ation is essential. Whether on the playing it is important to keep in mind that severe
|
|
|
- Ferdinand James
- 5 years ago
- Views:
Transcription
1 JENNIFER LAIO, MD, and BRUCE M. ZAGELBAUM, MD NYU School of Medicine, Manhasset, NY North Shore University Hospital, Eye injuries sustained in sports and recreational activities are common in the United States. Of the more than 2.4 million ocular injuries that occur each year, approximately 100,000 cases are sports related (Stock & Cornell, 1991). Once an eye injury is sustained, prompt evalu- With any eye injury, raold and treatment is ess~~ ntial for optimizing visual out( OM?. An emerqency first-ai d kit for oc~ examination should a lways be available, complete.,, atter hov injury see ation is essential. Whether on the playing field or in the office, it is important to keep in mind that severe underlying injuries may exist and vision-threatening complications may occur. A systematic approach including a careful history, complete examination of both eyes, and appropriate management is the key to reducing ocular morbidity from sports related injuries (Grewel et al., 1996; Zagelbaum, 1995a, 1995b. Sport-specific trends are well recognized in eye injuries. When evaluating sports related eye trauma, one should inquire about the environment in which the injury occurred and the mechanism of injury. It is important to note whether the patient wore contact lenses, glasses, or protective eyewear at the time of injury; these items should be inspected for damage. The examiner should also obtain the patient's ocular history including any past trauma or surgery to the eye concerned. Knowing the patient's baseline best-corrected vision helps in assessing the severity of the injury. Finally, questions regarding past medical history, medications (including eye drops), and allergies are obtained. A complete examination of both eyes enables an examiner to determine the nature and the extent of injury. In most instances, the initial examination of an athlete with an eye injury will take place at the sporting event. For this reason, an emergency first-aid kit for ocular examination should always be available. Examination should always include the following: Visual Acuity Ideally, visual acuity should be tested with a Snellen eye chart posted at 20 feet away or a pocket vision card held at a comfortable reading position. Each eye should be tested independently (the fellow eye is covered) for the best-corrected vision. Glasses or contact lenses, if worn, should be used. Start with the smallest line on the chart and move up, recording the smallest line where more than half of the letters are read accurately. When patients fail to see the largest line at 20 feet, they should be moved closer to the eye chart until they can see the larger print on the chart. The distance at which patients stand from the chart is noted in feet. The visual acuity will be I999 Human Kinetics. ATT L(5), pp. 36-L SEPTEMBER 1999 ATHLETIC THERAPY TODAY
2 that involves the margin should be evaluated by an ophthalmologist, as it may involve damage to the nasolacrimal system. Significantperiorbital edema and eccyhmosis should raise suspicion of an underlying orbital wall fracture. Palpate the area for subcutaneous emphysema, the orbital rim for bony displacement, and the cheek for hypesthesia (numbness). Pupils ipped ay~plicators(sterile Eye pad sleye shield (plastic or n Idpt: T.. - Sterile ocular irr igant (scxueeze b pica1 antibiotics (I.e., tomamy Contact lens case and sc Sterile gauze spcx-iges recorded by using the distance as the numerator. For instance, a patient seeing a line at 5 feet from the chart has visual acuity. If the patient cannot read the Snellen chart, he or she should be asked to count the examiner's fingers at different distances. If unable to count fingers, perception of hand movements or light should be recorded. A penlight or flashlight can be used as the light source. The results should be documented as finger counting or hand movements, light perception or no light perception. If a standard vision chart is not available, a newspaper or magazine can be used. In trauma cases, vision should be tested promptly for both medical and legal reasons. Any decrease in visual acuity is a red flag for the examiner to suspect a vision-threatening injury. Eyelids and Adnexa The lids and periorbital areas should be thoroughly inspected for abrasions, lacerations, foreign bodies, edema, erythema, and ecchymosis. A lid laceration ATHLETIC THERAPY TODAY Using a penlight, inspect both pupils for size, shape, and reaction to light. An irregularly peaked pupil warrants a careful examination for possible ruptured globe. Each pupil is tested individually for direct reaction to light and the consensual response is checked as well by swinging a penlight back and forth between the two pupils. Each pupil should normally constrict when the light is directed toward the fellow pupil. Detection of a paradoxical dilation of any pupil (relative afferent pupillary defect) is significant and requires evaluation by an ophthalmologist. Extraotular Movements Extraocular muscle function is tested by asking the patient to look up, down, right, and left without moving the head. It is important to look for limitations of movements in any gaze and see if there is any diplopia (double vision) in a particular gaze. The presence of any of the above may indicate an orbital fracture with muscle entrapment or hemorrhage. Anterior Segment The conjunctiva should be inspected for injection (redness), swelling, hemorrhage, lacerations, or foreign bodies. Applying fluorescein dye into the area helps visualization of transparent objects, such as glass and contact lens fragments. The cornea should also be checked for abrasions, lacerations, haziness, and foreign bodies. If a corneal laceration is present, this is a medical emergency and should be referred to an emergency room immediately. The anterior chamber-the space between the cornea and the iris plane-is examined for depth and hyphema (blood in the anterior chamber). One eye should be compared with the other for depth. The iris should be checked for any irregular shape. Although difficult, if the lens is viewed, its clarity should be noted. SEPTEMBER
3 Posterior S~grnent A good examination of the vitreous cavity, retina, choroid, and optic nerve requires both pupils to be dilated. When a patient is unconscious or confused, dilation should be deferred until a neurologic evaluation is done. A hand-held direct ophthalmoscope can be used to examine the posterior segment. Indirect ophthalmoscopy provides a broader view and is usually done by an ophthalmologist. Diagnsris and Managamsnt Corn~al Abrasion Corneal abrasions are among the most common sports related eye injuries. They result from a blunt or projectile object striking the eye. The corneal epithelium is disrupted and sloughs off, rendering the underlying layers susceptible to infection. Patients with corneal abrasions generally complain of foreign body sensation, pain, tearing, and sensitivity to light. Visual acuity is decreased to various degrees depending on the location of the abrasion. Other signs include conjunctival injection, eyelid swelling, and iritis (inflammation in anterior chamber). The cornea may be examined with a slit lamp or penlight with a cobalt blue filter. A drop of fluorescein dye with or without topical anesthetic is applied to the inferior cul-de-sac, the space between the lower lid and the globe. The dye is taken up by an epithelial defect and gives off a bright green fluorescent light when viewed with a penlight (Photo 1). A cobalt blue filter attached to a penlight allows a better view. The primary treatment for a corneal abrasion is a broad-spectrum topical antibiotic and a pressure