ACCACTGGGATACATCAG P cadherin CCCAAGTTCACTCAAGACACCTT ATCACAGAAGTGCCAGGCATT AGAGGGAGTGTTCCGGAG Podocyte cell surface protein genes b 1 -integrin GGGAATTTGCTAAATTTGAAAAGG TCACGGCACTCTTGTAAATAGGATT AATGCCAAGTGGGACAC Dystroglycan TTGCCTCCAGTGGAGAAATTATC GACGGCAGGGCCTCCTT AGGTGTCTGCAGCAGG Podocalyxin CCCTCTACGGCTGCTGTCA GCAGCTCCTCTGTGAGTCGTT TCCCAGAGGAAGGACCCA Aminopeptidase A GAGGACGGGCAAACCAAGA TCCTGGCATCTGTTGGTTCA ATAGCGGCCACTGAC GLEPP1 CGAATGTCGATGGTACAGACAGA CATCAGCTGCACGCACTGA AGCAGTACATCTTCATCC B7.1 GTCACAGAACTTCACCTGGGTAAA CGGAATTGTTTGCTTTTCATCA CCCCAGAAGACCC Megalin GAAAACCCAAACAGACAACGAACT GCATCCTTTACCTCACTGTCCAT TGAGAACCCAATCTACGCAG Podocyte intracellular protein genes a-actinin 4 TCAACTCCAAATGGGAGAAGGT CTGCTTGCTCTGCTCTTCCA CAGCTGGTGCCGAAG Cathepsin L GGCTATGGTTATGAAGGAACAGATTC CCATTCTTTACCCCAGCTGTTT TAAGGATAAATACTGGCTTGTCA Cathepsin D GCTAGGAGGCCAAAACTATGAACT TTTCCAGCCTGCGATACCTT CACCCAGAGAAGTACATAC Cathepsin B GGGTGATAATGGTTTCTTTAAAATCC CCACGATTTCTGATTCAATTCCA CAGAGGAGAGAACCAC GBM/matrix genes COL4A3 GGTTTTTCCTTCGTTATGTTTACAAGT GGGCGAGGCAAGTGCTT AGGCTCTGAGGGTGCT COL4A4 TCTGGATCGGGTACTCATTTCTAAT TGCCCGCCTCCTTGGT CACACTGGAGCTGGG Entactin GCAATGGAGCCTATAACATATTTGC CCCAGCGTTGCTGCTCTT ATGACAGGGAATCAATGG Agrin GGCTTCAGTGGTGTCATCCA GCAACACATGCTCCTGAGTCA CTAAGAGGCCATCAACT Perlecan-probe 1 CGTCAACACCAAGGACATCATC GAGAACTTGCCCCTGGTCAGT TGGTGCCCCAGATGT Perlecan-probe 2 CGAATATGAGTTCCAGTGCCTTT GGGTTCTCCTCATGCTCACAA TCAAGATGGCTTCAAAG b 2 -laminin ACAAGCCAGAGCAGAACAACTG CGCGTTCATTCTCTTCATATGTG TGTTGCAGGCTGCTC a 5 -laminin-probe 3 ATTCTCCAGCGCTTTTGCA GGCCAGGCAGCTTCAGACT CTTGGGAGCCCGCC a 5 -laminin-probe 4 TGAGGGAGCCGTCACATTAGA CCAGCTCCAGGCTCACATG CAAGGCCAAGATGC Transcriptional factor genes Pod1 GCCAACGACAAGTACGAGAATG GCCACCATAAAGGGCCAAGT ATTCACCCAGTCAACC LMX1B GGGTGACTACGAGAAGGAGAAAGAC CATCTTCATCCTCACTCTTCACAGA CCCGGATGAGTCTGA WT1 TGGTGCCCAGTACAGAATACACA GATACGCGCCGCACATC CCACGGTGTCTTCCGA Pax2 AATGTGTCAGGCACACAGACGTA GAGTGGTGCTCGCCATATCA CCCGTCGTGACCGGT Angiogenesis-related genes VEGF GCACTGGACCCTGGCTTTAC GTGCAGCCTGGGACCACTT CTGTACCTCCACCATGC Angiopoietin 1 CAGTACGACAGATTCCACATAGGAA TCCCCGTGTGACCCTTTAAA CCAGAAGCAGAACTACA Angiopoietin 2-probe 1 GGATGGCTCTGTCAACTTCTTCA CCGTCGATGTTCCCAAACC AACTGGGAGACCTATAAG Angiopoietin 2-probe 2 CAAGTGTTCCCAGATGCTCACA ACTGTCCATTCAAGTTGGAAGGA TGGTGGTTCGACGCAT TIE2 receptor GCCAAAATAGCAGATTTTGGATTG AGCCTTCCCATTGTCTTTTTCA CACGAGGTCAAGAAGT FLT1 AATCAAAACCTTTGAGGAGCTTTC GGTATCCAGATGATAGTCCTCAAACA CCAAATGCCACCTCC GBM, glomerular basement membrane; SD, slit diaphragm. *Derived from reference. 13 Kidney International (2007) 72,
10 proteinuria on day 5 (occasionally on day 4). Eighteen-hour urine collection was obtained in metabolic cages before killing, and proteinuria was assessed. After killing, heparinized serum was obtained by cardiac puncture, small sections preserved for histology as before, 13,14 and glomeruli isolated by sieving for total protein 13 and total RNA extraction using TRIzol (Invitrogen, Carlsbad, CA, USA). Total RNA quality and quantity were assessed using OD260, agarose gel electrophoresis, and the Agilent 2100 bioanalyzer. Quantification of total RNA extracted from different groups was done simultaneously, and cdna templates reverse-transcribed using 2 mg total RNA per template, Superscript III (Invitrogen), and three identical thermocyclers on the same day. RNase H was added to each template at the end of reverse transcription. Depending on the requirements of the experiment, cdna templates were generated per group. Templates were stored at 201C before conducting real-time PCR studies. Induction of PHN Male Wistar rats (n ¼ 4 rats/group, rats weigh g) were injected with 0.4 ml of sheep anti-rat Fx1a or control sheep serum (Sigma, St Louis, MO, USA) on two consecutive days, and proteinuria measured on days 3, 6, and 10 after the first injection. Rats typically become proteinuric on day 4 or day 5. Different groups of rats were killed on days 3, 6, and 10, kidneys removed, and processed as for the PAN group. Induction of PAN þ PHN combination We hypothesized that different models of proteinuria may have some common pathways or mechanisms, and that simultaneous induction of two models of podocyte injury with similar time of onset of proteinuria may modify the course of proteinuria. A pilot study (n ¼ 3/ male Wistar rats/group) in which rats were injected with puromycin þ anti-fx1a, puromycin þ normal sheep IgG, or anti-fx1a þ PBS, and the time of onset of proteinuria noted in all three groups. The puromycin þ anti-fx1a group developed proteinuria at the end of day 2, but not at the end of day 1 or day 1.5 after the first injection. The combination injected rats died of anasarca by day 8. The time of onset of proteinuria in the other two groups was unchanged compared to PAN or PHN, respectively. A detailed combination study was then conducted. Male Wistar rats (n ¼ 4 rats/group, rats weigh g) were injected with anti-fx1a as above on two consecutive days (PHN groups), or puromycin aminonucleoside (PAN groups), a combination of anti-fx1a on two consecutive days and puromycin aminonucleoside on day 0 (PAN þ PHN combination groups), control sheep serum (sheep serum groups) or PBS (PBS groups), and different groups killed on days 1.5, 3, 6, and 10. Kidneys from killed rats were processed as above. To ensure that morphological changes were unrelated to processing artifacts, the studies were repeated in rats in which kidneys were perfused via the aorta with PBS before killing. Corticosteroid treatment study The overall characteristics of the animals and procedures were identical to the other experiments discussed above. In the corticosteroid study, we repeated the PAN (days 1.5, 3, 6, and 10 time points) and the combination study (days 1.5, 3, and 6 time points), along with two additional studies. In the PAN-S study, rats were given 3 mg intraperitoneal 6a-methylprednisolone 21-hemisuccinate on alternate days, starting 24 h after injection of puromycin aminonucleoside. In view of the shorter lifespan of rats in the PAN þ PHN combination study, the above-mentioned corticosteroid dose was given intraperitoneally at the same time as disease induction (PAN þ PHN combination-s study), and then continued on alternate days. Corticosteroids did not alter the longevity of the rats with PAN þ PHN combination disease. Methods for extraction of total RNA and protein, and Westernblot protocols are described in previous publications. 