Impact of lung ultrasound on clinical decision making in critically ill patients
|
|
|
- Lenard Gardner
- 6 years ago
- Views:
Transcription
1 Intensive Care Med DOI /s ORIGINAL Nektaria Xirouchaki Eumorfia Kondili George Prinianakis Polychronis Malliotakis Dimitrios Georgopoulos Impact of lung ultrasound on clinical decision making in critically ill patients Received: 21 June 2013 Accepted: 4 October 2013 Ó Springer-Verlag Berlin Heidelberg and ESICM 2013 Take-home message: In mechanically ventilated critically ill patients lung ultrasound has a significant impact on clinical decision making and therapeutic management. Electronic supplementary material The online version of this article (doi: /s ) contains supplementary material, which is available to authorized users. N. Xirouchaki E. Kondili G. Prinianakis P. Malliotakis D. Georgopoulos ()) Department of Intensive Care Medicine, University Hospital of Heraklion, University of Crete, Heraklion, Crete, Greece georgop@med.uoc.gr Fax:? Abstract Purpose: To assess the impact of lung ultrasound (LU) on clinical decision making in mechanically ventilated critically ill patients. Methods: One hundred and eightynine patients took part in this prospective study. The patients were enrolled in the study when LU was requested by the primary physician for (1) unexplained deterioration of arterial blood gases and (2) a suspected pathologic entity [pneumothorax, significant pleural effusion (including parapneumonic effusion, empyema, or hemothorax), unilateral atelectasis (lobar or total), pneumonia and diffuse interstitial syndrome (pulmonary edema)]. Results: Two hundred and fiftythree LU examinations were performed; 108 studies (42.7 %) were performed for unexplained deterioration of arterial blood gases, and 145 (57.3 %) for a suspected pathologic entity (60 for pneumothorax, 34 for significant pleural effusion, 22 for diffuse interstitial syndrome, 15 for unilateral lobar or total lung atelectasis, and 14 for pneumonia). The net reclassification index was 85.6 %, indicating that LU significantly influenced the decision-making process. The management was changed directly as a result of information provided by the LU in 119 out of 253 cases (47 %). In 81 cases, the change in patient management involved invasive interventions (chest tube, bronchoscopy, diagnostic thoracentesis/fluid drainage, continuous venous venous hemofiltration, abdominal decompression, tracheotomy), and in 38 cases, non-invasive (PEEP change/titration, recruitment maneuver, diuretics, physiotherapy, change in bed position, antibiotics initiation/change). In 53 out of 253 cases (21 %), LU revealed findings which supported diagnoses not suspected by the primary physician (7 cases of pneumothorax, 9 of significant pleural effusion, 9 of pneumonia, 16 of unilateral atelectasis, and 12 of diffuse interstitial syndrome). Conclusion: Our study shows that LU has a significant impact on decision making and therapeutic management. Keywords Lung ultrasound Intensive care unit Pneumothorax Pleural effusion Consolidation Interstitial syndrome Pneumonia Introduction Lung ultrasound (LU) has emerged in recent years as a powerful diagnostic tool, and as such it is increasingly used in patients managed in intensive care units (ICUs). As a bedside non-invasive test with an excellent safety profile, LU can be performed repeatedly. Thus, it is an attractive alternative imaging technique for patients on
2 whom thoracic computed tomography (CT) cannot be performed on a routine basis or where chest X-ray presents serious limitations in terms of sensitivity and specificity of identifying lung pathologies [1, 2]. We have shown recently that in a mixed surgical medical ICU population of mechanically ventilated critically ill patients, LU identifies (with high diagnostic accuracy) the most common pathological abnormalities of the respiratory system encountered in these patients. Indeed, this technique has a diagnostic accuracy of % in identifying pneumothorax, consolidation, interstitial syndrome, and pleural effusion, and may therefore be considered an alternative to thoracic CT for critically ill patients [2]. In addition, it has been shown that on appropriate clinical grounds, LU may be of help in the diagnosis of pneumonia and to follow its course [3 5]. Nevertheless, the impact of LU on decision making, in the process of addressing specific clinical questions related to these pathologic entities, is not entirely clear. The aim of this study was to examine the impact of performing LU on clinical decision making in mechanically ventilated critically ill patients. Methods This study was conducted in a medical surgical ICU. The hospital ethics committee approved the study and waived the requirement for informed consent. One hundred and eighty-nine mechanically ventilated patients were involved in this prospective study. The patients were enrolled in the study when (a) LU was requested by the primary physician to address five questions related to corresponding suspected pathologic entities and (b) a single LU operator (NX) was available. The following questions were posed: (1) Does the patient have LU findings compatible with the diagnosis of pneumothorax (Q 1 )? (2) Is significant pleural effusion (including parapneumonic effusion, empyema, or hemothorax) present (Q 2 )? (3) Does this patient have LU findings compatible with the diagnosis of unilateral major consolidation/atelectasis (lobar or total lung) (Q 3 )? (4) Does this patient have LU findings compatible with the diagnosis of pneumonia (Q 4 )? (5) Does this patient have LU findings compatible with diffuse pulmonary edema of cardiogenic or non-cardiogenic origin (Q 5, interstitial syndrome)? These five questions, as judged by the primary physician, and based on clinical and laboratory grounds, were linked to the patient s current status. In addition, since all these pathologies may cause derangement of arterial blood gases, LU was also requested by the primary physician for unexplained and persistent deterioration of arterial blood gases (hypoxemia and/or hypercapnia, Q ABG ). The LU operator presented the information to the primary physician and was not involved in the decision-making process. Lung ultrasound Visualization of the lungs was performed using a microconvex 5 9 MHz transducer, appropriate for transthoracic examination (Hitachi EUB 8500), as described previously [2]. Access to standardized images (seashore sign, stratosphere sign) was possible. LU was performed with the patient in the supine and semi-lateral position, using a specific previously validated protocol [2]. The normal lung generates lung sliding and A lines (repetition lines parallel to the pleural line) [6 8]. Pneumothorax was diagnosed when the A line sign (only A lines visible) was associated with the stratosphere sign (complete abolition of lung sliding; the lung sliding in M-mode results in a sandy pattern, arising exactly from the pleural line). Local lung sliding, or B lines, exclude the diagnosis [9, 10]. The lung point sign [the fleeting appearance of a lung pattern (lung sliding or pathologic comet-tail artifacts) replacing a pneumothorax pattern (absent lung sliding plus exclusive horizontal lines) in a particular location of the chest wall], specific for pneumothorax, was additionally used [11]. LU findings of lung overdistension, which may be misclassified as compatible with pneumothorax, included the absence of lung point and predominance of A line static profile associated with lung sliding and remarkable diaphragmatic depression. Pleural effusion was determined as a hypoechoic or echoic structure. The power Doppler and quad sign (the pleural effusion is delineated by the pleural line, the shadow of the ribs, and mostly the lung line) and sinusoid sign (on M mode the lung line moves toward the pleural line) on inspiration were used for pleural effusion differentiation. For hemothorax, the plankton sign was additionally used (multiple echoes, mobile and whirling in real-time in pleural space) [2, 6, 12]. Consolidation/atelectasis was defined as an isoechoic tissue-like structure which is caused by the loss of lung aeration [13]. The following signs were used to characterize a specific lung area as atelectatic: lung sliding abolition; abolition of dynamic diaphragm movement and its elevation (more than 2 cm); the presence of a static air bronchogram within the consolidation; heart sign, and the presence of small pleural effusion. The lung pulse sign (the association of absent lung sliding with the perception of heart activity at the pleural line) was also used in the cases of complete total lung atelectasis (i.e., due to right or left main bronchus intubation) [14, 15]. A static air bronchogram was defined as hyperechoic punctiform images produced by trapped air, no longer aerated, inside a lung area. Posterolateral alveolar consolidation and/or pleural effusion was defined as PLAPS [3]. Pneumonia was characterized by (1) the presence of a bilateral or local B line pattern with or without lung sliding, (2) irregular boundaries created by the adjacent aerated lung (provided that an entire lobe was not affected), (3) vascular flow seen as a branching pattern in color or power Doppler
3 imaging, and (4) the presence of anterior lung consolidation with hyperechoic punctiform images within a lung area (dynamic air bronchogram) [3 5]. The dynamic air bronchogram (punctiform or linear hyperechoic artifacts) is characterized by the presence of dynamic lung movement during the respiratory cycle. This sign is usually associated with a non-retractile consolidation (i.e., not atelectasis) and indicates that this consolidation is pneumonia [16]. Interstitial syndrome was defined as the presence of multiple B lines in a specific lung area. B lines are welldefined hyperechoic comet-tail artifacts, arising from the pleural line and spreading up indefinitely, erasing A lines and moving with the lung sliding when lung sliding is present. The B lines, 7 ± 1 mm apart, indicate thickening of the interlobular septa (B7 lines) and 3 ± 1 mm apart indicate ground glass areas (B3 lines), as previously described. White lung was defined as completely white echographic lung fields with coalescent B lines and no horizontal reverberation [7, 8, 17 19]. Data analysis The yield of LU was defined in each clinical problem as the percentage of studies that either had positive findings with diagnostic implications or confidently excluded the suspected diagnosis. The findings from the LU were classified as either expected or unexpected by the primary physician. The net reclassification improvement (NRI) was used to assess the impact of LU on clinical decision making [20, 21]. In this calculation we defined an event or non-event as the agreement or disagreement between LU findings and clinical diagnosis of the primary physician, respectively. Further analysis was based on the influence [which included therapeutic or non-therapeutic (no action) interventions] and noninfluence of LU on the decision-making process. NRI (expressed as %) was calculated