Cerebral venous thrombosis: diagnosis dilemma
|
|
|
- Pierce Flowers
- 6 years ago
- Views:
Transcription
1 Neurology International 2011; volume 3:e13 Cerebral venous thrombosis: diagnosis dilemma Pipat Chiewvit, 1 Siriwan Piyapittayanan, 1 Niphon Poungvarin 2 1Department of Radiology, Division of Diagnostic Radiology, 2 Department of Medicine, Division of Neurology, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand Abstract Cerebral venous thrombosis is increasing common disease in daily practice with sharing clinical nonspecific symptoms. This disorder is potentially lethal but treatable, oftenly it was overlooked in both clinical and radiologic in routine practice. Whenever, clinical suspected, prompt investigation by noninvasive imaging Magnetic resonance (MR) or advanced modilities such as cerebral venous thrombosis (CVT), MRV (MR Venography) will helpful in prompt diagnosis and treatment. These imaging modalities may reveal either direct sign (visualization of intraluminal clot) and indirect signs (paranchymatous change, intracranial hemorrhage). By using of effective treatment will improve the prognosis of the patient. This review summarizes insights into etiology, incidence, imaging modalities and current of the treatment. Introduction Clinical manifestations of cerebral venous thrombosis (CVT) are often nonspecific, 1 thus making difficulty in definite diagnosis. 2 The presentation of venous thrombosis is usually subacute, with symptoms evolving over days to weeks. 3 Common presentation includes headache, focal neurologic deficits, seizures, and altered consciousness. 1 The other symptoms and signs include obscuration of vision, alteration of consciousness, nausea, vomiting, papilledema, cranial nerve palsies and coma. 4 Most patients with deep venous thrombosis presented with symptoms of elevated intracranial pressure. 5 There was no association between localization of headache and site of sinus thrombosis except sigmoid sinus thrombosis. About 61% of patients with involvement of sigmoid sinus alone or in combination with transverse sinus had pain in the occipital and neck regions. 6 Focal neurological deficit comprises hemiparesis usually with facial sparing and may occur depending on the area involved. 6,7 In some patients, contralateral cortical veins may be involved resulting in paresis or paralysis of the opposite lower limb. 7 Cranial nerve syndromes are seen with venous sinus thrombosis. 6 Sinus thrombosis may occur as part of the intracranial hypertension syndrome (also known as pseudotumor cerebri) and CVT should be excluded with imaging in all patients with such manifestation. 8 Isolated subarachnoid hemorrhage is a rare presentation of CVT 1,4,9 and should be considered in the workup, especially when the basilar cisterns are not involved. 6 Intracerebral hemorrhages (ICH) occur in approximately onethird of patients with CVT, and are usually associated with a more severe clinical presentation at onset and a worse outcome. 10 There are four statistically significant predictors influencing outcome of CVST. They were underlying malignancy, low GCS, presence of hemorrhagic infarction (for poor outcome), and involvement of lateral sinus (for good outcome). 11 Materials and Methods Etiology The etiology of CVT is multifactorial 1,3 and may involve one or more mechanisms. 1,6 No cause is identified in as many as 25%. 8 Changes in the vessel walls blood flow or coagulability of blood can develop cerebral venous thrombosis. 7 Causal factors may be classified as local (related to intrinsic or mechanical conditions of the cerebral veins and dural sinuses) or systemic (related to clinical conditions that promote thrombosis). 4,8 The local conditions that alter the venous blood flow, including brain and skull damage, intracranial and local regional infection may potentiate the development of thrombosis. 4,8 The systemic causes include hormonal (pregnancy or puerperium, estroprogestative and steroid therapy), surgery, immobilization, hematologic and hypercoagulable disorders, connective tissue disease, malignancy, systemic infection and dehydration. 4,8 The frequency of these etiologic factors depends on age. In neonates, acute systemic illness, such as shock or dehydration, may be the cause. Frequent causes in older children include local infection, such as otitis media, mastoiditis, and coagulopathy. In adults, intrinsic or acquired coagulopathies become the most important factors, contributing to as many as 70% of cases. Infection contributes to less than 10% of cases in adults. In women of childbearing age, oral contraceptive use and pregnancy are strong risk factors. 1 The main risk factors for deep venous cerebral thrombosis include oral anticonception, post partum, trauma, pregnancies, Crohn disease, sickle cell disease, tumor, protein S deficiency, Correspondence: Pipat Chiewvit, Department of Radiology, Division of Diagnostic radiology, Faculty of Siriraj Hospital, Mahidol University, Bangkok 10700, Thailand. siscv@mahidol.ac.th Key words: cerebral venous thrombosis, computed tomography, magnetic resonance. Received for publication: 5 September Accepted for publication: 22 September This work is licensed under a Creative Commons Attribution NonCommercial 3.0 License (CC BY- NC 3.0). Copyright P. Chiewvit et al., 2011 Licensee PAGEPress, Italy Neurology International 2011; 3:e13 doi: /ni.2011.e13 inflammation, paroxysmal nocturnal haemoglobinuria, diabetes mellitus, and nephrotic syndrome. 5 Incidence Cerebral venous thrombosis (CVT) is responsible for 1-2% of all strokes in adults 12 and affect all age groups. 13 They estimated annual incidence of 3-4 cases per million people and a mortality rate of 8%. 12 Isolated CVT (ICoVT) (ie, without sinus involvement) appears extremely rare and has been mainly reported as isolated case reports or in small series. 14 Multiple locations of thrombosis, particularly in the contiguous transverse and sigmoid sinuses, are found in as many as 90% of patients. 8 The deep cerebral veins (Figure 1) [ie, the internal cerebral veins (ICVs), the basal veins of Rosenthal (BVR) and their tributaries] are involved in approximately 10% of patients. 15 Cortical venous involvement is seen in 6% of patients but is likely to be underreported when the dominant imaging finding is dural sinus involvement. 8 Investigation Neuroimaging is usually contributing a key role in the diagnosis of CVT. Radiologist often plays an important role in establishing the diagnosis of CVT. Though angiography is still considered to be the gold standard. 2 Magnetic resonance (MR) imaging, un-enhanced computed tomography (CT), unenhanced time-offlight MR venography, and contrast materialenhanced MR venography and CT venography are particularly useful techniques for detecting cerebral venous and brain parenchymal changes that may be related to thrombosis. 9. The pathophysiology of brain parenchymal involvement in venous occlusion differs from that in arterial occlusion. 9 Mechanism for [page 50]
