A mathematical model of the effects of multiple myeloma on renal function
|
|
|
- Lorin Parrish
- 5 years ago
- Views:
Transcription
1 University of Iowa Iowa Research Online Theses and Dissertations Summer 2016 A mathematical model of the effects of multiple myeloma on renal function Julia Catherine Walk University of Iowa Copyright 2016 Julia Catherine Walk This dissertation is available at Iowa Research Online: Recommended Citation Walk, Julia Catherine. "A mathematical model of the effects of multiple myeloma on renal function." PhD (Doctor of Philosophy) thesis, University of Iowa, Follow this and additional works at: Part of the Applied Mathematics Commons
2 A MATHEMATICAL MODEL OF THE EFFECTS OF MULTIPLE MYELOMA ON RENAL FUNCTION by Julia Catherine Walk A thesis submitted in partial fulfillment of the requirements for the Doctor of Philosophy degree in Applied Mathematical and Computational Sciences in the Graduate College of The University of Iowa August 2016 Thesis Supervisor: Associate Professor Bruce Ayati
3 Copyright by JULIA CATHERINE WALK 2016 All Rights Reserved
4 Graduate College The University of Iowa Iowa City, Iowa CERTIFICATE OF APPROVAL PH.D. THESIS This is to certify that the Ph.D. thesis of Julia Catherine Walk has been approved by the Examining Committee for the thesis requirement for the Doctor of Philosophy degree in Applied Mathematical and Computational Sciences at the August 2016 graduation. Thesis committee: Bruce Ayati, Thesis Supervisor Victor Camillo Colleen Mitchell Gerhard Strohmer Keith Stroyan
5 ACKNOWLEDGEMENTS I have been fortunate to have a wonderful support system throughout graduate school, and I would like to thank a small number of the people who made up that group. First, a special thank you to Mom, Dad, Emily, Brett, and Jacob for your unconditional love and constant belief in me. To Katie, Lisa, Emiley, and Adrienne, thank you for standing by my side throughout these years, as you have throughout my life. I would like to thank my advisor, Bruce Ayati, for his mentorship and guidance. I greatly appreciate his patience and support, which has spanned from my first day of graduate school as his teaching assistant to this thesis work. I thank our collaborator, Sarah Holstein, for sharing her expertise on multiple myeloma and for her willingness to give her time to this project and answer my questions. Thank you to my Iowa friends, current and former graduate students alike; I have enjoyed working with you and learning from you. Thank you for your friendship and for sharing this stage of life with me. Special thanks to Cole, Catie, Christine, Rachael, Mario, Nathaniel, and Kevin for your encouragement and support. Thank you to the professors in the Luther College Math Department, especially Richard Bernatz and Eric Westlund, for encouraging my mathematical pursuits and for their dedication to excellence in teaching. I am grateful to those who had a role in the data collection and chart review: Dr. Nancy Rosenthal, Marilyn Rosenquist, Robin Kaefring, Shirley Wade, and Tania ii
6 Viet. Without their assistance, Appendix B and the larger data set from which it comes would not exist. I also would like to thank the Graduate College, the Department of Mathematics, and the program in Applied Mathematical and Computational Sciences for their generosity. My thesis work has been partially supported by the AMCS summer fellowship and the Post-Comprehensive Summer Research Award. iii
7 ABSTRACT Multiple myeloma is a type of plasma cell cancer which causes bone disease and is associated with many health challenges, including kidney damage. Most of this damage results from the overproduction of free light chain immunoglobulins by malignant plasma cells. When the number of free light chains in the blood surpasses the amount the kidney can filter, they interact with cells in the proximal tubule of the kidney, causing inflammation and tubulointerstitial fibrosis. Unfortunately, many of these patients are often diagnosed with end-stage renal failure, requiring dialysis for the remainder of their lives. This thesis introduces a mathematical model of the process of inflammation of the kidney caused by immunoglobulins produced by malignant plasma cells. We describe basic kidney physiology and anatomy, as well as the pathophysiology involved in kidney dysfunction associated with multiple myeloma. We then discuss mathematical background for the model, including Savageau s power law approximations. We present a simple model of normal dynamics between free light chain immunoglobulins and proximal tubule cells in the kidney, and analyze this model for steady state solutions and classify stability of equilibria. Next, we expand this model to include the tumor cells present in patients with multiple myeloma. Although there has been prior work in modeling renal physiology and multiple myeloma separately, there is no known prior mathematical work in modeling the process of kidney damage caused by multiple myeloma. Our model is an initial attempt to combine these two areas of iv
8 modeling, and captures the qualitative behavior of the cell populations involved in kidney damage caused by multiple myeloma. We discuss the computational results and significance of this model, and then explore patient data collection. We introduce measurable quantities for multiple myeloma and discuss what results are given by common blood and urine tests associated with multiple myeloma. We present initial analysis of data recorded in a chart review from three patients with multiple myeloma. Patient data could be used for parameter estimation and sensitivity analysis to validate our model. The long-term goal of the project is to calibrate the model with a specific patient s data, leading to a more accurate prognosis. This type of model could provide doctors with a tool to predict the likelihood of recovery of renal function after treatment. v
9 PUBLIC ABSTRACT The kidneys are organs that play several important roles in the body, including the removal of waste and the regulation of blood pressure. When the kidneys stop functioning correctly, the human body begins to shut down. Because many diseases affect the kidneys, it is important for doctors to be able to evaluate kidney function. We can think of the kidney as a black box doctors can measure inputs and outputs through blood and urine tests, but rarely know exactly what occurs inside the kidney. Mathematical models that help doctors use those measured inputs and outputs to make predictions are an important method of evaluating kidney function. This thesis focuses on the ways multiple myeloma, a type of plasma cell cancer, affects kidney function. In some patients with multiple myeloma, proteins produced by myeloma cells cause inflammation in the kidney, which causes loss of kidney function and greatly decreases life expectancy. In these chapters, we discuss kidney physiology and describe the process of inflammation caused by myeloma. We introduce the mathematical background for our model, present and analyze a model for kidney function in healthy patients, and then present our model for kidney function in patients with multiple myeloma. Finally, we discuss using the results of patient blood and urine tests as a way to improve our model s prediction potential. The long-term goal of the work in this thesis is to create a tool that physicians can use to more accurately predict the course of disease for multiple myeloma patients with kidney involvement. vi
10 TABLE OF CONTENTS LIST OF TABLES ix LIST OF FIGURES xi CHAPTER 1 INTRODUCTION TO MULTIPLE MYELOMA Risk Factors Pathology Renal Function and Anatomy Multiple Myeloma and the Kidneys Proximal Tubule Cell Injury Cast Formation SIMPLIFIED MODEL OF NORMAL PTC AND FLC DYNAMICS IN THE KIDNEY S-Systems Development of the Model Equilibria Proximal Tubule Cells Free Light Chains Renal Fibroblasts Parameter Estimation Stability Analysis A MODEL OF THE EFFECTS OF MULTIPLE MYELOMA ON KID- NEY FUNCTION Cancer Modeling Biological Background Epithelial-Mesenchymal Transition Development of the Model Computational Results PATIENT DATA COLLECTION Measurable Quantities Blood Tests vii
11 4.1.2 Urinalysis Data Collection Autologous Stem Cell Transplant Selected Patient Data Discussion Patient No Patient No Patient No CONCLUSIONS APPENDIX A MATLAB CODE FOR MODEL SIMULATIONS A.1 Chapter 3 Model A.2 Data Analysis Example B SELECTED PATIENT DATA B.1 Patient No B.2 Patient No B.3 Patient No REFERENCES viii
12 LIST OF TABLES Table 1.1 Median survival times of patients with MM classified by kidney function Parameters used in model simulations and equilibria calculations Requirements for stability of equilibrium points Results of steady-state analysis for parameters in Table Descriptions of cytokines produced after NF-κ B and MAPK activation Parameter values used in Section B.1 Description of abbreviations used to classify patient cases B.2 Patient No B.3 Patient No B.4 Patient No B.5 Patient No B.6 Patient No B.7 Patient No B.8 Patient No B.9 Patient No B.10 Patient No B.11 Patient No B.12 Patient No B.13 Patient No ix
13 B.14 Patient No B.15 Patient No B.16 Patient No B.17 Patient No B.18 Patient No B.19 Patient No B.20 Patient No B.21 Patient No x
14 LIST OF FIGURES Figure 1.1 Intact immunoglobulin Nephron anatomy Computational steady-state analysis at (P, L, F ) = (100, 10, 100) Flowchart of light-chain mediated renal damage in multiple myeloma Diagram of the process of EMT and fibrosis Computational results for Equations (3.1)-(3.4) Computational results for Equations (3.1)-(3.4) Data analysis of Patient No. 038: Serum creatinine Data analysis of Patient No. 038: IgA levels Data analysis of Patient No. 041: Serum creatinine Data analysis of Patient No. 041: IgG levels Data analysis of Patient No. 064: Serum creatinine Data analysis of Patient No. 064: IgG levels Data analysis of Patient No. 064: Relationship between serum creatinine and IgG levels xi
