On the concept of third occipital headache
|
|
|
- Abel Lewis
- 6 years ago
- Views:
Transcription
1 Journal of Neurology, Neurosurgery, and Psychiatry 1986;49: On the concept of third occipital headache NIKOLAI BOGDUK, ANTHONY MARSLAND From the Pain Clinic, Princess Alexandra Hospital, and the Department ofanatomy, University of Queensland, Brisbane, Australia SUMMARY One of the putatative causes of headache is osteoarthritis of the C2-3 zygapophysial joint. A technique for blocking the third occipital nerve which innervates this joint was devised and used as a screening procedure for headache mediated by this nerve. Seven out of ten consecutive patients presenting with suspected cervical headache were found to suffer pain mediated by the third occipital nerve and stemming from a C2-3 zygapophysial joint. Because third occipital headache may be indistinguishable clinically from tension or other forms of headache, third occipital nerve blocks are advocated as means of establishing this largely unrecognised diagnosis. It is well recognised that disorders of the cervical spine can be a source of headache' - and one such disorder is said to be osteoarthritis of the upper cervical joints. ' - 7 The upper cervical joints consist of the atlanto-occipital joints, the median and lateral atlanto-axial joints, and the C2-3 zygapophysial joints, but in general, these joints have been implicated only collectively in the pathogenesis of headache. Seldom has the symptom of headache actually been ascribed to osteoarthritis specifically of one or other of these joints. In fact, no studies have demonstrated that osteoarthritis of the atlanto-occipital joints can be a cause of headache, while the median atlanto-axial joint has been implicated only on the basis of circumstantial radiological evidence.8 Furthermore, regardless of perhaps long-held convictions, explicit evidence demonstrating that headaches can be caused by osteoarthritis of the lateral atlanto-axial joints has only recently appeared.9 The C2-3 zygapophysial joints are a less familiar potential source of headache. Anatomically, these joints differ markedly from the other upper cervical synovial joints. Whereas the joints of the atlas lie ventral to the emerging spinal nerves, the C2-3 zygapophysial joints lie behind the intervertebral foramina in sequence with the other zygapophysial joints and are the highest synovial joints associated with an intervertebral disc at the same level. Moreover, functionally they represent a transition zone between the Address for reprint requests: Dr N Bogduk, Department of Anatomy, University of Queensland, St Lucia, Queensland, 4067, Australia. Received 2 April 1985 and in revised form 4 November Accepted 9 November 1985 C1-2 level, which accommodates rotation of the head, and the lower cervical spine, which accommodates flexion and extension of the neck.10 Our attention was drawn to the role of the C2-3 joints in the pathogenesis of headache by two clinical reports. Trevor-Jones" reported three patients in whom he found the third occipital nerve to be entrapped by osteophytes from an arthritic C2-3 joint, and surgical release of the entrapment relieved their headaches. Maigne"2 reported 98 patients whose headaches he successfully treated with periarticular injections of local anaesthetic and manipulation of the C2-3 joints. There are, however, certain limitations to these two reports. Interesting though his findings were, Trevor-Jones did not describe how patients with third occipital nerve entrapment could be identified pre-operatively. The limitation of Maigne's report is that he used particular injections without radiological control, so it could be questioned whether the relief he obtained was due to selective anaesthetisation of the C2-3 joint. Notwithstanding these limitations, we were prompted by these reports and our awareness of the biomechanical vulnerability of the C2-3 zygapophysial joints to undertake a study of patients presenting with occipital or suboccipital headache, to test the hypothesis that their pain stemmed from the C2-3 zygapophysial joints. A previous anatomical study'3 had demonstrated the nerve supply to the C2-3 zygapophysial joints and the topographical and radiological disposition of the third occipital nerve, and this information was used to perform radiologically controlled blocks of the nerves supplying the C2-3 zygapophysial joints in the patients selected for study. 775
2 /s a 1 ~~~~Anatomy 776 Bogduk, Marsland performed. However, certain control observations were made when the opportunity presented itself in the course of related investigations or procedures. These included blocks of lower cervical dorsal rami"3 which were performed as a screening procedure for intercurrent neck pain; C2 ganglion blocks,"4 which were performed to exclude headache mediated by the C2 spinal nerve; and in one case, an intramuscular injection of local anaesthetic, performed during an gon _<Asgs; l i attempted intra-articular injection of steroids. E TON The C3 dorsal ramus is a short nerve that arises from the spinal nerve and passes backwards through the C2-3 intertransverse space where it divides into a lateral and two s medial branches. The lateral branch supplies the more superficial posterior cervical muscles."3 The deeper of the C3 VR > two [ medial N F u branches e!k winds around the waist of the C3 articular pillar and enters the multifidus muscle. The superficial In[i medial branch is known as the third occipital nerve. This nerve crosses the lateral and dorsal aspects of the lower half of the C2-3 zygapophysial joint (fig 1). It then passes across -,.the lamina of C3 before turning backwards and upwards to C4VR W e pierce semispinalis capitis and splenius capitis to become cutaneous over the suboccipital area. Articular branches of the C2-3 zygapophysial joint arise from the deep aspect of the third occipital nerve as it crosses the joint, or from a Fig 1 A sketch of a posterolateral view of the left third communicating loop between the third occipital nerve and occipital nerve (TON) seen crossing the lateral aspect and the C2 dorsal ramus, which crosses the dorsal aspect of the then the dorsal aspect of the lower half of the C2-3 joint"3 (fig 1). zygapophysial joint. A branch to semispinalis capitis (s) arises from the nerve as it crosses the lamina of C3 and before it turns dorsally to enter the skin. Articular branches to the joint arise from the deep aspect of the third occipital nerve or i from the communicating loop (c) to the C2 dorsal ramus. 4.. :X The greater occipital nerve (gon) is shown crossing the obliquus inferior and rectus capitis posterior major, and the lateral (1) and deep medial (dm) branches of the C3 dorsal ramus are shown crossing the C3 transverse process. VR: ventral rami. Methods Ten consecutive patients presenting with occipital or suboccipital headache were studied. The headache history was recorded in terms of site, radiation, frequency etc, according to the protocol suggested by Lance.5 A physical examination was performed including a thorough examination of the neck for abnormalities of movement and tenderness. Signs particularly sought were tenderness over the cervical zygapophysial joints, which was adopted as a putatative sign of cervical arthropathy, and reproduction of head pain by sustained pressure over any site of tenderness. All patients underwent diagnostic blocks of the third Fig 2 A postero-anterior radiograph of the C2-3 occipital nerve, ipsilateral to their complaint of pain, or zygapophysialjoints. The joints (zj) are seen as laterally bilaterally in cases of bilateral pain. Patients whose pain was convex silhouettes rising upwards from the concavity of the relieved by blocking the third occipital nerve underwent two C3 articular pillar, opposite the level of the C2 spinous or more repeat blocks, at intervals between one week and process (sp), and below the lateral atlanto-axialjoints. The one month, to confirm the response. target region for third occipital nerve blocks is shown by Because of ethical considerations, related mainly to the dotted lines. A needle rests at the lowest of three sitesfor radiation exposure involved in performing fluoroscopically injection (arrows) along the lateral margin of the controlled blocks, formal control blocks were not routinely radiographic silhouette. U