2 venous infarction is the obstruction of venous drainage with increasing venous pressure in the affected region of brain. CVT progresses to cerebral venous infarction in approximately 50% of cases. 4 Parenchymal changes may be secondary to cytotoxic edema, vasogenic edema, or intracranial hemorrhage. 9 The radiological signs of CVT are usually classified as direct and indirect. The direct signs consist of demonstration of the thrombus on imaging or indirect, as when there are ischemic or vascular changes related to the venous outflow disturbance. 3,4 Indirect signs are not specific, but they should draw attention and prompt searching for direct visualization of a cortical or sinus thrombus. 9 The indirect signs are such as parenchyma change by brain swelling, white matter edema, cortical sulci effacement, loss of gray-white matter differentiation, hemorrhagic infarction as hemorrhagic spot in white matter edema and yet Kozic et al. 16 found subtle curvilinear hyperdensities within the left posterior cerebral hemisphere associated with typical signs of developing venous infarction from dural venous thrombosis. Computed tomography CT is the initial modality of investigation of choice for most neurological conditions. Its widespread availability, comparatively shorter scan times and lower cost. 2 It is reported that in the acute phase of CVT, almost 38% of CT scans are normal. 5 Thrombus is visible on nonenhanced CT as a high-attenuation lesion in the venous channel, producing dense triangle or cord sign represents an intravascular acute blood clot. 3,4 This sign is reported in 20% of patients and takes approximately 1-2 weeks to disappear. However, similarly increased attenuation of the cerebral venous sinuses may also represent polycythemia, dehydration, a subjacent subarachnoid or subdural hemorrhage and nonmyelinated brain in neonates makes sinuses appear unusually attenuating. 4,8,9 Increased attenuation in the sinus (Figure 2A, Figure 3, Figure 4A,B) may be the only finding suggestive of sinus thrombosis on unenhanced CT images, and patients with this sign should be further evaluated with contrastenhanced CT, MR imaging, or both, in the proper clinical scenario. 8 Early changes in CVT are often subtle, with brain edema and swelling of the gyri. Venous infarction demonstrates as a low-attenuation lesion with or without subcortical hemorrhage (Figure 2A and Figure 4A,B). Brain lesions are related to a venous distribution (e.g. bilateral parasagittal hemispheric lesions-superior sagittal sinus thrombosis, ipsilateral temporooccipital and cerebellar lobe lesions-transverse sinus thrombosis, bilateral thalamic lesionsdeep cerebral venous thrombosis). In Crombe D et al. study, the most frequently encountered Figure 1. Computed-tomography scan demonstrates a) hyperdense of intraluminal blood clot in deep venous system (internal cerebral veins) (arrows); b) diffuse hypodensity areas in bilateral thalami and basal ganglia represent cerebral venous infarction. Figure 2 (A) Axial computed-tomography noncontrast study) demonstrated hyperdensity of acute thrombus in left transverse sigmoid sinus (white arrow) with mixed hypohyperdensity lesion at left parieto-temporal region, measured about cm in size (arrowhead). (B) Contrast enhanced computed-tomography scan shows filling defect in left transverse-sigmoid sinus (black arrow). All of these findings are suggestive of left sigmoid and transeverse sinovenous sinus thromboses with acute intracerebral hemorrhage. Figure 3. S/P fibrinolytic agent treatment for 6 months. Follow up revealed A) further resolving of hematoma and B) almost disappearance of intraluminal clot (black arrow). [page 51]
3 sign is a hypodensity of the thalami and internal capsule (76%) and hemorrhagic infarction (19%). The extensive edema of the thalami and basal ganglia (Figure 1) may cause hydrocephalus due to compression of the foramen of Monro or the third ventricle. 5 Thrombosis of a deep cerebral vein can very rarely occurring unilaterally. 4,9 On contrast administration, non visualization of the thrombosed sinus is seen as an empty delta sign (Figure 2B, 4B, 5A-C). 3 However, this direct evidence may be available in only 20-30% of cases of sinus thrombosis, and rarely in isolated cortical vein thrombosis. 3 Transcortical medullary veins can become sources of collateral blood drainage. Subsequent dilatation of these vessels causes them to be visible at contrast-enhanced CT. Tentorial enhancement is caused by prominence of dural collaterals. Small subdural hematomas or effusion are seen occasionally. 4,9 Because of volume averaging, conventional axial CT scans can fail to demonstrate a hyperattenuating sinus or an empty delta sign in the horizontal segment of the superior sagittal sinus or transverse sinus (Figure 6A- C). 4 The empty delta sign can disappear in chronic stages with enhancement of organized clot. 4 Variant anatomy of the torcular herophili is common and may lead to diagnostic error, particularly in the interpretation of CT images. A high or asymmetric bifurcation may resemble an intrasinus thrombus, produced a pseudo empty delta sign. 8 CT venography CTV (Figure 7A-D) has proved to be a reliable method to investigate the structure of the cerebral veins, with a reported sensitivity of 95% with multiplanar reformatted (MPR) images when compared with digital subtraction angiography (DSA) as the standard of reference. 4,9 CTV is a promising for better delineation of venous anatomy, and equally sensitive for demonstrating thrombosis. 3 However, common variants of the sinovenous system should not be mistaken for sinus thrombosis. 9 CT venography is standardized and involves the following steps: First, two-dimensional (2D) MPR images are used to visualize dural venous sinuses and cerebral veins, with adequate window level and width. Second, 2D maximum intensity projection (MIP) series are created and saved. Optional reformations include 3D MIP and volume rendering display algorithms. 4 CT and CTV remains a rapid screening modality for early diagnosis of CVT in the emergency setting. 3 In patients with unenhanced CT findings suggestive of venous thrombosis, Mutidetector Computed Tomography (MDCT) venography can be performed without delay to confirm the diagnosis and to start appropriate therapy immediately. 9 Magnetic resonance imaging Magnetic resonance imaging (MRI) with MR venography (Figure 8A-8H) has become the investigation of choice in diagnosis of CVT. MRI is more sensitive in picking up the thrombus, and demonstrates age dependant signal characteristics. 3 One of the most important findings on MRI is abnormal signal intensity within the venous structure, indicating altered flow and thrombus formation. Gradient recalled-echo (GRE) T2*WI is becoming more widely used as a standard MR pulse sequence because of its sensitivity to acute intracranial hemorrhage. The signal intensity of CVT and normal flow states can both be variable, leading to diagnostic confusion. 12 Acute stage thrombus (within the first 7 days after clinical symptoms) has been shown to exhibit very subtle signal intensity alterations on noncontrast MR that can be mimic a normal flow void on T2WI. 4,12 One of the major reasons for the variable appearances of venous thrombus is thought to be alterations in hemoglobin oxygenation and iron oxidation state within Figure 4. Axial compted-tomography noncontrast study revealed a) hyperdensity cord sign and intraluminal clot sign at anterior of superior sagittal sinus (arrow head) and right cortical vein (arrows). Contrast enhanced CT scan demonstrated b) empty delta sign (arrowhead). Figure 5. A,B,C. Computed-tomography brain scan in post contrast study revealed filling defect in superior sagittal sinus could be superior sagittal sinus thrombosis. Figure 6. Axial computed-tomography noncontrast study revealed A) isodensity lesion at right transverse sinus in non contrast image which showing as filling defect along right transverse sinus, right sigmoid sinus and right jugular bulb in post contrast image B,C), suggestive of partial venous sinus thrombosis. [page 52]