15 1 CHAPTER 1 INTRODUCTION TO MULTIPLE MYELOMA Multiple myeloma (MM) is a type of cancer characterized by malignant plasma cells. An important part of the immune system, long-lived plasma cells are found in the bone marrow. In multiple myeloma patients, malignant plasma cells are produced, causing painful bone disease, hypercalcemia, and anemia. More than 60% of patients report bone pain at the time of diagnosis [9]. Multiple myeloma also affects the kidney, and 20-40% of patients present with some degree of renal impairment at diagnosis [10]. The American Cancer Society estimates that in 2016, about 30,330 patients will be diagnosed with multiple myeloma and about 12,650 deaths will occur [29]. The five-year survival rate for patients with a single plasmacytoma, a tumor made up of malignant plasma cells, is 69.6%. In contrast, the five-year survival rate of patients with multiple myeloma, or the presence of more than one plasmacytoma, is 47.4% [16]. There is currently no cure for multiple myeloma, but recent advancements in treatment in the last fifteen years have contributed to an increase in patient overall survival rates. The median survival rate for patients diagnosed with MM at the Mayo Clinic before 2001 was 2.5 years, which increased to 6.1 years in patients diagnosed between 2006 and 2010 [24]. 1.1 Risk Factors There are few known risk factors for MM, the most prevalent being age, gender, and race. Multiple myeloma is more commonly diagnosed in older populations. The
16 2 median age of patients at diagnosis is 70, and less than 1% of patients are younger than 35 at diagnosis [9, 29]. Males are slightly more likely to develop MM; of the projected 30,330 new cases in 2016, 17,900 are expected to be diagnosed in men and 12,430 in women [29]. Multiple myeloma is more than twice as likely to occur in African American patients as in white Americans, for unknown reasons. Finally, family history can be a risk factor for MM. A person with an immediate family member with MM (parent or sibling) is four times more likely to be diagnosed with multiple myeloma. However, this accounts for a very small number of cases. 1.2 Pathology Multiple myeloma is characterized by malignant plasma cells, which are found in the bone marrow, the soft tissue inside the bone. Bone marrow contains the cells that give rise to those found in the blood: red blood cells, white blood cells, and platelets. White blood cells play a very important role in the immune system, and come in six types: neutrophils, basophils, eosinophils, lymphocytes, monocytes, and macrophages. Plasma cells are terminally differentiated B-lymphocytes (also called B-cells). Plasma cells produce proteins called antibodies or immunoglobulins, which are designed to bind to pathogens such as viruses or bacteria in the body, and signal the immune system to attack those pathogens. The immunoglobulins produced by plasma cells are formed by four components, two heavy chains and two light chains. The heavy chains bind to pathogens and signal the immune system to attack. The heavy chains are defined by five classes,
17 3 Figure 1.1: Intact immunoglobulin IgG, IgD, IgA, IgM, and IgE. Of these, IgG and IgA are the most common. The light chains are characterized as kappa light chains or lambda light chains. Figure 1.1 shows an intact immunoglobulin. The blue sections are heavy chains, where the dark blue sections show the parts of the immunoglobulin that bind to pathogens. The yellow sections are light chains. Light chains and heavy chains are produced separately, and assembled to make intact immunoglobulins. When the light chains are part of an intact immunoglobulin, they are called bound light chains. Light chains that are not attached to a set of heavy chains are called free light chains. Each plasma cell produces one type of heavy chain and one type of light chain for its lifetime, for example, IgG lambda. Clonal myeloma cells will produce monoclonal antibodies (M protein). For this reason, types of multiple myeloma are categorized and monitored by the types of heavy and light chain that are produced
18 4 in excess of normal amounts. Typically, myeloma cells will produce many more light chains than heavy chains, resulting in excess levels of free light chains in the blood [7]. Bone pain occurs in patients when myeloma cells interfere with the normal bone reconstruction system, designed to keep the bones healthy and strong. Myeloma cells make a substance that signals the normal bone destructors (called osteoclasts) to dissolve the bone more quickly, which inhibits the response by normal bone constructors (called osteoblasts), so bone is not rebuilt as quickly as it dissolves and the normal bone reconstruction system breaks down. This weakens bones and increases the chance of bone fracture. This same process can also increase the levels of calcium in the blood, leading to hypercalcemia [29]. In addition to bone disease, myeloma cells cause patients to be susceptible to low blood counts and anemia. This occurs when the production of malignant myeloma plasma cells takes over the bone marrow where normal blood cells are produced. Anemia is a condition characterized by low levels of red blood cells, and causes weakness and fatigue in patients. Multiple myeloma can also cause low levels of blood platelets (thrombocytopenia) and low levels of normal white blood cells (leukopenia). This can lead to increased infections in patients with MM [9]. In some patients with multiple myeloma, the excess M protein, particularly the free light chains, can cause renal insufficiency and eventually, renal failure and end-stage renal disease (ESRD). This process is the focus of our model. We will first discuss normal renal function, and then the renal pathophysiology that occurs
19 5 in patients with multiple myeloma. 1.3 Renal Function and Anatomy The kidneys are organs that serve as the body s filtering system, and play an important role in maintaining homeostasis, the process of keeping internal conditions relatively stable in the body. The kidneys keep substances in balance by regulation and removal of metabolic waste. The main functions of the kidneys include regulating water and electrolyte balance, regulating production of red blood cells and vitamin D, and the excretion of hormones. Most of the kidneys work involves transportation of water and solutes between the blood and filtration systems in the kidney via reabsorption. Reabsorption involves moving substances from the tubules into the surrounding tissue, and from there into surrounding blood vessels and back into circulation [5]. Any substance not transported back to the blood is excreted in urine. Humans have two kidneys, located on either side of the spine in the abdominal cavity. Each kidney is made up of systems of tubules, called nephrons, that make up the working units of the kidney (Figure 1.2). Each kidney has approximately 1 million nephrons. Although the kidneys make up only about 0.5% of total body weight, they receive 20% of the body s cardiac output [21]. Blood plasma comes to the kidney by way of the renal arteries, where it is filtered into the renal tubules through the glomeruli. In a single nephron, the plasma flows from the glomerulus through the first segment of the nephron, called the proximal tubule. The proximal tubule is lined by a single layer of epithelial cells, called proximal tubule cells. From the proximal
20 6 tubule, the plasma travels through the Loop of Henle, the distal tubule, the distal nephron, and eventually, to collecting ducts. Sections of the tubules reabsorb parts of the filtered plasma back into the blood, and the remaining portions travel through the tubules to collecting ducts to be excreted as urine. At some sections of the tubules, additional amounts of substance may be added via secretion to the excreted content to maintain balance. For example, in the loop of Henle, the descending limb can let water in and out easily, but has low permeability for ions such as sodium, while the ascending limb is impermeable to water, but is permeable to ions [5]. Using this system, the nephrons can monitor amounts of ions and water levels in the body and in the filtrate, so that the amounts of substance excreted by urine keep the amounts in the body at the appropriate levels for homeostasis. 1.4 Multiple Myeloma and the Kidneys Renal disease in multiple myeloma patients is usually present as proteinuria (excess serum proteins in the urine) [2, 20]. In general, kidney diseases related to multiple myeloma result from the kidneys reduced ability to properly filter substances. There are two common types of tubular kidney damage that we will consider: proximal tubular cell injury and cast formation. The sources of this damage are the M proteins discussed in section 1.2. The most common cause of severe renal failure in multiple myeloma patients is tubulointerstitial pathology resulting from high circulating concentrations of monoclonal Ig light chains [2]. Kidney failure is reversible in about 50% of patients who present with renal
21 7 Figure 1.2: Nephron anatomy. Image source:[6] insufficiency at diagnosis [3]. For the remaining patients, kidney function has a large effect on prognosis and expected survival time. In 2000, Knudsen et al. studied the effect of renal impairment in patients with MM on survival time. The median survival rates of patients in the study are listed in Table 1.1. The study also concluded that reversibility of renal failure in patients with some degree of renal impairment improves prognosis and survival time [19]. A more recent study involving patients who received treatment demonstrated that the median overall survival for patients with renal insufficiency (defined as creatinine > 2 mg/dl) was 42 months compared with 99 months for those without renal insufficiency [10]. Although patients who achieved a renal response following therapy had improved survival rates compared to
22 8 Renal Impairment Creatinine Level Median Survival Time None < 1.47 mg/dl 36 months Moderate mg/dl 18 months Severe > 2.26 mg/dl 13 months Table 1.1: Median survival times of patients with MM classified by kidney function, where creatinine level is used as indicator of kidney function [19]. those whose renal function did not improve, the overall survival was still significantly lower than that of patients without renal insufficiency Proximal Tubule Cell Injury Proximal tubule cell (PTC) injury is caused by free light chain interaction with PTCs. Free light chains can be toxic to PTCs by blocking transport of glucose, amino acids, or phosphates, activating tubulointerstitial fibrosis, and causing excess free light chain endocytosis [25]. Endocytosis is the process by which cells absorb proteins by engulfing them. It is important to note that not all monoclonal free light chains are toxic to the kidneys. It appears that toxicity depends on the structure of a particular individual s free light chains 3D structure or protein folding [2, 13]. While high amounts of light chains can be a sign of multiple myeloma, the more useful laboratory parameter is the serum kappa-lambda ratio. Normal kappa to lambda