Photo I The briaht stain lcentrallv located) appeared on thiipatientlicornea after fluorescein was applied. The staining area outlines the corneal abrasion present. patch. A cycloplegic agent (e.g., 1 % cyclopentolate hydrochloride) may be used for patient comfort. The patient should be evaluated the following day. Topical anesthetic agents should not be used to treat corneal abrasions. Their regular use may cause corneal epithelial defects, infiltrates, inflammation, severe pain, and decreased vision (Zagelbaum et al., 1994). A pressure patch should not be used for contact lens wearers, as this puts them at risk for developing further infection. Chato Z A subconjunctival hemorrhage is seen as blood loculated ~ Q ~ W the Q Q white ~ sclera and the overlying conjunctiva. Subtonjunctival Hemorrhag~ Breakage of small conjunctival vessels results in a blood loculus forming between the conjunctiva and the sclera (Photo 2). This is a common finding with blunt eye trauma and patients are usually asymptomatic. Upon initial examination, the hemorrhage should be traced to its posterior border in order to rule out a retrobulbar hemorrhage. The presence of other signs associated with retrobulbar hemorrhage, such as proptosis and limitation of extraocular movements, will further differentiate the two. Subconjunctival hemorrhage., usually resolves within 2 weeks and treatment is not necessary. When patients have marked subconjunctival hemorrhage in association with significant chemosis (swelling of bulbar conjunctiva) and/or decreased vision, a ruptured globe should be suspected. Prompt evaluation by an ophthalmologist is indicated.. Trau Traumatic iritis is an inflammation of the iris or ciliary body. Blunt trauma to the orbital region generally causes this condition. Patients typically complain of 38 1 SEPTEMBER 1999 ATHLETIC THERAPY TODAY
4 photophobia, pain, and decreased vision. The pupil may become miotic (constricted) and react poorly to light. The conjunctiva is injected, especially in the area directly surrounding the cornea (ciliary flush). Treatment of iritis consists of a topical steroid (e.g., prednisone acetate 1 %) to reduce inflammation and a cycloplegic agent (e.g., cyclopentolate hydrochloride 1 %) to reduce pain and photophobia. Topical steroids should be tapered off quickly when the inflammation is resolved. Eyelid Laceration Patients with eyelid lacerations should have a complete ocular examination before repair to ensure that there is no other ocular damage. If an eyelid laceration involves the lid margin or deep structures of upper eyelids, or if there is excessive loss of tissue, repair should be done by an ophthalmologist. Otherwise, the laceration may be closed by careful approximation of skin using 6-0 or 7-0 silk or nylon sutures. In preparation for the repair, the wound and surrounding tissues should be thoroughly irrigated with saline solution and cleaned with povidone iodine. Local anesthesia (e.g., 2 5% lidocaine with epinephrine) is used and sterile technique should be followed throughout the procedure. Tissues should be handled with care in an effort to preserve the structure of the lid. Sutures are generally removed within 7 days. Uyphema Hyphema is blood in the anterior chamber, usually as a result of blunt trauma or direct laceration to the globe. The blood comes from broken vessels in the iris or ciliary body. Patients often complain of decreased vision and pain. The blood exists in the anterior chamber as a clot, a pool of layered blood, or suspended red blood cells (microhyphema) (Photos 3 and 4). A complete eye examination should be performed to make sure the patient has not sustained a ruptured globe. Management of hyphema could be complicated and at least three issues should be addressed: (a) decrease the patient's discomfort, (b) minimize the chance of rebleeding, and (c) prevent complications. Long-standing hyphema can cause corneal staining and significant elevation of intraocular pressure. The Pketcl3 Bright red blood can be seen in the anterior chamber, between the cornea and the iris. This signifies a hyphema. Also note: (a) the subconjunctival hemorrhage present and (b) the irregular pupil. This patient actually had a ruptured globe. Photo 4 In this case the hyphema is layered. general recommendations for management include the following: a topical steroid or cycloplegic agent for patient comfort; an eye shield for protection; reduced activity level or bed rest; elevating the head of the bed 30" ; and avoiding aspirin or anticoagulants. Patients should be examined by an ophthalmologist daily. Patients who are unable to comply with the above regimen are admitted for hospitalization. Sometimes surgical intervention may be required for hyphema and its associated complications. Foreign Bodies Patients who complain of foreign body sensation, pain, photophobia, and tearing should be checked for the presence of foreign bodies. These tend to lodge on the corneal and conjunctival surfaces as well as in the conjunctival fornix. A penlight or slit-lamp allows direct visualization of the foreign body most of the time. Applying a drop of fluorescein dye onto the surface helps outline clear objects and detect associated ATHLETIC THERAPY TODAY SEPTEMBER
5 corneal and conjunctival damage. It is necessary to evert the upper eyelid to look for hidden foreign bodies. Treatment begins with administering a topical anesthetic drop to alleviate pain. Generous irrigation with saline is performed, directing the stream at the eye. A sterile cotton swab may be used to sweep away any loose foreign material. If a foreign body is embedded into the corneal surface, its removal requires the use of a 30-gauge needle or a foreign body spud. This is usually done by an ophthalmologist with the aid of a slit-lamp for magnification. A topical antibiotic drop or ointment is applied after removal. A pressure patch may necessary if a corneal abrasion has occurred. The patient can be managed with a topical antibiotic. Orbital Wall Fracture Orbital wall fractures, or "blowout fractures," often occur with blunt trauma to the orbit. Compact forces are transmitted to produce anteriorlposterior compression and equatorial expansion. Since the medial wall and the floor are the thinnest orbital bones, they tend to be fractured most frequently. Patients present with periorbital edema, ecchymosis, and pain. Other symptoms and signs include painful and limited eye movements (Photo 5), diplopia, subcutaneous emphysema, swelling of lids with nose blowing (due to fracture into the sinuses), hypesthesia in the upper cheek area, and enophthalmos (inward displaced eye). Radiological studies are indicated if patients have signs and symptoms of orbital wall fractures. Plain x- rays may be used, but CT scanning using thin 3-mm cuts (axial and coronal views) is preferred. Initial management of orbital wall fractures includes abroadspectrum oral antibiotic for prophylaxis and observation. Patients should avoid nose blowing if possible. Surgery is delayed for 10 to 14 days after the injury to allow the swelling to subside. Indications for surgical repair are persistent diplopia (secondary to entrapped extraocular muscle and tendon) or cosmetically significant enophthalmos (caused by prolapse of orbital content through a large bony defect). Ratptuhed Globe When evaluating a patient with an eye injury, one should always suspect a ruptured globe. The symptoms associated with a ruptured globe are typically pain and decreased vision. However, symptoms may be nonspecific and can vary in intensity. Alerting signs include excessive conjunctival hemorrhage and edema, irregular pupil shape, prolapsed iris through a wound (Photo 6), asymmetry of anterior chamber depth between both eyes, and very low intraocular pressure. PLapto 6 The iris is prolapsed through the eye, signifying a ruptured globe. When the diagnosis of a ruptured globe is made or strongly suspected, the affected eye should immediately be covered with a protective shield. Eyedrops should not be used and there should not be any manipulation of the eye or adnexa. The patient is not allowed to eat or drink, as prompt surgical intervention is generally required. If an intraocular foreign body is suspected, CT of the orbits should be performed. Photc E After sustaining blunt trauma, extraocular movements were checked. Note that upon upgaze, the left eye was unable to look up. A left orbital floor fracture was present with entrapment of the inferior rectus muscle. Posterior segment damage includes vitreous hemorrhage, commotio retinae, choroidal rupture, retinal 40 1 SEPTEMBER 1999 ATHLETIC THERAPY TODAY
