Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line.
|
|
|
- Frank Lang
- 5 years ago
- Views:
Transcription
1 Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma by written examination Isolate the main causes of facial trauma by written examination Define the geographic areas of the facial skeleton by written examination Define the most important aspect of prehospital care in facial trauma by examination
2 Facial Trauma This article deals with facial trauma, which is defined as injury to the soft tissues of the face (including the ear) and to the facial bony structure. Facial injuries require careful, thoughtful treatment because the patient s face is such a prime focus of attention by others. The cosmetic appearance of the face has an enormous impact on personality and social interactions. To allow features to be unnecessarily distorted as a result of inadequate care does great disservice to the patient and may lead to ongoing psychological problems. Facial trauma is a common problem in emergency medicine. It may be an isolated injury or may occur with other trauma. Although more than 50% of facial injuries in patients with major trauma continue to be caused by motor vehicle crashes, recent data indicate that the increasing use of active and passive automobile restraints is significantly reducing the frequency and magnitude of this problem. Other major causes of facial trauma include altercations, home accidents, athletic and work-related injuries, animal and human bites, domestic violence, and child abuse. In the pediatric age group, falls are a major cause of facial fractures, although some believe that pedantic facial trauma is relatively rare, composing less than 10% of all facial trauma seen in the general population. The presence of facial trauma in a child should immediately alert the paramedic to the possibility of child abuse or neglect. Increasing evidence also suggests that facial injuries may be a warning for possible domestic violence. Facial trauma usually presents a complex problem for the emergency room. The ability to provide definitive care depends on many variables. Multi-system trauma takes precedence, and the treatment of facial injuries may be relegated to a later time. Facial trauma also presents the problem of multi-turf territory, with
3 plastic surgeons, otolaryngologists, oral surgeons, and opthalmologists all laying claim to aspects of facial trauma (and often overlapping one another). The external bony facial skeleton is composed mainly of the frontal bone, temporal bones, nasal bone, zygomas, and mandible. These bones make up the horizontal and vertical buttresses that provide both support and strength to the face. The ethmoid, lacrimal and sphenoid bones contribute to the inner portions of the orbits. The facial skeleton is often divided into three geographic areas: the upper third, consisting of the section above the superior orbital rim; the middle third, or midface, consisting of the area from the superior orbital rim down through the maxillary teeth; and the lower third, consisting of the mandible. Facial Trauma may be classified as penetrating or blunt in origin. Penetrating trauma is more likely to produce a laceration, whereas blunt trauma is more likely to cause a contusion or bony disruption. A mixed class also exists. Facial trauma from vehicular crashes often involves rapid deceleration injuries, many of which could be avoided by using shoulder harnesses and having air bags in automobiles, and through helmet use by motorcycle riders. The speed at the time of the crash is important in terms of the disruptive tissue force generated. Evaluation starts with the history, and special attention to the mechanism of injury to determine which types of facial injury are probable and which must be ruled out. In some patients, obtaining the history comes only through us as paramedics before the patient becomes comatose. Make sure the receiving physician understands the mechanism of injury to enhance his clinical suspicions as to the nature of potential injuries. If the patient is cooperative, additional information can be sought about the location of facial pain, presence of diplopia or other vision problems, location of any facial numbness, pain on movement of the mandible, and presence of an abnormal bite.
