Ocular Trauma. Authors Dr Shrinkhal 1, Dr Kamya Sharma 2
|
|
|
- Eleanore Walton
- 5 years ago
- Views:
Transcription
1 International Journal of Emerging Trends in Science and Technology IC Value: (Index Copernicus) Impact Factor: DOI: Ocular Trauma Authors Dr Shrinkhal 1, Dr Kamya Sharma 2 1 Junior Resident, 2 Senior Resident Department of Ophthalmology, Institute of Medical Sciences, BHU, Varanasi , U.P., INDIA ABSTRACT Ocular trauma is one of the important causes of unilateral blindness and visual impairment across the world. In developed countries, most injuries are accidental, while assaults predominate as a cause in developing countries. Trauma may result in various forms of ocular injuries, ranging from minor insult to major functional impairment. Any ocular structure may be involved, and a careful, systematic approach to the examination of a patient is essential to avoid missing occult injury and resultant visual impairment. KEYWORDS: Lacerations of the eyelids, foreign bodies, corneal abrasions and erosions, globe rupture, chemical injury. INTRODUCTION Trauma is the most important cause of unilateral blindness in the world [1,2]. Up until the end of the last century, it accounted for approximately 1.6 million cases of blindness, 2.3 million cases of bilateral visual impairment and 19 million cases of unilateral vision loss worldwide [1]. The cause of the injuries varies. Work-related accidental injuries are prevalent in developing countries, while assaults are an important cause in developing countries [1,2,3]. Males are at higher risk than females (4:1). Most commonly involved age group is between years [2]. Injuries range from mild to severe, and can affect any anatomical structure of the eye. Quick assessment and expert management is very essential to preserve the vision. Approach to the Patient The evaluation of ocular trauma should include a focused history, systematic examination and appropriate special investigations. A good detailed history is valuable in anticipating and determining the nature and severity of the injury. Many injuries occur in the workplace. It is important to obtain information on the circumstances of the incident, as well as the use of appropriate protective eyewear [4,5]. The mechanism and object involved inform the nature of the tissue destruction. Blunt objects result in tissue contusion, and if severe, may cause globe rupture, while sharp objects cause lacerating and penetrating injuries. The exact time of the injury is also important in determining the treatment strategy [5]. It is important to remember that any anatomical structure may be involved. Basic evaluation involves inspection, which may be facilitated by the use of local anaesthetic drops and a speculum (if lid swelling is present). Visual acuity should be measured and documented as it is the most informative measure of ocular function, and is a prognostic factor in severe ocular trauma [4,5]. Eye movements should then be checked to determine deficits in ocular motility. An ocular movement exam should be omitted if the patient is suspected of having an open globe injury, in order to prevent prolapse of the intraocular contents. Each anatomical structure of the eye should then be examined with the aid of a good light source. Examination should begin with the lids and skin, Dr Shrinkhal et al Page 4794
2 followed by careful examination of the conjunctiva, cornea and sclera. If a corneal abrasion is suspected, the instillation of fluorescein drops will help to confirm the diagnosis [4]. Pupil responses should be tested and a note made on the presence of a relative afferent pupil defect. It should then be determined if there is red reflex, followed by fundoscopy. Imaging is a useful adjunct for further evaluation of the patient. Following blunt trauma, orbital and skull X-rays are useful in confirming fractures of the orbital wall and cranium. Orbital X-rays are also useful in verifying the presence and location of intraocular foreign bodies. Patients who have sustained penetrating injuries will require a computed tomography (CT) scan of the head to exclude possible intracranial injury [4,5]. Minor injuries can be managed at primary care level, while severe injuries require referral to a specialist for further treatment. Common eye injuries: Lacerations of the eyelids (Figure 1) The eyelids may be lacerated or avulsed, depending on the object causing injury like with sharp object, laceration occurs and by blunt object injury avulsion occurs [6,7]. These injuries may or may not involve the lid margin. Human and dog bites to the eye can also cause tissue loss, requiring the need for tissue grafting [5,7]. All three layers of the lid (skin, orbicularis and tarsal plate) may be involved. Repair requires careful anatomical realignment of these structures to prevent lid notching [5]. It is important to exclude possible globe penetration [5,7] in cases of sharp object injury, particularly in the presence of a fullthickness laceration. Lacerations involving the medial canthal area may also involve the nasolacrimal apparatus, leading to a chronic watery eye if not repaired [5,6]. Lacerations resulting in full-thickness injury, and its improper surgical management leads to incorrect realignment of the tarsal plate which may result in a lid margin notch which can cause chronic corneal irritation and scarring [5]. Abnormal Eye Movements Blunt or sharp injury can lead to abnormal ocular movements. It can be due to direct injury to the extraocular muscles (contusion or laceration), or due to mechanical infringement on the muscle (haematoma, blowout fracture or an orbital foreign body) [4]. Subperiosteal haematoma is a result of bleeding into the subperiosteal space, commonly following blunt trauma in children and young adults. Classical presentation is with downward proptosis, with an otherwise normal eye. A CT scan is useful to confirm the diagnosis and visualise the blood collection. Patients should be referred for drainage of the collection [4]. Blowout fractures result from blunt-force injury to the orbit, the transmitted force causing fracture of the weakest points of the orbit, mainly the floor and medial wall [4,8]. Clinically, the patient will have elevation deficit (due to entrapment of the inferior rectus in the fracture), loss of sensation at areas supplied by infraorbital nerve and subcutaneous crepitus [4]. Facial X-rays or a CT scan will show opacification of the maxillary sinus due to herniation of the orbital contents and [8] entrapment of the inferior rectus with characterstic tear drop sign. The patient should be referred to an ophthalmologist or maxillofacial surgeon for repair. Orbital foreign bodies can also cause mechanical restriction [4,8]. The limitation of movement will depend on the site of the foreign body and the affected muscles. A CT scan is investigation of choice to detect the presence of an orbital foreign body. Patients should be referred for removal of the foreign body. Dr Shrinkhal et al Page 4795