6 tears or detachment, retinal hemorrhage, and traumatic optic neuropathy. Patients usually complain of decreased vision, although they may be asymptomatic. In retinal detachment, patients often report seeing flashes of light, a gray shadow, or a curtainlshade being pulled over the eye. The posterior Segment is best examined by an ophthalmologist using indirect ophthalmoscopy. For cases when it is not possible to view the posterior segment, an ultrasound exam is necessary. RQ~QCQWC~S Grewal, R.K., Dhaliwal, D.K., Hersh, P.S., & Zagelbaum, B.M. (1996). Anterior segment injuries. In B.M. Zagelbaum ( ~ d. )Sports, ophthalmology (pp ). Cambridge: Blackwell Scientific. Stock, J.G., & Cornell, F.M. ( 1 991). Prevention of sports-related eye injury. American Fami& Physician, 14, Zagelbaum, B.M.(1995a). A close look at a "red eye": Diagnosing visionthreatening causes. The Physician and Sportsmedicine, 23(11), Zagelbaum, B.M. (1 995b). Examining a "red eye": Diagnosing non-visionthreating causes. The Physician and Sportsmedicine, 23(12), Zagelbaum, B.M., Tostanoski, J.R., Hochman, M.A., & Hersh, P.S. (1994). Topical lidocaine and proparacaine abuse. AmericanJournal ofemergency Medicine, 12, Qonclurionr 'ports in a wide range of injuries can eye injuries. An orderly and systematic approach in evaluating these injuries is necessary in order to identify and manage these conditions properly. Our role is to rapidly formulate a diagnosis, treatment, and plan that in the best 'Itimate outcome for the athlete. II ATHLETIC THERAPY TODAY Jennifer Laio is the chief resident in ophthalmology at North Shore University Hospital. New York University School of Medicine, in Manhasset, NY. She graduated from the State University of New York at Stony B ~ O O ~, Of Medicine, in Bruce M.ZQgelbaum is in private practice in Manhasset, NY, and is an assistant professor at North Shore University Hospital, NYU School of Medicine. He is the team ophthalmologist for several pro sports teams and also an ophthalmology consultant to the NFL. He is author of the textbook sports ~ ~ h t h a l m ~ l o ~ ~ SEPTEMBER
EYE INJURIES OBJECTIVES COMMON EYE EMERGENCIES 7/19/2017 IMPROVE ASSESSMENT OF EYE INJURIES
 EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
Ocular and periocular trauma
 Ocular and periocular trauma No financial disclosures. Tina Rutar M.D. Assistant Professor of Clinical Ophthalmology and Pediatrics Director, Visual Center for the Child University of California San Francisco
Ocular and periocular trauma No financial disclosures. Tina Rutar M.D. Assistant Professor of Clinical Ophthalmology and Pediatrics Director, Visual Center for the Child University of California San Francisco
Ocular and Periocular Trauma. Tina Rutar, MD. Assistant Professor of Ophthalmology and Pediatrics. Director, Visual Center for the Child
 Ocular and Periocular Trauma Tina Rutar, MD Assistant Professor of Ophthalmology and Pediatrics Director, Visual Center for the Child University of California, San Francisco Phone: 415-353-2560 Fax: 415-353-2468
Ocular and Periocular Trauma Tina Rutar, MD Assistant Professor of Ophthalmology and Pediatrics Director, Visual Center for the Child University of California, San Francisco Phone: 415-353-2560 Fax: 415-353-2468
Assessment and Management of Ocular Trauma. Disclosure I have no direct financial interests in today s subject matter. 3/25/2019. Normal Eye Anatomy
 Assessment and Management of Ocular Trauma Samiksha Fouzdar Jain, MD,FRCS Department of Ophthalmology & Visual Sciences Truhlsen Eye Institute Disclosure I have no direct financial interests in today s
Assessment and Management of Ocular Trauma Samiksha Fouzdar Jain, MD,FRCS Department of Ophthalmology & Visual Sciences Truhlsen Eye Institute Disclosure I have no direct financial interests in today s
EYE TRAUMA: INCIDENCE
 Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Ophthalmic Trauma Update
 Ophthalmic Trauma Update Richard S. Davidson, M.D. Professor of Ophthalmology Vice Chair for Quality and Clinical Affairs UCHealth Eye Center University of Colorado School of Medicine August 5, 2017 Financial
Ophthalmic Trauma Update Richard S. Davidson, M.D. Professor of Ophthalmology Vice Chair for Quality and Clinical Affairs UCHealth Eye Center University of Colorado School of Medicine August 5, 2017 Financial
UC SF. g h. Eye Trauma. Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California
 UC SF Eye Trauma sf g h Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California Goals Recognize vision threatening eye emergencies Treat them when we can Know when
UC SF Eye Trauma sf g h Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California Goals Recognize vision threatening eye emergencies Treat them when we can Know when
MRI masterfile Part 5 WM Heme Strokes.ppt 1
 Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
Clues of a Ruptured Globe
 Definition any eye that has sustained a full thickness traumatic disruption of the cornea or sclera Overwhelmingly, rupture accidents occur in young men, small children and the elderly Corneal laceration
Definition any eye that has sustained a full thickness traumatic disruption of the cornea or sclera Overwhelmingly, rupture accidents occur in young men, small children and the elderly Corneal laceration
PEDIATRIC OCULAR INJURIES. Sapna Tibrewal MD
 PEDIATRIC OCULAR INJURIES Sapna Tibrewal MD 1 Learning Objectives Learn to recognize the common pediatric ocular injuries Immediate management tips to be instituted in your office/ ER Know when to call
PEDIATRIC OCULAR INJURIES Sapna Tibrewal MD 1 Learning Objectives Learn to recognize the common pediatric ocular injuries Immediate management tips to be instituted in your office/ ER Know when to call
Ocular Urgencies and Emergencies
 Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
Management of specific eye problems in the ED
 of specific eye problems in the ED CORNEAL ABRASION Causes Foreign bodies Tangential shearing injuries, e.g. poking finger into eye Exact cause of injury (Remember to exclude possibility of intraocular
of specific eye problems in the ED CORNEAL ABRASION Causes Foreign bodies Tangential shearing injuries, e.g. poking finger into eye Exact cause of injury (Remember to exclude possibility of intraocular
Ocular Emergencies. What is an emergency to the patient is not necessarily an emergency to the staff
 OCULAR EMERGENCIES Ophthalmic Photographers Society November 15, 2013 Michael A. DellaVecchia MD PhD FACS Wills Eye Emergency Department Philadelphia PA Ocular Emergencies What is an emergency to the patient
OCULAR EMERGENCIES Ophthalmic Photographers Society November 15, 2013 Michael A. DellaVecchia MD PhD FACS Wills Eye Emergency Department Philadelphia PA Ocular Emergencies What is an emergency to the patient
Ocular Injuries in Sports. Rance McClain, D.O. Associate Dean, Clinical Sciences William Carey University FM/NMM-OMM/Sports Medicine