4 trapped red-blood cells or extracellularly within the thrombus itself. 12 In the acute stage, thrombus is usually isointense on T1WI and hypointense on T2WI (Figure 8A,B) and relates to paramagnetic deoxyhemoglobin within trapped red blood cells within the thrombus. However, by using of T2W_FLAIR as conventional sequence is also helpful in detection of acute thrombus. This will be high signal intensity in T2W_FLAIR sequence. 17 In the subacute phase (7-14 days) divided into early and late subacute phase. Thrombus signal intensity of early subacute phase appeared hypersignal intensity on T1WI, and hyposignal intensity on T2WI, relating to intracellular methemoglobin. A late subacute phase can occur relating to extracellular methemoglobin in the evolving hyalinizing thrombus, where there is hypersignal intensity on both T1WI and T2WI. In the chronic stage (greater than 15 days), signal intensity is typically isointense on T1WI and hyperintense on T2WI and is probably related to the vascularized connective tissue of chronic thrombus. 11 There has been recent interest in evaluating the appearance of intraluminal venous thrombi on DWI. Signal hyperintensity in thrombosed sinuses on diffusion weighted images, with corresponding diminishment in the mean apparent diffusion coefficient (ADC) values, has been described in 41% of patients with sinus thrombosis. The duration of clinical symptoms was longer and complete recanalization was less frequent in patients with restricted diffusion in the thrombus. 8 Parenchymal abnormalities are better depicted and more commonly identified on MRI than CT. 8 Diffused weighted MRI techniques allow subclassfication of parenchymal abnormalities as either primarily vasogenic edema (with increased ADC values presumably related to venous congestion) or primarily cytotoxic edema The hyposignal on ADC mapping can confirm this and make the (with decreased ADC values related to cellular energy disruption). 8 In contrast with arterial ischemic states, many parenchymal abnormalities secondary to venous occlusion are reversible. 8 The ADC mapping can make distinction between cytotoxic edema and venous congestion. An increased ADC values presumably related to venous congestion but decreased ADC values represent cytotoxic edema that related to cellular energy disruption. 5,8 On the T1 contrast enhanced images, the venous congestion causes a marked enhancement of the subependymal plexus and the medullary veins that run perpendicular to the wall of the lateral ventricles. 5 Hemorrhagic infarction can sometimes be present, cause susceptibility artefacts on T2*WI. 5 Thalamic edema is the imaging hallmark of deep venous occlusion (e.g. internal cerebral vein, vein of Galen, or straight sinus), demonstrated hypersignal intensity on the T2 and Figure 7. Axial computed-tomography scan demonstrates A,B) intraluminal hyperdensity of clot at right sided of superior sagittal sinus wall, cortical veins of right frontal regions (cord sign, arrow). CT venography showed C,D) no contrast filled in thrombosed cortical vein in right frontal region. The dural venous sinus is well opacity by contrast medium. Figure 8. Axial T1W, T2W and FLAIR demonstrate A,B,C) intermediate signal intensity T1W and hyposignal intensity T2W (acute thrombus) and high signal intensity of thrombus in FLAIR. Post gadolinium contrast study revealed D,E,F,G,H) empty delta sign (arrow) and tentorial dural enhancement (arrowhead). [Neurology International 2011; 3:e1] [page 53]
5 FLAIR weighted images. 5,8 It may extend into the caudate regions and deep white matter. Hemorrhage is noted in 19% of patients and typically is located in the thalami. Unilateral thalamic edema may occur but is rare. 8 The lack of flow-void in the deep venous system is very suggestive for a venous thrombosis. At present, MR has become the method of choice for the diagnosis and follow-up of deep venous thrombosis because of its sensitivity to blood flow, its ability to visualise thrombus, and its non-invasiveness. 5 Isolated cortical venous thrombosis is a relatively rare entity. 8 It is particularly difficult to diagnose by using only T1WI, T2WI, and MRV imaging for different reasons (e.g. cortical veins are extremely variable in number, size, and location; occluded small veins at the cortical level are difficult to identify by using these MRI; only the occlusion of the largest veins is detectable on MRV). 3 Typical parenchymal findings are areas of focal cortical edema or hemorrhage, which may be nonspecfic. 8 The hyperintense vein sign is seen on MRI. Blooming artifacts within the thrombosed veins can be a very useful adjunct finding on GRE images. 8 Pitfalls of MRI in the diagnosis of CVTinclude flow-related enhancement and refocusing of slow flow, which may mimic intraluminal thrombus, or paramagnetic blood products (intracellular deoxyhemoglobin or methemoglobin) mimicking a normal signal void on long repetition time images. 4 The low T2 signal intensity at the early stage can be interpreted as a flow-void. 5 The susceptibility effect of T2 * -weighted imaging does not always indicate intravascular thrombosis or blood products, since arterial flow voids, calcifications, and the bone surfaces of the skull commonly result in susceptibility artifacts. 4 Variants of normal venous anatomy may mimic sinus thrombosis. These can be subdivided into venous anatomic variants that mimic occlusion (sinus atresia or hypoplasia), asymmetric or variant sinus drainage (occipital sinuses, sinus duplication), and normal sinus filling defects (arachnoid granulations, intrasinus septa). Arachnoid granulations typically have signal intensity similar to those of cerebrospinal fluid and appear as focal rounded filling defects with a characteristic anatomic distribution. If they are large and appear in the dominant sinus or only in the transverse sinus, they could cause venous obstruction and lead to symptoms of venous hypertension. 8 MR venography MRI combined (Figure 9) with MR venography (MRV) has largely replaced invasive cerebral angiography and conventional CT. 2 CT is entirely normal in 10-20% of cases with proven CVT. MRV in conjunction with conventional MRI can accurately diagnose CVT and is reliable as the sole examination for this condition. MRV is currently considered to be the noninvasive test of choice for evaluation of the dural sinus. However, flow-related and susceptibility artifacts can impair the evaluation of the venous structures. The more invasive arterial DSA is still the standard of reference. 2 MRV may be performed without the use of a contrast agent using the time-of-flight (TOF) technique or the phase contrast technique. Because these techniques use MR flow phenomena for contrast generation, they are subject to flowrelated image artifacts. Similar to CTV, contrast-enhanced MRV (Figure 8D,E,F,G,H) takes advantage of luminal filling by contrast material rather than relying on the MR flow phenomena as in TOF or phase contrast MRV. Therefore, contrast-enhanced MRV is less likely to be affected by complex flow. Recently, gadolinium-enhanced MRV has been shown to be superior to TOF MRV and may offer the best evaluation using MRI. 12 In Meckel et al study, compare with MR and MRV sequences for the diagnostic accuracy of a combined dynamic and static contrast-enhanced MRV in CVT, found that combo-4d MRV demonstrated the highest overall sensitivity (binary test) among the 4 assessed techniques, T2w, GRE, TOF, 4D- MRV. 18 In dural venous sinus thrombosis alone, it showed the highest sensitivity (97%) and specificity (99%). 18 The combined analysis of dynamic contrastenhancement patterns enabled the identification of chronic sinus obliteration by its delayed enhancement characteristics on the dynamic part of combo-4d MRV. 18 A major drawback of static MRV approaches is that the imaging appearance of dural sinus thrombosis, in particular chronic thrombosis, can overlap with that of dural arteriovenous fistulas. This may lead to false diagnosis, as the latter entity frequently occurs as a sequelae of chronic CVT and is clinically initially often undiagnosed. 18 An irregular appearance of the sinus, with multiple intrasinus channels and dural collateral vessels, may be seen on MRV images and is characteristic of incomplete recanalization. 8 The artifacts on MRV can mimic with cerebral venous thrombosis by absence of normal flow signal in sinus or a vein. In 2D time-offlight imaging, flow gaps result from slow intravascular blood flow, in plane flow, and Figure 9. Axial noncontrast computed-tomography scan revealed A,B,C) hyperdense of cord sign in left cortical vein with noncontrast filling in post contrast enhanced study. Hemorrhagic spot in left parietal lobe is noted (arrow). Magnetic resonance imaging shows D,E,F) hyposignal T1W, T2W_FFE (shows blooming susceptibility effct (arrow) of hemorrhage in left parietal lobe. Post contrast enhanced MR venography showed G,H,I) a small filling defect at superior sagittal sinus (seen on 3D_T1W/Gd) and lacking of cortical vein of left high parietal region corresponding with CT imaging, compatible with cerebral venous thrombosis. [page 54]
