Thrombotic occlusions of the cerebral veins and sinuses occur
|
|
|
- Bryan Davis
- 5 years ago
- Views:
Transcription
1 Published February 12, 2009 as /ajnr.A1451 ORIGINAL RESEARCH J. Linn T. Pfefferkorn K. Ivanicova S. Müller-Schunk S. Hartz M. Wiesmann M. Dichgans H. Brückmann Noncontrast CT in Deep Cerebral Venous Thrombosis and Sinus Thrombosis: Comparison of its Diagnostic Value for Both Entities BACKGROUND AND PURPOSE: With its highly variable clinical presentation, the diagnosis of cerebral venous sinus thrombosis (SVT), and especially of deep venous thrombosis (DVT), as rare but important causes of stroke is challenging. Because noncontrast cranial CT (NCCT) is still the imaging technique of choice in most emergency departments, we aimed to investigate its value in the diagnosis of SVT and DVT. MATERIALS AND METHODS: Screening our patient data base, we identified 8 patients with DVT and 25 patients with SVT. We also included a control group of 36 patients who had presented with clinical signs of DVT or SVT but in whom thrombosis was subsequently excluded. MR imaging, multidetector row CT angiography (MDCTA), and/or digital subtraction angiography (DSA) were used as the reference standard. Three independent readers assessed the NCCTs for the presence of direct and indirect signs of DVT or SVT. Direct signs included the presence of hyperattenuated sinuses (ie, cord sign) or veins (ie, attenuated vein sign), whereas parenchymal edema and hemorrhage were indirect signs. RESULTS: The sensitivity and specificity of the attenuated vein sign for the diagnosis of DVT were 100%, and 99.4%, respectively, whereas the sensitivity and specificity of the cord sign for SVT were 64.6% and 97.2%, respectively. The sensitivity and specificity values of NCCT were 93.7% and 98% for intracerebral edema and 94.8% and 98.7% for intracerebral hemorrhages, respectively. CONCLUSIONS: Although NCCT is insufficient to exclude a SVT, its value in the emergency diagnosis of DVT seems to be very high. Received July 23, 2008; accepted after revision November 11. From the Departments of Neuroradiology (J.L., K.I., S.M.-S., S.H., M.W., H.B.) and Neurology (T.P., M.D.), University Hospital Munich, Munich, Germany. Previously presented in part at: 93rd Annual Assembly and Scientific Meeting of the Radiological Society of North America, November 30, 2007, Chicago, Ill. Please address correspondence to Jennifer Linn, MD, Department of Neuroradiology, University Hospital Munich, Marchioninistr 15, D Munich, Germany; linn@nrad.de DOI /ajnr.A1451 Thrombotic occlusions of the cerebral veins and sinuses occur with an estimated annual incidence of 3 to 4 cases per million adults. 1 They account for approximately 1% to 2% of all strokes in adults 2 and affect all age groups. The clinical signs are highly variable with headaches, seizures, focal neurologic deficits, and an impaired level of consciousness representing the most common symptoms. 3-5 Besides the patient s age, 6,7 the presence of parenchymal involvement, the interval from symptom to diagnosis, 8 and the site and extent of the thrombosis are important in the clinical presentation of thrombosis. 5,9,10 The deep cerebral veins (ie, the internal cerebral veins [ICVs], the basal veins of Rosenthal [BVR] and their tributaries) are involved in approximately 10% of patients. 11,12 Deep venous thrombosis (DVT) may result in unilateral or, more typically, bilateral venous congestion and venous infarction of the thalami and basal ganglia. 13 Involvement of the deep veins has been shown to be a risk factor for death and long-term sequelae. 11,12,14,15 During the past decade, greater awareness of the disease, improved neuroimaging techniques, and more effective treatment have improved the outcome, especially in sinus thrombosis (SVT). During the past decade, MR imaging has replaced digital subtraction angiography (DSA) in the imaging diagnosis of thrombosis of cerebral veins and sinuses. 1,10,16-18 More recently, several studies also proved a comparably high diagnostic value of multidetector row CT angiography (MDCTA) for the diagnosis of sinus thrombosis However, because of the wide clinical spectrum and often subacute or lingering onset, 13,16 the average delay from symptom onset to diagnosis is still 7 days, 1,11,16 if DVT or SVT are not suspected on the basis of the clinical presentation. Yet rapid diagnosis is essential, especially in patients with DVT, because these patients can deteriorate rapidly to coma 14,17 with a potentially fatal outcome. 14,23 As it is fast and widely available, noncontrast cranial CT (NCCT) is still often performed as a first-line investigation in the emergency setting in most institutions. With regard to SVT, direct and indirect signs have been described on NCCT. The cord sign a direct sign of SVT is defined as a homogeneous, hyperattenuated appearance of thrombosed venous sinuses on NCCT scans, and it is caused by the increased attenuation of the thrombotic material in the affected vessels It reflects a newly formed thrombus and is best seen within the first week of the disease. After 7 to 14 days, the thrombus becomes isoattenuated and then hypoattenuated. 25 Indirect signs of SVT include intracerebral hemorrhage and edema. 26 The same direct and indirect CT signs have been described for DVT; the hyperattenuated appearance of the affected veins often being named the attenuated vein sign. 10,13,26,27 Former studies found the sensitivity and specificity of the cord sign for SVT to be rather low. 17,24 To our knowledge, there are neither recent studies on this issue, which had been performed by using modern multidetector row CT scanners in patients with SVT, nor any systematic studies on the diagnostic value of the attenuated vein sign in DVT. Therefore, the aim of this study was to assess the sensitivity and specificity of BRAIN ORIGINAL RESEARCH AJNR Am J Neuroradiol : Copyright 2009 by American Society of Neuroradiology.
2 Table 1: Characteristics of patients with DVT Patient No. Age/ Sex Diagnosis Available Imaging Affected Venous Structures Parenchymal Changes Diagnostic Delay (d)# 1 39/f IDVT NCCT, MRI, MRA RICV, SS Edema right thalamus, caudate nucleus, putamen /f IDVT NCCT, CTA, MRI, MRA LTSV, both ICV, both BVR, VG, SS Edema thalami, caudate nuclei, putamen, 14 bilaterally 3 47/f IDVT NCCT, CTA, MRI, MRA, both ICV, VG, SS Hemorrhage left thalamus, edema both thalami 21 DSA 4 49/m IDVT NCCT, MRI, MRA, DSA LTSV, both ICV, both BVR, VG, SS Edema both thalami /f CDVT NCCT, CTA, MRI, MRA, Both TSV, both ICV, both BVR, VG, Edema both thalami, left caudate nucleus, 1 DSA SS, LTS putamen, bilaterally 6 27/m IDVT NCCT, CTA, MRI, MRA LTSV, both ICV, LBVR, VG, SS Edema both thalami, posterior part of left 28 hippocampus 7 41/f CDVT NCCT, CTA, MRI, MRA Both ICV, RBVR, VG, SS, RTS None /f CDVT NCCT, CTA, MRI, MRA Both ICV, RBVR, VG, SS, LTS, LSS SSS Edema both thalami, left parietal lobe, left occipital lobe, hemorrhage both thalami 6 Note: DVT indicates deep cerebral venous thrombosis; f, female; m, male; IDVT, isolated deep venous thrombosis; CDVT, combined deep venous thrombosis; NCCT, noncontrast cranial CT; CTA, CT angiography; MRI, MR imaging; MRA, MR angiography; DSA, digital subtraction angiography; ICV, internal cerebral veins; RICV, right internal cerebral vein; SS, straight sinus; TSV, thalamostriate vein; LTSV, left thalamostriate vein; BVR, basal veins of Rosenthal; LBVR, left basal vein of Rosenthal; RBVR, right basal vein of Rosenthal; VG, great vein of Galen; diagnostic delay #, time between onset of initial symptoms and definite diagnosis of DVT; LTS, left transverse sinus; RTS, right transverse sinus; LSS, left sigmoid sinus; SSS, superor sagittal sinus. NCCT in the diagnosis of DVT and to compare it with its value in the diagnosis of SVT. Materials and Methods Our institutional review board approved this study, and we performed our study in accordance with the Declaration of Helsinki. Definitions Here, we defined SVT as a thrombosis of the venous sinuses with or without involvement of cortical veins, but without involvement of the straight sinus (SS) or the deep cerebral veins (ie, ICVs, great vein of Galen [VG], BVR, and thalamostriate veins [TSV]). On the contrary, DVT was defined as a thrombotic occlusion of the above-mentioned deep cerebral veins, either isolated (IDVT; ie, without an involvement of the sagittal, transverse, or sigmoid sinus or cortical veins) or combined (CDVT; ie, with involvement of venous sinuses or cortical veins). Note that the SS was classified as belonging to the deep cerebral venous system. Subjects We used our electronic in-hospital data base of clinical records to search for the key words deep, venous, sinus, cerebral, and thrombosis to identify all patients with DVT or SVT who were admitted to our institution between 2002 and Patients had to meet the following inclusion criteria: 1. NCCT performed on admission. 