Water is the driving force of all nature. -Leonardo Da Vinci
|
|
|
- Shanon McCoy
- 6 years ago
- Views:
Transcription
1 URINARY SYSTEM Water is the driving force of all nature. -Leonardo Da Vinci
2 "What we do in this life echoes in eternity."
3 Urinary System Primary organs- Kidneys Accessory organs bilateral tubes that carry urine from the kidneys to the bladder expandable sac that serves as a reservoir for urine single tube that carries urine from the bladder to the outside of the body
4 Urinary Functions water content of plasma ions in plasma ph of plasma Return water & solutes to the bloodstream ( ) Transfers Urine Metabolites through Ureters to Urinary Bladder Filtrate Concentrated into Urine & Stored in the Bladder Nephrology- study of kidney physiology & pathology
5 Kidney Anatomy Location & External Anatomy of the Kidney Internal Anatomy of the Kidney Blood & Nerve Supply of the Kidney Nephrons
6 Urinary System Organs Figure 25.1a
7 Kidney Location & External Anatomy Figure 25.2a
8 Location & External Anatomy of the Kidneys Bean-shaped organs that lie in the superior lumbar region Extend from T12 to L3 kidneyis slightly lower than the left because ofits location under theliver Average adult kidney = 150 grams (about a 1/3 of a pound)
9 Location & External Anatomy of the Kidneys The medial surface is concave & has a renal hilusthat leads into a space called the renal sinus, where the blood vessels, nerves & lymphaticslie Surrounded by a fibrous, transparent renal capsule a fatty adipose capsule that cushions the organ & an outer fibrous renal fascia that anchors the kidney to surrounding structures
10 Internal Anatomy Figure 25.3b
11 Internal Anatomy of the Kidney 3 distinct regions of the kidney: Renal Cortex Renal Medulla Renal Pelvis
12 Renal Cortex the outeror more superficial tissue layer of the kidney Lighterin color than the deeper layers Extends into the deeper Medulla to form Renal Columns
13 Renal Medulla Organized into cone-shaped areas known as The narrow rounded end of each pyramid is known as a There are 8 to 16 pyramidsper kidney
14 A flat, funnel shaped tube that leads in the Ureter The pelvis branches is feed The pelvis branches is feed from short, wide tubes known as (calyx)
15 Renal Pelvis Renal Papilla feed into the Minor Calyces branch to form the cup-shaped much larger Major Calyces that empty into the Renal Pelvis & into the Ureter, which carries urine to the Urinary Bladder
16 Blood Supply of the Kidney The kidneys receive ¼ of the total cardiac output every minute by way of the large Renal arteries branch repeatedly within the kidneys to form small InterlobarArteriesthat extend into the cortex
17 Blood Supply of the Kidney Within the cortex, Afferent Arterioles branch from the Interlobararteries& carry the blood into (small filtering units) Nephronswhere plasma becomes filtrate & filtrate is converted into urine Efferent Arteriolesdrain blood out of the Nephrons & lead into Capillary Bedsthat surround each nephron
18 Blood Supply of the Kidney From the capillary beds, the blood enters small InterlobarVeinswhich merge to form larger & larger veins Eventually, blood drains from the Eventually, blood drains from the kidneys via the large, which dump into the Inferior Vena Cava
19 Nephrons Simplest structural & functional units of the kidneys that carry out processes that form Urine Each kidney contains over 1 million nephrons Each nephron functions as a small separations plant, in which wastes & excess substances are separated from the blood & incorporated in urine
20 Nephrons Each Nephronconsists of a Renal Corpusclecomposed of the (a tuft of capillaries) surrounded by the /Glomerular capsule
21 Nephrons continued The Renal Tubulebegins at the glomerularcapsule as the Proximal Convoluted Tubule, continues through a hairpin loop, the Loop of Henle& turns into a Distal Convoluted Tubulebefore emptying into a Collecting Duct
22 Nephrons continued The terms Proximal & Distal indicate the position of that part of the renal tubule relative to the renal corpuscle The Loop of Henlehas descending & ascending limbs
23 Nephrons continued The collecting ducts collect filtrate from many Nephrons, & extend through the renal pyramid to the renal papilla, where they empty into a minor calyx
24 Nephrons continued There are 2 types of nephrons: 85% Cortical Nephrons which are located almost entirely within the cortex 15% Juxtamedullary Nephrons located near the cortex-medulla junction
25 Nephrons continued The Arterioleleading into a Glomerulusis wider than the Arteriole carrying blood out of the Glomerulus Because the Bloodis coming into the glomerulusfaster than it is leaving, pressure builds up inside the glomerularcapillary bed The high pressure forces Plasma& solutes out & into the Bowman s capsule space, where it becomes known as Filtrate