3 On the concept of third occipital headache Radiology The constancy of the course of the third occipital nerve makes its location readily identifiable on postero-anterior radiographs. The proximal part of the nerve crosses the lower half of the silhouette of the C2-3 zygapophysial joint. This landmark is recognised as a convexity that rises upwards from the concavity of the C3 articular pillar, and usually lies horizontally opposite the level of the C2 spinous process and C2-3 disc space (fig 2). Because of the orientation of the joint, a distinct joint space is not always visible in a postero-anterior view, and cannot be relied upon as a landmark. A needle introduced onto the lateral margin of the silhouette, between its mid-point and lower end, will reliably encounter the third occipital nerve proximal to the origin of articular branches to the C2-3 joint. Third Occipital Nerve Blocks Third occipital nerve blocks were performed using fluoroscopic control with the patient lying prone on a table, the chest supported by a pillow and the head supported by a firm sponge cushion, leaving the mouth unobstructed. The C2-3 zygapophysial joint was visualised on the fluoroscope by appropriately adjusting the head tilt and opening the mouth. Once adequate orientation was achieved, the skin of the back of the neck was prepared as for an aseptic procedure and a puncture site was selected over the posterolateral aspect of the neck at the level of the C2 spinous process. The puncture site was determined radiographically by adjusting the position of the point of the needle on the skin so that its radiographic projection lay just lateral to the silhouette of the C2-3 joint. A 22 gauge, 70 mm needle was then inserted through the puncture site and directed ventrally and slightly medially into the neck muscles. The course of the needle, as it was advanced through the muscles, was repeatedly checked fluoroscopically, every 1 to 2 cm, to ensure that it travelled towards the back of the C2-3 joint. The dorsal aspect of the joint was the initial target in order to ensure the proper depth of insertion. Bony resistance coupled with the projection of the needle's point over the joint indicated that Iable Clinicalfeatures 777 it lay dorsal to the joint, and had not been misdirected ventrally in front of the joint. Once bone had been contacted, the needle was withdrawn slightly and readjusted laterally until its tip lay on the lateral margin of the silhouette (fig 2), all adjustments being monitored by repeated screening. Proper location of the point of the needle was confirmed radiographically and by the sensation that it rested on bone. That it lay on the very lateral margin of the joint was confirmed by adjusting the needle slightly more laterally to feel it slip ventrally off the margin. It was then repositioned. To block the third occipital nerve, three injections of 0 5 ml of 0 5% bupivicaine were performed: one at the midpoint of the convexity of the silhouette, one at its lower end, and the last between these two. Three such injections thoroughly bracket the course of the nerve, and the small volume used, while adequate to block the target nerve, minimised possible spread to adjacent levels. At the end of the procedure, the adequacy and accuracy of the block was confirmed clinically by examining for anaesthesia in the cutaneous distribution of the third occipital nerve. Results The essential clinical features of the patients studied are summarised in the table. All complained of occipital and suboccipital headache associated with pain radiating to the forehead or related regions. All had at least one feature that could be construed as suggesting a cervical origin for their pain such as a history of neck injury, precipitation of pain by neck movement, or cervical tenderness. Only one patient (number 1 1) suffered the associated features of photophobia, nausea and vomiting that strongly suggested a diagnosis of common migraine. Otherwise, the clinical features of the patients studied did not conform to those of any conventional diagnostic category, 'atient Sex Age Onset History Site Radiation Quality Frequency Aggravating Tender Restricted (yr) factors movements I M 46 IA 3 yr LSO L orbit Ache Constant Lifting Ex, Rot 2 F 53 S 2 yr 0 Orbits Ache Constant Neck extension Fl, Ex, L Rot 3 F 28 MVA 6 m SO Vertex Ache Constant Neck flexion C2-3 4 F 31 S 15 yr RO Vertex Ache Constant Reading C2-3 5 F 43 S 12 yr 0 Orbits Ache Constant - C2-3 6 F 30 MVA 3 yr RSO R orbit Ache Daily Neck movements Fl, Ex, R Rot 7 F 34 MVA 12 yr RO - Ache Constant Neck movements C2-3 8 M 52 S 24 yr SO Orbits Throb Constant Stress SO 9 M 52 S 20 yr SO Whole head Vice-like Constant - C2-3 Fl, Ex, Rot 3 M 29 S 20 yr 0 Orbits Throb Constant Neck movements Nausea, vomiting photophobia lotes: (1) The onset of headache is tabulated as spontaneous (S) or following an industrial accident (IA) or a motor vehicle accident (MVA). (2) The length f history is measured in years (yr) or months (m). (3) The principal site of pain is tabulated as suboccipital (SO) or occipital (0), prefixed by left (L) or right 1) as appropriate. (4) C2-3 refers to tenderness over the C2-3 zygapophysial joints. SO refers to tenderness in the suboccipital region. (5) Abbreviations used r movements are flexion (Fl), extension (Ex) and rotation (Rot) prefixed by left (L) or right (R) as appropriate. (6) Patient number 10 exhibited no signs in ie neck, but suffered nausea, vomiting and photophobia.
4 778 apart from possible tension headache. cervical headache or perhaps Seven of the ten patients responded to unilateral diagnostic blocks of a third occipital nerve. The response was complete relief of all pain for the duration of action of the anaesthetic used, associated with the elimination of aggravating factors. Subsequent blocks reproduced exactly the same relief. Three patients (numbers 9, 10 and 11) had no relief following blocks of their third occipital nerves bilaterally. Nor was there any relief following blocks of either the C4 dorsal rami or the C2 ganglia. Control observations corroborated the response in patients 1, 2, 5, 6 and 7. Patient number 1 underwent blocks of his C5, 6, 7 and C4 dorsal rami prior to third occipital nerve blocks. During none of these procedures did he report relief of his headache, but repeated blocks of his third occipital nerve consistently relieved his pain. This patient also underwent a single-blind investigation comparing the responses to short-acting (lignocaine) versus long-acting (bupivicaine) local anaesthetic. His headache was relieved for 1 hour after injection of lignocaine, but for 5 hours after using bupivicaine. Patient number 2 underwent C2 ganglion blocks as her differential diagnosis included lateral atlantoaxial arthritis, but these did not relieve her headaches, whereas three blocks of her left third occipital nerve consistently relieved her headaches, as did similar blocks on three further occasions in the course of various therapeutic procedures. Patient number 6 underwent blocks of her C5, 6 dorsal rami in the initial course of the investigation of her complaint of combined neck pain and headache. The C5, 6 blocks relieved her neck pain but did not influence her headaches. Reciprocally, the headaches, but not the neck pain, were repeatedly relieved by right third occipital nerve blocks. Patient number 7 underwent a block of her right greater occipital nerve as her diagnosis included neuroma formation on this nerve, but this did not influence her constant aching headaches which, on the other hand, were relieved by third occipital nerve blocks. During an unsuccessful attempt at injecting steroids into her right C2-3 zygapophysial joint, patient number 5 underwent an injection of local anaesthetic directed dorsal but superficial to the joint. This injection did not involve the third occipital nerve because no numbness ensued, and did not relieve her headache, but three effective blocks of the third occipital nerve, as evidence by numbness in the appropriate cutaneous field, succeeded in relieving her pain. Also, a single-blind