as follows: NRI (%) = P upevents P downevents P upnonevents P downnonevents ; where P up events is the number of event cases in which LU influenced the decision-making process/number of event cases. P down events is the number of event cases in which LU did not influence the decision-making process/number of events cases. P up nonevent is the number of non-event cases in which LU influenced the decision-making process/number of non-event cases. P down nonevent is the number of non-event cases in which LU did not influence the decision-making process/number of non-event cases. Results Two hundred and fifty-three LU studies were performed in 189 mechanically ventilated patients (see Electronic Supplementary Material for demographics and clinical characteristics of the patients). In all but one LU study, pathologic findings were observed. These findings were mainly compatible with consolidation (n = 223), pleural effusion (n = 221), and interstitial syndrome (n = 189). A general flow chart of the study is shown in Fig. 1. NRI was 85.6 %, indicating that LU had a high impact on the decision-making process. Figures 2, 3, 4, 5, 6, and 7, as well as figure legends, show in detail the results of LU in addressing each of the six prespecified clinical questions. Overall, 108 studies (42.7 %) were performed for unexplained deterioration of arterial blood gases (Q ABG ) and 145 (57.3 %) for a suspected pathological entity (Q 1 Q 5 ). When LU was performed for a suspected pathologic entity, the LU findings were compatible with the primary physician s clinical suspicion in 69.7 % of cases, while ten cases (6.9 %) supported something other than the suspected entity (Figs. 2, 3, 4, 5, 6). In the remaining 34 cases (23.4 %), the LU findings did not categorically support any of these pathologies and reflected the LU abnormalities usually encountered in mechanically ventilated critically ill patients (i.e., bilateral consolidation of dependent lung zone, bilateral pleural effusion, diffuse B lines). When LU was performed for Q ABG, pathologic findings were observed in all cases, with bilateral lower lobe consolidation, accompanied by pleural effusion, being the most common. In 43 cases (39.8 %), the LU findings were consistent with one of the five pathologic entities (as described above) and had an impact on patient management (Fig. 7). Overall, the management was changed directly as a result of information provided by the LU operator in 119 cases (47 %) (Fig. 1). In 81 cases, the change in patient management involved invasive interventions (i.e., chest tube, bronchoscopy, diagnostic thoracentesis/fluid drainage, continuous venous venous hemofiltration, abdominal decompression, tracheotomy), and in 38 cases, noninvasive (i.e., PEEP change/titration, recruitment maneuver, diuretics, physiotherapy, change in bed position, antibiotics initiation/change). In 53 cases (21 %), LU revealed findings which supported diagnoses not suspected by the primary physician. These included 7 cases of pneumothorax, 9 of significant pleural effusion, 9 of pneumonia, 16 of unilateral atelectasis (lobar or total), and 12 of diffuse interstitial syndrome (white lung). In 7 out of 253 cases, the primary physician ordered a thoracic CT scan to assist the decision-making process. In all cases CT confirmed the LU findings. In three cases, a thoracic CT was performed because pulmonary embolism was suspected, in two for further investigation of ARDS, in one for multiloculated parapneumonic effusion, and one for multiple trauma and esophageal rupture. In none of these cases was a bedside chest X-ray ordered. No further action was applied as a result of CT findings.
4 Fig. 1 Study flow chart. Lung ultrasound (LU). Q 1 Does this patient have LU findings compatible with the diagnosis of pneumothorax? Q 2 Is significant pleural effusion (including parapneumonic effusion, empyema, or hemothorax) present? Q 3 Does this patient have LU findings compatible with the diagnosis of unilateral major consolidation/atelectasis (lobar or total lung)? Q 4 Does this patient have LU findings compatible with the diagnosis of pneumonia? Q 5 Does this patient have LU findings compatible with diffuse pulmonary edema of cardiogenic or non-cardiogenic origin (interstitial syndrome)? Q ABG LU examination for unexplained and persistent deterioration of arterial blood gases. See text for explanation of net reclassification index Fig. 2 Lung ultrasound (LU) performed for question Q 1. Seven additional cases of pneumothorax were diagnosed when LU was performed for questions other than Q 1 (all from Q ABG group). a Stratosphere sign (arrow). b Lung point the fleeting appearance of a lung pattern (lung sliding or pathologic comet-tail artifacts) replacing a pneumothorax pattern (absent lung sliding plus exclusive horizontal lines) in a particular location of the chest wall (arrow) Discussion The main finding of this study was that in mechanically ventilated critically ill patients, LU has significant therapeutic impact by influencing the decision-making process, as indicated by the high NRI (85.6 %). The information provided by the LU study directly changed the management of these patients in 47 % of the reported cases. In the majority of the cases, the change in patient management involved invasive interventions. Furthermore, in one-fifth of the studies, LU revealed findings compatible with diagnoses not suspected by the primary physician.
5 Fig. 3 Lung ultrasound (LU) performed for question Q 2. Nine additional cases of significant pleural effusion (PE) were diagnosed when LU was performed for questions other than Q 2. Invasive interventions included chest tube placement in 7 cases (4 for hemothorax, 3 for empyema) and diagnostic thoracentesis and/or fluid drainage in 34 patients. a Complicated PE. b Abundant PE with floating lung. Tissue debris and diaphragms within pleura, the diaphragm, the consolidated lower lobe, PE, and floating lung are indicated by corresponding arrows Fig. 4 Lung ultrasound (LU) performed for question Q 3. Sixteen additional cases of atelectasis were diagnosed when LU was performed for questions other than Q 3. Seven out of 15 patients underwent therapeutic bronchoscopy. In eight patients, non-invasive therapy was applied (tight physiotherapy, changes in endotracheal tube position, and/ or changes in bed position). a Right lower lobe atelectasis (black arrows), associated with small pleural effusion (white arrow). Note the presence of pleural fluid within the interlobular fissure (black arrow). The patient underwent successful bronchoscopy due to arterial blood gases derangement. b Left lower lobe atelectasis in another patient. Note the air bronchogram (punctiform or linear hyperechoic artifacts) within consolidation (arrows) In our study, we examined the value of LU in addressing predefined clinical problems. We chose this study design because we, and others, have shown that LU may be used as an alternative to CT in critically ill patients (the gold standard for lung imaging in these patients) in identifying specific common lung pathologies, such as atelectasis, interstitial syndrome, pneumothorax, pleural effusion, and pneumonia [1, 2, 22]. For this reason, LU was performed when the primary physician suspected one of these pathologies. In addition, since these pathologies may lead to inefficient gas exchange, unexplained deterioration of arterial blood gases (unexplained persistent hypoxemia and/or hypercapnia) was also a reason for requesting LU study. An omission of this
6 Fig. 5 Lung ultrasound (LU) performed for question Q 4. Nine additional cases of pneumonia were diagnosed when LU was performed for questions other than Q 4. Invasive interventions included bronchoscopy with directed bronchoalveolar lavage (BAL) sampling and antibiotic modification (1 patient) and diagnostic thoracentesis for parapneumonic effusion evaluation (1 patient). Noninvasive interventions consisted of modification (step-up) or initiation of antibiotics. a Pneumonia with irregular boundaries and air bronchogram (black arrows) in right upper field. b Necrotic pneumonia with diaphragms and tissue within pleura (white arrow) Fig. 6 Lung ultrasound (LU) performed for question Q 5. Twelve additional cases of diffuse pulmonary edema were diagnosed when LU was performed for questions other than Q 5 (all from Q ABG group). Changes in medical treatment, consisting of higher PEEP application and aggressive diuretic therapy, were performed in seven patients with pulmonary edema due to congestive heart failure. Continuous venous venous hemofiltration (CVVH) was applied in three patients with ultrasound findings of lung congestion, due to overload. PEEP was titrated at higher levels in four patients with acute respiratory distress syndrome (ARDS)/white lung and was decreased in one patient with ultrasound findings of overdistension at non-dependent lung zones, and massive atelectasis at dependent zones, due to abdominal compartment syndrome. The latter patient underwent successful abdominal decompression by colonoscopy. a, b LU findings in two patients suffering from severe ARDS. Note the white lung pattern completely white echographic lung fields, with coalescent B lines and no horizontal reverberation (white arrows). Black arrows show the pleural line
7 Fig. 7 Lung ultrasound (LU) performed for Q ABG. LU provided critical information about the clinical status in 43 patients, and resulted in change in patient management. Note that in 65 out of 108 examinations, the main finding was bilateral posterolateral consolidation associated with pleural effusion. a Bilateral posterolateral consolidation (black arrows) associated with pleural effusion (PLAPS). Thick black arrow indicates the diaphragm. b Diffuse bilateral B lines well-defined hyperechoic comet-tail artifacts, arising from pleural line and spreading up indefinitely, erasing A lines and moving with the lung sliding when lung sliding is present (white arrow), in a patient with severe acute respiratory distress syndrome (ARDS). In this patient, PEEP was increased to 20 cmh 2 O after LU study design is that it does not permit an examination of the value of routine performance of LU in critically ill patients. LU was performed by a single operator (NX) with extensive experience of this imaging technique. Although LU can be performed by almost all attending physicians in our unit, we decided, for the purpose of a uniform interpretation of the findings, to involve a single operator in our LU studies. This should also minimize the influence of the variability of operator bias on the results, as the operator simply presented the findings to the primary physician and was not responsible for further patient management. However, the results of this study may not be applicable when LU is performed by less experienced operators. In all but one LU study, pathologic findings were observed. In the majority of the cases, these findings were compatible with consolidation, pleural effusion, and interstitial syndrome. This observation has been reported previously and reflects the