 Ocular Injuries in Sports Rance McClain, D.O. Associate Dean, Clinical Sciences William Carey University FM/NMM-OMM/Sports Medicine http://sudc.org/vienna/ Learning Objectives 1. Know the sport classification
Ocular Injuries in Sports Rance McClain, D.O. Associate Dean, Clinical Sciences William Carey University FM/NMM-OMM/Sports Medicine http://sudc.org/vienna/ Learning Objectives 1. Know the sport classification
Acute Eyes for ED. Enis Kocak. The Alfred Ophthalmology
 Acute Eyes for ED Enis Kocak The Alfred Ophthalmology The problem with eyes Things to cover Ocular anatomy Basic assessment Common presentations Eye first aid and procedures Ophthalmic emergencies What
Acute Eyes for ED Enis Kocak The Alfred Ophthalmology The problem with eyes Things to cover Ocular anatomy Basic assessment Common presentations Eye first aid and procedures Ophthalmic emergencies What
MRI masterfile Part 5 WM Heme Strokes.ppt 2
 Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
2/5/2018. Trauma. Subdivided into two main categories: Closed globe Open Globe
 1 2 3 4 5 Ocular Trauma Guide for Eye Care Office Staff Winter Thaw 2018 Aaron Yatskevich OD Definition A broad term used to describe a physical or chemical wound to the eye or eye socket. Ocular trauma
1 2 3 4 5 Ocular Trauma Guide for Eye Care Office Staff Winter Thaw 2018 Aaron Yatskevich OD Definition A broad term used to describe a physical or chemical wound to the eye or eye socket. Ocular trauma
Eye Trauma. Lid Laceration. Orbital Fracture
 Eye Trauma Lid Laceration The presence of a lid laceration, however insignificant, mandates careful exploration of the wound and examination of the globe. 1. Superficial lacerations parallel to the lid
Eye Trauma Lid Laceration The presence of a lid laceration, however insignificant, mandates careful exploration of the wound and examination of the globe. 1. Superficial lacerations parallel to the lid
PENETRATING EYE INJUIRES
 PENETRATING EYE INJUIRES King Harold receives a mortal penetrating injury to the eye at the Battle of Hastings 1066, Detail Bayeux Tapestry, Eleventh century. Then Earl William came from Normandy into
PENETRATING EYE INJUIRES King Harold receives a mortal penetrating injury to the eye at the Battle of Hastings 1066, Detail Bayeux Tapestry, Eleventh century. Then Earl William came from Normandy into
Sepideh Tara Rousta, MD FAAO Robert Wood Johnson University Hospital Saint Peter s University Hospital Wills Eye Hospital
 Sepideh Tara Rousta, MD FAAO Robert Wood Johnson University Hospital Saint Peter s University Hospital Wills Eye Hospital 14 mo old w R eye cross (parents) 9 mo old R eye crossing getting worse for past
Sepideh Tara Rousta, MD FAAO Robert Wood Johnson University Hospital Saint Peter s University Hospital Wills Eye Hospital 14 mo old w R eye cross (parents) 9 mo old R eye crossing getting worse for past
Ears. Mouth. Jowls 6 Major Bones of the Face Nasal bone Two
 1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
Ocular Trauma. Breaking Down Blunt. Blunt ocular trauma occurs frequently in sporting
 Focus on CME at the University of Saskatchewan Breaking Down Blunt Ocular Trauma By Dan Ash, MD, BA, FRCSC, FACS, FAAO Blunt ocular trauma occurs frequently in sporting activities, as well as in industrial
Focus on CME at the University of Saskatchewan Breaking Down Blunt Ocular Trauma By Dan Ash, MD, BA, FRCSC, FACS, FAAO Blunt ocular trauma occurs frequently in sporting activities, as well as in industrial
Acute Ophthalmology for A&E Practice
 Acute Ophthalmology for A&E Practice Dr. LEUNG Yu-lung, Dexter MBChB, BMedSci(Hons),FRCS (Glas),MRCS(Edin), DRCOphth(London),FCOphthHK, FHKAM(Ophth) Associate Consultant Clinical Assistant Professor (Honorary)
Acute Ophthalmology for A&E Practice Dr. LEUNG Yu-lung, Dexter MBChB, BMedSci(Hons),FRCS (Glas),MRCS(Edin), DRCOphth(London),FCOphthHK, FHKAM(Ophth) Associate Consultant Clinical Assistant Professor (Honorary)
Maxillofacial and Ocular Injuries
 Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Everyday Practice. Eye trauma: Primary care for general physicians
 VOL.. 15, NO.2, 85 2002 Everyday Practice Eye trauma: Primary care for general physicians H. K. TEWARI, ATUL KUMAR, GUNJAN PRAKASH INTRODUCTION The understanding of ocular trauma is important for the primary
VOL.. 15, NO.2, 85 2002 Everyday Practice Eye trauma: Primary care for general physicians H. K. TEWARI, ATUL KUMAR, GUNJAN PRAKASH INTRODUCTION The understanding of ocular trauma is important for the primary
Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS
 OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
5/2/2016 EYE EMERGENCIES. Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates. Anatomy. Tools
 EYE EMERGENCIES Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates Anatomy Tools 1 Contact dermatitis Blepharitis HSV Preseptal Cellulitis Anterior Chamber Subconjunctival hemorrhage
EYE EMERGENCIES Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates Anatomy Tools 1 Contact dermatitis Blepharitis HSV Preseptal Cellulitis Anterior Chamber Subconjunctival hemorrhage
The Emergent Eye in the Acute Setting
 The Emergent Eye in the Acute Setting Todd P. Margolis MD, PhD Professor of Ophthalmology & Director of the F.I. Proctor Foundation UCSF Physical Exam-- Visual Acuity Essential Corrected visual acuity
The Emergent Eye in the Acute Setting Todd P. Margolis MD, PhD Professor of Ophthalmology & Director of the F.I. Proctor Foundation UCSF Physical Exam-- Visual Acuity Essential Corrected visual acuity
Orbital and Ocular Adnexal Disorders with Red Eyes
 Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Eyes, ears, teeth and everything in between
 Eyes, ears, teeth and everything in between E M E R G E N C Y D E P A R T M E N T J U N I O R T E A C H created 14/11/10 by S.R. Bruijns, version 1.0 Objectives Eyes Ears Teeth Maxilla- facial EYES Approaching
Eyes, ears, teeth and everything in between E M E R G E N C Y D E P A R T M E N T J U N I O R T E A C H created 14/11/10 by S.R. Bruijns, version 1.0 Objectives Eyes Ears Teeth Maxilla- facial EYES Approaching
Assisting in Ophthalmology. Copyright 2011, 2007, 2003, 1999 by Saunders, an imprint of Elsevier Inc. All rights reserved.
 Assisting in Ophthalmology Learning Objectives Define, spell, and pronounce the terms listed in the vocabulary. Apply critical thinking skills in performing patient assessment and care. Explain the differences
Assisting in Ophthalmology Learning Objectives Define, spell, and pronounce the terms listed in the vocabulary. Apply critical thinking skills in performing patient assessment and care. Explain the differences
Paediatric acute ophthalmology. Harry Bradshaw
 Paediatric acute ophthalmology Harry Bradshaw Approach Red eye Leukocoria Neurological Trauma Visual loss Red eye Orbital Eyelid Conjunctiva Cornea Uvea Orbital Orbit fixed volume Contiguous with sinuses,
Paediatric acute ophthalmology Harry Bradshaw Approach Red eye Leukocoria Neurological Trauma Visual loss Red eye Orbital Eyelid Conjunctiva Cornea Uvea Orbital Orbit fixed volume Contiguous with sinuses,
THE RED EYE Cynthia McNamara, MD Week 25
 THE RED EYE Cynthia McNamara, MD Week 25 Educational Objectives: 1. Know the differential diagnosis and presentation of specific etiologies of the red eye 2. Be able to evaluate patients presenting with
THE RED EYE Cynthia McNamara, MD Week 25 Educational Objectives: 1. Know the differential diagnosis and presentation of specific etiologies of the red eye 2. Be able to evaluate patients presenting with
Emergency Ophthalmology Lawrence B. Stack, MD Handout can be found on lbstack.com/students/eye-handout.pdf
 Emergency Ophthalmology Lawrence B. Stack, MD Handout can be found on lbstack.com/students/eye-handout.pdf Summary Points: 1. Consult Ophthalmology if you can not account for change in visual acuity 2.