13,14 Imaging studies Immunofluorescence staining of tissue section was conducted as described previously. 1 Images were acquired in multichannel mode using a Zeiss Pascal 5 confocal laser microscope using the following laser and filter combinations: 488 nm argon laser and BP nm filter; 543 nm helium-neon laser and BP nm filter; and 633 nm helium-neon laser and LP 650 nm filter. Antibodies obtained from commercial sources include mouse antihuman WT1 (sc-7385; Santa Cruz Biotechnology, Santa Cruz, CA, USA), hamster anti-b7.1 (BD Biosciences, San Jose, CA, USA), mouse anti-rat CD45 (Cedarlane Laboratories, Hornby, Ontario, Canada), rabbit anti-rat albumin (Research Diagnostics Inc. (Flanders, NJ), mouse anti-rat b2g1 laminin (Abcam, Cambridge, MA, USA), rabbit anti-zhx1 (Bethyl laboratories, Montgomery, TX), mouse anti-zhx2 (Abnova, Taipei city, Taiwan), and anti- PCNA antibody (Dako Corporation, Glostrup, Denmark). Control immunostains with preimmune serum or normal IgG of the same species as the primary antibody were performed for each experiment. Techniques for electron microscopy and light microscopy are described elsewhere Statistical analysis Analysis of difference in proteinuria or gene expression involving three or more groups was conducted by ANOVA with post-analysis testing using GraphPad InStat software (version 3.05). Comparison of two groups was conducted using the unpaired Student s t-test in Microsoft Excel ACKNOWLEDGMENTS The authors thank Richard Quigg and William G Couser for generously providing anti-fx1a, and Roger Wiggins for anti-glepp1 antibodies. Some aspects of this study were presented as an oral free communication at the 2005 American Society of Nephrology meeting. Research support: This work was supported by the following research grants to Sumant S Chugh: Carl W. Gottschalk Research Scholar Award of the American Society of Nephrology, the Amgen Inc. Young Investigator Grant from the National Kidney Foundation, Norman S. Coplon Satellite Research Grant, and NIH grants DK61275, DK and DK Carmen Avila-Casado is a recipient of the CONACYT 111 grant. SUPPLEMENTARY MATERIAL Figure S6. Reduction of GLEPP1 protein (red) expression on day 3 of puromycin nephrosis prior to the onset of proteinuria. Figure S7. Additional confocal images showing the development of segmental (Panels B, C) to global (panels D to F) glomerular collapse by confocal imaging in day 6 PAN þ PHN rats. Figure S8. Confocal assessment of the expression of ZHX proteins (red) and WT1 (blue) in glomeruli on PHN day 10. REFERENCES 1. Liu G, Clement L, Kanwar YS et al. ZHX proteins regulate podocyte gene expression during the development of nephrotic syndrome. J Biol Chem 2006; 281: Kidney International (2007) 72,
11 2. Barisoni L, Kriz W, Mundel P, D Agati V. The dysregulated podocyte phenotype: a novel concept in the pathogenesis of collapsing idiopathic focal segmental glomerulosclerosis and HIV-associated nephropathy. J Am Soc Nephrol 1999; 10: Nakamura T, Ebihara I, Fukui M et al. Effects of methylprednisolone on glomerular and medullary mrna levels for extracellular matrices in puromycin aminonucleoside nephrosis. Kidney Int 1991; 40: Kaplan JM, Kim SH, North KN et al. Mutations in ACTN4, encoding alphaactinin-4, cause familial focal segmental glomerulosclerosis. Nat Genet 2000; 24: Boute N, Gribouval O, Roselli S et al. NPHS2, encoding the glomerular protein podocin, is mutated in autosomal recessive steroid-resistant nephrotic syndrome. Nat Genet 2000; 24: Kim JM, Wu H, Green G et al. CD2-associated protein haploinsufficiency is linked to glomerular disease susceptibility. Science 2003; 300: Barbaux S, Niaudet P, Gubler MC et al. Donor splice-site mutations in WT1 are responsible for Frasier syndrome. Nat Genet 1997; 17: Orloff MS, Iyengar SK, Winkler CA et al. Variants in the Wilms tumor gene are associated with focal segmental glomerulosclerosis in the African American population. Physiol Genomics 2005; 21: Thomas PE, Wharram BL, Goyal M et al. GLEPP1, a renal glomerular epithelial cell (podocyte) membrane protein-tyrosine phosphatase. Identification, molecular cloning, and characterization in rabbit. J Biol Chem 1994; 269: Kim YH, Goyal M, Wharram B et al. GLEPP1 receptor tyrosine phosphatase (Ptpro) in rat PAN nephrosis. A marker of acute podocyte injury. Nephron 2002; 90: Wharram BL, Goyal M, Gillespie PJ et al. Altered podocyte structure in GLEPP1 (Ptpro)-deficient mice associated with hypertension and low glomerular filtration rate. J Clin Invest 2000; 106: Reiser J, von Gersdorff G, Loos M et al. Induction of B7-1 in podocytes is associated with nephrotic syndrome. J Clin Invest 2004; 113: Liu G, Kaw B, Kurfis J et al. Neph1 and nephrin interaction in the slit diaphragm is an important determinant of glomerular permeability. J Clin Invest 2003; 112: Chugh S, Yuan H, Haydar S et al. Aminopeptidase A: a nephritogenic target antigen of nephrotoxic serum. Kidney Int 2001; 59: Avila-Casado MC, Perez-Torres I, Auron A et al. Proteinuria in rats induced by serum from patients with collapsing glomerulopathy. Kidney Int 2004; 66: Kidney International (2007) 72,
Glomerular Pathology- 1 Nephrotic Syndrome. Dr. Nisreen Abu Shahin
 Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Supplementary Information Titles
 Journal: Nature Medicine Supplementary Information Titles Article Title: Podocyte secreted Angiopoietin-like mediates proteinuria in glucocorticoid sensitive nephrotic syndrome Corresponding Author: Sumant
Journal: Nature Medicine Supplementary Information Titles Article Title: Podocyte secreted Angiopoietin-like mediates proteinuria in glucocorticoid sensitive nephrotic syndrome Corresponding Author: Sumant
3. PODOCYTE INJURY IN GLOMERULAR DISEASES
 How to Cite this article: Podocyte Injury in Glomerular Diseases - ejifcc 20/01 2009 http://www.ifcc.org 3. PODOCYTE INJURY IN GLOMERULAR DISEASES Mirjana Sabljar Matovinović Podocytes are injured in diabetic
How to Cite this article: Podocyte Injury in Glomerular Diseases - ejifcc 20/01 2009 http://www.ifcc.org 3. PODOCYTE INJURY IN GLOMERULAR DISEASES Mirjana Sabljar Matovinović Podocytes are injured in diabetic
Podocyte Biology and clinical applications Dr. F. Ahmadi Professor Of Nephrology TUMS
 Podocyte Biology and clinical applications Dr. F. Ahmadi Professor Of Nephrology TUMS Proteinuria is a major healthcare problem that affects several hundred million people worldwide. Proteinuria is a cardinal
