PANCREATITIS. By April McMurray. March 14, 2013 NDFS 356
|
|
|
- Norah Hensley
- 5 years ago
- Views:
Transcription
1 PANCREATITIS By April McMurray March 14, 2013 NDFS 356
2 INTRODUCTION The pancreas is a small gland that sits behind the stomach and plays an important role in digestion (1). Its head is situated within the curvature of the duodenum of the small intestine, where its secretions flow from the pancreatic duct through the Ampulla of Vater (2). The functional unit of the pancreas is the acinar cell, which is responsible for synthesizing, storing, secreting digestive enzymes into the pancreatic duct (3). The Islet of Langerhans are also an important unit of the pancreas, which have endocrine function and secrete hormones directly into the bloodstream (3). The pancreas has both endocrine and exocrine functions. The Islets of Langerhans produce the hormones insulin and glucagon to regulate the level of glucose in the blood (1). The blood flow in the pancreas follows from the islets to the acinar cells, allowing insulin to even affect the pancreatic exocrine function (3). Somatostatin, also produced by the pancreas, inhibits the release of these hormones, as well as the exocrine functions (3). The exocrine function of the pancreas is involved in digestion, as the digestive enzymes produced by the acinar cells are secreted into the pancreatic duct and into the duodenum (2). The pacreas can secrete up to 2.5 L per day (4). In addition to the digestive enzymes, the ductal epithelial cells secrete bicarbonate, and alkaline secretion which neutralizes the content of the stomach as is enters the small intestine (3). The major digestive enzymes are amylases, which digest starches and glycogen, lipases, which act together with bile salts to break down fat, and proteases, which cleave amino acids for the breakdown of protein (3). The pancreas is stimulated both by neural and hormonal responses, with ingested foods playing an important roll (2). The primary hormonal stimulants are secretin, acetylcholine (Ach), and cholecystokinin (CCK) (3). There are three phases during which the pancreas is stimulated to produce these digestive
3 enzymes. The cephalic phase is mediated by the vagus nerve and initiated by the sight, smell, taste, or even anticipation of food (2). The Acinar cells are stimulated but no bicarbonate is released (3). The second phase, the gastric phase, is initiated by gastric distention with the presence of food in the stomach (2). The intestinal phase, has the most potent effect on the pancreatic secretions, and is mediated by CCK (2). As food enters the small intestine, amylase, lipase and protease are all released from the pancreas into the duodenum (3). The duodenum is the most important site for lipase secretion, and it acts with bile salts for full digestive activity (3). The proteases, trypsin, chymotrypsin, and elastase, are stored in the pancreas in their inactive form and are activated when they enter the duodenum (3). DISEASE DESCRIPTION Pancreatitis is inflammation of the pancreas and is characterized by pancreatic edema, cellular exudate and fat necrosis (2). The release of active proteases within the pancreas stimulate auto-digestion and an intense inflammatory response (3). With a rapid onset, symptoms and side effects vary from mild to severe (3). Acute pancreatitis (AP) is a sudden attack and a full recovery is typical, whereas chronic pancreatitis (CP) is a more persistent condition and the pancreas can suffer more permanent damage (1). Cases of acute and chronic pancreatitis affect more than 80,000 Americans per year (5). PATHOPHYSIOLOGY The pathophysiology for pancreatitis is not entirely understood. Acinar cell injury is caused by the activation of trypsinogen to trypsin within the cells, enough to overwhelm the regular mechanisms such as pancreatic secretory trypsion inhibitor (PSTI) and alpha-antitrypsin (5). Trypsin in turn catalyzes more proteases to their active forms while still in the pancreas, causing a downward cycle of auto-digestion and protease activation (5). In experimental
4 pancreatitis, this can occur within 10 minutes of onset (5). It is still unclear as to the cause of the activation of trypsinogen to trypsin; causes include gallstones and alcohol abuse (although the mechanism is not fully understood), cystic fibrosis, genetic mutations and the presence of lysosomes (5). The progression of AP happens in two stages. The first stage typically lasts a week, and is characterized by the initiation of the inflammatory cascade (5). Signs of pancreatic ischemia, edema, and systemic inflammatory response syndrome (SIRS) are noted (5). Extrapancreatic organ failure sometimes occurs secondary to the inflammation, depending on the severity of the case (5) % of pancreatitis cases will resolve without progressing to the second stage (5). This second stage can last weeks to months, and is characterized by more severe pancreatic damage, necrosis, and multi-organ failure (5). Death can occur rapidly during the first two weeks if the case is severe enough (5). The pathophysiology of pancreatitic episodes in chronic pancreatitis are mostly the same as acute, but it is less understood than AP (6). There are several hypotheses explaining the mechanisms, but most lack evidence. The most supported hypothesis suggests that CP is caused from recurring episodes of acute pancreatitis (6). With similar features of the acute condition edema, inflammation, ischemia, necrosis this causes extensive damage and permanently scarred pancreatic tissue (6). Chronic pancreatitis can take years to develop, and can often have silent symptoms (6). However, with time, several complications can arise from the condition. Microcirculatory injury, inflammation, oxidative stress, bacterial translocation and fibrosis can occur (6). Sometimes pancreatic fluids can leak into other organs, causing damage (6). Other organs that are affected are the kidneys and lungs (6).