block, using lignocaine instead of bupivicaine, had an appropriately shortened duration of relief. Discussion Bogduk, Marsland That patients with C2-3 zygapophysial arthropathy should suffer headache is not surprising. In the spinal cord, terminals of the C3 spinal nerve overlap with terminals of the trigeminal nerve,"s -17 and the convergence between cervical and trigeminal afferents in the spinal grey matter provides a suitable neuroanatomical substrate for the referral of pain to the head. Previous studies have shown that noxious stimulation of the muscles and ligaments innervated by the upper three cervical dorsal rami can produce headache in normal volunteers.'8'20 The referral pattern of pain from cervical zygapophysial joints, however, has not been specifically studied, but such studies have been done in the lumbar region where zygapophysial pain can be referred to various regions of the lower limb.2' 22 Extrapolation of these results suggests that noxious stimulation of the upper cervical synovial joints could, like stimulation of the overlying muscles, cause headache. Third occipital nerve blocks were adopted in this study because they provide a convenient means of screening for painful disorders mediated by this nerve. The structures innervated by the third occipital nerve are only skin, part of the semispinalis capitis muscle, and the C2-3 zygapophysial joint.'3 There are no occult conditions of the skin, and no known conditions selectively affecting only that portion of semispinalis innervated by C3, that cause headache. The C2-3 zygapophysial joint is the only structure innervated by the third occipital nerve that could possibly be a source of chronic pain. Therefore, we believe that third occipital nerve blocks are adequately selective for painful disorders of the C2-3 zygapophysial joints. We elected to use nerve blocks rather than direct joint blocks because, technically, they are easier to perform and are less painful for the patient. Zygapophysial joint blocks involve a troublesome insertion of needles, and require screening in two orthogonal planes. Another limitation is that, in the case of markedly degenerated joints, it may not always be possible to introduce a needle into the eroded joint cavity. Moreover, although joint blocks might appear to be more selective for joint disorders, there is no guarantee that local anaesthetic, injected intra-articularly, remains within a zygapophysial joint cavity. Any leakage outside the joint compromises the selectivity of the block. For this reason we do not believe C2-3 joint blocks are necessarily superior to third occipital nerve blocks as a screening procedure for pain from these joints. The procedure we used is notably free of risks or major side effects. There are no major structures in the region injected. The vertebral artery lies ventral to
5 On the concept of third occipital headache zygapophysial joints, and so is protected from inadvertent puncture, so long as a posterior approach to the third occipital nerve is used. The spinal cord lies well medial to the target site for the local anaesthetic blocks, and so is not at risk, but it is to ensure that needles are not deflected towards the cord that repeated fluoroscopic screening should be used to monitor the progress of the needle. Similarly, penetration of the epidural space is avoided by directing the course of the needle strictly towards the zygapophysial joint. There should be no risk of the anaesthetic tracking into the epidural space, so long as the ligamentum flavum is intact, for this structure seals off the epidural space from the posterior muscular compartment into which the anaesthetic is injected. Otherwise, those precautions appropriate to any procedure involving the injection of local anaesthetics, need to be taken. The syringe should be drawn back prior to injection to avoid inadvertent intravascular injection into an intra-muscular vein, and the operator should be fully prepared to deal with the consequences of systemic injection or the rare allergic reaction to local anaesthetic. There is, however, one possible side-effect peculiar to injections in the upper cervical region, and this the complaint of light-headedness, dizziness or slight ataxia. It is due to interference by the local anaesthetic with the proprioceptive afferents from the upper cervical muscles involved in the tonic neck reflex, and has been discussed in previous studies of upper cervical blocks.14 It was reported regularly by our patients who, indeed, were forewarned of the possibility. The effect never outlasted the duration of action of the local anaesthetic used, and usually waned well before the pain relief ceased. It was never serious or incapacitating. By forewarning patients, and coaching them to rely more on visual cues for balance (by concentrating on the horizontal when walking), and reassuring that it is only a temporary effect, this side effect is easily tolerated. Whereas third occipital nerve blocks can be used to demonstrate that a C2-3 zygapophysial joint is the source of pain, these blocks, per se, do not reveal its actual cause. However, the causative pathology, in our cases, was most likely traumatic arthropathy or degenerative joint disease. Patients 1, 3, 6 and 7 all had histories of recent injuries to the neck, and patient 4 had a history of epilepsy since childhood that involved frequent falls. Thus, all of these patients could be viewed as possibly having sustained an injury to a C2-3 zygapophysial joint. Patient 2 had a history of diffuse degenerative disease of the spine, and it seemed not inappropriate that, as part of this disease, her C2-3 joints were involved. Analysis of the clinical features of our patients 779 failed to reveal any feature that might be construed as pathognomonic of third occipital headache or that might be used as a specific indication for third occipital nerve blocks. Although restricted neck movements and zygapophysial tenderness were adopted as putatative diagnostic signs, these features occurred in patients who failed to respond to adequate blocks of the third occipital nerve. Furthermore, plain radiographs of the neck revealed no feature in any of our patients that could be construed as indicative of C2-3 arthropathy. Thus, the only diagnostic feature of third occipital headache is positive response to third occipital nerve blocks, and it is our suggestion that these blocks should be performed whenever an alternative diagnosis cannot be confirmed and when third occipital headache might be suspected in the differential diagnosis of occipital pain. Whereas we concluded that those patients who responsed to third occipital nerve blocks were suffering pain stemming from their C2-3 zygapophysial joints, this diagnosis was excluded in the three patients who did not respond. The associated features of nausea, vomiting and photophobia described by patient 10 allowed us to endorse the diagnosis of common migraine, and accordingly, it is not suiprising that he did not respond to cervical nerve blocks. Patients 8 and 9 did not have features that permitted a diagnosis of migraine to be made with any certainty, but in patient number 8 migraine was considered the most likely differential diagnosis, and he, like patient 10, was referred for further neurological management. The limitations of neck movements described by patient 9 still strongly suggested a cervical cause for his headache, but his failure to respond to third occipital and C2 ganglion blocks excluded a source of pain in the territories of these nerves, and he was referred for further investigation of his headaches and neck pain. The principal aim of our report has been to endorse the concept of headache mediated by the third occipital nerve and stemming from the C2-3 zygapophysial joints, and to describe a means of objectively screening for and confirming this diagnosis. It was not our intention to address the issue of treatment, for this is still being evaluated. Howevei, to assuage any lingering doubts about our proposed concept, we offer a brief summary of the therapeutic responses of our patients. The patients have variously been treated by several techniques. These include intra-articular injections of steroids, cryocoagulation and radiofrequency coagulation of the third occipital nerve, and even open neurectomy. When used, each of these techniques provided total and sustained relief from headache. The confounding issue, however, has been the longevity of response that we have attained. Steroids have worked
