Everyday Practice. Eye trauma: Primary care for general physicians
|
|
|
- Virgil Underwood
- 5 years ago
- Views:
Transcription
1 VOL.. 15, NO.2, Everyday Practice Eye trauma: Primary care for general physicians H. K. TEWARI, ATUL KUMAR, GUNJAN PRAKASH INTRODUCTION The understanding of ocular trauma is important for the primary care physician. Whether based in an emergency room or a private office, a general physician will frequently encounter ocular injuries. Men are affected approximately nine times more often than women, and most victims are under 40 years of age. 1 The visual prognosis for eyes with major injuries has improved in the past two decades. 2The different modalities of injury are enumerated in Table I, while Table II lists the causes of ocular trauma in children in India in descending order of frequency (our experience). Unprotected sport is one of the common causes of eye trauma. The different sports commonly responsible for blunt as well as penetrating injury are listed in Table III. Evaluation of patients with suspected ocular trauma starts with a detailed history. 3 The examiner should have an understanding of the potential severity of the injury. Was a foreign body involved? (Any hole in the iris, not the pupil itself, is a pointer towards intraocular foreign body.) Are potential orbital fractures likely? Were chemicals used? Is a ruptured globe possible? It is critical to determine whether any life-threatening systemic injury has occurred concurrently; such injury should take precedence over the management of the ocular injury. GENERAL OCULAR EVALUATION A complete bilateral ocular examination is necessary in all cases of eye trauma, not only for treatment but also for medicolegal documentation. We have provided an algorithm to help general physicians gain confidence in providing primary care to ocular trauma victims as well as to help guide them as to when to refer the patient to a secondary-level hospital with ophthalmological expertise. For the primary care doctor the physical examination should include the face and lids, conjunctiva, pupils, evaluation of extraocular motility, anterior segment and the fundus. The three areas that provide the most valuable information are the pupil, visual acuity and red reflex (Table IV). If the vision is normal, the injury is likely to be mild or nonthreatening. The vision can be tested with the standard Snellen acuity chart in the office or with the help of a near card. If this is not available, the ability to read a newspaper puts the vision at about 20/50. The red reflex of a distant direct ophthalmoscopy (Fig. la) evaluates the ocular media. An abnormal red reflex is a good screening tool (Fig. 1b).It indicates that something is wrong with the media of the eye, but it will not localize the defect. All India Institute of Medical Sciences, New Delhi , India H. K. TEW ARI, ATUL KUMAR, GUNJAN PRAKASH Dr R.P. Centre for Ophthalmic Sciences Correspondence to A TUL KUMAR; akum66mm@ndfvsnl.net.in The National Medical Journal of India 2002 In evaluating the pupils, one should look for symmetry. Isolated blunt trauma to the globe with an irregular pupil indicates a tear of the sphincter muscle. A peaked pupil is a cause for worry as it may be associated with a globe perforation with iris prolapse into the wound. An afferent pupil defect is associated with optic nerve injury. ORBITAL FRACTURES Patients with a recent history of orbital trauma may complain of pain on attempting vertical eye movements, tenderness localized to a point at the infraorbital rim, binocular diplopia, or lid swelling, particularly after nose blowing. If the orbital floor is fractured, these patients frequently have diplopia that is worse on looking up, as the inferior rectus is trapped within the fracture site. Signs include ecchymosis and oedema of the eyelids (Fig. 1c), orbital subcutaneous or subconjunctival emphysema, hypoaesthesia in the distribution of the ipsilateral infraorbital nerve, enophthalmos and ptosis of the globe. Areas of a step-off fracture or discontinuity should be palpated for. A neurological evaluation is indicated if there is a history ofloss of consciousness. If a blowout fracture is present, the patient should be referred to an ophthalmologist. TABLEI. Ocular injuries (based on nature of work) Children at play Road traffic accident Industrial accident Civil disturbance Home accident Assault Adult sport Farm accident TABLEII. Common causes of ocular injuries in Indian children Sharp instrument Finger nail Road traffic accident Bow and arrow Animals Chemicals Gulli-danda Domestic TABLEIII. Sports causing ocular injuries Boxing/wrestling Badminton Squash Racing Cricket Archery Golf TABLEIV. Checklist for evaluation of ocular injury by a general physician I. Recognition of associated life-threatening injuries 2. Emergent eye conditions=-chemical injury and central retinal artery occlusion (require urgent management) 3. Concurrent medical illness such as diabetes, etc. 4. Eyelid and adnexal injury 5. Visual acuity (best corrected for both far and near) of the involved as well as uninvolved eye 6. Pupil: whether equal to that of the fellow eye, round, regular, reacting to light 7. Pupillary reactions: both direct and consensual 8. Anterior segment: torch-light examination of the cornea, conjunctiva and sclera 9. Anterior chamber: depth and regularity 10. Red reflex (posterior segment glow) with a direct ophthalmoscope
2 86 VOL. 15, NO.2, 2002 FIG1. (a) Illustration of distant direct ophthalmoscopy being performed at approximately 30 em. (b) Normal red reflex except for a small opacity due to cataract as pointed by the yellow arrow. (c) Lid laceration (arrow) with blow-out fracture. (d) Untreated post-traumatic endophthalmitis, poor visual prognosis ENDOPHTHALMITIS Traumatic endophthalmitis (infection ofthe vitreous) is characterized by a hypopyon with gray reflex on direct ophthalmoscopy. It should be diagnosed early and initial treatment with topical concentrated cefazolin (5%) and concentrated tobramycin (1.3%), one drop every 30 minutes, should be started along with intravenous antibiotics. The definitive treatment is intravitreal antibiotics (vancomycin 1 mg in 0.1 ml and ceftazidime 2.25 mg in 0.1 ml) and can be undertaken with due antiseptic precautions by an ophthalmologist. Therefore, when endophthalmitis is suspected, the patient must be referred to an ophthalmologist. This is crucial; done in time it can save the eye. Without treatment the eye will have an appearance as shown in Fig. 1d, when even vitrectomy (last resort) is not possible and evisceration might have to be carried out to relieve the patient's pain. TRAUMATIC HYPHAEMA Traumatic hyphaema (blood in the anterior chamber) can lead to devastating ocular complications (Fig. 2a). Patients may present with blurred vision, pain, photophobia and tearing following blunt, concussive injury to the eye or orbit. Circumstances surrounding the event, current medicines and previous ocular history are important pieces of data. Bleeding in the eye warrants eliciting a history of systemic blood disorders such as sickle cell anaemia, haemophilia and von Willebrand's disease. Ideally, every patient should be examined with a slit-lamp, but this may be impossible in a private office or in primary health centres. If a slit-lamp is not available, a penlight or an ophthalmoscope light can be used. To visualize the anterior chamber, tangential light is the most helpful. The patient should be given cycloplegics such as 1% atropine ointment thrice a day and topical steroids. If the intraocular pressure is 27 mmhg, it should be controlled using topical betablockers twice daily. When the intraocular pressure is very high (>35 mmhg), oral acetazolamide 500 mg twice daily should be prescribed and the patient referred to a specialized centre. To prevent re-bleeding, pain should be relieved only