critically ill population we studied [3]. The fact that almost all mechanically ventilated critically ill patients had pathologic findings in LU indicates that performing this imaging technique unselectively in these patients may not be helpful when planning the patients management. On the other hand, as our study has shown, ordering an LU examination on the basis of specific clinical problems may have a great impact on clinical decision making. In several cases (42.7 %) LU study was ordered for unexplained deterioration of gas exchange. This was not an unexpected finding. Mechanically ventilated patients very often exhibit derangement in gas exchange for several reasons related to pulmonary and extrapulmonary factors. In these patients acute hypoxia and/or hypercapnia may be due to increased V 0 /Q 0 inequalities, right to left shunt, and hypoventilation. It has been shown that LU can be used to diagnose most of the pathologic entities that can cause acute impairment in gas exchange, such as atelectasis, pneumothorax, and interstitial syndrome [2]. Therefore it is not surprising that in almost half of the cases LU was ordered for unexplained deterioration of gas exchange. Although in all cases LU revealed findings that could explain the blood gas abnormalities, in 38.9 % of cases the findings were compatible with a specific predefined diagnosis and appropriate action was taken. In the majority of cases (57.3 %), LU was performed for a suspected specific pathology. We should mention that in almost 50 % of these cases, LU was performed because pneumothorax was suspected. This high percentage is most likely due to the specific population studied and to the study s design. Several of our patients suffered from multiple trauma and/or ARDS necessitating the application of high PEEP. These patients have increased risk of pneumothorax, and in several cases, this forced the primary physician to order an LU study to address the issue of pneumothorax. The suspicion of
8 pneumothorax was confirmed only in 28 out of 60 cases (46.7 %). It is of interest to note that when LU was performed for deterioration of arterial blood gases, an additional seven cases of non-suspected pneumothoraces were diagnosed. This emphasizes the value of LU in the investigation of acute impairments of ABGs. Previous studies have also supported the value of LU in the diagnosis of respiratory system diseases and, indirectly, on the patients management. Yu et al. [22], in a small population of patients (n = 41), 19 of whom were managed in an ICU, performed LU when portable radiographs were difficult to interpret and showed that this technique was helpful in diagnosis (in 66 % of cases) and treatment planning (in 41 % of patients). Lichtenstein and Meziere [3], in an observational study, performed LU on consecutive patients admitted to the ICU with acute respiratory failure. These authors compared the LU results on initial presentation with the final diagnosis by the ICU team and demonstrated that LU findings immediately provided diagnosis of acute respiratory failure in 90.5 % of cases. Our study showed that in a large population of mechanically ventilated critically ill patients, whose clinical status necessitated a diagnostic procedure and therapeutic intervention, LU information provided to the primary physician changed the patients management in almost half of the cases. Furthermore, in one-fifth of the studies, LU revealed findings compatible with specific diagnoses not suspected by the primary physician. It follows that in the process of addressing specific questions, the LU has significant impact on decision making. To our knowledge, this is the first prospective study that clearly demonstrates the value of LU in the therapeutic management of ICU patients receiving mechanical ventilation. The aim of this prospective study was to examine the impact of LU on decision making and therapeutic management. Neither the decision-making process nor the therapeutic management was controlled. The primary physician was fully responsible for the patients management. Since LU findings were present in several primary physicians and there were no predefined, protocol-driven management guidelines, the patients were not followed prospectively to examine if the changes in their management due to LU findings were appropriate or successful. However, in several cases, the change in patient management was obviously appropriate, particularly when the change involved invasive interventions (i.e., chest tube insertion for pneumothorax. See also Electronic Supplementary Material for comments on the appropriateness of therapeutic interventions). A study of different design may examine the influence of LU on the outcome of patients. This study follows a previous one from the same department which showed that in an unselected general ICU population, LU, compared to chest X-ray, has a high diagnostic performance for the diagnosis of common pathologic conditions and may be used as an alternative to thoracic CT [2]. As a result, chest X-rays are not performed on a routine daily basis in our unit. It is likely that the impact of LU on decision making in this study was influenced by the results of our previous study (because LU operations were performed by the same operator) causing the primary physicians to rely on the LU findings to support their decision-making processes. We believe that this represents a major limitation of the study and may make it difficult to replicate in other ICUs. In conclusion, our study has shown that in mechanically ventilated critically ill patients, in the process of addressing specific clinical questions, LU has had a significant impact on decision making. Notwithstanding its limitations (i.e., operator dependence), LU is a powerful, non-invasive diagnostic tool in critically ill patients. Acknowledgments The authors would like to acknowledge G. Chlouverakis, Associate Professor of Biostatistics, for his contribution to the statistical analysis. Conflicts of interest On behalf of all authors, the corresponding author states that there is no conflict of interest. References 1. Lichtenstein D, Goldstein I, Mourgeon E, Cluzel P, Grenier P, Rouby JJ (2004) Comparative diagnostic performances of auscultation, chest radiography, and lung ultrasonography in acute respiratory distress syndrome. Anesthesiology 100: Xirouchaki N, Magkanas E, Vaporidi K, Kondili E, Plataki M, Patrianakos A, Akoumianaki E, Georgopoulos D (2011) Lung ultrasound in critically ill patients: comparison with bedside chest radiography. Intensive Care Med 37: Lichtenstein DA, Meziere GA (2008) Relevance of lung ultrasound in the diagnosis of acute respiratory failure: the BLUE protocol. Chest 134: Bouhemad B, Liu ZH, Arbelot C, Zhang M, Ferarri F, Le-Guen M, Girard M, Lu Q, Rouby JJ (2010) Ultrasound assessment of antibiotic-induced pulmonary reaeration in ventilatorassociated pneumonia. Crit Care Med 38: Blaivas M (2012) Lung ultrasound in evaluation of pneumonia. J Ultrasound Med 31:
9 6. Lichtenstein DA (2009) Ultrasound examination of the lungs in the intensive care unit. Pediatr Crit Care Med 10: Bouhemad B, Zhang M, Lu Q, Rouby JJ (2007) Clinical review: bedside lung ultrasound in critical care practice. Crit Care 11: Volpicelli G, Elbarbary M, Blaivas M, Lichtenstein DA, Mathis G, Kirkpatrick AW, Melniker L, Gargani L, Noble VE, Via G, Dean A, Tsung JW, Soldati G, Copetti R, Bouhemad B, Reissig A, Agricola E, Rouby JJ, Arbelot C, Liteplo A, Sargsyan A, Silva F, Hoppmann R, Breitkreutz R, Seibel A, Neri L, Storti E, Petrovic T (2012) International evidence-based recommendations for point-of-care lung ultrasound. Intensive Care Med 38: Lichtenstein DA, Meziere G, Lascols N, Biderman P, Courret JP, Gepner A, Goldstein I, Tenoudji-Cohen M (2005) Ultrasound diagnosis of occult pneumothorax. Crit Care Med 33: Volpicelli G (2011) Sonographic diagnosis of pneumothorax. Intensive Care Med 37(2): Lichtenstein D, Meziere G, Biderman P, Gepner A (2000) The lung point : an ultrasound sign specific to pneumothorax. Intensive Care Med 26: Maslove DM, Chen BT, Wang H, Kuschner WG (2012) The diagnosis and management of pleural effusions in the ICU. J Intensive Care Med 28: Lichtenstein DA, Lascols N, Meziere G, Gepner A (2004) Ultrasound diagnosis of alveolar consolidation in the critically ill. Intensive Care Med 30: Lichtenstein D (2005) Ultrasound diagnosis of atelectasis. Int J Intensive Care 12: Lichtenstein DA, Lascols N, Prin S, Meziere G (2003) The lung pulse : an early ultrasound sign of complete atelectasis. Intensive Care Med 29: Lichtenstein D, Meziere G, Seitz J (2009) The dynamic air bronchogram. A lung ultrasound sign of alveolar consolidation ruling out atelectasis. Chest 135: Lichtenstein D, Meziere G, Biderman P, Gepner A, Barre O (1997) The comet-tail artifact. An ultrasound sign of alveolar-interstitial syndrome. Am J Respir Crit Care Med 156: Mallamaci F, Benedetto FA, Tripepi R, Rastelli S, Castellino P, Tripepi G, Picano E, Zoccali C (2010) Detection of pulmonary congestion by chest ultrasound in dialysis patients. JACC Cardiovasc Imaging 3: Lichtenstein D (2012) Fluid administration limited by lung sonography: the place of lung ultrasound in assessment of acute circulatory failure (the FALLSprotocol). Expert Rev Respir Med 6: Pencina MJ, D Agostino RB, Vasan RS (2010) Statistical methods for assessment of added usefulness of new biomarkers. Clin Chem Lab Med 48: Steyerberg EW, Vickers AJ, Cook NR, Gerds T, Gonen M, Obuchowski N, Pencina MJ, Kattan MW (2010) Assessing the performance of prediction models: a framework for traditional and novel measures. Epidemiology 21: Yu CJ, Yang PC, Chang DB, Luh KT (1992) Diagnostic and therapeutic use of chest sonography: value in critically ill patients. AJR Am J Roentgenol 159:
Unusual new signs of pneumothorax at lung ultrasound
 Unusual new signs of pneumothorax at lung ultrasound Volpicelli et al. Volpicelli et al. Critical Ultrasound Journal 2013, 5:10 Volpicelli et al. Critical Ultrasound Journal 2013, 5:10 SHORT COMMUNICATION
Unusual new signs of pneumothorax at lung ultrasound Volpicelli et al. Volpicelli et al. Critical Ultrasound Journal 2013, 5:10 Volpicelli et al. Critical Ultrasound Journal 2013, 5:10 SHORT COMMUNICATION
Lung ultrasound in the critically ill patient Pleural Effusions
 Lung ultrasound in the critically ill patient Pleural Effusions Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida
Lung ultrasound in the critically ill patient Pleural Effusions Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida
Lung ultrasound in critically ill patients: comparison with bedside chest radiography
 Intensive Care Med (2011) 37:1488 1493 DOI 10.1007/s00134-011-2317-y ORIGINAL Nektaria Xirouchaki Eleftherios Magkanas Katerina Vaporidi Eumorfia Kondili Maria Plataki Alexandros Patrianakos Evaggelia
Intensive Care Med (2011) 37:1488 1493 DOI 10.1007/s00134-011-2317-y ORIGINAL Nektaria Xirouchaki Eleftherios Magkanas Katerina Vaporidi Eumorfia Kondili Maria Plataki Alexandros Patrianakos Evaggelia
Lung sonography in the diagnosis of pneumothorax.