Podocyte Biology and clinical applications Dr. F. Ahmadi Professor Of Nephrology TUMS Proteinuria is a major healthcare problem that affects several hundred million people worldwide. Proteinuria is a cardinal
A clinical syndrome, composed mainly of:
 Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
RENAL HISTOPATHOLOGY
 RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
Overview of glomerular diseases
 Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
Histopathology: Glomerulonephritis and other renal pathology
 Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Glomerular diseases mostly presenting with Nephritic syndrome
 Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
Dr Ian Roberts Oxford. Oxford Pathology Course 2010 for FRCPath Illustration-Cellular Pathology. Oxford Radcliffe NHS Trust
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Ordering Physician. Collected REVISED REPORT. Performed. IgG IF, Renal MCR. Lambda IF, Renal MCR. C1q IF, Renal. MCR Albumin IF, Renal MCR
 RenalPath Level IV Wet Ts IgA I Renal IgM I Renal Kappa I Renal Renal Bx Electron Microscopy IgG I Renal Lambda I Renal C1q I Renal C3 I Renal Albumin I Renal ibrinogen I Renal Mayo Clinic Dept. of Lab
RenalPath Level IV Wet Ts IgA I Renal IgM I Renal Kappa I Renal Renal Bx Electron Microscopy IgG I Renal Lambda I Renal C1q I Renal C3 I Renal Albumin I Renal ibrinogen I Renal Mayo Clinic Dept. of Lab
The evolution of the classification of nephrotic syndrome and the new taxonomy for the podocytopathies Laura Barisoni, MD
 The evolution of the classification of nephrotic syndrome and the new taxonomy for the podocytopathies Laura Barisoni, MD Department of Pathology and Medicine, Division of Nephrology New York University
The evolution of the classification of nephrotic syndrome and the new taxonomy for the podocytopathies Laura Barisoni, MD Department of Pathology and Medicine, Division of Nephrology New York University
Glomerular pathology-2 Nephritic syndrome. Dr. Nisreen Abu Shahin
 Glomerular pathology-2 Nephritic syndrome Dr. Nisreen Abu Shahin 1 The Nephritic Syndrome Pathogenesis: inflammation proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls
Glomerular pathology-2 Nephritic syndrome Dr. Nisreen Abu Shahin 1 The Nephritic Syndrome Pathogenesis: inflammation proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls
Genetics of Steroid Resistant Nephrotic syndrome. Velibor Tasic University Children s Hospital Skopje, Macedonia
 Genetics of Steroid Resistant Nephrotic syndrome Velibor Tasic University Children s Hospital Skopje, Macedonia Nephrotic syndrome - definition Oedema Massive proteinuria (> 50mg/kg/d or> 40mg/m2/h Hypoalbuminemia
Genetics of Steroid Resistant Nephrotic syndrome Velibor Tasic University Children s Hospital Skopje, Macedonia Nephrotic syndrome - definition Oedema Massive proteinuria (> 50mg/kg/d or> 40mg/m2/h Hypoalbuminemia
Glomerular pathology in systemic disease
 Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Pu Duann, MD, PhD Hideki G. Kawanishi, MD Eugene J. Gross, BS Prasun K. Datta, PhD Elias A. Lianos, MD, PhD
 Detection of Injury-induced Changes in Gene Expression of the Glomerular Epithelial Cell-specific Marker, Wilm s Tumor-1, by Laser Capture Microdissection Pu Duann, MD, PhD Hideki G. Kawanishi, MD Eugene
Detection of Injury-induced Changes in Gene Expression of the Glomerular Epithelial Cell-specific Marker, Wilm s Tumor-1, by Laser Capture Microdissection Pu Duann, MD, PhD Hideki G. Kawanishi, MD Eugene
Neph1 and nephrin interaction in the slit diaphragm is an important determinant of glomerular permeability
 Neph1 and nephrin interaction in the slit diaphragm is an important determinant of glomerular permeability Gang Liu, 1 Beenu Kaw, 2 Jayson Kurfis, 1 Syed Rahmanuddin, 1 Yashpal S. Kanwar, 3 and Sumant
Neph1 and nephrin interaction in the slit diaphragm is an important determinant of glomerular permeability Gang Liu, 1 Beenu Kaw, 2 Jayson Kurfis, 1 Syed Rahmanuddin, 1 Yashpal S. Kanwar, 3 and Sumant
Renal Pathology 1: Glomerulus. With many thanks to Elizabeth Angus PhD for EM photographs
 Renal Pathology 1: Glomerulus With many thanks to Elizabeth Angus PhD for EM photographs Anatomy of the Kidney http://www.yalemedicalgroup.org/stw/page.asp?pageid=stw028980 The Nephron http://www.beltina.org/health-dictionary/nephron-function-kidney-definition.html
Renal Pathology 1: Glomerulus With many thanks to Elizabeth Angus PhD for EM photographs Anatomy of the Kidney http://www.yalemedicalgroup.org/stw/page.asp?pageid=stw028980 The Nephron http://www.beltina.org/health-dictionary/nephron-function-kidney-definition.html
The evolution of the classification of nephrotic syndrome Laura Barisoni, MD
 The evolution of the classification of nephrotic syndrome Laura Barisoni, MD Department of Pathology and Medicine, Division of Nephrology New York University Old classification schemes: Proteinuria and
The evolution of the classification of nephrotic syndrome Laura Barisoni, MD Department of Pathology and Medicine, Division of Nephrology New York University Old classification schemes: Proteinuria and
CHAPTER 2. Primary Glomerulonephritis
 2nd Report of the PRIMARY GLOMERULONEPHRITIS CHAPTER 2 Primary Glomerulonephritis Sunita Bavanandan Lee Han Wei Lim Soo Kun 21 PRIMARY GLOMERULONEPHRITIS 2nd Report of the 2.1 Introduction This chapter
2nd Report of the PRIMARY GLOMERULONEPHRITIS CHAPTER 2 Primary Glomerulonephritis Sunita Bavanandan Lee Han Wei Lim Soo Kun 21 PRIMARY GLOMERULONEPHRITIS 2nd Report of the 2.1 Introduction This chapter
Expression of human nephrin mrna in diabetic nephropathy
 Nephrol Dial Transplant (2004) 19: 380 385 DOI: 10.1093/ndt/gfg545 Original Article Expression of human nephrin mrna in diabetic nephropathy Masao Toyoda, Daisuke Suzuki, Tomoya Umezono, Goro Uehara, Mayumi
Nephrol Dial Transplant (2004) 19: 380 385 DOI: 10.1093/ndt/gfg545 Original Article Expression of human nephrin mrna in diabetic nephropathy Masao Toyoda, Daisuke Suzuki, Tomoya Umezono, Goro Uehara, Mayumi
Focal Segmental Glomerulosclerosis and the Nephro6c Syndrome Dr. A. Gangji Dr. P. Marge>s
 Focal Segmental Glomerulosclerosis and the Nephro6c Syndrome Dr. A. Gangji Dr. P. Marge>s The basic facts about proteinuria and FSGS A primer on proteinuria Endothelium and glycocalyx Podocytes Pathology