3 Foreign Bodies (Figure 2): Common activities resulting in ocular injuries by foreign bodies are grinding, hammering, drilling and sawing. Foreign bodies can either be found on the conjunctiva (bulbar and tarsal) or cornea (Figure), or may be intraocular. It is important to take a detailed history of the exact mechanism of injury and materials involved in order to know what type of injury to expect [3,4,6]. Activities such as grinding result in low-velocity projectiles which often embed in the conjunctiva or cornea, while higher-velocity shrapnel, e.g. from hammering, is more likely to penetrate the globe and lodge intraocularly [4]. Patients will complain of a foreign body sensation. The affected eye will be red, painful and photophobic. The foreign body may be clearly seen as a dark spot on the conjunctiva or cornea (Figure). It may also be lodged in the tarsal conjunctiva, and can be missed if the lids (especially the upper lid) are not everted [4,6]. Fluorescein staining is useful in these cases when searching for linear corneal abrasions that may result from a subtarsal foreign body rubbing against the cornea. Conjunctival foreign bodies may be removed with a 26 G needle, following the instillation of local anaesthetic drops. Corneal foreign bodies may be removed similarly after liberal use of topical anaesthesia. If the foreign body persists, then the patient should be referred to an ophthalmologist. X-rays (or a CT scan, if available) are useful imaging modalities to confirm diagnosis and the location of an intraocular foreign body. Cases of intraocular foreign bodies must be referred to an ophthalmologist for further management. Missed foreign bodies can result in conditions such as endophthalmitis, particularly if organic matter is involved, or siderosis bulbi, if iron is involved [4,6]. Metallic foreign bodies, particularly iron and copper, are toxic to the retina and cause yellowbrown discolouration of the ocular tissue. Corneal abrasions and erosions (Figure 3): Abrasions and erosions of the cornea are very common ocular injuries [6,9]. Abrasions are caused by scratches from minor trauma, i.e. by fingernails and sand. Erosions occurs as a result of excessive ultraviolet (UV) exposure, with resultant epithelial damage, such as due to tanning on sunbeds, without wearing protective goggles. These lesions tend to be painful as a result of epithelial loss and exposure of the underlying nerve endings [4]. Patients present with a history of minor trauma to the eye or of excessive UV exposure. The affected eye or eyes are red and painful, and there is excessive lacrimation [4,9]. Fluorescein drops should be instilled to allow confirmation of the epithelial injury. A single linear defect is often seen in abrasions, while erosions tend to result in multiple punctate lesions [4]. Corneal epithelial recovery is rapid, and the management of abrasions and erosions essentially involves pain relief and infection prevention [4,6,9]. Cycloplegics should be prescribed to relieve associated ciliary spasm, analgesics for pain, and antibiotic ointment used as prophylaxis against secondary infection, while padding of the eyewill reduce discomfort from blinking and may aid corneal healing [4]. They must be advised to wear UV protection as a preventative measure. While local anaesthetic drops provide immediate pain relief, they should not be prescribed for patients to take home. A local anaesthetic inhibits corneal healing, and will make the patient unaware of any further insult to the cornea [4,9]. Dr Shrinkhal et al Page 4796
4 Penetrating injury or globe rupture (Figure 4): A sharp or severe blunt injury can result in globe disruption [4,10]. Most injuries will be easily detected on simple inspection. However, some injuries can be notorious to detect, if there is not a high index of suspicion, then sight-threatening injuries may be missed [4,5]. Signs of globe disruption include reduced visual acuity, distortion or an abnormally shaped pupil with poor pupillary response (D-shaped pupil due to iridodialysis), prolapse of the uveal tissue at the wound site, poor red reflex as a result of vitreous haemorrhage, hyphaema (blood in the anterior chamber) or retinal detachment, and an anterior chamber that appears deeper than the normal, fellow eye [4,5,10]. A high index of suspicion of globe penetration must be maintained for full-thickness lid lacerations, as well as sharp object injuries around the periorbita [4]. Management requires referral to an ophthalmologist within 24 hours for globe repair. While awaiting ophthalmology referral, drops should not be instilled in the eye. This is to prevent potentially toxic preservatives from affecting exposed intraocular tissue. A shield should be placed over the eye, without an underlying pressure dressing, in order to avoid further prolapse of intraocular content [4]. Patients with open globe injuries will require a CT scan of the head to exclude retained foreign material, as well as intracranial injury. Traumatic vascular events (Figure 5): Subconjunctival haemorrhage is common after minor trauma, coughing or valsalva manoeuvres [4]. It can also occur spontaneously in patients with hypertension, bleeding diathesis or those on anticoagulant medication [6]. It presents as a red area on the bulbar conjunctiva, which is easily identifiable as blood. It is usually painless. Management is often conservative provided the visual acuity, pupillary response, eye movements and fundus examination are all normal, and there are no signs of globe rupture. Patients with bilateral subconjunctival haemorrhage and an inability to identify the posterior extent thereof may be associated with an anterior base-of-skull fracture [4]. Hyphaema usually occurs after blunt trauma, and its severity can vary from mild to an anterior chamber filled with blood; the so-called 8-ball hyphaema [4,11]. Vision may be reduced according to the severity of the injury. Patients may experience pain, particularly if the intraocular pressure is raised. Most commonly, a fluid level of settled blood can be seen in the inferior part of the anterior chamber. Hyphaema can be complicated by a rebleed which most commonly occurs in the first five days following the initial bleed, and blood may also obstruct the trabecular meshwork, resulting in elevation of the intraocular pressure [4,11]. Prolonged raised intraocular pressure may result in corneal staining and optic atrophy. Thus, patients must be referred to an ophthalmologist within 24 hours to avoid these complications. Carotid cavernous fistula most commonly occurs as a result of penetrating eye injury, but may Dr Shrinkhal et al Page 4797