 Lung sonography in the diagnosis of pneumothorax. Poster No.: C-0526 Congress: ECR 2011 Type: Educational Exhibit Authors: K. Stefanidis, K. Vintzilaios, D. D. Cokkinos, E. Antypa, S. Dimopoulos, S. Nanas,
Lung sonography in the diagnosis of pneumothorax. Poster No.: C-0526 Congress: ECR 2011 Type: Educational Exhibit Authors: K. Stefanidis, K. Vintzilaios, D. D. Cokkinos, E. Antypa, S. Dimopoulos, S. Nanas,
A Practical Approach to Ultrasound Assessment of Respiratory Distress
 A Practical Approach to Ultrasound Assessment of Respiratory Distress Yanick Beaulieu, MD, FRCPC Director, Bedside Ultrasound Curriculum Division of Cardiology and Critical Care Hôpital du Sacré-Coeur
A Practical Approach to Ultrasound Assessment of Respiratory Distress Yanick Beaulieu, MD, FRCPC Director, Bedside Ultrasound Curriculum Division of Cardiology and Critical Care Hôpital du Sacré-Coeur
Bedside Sonographic Diagnosis of Pneumothorax in Pediatric Patients: A Preliminary Report Chia-Wang Tang 1, Kai-Sheng Hsieh 1 1
 ORIGINAL ARTICLE Bedside Sonographic Diagnosis of in Pediatric Patients: A Preliminary Report Chia-Wang Tang 1, Kai-Sheng Hsieh 1 1 Division of Pediatric Pulmonology, Department of Pediatrics, Kaohsiung
ORIGINAL ARTICLE Bedside Sonographic Diagnosis of in Pediatric Patients: A Preliminary Report Chia-Wang Tang 1, Kai-Sheng Hsieh 1 1 Division of Pediatric Pulmonology, Department of Pediatrics, Kaohsiung
Identification of lung sliding: a basic ultrasound technique with a steep learning curve
 SIGNA VITAE 2013; 8(1): 31-35 ORIGINAL Identification of lung sliding: a basic ultrasound technique with a steep learning curve MATEJ STRNAD SABINA ZADEL ZALIKA KLEMENC-KETIS MATEJ STRNAD ( ) SABINA ZADEL
SIGNA VITAE 2013; 8(1): 31-35 ORIGINAL Identification of lung sliding: a basic ultrasound technique with a steep learning curve MATEJ STRNAD SABINA ZADEL ZALIKA KLEMENC-KETIS MATEJ STRNAD ( ) SABINA ZADEL
Pediatric Lung Ultrasound (PLUS) In Diagnosis of Community Acquired Pneumonia (CAP)
 Pediatric Lung Ultrasound (PLUS) In Diagnosis of Community Acquired Pneumonia (CAP) Dr Neetu Talwar Senior Consultant, Pediatric Pulmonology Fortis Memorial Research Institute, Gurugram Study To compare
Pediatric Lung Ultrasound (PLUS) In Diagnosis of Community Acquired Pneumonia (CAP) Dr Neetu Talwar Senior Consultant, Pediatric Pulmonology Fortis Memorial Research Institute, Gurugram Study To compare
Chest Ultrasound: Pneumothorax
 WINFOCUS BASIC ECHO (WBE) Chest Ultrasound: Pneumothorax Mark Hamlin, MD, MS Associate Professor of Anesthesiology and Surgery University of Vermont College of Medicine Co-Director of Surgical Critical
WINFOCUS BASIC ECHO (WBE) Chest Ultrasound: Pneumothorax Mark Hamlin, MD, MS Associate Professor of Anesthesiology and Surgery University of Vermont College of Medicine Co-Director of Surgical Critical
The Intensive Care Unit
 Imaging of the ADRS patient: Risk of transportation and alternative to repetitive radiation exposure Jean-Jacques Rouby Pitié-Salpêtrière Hospital The Intensive Care Unit The Intensive Care Unit Multidisciplinary
Imaging of the ADRS patient: Risk of transportation and alternative to repetitive radiation exposure Jean-Jacques Rouby Pitié-Salpêtrière Hospital The Intensive Care Unit The Intensive Care Unit Multidisciplinary
OVERVIEW. Need for USG. Weaning assessment. Mechanics of USG. Pneumonia / VAP. Principles of lung USG. Prone position ventilation assessment
 OVERVIEW Need for USG Mechanics of USG Principles of lung USG BLUE protocol Alveolar syndrome Interstitial syndrome Weaning assessment Pneumonia / VAP Prone position ventilation assessment ETT positioning
OVERVIEW Need for USG Mechanics of USG Principles of lung USG BLUE protocol Alveolar syndrome Interstitial syndrome Weaning assessment Pneumonia / VAP Prone position ventilation assessment ETT positioning
Lung ultrasound in the critically ill patient BASICS
 Lung ultrasound in the critically ill patient BASICS Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida Introduction
Lung ultrasound in the critically ill patient BASICS Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida Introduction
Point-of-care lung ultrasound
 Ultrasound Point-of-care lung ultrasound Philips tutorial Michael B. Stone, MD, RDMS Director, Division of Emergency Ultrasound Department of Emergency Medicine Brigham and Women s Hospital, Boston, MA
Ultrasound Point-of-care lung ultrasound Philips tutorial Michael B. Stone, MD, RDMS Director, Division of Emergency Ultrasound Department of Emergency Medicine Brigham and Women s Hospital, Boston, MA
Definitions and diagnostic implications of terms used in the chest radiograph and lung ultrasound diagnoses of pneumonia.
 Supplementary 1 Definitions and diagnostic implications of terms used in the chest radiograph and lung ultrasound diagnoses of pneumonia. Imaging finding Definition Implication CR Consolidation Interstitial
Supplementary 1 Definitions and diagnostic implications of terms used in the chest radiograph and lung ultrasound diagnoses of pneumonia. Imaging finding Definition Implication CR Consolidation Interstitial
Bedside ultrasound - Lung ultrasound in the Intensive Care Unit
 Bedside ultrasound - Lung ultrasound in the Intensive Care Unit Kishore K. Pichamuthu, Professor, Department of Critical Care, Christian Medical College, Vellore. Summary In an ICU setting, ultrasonographic
Bedside ultrasound - Lung ultrasound in the Intensive Care Unit Kishore K. Pichamuthu, Professor, Department of Critical Care, Christian Medical College, Vellore. Summary In an ICU setting, ultrasonographic
This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors.