5 Eventually, pancreatitis will lead to both endocrine and exocrine failure. A consequence of exocrine dysfunction is steatorrhea. A feature of advanced conditions of chronic pancreatitis, steatorrhea doesn't occur until lipase secretions are less than 10% of the normal output (6). The poor digestion and absorption of fat causes loose, foul-smelling, fatty stools (6). A complication of endocrine dysfunction is diabetes mellitus. A slightly different condition than either type 1 or type 2, diabetes as a result of chronic pancreatitis is not caused by a complete destruction of the Islet of Langerhans, although some function is lost (6). For unknown reasons, the pancreas will still secrete some insulin if glucagon-like peptide 1 is administered (6). However, the pancreas' ability to secrete glucagon is completely lost, and patients receiving insulin therapy (eventually 50%) must monitor blood glucose carefully to not cause hypoglycemia (6) % of all CP patients will eventually get diabetes (6). ETIOLOGY The mechanisms of the causes of pancreatitis are still not fully understood, but as understanding increases, the number of idiopathic cases will decrease. The principal cause of acute pancreatitis is gallstones (5). Gallstones account for 40% of AP incidents (5). The small gallstones in particular, which are small enough to leave the gallbladder and get lodged in the pancreatic duct, causing an obstruction (5). AP will affect 3-7% of people with gallstones (5). The best way to treat this problem is to remove the gallstones, and in some cases, the gallbladder (5). Other types of obstructions which are less common causes of pancreatitis are biliary sludge and tumors (5). The next most common cause of acute pancreatitis is alcohol abuse. Accounting for roughly 30% of all AP, there are several hypotheses concerning the mechanism including an affect on the exocrine function of the pancreas, changes in lipid metabolism and oxidative stress
6 caused by heavy drinking (5). Another significant cause is hypertriglyceridemia, which accounts for 5% of AP, making it the third most common cause (5). AP patients may be found with blood triglyceride levels of 1,000 mg/dl, compared to the normal range of <150 mg/dl (5). Poorly controlled diabetic patients, alcoholics, and non-obese-non-alcoholic patients with drug-induced hypertriglyceridemia are at particular risk for developing AP (5). Other less common conditions that may cause AP include infections, vascular disease, trauma, post-ercp operations, postoperative and hereditary (5). Some of the causes in CP are similar to those of AP. In cases of CP, however, alcohol abuse is the greatest contributor, and accounts for 70% of all CP cases (6). However, pancreatitis is a condition that only affects 3-15% of the heavy drinking population (those who consume more than 14 grams of alcohol daily), so it appears that co-factors in conjunction with heavy drinking are also of significance (6). These co-factors may include genetic mutations, high dietary intake of fat and protein, the type of alcohol consumed, decreased antioxidant and trace elements and smoking (6). Smoking in particular has been found to be a significant co-factor, as 90% of patients with CP from alcohol abuse also smoke (6). The biggest recommendation for alcohol-induced CP patients is to cease drinking alcohol, which cannot stop or reverse damage done to the functioning pancreas, but it will slow the condition's progression (6). Tumors, scars, ductal stones and duodenal wall cysts are obstructions that can cause CP (6). Other causes are tobacco use, some tropical climates, genetic and autoimmune influences (6). Recurrent episodes of AP, regardless of the initial cause, can also eventually lead to CP (6). MEDICAL DIAGNOSIS The biggest symptom of pancreatitis is pain. Pain can reach is maximum intensity in 10-
7 20 minutes, and is steady and almost unbearable (5). Upper abdominal pain can radiate, belt-like, to the back (2). As the other symptoms of pancreatitis are similar to other GI disorders, such as nausea and vomiting, pain is often the biggest indicator of pancreatitis (5). The pain can be caused by increased pressure and ischemia in the pancreas or an increase innervation of the nociceptive nerves, stimulated by inflammation (6). Ecchymoses occurs in the flanks and is called Grey Turner's sign (5). Jaundice may occur if the bile duct is blocked (1). Hypotension, low urine output and dyspnea may also occur in more severe cases (2). The severe continuous pain, especially as seen with chronic pancreatitis, can cause a decrease in appetite, which can lead to weight loss and malnutrition over time (6). Complications like steatorrhea and diabetes, as mentioned above, are also symptoms of pancreatitis. The diagnosis for acute pancreatitis can be diagnosed by the symptoms, serum enzymes, or radiological imaging (5). Amylase and lipase levels are checked in the blood. The serum amylase test is quickly and easily performed, and is most specific to pancreatitis (7). When the acinar cells are damaged, excess amylase pours into the lymph and is picked up in the blood (7). Levels can rise up to two to three times more than the upper level of normal values within 12 hours of onset (7). Serum lipase is also a valuable diagnostic tool, as pancreatitis is the most common cause for elevated levels (7). Lipase can rise to five to ten times more than the normal values, and stays elevated longer (5-7 days) than amylase (7). There are several tests to determine the severity of pancreatitis. Ranson's criteria is the most commonly used tool, and it identifies 11 signs that can be measured in the first 48 hours of hospital admission to predict the severity and prognosis of the disease (krause). The Bedside Index for Severity in Acute Pancreatitis (BISAP) is a newer test that gives an early identification of at-risk patients and has been shown to be an accurate tool (8). The APACHE score, a
8 generalized scoring tool for many conditions, can also give a general sense of severity (8). Diagnosis for chronic pancreatitis is more difficult. There is a wide variety of tests, but no one test is better than the rest; different hospitals will run different tests as there is no gold standard (6). Long-term follow-up is often substituted for actual diagnostic tests (6). However, the existing tools that are used are separated into tests of functional or structural abnormalities. Direct tests examine pancreatic function based on direct hormonal stimulation (6). For example, the secretin stimulation test measures pancreatic secretions, particularly bicarbonate, in response to secretin, one of the pancreas' major stimulating hormones (2). A fecal fat test is an example of an indirect test, used to measure pancreatic function based on the total output of fecal fat per 24 hours in a 3-day stool collection (7). Structural abnormalities of the pancreas can be examined with ultrasounds or an endoscopic retrograde cholangiopancreatography (ERCP). An abdominal ultrasound can detect inflammation and abscess of the pancreas (pagana). Acute inflammation will be visualized as an enlarged edematous pancreas, whereas chronic inflammation will appear small and dense (7). An ERCP uses a fiberoptic endoscope to create radiographic visualizations of the bile and pancreatic ducts (7). It can also be used to incise the papillary muscle in the ampulla of Vater to remove gallstones (7). ERCP is a somewhat invasive tool, and is only used during surgical procedures, and not solely for an examination (6). MEDICAL TREATMENT The focus of pancreatitis treatment is often to relieve pain and focus on the patient's nutritional and metabolic needs (1). For AP patients, hydration and analgesia are important in relieving pain (5). In addition to managing pain, maintaining fluid balance can also dilute serum proteins and lower the hematocrit; in order to prevent necrosis, hematocrit should be below 45% (5). Respiratory and cardiovascular care should also be controlled, and blood levels of glucose,
9 insulin and electrolytes should be monitored carefully (5). To treat nausea and vomiting, AP patients should not consume anything orally for five to seven days (5). Antibiotics may be used for more severe cases where infection is present (5). Endoscopic interventions may also help increase the rate of recovery for severe AP (5). An urgent ERCP can help patients suffering from gallstones, and endoscopic stents placed early have shown to decrease pancreatic duct leakage and necrosis (5). Treatment for pancreatitis is also based on managing pain, although specific therapies should be used to treat individual conditions and complications, such as pseudocysts (6). Analgesics are also used to treat pain in CP, but most patients require more potent drugs (6). Although the risk of addiction is 10-30% if stronger analgesics, or even opoids in cases where analgesics are too weak, pain relief is the first priority (6). Cessation of alcohol and smoking reduces the permanently damaging effects of CP, although not completely, and also decreases pain (6). Some operational interventions may also be used to treat the pain and organ damage of CP. Endoscopic therapy, similar to its use with AP, can be used to improve pancreatic duct drainage, place stents and remove gallstones (6). Surgical therapy can be considered for patients with unbearable abdominal pain or complications of the surrounding organs (6). Surgery can also drain pancreatic ducts to relieve inflammation or take out portions of the pancreas and duodenum, or both, depending on the source of the pain and the ductal anatomy (6). The Whipple procedure is another procedure that can be performed to relieve pain and maintain CP. In this pancreaticduodenectomy, all or part of the pancreas and duodenum may be removed and the GI tract reattached (6). It is successful in its treatment of pain provides pain relief for 65-95% of patients but is also associated with high morbidity and mortality levels (6).