5 follow blunt trauma, particularly with base-ofskull fractures. There is direct arteriovenous communication between the internal carotid artery and the cavernous sinus. Patients present with conjunctival chemosis and dilated vessels, a pulsatile proptosis and a bruit on auscultation. A CT angiogram will confirm the diagnosis, and these patients require neurosurgical referral for embolisation of the fistula in order to prevent glaucoma, optic nerve and retinal damage [4]. Blunt injury or penetrating injury to lens can lead to cataract also (Figure) and coming of lens matter in anterior chamber (Figure). Lens particles in anterior chamber may block trabecular outflow leading to raised intraocular pressure. Lens AND Iris injuries: Blunt trauma, can result in iris sphincter and lens zonular injury [12]. The lens may then become partially displaced (subluxated) within the pupillary zone (Figure), or dislocate completely (Figure), either into the vitreous or the anterior chamber [4,12]. Anterior lens dislocation can cause trabecular outflow obstruction leading to elevated intraocular pressure. If it is observed that the lens has dislocated into the anterior chamber, and the eye feels hard and the patient has pain, referral to an ophthalmologist is necessary, usually within 24 hours for lens extraction [4]. Acetazolamide 500 mg BD orally should be administered in these cases, until an ophthalmologist sees. Iris injuriy can lead to Iridodialysis (Figure), Cyclodialysis. In these isolated cases, there will be decreased IOP due to increases aqueous outflow. Dr Shrinkhal et al Page 4798
6 Chemical Injury Chemical injuries most commonly occur in the workplace when adequate eye protection is not used [4,6,13]. Immediate management should be instituted prior to referral to an ophthalmologist for formal assessment [4,6]. The most common offending agents are alkaline in nature (commonly detergents and cleaning agents), followed by acids and particulate chemicals [13]. Alkalis are more likely to result in serious ocular damage (Figure) since these agents can readily diffuse through the cornea by saponification to cause intraocular damage. Acidic agents tend to cause surface coagulation which prevents further penetration [4,13]. Chemical damage can range from mild to severe corneal and intraocular injury, resulting in visual loss. Roper Hall classification is used for grading the injury. The mainstay of treatment is copious irrigation of the affected eye [4,13]. Local anaesthetic drops should be instilled. The lids may need to be held open and the eye irrigated for at least 30 minutes. If readily available, litmus or ph sticks can be used to determine the nature of the agent, but this should not delay irrigation. The fornices must be swept with a cotton bud to remove particulate matter. Patients should then be urgently referred to an ophthalmologist for further evaluation and management. Conclusion Ocular trauma is an important cause of visual impairment and unilateral blindness. The majority of injuries tends to be minor and can be managed in the primary healthcare setting. Knowledge of ocular anatomy, as well as careful examination, is crucial in the identification of vision threatening injuries. Features of severe injury include marked visual loss and a relative afferent pupil defect. Imaging modalities should be used in cases of severe injuries as a routine. If there is any doubt as to the nature and extent of the injury, patients should be referred to an ophthalmologist. Acknowledgement We are thankful to all our teachers for their constant academic help and inspiration. References 1. Négrel AD, Thylefors B. The global impact of eye injuries. Ophthalmic Epidemiol. 1998; 5(3): Thylefors B. Epidemiological patterns of ocular trauma. Aust NZ J Ophthalmol. 1992;20(2): Kuhn F, Mester V, Morris R, Dalma J. Eye injury epidemiology and prevention of ophthalmic injuries. In: Kuhn F, editor. Ocular trauma: principles and practice. New York: Thieme, 2002; p Du Toit N, Cook C. Ocular trauma. Cape Town: Juta, 2009; p Kuhn F, Pieramici D. Designing the management strategy. In: Kuhn F, editor. Ocular trauma: principles and practice. New York: Thieme, 2002; p Khaw P, Shah P, Elkington A. Injury to the eye. BMJ. 2004;328(7430): Long J, Tan T. Eyelid and lacrimal system trauma. In: Kuhn F, editor. Ocular trauma: principles and practice. New York: Thieme, 2002; p Long J, Tan T. Orbital trauma. In: Kuhn F, editor. Ocular trauma: principles and practice. New York: Thieme, 2002; p Wipperman J, Dorsch J. Evaluation and management of corneal abrasions. Am Fam Physician. 2013;87(2): Dalma-Weiszhausz J. Extrabulbar tissue prolapse. In: Kuhn F, editor. Ocular trauma: principles and practice. New York: Thieme, 2002; p Dr Shrinkhal et al Page 4799
7 11. Walton W, Von Hagen S, Grigorian R, Zarbin M. Management of traumatic hyphema. Surv Ophthalmol. 2002;47(4): Mester V, Kuhn F. Lens. In: Kuhn F, editor. Ocular trauma: principles and practice. New York, Thieme, 2002; p Wagoner M, Kenyon K. Chemical injuies: clinical course and management. Ocular trauma: principles and practice. New York: Thieme, 2002; p Dr Shrinkhal et al Page 4800
Ocular trauma. Abstract. Introduction. Approach to the patient. CPD Article: Ocular trauma
 Ocular trauma Abstract Mustak H, MBChB, DipOphth(SA), Registrar Division of Ophthalmology, Groote Schuur Hospital; University of Cape Town Du Toit N, MBChB, DipOphth(SA), FRCS(Ed), FCOphth(SA), MMed, Consultant
Ocular trauma Abstract Mustak H, MBChB, DipOphth(SA), Registrar Division of Ophthalmology, Groote Schuur Hospital; University of Cape Town Du Toit N, MBChB, DipOphth(SA), FRCS(Ed), FCOphth(SA), MMed, Consultant
Assessment and Management of Ocular Trauma. Disclosure I have no direct financial interests in today s subject matter. 3/25/2019. Normal Eye Anatomy
 Assessment and Management of Ocular Trauma Samiksha Fouzdar Jain, MD,FRCS Department of Ophthalmology & Visual Sciences Truhlsen Eye Institute Disclosure I have no direct financial interests in today s
Assessment and Management of Ocular Trauma Samiksha Fouzdar Jain, MD,FRCS Department of Ophthalmology & Visual Sciences Truhlsen Eye Institute Disclosure I have no direct financial interests in today s
Management of specific eye problems in the ED
 of specific eye problems in the ED CORNEAL ABRASION Causes Foreign bodies Tangential shearing injuries, e.g. poking finger into eye Exact cause of injury (Remember to exclude possibility of intraocular
of specific eye problems in the ED CORNEAL ABRASION Causes Foreign bodies Tangential shearing injuries, e.g. poking finger into eye Exact cause of injury (Remember to exclude possibility of intraocular
Ocular and Periocular Trauma. Tina Rutar, MD. Assistant Professor of Ophthalmology and Pediatrics. Director, Visual Center for the Child
 Ocular and Periocular Trauma Tina Rutar, MD Assistant Professor of Ophthalmology and Pediatrics Director, Visual Center for the Child University of California, San Francisco Phone: 415-353-2560 Fax: 415-353-2468
Ocular and Periocular Trauma Tina Rutar, MD Assistant Professor of Ophthalmology and Pediatrics Director, Visual Center for the Child University of California, San Francisco Phone: 415-353-2560 Fax: 415-353-2468