6 complex blood flow patterns. Most of the artifactual loss of vascular signal seen with the use of 2D MRV occurs in nondominant transverse sinuses. Depiction of flowing blood with time-of-flight imaging is limited when short T1 substances such as methemoglobin are present. 4 In 2D phase-contrast imaging, if blood flow is sufficiently slow, the motion-induced phase shifts may be inadequate to distinguish the flow from stationary tissue. Postcontrast 3D magnetization-prepared rapid gradientecho T1-weighted images are not affected by the angle between vessels and imaging slab or flow velocity. 4 Cerebral angiography With the advent of CTV and MRI (Figure 10A-J), digital subtraction angiography (DSA) is now rarely required for diagnosis 4 because its invasive procedure. However, in patients with subarachnoid hemorrhage and cerebral venous thrombosis, DSA should be considered to rule out other causes of rebleeding, such as distal aneurysm and dural arteriovenous fistula, before anticoagulant therapy is administered. 4 The techniques include standard arterial catheter angiography, thrombosis within the venous system was diagnosed from the venous phase of a cerebral angiogram. 15 This may directly show the non-filling of the larger veins when involved, appeared as partial or complete lack of filling of veins or sinuses. 3,4 The otherwise show increased tortuous collaterals around the thrombosed vein, the pseudophlebitic pattern. 3 The DSA is usually required for diagnostic confirmation in most cases of isolated cortical venous thrombosis to show indirect signs such as collateral venous pathways, tortuous veins, or delayed local venous drainage. 13 In addition, to evaluate the associated condition such as dural AVM in patient with venous sinus thrombosis, angiography plays role in definite diagnosis and for proper treatment planning. the sensitivity of MRI and CT, MRI seems superior to CT. 5 CTV more commonly shows sinuses or smaller cerebral veins with low flow as compared with MRV (2D phase contrast, 3D phase contrast, and 2D time of flight). Limitations of CTV include exposure to ionizing radiation, adverse reactions to iodinated contrast medium, and limited visualization of skull base structures in 3D display. 4 Treatment Medical treatment for this condition includes anticoagulation or local thrombolysis, which raises concerns about the associated high risk of intracerebral hemorrhage. 19 Systemic anticoagulation is the first-line treatment for cerebral venous thrombosis because of its efficacy, safety, and feasibility. 4 In CVT hemorrhage, use of heparin had generated enough evidence in treatment and thus it has emerged as a useful drug in the management of CVT. Heparin reduces both mortality and morbidity in CVT. 7 Yamini et al. reported on a patient with extensive cranial sinus thrombosis that did not improve after a 25 mg bolus of rt-pa. A continuous infusion of rt-pa was Compare modalities CTV has several advantages over DSA. It is less invasive and less expensive, and the shorter time to diagnosis in the initial workup. 4 MPR images from CTV were superior to DSA images in showing the cavernous sinus, inferior sagittal sinus, and basal vein of Rosenthal. 4 Reported advantages of CTV compared with MRI techniques are rapid image acquisition (reduction of motion-related artifacts), no contraindication to pacemaker and ferromagnetic devices, increased imaging resolution, and fewer equivocal imaging findings. No flow related artifacts have been reported with use of a contrast material bolus and acquisition in the venous phase. 4 High-resolution CT has been reported to be comparable or superior to MRV (2D-TOF or phase-contrast). 9 Comparing Figure 10. Computed-tomography (CT) noncontrast study demonstrated A) ill-defined hypodensity lesion at left parieto-occipital region with small internal slightly hyperdensity (HU~45) area. Effacement of left cerebral convexity is noted. After contrast medium administration in CT angiography there are B,C,D,E,F) multiple dilated, tortuous cortical vein of left temporal region. Selective arteriography of left occipital artery demonstrates G,H) dural arteriovenous shunt at left transverse sigmoid sinus with thrombosed blinded pouch of left sigmoid sinus (white arrow) with retrograde leptomeningeal venous drainage (arrow) corresponding to CTA. Completed obliteration of malignant dural AVM at left transverse sigmoid sinus status I,J)post acrylic glue embolization. [page 55]
7 administered at 1 mg/h for 19 hours 19 Low molecular weight heparin has also been found to be equally effective. Thrombolytic and fibrinolytic drugs like urokinase, streptokinase and oral anticoagulants, e.g., warfarin have also been tried and found to be effective in some cases (Figure 3). 7 Surgical management may include decompressive craniectomy, thrombectomy and evacuation of inter-cerebral haematoma need still further evaluation before it is recommended as a safe procedure. 7 Endovascular intervention with locally infused rt-pa, or mechanical thrombolysis using microwires or available commercial devices. 16 The adjunction of local thrombolysis is indicated in the rare cases of worsening despite adequate anticoagulation and optimal symptomatic and etiologic treatments. 4 The role of endovascular reopening of the dural sinuses with angioplasty and stent placement in the presence of severe intracranial venous hypertension is anecdotal, and long-term results are not known. 4 Prognosis Early clinical diagnosis and early institution of therapy specially heparin or thrombolytic therapy followed by oral anticoagulants have improved the prognosis of CVT. Srinivasan observed that mortality has been reduced from 50.6% to 10% in the last three decade. 20 The early convulso-paralytic state, impairment of consciousness, and presence of hemorrhagic infarcts are the factors adversely affecting prognosis. 7 Patient with intracerebral hemorrhage whose are older, men, having a thrombosis of the deep cerebral venous system or of the right lateral sinus, having a motor deficit, and having a right lateral sinus thrombosis are predictors of poor outcome. 7 The central nervous system infection is also increased risk of bad outcome. 4 The prognosis for return of function is believed to be somewhat better than for arterial stroke. 2 Conclusions The clinical manifestations of CVT are often non-specific and are easily mistaken for those caused by other neurological disease processes. Imaging plays a primary role in diagnosis. A variety of different imaging techniques are available for the diagnosis of the CVT. Daily routine practical work for diagnosis this condition include CT, CTV, MRI and MRV (TOF or contrast-enhanced MRV). CT scan include plain and dynamic sequences as CT venography are the simple, effective method to diagnosis of cerebral venous thrombosis and coule be the first screening method. Compare among those imaging modalities, MR is necessary in many situations without radiation exposure to confirm or exclude thrombosis such as clot identification, parenchyma changes to the most subtle condition as cortical cortical vein thrombosis by 3D or 4D MR venography. References 1. Poon CS, Chang JK, Swarnkar A, et al. Radiologic diagnosis of cerebral venous thrombosis: pictorial review. Am J Radiol 2007;189: S64 S Karthikeyan D, Vijay S, Kumar T, et al. Cerebral venous thrombosis-spectrum of CT findings. Neuroradiology 2004;14: Aliasgar V, Moiyadi M Ch, B Indira Devi. Posttraumatic non-sinus cerebral venous thrombosis. Indian J of Neurotrauma 2006;3: Rodallec MH, Krainik A, Feydy A, et al. Cerebral venous thrombosis and multidetector CT angiography: tips and tricks. RadioGraphics 2006;26:S5 S Crombe D, Haven Fr, Gille M. Isolated deep cerebral venous thrombosis diagnosed on CT and MR imaging. a case study and review literature