Emergency Ophthalmology Lawrence B. Stack, MD Handout can be found on lbstack.com/students/eye-handout.pdf Summary Points: 1. Consult Ophthalmology if you can not account for change in visual acuity 2.
10/4/2013. Bruce K.Williams, MSN, RN,ACNP-BC Sisters of Charity Providence Hospitals. What is the worst thing that can go wrong with an eye?
 Red Eyes, Red Alert! Bruce K.Williams, MSN, RN,ACNP-BC Sisters of Charity Providence Hospitals Red Eyes, Red Alert! Red Eyes, Red Alert! What is the worst thing that can go wrong with an eye? 1 Red Eyes,
Red Eyes, Red Alert! Bruce K.Williams, MSN, RN,ACNP-BC Sisters of Charity Providence Hospitals Red Eyes, Red Alert! Red Eyes, Red Alert! What is the worst thing that can go wrong with an eye? 1 Red Eyes,
02/03/2014. Average Length: 23mm (Infant ~16mm) Approximately the size of a quarter Volume: ~5mL
 Identify the anatomy of the eye. Explain the basic physiology of the parts of the eye. Briefly discuss various surgeries related to different parts of the anatomy. Average Length: 23mm (Infant ~16mm) Approximately
Identify the anatomy of the eye. Explain the basic physiology of the parts of the eye. Briefly discuss various surgeries related to different parts of the anatomy. Average Length: 23mm (Infant ~16mm) Approximately
Ocular Injuries. Chapter 14
 Ocular Injuries Chapter 14 Ocular Injuries Introduction The preservation of the eyes and eyesight of service personnel is an extremely important goal. Despite comprising as little as 0.1% of the total
Ocular Injuries Chapter 14 Ocular Injuries Introduction The preservation of the eyes and eyesight of service personnel is an extremely important goal. Despite comprising as little as 0.1% of the total
CASE PRESENTATION. DR.Sravani 1 st yr PG Dept of Ophthalmology
 CASE PRESENTATION DR.Sravani 1 st yr PG Dept of Ophthalmology Name : X X X X X Age : 50yrs Sex : male Occupation : Farmer Residence : Mothkur CHIEF COMPLAINTS : - Diminision of vision in Right Eye since
CASE PRESENTATION DR.Sravani 1 st yr PG Dept of Ophthalmology Name : X X X X X Age : 50yrs Sex : male Occupation : Farmer Residence : Mothkur CHIEF COMPLAINTS : - Diminision of vision in Right Eye since
DISCLOSURES. PEDIATRIC RED EYES Rachel M. Smith, OD, FCOVD HISTORY, HISTORY, HISTORY WHY RED EYES? EXAMINE THE EYE RED FLAGS TO REFER 3/25/2019
 DISCLOSURES Consultant/Speakers bureaus Research funding PEDIATRIC RED EYES Rachel M. Smith, OD, FCOVD Pediatric Optometrist Children s Hospital & Medical Center Stock ownership/corporate boards employment
DISCLOSURES Consultant/Speakers bureaus Research funding PEDIATRIC RED EYES Rachel M. Smith, OD, FCOVD Pediatric Optometrist Children s Hospital & Medical Center Stock ownership/corporate boards employment
CORNEAL CONDITIONS CORNEAL TRANSPLANTATION
 GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
Ocular Injuries. Chapter 14
 Ocular Injuries Chapter 14 Ocular Injuries Introduction The preservation of the eyes and eyesight of service personnel is an extremely important goal. Despite comprising as little as 0.1% of the total
Ocular Injuries Chapter 14 Ocular Injuries Introduction The preservation of the eyes and eyesight of service personnel is an extremely important goal. Despite comprising as little as 0.1% of the total
OPHTHALMOLOGIC PEARLS FOR THE NON- OPHTHALMOLOGIST. David G. Gross D.O. Deen-Gross Eye Centers Merrillville-Hobart Deengrosseye.
 OPHTHALMOLOGIC PEARLS FOR THE NON- OPHTHALMOLOGIST David G. Gross D.O. Deen-Gross Eye Centers Merrillville-Hobart Deengrosseye.com A FEW OF THE AREAS WE WILL DISCUSS Red Eye Glaucoma Neuro ophthalmic tid
OPHTHALMOLOGIC PEARLS FOR THE NON- OPHTHALMOLOGIST David G. Gross D.O. Deen-Gross Eye Centers Merrillville-Hobart Deengrosseye.com A FEW OF THE AREAS WE WILL DISCUSS Red Eye Glaucoma Neuro ophthalmic tid
Telephone Triage Urgency or Emergency? Mary E. Schmidt, ABOC, CPO
 Telephone Triage Urgency or Emergency? www.eyesystems.info Mary E. Schmidt, ABOC, CPO mary@eyesystems.info Definition of Triage The sorting of patient and allocation of care or treatment according to the
Telephone Triage Urgency or Emergency? www.eyesystems.info Mary E. Schmidt, ABOC, CPO mary@eyesystems.info Definition of Triage The sorting of patient and allocation of care or treatment according to the
Around The Globe in 60 Minutes
 Around The Globe in 60 Minutes Around the GLOBE in Sixty Minutes Basic Ocular Anatomy, Examination, and Diagnostic Techniques Introduction Focusing on canine and feline ocular anatomy and basic examination
Around The Globe in 60 Minutes Around the GLOBE in Sixty Minutes Basic Ocular Anatomy, Examination, and Diagnostic Techniques Introduction Focusing on canine and feline ocular anatomy and basic examination
Scrub In. What is the function of vitreous humor? What does the pupil do when exposed to bright light? a. Maintain eye shape and provide color vision
 Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
TRAUMA, TRAUMA A YOUNG PARENT WOULD HAVE HEARD THE TITLE AND IMMEDIATELY THOUGHT 10/24/2018 JAMES LEE, M.D., ASSISTANT PROFESSOR TECHNICIAN CONFERENCE
 TRAUMA, TRAUMA JAMES LEE, M.D., ASSISTANT PROFESSOR TECHNICIAN CONFERENCE OCT 26, 2018 A YOUNG PARENT WOULD HAVE HEARD THE TITLE AND IMMEDIATELY THOUGHT 1 GROSS PICTURES LET S START WITH EYELIDS Lacerations
TRAUMA, TRAUMA JAMES LEE, M.D., ASSISTANT PROFESSOR TECHNICIAN CONFERENCE OCT 26, 2018 A YOUNG PARENT WOULD HAVE HEARD THE TITLE AND IMMEDIATELY THOUGHT 1 GROSS PICTURES LET S START WITH EYELIDS Lacerations
Examining Children s Eyes
 Paediatric Ophthalmology What to refer & when? Aims Tips for assessing a child s eyes in general practice Common paediatric ophthalmology symptoms and signs What needs to be referred and when? MISS FARIHA
Paediatric Ophthalmology What to refer & when? Aims Tips for assessing a child s eyes in general practice Common paediatric ophthalmology symptoms and signs What needs to be referred and when? MISS FARIHA
SILA THONGLAI MD. Bangkok Eye center Bangkok Hospital Thailand
 SILA THONGLAI MD. Bangkok Eye center Bangkok Hospital Thailand Ocular Anatomy Bony Components of Orbit 1 1. Frontal bone 4 5 7 6 2. Zygomatic bone 3. Maxillary bone 4. Sphenoid bone 5. Ethmoid bone 2 3
SILA THONGLAI MD. Bangkok Eye center Bangkok Hospital Thailand Ocular Anatomy Bony Components of Orbit 1 1. Frontal bone 4 5 7 6 2. Zygomatic bone 3. Maxillary bone 4. Sphenoid bone 5. Ethmoid bone 2 3
Probe Selection A high frequency (7-12 MHz) linear array transducer should be used to visualize superficial structures (Image 1).