EYE TRAUMA: INCIDENCE
 Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Ocular and periocular trauma
 Ocular and periocular trauma No financial disclosures. Tina Rutar M.D. Assistant Professor of Clinical Ophthalmology and Pediatrics Director, Visual Center for the Child University of California San Francisco
Ocular and periocular trauma No financial disclosures. Tina Rutar M.D. Assistant Professor of Clinical Ophthalmology and Pediatrics Director, Visual Center for the Child University of California San Francisco
Acute Eyes for ED. Enis Kocak. The Alfred Ophthalmology
 Acute Eyes for ED Enis Kocak The Alfred Ophthalmology The problem with eyes Things to cover Ocular anatomy Basic assessment Common presentations Eye first aid and procedures Ophthalmic emergencies What
Acute Eyes for ED Enis Kocak The Alfred Ophthalmology The problem with eyes Things to cover Ocular anatomy Basic assessment Common presentations Eye first aid and procedures Ophthalmic emergencies What
UC SF. g h. Eye Trauma. Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California
 UC SF Eye Trauma sf g h Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California Goals Recognize vision threatening eye emergencies Treat them when we can Know when
UC SF Eye Trauma sf g h Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California Goals Recognize vision threatening eye emergencies Treat them when we can Know when
Eye Trauma. Lid Laceration. Orbital Fracture
 Eye Trauma Lid Laceration The presence of a lid laceration, however insignificant, mandates careful exploration of the wound and examination of the globe. 1. Superficial lacerations parallel to the lid
Eye Trauma Lid Laceration The presence of a lid laceration, however insignificant, mandates careful exploration of the wound and examination of the globe. 1. Superficial lacerations parallel to the lid
Ocular Urgencies and Emergencies
 Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
MRI masterfile Part 5 WM Heme Strokes.ppt 1
 Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
Injury. Contusion Lamellar Laceration Laceration Rupture. Penetrating IOFB. Perforating
 Mechanical Ocular Trauma Došková Hana, MD. Department of Ophthalmology Medicine Faculty of Masaryk University Brno General Considerations Ocular trauma constitude about 6% of all injuries, but eyes set
Mechanical Ocular Trauma Došková Hana, MD. Department of Ophthalmology Medicine Faculty of Masaryk University Brno General Considerations Ocular trauma constitude about 6% of all injuries, but eyes set
EYE INJURIES OBJECTIVES COMMON EYE EMERGENCIES 7/19/2017 IMPROVE ASSESSMENT OF EYE INJURIES
 EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
Examining Children s Eyes
 Paediatric Ophthalmology What to refer & when? Aims Tips for assessing a child s eyes in general practice Common paediatric ophthalmology symptoms and signs What needs to be referred and when? MISS FARIHA
Paediatric Ophthalmology What to refer & when? Aims Tips for assessing a child s eyes in general practice Common paediatric ophthalmology symptoms and signs What needs to be referred and when? MISS FARIHA
Ophthalmic Trauma Update
 Ophthalmic Trauma Update Richard S. Davidson, M.D. Professor of Ophthalmology Vice Chair for Quality and Clinical Affairs UCHealth Eye Center University of Colorado School of Medicine August 5, 2017 Financial
Ophthalmic Trauma Update Richard S. Davidson, M.D. Professor of Ophthalmology Vice Chair for Quality and Clinical Affairs UCHealth Eye Center University of Colorado School of Medicine August 5, 2017 Financial
Focusing on A&E. By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel
 Focusing on A&E By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel 01752 439331 Email sandra.cooper5@nhs.net sandracooper041@btinternet.com THINGS TO WORRY ABOUT WITH ANY EYE PROBLEM CHANGES IN VISION
Focusing on A&E By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel 01752 439331 Email sandra.cooper5@nhs.net sandracooper041@btinternet.com THINGS TO WORRY ABOUT WITH ANY EYE PROBLEM CHANGES IN VISION
2/5/2018. Trauma. Subdivided into two main categories: Closed globe Open Globe
 1 2 3 4 5 Ocular Trauma Guide for Eye Care Office Staff Winter Thaw 2018 Aaron Yatskevich OD Definition A broad term used to describe a physical or chemical wound to the eye or eye socket. Ocular trauma
1 2 3 4 5 Ocular Trauma Guide for Eye Care Office Staff Winter Thaw 2018 Aaron Yatskevich OD Definition A broad term used to describe a physical or chemical wound to the eye or eye socket. Ocular trauma
PENETRATING EYE INJUIRES
 PENETRATING EYE INJUIRES King Harold receives a mortal penetrating injury to the eye at the Battle of Hastings 1066, Detail Bayeux Tapestry, Eleventh century. Then Earl William came from Normandy into
PENETRATING EYE INJUIRES King Harold receives a mortal penetrating injury to the eye at the Battle of Hastings 1066, Detail Bayeux Tapestry, Eleventh century. Then Earl William came from Normandy into
MRI masterfile Part 5 WM Heme Strokes.ppt 2
 Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS
 OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
Ocular Emergencies. What is an emergency to the patient is not necessarily an emergency to the staff
 OCULAR EMERGENCIES Ophthalmic Photographers Society November 15, 2013 Michael A. DellaVecchia MD PhD FACS Wills Eye Emergency Department Philadelphia PA Ocular Emergencies What is an emergency to the patient
OCULAR EMERGENCIES Ophthalmic Photographers Society November 15, 2013 Michael A. DellaVecchia MD PhD FACS Wills Eye Emergency Department Philadelphia PA Ocular Emergencies What is an emergency to the patient
PEDIATRIC OCULAR INJURIES. Sapna Tibrewal MD
 PEDIATRIC OCULAR INJURIES Sapna Tibrewal MD 1 Learning Objectives Learn to recognize the common pediatric ocular injuries Immediate management tips to be instituted in your office/ ER Know when to call
PEDIATRIC OCULAR INJURIES Sapna Tibrewal MD 1 Learning Objectives Learn to recognize the common pediatric ocular injuries Immediate management tips to be instituted in your office/ ER Know when to call
SILA THONGLAI MD. Bangkok Eye center Bangkok Hospital Thailand
 SILA THONGLAI MD. Bangkok Eye center Bangkok Hospital Thailand Ocular Anatomy Bony Components of Orbit 1 1. Frontal bone 4 5 7 6 2. Zygomatic bone 3. Maxillary bone 4. Sphenoid bone 5. Ethmoid bone 2 3
SILA THONGLAI MD. Bangkok Eye center Bangkok Hospital Thailand Ocular Anatomy Bony Components of Orbit 1 1. Frontal bone 4 5 7 6 2. Zygomatic bone 3. Maxillary bone 4. Sphenoid bone 5. Ethmoid bone 2 3
Ophthalmology. Corneal Abrasion. History
 Ophthalmology Corneal Abrasion - Usually clear history of very recent trauma - Foreign Body Sensation - Pain +++ - Lacrimation - Photophobia Fig. 1 Corneal Abrasion - Abrasion stains yellow / green with
Ophthalmology Corneal Abrasion - Usually clear history of very recent trauma - Foreign Body Sensation - Pain +++ - Lacrimation - Photophobia Fig. 1 Corneal Abrasion - Abrasion stains yellow / green with