26 Nephrons continued The peritubularcapillariesarise from efferent arterioles draining the glomerulus& reabsorb solutes & water from the tubules (99% Reabsorption) Blood flow in the renal circulation is subject to high resistance in the afferent & efferent arterioles
27 Juxtaglomerular Apparatus structural arrangement between the afferent arteriole & the distal convoluted tubule The apparatus is composed of 2 cell types: Juxtaglomerular (JG) cells Macula densacells
28 Juxtaglomerular (JG) cells Smooth muscle cells in the wall of the afferent arteriole act as mechanoreceptors that sense changes in blood pressure in the afferent arteriole The JG cellsrelease (hormone) when the blood pressure in the afferent arteriole falls too low The sequence of events following the release of Reninwill be discussed later
29 Macula Densa cells DCT cells that act as osmoreceptors (Chemoreceptors), responding to changes in the solute concentration of the filtrate
30 Nephrons Figure 25.5b
31 Juxtaglomerular Apparatus Figure 25.6
32 Filtration Membrane Figure 25.7a
33 Filtration Membrane Figure 25.7c
34 Kidney Physiology: Mechanisms of Urine Formation As blood flows into the glomeruliin the kidneys, some of the plasma is forced out of the capillary bed & into the renal tubules to form filtrate (around 125ml per minute is formed) The filtrate contains everything found in blood plasma except proteins
35 Kidney Physiology: Mechanisms of Urine Formation By the time it has finished traveling through all parts of the renal tubule & enters the collecting ducts, it is Urine rine, which contains mostly metabolic wastes & unneeded substances
36 Kidney Physiology: Mechanisms of Urine Formation There are 2 major processes involved in the formation of urine: Step 1:GlomerularFiltration Step 2:Tubular Reabsorption Step 3 Step 3:Tubular Secretion Regulation of Urine Concentration & Volume
37 Step 1: Glomerular Filtration a passive, nonselective process in which hydrostatic pressure forces fluids outof the glomerulus& into the first part of the renal tubule (Bowman s Capsule) The surface area of the glomerulusis very large & it is more permeable to solutes than other capillary beds in the body
38 Step 1: GlomerularFiltration The blood pressure in the glomerulusis much higherthan in other capillary beds, so more plasma & solutes are forced out by the hydrostatic pressure 180 Lof filtrate are formed each day in the kidneys, compared to 3 or 4 L of interstitial fluid formed in the other capillary beds of the body
39 Step 1: GlomerularFiltration Smaller molecules such as glucose, amino acids, water, nitrogenous wastes (Urea) pass freely from the blood & into the renal tubule Larger molecules such as blood cells & proteins remain in the
40 Step 1: Glomerular Filtration GlomerularFiltration Rate(GFR) is the volume of filtrate formed each minute by all the glomeruliof the kidneys combined ( ml/min in each kidney) An increasein blood pressure the GFR A decreasein blood pressure the GFR
41 Step 1: Glomerular Filtration Maintenance of a relatively constant GFR is important because reabsorptionof water & solutes depends on how quickly filtrate flows through the tubules If the rate of filtrate flow through the renal tubules is too fast, such as would occur with high blood pressure, then the flow of filtrate is too fast & valuable substances are lost in the urine rather than reabsorbed into the blood If the rate of filtrate flow is too low, as would occur with low blood pressure, too much of the filtrate is reabsorbed, including waste products
42 Step 1: Glomerular Filtration GFR is held relatively constant through intrinsic autoregulatory mechanisms, extrinsic hormonal mechanisms & neural mechanisms Intrinsic controls Extrinsic controls
43 Intrinsic controls of GFR Increased blood pressure causes smooth muscles in afferent arterioles to constrict, thus reducing blood flow (Myogenic mechanism- mechanoreceptors) Decreased blood pressure causes the smooth muscles to relax, resulting in blood vessel dilation & increased blood flow A reduced flow of filtrate, or decreased concentration of filtrate, in the DCT causes Macula DensaCells to release chemicals that dilatethe afferent arterioles Increased flow of filtrate, to increased concentration of filtrate, in the DCT causes Macula DensaCells to release chemicals that constrict the afferent arterioles