4 Facial structures should be inspected for deformity and asymmetry, both of which may indicate underlying bony disruption. Documentation in the patient narrative of the appearance of the patient is important. By one estimate, up to 25% of all significant facial trauma cases result in litigation. Enophthalmos, the sinking of the eyeball into the orbit, or one eyeball looking in a different direction, (entrapment of inferior rectus muscle) must be specifically sought if a blowout fracture of the orbit is suspected. Ocular integrity and visual acuity, along with examination of extraocular movement should be included in your exam if life-threatening injuries are not present. The position and integrity of the nasal septum should be observed, and the presence of a septal hematoma should be sought. The patient should be observed for cerebrospinal fluid (CSF) rhinorrhea as an indication of a fracture of the cribriform plate or associated structures. The presence of a rapidly advancing outer ring when a drop of the discharge is placed on a gauze pad may indicate the presence of CSF. Motor sensory function should be evaluated next. The motor and sensory examination will be difficult or impossible in the patient with altered mental status and should be documented thoroughly in your patient narrative. All three major branches of the trigeminal nerve should be tested for sensation on each side of the face. Having the patient wrinkle the forehead, smile, bare the teeth and close the eye tightly checks motor function of the facial nerve. Palpation of the facial structures is the next step in the evaluation process. Tenderness, bony defects, creptius, and false motion should all be sought as evidence of disruption of the skeleton. Specific attention should be paid to the infraorbital and supraorbital ridges, the zygoma,
5 nasal bones, mandible, and lower maxilla. Make sure the teeth are not loose or blocking the airway. The most important aspect of prehospital care in facial trauma is the maintenance of a clear airway. Airway compromise can be a direct result of the injury, with disruption of the bony and cartilaginous architecture supporting the airway, or it may be caused by obstruction by soft tissue, hemorrhage, vomitus, or avulsed parts. If cervical spine injury is possible (e.g., by the mechanism of injury, an altered sensorium, or cervical spine tenderness) and if airway protection I required, careful oral intubation may be performed with cervical spine in-line stabilization. Nasotracheal intubation may also be performed after cervical spine immobilization, although this is controversial in patients with potential cribriform plate disruption. This procedure may also be contraindicated if laryngeal trauma may be present. In these cases, airway patency may be temporarily achieved by turning the patient to one side on a backboard after immobilization. Percutaneous transtracheal ventilation and cricothyrotomy are alternate modes of airway maintenance that may also be applicable in these patients. Most patients with facial trauma must be assumed, until proved otherwise, to have sustained cervical spine trauma. Initial management of the airway should include the removal of any loose material (teeth, blood clots, soft tissue, foreign material) from the oropharynx. If the patient is obtunded but breathing well, (pulse ox above 92%), without hemorrhage into the airway, an oropharyngeal or nasopharyngeal airway may be adequate to ensure airway patency. Shock, if present, must be treated. The presence of shock as a result of facial trauma alone is extremely rare, and an additional source must be sought. Hemorrhage caused by facial trauma usually can be controlled in the field with direct pressure. A pressure dressing may be helpful, but care must be taken not to compromise the airway.
6 Large avulsion flaps are best treated by the removal of gross contamination, irrigation with normal saline if conditions permit, and replacement of the flap on its bed. Foreign bodies impaled through the cheek may be removed in the field only when the airway is compromised. All other impaled foreign bodies should be left in place until surgery. Patients should be carefully stabilized before transport. All completely avulsed tissues and organs should be recovered, if possible, irrigated with normal saline and transported in an NSsoaked gauze sponge. This specifically applies to teeth, ears, the nose, and large soft tissue defects. As with any traumatic injury, the mechanism of injury should be assessed at the scene, with this information transmitted to the receiving hospital. This information is valuable in anticipating accompanying injuries and in determining priorities for the patient s care. It is important to document the patient s level of consciousness, sensory motor functions and any changes during transport. In all facial trauma, the paramedic should be alert to accompanying head injury.