5/2/2016 EYE EMERGENCIES. Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates. Anatomy. Tools
 EYE EMERGENCIES Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates Anatomy Tools 1 Contact dermatitis Blepharitis HSV Preseptal Cellulitis Anterior Chamber Subconjunctival hemorrhage
EYE EMERGENCIES Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates Anatomy Tools 1 Contact dermatitis Blepharitis HSV Preseptal Cellulitis Anterior Chamber Subconjunctival hemorrhage
Ocular Injuries in Sports. Rance McClain, D.O. Associate Dean, Clinical Sciences William Carey University FM/NMM-OMM/Sports Medicine
 Ocular Injuries in Sports Rance McClain, D.O. Associate Dean, Clinical Sciences William Carey University FM/NMM-OMM/Sports Medicine http://sudc.org/vienna/ Learning Objectives 1. Know the sport classification
Ocular Injuries in Sports Rance McClain, D.O. Associate Dean, Clinical Sciences William Carey University FM/NMM-OMM/Sports Medicine http://sudc.org/vienna/ Learning Objectives 1. Know the sport classification
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
PAINFUL PAINLESS Contact lens user BOV
 Common Causes Allergies Infections Ocular Cornea, uveitis, endophthalmitis Orbital Orbital cellulitis Inflammation Uveitis Scleritis / episcleritis Glaucomas Trauma Foreign bodies Chemical injuries History
Common Causes Allergies Infections Ocular Cornea, uveitis, endophthalmitis Orbital Orbital cellulitis Inflammation Uveitis Scleritis / episcleritis Glaucomas Trauma Foreign bodies Chemical injuries History
Paediatric acute ophthalmology. Harry Bradshaw
 Paediatric acute ophthalmology Harry Bradshaw Approach Red eye Leukocoria Neurological Trauma Visual loss Red eye Orbital Eyelid Conjunctiva Cornea Uvea Orbital Orbit fixed volume Contiguous with sinuses,
Paediatric acute ophthalmology Harry Bradshaw Approach Red eye Leukocoria Neurological Trauma Visual loss Red eye Orbital Eyelid Conjunctiva Cornea Uvea Orbital Orbit fixed volume Contiguous with sinuses,
Ocular Emergencies. Pisit Preechawat, MD Department of Ophthalmology, Ramathibodi Hospital
 Ocular Emergencies Pisit Preechawat, MD Department of Ophthalmology, Ramathibodi Hospital Ocular Anatomy Bony Components of Orbit 1 1. Frontal bone 4 5 7 6 2. Zygomatic bone 3. Maxillary bone 4. Sphenoid
Ocular Emergencies Pisit Preechawat, MD Department of Ophthalmology, Ramathibodi Hospital Ocular Anatomy Bony Components of Orbit 1 1. Frontal bone 4 5 7 6 2. Zygomatic bone 3. Maxillary bone 4. Sphenoid
Clues of a Ruptured Globe
 Definition any eye that has sustained a full thickness traumatic disruption of the cornea or sclera Overwhelmingly, rupture accidents occur in young men, small children and the elderly Corneal laceration
Definition any eye that has sustained a full thickness traumatic disruption of the cornea or sclera Overwhelmingly, rupture accidents occur in young men, small children and the elderly Corneal laceration
REFERRAL GUIDELINES: OPHTHALMOLOGY
 Outpatient Referral Guidelines Page 1 1 REFERRAL GUIDELINES: OPHTHALMOLOGY Date of birth Demographic Contact details (including mobile phone) Clinical Reason for referral Duration of symptoms Essential
Outpatient Referral Guidelines Page 1 1 REFERRAL GUIDELINES: OPHTHALMOLOGY Date of birth Demographic Contact details (including mobile phone) Clinical Reason for referral Duration of symptoms Essential
Sepideh Tara Rousta, MD FAAO Robert Wood Johnson University Hospital Saint Peter s University Hospital Wills Eye Hospital
 Sepideh Tara Rousta, MD FAAO Robert Wood Johnson University Hospital Saint Peter s University Hospital Wills Eye Hospital 14 mo old w R eye cross (parents) 9 mo old R eye crossing getting worse for past
Sepideh Tara Rousta, MD FAAO Robert Wood Johnson University Hospital Saint Peter s University Hospital Wills Eye Hospital 14 mo old w R eye cross (parents) 9 mo old R eye crossing getting worse for past
Maxillofacial and Ocular Injuries
 Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Everyday Practice. Eye trauma: Primary care for general physicians
 VOL.. 15, NO.2, 85 2002 Everyday Practice Eye trauma: Primary care for general physicians H. K. TEWARI, ATUL KUMAR, GUNJAN PRAKASH INTRODUCTION The understanding of ocular trauma is important for the primary
VOL.. 15, NO.2, 85 2002 Everyday Practice Eye trauma: Primary care for general physicians H. K. TEWARI, ATUL KUMAR, GUNJAN PRAKASH INTRODUCTION The understanding of ocular trauma is important for the primary
Ocular Lecture. Sue Bednar NP Ali Atwater PA-C
 Ocular Lecture Sue Bednar NP Ali Atwater PA-C Triaging Ocular Complaints Painful Eye/Red eye +/-blurry vision +/-visual loss +/-floaters +/-fevers If any of the above findings exist, pt is likely to have
Ocular Lecture Sue Bednar NP Ali Atwater PA-C Triaging Ocular Complaints Painful Eye/Red eye +/-blurry vision +/-visual loss +/-floaters +/-fevers If any of the above findings exist, pt is likely to have
Ocular Trauma. Breaking Down Blunt. Blunt ocular trauma occurs frequently in sporting
 Focus on CME at the University of Saskatchewan Breaking Down Blunt Ocular Trauma By Dan Ash, MD, BA, FRCSC, FACS, FAAO Blunt ocular trauma occurs frequently in sporting activities, as well as in industrial
Focus on CME at the University of Saskatchewan Breaking Down Blunt Ocular Trauma By Dan Ash, MD, BA, FRCSC, FACS, FAAO Blunt ocular trauma occurs frequently in sporting activities, as well as in industrial
Eyes, ears, teeth and everything in between
 Eyes, ears, teeth and everything in between E M E R G E N C Y D E P A R T M E N T J U N I O R T E A C H created 14/11/10 by S.R. Bruijns, version 1.0 Objectives Eyes Ears Teeth Maxilla- facial EYES Approaching
Eyes, ears, teeth and everything in between E M E R G E N C Y D E P A R T M E N T J U N I O R T E A C H created 14/11/10 by S.R. Bruijns, version 1.0 Objectives Eyes Ears Teeth Maxilla- facial EYES Approaching
Ears. Mouth. Jowls 6 Major Bones of the Face Nasal bone Two
 1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
Ocular Anatomy for the Paraoptometric
 Ocular Anatomy for the Paraoptometric Minnesota Optometric Association Paraoptometric CE Friday September 30, 2016 Lindsay A. Sicks, OD, FAAO Assistant Professor, Illinois College of Optometry lsicks@ico.edu
Ocular Anatomy for the Paraoptometric Minnesota Optometric Association Paraoptometric CE Friday September 30, 2016 Lindsay A. Sicks, OD, FAAO Assistant Professor, Illinois College of Optometry lsicks@ico.edu
THE 35 GOLDEN EYE RULES
 THE 35 GOLDEN EYE RULES The Sense of Sight, from La Dame a la Licorne, The Lady and the Unicorn Tapestries, Late 15th Century Flemish Tapestry in wool and silk, Musée Nationale du Moyen Age, Paris. 1.
THE 35 GOLDEN EYE RULES The Sense of Sight, from La Dame a la Licorne, The Lady and the Unicorn Tapestries, Late 15th Century Flemish Tapestry in wool and silk, Musée Nationale du Moyen Age, Paris. 1.