 This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. - Figure S1: The four quadrant approach lung ultrasound at the bedside. * The anterolateral
This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. - Figure S1: The four quadrant approach lung ultrasound at the bedside. * The anterolateral
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
ASSESSMENT OF LUNG PARENCHYMAL ABNORMALITIES
 2016 by the author Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as
2016 by the author Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as
Ultrasound for Lung Monitoring of Ventilated Patients
 Clinical Concepts and Commentary Jerrold H. Levy, M.D., F.A.H.A., F.C.C.M., Editor Ultrasound for Lung Monitoring of Ventilated Patients Belaïd Bouhemad, M.D., Ph.D., Silvia Mongodi, M.D., Gabriele Via,
Clinical Concepts and Commentary Jerrold H. Levy, M.D., F.A.H.A., F.C.C.M., Editor Ultrasound for Lung Monitoring of Ventilated Patients Belaïd Bouhemad, M.D., Ph.D., Silvia Mongodi, M.D., Gabriele Via,
Lung Ultrasound for Critical Care Physiotherapists: A Narrative Review
 INVITED REVIEW Lung Ultrasound for Critical Care Physiotherapists: A Narrative Review Maja Leech 1 *, Bernie Bissett 1,2, Marta Kot 3 & George Ntoumenopoulos 4 1 Physiotherapy Department, Canberra Hospital,
INVITED REVIEW Lung Ultrasound for Critical Care Physiotherapists: A Narrative Review Maja Leech 1 *, Bernie Bissett 1,2, Marta Kot 3 & George Ntoumenopoulos 4 1 Physiotherapy Department, Canberra Hospital,
CHEST Recent Advances in Chest Medicine
 CHEST Recent Advances in Chest Medicine Thoracic Ultrasonography for the Pulmonary Specialist Seth J. Koenig, MD; Mangala Narasimhan, DO, FCCP; and Paul H. Mayo, MD, FCCP Thoracic ultrasonography is a
CHEST Recent Advances in Chest Medicine Thoracic Ultrasonography for the Pulmonary Specialist Seth J. Koenig, MD; Mangala Narasimhan, DO, FCCP; and Paul H. Mayo, MD, FCCP Thoracic ultrasonography is a
Lung ultrasound: Present and future
 Review Article Lung ultrasound: Present and future Ashish Saraogi Department of Anaesthesiology, National Institute of Medical Sciences and Research, Jaipur, Rajasthan, India ABSTRACT The scope of ultrasound
Review Article Lung ultrasound: Present and future Ashish Saraogi Department of Anaesthesiology, National Institute of Medical Sciences and Research, Jaipur, Rajasthan, India ABSTRACT The scope of ultrasound
Pulmonary Ultrasound in Emergency Medicine and Critical Care
 Pulmonary Ultrasound in Emergency Medicine and Critical Care www.rmgultrasound.com Author: Virginia M Stewart, MD RDMS RDCS RDMSK Dr Stewart is a practicing Emergency Physician in Eastern Virginia, USA.
Pulmonary Ultrasound in Emergency Medicine and Critical Care www.rmgultrasound.com Author: Virginia M Stewart, MD RDMS RDCS RDMSK Dr Stewart is a practicing Emergency Physician in Eastern Virginia, USA.
Ultrasound. FAST Focused Assessment with Sonography in Trauma
 Ultrasound FAST Focused Assessment with Sonography in Trauma Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida
Ultrasound FAST Focused Assessment with Sonography in Trauma Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida
Usefulness of transthoracic lung ultrasound for the diagnosis of mild pneumothorax
 Original Article J Vet Sci 2018, 19(5), 660-666 ㆍ https://doi.org/10.4142/jvs.2018.19.5.660 JVS Usefulness of transthoracic lung ultrasound for the diagnosis of mild pneumothorax Tae Sung Hwang 1, Young
Original Article J Vet Sci 2018, 19(5), 660-666 ㆍ https://doi.org/10.4142/jvs.2018.19.5.660 JVS Usefulness of transthoracic lung ultrasound for the diagnosis of mild pneumothorax Tae Sung Hwang 1, Young
MINERVA MEDICA COPYRIGHT REVIEW ARTICLE D. LICHTENSTEIN. Resuscitation Service, Ambroise-Paré Hospital, Boulogne, France ABSTRACT
 MINERVA ANESTESIOL 2009;75:313-7 REVIEW ARTICLE Lung ultrasound in acute respiratory failure an introduction to the BLUE-protocol D. Resuscitation Service, Ambroise-Paré Hospital, Boulogne, France ABSTRACT
MINERVA ANESTESIOL 2009;75:313-7 REVIEW ARTICLE Lung ultrasound in acute respiratory failure an introduction to the BLUE-protocol D. Resuscitation Service, Ambroise-Paré Hospital, Boulogne, France ABSTRACT
Contents& & & 1.! Ultrasound&basics& 1! 2.! Image&generation& 15!
 A l i n e press é % % % Contents& & & 1. Ultrasound&basics& 1 1.1. What,is,ultrasound?, 1 1.2. Ultrasound,probes,send,and,receive,ultrasound, 3 1.3. How,does,ultrasound,behave,travelling,through,tissue?,
A l i n e press é % % % Contents& & & 1. Ultrasound&basics& 1 1.1. What,is,ultrasound?, 1 1.2. Ultrasound,probes,send,and,receive,ultrasound, 3 1.3. How,does,ultrasound,behave,travelling,through,tissue?,
Ultrasound in the ICU
 Ultrasound in the ICU Kristine E. W. Breyer, MD Assistant Professor Anesthesia & Critical Care Medicine UCSF DISCLOSURES: NONE Definition The Ultrasound Exam Types & Uses Training Clinical Examples Objectives
Ultrasound in the ICU Kristine E. W. Breyer, MD Assistant Professor Anesthesia & Critical Care Medicine UCSF DISCLOSURES: NONE Definition The Ultrasound Exam Types & Uses Training Clinical Examples Objectives
Lung Ultrasound in Diagnosis of Acute Respiratory Failure: BLUE Protocol Based Evaluation
 Lung Ultrasound in Diagnosis of Acute Respiratory Failure: BLUE Protocol Based Evaluation Niyas. K. Naseer 1, Muhammad Shafeek 2*, Rajani. M 3, Manoj. D. K 3 1Junior Resident, 2* Assistant Professor, 3
Lung Ultrasound in Diagnosis of Acute Respiratory Failure: BLUE Protocol Based Evaluation Niyas. K. Naseer 1, Muhammad Shafeek 2*, Rajani. M 3, Manoj. D. K 3 1Junior Resident, 2* Assistant Professor, 3
NON INVASIVE LIFE SAVERS. Ultrasound in PICU
 VOL 1 NO.1 Jan March 2014 54 Table 1. Selected Applications of Point-of-Care Ultrasonography, According to Medical Specialty. Specialty Ultrasound Applications Anesthesia Cardiology Guidance for vascular
VOL 1 NO.1 Jan March 2014 54 Table 1. Selected Applications of Point-of-Care Ultrasonography, According to Medical Specialty. Specialty Ultrasound Applications Anesthesia Cardiology Guidance for vascular
Introduction to transthoracic ultrasound for the pulmonologist
 Review Introduction to transthoracic ultrasound for the pulmonologist Clementine Bostantzoglou 1, Charalampos Moschos 2 1 7 th Pulmonary Department, Sotiria Hospital for Chest Diseases, Athens, Greece
Review Introduction to transthoracic ultrasound for the pulmonologist Clementine Bostantzoglou 1, Charalampos Moschos 2 1 7 th Pulmonary Department, Sotiria Hospital for Chest Diseases, Athens, Greece
Current Opinion in Anesthesiology Basic concepts in the use of thoracic and lung ultrasound
 Manuscript Number: Current Opinion in Anesthesiology Basic concepts in the use of thoracic and lung ultrasound --Manuscript Draft-- Full Title: Article Type: Corresponding Author: Basic concepts in the
Manuscript Number: Current Opinion in Anesthesiology Basic concepts in the use of thoracic and lung ultrasound --Manuscript Draft-- Full Title: Article Type: Corresponding Author: Basic concepts in the
Objectives. The Extended FAST Exam. Focused Assessment e With Sonography In. Trauma (FAST)
 Northern California Emergency Ultrasound Course Objectives The Extended FAST Exam Rimon Bengiamin, MD, RDMS UC SF Discuss the components of the EFAST exam Evaluate the utility of the EFAST Review how to
Northern California Emergency Ultrasound Course Objectives The Extended FAST Exam Rimon Bengiamin, MD, RDMS UC SF Discuss the components of the EFAST exam Evaluate the utility of the EFAST Review how to
Lung ultrasound for severe acute dyspnea evaluation in critical care patients
 Page 950 VOJNOSANITETSKI PREGLED Vojnosanit Pregl 2016; 73(10): 950 955. PRACTICAL ADVICE FOR PHYSICIANS UDC: 616-08-039.74::616.14-073.432.19 DOI: 10.2298/VSP150609085R Lung ultrasound for severe acute
Page 950 VOJNOSANITETSKI PREGLED Vojnosanit Pregl 2016; 73(10): 950 955. PRACTICAL ADVICE FOR PHYSICIANS UDC: 616-08-039.74::616.14-073.432.19 DOI: 10.2298/VSP150609085R Lung ultrasound for severe acute
Initially for cardiac echo Subsequent studies non-cardiac applications
 No disclosures But Heavy accent Initially for cardiac echo Subsequent studies non-cardiac applications 1973: Goldberg et al in JCUS 30 mediastinal masses in pts. age 1-84 yrs. 1977: Kangarloo et al in
No disclosures But Heavy accent Initially for cardiac echo Subsequent studies non-cardiac applications 1973: Goldberg et al in JCUS 30 mediastinal masses in pts. age 1-84 yrs. 1977: Kangarloo et al in
Could the use of bedside lung ultrasound reduce the number of chest x-rays in the intensive care unit?
 Brogi et al. Cardiovascular Ultrasound (2017) 15:23 DOI 10.1186/s12947-017-0113-8 RESEARCH Open Access Could the use of bedside lung ultrasound reduce the number of chest x-rays in the intensive care unit?
