The Functional Adaptation of the Diseased Kidney. I. Glomerular Filtration Rate *
|
|
|
- Coral Lester
- 6 years ago
- Views:
Transcription
1 Journal of Clinical Investigation Vol. 43, No. 10, 1964 The Functional Adaptation of the Diseased Kidney. I. Glomerular Filtration Rate * NEAL S. BRICKERt SAULO KLAHR, AND RICHARD E. RIESELBACH t (From the Renial Division, Department of Internal Medicine, Washington University School of Medicine, St. Louis, Mo.) In accounting for the functional capabilities as well as for certain of the functional limitations of the chronically diseased kidney, it has been postulated that, as the nephron population decreases, glomerular filtration rate (GFR) increases adaptively in the surviving nephrons (1, 2). This type of functional adaptation is reminiscent of the compensatory hypertrophy that occurs in a normal kidney after removal of the opposite organ (3, 4); however, support for its occurrence in the diseased kidney is largely circumstantial. Yet it is essential to the ultimate and complete understanding of the functional organization of the chronically diseased kidney to know whether or not this phenomenon actually occurs in advancing renal disease. The basic difficulty in examining this question experimentally has been the lack of an appropriate experimental model. The detection of a change in the level of GFR per nephron requires not only the serial measurement of filtration rate, but either a direct method for counting the number of functioning nephrons, or an indirect, but meaningful, index of the functioning nephron population. To count the functioning nephrons in the diseased kidney requires the quantitative correction for nonfiltering and other nonurine forming nephrons. Although the existence of these units may be detected in vivo in the experimentally diseased kidney (5), the available methods do not permit their accurate quantification. Thus the direct approach has not yet lent itself to a defini- * Submitted for publication April 6, 1964; accepted June 17, Supported by the National Institutes of Health (grant A-2667), the Department of the Army, Research and Development Branch (contract no. DA MD-772), and a grant-in-aid from the American Heart Association. t Work performed during the tenure of an established investigatorship, American Heart Association. tresearch fellow, U. S. Public Health Service. tive analysis of the problem, although further refinements in methodology could make this possible. In the present studies, the alternative approach has been taken. An indirect method has been used that provides a frame of reference for the functioning nephron population. This is less complex than the direct method, but it appears to bypass the methodologic barrier. The results provide unequivocal evidence that the experimentally diseased kidney of the dog is capable of undergoing a marked and sustained increase in GFR when the total (bilateral) nephron population is decreased. Methods One hundred and twenty-four experiments were performed on 26 female mongrel dogs. In each animal, two permanent hemibladders were constructed surgically to allow for the serial examination of renal function of both kidneys simultaneously. The experimental design was as follows: Control studies were performed when both kidneys were normal in order to establish the level of the GFR before there was any reduction in the nephron population. These measurements comprise the stage I studies. Pyelonephritis then was induced in one kidney of each animal, and the contralateral kidney was left unaltered. From 22 to 120 days later (mean 38 days) renal function was measured simultaneously in the diseased and contralateral control kidneys. These data comprise the stage II studies. In 5 dogs, two or more stage II studies were performed. The next step was designed to decrease the total number of functioning nephrons without decreasing further the nephron population of the diseased kidney. To accomplish this, the control kidney was either removed surgically (21 dogs) or subjected to ureteral ligation (5 dogs). The function of the diseased kidney then was restudied. The latter measurements, designated as stage III, were performed from 24 hours to 52 days after the removal or ureteral ligation of the control kidney. One study was performed in stage III on 15 dogs, and two or more studies were performed on 11 dogs. In each animal the values obtained from the diseased kidney in stage III were compared with the values from the same kidney in stage II. 1915
2 1916 N. S. BRICKER, S. KLAHR, AND R. E. RIESELBACH Experiments were performed either on hydropenic animals receiving mannitol infusions or on animals undergoing water diuresis. In each dog, the experimental conditions were identical in successive studies, except that the infusion rates were decreased in stage III to allow for the reduction in nephron population. GFR was measured in all experiments using the exogenous creatinine clearance, and creatinine was determined according to the method of Bonsnes and Taussky (6). In addition, the clearance of para-aminohippurate (PAH) was determined in 50 experiments on 14 animals. PAH was determined according to the method of Smith and associates (7). The technique employed for the induction of experimental pyelonephritis was as follows: The animals were anesthetized with sodium pentobarbital, and one kidney was exposed through a flank incision. The renal parenchyma then was punctured approximately 400 times with an electrically heated 18-gauge cautery needle. The punctures were applied diffusely over the entire renal parenchyma, and the depth of puncture was approximately 1.5 cm, a distance sufficient to enter the medulla. In some animals, 50 or more additional punctures were made with a hypodermic needle repeatedly dipped into the broth culture of pathogenic bacteria. Electrocautery was not used in association with the latter needle tracts. One to 2 ml of nutrient broth culture of Escherichia coli was administered intravenously through a peripheral vein. The organisms were obtained either from infected urine of patients or from dogs with pyelonephritis. They were isolated initially on MacConkey's medium and were incubated in plain nutrient broth for 4 to 6 hours before injection. The usual intravenous inoculum contained approximately 2 X 107 organisms. After completion of this procedure, and after assuring complete hemostasis, the kidney was replaced in the renal fossa and the wound closed. The morphologic characteristics of the experimentally diseased kidneys are as follows: The involved organs become swollen and hyperemic during the first week following inj ection. Within 2 weeks, however, the renal parenchyma consistently demonstrates contraction and TABLE I Glomerular filtration rate (GFR) in dogs in which two