with acetaminophen; aspirin and ibuprofen should be avoided. CORNEAL ABRASION A primary care physician can easily evaluate the cornea. This begins with inspection of the corneal epithelium. Trauma that disrupts the corneal epithelium is painful and the patient is uncomfortable. To detect an abrasion, a fluorescein strip is gently placed on the bulbar conjunctiva or that of the lower lid (Table V and Fig. 2b). If the strip is touched to the cornea, the fluorescein could be concentrated at the touched site and could falsely signal an abrasion. TABLE V. Superficial corneal abrasions Steps of management Refer immediately if... Anaesthetize the eye with topical agent Test vision when pain and tearing have abated Retract lower lid, and touch the end of a dry fluorescein sodium strip to the lower cul-de-sac Have the patient blink to distribute fluorescein evenly Inspect the cornea with cobalt blue light incorporated into the direct ophthalmoscope Continue topical antibiotic prophylaxis once or twice a day until the abrasion heals Apply a drop of homatropine 2% eye drops, then apply a bland antibiotic ophthalmic ointment Prescribe topical non-steroidal antiinflammatory agent, four times daily, for pain Record size and location on every follow up visit Pain incompletely relieved with topical anaesthetic The patient has decreased vision A corneal opacity is present or develops Reliable fluorescein strip is not available Cobalt blue light is not available to rule out corneal epithelial abrasion Abrasion involving more than twothirds of the total corneal area Pain not relieved within 6 hours of applying the cycloplegic eye drops Size of abrasion has not decreased to less than half within 24 hours Abrasion has not healed completely within 72 hours Re-examine daily until fluorescein staining completely resolves
3 TEWARI et al.: EYE TRAUMA: PRIMARY CARE 87 FIG2. (a) Post-traumatic hyphaema (b) Technique of inserting fluorescein stain in the eye with a fluorescein strip. (c) Sodium fluorescein staining the corneal abrasion as the stroma is exposed due to loss of overlying epithelium. (d) Full-thickness corneal laceration with a flat anterior chamber. Do not check ocular movements or intraocular pressure If the epithelium is damaged, the fluorescein will adhere to the basement membrane and when cobalt blue light (usually present in the direct ophthalmoscope) is used, it will fluoresce brightly, confirming the presence of an abrasion (Fig. 2c). Once an abrasion is detected, laceration of the corneal stroma should be ruled out. If a laceration is suspected, a referral is necessary. A patient with corneal abrasion is treated with antibiotic drops or ointment four times a day till the abrasion heals. An initial 24hour patch with an antibiotic-steroid eye ointment is highly recommended. Thereafter, a patch is used if the patient feels less pain with the eye covered. A corneal abrasion needs to be followed up daily to look for signs of infection. If there is no improvement after 48 hours, the patient should be referred. The vision and the size of the abrasion should always be documented during the initial examination and at all follow up examinations. Worsening of vision may indicate a corneal infection and the patient should be referred. CORNEAL LACERATION In a patient with a corneal laceration (Fig. 2d) there is intense pain initially which may diminish slightly due to corneal desensitization. Patients have photophobia and profuse lacrimation. There is marked associated uveitis and the anterior chamber is shallow or even flat in a full-thickness laceration." Visual acuity is substantially reduced. The diagnosis of corneal laceration must be made early and with as little intervention as possible. Measurement of the intraocular pressure should be avoided in any patient suspected to have a full-thickness laceration, as any pressure applied to the globe may cause uveal tissue to extrude through the wound. Unnecessary manipulation of an eye with a full-thickness laceration should be avoided. An eye shield is used to protect the eye. The laceration should be surgically repaired by a corneal specialist at the earliest. The patient should be warned that the initial visual acuity may represent the best vision that can be expected after surgical repair. Although vision may improve after surgical repair, it is best not to raise a patient's expectations. CORNEAL FOREIGN BODY Patients who have a foreign body on the cornea generally present with pain. Excessive tearing, blurred vision and photophobia are also common. The most critical sign is the finding of particulate matter at the surface of, or embedded within, the cornea (Fig. 3a). Ensure that the object has not perforated the cornea. If no penetration has taken place, the object should be removed under topical anaesthesia (1-2 drops of 0.5% proparacaine). A direct stream of sterile irrigating solution may be sufficient to dislodge some small foreign bodies. If irrigation does not help, consider thatthe foreign body is likely to be embedded. The instrument of choice in this case is a spud (Figs 3b and c) that allows the foreign body to be excavated and flicked off from the surface. If this is also unsuccessful, refer the patient to a secondary-level hospital where it can be removed under slit-lamp illumination and magnification. When a corneal foreign body is in the line of the visual axis, patients should be counselled about the possible loss of visual acuity due to unavoidable scarring; this should be well documented to avoid clinicolegal ramifications. The patient should also be counselled about the possibility of a scar remaining on the cornea that might be cosmetically bothersome. A conjunctival foreign body can be removed in a similar way, or by using a pair offorceps or a cotton-tipped applicator (Fig. 3d). If a general physician is unable to rule out the possibility of a penetrating ocular injury, a shield should be applied to the affected eye (without any topical medication) and the patient referred immediately to an ophthalmologist. EYELID TRAUMA While evaluating the lids one should consider damage to the globe. Are there puncture wounds? Are there lacerations (Fig. 4a)? If there are lacerations, are they full-thickness or partial? Do they include the lid margin? A laceration involving the lid margin needs to be referred to an ophthalmologist because simple repair will leave a lid notch that will be cosmetically unacceptable. One must also suspect canalicular involvement if the lacerations are at the medial aspect of the
4 88 VOL. 15, NO. 2,2002 FIG3. (a) Corneal foreign body with surrounding iron rusting as indicated by red arrow. (b) Illustration of the technique to remove a corneal foreign body with a spud. (c) A foreign body can be removed with the naked eye with adequate illumination. (d) Foreign body over the upper palpebral conjunctiva being removed with a cotton bud lids. Frequently, the internal aspect of an external wound can be extensive and involve the canalicular system. Blunt trauma or contusion (Fig. 4b) to the eyelids is a nonpenetrating injury by an external force that does not break or lacerate the epidermis or dermis. Care should be taken to ensure that the globe has not been ruptured. Ten-minute ice compresses applied every 2 hours can reduce post-traumatic oedema if applied within the first two days of injury. CHEMICAL BURNS The substance, its concentration, and the duration of contact determine the severity of chemical burns of the eyelids. Acid burns are usually self-limiting and not as destructive as alkali burns. An accurate history is necessary to determine the time of injury, the nature of the chemical and the duration of exposure before irrigation. However, no time should be wasted on eye examinationtreatment should be started first, as this can save the eye. Emergent treatment includes copious irrigation of the eyelids, preferably with saline or Ringer's lactate solution for at least 30 minutes. If neither of these is available, non-sterile water should be used. Cool milk can also be used in case of emergencies. Chemical burn is one of the few conditions of the eye in which, if the treatment is started early enough, the prognosis is good. The lower and upper fornices should be irrigated. Manual use of intravenous tubing connected to an irrigation solution facilitates the irrigation process. Five minutes after ceasing irrigation, litmus paper should be touched to the inferior fornix. If the ph is not neutral (ph=7), irrigation should be continued. FIG4. (a) Lid laceration over the upper temporal part of the eyelid. (b) Blunt trauma leading to peri-orbital ecchymosis. (c) Small subconjunctival haemorrhage with less possibility of globe rupture. (d) Large subconjunctival haemorrhage with high possibility of globe rupture