 ! Teresa S. Wu, MD, FACEP Director, Emergency Ultrasound Program & Fellowships Co-Director, Women s Imaging Fellowship Maricopa Medical Center Associate Professor, Emergency Medicine Director, Simulation
! Teresa S. Wu, MD, FACEP Director, Emergency Ultrasound Program & Fellowships Co-Director, Women s Imaging Fellowship Maricopa Medical Center Associate Professor, Emergency Medicine Director, Simulation
Ocular Lecture. Sue Bednar NP Ali Atwater PA-C
 Ocular Lecture Sue Bednar NP Ali Atwater PA-C Triaging Ocular Complaints Painful Eye/Red eye +/-blurry vision +/-visual loss +/-floaters +/-fevers If any of the above findings exist, pt is likely to have
Ocular Lecture Sue Bednar NP Ali Atwater PA-C Triaging Ocular Complaints Painful Eye/Red eye +/-blurry vision +/-visual loss +/-floaters +/-fevers If any of the above findings exist, pt is likely to have
Frequently Asked Questions about General Ophthalmology:
 1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
Dr Jo-Anne Pon. Dr Sean Every. 8:30-9:25 WS #70: Eye Essentials for GPs 9:35-10:30 WS #80: Eye Essentials for GPs (Repeated)
 Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
Joint Theater Trauma System Clinical Practice Guideline
 INITIAL CARE OF OCULAR AND ADNEXAL INJURIES BY NON- OPHTHALMOLOGISTS AT ROLE 1, ROLE 2, and NON-OPHTHALMIC ROLE 3 FACILITIES Original Release/Approval 1 Aug 2007 Note: This CPG requires an annual review.
INITIAL CARE OF OCULAR AND ADNEXAL INJURIES BY NON- OPHTHALMOLOGISTS AT ROLE 1, ROLE 2, and NON-OPHTHALMIC ROLE 3 FACILITIES Original Release/Approval 1 Aug 2007 Note: This CPG requires an annual review.
Ocular Anatomy for the Paraoptometric
 Ocular Anatomy for the Paraoptometric Minnesota Optometric Association Paraoptometric CE Friday September 30, 2016 Lindsay A. Sicks, OD, FAAO Assistant Professor, Illinois College of Optometry lsicks@ico.edu
Ocular Anatomy for the Paraoptometric Minnesota Optometric Association Paraoptometric CE Friday September 30, 2016 Lindsay A. Sicks, OD, FAAO Assistant Professor, Illinois College of Optometry lsicks@ico.edu
Focusing on A&E. By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel
 Focusing on A&E By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel 01752 439331 Email sandra.cooper5@nhs.net sandracooper041@btinternet.com THINGS TO WORRY ABOUT WITH ANY EYE PROBLEM CHANGES IN VISION
Focusing on A&E By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel 01752 439331 Email sandra.cooper5@nhs.net sandracooper041@btinternet.com THINGS TO WORRY ABOUT WITH ANY EYE PROBLEM CHANGES IN VISION
Ocular Emergencies. Pisit Preechawat, MD Department of Ophthalmology, Ramathibodi Hospital
 Ocular Emergencies Pisit Preechawat, MD Department of Ophthalmology, Ramathibodi Hospital Ocular Anatomy Bony Components of Orbit 1 1. Frontal bone 4 5 7 6 2. Zygomatic bone 3. Maxillary bone 4. Sphenoid
Ocular Emergencies Pisit Preechawat, MD Department of Ophthalmology, Ramathibodi Hospital Ocular Anatomy Bony Components of Orbit 1 1. Frontal bone 4 5 7 6 2. Zygomatic bone 3. Maxillary bone 4. Sphenoid
ASSESSING THE EYES. Structures. Eyelids Extraocularmuscles Eyelashes Lacrimal glands: Lacrimal ducts Cornea Conjunctiva Sclera Pupils Iris.
 ASSESSING THE EYES Structures External Eyelids Extraocularmuscles Eyelashes Lacrimal glands: Lacrimal ducts Cornea Conjunctiva Sclera Pupils Iris 1 2 Structures Internal Optic disc Physiological cup Retinal
ASSESSING THE EYES Structures External Eyelids Extraocularmuscles Eyelashes Lacrimal glands: Lacrimal ducts Cornea Conjunctiva Sclera Pupils Iris 1 2 Structures Internal Optic disc Physiological cup Retinal
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Injury. Contusion Lamellar Laceration Laceration Rupture. Penetrating IOFB. Perforating
 Mechanical Ocular Trauma Došková Hana, MD. Department of Ophthalmology Medicine Faculty of Masaryk University Brno General Considerations Ocular trauma constitude about 6% of all injuries, but eyes set
Mechanical Ocular Trauma Došková Hana, MD. Department of Ophthalmology Medicine Faculty of Masaryk University Brno General Considerations Ocular trauma constitude about 6% of all injuries, but eyes set
Developed by Bradford J. Shingleton, MD, in conjunction with the Ophthalmology Liaisons Committee of the American Academy of Ophthalmology
 Developed by Bradford J. Shingleton, MD, in conjunction with the Ophthalmology Liaisons Committee of the American Academy of Ophthalmology Reviewer, 2009 Revision Mary A. O'Hara, MD Executive Editor, 2009
Developed by Bradford J. Shingleton, MD, in conjunction with the Ophthalmology Liaisons Committee of the American Academy of Ophthalmology Reviewer, 2009 Revision Mary A. O'Hara, MD Executive Editor, 2009
PAINFUL PAINLESS Contact lens user BOV
 Common Causes Allergies Infections Ocular Cornea, uveitis, endophthalmitis Orbital Orbital cellulitis Inflammation Uveitis Scleritis / episcleritis Glaucomas Trauma Foreign bodies Chemical injuries History
Common Causes Allergies Infections Ocular Cornea, uveitis, endophthalmitis Orbital Orbital cellulitis Inflammation Uveitis Scleritis / episcleritis Glaucomas Trauma Foreign bodies Chemical injuries History
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
By Darlene Jones, Nurse. May 2017
 By Darlene Jones, Nurse May 2017 Disclosure of potential conflict of interest Darlene Jones, Nurse I have no conflict of interest Course objectives Become familiar with the different pathologies in ophthalmology
By Darlene Jones, Nurse May 2017 Disclosure of potential conflict of interest Darlene Jones, Nurse I have no conflict of interest Course objectives Become familiar with the different pathologies in ophthalmology
Dry Eye Assessment and Management Study ELIGIBILITY OCULAR EVALUATION FORM
 Page 1 of 13 BEFORE COMPLETING THE OCULAR EXAMINATION, YOU MUST BE ABLE TO ANSWER YES TO THE FOLLOWING QUESTIONS: Have you done MMP9? (SVonly) The Following are done at Baseline: Have you done Tear Osmolarity?