2. Availability of at least 1 of the following additional imaging modalities: 1) MR imaging including a T2*-weighted sequence and a venous MR angiography (vmra) or 2) MDCTA. The presence of an isolated thrombosis of cortical veins without sinus involvement was an exclusion criterion. Eight patients with DVT (5 with IDVT, 3 with CDVT; 6 women; mean age, 38.9 years; age range, years; Table 1) and 25 patients with SVT (18 women; mean age, 43.5 years; age range, years; Table 2) matched the criteria and were included. Data on the clinical presentation of 3 of the patients with DVT have been previously published, 28 but imaging data have not been reported in a similar fashion. In addition, we included 36 consecutive patients (22 women; mean age, 41.2 years; age range, years) who initially presented with clinical symptoms of DVT or SVT and who had undergone an NCCT but in which all other imaging modalities showed no pathologic findings and clinical follow-up was uneventful (control group). The patients from the control group also had to meet the abovementioned inclusion criteria. Available Imaging NCCT had been performed in all patients included in the study (n 69). MR imaging including vmra and a T2*-weighted sequence was available in all patients with DVT, in 23 patients with SVT, and in 18 patients of the control group. MDCTA had been performed in 6 patients with DVT, 19 patients with SVT, and 26 patients from the control group. In addition, DSA was available in 4 patients with DVT, 7 patients with SVT, and 5 patients from the control group (Tables 1 3). Imaging Parameters All examinations had been performed under the following clinical routine conditions: NCCT and MDCTA were conducted on a 4-detector row CT (Aquilion; Toshiba, Neuss, Germany). NCCTs were performed with 120 kv, 300 mas, a collimation of 2.5 mm, a section width of 5 mm, and a reconstruction increment of 5 mm. For the MDCTA, the following parameters were used: 120 kv, 120 to 140 mas; collimation, mm; 120-mL contrast agent with an iodine concentration of 300 mg/ ml; injection rate, 5 ml/s, and delay, 35 s. MR imaging was performed on 1.5T scanners (Magnetom Vision or Symphony; Siemens, Erlangen, Germany). The following sequences were available: 1) DWI-sequence with b-values of 0 and 1000, and 3 gradient directions (TR, 4200 ms; TE, 139 ms; section thickness, 5 mm; FOV, 210 mm; matrix size, 128; gap spacing, 30%; 2 signal intensity averages, 23 sections); 2) proton attenuation- and T2- weighted SE-sequence, acquired as a dual-echo acquisition (TR, 2210 ms; TE, 85/14 ms; section thickness, 6 mm; FOV, 210 mm; matrix size, 256; gap spacing, 30%; 1 signal intensity average, 23 sections); 3) T1-weighted SE-sequence (TR, 665 ms; TE, 14 ms; section thickness, 6 mm; FOV, 210 mm; matrix size, 256; gap spacing, 30%; 1 signal intensity average, 23 sections); 4) T2*-weighted gradient-echo sequence (TR, 1000 ms; TE, 22 ms; section thickness, 5 mm; FOV, 210 mm; matrix size, 256; gap spacing, 30%; 1 signal intensity average, 19 sections); 5) fluid-attenuated inversion recovery (FLAIR) sequence 2 Linn AJNR
3 Table 2: Characteristics of patients with SVT Patient No. Age/Sex Available Imaging Affected Sinuses Parenchymal Changes Diagnostic Delay (d)# 1 37/f NCCT, CTA, MRI, MRA SSS, LTS, LSS None /f NCCT, CTA SSS, RTS None /f NCCT, CTA, MRI, MRA SSS None /f NCCT, MRI, MRA, DSA SSS, LTS, LSS None /f NCCT, CTA, MRI, MRA SSS, RTS None /m NCCT, CTA, MRI, MRA SSS, RTS Edema and hemorrhage, right occipital lobe /f NCCT, CTA, MRI, MRA SSS, RSS, CV Edema and hemorrhage, right frontal lobe /f NCCT, CTA, MRI, MRA LTS Edema, left frontal lobe /f NCCT, MRI, MRA, DSA SSS, LTS, LSS, CV Edema and hemorrhage, right parietal lobe /m NCCT, CTA, MRI, MRA, DSA SSS, RTS Edema and hemorrhage, right parietal lobe /f NCCT, CTA, MRI, MRA LTS, LSS, RSS Edema, left parietal and temporal lobes /f NCCT, CTA, MRI, MRA, DSA SSS, LTS, LSS Edema and hemorrhage, left occipital lobe /f NCCT, MRI, MRA, DSA SSS, RTS, RSS None /m NCCT, CTA, MRI, MRA LTS, RTS None /f NCCT, CTA, MRI, MRA SSS, RTS, CV Edema and hemorrhage, left frontal and occipital 0 lobes 16 64/f NCCT, CTA SSS, LTS, LSS Edema, left parietal lobe /f NCCT, CTA, MRI, MRA LTS, LSS None /m NCCT, MRI, MRA, DSA SSS, LTS, LSS Edema and hemorrhage, right parietal lobe /m NCCT, MRI, MRA SSS, LTS, LSS Edema, left frontal lobe /f NCCT, CTA, MRI, MRA LSS None /f NCCT, CTA, MRI, MRA SSS, LTS, CV None /m NCCT, CTA, MRI, MRA LTS, LSS None /f NCCT, CTA, MRI, MRA LTS, LSS Edema and hemorrhage, left occipital lobe /f NCCT, CTA, MRI, MRA SSS Edema and hemorrhage, right frontal lobe /m NCCT, MRI, MRA, DSA SSS, LTS, LSS Edema and hemorrhage, right frontal lobe 0 Note: SVT indicates sinus thrombosis; RSS, right sigmoid sinus; CV, cortical veins. Table 3: Available imaging modalities* Patient Group Total MRI, DSA, MDCTA MRI, DSA MRI, MDCTA MRI alone MDCTA alone DVT 8 (100) 2 (25) 1 (12.5) 4 (50) 1 (12.5) 0 (0) SVT 25 (100) 2 (8) 5 (20) 15 (60) 1 (4) 2 (8) Control 36 (100) 0 (0) 5 (13.9) 9 (25) 5 (13.9) 17 (47.2) Total 69 (100) 4 (5.8) 11 (15.9) 28 (40.6) 7 (10.1) 19 (27.5) Note: MRI indicates magnetic resonance imaging including venous MR angiography and T2*-weighted images; DSA, digital subtraction angiography; MDCTA, multi-detector row CT angiography; DVT, deep venous thrombosis; SVT, sinus thrombosis. * Data are given as numbers (percentages). (TR, 7500 ms; TE, 74 ms; TI, 2500 ms; section thickness, 5 mm; FOV, 220 mm; matrix size, 256; gap spacing, 30%; 1 signal intensity average, 19 sections); and 6) venous 2D-time of flight MR angiography with arterial saturation pulses (TR, 24 ms; TE, 5.6 ms; flip angle, 50 ; section thickness, 3 mm; FOV, 210 mm; matrix size, 256; gap spacing, 10%; 1 signal intensity average, 50 sections). DSA was performed on a biplanar DSA unit (Neurostar; Siemens) including selective catheterizations of both internal carotid arteries and the dominant vertebral artery, late venous phases, and oblique projections to better analyze the venous and sinus structures. Image Interpretation In total, 69 NCCT scans were analyzed independently by 3 experienced neuroradiologists, who were blinded to the clinical data and patient identification information. Image interpretation was performed on a standard PACS workstation. Reading orders were randomized, and standardized evaluation forms were used. The readers evaluated the NCCTs for the presence or absence of hyperattenuated sinuses (ie, cord sign) or cerebral veins (ie, attenuated vein sign). The following venous structures were evaluated in the listed sequence: superior sagittal sinus (SSS), inferior sagittal sinus (ISS), right and left transverse sinuses (RTS and LTS), right and left sigmoid sinuses, SS, right and left ICVs, VG, right and left BVR, and right and left TSVs. If readers classified a sinus or vein as hyperattenuated, they documented the mean attenuation of the respective venous structure in Hounsfield units (HU). The HU of veins or sinuses that were not classified as hyperattenuated were not noted because these venous structures could not, in all cases, be reliably differentiated from surrounding brain parenchyma on NCCT. Readers had to decide whether they interpreted the presence of a hyperattenuated vein or sinus as indicative of an SVT or a DVT. Whenever a thrombosis was suspected, the involved venous structures and the presence of intracerebral edema or hemorrhage were noted. The diagnostic confidence regarding the presence or absence of a DVT or SVT was rated on a 5-point scale (1, absolutely certain; 2, very certain; 3, certain; 4, not very certain; 5, uncertain). After having evaluated all NCCT datasets, readers performed a consensus reading to obtain a reference standard. They collaboratively reviewed all available imaging modalities including follow-ups of any respective patient. Furthermore, readers studied the clinical records to take the clinical and outcome information into account. They subsequently determined, in consensus, 1) the overall presence of a DVT or a SVT; 2) if applicable, the extent of the respective thrombosis, (ie, the involvement of the individual veins and sinuses); 3) the presence of an intracerebral AJNR Am J Neuroradiol :
4 Table 4: Results of the readings veins Venous Blinded Readings Consensus Reading Structure Dense Vein Sign tp fp tn fn Intraobserver Agreement ( values) Sensitivity (95% CI)* Specificity (95% CI)* SS ( ) 99.5 ( ) LICV ( ) 99.5 ( ) RICV ( ) 99.5 ( ) VG ( ) 99.5 ( ) LBVR ( ) 100 (99 100) RBVR ( ) 100 ( ) LTSV (83 100) 99.5 ( ) RTSV ( ) 98 ( ) Total ( ) 99.4 ( ) Note: tp indicates true-positive; fp, false-positive; tn, true-negative; fn, false-negative; 95% CI, 95% confidence interval; LICV, left internal cerebral vein; RTSV, right thalamostriate vein. * Data are given in percentages. edema; or 4) intracerebral hemorrhage or hemorrhagic transformation of a venous infarction. If there were any discrepant findings between the different modalities, the reference standard was based on the results of the T2*-weighted images and the source images of the vmra, if applicable. 18 In cases in which no MR imaging was available, this evaluation was done on the basis of MDCTA. 19,20 Whenever DSA was available, it was additionally evaluated. With regard to intracerebral edema and hemorrhage, proton attenuation/t2-weighted, FLAIR (for edema), and T2*-weighted images (for hemorrhage) were given precedence if available. In the remaining cases in which only NCCT and MDCTA had been performed, follow-up NCCTs were available and were reviewed together with the initial NCCT during the consensus reading to determine whether edema or hemorrhage was present. Statistical Analysis All available data were entered into a data base and were analyzed with standard software (Excel and Access; Microsoft, Redmond, Wash). Sensitivity and specificity parameters of the attenuated vein sign and the cord sign for the diagnosis of DVT and SVT, respectively, as well as their respective 95% confidence intervals, were calculated. To determine the interobserver agreement regarding the presence of hyperattenuated veins and sinuses, multirater values were calculated as described in the literature. 29 The values can range from 1.0 to 1.0, with 1.0 indicating perfect disagreement below chance, 0.0 indicating agreement equal to chance, and 1.0 indicating perfect agreement above chance. 