6 780 for periods of between 2 weeks and 4 months. Cryocoagulation has lasted between three and six weeks, while radiofrequency coagulation has produced relief in excess of 3 months, and has lasted 12 months in one case. Open neurectomy has achieved the longest responses, so far, of 18 and 24 months. We offer this summary of therapy, however, not to recommend any particular technique, but to illustrate that, having made the diagnosis of third occipital headache stemming from a C2-3 zygapophysial joint, treatment directed at either the joint or its nerve supply succeeded in producing relief. The recurrence of pain is the problem, but we do not interpret it as an indictment of the diagnosis, but rather as reflecting the limitations of the therapeutic techniques used. Steroids may not be applicable in arthropathy that is perhaps not inflammatory, and neurotomy is compromised by the eventual regeneration of the nerve. Our further studies are directed at refining the indications and optimal application of these techniques. With respect to open neurectomy, while this appeared a legitimate option in two of our early patients and was effective in relieving their headache, one of them developed neuroma pain that eventually had to be treated by C3 rhizotomy. It is because of the development of iatrogenic neuromata that we advise against using third occipital neurectomy until adequate means of combating neuroma formation are devised. It is perhaps remarkable that we identified seven patients with third occipital headache in a consecutive series of ten patients, but we point out that this was not due to any preselection on our part, and rather, probably reflects the referral pattern to our Pain Clinic at the time of the study. However, this high incidence may, alternatively, reflect an actual high incidence in the community of a condition that has remained unrecognised by specialists dealing with headache, and perhaps misdiagnosed as tension headache. It is for this reason, and lest such patients continue to remain unrecognised, that we report the concept of third occipital headache and a means for its objective diagnosis. In this context, third occipital headache must be viewed as only one of the possible differential diagnoses of headaches of cervical origin. As mentioned in the introduction, arthritis of the C1-2 joints is another possibility. However, at present, there are no established, validated clinical clues that might be used by a practitioner to determine beforehand which patients will respond to third occipital, as opposed to CI-2, or other, blocks. We suggest only that a high degree of suspicion be maintained in patients with occipital pain of unknown origin, and advise that an armamentarium of techniques is available to pursue the diagnosis. Descriptions of techniques to block the lat- Bogduk, Marsland eral atlanto-axial joints,9 the C2 ganglion,14 and the lower cervical dorsal rami'3 are available in the literature. To these we now add the technique for third occipital nerve blocks. References Ad Hoc Committee on Classification of Headache. Classification of headache. JAMA 1962;179: Adams RD. Headache. In: Petersdorf RG, Adams RD, Braunwald E, Isselbacher KJ, Martin JB, Wilson JD, eds. Harrison's Principles ofinternal Medicine. 10th ed. New York: MzGraw-Hill, 1983;Ch 3: Edmeads J. Headaches and head pains associated with diseases of the cervical spine. Med Clin North Am 1978;62: Friedman AP. Headache. In: Baker AB, Baker LH, eds. Clinical Neurology. Vol 2. Philadelphia: Harper and Row, 1983;Ch 13: Lance JW. Mechanism and Management of Headache. 4th ed. London: Butterworths, Wilkinson M. Symptomatology. In: Wilkinson M, ed. Cervical Spondylosis. 2nd ed. London: Heinemann, 1971;Ch 4: 'Brain L. Some unsolved problems of cervical spondylosis. Br Med J 1963;1: Fournier AM, Rathelot P. L'arthrose atlo-odontoidienne. Presse Medicale 1960;68: Ehni G, Benner B. Occipital neuralgia and the C1-2 arthrosis syndrome. J Neurosurg 1984;61: Mestdagh H. Morphological aspects and biomechanical properties of the vertebroaxial joint (C2-C3). Acta Morphol Neerlando-Scand 1976;14: l Trevor-Jones R. Osteoarthritis of the paravertebral joints of the second and third cervical vertebrae as a cause of occipital headache. S Afr Med J 1964;38: Maigne R,. Signes cliniques des cephalees cervicales: leur traitement. Medecine et Hygiene 1981;39: Bogduk N. The clinical anatomy of the cervical dorsal rami. Spine 1982;7: Bogduk N. Local anaesthetic blocks of the second cervical ganglion. A technique with application in occipital headache. Cephalalgia 1981;1: "5Kerr FWL. Structural relation of the trigeminal spinal tract to upper cervical roots and the solitary nucleus in the cat. Exp Neurol 1961;4: Escolar J. The afferent connections of the 1st, 2nd, and 3rd cervical nerves in the cat. J Comp Neurol 1948; 89: Kerr FWL, Olafson RA. Trigeminal and cervical volleys. Arch Neurol 1961;5: Cyriax J. Rheumatic headache. Br Med J 1938;2: Campbell DG, Parsons CM. Referred head pain and its concomitants. J Nerv Ment Dis 1944;99: Feinstein B,.Langton JBK, Jameson RM, Schiller F. Experiments on referred pain from deep somatic tissues. J Bone Joint Surg 1954;36A: McCall IW, Park WM, O'Brien JP. Induced pain referral from posterior lumbar elements in normal subjects. Spine 1979;4: Mooney V, Robertson J. The facet syndrome. Clin Orthop 1976;115:
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Cervical Cooled RF Training Presentation
 Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Dr Peter Gendall. Mr Steve August. Professor Nik Bogduk. Musculoskeletal Radiologist Hamilton. Physiotherapist Dunedin
 Professor Nik Bogduk Professor Pain Medicine University of Newcastle Mr Steve August Physiotherapist Dunedin Dr Peter Gendall Musculoskeletal Radiologist Hamilton 8:30-10:30 WS #5: Musculoskeletal Medicine
Professor Nik Bogduk Professor Pain Medicine University of Newcastle Mr Steve August Physiotherapist Dunedin Dr Peter Gendall Musculoskeletal Radiologist Hamilton 8:30-10:30 WS #5: Musculoskeletal Medicine
Cervical Spine Anatomy and Biomechanics. Typical Cervical Vertebra C3 6. Typical Cervical Vertebra Anterior 10/5/2017
 Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Technical Note NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE FLUOROSCOPIC VIEWS DURING CERVICAL RADIOFREQUENCY NEUROTOMY.
 Technical Note Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 4, pp127-131 2018, American Society of Interventional Pain Physicians NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE
Technical Note Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 4, pp127-131 2018, American Society of Interventional Pain Physicians NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
Bony framework of the vertebral column Structure of the vertebral column
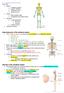 5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
SURGICAL AND RADIOGRAPHIC ANATOMY of LUMBAR RADIOFREQUENCY MEDIAL BRANCH NEUROTOMY
 SURGICAL AND RADIOGRAPHIC ANATOMY of LUMBAR RADIOFREQUENCY MEDIAL BRANCH NEUROTOMY Prepared for the Spine Intervention Society by Professor Nikolai Bogduk MD, PhD, DSc University of Newcastle, Royal Newcastle
SURGICAL AND RADIOGRAPHIC ANATOMY of LUMBAR RADIOFREQUENCY MEDIAL BRANCH NEUROTOMY Prepared for the Spine Intervention Society by Professor Nikolai Bogduk MD, PhD, DSc University of Newcastle, Royal Newcastle
E xperimental studies on normal volunteers have indicated
 88 PAPER Radiofrequency neurotomy for the treatment of third occipital headache J Govind, W King, B Bailey, N Bogduk... See end of article for authors affiliations... Correspondence to: Professor N Bogduk,
88 PAPER Radiofrequency neurotomy for the treatment of third occipital headache J Govind, W King, B Bailey, N Bogduk... See end of article for authors affiliations... Correspondence to: Professor N Bogduk,
Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D.
 Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D. Chest cavity - bony structures Chest cavity- bony structures Sternum Ribs True ribs: first seven pairs connect
Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D. Chest cavity - bony structures Chest cavity- bony structures Sternum Ribs True ribs: first seven pairs connect
Classification of the nervous system. Prof. Dr. Nikolai Lazarov 2
 1 1. Formation and general organization 2. Spinal ganglia 3. Zonal and segmental innervation 4. Dorsal rami of the spinal nerves 5. Ventral rami of the spinal nerves 6. Cervical plexus Classification of
1 1. Formation and general organization 2. Spinal ganglia 3. Zonal and segmental innervation 4. Dorsal rami of the spinal nerves 5. Ventral rami of the spinal nerves 6. Cervical plexus Classification of
The Back. Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa
 The Back Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa The spine has to meet 2 functions Strength Mobility Stability of the vertebral column is provided by: Deep intrinsic muscles of the back Ligaments
The Back Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa The spine has to meet 2 functions Strength Mobility Stability of the vertebral column is provided by: Deep intrinsic muscles of the back Ligaments
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
Transitioning to the Suboccipital Triangle. Suboccipital Triangle
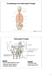 Transitioning to the Suboccipital Triangle Syllabus p. 14-15 Suboccipital Triangle Borders -Rectus capitis posterior major -Obliquus capitis superior -Obliquus capitis inferior Contents -Vertebral artery
Transitioning to the Suboccipital Triangle Syllabus p. 14-15 Suboccipital Triangle Borders -Rectus capitis posterior major -Obliquus capitis superior -Obliquus capitis inferior Contents -Vertebral artery
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5. September 30, 2011
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
Cervical Zygapophysial Joint Pain Maps
 Blackwell Publishing IncMalden, USAPMEPain Medicine526-2375American Academy of Pain Medicine? 200684344353 Original ArticleCervical Zygapophysial Joint Pain PatternsCooper et al. PAIN MEDICINE Volume 8
Blackwell Publishing IncMalden, USAPMEPain Medicine526-2375American Academy of Pain Medicine? 200684344353 Original ArticleCervical Zygapophysial Joint Pain PatternsCooper et al. PAIN MEDICINE Volume 8
Review Article. The Management of the Atlanto-Occipital and Atlanto-Axial Joint Pain
 Ogoke Atlanto-Occipital and Atlanto-Axial Joint Pain 289 Pain Physician, Volume 3, Number 3, pp 289-293 2000, Association of Pain Management Anesthesiologists Review Article The Management of the Atlanto-Occipital
Ogoke Atlanto-Occipital and Atlanto-Axial Joint Pain 289 Pain Physician, Volume 3, Number 3, pp 289-293 2000, Association of Pain Management Anesthesiologists Review Article The Management of the Atlanto-Occipital
THE VERTEBRAL COLUMN. Average adult length: In male: about 70 cms. In female: about 65 cms.
 THE VERTEBRAL COLUMN Average adult length: In male: about 70 cms. In female: about 65 cms. 1 Vertebral Column (Regions and Curvatures) Curvatures of the vertebral column: A. Primary curvature: C-shaped;
THE VERTEBRAL COLUMN Average adult length: In male: about 70 cms. In female: about 65 cms. 1 Vertebral Column (Regions and Curvatures) Curvatures of the vertebral column: A. Primary curvature: C-shaped;
US-GUIDED INTRA-ARTICULAR INJECTION TECHNIQUE OF FACETS JOINT
 US-GUIDED INTRA-ARTICULAR INJECTION TECHNIQUE OF FACETS JOINT www.ecografieinfiltrazioni.it Dott. Luca Di Sante LBP is a major cause of disability, the exact pathogenesis of acute LBP remains unclear The
US-GUIDED INTRA-ARTICULAR INJECTION TECHNIQUE OF FACETS JOINT www.ecografieinfiltrazioni.it Dott. Luca Di Sante LBP is a major cause of disability, the exact pathogenesis of acute LBP remains unclear The
Ultrasound-guided Pulsed Radiofrequency of the Third Occipital Nerve
 Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi. E mail: a.al E. mail:
 Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
VERTEBRAL COLUMN VERTEBRAL COLUMN
 VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
Cervical Cooled-RF Training Presentation
 Cervical Cooled-RF Training Presentation AGENDA Patient Selection Anatomy Overview Technique Diagnostic Block Cooled-RF Precautions Summary Patient Selection Cervical Zygapophyseal Joint Pain Cervical
Cervical Cooled-RF Training Presentation AGENDA Patient Selection Anatomy Overview Technique Diagnostic Block Cooled-RF Precautions Summary Patient Selection Cervical Zygapophyseal Joint Pain Cervical
Any of the vertebra in the cervical (neck) region of the spinal column. The cervical vertebra are the smallest vertebra in the spine, reflective of th
 Any of the vertebra in the cervical (neck) region of the spinal column. The cervical vertebra are the smallest vertebra in the spine, reflective of the fact that they support the least load. In humans,
Any of the vertebra in the cervical (neck) region of the spinal column. The cervical vertebra are the smallest vertebra in the spine, reflective of the fact that they support the least load. In humans,
Cervical Spine: Pearls and Pitfalls
 Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Anatomy and Physiology II. Spine
 Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Thoracic and Lumbar Spine Anatomy.
 Thoracic and Lumbar Spine Anatomy www.fisiokinesiterapia.biz Thoracic Vertebrae Bodies Pedicles Laminae Spinous Processes Transverse Processes Inferior & Superior Facets Distinguishing Feature Costal Fovea
Thoracic and Lumbar Spine Anatomy www.fisiokinesiterapia.biz Thoracic Vertebrae Bodies Pedicles Laminae Spinous Processes Transverse Processes Inferior & Superior Facets Distinguishing Feature Costal Fovea
_CH01redo.qxd 9/24/07 3:07 PM Page 1. [Half-Title to come]
![_CH01redo.qxd 9/24/07 3:07 PM Page 1. [Half-Title to come] _CH01redo.qxd 9/24/07 3:07 PM Page 1. [Half-Title to come]](/thumbs/81/84146690.jpg) 10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 1 [Half-Title to come] 10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 2 THE BACK Lippincott Williams & Wilkins atlas of ANATOMY CHAPTER 1 Plate 1-01 Palpable Structures
10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 1 [Half-Title to come] 10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 2 THE BACK Lippincott Williams & Wilkins atlas of ANATOMY CHAPTER 1 Plate 1-01 Palpable Structures
You have 24 vertebrae in your spinal column. Two are special enough to be individually named.