5 TEWARI et al.: EYE TRAUMA: PRIMARY CARE After irrigation, the fornices should be further examined, and any sequestered particles of caustic material and necrotic conjunctiva should be removed. The periocular skin should be cleaned. Contaminated clothes of the patient should be removed to prevent further damage. Therapy for uveitis (e.g. 1% atropine ointment thrice daily) along with topical antibiotic ointments (e.g. ciprofloxacin four times a day) and oral ocular hypotensive medication (e.g. acetazolamide) as well as oral pain medication should be used as needed. SUBCONJUNCTIVAL HAEMORRHAGE Subconjunctival haemorrhage is usually benign and self-limiting (Fig. 4c). No treatment is required. The conjunctiva should be inspected for evidence of foreign bodies. The upper lid should be everted and injuries looked for. If there is a laceration of the conjunctiva, a possible globe injury should be suspected. The sclera is a resilient structure and commonly spared in a conjunctival laceration. However, globe rupture (Fig. 4d) is a possibility and appropriate signs and symptoms as already described should be looked for. POSTERIOR SEGMENT TRAUMA For the primary care physician, the most important structures to examine are the optic nerve and the macula. These can be visualized by a direct ophthalmoscope. The view of the optic nerve can determine if papilloedema is present, which is important, especially in cases of head injury. Trauma can cause a retinal tear. If this is not detected, vitreous fluid can enter the retinal tear and detach the retina. If a retinal tear is detected, treatment can prevent a retinal detachment. Blood in the vitreous should make one suspect a retinal tear. The best way to view the retina is by indirect ophthalmoscopy. If needed, the patient should be referred. PRECAUTIONS The general physician should know when to stop. He should do no further harm to the injury by doing more than required. Moreover, an overenthusiastic physician might land up in trouble himself, in this era of consumerism. A useful guide of dos and don'ts is provided in Table VI. CONCLUSION Most of the visual disability resulting from trauma can be prevented by protective eyewear. A brief review is therefore mandatory. Any eyewear designed for protection should have good optical quality, be light in weight, comfortable, durable, easy to maintain, non-flammable, non-irritant, cosmetically acceptable and compatible with other protective devices. Polycarbonate lenses are recommended for all children, functionally one-eyed people and active adults. For sports that have a potential for eye contact with a ball, 3 mm thick polycarbonate lenses should be used. A helmet with a face shield over the safety glasses should be used in unsafe areas such as factories, etc. Glass lenses, ordinary plastic lenses, open eye guards and contact lenses do not give adequate eye protection. Ocular trauma is so common that a general practitioner encounters it frequently. Given that it can be successfully treated TABLE Orbital fracture Endophthalmitis Hyphaema VI. List of dos and don'ts for a general physician Do Refer Start topical antibiotics Startcycloplegics and Don't Corneal laceration Corneal foreign body refer Corneal abrasion Patch, if no contraindi- Hesitate to refer cation Referirnmediately Remove, if no perforation Eyelid trauma Evaluate for globellid margin/canalicular involvement Intervene Ignore Prescribe aspirin, etc. Manipulate the globe Intervene, iffullthickness corneal involvement 89 Repair, if any of these is present Chemical burns Copious irrigation with Wait for history or Ringer's solution evaluation Subconjunctival haemorrhage Inspectforoccultglobe Try to drain the rupture, visual acuity, haemorrhage foreign bodies Posterior segment trauma Referimmediately Try to intervene Assessment ( Pupillary reflex j of a patient with ocular trauma ( Ocular trauma Photographic documentation ). L-..., ( Visual acuity of both eyes) ( Direct ophthalmoscopy '-----'----'---'r-~---. ( History ) ( Blunt injury) ( Motility ( Bony defect) ( Enophthalmos) ( Diplopia) ( Skin sensation) I (Penetrating ( Cornea injury ( Bulparconjunctiva) Depth, regularity of } [ anterior chamber ( Anterior segment) Suspect intraocular 1 [ foreign body with good visual prognosis, close cooperation is essential to improve care delivery. An algorithmic outline (box), for assessing a patient with ocular trauma in a primary care setting would be useful. While much of the management must take place in a specialist hospital, it is hoped that screening along with primary care can be undertaken at the level of the general practitioner. This can only be properly achieved, however, if primary care providers are comfortable in interpreting the relevant signs and symptoms and coordinating the subsequent management. REFERENCES I Katz J, Tielsch JM. Lifetime prevalence of ocular injuries from Baltimore Eye Survey. Arch OphthalmoI1993;111: EsmaeJi B, Elner SG, Schork A, Elner VM. Visual outcome and ocular survival after penetrating trauma. Ophthalmology 1995;102: MacCumber MW. Management of ocular injuries and emergencies, Philadelphia: Lippincott-Raven, Cherry PMH. Rupture of the globe. Arch OphthalmoI1966;76:678.
Ocular and periocular trauma
 Ocular and periocular trauma No financial disclosures. Tina Rutar M.D. Assistant Professor of Clinical Ophthalmology and Pediatrics Director, Visual Center for the Child University of California San Francisco
Ocular and periocular trauma No financial disclosures. Tina Rutar M.D. Assistant Professor of Clinical Ophthalmology and Pediatrics Director, Visual Center for the Child University of California San Francisco
Ocular and Periocular Trauma. Tina Rutar, MD. Assistant Professor of Ophthalmology and Pediatrics. Director, Visual Center for the Child
 Ocular and Periocular Trauma Tina Rutar, MD Assistant Professor of Ophthalmology and Pediatrics Director, Visual Center for the Child University of California, San Francisco Phone: 415-353-2560 Fax: 415-353-2468
Ocular and Periocular Trauma Tina Rutar, MD Assistant Professor of Ophthalmology and Pediatrics Director, Visual Center for the Child University of California, San Francisco Phone: 415-353-2560 Fax: 415-353-2468
Assessment and Management of Ocular Trauma. Disclosure I have no direct financial interests in today s subject matter. 3/25/2019. Normal Eye Anatomy
 Assessment and Management of Ocular Trauma Samiksha Fouzdar Jain, MD,FRCS Department of Ophthalmology & Visual Sciences Truhlsen Eye Institute Disclosure I have no direct financial interests in today s
Assessment and Management of Ocular Trauma Samiksha Fouzdar Jain, MD,FRCS Department of Ophthalmology & Visual Sciences Truhlsen Eye Institute Disclosure I have no direct financial interests in today s
EYE TRAUMA: INCIDENCE
 Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Eye Trauma. Lid Laceration. Orbital Fracture