23 9 ratio is , compared to in situations of renal impairment [15]. When the level of either kappa or lambda light chains is very high and the other is normal to very low, the ratio is considered abnormal, which suggests the presence of clonal plasma cells. One way free light chains can be toxic to PTCs is by activating tubulointerstitial fibrosis. Tubulointerstitial fibrosis is the process initiated by the interaction between proximal tubule cells and free light chains, which activates inflammatory pathways in the kidney. Sustained inflammation causes the excess accumulation of extracellular materix (ECM), which is eventually replaced by scar tissue [11]. ECM, which is made up of proteins and collagens, provides structural support to surrounding cells and most cells cannot survive unless they are anchored to the ECM. The scar tissue that replaces ECM is part of the formation of excess fibrous tissue that characterizes fibrosis. This process is considered to be largely irreversible, and leads to the loss of function of proximal tubule cells and end-stage renal disease. Because tubulointersititial fibrosis begins with the interaction between proximal tubule cells and free light chains, the main goal of treatment is to reduce light chain production by killing the malignant plasma cells [20]. Initial treatment includes chemotherapy drugs, hydration, and in some cases the use of bisphosphonates to lower calcium levels. Plasmapheresis, which involves removing the blood plasma from the body, reducing plasma concentration of light chains, and returning it to the body, is occasionally used in cases with very high free light chain levels and acute renal failure. This is similar to hemodialysis, which is used to remove waste from the blood. Both
24 10 plasmapheresis and hemodialysis use machines to perform the kidneys usual job of filtering the blood. Renal transplantation is generally not considered because of the poor prognosis of patients with MM [20] Cast Formation Cast formation (also called cast nephropathy or myeloma kidney) occurs most frequently in the distal tubule of the nephron, when the non-endocytosed free light chains precipitate, forming solids called tubular casts within the kidney tubules. These casts are formed by the reaction of M proteins with Tamm-Horsfall protein. The casts partially or totally block the kidney tubules, which increases intraluminal pressure, reduces GFR (the sum of filtration rates of functioning nephrons), blood flow, and tubular clearance of the light chains, which increases serum light chain levels (causing a positive feedback loop or cycle). Unless the casts are removed, the result is permanent nephron loss. In addition to cast nephropathy, there are many other conditions that can contribute to myeloma-related kidney failure. Included among that group are light chain amyloidosis, light chain deposition disease, and acquired adult Fanconi syndrome, which all affect the kidneys to some degree in patients with MM [20, 4]. Renal dysfunction due to any underlying cause plays a notable role in the expected survival time of patients with MM and represents a significant clinical problem. We focus on modeling proximal tubule cell injury as an initial attempt to understand what occurs in the kidneys of patients with MM. The biological background discussed here, par-
25 11 ticularly in Section 1.4.1, will be further explored in Chapter 3 as the basis of the mathematical model presented in that chapter.
26 12 CHAPTER 2 SIMPLIFIED MODEL OF NORMAL PTC AND FLC DYNAMICS IN THE KIDNEY To preface building a model that analyzes the effect of multiple myeloma on kidney function, we developed a model that describes the dynamics between the renal proximal tubules cells and free light chains in a healthy patient. The model is a system of ordinary differential equations describing the populations of proximal tubule cells, free light chains, and renal fibroblasts. Power law approximations are used to describe the effect of populations on the growth rate of other populations involved. 2.1 S-Systems Our model makes use of the functionality of S-systems, which are based on power laws. Power laws, as investigated by Voit and Savageau, have been shown to be a reasonable approximation for describing rate laws in many biological systems. The S in S-system refers to synergism and saturation in the system, two key properties of biological and biochemical systems [27]. That is, S-systems capture both the interactions between cell populations and the saturation levels (if applicable) for the populations in the system. S-systems have several additional properties that make them useful for modeling the complex nonlinear systems found in biology. In particular, they have been shown to capture the nonlinearity that is characteristic of many biological systems. They are analytically convenient, as in many cases they can be analyzed with linear methods while still providing a nonlinear representation.
27 13 S-systems also have the advantageous property that all parameters have a clearly defined biological meaning. In contrast to other types of models that contain parameters that are mathematically necessary but lacking biological justification, the parameters in S-systems can, in principle, be measured. Even if there are no experimental methods available to measure a growth or decay rate, the parameter still has biological meaning. S-systems are based on the following general formulation of the rate of change of a population X i : dx i dt = R + i R i for i = 1, 2,..., n, (2.1) where R + i represents the growth or production of X i and R i represents depletion or decay of X i. The production and depletion of X i depend on some other number of populations in the system, so Equation (2.1) can be written as dx i dt = R + i (X 1, X 2,...X n ) R i (X 1, X 2,..., X n ), (2.2) where it is possible that R + i and R i are sums of functions. Note that Equation (2.2) is a general formula, and R + i and R i may or may not depend on all populations X 1,..., X n (including X i ). The power law formulation, described in more detail in [30, 28, 27], defines R + i and R i as R + i (X 1, X 2,..., X n ) = α i X g i1 1 X g ij n, (2.3) R i (X 1, X 2,..., X n ) = β i X h i1 1 X h ij n, (2.4) where α i and β i are rate constants. Combining Equations (2.3) and (2.4) with (2.2),
28 14 we have dx i dt = α i X g i1 1 X g ij n β i X h i1 1 X h ij n. (2.5) Now, rewriting the products, and recalling that R + i and R i may be sums of functions, we arrive at the general form for S-systems: dx i dt = k α k j X g ij j k β k j X h ij j. (2.6) This gives a model for the rate of change of the X i population. The first term represents the components of the system that influence the growth of X i, and the second term is made up of those populations and factors that influence the decay of the X i population. The rate constants are {α k } and {β k }, where the α k are growth constants and the β k are decay constants. The powers g ij and h ij are the orders of reaction with respect to X i for production and degradation of X j, respectively. 2.2 Development of the Model Based on interactions between cell populations, the equations for the model are described verbally by Change in PTCs = + natural PTC production natural PTC death (apoptosis), Change in FLCs = + natural FLC production natural removal of FLCs, Change in Fibroblasts = + natural fibroblast production natural fibroblast death.
29 15 The verbal description of our model is defined mathematically using the following dependent variables: P (t) = the population of proximal tubule cells at time t, L(t) = the amount of free light chains at time t, F (t) = the population of renal fibroblasts at time t. The system of differential equations below, a modified S-system, describes the dynamics of cell populations in the kidney: We define ) g1 d dt P (t) = β P P g 2 (1 LLS + }{{} 1 µ P P, (2.7) }{{} ( d dt L(t) = γ LL 1 Ḽ ) µ L L, (2.8) L }{{} + }{{} 3 ( d dt F (t) = γ F F 1 FˆF ) µ F F. (2.9) }{{} + }{{} ˆL = L minγ L γ L µ L, ˆF = γ F F max, γ F µ F (x) + = x, if x 0, 0, if x < 0. The use of the (x) + function ensures the non-negativity of the first terms in (2.7)-(2.9). The processes each term represents are: 1 represents the proliferation rate of the proximal tubule cells, incorporating that the presence of free light chains decreases the proliferation of proximal tubule
30 16 cells. The PTC proliferation rate is β P and L S is the FLC saturation constant. This term is always non-negative. The parameter g 1 describes the strength of FLCs on inhibited PTC growth, and g 2 describes the strength of the PTC population on its own growth. 2 represents natural death of proximal tubule cells. The PTC apoptosis rate is µ P. 3 represents the growth in the number of circulating free light chains. The parameters L min represents the minimum number of FLCs and γ L is the free light chain growth constant. This term is always non-negative; ˆL is defined as ˆL = L minγ L γ L µ L. 4 represents natural removal of free light chains, and µ L is the natural removal rate. 5 represents growth in the number of renal fibroblasts. The parameter F represents the maximum percentage of renal fibroblasts and γ F is the fibroblast growth constant. This term is always non-negative; ˆF is defined as ˆF = γ F F max γ F µ F 6 represents natural death of the fibroblast population, where µ F is the fibroblast natural apoptosis rate. 2.3 Equilibria The equilibrium point of the system is the point that gives a constant solution to all three differential equations. Solving for the equilibria of each equation is done by setting dx i dt = 0 for all populations X i. The equilibria, or steady states, for proximal tubule cells (2.1), free light chains (2.2) and fibroblasts (2.3) can be found both analytically and computationally.