 You have 24 vertebrae in your spinal column. Two are special enough to be individually named. Your atlas (C01) and axis (C02) are very important vertebrae. Without them, head and neck movement would be
You have 24 vertebrae in your spinal column. Two are special enough to be individually named. Your atlas (C01) and axis (C02) are very important vertebrae. Without them, head and neck movement would be
An anatomical basis for the Neck-Tongue Syndrome
 Journal of Neurology, Neurosurgery, and Psychiatry, 1981, 44, 202-208 An anatomical basis for the Neck-Tongue Syndrome NIKOLAI BOGDUK From the Division of Neurology, The Prince Henry Hospital, Little Bay,
Journal of Neurology, Neurosurgery, and Psychiatry, 1981, 44, 202-208 An anatomical basis for the Neck-Tongue Syndrome NIKOLAI BOGDUK From the Division of Neurology, The Prince Henry Hospital, Little Bay,
The Back OUTLINE. Vertebral Column (review) Craniovertebral Joints Dorsal Scapular Region(review) Muscles of the Back Suboccipital Region
 The Back OUTLINE Vertebral Column (review) Craniovertebral Joints Dorsal Scapular Region(review) Muscles of the Back Suboccipital Region Dept. of Human Anatomy, Si Chuan University Zhou hongying eaglezhyxzy@163.com
The Back OUTLINE Vertebral Column (review) Craniovertebral Joints Dorsal Scapular Region(review) Muscles of the Back Suboccipital Region Dept. of Human Anatomy, Si Chuan University Zhou hongying eaglezhyxzy@163.com
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
The vault bones Frontal Parietals Occiput Temporals Sphenoid Ethmoid
 The Vertebral Column Head, Neck and Spine Bones of the head Some consider the bones of the head in terms of the vault bones and the facial bones hanging off the front of them The vault bones Frontal Parietals
The Vertebral Column Head, Neck and Spine Bones of the head Some consider the bones of the head in terms of the vault bones and the facial bones hanging off the front of them The vault bones Frontal Parietals
Gross Morphology of Spinal Cord
 Gross Morphology of Spinal Cord Done By : Rahmeh Alsukkar ** I did my best and sorry for any mistake ** the sheet does not contain pictures, tables and some slides so please be careful and go back to slides
Gross Morphology of Spinal Cord Done By : Rahmeh Alsukkar ** I did my best and sorry for any mistake ** the sheet does not contain pictures, tables and some slides so please be careful and go back to slides
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
Muscles of the Upper Limb that are dissected in the Back Region Muscle Origin Insertion Action Innervation Artery Notes
 Muscles of Upper Limb that are dissected in Back Region Muscle Origin Insertion Action Innervation Artery Notes floor of thoraco thoraco inserting spines from intertubercular arm nerve (C7,8) a. tendon
Muscles of Upper Limb that are dissected in Back Region Muscle Origin Insertion Action Innervation Artery Notes floor of thoraco thoraco inserting spines from intertubercular arm nerve (C7,8) a. tendon
Patient Information: Lumbar Rhizotomy (Facet medial branch neurotomy)
 Patient Information: Lumbar Rhizotomy (Facet medial branch neurotomy) WHAT IS IT? Lumbar rhizotomy (also called facet medial branch neurotomy) is a procedure to treat back pain. It involves placing needles
Patient Information: Lumbar Rhizotomy (Facet medial branch neurotomy) WHAT IS IT? Lumbar rhizotomy (also called facet medial branch neurotomy) is a procedure to treat back pain. It involves placing needles
Department of Neurology/Division of Anatomical Sciences
 Spinal Cord I Lecture Outline and Objectives CNS/Head and Neck Sequence TOPIC: FACULTY: THE SPINAL CORD AND SPINAL NERVES, Part I Department of Neurology/Division of Anatomical Sciences LECTURE: Monday,
Spinal Cord I Lecture Outline and Objectives CNS/Head and Neck Sequence TOPIC: FACULTY: THE SPINAL CORD AND SPINAL NERVES, Part I Department of Neurology/Division of Anatomical Sciences LECTURE: Monday,
Craniovertebral Junction Embryology and Anatomy. Presented by: Amandeep Moderators: S.S.Kale G.D.Satyarthi. CVJ-Embryology & Anatomy
 Craniovertebral Junction Embryology and Anatomy Presented by: Amandeep Moderators: S.S.Kale G.D.Satyarthi CVJ-Embryology & Anatomy CVJ-Embryology SOMITE-The building block of vertebrae, skeletal muscle
Craniovertebral Junction Embryology and Anatomy Presented by: Amandeep Moderators: S.S.Kale G.D.Satyarthi CVJ-Embryology & Anatomy CVJ-Embryology SOMITE-The building block of vertebrae, skeletal muscle
Gross Morphology of Spinal Cord
 Gross Morphology of Spinal Cord Lecture Objectives Describe the gross anatomical features of the spinal cord. Describe the level of the different spinal segments compared to the level of their respective
Gross Morphology of Spinal Cord Lecture Objectives Describe the gross anatomical features of the spinal cord. Describe the level of the different spinal segments compared to the level of their respective
Main Menu. Trunk and Spinal Column click here. The Power is in Your Hands
 1 The Trunk and Spinal Column click here Main Menu K.9 http://www.handsonlineeducation.com/classes/k9/k9entry.htm[3/27/18, 2:00:55 PM] The Trunk and Spinal Column Vertebral column complex 24 intricate
1 The Trunk and Spinal Column click here Main Menu K.9 http://www.handsonlineeducation.com/classes/k9/k9entry.htm[3/27/18, 2:00:55 PM] The Trunk and Spinal Column Vertebral column complex 24 intricate
Anatomy of the Thorax
 Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN
 INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN Dr John MacVicar, Medical Director Southern Rehab, Christchurch, NZ AOCPRM Nov 23 rd 2018 INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN An evidence-based
INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN Dr John MacVicar, Medical Director Southern Rehab, Christchurch, NZ AOCPRM Nov 23 rd 2018 INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN An evidence-based
VERTEBRAL COLUMN ANATOMY IN CNS COURSE
 VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
Facet syndrome in the cervical (upper) spine
 Dr. Michael J Walls, MD 320 Thomas More Parkway. Ste 202 Crestview Hills, KY 41017 Phone: (859) 331-0956 Facet syndrome in the cervical (upper) spine Cervical facet syndrome, also known as cervical facet
Dr. Michael J Walls, MD 320 Thomas More Parkway. Ste 202 Crestview Hills, KY 41017 Phone: (859) 331-0956 Facet syndrome in the cervical (upper) spine Cervical facet syndrome, also known as cervical facet
INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW
 INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW CDC REPORT - CAUSES OF DISABILITY, 2005 REVIEW QUESTIONS ABOUT DISC HERNIATION IN THE NATIONAL
INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW CDC REPORT - CAUSES OF DISABILITY, 2005 REVIEW QUESTIONS ABOUT DISC HERNIATION IN THE NATIONAL
Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms.
 RHEUMATOID SPINE Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms. When neurology is present it may manifest
RHEUMATOID SPINE Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms. When neurology is present it may manifest
Radiofrequency Ablation 101
 Radiofrequency Ablation 101 Neuroscience Summit September 10, 2016 Chris Pratt, DO Texas Health Care Pain Management 1651 West Rosedale Street, Suite #205 Fort Worth, Texas 71604 What s in a name? Radiofrequency
Radiofrequency Ablation 101 Neuroscience Summit September 10, 2016 Chris Pratt, DO Texas Health Care Pain Management 1651 West Rosedale Street, Suite #205 Fort Worth, Texas 71604 What s in a name? Radiofrequency
Structure and Function of the Vertebral Column
 Structure and Function of the Vertebral Column Posture Vertebral Alignment Does it really matter? Yes it does! Postural Curves The vertebral column has a series of counterbalancing curves posterior anterior
Structure and Function of the Vertebral Column Posture Vertebral Alignment Does it really matter? Yes it does! Postural Curves The vertebral column has a series of counterbalancing curves posterior anterior
Embriologically, The head is formed from the first two cervical segments (except the mandible, which is formed by the third). The first and second
 Embriologically, The head is formed from the first two cervical segments (except the mandible, which is formed by the third). The first and second cervical vertebra are also derived from these two segments.