Focal Segmental Glomerulosclerosis and the Nephro6c Syndrome Dr. A. Gangji Dr. P. Marge>s The basic facts about proteinuria and FSGS A primer on proteinuria Endothelium and glycocalyx Podocytes Pathology
Section Title. Subject Index
 Section Title Subject Index Acute kidney injury definitions 287 289 hypoxia 287, 290 overview 286, 287 sublethal tubular injury adaptive responses 292, 293 combination of sublethal injuries 291, 292 detection
Section Title Subject Index Acute kidney injury definitions 287 289 hypoxia 287, 290 overview 286, 287 sublethal tubular injury adaptive responses 292, 293 combination of sublethal injuries 291, 292 detection
Case # 2 3/27/2017. Disclosure of Relevant Financial Relationships. Clinical history. Clinical history. Laboratory findings
 Case # 2 Christopher Larsen, MD Arkana Laboratories Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content
Case # 2 Christopher Larsen, MD Arkana Laboratories Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content
Nephritic vs. Nephrotic Syndrome
 Page 1 of 18 Nephritic vs. Nephrotic Syndrome Terminology: Glomerulus: A network of blood capillaries contained within the cuplike end (Bowman s capsule) of a nephron. Glomerular filtration rate: The rate
Page 1 of 18 Nephritic vs. Nephrotic Syndrome Terminology: Glomerulus: A network of blood capillaries contained within the cuplike end (Bowman s capsule) of a nephron. Glomerular filtration rate: The rate
Case Presentation Turki Al-Hussain, MD
 Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
INTRODUCTION TO GLOMERULAR DISEASES
 INTRODUCTION TO GLOMERULAR DISEASES Goal: to explain the general mechanisms leading to glomerular diseases and to analyze what is known about their relationship to morphologic and clinical manifestations
INTRODUCTION TO GLOMERULAR DISEASES Goal: to explain the general mechanisms leading to glomerular diseases and to analyze what is known about their relationship to morphologic and clinical manifestations
CHAPTER 2 PRIMARY GLOMERULONEPHRITIS
 CHAPTER 2 Sunita Bavanandan Lim Soo Kun 19 5th Report of the 2.1: Introduction This chapter covers the main primary glomerulonephritis that were reported to the MRRB from the years 2005-2012. Minimal change
CHAPTER 2 Sunita Bavanandan Lim Soo Kun 19 5th Report of the 2.1: Introduction This chapter covers the main primary glomerulonephritis that were reported to the MRRB from the years 2005-2012. Minimal change
General introduction. General introduction
 General introduction 1 Chapter 1 Proteinuria is the excretion of proteins into the urine. Presence of abnormal proteinuria, the urinary excretion of abnormal amounts of serum proteins (briefly called proteinuria),
General introduction 1 Chapter 1 Proteinuria is the excretion of proteins into the urine. Presence of abnormal proteinuria, the urinary excretion of abnormal amounts of serum proteins (briefly called proteinuria),
Surgical Pathology Report
 Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
C1q nephropathy the Diverse Disease
 C1q nephropathy the Diverse Disease Danica Galešić Ljubanović School of Medicine, University of Zagreb Dubrava University Hospital Zagreb, Croatia Definition Dominant or codominant ( 2+), mesangial staining
C1q nephropathy the Diverse Disease Danica Galešić Ljubanović School of Medicine, University of Zagreb Dubrava University Hospital Zagreb, Croatia Definition Dominant or codominant ( 2+), mesangial staining
Ectopic Notch Activation in Developing Podocytes Causes Glomerulosclerosis
 Ectopic Notch Activation in Developing Podocytes Causes Glomerulosclerosis Aoife M. Waters,* Megan Y.J. Wu,* Tuncer Onay,* Jacob Scutaru,* Ju Liu, Corrinne G. Lobe, Susan E. Quaggin, and Tino D. Piscione*
Ectopic Notch Activation in Developing Podocytes Causes Glomerulosclerosis Aoife M. Waters,* Megan Y.J. Wu,* Tuncer Onay,* Jacob Scutaru,* Ju Liu, Corrinne G. Lobe, Susan E. Quaggin, and Tino D. Piscione*
Interesting case seminar: Native kidneys Case Report:
 Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab
 TRANSPLANTATION Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab Khadijeh Makhdoomi, 1,2 Saeed Abkhiz, 1,2 Farahnaz Noroozinia, 1,3
TRANSPLANTATION Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab Khadijeh Makhdoomi, 1,2 Saeed Abkhiz, 1,2 Farahnaz Noroozinia, 1,3
The spectrum of primary nephrotic syndrome includes a
 In-Depth Review A Proposed Taxonomy for the Podocytopathies: A Reassessment of the Primary Nephrotic Diseases Laura Barisoni,* H. William Schnaper, and Jeffrey B. Kopp *Department of Pathology, New York
In-Depth Review A Proposed Taxonomy for the Podocytopathies: A Reassessment of the Primary Nephrotic Diseases Laura Barisoni,* H. William Schnaper, and Jeffrey B. Kopp *Department of Pathology, New York
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
Pathophysiology of focal segmental glomerulosclerosis
 Pediatr Nephrol (2007) 22:350 354 DOI 10.1007/s00467-006-0357-2 EDUCATIONAL FEATURE Pathophysiology of focal segmental glomerulosclerosis Kimberly Reidy & Frederick J. Kaskel Received: 1 June 2006 /Revised:
Pediatr Nephrol (2007) 22:350 354 DOI 10.1007/s00467-006-0357-2 EDUCATIONAL FEATURE Pathophysiology of focal segmental glomerulosclerosis Kimberly Reidy & Frederick J. Kaskel Received: 1 June 2006 /Revised:
Minimal change disease and idiopathic FSGS: manifestations of the same disease
 PERSPECTIVES OPINION Minimal change disease and idiopathic FSGS: manifestations of the same disease Rutger J. Maas 1, Jeroen K. Deegens 1, Bart Smeets 2, Marcus J. Moeller 3 and Jack F. Wetzels 1 Abstract
PERSPECTIVES OPINION Minimal change disease and idiopathic FSGS: manifestations of the same disease Rutger J. Maas 1, Jeroen K. Deegens 1, Bart Smeets 2, Marcus J. Moeller 3 and Jack F. Wetzels 1 Abstract
The Ebf1 knockout mouse and glomerular maturation
 Repository of the Max Delbrück Center for Molecular Medicine (MDC) Berlin (Germany) http://edoc.mdc-berlin.de/14009/ The Ebf1 knockout mouse and glomerular maturation Schmidt-Ott, K.M. Published in final
Repository of the Max Delbrück Center for Molecular Medicine (MDC) Berlin (Germany) http://edoc.mdc-berlin.de/14009/ The Ebf1 knockout mouse and glomerular maturation Schmidt-Ott, K.M. Published in final
Journal Club. 03/04/2012 Lama Nazzal
 Journal Club 03/04/2012 Lama Nazzal NOTCH and the kidneys Is an evolutionarily conserved cell cell communication mechanism. Is a regulator of cell specification, differentiation, and tissue patterning.