review. JBR BTR 2003; 86: Wasay M, Kojan S, Dai AI, et al. Headache in cerebral venous thrombosis: incidence, pattern and location in 200 consecutive patients. J Headache Pain 2010;11: Prakash C, Bansal BC. Cerebral venous thrombosis. J India Aca Clin Med 2000;5: Leach JL, Fortuna RB, Jones BV, et al. Imaging of cerebral venous thrombosis: current techniques, spectrum of findings, and diagnostic pitfalls. Radiographic 2006; 26:S19-S Mahmoud MAL, Elbeblawy MMS. The role of multidetector CT venography in diagnosis of cerebral venous sinus thrombosis. Research J Med Med Sc 2009;4: Girot M, Ferro JM, Canhao P, et al. Predictors of outcome in patients with cerebral venous thrombosis and intracerebral hemorrhage. Stroke 2007;38: Poungvarin N,Prayoonwiwat N, Ratanakorn D, et al. Thai venous stroke prognostic score: TV-SPSS. J Med Assoc Thai 2009;92: Leach JL, Strub WM, Gaskill-Shipley MF. Cerebral venous thrombus signal intensity and susceptibility effects on gradient recalled-echo MR imaging. Am J Neuroradiol 2007;28: Linn J, Pfefferkorn T, Ivanicova K, et al. Noncontrast CT in deep cerebral venous thrombosis and sinus thrombosis: comparison of its diagnostic value for both entities. Am J Neuroradiol 2009;A Boukobza M, Crassard I, Bousser MGH, et al. MR Imaging features of isolated cortical vein thrombosis: diagnosis and follow-up. Am J Neuroradiol 2009;30: Teasdale E. Cerebral venous thrombosis: making the most of imaging. J R Soc Med 2000;93: Kozic D, Zarkov M, Semnic RR, et.al. Overlooked early CT signs of cerebral venous thrombosis with lethal outcome. Acta Neurol Belg 2010;110: Latchaw RE, Alberts MJ, Lev MH, et.al. Recommendations for Imaging of Acute Ischemia Stroke: A Scientific Statement From the American Heart Association. Stroke 2009;40: Meckel S, Reisinger C, Bremerich J, et al. Cerebral venous thrombosis: diagnostic accuracy of combined, dynamic and static, contrast-enhanced 4D MR venography. Am J Neuroradiol 2010;31: Khan S-NH, Adeoye O, Abruzzo TA, et al. Intracranial dural sinus thrombosis: novel use of a mechanical thrombectomy catheter and review of management strategies. CM&R 2009;7: Srinivasan K. Cerebral venous and arterial thrombosis in pregnancy and puerperium. Angiology 1983;134: [page 56]
41 year old female with headache. Elena G. Violari MD and Leo Wolansky MD
 41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
Computed tomography in the evaluation of cerebral venous sinus thrombosis
 Computed tomography in the evaluation of cerebral venous sinus thrombosis Poster No.: C-0090 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. Avsenik, K. Surlan Popovic; Ljubljana/SI
Computed tomography in the evaluation of cerebral venous sinus thrombosis Poster No.: C-0090 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. Avsenik, K. Surlan Popovic; Ljubljana/SI
ORIGINAL ARTICLE. Evaluation of Cerebral Venous Thrombosis by CT, MRI and MR Venography
 16 Journal of The Association of Physicians of India Vol. 65 November 2017 ORIGINAL ARTICLE Evaluation of Cerebral Venous Thrombosis by CT, MRI and MR Venography Pratibha Issar 1, Sirasapalli Chinna 2,
16 Journal of The Association of Physicians of India Vol. 65 November 2017 ORIGINAL ARTICLE Evaluation of Cerebral Venous Thrombosis by CT, MRI and MR Venography Pratibha Issar 1, Sirasapalli Chinna 2,
Radiologic diagnosis of cerebral venous thrombosis and its differential diagnosis
 Radiologic diagnosis of cerebral venous thrombosis and its differential diagnosis Poster No.: C-0628 Congress: ECR 2014 Type: Educational Exhibit Authors: A. M. Vargas Díaz, C. Fernández Rey, D. Garcia
Radiologic diagnosis of cerebral venous thrombosis and its differential diagnosis Poster No.: C-0628 Congress: ECR 2014 Type: Educational Exhibit Authors: A. M. Vargas Díaz, C. Fernández Rey, D. Garcia
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT
 Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Transverse Dural Sinus Thrombosis Joseph Junewick, MD FACR
 Transverse Dural Sinus Thrombosis Joseph Junewick, MD FACR 03/19/2010 History Child with headache and otomastoiditis. Diagnosis Dural venous thrombosis secondary to mastoiditis Discussion The cerebral
Transverse Dural Sinus Thrombosis Joseph Junewick, MD FACR 03/19/2010 History Child with headache and otomastoiditis. Diagnosis Dural venous thrombosis secondary to mastoiditis Discussion The cerebral
Sinus Venous Thrombosis
 Sinus Venous Thrombosis Joseph J Gemmete, MD FACR, FSIR, FAHA Professor Departments of Radiology and Neurosurgery University of Michigan Hospitals Ann Arbor, MI Outline Introduction Medical Treatment Options
Sinus Venous Thrombosis Joseph J Gemmete, MD FACR, FSIR, FAHA Professor Departments of Radiology and Neurosurgery University of Michigan Hospitals Ann Arbor, MI Outline Introduction Medical Treatment Options
Intracranial spontaneous hemorrhage mechanisms, imaging and management
 Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
The Role of Multidetector CT Venography in Diagnosis of Cerebral Venous Sinus Thrombosis
 Research Journal of Medicine and Medical Sciences, 4(2): 284-289, 2009 2009, INSInet Publication The Role of Multidetector CT Venography in Diagnosis of Cerebral Venous Sinus Thrombosis 1 Mohamed Abdel
Research Journal of Medicine and Medical Sciences, 4(2): 284-289, 2009 2009, INSInet Publication The Role of Multidetector CT Venography in Diagnosis of Cerebral Venous Sinus Thrombosis 1 Mohamed Abdel
ISCHEMIC STROKE IMAGING
 ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Normal Variations and Artifacts in MR Venography that may cause Pitfalls in the Diagnosis of Cerebral Venous Sinus Thrombosis.
 Normal Variations and Artifacts in MR Venography that may cause Pitfalls in the Diagnosis of Cerebral Venous Sinus Thrombosis. Poster No.: R-0005 Congress: 2015 ASM Type: Scientific Exhibit Authors: A.
Normal Variations and Artifacts in MR Venography that may cause Pitfalls in the Diagnosis of Cerebral Venous Sinus Thrombosis. Poster No.: R-0005 Congress: 2015 ASM Type: Scientific Exhibit Authors: A.
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
C. Douglas Phillips, MD FACR Director of Head and Neck Imaging Weill Cornell Medical College NewYork-Presbyterian Hospital
 C. Douglas Phillips, MD FACR Director of Head and Neck Imaging Weill Cornell Medical College NewYork-Presbyterian Hospital I have no financial disclosures Understand range of pathology that may present
C. Douglas Phillips, MD FACR Director of Head and Neck Imaging Weill Cornell Medical College NewYork-Presbyterian Hospital I have no financial disclosures Understand range of pathology that may present
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
Spectrum of CT and MR Findings for Cerebral Venous Sinus Thrombosis
 Spectrum of CT and MR Findings for Cerebral Venous Sinus Thrombosis Poster No.: C-0946 Congress: ECR 2014 Type: Educational Exhibit Authors: D. Singh, K. L. Mc Lean; Brisbane, QL/AU Keywords: Diagnostic
Spectrum of CT and MR Findings for Cerebral Venous Sinus Thrombosis Poster No.: C-0946 Congress: ECR 2014 Type: Educational Exhibit Authors: D. Singh, K. L. Mc Lean; Brisbane, QL/AU Keywords: Diagnostic
Endovascular Thrombolysis in Deep Cerebral Venous Thrombosis
 Endovascular Thrombolysis in Deep Cerebral Venous Thrombosis Michael P. Spearman, Charles A. Jungreis, Joseph J. Wehner, Peter C. Gerszten, and William C. Welch Summary: We present two cases of acute thrombosis
Endovascular Thrombolysis in Deep Cerebral Venous Thrombosis Michael P. Spearman, Charles A. Jungreis, Joseph J. Wehner, Peter C. Gerszten, and William C. Welch Summary: We present two cases of acute thrombosis
Neuroimaging of Cerebral Venous Thrombosis (CVT) Old Dilemma and the New Diagnostic Methods
 Signature: Pol J Radiol, 2015; 80: 368-373 DOI: 10.12659/PJR.894386 ORIGINL RTICLE Received: 2015.04.15 ccepted: 2015.04.26 Published: 2015.07.25 uthors Contribution: Study Design Data Collection C Statistical
Signature: Pol J Radiol, 2015; 80: 368-373 DOI: 10.12659/PJR.894386 ORIGINL RTICLE Received: 2015.04.15 ccepted: 2015.04.26 Published: 2015.07.25 uthors Contribution: Study Design Data Collection C Statistical
