Methods ORIGINAL ARTICLES ABSTRACT
|
|
|
- Elinor Fletcher
- 5 years ago
- Views:
Transcription
1 Bedside lung ultrasound, mobile radiography and physical examination: a comparative analysis of diagnostic tools in the critically ill Andrew J Inglis, Marek Nalos, Kwan-Hing Sue, Jan Hruby, Daniel M Campbell, Rachel M Braham, Sam R Orde Clinical examination of the respiratory system is a standard part of daily evaluation in the critically ill. Typically, physical examination (Ex) and bedside chest xray () are the mainstays of assessment, and computed tomography (CT) is considered the reference standard. 1,2 Significant limitations are associated with each of the methods. Ex is subjective and prone to inter-rater variability, and auscultation can be difficult in patients who are mechanically ventilated because transmitted sounds from the ventilator can alter pathologically significant sounds. 3,4 Portable, although done at the bedside with relatively rapid acquisition of results, is often hindered by inadequate patient positioning, the necessity for anteroposterior imaging and exposing patients to harmful radiation. CT provides superior imaging resolution and diagnostic accuracy but there are significant drawbacks to this technique, such as transport of unstable patients, logistical delays and considerable radiation exposure. The use of bedside lung ultrasound () in the intensive care unit is increasing due to its ease of use, accessibility, safety profile, immediate feedback and diagnostic accuracy. 1,2,5-9 Studies to date have focused on compared with reference standards such as CT, and have generally shown to have a high degree of diagnostic accuracy. 4,10 We aimed to study the performance and agreement of Ex, and in detecting and assessing the severity of pleural effusion, alveolar interstitial syndrome (AIS) and alveolar consolidation in critically ill patients. Methods Patients We prospectively included 145 adult ICU patients over a 1-year period at Nepean Hospital, Kingswood, New South Wales, Australia. Eighty-three patients were men and 62 were women, with an average age of 62 years (SD, 19 years). Sixty-three patients were mechanically ventilated. A primary respiratory condition was the most common reason for admission (37%); 19% of patients were admitted with a primary cardiovascular condition and 13% of patients were admitted for non-respiratory-related sepsis. The remainder were admitted for a variety of other indications, including seizures, acute renal failure, pancreatitis, trauma and diabetic ketoacidosis. The Nepean Blue Mountains ABSTRACT Objective: To compare lung ultrasonography (), chest xray () and physical examination (Ex) for the detection of pathological abnormalities in the lungs of critically ill patients. Design, setting and participants: A prospective cohort study of 145 patients in the intensive care unit of a tertiary teaching hospital who were undergoing echocardiography for a clinical indication. Main outcome measures: Each patient was independently assessed by Ex, and on the same day. Examiners were asked to comment on the presence or absence and severity of pleural effusion, lung consolidation and alveolar interstitial syndrome (AIS). Independent expert examiners performed the and an independent radiologist reported on the. Results: Ex, and were in fair agreement with each other in detecting a pulmonary abnormality ( v, κ = 0.31; v Ex, κ = 0.29; v Ex, κ = 0.22). detected more abnormalities than did (16.2%; c 2 = 64.1; P < 0.001) or Ex (23.5%; c 2 = 121.9; P < 0.001). detected more pleural effusions than (9.3%; c 2 = 7.6; κ = 0.39), but detected more pleural effusions than Ex (22.8%; c 2 = 36.4; κ = 0.18). There was no significant difference in the performance of and in quantifying the size of a pleural effusion (Z = 1.2; P = 0.23). Ex underestimated size compared with or. detected more consolidation than (17%; c 2 = 115.9; P < 0.001) and Ex (16.2%; c 2 = 90.3; P < 0.001). We saw no difference in performance between and Ex in detecting lung consolidation (0.9%; c 2 = 0.51; P < 0.48). detected more cases of AIS than (5.5%; c 2 = 7.9; P = 0.005) and Ex (13%; c 2 = 25.8; P < 0.001). Conclusions: There was only fair-to-moderate agreement between, and Ex in detecting pulmonary abnormalities, including pleural effusion, lung consolidation and AIS. The higher rate of detection from, combined with its ease of use and increasing accessibility, makes for a powerful diagnostic tool in the ICU. Crit Care Resusc 2016; 18:
2 Figure 1. Lung ultrasound and radiological analysis of pleural effusion = lung ultrasound. = chest x-ray. Absent = images of normal lungs. Small, moderate, large = volume of pleural effusion. R = right-sided probe position. L = left-sided probe position, in basal lung region, mid-axillary line. Human Research Ethics Committee approved the study, and authority for consent was waived because imaging was considered standard care in our ICU. Patients were included if they were undergoing a cardiac ultrasound (US) examination during their ICU stay. Lung ultrasonography was performed using a Vivid 7 or Vivid I echocardiography machine (GE Healthcare) by sonographers fully trained in echocardiography. The patients were positioned supine at 15 30, with their heads up. Six lung regions were examined: bilateral basal regions at the mid-axillary line at the level of intercostal spaces 6 10, with a posteriocaudal orientation of the US probe after correct position was ascertained by imaging of the diaphragm bilateral anterior intercostal spaces 2 3 in the midclavicular line bilateral anterior intercostal space 4 in the mid-clavicular line. Normal lung was defined as equidistant horizontal artefact lines (A-lines) being present, with no pathological changes seen, which represent reverberation artefact signals originating from the multiple reflections of the US signal between the pleural surface and the US transducer. The presence or absence of pleural effusion was recorded and, if present, the size of the effusions was recorded as small (maximal diameter, < 2 cm), moderate (maximal diameter, 2 4 cm) or large (maximal diameter, > 4 cm). Figure 1 compares the normal and examinations with pleural effusion of varying severity. An increasing hypoechoic signal on corresponds to fluid accumulation in the pleural cavity The presence or absence of lung consolidation in each region was also recorded, indicated by a liver-like or tissue appearance of the lung (known as sonographic hepatisation), with air bronchograms sometimes seen (Figure 2). 14,15 AIS was defined by the presence of B-lines or lung rockets. 6,16 These sonographic artefacts represent increased extravascular lung fluid. They take the appearance of hyperechoic beams resembling searchlights or the fire trail of an ascending rocket. These artefacts traverse the entire sonographic image. The presence of three to five B-lines was considered to represent interstitial accumulation of extravascular lung fluid. The presence of more than five B-lines was considered to represent consistent alveolar pulmonary oedema (see Figure 2). Chest radiography An independent radiologist (K-H S), blinded to the Ex or findings, reviewed all routine portable images taken in erect or semi-erect position. The lung zones were described as upper lung, mid-lung or lower lung fields, based on the upper and lower hilar line. The presence of pleural effusion was diagnosed when homogeneous opacification in the lower lung or mid-lung fields was present, with signs of typical gravity dependence. Pleural effusion was quantified based on estimated volumes (using meniscus position on imaging): small (< 400 ml), moderate ( ml) or large 117
3 Figure 2. Lung ultrasound and radiological analysis of consolidation and alveolar interstitial syndrome = lung ultrasound. = chest x-ray. Absent = images of normal lungs. probe positions: R2 = right second intercostal space, mid-clavicular line; L2 = left second intercostal space, mid-clavicular line; LB = left basal lung region, mid-axillary line. (> 800 ml). 17 Alveolar consolidation was defined as lungzone opacification with air bronchograms present. One or more of the following findings defined AIS: heterogeneous or patchy lung field opacification, septal (Kerley-B) lines and reticulonodular pattern. Physical examination We performed Ex by auscultation with the patient in the supine or semi-erect position (head of bed at 30 elevation) and classified results as normal, pleural effusion, consolidation or AIS, corresponding to the suggested definitions of Loudon and Murphy, 18 as have been used in previous studies. 4 Anterior, lateral and posterior lung regions on either side were systematically examined, with each region divided into an upper and lower region. A normal Ex result was defined as the presence of vesicular breath sounds and the absence of any adventitious sounds. Pleural effusion was defined as the absence of normal vesicular breath sounds. We asked the clinical examiner to estimate whether the pleural effusion was small, moderate or large, and this was largely subjective, based on the examiner s experience. The examiner also recorded the number of regions in which clinical signs were elucidated. Alveolar consolidation was identified by bronchial breath sounds, and AIS was identified by inspiratory crepitations or crackles. Fine crackles and coarse crackles were interpreted as low-severity and highseverity AIS, respectively. All modalities of assessment were completed as soon as practical, and always within 12 hours of each other. Statistical analysis We used SPSS Statistics, version 20 (IBM) for our statistical analysis. We collected all data in an ordinal format and tested measures of agreement using kappa analysis. When data were non-dichotomous, we used the weighted kappa statistic. Differences in the dichotomous data were analysed with McNemar analysis, using P < 0.05 to indicate statistical significance. The Wilcoxon rank sum test was used to compare differences in non-dichotomous data. We used a Bonferroni adjustment for the three-way comparison, hence P = was used as the cut-off in determining statistical significance. Results Normal v abnormal A total of 870 lung regions were examined by, and Ex. Out of 145 patients, identified 125 patients (86%) with some abnormality. Similarly, identified 120 patients (83%) with an abnormality, and Ex identified 84 patients (60%) with an abnormality. and agreed 65% of the time that an abnormality was present; and Ex 70% of the time, and and Ex 61% of the time. Table 1 outlines the performance of each of the diagnostic modalities as a three-way comparison of each of their abilities in detecting an abnormality (pleural effusion, consolidation or AIS). Each of, and Ex showed fair agreement with each other, but detected more 118