Conjunctival Hemorrhage
 IN THE NAME OF GOD Lid Laceration Conjunctival Hemorrhage a) No therapy is necessary b) Usually resolve in 7-12 days. Subconjunctival Hemorrhage Corneal Abrasion Abrasions Many small abrasions can
IN THE NAME OF GOD Lid Laceration Conjunctival Hemorrhage a) No therapy is necessary b) Usually resolve in 7-12 days. Subconjunctival Hemorrhage Corneal Abrasion Abrasions Many small abrasions can
Around The Globe in 60 Minutes
 Around The Globe in 60 Minutes Around the GLOBE in Sixty Minutes Basic Ocular Anatomy, Examination, and Diagnostic Techniques Introduction Focusing on canine and feline ocular anatomy and basic examination
Around The Globe in 60 Minutes Around the GLOBE in Sixty Minutes Basic Ocular Anatomy, Examination, and Diagnostic Techniques Introduction Focusing on canine and feline ocular anatomy and basic examination
LECTURE # 7 EYECARE REVIEW: PART III
 LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
MANAGEMENT OF CONTUSION INJURY OF THE EYE A CLINICAL STUDY
 MANAGEMENT OF CONTUSION INJURY OF THE EYE A CLINICAL STUDY *Gururaj Veeranna Wali and Pranesh Kulkarni Department of Ophthalmology, KBIMS Gulbarga, Karnataka, India *Author for Correspondence ABSTRACT
MANAGEMENT OF CONTUSION INJURY OF THE EYE A CLINICAL STUDY *Gururaj Veeranna Wali and Pranesh Kulkarni Department of Ophthalmology, KBIMS Gulbarga, Karnataka, India *Author for Correspondence ABSTRACT
The Orbit. The Orbit OCULAR ANATOMY AND DISSECTION 9/25/2014. The eye is a 23 mm organ...how difficult can this be? Openings in the orbit
 The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
CORNEAL CONDITIONS CORNEAL TRANSPLANTATION
 GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
02/03/2014. Average Length: 23mm (Infant ~16mm) Approximately the size of a quarter Volume: ~5mL
 Identify the anatomy of the eye. Explain the basic physiology of the parts of the eye. Briefly discuss various surgeries related to different parts of the anatomy. Average Length: 23mm (Infant ~16mm) Approximately
Identify the anatomy of the eye. Explain the basic physiology of the parts of the eye. Briefly discuss various surgeries related to different parts of the anatomy. Average Length: 23mm (Infant ~16mm) Approximately
Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI. Monitor the vital signs. Monitor the vital signs. Complications of Facial Traumas.
 Complications of Facial Traumas 1) Immediate Complications 2) Late Complications Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor Oral & Maxillofacial Surgeon Taibah University Monitor
Complications of Facial Traumas 1) Immediate Complications 2) Late Complications Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor Oral & Maxillofacial Surgeon Taibah University Monitor
INJURIES OF EYE AND ITS ACCESSORY ORGANS
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org Corneal and conjunctival foreign bodies are among the most frequent reasons for seeking emergency ophthalmological aid. The foreign bodies
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org Corneal and conjunctival foreign bodies are among the most frequent reasons for seeking emergency ophthalmological aid. The foreign bodies
 Traumatic Cataract Orbital Wall Fracture Vitreous Hemorrhage Optic Disc Hemorrhage a) Amblyopia b) Strabismus c) Trauma Playing with other children Sports Fire works BB gun Injecting needles .
Traumatic Cataract Orbital Wall Fracture Vitreous Hemorrhage Optic Disc Hemorrhage a) Amblyopia b) Strabismus c) Trauma Playing with other children Sports Fire works BB gun Injecting needles .
TRAUMA, TRAUMA A YOUNG PARENT WOULD HAVE HEARD THE TITLE AND IMMEDIATELY THOUGHT 10/24/2018 JAMES LEE, M.D., ASSISTANT PROFESSOR TECHNICIAN CONFERENCE
 TRAUMA, TRAUMA JAMES LEE, M.D., ASSISTANT PROFESSOR TECHNICIAN CONFERENCE OCT 26, 2018 A YOUNG PARENT WOULD HAVE HEARD THE TITLE AND IMMEDIATELY THOUGHT 1 GROSS PICTURES LET S START WITH EYELIDS Lacerations
TRAUMA, TRAUMA JAMES LEE, M.D., ASSISTANT PROFESSOR TECHNICIAN CONFERENCE OCT 26, 2018 A YOUNG PARENT WOULD HAVE HEARD THE TITLE AND IMMEDIATELY THOUGHT 1 GROSS PICTURES LET S START WITH EYELIDS Lacerations
ation is essential. Whether on the playing it is important to keep in mind that severe
 JENNIFER LAIO, MD, and BRUCE M. ZAGELBAUM, MD NYU School of Medicine, Manhasset, NY North Shore University Hospital, Eye injuries sustained in sports and recreational activities are common in the United
JENNIFER LAIO, MD, and BRUCE M. ZAGELBAUM, MD NYU School of Medicine, Manhasset, NY North Shore University Hospital, Eye injuries sustained in sports and recreational activities are common in the United
Case #1: 68 M with floaters OS
 Case #1: 68 M with floaters OS Point-of-Care Ocular Sonography for the Emergency Department Nate Teismann MD Dept of Emergency Medicine, UCSF Topics in EM 2012 Acute onset of dark spots in L eye 2 days
Case #1: 68 M with floaters OS Point-of-Care Ocular Sonography for the Emergency Department Nate Teismann MD Dept of Emergency Medicine, UCSF Topics in EM 2012 Acute onset of dark spots in L eye 2 days
Andrew J. Hendershot, MD Havener Eye Institute The Ohio State University s Wexner Medical Center
 Ocular Trauma for the Primary Care Physician Andrew J. Hendershot, MD Havener Eye Institute The Ohio State University s Wexner Medical Center Relevance Often those with minor eye injuries will first seek
Ocular Trauma for the Primary Care Physician Andrew J. Hendershot, MD Havener Eye Institute The Ohio State University s Wexner Medical Center Relevance Often those with minor eye injuries will first seek
Differential diagnosis of the red eye. Carol Slight Nurse Practitioner Ophthalmology
 Differential diagnosis of the red eye Carol Slight Nurse Practitioner Ophthalmology The red eye Conjunctivitis HSV Keratitis Acute angle closure glaucoma Anterior Uveitis Red eye Scleritis Subconjunctival
Differential diagnosis of the red eye Carol Slight Nurse Practitioner Ophthalmology The red eye Conjunctivitis HSV Keratitis Acute angle closure glaucoma Anterior Uveitis Red eye Scleritis Subconjunctival
Carotid Cavernous Fistula
 Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
OPHTHALMOLOGIC PEARLS FOR THE NON- OPHTHALMOLOGIST. David G. Gross D.O. Deen-Gross Eye Centers Merrillville-Hobart Deengrosseye.
 OPHTHALMOLOGIC PEARLS FOR THE NON- OPHTHALMOLOGIST David G. Gross D.O. Deen-Gross Eye Centers Merrillville-Hobart Deengrosseye.com A FEW OF THE AREAS WE WILL DISCUSS Red Eye Glaucoma Neuro ophthalmic tid
OPHTHALMOLOGIC PEARLS FOR THE NON- OPHTHALMOLOGIST David G. Gross D.O. Deen-Gross Eye Centers Merrillville-Hobart Deengrosseye.com A FEW OF THE AREAS WE WILL DISCUSS Red Eye Glaucoma Neuro ophthalmic tid
Speaker Disclosure Statement. " Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose.