 Eye Trauma Lid Laceration The presence of a lid laceration, however insignificant, mandates careful exploration of the wound and examination of the globe. 1. Superficial lacerations parallel to the lid
Eye Trauma Lid Laceration The presence of a lid laceration, however insignificant, mandates careful exploration of the wound and examination of the globe. 1. Superficial lacerations parallel to the lid
Management of specific eye problems in the ED
 of specific eye problems in the ED CORNEAL ABRASION Causes Foreign bodies Tangential shearing injuries, e.g. poking finger into eye Exact cause of injury (Remember to exclude possibility of intraocular
of specific eye problems in the ED CORNEAL ABRASION Causes Foreign bodies Tangential shearing injuries, e.g. poking finger into eye Exact cause of injury (Remember to exclude possibility of intraocular
UC SF. g h. Eye Trauma. Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California
 UC SF Eye Trauma sf g h Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California Goals Recognize vision threatening eye emergencies Treat them when we can Know when
UC SF Eye Trauma sf g h Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California Goals Recognize vision threatening eye emergencies Treat them when we can Know when
Acute Eyes for ED. Enis Kocak. The Alfred Ophthalmology
 Acute Eyes for ED Enis Kocak The Alfred Ophthalmology The problem with eyes Things to cover Ocular anatomy Basic assessment Common presentations Eye first aid and procedures Ophthalmic emergencies What
Acute Eyes for ED Enis Kocak The Alfred Ophthalmology The problem with eyes Things to cover Ocular anatomy Basic assessment Common presentations Eye first aid and procedures Ophthalmic emergencies What
Ocular Urgencies and Emergencies
 Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
EYE INJURIES OBJECTIVES COMMON EYE EMERGENCIES 7/19/2017 IMPROVE ASSESSMENT OF EYE INJURIES
 EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
Ophthalmic Trauma Update
 Ophthalmic Trauma Update Richard S. Davidson, M.D. Professor of Ophthalmology Vice Chair for Quality and Clinical Affairs UCHealth Eye Center University of Colorado School of Medicine August 5, 2017 Financial
Ophthalmic Trauma Update Richard S. Davidson, M.D. Professor of Ophthalmology Vice Chair for Quality and Clinical Affairs UCHealth Eye Center University of Colorado School of Medicine August 5, 2017 Financial
MRI masterfile Part 5 WM Heme Strokes.ppt 1
 Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
PEDIATRIC OCULAR INJURIES. Sapna Tibrewal MD
 PEDIATRIC OCULAR INJURIES Sapna Tibrewal MD 1 Learning Objectives Learn to recognize the common pediatric ocular injuries Immediate management tips to be instituted in your office/ ER Know when to call
PEDIATRIC OCULAR INJURIES Sapna Tibrewal MD 1 Learning Objectives Learn to recognize the common pediatric ocular injuries Immediate management tips to be instituted in your office/ ER Know when to call
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS
 OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
Ocular Emergencies. What is an emergency to the patient is not necessarily an emergency to the staff
 OCULAR EMERGENCIES Ophthalmic Photographers Society November 15, 2013 Michael A. DellaVecchia MD PhD FACS Wills Eye Emergency Department Philadelphia PA Ocular Emergencies What is an emergency to the patient
OCULAR EMERGENCIES Ophthalmic Photographers Society November 15, 2013 Michael A. DellaVecchia MD PhD FACS Wills Eye Emergency Department Philadelphia PA Ocular Emergencies What is an emergency to the patient
Examining Children s Eyes
 Paediatric Ophthalmology What to refer & when? Aims Tips for assessing a child s eyes in general practice Common paediatric ophthalmology symptoms and signs What needs to be referred and when? MISS FARIHA
Paediatric Ophthalmology What to refer & when? Aims Tips for assessing a child s eyes in general practice Common paediatric ophthalmology symptoms and signs What needs to be referred and when? MISS FARIHA
2/5/2018. Trauma. Subdivided into two main categories: Closed globe Open Globe
 1 2 3 4 5 Ocular Trauma Guide for Eye Care Office Staff Winter Thaw 2018 Aaron Yatskevich OD Definition A broad term used to describe a physical or chemical wound to the eye or eye socket. Ocular trauma
1 2 3 4 5 Ocular Trauma Guide for Eye Care Office Staff Winter Thaw 2018 Aaron Yatskevich OD Definition A broad term used to describe a physical or chemical wound to the eye or eye socket. Ocular trauma
MRI masterfile Part 5 WM Heme Strokes.ppt 2
 Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
Ocular Injuries in Sports. Rance McClain, D.O. Associate Dean, Clinical Sciences William Carey University FM/NMM-OMM/Sports Medicine
 Ocular Injuries in Sports Rance McClain, D.O. Associate Dean, Clinical Sciences William Carey University FM/NMM-OMM/Sports Medicine http://sudc.org/vienna/ Learning Objectives 1. Know the sport classification
Ocular Injuries in Sports Rance McClain, D.O. Associate Dean, Clinical Sciences William Carey University FM/NMM-OMM/Sports Medicine http://sudc.org/vienna/ Learning Objectives 1. Know the sport classification
ation is essential. Whether on the playing it is important to keep in mind that severe
 JENNIFER LAIO, MD, and BRUCE M. ZAGELBAUM, MD NYU School of Medicine, Manhasset, NY North Shore University Hospital, Eye injuries sustained in sports and recreational activities are common in the United
JENNIFER LAIO, MD, and BRUCE M. ZAGELBAUM, MD NYU School of Medicine, Manhasset, NY North Shore University Hospital, Eye injuries sustained in sports and recreational activities are common in the United
Injury. Contusion Lamellar Laceration Laceration Rupture. Penetrating IOFB. Perforating
 Mechanical Ocular Trauma Došková Hana, MD. Department of Ophthalmology Medicine Faculty of Masaryk University Brno General Considerations Ocular trauma constitude about 6% of all injuries, but eyes set
Mechanical Ocular Trauma Došková Hana, MD. Department of Ophthalmology Medicine Faculty of Masaryk University Brno General Considerations Ocular trauma constitude about 6% of all injuries, but eyes set
Ophthalmology. Corneal Abrasion. History
 Ophthalmology Corneal Abrasion - Usually clear history of very recent trauma - Foreign Body Sensation - Pain +++ - Lacrimation - Photophobia Fig. 1 Corneal Abrasion - Abrasion stains yellow / green with
Ophthalmology Corneal Abrasion - Usually clear history of very recent trauma - Foreign Body Sensation - Pain +++ - Lacrimation - Photophobia Fig. 1 Corneal Abrasion - Abrasion stains yellow / green with
Ocular Trauma. Breaking Down Blunt. Blunt ocular trauma occurs frequently in sporting
 Focus on CME at the University of Saskatchewan Breaking Down Blunt Ocular Trauma By Dan Ash, MD, BA, FRCSC, FACS, FAAO Blunt ocular trauma occurs frequently in sporting activities, as well as in industrial
Focus on CME at the University of Saskatchewan Breaking Down Blunt Ocular Trauma By Dan Ash, MD, BA, FRCSC, FACS, FAAO Blunt ocular trauma occurs frequently in sporting activities, as well as in industrial
Focusing on A&E. By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel
 Focusing on A&E By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel 01752 439331 Email sandra.cooper5@nhs.net sandracooper041@btinternet.com THINGS TO WORRY ABOUT WITH ANY EYE PROBLEM CHANGES IN VISION
Focusing on A&E By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel 01752 439331 Email sandra.cooper5@nhs.net sandracooper041@btinternet.com THINGS TO WORRY ABOUT WITH ANY EYE PROBLEM CHANGES IN VISION
THE 35 GOLDEN EYE RULES
 THE 35 GOLDEN EYE RULES The Sense of Sight, from La Dame a la Licorne, The Lady and the Unicorn Tapestries, Late 15th Century Flemish Tapestry in wool and silk, Musée Nationale du Moyen Age, Paris. 1.
THE 35 GOLDEN EYE RULES The Sense of Sight, from La Dame a la Licorne, The Lady and the Unicorn Tapestries, Late 15th Century Flemish Tapestry in wool and silk, Musée Nationale du Moyen Age, Paris. 1.