4 Table 1. Comparison of lung ultrasound, chest x-ray and physical examination for detecting any abnormality in critically ill patients Table 2. Comparison of lung ultrasound, chest x-ray and physical examination for detecting pleural effusion in critically ill patients Abnormality detected (n) PE detected (n) Abnormality detected No Yes Total k (P) c 2 (P) abnormalities than (436 v 295), which in turn detected more abnormalities than Ex (295 v 232). The difference in the percentage of lung regions that had abnormalities detected by compared with was 16.2% (95% CI, 12.5% 20%). The corresponding values for v Ex and v Ex were 7.2% (95% CI, 3.6% 10.9%) and 23.5% (95% CI, 19.6% 27.3%), respectively. Pleural effusion No Yes Total No Yes Total No Yes Total = chest x-ray. = lung ultrasound. k = kappa statistic. c 2 = McNemar test statistic. We examined 290 lung regions for pleural effusion (bilateral basal regions in each of 145 patients). Of the 145 patients, identified 98 patients (68%), identified 104 patients (72%) and Ex identified 48 patients (33%) with pleural effusion. and agreed in 69% of cases that a pleural effusion was present; and Ex agreed in 55% of cases; and agreed with Ex in 60% of cases (Table 2). had moderate agreement with and slight agreement with Ex findings. had slight agreement with Ex findings. was interpreted as positive for pleural effusion more often (165/290 regions) than each of (138/290 regions) and Ex (138/290 regions). The difference in the percentage of lung regions identified as having effusion, as detected by and, was 9.3% (95% CI, 3% 15.6%). Similarly, for v Ex, the proportion difference was 32% (95% CI, 25.3% 38.9%), and for v Ex, the corresponding value was 22.8% (95% CI, 16% 29.6%). is considered equal to CT for diagnosis of pleural PE detected No Yes Total k (P) c 2 (P) effusion and can be considered the gold standard. The diagnostic performance of was calculated as: sensitivity, 0.76; specificity, 0.62; and diagnostic accuracy, We determined the sensitivity of Ex to be 0.34; specificity, 0.84; and diagnostic accuracy, For quantifying the size of pleural effusion, exact agreement was achieved in 54% of cases between and ; 49% of cases between and Ex; and 52% of cases between and Ex. There was moderate agreement between and, slight agreement between and Ex, and slight agreement between and Ex (Table 3). However, according to Wilcoxon rank sum analysis, there was no significant difference between and in quantification of pleural effusions. Conversely, there was a significant difference in the quantification of pleural effusion between and Ex, with Ex underestimating severity compared with. Similarly, Ex underestimated size of pleural effusion when compared with. Lung consolidation No Yes Total (< 0.001) (0.006) No Yes Total No Yes Total (< 0.001) (<0.001) PE = pleural effusion. = chest x-ray. = lung ultrasound. k = kappa statistic. c 2 = McNemar test statistic. Of 145 patients examined, identified 102 patients with lung consolidation (70%), identified 38 patients (26%) and Ex identified 26 patients (18%). With examination for presence or absence of consolidation, there was agreement between and in 78% of cases, between and Ex in 89% of cases, and between and Ex in 75% of cases. There was only slight statistical agreement between each of the three modalities (Table 4). detected more 119
5 Table 3. Comparison of lung ultrasound (), chest x-ray () and physical examination (Ex) in quantifying the volume of pleural effusion (PE) in critically ill patients Volume of PE Absent Small Medium Large Total k Wilcoxon Volume of PE Absent <, 64 Small (P < 0.001) >, 70 Medium =, 156 Large Z = 1.2 Total P = 0.23 Absent Ex <, 116 Small (P = 0.001) Ex >, 31 Medium Ex =, 143 Large Z = 6.7 Total P < Absent Ex <, 109 Small (P = 0.002) Ex >, 29 Medium Ex =, 152 Large Z = 6.6 Total P = consolidation than either of and Ex. Compared with, differences in the proportion of the study population with positive results for were 17% (95% CI, 14.2% 20%) and, for Ex, 16.2% (95% CI, 13.1% 19.3%). There was no significant difference between and Ex in detecting consolidation, with a proportion difference of 0.9% (95% CI, 1.3% to 3.1%). Compared with, the sensitivity of was 0.17; specificity, 0.97; and diagnostic accuracy, Compared with, the sensitivity of Ex was calculated as 0.12; specificity, 0.94; and diagnostic accuracy, Alveolar interstitial syndrome Of the 145 patients, 90 (62%) were identified as having AIS using, 62 (43%) were identified with AIS using, and 52 (36%) were identified with AIS using Ex. Analysis for the presence or absence of AIS showed that agreed with in 68% of cases and with Ex in 77% of cases. There was agreement between and Ex in 67% of cases. Statistical agreement was slight, at best, between and each of Ex and, and there was no statistical agreement between and Ex. detected more cases of AIS than (5.5%; 95% CI, 1.8% 9.3%) and Ex (13%; 95% CI, 8.1% 17.8%). was shown to detect more AIS than Ex (4.5%; 95% CI, 1.3% 7.7%). Table 5 shows these comparisons. Absolute agreement between and in quantifying the severity of AIS was 65%. The corresponding value for comparison of with Ex was 73%, and for with Ex was 65%. Again, statistical agreement was only slight. Ex underestimated the severity of AIS compared with and ; although tended to underestimate AIS severity when compared with, the difference was not significant (Table 6). The sensitivity of was calculated as 0.25; specificity, 0.82; and diagnostic accuracy, The sensitivity of Ex was calculated as 0.14; specificity, 0.85; and diagnostic accuracy, Discussion We compared findings from bedside, portable and Ex in critically ill adult patients undergoing a transthoracic echocardiogram. We measured the ability of, and Ex to detect pleural effusion, lung consolidation and AIS. detected substantially more abnormalities than or Ex. Agreements between and, and between and Ex, were fair at best. The numbers of abnormalities detected by and Ex were more comparable. Given that there were consistently more abnormalities detected by, our data suggest that the cases in which and are in agreement are different from the cases in which and Ex are in agreement, which further highlights the potential 120
6 Table 4. Comparison of lung ultrasound, chest x-ray and physical examination in assessing the presence or absence of lung consolidation in critically ill patients Table 5. Comparison of lung ultrasound, chest x-ray and physical examination in assessing the presence or absence of alveolar interstitial syndrome in critically ill patients Consolidation detected (n) AIS detected (n) Consolidation detected No Yes Total k (P) c 2 (P) No Yes Total No Yes Total (< 0.001) (0.48) No Yes Total (0.002) (< 0.001) = chest x-ray. = lung ultrasound. k = kappa statistic. c 2 = McNemar test statistic. errors in interpretation of images and Ex findings. It should be noted that although detected substantially more abnormalities than, the numbers of patients detected with an abnormality using these techniques were comparable (86% using, and 83% using ). The likelihood that some patients had pathological changes in multiple lung regions may explain this. For example, a patient in whom four lung regions were identified as having pathological changes according to, but only two lung regions were identified as having pathological changes according to, would show that would detect more abnormalities, on a lung-region basis, while still identified the patient as having an abnormality. Pleural effusions were detected using each of the three techniques explored in this study. We found significant association between, and Ex in the detection and quantification of pleural effusions. and had moderate agreement for detection and quantification of the size of pleural effusions. When the two imaging modalities were compared with Ex, agreement was substantially smaller. detected considerably more pleural effusions than or Ex, and we believe this reflects the previously reported accuracy and superiority of the technique. 