Journal Club 03/04/2012 Lama Nazzal NOTCH and the kidneys Is an evolutionarily conserved cell cell communication mechanism. Is a regulator of cell specification, differentiation, and tissue patterning.
Urinary CD80 as a Replacement for Renal Biopsy for Diagnosis of Pediatric Minimal Change Disease
 KIDNEY DISEASES Urinary CD80 as a Replacement for Renal Biopsy for Diagnosis of Pediatric Minimal Change Disease Heba Mostafa Ahmed, 1 Dina Ahmed Ezzat, 1 Noha A Doudar, 2 Mai Adel 1 1 Departement of Pediatrics,
KIDNEY DISEASES Urinary CD80 as a Replacement for Renal Biopsy for Diagnosis of Pediatric Minimal Change Disease Heba Mostafa Ahmed, 1 Dina Ahmed Ezzat, 1 Noha A Doudar, 2 Mai Adel 1 1 Departement of Pediatrics,
Light and electron microscopical studies of focal glomerular sclerosis
 J. clin. Path., 1971, 24, 846-850 Light and electron microscopical studies of focal glomerular sclerosis A. H. NAGI, F. ALEXANDER, AND R. LANNIGAN From the Department of Pathology, Queen's University of
J. clin. Path., 1971, 24, 846-850 Light and electron microscopical studies of focal glomerular sclerosis A. H. NAGI, F. ALEXANDER, AND R. LANNIGAN From the Department of Pathology, Queen's University of
Elevated Serum Creatinine, a simplified approach
 Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Clinical Case Presentation. Dana Assis, MD
 Clinical Case Presentation Dana Assis, MD 4.12.2016 Clinical Presentation 63 year old male with medical history AIDS (CD4 11, VL 62K), Hep C cirrhosis (never treated), DM II c/b diabetic retinopathy, HTN,
Clinical Case Presentation Dana Assis, MD 4.12.2016 Clinical Presentation 63 year old male with medical history AIDS (CD4 11, VL 62K), Hep C cirrhosis (never treated), DM II c/b diabetic retinopathy, HTN,
Monoclonal Gammopathies and the Kidney. Tibor Nádasdy, MD The Ohio State University, Columbus, OH
 Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
INTRODUCTION TO GLOMERULAR DISEASES
 INTRODUCTION TO GLOMERULAR DISEASES Goals: to explain the general mechanisms leading to glomerular diseases and to analyze what is known about their relationship to morphologic and clinical manifestations
INTRODUCTION TO GLOMERULAR DISEASES Goals: to explain the general mechanisms leading to glomerular diseases and to analyze what is known about their relationship to morphologic and clinical manifestations
A familial childhood-onset relapsing nephrotic syndrome
 the renal consult http://www.kidney-international.org & 2007 International Society of Nephrology A familial childhood-onset relapsing nephrotic syndrome A Kitamura,5, H Tsukaguchi 2,5, R Hiramoto, A Shono
the renal consult http://www.kidney-international.org & 2007 International Society of Nephrology A familial childhood-onset relapsing nephrotic syndrome A Kitamura,5, H Tsukaguchi 2,5, R Hiramoto, A Shono
Familial DDD associated with a gain-of-function mutation in complement C3.
 Familial DDD associated with a gain-of-function mutation in complement C3. Santiago Rodríguez de Córdoba, Centro de investigaciones Biológicas, Madrid Valdés Cañedo F. and Vázquez- Martul E., Complejo
Familial DDD associated with a gain-of-function mutation in complement C3. Santiago Rodríguez de Córdoba, Centro de investigaciones Biológicas, Madrid Valdés Cañedo F. and Vázquez- Martul E., Complejo
Lab 3, case 1. Is this an example of nephrotic or nephritic syndrome? Why? Which portion of the nephron would you expect to be abnormal?
 Lab 3, case 1 12-year-old Costa Rican boy is brought into clinic by his parents because of dark brownish-red urine over the last 24 hours. The family has been visiting friends in Indianapolis for two weeks.
Lab 3, case 1 12-year-old Costa Rican boy is brought into clinic by his parents because of dark brownish-red urine over the last 24 hours. The family has been visiting friends in Indianapolis for two weeks.
Genetic Testing of Children with Steroid Resistant Nephrotic Syndrome
 The 5 th Global Congress For Consensus in Pediatrics & Child Health Genetic Testing of Children with Steroid Resistant Nephrotic Syndrome Fang Wang Peking University First Hospital Nephrotic Syndrome (NS)
The 5 th Global Congress For Consensus in Pediatrics & Child Health Genetic Testing of Children with Steroid Resistant Nephrotic Syndrome Fang Wang Peking University First Hospital Nephrotic Syndrome (NS)
DEVELOPMENT OF A NOVEL DIAGNOSTIC TEST USING PODOCYTURIA AS A BIOMARKER FOR DETECTION OF KIDNEY DAMAGE. An Undergraduate Research Scholars Thesis
 DEVELOPMENT OF A NOVEL DIAGNOSTIC TEST USING PODOCYTURIA AS A BIOMARKER FOR DETECTION OF KIDNEY DAMAGE An Undergraduate Research Scholars Thesis by EESHA FAROOQI Submitted to Honors and Undergraduate Research
DEVELOPMENT OF A NOVEL DIAGNOSTIC TEST USING PODOCYTURIA AS A BIOMARKER FOR DETECTION OF KIDNEY DAMAGE An Undergraduate Research Scholars Thesis by EESHA FAROOQI Submitted to Honors and Undergraduate Research
Association analysis of podocyte slit diaphragm genes as candidates for diabetic nephropathy
 Diabetologia (2008) 51:86 90 DOI 10.1007/s00125-007-0854-2 SHORT COMMUNICATION Association analysis of podocyte slit diaphragm genes as candidates for diabetic nephropathy P. Ihalmo & M. Wessman & M. A.
Diabetologia (2008) 51:86 90 DOI 10.1007/s00125-007-0854-2 SHORT COMMUNICATION Association analysis of podocyte slit diaphragm genes as candidates for diabetic nephropathy P. Ihalmo & M. Wessman & M. A.