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma The face is vital to human appearance and function. Facial injuries can impair a patient
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma The face is vital to human appearance and function. Facial injuries can impair a patient
Maxillofacial and Ocular Injuries
 Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Overview. Overview. Chapter 30. Injuries to the Head and Spine 9/11/2012. Review of the Nervous and Skeletal Systems. Devices for Immobilization
 Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
TRAUMA TO THE FACE AND MOUTH
 Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Ears. Mouth. Jowls 6 Major Bones of the Face Nasal bone Two
 1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
North Oaks Trauma Symposium Friday, November 3, 2017
 + Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
+ Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
Face and Throat Injuries. Chapter 26
 Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Skin Anatomy and Physiology
 Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Epidemiology 3002). Epidemiology and Pathophysiology
 Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Injuries to the head and spine
 Injuries to the head and spine Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Nervous System Two sub-systems Central Nervous System ( CNS ) Brain and spinal cord Peripheral Nervous System 12 cranial
Injuries to the head and spine Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Nervous System Two sub-systems Central Nervous System ( CNS ) Brain and spinal cord Peripheral Nervous System 12 cranial
Facial Trauma. Rural Emergency Services and Trauma Symposium 2008
 Rural Emergency Services and Trauma Symposium 2008 Facial Trauma Mitchell Stotland, MD Associate Professor of Surgery and Pediatrics Dartmouth-Hitchcock Medical Center Children s Hospital of Dartmouth
Rural Emergency Services and Trauma Symposium 2008 Facial Trauma Mitchell Stotland, MD Associate Professor of Surgery and Pediatrics Dartmouth-Hitchcock Medical Center Children s Hospital of Dartmouth
SPINAL IMMOBILIZATION
 Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
DR. SAAD AL-MUHAYAWI, M.D., FRCSC. ORL Head & Neck Surgery
 TRAUMA IN ORL DR. SAAD AL-MUHAYAWI, M.D., FRCSC Associate Professor & Consultant ORL Head & Neck Surgery TYPES OF TRAUMA EAR & TEMPORAL BONE TRAUMA NOSE & FACIAL BONES TRAUMA LARYNGEAL TRAUMA NECK TRAUMA
TRAUMA IN ORL DR. SAAD AL-MUHAYAWI, M.D., FRCSC Associate Professor & Consultant ORL Head & Neck Surgery TYPES OF TRAUMA EAR & TEMPORAL BONE TRAUMA NOSE & FACIAL BONES TRAUMA LARYNGEAL TRAUMA NECK TRAUMA
Oral and Maxillofacial Surgeons and the seriously injured patient. Barts and The London NHS Trust
 Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI. Monitor the vital signs. Monitor the vital signs. Complications of Facial Traumas.
 Complications of Facial Traumas 1) Immediate Complications 2) Late Complications Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor Oral & Maxillofacial Surgeon Taibah University Monitor
Complications of Facial Traumas 1) Immediate Complications 2) Late Complications Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor Oral & Maxillofacial Surgeon Taibah University Monitor
Bones of the skull & face
 Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and
 1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
Facial Sports Injuries
 Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Injuries to the Head and Spine
 Injuries to the Head and Spine Anatomy Review Skull Protects the brain Made up of several bones with seam like sutures Regions of the scalp-frontal, occipital, parietal, temporal Bones of face Orbits Mandible
Injuries to the Head and Spine Anatomy Review Skull Protects the brain Made up of several bones with seam like sutures Regions of the scalp-frontal, occipital, parietal, temporal Bones of face Orbits Mandible
Dr. Sami Zaqout, IUG Medical School
 The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
Basic Assessment and Treatment of Trauma
 Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
15. Facial and dental injuries
 15. Facial and dental injuries Priorities in management Best practice is based on current APLS / ATLS guidelines. Maxillofacial injuries will often take a lower priority than other potentially life or
15. Facial and dental injuries Priorities in management Best practice is based on current APLS / ATLS guidelines. Maxillofacial injuries will often take a lower priority than other potentially life or
Selective Spine Assessment & Spinal Motion Restriction
 Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition
 Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition 1. When performing the four-rescuer log roll, which responder pulls the board into position? A.) Head B.) Waist C.) Knee D.) Shoulder
Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition 1. When performing the four-rescuer log roll, which responder pulls the board into position? A.) Head B.) Waist C.) Knee D.) Shoulder
Focused History and Physical Examination of the
 Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
Chapter 11: Maxillofacial Trauma
 The American Academy of Otolaryngology Head and Neck Surgery Foundation (AAO-HNSF) Presents... Chapter 11: Maxillofacial Trauma Daiichi Pharmaceutical Corporation, marketers and distributors of FLOXIN
The American Academy of Otolaryngology Head and Neck Surgery Foundation (AAO-HNSF) Presents... Chapter 11: Maxillofacial Trauma Daiichi Pharmaceutical Corporation, marketers and distributors of FLOXIN
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
CT of Maxillofacial Injuries
 CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
Shenandoah Co. Fire & Rescue. Injuries to. and Spine. December EMS Training Bill Streett Training Section Chief
 Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Eyes, ears, teeth and everything in between
 Eyes, ears, teeth and everything in between E M E R G E N C Y D E P A R T M E N T J U N I O R T E A C H created 14/11/10 by S.R. Bruijns, version 1.0 Objectives Eyes Ears Teeth Maxilla- facial EYES Approaching
Eyes, ears, teeth and everything in between E M E R G E N C Y D E P A R T M E N T J U N I O R T E A C H created 14/11/10 by S.R. Bruijns, version 1.0 Objectives Eyes Ears Teeth Maxilla- facial EYES Approaching
Maxillofacial Injuries Practical Tips
 Saturday, October 29, 2016 Maxillofacial Injuries Practical Tips Suyash Mohan MD, PDCC THE ROOTS OF PENN RADIOLOGY RADIOLOGICAL Assistant Professor of Radiology Assistant Professor of Neurosurgery Neuroradiology
Saturday, October 29, 2016 Maxillofacial Injuries Practical Tips Suyash Mohan MD, PDCC THE ROOTS OF PENN RADIOLOGY RADIOLOGICAL Assistant Professor of Radiology Assistant Professor of Neurosurgery Neuroradiology
Abdomen and Genitalia Injuries. Chapter 28
 Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Chapter 27 - Face and Neck Injuries
 1 2 3 4 5 6 7 8 9 National EMS Education Standard Competencies (1 of 5) Medicine Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
1 2 3 4 5 6 7 8 9 National EMS Education Standard Competencies (1 of 5) Medicine Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
CT of Maxillofacial Fracture Patterns. CT of Maxillofacial Fracture Patterns
 CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
Assessment and Management of Ocular Trauma. Disclosure I have no direct financial interests in today s subject matter. 3/25/2019. Normal Eye Anatomy
 Assessment and Management of Ocular Trauma Samiksha Fouzdar Jain, MD,FRCS Department of Ophthalmology & Visual Sciences Truhlsen Eye Institute Disclosure I have no direct financial interests in today s
Assessment and Management of Ocular Trauma Samiksha Fouzdar Jain, MD,FRCS Department of Ophthalmology & Visual Sciences Truhlsen Eye Institute Disclosure I have no direct financial interests in today s
Chapter 7: Head & Neck
 Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
 Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Chapter 28. Objectives. Objectives 01/09/2013. Bleeding and Soft-Tissue Trauma
 Chapter 28 Bleeding and Soft-Tissue Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define
Chapter 28 Bleeding and Soft-Tissue Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define
Anatomy of. External NOSE. By Dr Farooq Aman Ullah Khan PMC
 Anatomy of External NOSE By Dr Farooq Aman Ullah Khan PMC 24 th Nov. 2017 The External Nose Descriptions of the nose always begin with that part of it which is covered by the skin, i.e., the EXPOSED PART
Anatomy of External NOSE By Dr Farooq Aman Ullah Khan PMC 24 th Nov. 2017 The External Nose Descriptions of the nose always begin with that part of it which is covered by the skin, i.e., the EXPOSED PART
Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. Railway accidents injured pedal cyclist
 Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. ICD Code ICD-9 E800-E807(.3) E810-E816, E818-E819(.6) E820-E825(.6) E826-E829(.1) ICD-10-CA V10-V19 (including all
Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. ICD Code ICD-9 E800-E807(.3) E810-E816, E818-E819(.6) E820-E825(.6) E826-E829(.1) ICD-10-CA V10-V19 (including all
Chapter 24 Soft Tissue Injuries Presentation Notes
 Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Clues of a Ruptured Globe
 Definition any eye that has sustained a full thickness traumatic disruption of the cornea or sclera Overwhelmingly, rupture accidents occur in young men, small children and the elderly Corneal laceration
Definition any eye that has sustained a full thickness traumatic disruption of the cornea or sclera Overwhelmingly, rupture accidents occur in young men, small children and the elderly Corneal laceration
Assessment of the Trauma Patient