Embriologically, The head is formed from the first two cervical segments (except the mandible, which is formed by the third). The first and second cervical vertebra are also derived from these two segments.
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Diagnostic cervical and lumbar medial branch blocks
 Considered Judgement Form This form is a checklist of issues that may be considered by the Purchasing Guidance Advisory Group when making purchasing recommendations Meeting date: 2 November 2015 Topic:
Considered Judgement Form This form is a checklist of issues that may be considered by the Purchasing Guidance Advisory Group when making purchasing recommendations Meeting date: 2 November 2015 Topic:
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E
 Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Fluoroscopically-Guided Injections to Treat Kissing Spine Disease
 Pain Physician 2008; 11:549-554 ISSN 1533-3159 Case Report Fluoroscopically-Guided Injections to Treat Kissing Spine Disease Timothy J. Lamer, MD 1, Jeffrey M. Tiede, MD 2 and Douglas S. Fenton, MD 3 From:
Pain Physician 2008; 11:549-554 ISSN 1533-3159 Case Report Fluoroscopically-Guided Injections to Treat Kissing Spine Disease Timothy J. Lamer, MD 1, Jeffrey M. Tiede, MD 2 and Douglas S. Fenton, MD 3 From:
Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS AND PAIN
 Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
2/5/2019. Facet Joint Pain. Biomechanics
 Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion
 Pain Physician 2011; 14:195-210 ISSN 1533-3159 Technical Report Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion Jie Zhu, MD 1,2, Frank J. E. Falco, MD 1, 2, C. Obi
Pain Physician 2011; 14:195-210 ISSN 1533-3159 Technical Report Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion Jie Zhu, MD 1,2, Frank J. E. Falco, MD 1, 2, C. Obi
Cervicogenic headache is characterized by a chronic unilateral
 Review Article Cervicogenic Headache Sithapan Munjupong, MD 1,2 Abstract Cervicogenic headache is characterized by chronic unilateral headache that is radiated from the upper cervical spine. The trigeminocervical
Review Article Cervicogenic Headache Sithapan Munjupong, MD 1,2 Abstract Cervicogenic headache is characterized by chronic unilateral headache that is radiated from the upper cervical spine. The trigeminocervical
Anatomy of the Spine. Figure 1. (left) The spine has three natural curves that form an S-shape; strong muscles keep our spine in alignment.
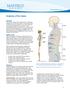 1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
1 Fatty Infiltration in the Cervical Extensor Muscles in Persistent Whiplash- Associated Disorders: A Magnetic Resonance Imaging Analysis
 1 Fatty Infiltration in the Cervical Extensor Muscles in Persistent Whiplash- Associated Disorders: A Magnetic Resonance Imaging Analysis Spine Volume 31(22) October 15, 2006 pp E847-E855 Elliott, James;
1 Fatty Infiltration in the Cervical Extensor Muscles in Persistent Whiplash- Associated Disorders: A Magnetic Resonance Imaging Analysis Spine Volume 31(22) October 15, 2006 pp E847-E855 Elliott, James;
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Diaphragm and intercostal muscles. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Cervical facet radiofrequency
 Techniques in Regional Anesthesia and Pain Management (2005) 9, 81-85 Cervical facet radiofrequency Ricardo Vallejo, MD, PhD, FIPP From the Millenium Pain Center, Bloomington, Illinois; and Illinois State
Techniques in Regional Anesthesia and Pain Management (2005) 9, 81-85 Cervical facet radiofrequency Ricardo Vallejo, MD, PhD, FIPP From the Millenium Pain Center, Bloomington, Illinois; and Illinois State
It consist of two components: the outer, laminar fibrous container (or annulus), and the inner, semifluid mass (the nucleus pulposus).
 Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
Lumbar Facet Joint Interventions
 Krishna Poddar, Rachit Gulati PRACTITIONERS SECTION 10.5005/jp-journals-10046-0063 1 Krishna Poddar, 2 Rachit Gulati ABSTRACT Facet joints or zygapophyseal joints are paired synovial joints in the vertebrae
Krishna Poddar, Rachit Gulati PRACTITIONERS SECTION 10.5005/jp-journals-10046-0063 1 Krishna Poddar, 2 Rachit Gulati ABSTRACT Facet joints or zygapophyseal joints are paired synovial joints in the vertebrae
Human Anatomy Biology 351
 nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
Spinal and Referred Pain Terminology
 Spinal and Referred Pain Terminology Concepts and Terms Jim Borowczyk and John MacVicar South GP CME 2017 Low Back Pain Lumbar Spinal Pain Is pain perceived as arising anywhere within a region bounded
Spinal and Referred Pain Terminology Concepts and Terms Jim Borowczyk and John MacVicar South GP CME 2017 Low Back Pain Lumbar Spinal Pain Is pain perceived as arising anywhere within a region bounded
8/4/2012. Causes and Cures. Nucleus pulposus. Annulus fibrosis. Vertebral end plate % water. Deforms under pressure
 Causes and Cures Intervertebral discs Facet (zygopophyseal) joints Inter body joints Spinal nerve roots Nerve compression Pathological conditions Video Causes of back pain Nucleus pulposus Annulus fibrosis
Causes and Cures Intervertebral discs Facet (zygopophyseal) joints Inter body joints Spinal nerve roots Nerve compression Pathological conditions Video Causes of back pain Nucleus pulposus Annulus fibrosis
Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain
 International Journal of Anesthesiology Research, 2015, 3, 37-43 37 Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain Michael Meng 1, Reid
International Journal of Anesthesiology Research, 2015, 3, 37-43 37 Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain Michael Meng 1, Reid
REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES
 REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES 1. A 28-year-old-women presented to the hospital emergency room with intense lower back spasms in the context of coughing during an upper respiratory
REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES 1. A 28-year-old-women presented to the hospital emergency room with intense lower back spasms in the context of coughing during an upper respiratory
POSTERIOR 1. situated behind: situated at or toward the hind part of the body :
 ANATOMICAL LOCATION Anatomy is a difficult subject with a large component of memorization. There is just no way around that, but we have made every effort to make this course diverse and fun. The first
ANATOMICAL LOCATION Anatomy is a difficult subject with a large component of memorization. There is just no way around that, but we have made every effort to make this course diverse and fun. The first
5 minutes: Attendance and Breath of Arrival. 50 minutes: Problem-Solving: Back
 Low Back Pain 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem-Solving: Back Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of
Low Back Pain 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem-Solving: Back Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of
SpineFAQs. Lumbar Spondylolisthesis
 SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
Re: Treatment Modalities for Facetogenic Pain, Policy #141