10 Complications arise in half of these patients. Because of this, some recently developed procedures are being tried, with substantial success, to not disrupt the GI as much as the Whipple procedure (6). MEDICAL NUTRITION THERAPY As some of the pain associated with the secretory mechanisms of the pancreas, following a diet that causes as little stimulation as possible can help manage the pain (2). Medical nutritional therapy also involves replacement of important nutrients lost through poor digestion and malabsorption (4). It was previously considered an acceptable treatment to keep patients NPO in order to stimulate the pancreas as little as possible, (4). However, that recommendation now only remains for milder cases of AP (4). The reason for this is that with the intense inflammatory response stimulated by pancreatitis, nutritional support also needs to address the metabolic needs, such as nitrogen balance, to overcome the inflammation (9). Therefore, the goal of nutritional support for pancreatitis is to provide for the metabolic needs without overstimulating the pancreas (9), and parenteral nutrition should only be maintained long enough to reduce nausea and vomiting (5). Early refeeding, even in severe cases of AP, can improve the outcome if serum lipase can be brought back down to levels no more than three times within the normal range (5). Furthermore, enteral nutrition reduces blood glucose, sepsis, further complications, and overall leads to a shorter hospital stay (5), especially if initiated within 48 hours of admission (4), and does not seem to affect mortality (9). Low-fat or clear liquid diets have appeared to be sufficient in reducing pancreatic stimulations (5), and even a full solid diet as the initial meal can reduce hospital stay for patients with mild AP (10). Some complementary and alternative medicines have been shown to be effective in nutrition intervention. Antioxidants have been shown to help reduce pain in CP patients (6).
11 Although they do not have a very significant effect, they do reduce oxidative stress, which is a strong activator of CP (6). It is also risk free, and therefore is used at times to at least provide some pain relief (6). Pancreatic enzyme therapy is another alternative treatment. It activates the feedback control to reduce enzyme activity, which in turn decreases pain (6). Enzymes should be administered to the small bowel to decrease CCK release (6). The Cochrane Library suggests that there is evidence that there may be some benefit to using pancreatic enzyme treatment, although more research should be conducted (11). Through the course of 10 trials, a significant reduction of fecal fat was observed, although both the specific enzyme and timing of administration had insignificant outcomes (11). Overall, the benefits of pancreatic enzymes are still debatable and require further research. In CP, the prolonged dysfunction of the pancreas can lead to malabsorption and malnutrition (4). Steatorrhea can be treated with enzymes and lipase supplements (6). However, this has several problems associated with it: lipase supplements are not potent, nor can they survive the gastric acid of the stomach well (6). Larger supplements made to counteract this often take too long and become active too far along the GI tract to do much good (6). The lack of success also leads to difficulty to get patients to comply faithfully with their prescription, but if one appropriately lipase supplementation does show improvement (6). Treatment of diabetes is also important, and it differs from interventions for type 1 or type 2 diabetics. CP patients with diabetes are mainly treated by monitoring urine glucose loss in place of tight control of blood glucose in order to prevent hypoglycemia, due to the fact that glucagon cannot be produced (6) Other nutritional therapy is similar to that of type 1 or 2, and
12 the same complications, such as neuropathy, retinopathy, nephropathy, should be monitored closely (6). CONCLUSION Despite good adherence to medical and nutritional interventions, complications may be unescapable, but most people with either chronic or acute pancreatitis can have a good prognosis if treatment and nutrition therapy is followed carefully (1).
13 REFERENCES 1. American Gastroenterological Association. Patient center: Understanding pancreatitis. Available at: Accessed March 9, Hasse JM, Matarese LE. Medical nutrition therapy for hepatobiliary and pancreatitc disorders. In: Mahan LK, Escott-Stump S, Raymond JL. Krause's Food, Nutrition, & Diet Therapy. 13 th ed. Philadelphia: Elsevier; 2012: Pandol, SJ. Pancreatic secretion. In: Feldman M, Friedman LS, Brandt LJ. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 9 th ed. Philadelphia: Saunders Elsevier; 2010: ADA Nutrition Care Manual. Pancreatitis. Available at _id= Accessed March 9, Tenner S, Steinberg WM. Acute pancreatitis. In: Feldman M, Friedman LS, Brandt LJ. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 9 th ed. Philadelphia: Saunders Elsevier; 2010: Forsmar CE. Chronic pancreatitis. In: Feldman M, Friedman LS, Brandt LJ. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 9 th ed. Philadelphia: Saunders Elsevier; 2010: Pagana KD, Pagana TJ. Mosby's Manual of Diagnostic and Laboratory Tests. 4 th ed. St Louis: Mosby Inc; Papachristou GI, Muddana V, Yadav D, et al. Compaison of BISAP, Ranson's APACHE-II and CTSI scores in predicting organ failure, complications, and mortality in acute pancreatitis. Am J Gastroenterol. 2010;105(2): Ioannidis O, Laverentieva A, Botsios D. Nutrition support in acute pancreatitis. JOP. 2008; 9(4): Moraes JM, Felga GE, Chebli LA, et al. A full solid diet as the initial meal in mild acute pancreatitis is safe and result in a shorter length of hospitalization: Results from a prospective, randomized, controlled, double-blind clinical trial. J Clin Gastroenterol. 2010; 44(7): Shafiq N, Rana S, Bhasin D, et al. Pancreatic enzymes for chronic pancreatitis. Chocrane Database of Systematic Reviews. 2009; 4:CD Perwaiz A, Singh A, Chaudhary A. Surgery for Chronic Pancreatitis. Indian J Surg. 2012; 74(1):47-54.
Pancreatitis. Acute Pancreatitis
 Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
What Is Pancreatitis?
 What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
Diagnosis of chronic Pancreatitis. Christoph Beglinger, University Hospital Basel, Switzerland
 Diagnosis of chronic Pancreatitis Christoph Beglinger, University Hospital Basel, Switzerland Pancreatitis Pancreas Pancreas - an organ that makes bicarbonate to neutralize gastric acid, enzymes to digest
Diagnosis of chronic Pancreatitis Christoph Beglinger, University Hospital Basel, Switzerland Pancreatitis Pancreas Pancreas - an organ that makes bicarbonate to neutralize gastric acid, enzymes to digest
Week 3 The Pancreas: Pancreatic ph buffering:
 Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Case Study BMIs in the range of are considered overweight. Therefore, F.V. s usual BMI indicates that she was overweight.