44 Extrinsic controls of GFR When the body is at rest, the autoregulatory mechanisms listed above are in charge. In times of Stress neural mechanisms take over Stress Neural mechanisms are stress-induced sympathetic responses that inhibit filtrate formation by constricting the afferent arterioles & decreasing the production of filtrate When blood pressure in the afferent arterioles drops (due to hemorrhaging, dehydration, etc.) the JG cells release the hormone Renin, which starts the Renin- Angiotensin System
45 Step 1: Glomerular Filtration Angiotensinogen(Renin) Angiotensin I ACE (in lungs) Angiotensin II Angiotensin II has the following effects: Stimulates the adrenal cortex to release aldosterone, which increases Na + reabsorptionin the renal tubules Water follows the Na + back into the bloodstream, so urine volume decreases Stimulates vasocontrictionof systemic arterioles, leading to increased blood pressure Stimulates the thirst center in the hypothalamus, leading to the sensation of thirst (+ADH)
46 Step 2: Tubular Reabsorption The total blood volume filters into the renal tubules every minutes& if most it were not reabsorbed, all the plasma would be drained from the body in less than 30 minutes! Fortunately, most of the contents of the filtrate are reabsorbed into the bloodstreamas the filtrate moves through the different parts of the nephron tubules This process is known as Tubular Reabsorption
47 Step 2: Tubular Reabsorption Tubular reabsorptionbegins as soon as the filtrate enters the proximal convoluted tubule & involves near total reabsorptionof organic nutrients such as glucose & amino acids Reabsorption of water& ions is primarily under hormonal control & is constantly adjusted The most abundant cationof the filtrate is + & its reabsorptionis always by means of active transport This accounts for 80% of the ATP energy used during the active transport processes of reabsorption
48 Step 2: Tubular Reabsorption Obligatory water reabsorption occurs in waterpermeable regions of the tubules in response to the osmotic gradients created by active transport of Na + Recall that water follows salt in the body Secondary active transport is responsible for absorption of glucose, amino acids, vitamins & most cations& occurs when solutes are co-transported with Na + when it moves along its concentration gradient Nonreabsorbedor incompletely reabsorbed substances remain in the filtrate due to a lack of carrier molecules, lipid insolubility or large size (urea, creatinine& uric acid)
49 Step 2: Tubular Reabsorption Different areas of the tubules have different absorptive capabilities The (PCT) is most active in reabsorption, with most selective reabsorptionoccurring there All glucose & amino acids 65% of the Na + & water 90% of the bicarbonate 50% of the Cl - 55% of the K +
50 Step 2: Tubular Reabsorption Loop of Henle Descending Limb of the Loop of Henleis to water, while the Ascending Limb of the Loop of Henle is to water, but permeable to electrolytes
51 Step 2: Tubular Reabsorption Distal Convoluted Tubule & Collecting Duct reabsorptiondepends on body needs Na + & water permeability regulated by 3 hormones: Aldosterone Na+ permeablity& reabsorption, which waterreabsorption UV, BV & BP AntidiureticHormone makes collecting ducts more permeable to water, water reabsorption UV, BV & BP AtrialNatriureticPeptide inhibits Na + reabsorption, so more Na + & water remain as part of the Urine UV, BV & BP
52 Step 3: Tubular Secretion Some unwanted substances are eliminated in Urinesimply because they are not reabsorbed from the filtrate Others must be actively secreted into the filtrate to become part of the Urine
53 Step 3: Tubular Secretion of unwanted solutes (such as drugs) solutes that were reabsorbed (such as urea & uric acid) the body of excess K + blood ph
54 Step 3: Tubular Secretion Tubular secretion is most active in the (PCT), but occurs in the collecting ducts & distal convoluted tubules, as well
55 Regulation of Urine Concentration & Volume Osmolarity salt in H 2 O One of the critical functions of the kidney is to keep the solute load of body fluids constant by regulating Urineconcentration & volume
56 Countercurrent Mechanism prevents rapid removal of salt & establish water recovery Involves interaction between filtrate flow through the Loops of Henle of Juxtamedullary Nephrons & the flow of blood through the Vasa Recta Since Wateris freely absorbed from the descending limb of the loop of Henle, filtrate concentration increases as Water is reabsorbed The ascending limb is permeable to solutes, but not to Water, so the filtrate is diluted as solutes are removed & Water remains
57 Regulation of Urine Concentration & Volume Since tubular filtrate is diluted as it travels through the ascending limb of the loop of Henle, production of a dilute Urineis accomplished by simply allowing filtrate to pass on to the renal pelvis Formation of a concentrated Urine occurs in response to the release of ADH, which makes the collecting ducts permeable to Water& increases Water uptake from the Urine Diuretics act to increase Urineoutput by either acting as an osmotic diuretic or by inhibiting Na + & resulting obligatory Water reabsorption