 Speaker Disclosure Statement Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose. Diabetes Morbidity Diabetes doubles the risk of stroke. Diabetes quadruples the risk of
Speaker Disclosure Statement Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose. Diabetes Morbidity Diabetes doubles the risk of stroke. Diabetes quadruples the risk of
Traumatic Partial Optic Nerve Avulsion with Globe luxation. Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine
 Traumatic Partial Optic Nerve Avulsion with Globe luxation Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine A 23 year old male patient presented to the emergency department in
Traumatic Partial Optic Nerve Avulsion with Globe luxation Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine A 23 year old male patient presented to the emergency department in
Closed globe injuries, ocular and social consequences
 Closed globe injuries, ocular and social consequences Trauma is the set of local and general disorders that arise from the action of a violent foreign agent. Eye trauma is a pathology commonly found in
Closed globe injuries, ocular and social consequences Trauma is the set of local and general disorders that arise from the action of a violent foreign agent. Eye trauma is a pathology commonly found in
Dr Jo-Anne Pon. Dr Sean Every. 8:30-9:25 WS #70: Eye Essentials for GPs 9:35-10:30 WS #80: Eye Essentials for GPs (Repeated)
 Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC
 CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
HANDBOOK FOR JUNIOR RESIDENTS AND MEDICAL STUDENTS LEARNING EMERGENCY OPHTHALMOLOGY
 HANDBOOK FOR JUNIOR RESIDENTS AND MEDICAL STUDENTS LEARNING EMERGENCY OPHTHALMOLOGY Compiled by The Task Force on Undergraduate Teaching in Ophthalmology of the International Council of Ophthalmology and
HANDBOOK FOR JUNIOR RESIDENTS AND MEDICAL STUDENTS LEARNING EMERGENCY OPHTHALMOLOGY Compiled by The Task Force on Undergraduate Teaching in Ophthalmology of the International Council of Ophthalmology and
1 Eyelids. Lacrimal Apparatus. Orbital Region. 3 The Orbit. The Eye
 1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
For further reading we recommend the following excellent textbooks:
 FURTHER READING Intravitreal Injections Downloaded from www.worldscientific.com For further reading we recommend the following excellent textbooks: Clinical Anatomy of the Eye by Richard S Snell and Michael
FURTHER READING Intravitreal Injections Downloaded from www.worldscientific.com For further reading we recommend the following excellent textbooks: Clinical Anatomy of the Eye by Richard S Snell and Michael
THE CHRONIC GLAUCOMAS
 THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
Ocular Injuries. Chapter 14
 Ocular Injuries Chapter 14 Ocular Injuries Introduction The preservation of the eyes and eyesight of service personnel is an extremely important goal. Despite comprising as little as 0.1% of the total
Ocular Injuries Chapter 14 Ocular Injuries Introduction The preservation of the eyes and eyesight of service personnel is an extremely important goal. Despite comprising as little as 0.1% of the total
GNK485 The eye and related structures. Prof MC Bosman 2012
 GNK485 The eye and related structures Prof MC Bosman 2012 Surface anatomy Bony orbit Eyeball and Lacrimal apparatus Extra-ocular muscles Movements of the eye Innervation Arterial supply and venous drainage
GNK485 The eye and related structures Prof MC Bosman 2012 Surface anatomy Bony orbit Eyeball and Lacrimal apparatus Extra-ocular muscles Movements of the eye Innervation Arterial supply and venous drainage
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
Ocular Injuries. Chapter 14
 Ocular Injuries Chapter 14 Ocular Injuries Introduction The preservation of the eyes and eyesight of service personnel is an extremely important goal. Despite comprising as little as 0.1% of the total
Ocular Injuries Chapter 14 Ocular Injuries Introduction The preservation of the eyes and eyesight of service personnel is an extremely important goal. Despite comprising as little as 0.1% of the total
DEFINITION Corneal abrasion is a defect in the corneal surface epithelium due to scraping or rubbing of the corneal epithelium.
 DEFINITION Corneal abrasion is a defect in the corneal surface epithelium due to scraping or rubbing of the corneal epithelium. IMMEDIATE CONSULTATION REQUIRED IN THE FOLLOWING SITUATIONS Dendritic pattern
DEFINITION Corneal abrasion is a defect in the corneal surface epithelium due to scraping or rubbing of the corneal epithelium. IMMEDIATE CONSULTATION REQUIRED IN THE FOLLOWING SITUATIONS Dendritic pattern
Orbital and Ocular Adnexal Disorders with Red Eyes
 Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
OOGZIEKTEN VOOR DE HUISARTS F. GOES, JR.
 OOGZIEKTEN VOOR DE HUISARTS F. GOES, JR. HET RODE OOG F. GOES, JR. Condition Signs Symptoms Causes Conjunctivitis Viral Normal vision, normal pupil size Mild to no pain, diffuse Adenovirus (most common),
OOGZIEKTEN VOOR DE HUISARTS F. GOES, JR. HET RODE OOG F. GOES, JR. Condition Signs Symptoms Causes Conjunctivitis Viral Normal vision, normal pupil size Mild to no pain, diffuse Adenovirus (most common),
Scrub In. What is the function of vitreous humor? What does the pupil do when exposed to bright light? a. Maintain eye shape and provide color vision
 Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Primary Angle Closure Glaucoma
 www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
Ocular warning signs in GP practice: Paediatric Eye Pointers
 Ocular warning signs in GP practice: Paediatric Eye Pointers Dr Benjamin Chang MB, BCh, BAO, MMedSci, FRCS(Irel), FRCS(Edin), FRCOphth(Lond) Senior Consultant Ophthalmology and Visual Sciences Khoo Teck
Ocular warning signs in GP practice: Paediatric Eye Pointers Dr Benjamin Chang MB, BCh, BAO, MMedSci, FRCS(Irel), FRCS(Edin), FRCOphth(Lond) Senior Consultant Ophthalmology and Visual Sciences Khoo Teck
Index. C Canalicular system, 4 Carbonic anhydrase inhibitors, 29 30
 A Acanthamoeba keratitis (AK), 82, 83 Acute angle-closure crisis, 156 Acute angle-closure glaucoma (AACG), 121, 141, 284 causes of, 122 clinical presentation, 153 evaluation, 156 157 management/treatment,
A Acanthamoeba keratitis (AK), 82, 83 Acute angle-closure crisis, 156 Acute angle-closure glaucoma (AACG), 121, 141, 284 causes of, 122 clinical presentation, 153 evaluation, 156 157 management/treatment,
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White
 Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Intravitreal Injection
 for patients Eye Clinic Ipswich Hospital Tel: 01473 703230 Intravitreal Injection What is an intravitreal injection? An intravitreal injection is the injection of a drug into the vitreous body (the jelly