C3 GLOMERULOPATHIES. Budapest Nephrology School Zoltan Laszik
 C3 GLOMERULOPATHIES Budapest Nephrology School 8.30.2018. Zoltan Laszik 1 Learning Objectives Familiarize with the pathogenetic mechanisms of glomerular diseases Learn the pathologic landscape and clinical
C3 GLOMERULOPATHIES Budapest Nephrology School 8.30.2018. Zoltan Laszik 1 Learning Objectives Familiarize with the pathogenetic mechanisms of glomerular diseases Learn the pathologic landscape and clinical
Crescentic Glomerulonephritis (RPGN)
 Crescentic Glomerulonephritis (RPGN) Background Rapidly progressive glomerulonephritis (RPGN) is defined as any glomerular disease characterized by extensive crescents (usually >50%) as the principal histologic
Crescentic Glomerulonephritis (RPGN) Background Rapidly progressive glomerulonephritis (RPGN) is defined as any glomerular disease characterized by extensive crescents (usually >50%) as the principal histologic
An unusual association between focal segmental sclerosis and lupus nephritis: a distinct concept from lupus podocytopathy?
 CEN Case Rep (2015) 4:70 75 DOI 10.1007/s13730-014-0142-1 CASE REPORT An unusual association between focal segmental sclerosis and lupus nephritis: a distinct concept from lupus podocytopathy? Hironari
CEN Case Rep (2015) 4:70 75 DOI 10.1007/s13730-014-0142-1 CASE REPORT An unusual association between focal segmental sclerosis and lupus nephritis: a distinct concept from lupus podocytopathy? Hironari
Dense deposit disease with steroid pulse therapy
 Case Report Dense deposit disease with steroid pulse therapy Jun Odaka, Takahiro Kanai, Takane Ito, Takashi Saito, Jun Aoyagi, and Mariko Y Momoi Abstract Treatment of dense deposit disease DDD has not
Case Report Dense deposit disease with steroid pulse therapy Jun Odaka, Takahiro Kanai, Takane Ito, Takashi Saito, Jun Aoyagi, and Mariko Y Momoi Abstract Treatment of dense deposit disease DDD has not
A Compendium of Urinary Biomarkers Indicative of Glomerular Podocytopathy
 A Compendium of Urinary Biomarkers Indicative of Glomerular Podocytopathy The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation
A Compendium of Urinary Biomarkers Indicative of Glomerular Podocytopathy The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation
CASE OF THE WEEK 1
 www.nephro-pathology.com CASE OF THE WEEK 1 Clinical Presentation: A 17 year old Indian boy presented with anasarca, decreased urine output and episodes of nausea and vomiting over the last three weeks.
www.nephro-pathology.com CASE OF THE WEEK 1 Clinical Presentation: A 17 year old Indian boy presented with anasarca, decreased urine output and episodes of nausea and vomiting over the last three weeks.
Plasma soluble urokinase receptor levels are increased but do not distinguish primary from secondary focal segmental glomerulosclerosis
 http://www.kidney-international.org & 213 International Society of Nephrology see commentary on page 235 Plasma soluble urokinase receptor levels are increased but do not distinguish primary from secondary
http://www.kidney-international.org & 213 International Society of Nephrology see commentary on page 235 Plasma soluble urokinase receptor levels are increased but do not distinguish primary from secondary
Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/-
 Supplemental Material Results. Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/- and Slc2a7 -/- mice. The expression of AE1 in the kidney was examined in Slc26a7 KO mice.
Supplemental Material Results. Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/- and Slc2a7 -/- mice. The expression of AE1 in the kidney was examined in Slc26a7 KO mice.
CASE 3 AN UNUSUAL CASE OF NEPHROTIC SYNDROME
 CASE 3 AN UNUSUAL CASE OF NEPHROTIC SYNDROME Dr Seethalekshmy N.V., Dr.Annie Jojo, Dr Hiran K.R., Amrita institute of Medical Sciences, Kochi, Kerala Case history 34 year old gentleman Nephrotic range
CASE 3 AN UNUSUAL CASE OF NEPHROTIC SYNDROME Dr Seethalekshmy N.V., Dr.Annie Jojo, Dr Hiran K.R., Amrita institute of Medical Sciences, Kochi, Kerala Case history 34 year old gentleman Nephrotic range
Membranous nephropathy. By Mohammed Kamal Nassar, MD Lecturer of Nephrology Mansoura University
 Membranous nephropathy By Mohammed Kamal Nassar, MD Lecturer of Nephrology Mansoura University Membranous nephropathy Definition: Immune complex glomerular disease in which immune deposits of IgG and complement
Membranous nephropathy By Mohammed Kamal Nassar, MD Lecturer of Nephrology Mansoura University Membranous nephropathy Definition: Immune complex glomerular disease in which immune deposits of IgG and complement
Supplementary Figure 1: Hsp60 / IEC mice are embryonically lethal (A) Light microscopic pictures show mouse embryos at developmental stage E12.
 Supplementary Figure 1: Hsp60 / IEC mice are embryonically lethal (A) Light microscopic pictures show mouse embryos at developmental stage E12.5 and E13.5 prepared from uteri of dams and subsequently genotyped.
Supplementary Figure 1: Hsp60 / IEC mice are embryonically lethal (A) Light microscopic pictures show mouse embryos at developmental stage E12.5 and E13.5 prepared from uteri of dams and subsequently genotyped.
Cells and reagents. Synaptopodin knockdown (1) and dynamin knockdown (2)
 Supplemental Methods Cells and reagents. Synaptopodin knockdown (1) and dynamin knockdown (2) podocytes were cultured as described previously. Staurosporine, angiotensin II and actinomycin D were all obtained
Supplemental Methods Cells and reagents. Synaptopodin knockdown (1) and dynamin knockdown (2) podocytes were cultured as described previously. Staurosporine, angiotensin II and actinomycin D were all obtained
A new mouse experimental model of focal segmental glomerulosclerosis produced by the administration of polyclonal anti-mouse nephrin antibody
 Original Contribution Kitasato Med J 2015; 45: 29-37 A new mouse experimental model of focal segmental glomerulosclerosis produced by the administration of polyclonal anti-mouse nephrin antibody Chikako
Original Contribution Kitasato Med J 2015; 45: 29-37 A new mouse experimental model of focal segmental glomerulosclerosis produced by the administration of polyclonal anti-mouse nephrin antibody Chikako
The topic of normal vascular and glomerular anatomy is introduced
 Normal Vascular and Glomerular Anatomy Arthur H. Cohen Richard J. Glassock The topic of normal vascular and glomerular anatomy is introduced here to serve as a reference point for later illustrations of
Normal Vascular and Glomerular Anatomy Arthur H. Cohen Richard J. Glassock The topic of normal vascular and glomerular anatomy is introduced here to serve as a reference point for later illustrations of
Glomerulonephritis. Dr Rodney Itaki Anatomical Pathology Discipline.
 Glomerulonephritis Dr Rodney Itaki Anatomical Pathology Discipline. University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology Gross anatomy Ref: Goggle Images Microanatomy
Glomerulonephritis Dr Rodney Itaki Anatomical Pathology Discipline. University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology Gross anatomy Ref: Goggle Images Microanatomy
Nature Immunology: doi: /ni eee Supplementary Figure 1
 eee Supplementary Figure 1 Hyphae induce NET release, but yeast do not. (a) NET release by human peripheral neutrophils stimulated with a hgc1 yeast-locked C. albicans mutant (yeast) or pre-formed WT C.
eee Supplementary Figure 1 Hyphae induce NET release, but yeast do not. (a) NET release by human peripheral neutrophils stimulated with a hgc1 yeast-locked C. albicans mutant (yeast) or pre-formed WT C.