29 We calculated and compared the mean attenuation values (HU) of the hyperattenuated sinuses and the hyperattenuated veins using the Student t test. We assessed hematocrit values via the clinical records and performed comparisons between the mean values of the following different patient subgroups using the Student t test: all men (n 23), all women (n 46), men with DVT (n 2), men with SVT (n 7), male control subjects (n 14), men with cord sign (n 14), men with attenuated vein sign (n 2), men without hyperattenuated veins or sinuses (n 7), women with DVT (n 6), women with SVT (n 18), female control subjects (n 22), women with cord sign (n 25), women with attenuated vein sign (n 7), and women without hyperattenuated veins or sinuses (n 14). Results Clinical Data The most common clinical symptoms in patients with DVT were headache (n 7), confusion (n 3), reduction of vigilance (n 3), paresis of variable degree (n 2), and loss of consciousness (n 2). D-dimer values were elevated ( 0.5 ng/ml) in 6 patients (mean, 6.4 ng/ml; range, ng/ ml) and were within normal limits ( 0.5 ng/ml) in 2. The mean interval (ie, diagnostic delay) from initial symptom onset to the definite diagnosis of DVT was 10.9 days in the patients with DVT (Table 1). Regarding the mean hematocrit values, there were no significant differences between the different patient subgroups. The P values ranged from ( all men vs all women ) to 1 ( men with cord sign vs men without hyperattenuated veins or sinuses ). Imaging In total, 207 readings were performed, and 2898 venous structures (ie, 1242 sinuses and 1656 veins) were evaluated by each reader, resulting in a total of 8694 single assessments. A cord sign was found in 116 sinuses and an attenuated vein sign in 138 veins. The results of the consensus reading regarding the patients with DVT are detailed in Table 4. In detail, the readers noted the venous sinuses and the deep cerebral veins as hyperattenuated in the following percentages of cases: the SSS in 21.7%, the ISS in 3.9%, the TS in 9.7% and 8.7% (right and left side, respectively), the sigmoid sinuses in 5.3% and 6.8% (right and left side, respectively), the VG in 11.6%, the BVR in 6.8% and 5.3% (right and left side, respectively), both ICVs in 11.6%, and the TSV in 4.3% and 6.3% (right and left side, respectively; Tables 4 and 5). The mean attenuation of the hyperattenuated sinuses and veins was measured as HU and HU, respectively. A DVT was diagnosed by the readers in 13.5% (28/207 readings; Fig 1) and a SVT in 27.1% of patients (56/207 readings; Fig 2). There was 1 false-positive diagnosis of a CDVT in a 20-year-old male patient with SVT of the SSS. In contrast, there were 28 false-negative and 5 false-positive diagnoses of SVT (Fig 2). Thus, the sensitivity of the attenuated vein sign for the presence of DVT (isolated or combined) was 100%, whereas its specificity was 99.4%. In contrast, the sensitivity and specificity of the cord sign for the diagnosis of SVT (without involvement of the deep cerebral veins) were 64.6% and 97.2%, respectively. Tables 4 and 5 summarize the results of the readers evaluation regarding the extent of the DVT or SVT (ie, regarding the veins and sinuses involved, including false-positive and false-negative results). Concerning the individual venous structures, the attenuated vein sign showed a sensitivity and specificity of 93.5% and 99.4%, respectively, for correct detec- 4 Linn AJNR
5 Table 5: Results of the readings sinus Blinded Reading Consensus Reading Sinus Cord Sign tp fp tn fn Interobserver Agreement ( values) Sensitivity (95% CI)* Specificity (95% CI)* SSS ( ) 93.9 ( ) ISS (0 53.3) 96.1 ( ) LTS ( ) 95.4 ( ) RTS ( ) 93.4 ( ) LSS ( ) 95.9 ( ) RSS (2 39.1) 94.9 ( ) Total ( ) 95 ( ) Note: ISS indicates inferior sagittal sinus. * Data are given in percentages. Fig 1. Patient 5. A 31-year-old woman with combined deep cerebral venous thrombosis of the TSV, the ICVs, the BVR, the VG, the SS, and the LTS. A, The NCCT scan demonstrates an attenuated vein sign in both ICVs (thin arrows), in the SS (crossed arrow) as well as bilateral edema in the thalami and in the putamen (thick arrows). B, Multiplanar sagittal reconstruction of an MDCTA. The thrombosis is visualized indirectly by demonstration of contrast-filling defects in the ICVs (thin arrow) and the SS (crossed arrows). C, An axial proton-attenuationweighted MR image (acquired as a dual-echo acquisition) also depicts the bilateral edema in the thalamus and the putamen as well as edema in the left caudate nucleus as hyperintense areas (dotted arrows). D, Diffusion-weighted image (b-value 1000) and the apparent diffusion coefficient map (E) show a restriction of diffusion in the respective areas (dotted arrows). tion of the individually affected deep cerebral veins, whereas the cord sign showed sensitivity and specificity values of 33.9% and 95%, respectively, for the sinuses. The 95% confidence intervals of both patient groups did not overlap (Tables 4 and 5). NCCT detected intracerebral edema with a sensitivity of 93.7% and a specificity of 98%, respectively, and hemorrhage or hemorrhagic transformations with a sensitivity and specificity of 94.8% and 98.7%, respectively. The mean diagnostic confidence regarding the presence or absence of a DVT was rated as 1.1 (ie, absolutely certain), whereas it was 3.7 (ie, not very certain) for SVT. The interobserver agreement for the AJNR Am J Neuroradiol :
6 Fig 2. Examples for true-positive, false-positive, and false-negative cord signs in the evaluation of sinus thrombosis. A, A 35-year-old woman with an SVT of the SSS and the RTS, who presented with headache and nausea. The NCCT scan shows a true-positive cord sign in the SSS (dotted arrow) and the RTS (arrows). The case of this patient was judged as positive with regard to the presence of a cord sign by all 3 readers. B, A 27-year-old woman in the control group, who initially presented with headache, but all other available imaging modalities showed no pathologic findings and clinical follow-up was uneventful. The RTS appeared hyperattenuated on NCCT (arrows). This finding was interpreted as a cord sign by all readers, resulting in the false-positive diagnosis of a SVT in this patient. C and D, A 45-year old woman with headache and nausea and a SVT involving the RTS and the SSS. The NCCT scan (C) shows no hyperattenuated signal intensity (ie, no cord sign) in the RTS or the SSS: The case of this patient was judged as false-negative regarding the presence of a cord sign by all readers. D, Multiplanar sagittal reconstruction of a MDCTA demonstrates contrast-filling defects in the RTS (arrow) and in the SSS (dotted arrow), indicating an SVT. presence of an attenuated vein sign was ( range for individual veins, ; Table 4) and 0.80 for the cord sign ( range for individual sinuses, ; Table 5). Discussion Because prompt therapy of cerebral venous thrombosis has a great impact on clinical outcome, early diagnosis is essential, especially in patients with involvement of the deep cerebral veins. 14,17 The diagnosis is still often made with considerable delay, which is also reflected by the mean interval from symptom onset to diagnosis in our patients with DVT. One of the main factors contributing to this delay is the marked variability of the clinical presentation. 13,14 In our series, no single symptom or sign was present in all of our patients with DVT. In addition, laboratory tests seem less useful in the diagnosis of DVT. Normal D-dimer levels have been shown to have a high negative predictive value in patients with suspected cerebral venous occlusive disease. 1 However, we found levels to be within normal limits in 2 of our 8 patients with DVT. This finding might be related to the relatively small thrombus volume in patients with IDVT. These results suggest that D-dimer is of limited value in the exclusion of DVT, further emphasizing the importance of imaging. During the past decade, DSA has been superseded by MR imaging and CTA in the imaging diagnosis of thrombosis of the cerebral veins and sinuses, which both have high diagnostic values for this disease. 1,10,17-22 Nevertheless, in most institutions, NCCT is still the first-line imaging method in the emergency department setting, especially in patients with unspecific neurologic symptoms. This is because of its wide availability and its short examination time with very limited demand on patient cooperation. 21 Using a blinded-reader approach and a control group of patients without any pathologic conditions of the cerebral venous system, we clearly demonstrated that the attenuated vein sign in DVT, as a direct NCCT sign, is much more sensitive and specific than the cord sign in SVT. Although the sensitivity of the cord sign for SVT in our study was slightly higher than previously reported in older studies (25% 56%), 24,26 it was, nevertheless, much too low (64.6%) to allow the use of NCCT in excluding an SVT. With regard to DVT, an attenuated vein sign has been described in several case reports, 13,30-33 but its diagnostic value has never been assessed systematically. Here, we demonstrated that NCCT is very helpful in the diagnosis of DVT, as the attenuated vein sign shows both a high sensitivity and a high specificity for DVT. The interobserver agreement for the presence of an attenuated vein sign was excellent for all veins, and it was good to excellent for the presence of a cord sign for all sinuses. Nevertheless, the diagnostic confidence for the diagnosis of DVT was higher than for SVT. In our study, NCCT in patients with DVT or SVT and in 6 Linn AJNR