for patients Eye Clinic Ipswich Hospital Tel: 01473 703230 Intravitreal Injection What is an intravitreal injection? An intravitreal injection is the injection of a drug into the vitreous body (the jelly
The eye in ED. Dr Steve Costa Emergency Medicine Training Hub Ballarat & Grampians Region 18 th July 2013
 The eye in ED Dr Steve Costa Emergency Medicine Training Hub Ballarat & Grampians Region 18 th July 2013 Learning objectives Diagnostic reasoning Describe the common injuries and diagnostic dilemmas seen
The eye in ED Dr Steve Costa Emergency Medicine Training Hub Ballarat & Grampians Region 18 th July 2013 Learning objectives Diagnostic reasoning Describe the common injuries and diagnostic dilemmas seen
10 EYE EMERGENCIES. Who goes, who you better not send! Brant Slomovic, MD, FRCPC University Health Network
 10 EYE EMERGENCIES Who goes, who you better not send! Brant Slomovic, MD, FRCPC University Health Network DISCLOSURES I have none PVD CASE 1 WHAT IS A PVD? a process of aging (45-55) liquefaction of vitreous
10 EYE EMERGENCIES Who goes, who you better not send! Brant Slomovic, MD, FRCPC University Health Network DISCLOSURES I have none PVD CASE 1 WHAT IS A PVD? a process of aging (45-55) liquefaction of vitreous
WGA. The Global Glaucoma Network
 The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
By Darlene Jones, Nurse. May 2017
 By Darlene Jones, Nurse May 2017 Disclosure of potential conflict of interest Darlene Jones, Nurse I have no conflict of interest Course objectives Become familiar with the different pathologies in ophthalmology
By Darlene Jones, Nurse May 2017 Disclosure of potential conflict of interest Darlene Jones, Nurse I have no conflict of interest Course objectives Become familiar with the different pathologies in ophthalmology
Vision I. Steven McLoon Department of Neuroscience University of Minnesota
 Vision I Steven McLoon Department of Neuroscience University of Minnesota 1 Eye Cornea Sclera Conjunctiva 2 Eye The conjunctiva lines the inner surface of the eyelids and outer surface of the sclera. 3
Vision I Steven McLoon Department of Neuroscience University of Minnesota 1 Eye Cornea Sclera Conjunctiva 2 Eye The conjunctiva lines the inner surface of the eyelids and outer surface of the sclera. 3
PRODUCTION ANIMAL AND EQUINE OPHTHALMOLOGY
 REF. NO. TITLE: C-VO.2 PRODUCTION ANIMAL AND EQUINE OPHTHALMOLOGY VALUE: 10 CREDITS NOTIONAL STUDY HOURS: 100 This module is intended to cover the theoretical knowledge of both Production Animal and Equine
REF. NO. TITLE: C-VO.2 PRODUCTION ANIMAL AND EQUINE OPHTHALMOLOGY VALUE: 10 CREDITS NOTIONAL STUDY HOURS: 100 This module is intended to cover the theoretical knowledge of both Production Animal and Equine
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
JINNAH SINDH MEDICAL UNIVERSITY STUDY GUIDE- OPHTHALMOLOGY YEAR 4,
 INTRODUCTION Pakistan, the 7th most populous country in the world, has an urban population of 38.8% and rural dwellers of 61.2%. The country has faced challenges with vision impairment and blindness as
INTRODUCTION Pakistan, the 7th most populous country in the world, has an urban population of 38.8% and rural dwellers of 61.2%. The country has faced challenges with vision impairment and blindness as
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg
 An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
Frequently Asked Questions about General Ophthalmology:
 1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
TRAUMATIC CATARACT DR.KHUTEJA FATIMA IIND YEAR PG DEPT OF OPHTHALMOLOGY
 TRAUMATIC CATARACT DR.KHUTEJA FATIMA IIND YEAR PG DEPT OF OPHTHALMOLOGY Traumatic cataract :Traumatic lens damage caused by mechanical injury and by physical forces (Ionising radiation,ir radiation, electrical
TRAUMATIC CATARACT DR.KHUTEJA FATIMA IIND YEAR PG DEPT OF OPHTHALMOLOGY Traumatic cataract :Traumatic lens damage caused by mechanical injury and by physical forces (Ionising radiation,ir radiation, electrical
Ocular Trauma Chemical Injuries
 Ocular Trauma Chemical Injuries Ramesh Venkatesh*, Hemkala L Trivedi** Introduction Background : Chemical injuries to the eye represent one of the true ophthalmic emergencies. While almost any chemical
Ocular Trauma Chemical Injuries Ramesh Venkatesh*, Hemkala L Trivedi** Introduction Background : Chemical injuries to the eye represent one of the true ophthalmic emergencies. While almost any chemical
Cairo University Faculty of Medicine. Course Specifications Course title: Ophthalmology (Code): OPH-409. Department of Ophthalmology
 Cairo University Faculty of Medicine Department of Ophthalmology Course Specifications Course title: Ophthalmology (Code): OPH-409 Department of Ophthalmology Fourth academic year of M.B.B.Ch. program
Cairo University Faculty of Medicine Department of Ophthalmology Course Specifications Course title: Ophthalmology (Code): OPH-409 Department of Ophthalmology Fourth academic year of M.B.B.Ch. program
LENS INDUCED GLAUCOMA
 LENS INDUCED GLAUCOMA PRESENTER P SHILPA RAVI 2 ND YEAR PG DEPT OF OPHTHALMOLOGY LENS INDUCED GLAUCOMA It is a form of secondary glaucoma where intraocular pressure is raised due to disorder in crystalline
LENS INDUCED GLAUCOMA PRESENTER P SHILPA RAVI 2 ND YEAR PG DEPT OF OPHTHALMOLOGY LENS INDUCED GLAUCOMA It is a form of secondary glaucoma where intraocular pressure is raised due to disorder in crystalline
University of Florida ORBIT
 University of Florida ORBIT Dog Airedale Bulldog Great Dane Cat Horse bones EOM in fascial slings Periorbita: orbital septum to tarsal plate Periosteum of optic canal to optic nerve dura Tenon s capsule
University of Florida ORBIT Dog Airedale Bulldog Great Dane Cat Horse bones EOM in fascial slings Periorbita: orbital septum to tarsal plate Periosteum of optic canal to optic nerve dura Tenon s capsule
DISCLOSURES. PEDIATRIC RED EYES Rachel M. Smith, OD, FCOVD HISTORY, HISTORY, HISTORY WHY RED EYES? EXAMINE THE EYE RED FLAGS TO REFER 3/25/2019
 DISCLOSURES Consultant/Speakers bureaus Research funding PEDIATRIC RED EYES Rachel M. Smith, OD, FCOVD Pediatric Optometrist Children s Hospital & Medical Center Stock ownership/corporate boards employment
DISCLOSURES Consultant/Speakers bureaus Research funding PEDIATRIC RED EYES Rachel M. Smith, OD, FCOVD Pediatric Optometrist Children s Hospital & Medical Center Stock ownership/corporate boards employment
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit
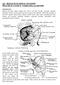 213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit OSTEOLOGY Identify the bones which comprise the walls of the orbit: maxilla, zygomatic, ethmoid, lachrymal, frontal, and
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit OSTEOLOGY Identify the bones which comprise the walls of the orbit: maxilla, zygomatic, ethmoid, lachrymal, frontal, and
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