4,19,20 Lung consolidation was detected by with much greater frequency than by or Ex. This is shown in the absolute number of cases detected and supported by the large statistical differences we determined with the AIS detected No Yes Total k (P) c 2 (P) No Yes Total (0.019) (0.005) No Yes Total (< 0.001) (0.008) No Yes Total (0.6) (< 0.001) AIS = alveolar interstitial syndrome. = chest x-ray. = lung ultrasound. k = kappa statistic. c 2 = McNemar test statistic. McNemar test (Table 4). Additionally, no difference was observed in the cases determined to be either positive or negative for lung consolidation using the and Ex techniques. Except for the slight agreement between and Ex in detection of AIS, agreement between these techniques and failed to reach a level beyond that due to chance alone. However, the McNemar test revealed there was a significant difference between the number of cases of AIS detected by when compared with and Ex. Quantification of AIS showed modest agreement between the techniques. There have been several studies published that evaluate the performance of against other diagnostic techniques. 19,21-29 Essentially, these studies have repeatedly shown that has superior sensitivity and diagnostic accuracy in detecting various pulmonary pathological changes, compared with. Lichtenstein and colleagues directly compared with, auscultation and the gold standard CT, 4 but this study was designed to look at only the techniques themselves; a single clinician examining all patients with auscultation, a single operator acquiring and interpreting all images by, a single radiologist interpreting CT data and another radiologist interpreting plain films. Furthermore, the patients included in the study had already been diagnosed with, and were being treated for, acute respiratory distress syndrome. It was a well designed study but did not necessarily reflect how 121
7 Table 6. Comparison of lung ultrasound, chest x-ray and physical examination in assessing the severity of alveolar interstitial syndrome in critically ill patients AIS severity (n) Nil Low High Total k (P) Wilcoxon AIS level Nil <, 178 Low (0.012) >, 124 High =, 568 Total Z = 2.3 P = Nil < Ex, 99 Low (< 0.001) > Ex, 133 High = Ex, 638 Total Z = 2.5 P = Nil < Ex, 109 Low (0.301) > Ex, 197 High = Ex 564 Total Z = 4.6 P < AIS = alveolar interstitial syndrome. = chest x-ray. = lung ultrasound. k = kappa statistic. c 2 = McNemar test statistic. patients are assessed in an ICU. Typically, multiple clinicians are involved in patient assessment and interpretation of diagnostic imaging. It would therefore be useful to see how, and Ex agree with each other in daily practice. In other words, how well do the three diagnostic methods agree with each other given that, in reality, interobserver variability is not excluded? Our study did not make use of the gold standard CT technique, so agreement or disagreement between, and Ex can only be used as measures of consistency. However, Lichtenstein and colleagues have shown to perform extremely well when compared with CT in detecting effusion, consolidation and AIS. 4 Therefore, if one were to use as a surrogate standard for each of these pathological states, it can be shown that the technique outperforms both and Ex. A possible explanation may come from an understanding of the differences between the three pathological conditions examined in our study. Pleural effusion, lung consolidation and AIS all involve excess extravascular fluid within the chest cavity, and a factor to consider is the distribution of that fluid. Hence, it makes sense to define a ratio of volume:volumeof-distribution. In an appropriately positioned patient, the volume of fluid in pleural effusion accumulates in the most dependent space in the pleural cavity. AIS and lung consolidation involve excess extravascular fluid within the lung tissue. It can be argued that, in AIS, this extra fluid is distributed over a wider area, meaning its appearance on is less defined. In AIS, adventitious sounds heard on auscultation are also less defined and more likely to be masked by noises from a mechanical ventilator. Furthermore, the position of a patient may influence clinical signs of excess extravascular fluid. In pleural effusion, changes in the position of a patient will influence the regions in which clinical signs of excess fluid may be detected, as the fluid shifts with repositioning. 30 It was partly for this reason that we tried to maintain a consistent patient position for evaluation of respiratory pathological conditions. Gazon and colleagues have also performed an agreement analysis, comparing detection of each of the above pathological conditions with and. 28 In their study of 50 patients, they performed independent interpretation of the and images. Only moderate agreement between the two examination modalities was observed, similar to our findings. The selection criteria for Gazon and colleagues study included any patient whose clinical examination warranted further exploration for lung disease. Based on their screening, we would expect the prevalence of lung abnormality to be higher than in randomly selected patients, as was the case for our patients. 122
8 For the elements of Gazon and colleagues study that parallel ours (ie, v ), the determined measure of agreement (kappa) is comparable to that of our study for overall abnormality detection of v (0.42 v 0.31), pleural effusion (0.46 v 0.39) and alveolar consolidation (0.24 v 0.19); but kappa is not comparable for AIS (0.49 v 0.01). This can be readily explained by the effect of prevalence on the determination of kappa. In the absence of a gold standard of reference, our data, and those of Gazon and colleagues, rely on the observed marginal total values of the contingency tables. These may serve as surrogates for prevalence. 31 The observed marginal total affects kappa in much the same way as prevalence affects positive predictive values. 31 Our observed marginal frequencies for each of total abnormalities, pleural effusion and alveolar consolidation were comparable, but for AIS they were not. In the population we studied, AIS is a less common occurrence than in the population studied by Gazon and colleagues (98/200 patients were AIS-positive using in their study, compared with 217/870 AISpositive patients using in our study). Our study was affected by several limitations, the largest of which was the lack of comparison with CT imaging, regarded as the gold standard. We found that the number of patients who also had CT imaging (independently of our study) would not have contributed enough to our data for our population studied. Similar to the work of Lichtenstein and colleagues, 4 inclusion of comparison with CT imaging would have allowed us to derive sensitivity and specificity data. That data would have allowed us to more objectively compare the performance of the three other diagnostic modalities. However, as discussed above, CT has disadvantages that preclude its more routine use, and it is instructive to know how consistently, and Ex agree with each other in the diagnostic assessment of a patient. Given the already high sensitivity and specificity of for many lung conditions (including those dealt with here), our current data show that largely outperforms and Ex in detecting and quantifying the severity of some of the more common pulmonary conditions that occur in the ICU. Conclusion has a growing reputation for being a highly sensitive and specific diagnostic test for pulmonary conditions in hospitalised patients, including the critically ill. Our study shows the real-world performance of compared with bedside and Ex. The ability of to detect more abnormalities than the other two techniques makes it an attractive diagnostic tool for the treating physician. Future studies on interobserver variability of, Ex and would further aid in comparing how well each technique performs in diagnostic evaluation of critically ill patients in daily practice. Acknowledgements We thank the sonographers at Nepean Hospital Intensive Care Unit Cardiovascular Ultrasound Laboratory for their help in obtaining some of the images. Competing interests None declared. Author details Andrew J Inglis, Resident Marek Nalos, Intensivist Kwan-Hing Sue, Radiologist Jan Hruby, Anaesthetist Daniel M Campbell, Resident Rachel M Braham, Resident Sam R Orde, Intensivist Department of Intensive Care Medicine, Nepean Hospital, Sydney, NSW, Australia. Correspondence: mareknalos@gmail.com References 1 Lichtenstein DA. Lung ultrasound in the critically ill. Ann Intensive Care 2014; 4: 1. 2 Lichtenstein DA. Ultrasound examination of the lungs in the intensive care unit. Pediatr Crit Care Med 2009; 10: Brooks D, Thomas J. Interrater reliability of auscultation of breath sounds among physical therapists. Phys Ther 1995; 75: Lichtenstein D, Goldstein I, Mourgeon E, et al. Comparative diagnostic performances of auscultation, chest radiography, and lung ultrasonography in acute respiratory distress syndrome. Anesthesiol 2004; 100: Barillari A, Fioretti M. Lung ultrasound: a new tool for the emergency physician. Intern Emerg Med 2010; 5: Lichtenstein DA, Mezière GA, Lagoueyte J-F, et al. A-lines and B-lines: lung ultrasound as a bedside tool for predicting pulmonary artery occlusion pressure in the critically ill. Chest 2009; 136: Hew M, Heinze S. Chest ultrasound in practice: a review of utility in the clinical setting. Internal Med J 2012; 42: Volpicelli G. Point-of-care lung ultrasound. Praxis (Bern 1994) 2014; 103: Bouhemad B, Zhang M, Lu Q, Rouby J-J. Clinical review: bedside lung ultrasound in critical care practice. Crit Care 2007; 11: Nazerian P, Volpicelli G, Vanni S, et al. Accuracy of lung ultrasound for the diagnosis of consolidations when compared with chest computed tomography. Am J Emerg Med 2015; 33: Joyner CR, Herman RJ, Reid JM. Reflected ultrasound in the detection and localization of pleural effusion. JAMA 1967; 200: Sandweiss DA, Hanson JC, Gosink BB, Moser KM. Ultrasound in diagnosis, localization, and treatment of loculated pleural empyema. Ann Intern Med 1975; 82:
9 13 Doust BD, Baum JK, Maklad NF, Doust VL. Ultrasonic evaluation of pleural opacities. Radiol 1975; 114: Yang PC, Luh KT, Chang DB, et al. Ultrasonographic evaluation of pulmonary consolidation. Am Rev Respir Dis 1992; 146: Weinberg B, Diakoumakis EE, Kass EG, et al. The air bronchogram: sonographic demonstration. AJR Am J Roentgenol 1986; 147: Picano E, Frassi F, Agricola E, et al. Ultrasound lung comets: a clinically useful sign of extravascular lung water. J Am Soc Echocardiography 2006; 19: Blackmore CC, Black WC, Dallas RV, Crow HC. Pleural fluid volume estimation: a chest radiograph prediction rule. Acad Radiol 1996; 3: Loudon R, Murphy RL. Lung sounds. Am Rev Respir Dis 1984; 130: Xirouchaki N, Magkanas E, Vaporidi K, et al. Lung ultrasound in critically ill patients: comparison with bedside chest radiography. Intensive Care Med 2011; 37: Rocco M, Carbone I, Morelli A, et al. Diagnostic accuracy of bedside ultrasonography in the ICU: feasibility of detecting pulmonary effusion and lung contusion in patients on respiratory support after severe blunt thoracic trauma. Acta Anaesthesiol Scand 2008; 52: Bourcier J-E, Paquet J, Seinger M, et al. Performance comparison of lung ultrasound and chest x-ray for the diagnosis of pneumonia in the ED. Am J Emerg Med 2014; 32: Martindale JL, Noble VE, Liteplo A. Diagnosing pulmonary edema: lung ultrasound versus chest radiography. Eur J Emerg Med 2013; 20: Volpicelli G, Cardinale L, Berchialla P, et al. A comparison of different diagnostic tests in the bedside evaluation of pleuritic pain in the ED. Am J Emerg Med 2012; 30: Volpicelli G, Caramello V, Cardinale L, et al. Bedside ultrasound of the lung for the monitoring of acute decompensated heart failure. Am J Emerg Med 2008; 26: Baldi G, Gargani L, Abramo A, et al. Lung water assessment by lung ultrasonography in intensive care: a pilot study. Intensive Care Med 2013; 39: Cibinel GA, Casoli G, Elia F, et al. Diagnostic accuracy and reproducibility of pleural and lung ultrasound in discriminating cardiogenic causes of acute dyspnea in the emergency department. Intern Emerg Med 2012; 7: Cortellaro F, Colombo S, Coen D, Duca PG. Lung ultrasound is an accurate diagnostic tool for the diagnosis of pneumonia in the emergency department. Emerg Med J 2012; 29: Gazon M, Eboumbou N, Robert M-O, et al. Agreement between lung ultrasonography and chest radiography in the intensive care unit [French]. Ann Fr Anesth Reanim 2011; 30: Caiulo VA, Gargani L, Caiulo S, et al. Lung ultrasound in bronchiolitis: comparison with chest X-ray. Eur J Pediatr 2011; 170: Frasure SE, Matilsky DK, Siadecki SD, et al. Impact of patient positioning on lung ultrasound findings in acute heart failure. Eur Heart J Acute Cardiovasc Care 2015; 4: Feinstein AR, Cicchetti DV. High agreement but low kappa: I. The problems of two paradoxes. J Clin Epidemiol 1990; 43: o 124
Pediatric Lung Ultrasound (PLUS) In Diagnosis of Community Acquired Pneumonia (CAP)
 Pediatric Lung Ultrasound (PLUS) In Diagnosis of Community Acquired Pneumonia (CAP) Dr Neetu Talwar Senior Consultant, Pediatric Pulmonology Fortis Memorial Research Institute, Gurugram Study To compare
Pediatric Lung Ultrasound (PLUS) In Diagnosis of Community Acquired Pneumonia (CAP) Dr Neetu Talwar Senior Consultant, Pediatric Pulmonology Fortis Memorial Research Institute, Gurugram Study To compare
A Practical Approach to Ultrasound Assessment of Respiratory Distress
 A Practical Approach to Ultrasound Assessment of Respiratory Distress Yanick Beaulieu, MD, FRCPC Director, Bedside Ultrasound Curriculum Division of Cardiology and Critical Care Hôpital du Sacré-Coeur
A Practical Approach to Ultrasound Assessment of Respiratory Distress Yanick Beaulieu, MD, FRCPC Director, Bedside Ultrasound Curriculum Division of Cardiology and Critical Care Hôpital du Sacré-Coeur
Bedside Sonographic Diagnosis of Pneumothorax in Pediatric Patients: A Preliminary Report Chia-Wang Tang 1, Kai-Sheng Hsieh 1 1
 ORIGINAL ARTICLE Bedside Sonographic Diagnosis of in Pediatric Patients: A Preliminary Report Chia-Wang Tang 1, Kai-Sheng Hsieh 1 1 Division of Pediatric Pulmonology, Department of Pediatrics, Kaohsiung
ORIGINAL ARTICLE Bedside Sonographic Diagnosis of in Pediatric Patients: A Preliminary Report Chia-Wang Tang 1, Kai-Sheng Hsieh 1 1 Division of Pediatric Pulmonology, Department of Pediatrics, Kaohsiung
Chest Ultrasound: Pneumothorax
 WINFOCUS BASIC ECHO (WBE) Chest Ultrasound: Pneumothorax Mark Hamlin, MD, MS Associate Professor of Anesthesiology and Surgery University of Vermont College of Medicine Co-Director of Surgical Critical
WINFOCUS BASIC ECHO (WBE) Chest Ultrasound: Pneumothorax Mark Hamlin, MD, MS Associate Professor of Anesthesiology and Surgery University of Vermont College of Medicine Co-Director of Surgical Critical
ASSESSMENT OF LUNG PARENCHYMAL ABNORMALITIES
 2016 by the author Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as
2016 by the author Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as
Role of Transthoracic Ultrasound in Detection of Pneumonia in ICU Patients
 Med. J. Cairo Univ., Vol. 83, No. 1, June: 307-314, 2015 www.medicaljournalofcairouniversity.net Role of Transthoracic Ultrasound in Detection of Pneumonia in ICU Patients FARES AUF, M.D.; AHMED ABO-NAGLH,
Med. J. Cairo Univ., Vol. 83, No. 1, June: 307-314, 2015 www.medicaljournalofcairouniversity.net Role of Transthoracic Ultrasound in Detection of Pneumonia in ICU Patients FARES AUF, M.D.; AHMED ABO-NAGLH,
Lung ultrasound in the critically ill patient Pleural Effusions
 Lung ultrasound in the critically ill patient Pleural Effusions Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida
Lung ultrasound in the critically ill patient Pleural Effusions Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida
ULTRASONIC EVALUATION OF INTRATHORACIC MASSES
 ULTRASONIC EVALUATION OF INTRATHORACIC MASSES by Alan H. Wolson, MD ABSTRACT B mode ultrasound can be used to evaluate intrathoracic masses that contact the chest wall. It provides a noninvasive technique
ULTRASONIC EVALUATION OF INTRATHORACIC MASSES by Alan H. Wolson, MD ABSTRACT B mode ultrasound can be used to evaluate intrathoracic masses that contact the chest wall. It provides a noninvasive technique
The Intensive Care Unit
 Imaging of the ADRS patient: Risk of transportation and alternative to repetitive radiation exposure Jean-Jacques Rouby Pitié-Salpêtrière Hospital The Intensive Care Unit The Intensive Care Unit Multidisciplinary
Imaging of the ADRS patient: Risk of transportation and alternative to repetitive radiation exposure Jean-Jacques Rouby Pitié-Salpêtrière Hospital The Intensive Care Unit The Intensive Care Unit Multidisciplinary
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Lung
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Lung Page 1 of 8 01/17 Lung Syllabus Purpose: This unit is designed to cover the theoretical and practical curriculum for lung ultrasound in
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Lung Page 1 of 8 01/17 Lung Syllabus Purpose: This unit is designed to cover the theoretical and practical curriculum for lung ultrasound in
This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors.
 This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. - Figure S1: The four quadrant approach lung ultrasound at the bedside. * The anterolateral
This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. - Figure S1: The four quadrant approach lung ultrasound at the bedside. * The anterolateral
Using Lung Ultrasound to Diagnose and Manage Acute Heart Failure
 Using Lung Ultrasound to Diagnose and Manage Acute Heart Failure Jennifer Martindale, MD Assistant Professor Department of Emergency Medicine SUNY Downstate/Kings County Hospital Brooklyn, NY What is acute
Using Lung Ultrasound to Diagnose and Manage Acute Heart Failure Jennifer Martindale, MD Assistant Professor Department of Emergency Medicine SUNY Downstate/Kings County Hospital Brooklyn, NY What is acute
Definitions and diagnostic implications of terms used in the chest radiograph and lung ultrasound diagnoses of pneumonia.
 Supplementary 1 Definitions and diagnostic implications of terms used in the chest radiograph and lung ultrasound diagnoses of pneumonia. Imaging finding Definition Implication CR Consolidation Interstitial
Supplementary 1 Definitions and diagnostic implications of terms used in the chest radiograph and lung ultrasound diagnoses of pneumonia. Imaging finding Definition Implication CR Consolidation Interstitial
Lung ultrasound in critically ill patients: comparison with bedside chest radiography
 Intensive Care Med (2011) 37:1488 1493 DOI 10.1007/s00134-011-2317-y ORIGINAL Nektaria Xirouchaki Eleftherios Magkanas Katerina Vaporidi Eumorfia Kondili Maria Plataki Alexandros Patrianakos Evaggelia
Intensive Care Med (2011) 37:1488 1493 DOI 10.1007/s00134-011-2317-y ORIGINAL Nektaria Xirouchaki Eleftherios Magkanas Katerina Vaporidi Eumorfia Kondili Maria Plataki Alexandros Patrianakos Evaggelia
Lung sonography in the diagnosis of pneumothorax.