58 Renal Clearance the volume of plasma that is cleared of a specific substance in a given time is used as a clearance standard to determine glomerularfiltration rate since it is not reabsorbed, stored, or secreted If the clearance value for a substance is less than that for inulin, then some of the substance is being reabsorbed If the clearance value is greater than the inulin clearance rate, then some of the substance is being secreted A clearance value of zero indicates the substance is completely reabsorbed
59 Glomerular Filtration Rate Figure 25.9
60 Mechanisms of Urine Formation Urine formation & adjustment of blood composition involves 3 major processes Glomerular Filtration Tubular Reabsorption Tubular Secretion Figure 25.8
61 Formation of Dilute & Concentrated Urine Osmolality- Osmolarity- Figure 25.15a, b
62 Formation of Dilute & Concentrated Urine Dilute Urine Hypoosmotic Lack of ADH Low Osmolality70 mosm(1/4 the concentration of glomerular filtrate or plasma) Concentrated Urine Hyperosmotic ADH inhibits Diuresisdecreases water volume of the urine tied to survivability w/o water High Osmolality 1200 mosm
63 Ureters Bilateral tubes that actively convey Urinefrom the kidneys to the bladder (10 long/1/16-1/4 mm in diameter) Ureterwalls consist of an inner mucosa continuous with the kidney pelvis & the bladder, a doublelayered muscularis& a connective tissue adventitia covering the external surface Increased Urinary Pressure w/in the Bladder compresses ureteropening Preventing Urine Backflow
64 Urinary Bladder a muscular sac lined with transitional epithelium that expands as Urineis produced by the kidneys Allows for Urine storage until voiding is convenient (& socially acceptable!) The bladder wall contains 3layers: an outer adventitia a middle layer of Detrusormuscle an inner mucosa highly folded to allow for bladder distention without a large increase in internal pressure
65 Urinary Bladder Maximum capacity is around ml/1l (1 quart) It can burst if overextended A moderately full bladder holds around 500 ml (1 pint) Every 200mL Urge to Urinate
66 Urethra Muscular discharge tube that drains Urine from the body 2 long in females 9 long in males 2 sphincter muscles associated with the urethra: the internal urinary sphincter-involuntary & formed from detrusor muscle the external urinary sphincter-voluntary & formed by the skeletal muscle The external urethral orifice lies between the clitoris & vaginal opening in females, or occurs at the tip of the penis in males
67 Trigone Seen on the inside of the Urinary Bladder formed by the 2Ureters & the Urethra
68 Lower Urinary System Structures Figure 25.18a. b
69 Urine Physical Characteristics Freshly voided urine is clear and pale to deep yellow due to a pigment resulting from the destruction of hemoglobin The more concentrated the Urine, the deeper yellow its color Pink or brown Urinemay be due to ingestion of certain foods or the presence of blood Drugs & vitamin supplements may also alter Urine color Cloudy Urine may indicate a urinary tract infection
70 Urine Fresh Urineis slightly aromatic, but develops an ammonia odor if allowed to stand, due to bacterial metabolism of urea Intake of drugs & certain vegetables can alter Urinesmell Diabetes Diabetescan cause Urine Urine to smell fruity due to the presence of acetone
71 Urine Urine Urine is usually slightly acidic (around ph ), but can vary from about in response to changes in metabolism or diet Specific Gravity-(Mass) depends on solute concentration ( ) Heavier than distilled water Protein/Glucose
72 Chemical Composition Urine Urine Volume is about 95% water & 5% solutes Pass 1-2 L/daily (depending on intake) The largest component of Urine by weight, other than water, is Urea (formed from Amino Acids) Urea formed from various substances & ammonia (a metabolic waste product that has no physiological function & must be neutralized) Other nitrogenous wastes include Creatinine(a metabolite of creatinephosphate in skeletal muscle) & Uric acid(an end product of nucleic acid metabolism) Blood Urea Nitrogen(BUN) measures renal efficiency & damage
73 Micturition Urination the act of voiding or emptying the bladder As Urine accumulates, distention of the bladder activates stretch receptors, which trigger spinal reflexes, resulting in contraction of the internal & external sphincters & inhibition of the detrusor muscle of the bladder This results in storage of Urine When Urinelevels reach around 200 ml in the bladder, afferent impulses from stretch receptors are transmitted to the brain, creating the urge to void Reflex contractions of the bladder become more & more frequent & urgent