The podocyte, a key cell involved in glomerulosclerosis,
 Podocyte Hypertrophy, Adaptation, and Decompensation Associated with Glomerular Enlargement and Glomerulosclerosis in the Aging Rat: Prevention by Calorie Restriction Jocelyn E. Wiggins,* Meera Goyal,
Podocyte Hypertrophy, Adaptation, and Decompensation Associated with Glomerular Enlargement and Glomerulosclerosis in the Aging Rat: Prevention by Calorie Restriction Jocelyn E. Wiggins,* Meera Goyal,
BRIEF REPORT. N Engl J Med, Vol. 344, No. 26 June 28,
 BRIEF REPORT Brief Report NEPHROPATHY AND ESTABLISHMENT OF A RENAL RESERVOIR OF HIV TYPE 1 DURING PRIMARY INFECTION JONATHAN A. WINSTON, M.D., LESLIE A. BRUGGEMAN, PH.D., MICHAEL D. ROSS, B.S., JEFFREY
BRIEF REPORT Brief Report NEPHROPATHY AND ESTABLISHMENT OF A RENAL RESERVOIR OF HIV TYPE 1 DURING PRIMARY INFECTION JONATHAN A. WINSTON, M.D., LESLIE A. BRUGGEMAN, PH.D., MICHAEL D. ROSS, B.S., JEFFREY
renoprotection therapy goals 208, 209
 Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Eremina V, Jefferson JA, Kowalewska J, et al. VEGF inhibition
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Eremina V, Jefferson JA, Kowalewska J, et al. VEGF inhibition
Idiopathic focal segmental glomerulosclerosis: a favourable prognosis in untreated patients?
 O R I G N A L A R T I C L E Idiopathic focal segmental glomerulosclerosis: a favourable prognosis in untreated patients? J.K.J. Deegens 1* K.J.M. Assmann 2, E.J. Steenbergen 2, L.B. Hilbrands 1, P.G.G.
O R I G N A L A R T I C L E Idiopathic focal segmental glomerulosclerosis: a favourable prognosis in untreated patients? J.K.J. Deegens 1* K.J.M. Assmann 2, E.J. Steenbergen 2, L.B. Hilbrands 1, P.G.G.
Department of Surgery, National Defense Medical Collage, Tokorozawa, Saitama
 Original Contribution Kitasato Med J 2011; 41: 115-122 Injection of rabbit polyclonal antibodies induced by genetic immunization with rat nephrin cdna causes massive proteinuria in the rat: a new model
Original Contribution Kitasato Med J 2011; 41: 115-122 Injection of rabbit polyclonal antibodies induced by genetic immunization with rat nephrin cdna causes massive proteinuria in the rat: a new model
(a) Significant biological processes (upper panel) and disease biomarkers (lower panel)
 Supplementary Figure 1. Functional enrichment analyses of secretomic proteins. (a) Significant biological processes (upper panel) and disease biomarkers (lower panel) 2 involved by hrab37-mediated secretory
Supplementary Figure 1. Functional enrichment analyses of secretomic proteins. (a) Significant biological processes (upper panel) and disease biomarkers (lower panel) 2 involved by hrab37-mediated secretory
Renal Physiology - Lectures
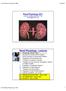 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Online Appendix Material and Methods: Pancreatic RNA isolation and quantitative real-time (q)rt-pcr. Mice were fasted overnight and killed 1 hour (h)
 Online Appendix Material and Methods: Pancreatic RNA isolation and quantitative real-time (q)rt-pcr. Mice were fasted overnight and killed 1 hour (h) after feeding. A small slice (~5-1 mm 3 ) was taken
Online Appendix Material and Methods: Pancreatic RNA isolation and quantitative real-time (q)rt-pcr. Mice were fasted overnight and killed 1 hour (h) after feeding. A small slice (~5-1 mm 3 ) was taken
Glomerular Diseases. Anna Vinnikova, MD Nephrology
 Glomerular Diseases Anna Vinnikova, MD Nephrology Classification of Glomerular Diseases http://what-when-how.com/acp-medicine/glomerular-diseases-part-1/ Classification of pathologic and clinical manifestations
Glomerular Diseases Anna Vinnikova, MD Nephrology Classification of Glomerular Diseases http://what-when-how.com/acp-medicine/glomerular-diseases-part-1/ Classification of pathologic and clinical manifestations
EXPERIMENTAL GLOMERULONEPHRITIS BY ANTI-KIDNEY MITOCHONDRIAL ANTISERUM IN THE RABBIT
 INTRODUCTION OF EXPERIMENTAL GLOMERULONEPHRITIS BY ANTI-KIDNEY MITOCHONDRIAL ANTISERUM IN THE RABBIT A. Z. BARABAS,* B.V.M.&S., M.R.C.V.S., D.V.S.M., M.Sc., Ph.D., A. H. NAGI,* M.B., B.S. R. LANNIGAN,t
INTRODUCTION OF EXPERIMENTAL GLOMERULONEPHRITIS BY ANTI-KIDNEY MITOCHONDRIAL ANTISERUM IN THE RABBIT A. Z. BARABAS,* B.V.M.&S., M.R.C.V.S., D.V.S.M., M.Sc., Ph.D., A. H. NAGI,* M.B., B.S. R. LANNIGAN,t
As outlined under External contributions (see appendix 7.1), the group of Prof. Gröne at the
 3 RESULTS As outlined under External contributions (see appendix 7.1), the group of Prof. Gröne at the DKFZ in Heidelberg (Dept. of Cellular and Molecular pathology) contributed to this work by performing
3 RESULTS As outlined under External contributions (see appendix 7.1), the group of Prof. Gröne at the DKFZ in Heidelberg (Dept. of Cellular and Molecular pathology) contributed to this work by performing
The relationship among nephrin, podocin, CD2AP, and a-actinin might not be a true interaction in podocyte
 http://www.kidney-international.org & 26 International Society of Nephrology original article The relationship among nephrin, podocin,, and a-actinin might not be a true interaction in podocyte Q Fan,2,
http://www.kidney-international.org & 26 International Society of Nephrology original article The relationship among nephrin, podocin,, and a-actinin might not be a true interaction in podocyte Q Fan,2,
RECURRENT AND DE NOVO RENAL DISEASES IN THE ALLOGRAFT. J. H. Helderman,MD,FACP,FAST
 RECURRENT AND DE NOVO RENAL DISEASES IN THE ALLOGRAFT J. H. Helderman,MD,FACP,FAST Vanderbilt University Medical Center Professor of Medicine, Pathology and Immunology Medical Director, Vanderbilt Transplant
RECURRENT AND DE NOVO RENAL DISEASES IN THE ALLOGRAFT J. H. Helderman,MD,FACP,FAST Vanderbilt University Medical Center Professor of Medicine, Pathology and Immunology Medical Director, Vanderbilt Transplant
ACCME/Disclosure. Case #1. Case History. Dr. Bracamonte has nothing to disclose
 Case #1 ACCME/Disclosure Dr. Erika Bracamonte Associate Professor of Pathology University of Arizona, College of Medicine Banner University Medical Center, Tucson Dr. Bracamonte has nothing to disclose
Case #1 ACCME/Disclosure Dr. Erika Bracamonte Associate Professor of Pathology University of Arizona, College of Medicine Banner University Medical Center, Tucson Dr. Bracamonte has nothing to disclose
Dr Ian Roberts Oxford. Oxford Pathology Course 2010 for FRCPath Illustration-Cellular Pathology. Oxford Radcliffe NHS Trust
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Plan of attack: Diagnostic approach to the renal biopsy Differential diagnosis of the clinical syndromes of renal disease Microscopy Step
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Plan of attack: Diagnostic approach to the renal biopsy Differential diagnosis of the clinical syndromes of renal disease Microscopy Step
The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells
 1 SUPPLEMENTARY INFORMATION The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells Karin Loser 1,2,6, Thomas Vogl 2,3, Maik Voskort 1, Aloys
1 SUPPLEMENTARY INFORMATION The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells Karin Loser 1,2,6, Thomas Vogl 2,3, Maik Voskort 1, Aloys
Chapter 6: Idiopathic focal segmental glomerulosclerosis in adults Kidney International Supplements (2012) 2, ; doi: /kisup.2012.