 Morgan McFarlane February 26 th, 2013 HHP 439 Professor White Case Study 7.10 1. What is your interpretation of F.V. s clinical data? F.V. s clinical data includes chronic abdominal pain, loose stools,
Morgan McFarlane February 26 th, 2013 HHP 439 Professor White Case Study 7.10 1. What is your interpretation of F.V. s clinical data? F.V. s clinical data includes chronic abdominal pain, loose stools,
Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4)
 Vert Phys PCB3743 Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4) T. Houpt, Ph.D. Anatomy of Digestive System Peristalsis Stomach and Acid Secretion Liver and Bile Secretion Pancreas and pancreatic
Vert Phys PCB3743 Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4) T. Houpt, Ph.D. Anatomy of Digestive System Peristalsis Stomach and Acid Secretion Liver and Bile Secretion Pancreas and pancreatic
Diseases of pancreas - Chronic pancreatitis
 Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
1-It is to prevent back flow of fecal content from colon into small intestine.
 Function of the ileocecal valve: 1-It is to prevent back flow of fecal content from colon into small intestine. 2-The wall of the ileum for several centimeters preceding valve has a thickened muscular
Function of the ileocecal valve: 1-It is to prevent back flow of fecal content from colon into small intestine. 2-The wall of the ileum for several centimeters preceding valve has a thickened muscular
Causes of pancreatic insufficiency. Eugen Dumitru
 Causes of pancreatic insufficiency Eugen Dumitru Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes 3. The Consequences Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes
Causes of pancreatic insufficiency Eugen Dumitru Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes 3. The Consequences Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes
DIGESTIVE. CHAPTER 17 Lecture: Part 1 Part 2 BIO 212: ANATOMY & PHYSIOLOGY II
 BIO 212: ANATOMY & PHYSIOLOGY II CHAPTER 17 Lecture: DIGESTIVE Part 1 Part 2 Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. SMALL INTESTINE DUODENUM > JEJUNUM
BIO 212: ANATOMY & PHYSIOLOGY II CHAPTER 17 Lecture: DIGESTIVE Part 1 Part 2 Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. SMALL INTESTINE DUODENUM > JEJUNUM
Nutrition in Pancreatic Disease Topic 14
 Nutrition in Pancreatic Disease Topic 14 Module 14.2 Chronic Pancreatitis Learning objectives Johann Ockenga, MD, Prof. Dep. of Gastroenterology, Endocrinology & Nutrition, Klinikum Bremen Mitte, St. Juergensstrasse
Nutrition in Pancreatic Disease Topic 14 Module 14.2 Chronic Pancreatitis Learning objectives Johann Ockenga, MD, Prof. Dep. of Gastroenterology, Endocrinology & Nutrition, Klinikum Bremen Mitte, St. Juergensstrasse
Prof. (DR.) MD. ISMAIL PATWARY. MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet
 Prof. (DR.) MD. ISMAIL PATWARY MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet CHRONIC PANCREATITIS Defined as a progressive inflammatory
Prof. (DR.) MD. ISMAIL PATWARY MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet CHRONIC PANCREATITIS Defined as a progressive inflammatory
Why would fatty foods aggravate the patient s RUQ pain? What effect does cholecystokinin (CCK) have on gastric emptying?
 CASE 28 A 43-year-old woman presents to the emergency department with the acute onset of abdominal pain. Her pain is located to the right upper quadrant (RUQ) and radiates to the right shoulder. She reports
CASE 28 A 43-year-old woman presents to the emergency department with the acute onset of abdominal pain. Her pain is located to the right upper quadrant (RUQ) and radiates to the right shoulder. She reports
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
Chronic Pancreatitis (1 of 4) i
 Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
ESPEN Congress The Hague 2017
 ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
Physiology 12. Overview. The Gastrointestinal Tract. Germann Ch 19
 Physiology 12 The Gastrointestinal Tract Germann Ch 19 Overview 1 Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
Physiology 12 The Gastrointestinal Tract Germann Ch 19 Overview 1 Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
Chapter 15 Gastrointestinal System
 Chapter 15 Gastrointestinal System Dr. LL Wang E-mail: wanglinlin@zju.edu.cn Rm 608, Block B, Research Building, School of Medicine, Zijingang Campus Pancreatic Secretion The exocrine cells in the pancreas
Chapter 15 Gastrointestinal System Dr. LL Wang E-mail: wanglinlin@zju.edu.cn Rm 608, Block B, Research Building, School of Medicine, Zijingang Campus Pancreatic Secretion The exocrine cells in the pancreas
Pathophysiology ACUTE PANCREATITIS
 Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
Preview of the Medifocus Guidebook on: Chronic Pancreatitis Updated July 4, 2018
 Preview of the Medifocus Guidebook on: Chronic Pancreatitis Updated July 4, 2018 This document is only a SHORT PREVIEW of the Medifocus Guidebook on Chronic Pancreatitis. It is intended primarily to give
Preview of the Medifocus Guidebook on: Chronic Pancreatitis Updated July 4, 2018 This document is only a SHORT PREVIEW of the Medifocus Guidebook on Chronic Pancreatitis. It is intended primarily to give
16 April 2010 Resident Teaching Conference. Pancreatitis. W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D.
 16 April 2010 Resident Teaching Conference Pancreatitis W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D. Santorini Wirsung anatomy.med.umich.edu/.../ duodenum_ans.html Bud and ductology Ventral pancreatic
16 April 2010 Resident Teaching Conference Pancreatitis W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D. Santorini Wirsung anatomy.med.umich.edu/.../ duodenum_ans.html Bud and ductology Ventral pancreatic
Sphincters heartburn diaphragm The Stomach gastric glands pepsin, chyme The Small Intestine 1-Digestion Is Completed in the Small Intestine duodenum
 Sphincters are muscles that encircle tubes and act as valves. The tubes close when the sphincters contract and they open when the sphincters relax. When food or saliva is swallowed, the sphincter relaxes
Sphincters are muscles that encircle tubes and act as valves. The tubes close when the sphincters contract and they open when the sphincters relax. When food or saliva is swallowed, the sphincter relaxes
PHYSIOLOGY OF THE DIGESTIVE SYSTEM
 Student Name CHAPTER 26 PHYSIOLOGY OF THE DIGESTIVE SYSTEM D igestion is the process of breaking down complex nutrients into simpler units suitable for absorption. It involves two major processes: mechanical
Student Name CHAPTER 26 PHYSIOLOGY OF THE DIGESTIVE SYSTEM D igestion is the process of breaking down complex nutrients into simpler units suitable for absorption. It involves two major processes: mechanical
Chronic Pancreatitis. Ara Sahakian, M.D. Assistant Professor of Medicine USC core lecture
 Chronic Pancreatitis Ara Sahakian, M.D. Assistant Professor of Medicine USC core lecture What is Chronic Pancreatitis Progressive inflammatory disease Pancreatic parenchyma replaced w/fibrous tissue Destruction
Chronic Pancreatitis Ara Sahakian, M.D. Assistant Professor of Medicine USC core lecture What is Chronic Pancreatitis Progressive inflammatory disease Pancreatic parenchyma replaced w/fibrous tissue Destruction
Overview. Physiology 1. The Gastrointestinal Tract. Guyton section XI
 Overview Physiology 1 The Gastrointestinal Tract Guyton section XI Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
Overview Physiology 1 The Gastrointestinal Tract Guyton section XI Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
The Digestive System. What is the advantage of a one-way gut? If you swallow something, is it really inside you?