74 Micturition Voluntary initiation of voiding reflexes results in activation of the micturition center of the pons, which signals parasympathetic motor neurons that stimulate contraction of the detrusor muscle & relaxation of the urinary sphincters Choosing not to void ( holding it ) causes the reflex bladder contractions to subside temporarily & the external sphincter can remain voluntarily closed through Cortical Inhibition
75 Micturition The urge to void becomes irresistible when the urine volume in the bladder reaches ml, at which point micturition will occur (regardless of circumstances!) Internal sphincter (involuntary) External sphincter (voluntary) Micturition Reflex(Pons) every 200 ml After micturition, only about 10 ml of Urine remain in the bladder
76 Micturition (Voiding or Urination) Figure 25.20a, b
77 Renal Hormones ANP (Atrial Natriuretic Peptide) ADH (Vasopressin) Renin-Angiotensin Aldosterone
78 Atrial Natriuretic Peptide High Na or BV ANP Released by the Heart GFR/inhibitNa+ reabsorption& inhibits Renin secretion Natriuresis Na+ excretion & Urine output by water volume in urine BV & BP Diuresis (urine output)- urine BV & BP Inhibit Na+ reabsorption Waterfollows out collecting duct urine volume
79 AntidiureticHormone Vasopressin released by the? Alcohol & Caffeine reduce ADH higher Urine output Inhibits diuresis Water reabsorptionby action on the Collecting Duct Osmoreceptor in Hypothalamus- Neurohypophysis monitor an increase BV & regulate Water Waterreabsorption accordingly High ADH Highly concentrated Urine500 ml/day Low ADH dilute Urine2 L
80 Renin~Angiotensin~Aldosterone Angiotensinogen Angiotensin I (Renin) ACE(AngiotensinConverting Enzyme) converts Angiotensin I Angiotensin II GFR by vasoconstriction of afferent arterioles Enhance Na +, Cl - & waterreabsorption BV Stimulates Adrenal Cortex to release Aldosterone
81 Aldosterone released by reabsorb Na +, secrete K + Water follows Na + BV & BP Renin Angiotensin Aldosterone BV & BP less stretch JG cells release of Reninor Symp BP & BV (Hepatocyte) Angiotensinogen (Renin) AngiotensinI (ACE) AngiotensinII (vasoconstrictor) Aldosterone
82 Urinary System Objectives Correlate Nephron Structure to Urine Formation Describe Urine Formation Examine the Role of Hormonal Control in Kidney Function Explain the Role of the Kidney s Vascular System in Urine Formation
83 Urinary System Objectives Explain the Normal & Abnormal Constituents of Urine & their Significance Examine the role of Hormonal Control in Kidney Function Understand the role of Filtration & Reabsorption in Urine Formation Homeostatic Imbalances & Urinary Pathologies
Chapter 25: Urinary System
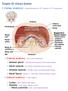 Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Functions of the Urinary System
 The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Regulate aspects of homeostasis Water balance Electrolytes Acid-base balance in the blood
The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Regulate aspects of homeostasis Water balance Electrolytes Acid-base balance in the blood
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
The Urinary System. Copyright 2003 Pearson Education, Inc. publishing as Benjamin Cummings
 The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Functions of the Urinary System Regulate aspects of homeostasis Water balance Electrolytes
The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Functions of the Urinary System Regulate aspects of homeostasis Water balance Electrolytes
Chapter 17: Urinary System
 Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
CHAPTER 25 URINARY. Urinary system. Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1. functions
 CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Urinary System BIO 250. Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat. Routes of Waste Elimination
 Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Chapter 26 The Urinary System
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
General Anatomy of Urinary System
 General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
Lab Activity 31. Anatomy of the Urinary System. Portland Community College BI 233
 Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
28/04/2013 LEARNING OUTCOME C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS STUDENT ACHIEVEMENT INDICATORS URINARY SYSTEM & EXCRETION
 LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
A. Incorrect! The urinary system is involved in the regulation of blood ph. B. Correct! The urinary system is involved in the synthesis of vitamin D.
 Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
active transport of! Na. C. Tubular Reabsorption of Nutrients, Water, and Ions (p. 979; Fig )
 The Urinary System Outline 25.1 The kidneys have three distinct regions and a rich blood supply (pp. 963 965; Figs. 25.1 25.5) A. Location and External Anatomy (p. 963; Figs. 25.1 25.3) 1. The kidneys
The Urinary System Outline 25.1 The kidneys have three distinct regions and a rich blood supply (pp. 963 965; Figs. 25.1 25.5) A. Location and External Anatomy (p. 963; Figs. 25.1 25.3) 1. The kidneys
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Copyright 2003 Pearson Education, Inc. publishing as Benjamin Cummings. Dr. Nabil Khouri
 Dr. Nabil Khouri Objectives: General objectives: - to identify the kidney s structures, function and location - to analyze the relationship between microscopic structure and function Specific objectives:
Dr. Nabil Khouri Objectives: General objectives: - to identify the kidney s structures, function and location - to analyze the relationship between microscopic structure and function Specific objectives:
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph
 The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
The Urinary System 15PART A. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART A Functions of the Urinary System Elimination of waste products Nitrogenous
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART A Functions of the Urinary System Elimination of waste products Nitrogenous
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Figure 26.1 An Introduction to the Urinary System
 Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
Unit 15: The Urinary System
 Unit 15: The Urinary System I. Functions of the Urinary System A. Elimination of waste products 1. Nitrogenous wastes 2. Toxins 3. Drugs B. Regulate aspects of homeostasis 1. Water balance 2. Electrolytes
Unit 15: The Urinary System I. Functions of the Urinary System A. Elimination of waste products 1. Nitrogenous wastes 2. Toxins 3. Drugs B. Regulate aspects of homeostasis 1. Water balance 2. Electrolytes
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
URINARY SYSTEM. Urinary System
 URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Urinary System. BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College
 Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Unit 15 - The Urinary System 1
 Unit 15 - The Urinary System 1 I. Unit 15: The Urinary System A. Functions of the Urinary System 1. Elimination of waste products a) Nitrogenous wastes b) Toxins c) Drugs 2. Regulate aspects of homeostasis
Unit 15 - The Urinary System 1 I. Unit 15: The Urinary System A. Functions of the Urinary System 1. Elimination of waste products a) Nitrogenous wastes b) Toxins c) Drugs 2. Regulate aspects of homeostasis
organs of the urinary system
 organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Unit #4 Waste and Excretion. The Kidneys
 Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
1. The Fibrous Capsule covers the outside of the kidney. It is made of fat and fibers.
 Slide 2 The kidney has a number of functions. First is the excretion of toxic metabolic waste through urine production. The kidneys filter blood plasma and as a result of filtering blood, the kidneys help
Slide 2 The kidney has a number of functions. First is the excretion of toxic metabolic waste through urine production. The kidneys filter blood plasma and as a result of filtering blood, the kidneys help
Urinary System. Chapter 17 7/19/11. Introduction
 7/19/11 Chapter 17 Urinary System Introduction A. The urinary system consists of two kidneys that filter the blood, two ureters, a urinary bladder, and a urethra to convey waste substances to the outside.
7/19/11 Chapter 17 Urinary System Introduction A. The urinary system consists of two kidneys that filter the blood, two ureters, a urinary bladder, and a urethra to convey waste substances to the outside.