 Lung sonography in the diagnosis of pneumothorax. Poster No.: C-0526 Congress: ECR 2011 Type: Educational Exhibit Authors: K. Stefanidis, K. Vintzilaios, D. D. Cokkinos, E. Antypa, S. Dimopoulos, S. Nanas,
Lung sonography in the diagnosis of pneumothorax. Poster No.: C-0526 Congress: ECR 2011 Type: Educational Exhibit Authors: K. Stefanidis, K. Vintzilaios, D. D. Cokkinos, E. Antypa, S. Dimopoulos, S. Nanas,
Elderly Man with Dyspnoea
 Asia Pacific Family Medicine, 2004; 3 (1-2): 46-50 RADIOLOGY SERIES Elderly Man with Dyspnoea Wei-Yang LIM Faculty of Medicine National University of Singapore, Singapore Wilfred CG PEH Singapore Health
Asia Pacific Family Medicine, 2004; 3 (1-2): 46-50 RADIOLOGY SERIES Elderly Man with Dyspnoea Wei-Yang LIM Faculty of Medicine National University of Singapore, Singapore Wilfred CG PEH Singapore Health
Ultrasound. FAST Focused Assessment with Sonography in Trauma
 Ultrasound FAST Focused Assessment with Sonography in Trauma Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida
Ultrasound FAST Focused Assessment with Sonography in Trauma Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida
CLINICAL INVESTIGATIONS. Materials and Methods
 CLINICAL INVESTIGATIONS Anesthesiology 2004; 100:9 15 2004 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Comparative Diagnostic Performances of Auscultation, Chest Radiography,
CLINICAL INVESTIGATIONS Anesthesiology 2004; 100:9 15 2004 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Comparative Diagnostic Performances of Auscultation, Chest Radiography,
Accuracy of Lung Ultrasonography in Diagnosis of Community Acquired Pneumonia as Compared to Chest X-Ray in Pediatric Age Group
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (8), Page 4977-4983 Accuracy of Lung Ultrasonography in Diagnosis of Community Acquired Pneumonia as Compared to Chest X-Ray in Pediatric Age
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (8), Page 4977-4983 Accuracy of Lung Ultrasonography in Diagnosis of Community Acquired Pneumonia as Compared to Chest X-Ray in Pediatric Age
Point-of-care lung ultrasound
 Ultrasound Point-of-care lung ultrasound Philips tutorial Michael B. Stone, MD, RDMS Director, Division of Emergency Ultrasound Department of Emergency Medicine Brigham and Women s Hospital, Boston, MA
Ultrasound Point-of-care lung ultrasound Philips tutorial Michael B. Stone, MD, RDMS Director, Division of Emergency Ultrasound Department of Emergency Medicine Brigham and Women s Hospital, Boston, MA
Bedside ultrasound - Lung ultrasound in the Intensive Care Unit
 Bedside ultrasound - Lung ultrasound in the Intensive Care Unit Kishore K. Pichamuthu, Professor, Department of Critical Care, Christian Medical College, Vellore. Summary In an ICU setting, ultrasonographic
Bedside ultrasound - Lung ultrasound in the Intensive Care Unit Kishore K. Pichamuthu, Professor, Department of Critical Care, Christian Medical College, Vellore. Summary In an ICU setting, ultrasonographic
Unusual new signs of pneumothorax at lung ultrasound
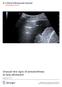 Unusual new signs of pneumothorax at lung ultrasound Volpicelli et al. Volpicelli et al. Critical Ultrasound Journal 2013, 5:10 Volpicelli et al. Critical Ultrasound Journal 2013, 5:10 SHORT COMMUNICATION
Unusual new signs of pneumothorax at lung ultrasound Volpicelli et al. Volpicelli et al. Critical Ultrasound Journal 2013, 5:10 Volpicelli et al. Critical Ultrasound Journal 2013, 5:10 SHORT COMMUNICATION
Role of Chest Ultrasonography in the Diagnosis of Acute Pulmonary Edema.
 Role of Chest Ultrasonography in the Diagnosis of Acute Pulmonary Edema Tamer Abudalla Helmy 1, Mamdouh Zidan 2 and Mohamed Khamis 1 1. Department of Critical Care Medicine, Faculty of Medicine, Alexandria
Role of Chest Ultrasonography in the Diagnosis of Acute Pulmonary Edema Tamer Abudalla Helmy 1, Mamdouh Zidan 2 and Mohamed Khamis 1 1. Department of Critical Care Medicine, Faculty of Medicine, Alexandria
Ultrasound in the ICU
 Ultrasound in the ICU Kristine E. W. Breyer, MD Assistant Professor Anesthesia & Critical Care Medicine UCSF DISCLOSURES: NONE Definition The Ultrasound Exam Types & Uses Training Clinical Examples Objectives
Ultrasound in the ICU Kristine E. W. Breyer, MD Assistant Professor Anesthesia & Critical Care Medicine UCSF DISCLOSURES: NONE Definition The Ultrasound Exam Types & Uses Training Clinical Examples Objectives
10/17/2016. Nuts and Bolts of Thoracic Radiology. Objectives. Techniques
 Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
CHEST Recent Advances in Chest Medicine
 CHEST Recent Advances in Chest Medicine Thoracic Ultrasonography for the Pulmonary Specialist Seth J. Koenig, MD; Mangala Narasimhan, DO, FCCP; and Paul H. Mayo, MD, FCCP Thoracic ultrasonography is a
CHEST Recent Advances in Chest Medicine Thoracic Ultrasonography for the Pulmonary Specialist Seth J. Koenig, MD; Mangala Narasimhan, DO, FCCP; and Paul H. Mayo, MD, FCCP Thoracic ultrasonography is a
Interpreting thoracic x-ray of the supine immobile patient: Syllabus
 Interpreting thoracic x-ray of the supine immobile patient: Syllabus Johannes Godt Dep. of Radiology and Nuclear Medicine Oslo University Hospital Ullevål NORDTER 2017, Helsinki Content - Why bedside chest
Interpreting thoracic x-ray of the supine immobile patient: Syllabus Johannes Godt Dep. of Radiology and Nuclear Medicine Oslo University Hospital Ullevål NORDTER 2017, Helsinki Content - Why bedside chest
Initially for cardiac echo Subsequent studies non-cardiac applications
 No disclosures But Heavy accent Initially for cardiac echo Subsequent studies non-cardiac applications 1973: Goldberg et al in JCUS 30 mediastinal masses in pts. age 1-84 yrs. 1977: Kangarloo et al in
No disclosures But Heavy accent Initially for cardiac echo Subsequent studies non-cardiac applications 1973: Goldberg et al in JCUS 30 mediastinal masses in pts. age 1-84 yrs. 1977: Kangarloo et al in
Role of chest ultrasonography in the prognostic evaluation of patients with community acquired pneumonia: a prospective study
 International Journal of Research in Medical Sciences Rennis KD et al. Int J Res Med Sci. 2017 Jan;5(1):25-30 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20164510
International Journal of Research in Medical Sciences Rennis KD et al. Int J Res Med Sci. 2017 Jan;5(1):25-30 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20164510
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
Lung ultrasound in the critically ill patient BASICS
 Lung ultrasound in the critically ill patient BASICS Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida Introduction
Lung ultrasound in the critically ill patient BASICS Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida Introduction
Lung Ultrasound in Diagnosis of Acute Respiratory Failure: BLUE Protocol Based Evaluation
 Lung Ultrasound in Diagnosis of Acute Respiratory Failure: BLUE Protocol Based Evaluation Niyas. K. Naseer 1, Muhammad Shafeek 2*, Rajani. M 3, Manoj. D. K 3 1Junior Resident, 2* Assistant Professor, 3
Lung Ultrasound in Diagnosis of Acute Respiratory Failure: BLUE Protocol Based Evaluation Niyas. K. Naseer 1, Muhammad Shafeek 2*, Rajani. M 3, Manoj. D. K 3 1Junior Resident, 2* Assistant Professor, 3
ARDS - a must know. Page 1 of 14
 ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
The efficacy of bedside chest ultrasound: from accuracy to outcomes
 EUROPEAN RESPIRATORY UPDATE EFFICACY OF BEDSIDE CHEST ULTRASOUND The efficacy of bedside chest ultrasound: from accuracy to outcomes Mark Hew 1,2 and Tunn Ren Tay 1,3 Affiliations: 1 Allergy, Immunology
EUROPEAN RESPIRATORY UPDATE EFFICACY OF BEDSIDE CHEST ULTRASOUND The efficacy of bedside chest ultrasound: from accuracy to outcomes Mark Hew 1,2 and Tunn Ren Tay 1,3 Affiliations: 1 Allergy, Immunology
Impact of lung ultrasound on clinical decision making in critically ill patients
 Intensive Care Med DOI 10.1007/s00134-013-3133-3 ORIGINAL Nektaria Xirouchaki Eumorfia Kondili George Prinianakis Polychronis Malliotakis Dimitrios Georgopoulos Impact of lung ultrasound on clinical decision
Intensive Care Med DOI 10.1007/s00134-013-3133-3 ORIGINAL Nektaria Xirouchaki Eumorfia Kondili George Prinianakis Polychronis Malliotakis Dimitrios Georgopoulos Impact of lung ultrasound on clinical decision
Landmark articles on ventilation
 Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
RSV infection and lung ultrasound