 March 30, 2017 Blue Cross and Blue Shield of Alabama Attn: Health Management - Medical Policy P.O. Box 995 Birmingham, AL 35298-0001 Fax: 205-220-0878 Re: Treatment Modalities for Facetogenic Pain, Policy
March 30, 2017 Blue Cross and Blue Shield of Alabama Attn: Health Management - Medical Policy P.O. Box 995 Birmingham, AL 35298-0001 Fax: 205-220-0878 Re: Treatment Modalities for Facetogenic Pain, Policy
CLINICAL NOTES. Aust. J. Physiother. 26:5, October,
 CLINICAL NOTES COMBINED MOVEMENTS IN THE CERVICAL SPINE (C2-7) THEIR VALUE IN EXAMINATION AND TECHNIQUE CHOICE Brian C. Edwards Private Practitioner Lecturer in Manipulative Therapy, Western Australian
CLINICAL NOTES COMBINED MOVEMENTS IN THE CERVICAL SPINE (C2-7) THEIR VALUE IN EXAMINATION AND TECHNIQUE CHOICE Brian C. Edwards Private Practitioner Lecturer in Manipulative Therapy, Western Australian
Neck Pain Guide. Understanding Causes, Treatment and Prevention
 Neck Pain Guide Understanding Causes, Treatment and Prevention Neck pain may be more than a nuisance; it could be a symptom of an underlying condition. Use this guide to help you understand common causes
Neck Pain Guide Understanding Causes, Treatment and Prevention Neck pain may be more than a nuisance; it could be a symptom of an underlying condition. Use this guide to help you understand common causes
2 Back and Spinal Cord
 2 Back and Spinal Cord Cards 2-1 to 2-24 Bones and Joints 2-1 Vertebral Column 2-2 Cervical Vertebrae 2-3 Thoracic Vertebrae 2-4 Lumbar Vertebra 2-5 Lumbar Vertebrae 2-6 Vertebral Ligaments: Lumbar Region
2 Back and Spinal Cord Cards 2-1 to 2-24 Bones and Joints 2-1 Vertebral Column 2-2 Cervical Vertebrae 2-3 Thoracic Vertebrae 2-4 Lumbar Vertebra 2-5 Lumbar Vertebrae 2-6 Vertebral Ligaments: Lumbar Region
Blair Radiology Exam Examination Packet
 Blair Radiology Exam Examination Packet This packet is made of up five sections: Examiner s Instructions, Applicant Requirements, Analysis Rubric, Overall Result and Comments and Exam Form. The Exam Form
Blair Radiology Exam Examination Packet This packet is made of up five sections: Examiner s Instructions, Applicant Requirements, Analysis Rubric, Overall Result and Comments and Exam Form. The Exam Form
THE OSTEOPATHIC WORKSHOP: NECK PAIN
 THE OSTEOPATHIC WORKSHOP: NECK PAIN Trevine R. Albert, D.O. M.S. Family Medicine Neuromusculoskeletal Medicine PGY-3 2018 FSACOFP Convention DISCLOSURES There are no actual or potential personal, financial
THE OSTEOPATHIC WORKSHOP: NECK PAIN Trevine R. Albert, D.O. M.S. Family Medicine Neuromusculoskeletal Medicine PGY-3 2018 FSACOFP Convention DISCLOSURES There are no actual or potential personal, financial
Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner
 Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner Eric Chaconas PT, PhD, DPT, FAAOMPT Assistant Professor and Assistant Program Director Doctor of Physical Therapy Program Eric
Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner Eric Chaconas PT, PhD, DPT, FAAOMPT Assistant Professor and Assistant Program Director Doctor of Physical Therapy Program Eric
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton
 Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Gross Anatomy of Lower Spinal Cord
 Chapter 13 Spinal Cord, Spinal Nerves and Somatic Reflexes Spinal cord Spinal nerves Somatic reflexes Gross Anatomy of Lower Spinal Cord Meninges of Vertebra & Spinal Cord Spina Bifida Congenital defect
Chapter 13 Spinal Cord, Spinal Nerves and Somatic Reflexes Spinal cord Spinal nerves Somatic reflexes Gross Anatomy of Lower Spinal Cord Meninges of Vertebra & Spinal Cord Spina Bifida Congenital defect
MEDICAL HISTORY CHIRO PHYSICAL
 Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
CERVICAL SPINE TIPS A
 CERVICAL SPINE TIPS A Musculoskeletal Approach to managing Neck Pain An ALGORITHM, as a management guide Rick Bernau & Ian Wallbridge June 2010 THE PROCESS An interactive approach to the management of
CERVICAL SPINE TIPS A Musculoskeletal Approach to managing Neck Pain An ALGORITHM, as a management guide Rick Bernau & Ian Wallbridge June 2010 THE PROCESS An interactive approach to the management of
Re: Occipital Neuralgia and Headache Treatment, Policy Number: 2018T0080Y
 May 10, 2018 United Healthcare Medical Policy Department 9500 Bren Road East Minnetonka, MN 55343 via Email: mpq@uhc.com Re: Occipital Neuralgia and Headache Treatment, Policy Number: 2018T0080Y To Whom
May 10, 2018 United Healthcare Medical Policy Department 9500 Bren Road East Minnetonka, MN 55343 via Email: mpq@uhc.com Re: Occipital Neuralgia and Headache Treatment, Policy Number: 2018T0080Y To Whom
SPINAL INJECTIONS SECTION 5 SPINAL INJECTION GUIDELINES 219
 SECTION 5 SPINAL INJECTIONS SPINAL INJECTION GUIDELINES 219 Overview 219 Safety 219 Accuracy 220 Efficacy 220 Indications for spinal injection 221 Summary 222 EXAMINATION OF THE SPINE 223 CAUDAL EPIDURAL
SECTION 5 SPINAL INJECTIONS SPINAL INJECTION GUIDELINES 219 Overview 219 Safety 219 Accuracy 220 Efficacy 220 Indications for spinal injection 221 Summary 222 EXAMINATION OF THE SPINE 223 CAUDAL EPIDURAL
human anatomy 2015 lecture four Dr meethak ali ahmed neurosurgeon
 The Vertebral Column the vertebral columnis central pillar of the body.it serve to protect the spinal cord and support the weight of the head trunk, which it transmits to the hip bones & the lower limbs.
The Vertebral Column the vertebral columnis central pillar of the body.it serve to protect the spinal cord and support the weight of the head trunk, which it transmits to the hip bones & the lower limbs.
Interventional Pain. Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care
 Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
STERNUM. Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts:
 STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
Imaging of Cervical Spine Trauma Tudor H Hughes, M.D.
 Imaging of Cervical Spine Trauma Tudor H Hughes, M.D. General Considerations Most spinal fractures are due to a single episode of major trauma. Fatigue fractures of the spine are unusual except in the
Imaging of Cervical Spine Trauma Tudor H Hughes, M.D. General Considerations Most spinal fractures are due to a single episode of major trauma. Fatigue fractures of the spine are unusual except in the
MD Bones & Joints of the Back. A/Prof Chris Briggs Department of Anatomy & Neuroscience
 MD 2017 Bones & Joints of the Back A/Prof Chris Briggs Department of Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
MD 2017 Bones & Joints of the Back A/Prof Chris Briggs Department of Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
A Patient s Guide to Pain Management: Radiofrequency Ablation
 A Patient s Guide to Pain Management: Radiofrequency Ablation 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Pain Management: Radiofrequency Ablation 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
ESSENTIALPRINCIPLES. Part II. Cervical Injuries
 ESSENTIALPRINCIPLES Part II Cervical Injuries By Ben E. Benjamin 86 MASSAGE & BODYWORK AUGUST/SEPTEMBER 2005 In the last article, we took a broad look at cervical injuries, discussing the anatomy of this
ESSENTIALPRINCIPLES Part II Cervical Injuries By Ben E. Benjamin 86 MASSAGE & BODYWORK AUGUST/SEPTEMBER 2005 In the last article, we took a broad look at cervical injuries, discussing the anatomy of this