 CHAPTER 10 Assessment of the Trauma Patient Overall Assessment Scheme Scene Size-Up Initial Assessment Trauma Physical Exam Vital Signs & SAMPLE History Medical SAMPLE History Physical Exam & Vital Signs
CHAPTER 10 Assessment of the Trauma Patient Overall Assessment Scheme Scene Size-Up Initial Assessment Trauma Physical Exam Vital Signs & SAMPLE History Medical SAMPLE History Physical Exam & Vital Signs
 International Trauma Life Support for Prehospital Care Providers Sixth Edition Patricia M. Hicks, MS, NREMTP Roy Alson, PhD, MD, FACEP Donna Hastings, EMT-P John Emory Campbell, MD, FACEP and Alabama Chapter,
International Trauma Life Support for Prehospital Care Providers Sixth Edition Patricia M. Hicks, MS, NREMTP Roy Alson, PhD, MD, FACEP Donna Hastings, EMT-P John Emory Campbell, MD, FACEP and Alabama Chapter,
TRAUMA PATIENT ASSESSMENT
 SECTION: Adult Trauma Emergencies PROTOCOL TITLE: Injury General Trauma Management REVISED: 06/2015 OVERVIEW Each year, one out of three Americans sustains a traumatic injury. Trauma is a major cause of
SECTION: Adult Trauma Emergencies PROTOCOL TITLE: Injury General Trauma Management REVISED: 06/2015 OVERVIEW Each year, one out of three Americans sustains a traumatic injury. Trauma is a major cause of
Pediatric Trauma Care
 2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
Chapter 7 Part A The Skeleton
 Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
MEDICAL CONTROL POLICY STATEMENT/ADVISORY. Re: Spinal Injury Assessment & Spinal Precautions Procedure
 MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
Trigeminal Nerve Worksheets, Distributions Page 1
 Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
oriented evaluation of your patient and establishing priorities of care based on existing and
 1 Chapter 12: Patient Assessment in the Field 2 Patient assessment means conducting a - oriented evaluation of your patient and establishing priorities of care based on existing and potential threats to
1 Chapter 12: Patient Assessment in the Field 2 Patient assessment means conducting a - oriented evaluation of your patient and establishing priorities of care based on existing and potential threats to
Dr. Sami Zaqout Faculty of Medicine IUG
 The Nose External Nose Nasal Cavity External Nose Blood and Nerve Supplies of the External Nose Blood Supply of the External Nose The skin of the external nose Branches of the ophthalmic and the maxillary
The Nose External Nose Nasal Cavity External Nose Blood and Nerve Supplies of the External Nose Blood Supply of the External Nose The skin of the external nose Branches of the ophthalmic and the maxillary
MRI masterfile Part 5 WM Heme Strokes.ppt 2
 Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
Student Notes Chapter 25: Face and Neck Injuries 1. Chapter 25. Face and Neck Injuries
 Student Notes Chapter 25: Face and Neck Injuries 1 Chapter 25 Face and Neck Injuries Unit Summary After students complete this chapter and the related course work, they will understand how to manage trauma-related
Student Notes Chapter 25: Face and Neck Injuries 1 Chapter 25 Face and Neck Injuries Unit Summary After students complete this chapter and the related course work, they will understand how to manage trauma-related
Sanders: Mosby's Paramedic Textbook, Revised 3 rd Edition PowerPoint Lecture Notes Chapter 24: Head and Facial Traumas
 Sanders: Mosby's Paramedic Textbook, Revised 3 rd Edition PowerPoint Lecture Notes Chapter 24: Head and Facial Traumas Chapter 24 Head and Facial Trauma Objectives Describe mechanism of injury, assessment,
Sanders: Mosby's Paramedic Textbook, Revised 3 rd Edition PowerPoint Lecture Notes Chapter 24: Head and Facial Traumas Chapter 24 Head and Facial Trauma Objectives Describe mechanism of injury, assessment,
HEAD AND NECK ANATOMY PRACTICE QUESTIONS
 HEAD AND NECK ANATOMY PRACTICE QUESTIONS 1. A patient complains that he has lost sensation on his face and that the skin of his face feels numb. The physician tests tactile acuity by touching the forehead
HEAD AND NECK ANATOMY PRACTICE QUESTIONS 1. A patient complains that he has lost sensation on his face and that the skin of his face feels numb. The physician tests tactile acuity by touching the forehead
Chapter 28 - Head and Spine Injuries
 1 2 3 4 National EMS Education Standard Competencies (1 of 4) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely injured
1 2 3 4 National EMS Education Standard Competencies (1 of 4) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely injured
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #2 Blunt Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #2 Blunt Trauma Blunt trauma is the most common cause of traumatic death and disability. The definition
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #2 Blunt Trauma Blunt trauma is the most common cause of traumatic death and disability. The definition
Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing
 1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D.