STROKE - IMAGING. Dr RAJASEKHAR REDDY 2nd Yr P.G. RADIODIAGNOSIS KIMS,Narkatpalli.
 STROKE - IMAGING Dr RAJASEKHAR REDDY 2nd Yr P.G. RADIODIAGNOSIS KIMS,Narkatpalli. STROKE Describes a clinical event that consists of sudden onset of neurological symptoms Types Infarction - occlusion of
STROKE - IMAGING Dr RAJASEKHAR REDDY 2nd Yr P.G. RADIODIAGNOSIS KIMS,Narkatpalli. STROKE Describes a clinical event that consists of sudden onset of neurological symptoms Types Infarction - occlusion of
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution
 CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
CASE PRESENTATION. Key Words: cerebral venous thrombosis, internal jugular vein stenosis, thrombolysis, stenting (Kaohsiung J Med Sci 2005;21:527 31)
 Treatment of cerebral venous thrombosis SUCCESSFUL TREATMENT OF CEREBRAL VENOUS THROMBOSIS ASSOCIATED WITH BILATERAL INTERNAL JUGULAR VEIN STENOSIS USING DIRECT THROMBOLYSIS AND STENTING: A CASE REPORT
Treatment of cerebral venous thrombosis SUCCESSFUL TREATMENT OF CEREBRAL VENOUS THROMBOSIS ASSOCIATED WITH BILATERAL INTERNAL JUGULAR VEIN STENOSIS USING DIRECT THROMBOLYSIS AND STENTING: A CASE REPORT
Essentials of Clinical MR, 2 nd edition. 99. MRA Principles and Carotid MRA
 99. MRA Principles and Carotid MRA As described in Chapter 12, time of flight (TOF) magnetic resonance angiography (MRA) is commonly utilized in the evaluation of the circle of Willis. TOF MRA allows depiction
99. MRA Principles and Carotid MRA As described in Chapter 12, time of flight (TOF) magnetic resonance angiography (MRA) is commonly utilized in the evaluation of the circle of Willis. TOF MRA allows depiction
Cerebral Venous Thrombosis: Imaging and Spectrum of Etiologies
 Cerebral Venous Thrombosis: Imaging and Spectrum of Etiologies Poster No.: C-0787 Congress: ECR 2013 Type: Educational Exhibit Authors: B. Alami, S. Bellakhdar, M. Jaffal, O. Addou, M. Maaroufi, M. Boubou,
Cerebral Venous Thrombosis: Imaging and Spectrum of Etiologies Poster No.: C-0787 Congress: ECR 2013 Type: Educational Exhibit Authors: B. Alami, S. Bellakhdar, M. Jaffal, O. Addou, M. Maaroufi, M. Boubou,
Etiology, clinical manifestation and radiological findings in cerebral venous and sinus thrombosis
 ORIGINAL ARTICLE Journal of Pre-Clinical and Clinical Research, 2012, Vol 6, No 2, 105-110 www.jpccr.eu Etiology, clinical manifestation and radiological findings in cerebral venous and sinus thrombosis
ORIGINAL ARTICLE Journal of Pre-Clinical and Clinical Research, 2012, Vol 6, No 2, 105-110 www.jpccr.eu Etiology, clinical manifestation and radiological findings in cerebral venous and sinus thrombosis
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Radiologic Diagnosis of Cerebral Venous Thrombosis: Pictorial Review
 JR Integrative Imaging LIFELONG LERNING FOR RDIOLOGY Radiologic Diagnosis of erebral Venous Thrombosis: Pictorial Review olin S. Poon 1,2, Ja-Kwei hang 1, mar Swarnkar 1, Michele H. Johnson 2, John Wasenko
JR Integrative Imaging LIFELONG LERNING FOR RDIOLOGY Radiologic Diagnosis of erebral Venous Thrombosis: Pictorial Review olin S. Poon 1,2, Ja-Kwei hang 1, mar Swarnkar 1, Michele H. Johnson 2, John Wasenko
THE INNOCUOUS HEADACHE THAT TURNED SINISTER
 CHAPTER 54 THE INNOCUOUS HEADACHE THAT TURNED SINISTER K. RAVISHANKAR, MD Case History A 42-year-old businessman was seen in our Headache Clinic with complaints of near-daily, continuous head pain for
CHAPTER 54 THE INNOCUOUS HEADACHE THAT TURNED SINISTER K. RAVISHANKAR, MD Case History A 42-year-old businessman was seen in our Headache Clinic with complaints of near-daily, continuous head pain for
Acute stroke imaging
 Acute stroke imaging Aims Imaging modalities and differences Why image acute stroke Clinical correlation to imaging appearance What is stroke Classic definition: acute focal injury to the central nervous
Acute stroke imaging Aims Imaging modalities and differences Why image acute stroke Clinical correlation to imaging appearance What is stroke Classic definition: acute focal injury to the central nervous
Cerebral Venous Thrombosis: Imaging and Spectrum of Etiologies
 Cerebral Venous Thrombosis: Imaging and Spectrum of Etiologies Poster No.: C-0787 Congress: ECR 2013 Type: Educational Exhibit Authors: B. Alami, S. Bellakhdar, M. Jaffal, O. Addou, M. Maaroufi, M. Boubou,
Cerebral Venous Thrombosis: Imaging and Spectrum of Etiologies Poster No.: C-0787 Congress: ECR 2013 Type: Educational Exhibit Authors: B. Alami, S. Bellakhdar, M. Jaffal, O. Addou, M. Maaroufi, M. Boubou,
Role of magnetic resonance venography in evaluation of cerebral veins and sinuses occlusion
 Alexandria Journal of Medicine (2012) 48, 29 34 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Role of magnetic resonance venography in
Alexandria Journal of Medicine (2012) 48, 29 34 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Role of magnetic resonance venography in
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
L M Thornton, MD; L Lanier, MD; C L Sistrom, MD; D Rajderkar, MD; A Mancuso, MD; IM Schmalfuss, MD University of Florida, Gainesville Department of
 L M Thornton, MD; L Lanier, MD; C L Sistrom, MD; D Rajderkar, MD; A Mancuso, MD; IM Schmalfuss, MD University of Florida, Gainesville Department of Radiology RSNA Annual Meeting 2016 Trainee call readiness
L M Thornton, MD; L Lanier, MD; C L Sistrom, MD; D Rajderkar, MD; A Mancuso, MD; IM Schmalfuss, MD University of Florida, Gainesville Department of Radiology RSNA Annual Meeting 2016 Trainee call readiness
Role of MRI in Evaluation of Cerebral Venous Thrombosis
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 6 Ver. 11 (June. 2018), PP 06-12 www.iosrjournals.org Role of MRI in Evaluation of Cerebral
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 6 Ver. 11 (June. 2018), PP 06-12 www.iosrjournals.org Role of MRI in Evaluation of Cerebral
Comparison of Five Major Recent Endovascular Treatment Trials
 Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
NEURORADIOLOGY Part I
 NEURORADIOLOGY Part I Vörös Erika University of Szeged Department of Radiology SZEGED BRAIN IMAGING METHODS Plain film radiography Ultrasonography (US) Computer tomography (CT) Magnetic resonance imaging
NEURORADIOLOGY Part I Vörös Erika University of Szeged Department of Radiology SZEGED BRAIN IMAGING METHODS Plain film radiography Ultrasonography (US) Computer tomography (CT) Magnetic resonance imaging
Cerebral MR Venography: Normal Anatomy and Potential Diagnostic Pitfalls
 AJNR Am J Neuroradiol 21:74 78, January 2000 Cerebral MR Venography: Normal Anatomy and Potential Diagnostic Pitfalls R. H. Ayanzen, C. R. Bird, P. J. Keller, F. J. McCully, M. R. Theobald, and J. E. Heiserman
AJNR Am J Neuroradiol 21:74 78, January 2000 Cerebral MR Venography: Normal Anatomy and Potential Diagnostic Pitfalls R. H. Ayanzen, C. R. Bird, P. J. Keller, F. J. McCully, M. R. Theobald, and J. E. Heiserman
Neuroradiology. of Stroke and Headaches
 Neuroradiology of Stroke and Headaches Learning Objec:ves 1. Iden:fy T1 and T2 sequences 2. Recall the normal anatomy of the intracranial circula:on 3. Apply appropriate CT and MR imaging of the brain
Neuroradiology of Stroke and Headaches Learning Objec:ves 1. Iden:fy T1 and T2 sequences 2. Recall the normal anatomy of the intracranial circula:on 3. Apply appropriate CT and MR imaging of the brain
CT angiography and its role in the investigation of intracranial haemorrhage
 CT angiography and its role in the investigation of intracranial haemorrhage RD Magazine, 39, 458, 29-30 Dr M Igra Radiology SPR Leeds General Infirmary Dr I Djoukhadar Research fellow Wolfson Molecular
CT angiography and its role in the investigation of intracranial haemorrhage RD Magazine, 39, 458, 29-30 Dr M Igra Radiology SPR Leeds General Infirmary Dr I Djoukhadar Research fellow Wolfson Molecular
Department of Radiology University of California San Diego. MR Angiography. Techniques & Applications. John R. Hesselink, M.D.