 The Digestive System What is the advantage of a one-way gut?! If you swallow something, is it really inside you? Functions and Processes of the Digestive System: Move nutrients, water, electrolytes from
The Digestive System What is the advantage of a one-way gut?! If you swallow something, is it really inside you? Functions and Processes of the Digestive System: Move nutrients, water, electrolytes from
The Small Intestine. The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine.
 The Small Intestine The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine. approximately six metres (the longest section of your digestive
The Small Intestine The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine. approximately six metres (the longest section of your digestive
Physiology Unit 4 DIGESTIVE PHYSIOLOGY
 Physiology Unit 4 DIGESTIVE PHYSIOLOGY In Physiology Today Functions Motility Ingestion Mastication Deglutition Peristalsis Secretion 7 liters/day! Exocrine/endocrine Digestion Absorption Digestion of
Physiology Unit 4 DIGESTIVE PHYSIOLOGY In Physiology Today Functions Motility Ingestion Mastication Deglutition Peristalsis Secretion 7 liters/day! Exocrine/endocrine Digestion Absorption Digestion of
Identification of Serum mirnas as prospective Bio-markers for acute and chronic pancreatitis Dr. Jeyaparvathi Somasundaram
 Identification of Serum mirnas as prospective Bio-markers for acute and chronic pancreatitis Dr. Jeyaparvathi Somasundaram Assistant Professor, Department of Biotechnoloy, Lady Doak College, Madurai. Acute
Identification of Serum mirnas as prospective Bio-markers for acute and chronic pancreatitis Dr. Jeyaparvathi Somasundaram Assistant Professor, Department of Biotechnoloy, Lady Doak College, Madurai. Acute
University of Buea. Faculty of Health Sciences. Programme in Medicine
 Faculty of Health Sciences University of Buea Wednesday, 28 th January 2009 Time: 8 00-10 00 Programme in Medicine MED 303 (Gastrointestinal Physiology) EXAMS (2008-2009) Identify the letter of the choice
Faculty of Health Sciences University of Buea Wednesday, 28 th January 2009 Time: 8 00-10 00 Programme in Medicine MED 303 (Gastrointestinal Physiology) EXAMS (2008-2009) Identify the letter of the choice
Pancreatic Benign April 27, 2016
 Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland
 pancreas Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland Acute pancreatitis Inflammation of the pancreas associated with acinar cell injury Clinical features: 1-abdominal pain cardinal
pancreas Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland Acute pancreatitis Inflammation of the pancreas associated with acinar cell injury Clinical features: 1-abdominal pain cardinal
Control of Glucose Metabolism
 Glucose Metabolism Control of Glucose Metabolism The pancreas is both an exocrine and endocrine gland. It secretes digestive enzymes into the duodenum (exocrine) and 3 specific hormones into the bloodstream
Glucose Metabolism Control of Glucose Metabolism The pancreas is both an exocrine and endocrine gland. It secretes digestive enzymes into the duodenum (exocrine) and 3 specific hormones into the bloodstream
Digestive System Module 6: Accessory Organs in Digestion: The Liver, Pancreas, and Gallbladder
 Connexions module: m49293 1 Digestive System Module 6: Accessory Organs in Digestion: The Liver, Pancreas, and Gallbladder Donna Browne Based on Accessory Organs in Digestion: The Liver, Pancreas, and
Connexions module: m49293 1 Digestive System Module 6: Accessory Organs in Digestion: The Liver, Pancreas, and Gallbladder Donna Browne Based on Accessory Organs in Digestion: The Liver, Pancreas, and
Bio& 242 Unit 1 / Lecture 4
 Bio& 242 Unit 1 / Lecture 4 system: Gastric hormones GASTRIN: Secretion: By enteroendocrine (G) in gastric pits of the mucosa. Stimulus: Stomach distention and acid ph of chyme causes Gastrin. Action:
Bio& 242 Unit 1 / Lecture 4 system: Gastric hormones GASTRIN: Secretion: By enteroendocrine (G) in gastric pits of the mucosa. Stimulus: Stomach distention and acid ph of chyme causes Gastrin. Action:
18. PANCREATIC FUNCTION AND METABOLISM. Pancreatic secretions ISLETS OF LANGERHANS. Insulin
 18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
NOTES: The Digestive System (Ch 14, part 2)
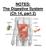 NOTES: The Digestive System (Ch 14, part 2) PANCREAS Structure of the pancreas: The pancreas produces PANCREATIC JUICE that is then secreted into a pancreatic duct. The PANCREATIC DUCT leads to the The
NOTES: The Digestive System (Ch 14, part 2) PANCREAS Structure of the pancreas: The pancreas produces PANCREATIC JUICE that is then secreted into a pancreatic duct. The PANCREATIC DUCT leads to the The
Focus on Cystic Fibrosis. Cystic Fibrosis. Cystic Fibrosis
 Focus on (Relates to Chapter 29, Nursing Management: Obstructive Pulmonary Diseases, in the textbook) Copyright 2011, 2007 by Mosby, Inc., an affiliate of Elsevier Inc. Autosomal recessive, multisystem
Focus on (Relates to Chapter 29, Nursing Management: Obstructive Pulmonary Diseases, in the textbook) Copyright 2011, 2007 by Mosby, Inc., an affiliate of Elsevier Inc. Autosomal recessive, multisystem
Anatomy of the biliary tract
 Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
- Digestion occurs during periods of low activity - Produces more energy than it uses. - Mucosa
 Introduction Digestive System Chapter 29 Provides processes to break down molecules into a state easily used by cells - A disassembly line: Starts at the mouth and ends at the anus Digestive functions
Introduction Digestive System Chapter 29 Provides processes to break down molecules into a state easily used by cells - A disassembly line: Starts at the mouth and ends at the anus Digestive functions
The Endocrine Pancreas (Chapter 10) *
 OpenStax-CNX module: m62118 1 The Endocrine Pancreas (Chapter 10) * Ildar Yakhin Based on The Endocrine Pancreas by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons
OpenStax-CNX module: m62118 1 The Endocrine Pancreas (Chapter 10) * Ildar Yakhin Based on The Endocrine Pancreas by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons
This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated.