or more studies were made in stage 11* GFRstage Dog GFR-stage II III (34) 24.7 (40) (26) 7.3 (32) (26) 23.0 (33) (53) 18.7 (63) (8) 17.4 (14) 20.1 (21) 16.5 (30) 17.3 (42) 31.7 A 6.4 (23) 5.7 (34) B 14.4 (24) 14.1 (37) C 4.7 (7) 6.0 (14) 6.8 (20) 6.1 (28) * Numbers designating dogs correspond to those used in Table II' Numbers in parentheses indicate the interval in days following induction of experimental pyelonephritis. The three dogs labeled A, B, and C were not subjected to stage III studies. In two of these, disease was induced in the contralateral kidney; the third died after nephrectomy. scarring. Microscopically, the pathologic changes appear in radially oriented bands involving both cortex and medulla. Although the disease presumably originates in and around the needle tracts, the extension of the pathologic changes obscures the puncture sites and precludes establishment of the foregoing relationship. The microscopic abnormalities include mononuclear cell infiltration, tubular dilatation, intratubular casts, and fibrosis. Periodic acid Schiff stains demonstrate occasional thickening of glomerular basement membranes. The composite lesion resembles closely that seen in human chronic pyelonephritis. In most animals, viable bacteria may be recovered from the involved kidneys at autopsy, although the interval between induction and death may be many months. GFR typically stabilizes within 2 weeks after induction of disease, and as long as the contralateral kidney remains free of disease, GFR rarely increases after the second to third week. The characteristic response is for values either to remain constant or to decrease with time. Serial studies on a representative animal with experimental pyelonephritis have been published previously (8), and data from several of the dogs in the present series in which more than one study was performed in stage II are shown in Table I. Results GFR in the diseased kidney increased in 25 of 26 dogs after eliminating the functional contribution of the contralateral control kidney. The average increment in GFR for the group between stages II and III was 60.6%o.1 The average increment for the 21 animals subjected to unilateral nephrectomy was 58.1%, whereas the value for the 5 animals subjected to ureteral ligation was 71%. A complete tabulation of these data is included in Table II. The results from the 11 dogs in which serial studies were performed in stage III are shown in Table III. A decrease in GFR with time would not be unexpected in view of the fact that the pyelonephritic lesions remain active as judged by both histologic and bacteriologic criteria; in addition the cystotomy tubes draining the hemibladders are prone to obstruction, and once this occurs renal function deteriorates rapidly. Despite these considerations, GFR tended either to remain constant or to increase with time. When all stage III values are averaged for each of the 11 dogs in which two or more studies were performed in stage III, 1 In the 11 dogs in which more than one study was performed in stage III, the maximal value was used for these calculations.
3 ADAPTIVE INCREASE IN GFR IN THE DISEASED KIDNEY 1917 TABLE II Glomerular filtration rate in the experimentally diseased kidney of the dog before and after ureteral ligation or removal of the contralateral kidney Stage III Stage II Days after ureteral Days after ligation or Per cent Dog GFR induction GFR nephrectomy increase ml/min ml/min Ureteral ligation Mean value Nephrectomy Mean value Mean value for all dogs 60.6 the mean of these averages is 53% greater than the corresponding stage II values. Sequential measurements of PAH clearance were performed in 14 dogs (Table IV). In 5 of these, two studies and in a sixth dog four studies were performed in stage III. The average value obtained in stage III for all animals (using the maximal values in the 6 dogs with more than one study) was 66.5% greater than in stage II.2 The 2 The total increment in renal plasma flow per functioning nephron probably was greater than 66% in that PAH clearance increased in the normal kidneys between stages I and II by an average of 27.2%. An equivalent increment may be presumed to have occurred in the residual nephrons of the diseased kidneys between stages I and II. increase in GFR in the same animals for the same experiments was 69.8%o. Discussion GFR of the diseased kidney of the dog has been found to increase adaptively as the nephron population decreases. This was demonstrated by measuring GFR of the diseased organ first with a contralateral kidney contributing to function (stage II) and again after the function of the contralateral kidney had been eliminated (stage III). The total number of nephrons in the diseased organs could not have increased between stage II and stage III, unless nonfunctioning nephrons became
4 1918 N. S. BRICKER, S. KLAHR, AND R. E. RIESELBACH TABLE III Glomerular filtration rate in the 11 dogs in which two or more studies were made in stage 111* GFR- Dog stage II GFR-stage III ml/mmn ml/min (21) 23.7 (24) 30.0 (37) 31.7 (51) (4) 13.6 (21) 12.9 (31) 13.1 (37) (6) 38.3 (14) 32.2 (41) (5) 10.5 (8) 10.5 (11) (7) 7.8 (9) 12.6 (28) (13) 16.4 (41) (4) 18.8 (13) (2) 24.3 (11) (2) 17.2 (33) (3) 31.7 (12) (2) 33.2 (52) * Numbers designating dogs correspond to those used in Table II. Numbers in parentheses indicate the number of days following ablation of function of control kidney. functional. Rather, it seems more likely that any change in nephron population would consist of a decrease, due to progression of the parenchymal disease. Hence, the increments in GFR that were observed in 25 out of 26 dogs, and which for the group averaged 60.6%b, suggest that the average value for GFR per functioning nephron increased adaptively. The mechanisms initiating the increase in GFR are unknown. That hemodynamic factors resulting from rerouting of blood from the low pressure vascular bed of the control kidney may play a role is suggested by the marked increments in GFR observed as early as 24 hours after ablation of the function of the control kidney. On the other hand, this could not represent the sole explanation inasmuch as the magnitude of the in- TABLE IV Clearance of para-aminohippurate (PAH) in the experimentally diseased kidney of the dog before and after ablation of function of the contralateral uninvolved kidney* Dog Stage II Stage III ml/min ml/min (2) (3) (13) (11) (11) (14) (4) (6) (13) 54.6 (41) (11) 44.8 (37) (2) 60.6 (33) (3) (10) (3) (12) (21) 90.0 (24) (37) (51) * Numbers designating dogs correspond to those used in Table II. Numbers in parentheses indicate the number of days following ablation of function of control kidney. crement was no less (and indeed it appeared to be somewhat greater) in those animals subjected to ureteral ligation than in