 RSV infection and lung ultrasound Neonatology Clinic, University Hospital, Krakow Joanna Hurkała Joanna Pietras Agnieszka Ochoda-Mazur Poznań, 28.09.2018 1 Disclosure In relations to this presentation,
RSV infection and lung ultrasound Neonatology Clinic, University Hospital, Krakow Joanna Hurkała Joanna Pietras Agnieszka Ochoda-Mazur Poznań, 28.09.2018 1 Disclosure In relations to this presentation,
4/16/2017. Learning Objectives. Interpretation of the Chest Radiograph. Components. Production of the Radiograph. Density & Appearance
 Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
OVERVIEW. Need for USG. Weaning assessment. Mechanics of USG. Pneumonia / VAP. Principles of lung USG. Prone position ventilation assessment
 OVERVIEW Need for USG Mechanics of USG Principles of lung USG BLUE protocol Alveolar syndrome Interstitial syndrome Weaning assessment Pneumonia / VAP Prone position ventilation assessment ETT positioning
OVERVIEW Need for USG Mechanics of USG Principles of lung USG BLUE protocol Alveolar syndrome Interstitial syndrome Weaning assessment Pneumonia / VAP Prone position ventilation assessment ETT positioning
Radiographic signs of pulmonary embolism and pulmonary infarction
 Thlorax (1973), 28, 198. Radiographic signs of pulmonary embolism and pulmonary infarction S. TALBOT, B. S. WORTHINGTON, and E. J. ROEBUCK General Hospital, Nottingham A comparative analysis of the radiographic
Thlorax (1973), 28, 198. Radiographic signs of pulmonary embolism and pulmonary infarction S. TALBOT, B. S. WORTHINGTON, and E. J. ROEBUCK General Hospital, Nottingham A comparative analysis of the radiographic
Quantification of pleural effusion on CT by simple measurement
 Quantification of pleural effusion on CT by simple measurement Martin Hazlinger a, Filip Ctvrtlik a, Katerina Langova b, Miroslav Herman a Aims. To find the simplest method for quantifying pleural effusion
Quantification of pleural effusion on CT by simple measurement Martin Hazlinger a, Filip Ctvrtlik a, Katerina Langova b, Miroslav Herman a Aims. To find the simplest method for quantifying pleural effusion
EVALUATION OF MODIFIED EXTRAORAL TECHNIQUE IN ZYGOMATIC ARCH EXAMINATION
 EVALUATION OF MODIFIED EXTRAORAL TECHNIQUE IN ZYGOMATIC ARCH EXAMINATION Aditya Dupare 1 *, Apeksha Dhole (Balpande) 2, Mukta Motwani 3, Anuraag Choudhary 4 1. Post graduate student, Department of oral
EVALUATION OF MODIFIED EXTRAORAL TECHNIQUE IN ZYGOMATIC ARCH EXAMINATION Aditya Dupare 1 *, Apeksha Dhole (Balpande) 2, Mukta Motwani 3, Anuraag Choudhary 4 1. Post graduate student, Department of oral
A pictorial review of thoracic imaging of intensive care patients
 A pictorial review of thoracic imaging of intensive care patients Poster No.: C-1003 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: E. Y. P. Lee, H. C. Mathias; Cardiff/UK Keywords:
A pictorial review of thoracic imaging of intensive care patients Poster No.: C-1003 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: E. Y. P. Lee, H. C. Mathias; Cardiff/UK Keywords:
Robert Erickson, RRT-NPS, RPFT
 Robert Erickson, RRT-NPS, RPFT Clinical Systems Manager Respiratory Care Community Hospital, Munster Indiana Community Healthcare System boberrtrpft@gmail.com This work is licensed under a Creative Commons
Robert Erickson, RRT-NPS, RPFT Clinical Systems Manager Respiratory Care Community Hospital, Munster Indiana Community Healthcare System boberrtrpft@gmail.com This work is licensed under a Creative Commons
Lung ultrasound for the diagnosis of community-acquired pneumonia in children
 Pediatr Radiol (2017) 47:1412 1419 DOI 10.1007/s00247-017-3910-1 MINISYMPOSIUM: IMAGING PNEUMONIA Lung ultrasound for the diagnosis of community-acquired pneumonia in children Jacob A. M. Stadler 1 & Savvas
Pediatr Radiol (2017) 47:1412 1419 DOI 10.1007/s00247-017-3910-1 MINISYMPOSIUM: IMAGING PNEUMONIA Lung ultrasound for the diagnosis of community-acquired pneumonia in children Jacob A. M. Stadler 1 & Savvas
Case N 1. Anterior thoracic paint with increasing dyspnea for few days. No cough. Decrease of cardiac sounds. Courtesy Dr Van den Homberg-Tanzania
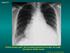 Case N 1 Anterior thoracic paint with increasing dyspnea for few days. No cough. Decrease of cardiac sounds Courtesy Dr Van den Homberg-Tanzania Case N 1 Enlargment of cardiac silhouette. Notice the symetry
Case N 1 Anterior thoracic paint with increasing dyspnea for few days. No cough. Decrease of cardiac sounds Courtesy Dr Van den Homberg-Tanzania Case N 1 Enlargment of cardiac silhouette. Notice the symetry
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Lung
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Lung ASUM Quality CCPU Syllabi Released: 21 March 2013 Approved by: CEO Lung Purpose: This unit is designed to cover the theoretical and practical
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Lung ASUM Quality CCPU Syllabi Released: 21 March 2013 Approved by: CEO Lung Purpose: This unit is designed to cover the theoretical and practical
Objectives. The Extended FAST Exam. Focused Assessment e With Sonography In. Trauma (FAST)
 Northern California Emergency Ultrasound Course Objectives The Extended FAST Exam Rimon Bengiamin, MD, RDMS UC SF Discuss the components of the EFAST exam Evaluate the utility of the EFAST Review how to
Northern California Emergency Ultrasound Course Objectives The Extended FAST Exam Rimon Bengiamin, MD, RDMS UC SF Discuss the components of the EFAST exam Evaluate the utility of the EFAST Review how to
The new ARDS definitions: what does it mean?
 The new ARDS definitions: what does it mean? Richard Beale 7 th September 2012 METHODS ESICM convened an international panel of experts, with representation of ATS and SCCM The objectives were to update
The new ARDS definitions: what does it mean? Richard Beale 7 th September 2012 METHODS ESICM convened an international panel of experts, with representation of ATS and SCCM The objectives were to update
Using Ultrasound Lung Comets in the Diagnosis of High Altitude Pulmonary Edema: Fact or Fiction?
 WILDERNESS & ENVIRONMENTAL MEDICINE, 24, 159 164 (2013) REVIEW ARTICLE Using Ultrasound Lung Comets in the Diagnosis of High Altitude Pulmonary Edema: Fact or Fiction? Yashvi Wimalasena, BM, FCEM, DiMM;
WILDERNESS & ENVIRONMENTAL MEDICINE, 24, 159 164 (2013) REVIEW ARTICLE Using Ultrasound Lung Comets in the Diagnosis of High Altitude Pulmonary Edema: Fact or Fiction? Yashvi Wimalasena, BM, FCEM, DiMM;
Non Invasive Hemodynamic Monitoring in the ED
 Is haemodinamic monitoring useful in the ED? Non Invasive Hemodynamic Monitoring in the ED Roberta PETRINO Director Emergency Medicine Unit S. Andrea Hospital, Vercelli - Italy EuSEM Vice-president Helps
Is haemodinamic monitoring useful in the ED? Non Invasive Hemodynamic Monitoring in the ED Roberta PETRINO Director Emergency Medicine Unit S. Andrea Hospital, Vercelli - Italy EuSEM Vice-president Helps
Accuracy of lung ultrasonography in diagnosis of community acquired pneumonia in hospitalized children as compared to chest x-ray
 International Journal of Contemporary Pediatrics Tirdia PR et al. Int J Contemp Pediatr. 2016 Aug;3(3):1026-1031 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Research Article DOI: http://dx.doi.org/10.18203/2349-3291.ijcp20162385
International Journal of Contemporary Pediatrics Tirdia PR et al. Int J Contemp Pediatr. 2016 Aug;3(3):1026-1031 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Research Article DOI: http://dx.doi.org/10.18203/2349-3291.ijcp20162385
Extended FAST Exam. Goal of Trauma Care. Golden Hour of Trauma
 Extended FAST Exam Goal of Trauma Care Golden Hour of Trauma Best INITIAL screening modality in trauma efast 2014 LLSA Article (ACEP Policy Statement) Level B Recommendation: In hemodynamically unstable
Extended FAST Exam Goal of Trauma Care Golden Hour of Trauma Best INITIAL screening modality in trauma efast 2014 LLSA Article (ACEP Policy Statement) Level B Recommendation: In hemodynamically unstable
Chest X rays and Case Studies. No disclosures. Outline 5/31/2018. Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital
 Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Auscultation of the lung
 Auscultation of the lung Auscultation of the lung by the stethoscope. *Compositions of the stethoscope: 1-chest piece 2-Ear piece 3-Rubber tubs *Auscultation area of the lung(triangle of auscultation).
Auscultation of the lung Auscultation of the lung by the stethoscope. *Compositions of the stethoscope: 1-chest piece 2-Ear piece 3-Rubber tubs *Auscultation area of the lung(triangle of auscultation).