31 Proximal Tubule Cells Recall that the proximal tubule cell population dynamics is given by ) g1 dp (1 dt = β LLS P g 2 µ P P. + In solving dp dt = 0, we consider three cases: Case 1: FLC Saturation (L = L S ). Then 1 L L S = 0 and we have: 0 = β P 0 g 1 P g 2 µ P P, 0 = µ P P. This result implies that P = 0, since we assume µ P is always non-zero. Case 2: L = 0 (abiological). Then 1 L L S = 1 and we have: 0 = β(1) g 1 P g 2 µ P P, µ P P = βp g 2, P = β µ P P g 2, P 1 g 2 = β µ P, ( β P = µ P ) 1 1 g 2. Note that this is a mathematical equilibrium value, but does not have value biologically as even healthy patients have some small level of serum free light chains. Case 3: Suppose 0 < 1 L L S < 1. Then ( 0 = β 1 L ) g1 P g 2 µ P P, L S 0 = P [ ) g1 ] β (1 LLS P g2 1 µ P.
32 18 From this factored expression, we have that either P = 0 or β ( 1 L L S ) g1 P g 2 1 µ P = 0. In the latter case: β ( 1 L L S ) g1 P g 2 1 µ P = 0, β ( 1 L L S ) g1 P g 2 1 = µ P, P g 2 1 = P = µ P ) g1, β (1 LLS ( ) ) 1 g1 µ P (1 LLS g 2 1. β Our three cases give us three equilbria for the PTC population at P = 0, P = ( ) ) 1 g1 g 1 g and P = (1 LLS. ) 1 β µ P ( µ P β Free Light Chains Equation (2.2) describes the behavior of the free light chain population: ( dl dt = γ LL 1 Ḽ ) µ L L. L + Solving dl dt = 0 yields: ( 0 = γ L L 1 Ḽ ) L + ( 0 = L [γ L 1 Ḽ ) L µ L L, + µ L ].
33 19 ( ) This implies either L = 0, or γ L 1 Ḽ µ L L = 0. For the second case, + ( µ L = γ L 1 Ḽ ), L Since ˆL = µ L γ L = 1 Ḽ L, 1 µ L = Ḽ γ L L, ( ˆL 1 µ ) L = L. γ L L min 1 µ L γ L, this simplifies to L = L min. Thus, the equilibria for the free light chain population are L = 0 and L = L min. As noted above, L = 0 is a mathematical equilibrium, but is not useful biologically, as healthy patients all have some small level of serum free light chains present Renal Fibroblasts Recall that the equation describing the rate of change of the renal fibroblast population is given by ( df dt = γ F F 1 FˆF ) µ F F. + Solving df dt = 0 yields ( 0 = γ F F 1 FˆF ) + ( 0 = F [γ F 1 FˆF ) µ F F, + µ F ].
34 20 ( ) This implies either F = 0 or γ F 1 FˆF µ F = 0. For the second case, + ( 0 = γ F 1 FˆF ) µ F = γ F ( 1 FˆF µ F = γ F γ F F ˆF, µ F γ F = γ F F ˆF, ˆF (µ F γ F ) γ F = F. + ), µ F, Since ˆF = γ F F max γ F µ F, this simplifies to F = F max. Thus, the equilibria for the renal fibroblast population are F = 0 and F = F max. 2.4 Parameter Estimation Normal serum free light chain levels for a healthy patient are roughly 10 mg/l, so this was used for L min [7]. The FLC saturation constant L S was set to 1000 mg/l, as this is the threshold at which kidney problems typically occur [12]. All other parameters for this model were obtained for the model using heuristic parameter estimation to a generic response. We determine and scale our parameters so that the steady state for Case 3 of the PTC population is normalized to P = 100. Recall that the steady state satisfies β ( 1 L L S ) g1 P g 2 1 µ P = 0.
35 21 Parameter name symbol value units FLC growth constant γ L.005 1/(% cells days) Fibroblast growth constant γ F.004 L/(mg days) PTC proliferation constant β P.055 1/days FLC saturation constant L S 1000 mg/l Minimum FLC level L min 10 mg/l Maximum fibroblast population F max 100 percentage PTC natural apoptosis rate µ P.045 1/days Natural FLC apoptosis rate µ L /days Natural fibroblast apoptosis rate Strength of FLC on PTC growth Strength of PTC on its own growth µ F /days g 1 1 dimensionless g dimensionless Table 2.1: Parameters used in model simulations and equilibria calculations.
36 Stability Analysis Consider the system of ODEs X = f ( X ), where we define f ( X ) = (f1 ( X ), f 2 ( X ), f 3 ( X )) T and the dot denotes differentiation with respect to time. For our model, X = (P, L, F ) T, and the f i are defined by f 1 ( ( X ) = β P 1 L ) g1 P g 2 µ P P, L S + f 2 ( ( X ) = γ L L 1 Ḽ ) µ L L, L + f 3 ( ( X ) = γ F F 1 FˆF ) µ F F. To determine the stability of the nonlinear system at its equilibrium point, the system is linearized by finding the Jacobi matrix J = (a ij ) where a ij = f i X j i = 1, 2, 3 and j = 1, 2, 3. Finding the partial derivatives of the equations f 1, f 2, and f 3 yields the following Jacobi matrix: + for β P (1 L L S ) g 1 + g 2 P g2 1 µ P β P L S g 1 P g 2 (1 L L S ) g 1 1 J = γ L 2Lγ L ˆL µ L γ F 2F γ F ˆF. µ F The Jacobian is then evaluated at its eight equilibrium points. The local stability of the system is determined by finding the eigenvalues λ i of the Jacobi matrix J. An
37 23 equilibrium point is asymptotically stable if and only if all eigenvalues of J evaluated at the point are have negative real values (Re(λ i ) < 0 for all i). An equilibrium point is unstable if at least one eigenvalue of J evaluated at the point has positive real value (Re(λ i ) > 0 for some i). To find the eigenvalues and analyze stability of the steady state solutions, we solve the characteristic equation det(j λi) = 0, for λ. Eigenvectors of the system can be used to analyze the directions of the subspaces of the linearized system, and are found by solving (J λi) v = 0, where each eigenvalue λ is used to find corresponding eigenvector v. The only equilibrium point for which all three populations are non-zero is the point ( (P, L, F ) = µ P β P (1 LLS ) g1 ) 1 g 2 1, L min, F max. At this point, the Jacobian is given by the following matrix: g 2 µ P µ P β P L S g 1 (P ) g 2 (1 L L S ) g J = 0 µ L γ L µ F γ F This is a triangular matrix, so the eigenvalues are the entries on the diagonal. The equilibrium point is stable when g 2 < 1 (since we assume µ p > 0), γ L > µ L, and
38 24 γ F > µ F, which gives negative real-valued eigenvalues. MATLAB was used in the following calculations of the Jacobian for the current parameters from Table 2.1, for which ( (P, L, F ) = µ P β P (1 LLS ) g1 ) 1 g 2 1 For these parameter values, the Jacobian is, L min, F max = (100, 10, 100) J (100,10,100) = , which has the following eigenvalues: λ λ 2 = λ MATLAB was then used to solve for the corresponding eigenvectors: λ 1 = = v 1 = ( , 1, 0) T, λ 2 = = v 2 = (0, 0, 1) T, λ 3 = = v 3 = (1, 0, 0) T. At (P, L, F ) = (100, 10, 100), λ i < 0 for i = 1, 2, 3, so it is an asymptotically stable equilibrium point. This behavior is verified by Figure (2.1), which shows the system tending to the steady state at various initial values. PTC and renal fibroblast populations are interpreted as percentages and FLC population is measured in mg/l. At the trivial equilibrium point (P, L, F ) = (0, 0, 0), the Jacobi matrix is
39 25 µ P 0 0 J (0,0,0) = 0 γ L µ L γ F µ F Since this is a diagonal matrix, the eigenvalues are the entries on the diagonal. For the eigenvalues to be negative real values, we require µ P > 0, γ L < µ L, and γ F < µ F. For the parameters in Table 2.1 the Jacobian is J (0,0,0) = Solving for the eigenvalues gives us λ λ 2 = λ Two eigenvalues (λ 2 and λ 3 ) have positive real value, and λ 1 is negative, therefore the trivial steady state is an unstable equilibrium point, a saddle point for the current ( ) 1 β 1 g parameters. We note that (0, 0, 0) is abiological, when L = 0 we have P = P 2 µ P. ( ) 1 β 1 g Other mathematical steady state points are when P = P 2 µ P, which is true when L = 0. There is no restriction on the renal fibroblast population, so this gives us two equilibrium points to check, when F = 0 and F = F max. When F = 0, we have the equilibrium point (P, L, F ) = ( (βp µ P ) 1 1 g 2, 0, 0 ).