 Department of Radiology University of California San Diego MR Angiography Techniques & Applications John R. Hesselink, M.D. Vascular Imaging Arterial flow void Flow enhancement Gadolinium enhancement Vascular
Department of Radiology University of California San Diego MR Angiography Techniques & Applications John R. Hesselink, M.D. Vascular Imaging Arterial flow void Flow enhancement Gadolinium enhancement Vascular
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases
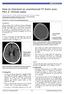 How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
Acute stroke. Ischaemic stroke. Characteristics. Temporal classification. Clinical features. Interpretation of Emergency Head CT
 Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
Dural Arteriovenous Malformations and Fistulae (DAVM S DAVF S)
 Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
Background. Recommendations for Imaging of Acute Ischemic Stroke: A Scientific Statement From the American Heart Association
 for Imaging of Acute Ischemic Stroke: A Scientific Statement From the American Heart Association An Scientific Statement from the Stroke Council, American Heart Association and American Stroke Association
for Imaging of Acute Ischemic Stroke: A Scientific Statement From the American Heart Association An Scientific Statement from the Stroke Council, American Heart Association and American Stroke Association
A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence
 A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence Poster No.: C-1347 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Hodel, A. GUILLONNET, M. Rodallec, S. GERBER, R. 1
A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence Poster No.: C-1347 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Hodel, A. GUILLONNET, M. Rodallec, S. GERBER, R. 1
Cortical vein thrombosis in adult patients of cerebral venous sinus thrombosis correlates with poor outcome and brain lesions: a retrospective study
 Liang et al. BMC Neurology (2017) 17:219 DOI 10.1186/s12883-017-0995-y RESEARCH ARTICLE Open Access Cortical vein thrombosis in adult patients of cerebral venous sinus thrombosis correlates with poor outcome
Liang et al. BMC Neurology (2017) 17:219 DOI 10.1186/s12883-017-0995-y RESEARCH ARTICLE Open Access Cortical vein thrombosis in adult patients of cerebral venous sinus thrombosis correlates with poor outcome
UPSTATE Comprehensive Stroke Center. Neurosurgical Interventions Satish Krishnamurthy MD, MCh
 UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
For Emergency Doctors. Dr Suzanne Smallbane November 2011
 For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
Non-Traumatic Neuro Emergencies
 Department of Radiology University of California San Diego Non-Traumatic Neuro Emergencies John R. Hesselink, M.D. Nontraumatic Neuroemergencies 1. Acute focal neurological deficit 2. Worst headache of
Department of Radiology University of California San Diego Non-Traumatic Neuro Emergencies John R. Hesselink, M.D. Nontraumatic Neuroemergencies 1. Acute focal neurological deficit 2. Worst headache of
Applicable Neuroradiology
 For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
2. Subarachnoid Hemorrhage
 Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Neuroradiology: Imaging and Stroke
 Neuroradiology: Imaging and Stroke Stroke 2017 William Gallmann January 28, 2017 Stroke Arterial ischemia/infarct accounts for ~85% Cerebral venous occlusions - 0.5-1% Spontaneous intracranial hemorrhage
Neuroradiology: Imaging and Stroke Stroke 2017 William Gallmann January 28, 2017 Stroke Arterial ischemia/infarct accounts for ~85% Cerebral venous occlusions - 0.5-1% Spontaneous intracranial hemorrhage
EPIDEMIOLOGY ETIOLOGY. 1. Infection extension from paranasal sinuses, middle ear (via emissary veins), face, oropharynx
 CEREBRAL VENOUS THROMBOSIS Vas13 (1) Cerebral Venous Thrombosis (CVT) Last updated: September 5, 2017 ETIOLOGY... 1 PATHOPHYSIOLOGY... 1 CLINICAL FEATURES... 2 SUPERIOR SAGITTAL SINUS THROMBOSIS... 2 LATERAL
CEREBRAL VENOUS THROMBOSIS Vas13 (1) Cerebral Venous Thrombosis (CVT) Last updated: September 5, 2017 ETIOLOGY... 1 PATHOPHYSIOLOGY... 1 CLINICAL FEATURES... 2 SUPERIOR SAGITTAL SINUS THROMBOSIS... 2 LATERAL
CASE OF THE WEEK PROFESSOR YASSER METWALLY. A 40 years old female patient presented with headache, fits, and disturbed level of consciousness.
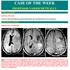 CASE OF THE WEEK PROFESSOR YASSER METWALLY CLINICAL PICTURE CLINICAL PICTURE A 40 years old female patient presented with headache, fits, and disturbed level of consciousness. RADIOLOGICAL FINDINGS RADIOLOGICAL
CASE OF THE WEEK PROFESSOR YASSER METWALLY CLINICAL PICTURE CLINICAL PICTURE A 40 years old female patient presented with headache, fits, and disturbed level of consciousness. RADIOLOGICAL FINDINGS RADIOLOGICAL
NEURORADIOLOGY DIL part 4
 NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
SWI including phase and magnitude images
 On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
Cerebral Venous Sinus Thrombosis - Diagnostic Strategies and Prognostic Models: A Review
 Royal College of Surgeons in Ireland e-publications@rcsi General Practice Articles Department of General Practice 1-1-2012 Cerebral Venous Sinus Thrombosis - Diagnostic Strategies and Prognostic Models:
Royal College of Surgeons in Ireland e-publications@rcsi General Practice Articles Department of General Practice 1-1-2012 Cerebral Venous Sinus Thrombosis - Diagnostic Strategies and Prognostic Models:
Attenuation value in HU From -500 To HU From -10 To HU From 60 To 90 HU. From 200 HU and above
 Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Etiology, clinical profile in cortical venous thrombosis
 International Journal of Advances in Medicine Pazare AR et al. Int J Adv Med. 2018 Oct;5(5):xxx-xxx http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20183365
International Journal of Advances in Medicine Pazare AR et al. Int J Adv Med. 2018 Oct;5(5):xxx-xxx http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20183365
Benign brain lesions
 Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Intrasinus Thrombolysis by Mechanical and Urokinase for Severe Cerebral Venous Sinus Thrombosis : A Case Report
 122 Intrasinus Thrombolysis by Mechanical and Urokinase for Severe Cerebral Venous Sinus Thrombosis : A Case Report Wen-Sou Lin 1, Hung-Wen Kao 2, Chun-Jen Hsueh 2, Chun-An Cheng 3 Abstract- Purpose: Cerebral
122 Intrasinus Thrombolysis by Mechanical and Urokinase for Severe Cerebral Venous Sinus Thrombosis : A Case Report Wen-Sou Lin 1, Hung-Wen Kao 2, Chun-Jen Hsueh 2, Chun-An Cheng 3 Abstract- Purpose: Cerebral
Cerebral Venous Thrombosis: A Potential Mimic of Primary Traumatic Brain Injury in Infants
 Pediatric Imaging Clinical Perspective Krasnokutsky Cerebral Venous Thrombosis in Infants Pediatric Imaging Clinical Perspective Michael V. Krasnokutsky 1 Krasnokutsky MV Keywords: abusive head injury,
Pediatric Imaging Clinical Perspective Krasnokutsky Cerebral Venous Thrombosis in Infants Pediatric Imaging Clinical Perspective Michael V. Krasnokutsky 1 Krasnokutsky MV Keywords: abusive head injury,
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
Magnetic Resonance Imaging. Basics of MRI in practice. Generation of MR signal. Generation of MR signal. Spin echo imaging. Generation of MR signal
 Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign
 Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
Place for Interventional Radiology in Acute Stroke
 Place for Interventional Radiology in Acute Stroke Dr Lakmalie Paranahewa MBBS, MD(Radiology), FRCR Consultant Interventional Radiologist Asiri Group of Hospitals Objectives Imaging in Stroke Neurovascular
Place for Interventional Radiology in Acute Stroke Dr Lakmalie Paranahewa MBBS, MD(Radiology), FRCR Consultant Interventional Radiologist Asiri Group of Hospitals Objectives Imaging in Stroke Neurovascular
l' ".'"` va" Fig. 1 Patient 1. Precontrast computed tomographic scans demonstrating areas of increased attenuation
 136 -. i 'sit'' -k tz#. / e, = r + -e l' ".'"` va" "t 'hua th ;] fteqhiv.r'" ' Fig. 1 Patient 1. Precontrast computed tomographic scans demonstrating areas of increased attenuation in the region of the
136 -. i 'sit'' -k tz#. / e, = r + -e l' ".'"` va" "t 'hua th ;] fteqhiv.r'" ' Fig. 1 Patient 1. Precontrast computed tomographic scans demonstrating areas of increased attenuation in the region of the
1998 Plenary Session: Imaging Symposium
 1998 Plenary Session: Imaging Symposium LEARNING OBJECTIVE Understand the characteristic imaging findings of acute cerebral infarction and dural sinus thrombosis and be familiar with the current best imaging
1998 Plenary Session: Imaging Symposium LEARNING OBJECTIVE Understand the characteristic imaging findings of acute cerebral infarction and dural sinus thrombosis and be familiar with the current best imaging