7 patients from the control group had been performed under exactly the same conditions. This provides evidence that the observed value of NCCT in the diagnosis of DVT compared with SVT does not result from the improvement in NCCT imaging quality compared with older studies 24,26 but is rather the result of other factors. One possible reason for the different findings in DVT compared with SVT is that the deep cerebral veins are much less prone to partial volume effects compared with the venous sinuses. The sinuses are located in the immediate vicinity to the skull. Thus, partial volume effects can result in a false-positive cord sign. 34 Another potential pitfall might be that flowing venous blood can also appear mildly hyperattenuated, probably because of high hematocrit values. 25,35 This mechanism might have been the case in the 20- year-old patient with SVT in our study, who presented with a hematocrit level of 0.49 and in whom involvement of the deep cerebral veins was wrongly diagnosed by 1 of the readers. A possible explanation for false-negative hyperattenuated sinuses in SVT might be the less severe clinical presentation of an isolated thrombosis of 1 sinus (eg, the transverse sinus) compared with DVT. If imaging is not performed immediately after onset of symptoms but with a considerable delay because symptoms are unspecific and are less severe, the thrombus might already be isoattenuated, resulting in false-negative imaging findings. As the hematocrit values did not differ significantly between the patients with SVT, patients with DVT, and patients from the control group, they cannot account for the different findings in patients with DVT compared with those with SVT. On the basis of our findings, we hypothesize that the hyperattenuation of the thrombotic material found in patients with DVT might result in false-negative results on contrastenhanced CT studies (or even on CT angiography) because the hyperattenuated thrombus might mimic flow in thrombosed deep cerebral veins. Because systematic studies on this topic are not available to date, we strongly recommend the performance of an NCCT scan as the first step in every case of suspected venous thrombosis. Although parenchymal changes are seen more readily on MR imaging than on CT, 17,19,34 NCCTs showed high sensitivity and specificity values for the detection of intracerebral edema (93.7% and 98%, respectively) and hemorrhage (94.8% and 98.7%, respectively) as thrombosis sequelae. Some limitations of our study need to be taken into account. First, the presence of indirect signs (edema or hemorrhage) in most cases with DVT might bias the reader toward the diagnosis of DVT. Yet, even when these changes were subtle, or even absent, the attenuated vein sign was present. Second, MR imaging was not available in all patients; thus, the reference standard had to be obtained on the basis of MDCTA in 27.5% of patients (8% of patients with SVT and 47.2% of patients from the control group). Nevertheless, the sensitivity and specificity of this imaging technique for the diagnosis of SVT have been shown to be very high. 19,20 Third, we used a venous time-of-flight MR angiography instead of a contrast-enhanced MR angiography. Two drawbacks of the time-of-flight technique have to be considered: 1) a subacute, hyperintense thrombus could potentially simulate flow on time-offlight-mr angiography, 10 and 2) the lack of flow in a vessel might be caused by acute thrombosis, but it might also be because of hypoplasia or aplasia of the respective vessel. 17,24,36 Nevertheless, our protocol included a venous time-of-flight MR angiography, as this technique does not require the intravenous application of contrast agent, which constitutes a major advantage, especially in patients with impaired renal function. Furthermore, we took advantage of the other available imaging modalities and sequences, predominately the T2*- weighted images, as a reference standard, which have been shown to have a high sensitivity for the diagnosis of SVT. 18 In addition, the sample size of our study was relatively small. However, DVT is a rare disease, rendering the recruitment of large patient populations difficult. Because the 8 patients with DVT were assessed by a blinded, multiple-reader approach, this shortcoming may not necessarily limit the scope of our observations. Conclusions Our study revealed a high sensitivity and specificity of the attenuated vein sign for the diagnosis of DVT, which was not true for SVT. Thus, the value of NCCT in the emergency department diagnosis of DVT is very high compared with its value in patients with SVT. Our findings implicate the following consequences for patient management: 1. If an attenuated vein sign or a cord sign is present, the suspicion of a DVT or SVT should be high, and a venous CTA should be performed immediately to confirm the diagnosis. 2. The absence of an attenuated vein sign (and any hemorrhage or edema) makes a DVT very unlikely. 3. The absence of a cord sign does not exclude an SVT. Thus, venous CTA must be performed in addition to NCCT if SVT is suspected clinically. Acknowledgment We thank Mrs. V. Schop f for reviewing the statistics. References 1. Stam J. Current concepts: thrombosis of the cerebral veins and sinuses. N Engl J Med 2005;352: Bogousslavasky J, Pierre P. Ischaemic stroke in patients under age 45. Neurol Clin 1992;10: Ameri A, Bousser MG. Cerebral venous thrombosis. Neurol Clin 1992;10: Villringer A, Mehraen S, Einhäupl KM. Pathophysiological aspects of cerebral sinus venous thrombosis. J Neuroradiol 1994;21: Bousser MG, Chiras J, Bories J, et al. Cerebral venous thrombosis - a review of 38 cases. Stroke 1985;16: deveber G, Andrew M, Adams C, et al. The Canadian Pediatric Ischemic Stroke Study Group: cerebral sinovenous thrombosis in children. N Engl J Med 2001;345: Ferro JM, Canhão P, Bousser MG, et al. ISCVT Investigators: cerebral vein and dural sinus thrombosis in elderly patients. Stroke 2005;36: Ferro JM, Lopes MG, Rosas MJ, et al. VENOPORT Investigators: delay in hospital admission of patients with cerebral vein and dural sinus thrombosis. Cerebrovasc Dis 2005;19: Ferro JM, Canhão P. Acute treatment of cerebral venous and dural sinus thrombosis. Curr Treat Options Neurol 2008;10: Lafitte F, Boukobza M, Guichard JP, et al. MRI and MRA for diagnosis and follow-up of cerebral venous thrombosis (CVT). Clin Radiol 1997;52: Ferro JM, Canhão P, Stam J, et al. ISCVT Investigators: prognosis of cerebral vein and dural sinus thrombosis: results of the International Study on Cerebral Vein and Dural Sinus Thrombosis (ISCVT). Stroke 2004;35: Canhão P, Ferro JM, Lindgren AG, et al. ISCVT Investigators: causes and predictors of death in cerebral venous thrombosis. Stroke 2005;6: van den Bergh WM, van der Schaaf I, van Gijn J. The spectrum of presentations of venous infarction caused by deep cerebral vein thrombosis. Neurology 2005;65: AJNR Am J Neuroradiol :
8 14. Crawford SC, Digre KB, Palmer CA, et al. Thrombosis of the deep venous drainage of the brain in adults. Analysis of seven cases with review of the literature. Arch Neurol 1995;52: Girot M, Ferro JM, Canhão P, et al. ISCVT Investigators. Predictors of outcome in patients with cerebral venous thrombosis and intracerebral hemorrhage. Stroke 2007;38: Masuhr F, Mehraein S, Einhäupl K. Cerebral venous and sinus thrombosis. J Neurol 2004;251: Renowden S. Cerebral venous sinus thrombosis. Eur Radiol 2004;14: Idbaih A, Boukobza M, Crassard I, et al. MRI of clot in cerebral venous thrombosis: high diagnostic value of susceptibility-weighted images. Stroke 2006;37: Linn J, Ertl-Wagner B, Seelos KC, et al. Diagnostic value of multidetector-row CT angiography in the evaluation of thrombosis of the cerebral venous sinuses. AJNR Am J Neuroradiol 2007;28: Gaikwad AB, Mudalgi BA, Patankar KB, et al. Diagnostic role of 64-slice multidetector row CT scan and CT venogram in cases of cerebral venous thrombosis. Emerg Radiol 2008;15: Rodallec MH, Krainik A, Feydy A, et al. Cerebral venous thrombosis and multidetector CT angiography: tips and tricks. Radiographics 2006;26 Suppl 1:S Leach JL, Fortuna RB, Jones BV, et al. Imaging of cerebral venous thrombosis: current techniques, spectrum of findings, and diagnostic pitfalls. Radiographics 2006;26 Suppl 1:S Canu C, Barinagarrementeria F. Cerebral venous thrombosis associated with pregnancy and puerperium: a review of 67 cases. Stroke 1993;24: Teasdale E. Cerebral venous thrombosis: making the most of imaging. J R Soc Med 2000;93: Vijay RK. The cord sign. Radiology 2006;240: Virapongse C, Cazenave C, Quisling R, et al. The empty delta sign: frequency and significance in 76 cases of dural sinus thrombosis. Radiology 1987;162: Iwashita T, Kitazawa K, Koyama J, et al. Subtle computed tomography abnormalities in cerebral deep sinus thrombosis. J Clin Neurosci 2007;14: Bender A, Schulte-Altedorneburg G, Mayer T, et al. Outcome of severe cerebral venous and sinus thrombosis. J Neurol 2007;254: Randolph JJ. Free-marginal multirater kappa: an alternative to Fleiss fixedmarginal multirater kappa. Joensuu University Learning and Instruction Symposium, Joensuu, Finland, October 14 15, Keller E, Flacke S, Urbach H, et al. Diffusion- and perfusion-weighted magnetic resonance imaging in deep cerebral venous thrombosis. Stroke 1999;30: Nagi S, Kaddour C, Soukri I, et al. Deep cerebral venous system thrombosis: report of two cases. J Radiol 2006;87: Eick JJ, Miller KD, Bell KA, et al. Computed tomography of deep cerebral venous thrombosis in children. Radiology 1981;140: Nagatomo Y, Yanaka K, Kamezaki T, et al. Recovery from primary deep cerebral venous sinus thrombosis with recanalisation. Neuroradiology 1995;37: Padayachee TS, Bingham JB, Graves MJ. Dural sinus thrombosis. Diagnosis and follow up by magnetic resonance, angiography and imaging. Neuroradiology 1991;33: Provenzale JM, Joseph GJ, Barboriak DP. Dural sinus thrombosis: findings on CT and MR imaging and diagnostic pitfalls. AJR Am J Roentgenol 1998;170: Ayanzen RH, Bird CR, Keller PJ, et al. Cerebral MR venography: normal anatomy and potential diagnostic pitfalls. AJNR Am J Neuroradiol 2000;21: Linn AJNR
41 year old female with headache. Elena G. Violari MD and Leo Wolansky MD
 41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
Computed tomography in the evaluation of cerebral venous sinus thrombosis
 Computed tomography in the evaluation of cerebral venous sinus thrombosis Poster No.: C-0090 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. Avsenik, K. Surlan Popovic; Ljubljana/SI
Computed tomography in the evaluation of cerebral venous sinus thrombosis Poster No.: C-0090 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. Avsenik, K. Surlan Popovic; Ljubljana/SI
Normal Variations and Artifacts in MR Venography that may cause Pitfalls in the Diagnosis of Cerebral Venous Sinus Thrombosis.