those in which the control kidney was removed (Table II) ; yet in the former group, it may be assumed that an appreciable amount of blood continued to flow through the obstructed kidneys (9, 10). The data obtained from the animals with unilateral hydronephrosis also imply that the increment in GFR is largely independent of the number of perfused nephrons, in contradistinction to the number of urine-forming nephrons. The rapidity of onset of the adaptive increment speaks against the possibility that retention of some unidentified substance is primarily responsible for the adaptation. Whether hormonal factors influence these changes, as they appear to influence compensatory hypertrophy in a normal kidney (11, 12), cannot be evaluated at the present time. Detailed exploration of the mechanisms responsible for the increase in filtration rate in the diseased kidney may well provide a fertile field for future investigation. From the point of view of the functional organization of a nephron, chronic hyperfiltration has intriguing implications. This single change, in a function that is mediated entirely by physical forces, must evoke major alterations in energydependent tubular transport systems. The most obvious effect of hyperfiltration would be to increase the excretory capacity of a nephron. However, if the increase in GFR is appreciable, it must alter profoundly the transport requirements of the tubular epithelial cells. Changes in excretory patterns. Hyperfiltration will result in an increase in the filtered load of all filtered solutes, and unless 100%o of the additional filtered load is reabsorbed, the excretion rate (all other things being equal) must increase. This is clearly evident for substances that are excreted predominantly by glomerular filtration. For example, for any given number of nephrons, an adaptive increment in GFR per nephron would increase the rate of excretion of creatinine and urea and would slow the rate of accumulation of these solutes in body fluids with advancing disease. Hyperfiltration would contribute importantly to the maintenance of sodium balance on an unrestricted salt intake. For this balance to be maintained, the average daily rate of excretion of so-
5 ADAPTIVE INCREASE IN GFR IN THE DISEASED KIDNEY 1919 dium per nephron must increase as the number of surviving nephrons decreases. A progressive increment in the filtered load of sodium per nephron would greatly facilitate this regulation. Hyperfiltration also would affect the excretion, and the maintenance of balance, of actively transported species other than sodium ions. For exexample, the excretion rate of phosphate relative to the filtered load increases as renal disease advances (13). One mechanism proposed for this adaptation is secondary hyperparathyroidism. However, hyperfiltration could contribute to the relative phosphaturia. The implications of hyperfiltration might even extend to protein excretion. For example, in pyelonephritis, pathologic involvement of the glomeruli is unusual, yet proteinuria occurs with considerable frequency. If some protein normally enters the glomerular filtrate, an increase in GFR per nephron should lead to a concomitant increase in this physiologic protein filtration, and unless the tubular reabsorption of protein increased to equal the filtered load, protein would escape into the urine.3 Changes in tubular transport. There is a growing body of evidence to support the view that a considerable portion of the work of the renal tubular epithelial cells is involved in the active transport of sodium (14, 15). Simple calculations dictate that if the average value for GFR per nephron increases by 50%o, the great majority of the extra filtered sodium must be reabsorbed, even though the excretion rate (per nephron) increases by as much as tenfold. Thus in advanced renal disease, it is very unusual for more than 15 to 20% of the total filtered load of sodium to be excreted (16). It is implicit, therefore, that the increase in the filtered load far exceeds the increase in excretion. Hence, the rate of active sodium transport per nephron must be supernormal under basal conditions, and hyperfiltration will lead to an increase in work and an associated increase in energy production in each surviving nephron. 3 The hyperperfusion of glomerular capillaries that appears to accompany hyperfiltration (i.e., renal plasma flow as well as GFR increased adaptively) might also contribute to proteinuria by decreasing the barrier to protein filtration and thereby increasing further the filtered load of protein entering the tubular fluid. Hyperfiltration would also necessitate an alteration in the rate limiting events controlling active transport of other species. For example, there would be an increase in the filtered load of glucose and amino acids per nephron, and complete conservation of these solutes would require an augmentation of transport rates under steady state conditions. Observations to be reported separately show an increase in the maximal velocity of transport of PAH (17) and ammonium (18) in uremic dogs. The latter substances, however, are both secreted, and the influence of filtration rate on the adaptive changes is not apparent. The extrapolation of the results of these studies to man with naturally occurring chronic renal disease must be made with a certain degree of caution. In the latter situation, the rate of progression of the disease may be extremely slow, and the decrease in nephron population would occur gradually. In the present studies, the nephron population was decreased abruptly, although in those animals in which the ureter of the control kidney was ligated, the number of nephrons contributing to urine formation was decreased without a corresponding decrement in the number of viable nephrons, or in the blood supply to these nephrons. Nevertheless, it may be concluded from these studies that the severely diseased kidney is capable of undergoing a marked and sustained increase in GFR. Presumably the same adaptation could occur in chronic progressive renal disease in man. If so, the possibility exists that GFR may increase to different degrees in different diseases, and this phenomenon could well explain some of the functional differences among various forms of chronic Bright's disease. For example, in glomerulonephritis, hypertension, and other diseases that preferentially affect either the glomeruli or the preglomerular arterioles, the increment in GFR per nephron could be less marked than in pyelonephritis. This could contribute to the differences observed in group plots of patients with glomerulonephritis versus those with pyelonephritis (19, 20). Thus, with a greater GFR per nephron, one would expect a greater saltlosing tendency, and an earlier loss of concentrating ability. The fact that acidosis appears to occur somewhat earlier in pyelonephritis than in glomerulonephritis might also be more amenable