Brogi et al. Cardiovascular Ultrasound (2017) 15:23 DOI 10.1186/s12947-017-0113-8 RESEARCH Open Access Could the use of bedside lung ultrasound reduce the number of chest x-rays in the intensive care unit?
Ultrasound-guided Aspiration of the Iatrogenic Pneumothorax Caused by Paravertebral Block
 Case Report Korean J Pain 2012 January; Vol. 25, No. 1: 33-37 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.33 Ultrasound-guided Aspiration of the Iatrogenic Pneumothorax Caused
Case Report Korean J Pain 2012 January; Vol. 25, No. 1: 33-37 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.33 Ultrasound-guided Aspiration of the Iatrogenic Pneumothorax Caused
The Inspiration of Venue Ultrasound
 The Inspiration of Venue Ultrasound The papers that inspired the designers Venue is a special kind of ultrasound system. It has been designed for many applications. Among its capabilities is a set of tools
The Inspiration of Venue Ultrasound The papers that inspired the designers Venue is a special kind of ultrasound system. It has been designed for many applications. Among its capabilities is a set of tools
Using Ultrasound Lung Comets in the Diagnosis of High Altitude Pulmonary Edema: Fact or Fiction?
 WILDERNESS & ENVIRONMENTAL MEDICINE, 24, 159 164 (2013) REVIEW ARTICLE Using Ultrasound Lung Comets in the Diagnosis of High Altitude Pulmonary Edema: Fact or Fiction? Yashvi Wimalasena, BM, FCEM, DiMM;
WILDERNESS & ENVIRONMENTAL MEDICINE, 24, 159 164 (2013) REVIEW ARTICLE Using Ultrasound Lung Comets in the Diagnosis of High Altitude Pulmonary Edema: Fact or Fiction? Yashvi Wimalasena, BM, FCEM, DiMM;
Methods ORIGINAL ARTICLES ABSTRACT
 Bedside lung ultrasound, mobile radiography and physical examination: a comparative analysis of diagnostic tools in the critically ill Andrew J Inglis, Marek Nalos, Kwan-Hing Sue, Jan Hruby, Daniel M Campbell,
Bedside lung ultrasound, mobile radiography and physical examination: a comparative analysis of diagnostic tools in the critically ill Andrew J Inglis, Marek Nalos, Kwan-Hing Sue, Jan Hruby, Daniel M Campbell,
ARDS - a must know. Page 1 of 14
 ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
10/17/2016. Nuts and Bolts of Thoracic Radiology. Objectives. Techniques
 Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
RSV infection and lung ultrasound
 RSV infection and lung ultrasound Neonatology Clinic, University Hospital, Krakow Joanna Hurkała Joanna Pietras Agnieszka Ochoda-Mazur Poznań, 28.09.2018 1 Disclosure In relations to this presentation,
RSV infection and lung ultrasound Neonatology Clinic, University Hospital, Krakow Joanna Hurkała Joanna Pietras Agnieszka Ochoda-Mazur Poznań, 28.09.2018 1 Disclosure In relations to this presentation,
Landmark articles on ventilation
 Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Thoracic Ultrasound: Pictorial review of pneumothorax, the fastest and easiest method to diagnose.
 Thoracic Ultrasound: Pictorial review of pneumothorax, the fastest and easiest method to diagnose. Poster No.: C-1588 Congress: ECR 2014 Type: Educational Exhibit Authors: J. A. Guirola, V. Mayoral Campos,
Thoracic Ultrasound: Pictorial review of pneumothorax, the fastest and easiest method to diagnose. Poster No.: C-1588 Congress: ECR 2014 Type: Educational Exhibit Authors: J. A. Guirola, V. Mayoral Campos,
Lung ultrasound: routine practice for the next generation of internists
 REVIEW Lung ultrasound: routine practice for the next generation of internists H.R.W. Touw 1,2, P.R. Tuinman* 1,3,4, H.P.M.M. Gelissen 1, E. Lust 1, P.W.G. Elbers 1,3,4 Departments of 1 Intensive Care
REVIEW Lung ultrasound: routine practice for the next generation of internists H.R.W. Touw 1,2, P.R. Tuinman* 1,3,4, H.P.M.M. Gelissen 1, E. Lust 1, P.W.G. Elbers 1,3,4 Departments of 1 Intensive Care
Role of Transthoracic Ultrasound in Detection of Pneumonia in ICU Patients
 Med. J. Cairo Univ., Vol. 83, No. 1, June: 307-314, 2015 www.medicaljournalofcairouniversity.net Role of Transthoracic Ultrasound in Detection of Pneumonia in ICU Patients FARES AUF, M.D.; AHMED ABO-NAGLH,
Med. J. Cairo Univ., Vol. 83, No. 1, June: 307-314, 2015 www.medicaljournalofcairouniversity.net Role of Transthoracic Ultrasound in Detection of Pneumonia in ICU Patients FARES AUF, M.D.; AHMED ABO-NAGLH,
BLUE-Protocol and FALLS-Protocol Two Applications of Lung Ultrasound in the Critically Ill
 [ Recent Advances in Chest Medicine ] BLUE-Protocol and FALLS-Protocol Two Applications of Lung Ultrasound in the Critically Ill Daniel A. Lichtenstein, MD, FCCP This review article describes two protocols
[ Recent Advances in Chest Medicine ] BLUE-Protocol and FALLS-Protocol Two Applications of Lung Ultrasound in the Critically Ill Daniel A. Lichtenstein, MD, FCCP This review article describes two protocols
ECBSE Chest 29/01/2014 / 1:52 1. EFSUMB European Course Book Student Edition Editors: Jan Tuma, Radu Badea, Christoph F. Dietrich.
 ECBSE Chest 29/01/2014 / 1:52 1 EFSUMB European Course Book Student Edition Editors: Jan Tuma, Radu Badea, Christoph F. Dietrich Chest Gebhard Mathis Internistische Praxis, Rankweil, Austria Corresponding
ECBSE Chest 29/01/2014 / 1:52 1 EFSUMB European Course Book Student Edition Editors: Jan Tuma, Radu Badea, Christoph F. Dietrich Chest Gebhard Mathis Internistische Praxis, Rankweil, Austria Corresponding
Chest Sonography in the Diagnosis of Pneumothorax
 Original Article Chest Sonography in the Diagnosis of Pneumothorax Jitendra Balesa 1, Vinita Rathi 1, Sunil Kumar 2 and Anupama Tandon 1 Departments of Radiology and Imaging 1 and Surgery 2, University
Original Article Chest Sonography in the Diagnosis of Pneumothorax Jitendra Balesa 1, Vinita Rathi 1, Sunil Kumar 2 and Anupama Tandon 1 Departments of Radiology and Imaging 1 and Surgery 2, University
Case Study #2. Case Study #1 cont 9/28/2011. CAPA 2011 Christy Wilson PA C. LH is 78 yowf with PMHx of metz breast CA presents
 Case Study #1 CAPA 2011 Christy Wilson PA C 46 yo female presents with community acquired PNA (CAP). Her condition worsened and she was transferred to the ICU and placed on mechanical ventilation. Describe
Case Study #1 CAPA 2011 Christy Wilson PA C 46 yo female presents with community acquired PNA (CAP). Her condition worsened and she was transferred to the ICU and placed on mechanical ventilation. Describe
Simplified lung ultrasound protocol shows excellent prediction of extravascular lung water in ventilated intensive care patients
 Enghard et al. Critical Care (2015) 19:36 DOI 10.1186/s13054-015-0756-5 RESEARCH Open Access Simplified lung ultrasound protocol shows excellent prediction of extravascular lung water in ventilated intensive
Enghard et al. Critical Care (2015) 19:36 DOI 10.1186/s13054-015-0756-5 RESEARCH Open Access Simplified lung ultrasound protocol shows excellent prediction of extravascular lung water in ventilated intensive
CLINICAL INVESTIGATIONS. Materials and Methods
 CLINICAL INVESTIGATIONS Anesthesiology 2004; 100:9 15 2004 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Comparative Diagnostic Performances of Auscultation, Chest Radiography,
CLINICAL INVESTIGATIONS Anesthesiology 2004; 100:9 15 2004 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Comparative Diagnostic Performances of Auscultation, Chest Radiography,
Lung ultrasound in follow-up of low birth weight with respiratory distress syndrome: clinical application and reduction of x-rays examinations
 Lung ultrasound in follow-up of low birth weight with respiratory distress syndrome: clinical application and reduction of x-rays examinations Poster No.: C-1724 Congress: ECR 2011 Type: Scientific Paper
Lung ultrasound in follow-up of low birth weight with respiratory distress syndrome: clinical application and reduction of x-rays examinations Poster No.: C-1724 Congress: ECR 2011 Type: Scientific Paper
Interpreting thoracic x-ray of the supine immobile patient: Syllabus
 Interpreting thoracic x-ray of the supine immobile patient: Syllabus Johannes Godt Dep. of Radiology and Nuclear Medicine Oslo University Hospital Ullevål NORDTER 2017, Helsinki Content - Why bedside chest
Interpreting thoracic x-ray of the supine immobile patient: Syllabus Johannes Godt Dep. of Radiology and Nuclear Medicine Oslo University Hospital Ullevål NORDTER 2017, Helsinki Content - Why bedside chest
Canadian Trauma Trials Collaborative. Occult Pneumothorax in Critical Care (OPTICC): Standardized Data Collection Sheet
 Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings
 Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings Poster No.: C-2067 Congress: ECR 2017 Type: Educational Exhibit Authors: J. M. Almeida, N. Antunes, C. Leal, L. Figueiredo ; Lisboa/PT,
Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings Poster No.: C-2067 Congress: ECR 2017 Type: Educational Exhibit Authors: J. M. Almeida, N. Antunes, C. Leal, L. Figueiredo ; Lisboa/PT,
Usefulness of Cardiothoracic Chest Ultrasound in the Management of Acute Respiratory Failure in Critical Care Practice
 CHEST Original Research CRITICAL CARE Usefulness of Cardiothoracic Chest Ultrasound in the Management of Acute Respiratory Failure in Critical Care Practice Stein Silva, MD, PhD ; Caroline Biendel, MD
CHEST Original Research CRITICAL CARE Usefulness of Cardiothoracic Chest Ultrasound in the Management of Acute Respiratory Failure in Critical Care Practice Stein Silva, MD, PhD ; Caroline Biendel, MD
The efficacy of bedside chest ultrasound: from accuracy to outcomes
 EUROPEAN RESPIRATORY UPDATE EFFICACY OF BEDSIDE CHEST ULTRASOUND The efficacy of bedside chest ultrasound: from accuracy to outcomes Mark Hew 1,2 and Tunn Ren Tay 1,3 Affiliations: 1 Allergy, Immunology
EUROPEAN RESPIRATORY UPDATE EFFICACY OF BEDSIDE CHEST ULTRASOUND The efficacy of bedside chest ultrasound: from accuracy to outcomes Mark Hew 1,2 and Tunn Ren Tay 1,3 Affiliations: 1 Allergy, Immunology
4/16/2017. Learning Objectives. Interpretation of the Chest Radiograph. Components. Production of the Radiograph. Density & Appearance
 Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
Is thoracic ultrasound a viable alternative to conventional imaging in the critical care setting?