 Normal Variations and Artifacts in MR Venography that may cause Pitfalls in the Diagnosis of Cerebral Venous Sinus Thrombosis. Poster No.: R-0005 Congress: 2015 ASM Type: Scientific Exhibit Authors: A.
Normal Variations and Artifacts in MR Venography that may cause Pitfalls in the Diagnosis of Cerebral Venous Sinus Thrombosis. Poster No.: R-0005 Congress: 2015 ASM Type: Scientific Exhibit Authors: A.
Magnetic Resonance Imaging. Basics of MRI in practice. Generation of MR signal. Generation of MR signal. Spin echo imaging. Generation of MR signal
 Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Transverse Dural Sinus Thrombosis Joseph Junewick, MD FACR
 Transverse Dural Sinus Thrombosis Joseph Junewick, MD FACR 03/19/2010 History Child with headache and otomastoiditis. Diagnosis Dural venous thrombosis secondary to mastoiditis Discussion The cerebral
Transverse Dural Sinus Thrombosis Joseph Junewick, MD FACR 03/19/2010 History Child with headache and otomastoiditis. Diagnosis Dural venous thrombosis secondary to mastoiditis Discussion The cerebral
Optimized phase contrast MRV technique outperforms timeof-flight in the diagnosis of cerebral venous thrombosis
 Optimized phase contrast MRV technique outperforms timeof-flight in the diagnosis of cerebral venous thrombosis Poster No.: C-3377 Congress: ECR 2010 Type: Topic: Authors: Keywords: DOI: Scientific Exhibit
Optimized phase contrast MRV technique outperforms timeof-flight in the diagnosis of cerebral venous thrombosis Poster No.: C-3377 Congress: ECR 2010 Type: Topic: Authors: Keywords: DOI: Scientific Exhibit
Methods. Yahya Paksoy, Bülent Oğuz Genç, and Emine Genç. AJNR Am J Neuroradiol 24: , August 2003
 AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
Cerebral MR Venography: Normal Anatomy and Potential Diagnostic Pitfalls
 AJNR Am J Neuroradiol 21:74 78, January 2000 Cerebral MR Venography: Normal Anatomy and Potential Diagnostic Pitfalls R. H. Ayanzen, C. R. Bird, P. J. Keller, F. J. McCully, M. R. Theobald, and J. E. Heiserman
AJNR Am J Neuroradiol 21:74 78, January 2000 Cerebral MR Venography: Normal Anatomy and Potential Diagnostic Pitfalls R. H. Ayanzen, C. R. Bird, P. J. Keller, F. J. McCully, M. R. Theobald, and J. E. Heiserman
Role of MRI in Evaluation of Cerebral Venous Thrombosis
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 6 Ver. 11 (June. 2018), PP 06-12 www.iosrjournals.org Role of MRI in Evaluation of Cerebral
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 6 Ver. 11 (June. 2018), PP 06-12 www.iosrjournals.org Role of MRI in Evaluation of Cerebral
Evaluation of the Effect of Hemoglobin or Hematocrit Level on Dural Sinus Density Using Unenhanced Computed Tomography
 Original Article http://dx.doi.org/1.3349/ymj.213.54.1.28 pissn: 513-5796, eissn: 1976-2437 Yonsei Med J 54(1):28-33, 213 Evaluation of the Effect of Hemoglobin or Hematocrit Level on Dural Sinus Density
Original Article http://dx.doi.org/1.3349/ymj.213.54.1.28 pissn: 513-5796, eissn: 1976-2437 Yonsei Med J 54(1):28-33, 213 Evaluation of the Effect of Hemoglobin or Hematocrit Level on Dural Sinus Density
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
The Role of Multidetector CT Venography in Diagnosis of Cerebral Venous Sinus Thrombosis
 Research Journal of Medicine and Medical Sciences, 4(2): 284-289, 2009 2009, INSInet Publication The Role of Multidetector CT Venography in Diagnosis of Cerebral Venous Sinus Thrombosis 1 Mohamed Abdel
Research Journal of Medicine and Medical Sciences, 4(2): 284-289, 2009 2009, INSInet Publication The Role of Multidetector CT Venography in Diagnosis of Cerebral Venous Sinus Thrombosis 1 Mohamed Abdel
Diagnostic improvement from average image in acute ischemic stroke
 Diagnostic improvement from average image in acute ischemic stroke N. Magne (1), E.Tollard (1), O. Ozkul- Wermester (2), V. Macaigne (1), J.-N. Dacher (1), E. Gerardin (1) (1) Department of Radiology,
Diagnostic improvement from average image in acute ischemic stroke N. Magne (1), E.Tollard (1), O. Ozkul- Wermester (2), V. Macaigne (1), J.-N. Dacher (1), E. Gerardin (1) (1) Department of Radiology,
Cortical vein thrombosis in adult patients of cerebral venous sinus thrombosis correlates with poor outcome and brain lesions: a retrospective study
 Liang et al. BMC Neurology (2017) 17:219 DOI 10.1186/s12883-017-0995-y RESEARCH ARTICLE Open Access Cortical vein thrombosis in adult patients of cerebral venous sinus thrombosis correlates with poor outcome
Liang et al. BMC Neurology (2017) 17:219 DOI 10.1186/s12883-017-0995-y RESEARCH ARTICLE Open Access Cortical vein thrombosis in adult patients of cerebral venous sinus thrombosis correlates with poor outcome
ORIGINAL ARTICLE. Evaluation of Cerebral Venous Thrombosis by CT, MRI and MR Venography
 16 Journal of The Association of Physicians of India Vol. 65 November 2017 ORIGINAL ARTICLE Evaluation of Cerebral Venous Thrombosis by CT, MRI and MR Venography Pratibha Issar 1, Sirasapalli Chinna 2,
16 Journal of The Association of Physicians of India Vol. 65 November 2017 ORIGINAL ARTICLE Evaluation of Cerebral Venous Thrombosis by CT, MRI and MR Venography Pratibha Issar 1, Sirasapalli Chinna 2,
Role of magnetic resonance venography in evaluation of cerebral veins and sinuses occlusion
 Alexandria Journal of Medicine (2012) 48, 29 34 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Role of magnetic resonance venography in
Alexandria Journal of Medicine (2012) 48, 29 34 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Role of magnetic resonance venography in
l' ".'"` va" Fig. 1 Patient 1. Precontrast computed tomographic scans demonstrating areas of increased attenuation
 136 -. i 'sit'' -k tz#. / e, = r + -e l' ".'"` va" "t 'hua th ;] fteqhiv.r'" ' Fig. 1 Patient 1. Precontrast computed tomographic scans demonstrating areas of increased attenuation in the region of the
136 -. i 'sit'' -k tz#. / e, = r + -e l' ".'"` va" "t 'hua th ;] fteqhiv.r'" ' Fig. 1 Patient 1. Precontrast computed tomographic scans demonstrating areas of increased attenuation in the region of the
Saudi Journal of Medicine (SJM)
 Saudi Journal of Medicine (SJM) Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-3389 (Print) ISSN 2518-3397 (Online) Clinical Profile and Radiological
Saudi Journal of Medicine (SJM) Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-3389 (Print) ISSN 2518-3397 (Online) Clinical Profile and Radiological
Intrasinus Thrombolysis by Mechanical and Urokinase for Severe Cerebral Venous Sinus Thrombosis : A Case Report
 122 Intrasinus Thrombolysis by Mechanical and Urokinase for Severe Cerebral Venous Sinus Thrombosis : A Case Report Wen-Sou Lin 1, Hung-Wen Kao 2, Chun-Jen Hsueh 2, Chun-An Cheng 3 Abstract- Purpose: Cerebral
122 Intrasinus Thrombolysis by Mechanical and Urokinase for Severe Cerebral Venous Sinus Thrombosis : A Case Report Wen-Sou Lin 1, Hung-Wen Kao 2, Chun-Jen Hsueh 2, Chun-An Cheng 3 Abstract- Purpose: Cerebral
Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results of Cerebral Perfusion MR Imaging
 pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
Detectability of unruptured intracranial aneurysms on thinslice non-contrast-enhanced CT
 Detectability of unruptured intracranial aneurysms on thinslice non-contrast-enhanced CT Poster No.: C-9 Congress: ECR 5 Type: Scientific Exhibit Authors: M. Nakadate, Y. Iwasa, M. Kishino, U. Tateishi;
Detectability of unruptured intracranial aneurysms on thinslice non-contrast-enhanced CT Poster No.: C-9 Congress: ECR 5 Type: Scientific Exhibit Authors: M. Nakadate, Y. Iwasa, M. Kishino, U. Tateishi;
Sinus Venous Thrombosis
 Sinus Venous Thrombosis Joseph J Gemmete, MD FACR, FSIR, FAHA Professor Departments of Radiology and Neurosurgery University of Michigan Hospitals Ann Arbor, MI Outline Introduction Medical Treatment Options
Sinus Venous Thrombosis Joseph J Gemmete, MD FACR, FSIR, FAHA Professor Departments of Radiology and Neurosurgery University of Michigan Hospitals Ann Arbor, MI Outline Introduction Medical Treatment Options
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT
 Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Improving the diagnostic quality of CT venography - a question of timing gone wrong?