6 1920 N. S. BRICKER, S. KLAHR, AND R. E. RIESELBACH to explanation if, for a given filtration rate, there were fewer nephrons in pyelonephritis than in glomerulonephritis. One final point deserves emphasis. The present studies underscore the need to differentiate conceptually between solute diuresis due to hyperfiltration and that due to an osmotic diuresis such as might be induced by high filtered loads of urea in the uremic state. In the former situation, net transport of sodium and other solutes is increased, whereas in the latter, net reabsorption of sodium is diminished. The implications of sodium loss during salt deprivation could be quite different (in terms of the functional integrity of the nephron) if net sodium reabsorption were supernormal than if it were decreased. Summary These experiments were designed to investigate the capacity of the residual nephrons of the experimentally diseased kidney of the dog to undergo an adaptive increase in glomerular filtration. Glomerular filtration rate (GFR) was measured in both kidneys of 26 dogs with unilateral renal disease. Thereafter, the uninvolved contralateral kidney was either removed (21 dogs) or its ureter ligated (5 dogs). GFR increased in the diseased kidneys in 25 of the 26 animals; the average increment for the group was 60.6%. Renal plasma flow was measured in 14 of these animals, and the average increment in this function was 66.5 %. The mechanisms underlying the adaptive increase in filtration rate are poorly understood; however, the influence of this adaptation on the functional characteristics of the nephron is striking. Hyperfiltration of the degree noted in these studies must lead not only to an increase in excretory capacity but to an increase in active transport of a number of solutes including sodium. Supernormal rates of sodium transport under basal conditions in turn would necessitate an increase in basal energy production and utilization per nephron. If similar degrees of hyperfiltration occur in man with chronic renal disease, this adaptation could contribute importantly both to the functional capabilities and to certain of the functional limitations observed in the chronically diseased kidney. References 1. Platt, R. Structural and functional adaptation in renal failure. Brit. med. J. 1952, 1, Bricker, N. S. Chronic progressive renal disease: pathologic physiology and relation to treatment. Progr. cardiovasc. Dis. 1961, 4, 170. Heart, Kidney and Electrolytes, C. K. Friedberg, Ed. New York, Grune & Stratton, Addis, T., B. A. Myers, and J. Oliver. The regulation of renal activity. IX. The effect of unilateral nephrectomy on the function and structure of the remaining kidney. Arch. intern. Med. 1924, 34, Kohlberg, A. Relations of renal tubular and glomerular function as influenced by 75 per cent reduction of nephron population. Scand. J. clin. Lab. Med. 1959, 11 (suppl.), Damadian, R. V., E. Shwayri, and N. S. Bricker. Demonstration of a population of nephrons in diseased kidneys with perfused glomeruli that do not contribute to urine formation. In preparation. 6. Bonsnes, R. W., and H. H. Taussky. On the colorimetric determination of creatinine by the Jaffe reaction. J. biol. Chem. 1945, 158, Smith, H. W., N. Finkelstein, L. Aliminosa, B. Crawford, and M. Graber. The renal clearances of substituted hippuric acid derivatives and other aromatic acids in dog and man. J. clin. Invest. 1945, 24, Bricker, N. S., P. A. F. Morrin, and S. W. Kime, Jr. The pathologic physiology of chronic Bright's disease: an exposition of the "intact nephron hypothesis." Amer. J. Med. 1960, 28, Selkurt, E. E. Effect of ureteral blockage on renal blood flow and urinary concentrating ability. Amer. J. Physiol. 1963, 205, Levy, S. E., M. F. Mason, T. R. Harrison, and A. Blalock. The effects of ureteral occlusion on the blood flow and oxygen consumption of the kidneys of unanesthetized dogs. Surgery 1937, 1, Winternitz, M. C., and L. L. Waters. The effect of hypophysectomy on compensatory renal hypertrophy in dogs. Yale J. Biol. Med. 1940, 12, Zeckwer, I. T. Compensatory growth of the kidney after unilateral nephrectomy in thyroidectomized rats. Amer. J. Physiol. 1946, 145, Goldman, R., and S. H. Bassett. Phosphorous excretion in renal failure. J. clin. Invest. 1954, 33, Kramer, J., and P. Deetjan. Sodium reabsorption and oxygen consumption in the mammalian kidney. Proc. 1st Int. Congr. Nephrol. 1961, Thaysen, J. H., N. A. Lassen, and 0. Munck. Sodium transport and oxygen consumption in the mammalian kidney. Proc. 1st Int. Congr. Nephrol. 1961, 692.
7 ADAPTIVE INCREASE IN GFR IN THE DISEASED KIDNEY Nickel, J. F., P. B. Lowrance, E. Leifer, and S. E. Bradley. Renal function, electrolyte excretion and body fluids in patients with chronic renal insufficiency before and after sodium deprivation. J. clin. Invest. 1953, 32, Rieselbach, R. E., L. E. Todd, M. Rosenthal, and N. S. Bricker. Adaptive capacity of the residual nephrons of the chronically diseased kidney in the dog (abstract). J. Lab. clin. Med. 1963, 62, Dorhout Mees, E. J., M. Machado, and N. S. Bricker. Unpublished observations. 19. Hodler, J. Etude de l'acidose au cours de pyelonephrites, de glomerulonephrites et de nephroscleroses avancees. Proc. 1st Int. Congr. Nephrol. 1961, Brod, J., V. Prat, and R. Dejdar. Early functional diagnosis of chronic pyelonephritis with some remarks on the pathogenesis of the pyelonephritic contracted kidney in Biology of Pyelonephritis, Henry Ford International Symposium. Boston, Little, Brown, 1960, p. 311.
The Control of Phosphate Exeretion in Uremia *
 Journal of Clinical Investigation Vol. 5, No. 5, 19 The Control of Phosphate Exeretion in Uremia * E. SLATOPOLSKY, L. GRADOWSKA, C. KASHEMSANT, R. KELTNER, C. MANLEY, AND N. S. BRICKER t (From the Renal
Journal of Clinical Investigation Vol. 5, No. 5, 19 The Control of Phosphate Exeretion in Uremia * E. SLATOPOLSKY, L. GRADOWSKA, C. KASHEMSANT, R. KELTNER, C. MANLEY, AND N. S. BRICKER t (From the Renal
A. Correct! Flushing acids from the system will assist in re-establishing the acid-base equilibrium in the blood.
 OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
Early Experimental Pyelonephritis
 Urinary Concentrating Ability in Early Experimental Pyelonephritis DONALD KAYE and HEONIR Roca- From the Department of Medicine, Woman's Medical College of Pennsylvania, Philadelphia, Pennsylvania 19129
Urinary Concentrating Ability in Early Experimental Pyelonephritis DONALD KAYE and HEONIR Roca- From the Department of Medicine, Woman's Medical College of Pennsylvania, Philadelphia, Pennsylvania 19129
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
QUANTITATIVE HISTOCHEMISTRY OF THE NEPHRON. V.