 British Journal of Anaesthesia 111 (2): 152 60 (2013) Advance Access publication 12 April 2013. doi:10.1093/bja/aet076 REVIEW ARTICLES Is thoracic ultrasound a viable alternative to conventional imaging
British Journal of Anaesthesia 111 (2): 152 60 (2013) Advance Access publication 12 April 2013. doi:10.1093/bja/aet076 REVIEW ARTICLES Is thoracic ultrasound a viable alternative to conventional imaging
Review Clinical review: Bedside lung ultrasound in critical care practice Bélaïd Bouhemad 1, Mao Zhang 2, Qin Lu 1 and Jean-Jacques Rouby 1
 Review Clinical review: Bedside lung ultrasound in critical care practice Bélaïd Bouhemad 1, Mao Zhang 2, Qin Lu 1 and Jean-Jacques Rouby 1 1 Surgical Intensive Care Unit, Pierre Viars, Department of Anesthesiology
Review Clinical review: Bedside lung ultrasound in critical care practice Bélaïd Bouhemad 1, Mao Zhang 2, Qin Lu 1 and Jean-Jacques Rouby 1 1 Surgical Intensive Care Unit, Pierre Viars, Department of Anesthesiology
Ultrasound basics Part 1
 Ultrasound basics Part 1 'Ultrasound enhanced critical care medicine' Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville,
Ultrasound basics Part 1 'Ultrasound enhanced critical care medicine' Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville,
Role of Chest Ultrasonography in the Diagnosis of Acute Pulmonary Edema.
 Role of Chest Ultrasonography in the Diagnosis of Acute Pulmonary Edema Tamer Abudalla Helmy 1, Mamdouh Zidan 2 and Mohamed Khamis 1 1. Department of Critical Care Medicine, Faculty of Medicine, Alexandria
Role of Chest Ultrasonography in the Diagnosis of Acute Pulmonary Edema Tamer Abudalla Helmy 1, Mamdouh Zidan 2 and Mohamed Khamis 1 1. Department of Critical Care Medicine, Faculty of Medicine, Alexandria
Introduction to Chest Radiography
 Introduction to Chest Radiography RSTH 366: DIAGNOSTIC TECHNIQUES Alan Alipoon BS, RCP, RRT Instructor Department of Cardiopulmonary Sciences 1 Introduction Discovered in 1895 by Wilhelm Roentgen Terminology
Introduction to Chest Radiography RSTH 366: DIAGNOSTIC TECHNIQUES Alan Alipoon BS, RCP, RRT Instructor Department of Cardiopulmonary Sciences 1 Introduction Discovered in 1895 by Wilhelm Roentgen Terminology
Management of Pleural Effusion
 Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
"Pediatric chest: From x-ray to ultrasound. A pictorial review of 173 patients"
 "Pediatric chest: From x-ray to ultrasound. A pictorial review of 173 patients" Poster No.: C-0451 Congress: ECR 2014 Type: Educational Exhibit Authors: S. FYGETAKI, I. Tritou, S. Stefanaki, S. Antonopoulos,
"Pediatric chest: From x-ray to ultrasound. A pictorial review of 173 patients" Poster No.: C-0451 Congress: ECR 2014 Type: Educational Exhibit Authors: S. FYGETAKI, I. Tritou, S. Stefanaki, S. Antonopoulos,
A pictorial review of thoracic imaging of intensive care patients
 A pictorial review of thoracic imaging of intensive care patients Poster No.: C-1003 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: E. Y. P. Lee, H. C. Mathias; Cardiff/UK Keywords:
A pictorial review of thoracic imaging of intensive care patients Poster No.: C-1003 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: E. Y. P. Lee, H. C. Mathias; Cardiff/UK Keywords:
The new ARDS definitions: what does it mean?
 The new ARDS definitions: what does it mean? Richard Beale 7 th September 2012 METHODS ESICM convened an international panel of experts, with representation of ATS and SCCM The objectives were to update
The new ARDS definitions: what does it mean? Richard Beale 7 th September 2012 METHODS ESICM convened an international panel of experts, with representation of ATS and SCCM The objectives were to update
Clinical Study Lung Ultrasound Diagnostic Accuracy in Neonatal Pneumothorax
 Canadian Respiratory Journal Volume 2016, Article ID 6515069, 5 pages http://dx.doi.org/10.1155/2016/6515069 Clinical Study Lung Ultrasound Diagnostic Accuracy in Neonatal Pneumothorax Luigi Cattarossi,
Canadian Respiratory Journal Volume 2016, Article ID 6515069, 5 pages http://dx.doi.org/10.1155/2016/6515069 Clinical Study Lung Ultrasound Diagnostic Accuracy in Neonatal Pneumothorax Luigi Cattarossi,
Systematic review and meta analysis for the use of ultrasound versus radiology in diagnosing of pneumonia
 DOI 10.1186/s13089-017-0059-y REVIEW Open Access Systematic review and meta analysis for the use of ultrasound versus radiology in diagnosing of pneumonia Saeed Ali Alzahrani 1, Majid Abdulatief Al Salamah
DOI 10.1186/s13089-017-0059-y REVIEW Open Access Systematic review and meta analysis for the use of ultrasound versus radiology in diagnosing of pneumonia Saeed Ali Alzahrani 1, Majid Abdulatief Al Salamah
World Journal of Radiology
 W J R World Journal of Radiology Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4329/wjr.v6.i6.230 World J Radiol 2014 June 28; 6(6): 230-237
W J R World Journal of Radiology Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4329/wjr.v6.i6.230 World J Radiol 2014 June 28; 6(6): 230-237
The Irregular Diaphragmatic Pleural Interface
 CSE SERIES The Irregular Diaphragmatic Pleural Interface Novel Sonographic Sign Facilitating the Diagnosis of Pneumonia Jacob O. vila, MD, RDMS, Vicki E. Noble, MD Videos online at www.jultrasoundmed.org
CSE SERIES The Irregular Diaphragmatic Pleural Interface Novel Sonographic Sign Facilitating the Diagnosis of Pneumonia Jacob O. vila, MD, RDMS, Vicki E. Noble, MD Videos online at www.jultrasoundmed.org
Best of Pulmonary Jennifer R. Hucks, MD University of South Carolina School of Medicine
 Best of Pulmonary 2012-2013 Jennifer R. Hucks, MD University of South Carolina School of Medicine Topics ARDS- Berlin Definition Prone Positioning For ARDS Lung Protective Ventilation In Patients Without
Best of Pulmonary 2012-2013 Jennifer R. Hucks, MD University of South Carolina School of Medicine Topics ARDS- Berlin Definition Prone Positioning For ARDS Lung Protective Ventilation In Patients Without
Chest X rays and Case Studies. No disclosures. Outline 5/31/2018. Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital
 Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Chapter 17 Lung Ultrasound in Anaesthesia and Critical Care Medicine
 Chapter 17 Lung Ultrasound in Anaesthesia and Critical Care Medicine David Canty, Kavi Haji, André Denault, and Alistair Royse Abstract Lung ultrasound (respiratory or thoracic ultrasound) has traditionally
Chapter 17 Lung Ultrasound in Anaesthesia and Critical Care Medicine David Canty, Kavi Haji, André Denault, and Alistair Royse Abstract Lung ultrasound (respiratory or thoracic ultrasound) has traditionally
Original Article Ultrasound reaeration scores to assess lung recruitment in rabbits with acute respiratory distress syndrome
 Int J Clin Exp Med 2018;11(8):7761-7769 www.ijcem.com /ISSN:1940-5901/IJCEM0077713 Original Article Ultrasound reaeration scores to assess lung recruitment in rabbits with acute respiratory distress syndrome
Int J Clin Exp Med 2018;11(8):7761-7769 www.ijcem.com /ISSN:1940-5901/IJCEM0077713 Original Article Ultrasound reaeration scores to assess lung recruitment in rabbits with acute respiratory distress syndrome
B. Chinardet, H. Brisson, C. Arbelot, O. Langeron, J.-J. Rouby and Q. Lu
 (Acta Anaesth. Belg., 2016, 67, 29-35) Ultrasound assessment of lung consolidation and reaeration after pleural effusion drainage in patients with Acute Respiratory Distress Syndrome : a pilot study B.