Page 1 of 13 BEFORE COMPLETING THE OCULAR EXAMINATION, YOU MUST BE ABLE TO ANSWER YES TO THE FOLLOWING QUESTIONS: Have you done MMP9? (SVonly) The Following are done at Baseline: Have you done Tear Osmolarity?
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
Ophthalmology. Corneal Abrasion. History
 Ophthalmology Corneal Abrasion - Usually clear history of very recent trauma - Foreign Body Sensation - Pain +++ - Lacrimation - Photophobia Fig. 1 Corneal Abrasion - Abrasion stains yellow / green with
Ophthalmology Corneal Abrasion - Usually clear history of very recent trauma - Foreign Body Sensation - Pain +++ - Lacrimation - Photophobia Fig. 1 Corneal Abrasion - Abrasion stains yellow / green with
Basic microsurgical suturing techniques for beginners
 ESCRS 2014 Basic microsurgical suturing techniques for beginners Trauma, sclera, trabeculectomy B.O. Bachmann Dept. of Ophthalmology, University of Cologne, Germany Financial interests: none Investigating
ESCRS 2014 Basic microsurgical suturing techniques for beginners Trauma, sclera, trabeculectomy B.O. Bachmann Dept. of Ophthalmology, University of Cologne, Germany Financial interests: none Investigating
Flashers and Floaters
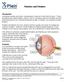 Flashers and Floaters Introduction Sometimes people see small, moving spots or specks in their field of vision. These sensations are called floaters. About 7 out of 10 people experience floaters at some
Flashers and Floaters Introduction Sometimes people see small, moving spots or specks in their field of vision. These sensations are called floaters. About 7 out of 10 people experience floaters at some
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg
 An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI. Monitor the vital signs. Monitor the vital signs. Complications of Facial Traumas.
 Complications of Facial Traumas 1) Immediate Complications 2) Late Complications Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor Oral & Maxillofacial Surgeon Taibah University Monitor
Complications of Facial Traumas 1) Immediate Complications 2) Late Complications Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor Oral & Maxillofacial Surgeon Taibah University Monitor
For further reading we recommend the following excellent textbooks:
 FURTHER READING Intravitreal Injections Downloaded from www.worldscientific.com For further reading we recommend the following excellent textbooks: Clinical Anatomy of the Eye by Richard S Snell and Michael
FURTHER READING Intravitreal Injections Downloaded from www.worldscientific.com For further reading we recommend the following excellent textbooks: Clinical Anatomy of the Eye by Richard S Snell and Michael
I Spy A Red Eye: Assessment & Management of Common Ocular Conditions In Primary Care
 I Spy A Red Eye: Assessment & Management of Common Ocular Conditions Jody Agins MSN, RNP, FNP/GNP-BC mrsjaginsnp@gmail.com Objectives Review procedures for assessment of conjunctival inflammation Differentiate
I Spy A Red Eye: Assessment & Management of Common Ocular Conditions Jody Agins MSN, RNP, FNP/GNP-BC mrsjaginsnp@gmail.com Objectives Review procedures for assessment of conjunctival inflammation Differentiate
Pediatric Ophthalmic Infections and Injuries Honey Herce, MD
 Pediatric Ophthalmic Infections and Injuries Honey Herce, MD Assistant Professor in the Department of Ophthalmology Texas Children's Hospital Baylor College of Medicine Pediatric Ophthalmic Infections
Pediatric Ophthalmic Infections and Injuries Honey Herce, MD Assistant Professor in the Department of Ophthalmology Texas Children's Hospital Baylor College of Medicine Pediatric Ophthalmic Infections
Post- interven+on data and new pro forma. Improving the management of pa0ents with acute red eyes in a large London Accident and Emergency Department
 Post- interven+on data and new pro Improving the management of paents with acute red eyes in a large London Accident and Emergency Department Rela+onship between the use of clerking pro s for pa+ents with
Post- interven+on data and new pro Improving the management of paents with acute red eyes in a large London Accident and Emergency Department Rela+onship between the use of clerking pro s for pa+ents with
Learn Connect Succeed. JCAHPO Regional Meetings 2017
 Learn Connect Succeed JCAHPO Regional Meetings 2017 Intravitreal Injection Technique Updated Recommendations from an Expert Panel Sophie J. Bakri, M.D. Professor of Ophthalmology Vitreoretinal Diseases
Learn Connect Succeed JCAHPO Regional Meetings 2017 Intravitreal Injection Technique Updated Recommendations from an Expert Panel Sophie J. Bakri, M.D. Professor of Ophthalmology Vitreoretinal Diseases
THE 35 GOLDEN EYE RULES
 THE 35 GOLDEN EYE RULES The Sense of Sight, from La Dame a la Licorne, The Lady and the Unicorn Tapestries, Late 15th Century Flemish Tapestry in wool and silk, Musée Nationale du Moyen Age, Paris. 1.
THE 35 GOLDEN EYE RULES The Sense of Sight, from La Dame a la Licorne, The Lady and the Unicorn Tapestries, Late 15th Century Flemish Tapestry in wool and silk, Musée Nationale du Moyen Age, Paris. 1.
LECTURE # 7 EYECARE REVIEW: PART III
 LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Complete Visual Rehabilitation in a Patient with No Light Perception after Surgical Management of a Penetrating Open-Globe Injury: A Case Report
 Published online: June 23, 2015 1663 2699/15/0062 0204$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: June 23, 2015 1663 2699/15/0062 0204$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
generic name brand name duration
 SLIT LAMP MICROSCOPY SKILL SESSION The evaluation of all eye complaints begins with the history. All patients with eye complaints should have their visual acuity checked. Tetanus status R/O alkali/chemical
SLIT LAMP MICROSCOPY SKILL SESSION The evaluation of all eye complaints begins with the history. All patients with eye complaints should have their visual acuity checked. Tetanus status R/O alkali/chemical
Faculty Financial Disclosure. Learning Objectives: Office Ophthalmology. Basic Eye Exam: What s in your pocket/office? Office Ophthalmology
 Faculty Financial Disclosure Office Ophthalmology Lynn K. Gordon, MD, PhD, has no financial relationships to disclose. Lynn K. Gordon, MD, PhD Professor and Vernon O Underwood Family Chair Department of
Faculty Financial Disclosure Office Ophthalmology Lynn K. Gordon, MD, PhD, has no financial relationships to disclose. Lynn K. Gordon, MD, PhD Professor and Vernon O Underwood Family Chair Department of
Wildlife Ophthalmology D R. H E A T H E R R E I D T O R O N T O W I L D L I F E C E N T R E T O R O N T O, O N C A N A D A
 Wildlife Ophthalmology D R. H E A T H E R R E I D T O R O N T O W I L D L I F E C E N T R E T O R O N T O, O N C A N A D A Why understand eyes? Wildlife need to have excellent vision to survive in the
Wildlife Ophthalmology D R. H E A T H E R R E I D T O R O N T O W I L D L I F E C E N T R E T O R O N T O, O N C A N A D A Why understand eyes? Wildlife need to have excellent vision to survive in the
Facial Trauma. Facial Trauma. Facial Trauma
 Facial Trauma Facial Trauma Brian Bast DMD, MD Department of Oral and Maxillofacial Surgery University of California, San Francisco School of Dentistry Brian Bast DMD, MD Department of Oral and Maxillofacial