Sepideh Tara Rousta, MD FAAO Robert Wood Johnson University Hospital Saint Peter s University Hospital Wills Eye Hospital
 Sepideh Tara Rousta, MD FAAO Robert Wood Johnson University Hospital Saint Peter s University Hospital Wills Eye Hospital 14 mo old w R eye cross (parents) 9 mo old R eye crossing getting worse for past
Sepideh Tara Rousta, MD FAAO Robert Wood Johnson University Hospital Saint Peter s University Hospital Wills Eye Hospital 14 mo old w R eye cross (parents) 9 mo old R eye crossing getting worse for past
5/2/2016 EYE EMERGENCIES. Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates. Anatomy. Tools
 EYE EMERGENCIES Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates Anatomy Tools 1 Contact dermatitis Blepharitis HSV Preseptal Cellulitis Anterior Chamber Subconjunctival hemorrhage
EYE EMERGENCIES Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates Anatomy Tools 1 Contact dermatitis Blepharitis HSV Preseptal Cellulitis Anterior Chamber Subconjunctival hemorrhage
CORNEAL CONDITIONS CORNEAL TRANSPLANTATION
 GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
PENETRATING EYE INJUIRES
 PENETRATING EYE INJUIRES King Harold receives a mortal penetrating injury to the eye at the Battle of Hastings 1066, Detail Bayeux Tapestry, Eleventh century. Then Earl William came from Normandy into
PENETRATING EYE INJUIRES King Harold receives a mortal penetrating injury to the eye at the Battle of Hastings 1066, Detail Bayeux Tapestry, Eleventh century. Then Earl William came from Normandy into
Paediatric acute ophthalmology. Harry Bradshaw
 Paediatric acute ophthalmology Harry Bradshaw Approach Red eye Leukocoria Neurological Trauma Visual loss Red eye Orbital Eyelid Conjunctiva Cornea Uvea Orbital Orbit fixed volume Contiguous with sinuses,
Paediatric acute ophthalmology Harry Bradshaw Approach Red eye Leukocoria Neurological Trauma Visual loss Red eye Orbital Eyelid Conjunctiva Cornea Uvea Orbital Orbit fixed volume Contiguous with sinuses,
Clues of a Ruptured Globe
 Definition any eye that has sustained a full thickness traumatic disruption of the cornea or sclera Overwhelmingly, rupture accidents occur in young men, small children and the elderly Corneal laceration
Definition any eye that has sustained a full thickness traumatic disruption of the cornea or sclera Overwhelmingly, rupture accidents occur in young men, small children and the elderly Corneal laceration
Ears. Mouth. Jowls 6 Major Bones of the Face Nasal bone Two
 1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
Ocular Trauma. Authors Dr Shrinkhal 1, Dr Kamya Sharma 2
 International Journal of Emerging Trends in Science and Technology IC Value: 76.89 (Index Copernicus) Impact Factor: 2.838 DOI: https://dx.doi.org/10.18535/ijetst/v3i12.01 Ocular Trauma Authors Dr Shrinkhal
International Journal of Emerging Trends in Science and Technology IC Value: 76.89 (Index Copernicus) Impact Factor: 2.838 DOI: https://dx.doi.org/10.18535/ijetst/v3i12.01 Ocular Trauma Authors Dr Shrinkhal
For further reading we recommend the following excellent textbooks:
 FURTHER READING Intravitreal Injections Downloaded from www.worldscientific.com For further reading we recommend the following excellent textbooks: Clinical Anatomy of the Eye by Richard S Snell and Michael
FURTHER READING Intravitreal Injections Downloaded from www.worldscientific.com For further reading we recommend the following excellent textbooks: Clinical Anatomy of the Eye by Richard S Snell and Michael
Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
SILA THONGLAI MD. Bangkok Eye center Bangkok Hospital Thailand
 SILA THONGLAI MD. Bangkok Eye center Bangkok Hospital Thailand Ocular Anatomy Bony Components of Orbit 1 1. Frontal bone 4 5 7 6 2. Zygomatic bone 3. Maxillary bone 4. Sphenoid bone 5. Ethmoid bone 2 3
SILA THONGLAI MD. Bangkok Eye center Bangkok Hospital Thailand Ocular Anatomy Bony Components of Orbit 1 1. Frontal bone 4 5 7 6 2. Zygomatic bone 3. Maxillary bone 4. Sphenoid bone 5. Ethmoid bone 2 3
Dr Jo-Anne Pon. Dr Sean Every. 8:30-9:25 WS #70: Eye Essentials for GPs 9:35-10:30 WS #80: Eye Essentials for GPs (Repeated)
 Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
DEFINITION Corneal abrasion is a defect in the corneal surface epithelium due to scraping or rubbing of the corneal epithelium.
 DEFINITION Corneal abrasion is a defect in the corneal surface epithelium due to scraping or rubbing of the corneal epithelium. IMMEDIATE CONSULTATION REQUIRED IN THE FOLLOWING SITUATIONS Dendritic pattern
DEFINITION Corneal abrasion is a defect in the corneal surface epithelium due to scraping or rubbing of the corneal epithelium. IMMEDIATE CONSULTATION REQUIRED IN THE FOLLOWING SITUATIONS Dendritic pattern
Frequently Asked Questions about General Ophthalmology:
 1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
Ocular trauma. Abstract. Introduction. Approach to the patient. CPD Article: Ocular trauma
 Ocular trauma Abstract Mustak H, MBChB, DipOphth(SA), Registrar Division of Ophthalmology, Groote Schuur Hospital; University of Cape Town Du Toit N, MBChB, DipOphth(SA), FRCS(Ed), FCOphth(SA), MMed, Consultant
Ocular trauma Abstract Mustak H, MBChB, DipOphth(SA), Registrar Division of Ophthalmology, Groote Schuur Hospital; University of Cape Town Du Toit N, MBChB, DipOphth(SA), FRCS(Ed), FCOphth(SA), MMed, Consultant
Maxillofacial and Ocular Injuries
 Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
MANAGEMENT OF CONTUSION INJURY OF THE EYE A CLINICAL STUDY
 MANAGEMENT OF CONTUSION INJURY OF THE EYE A CLINICAL STUDY *Gururaj Veeranna Wali and Pranesh Kulkarni Department of Ophthalmology, KBIMS Gulbarga, Karnataka, India *Author for Correspondence ABSTRACT
MANAGEMENT OF CONTUSION INJURY OF THE EYE A CLINICAL STUDY *Gururaj Veeranna Wali and Pranesh Kulkarni Department of Ophthalmology, KBIMS Gulbarga, Karnataka, India *Author for Correspondence ABSTRACT
SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM
 Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM FML Liquifilm Sterile Eye Suspension COMPOSITION FML Liquifilm Sterile Eye Suspension contains: Fluorometholone 1,0 mg/ml Liquifilm
Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM FML Liquifilm Sterile Eye Suspension COMPOSITION FML Liquifilm Sterile Eye Suspension contains: Fluorometholone 1,0 mg/ml Liquifilm
PRODUCTION ANIMAL AND EQUINE OPHTHALMOLOGY
 REF. NO. TITLE: C-VO.2 PRODUCTION ANIMAL AND EQUINE OPHTHALMOLOGY VALUE: 10 CREDITS NOTIONAL STUDY HOURS: 100 This module is intended to cover the theoretical knowledge of both Production Animal and Equine
REF. NO. TITLE: C-VO.2 PRODUCTION ANIMAL AND EQUINE OPHTHALMOLOGY VALUE: 10 CREDITS NOTIONAL STUDY HOURS: 100 This module is intended to cover the theoretical knowledge of both Production Animal and Equine
Eyes, ears, teeth and everything in between
 Eyes, ears, teeth and everything in between E M E R G E N C Y D E P A R T M E N T J U N I O R T E A C H created 14/11/10 by S.R. Bruijns, version 1.0 Objectives Eyes Ears Teeth Maxilla- facial EYES Approaching
Eyes, ears, teeth and everything in between E M E R G E N C Y D E P A R T M E N T J U N I O R T E A C H created 14/11/10 by S.R. Bruijns, version 1.0 Objectives Eyes Ears Teeth Maxilla- facial EYES Approaching
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
By Darlene Jones, Nurse. May 2017
 By Darlene Jones, Nurse May 2017 Disclosure of potential conflict of interest Darlene Jones, Nurse I have no conflict of interest Course objectives Become familiar with the different pathologies in ophthalmology
By Darlene Jones, Nurse May 2017 Disclosure of potential conflict of interest Darlene Jones, Nurse I have no conflict of interest Course objectives Become familiar with the different pathologies in ophthalmology
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
Conjunctival Hemorrhage
 IN THE NAME OF GOD Lid Laceration Conjunctival Hemorrhage a) No therapy is necessary b) Usually resolve in 7-12 days. Subconjunctival Hemorrhage Corneal Abrasion Abrasions Many small abrasions can
IN THE NAME OF GOD Lid Laceration Conjunctival Hemorrhage a) No therapy is necessary b) Usually resolve in 7-12 days. Subconjunctival Hemorrhage Corneal Abrasion Abrasions Many small abrasions can
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg
 An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
Acute Ophthalmology for A&E Practice
 Acute Ophthalmology for A&E Practice Dr. LEUNG Yu-lung, Dexter MBChB, BMedSci(Hons),FRCS (Glas),MRCS(Edin), DRCOphth(London),FCOphthHK, FHKAM(Ophth) Associate Consultant Clinical Assistant Professor (Honorary)
Acute Ophthalmology for A&E Practice Dr. LEUNG Yu-lung, Dexter MBChB, BMedSci(Hons),FRCS (Glas),MRCS(Edin), DRCOphth(London),FCOphthHK, FHKAM(Ophth) Associate Consultant Clinical Assistant Professor (Honorary)
HANDBOOK FOR JUNIOR RESIDENTS AND MEDICAL STUDENTS LEARNING EMERGENCY OPHTHALMOLOGY
 HANDBOOK FOR JUNIOR RESIDENTS AND MEDICAL STUDENTS LEARNING EMERGENCY OPHTHALMOLOGY Compiled by The Task Force on Undergraduate Teaching in Ophthalmology of the International Council of Ophthalmology and
HANDBOOK FOR JUNIOR RESIDENTS AND MEDICAL STUDENTS LEARNING EMERGENCY OPHTHALMOLOGY Compiled by The Task Force on Undergraduate Teaching in Ophthalmology of the International Council of Ophthalmology and
Complete Visual Rehabilitation in a Patient with No Light Perception after Surgical Management of a Penetrating Open-Globe Injury: A Case Report
 Published online: June 23, 2015 1663 2699/15/0062 0204$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: June 23, 2015 1663 2699/15/0062 0204$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
ASSESSING THE EYES. Structures. Eyelids Extraocularmuscles Eyelashes Lacrimal glands: Lacrimal ducts Cornea Conjunctiva Sclera Pupils Iris.