Classical CNS Disease Patterns
 Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Marc Norman, Ph.D. - Do Not Use without Permission 1. Cerebrovascular Accidents. Marc Norman, Ph.D. Department of Psychiatry
 Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
Index. aneurysm, 92 carotid occlusion, 94 ICA stenosis, 95 intracranial, 92 MCA, 94
 A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
CT INTERPRETATION COURSE
 CT INTERPRETATION COURSE Introductory Lecture on Basic Principles ASTRACAT 2012 Part One Stroke is a Clinical Diagnosis A clinical syndrome characterised by rapidly developing clinical symptoms and/or
CT INTERPRETATION COURSE Introductory Lecture on Basic Principles ASTRACAT 2012 Part One Stroke is a Clinical Diagnosis A clinical syndrome characterised by rapidly developing clinical symptoms and/or
An Introduction to Imaging the Brain. Dr Amy Davis
 An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
Methods. Yahya Paksoy, Bülent Oğuz Genç, and Emine Genç. AJNR Am J Neuroradiol 24: , August 2003
 AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CEREBRAL VENOUS SINUS THROMBOSIS: A REPORT OF TWO CASES
 220 EST FRIN MEDIL JOURNL May 2010 East frican Medical Journal Vol. 87 No. 5 May 2010 ERERL VENOUS SINUS THROMOSIS: REPORT OF TWO SES. K. Onyambu, Mh, MMed (Diag. Radiol), Lecturer, Department of Diagnostic
220 EST FRIN MEDIL JOURNL May 2010 East frican Medical Journal Vol. 87 No. 5 May 2010 ERERL VENOUS SINUS THROMOSIS: REPORT OF TWO SES. K. Onyambu, Mh, MMed (Diag. Radiol), Lecturer, Department of Diagnostic
Outline. Neuroradiology. Diffusion Imaging in. Clinical Applications of. Basics of Diffusion Imaging. Basics of Diffusion Imaging
 Clinical Applications of Diffusion Imaging in Neuroradiology No disclosures Stephen F. Kralik Assistant Professor of Radiology Indiana University School of Medicine Department of Radiology and Imaging
Clinical Applications of Diffusion Imaging in Neuroradiology No disclosures Stephen F. Kralik Assistant Professor of Radiology Indiana University School of Medicine Department of Radiology and Imaging
CT - Brain Examination
 CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER
 CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER CLEAR Surgical Center Team July 2011 Trial Enrollment Status Updates Insert latest enrollment update chart from most recent CLEAR newsletter Imaging
CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER CLEAR Surgical Center Team July 2011 Trial Enrollment Status Updates Insert latest enrollment update chart from most recent CLEAR newsletter Imaging
CASE OF THE WEEK PROFESSOR YASSER METWALLY
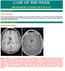 CLINICAL PICTURE CLINICAL PICTURE 26 years old male patient presented clinically with a grand male fit, confusion, fever, headache, and nausea. Examination showed bilateral papilledema and left sided extensor
CLINICAL PICTURE CLINICAL PICTURE 26 years old male patient presented clinically with a grand male fit, confusion, fever, headache, and nausea. Examination showed bilateral papilledema and left sided extensor
Subarachnoid Hemorrhage as a Complication of Cerebral Venous Thrombosis
 Mitali Madhusmita et al CASE REPORT 10.5005/jp-journals-10036-1183 Subarachnoid Hemorrhage as a Complication of Cerebral Venous Thrombosis 1 Mitali Madhusmita, 2 Archana Bhate, 3 Anannya Mukherji ABSTRACT
Mitali Madhusmita et al CASE REPORT 10.5005/jp-journals-10036-1183 Subarachnoid Hemorrhage as a Complication of Cerebral Venous Thrombosis 1 Mitali Madhusmita, 2 Archana Bhate, 3 Anannya Mukherji ABSTRACT
Journal of Radiology Case Reports
 Pediatric Holohemispheric Developmental Venous Anomaly: Definitive characterization by 3D Susceptibility Weighted Magnetic Resonance Angiography Michael A. Casey 1, Sourabh Lahoti 2, Ajeet Gordhan 2* 1.
Pediatric Holohemispheric Developmental Venous Anomaly: Definitive characterization by 3D Susceptibility Weighted Magnetic Resonance Angiography Michael A. Casey 1, Sourabh Lahoti 2, Ajeet Gordhan 2* 1.
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
Vascular Malformations of the Brain: A Review of Imaging Features and Risks
 Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
CT INTERPRETATION COURSE
 CT INTERPRETATION COURSE Refresher Course ASTRACAT October 2012 Stroke is a Clinical Diagnosis A clinical syndrome characterised by rapidly developing clinical symptoms and/or signs of focal loss of cerebral
CT INTERPRETATION COURSE Refresher Course ASTRACAT October 2012 Stroke is a Clinical Diagnosis A clinical syndrome characterised by rapidly developing clinical symptoms and/or signs of focal loss of cerebral
Hemorrhagic infarction due to transverse sinus thrombosis mimicking cerebral abscesses
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 2 Hemorrhagic infarction due to transverse sinus thrombosis mimicking cerebral abscesses N Barua, M Bradley, N Patel Citation N Barua, M Bradley,
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 2 Hemorrhagic infarction due to transverse sinus thrombosis mimicking cerebral abscesses N Barua, M Bradley, N Patel Citation N Barua, M Bradley,
Sinus and Cerebral Vein Thrombosis
 Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
Intracranial venous sector thrombectomy with endovascular thromboaspiration system
 Intracranial venous sector thrombectomy with endovascular thromboaspiration system Poster No.: C-1191 Congress: ECR 2015 Type: Scientific Exhibit Authors: D. D. J. De la Rosa Porras, E. Castro Reyes, J.
Intracranial venous sector thrombectomy with endovascular thromboaspiration system Poster No.: C-1191 Congress: ECR 2015 Type: Scientific Exhibit Authors: D. D. J. De la Rosa Porras, E. Castro Reyes, J.
NEURO IMAGING OF ACUTE STROKE
 1 1 NEURO IMAGING OF ACUTE STROKE ALICIA RICHARDSON, MSN, RN, ACCNS-AG, ANVP-BC WENDY SMITH, MA, RN, MBA, SCRN, FAHA LYNN HUNDLEY, APRN, CNRN, CCNS, ANVP-BC 2 2 1 DISCLOSURES Alicia Richardson: Stryker
1 1 NEURO IMAGING OF ACUTE STROKE ALICIA RICHARDSON, MSN, RN, ACCNS-AG, ANVP-BC WENDY SMITH, MA, RN, MBA, SCRN, FAHA LYNN HUNDLEY, APRN, CNRN, CCNS, ANVP-BC 2 2 1 DISCLOSURES Alicia Richardson: Stryker
Dural sinus thrombosis identified by point-of-care ultrasound
 https://doi.org/10.15441/ceem.17.237 Dural sinus thrombosis identified by point-of-care ultrasound Laura T. Director, David C. Mackenzie Department of Emergency Medicine, Maine Medical Center, Portland,
https://doi.org/10.15441/ceem.17.237 Dural sinus thrombosis identified by point-of-care ultrasound Laura T. Director, David C. Mackenzie Department of Emergency Medicine, Maine Medical Center, Portland,
MR Imaging with the CCSVI or Haacke protocol
 MR Imaging with the CCSVI or Haacke protocol Reports from the Haacke protocol are often made available to the patients. The report consists of four major components: 1. anatomical images of major neck
MR Imaging with the CCSVI or Haacke protocol Reports from the Haacke protocol are often made available to the patients. The report consists of four major components: 1. anatomical images of major neck
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
MR Flow Imaging in Vascular Malformations Using Gradient Recalled Acquisition
 637 MR Flow Imaging in Vascular Malformations Using Gradient Recalled Acquisition William M. Needell 1 Kenneth R. Maravilla Twenty patients with known or suspected intracranial vascular lesions were evaluated
637 MR Flow Imaging in Vascular Malformations Using Gradient Recalled Acquisition William M. Needell 1 Kenneth R. Maravilla Twenty patients with known or suspected intracranial vascular lesions were evaluated
Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA)
 Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA) Dr.Mohamed hamdy ibrahim MBBC,MSc,MD, PhD Neurology Degree Kings lake university (USA). Fellow
Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA) Dr.Mohamed hamdy ibrahim MBBC,MSc,MD, PhD Neurology Degree Kings lake university (USA). Fellow
CEREBRO VASCULAR ACCIDENTS
 CEREBRO VASCULAR S MICHAEL OPONG-KUSI, DO MBA MORTON CLINIC, TULSA, OK, USA 8/9/2012 1 Cerebrovascular Accident Third Leading cause of deaths (USA) 750,000 strokes in USA per year. 150,000 deaths in USA
CEREBRO VASCULAR S MICHAEL OPONG-KUSI, DO MBA MORTON CLINIC, TULSA, OK, USA 8/9/2012 1 Cerebrovascular Accident Third Leading cause of deaths (USA) 750,000 strokes in USA per year. 150,000 deaths in USA
Vascular Malformations
 Vascular Malformations LTC Robert Shih Chief of Neuroradiology Walter Reed Medical Center Special thanks to LTC Alice Smith (retired) Disclosures: None. This presentation reflects the personal views of
Vascular Malformations LTC Robert Shih Chief of Neuroradiology Walter Reed Medical Center Special thanks to LTC Alice Smith (retired) Disclosures: None. This presentation reflects the personal views of