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Lung
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Lung Page 1 of 8 12/15 Lung Syllabus Purpose: This unit is designed to cover the theoretical and practical curriculum for lung ultrasound in
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Lung Page 1 of 8 12/15 Lung Syllabus Purpose: This unit is designed to cover the theoretical and practical curriculum for lung ultrasound in
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous structures - Significant thoracic inj
 PEDIATRIC CHEST TRAUMA Children are not small adults Role of imaging Spectrum of injury Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous
PEDIATRIC CHEST TRAUMA Children are not small adults Role of imaging Spectrum of injury Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous
Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations
 Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations TECHNICAL EVALUATION 1. Projection: AP/PA view To differentiate between AP & PA films,
Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations TECHNICAL EVALUATION 1. Projection: AP/PA view To differentiate between AP & PA films,
POCUS for the Internist: Lungs & Pericardial Effusions
 POCUS for the Internist: Lungs & Pericardial Effusions Jeremy S. Boyd, MD, FACEP Asst. Professor of Emergency Medicine Vanderbilt University Medical Illustrations courtesy of Robinson Ferre, MD, FACEP
POCUS for the Internist: Lungs & Pericardial Effusions Jeremy S. Boyd, MD, FACEP Asst. Professor of Emergency Medicine Vanderbilt University Medical Illustrations courtesy of Robinson Ferre, MD, FACEP
UERMMMC Department of Radiology. Basic Chest Radiology
 UERMMMC Department of Radiology Basic Chest Radiology PHYSICS DENSITIES BONE SOFT TISSUES WATER FAT AIR TELEROENTGENOGRAM Criteria for an Ideal Chest Radiograph 1. Upright 2. Posteroanterior View 3. Full
UERMMMC Department of Radiology Basic Chest Radiology PHYSICS DENSITIES BONE SOFT TISSUES WATER FAT AIR TELEROENTGENOGRAM Criteria for an Ideal Chest Radiograph 1. Upright 2. Posteroanterior View 3. Full
Chest X-ray Interpretation
 Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
The Irregular Diaphragmatic Pleural Interface
 CSE SERIES The Irregular Diaphragmatic Pleural Interface Novel Sonographic Sign Facilitating the Diagnosis of Pneumonia Jacob O. vila, MD, RDMS, Vicki E. Noble, MD Videos online at www.jultrasoundmed.org
CSE SERIES The Irregular Diaphragmatic Pleural Interface Novel Sonographic Sign Facilitating the Diagnosis of Pneumonia Jacob O. vila, MD, RDMS, Vicki E. Noble, MD Videos online at www.jultrasoundmed.org
TB Radiology for Nurses Garold O. Minns, MD
 TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
Most infants and children admitted to
 Paediatrica Indonesiana VOLUME 53 January NUMBER 1 Original Article Correlation between chest x-ray findings and outcomes of patients with mechanical ventilation Indah Nurhayati 1, Muhammad Supriatna 1,
Paediatrica Indonesiana VOLUME 53 January NUMBER 1 Original Article Correlation between chest x-ray findings and outcomes of patients with mechanical ventilation Indah Nurhayati 1, Muhammad Supriatna 1,
Original Article. Summary
 Original Article doi:10.1111/anae.14243 Lung ultrasound compared with chest X-ray in diagnosing postoperative pulmonary complications following cardiothoracic surgery: a prospective observational study*
Original Article doi:10.1111/anae.14243 Lung ultrasound compared with chest X-ray in diagnosing postoperative pulmonary complications following cardiothoracic surgery: a prospective observational study*
8.0 Parenteral Nutrition vs. Standard care May 2015
 8.0 Parenteral Nutrition vs. Standard care May 015 015 Recommendation: Based on 6 level studies, in critically ill patients with an intact gastrointestinal tract, we recommend that parenteral nutrition
8.0 Parenteral Nutrition vs. Standard care May 015 015 Recommendation: Based on 6 level studies, in critically ill patients with an intact gastrointestinal tract, we recommend that parenteral nutrition
CHEST INJURY PULMONARY CONTUSION
 CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
BIOE221. Session 5. Examination of Thorax- Respiratory system. Bioscience Department. Endeavour College of Natural Health endeavour.edu.
 BIOE221 Session 5 Examination of Thorax- Respiratory system Bioscience Department Session Objectives Understand the structure of the thorax and the organs contained in this cavity Understand the importance
BIOE221 Session 5 Examination of Thorax- Respiratory system Bioscience Department Session Objectives Understand the structure of the thorax and the organs contained in this cavity Understand the importance
Differential diagnosis
 Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
MINERVA MEDICA COPYRIGHT REVIEW ARTICLE D. LICHTENSTEIN. Resuscitation Service, Ambroise-Paré Hospital, Boulogne, France ABSTRACT
 MINERVA ANESTESIOL 2009;75:313-7 REVIEW ARTICLE Lung ultrasound in acute respiratory failure an introduction to the BLUE-protocol D. Resuscitation Service, Ambroise-Paré Hospital, Boulogne, France ABSTRACT
MINERVA ANESTESIOL 2009;75:313-7 REVIEW ARTICLE Lung ultrasound in acute respiratory failure an introduction to the BLUE-protocol D. Resuscitation Service, Ambroise-Paré Hospital, Boulogne, France ABSTRACT
Interactive Lecture. Lecture 7 - Interactive. Radiology of cardiorespiratory disease. Editing File. Done By. Color Coding Important Notes Extra
 Lecture 7 - Interactive 436 Teams Interactive Lecture Radiology of cardiorespiratory disease Done By Team Leaders: Khalid Alshehri Hanin Bashaikh Team Members: Ghaida Alsaeed Maha Alissa Nawwaf AlHarbi
Lecture 7 - Interactive 436 Teams Interactive Lecture Radiology of cardiorespiratory disease Done By Team Leaders: Khalid Alshehri Hanin Bashaikh Team Members: Ghaida Alsaeed Maha Alissa Nawwaf AlHarbi
Inter-Observer and Intra-Observer Variability In the Assessment of The Paranasal Sinuses Radiographs
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 5 Number 2 Inter-Observer and Intra-Observer Variability In the Assessment of The Paranasal Sinuses Radiographs A Norie, R Ahmad, W Liew, M
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 5 Number 2 Inter-Observer and Intra-Observer Variability In the Assessment of The Paranasal Sinuses Radiographs A Norie, R Ahmad, W Liew, M
Lung ultrasound in follow-up of low birth weight with respiratory distress syndrome: clinical application and reduction of x-rays examinations
 Lung ultrasound in follow-up of low birth weight with respiratory distress syndrome: clinical application and reduction of x-rays examinations Poster No.: C-1724 Congress: ECR 2011 Type: Scientific Paper
Lung ultrasound in follow-up of low birth weight with respiratory distress syndrome: clinical application and reduction of x-rays examinations Poster No.: C-1724 Congress: ECR 2011 Type: Scientific Paper
Pulmonary Embolism. Thoracic radiologist Helena Lauri
 Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Pulmonary Ultrasound in Emergency Medicine and Critical Care
 Pulmonary Ultrasound in Emergency Medicine and Critical Care www.rmgultrasound.com Author: Virginia M Stewart, MD RDMS RDCS RDMSK Dr Stewart is a practicing Emergency Physician in Eastern Virginia, USA.
Pulmonary Ultrasound in Emergency Medicine and Critical Care www.rmgultrasound.com Author: Virginia M Stewart, MD RDMS RDCS RDMSK Dr Stewart is a practicing Emergency Physician in Eastern Virginia, USA.
Identification of lung sliding: a basic ultrasound technique with a steep learning curve
 SIGNA VITAE 2013; 8(1): 31-35 ORIGINAL Identification of lung sliding: a basic ultrasound technique with a steep learning curve MATEJ STRNAD SABINA ZADEL ZALIKA KLEMENC-KETIS MATEJ STRNAD ( ) SABINA ZADEL
SIGNA VITAE 2013; 8(1): 31-35 ORIGINAL Identification of lung sliding: a basic ultrasound technique with a steep learning curve MATEJ STRNAD SABINA ZADEL ZALIKA KLEMENC-KETIS MATEJ STRNAD ( ) SABINA ZADEL
Diagnostic Accuracy of Ultrasonography in the Acute Assessment of Common Thoracic Lesions After Trauma
 CHEST Original Research CRITICAL CARE Diagnostic Accuracy of Ultrasonography in the Acute Assessment of Common Thoracic Lesions After Trauma Anne-Claire Hyacinthe, MD ; Christophe Broux, MD ; Gilles Francony,
CHEST Original Research CRITICAL CARE Diagnostic Accuracy of Ultrasonography in the Acute Assessment of Common Thoracic Lesions After Trauma Anne-Claire Hyacinthe, MD ; Christophe Broux, MD ; Gilles Francony,
NON INVASIVE LIFE SAVERS. Ultrasound in PICU
 VOL 1 NO.1 Jan March 2014 54 Table 1. Selected Applications of Point-of-Care Ultrasonography, According to Medical Specialty. Specialty Ultrasound Applications Anesthesia Cardiology Guidance for vascular
VOL 1 NO.1 Jan March 2014 54 Table 1. Selected Applications of Point-of-Care Ultrasonography, According to Medical Specialty. Specialty Ultrasound Applications Anesthesia Cardiology Guidance for vascular
8/14/2017. Objective: correlate radiographic findings of common lung diseases to actual lung pathologic features
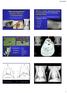 What is that lung disease? Pulmonary Patterns & Correlated Pathology Dr. Russell Tucker, DACVR Objective: correlate radiographic findings of common lung diseases to actual lung pathologic features Improved
What is that lung disease? Pulmonary Patterns & Correlated Pathology Dr. Russell Tucker, DACVR Objective: correlate radiographic findings of common lung diseases to actual lung pathologic features Improved
Lung ultrasound: Present and future
 Review Article Lung ultrasound: Present and future Ashish Saraogi Department of Anaesthesiology, National Institute of Medical Sciences and Research, Jaipur, Rajasthan, India ABSTRACT The scope of ultrasound
Review Article Lung ultrasound: Present and future Ashish Saraogi Department of Anaesthesiology, National Institute of Medical Sciences and Research, Jaipur, Rajasthan, India ABSTRACT The scope of ultrasound
Case Study #2. Case Study #1 cont 9/28/2011. CAPA 2011 Christy Wilson PA C. LH is 78 yowf with PMHx of metz breast CA presents
 Case Study #1 CAPA 2011 Christy Wilson PA C 46 yo female presents with community acquired PNA (CAP). Her condition worsened and she was transferred to the ICU and placed on mechanical ventilation. Describe
Case Study #1 CAPA 2011 Christy Wilson PA C 46 yo female presents with community acquired PNA (CAP). Her condition worsened and she was transferred to the ICU and placed on mechanical ventilation. Describe
Min Hur, Eun-Hee Kim, In-Kyung Song, Ji-Hyun Lee, Hee-Soo Kim, and Jin Tae Kim INTRODUCTION. Clinical Research
 Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Huan Ma 1,2 *, Daozheng Huang 3 *, Liheng Guo 2, Quanfu Chen 2, Wenzhao Zhong 4, Qingshan Geng 1, Minzhou Zhang 2.