 A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Overview of Gastroenterology
 Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Overview of Gastroenterology Gastroenterology Made Really Simple! Food Waste
Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Overview of Gastroenterology Gastroenterology Made Really Simple! Food Waste
Chapter 26 The Digestive System
 Chapter 26 The Digestive System Digestive System Gastroenterology is the study of the stomach and intestine. Digestion Catabolism Absorption Anabolism The actions of the digestive system are controlled
Chapter 26 The Digestive System Digestive System Gastroenterology is the study of the stomach and intestine. Digestion Catabolism Absorption Anabolism The actions of the digestive system are controlled
Chronic Pancreatitis
 Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
LAPAROSCOPIC GALLBLADDER SURGERY
 LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
Diseases of exocrine pancreas
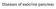 Diseases of exocrine pancreas The exocrine pancreas constitutes 80% to 85% of the organ and is composed of acinar cells that secrete enzymes needed for digestion. the accessory duct of Santorini, the main
Diseases of exocrine pancreas The exocrine pancreas constitutes 80% to 85% of the organ and is composed of acinar cells that secrete enzymes needed for digestion. the accessory duct of Santorini, the main
e. Undigested material is compacted and stored until the colon is full. When the colon is full, a signal to empty it is sent by sensors in the walls
 Digestive System 1. General a. Animals obtain energy by breaking food molecules into smaller pieces. b. The basic fuel molecules are amino acids, lipids and sugars c. Digestion is the chemical breakdown
Digestive System 1. General a. Animals obtain energy by breaking food molecules into smaller pieces. b. The basic fuel molecules are amino acids, lipids and sugars c. Digestion is the chemical breakdown
Learning Targets. The Gastrointestinal (GI) Tract. Also known as the alimentary canal. Hollow series of organs that food passes through
 Digestion the multistep process of breaking down food into molecules the body can use Learning Targets Describe the path food takes through the digestive system. Identify the major organs of the digestive
Digestion the multistep process of breaking down food into molecules the body can use Learning Targets Describe the path food takes through the digestive system. Identify the major organs of the digestive
What Are Gallstones? GALLSTONES. Gallstones are pieces of hard, solid matter that form over time in. the gallbladder of some people.
 What Are Gallstones? Gallstones are pieces of hard, solid matter that form over time in the gallbladder of some people. The gallbladder sits under the liver and stores bile (a key digestive juice ). Gallstones
What Are Gallstones? Gallstones are pieces of hard, solid matter that form over time in the gallbladder of some people. The gallbladder sits under the liver and stores bile (a key digestive juice ). Gallstones
Exocrine functions: secretion of digestive enzymes (eg. lipase, amylase,
 Chapter 91 Pancreas Episode Overview: 1. List 10 differential diagnoses for acute pancreatitis 2. List 10 causes of pancreatitis. Which are most common in adults? Which one is most common in pediatrics?
Chapter 91 Pancreas Episode Overview: 1. List 10 differential diagnoses for acute pancreatitis 2. List 10 causes of pancreatitis. Which are most common in adults? Which one is most common in pediatrics?
Gastrointestinal Anatomy and Physiology. Bio 219 Napa Valley College Dr. Adam Ross
 Gastrointestinal Anatomy and Physiology Bio 219 Napa Valley College Dr. Adam Ross Functions of digestive system Digestion Breakdown of food (chemically) using enzymes, acid, and water Absorption Nutrients,
Gastrointestinal Anatomy and Physiology Bio 219 Napa Valley College Dr. Adam Ross Functions of digestive system Digestion Breakdown of food (chemically) using enzymes, acid, and water Absorption Nutrients,
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 13 THE DIGESTIVE SYSTEM
 ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 13 THE DIGESTIVE SYSTEM The digestive system also known as the alimentary canal or gastrointestinal tract consists of a series of hollow organs joined in a
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 13 THE DIGESTIVE SYSTEM The digestive system also known as the alimentary canal or gastrointestinal tract consists of a series of hollow organs joined in a
Pancreatitis. By: Casey Allred, Kerri Bell, Chelsey Evans, Jillayne Gee and Bonnie Ross. March 8, 2010 NDFS 356
 Pancreatitis By: Casey Allred, Kerri Bell, Chelsey Evans, Jillayne Gee and Bonnie Ross March 8, 2010 NDFS 356 1 INTRODUCTION Pancreatitis is a condition that requires special medical and nutritional attention.
Pancreatitis By: Casey Allred, Kerri Bell, Chelsey Evans, Jillayne Gee and Bonnie Ross March 8, 2010 NDFS 356 1 INTRODUCTION Pancreatitis is a condition that requires special medical and nutritional attention.
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
Chapter 14: The Digestive System
 Chapter 14: The Digestive System Digestive system consists of Muscular tube (digestive tract) alimentary canal Accessory organs teeth, tongue, glandular organs 6 essential activities 1. 2. 3. 4. 5. 6.
Chapter 14: The Digestive System Digestive system consists of Muscular tube (digestive tract) alimentary canal Accessory organs teeth, tongue, glandular organs 6 essential activities 1. 2. 3. 4. 5. 6.
Emergency Surgery Course Graz, March ACUTE PANCREATITIS. Carlos Mesquita Coimbra
 ACUTE PANCREATITIS Carlos Mesquita Coimbra ESSENTIALS (1) AP occurs when digestive enzymes become activated while still in the pancreas, causing inflammation repeated bouts of AP can lead to chronic pancreatitis
ACUTE PANCREATITIS Carlos Mesquita Coimbra ESSENTIALS (1) AP occurs when digestive enzymes become activated while still in the pancreas, causing inflammation repeated bouts of AP can lead to chronic pancreatitis
ACG Clinical Guideline: Management of Acute Pancreatitis
 ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
Chapter 20 The Digestive System Exam Study Questions
 Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
The incidence of pancreatic cancer is rising in India and is higher in the urban male population in the western and northern parts of India.
 Published on: 9 Jun 2015 Pancreatic Cancer What Is Cancer? The body is made up of cells, which grow and die in a controlled way. Sometimes, cells keep on growing without control, causing an abnormal growth
Published on: 9 Jun 2015 Pancreatic Cancer What Is Cancer? The body is made up of cells, which grow and die in a controlled way. Sometimes, cells keep on growing without control, causing an abnormal growth
- Digestion occurs during periods of low activity - Produces more energy than it uses. 3 Copyright 2016 by Elsevier Inc. All rights reserved.
 Introduction Digestive System Chapter 29 Provides processes to break down molecules into a state easily used by cells - A disassembly line: Starts at the mouth and ends at the anus Digestive functions
Introduction Digestive System Chapter 29 Provides processes to break down molecules into a state easily used by cells - A disassembly line: Starts at the mouth and ends at the anus Digestive functions
LOKUN! I got stomach ache!
 LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
Chapter 20 The Digestive System Exam Study Questions
 Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Energy, Chemical Reactions and Enzymes
 Phosphorylation Hydrolysis Energy, Chemical Reactions and Enzymes Chapter 2 (selections) What is Energy? Energy is the capacity to do work Potential Energy Kinetic Energy Chemical Bond Energy Like a rechargeable
Phosphorylation Hydrolysis Energy, Chemical Reactions and Enzymes Chapter 2 (selections) What is Energy? Energy is the capacity to do work Potential Energy Kinetic Energy Chemical Bond Energy Like a rechargeable
Assessment and Management of Patients With Biliary Disorders
 Assessment and Management of Patients With Biliary Disorders Anatomic and Physiologic Overview a pear-shaped, hollow, saclike organ, 7.5 to 10 cm long, lies in a shallow depression on the inferior surface
Assessment and Management of Patients With Biliary Disorders Anatomic and Physiologic Overview a pear-shaped, hollow, saclike organ, 7.5 to 10 cm long, lies in a shallow depression on the inferior surface
Understandings, Applications & Skills
 D.2 Digestion Understandings, Applications & Skills Statement D.2.U1 Nervous and hormonal mechanisms control the secretion of digestive juices. D.2.U2 Exocrine glands secrete to the surface of the body
D.2 Digestion Understandings, Applications & Skills Statement D.2.U1 Nervous and hormonal mechanisms control the secretion of digestive juices. D.2.U2 Exocrine glands secrete to the surface of the body
Bile composition. Pathophysiology of Gallstone Formation and Pancreatitis. Bile
 Bile composition Pathophysiology of Gallstone Formation and Pancreatitis Robert F. Schwabe rfs2102@columbia.edu Phospholipids Miscellaneous (Pigment, Protein) (Lecithin) Bile Salts 0.7% 4% H 2 0 1% 12%
Bile composition Pathophysiology of Gallstone Formation and Pancreatitis Robert F. Schwabe rfs2102@columbia.edu Phospholipids Miscellaneous (Pigment, Protein) (Lecithin) Bile Salts 0.7% 4% H 2 0 1% 12%
Ali Yaghi. Yaseen Fatayer. M.Khatatbeh
 6 Ali Yaghi Yaseen Fatayer M.Khatatbeh P a g e 1 pancreatic secretions note: The pancreas has endocrine (secretions are released toward the blood) and exocrine(secretions are released through the canalicular
6 Ali Yaghi Yaseen Fatayer M.Khatatbeh P a g e 1 pancreatic secretions note: The pancreas has endocrine (secretions are released toward the blood) and exocrine(secretions are released through the canalicular
PATHOLOGY MCQs. The Pancreas
 PATHOLOGY MCQs The Pancreas A patient with cystic fibrosis is characteristically: A. more than 45 years of age B. subject to recurring pulmonary infections C. obese D. subject to spontaneous fractures
PATHOLOGY MCQs The Pancreas A patient with cystic fibrosis is characteristically: A. more than 45 years of age B. subject to recurring pulmonary infections C. obese D. subject to spontaneous fractures
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Severe necrotizing pancreatitis. ICU Fellowship Training Radboudumc
 Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Evaluation of Suspected Pancreatic Cancer
 Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM TYPES OF DIGESTIVE SYSTEMS Ingested food may be stored or first subjected to physical fragmentation Chemical digestion occurs next Hydrolysis reactions liberate the subunit molecules
THE DIGESTIVE SYSTEM TYPES OF DIGESTIVE SYSTEMS Ingested food may be stored or first subjected to physical fragmentation Chemical digestion occurs next Hydrolysis reactions liberate the subunit molecules
CLASSIFICATION OF CHRONIC PANCREATITIS
 CLASSIFICATION OF CHRONIC PANCREATITIS EAGE, Podstgraduate Course, Prague, April 2010. Tomica Milosavljević School of Medicine, University of Belgrade Clinical Center of Serbia,Belgrade The phrase chronic
CLASSIFICATION OF CHRONIC PANCREATITIS EAGE, Podstgraduate Course, Prague, April 2010. Tomica Milosavljević School of Medicine, University of Belgrade Clinical Center of Serbia,Belgrade The phrase chronic
Pancreatic Lesions. Valerie Jefford Pediatric Surgery Rounds June 6, 2003
 Pancreatic Lesions Valerie Jefford Pediatric Surgery Rounds June 6, 2003 Embryology 4 th week 2 buds of endodermal origin from caudal foregut Dorsal and ventral bud Ventral migrates dorsally with CBD (below/behind
Pancreatic Lesions Valerie Jefford Pediatric Surgery Rounds June 6, 2003 Embryology 4 th week 2 buds of endodermal origin from caudal foregut Dorsal and ventral bud Ventral migrates dorsally with CBD (below/behind
Biology 12 - Digestion Notes
 Biology 12 - Digestion Notes Anatomy Physiology Functions of the Digestive System -------------------------------------------------------------------------------------- food (enzymes, bile, HCl) to assist
Biology 12 - Digestion Notes Anatomy Physiology Functions of the Digestive System -------------------------------------------------------------------------------------- food (enzymes, bile, HCl) to assist
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine
 Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
Includes mouth, pharynx, esophagus, stomach, small intestine, large intestine, rectum, anus. Salivary glands, liver, gallbladder, pancreas
 Chapter 14 The Digestive System and Nutrition Digestive System Brings Nutrients Into the Body The digestive system includes Gastrointestinal (GI) tract (hollow tube) Lumen: space within this tube Includes
Chapter 14 The Digestive System and Nutrition Digestive System Brings Nutrients Into the Body The digestive system includes Gastrointestinal (GI) tract (hollow tube) Lumen: space within this tube Includes
X-Plain Pancreatic Cancer Reference Summary
 X-Plain Pancreatic Cancer Reference Summary Introduction Pancreatic cancer is the 4th leading cause of cancer deaths in the U.S. About 37,000 new cases of pancreatic cancer are diagnosed each year in the
X-Plain Pancreatic Cancer Reference Summary Introduction Pancreatic cancer is the 4th leading cause of cancer deaths in the U.S. About 37,000 new cases of pancreatic cancer are diagnosed each year in the
Extrahepatic Bile Duct Ostruction (Blockage of the Extrahepatic or Common Bile Duct) Basics
 Extrahepatic Bile Duct Ostruction (Blockage of the Extrahepatic or Common Bile Duct) Basics OVERVIEW The liver is the largest gland in the body; it has many functions, including production of bile (a fluid
Extrahepatic Bile Duct Ostruction (Blockage of the Extrahepatic or Common Bile Duct) Basics OVERVIEW The liver is the largest gland in the body; it has many functions, including production of bile (a fluid
My dog or cat has pancreas problems what do I do now?