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
Waste. Urinary System Anatomy Urinary Section pages 5-8. Urinary System. Urinary System. Nitrogenous Wastes. Nitrogenous Wastes 4/22/2016
 Waste Urinary System Anatomy Urinary Section pages 5-8 Metabolism produces waste products What is the primary waste product of cellular respiration? How does the body dispose of it? Urinary System Urinary
Waste Urinary System Anatomy Urinary Section pages 5-8 Metabolism produces waste products What is the primary waste product of cellular respiration? How does the body dispose of it? Urinary System Urinary
Copyright 2010 Pearson Education, Inc. Urinary System
 Urinary System What are the organs that comprise the urinary system? Urinary System Organs Kidneys Urinary bladder Ureters Urethra Hepatic veins (cut) Esophagus (cut) Inferior vena cava Adrenal gland Aorta
Urinary System What are the organs that comprise the urinary system? Urinary System Organs Kidneys Urinary bladder Ureters Urethra Hepatic veins (cut) Esophagus (cut) Inferior vena cava Adrenal gland Aorta
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
AP2, Lab 7 - THE URINARY SYSTEM
 AP2, Lab 7 - THE URINARY SYSTEM I. SYSTEM COMPONENTS (Figs. 25.1 25.4) KIDNEYS Each kidney contains approx. 1,000,000 tubular NEPHRONS which produce FILTRATE from the plasma and then add to or take from
AP2, Lab 7 - THE URINARY SYSTEM I. SYSTEM COMPONENTS (Figs. 25.1 25.4) KIDNEYS Each kidney contains approx. 1,000,000 tubular NEPHRONS which produce FILTRATE from the plasma and then add to or take from
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Urinary System and Fluid Balance. Urine Production
 Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
The Urinary System Pearson Education, Inc.
 26 The Urinary System Introduction The urinary system does more than just get rid of liquid waste. It also: Regulates plasma ion concentrations Regulates blood volume and blood pressure Stabilizes blood
26 The Urinary System Introduction The urinary system does more than just get rid of liquid waste. It also: Regulates plasma ion concentrations Regulates blood volume and blood pressure Stabilizes blood
Human Anatomy Unit 3 URINARY SYSTEM
 Human Anatomy Unit 3 URINARY SYSTEM In Anatomy Today Components Kidneys Ureters Urinary bladder Urethra Functions Storage of urine Bladder stores up to 1 L of urine Excretion of urine Transport of urine
Human Anatomy Unit 3 URINARY SYSTEM In Anatomy Today Components Kidneys Ureters Urinary bladder Urethra Functions Storage of urine Bladder stores up to 1 L of urine Excretion of urine Transport of urine
Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden
 Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden The urinary system is important because it performs vital excretory functions Takes blood from renal arteries into the kidney to filtrate
Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden The urinary system is important because it performs vital excretory functions Takes blood from renal arteries into the kidney to filtrate
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
First is Urine Production. We ll discuss the specifics of this process momentarily.
 1 2 The kidney has a number of functions. First is Urine Production. We ll discuss the specifics of this process momentarily. Next, the kidneys filter blood. As a result of filtering blood, the kidneys
1 2 The kidney has a number of functions. First is Urine Production. We ll discuss the specifics of this process momentarily. Next, the kidneys filter blood. As a result of filtering blood, the kidneys
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
URINARY SYSTEM CHAPTER 28 I ANATOMY OF THE URINARY SYSTEM. Student Name
 Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
Urinary system. Urinary system
 INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 16 Urinary System 1 The Kidneys Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Functions of Urinary system o The Kidneys:
BIOH122 Human Biological Science 2 Session 16 Urinary System 1 The Kidneys Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Functions of Urinary system o The Kidneys:
P215 Spring 2018: Renal Physiology Chapter 18: pp , Chapter 19: pp ,
 P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
Ch17-18 Urinary System
 Ch17-18 Urinary System Main Function: Filter the blood Other Functions: maintain purity and consistency of internal fluids eliminates nitrogenous wastes, toxins, and drugs from the body regulates blood
Ch17-18 Urinary System Main Function: Filter the blood Other Functions: maintain purity and consistency of internal fluids eliminates nitrogenous wastes, toxins, and drugs from the body regulates blood
Chapter 23. The Nephron. (functional unit of the kidney
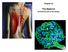 Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
The Urinary System. Medical Assisting Third Edition. Booth, Whicker, Wyman, Pugh, Thompson The McGraw-Hill Companies, Inc. All rights reserved
 The Urinary System PowerPoint presentation to accompany: Medical Assisting Third Edition Booth, Whicker, Wyman, Pugh, Thompson 30-2 Learning Outcomes 30.1 Describe the structure, location, and functions
The Urinary System PowerPoint presentation to accompany: Medical Assisting Third Edition Booth, Whicker, Wyman, Pugh, Thompson 30-2 Learning Outcomes 30.1 Describe the structure, location, and functions
BIOLOGY - CLUTCH CH.44 - OSMOREGULATION AND EXCRETION.