(Acta Anaesth. Belg., 2016, 67, 29-35) Ultrasound assessment of lung consolidation and reaeration after pleural effusion drainage in patients with Acute Respiratory Distress Syndrome : a pilot study B.
Lung Ultrasound Predicts Well Extravascular Lung Water but Is of Limited Usefulness in the Prediction of Wedge Pressure
 CRITICAL CARE MEDICINE Lung Ultrasound Predicts Well Extravascular Lung Water but Is of Limited Usefulness in the Prediction of Wedge Pressure Giovanni Volpicelli, M.D.,
CRITICAL CARE MEDICINE Lung Ultrasound Predicts Well Extravascular Lung Water but Is of Limited Usefulness in the Prediction of Wedge Pressure Giovanni Volpicelli, M.D.,
Shedding Light on Neonatal X-rays. Objectives. Indications for X-Rays 5/14/2018
 Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
Diagnostic Accuracy of Ultrasonography in the Acute Assessment of Common Thoracic Lesions After Trauma
 CHEST Original Research CRITICAL CARE Diagnostic Accuracy of Ultrasonography in the Acute Assessment of Common Thoracic Lesions After Trauma Anne-Claire Hyacinthe, MD ; Christophe Broux, MD ; Gilles Francony,
CHEST Original Research CRITICAL CARE Diagnostic Accuracy of Ultrasonography in the Acute Assessment of Common Thoracic Lesions After Trauma Anne-Claire Hyacinthe, MD ; Christophe Broux, MD ; Gilles Francony,
Efficacy of ultrasonography and computed tomography in differentiating transudate from exudate in patients with pleural effusion
 Efficacy of ultrasonography and computed tomography in differentiating transudate from exudate in patients with pleural effusion Purpose: To evaluate USG and CT imaging findings in differentiating transudative
Efficacy of ultrasonography and computed tomography in differentiating transudate from exudate in patients with pleural effusion Purpose: To evaluate USG and CT imaging findings in differentiating transudative
Pneumothorax. Defined as air in the pleural space which can occur through a number of mechanisms
 Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis?
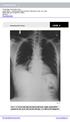 1 Interpreting Chest X-Rays CASE 1 Fig. 1.1 Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis? CASE 1 Interpreting
1 Interpreting Chest X-Rays CASE 1 Fig. 1.1 Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis? CASE 1 Interpreting
New respiratory symptoms and lung imaging findings in a woman with polymyositis
 Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Initially for cardiac echo Subsequent studies non-cardiac applications
 Initially for cardiac echo Subsequent studies non-cardiac applications 1973: Goldberg et al in JCUS 30 mediastinal masses in pts. age 1-84 yrs. 1977: Kangarloo et al in Radiology Juxtadiaphragmatic lesions
Initially for cardiac echo Subsequent studies non-cardiac applications 1973: Goldberg et al in JCUS 30 mediastinal masses in pts. age 1-84 yrs. 1977: Kangarloo et al in Radiology Juxtadiaphragmatic lesions
ACUTE RESPIRATORY DISTRESS SYNDROME
 ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
Diagnostic Approach to Pleural Effusion
 Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Comparison of automated and static pulse respiratory mechanics during supported ventilation
 Comparison of automated and static pulse respiratory mechanics during supported ventilation Alpesh R Patel, Susan Taylor and Andrew D Bersten Respiratory system compliance ( ) and inspiratory resistance
Comparison of automated and static pulse respiratory mechanics during supported ventilation Alpesh R Patel, Susan Taylor and Andrew D Bersten Respiratory system compliance ( ) and inspiratory resistance
MRSA pneumonia mucus plug burden and the difficult airway
 Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Lung ultrasound a primary survey of the acutely dyspneic patient
 Lee Journal of Intensive Care (2016) 4:57 DOI 10.1186/s40560-016-0180-1 REVIEW Lung ultrasound a primary survey of the acutely dyspneic patient Francis Chun Yue Lee 1,2 Open Access Abstract There has been
Lee Journal of Intensive Care (2016) 4:57 DOI 10.1186/s40560-016-0180-1 REVIEW Lung ultrasound a primary survey of the acutely dyspneic patient Francis Chun Yue Lee 1,2 Open Access Abstract There has been
PATIENT DATA EVALUATION AND RECOMMENDATION: IMAGING STUDIES
 PATIENT DATA EVALUATION AND RECOMMENDATION: IMAGING STUDIES Robert Harwood, MSA, RRT-NPS Objectives At the end of this presentation the student should be able to: Describe the indications of a chest radiograph.
PATIENT DATA EVALUATION AND RECOMMENDATION: IMAGING STUDIES Robert Harwood, MSA, RRT-NPS Objectives At the end of this presentation the student should be able to: Describe the indications of a chest radiograph.
Ultrasonido Pulmonar. Dra. Adriana Denise Zepeda Mendoza. Medicina de Urgencias Medicina del Enfermo en Estado Crí=co Grupo GMEMI.
 Ultrasonido Pulmonar. Dra. Adriana Denise Zepeda Mendoza. Medicina de Urgencias Medicina del Enfermo en Estado Crí=co Grupo GMEMI. Obje=vos Conocer los diferentes patrones ultrasonográficos pulmonares.
Ultrasonido Pulmonar. Dra. Adriana Denise Zepeda Mendoza. Medicina de Urgencias Medicina del Enfermo en Estado Crí=co Grupo GMEMI. Obje=vos Conocer los diferentes patrones ultrasonográficos pulmonares.
POCUS for the Internist: Lungs & Pericardial Effusions
 POCUS for the Internist: Lungs & Pericardial Effusions Jeremy S. Boyd, MD, FACEP Asst. Professor of Emergency Medicine Vanderbilt University Medical Illustrations courtesy of Robinson Ferre, MD, FACEP
POCUS for the Internist: Lungs & Pericardial Effusions Jeremy S. Boyd, MD, FACEP Asst. Professor of Emergency Medicine Vanderbilt University Medical Illustrations courtesy of Robinson Ferre, MD, FACEP
TB Radiology for Nurses Garold O. Minns, MD
 TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
EUROPEAN ASSOCIATION OF VETERINARY DIAGNOSTIC IMAGING EUROPEAN COLLEGE OF VETERINARY DIAGNOSTIC IMAGING
 EISAGOGIKO EUROPEAN ASSOCIATION OF VETERINARY DIAGNOSTIC IMAGING EUROPEAN COLLEGE OF VETERINARY DIAGNOSTIC IMAGING ARISTOTLE UNIVERSITY OF THESSALONIKI SCHOOL OF VETERINARY MEDICINE SECTION OF RADIOLOGY
EISAGOGIKO EUROPEAN ASSOCIATION OF VETERINARY DIAGNOSTIC IMAGING EUROPEAN COLLEGE OF VETERINARY DIAGNOSTIC IMAGING ARISTOTLE UNIVERSITY OF THESSALONIKI SCHOOL OF VETERINARY MEDICINE SECTION OF RADIOLOGY
Role of chest ultrasonography in the prognostic evaluation of patients with community acquired pneumonia: a prospective study
 International Journal of Research in Medical Sciences Rennis KD et al. Int J Res Med Sci. 2017 Jan;5(1):25-30 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20164510
International Journal of Research in Medical Sciences Rennis KD et al. Int J Res Med Sci. 2017 Jan;5(1):25-30 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20164510
The clinical sign of pleurisy is characterized by a
 Contrast-Enhanced Sonography for Differential Diagnosis of Pleurisy and Focal Pleural Lesions of Unknown Cause* Christian Görg, MD; Tillmann Bert, MD; and Konrad Görg, MD Background: Ultrasound enables
Contrast-Enhanced Sonography for Differential Diagnosis of Pleurisy and Focal Pleural Lesions of Unknown Cause* Christian Görg, MD; Tillmann Bert, MD; and Konrad Görg, MD Background: Ultrasound enables
Accuracy of lung ultrasonography in diagnosis of community acquired pneumonia in hospitalized children as compared to chest x-ray
 International Journal of Contemporary Pediatrics Tirdia PR et al. Int J Contemp Pediatr. 2016 Aug;3(3):1026-1031 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Research Article DOI: http://dx.doi.org/10.18203/2349-3291.ijcp20162385
International Journal of Contemporary Pediatrics Tirdia PR et al. Int J Contemp Pediatr. 2016 Aug;3(3):1026-1031 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Research Article DOI: http://dx.doi.org/10.18203/2349-3291.ijcp20162385