 QUANTITATIVE HISTOCHEMISTRY OF THE NEPHRON. V. ALKALINE PHOSPHATASE AND LACTIC DEHYDROGENASE ACTIVITIES IN LUPUS NEPHRITIS * By VICTOR E. POLLAK,t SJOERD L. BONTING, ROBERT C. MUEHRCKE AND ROBERT M. KARK
QUANTITATIVE HISTOCHEMISTRY OF THE NEPHRON. V. ALKALINE PHOSPHATASE AND LACTIC DEHYDROGENASE ACTIVITIES IN LUPUS NEPHRITIS * By VICTOR E. POLLAK,t SJOERD L. BONTING, ROBERT C. MUEHRCKE AND ROBERT M. KARK
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
The Excretory System
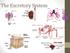 The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
Structural and Functional Adaptation after Reduction of Nephron Population
 TIlE YALE JOUJRNAL OF BIOLOGY AND MEDICINE 52 (1979), 271-287 Structural and Functional Adaptation after Reduction of Nephron Population FREDRIC 0. FINKELSTEIN AND JOHN P. HAYSLETT Departments of Medicine
TIlE YALE JOUJRNAL OF BIOLOGY AND MEDICINE 52 (1979), 271-287 Structural and Functional Adaptation after Reduction of Nephron Population FREDRIC 0. FINKELSTEIN AND JOHN P. HAYSLETT Departments of Medicine
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
EXCRETION IN HUMANS 31 JULY 2013
 EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Pressure Diuresis 9 Sample Student Essays
 Pressure Diuresis 9 Sample Student Essays Below please find assembled consecutively in one document the brief analyses submitted by nine students in Mammalian Physiology 08 to the Teach Yourself Pressure
Pressure Diuresis 9 Sample Student Essays Below please find assembled consecutively in one document the brief analyses submitted by nine students in Mammalian Physiology 08 to the Teach Yourself Pressure
The Excretory System. Biology 20
 The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
PARTS OF THE URINARY SYSTEM
 EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Lecture-2 Review of the previous lecture:
 Lecture-2 Review of the previous lecture: -Kidney s function is to clean the blood by the removing of the waste plus adding some valuable substances -kidney failure will lead to death for many reasons,
Lecture-2 Review of the previous lecture: -Kidney s function is to clean the blood by the removing of the waste plus adding some valuable substances -kidney failure will lead to death for many reasons,
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
HUMAN SUBJECT 1. Syracuse, N. Y.) the urine of increasing quantities of these buffers, it has been found in man as in the dog that (1)
 THE RENAL REGULATION OF ACID-BASE BALANCE IN MAN. II. FACTORS AFFECTING THE EXCRETION OF TITRATABLE ACID BY THE NORMAL HUMAN SUBJECT 1 By W. A. SCHIESS, J. L. AYER, W. D. LOTSPEICH AND R. F. PITTS WITH
THE RENAL REGULATION OF ACID-BASE BALANCE IN MAN. II. FACTORS AFFECTING THE EXCRETION OF TITRATABLE ACID BY THE NORMAL HUMAN SUBJECT 1 By W. A. SCHIESS, J. L. AYER, W. D. LOTSPEICH AND R. F. PITTS WITH
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
(Received 23 January 1961) Crawford & Kennedy (1959) found the prolonged saluretic and diuretic
 454 J. Phyeiol. (1961), 157, pp. 454-461 With 3 text-figure Printed in Great Britain THE ACTION OF CHLOROTHIAZIDE IN THE PERFUSED CAT KIDNEY BY T. DE LIMA AND MARY F. LOCKETT From the Department of Physiology
454 J. Phyeiol. (1961), 157, pp. 454-461 With 3 text-figure Printed in Great Britain THE ACTION OF CHLOROTHIAZIDE IN THE PERFUSED CAT KIDNEY BY T. DE LIMA AND MARY F. LOCKETT From the Department of Physiology
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Filtration and Reabsorption Amount Filter/d
 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD Contact me at lharris@lsuhsc.edu Renal Physiology Lecture 3 Renal Clearance and Glomerular Filtration Filtration and Reabsorption Amount Filter/d Amount
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD Contact me at lharris@lsuhsc.edu Renal Physiology Lecture 3 Renal Clearance and Glomerular Filtration Filtration and Reabsorption Amount Filter/d Amount
On the Adaptation in Sodium Excretion in Chronic Uremia
 On the Adaptation in Sodium Excretion in Chronic Uremia THE EFFECTS OF "PROPORTIONAL REDUCTION" OF SODIUM INTAKE R. WILLIAM SCHMIDT, JACQUES J. BOURGOIGNIE, and NEAL S. BRICKER From the Division of Nephrology,
On the Adaptation in Sodium Excretion in Chronic Uremia THE EFFECTS OF "PROPORTIONAL REDUCTION" OF SODIUM INTAKE R. WILLIAM SCHMIDT, JACQUES J. BOURGOIGNIE, and NEAL S. BRICKER From the Division of Nephrology,
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
BIOL 2402 Renal Function
 BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
Biology Slide 1 of 36
 Biology 1 of 36 38 3 The Excretory System 2 of 36 Functions of the Excretory System 1.Function: process which eliminates metabolic wastes 3 of 36 Functions of the Excretory System (The skin excretes excess
Biology 1 of 36 38 3 The Excretory System 2 of 36 Functions of the Excretory System 1.Function: process which eliminates metabolic wastes 3 of 36 Functions of the Excretory System (The skin excretes excess
Functions of the kidney:
 Diseases of renal system : Normal anatomy of renal system : Each human adult kidney weighs about 150 gm, the ureter enters the kidney at the hilum, it dilates into a funnel-shaped cavity, the pelvis, from
Diseases of renal system : Normal anatomy of renal system : Each human adult kidney weighs about 150 gm, the ureter enters the kidney at the hilum, it dilates into a funnel-shaped cavity, the pelvis, from
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
Kidney Physiology. Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed
 Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Alterations of Renal and Urinary Tract Function
 Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
simultaneously excreted. They also brought forward some evidence to
 THE EXCRETION OF CHLORIDES AND BICARBON- ATES BY THE HUMAN KIDNEY. BY H. W. DAVIES, M.B., B.S., J. B. S. HALDANE, M.A. AND G. L. PESKETT, B.A. (From the Laboratory, Cherwell, Oxford.) AM BARD and PAPI
THE EXCRETION OF CHLORIDES AND BICARBON- ATES BY THE HUMAN KIDNEY. BY H. W. DAVIES, M.B., B.S., J. B. S. HALDANE, M.A. AND G. L. PESKETT, B.A. (From the Laboratory, Cherwell, Oxford.) AM BARD and PAPI
CONCERNING THE EFFECTS OF MAGNESIUM SULFATE ON RENAL FUNCTION, ELECTROLYTE EXCRETION, AND CLEARANCE OF MAGNESIUM
 CONCERNING THE EFFECTS OF MAGNESIUM SULFATE ON RENAL FUNCTION, ELECTROLYTE EXCRETION, AND CLEARANCE OF MAGNESIUM B. I. Heller,, J. F. Hammarsten, F. L. Stutzman J Clin Invest. 1953;32(9):858-861. https://doi.org/10.1172/jci102803.