 Original Article Strong correlation between lung ultrasound and chest computerized tomography imaging for the detection of acute lung injury/acute respiratory distress syndrome in rats Huan Ma 1,2 *, Daozheng
Original Article Strong correlation between lung ultrasound and chest computerized tomography imaging for the detection of acute lung injury/acute respiratory distress syndrome in rats Huan Ma 1,2 *, Daozheng
Radiology of the respiratory/cardiac diseases (part 2)
 Cardiology Cycle - Lecture 6 436 Teams Radiology of the respiratory/cardiac diseases (part 2) Objectives Done By Team Leaders: Khalid Alshehri Hanin Bashaikh Team Members: Leena Alwakeel Aroob Alhuthail
Cardiology Cycle - Lecture 6 436 Teams Radiology of the respiratory/cardiac diseases (part 2) Objectives Done By Team Leaders: Khalid Alshehri Hanin Bashaikh Team Members: Leena Alwakeel Aroob Alhuthail
Introduction to Chest Radiography
 Introduction to Chest Radiography RSTH 366: DIAGNOSTIC TECHNIQUES Alan Alipoon BS, RCP, RRT Instructor Department of Cardiopulmonary Sciences 1 Introduction Discovered in 1895 by Wilhelm Roentgen Terminology
Introduction to Chest Radiography RSTH 366: DIAGNOSTIC TECHNIQUES Alan Alipoon BS, RCP, RRT Instructor Department of Cardiopulmonary Sciences 1 Introduction Discovered in 1895 by Wilhelm Roentgen Terminology
Differentiation of Pleural Effusions From Parenchymal Opacities: Accuracy of Bedside Chest Radiography
 Cardiopulmonary Imaging Original Research Kitazono et al. Chest Radiography of Pleural Effusions Cardiopulmonary Imaging Original Research Mary T. Kitazono 1 Charles T. Lau Andrea N. Parada Pooja Renjen
Cardiopulmonary Imaging Original Research Kitazono et al. Chest Radiography of Pleural Effusions Cardiopulmonary Imaging Original Research Mary T. Kitazono 1 Charles T. Lau Andrea N. Parada Pooja Renjen
d) Always ensure patient comfort. Be considerate and warm the diaphragm of your stethoscope with your hand before auscultation.
 Auscultation Auscultation is perhaps the most important and effective clinical technique you will ever learn for evaluating a patient s respiratory function. Before you begin, there are certain things
Auscultation Auscultation is perhaps the most important and effective clinical technique you will ever learn for evaluating a patient s respiratory function. Before you begin, there are certain things
Original article Paediatrics Today 2016;12(1): DOI /p
 Original article Paediatrics Today 2016;12(1):139-148 DOI 10.5457/p2005-114.150 ABDOMINAL ULTRASOUND IN CHILDREN - ARE WE CAREFUL ENOUGH WHEN IT COMES TO LUNG BASES? Jovan LOVRENSKI 1*, Dajana POPADIĆ
Original article Paediatrics Today 2016;12(1):139-148 DOI 10.5457/p2005-114.150 ABDOMINAL ULTRASOUND IN CHILDREN - ARE WE CAREFUL ENOUGH WHEN IT COMES TO LUNG BASES? Jovan LOVRENSKI 1*, Dajana POPADIĆ
(true) Disease Condition Test + Total + a. a + b True Positive False Positive c. c + d False Negative True Negative Total a + c b + d a + b + c + d
 Biostatistics and Research Design in Dentistry Reading Assignment Measuring the accuracy of diagnostic procedures and Using sensitivity and specificity to revise probabilities, in Chapter 12 of Dawson
Biostatistics and Research Design in Dentistry Reading Assignment Measuring the accuracy of diagnostic procedures and Using sensitivity and specificity to revise probabilities, in Chapter 12 of Dawson
Radiological evaluation of neonatal lesions in 118 neonates
 Original Research Article ISSN: 394-006 (P) Radiological evaluation of neonatal thoracic lesions in 8 neonates Konark Sarvaiya *, Himanshu Singla, Nirav Patel, Jai Inder Dhillon, Babubhai Patel 3 nd year
Original Research Article ISSN: 394-006 (P) Radiological evaluation of neonatal thoracic lesions in 8 neonates Konark Sarvaiya *, Himanshu Singla, Nirav Patel, Jai Inder Dhillon, Babubhai Patel 3 nd year
Background: Bedside ultrasound is emerging as a useful tool in the assessment of
 Abstract: Background: Bedside ultrasound is emerging as a useful tool in the assessment of intravascular volume status by examining measurements of the inferior vena cava (IVC). Many previous studies do
Abstract: Background: Bedside ultrasound is emerging as a useful tool in the assessment of intravascular volume status by examining measurements of the inferior vena cava (IVC). Many previous studies do
Journal Club American Journal of Respiratory and Critical Care Medicine. Zhang Junyi
 Journal Club 2018 American Journal of Respiratory and Critical Care Medicine Zhang Junyi 2018.11.23 Background Mechanical Ventilation A life-saving technique used worldwide 15 million patients annually
Journal Club 2018 American Journal of Respiratory and Critical Care Medicine Zhang Junyi 2018.11.23 Background Mechanical Ventilation A life-saving technique used worldwide 15 million patients annually
Observer variation for radiography, computed tomography, and magnetic resonance imaging of occult hip fractures
 Observer variation for radiography, computed tomography, and magnetic resonance imaging of occult hip fractures Collin, David; Dunker, Dennis; Gothlin, Jan H.; Geijer, Mats Published in: Acta Radiologica
Observer variation for radiography, computed tomography, and magnetic resonance imaging of occult hip fractures Collin, David; Dunker, Dennis; Gothlin, Jan H.; Geijer, Mats Published in: Acta Radiologica
Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis?
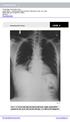 1 Interpreting Chest X-Rays CASE 1 Fig. 1.1 Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis? CASE 1 Interpreting
1 Interpreting Chest X-Rays CASE 1 Fig. 1.1 Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis? CASE 1 Interpreting
Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings
 Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings Poster No.: C-2067 Congress: ECR 2017 Type: Educational Exhibit Authors: J. M. Almeida, N. Antunes, C. Leal, L. Figueiredo ; Lisboa/PT,
Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings Poster No.: C-2067 Congress: ECR 2017 Type: Educational Exhibit Authors: J. M. Almeida, N. Antunes, C. Leal, L. Figueiredo ; Lisboa/PT,
DIASTOLOGY DON T BE SUCH A STIFF
 DIASTOLOGY DON T BE SUCH A STIFF Michael Mallin, MD University of Utah Director Emergency Ultrasound www.ultrasoundpodcast.com Warning: The education found within this presentation is not approved by anyone
DIASTOLOGY DON T BE SUCH A STIFF Michael Mallin, MD University of Utah Director Emergency Ultrasound www.ultrasoundpodcast.com Warning: The education found within this presentation is not approved by anyone
ORIGINAL ARTICLE. Role of Ultrasound in Evaluation of Undifferentiated Shock in ICU Settings
 Journal of The Association of Physicians of India Vol. 66 August 2018 13 Role of Ultrasound in Evaluation of Undifferentiated Shock in ICU Settings Tanvi Vaidya 1*, Pradeep D costa 2, Satish Pande 3 ORIGINAL
Journal of The Association of Physicians of India Vol. 66 August 2018 13 Role of Ultrasound in Evaluation of Undifferentiated Shock in ICU Settings Tanvi Vaidya 1*, Pradeep D costa 2, Satish Pande 3 ORIGINAL
Lung ultrasound: routine practice for the next generation of internists
 REVIEW Lung ultrasound: routine practice for the next generation of internists H.R.W. Touw 1,2, P.R. Tuinman* 1,3,4, H.P.M.M. Gelissen 1, E. Lust 1, P.W.G. Elbers 1,3,4 Departments of 1 Intensive Care
REVIEW Lung ultrasound: routine practice for the next generation of internists H.R.W. Touw 1,2, P.R. Tuinman* 1,3,4, H.P.M.M. Gelissen 1, E. Lust 1, P.W.G. Elbers 1,3,4 Departments of 1 Intensive Care