 Improving the diagnostic quality of CT venography - a question of timing gone wrong? Poster No.: C-0432 Congress: ECR 2011 Type: Scientific Exhibit Authors: H. Al-Chalabi, K. Mankad, H. S. CHANDRASHEKAR,
Improving the diagnostic quality of CT venography - a question of timing gone wrong? Poster No.: C-0432 Congress: ECR 2011 Type: Scientific Exhibit Authors: H. Al-Chalabi, K. Mankad, H. S. CHANDRASHEKAR,
Hemorrhagic infarction due to transverse sinus thrombosis mimicking cerebral abscesses
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 2 Hemorrhagic infarction due to transverse sinus thrombosis mimicking cerebral abscesses N Barua, M Bradley, N Patel Citation N Barua, M Bradley,
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 2 Hemorrhagic infarction due to transverse sinus thrombosis mimicking cerebral abscesses N Barua, M Bradley, N Patel Citation N Barua, M Bradley,
Endovascular Thrombolysis in Deep Cerebral Venous Thrombosis
 Endovascular Thrombolysis in Deep Cerebral Venous Thrombosis Michael P. Spearman, Charles A. Jungreis, Joseph J. Wehner, Peter C. Gerszten, and William C. Welch Summary: We present two cases of acute thrombosis
Endovascular Thrombolysis in Deep Cerebral Venous Thrombosis Michael P. Spearman, Charles A. Jungreis, Joseph J. Wehner, Peter C. Gerszten, and William C. Welch Summary: We present two cases of acute thrombosis
Dural sinus thrombosis identified by point-of-care ultrasound
 https://doi.org/10.15441/ceem.17.237 Dural sinus thrombosis identified by point-of-care ultrasound Laura T. Director, David C. Mackenzie Department of Emergency Medicine, Maine Medical Center, Portland,
https://doi.org/10.15441/ceem.17.237 Dural sinus thrombosis identified by point-of-care ultrasound Laura T. Director, David C. Mackenzie Department of Emergency Medicine, Maine Medical Center, Portland,
Intracranial spontaneous hemorrhage mechanisms, imaging and management
 Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
Modifi ed CT perfusion contrast injection protocols for improved CBF quantifi cation with lower temporal sampling
 Investigations and research Modifi ed CT perfusion contrast injection protocols for improved CBF quantifi cation with lower temporal sampling J. Wang Z. Ying V. Yao L. Ciancibello S. Premraj S. Pohlman
Investigations and research Modifi ed CT perfusion contrast injection protocols for improved CBF quantifi cation with lower temporal sampling J. Wang Z. Ying V. Yao L. Ciancibello S. Premraj S. Pohlman
Multisection CT Venography of the Dural Sinuses and Cerebral Veins by Using Matched Mask Bone Elimination
 AJNR Am J Neuroradiol 25:787 791, May 2004 Case Report Multisection CT Venography of the Dural Sinuses and Cerebral Veins by Using Matched Mask Bone Elimination Charles B. L. M. Majoie, Marcel van Straten,
AJNR Am J Neuroradiol 25:787 791, May 2004 Case Report Multisection CT Venography of the Dural Sinuses and Cerebral Veins by Using Matched Mask Bone Elimination Charles B. L. M. Majoie, Marcel van Straten,
Radiologic diagnosis of cerebral venous thrombosis and its differential diagnosis
 Radiologic diagnosis of cerebral venous thrombosis and its differential diagnosis Poster No.: C-0628 Congress: ECR 2014 Type: Educational Exhibit Authors: A. M. Vargas Díaz, C. Fernández Rey, D. Garcia
Radiologic diagnosis of cerebral venous thrombosis and its differential diagnosis Poster No.: C-0628 Congress: ECR 2014 Type: Educational Exhibit Authors: A. M. Vargas Díaz, C. Fernández Rey, D. Garcia
Department of Radiology University of California San Diego. MR Angiography. Techniques & Applications. John R. Hesselink, M.D.
 Department of Radiology University of California San Diego MR Angiography Techniques & Applications John R. Hesselink, M.D. Vascular Imaging Arterial flow void Flow enhancement Gadolinium enhancement Vascular
Department of Radiology University of California San Diego MR Angiography Techniques & Applications John R. Hesselink, M.D. Vascular Imaging Arterial flow void Flow enhancement Gadolinium enhancement Vascular
L M Thornton, MD; L Lanier, MD; C L Sistrom, MD; D Rajderkar, MD; A Mancuso, MD; IM Schmalfuss, MD University of Florida, Gainesville Department of
 L M Thornton, MD; L Lanier, MD; C L Sistrom, MD; D Rajderkar, MD; A Mancuso, MD; IM Schmalfuss, MD University of Florida, Gainesville Department of Radiology RSNA Annual Meeting 2016 Trainee call readiness
L M Thornton, MD; L Lanier, MD; C L Sistrom, MD; D Rajderkar, MD; A Mancuso, MD; IM Schmalfuss, MD University of Florida, Gainesville Department of Radiology RSNA Annual Meeting 2016 Trainee call readiness
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
1998 Plenary Session: Imaging Symposium
 1998 Plenary Session: Imaging Symposium LEARNING OBJECTIVE Understand the characteristic imaging findings of acute cerebral infarction and dural sinus thrombosis and be familiar with the current best imaging
1998 Plenary Session: Imaging Symposium LEARNING OBJECTIVE Understand the characteristic imaging findings of acute cerebral infarction and dural sinus thrombosis and be familiar with the current best imaging
ISCHEMIC STROKE IMAGING
 ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
MR Imaging with the CCSVI or Haacke protocol
 MR Imaging with the CCSVI or Haacke protocol Reports from the Haacke protocol are often made available to the patients. The report consists of four major components: 1. anatomical images of major neck
MR Imaging with the CCSVI or Haacke protocol Reports from the Haacke protocol are often made available to the patients. The report consists of four major components: 1. anatomical images of major neck
Aneesh T., Hemamalini Gururaj*, Arpitha J. S., Anusha Rao, Vaishnavi Chakravarthy, Abhiman Shetty
 International Journal of Research in Medical Sciences Aneesh T et al. Int J Res Med Sci. 2017 Jul;5(7):3023-3028 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20172981
International Journal of Research in Medical Sciences Aneesh T et al. Int J Res Med Sci. 2017 Jul;5(7):3023-3028 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20172981
Anatomic Evaluation of the Circle of Willis: MR Angiography versus Intraarterial Digital Subtraction Angiography
 Anatomic Evaluation of the Circle of Willis: MR Angiography versus Intraarterial Digital Subtraction Angiography K. W. Stock, S. Wetzel, E. Kirsch, G. Bongartz, W. Steinbrich, and E. W. Radue PURPOSE:
Anatomic Evaluation of the Circle of Willis: MR Angiography versus Intraarterial Digital Subtraction Angiography K. W. Stock, S. Wetzel, E. Kirsch, G. Bongartz, W. Steinbrich, and E. W. Radue PURPOSE:
A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence
 A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence Poster No.: C-1347 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Hodel, A. GUILLONNET, M. Rodallec, S. GERBER, R. 1
A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence Poster No.: C-1347 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Hodel, A. GUILLONNET, M. Rodallec, S. GERBER, R. 1
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
Blunt Carotid Injury- CT Angiography is Adequate For Screening. Kelly Knudson, M.D. UCHSC April 3, 2006
 Blunt Carotid Injury- CT Angiography is Adequate For Screening Kelly Knudson, M.D. UCHSC April 3, 2006 CT Angiography vs Digital Subtraction Angiography Blunt carotid injury screening is one of the very
Blunt Carotid Injury- CT Angiography is Adequate For Screening Kelly Knudson, M.D. UCHSC April 3, 2006 CT Angiography vs Digital Subtraction Angiography Blunt carotid injury screening is one of the very
Comparison of Five Major Recent Endovascular Treatment Trials
 Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord
 The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
Rajat Malhotra 1*, Abhay G. Kakade 2 and Nilesh Choudhari 2
 MVP Journal of Medical Sciences, Vol 4(1), 89 96, JanuaryJune 2017 ISSN (Print) : 2348 263X ISSN (Online) : 23482648 DOI: 10.18311/mvpjms/2017/v4i1/737 Magnetic Resonance Venography Proving its Utility
MVP Journal of Medical Sciences, Vol 4(1), 89 96, JanuaryJune 2017 ISSN (Print) : 2348 263X ISSN (Online) : 23482648 DOI: 10.18311/mvpjms/2017/v4i1/737 Magnetic Resonance Venography Proving its Utility
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign
 Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
Whole-Brain Computed Tomographic Perfusion Imaging in Acute Cerebral Venous Sinus Thrombosis
 Published online: January 27, 2016 1664 9737/16/0044 0104$39.50/0 Original Paper Whole-Brain Computed Tomographic Perfusion Imaging in Acute Cerebral Venous Sinus Thrombosis Maxim Mokin a, e Chelsey C.
Published online: January 27, 2016 1664 9737/16/0044 0104$39.50/0 Original Paper Whole-Brain Computed Tomographic Perfusion Imaging in Acute Cerebral Venous Sinus Thrombosis Maxim Mokin a, e Chelsey C.
The Role of Neuroimaging in Acute Stroke. Bradley Molyneaux, HMS IV
 The Role of Neuroimaging in Acute Stroke Bradley Molyneaux, HMS IV Patient CR 62 yo F w/ 2 wk h/o altered mental status Presents to ED w/ confusion following a fall 1 day prior New onset left facial droop
The Role of Neuroimaging in Acute Stroke Bradley Molyneaux, HMS IV Patient CR 62 yo F w/ 2 wk h/o altered mental status Presents to ED w/ confusion following a fall 1 day prior New onset left facial droop
Cerebral Sinus Thrombosis with Intracerebral Hemorrhage in Pregnancy: A Case Report
 189 Cerebral Sinus Thrombosis with Intracerebral Hemorrhage in Pregnancy: A Case Report Hung-Shih Lin 1, Jui-Feng Lin 1, Cheng-Kuei Chang 1,2, Cheng-Chia Tsai 1, and Shiu-Jau Chen 1 Abstract- A 29-year-old
189 Cerebral Sinus Thrombosis with Intracerebral Hemorrhage in Pregnancy: A Case Report Hung-Shih Lin 1, Jui-Feng Lin 1, Cheng-Kuei Chang 1,2, Cheng-Chia Tsai 1, and Shiu-Jau Chen 1 Abstract- A 29-year-old
Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy
 AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
Neuroradiology MR Protocols
 Neuroradiology MR Protocols Brain protocols N 1: Brain MRI without contrast N 2: Pre- and post-contrast brain MRI N 3 is deleted N 4: Brain MRI without or pre-/post-contrast (seizure protocol) N 5: Pre-
Neuroradiology MR Protocols Brain protocols N 1: Brain MRI without contrast N 2: Pre- and post-contrast brain MRI N 3 is deleted N 4: Brain MRI without or pre-/post-contrast (seizure protocol) N 5: Pre-
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution
 CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
Reversible MR Imaging Abnormalities following Cerebral Venous Thrombosis
 AJNR Am J Neuroradiol 26:607 613, March 2005 Reversible MR Imaging Abnormalities following Cerebral Venous Thrombosis Carina Röttger, Susan Trittmacher, Tibo Gerriets, Franz Blaes, Manfred Kaps, and Erwin
AJNR Am J Neuroradiol 26:607 613, March 2005 Reversible MR Imaging Abnormalities following Cerebral Venous Thrombosis Carina Röttger, Susan Trittmacher, Tibo Gerriets, Franz Blaes, Manfred Kaps, and Erwin
OBJECTIVES. At the end of the lecture, students should be able to: List the cerebral arteries.
 DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: List the cerebral arteries. Describe the cerebral arterial supply regarding the origin, distribution and branches.
DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: List the cerebral arteries. Describe the cerebral arterial supply regarding the origin, distribution and branches.
Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA)
 Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA) Dr.Mohamed hamdy ibrahim MBBC,MSc,MD, PhD Neurology Degree Kings lake university (USA). Fellow
Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA) Dr.Mohamed hamdy ibrahim MBBC,MSc,MD, PhD Neurology Degree Kings lake university (USA). Fellow
Attenuation value in HU From -500 To HU From -10 To HU From 60 To 90 HU. From 200 HU and above
 Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Hemodynamic patterns of status epilepticus detected by susceptibility weighted imaging (SWI)
 Hemodynamic patterns of status epilepticus detected by susceptibility weighted imaging (SWI) Poster No.: C-1086 Congress: ECR 014 Type: Scientific Exhibit Authors: J. AELLEN, E. Abela, R. Kottke, E. Springer,
Hemodynamic patterns of status epilepticus detected by susceptibility weighted imaging (SWI) Poster No.: C-1086 Congress: ECR 014 Type: Scientific Exhibit Authors: J. AELLEN, E. Abela, R. Kottke, E. Springer,
L-Asparaginase Therapy with Concomitant Cranial Venous Thrombosis: Can Mri Help Avoiding Stroke
 Journal of the Egyptian Nat. Cancer Inst., Vol. 21, No. 1, March: 43-50, 2009 L-Asparaginase Therapy with Concomitant Cranial Venous Thrombosis: Can Mri Help Avoiding Stroke ALAA M. ELORABY, M.D. The Department
Journal of the Egyptian Nat. Cancer Inst., Vol. 21, No. 1, March: 43-50, 2009 L-Asparaginase Therapy with Concomitant Cranial Venous Thrombosis: Can Mri Help Avoiding Stroke ALAA M. ELORABY, M.D. The Department
NEURORADIOLOGY DIL part 4
 NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
MR Advance Techniques. Vascular Imaging. Class II
 MR Advance Techniques Vascular Imaging Class II 1 Vascular Imaging There are several methods that can be used to evaluate the cardiovascular systems with the use of MRI. MRI will aloud to evaluate morphology
MR Advance Techniques Vascular Imaging Class II 1 Vascular Imaging There are several methods that can be used to evaluate the cardiovascular systems with the use of MRI. MRI will aloud to evaluate morphology
Cerebral vein thrombosis
 Intern Emerg Med (2010) 5:27 32 DOI 10.1007/s11739-009-0329-1 IM - REVIEW Cerebral vein thrombosis Francesco Dentali Walter Ageno Received: 24 March 2009 / Accepted: 3 October 2009 / Published online:
Intern Emerg Med (2010) 5:27 32 DOI 10.1007/s11739-009-0329-1 IM - REVIEW Cerebral vein thrombosis Francesco Dentali Walter Ageno Received: 24 March 2009 / Accepted: 3 October 2009 / Published online:
Etiology, clinical manifestation and radiological findings in cerebral venous and sinus thrombosis
 ORIGINAL ARTICLE Journal of Pre-Clinical and Clinical Research, 2012, Vol 6, No 2, 105-110 www.jpccr.eu Etiology, clinical manifestation and radiological findings in cerebral venous and sinus thrombosis
ORIGINAL ARTICLE Journal of Pre-Clinical and Clinical Research, 2012, Vol 6, No 2, 105-110 www.jpccr.eu Etiology, clinical manifestation and radiological findings in cerebral venous and sinus thrombosis
Internal Carotid Artery Dissection
 May 2011 Internal Carotid Artery Dissection Carolyn April, HMS IV Agenda Presentation of a clinical case Discussion of the clinical features of ICA dissection Discussion of the imaging modalities used
May 2011 Internal Carotid Artery Dissection Carolyn April, HMS IV Agenda Presentation of a clinical case Discussion of the clinical features of ICA dissection Discussion of the imaging modalities used
Research Article Cerebral Venous Sinus Thrombosis, a Nonenhanced CT Diagnosis?
 Radiology Research and Practice Volume 215, Article ID 581437, 5 pages http://dx.doi.org/1.1155/215/581437 Research Article Cerebral Venous Sinus Thrombosis, a Nonenhanced CT Diagnosis? Ali Alsafi, Amish
Radiology Research and Practice Volume 215, Article ID 581437, 5 pages http://dx.doi.org/1.1155/215/581437 Research Article Cerebral Venous Sinus Thrombosis, a Nonenhanced CT Diagnosis? Ali Alsafi, Amish
Cerebral venous thrombosis: diagnosis dilemma
 Neurology International 2011; volume 3:e13 Cerebral venous thrombosis: diagnosis dilemma Pipat Chiewvit, 1 Siriwan Piyapittayanan, 1 Niphon Poungvarin 2 1Department of Radiology, Division of Diagnostic
Neurology International 2011; volume 3:e13 Cerebral venous thrombosis: diagnosis dilemma Pipat Chiewvit, 1 Siriwan Piyapittayanan, 1 Niphon Poungvarin 2 1Department of Radiology, Division of Diagnostic
JMSCR Vol 05 Issue 03 Page March 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i3.55 Imaging of Postpartum Encephalopathy:
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i3.55 Imaging of Postpartum Encephalopathy:
Review Article Differentiating between Hemorrhagic Infarct and Parenchymal Intracerebral Hemorrhage
 Hindawi Publishing Corporation Radiology Research and Practice Volume 2012, Article ID 475497, 11 pages doi:10.1155/2012/475497 Review Article Differentiating between Hemorrhagic Infarct and Parenchymal
Hindawi Publishing Corporation Radiology Research and Practice Volume 2012, Article ID 475497, 11 pages doi:10.1155/2012/475497 Review Article Differentiating between Hemorrhagic Infarct and Parenchymal
AJNR Am J Neuroradiol 23: , November/December 2002
 AJNR Am J Neuroradiol 23:1739 1746, November/December 2002 Normal Structures in the Intracranial Dural Sinuses: Delineation with 3D Contrast-enhanced Magnetization Prepared Rapid Acquisition Gradient-Echo
AJNR Am J Neuroradiol 23:1739 1746, November/December 2002 Normal Structures in the Intracranial Dural Sinuses: Delineation with 3D Contrast-enhanced Magnetization Prepared Rapid Acquisition Gradient-Echo
Ayman Mahmoud Alboudi MD, MSc Rashid Hospital, Dubai, UAE
 Systemic Varicella Zoster Infection Causing Cerebral Venous Thrombosis and Revealing Prothrombotic State Ayman Mahmoud Alboudi MD, MSc Rashid Hospital, Dubai, UAE CVT is a rare disorder with incidence
Systemic Varicella Zoster Infection Causing Cerebral Venous Thrombosis and Revealing Prothrombotic State Ayman Mahmoud Alboudi MD, MSc Rashid Hospital, Dubai, UAE CVT is a rare disorder with incidence
SWI including phase and magnitude images
 On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
STROKE - IMAGING. Dr RAJASEKHAR REDDY 2nd Yr P.G. RADIODIAGNOSIS KIMS,Narkatpalli.
 STROKE - IMAGING Dr RAJASEKHAR REDDY 2nd Yr P.G. RADIODIAGNOSIS KIMS,Narkatpalli. STROKE Describes a clinical event that consists of sudden onset of neurological symptoms Types Infarction - occlusion of
STROKE - IMAGING Dr RAJASEKHAR REDDY 2nd Yr P.G. RADIODIAGNOSIS KIMS,Narkatpalli. STROKE Describes a clinical event that consists of sudden onset of neurological symptoms Types Infarction - occlusion of
Cerebral malaria: MR imaging spectrum
 Cerebral malaria: MR imaging spectrum Poster No.: C-2705 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: P. S. Naphade, M. D. Agrawal, S. S. Sankhe, K. M. Siva, B. K. Jain; Mumbai/IN
Cerebral malaria: MR imaging spectrum Poster No.: C-2705 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: P. S. Naphade, M. D. Agrawal, S. S. Sankhe, K. M. Siva, B. K. Jain; Mumbai/IN
Etiology, clinical profile in cortical venous thrombosis
 International Journal of Advances in Medicine Pazare AR et al. Int J Adv Med. 2018 Oct;5(5):xxx-xxx http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20183365
International Journal of Advances in Medicine Pazare AR et al. Int J Adv Med. 2018 Oct;5(5):xxx-xxx http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20183365
NEURORADIOLOGY Part I
 NEURORADIOLOGY Part I Vörös Erika University of Szeged Department of Radiology SZEGED BRAIN IMAGING METHODS Plain film radiography Ultrasonography (US) Computer tomography (CT) Magnetic resonance imaging
NEURORADIOLOGY Part I Vörös Erika University of Szeged Department of Radiology SZEGED BRAIN IMAGING METHODS Plain film radiography Ultrasonography (US) Computer tomography (CT) Magnetic resonance imaging
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Role of Diffusion weighted Imaging in the Evaluation of Intracranial Tumors
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 12 Ver. IX (December. 2016), PP 99-104 www.iosrjournals.org Role of Diffusion weighted Imaging
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 12 Ver. IX (December. 2016), PP 99-104 www.iosrjournals.org Role of Diffusion weighted Imaging
Case Post traumatic cerebral venous thrombosis
 Case 12382 Post traumatic cerebral venous thrombosis AMMOR H Section: Neuroradiology Published: 2015, Jan. 20 Patient: 16 year(s), male Authors' Institution Hôpital Moulay El Hassan Ben El. Mehdi. Laayoune.