40 26 The Jacobi matrix at this point is: [ ( β P J ( ) ( ) 1 βp = 1 g 2,0,0 µ P µ P ) 1 1 g 2 ] g2 1 β P g 2 µ P β P g 1 ( ) g2 β 1 g P 2 L S µ P 0 0 γ L µ L γ F µ F, = J ( ) ( ) 1 βp = 1 g 2,0,0 µ P µ P (g 2 1) β P g 1 ( ) g2 β 1 g P 2 L S µ P 0 0 γ L µ L γ F µ F. This is a triangular matrix, so the eigenvalues are the diagonal entries: λ 1 µ P (g 2 1) λ 2 = λ 3 γ L µ L γ F µ F. For this equilibrium point to be stable, we require g 2 < 1 (since we assume µ P > 0), γ L < µ L and γ F < µ F. For parameters in Table 2.1, the equilibrium point is (P, L, F ) = and the Jacobi matrix is ( (βp µ P ) 1 1 g 2, 0, 0 ) = ( , 0, 0), J ( ,0,0) = The eigenvalues of this matrix are
41 27 λ λ 2 = λ We have λ 1 < 0, λ 2 > 0, λ 3 > 0, so (P, L, F ) = ( , 0, 0) is an unstable equilibrium point for the current parameters. Next we check the case above where F = F max, the equilibrium point (P, L, F ) = ( (βp In this case, the simplified Jacobi matrix is µ P ) 1 1 g 2, 0, Fmax ). J ( ( ) 1 βp = 1 g 2,0,F µ max) P µ P (g 2 1) β P g 1 ( ) g2 β 1 g 2 L S µ P 0 0 γ L µ L µ F γ F. For this equilibrium point to be stable, we require g 2 < 1, γ L < µ L, and µ F < γ F. Evaluating at the parameters from Table 2.1 results in the equilibrium point (P, L, F ) = and the Jacobian ( (βp µ P ) 1 1 g 2, 0, Fmax ) = ( , 0, 100), J ( ,0,100) = , which has the following eigenvalues:
42 28 λ λ 2 = λ The eigenvalue λ 2 > 0, so we conclude that the equilibrium point (P, L, F ) = ( , 0, 100) is unstable for the current parameters. The next equilibrium point we analyze is (P, L, F ) = (0, 0, F max ). At this point, the Jacobi matrix is µ P 0 0 J (0,0,Fmax) = 0 γ L µ L µ F γ F For this equilibrium point to be stable, we require γ L < µ L, µ F < γ F, and µ P > 0. For our parameter set, F max = 100, and evaluating at (P, L, F ) = (0, 0, 100) gives us the following Jacobi matrix: J (0,0,100) = Solving for the eigenvalues gives us λ λ 2 = λ Therefore, (P, L, F ) = (0, 0, 100) is an unstable equilibrium point of our system with current parameter values.
43 29 The next equilibrium point is (P, L, F ) = (0, L min, 0). At this point, the Jacobi matrix is µ P 0 0 J (0,Lmin,0) = 0 µ L γ L γ F µ F For stability of this equilibrium point, we require µ P > 0, µ L < γ L, and γ F < µ F. We set L min = 10 and evaluate with parameters from Table 2.1 at (P, L, F ) = (0, 10, 0) to find the following Jacobian: J (0,10,0) = The eigenvalues of this matrix are λ λ 2 = λ Thus (P, L, F ) = (0, 10, 0) is an unstable equilibrium point for current parameter values. The next equilibrium point is (P, L, F ) = (0, L min, F max ). The Jacobian evaluated at this point reduces to µ P 0 0 J (0,Lmin,0) = 0 µ L γ L µ F γ F
44 30 For this equilibrium point to be stable, we require µ P > 0, µ L < γ L, and µ F < γ F. At L min = 10 and F max = 100, (P, L, F ) = (0, 10, 100) and the Jacobian is J (0,10,100) = The eigenvalues of this matrix are found to be λ λ 2 = λ At (P, L, F ) = (0, 10, 100), we have only negative real eigenvalues, so this is a stable equilibrium point. Note that this point is not biologically relevant to our model, as a patient without any proximal tubule cells would not have working kidney. The final equilibrium point is ( (P, L, F ) = µ P β P (1 LLS ) g1 ) 1 g 2 1, L min, 0. At this point, the reduced form of the Jacobian matrix is given by g 2 µ P µ P β P L S g 1 (P ) g 2 (1 L L S ) g J (P,L,F ) = 0 µ L γ L γ F µ F For this equilibrium to be stable, we require g 2 < 1 (since we assume µ P > 0),
45 31 µ L < γ L, and µ F > γ F. For the parameter values in Table 2.1, the equilibrium point is ( (P, L, F ) = µ P β P (1 LLS ) g1 ) 1 g 2 1, L min, 0 = (100, 10, 0). For these parameter values, the Jacobian is J (100,10,0) = The eigenvalues of this matrix are λ λ 2 = λ We have two negative real-valued eigenvalues and one positive real-valued eigenvalue, so (P, L, F ) = (100, 10, 0) is an unstable equilibrium point. Tables 2.2 and 2.3 summarize the results of the above work. This model shows the behavior we would expect to see for kidney function in a healthy patient. We have a stable equilibrium point at (P, L, F ) = (100, 10, 100), which is both biologically and mathematically relevant. The PTC population and renal fibroblast population measurements are interpreted as percentages. This means that a healthy patient with 100% PTCs and renal fibroblasts, and the minimum healthy levels of serum free light chains (L min = 10 mg/l) can expect to stay in a healthy state without any outside intervention. In the next chapter, we explore what happens to the system upon introduction of myeloma tumor cells.
46 32 (P, L, F ) Requirements for Stability ( ( ( ) ) ) 1 µp β P 1 L g1 g 2 1 L S, Lmin, F max γ F > µ F, γ L > µ L, g 2 < 1 ( ( ( ) ) ) 1 µp β P 1 L g1 g 2 1 L S, Lmin, 0 γ F < µ F, γ L > µ L, g 2 < 1 ( ( ) ) 1 β 1 g P 2 µ P, 0, F max γ F > µ F, γ L < µ L, g 2 < 1 ( ( ) ) 1 β 1 g P 2 µ P, 0, 0 γ F < µ F, γ L < µ L, g 2 < 1 (0, L min, F max ) γ F > µ F, γ L > µ L, µ P > 0 (0, L min, 0) γ F < µ F, γ L > µ L, µ P > 0 (0, 0, F max ) γ F > µ F, γ L < µ L, µ P > 0 (0, 0, 0) γ F < µ F, γ L < µ L, µ P > 0 Table 2.2: Requirements for stability of equilibrium points of the model described by Equations
47 33 (P, L, F ) Stability (100, 10, 100) stable (100, 10, 0) unstable ( , 0, 100) unstable ( , 0, 0) unstable (0, 10, 100) stable (0, 10, 0) unstable (0, 0, 100) unstable (0, 0, 0) unstable Table 2.3: Results of steady-state analysis for parameters in Table 2.1, including eight equilibrium points and their stability found using parameters listed in Table 2.1.
48 PTC Population 100 PTC Population 100 PTC Population Time (days) Time (days) Time (days) (a) P(0)=95 (b) P(0)=100 (c) P(0)= FLC Population 10 FLC Population 10 FLC Population Time (days) Time (days) Time (days) (d) L(0)=5 (e) L(0)=10 (f) L(0)= Fibroblast Population 100 Fibroblast Population 100 Fibroblast Population Time (days) Time (days) Time (days) (g) F(0)=95 (h) F(0)=100 (i) F(0)=105 Figure 2.1: Computational steady-state analysis at (P, L, F ) = (100, 10, 100) of PTCs, FLCs, and renal fibroblasts.