 1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
Older age, MVC and TBI higher incidence. Facial fractures a distracting injury? Carotid artery injury. Blindness may occur with facial fractures
 Dr Donald C. DeLisi Jr Oral & Maxillofacial Surgeon Multisystem injury 20 50% Nasal and mandibular fractures most common in community ED s Midface and zygomatic injuries most common in Trauma centers 25%
Dr Donald C. DeLisi Jr Oral & Maxillofacial Surgeon Multisystem injury 20 50% Nasal and mandibular fractures most common in community ED s Midface and zygomatic injuries most common in Trauma centers 25%
Skeletal System -Axial System. Chapter 7 Part A
 Skeletal System -Axial System Chapter 7 Part A Skeleton Learn: Names of the s. Identify specific landmarks that allow: Bones to fit into each other, Organs to fit into the cavities, Muscles to attach,
Skeletal System -Axial System Chapter 7 Part A Skeleton Learn: Names of the s. Identify specific landmarks that allow: Bones to fit into each other, Organs to fit into the cavities, Muscles to attach,
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
Facial Trauma ASHNR. Disclosures: Acknowledgments: None. Edward P. Quigley, III, MD PhD University of Utah
 Disclosures: Facial Trauma ASHNR Edward P. Quigley, III, MD PhD University of Utah None Acknowledgments: Dr. Rebecca Cornelius Dr. Ilona M. Schmalfuss Dr. Richard Wiggins III Dr. Yoshimi Anzai Dr. Lindell
Disclosures: Facial Trauma ASHNR Edward P. Quigley, III, MD PhD University of Utah None Acknowledgments: Dr. Rebecca Cornelius Dr. Ilona M. Schmalfuss Dr. Richard Wiggins III Dr. Yoshimi Anzai Dr. Lindell
Chapter 30 Putting It All Together for the Trauma Patient
 Chapter 30 Putting It All Together for the Trauma Patient Putting It All Together Balance need for prompt transport vs. treatment on scene. Select critical interventions to implement at scene of multipletrauma
Chapter 30 Putting It All Together for the Trauma Patient Putting It All Together Balance need for prompt transport vs. treatment on scene. Select critical interventions to implement at scene of multipletrauma
PTERYGOPALATINE FOSSA
 PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
Pre-hospital Trauma Life Support. Rattiya Banjungam Emergency Physician, Khon Kaen Hospital
 Pre-hospital Trauma Life Support Rattiya Banjungam Emergency Physician, Khon Kaen Hospital Golden principles of Prehospital Trauma Care Golden Hour There is a golden hour if you are critically injured,
Pre-hospital Trauma Life Support Rattiya Banjungam Emergency Physician, Khon Kaen Hospital Golden principles of Prehospital Trauma Care Golden Hour There is a golden hour if you are critically injured,
Nasal region. cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?
 Nasal region skull bones: nasal and frontal processes of maxilla cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?) 1 Nasal cavity Roof
Nasal region skull bones: nasal and frontal processes of maxilla cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?) 1 Nasal cavity Roof
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL
 What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton
 Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
EYE INJURIES OBJECTIVES COMMON EYE EMERGENCIES 7/19/2017 IMPROVE ASSESSMENT OF EYE INJURIES
 EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
Chapter 32. Objectives. Objectives 01/09/2013. Spinal Column and Spinal Cord Trauma
 Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
Face. Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face
 Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System
 1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
Facial Trauma Emergencies in Sports: Recognition and Management
 Facial Trauma Emergencies in Sports: Recognition and Management CENTRAL CONNECTICUT STATE UNIVERSITY SPORTS MEDICINE SYMPOSIUM MARCH 5, 2019 MARK C. FLETCHER, DMD, MD, FACS CLINICAL ASSISTANT PROFESSOR;
Facial Trauma Emergencies in Sports: Recognition and Management CENTRAL CONNECTICUT STATE UNIVERSITY SPORTS MEDICINE SYMPOSIUM MARCH 5, 2019 MARK C. FLETCHER, DMD, MD, FACS CLINICAL ASSISTANT PROFESSOR;
ATLS: Initial Assessment and Management. SAUSHEC Medical Student Lecture Series
 ATLS: Initial Assessment and Management SAUSHEC Medical Student Lecture Series Objectives Identify sequence of priorities in assessing the multiply injured patient Apply principles outlined in primary