Case 12382 Post traumatic cerebral venous thrombosis AMMOR H Section: Neuroradiology Published: 2015, Jan. 20 Patient: 16 year(s), male Authors' Institution Hôpital Moulay El Hassan Ben El. Mehdi. Laayoune.
Stroke Imaging Basics. Jeremy Hopkin M.D.
 Stroke Imaging Basics Jeremy Hopkin M.D. Goals Introduce the basic physical properties of imaging used in stroke. Understand why each modality is used in the setting of stroke. Understand some strengths
Stroke Imaging Basics Jeremy Hopkin M.D. Goals Introduce the basic physical properties of imaging used in stroke. Understand why each modality is used in the setting of stroke. Understand some strengths
Evaluation and managment of CVT (Continuum).pdf
 University of Toronto From the SelectedWorks of Gustavo Saposnik 2015 Evaluation and managment of CVT (Continuum).pdf Gustavo Saposnik Available at: http://works.bepress.com/gustavo_saposnik/73/ Review
University of Toronto From the SelectedWorks of Gustavo Saposnik 2015 Evaluation and managment of CVT (Continuum).pdf Gustavo Saposnik Available at: http://works.bepress.com/gustavo_saposnik/73/ Review
Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case
 Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case Soo-Bin Yim, M.D., Jong-Sung Kim, M.D., Yang Kwon,M.D.*, Choong-Gon
Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case Soo-Bin Yim, M.D., Jong-Sung Kim, M.D., Yang Kwon,M.D.*, Choong-Gon
CASE PRESENTATION. Key Words: cerebral venous thrombosis, internal jugular vein stenosis, thrombolysis, stenting (Kaohsiung J Med Sci 2005;21:527 31)
 Treatment of cerebral venous thrombosis SUCCESSFUL TREATMENT OF CEREBRAL VENOUS THROMBOSIS ASSOCIATED WITH BILATERAL INTERNAL JUGULAR VEIN STENOSIS USING DIRECT THROMBOLYSIS AND STENTING: A CASE REPORT
Treatment of cerebral venous thrombosis SUCCESSFUL TREATMENT OF CEREBRAL VENOUS THROMBOSIS ASSOCIATED WITH BILATERAL INTERNAL JUGULAR VEIN STENOSIS USING DIRECT THROMBOLYSIS AND STENTING: A CASE REPORT
Frequency and temporal profile of recanalization after cerebral vein and sinus thrombosis
 ORIGINAL ARTICLE Frequency and temporal profile of recanalization after cerebral vein and sinus thrombosis C. Herweh a, M. Griebe b, C. Geisb usch c, K. Szabo b, E. Neumaier-Probst d, M. G. Hennerici b,
ORIGINAL ARTICLE Frequency and temporal profile of recanalization after cerebral vein and sinus thrombosis C. Herweh a, M. Griebe b, C. Geisb usch c, K. Szabo b, E. Neumaier-Probst d, M. G. Hennerici b,
Subarachnoid Hemorrhage as a Complication of Cerebral Venous Thrombosis
 Mitali Madhusmita et al CASE REPORT 10.5005/jp-journals-10036-1183 Subarachnoid Hemorrhage as a Complication of Cerebral Venous Thrombosis 1 Mitali Madhusmita, 2 Archana Bhate, 3 Anannya Mukherji ABSTRACT
Mitali Madhusmita et al CASE REPORT 10.5005/jp-journals-10036-1183 Subarachnoid Hemorrhage as a Complication of Cerebral Venous Thrombosis 1 Mitali Madhusmita, 2 Archana Bhate, 3 Anannya Mukherji ABSTRACT
Place for Interventional Radiology in Acute Stroke
 Place for Interventional Radiology in Acute Stroke Dr Lakmalie Paranahewa MBBS, MD(Radiology), FRCR Consultant Interventional Radiologist Asiri Group of Hospitals Objectives Imaging in Stroke Neurovascular
Place for Interventional Radiology in Acute Stroke Dr Lakmalie Paranahewa MBBS, MD(Radiology), FRCR Consultant Interventional Radiologist Asiri Group of Hospitals Objectives Imaging in Stroke Neurovascular
Supplementary Appendix
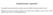 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Carrera J-P, Forrester N, Wang E, et al. Eastern equine encephalitis
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Carrera J-P, Forrester N, Wang E, et al. Eastern equine encephalitis
Imaging Acute Stroke and Cerebral Ischemia
 Department of Radiology University of California San Diego Imaging Acute Stroke and Cerebral Ischemia John R. Hesselink, M.D. Causes of Stroke Arterial stenosis Thrombosis Embolism Dissection Hypotension
Department of Radiology University of California San Diego Imaging Acute Stroke and Cerebral Ischemia John R. Hesselink, M.D. Causes of Stroke Arterial stenosis Thrombosis Embolism Dissection Hypotension
Magnetic Resonance Angiography
 Magnetic Resonance Angiography 1 Magnetic Resonance Angiography exploits flow enhancement of GR sequences saturation of venous flow allows arterial visualization saturation of arterial flow allows venous
Magnetic Resonance Angiography 1 Magnetic Resonance Angiography exploits flow enhancement of GR sequences saturation of venous flow allows arterial visualization saturation of arterial flow allows venous
Improvement of Image Quality with ß-Blocker Premedication on ECG-Gated 16-MDCT Coronary Angiography
 16-MDCT Coronary Angiography Shim et al. 16-MDCT Coronary Angiography Sung Shine Shim 1 Yookyung Kim Soo Mee Lim Received December 1, 2003; accepted after revision June 1, 2004. 1 All authors: Department
16-MDCT Coronary Angiography Shim et al. 16-MDCT Coronary Angiography Sung Shine Shim 1 Yookyung Kim Soo Mee Lim Received December 1, 2003; accepted after revision June 1, 2004. 1 All authors: Department
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Magnetic Resonance Imaging in Basilar Artery Occlusion Richard du Mesnil de Rochemont, MD; Tobias Neumann-Haefelin, MD; Joachim Berkefeld, MD; Matthias Sitzer, MD; Heinrich Lanfermann,
ORIGINAL CONTRIBUTION Magnetic Resonance Imaging in Basilar Artery Occlusion Richard du Mesnil de Rochemont, MD; Tobias Neumann-Haefelin, MD; Joachim Berkefeld, MD; Matthias Sitzer, MD; Heinrich Lanfermann,
Vascular Malformations of the Brain: A Review of Imaging Features and Risks
 Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
CT angiography and its role in the investigation of intracranial haemorrhage
 CT angiography and its role in the investigation of intracranial haemorrhage RD Magazine, 39, 458, 29-30 Dr M Igra Radiology SPR Leeds General Infirmary Dr I Djoukhadar Research fellow Wolfson Molecular
CT angiography and its role in the investigation of intracranial haemorrhage RD Magazine, 39, 458, 29-30 Dr M Igra Radiology SPR Leeds General Infirmary Dr I Djoukhadar Research fellow Wolfson Molecular
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
3D time-of-flight (3D TOF) MR angiography (MRA)
 ORIGINAL RESEARCH H.A. Deutschmann M. Augustin J. Simbrunner B. Unger H. Schoellnast G.A. Fritz G.E. Klein Diagnostic Accuracy of 3D Time-of-Flight MR Angiography Compared with Digital Subtraction Angiography
ORIGINAL RESEARCH H.A. Deutschmann M. Augustin J. Simbrunner B. Unger H. Schoellnast G.A. Fritz G.E. Klein Diagnostic Accuracy of 3D Time-of-Flight MR Angiography Compared with Digital Subtraction Angiography
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
Spectrum of CT and MR Findings for Cerebral Venous Sinus Thrombosis
 Spectrum of CT and MR Findings for Cerebral Venous Sinus Thrombosis Poster No.: C-0946 Congress: ECR 2014 Type: Educational Exhibit Authors: D. Singh, K. L. Mc Lean; Brisbane, QL/AU Keywords: Diagnostic
Spectrum of CT and MR Findings for Cerebral Venous Sinus Thrombosis Poster No.: C-0946 Congress: ECR 2014 Type: Educational Exhibit Authors: D. Singh, K. L. Mc Lean; Brisbane, QL/AU Keywords: Diagnostic
SWISS SOCIETY OF NEONATOLOGY. Neonatal cerebral infarction
 SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
While MR imaging is superior in the diagnosis of acute
 ORIGINAL RESEARCH X.-C. Wang P.-Y. Gao J. Xue G.-R. Liu L. Ma Identification of Infarct Core and Penumbra in Acute Stroke Using CT Perfusion Source Images BACKGROUND AND PURPOSE: CT perfusion (CTP) mapping
ORIGINAL RESEARCH X.-C. Wang P.-Y. Gao J. Xue G.-R. Liu L. Ma Identification of Infarct Core and Penumbra in Acute Stroke Using CT Perfusion Source Images BACKGROUND AND PURPOSE: CT perfusion (CTP) mapping
The Alberta Stroke Program Early CT Score (ASPECTS) is a
 ORIGINAL RESEARCH K. Lin O. Rapalino M. Law J.S. Babb K.A. Siller B.K. Pramanik Accuracy of the Alberta Stroke Program Early CT Score during the First 3 Hours of Middle Cerebral Artery Stroke: Comparison
ORIGINAL RESEARCH K. Lin O. Rapalino M. Law J.S. Babb K.A. Siller B.K. Pramanik Accuracy of the Alberta Stroke Program Early CT Score during the First 3 Hours of Middle Cerebral Artery Stroke: Comparison