 ASSESSING THE EYES Structures External Eyelids Extraocularmuscles Eyelashes Lacrimal glands: Lacrimal ducts Cornea Conjunctiva Sclera Pupils Iris 1 2 Structures Internal Optic disc Physiological cup Retinal
ASSESSING THE EYES Structures External Eyelids Extraocularmuscles Eyelashes Lacrimal glands: Lacrimal ducts Cornea Conjunctiva Sclera Pupils Iris 1 2 Structures Internal Optic disc Physiological cup Retinal
Ocular Emergencies. Pisit Preechawat, MD Department of Ophthalmology, Ramathibodi Hospital
 Ocular Emergencies Pisit Preechawat, MD Department of Ophthalmology, Ramathibodi Hospital Ocular Anatomy Bony Components of Orbit 1 1. Frontal bone 4 5 7 6 2. Zygomatic bone 3. Maxillary bone 4. Sphenoid
Ocular Emergencies Pisit Preechawat, MD Department of Ophthalmology, Ramathibodi Hospital Ocular Anatomy Bony Components of Orbit 1 1. Frontal bone 4 5 7 6 2. Zygomatic bone 3. Maxillary bone 4. Sphenoid
PAINFUL PAINLESS Contact lens user BOV
 Common Causes Allergies Infections Ocular Cornea, uveitis, endophthalmitis Orbital Orbital cellulitis Inflammation Uveitis Scleritis / episcleritis Glaucomas Trauma Foreign bodies Chemical injuries History
Common Causes Allergies Infections Ocular Cornea, uveitis, endophthalmitis Orbital Orbital cellulitis Inflammation Uveitis Scleritis / episcleritis Glaucomas Trauma Foreign bodies Chemical injuries History
Phone Triage for Optometric Staff ???????? CHEMICAL BURN CHEMICAL BURN
 Phone Triage for Optometric Staff There are very few ocular emergencies that you will have to deal with in practice, but it is imperative that you be able to Michelle Welch, O.D. NSU Oklahoma College of
Phone Triage for Optometric Staff There are very few ocular emergencies that you will have to deal with in practice, but it is imperative that you be able to Michelle Welch, O.D. NSU Oklahoma College of
Ocular warning signs in GP practice: Paediatric Eye Pointers
 Ocular warning signs in GP practice: Paediatric Eye Pointers Dr Benjamin Chang MB, BCh, BAO, MMedSci, FRCS(Irel), FRCS(Edin), FRCOphth(Lond) Senior Consultant Ophthalmology and Visual Sciences Khoo Teck
Ocular warning signs in GP practice: Paediatric Eye Pointers Dr Benjamin Chang MB, BCh, BAO, MMedSci, FRCS(Irel), FRCS(Edin), FRCOphth(Lond) Senior Consultant Ophthalmology and Visual Sciences Khoo Teck
Differential diagnosis of the red eye. Carol Slight Nurse Practitioner Ophthalmology
 Differential diagnosis of the red eye Carol Slight Nurse Practitioner Ophthalmology The red eye Conjunctivitis HSV Keratitis Acute angle closure glaucoma Anterior Uveitis Red eye Scleritis Subconjunctival
Differential diagnosis of the red eye Carol Slight Nurse Practitioner Ophthalmology The red eye Conjunctivitis HSV Keratitis Acute angle closure glaucoma Anterior Uveitis Red eye Scleritis Subconjunctival
Ocular Injuries. Chapter 14
 Ocular Injuries Chapter 14 Ocular Injuries Introduction The preservation of the eyes and eyesight of service personnel is an extremely important goal. Despite comprising as little as 0.1% of the total
Ocular Injuries Chapter 14 Ocular Injuries Introduction The preservation of the eyes and eyesight of service personnel is an extremely important goal. Despite comprising as little as 0.1% of the total
CASE PRESENTATION. DR.Sravani 1 st yr PG Dept of Ophthalmology
 CASE PRESENTATION DR.Sravani 1 st yr PG Dept of Ophthalmology Name : X X X X X Age : 50yrs Sex : male Occupation : Farmer Residence : Mothkur CHIEF COMPLAINTS : - Diminision of vision in Right Eye since
CASE PRESENTATION DR.Sravani 1 st yr PG Dept of Ophthalmology Name : X X X X X Age : 50yrs Sex : male Occupation : Farmer Residence : Mothkur CHIEF COMPLAINTS : - Diminision of vision in Right Eye since
INDICATIONS For steroid responsive inflammation of the palpebral and bulbar conjunctiva, cornea, and anterior segment of the eye globe.
 Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM PRED FORTE Sterile Eye Suspension COMPOSITION PRED FORTE Sterile Eye Suspension contains: Prednisolone acetate 10 mg/ml Preservative:
Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM PRED FORTE Sterile Eye Suspension COMPOSITION PRED FORTE Sterile Eye Suspension contains: Prednisolone acetate 10 mg/ml Preservative:
PREAMBLE TO MSC PAYMENT SCHEDULE: OPTOMETRY SERVICES
 PREAMBLE TO MSC PAYMENT SCHEDULE: OPTOMETRY SERVICES A. GENERAL PROVISIONS 1. Eye Examination Benefits Optometric benefits are services defined in Section 23 of the Medical and Health Care Services Regulations,
PREAMBLE TO MSC PAYMENT SCHEDULE: OPTOMETRY SERVICES A. GENERAL PROVISIONS 1. Eye Examination Benefits Optometric benefits are services defined in Section 23 of the Medical and Health Care Services Regulations,
Ocular Injuries. Chapter 14
 Ocular Injuries Chapter 14 Ocular Injuries Introduction The preservation of the eyes and eyesight of service personnel is an extremely important goal. Despite comprising as little as 0.1% of the total
Ocular Injuries Chapter 14 Ocular Injuries Introduction The preservation of the eyes and eyesight of service personnel is an extremely important goal. Despite comprising as little as 0.1% of the total
9/23/2014. Emily Thomas, O.D. MOA Paraoptometric Education October 5, 2014
 Emily Thomas, O.D. MOA Paraoptometric Education October 5, 2014 Anterior toward the front of the body Posterior toward the rear of the body Unilateral only one eye involved Bilateral both eyes involved
Emily Thomas, O.D. MOA Paraoptometric Education October 5, 2014 Anterior toward the front of the body Posterior toward the rear of the body Unilateral only one eye involved Bilateral both eyes involved
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
OPHTHALMOLOGIC PEARLS FOR THE NON- OPHTHALMOLOGIST. David G. Gross D.O. Deen-Gross Eye Centers Merrillville-Hobart Deengrosseye.