49 35 CHAPTER 3 A MODEL OF THE EFFECTS OF MULTIPLE MYELOMA ON KIDNEY FUNCTION 3.1 Cancer Modeling In this chapter, we will use the simplified model for a healthy patient from Chapter 2 and add the effect of the myeloma tumor. The creation of mathematical models of cancer and running computer simulations (called in silico experiments) gives researchers an opportunity to test hypotheses via the model before spending time and resources on clinical trials or in vitro experiments. Mathematical modeling of tumors as a method of in silico experimentation has a long history, cataloged in [26, 8], among others. The most common tumor growth laws are: Exponential growth functions Power law functions Logistic growth functions Gompertz growth functions von Bertalanffy growth functions The type of model chosen depends on the type of cancer being modeled and the growing environment of the cancer. While one growth function may be sufficient for a model of cancer in mice or in vitro, a different growth function may be required to model the growth of the same cancer in humans. In our model, we use the Gompertz growth function, which was originally developed in 1825 as a model of human mortality, and first proposed as a tumor
50 36 growth model in 1965 [8]. It is similar to an exponential growth model, but assumes a time-dependent growth rate. The Gompertz curve is sigmoidal, and reaches an asymptote as time goes on (suggesting a carrying capacity for tumor load). The Gompertz growth function has the form: V (t) = V 0 e r 0 ρ (1 e ρt), (3.1) where r 0 is the growth rate at time t = 0, V 0 is the initial volume of the tumor, and ρ is the rate at which the growth rate increases (making the growth rate timedependent). An equivalent form of the Gompertz growth function as an ordinary differential equation (ODE), which we will use, is ( ) d K(t) V (t) = ρv (t) ln, (3.2) dt V (t) where K(t) is the carrying capacity of the tumor. By using the concept of tumor load carrying capacity, the Gompertz model captures the decrease in tumor growth rate over time. It has been used to model the growth of myeloma in [1] and will be used in the model presented here. An advantage of the form of Equation (3.2) over (3.1) is that the ODE form can be modified and coupled to other system components more easily. 3.2 Biological Background In Chapter 1 we introduced what happens in the kidneys of patients with MM via proximal tubule cell injury. To better identify the various cell populations and how they interact upon introduction of myeloma cells, we present a flowchart in
51 37 Increased FLC production by myeloma cells Increased light chain endocytosis by PTCs via cubulin/megalin Precipitation of nonendocytosed FLC NF-κB, MAPK activation in PTCs Tubular casts Proinflammatory and fibrotic pathways, EMT IL-6, CCL2, IL-8, TGF-β production by PTCs Upstream obstruction Renal interstitial fibrosis, PTC apoptosis Chronic renal failure Figure 3.1: Flowchart of light-chain mediated renal damage in multiple myeloma, courtesy of Dr. Sarah Holstein.
52 38 Figure 3.1. The increased monoclonal protein production by the abnormal myeloma cells leads to an increased level of free light chain molecules circulating in the blood. These free light chains are either endocytosed (and follow the blue section of Figure 3.1, or precipitated (and follow the yellow section of Figure 3.1). In the primary situation that our model addresses, the increased free light chain production leads to increased light chain endocytosis by proximal tubule cells via cubilin/megalin complex. Cubilin and megalin are two endocytic receptors that play important roles in renal tubular clearance and re-absorption of proteins. They initiate receptor-mediated endocytosis, a process by which cells internalize molecules. This involves an inward budding of plasma membrane vesicles containing the monoclonal proteins with receptor sites specific to the molecules being internalized. This increased light chain endocytosis activates NF-κB and MAPK in the proximal tubule cells. NF-κB is a protein complex involved in regulating the immune system s response to inflammation, and is responsible for cytokine production. Mitogen-activated protein kinases (MAPK) direct the cellular response to mitogens and proinflammatory cytokines, which are small proteins important in cell-signaling. The activation of NF-κB and MAPK initiates the production of several different types of cytokines and growth factors by the proximal tubule cells: IL-6, CCL2, IL-8 and TGF-β. Further description is provided in Table 3.1. These cytokines and growth factors initiate proinflammatory and fibrotic pathways, which in turn initiate Epithelial-Mesenchymal Transition (EMT), type 2.
53 39 Name Description CCL2 IL-6 IL-8 TGF-β Recruits memory T-cells and dendritic cells to inflammation sites Produced by T-cells and macrophages to stimulate immune response; acts as a proinflammatory cytokine Produced by macrophages and epithelial cells, induces chemotaxis in neutrophils and sends them to site of inflammation Controls cell growth, apoptosis, and proliferation Table 3.1: Descriptions of cytokines produced after NF-κ B and MAPK activation Epithelial-Mesenchymal Transition Epithelial-mesenchymal transition (EMT) plays many important roles in the body, and is one of the ways that cells change and grow. EMT is classified into three distinct types. Type 1 EMTs are those associated with formation of the embryo and organ development. Type 2 EMTs are a way for the body to heal wounds and regenerate tissue. This type is also associated with organ fibrosis. Type 3 EMTs are associated with cancer, and is a way that epithelial cancer cells metastasize and spread through the body [18]. Because our model concerns fibrosis in the kidney, we focus on type 2 EMT. During type 2 EMT, polarized epithelial cells (such as those that line the kidney tubules, in our case, proximal tubule cells) change to assume mesenchymal cell characteristics. This process is illustrated and further described in Figure 3.2.
54 40 This allows these cells increased ability to migrate to an infection site, increased resistance to apoptosis, and increased production of ECM material. Type 2 EMTs occur over extended periods of time, and can eventually permanently damage an organ if the source of inflammation is not removed or destroyed [18]. In the context of renal interstitial fibrosis, the sustained inflammation in proximal tubule epithelial cells and resulting fibrosis cause a disruption in the normal genesis and breakdown cycle of ECM, which leads to excessive ECM accumulation [22]. Eventually, scar tissue replaces ECM accumulation, and causes loss of function of PTCs. Ultimately, end-stage renal failure can develop. The secondary situation (the yellow section of Figure 3.1) is related to cast formation discussed in Chapter 1. The free light chains that did not go through endocytosis react with Tamm-Horsfall protein, forming tubular casts within the kidney tubules, usually the distal tubules or collecting ducts. The casts increase intraluminal pressure, reduce blood flow and tubular clearance of free light chains. This reduced clearance of free light contributes to the increased level of serum free light chains, and the cycle begins again. Without removal, tubular casts cause permanent nephron loss. 3.3 Development of the Model Based on interactions between cell populations described by Figure 3.1, the model presented in Chapter 2 was modified to include the introduction of a tumor of myeloma cells. Terms were added to capture the increased production of free light chains by the myeloma cells, and to account for proximal tubule cells that underwent
55 41 Figure 3.2: Diagram of the process of EMT and fibrosis, based on a figure in [18]. This diagram shows Type 2 EMTs, which is associated with organ fibrosis. the left side of the figure is a cross section of a tubule before EMT occurs. On The tubule is lined with epithelial cells, which are anchored to the basement membrane, a special type of extracellular matrix. On the right side of the figure is the tubule as EMT takes place. The immune system response to inflammation causes disruption of the normal healing cycle, and the epithelial cells lose polarity (become detached from the basement membrane), and undergo EMT to turn into mesenchymal cells (myofibroblasts) or apoptosis. Many more cells undergo apoptosis than EMT.
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Tarek ElBaz, MD. Prof. Internal Medicine Chief, Division of Renal Medicine Al Azhar University President, ESNT
 The Kidney in Multiple Myeloma Tarek ElBaz, MD. Prof. Internal Medicine Chief, Division of Renal Medicine Al Azhar University President, ESNT Normal Cell Plasma cells produce antibodies that bind to antigens,
The Kidney in Multiple Myeloma Tarek ElBaz, MD. Prof. Internal Medicine Chief, Division of Renal Medicine Al Azhar University President, ESNT Normal Cell Plasma cells produce antibodies that bind to antigens,
Jo Abraham MD Division of Nephrology University of Utah
 Jo Abraham MD Division of Nephrology University of Utah 68 year old male presented 3 weeks ago with a 3 month history of increasing fatigue He reported a 1 week history of increasing dyspnea with a productive
Jo Abraham MD Division of Nephrology University of Utah 68 year old male presented 3 weeks ago with a 3 month history of increasing fatigue He reported a 1 week history of increasing dyspnea with a productive
Chapter 13 The Urinary System
 Biology 12 Name: Urinary System Per: Date: Chapter 13 The Urinary System Complete using BC Biology 12, page 408-435 13.1 The Urinary System pages 412-413 1. As the kidneys produce urine, they carry out
Biology 12 Name: Urinary System Per: Date: Chapter 13 The Urinary System Complete using BC Biology 12, page 408-435 13.1 The Urinary System pages 412-413 1. As the kidneys produce urine, they carry out
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
PARTS OF THE URINARY SYSTEM
 EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
12/7/10. Excretory System. The basic function of the excretory system is to regulate the volume and composition of body fluids by:
 Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
1. remove: waste products: urea, creatinine, and uric acid foreign chemicals: drugs, water soluble vitamins, and food additives, etc.
 Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
November 30, 2016 & URINE FORMATION
 & URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
& URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Excretion and Water Balance
 Excretion and Water Balance In the body, water is found in three areas, or compartments: Plasma, the liquid portion of the blood without the blood cells, makes up about 7 percent of body fluid. The intercellular
Excretion and Water Balance In the body, water is found in three areas, or compartments: Plasma, the liquid portion of the blood without the blood cells, makes up about 7 percent of body fluid. The intercellular
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Homeostatic Regulation
 Homeostatic Regulation A hormone is :a Water-soluble hormones: Composed of amino acids and bind a receptor protein on the of the target cell. This starts a signal cascade inside the cell and the signal
Homeostatic Regulation A hormone is :a Water-soluble hormones: Composed of amino acids and bind a receptor protein on the of the target cell. This starts a signal cascade inside the cell and the signal
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
The Excretory System
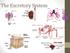 The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
PHGY210 Renal Physiology
 PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
Chapter 12. Excretion and the Interaction of Systems
 Chapter 12 Excretion and the Interaction of Systems 1 2 Goals for This Chapter 1. Identify the main structures and functions of the human excretory system 2. Explain the function of the nephron 3. Describe
Chapter 12 Excretion and the Interaction of Systems 1 2 Goals for This Chapter 1. Identify the main structures and functions of the human excretory system 2. Explain the function of the nephron 3. Describe
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
Urinary System BIO 250. Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat. Routes of Waste Elimination
 Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Excretory System. Biology 2201
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System. Excretory System
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Unit #4 Waste and Excretion. The Kidneys
 Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Kidney Physiology. Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed
 Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Question 1: Solution 1: Question 2: Question 3: Question 4: Class X The Excretory System Biology
 A. MULTIPLE CHOICE TYPE: (select the most appropriate option in each case) Book Name: Selina Concise Question 1: Excretion primarily involves (a) removal of all byproducts during catabolism (b) removal
A. MULTIPLE CHOICE TYPE: (select the most appropriate option in each case) Book Name: Selina Concise Question 1: Excretion primarily involves (a) removal of all byproducts during catabolism (b) removal
Anatomy/Physiology Study Guide: Unit 9 Excretory System
 Anatomy/Physiology Study Guide: Unit 9 Excretory System 1) In the space below, list the primary structures (organs) and their corresponding functions. Structures: Functions: KIDNEY 1) URETER BLADDER URETHRA
Anatomy/Physiology Study Guide: Unit 9 Excretory System 1) In the space below, list the primary structures (organs) and their corresponding functions. Structures: Functions: KIDNEY 1) URETER BLADDER URETHRA
WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure
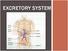 EXCRETORY SYSTEM WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure These wastes include: Carbon dioxide Mostly through breathing
EXCRETORY SYSTEM WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure These wastes include: Carbon dioxide Mostly through breathing
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
A. Incorrect! The urinary system is involved in the regulation of blood ph. B. Correct! The urinary system is involved in the synthesis of vitamin D.
 Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
A. Correct! Flushing acids from the system will assist in re-establishing the acid-base equilibrium in the blood.
 OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
Na concentration in the extracellular compartment is 140
 هللامسب Na regulation: Na concentration in the extracellular compartment is 140 meq\l. Na is important because: -It determines the volume of extracellular fluid : the more Na intake will expand extracellular
هللامسب Na regulation: Na concentration in the extracellular compartment is 140 meq\l. Na is important because: -It determines the volume of extracellular fluid : the more Na intake will expand extracellular
YR10. IGCSE Biology. Homeostasis
 YR10 IGCSE Biology Homeostasis Name: Prepared by William Green DBGS 2010 Homeostasis Body cells work best if they have the correct conditions e.g. 1. 2. 3. Write the definition of Homeostasis in the box
YR10 IGCSE Biology Homeostasis Name: Prepared by William Green DBGS 2010 Homeostasis Body cells work best if they have the correct conditions e.g. 1. 2. 3. Write the definition of Homeostasis in the box
Urinary System. Analyze the Anatomy and Physiology of the urinary system
 Urinary System Analyze the Anatomy and Physiology of the urinary system Kidney Bean-shaped Located between peritoneum and the back muscles (retroperitoneal) Renal pelvis funnelshaped structure at the beginning
Urinary System Analyze the Anatomy and Physiology of the urinary system Kidney Bean-shaped Located between peritoneum and the back muscles (retroperitoneal) Renal pelvis funnelshaped structure at the beginning
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Science of Veterinary Medicine. Urinary System Unit Handouts
 Science of Veterinary Medicine Urinary System Unit Handouts Urinary System Functions of the Urinary System Elimination of waste products Regulate aspects of homeostasis Organs of the Urinary system The
Science of Veterinary Medicine Urinary System Unit Handouts Urinary System Functions of the Urinary System Elimination of waste products Regulate aspects of homeostasis Organs of the Urinary system The
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
P215 Spring 2018: Renal Physiology Chapter 18: pp , Chapter 19: pp ,
 P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
Unit 4 Homeostasis. The term homeostasis refers to the body s attempt. Your body systems must to maintain a stable internal environment -
 Unit 4 Homeostasis The term homeostasis refers to the body s attempt Your body systems must to maintain a stable internal environment - The body is trying to maintain, through a series of monitored adjustments.
Unit 4 Homeostasis The term homeostasis refers to the body s attempt Your body systems must to maintain a stable internal environment - The body is trying to maintain, through a series of monitored adjustments.
HIHIM 409 7/26/2009. Kidney and Nephron. Fermamdo Vega, M.D. 1
 Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
The Urinary S. (Chp. 10) & Excretion. What are the functions of the urinary system? Maintenance of water-salt and acidbase
 10.1 Urinary system The Urinary S. (Chp. 10) & Excretion 10.1 Urinary system What are the functions of the urinary system? 1. Excretion of metabolic wastes (urea, uric acid & creatinine) 1. Maintenance
10.1 Urinary system The Urinary S. (Chp. 10) & Excretion 10.1 Urinary system What are the functions of the urinary system? 1. Excretion of metabolic wastes (urea, uric acid & creatinine) 1. Maintenance
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
Functional morphology of kidneys Clearance
 Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
You will test a sample of the patient s urine to determine if her kidneys are functioning normally.
 STO-118 A Kidney Problem? The Case Ten years ago, your patient was diagnosed with Type 2 diabetes. She has been careless about following the treatment needed to keep her blood glucose levels regulated.
STO-118 A Kidney Problem? The Case Ten years ago, your patient was diagnosed with Type 2 diabetes. She has been careless about following the treatment needed to keep her blood glucose levels regulated.
Kidney Lab. Name: By the end of this lab, you should:
 Kidney Lab Name: Kidneys do a grand job removing the toxic waste products of metabolism. This process is called excretion. Our kidneys produce urine which contains urea, excess salts and excess water.
Kidney Lab Name: Kidneys do a grand job removing the toxic waste products of metabolism. This process is called excretion. Our kidneys produce urine which contains urea, excess salts and excess water.
Urinary System and Fluid Balance. Urine Production
 Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Acute Kidney Injury (AKI) Undergraduate nurse education
 Acute Kidney Injury (AKI) Undergraduate nurse education Year One Developed Summer 2017 Overview Basic A & P of: Urinary system Kidneys Followed by: Introduction to Acute Kidney Injury Urinary System The
Acute Kidney Injury (AKI) Undergraduate nurse education Year One Developed Summer 2017 Overview Basic A & P of: Urinary system Kidneys Followed by: Introduction to Acute Kidney Injury Urinary System The
BIOLOGY - CLUTCH CH.44 - OSMOREGULATION AND EXCRETION.