CONCERNING THE EFFECTS OF MAGNESIUM SULFATE ON RENAL FUNCTION, ELECTROLYTE EXCRETION, AND CLEARANCE OF MAGNESIUM B. I. Heller,, J. F. Hammarsten, F. L. Stutzman J Clin Invest. 1953;32(9):858-861. https://doi.org/10.1172/jci102803.
Effect of Growth Hormone on Tubular Transport of Phosphate
 Journal of Clinical Investigation Vol. 43, No. 8, 1964 Effect of Growth Hormone on Tubular Transport of Phosphate in Normal and Parathyroidectomized Dogs * JACQUES CORVILAIN AND MAURICE ABRAMOW WITH THE
Journal of Clinical Investigation Vol. 43, No. 8, 1964 Effect of Growth Hormone on Tubular Transport of Phosphate in Normal and Parathyroidectomized Dogs * JACQUES CORVILAIN AND MAURICE ABRAMOW WITH THE
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Excretory System. Biology 2201
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System. Excretory System
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
Renal Physiology. April, J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine.
 Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
You should know the T max for any substance that you use and for PAH ; T max = mg / min
 Tubular function - What is clearance? o clearance referred to the theoretical volume of plasma from which a substance is cleared ( cleaned ) over a period of time and so its unit would be ((ml/min)) -
Tubular function - What is clearance? o clearance referred to the theoretical volume of plasma from which a substance is cleared ( cleaned ) over a period of time and so its unit would be ((ml/min)) -
Lab 19 The Urinary System
 Lab 19 The Urinary System Laboratory Objectives Identify and describe the micro- and macroscopic anatomy of the kidney. Track the blood flow in and out of the kidney. Compare blood, glomerular filtrate,
Lab 19 The Urinary System Laboratory Objectives Identify and describe the micro- and macroscopic anatomy of the kidney. Track the blood flow in and out of the kidney. Compare blood, glomerular filtrate,
Question 1: Solution 1: Question 2: Question 3: Question 4: Class X The Excretory System Biology
 A. MULTIPLE CHOICE TYPE: (select the most appropriate option in each case) Book Name: Selina Concise Question 1: Excretion primarily involves (a) removal of all byproducts during catabolism (b) removal
A. MULTIPLE CHOICE TYPE: (select the most appropriate option in each case) Book Name: Selina Concise Question 1: Excretion primarily involves (a) removal of all byproducts during catabolism (b) removal
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
Chapter 10: Urinary System & Excretion
 Chapter 10: Urinary System & Excretion Organs of Urinary System Kidneys (2) form urine Ureters (2) Carry urine from kidneys to bladder Bladder Stores urine Urethra Carries urine from bladder to outside
Chapter 10: Urinary System & Excretion Organs of Urinary System Kidneys (2) form urine Ureters (2) Carry urine from kidneys to bladder Bladder Stores urine Urethra Carries urine from bladder to outside
Physiology Lecture 2. What controls GFR?
 Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Chapter 23. Composition and Properties of Urine
 Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
Effect of an Intravenous Sodium Chloride Load on Renal Hemodynamics and Electrolyte Excretion in Essential Hypertension
 Effect of an Intravenous Sodium Chloride Load on Renal Hemodynamics and Electrolyte Excretion in Essential Hypertension BY PAUL T. COTTIER, M.D., JOHN M. WELLER, M.D., AND SIBLEY W. HOOBLER, M.D. Excretion
Effect of an Intravenous Sodium Chloride Load on Renal Hemodynamics and Electrolyte Excretion in Essential Hypertension BY PAUL T. COTTIER, M.D., JOHN M. WELLER, M.D., AND SIBLEY W. HOOBLER, M.D. Excretion
41B. Metabolism produces wastes that must be eliminated from the body. This. Renal System Physiology: Computer Simulation
 41B E X E R C I S E Renal System Physiology: Computer Simulation O B J E C T I V E S 1. To define the following terms: glomerulus, glomerular capsule, renal corpuscle, renal tubule, nephron, proximal convoluted
41B E X E R C I S E Renal System Physiology: Computer Simulation O B J E C T I V E S 1. To define the following terms: glomerulus, glomerular capsule, renal corpuscle, renal tubule, nephron, proximal convoluted
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
Use the following diagram to answer the next question. 1. In the diagram above, pressure filtration occurs in a. W b. X c. Y d. Z
 Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Urinary System BIO 250. Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat. Routes of Waste Elimination
 Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
dynamic action of ingested amino acids effected
 THE.EFFECT OF GLYCINE ON THE PRODUCTION AND EXCRETION OF URIC ACID1 BY MEYER FRIEDMAN (Fromn the Harold Brunn Institute for Cardiovascular Research, San Francisco, California) Mt. Zion Hospital, (Received
THE.EFFECT OF GLYCINE ON THE PRODUCTION AND EXCRETION OF URIC ACID1 BY MEYER FRIEDMAN (Fromn the Harold Brunn Institute for Cardiovascular Research, San Francisco, California) Mt. Zion Hospital, (Received
Renal Clearance. Dr. Eman El Eter
 Renal Clearance Dr. Eman El Eter Concept of clearance Clearance is the volume of plasma that is completely cleared of a substance each minute. Example: Renal clearance of Substance X is defined as the
Renal Clearance Dr. Eman El Eter Concept of clearance Clearance is the volume of plasma that is completely cleared of a substance each minute. Example: Renal clearance of Substance X is defined as the
hold for the human kidney.2 Shannon and Smith (4) have rightfully stressed
 THE RENAL EXCRETION OF INULIN AT LOW PLASMA CONCEN- TRATIONS OF THIS COMPOUND, AND ITS RELATIONSHIP TO THE GLOMERULAR FILTRATION RATE IN NORMAL, NEPHRITIC AND HYPERTENSIVE INDIVIDUALS' By BENJAMIN F. MILLER,
THE RENAL EXCRETION OF INULIN AT LOW PLASMA CONCEN- TRATIONS OF THIS COMPOUND, AND ITS RELATIONSHIP TO THE GLOMERULAR FILTRATION RATE IN NORMAL, NEPHRITIC AND HYPERTENSIVE INDIVIDUALS' By BENJAMIN F. MILLER,
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
A. Incorrect! The urinary system is involved in the regulation of blood ph. B. Correct! The urinary system is involved in the synthesis of vitamin D.
 Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
M6ller, McIntosh and Van Slyke (5) has been employed. The cases. changes in functional activity. Indications suggesting that such changes
 STUDIES OF UREA EXCRETION. VIII. THE EFFECTS ON THE UREA CLEARANCE OF CHANGES IN PROTEIN AND SALT CONTENTS OF THE DIET BY CUTHBERT L. COPE I (From the Hospital of the Rockefeller Institute for Medical
STUDIES OF UREA EXCRETION. VIII. THE EFFECTS ON THE UREA CLEARANCE OF CHANGES IN PROTEIN AND SALT CONTENTS OF THE DIET BY CUTHBERT L. COPE I (From the Hospital of the Rockefeller Institute for Medical
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
28/04/2013 LEARNING OUTCOME C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS STUDENT ACHIEVEMENT INDICATORS URINARY SYSTEM & EXCRETION
 LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
organs of the urinary system
 organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
PHSI2006/2906: Integrated Physiology B
 PHSI2006/2906: Integrated Physiology B TOPIC 1: RESPIRATION 1. The Mechanics of Breathing...2 2. Work of Breathing....5 3. Pulmonary Gas Exchange.. 10 4. Transport of Oxygen...16 5. Control of Respiration...20
PHSI2006/2906: Integrated Physiology B TOPIC 1: RESPIRATION 1. The Mechanics of Breathing...2 2. Work of Breathing....5 3. Pulmonary Gas Exchange.. 10 4. Transport of Oxygen...16 5. Control of Respiration...20
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
JINNAH SINDH MEDICAL UNIVERSITY
 MODULE TITLE INTRODUCTION TARGET STUDENTS DURATION MODULE OUTCOMES Spiral -1 Renal and Excretory-1 Module The Renal and Excretory-1 Module is designed to help the learners understand how the urinary system
MODULE TITLE INTRODUCTION TARGET STUDENTS DURATION MODULE OUTCOMES Spiral -1 Renal and Excretory-1 Module The Renal and Excretory-1 Module is designed to help the learners understand how the urinary system
Urine Formation by the Kidneys: I. Glomerular Filtration, Renal Blood Flow and Their Control.
 Urine Formation by the Kidneys: I. Glomerular Filtration, Renal Blood Flow and Their Control. Chapter 26 Yanal A Shafagoj. MD. PhD Lecture-1 Introduction 31/3/2015 1 University of Jordan Faculty of Medicine
Urine Formation by the Kidneys: I. Glomerular Filtration, Renal Blood Flow and Their Control. Chapter 26 Yanal A Shafagoj. MD. PhD Lecture-1 Introduction 31/3/2015 1 University of Jordan Faculty of Medicine
PHGY210 Renal Physiology
 PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
EXCRETORY SYSTEM E. F. G. H.
 XRTORY SYSTM 1. Label the following parts of the nephron in the diagram below:..... F. G. H. I. J. K. L. 2. Identify the following as either True or False: There is a greater osmotic concentration in the
XRTORY SYSTM 1. Label the following parts of the nephron in the diagram below:..... F. G. H. I. J. K. L. 2. Identify the following as either True or False: There is a greater osmotic concentration in the
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
12/7/10. Excretory System. The basic function of the excretory system is to regulate the volume and composition of body fluids by:
 Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
man of the effects of diabetes and of insulin on the maximum ability of the tubules to reabsorb glucose.