 OPHTHALMOLOGIC PEARLS FOR THE NON- OPHTHALMOLOGIST David G. Gross D.O. Deen-Gross Eye Centers Merrillville-Hobart Deengrosseye.com A FEW OF THE AREAS WE WILL DISCUSS Red Eye Glaucoma Neuro ophthalmic tid
OPHTHALMOLOGIC PEARLS FOR THE NON- OPHTHALMOLOGIST David G. Gross D.O. Deen-Gross Eye Centers Merrillville-Hobart Deengrosseye.com A FEW OF THE AREAS WE WILL DISCUSS Red Eye Glaucoma Neuro ophthalmic tid
Information for Patients. Deep sclerectomy for the treatment of Glaucoma
 Manchester Royal Eye Hospital Glaucoma Services Information for Patients Deep sclerectomy for the treatment of Glaucoma Introduction This leaflet provides information for patients being offered deep sclerectomy
Manchester Royal Eye Hospital Glaucoma Services Information for Patients Deep sclerectomy for the treatment of Glaucoma Introduction This leaflet provides information for patients being offered deep sclerectomy
Texas Definition of Eye Exam. Definitions of Eye Examinations BILLING AND CODING: WHY IS THIS STUFF SO HARD? Optometry School Definition
 BILLING AND CODING: WHY IS THIS STUFF SO HARD? Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com Definitions of Eye Examinations Optometry School definition
BILLING AND CODING: WHY IS THIS STUFF SO HARD? Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com Definitions of Eye Examinations Optometry School definition
THE RED EYE Cynthia McNamara, MD Week 25
 THE RED EYE Cynthia McNamara, MD Week 25 Educational Objectives: 1. Know the differential diagnosis and presentation of specific etiologies of the red eye 2. Be able to evaluate patients presenting with
THE RED EYE Cynthia McNamara, MD Week 25 Educational Objectives: 1. Know the differential diagnosis and presentation of specific etiologies of the red eye 2. Be able to evaluate patients presenting with
The Emergent Eye in the Acute Setting
 The Emergent Eye in the Acute Setting Todd P. Margolis MD, PhD Professor of Ophthalmology & Director of the F.I. Proctor Foundation UCSF Physical Exam-- Visual Acuity Essential Corrected visual acuity
The Emergent Eye in the Acute Setting Todd P. Margolis MD, PhD Professor of Ophthalmology & Director of the F.I. Proctor Foundation UCSF Physical Exam-- Visual Acuity Essential Corrected visual acuity
Wildlife Ophthalmology D R. H E A T H E R R E I D T O R O N T O W I L D L I F E C E N T R E T O R O N T O, O N C A N A D A
 Wildlife Ophthalmology D R. H E A T H E R R E I D T O R O N T O W I L D L I F E C E N T R E T O R O N T O, O N C A N A D A Why understand eyes? Wildlife need to have excellent vision to survive in the
Wildlife Ophthalmology D R. H E A T H E R R E I D T O R O N T O W I L D L I F E C E N T R E T O R O N T O, O N C A N A D A Why understand eyes? Wildlife need to have excellent vision to survive in the
A Guide to Administering
 A Guide to Administering INDICATIONS AND USAGE YUTIQ (fluocinolone acetonide intravitreal implant) 0.18 mg is indicated for the treatment of chronic non-infectious uveitis affecting the posterior segment
A Guide to Administering INDICATIONS AND USAGE YUTIQ (fluocinolone acetonide intravitreal implant) 0.18 mg is indicated for the treatment of chronic non-infectious uveitis affecting the posterior segment
LECTURE # 7 EYECARE REVIEW: PART III
 LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
Around The Globe in 60 Minutes
 Around The Globe in 60 Minutes Around the GLOBE in Sixty Minutes Basic Ocular Anatomy, Examination, and Diagnostic Techniques Introduction Focusing on canine and feline ocular anatomy and basic examination
Around The Globe in 60 Minutes Around the GLOBE in Sixty Minutes Basic Ocular Anatomy, Examination, and Diagnostic Techniques Introduction Focusing on canine and feline ocular anatomy and basic examination
Differential Diagnosis of Conjunctivitis and Keratoconjunctivitis
 Differential Diagnosis of Conjunctivitis and Keratoconjunctivitis Dr. Victor Malinovsky 2006 Mechanical-Physical Trauma Corneal Abrasions Abrasions (interpalpebral/variable): a focal loss of epithelium
Differential Diagnosis of Conjunctivitis and Keratoconjunctivitis Dr. Victor Malinovsky 2006 Mechanical-Physical Trauma Corneal Abrasions Abrasions (interpalpebral/variable): a focal loss of epithelium
 Traumatic Cataract Orbital Wall Fracture Vitreous Hemorrhage Optic Disc Hemorrhage a) Amblyopia b) Strabismus c) Trauma Playing with other children Sports Fire works BB gun Injecting needles .
Traumatic Cataract Orbital Wall Fracture Vitreous Hemorrhage Optic Disc Hemorrhage a) Amblyopia b) Strabismus c) Trauma Playing with other children Sports Fire works BB gun Injecting needles .