 http://www.kidney-international.org chapter 6 & 2012 KDIGO Chapter 6: Idiopathic focal segmental glomerulosclerosis in adults Kidney International Supplements (2012) 2, 181 185; doi:10.1038/kisup.2012.19
http://www.kidney-international.org chapter 6 & 2012 KDIGO Chapter 6: Idiopathic focal segmental glomerulosclerosis in adults Kidney International Supplements (2012) 2, 181 185; doi:10.1038/kisup.2012.19
Pathology of Complement Mediated Renal Disease
 Pathology of Complement Mediated Renal Disease Mariam Priya Alexander, MD Associate Professor of Pathology GN Symposium Hong Kong Society of Nephrology July 8 th, 2017 2017 MFMER slide-1 The complement
Pathology of Complement Mediated Renal Disease Mariam Priya Alexander, MD Associate Professor of Pathology GN Symposium Hong Kong Society of Nephrology July 8 th, 2017 2017 MFMER slide-1 The complement
Membranoproliferative Glomerulonephritis
 Membranoproliferative Glomerulonephritis MPGN is characterizedby alterations in the GBM and mesangium and by proliferation of glomerular cells. 5% to 10% of cases of 1ry nephrotic syndrome in children
Membranoproliferative Glomerulonephritis MPGN is characterizedby alterations in the GBM and mesangium and by proliferation of glomerular cells. 5% to 10% of cases of 1ry nephrotic syndrome in children
University of Bristol - Explore Bristol Research. Peer reviewed version. Link to published version (if available): 10.
 Prasad, R., Hadjidemetriou, I., Maharaj, A., Meimaridou, E., Buonocore, F., Saleem, M.,... Metherell, L. A. (2017). Sphingosine-1-phosphate lyase mutations cause primary adrenal insufficiency and steroid-resistant
Prasad, R., Hadjidemetriou, I., Maharaj, A., Meimaridou, E., Buonocore, F., Saleem, M.,... Metherell, L. A. (2017). Sphingosine-1-phosphate lyase mutations cause primary adrenal insufficiency and steroid-resistant
Islet viability assay and Glucose Stimulated Insulin Secretion assay RT-PCR and Western Blot
 Islet viability assay and Glucose Stimulated Insulin Secretion assay Islet cell viability was determined by colorimetric (3-(4,5-dimethylthiazol-2-yl)-2,5- diphenyltetrazolium bromide assay using CellTiter
Islet viability assay and Glucose Stimulated Insulin Secretion assay Islet cell viability was determined by colorimetric (3-(4,5-dimethylthiazol-2-yl)-2,5- diphenyltetrazolium bromide assay using CellTiter
Suppl Video: Tumor cells (green) and monocytes (white) are seeded on a confluent endothelial
 Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
Glomerular Aging and Focal Global Glomerulosclerosis: A Podometric Perspective
 Glomerular Aging and Focal Global Glomerulosclerosis: A Podometric Perspective Jeffrey B. Hodgin,* Markus Bitzer, Larysa Wickman, Farsad Afshinnia, Su Q Wang, Christopher O Connor,* Yan Yang, Chrysta Meadowbrooke,
Glomerular Aging and Focal Global Glomerulosclerosis: A Podometric Perspective Jeffrey B. Hodgin,* Markus Bitzer, Larysa Wickman, Farsad Afshinnia, Su Q Wang, Christopher O Connor,* Yan Yang, Chrysta Meadowbrooke,
Focal Segmental Glomerulosclerosis and the Nephro6c Syndrome Dr. A. Gangji Dr. P. Marge>s. Part 1: Clinical
 Focal Segmental Glomerulosclerosis and the Nephro6c Syndrome Dr. A. Gangji Dr. P. Marge>s Part 1: Clinical Pa#ent DM 18 year old McMaster student Back pain, severe fa#gue Oct 2006 Leg swelling to ER Nov
Focal Segmental Glomerulosclerosis and the Nephro6c Syndrome Dr. A. Gangji Dr. P. Marge>s Part 1: Clinical Pa#ent DM 18 year old McMaster student Back pain, severe fa#gue Oct 2006 Leg swelling to ER Nov
Supplemental Figure 1. Quantification of proliferation in thyroid of WT, Ctns -/- and grafted
 Supplemental Figure 1. Quantification of proliferation in thyroid of WT, Ctns -/- and grafted Ctns -/- mice. Cells immunolabeled for the proliferation marker (Ki-67) were counted in sections (n=3 WT, n=4
Supplemental Figure 1. Quantification of proliferation in thyroid of WT, Ctns -/- and grafted Ctns -/- mice. Cells immunolabeled for the proliferation marker (Ki-67) were counted in sections (n=3 WT, n=4
Figure S1. Reduction in glomerular mir-146a levels correlate with progression to higher albuminuria in diabetic patients.
 Supplementary Materials Supplementary Figures Figure S1. Reduction in glomerular mir-146a levels correlate with progression to higher albuminuria in diabetic patients. Figure S2. Expression level of podocyte
Supplementary Materials Supplementary Figures Figure S1. Reduction in glomerular mir-146a levels correlate with progression to higher albuminuria in diabetic patients. Figure S2. Expression level of podocyte
Clinical and pathologic characteristics of focal segmental glomerulosclerosis pathologic variants
 original article http://www.kidney-international.org & 2006 International Society of Nephrology Clinical and pathologic characteristics of focal segmental glomerulosclerosis pathologic variants DB Thomas
original article http://www.kidney-international.org & 2006 International Society of Nephrology Clinical and pathologic characteristics of focal segmental glomerulosclerosis pathologic variants DB Thomas
PRIMARY FOCAL SEGMENTAL GLOMERULOSCLEROSIS: WHY ARE PIECES OF THIS PUZZLE STILL MISSING?
 PRIMARY FOCAL SEGMENTAL GLOMERULOSCLEROSIS: WHY ARE PIECES OF THIS PUZZLE STILL MISSING? *Hernán Trimarchi Nephrology Service, Hospital Británico de Buenos Aires, Buenos Aires, Argentina *Correspondence
PRIMARY FOCAL SEGMENTAL GLOMERULOSCLEROSIS: WHY ARE PIECES OF THIS PUZZLE STILL MISSING? *Hernán Trimarchi Nephrology Service, Hospital Británico de Buenos Aires, Buenos Aires, Argentina *Correspondence