 !! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
!! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
19. RENAL PHYSIOLOGY ROLE OF THE URINARY SYSTEM THE URINARY SYSTEM. Components and function. V BS 122 Physiology II 151 Class of 2011
 19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
12/7/10. Excretory System. The basic function of the excretory system is to regulate the volume and composition of body fluids by:
 Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Lesson 14.1: Learning the Key Terms
 209 Lesson 14.1: Learning the Key Terms Directions: Place the letter of the best definition next to each key term. 1. collecting duct 2. distal convoluted tubule 3. glomerulus 4. nephron 5. nephron loop
209 Lesson 14.1: Learning the Key Terms Directions: Place the letter of the best definition next to each key term. 1. collecting duct 2. distal convoluted tubule 3. glomerulus 4. nephron 5. nephron loop
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Class XI Chapter 19 Excretory Products and their Elimination Biology
 Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
Excretion and Waste Management. Biology 30S - Miss Paslawski
 Excretion and Waste Management Biology 30S - Miss Paslawski Lesson 1 Waste Products and Organs 2 3 Excretion Excretion: Process by which dissolved metabolic wastes are separated from body fluids and removed
Excretion and Waste Management Biology 30S - Miss Paslawski Lesson 1 Waste Products and Organs 2 3 Excretion Excretion: Process by which dissolved metabolic wastes are separated from body fluids and removed
Chapter 11 Lecture Outline
 Chapter 11 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Chapter 11 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Urinary System URINARY SYSTEM
 URINARY SYSTEM The urinary system consists of two kidneys, two ureters, the urinary bladder, and the urethra. The formation of urine is the function of the kidneys, and the rest of the system is responsible
URINARY SYSTEM The urinary system consists of two kidneys, two ureters, the urinary bladder, and the urethra. The formation of urine is the function of the kidneys, and the rest of the system is responsible
Urinary System kidneys, ureters, bladder & urethra
 Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
The Urinary System PART A
 15 The Urinary System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Functions of the Urinary
15 The Urinary System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Functions of the Urinary
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Histology Urinary system
 Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Chapter 16 Lecture Outline
 Chapter 16 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Chapter 16 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Excretory Lecture Test Questions Set 1
 Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Other Factors Affecting GFR. Chapter 25. After Filtration. Reabsorption and Secretion. 5 Functions of the PCT
 Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Chapter 24: The Urinary System
 Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
The Urinary System. Jim Swan
 The Urinary System Jim Swan These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best
The Urinary System Jim Swan These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best
The Urinary System Dr. Gary Mumaugh
 The Urinary System Dr. Gary Mumaugh Functions of the Urinary System Filter 200 liters of blood daily, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Regulate volume and chemical
The Urinary System Dr. Gary Mumaugh Functions of the Urinary System Filter 200 liters of blood daily, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Regulate volume and chemical
Waste Products & Kidney Function
 Waste Products & Kidney Function urinary system principal means of metabolic waste removal urinary system is closely associated with reproductive system urogenital system share embryonic development share
Waste Products & Kidney Function urinary system principal means of metabolic waste removal urinary system is closely associated with reproductive system urogenital system share embryonic development share
URINARY SYSTEM ANATOMY
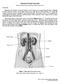 URINARY SYSTEM ANATOMY Adapted from Human Anatomy & Physiology Marieb and Hoehn (9 th ed.) OVERVIEW Metabolism of nutrients by the body produces wastes that must be removed from the body. Although excretory
URINARY SYSTEM ANATOMY Adapted from Human Anatomy & Physiology Marieb and Hoehn (9 th ed.) OVERVIEW Metabolism of nutrients by the body produces wastes that must be removed from the body. Although excretory
The Excretory System. Biology 20
 The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
PARTS OF THE URINARY SYSTEM
 EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Urinary System Functions of the Urinary system (renal) A. B. C.
 Urinary System Functions of the Urinary system (renal) A. B. C. I. Overview of fluids A. Normal volumes 1. fluid intake a. = 1500 ml b. = 750 ml c. = 250 ml (remember ETS) d. total = 2500 ml/day 2. fluid
Urinary System Functions of the Urinary system (renal) A. B. C. I. Overview of fluids A. Normal volumes 1. fluid intake a. = 1500 ml b. = 750 ml c. = 250 ml (remember ETS) d. total = 2500 ml/day 2. fluid
Urinary System kidneys, ureters, bladder & urethra
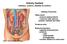 Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
Urinary bladder provides a temporary storage reservoir for urine
 Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
The Urinary System 15PART B. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