Facial Trauma Facial Trauma Brian Bast DMD, MD Department of Oral and Maxillofacial Surgery University of California, San Francisco School of Dentistry Brian Bast DMD, MD Department of Oral and Maxillofacial
Traumatic Partial Optic Nerve Avulsion with Globe luxation. Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine
 Traumatic Partial Optic Nerve Avulsion with Globe luxation Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine A 23 year old male patient presented to the emergency department in
Traumatic Partial Optic Nerve Avulsion with Globe luxation Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine A 23 year old male patient presented to the emergency department in
Glaucoma. Cornea. Iris
 Glaucoma Introduction Glaucoma is a group of eye diseases that can lead to blindness if not treated. Openangle glaucoma, the most common form of glaucoma, affects about 3 million Americans. Half of those
Glaucoma Introduction Glaucoma is a group of eye diseases that can lead to blindness if not treated. Openangle glaucoma, the most common form of glaucoma, affects about 3 million Americans. Half of those
Conjunctival Hemorrhage
 IN THE NAME OF GOD Lid Laceration Conjunctival Hemorrhage a) No therapy is necessary b) Usually resolve in 7-12 days. Subconjunctival Hemorrhage Corneal Abrasion Abrasions Many small abrasions can
IN THE NAME OF GOD Lid Laceration Conjunctival Hemorrhage a) No therapy is necessary b) Usually resolve in 7-12 days. Subconjunctival Hemorrhage Corneal Abrasion Abrasions Many small abrasions can
Eye Examination Techniques in Horses
 Eye Examination Techniques in Horses Dennis E. Brooks DVM, PhD Dip ACVO University of Florida brooksd@mail.vetmed.ufl.edu Basic Instruments How to tell the potential of vision? PLRs (retina, CN 2, chiasm,
Eye Examination Techniques in Horses Dennis E. Brooks DVM, PhD Dip ACVO University of Florida brooksd@mail.vetmed.ufl.edu Basic Instruments How to tell the potential of vision? PLRs (retina, CN 2, chiasm,
Index. C Canalicular system, 4 Carbonic anhydrase inhibitors, 29 30
 A Acanthamoeba keratitis (AK), 82, 83 Acute angle-closure crisis, 156 Acute angle-closure glaucoma (AACG), 121, 141, 284 causes of, 122 clinical presentation, 153 evaluation, 156 157 management/treatment,
A Acanthamoeba keratitis (AK), 82, 83 Acute angle-closure crisis, 156 Acute angle-closure glaucoma (AACG), 121, 141, 284 causes of, 122 clinical presentation, 153 evaluation, 156 157 management/treatment,
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line.
 Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
DEFINITION Corneal abrasion is a defect in the corneal surface epithelium due to scraping or rubbing of the corneal epithelium.
 DEFINITION Corneal abrasion is a defect in the corneal surface epithelium due to scraping or rubbing of the corneal epithelium. IMMEDIATE CONSULTATION REQUIRED IN THE FOLLOWING SITUATIONS Dendritic pattern
DEFINITION Corneal abrasion is a defect in the corneal surface epithelium due to scraping or rubbing of the corneal epithelium. IMMEDIATE CONSULTATION REQUIRED IN THE FOLLOWING SITUATIONS Dendritic pattern
TRAUMA TO THE FACE AND MOUTH
 Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
OPHTHALMOLOGY AND ULTRASOUND
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk OPHTHALMOLOGY AND ULTRASOUND Author : JAMES OLIVER Categories : Vets Date : April 28, 2008 JAMES OLIVER discusses why ultrasound
Vet Times The website for the veterinary profession https://www.vettimes.co.uk OPHTHALMOLOGY AND ULTRASOUND Author : JAMES OLIVER Categories : Vets Date : April 28, 2008 JAMES OLIVER discusses why ultrasound
Sense of Vision. Chapter 8. The Eye and Vision. The Eye Orbit. Eyebrows, Eyelids, Eyelashes. Accessory Organs 5/3/2016.
 Sense of Vision Chapter 8 Special Senses The Eye and Vision 70 percent of all sensory receptors are in the eyes Each eye has over 1 million nerve fibers Protection for the eye Most of the eye is enclosed
Sense of Vision Chapter 8 Special Senses The Eye and Vision 70 percent of all sensory receptors are in the eyes Each eye has over 1 million nerve fibers Protection for the eye Most of the eye is enclosed
Andrew J. Hendershot, MD Havener Eye Institute The Ohio State University s Wexner Medical Center
 Ocular Trauma for the Primary Care Physician Andrew J. Hendershot, MD Havener Eye Institute The Ohio State University s Wexner Medical Center Relevance Often those with minor eye injuries will first seek
Ocular Trauma for the Primary Care Physician Andrew J. Hendershot, MD Havener Eye Institute The Ohio State University s Wexner Medical Center Relevance Often those with minor eye injuries will first seek
10 EYE EMERGENCIES. Who goes, who you better not send! Brant Slomovic, MD, FRCPC University Health Network
 10 EYE EMERGENCIES Who goes, who you better not send! Brant Slomovic, MD, FRCPC University Health Network DISCLOSURES I have none PVD CASE 1 WHAT IS A PVD? a process of aging (45-55) liquefaction of vitreous
10 EYE EMERGENCIES Who goes, who you better not send! Brant Slomovic, MD, FRCPC University Health Network DISCLOSURES I have none PVD CASE 1 WHAT IS A PVD? a process of aging (45-55) liquefaction of vitreous
Phone Triage for Optometric Staff ???????? CHEMICAL BURN CHEMICAL BURN
 Phone Triage for Optometric Staff There are very few ocular emergencies that you will have to deal with in practice, but it is imperative that you be able to Michelle Welch, O.D. NSU Oklahoma College of
Phone Triage for Optometric Staff There are very few ocular emergencies that you will have to deal with in practice, but it is imperative that you be able to Michelle Welch, O.D. NSU Oklahoma College of
Identify the choice that best completes the statement or answers the question.
 Chapter 5. The Eye Multiple Choice Identify the choice that best completes the statement or answers the question. 1. The most common type of eye disorder is: A. Refractive errors B. Macular conditions
Chapter 5. The Eye Multiple Choice Identify the choice that best completes the statement or answers the question. 1. The most common type of eye disorder is: A. Refractive errors B. Macular conditions
Ocular trauma. Abstract. Introduction. Approach to the patient. CPD Article: Ocular trauma
 Ocular trauma Abstract Mustak H, MBChB, DipOphth(SA), Registrar Division of Ophthalmology, Groote Schuur Hospital; University of Cape Town Du Toit N, MBChB, DipOphth(SA), FRCS(Ed), FCOphth(SA), MMed, Consultant
Ocular trauma Abstract Mustak H, MBChB, DipOphth(SA), Registrar Division of Ophthalmology, Groote Schuur Hospital; University of Cape Town Du Toit N, MBChB, DipOphth(SA), FRCS(Ed), FCOphth(SA), MMed, Consultant
Ocular Trauma. Authors Dr Shrinkhal 1, Dr Kamya Sharma 2
 International Journal of Emerging Trends in Science and Technology IC Value: 76.89 (Index Copernicus) Impact Factor: 2.838 DOI: https://dx.doi.org/10.18535/ijetst/v3i12.01 Ocular Trauma Authors Dr Shrinkhal
International Journal of Emerging Trends in Science and Technology IC Value: 76.89 (Index Copernicus) Impact Factor: 2.838 DOI: https://dx.doi.org/10.18535/ijetst/v3i12.01 Ocular Trauma Authors Dr Shrinkhal