 TROVET Digestion Support, dietary supplement for the targeted tackling of pancreas problems in dogs and cats My dog or cat has pancreas problems what do I do now? reliable and affordable dietary pet food
TROVET Digestion Support, dietary supplement for the targeted tackling of pancreas problems in dogs and cats My dog or cat has pancreas problems what do I do now? reliable and affordable dietary pet food
MCT AND THE ROLES NUTRITION
 MCT AND THE ROLES NUTRITION Nguyen Hoang Nhut Hoa Department of Nutrition Children's Hospital 2 OBJECTIVES Structure Absorption and metabolic Effects of MCT in the treatment of certain diseases Demand
MCT AND THE ROLES NUTRITION Nguyen Hoang Nhut Hoa Department of Nutrition Children's Hospital 2 OBJECTIVES Structure Absorption and metabolic Effects of MCT in the treatment of certain diseases Demand
Paneth Cells. Road Map to the Finish. No Review this Friday. Today 11/29 Finish digestion/accessory organs. Wednesday 12/1 Immune System I
 Road Map to the Finish No Review this Friday Today 11/29 Finish digestion/accessory organs Wednesday 12/1 Immune System I Paneth Cells - base of intestinal glands -! large -! intense acidophilic granules
Road Map to the Finish No Review this Friday Today 11/29 Finish digestion/accessory organs Wednesday 12/1 Immune System I Paneth Cells - base of intestinal glands -! large -! intense acidophilic granules
Digestive Care Advisor Training #1. Digestion 101 & H.O.P.E.
 Digestive Care Advisor Training #1 & H.O.P.E. The Digestive System in Brief The Process of Digestion The human digestive system is a complex series of organs and glands that process food and excrete waste.
Digestive Care Advisor Training #1 & H.O.P.E. The Digestive System in Brief The Process of Digestion The human digestive system is a complex series of organs and glands that process food and excrete waste.
Acute Pancreatitis. What is the Pancreas? What does it do? What is acute pancreatitis? What causes acute pancreatitis? What symptoms do you get?
 In association with: Primary Care Society for Gastroenterology INFORMATION ABOUT Acute Pancreatitis www.corecharity.org.uk What is the Pancreas? What does it do? What is acute pancreatitis? What causes
In association with: Primary Care Society for Gastroenterology INFORMATION ABOUT Acute Pancreatitis www.corecharity.org.uk What is the Pancreas? What does it do? What is acute pancreatitis? What causes
For family, friends and caregivers of a patient with pancreatitis in the Medical Surgical Intensive Care Unit (MSICU)
 Form: D-8705 Pancreatitis For family, friends and caregivers of a patient with pancreatitis in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information about: The causes
Form: D-8705 Pancreatitis For family, friends and caregivers of a patient with pancreatitis in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information about: The causes
Chronic Pancreatitis
 Supportive module 2: Basics of diagnosis, treatment and prevention of major gastroenterological diseases Chronic Pancreatitis LECTURE IN INTERNAL MEDICINE FOR IV COURSE STUDENTS M. Yabluchansky, L. Bogun,
Supportive module 2: Basics of diagnosis, treatment and prevention of major gastroenterological diseases Chronic Pancreatitis LECTURE IN INTERNAL MEDICINE FOR IV COURSE STUDENTS M. Yabluchansky, L. Bogun,
What location in the gastrointestinal (GI) tract has tight, or impermeable, junctions between the epithelial cells?
 CASE 32 A 17-year-old boy presents to his primary care physician with complaints of diarrhea for the last 2 days. The patient states that he just returned to the United States after visiting relatives
CASE 32 A 17-year-old boy presents to his primary care physician with complaints of diarrhea for the last 2 days. The patient states that he just returned to the United States after visiting relatives
UPPER GI DISEASES 11/15/2014. Lesson Objectives. GI Tract Review. NUTR 2050 Nutrition for Nursing Professionals. Mrs. Deborah A. Hutcheon, MS, RD, LD
 UPPER GI DISEASES NUTR 2050 Nutrition for Nursing Professionals Mrs. Deborah A. Hutcheon, MS, RD, LD Lesson Objectives At the end of the lesson, the student will be able to: 1. Describe causes and contributing
UPPER GI DISEASES NUTR 2050 Nutrition for Nursing Professionals Mrs. Deborah A. Hutcheon, MS, RD, LD Lesson Objectives At the end of the lesson, the student will be able to: 1. Describe causes and contributing
Acute pancreatitis. Information for patients Hepatobiliary
 Acute pancreatitis Information for patients Hepatobiliary What is acute pancreatitis? Acute pancreatitis is an inflammation of the pancreas gland. The main symptoms are: severe abdominal pain severe back
Acute pancreatitis Information for patients Hepatobiliary What is acute pancreatitis? Acute pancreatitis is an inflammation of the pancreas gland. The main symptoms are: severe abdominal pain severe back
Gastrointestinal Physiology. Secretion
 Gastrointestinal Physiology Secretion Fig. 24.26 Functions Provided by secretory glands which serve 2 functions: - Digestive enzymes. - Lubrication and protection of the mucosa. Types of secretory structures
Gastrointestinal Physiology Secretion Fig. 24.26 Functions Provided by secretory glands which serve 2 functions: - Digestive enzymes. - Lubrication and protection of the mucosa. Types of secretory structures
DIGESTIVE SYSTEM II ACCESSORY DIGESTIVE ORGANS
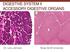 DIGESTIVE SYSTEM II ACCESSORY DIGESTIVE ORGANS Dr. Larry Johnson Texas A& M University Objectives Distinguish between the parotid and submandibular salivary glands. Understand and identify the structural
DIGESTIVE SYSTEM II ACCESSORY DIGESTIVE ORGANS Dr. Larry Johnson Texas A& M University Objectives Distinguish between the parotid and submandibular salivary glands. Understand and identify the structural
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, ,
 IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
The process by which nutrient molecules pass through the wall of your digestive system into your blood. ABSORPTION AS RELATED TO DIGESTION
 ABSORPTION AS RELATED TO DIGESTION The process by which nutrient molecules pass through the wall of your digestive system into your blood. 3 FUNCTIONS OF DIGESTION Breaks down food into molecules the body
ABSORPTION AS RELATED TO DIGESTION The process by which nutrient molecules pass through the wall of your digestive system into your blood. 3 FUNCTIONS OF DIGESTION Breaks down food into molecules the body
Malabsorption: etiology, pathogenesis and evaluation
 Malabsorption: etiology, pathogenesis and evaluation Peter HR Green NORMAL ABSORPTION Coordination of gastric, small intestinal, pancreatic and biliary function Multiple mechanisms Fat protein carbohydrate
Malabsorption: etiology, pathogenesis and evaluation Peter HR Green NORMAL ABSORPTION Coordination of gastric, small intestinal, pancreatic and biliary function Multiple mechanisms Fat protein carbohydrate