ATLS: Initial Assessment and Management SAUSHEC Medical Student Lecture Series Objectives Identify sequence of priorities in assessing the multiply injured patient Apply principles outlined in primary
Ocular and Periocular Trauma. Tina Rutar, MD. Assistant Professor of Ophthalmology and Pediatrics. Director, Visual Center for the Child
 Ocular and Periocular Trauma Tina Rutar, MD Assistant Professor of Ophthalmology and Pediatrics Director, Visual Center for the Child University of California, San Francisco Phone: 415-353-2560 Fax: 415-353-2468
Ocular and Periocular Trauma Tina Rutar, MD Assistant Professor of Ophthalmology and Pediatrics Director, Visual Center for the Child University of California, San Francisco Phone: 415-353-2560 Fax: 415-353-2468
Chapter 7. Skeletal System
 Chapter 7 Skeletal System 1 Skull A. The skull is made up of 22 bones: 8 cranial bones, 13 facial bones, and the mandible. B. The Cranium encloses and protects the brain, provides attachments for muscles,
Chapter 7 Skeletal System 1 Skull A. The skull is made up of 22 bones: 8 cranial bones, 13 facial bones, and the mandible. B. The Cranium encloses and protects the brain, provides attachments for muscles,
3-Deep fascia: is absent (except over the parotid gland & buccopharngeal fascia covering the buccinator muscle)
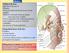 The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
Anatomy and Physiology of the Head 9/10/2015
 Kevin Badgley, E I/C Paramedic At the end of this seminar the participant will be able to: Describe potential facial injuries Describe potential complications of facial injuries Describe potential neck
Kevin Badgley, E I/C Paramedic At the end of this seminar the participant will be able to: Describe potential facial injuries Describe potential complications of facial injuries Describe potential neck
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
Facial and Temporal Bone Trauma Diagnostic imaging and therapeutic challenges in emergency
 Facial and Temporal Bone Trauma Diagnostic imaging and therapeutic challenges in emergency ATTYE A, KRAINIK A Department of Neuroradiology and MRI University Hospital Grenoble / University Grenoble Alpes
Facial and Temporal Bone Trauma Diagnostic imaging and therapeutic challenges in emergency ATTYE A, KRAINIK A Department of Neuroradiology and MRI University Hospital Grenoble / University Grenoble Alpes
MRI masterfile Part 5 WM Heme Strokes.ppt 1
 Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
EMS Spinal Assessment and Precautions
 EMS Spinal Assessment and Precautions Adapted from a presentation prepared by Chelsea C. White IV, MD, NREMT-P Medical Director, Bernalillo County Fire Department Robert M. Domeier, MD, EMS Medical Director,
EMS Spinal Assessment and Precautions Adapted from a presentation prepared by Chelsea C. White IV, MD, NREMT-P Medical Director, Bernalillo County Fire Department Robert M. Domeier, MD, EMS Medical Director,
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Restore adequate respiratory and circulatory conditions. Reduce pain
 Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
Trauma Registry Documentation December 16, 2014
 Trauma Registry Documentation December 16, 2014 The State of Florida now requires ALL Acute Care hospitals to submit data to the statetrauma Registry. Although Baptist Health hospitals are NOT Trauma Centers
Trauma Registry Documentation December 16, 2014 The State of Florida now requires ALL Acute Care hospitals to submit data to the statetrauma Registry. Although Baptist Health hospitals are NOT Trauma Centers
MASSACHUSETTS DEPARTMENT OF PUBLIC HEALTH OFFICE OF EMERGENCY MEDICAL SERVICES Basic EMT Practical Examination Cardiac Arrest Management
 Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
Skeletal system. Prof. Abdulameer Al-Nuaimi. E. mail:
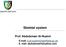 Skeletal system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Functions of Bone and The Skeletal System Support: The skeleton serves as the structural framework
Skeletal system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Functions of Bone and The Skeletal System Support: The skeleton serves as the structural framework
Ocular Urgencies and Emergencies
 Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