 !! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
!! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
Lesson Overview. The Excretory System. Lesson Overview The Excretory System
 Lesson Overview 30.4 THINK ABOUT IT It s a hot day and you gulp down water. As you drink, you begin to wonder. Where s all that water going? Will it just dilute your blood, or is something in your body
Lesson Overview 30.4 THINK ABOUT IT It s a hot day and you gulp down water. As you drink, you begin to wonder. Where s all that water going? Will it just dilute your blood, or is something in your body
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
5.Which part of the nephron removes water, ions and nutrients from the blood?
 Uro question 1.While reading a blood test I notice a high level of creatinine, I could assume from this that A) There is a possibility of a UTI B) There is a possibility of diabetes C) There is a possibility
Uro question 1.While reading a blood test I notice a high level of creatinine, I could assume from this that A) There is a possibility of a UTI B) There is a possibility of diabetes C) There is a possibility
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Excretion and Water Balance
 Excretion and Water Balance 1. Osmoregulation (water balance) a. Most marine invertebrates are osmoconformers in which the concentration of solutes in their body fluid is equal to that of their environment.
Excretion and Water Balance 1. Osmoregulation (water balance) a. Most marine invertebrates are osmoconformers in which the concentration of solutes in their body fluid is equal to that of their environment.
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Chapter 32 Excretion
 Chapter 32 Excretion 3.4 Learning Objectives 3.4.6 The Excretory System in Humans 1. Role of the excretory system in homeostasis. 2. Importance of temperature regulation within the body. 3. Outline the
Chapter 32 Excretion 3.4 Learning Objectives 3.4.6 The Excretory System in Humans 1. Role of the excretory system in homeostasis. 2. Importance of temperature regulation within the body. 3. Outline the
EXCRETION IN HUMANS 31 JULY 2013
 EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
What is excretion? Excretion is the removal of metabolic waste from the body.
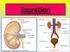 Excretion What is excretion? Excretion is the removal of metabolic waste from the body. Excretion in Plants Plants produce very little waste products. Plants lose oxygen and water vapour through the stomata.
Excretion What is excretion? Excretion is the removal of metabolic waste from the body. Excretion in Plants Plants produce very little waste products. Plants lose oxygen and water vapour through the stomata.
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Osmoregulation and the Excretory System
 Honors Biology Study Guide Chapter 25.4 25.10 Name Osmoregulation and the Excretory System FUNCTIONS OF THE EXCRETORY SYSTEM OSMOREGULATION Freshwater: Marine: Land Animals: Sources of Nitrogenous Wastes?
Honors Biology Study Guide Chapter 25.4 25.10 Name Osmoregulation and the Excretory System FUNCTIONS OF THE EXCRETORY SYSTEM OSMOREGULATION Freshwater: Marine: Land Animals: Sources of Nitrogenous Wastes?
Fifth Year Biology. Excretion. Miss Rochford
 Fifth Year Biology Excretion Miss Rochford In this Topic Excretion in plants Excretion and homeostasis Skin Organs of excretion Urinary system Kidneys Nephron Control of urine volume Characteristics of
Fifth Year Biology Excretion Miss Rochford In this Topic Excretion in plants Excretion and homeostasis Skin Organs of excretion Urinary system Kidneys Nephron Control of urine volume Characteristics of
Mathematics Meets Oncology
 .. Mathematics Meets Oncology Mathematical Oncology Philippe B. Laval Kennesaw State University November 12, 2011 Philippe B. Laval (Kennesaw State University)Mathematics Meets Oncology November 12, 2011
.. Mathematics Meets Oncology Mathematical Oncology Philippe B. Laval Kennesaw State University November 12, 2011 Philippe B. Laval (Kennesaw State University)Mathematics Meets Oncology November 12, 2011
Bio 322 Human Anatomy Objectives for the laboratory exercise Urinary System Filtration Reabsorption Secretion Concentration
 Bio 322 Human Anatomy Objectives for the laboratory exercise Urinary System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 25 For this lab you will use parts
Bio 322 Human Anatomy Objectives for the laboratory exercise Urinary System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 25 For this lab you will use parts
The Urinary System. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Plasma cell myeloma (multiple myeloma)
 Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Quantitative protein estimation of Urine
 Quantitative protein estimation of Urine 1 In a healthy renal and urinary tract system, the urine contains no protein or only trace amounts. The presence of increased amounts of protein in the urine can
Quantitative protein estimation of Urine 1 In a healthy renal and urinary tract system, the urine contains no protein or only trace amounts. The presence of increased amounts of protein in the urine can
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
EXCRETORY SYSTEM E. F. G. H.
 XRTORY SYSTM 1. Label the following parts of the nephron in the diagram below:..... F. G. H. I. J. K. L. 2. Identify the following as either True or False: There is a greater osmotic concentration in the
XRTORY SYSTM 1. Label the following parts of the nephron in the diagram below:..... F. G. H. I. J. K. L. 2. Identify the following as either True or False: There is a greater osmotic concentration in the
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
1. The Fibrous Capsule covers the outside of the kidney. It is made of fat and fibers.
 Slide 2 The kidney has a number of functions. First is the excretion of toxic metabolic waste through urine production. The kidneys filter blood plasma and as a result of filtering blood, the kidneys help
Slide 2 The kidney has a number of functions. First is the excretion of toxic metabolic waste through urine production. The kidneys filter blood plasma and as a result of filtering blood, the kidneys help
Question Answer Mark Guidance 1 (a) 93 (to nearest whole number) / 93.4 (to 3 sig figs) ; per million (people) / million -1 ;
 Question Answer Mark Guidance 1 (a) 93 (to nearest whole number) / 93.4 (to 3 sig figs) ; per million (people) / million -1 ; Crect answer with crect units = 2 marks Crect answer with no/increct units
Question Answer Mark Guidance 1 (a) 93 (to nearest whole number) / 93.4 (to 3 sig figs) ; per million (people) / million -1 ; Crect answer with crect units = 2 marks Crect answer with no/increct units
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
The UK Renal Registry collects national data about the causes and treatment of kidney failure.
 1 Kidney failure is a serious condition. Many kidney patients receive some form of renal replacement therapy (RRT) such as dialysis. The UK Renal Registry collects national data about the causes and treatment
1 Kidney failure is a serious condition. Many kidney patients receive some form of renal replacement therapy (RRT) such as dialysis. The UK Renal Registry collects national data about the causes and treatment
The kidneys are excretory and regulatory organs. By
 exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Renal System Physiology
 M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
Renal Functions: Renal Functions: Renal Function: Produce Urine
 Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
The Excretory System. Biology 20
 The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
Urinary system. Lab-7
 Urinary system Lab-7 Excretion: processes that remove wastes and excess materials from the body Urinary system (kidneys): excretes nitrogenous wastes, excess solutes, and water The Kidneys Regulate Water
Urinary system Lab-7 Excretion: processes that remove wastes and excess materials from the body Urinary system (kidneys): excretes nitrogenous wastes, excess solutes, and water The Kidneys Regulate Water
Interesting case seminar: Native kidneys Case Report:
 Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
WJEC. BY4 Kidney Questions
 NAME: OPTION GROUP WJEC BY4 Kidney Questions Question Book 2 (Legacy Qs from Jan 2000 to June 2014) Question Number(s) Due Date & Pass Mark Homework Mark Resist Question number(s) Resist Due Date & Pass
NAME: OPTION GROUP WJEC BY4 Kidney Questions Question Book 2 (Legacy Qs from Jan 2000 to June 2014) Question Number(s) Due Date & Pass Mark Homework Mark Resist Question number(s) Resist Due Date & Pass
Biology Slide 1 of 36
 Biology 1 of 36 38 3 The Excretory System 2 of 36 Functions of the Excretory System 1.Function: process which eliminates metabolic wastes 3 of 36 Functions of the Excretory System (The skin excretes excess
Biology 1 of 36 38 3 The Excretory System 2 of 36 Functions of the Excretory System 1.Function: process which eliminates metabolic wastes 3 of 36 Functions of the Excretory System (The skin excretes excess
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX
 One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Lesson 14.1: Learning the Key Terms
 209 Lesson 14.1: Learning the Key Terms Directions: Place the letter of the best definition next to each key term. 1. collecting duct 2. distal convoluted tubule 3. glomerulus 4. nephron 5. nephron loop
209 Lesson 14.1: Learning the Key Terms Directions: Place the letter of the best definition next to each key term. 1. collecting duct 2. distal convoluted tubule 3. glomerulus 4. nephron 5. nephron loop
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Chapter 6: Skeletal System: Bones and Bone Tissue
 Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
28/04/2013 LEARNING OUTCOME C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS STUDENT ACHIEVEMENT INDICATORS URINARY SYSTEM & EXCRETION
 LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