 EFFECT OF DIABETES AND INSULIN ON THE MAXIMUM CA- PACITY OF THE RENAL TUBULES TO REABSORB GLUCOSE t By SAUL J. FARBER, EUGENE Y. BERGER, AND DAVID P. EARLE (From the Department of Medicine, New York University
EFFECT OF DIABETES AND INSULIN ON THE MAXIMUM CA- PACITY OF THE RENAL TUBULES TO REABSORB GLUCOSE t By SAUL J. FARBER, EUGENE Y. BERGER, AND DAVID P. EARLE (From the Department of Medicine, New York University
Functions of the Urinary System
 The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Regulate aspects of homeostasis Water balance Electrolytes Acid-base balance in the blood
The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Regulate aspects of homeostasis Water balance Electrolytes Acid-base balance in the blood
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Excretory Lecture Test Questions Set 1
 Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Studies on the Control of Sodium Excretion
 Studies on the Control of Sodium Excretion in Experimental Uremia RAYMOND G. SCHULTZE, HowARD S. SHAPIRo, and NEAL S. BRICKER From the Renal Division, Department of Internal Medicine, Washington University
Studies on the Control of Sodium Excretion in Experimental Uremia RAYMOND G. SCHULTZE, HowARD S. SHAPIRo, and NEAL S. BRICKER From the Renal Division, Department of Internal Medicine, Washington University
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
PHYSICAL PROPERTIES AND DETECTION OF NORMAL CONSTITUENTS OF URINE
 PHYSICAL PROPERTIES AND DETECTION OF NORMAL CONSTITUENTS OF URINE - OBJECTIVES: 1- The simple examination of urine. 2- To detect some of the normal organic constituents of urine. 3- To detect some of the
PHYSICAL PROPERTIES AND DETECTION OF NORMAL CONSTITUENTS OF URINE - OBJECTIVES: 1- The simple examination of urine. 2- To detect some of the normal organic constituents of urine. 3- To detect some of the
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
College of Medicine, Newcastle-upon-Tyne.)
 GLUCOSE ABSORPTION IN THE RENAL TUBULES OF THE FROG. BY G. A. CLARK. (From the Physiological Laboratory of the University of Durham College of Medicine, Newcastle-upon-Tyne.) OPINION is divided on the
GLUCOSE ABSORPTION IN THE RENAL TUBULES OF THE FROG. BY G. A. CLARK. (From the Physiological Laboratory of the University of Durham College of Medicine, Newcastle-upon-Tyne.) OPINION is divided on the
Chapter 20 Diseases of the kidney:
 Chapter 20 Diseases of the kidney: 1. Which of the following is seen in Nephrotic syndrome (2000, 2004) (a) Albumin is lost in the urine, while other globulins are unaffected (b) Early hypertension (c)
Chapter 20 Diseases of the kidney: 1. Which of the following is seen in Nephrotic syndrome (2000, 2004) (a) Albumin is lost in the urine, while other globulins are unaffected (b) Early hypertension (c)
You will test a sample of the patient s urine to determine if her kidneys are functioning normally.
 STO-118 A Kidney Problem? The Case Ten years ago, your patient was diagnosed with Type 2 diabetes. She has been careless about following the treatment needed to keep her blood glucose levels regulated.
STO-118 A Kidney Problem? The Case Ten years ago, your patient was diagnosed with Type 2 diabetes. She has been careless about following the treatment needed to keep her blood glucose levels regulated.
After studying this lecture, you should be able to...
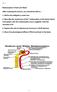 Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
The Urinary System. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
EFFECTS OF PROBENECID, SODIUM SALICYLATE, 2,4-DINITROPHENOL AND PYRAZINAMIDE ON RENAL SECRETION OF URIC ACID IN CHICKENS
 8189 EFFECTS OF PROBENECID, SODIUM SALICYLATE, 2,4-DINITROPHENOL AND PYRAZINAMIDE ON RENAL SECRETION OF URIC ACID IN CHICKENS BOHDAN R. NECHAY AND LARYSSA NECHAY Department of Pharmacology and Therapeutics,
8189 EFFECTS OF PROBENECID, SODIUM SALICYLATE, 2,4-DINITROPHENOL AND PYRAZINAMIDE ON RENAL SECRETION OF URIC ACID IN CHICKENS BOHDAN R. NECHAY AND LARYSSA NECHAY Department of Pharmacology and Therapeutics,
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
UNIT 3 Conditions supporting life
 Biology Form 4 Page 32 Ms. R. Buttigieg UNIT 3 Conditions supporting life In this unit we shall be seeing how an important condition that supports life is the ability of the organism to maintain a constant
Biology Form 4 Page 32 Ms. R. Buttigieg UNIT 3 Conditions supporting life In this unit we shall be seeing how an important condition that supports life is the ability of the organism to maintain a constant
entirely by glomerular filtration and was neither reabsorbed nor secreted
 6I2.46I.63 INORGANIC SULPHATE EXCRETION BY THE HUMAN KIDNEY. BY CUTHBERT L. COPE. (From the Biochemistry Department, Oxford, and the Radcliffe Infirmary, Oxford.) IN putting forward his modern theory of
6I2.46I.63 INORGANIC SULPHATE EXCRETION BY THE HUMAN KIDNEY. BY CUTHBERT L. COPE. (From the Biochemistry Department, Oxford, and the Radcliffe Infirmary, Oxford.) IN putting forward his modern theory of
Excretion and Water Balance
 Excretion and Water Balance In the body, water is found in three areas, or compartments: Plasma, the liquid portion of the blood without the blood cells, makes up about 7 percent of body fluid. The intercellular
Excretion and Water Balance In the body, water is found in three areas, or compartments: Plasma, the liquid portion of the blood without the blood cells, makes up about 7 percent of body fluid. The intercellular
SUSCEPTIBILITY OF RATS WITH HORMONAL HYPERTENSION
 SUSCEPTIBILITY OF RATS WITH HORMONAL HYPERTENSION TO EXPERIMENTAL PYELONEPHRITIS 1, 2 By JAMES W. WOODS (From the Department of Medicine, University of North Carolina School of Medicine, Chapel Hill, N.
SUSCEPTIBILITY OF RATS WITH HORMONAL HYPERTENSION TO EXPERIMENTAL PYELONEPHRITIS 1, 2 By JAMES W. WOODS (From the Department of Medicine, University of North Carolina School of Medicine, Chapel Hill, N.
RENAL FUNCTION An Overview
 RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