For details on measurement and recording of visual acuity, refer to Annex 1. VISION INTERPRETING RESULTS ABSTRACT
 management update on functional decline in older adults 2012 Unit No. 5 VISION Dr Au Eong Kah Guan, Ms Yulianti, Ms Fifiana ABSTRACT Among Singaporean adults of Chinese origin aged 40 to 79 years old,
management update on functional decline in older adults 2012 Unit No. 5 VISION Dr Au Eong Kah Guan, Ms Yulianti, Ms Fifiana ABSTRACT Among Singaporean adults of Chinese origin aged 40 to 79 years old,
Developed by Bradford J. Shingleton, MD, in conjunction with the Ophthalmology Liaisons Committee of the American Academy of Ophthalmology
 Developed by Bradford J. Shingleton, MD, in conjunction with the Ophthalmology Liaisons Committee of the American Academy of Ophthalmology Reviewer, 2009 Revision Mary A. O'Hara, MD Executive Editor, 2009
Developed by Bradford J. Shingleton, MD, in conjunction with the Ophthalmology Liaisons Committee of the American Academy of Ophthalmology Reviewer, 2009 Revision Mary A. O'Hara, MD Executive Editor, 2009
Open globe injuries in children: factors predictive of a poor final visual acuity
 (2009) 23, 621 625 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye Open globe injuries in children: factors predictive of a poor final visual acuity A Gupta,
(2009) 23, 621 625 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye Open globe injuries in children: factors predictive of a poor final visual acuity A Gupta,
Eye and Ocular Adnexa, Auditory Systems
 Eye and Ocular Adnexa, Auditory Systems CPT copyright 2011 American Medical Association. All rights reserved. Fee schedules, relative value units, conversion factors and/or related components are not assigned
Eye and Ocular Adnexa, Auditory Systems CPT copyright 2011 American Medical Association. All rights reserved. Fee schedules, relative value units, conversion factors and/or related components are not assigned
Telephone Triage Urgency or Emergency? Mary E. Schmidt, ABOC, CPO
 Telephone Triage Urgency or Emergency? www.eyesystems.info Mary E. Schmidt, ABOC, CPO mary@eyesystems.info Definition of Triage The sorting of patient and allocation of care or treatment according to the
Telephone Triage Urgency or Emergency? www.eyesystems.info Mary E. Schmidt, ABOC, CPO mary@eyesystems.info Definition of Triage The sorting of patient and allocation of care or treatment according to the
AUSTRALIAN PRODUCT INFORMATION FLAREX (FLUOROMETHOLONE ACETATE) EYE DROPS SUSPENSION
 AUSTRALIAN PRODUCT INFORMATION FLAREX (FLUOROMETHOLONE ACETATE) EYE DROPS SUSPENSION 1 NAME OF THE MEDICINE Fluorometholone acetate. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION The active ingredient in
AUSTRALIAN PRODUCT INFORMATION FLAREX (FLUOROMETHOLONE ACETATE) EYE DROPS SUSPENSION 1 NAME OF THE MEDICINE Fluorometholone acetate. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION The active ingredient in
New Zealand Data Sheet
 New Zealand Data Sheet Prednisolone-AFT 1% Prednisolone acetate (Ph Eur) 1% w/v ophthalmic suspension Presentation Prednisolone-AFT 1% is a milky white suspension in an eyedropper bottle for ophthalmic
New Zealand Data Sheet Prednisolone-AFT 1% Prednisolone acetate (Ph Eur) 1% w/v ophthalmic suspension Presentation Prednisolone-AFT 1% is a milky white suspension in an eyedropper bottle for ophthalmic
Cairo University Faculty of Medicine. Course Specifications Course title: Ophthalmology (Code): OPH-409. Department of Ophthalmology
 Cairo University Faculty of Medicine Department of Ophthalmology Course Specifications Course title: Ophthalmology (Code): OPH-409 Department of Ophthalmology Fourth academic year of M.B.B.Ch. program
Cairo University Faculty of Medicine Department of Ophthalmology Course Specifications Course title: Ophthalmology (Code): OPH-409 Department of Ophthalmology Fourth academic year of M.B.B.Ch. program
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION Contents METHODS... 2 Inclusion and exclusion criteria... 2 Supplementary table S1... 2 Assessment of abnormal ocular signs and symptoms... 3 Supplementary table S2... 3 Ocular
SUPPLEMENTARY INFORMATION Contents METHODS... 2 Inclusion and exclusion criteria... 2 Supplementary table S1... 2 Assessment of abnormal ocular signs and symptoms... 3 Supplementary table S2... 3 Ocular
NEW ZEALAND DATA SHEET 1. PRODUCT NAME
 NEW ZEALAND DATA SHEET 1. PRODUCT NAME Flucon fluorometholone 0.1% Eye Drops Suspension 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each ml of Flucon contains 1.0 mg of fluorometholone (0.1% w/v). Excipient
NEW ZEALAND DATA SHEET 1. PRODUCT NAME Flucon fluorometholone 0.1% Eye Drops Suspension 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each ml of Flucon contains 1.0 mg of fluorometholone (0.1% w/v). Excipient
TRAUMATIC CATARACT DR.KHUTEJA FATIMA IIND YEAR PG DEPT OF OPHTHALMOLOGY
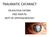 TRAUMATIC CATARACT DR.KHUTEJA FATIMA IIND YEAR PG DEPT OF OPHTHALMOLOGY Traumatic cataract :Traumatic lens damage caused by mechanical injury and by physical forces (Ionising radiation,ir radiation, electrical
TRAUMATIC CATARACT DR.KHUTEJA FATIMA IIND YEAR PG DEPT OF OPHTHALMOLOGY Traumatic cataract :Traumatic lens damage caused by mechanical injury and by physical forces (Ionising radiation,ir radiation, electrical
10/4/2013. Bruce K.Williams, MSN, RN,ACNP-BC Sisters of Charity Providence Hospitals. What is the worst thing that can go wrong with an eye?
 Red Eyes, Red Alert! Bruce K.Williams, MSN, RN,ACNP-BC Sisters of Charity Providence Hospitals Red Eyes, Red Alert! Red Eyes, Red Alert! What is the worst thing that can go wrong with an eye? 1 Red Eyes,
Red Eyes, Red Alert! Bruce K.Williams, MSN, RN,ACNP-BC Sisters of Charity Providence Hospitals Red Eyes, Red Alert! Red Eyes, Red Alert! What is the worst thing that can go wrong with an eye? 1 Red Eyes,
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Orbital and Ocular Adnexal Disorders with Red Eyes
 Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
02/03/2014. Average Length: 23mm (Infant ~16mm) Approximately the size of a quarter Volume: ~5mL
 Identify the anatomy of the eye. Explain the basic physiology of the parts of the eye. Briefly discuss various surgeries related to different parts of the anatomy. Average Length: 23mm (Infant ~16mm) Approximately
Identify the anatomy of the eye. Explain the basic physiology of the parts of the eye. Briefly discuss various surgeries related to different parts of the anatomy. Average Length: 23mm (Infant ~16mm) Approximately
JINNAH SINDH MEDICAL UNIVERSITY STUDY GUIDE- OPHTHALMOLOGY YEAR 4,
 INTRODUCTION Pakistan, the 7th most populous country in the world, has an urban population of 38.8% and rural dwellers of 61.2%. The country has faced challenges with vision impairment and blindness as
INTRODUCTION Pakistan, the 7th most populous country in the world, has an urban population of 38.8% and rural dwellers of 61.2%. The country has faced challenges with vision impairment and blindness as
Resources from the American Academy of Ophthalmology...1 Meet the Eye Care Team...1 Eye Myths... 3
 CONTENTS Preface...ix Acknowledgments... x About the Executive Editors... x Introduction to Ophthalmology... 1 Resources from the American Academy of Ophthalmology...1 Meet the Eye Care Team...1 Eye Myths...
CONTENTS Preface...ix Acknowledgments... x About the Executive Editors... x Introduction to Ophthalmology... 1 Resources from the American Academy of Ophthalmology...1 Meet the Eye Care Team...1 Eye Myths...
The Orbit. The Orbit OCULAR ANATOMY AND DISSECTION 9/25/2014. The eye is a 23 mm organ...how difficult can this be? Openings in the orbit
 The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
Emergency Ophthalmology Lawrence B. Stack, MD Handout can be found on lbstack.com/students/eye-handout.pdf
 Emergency Ophthalmology Lawrence B. Stack, MD Handout can be found on lbstack.com/students/eye-handout.pdf Summary Points: 1. Consult Ophthalmology if you can not account for change in visual acuity 2.
Emergency Ophthalmology Lawrence B. Stack, MD Handout can be found on lbstack.com/students/eye-handout.pdf Summary Points: 1. Consult Ophthalmology if you can not account for change in visual acuity 2.
Pediatric traumatic cataract Presentation and Management. Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017
 Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Traumatic Partial Optic Nerve Avulsion with Globe luxation. Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine
 Traumatic Partial Optic Nerve Avulsion with Globe luxation Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine A 23 year old male patient presented to the emergency department in
Traumatic Partial Optic Nerve Avulsion with Globe luxation Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine A 23 year old male patient presented to the emergency department in
Corneal Ulceration. Client Information Sheet Copyright Bilton Veterinary Centre All rights Reserved. What is the cornea?
 What is the cornea? Corneal Ulceration The cornea is the central clear part of the eye that is surrounded by the white of the eye called the Sclera. Looking through the cornea, you can see the coloured
What is the cornea? Corneal Ulceration The cornea is the central clear part of the eye that is surrounded by the white of the eye called the Sclera. Looking through the cornea, you can see the coloured
