suggested by Katz and Gauchat (3) for the ex- diaphragm during inspiration, traction is applied Dornhorst, Howard, and Leathart (2), using an
|
|
|
- Lorena Edwards
- 5 years ago
- Views:
Transcription
1 Journal of Clinical Investigation Vol. 42, No. 2, 1963 THE MECHANISM OF PULSUS PARADOXUS DURING ACUTE PERICARDIAL TAMPONADE * By RICHARD J. GOLINKO,t NEVILLE KAPLAN, AND ABRAHAM M. RUDOLPH t (From the Departments of Pediatrics and Radiology, Albert Einstein College of Medicine, New York, N. Y.) (Submitted for publication June 5, 1962; accepted November 1, 1962) A small fall in systemic arterial pressure during inspiration has been observed to occur in normal individuals. The term "pulsus paradoxus" has been applied to an accentuation of this phenomenon as it occurs in patients with pericardial tamponade. The mechanism for this increased respiratory variation of systemic arterial pressure during pericardial tamponade has interested many observers. Several explanations, based on observations in experimental animals and man, have been proposed to explain the hemodynamic alterations responsible for pulsus paradoxus. Wood (1) has suggested that with the descent of the diaphragm during inspiration, traction is applied to the pericardium, raising intrapericardial pressure and interfering with left ventricular filling. Dornhorst, Howard, and Leathart (2), using an experimental model, claimed that filling of the right ventricle during inspiration raised intrapericardial pressure, which then interfered with left ventricular filling. Much earlier, Katz and Gauchat (3) demonstrated a decrease in the pressure gradient between superior vena cava and right atrium during inspiration. On the basis of this observation, they postulated that a similar mechanism on the left side could explain the paradoxical pulse in pericardial tamponade. Recently, Sharp and co-workers (4) had an opportunity to perform an acute tamponade experiment in a man who required permanent cannulation of the pericardial sac. Their data, not based on actual measurement of pulmonary venous and left atrial pressures, indicated that the mechanism suggested by Katz and Gauchat (3) for the ex- * Supported by grant H-5686 from the U. S. Public Health Service and a grant-in-aid from the American Heart Association; presented in part at the American Heart Association meetings, Miami, Fla., October, t Research Fellow, U. S. Public Health Service. t Established Investigator, American Heart Association. aggerated respiratory variation in systemic arterial pressure probably also applied to man. Since the pulmonary veins are thin-walled structures higaly susceptible to fluctuations in intrathoracic pressure, we considered a disturbance of the gradient between pulmonary venous and left atrial pressure as a possible explanation for the fundamental circulatory defect responsible for the exaggerated respiratory variation in pulse that is characteristic of pericardial tamponade. This study was designed to investigate this possibility and thereby further clarify the dynamics of pulsus paradoxus. METHODS Five mongrel dogs weighing 15 to 20 kg were anesthetized with intravenous sodium pentobarbital, 30 mg per kg. An endotracheal tube with rubber cuff was inserted and positive-pressure ventilation was maintained by means of a Harvard respiratory pump. A positive end-expiratory pressure of 3 cm water was maintained to prevent collapse of the lungs when the chest was opened. The chest was opened by a transverse thoracotomy in the fourth left intercostal space. Through a small opening in the pericardium, polyvinyl catheters (0.070 inch outside diameter, inch inside diameter) were inserted into the left atrium through the appendage and into the left ventricle. A no. 14 thin-walled needle was inserted in the left lower pulmonary vein beyond the left atrial junction through a purse-string suture. A soft polyvinyl catheter (0.052 inch outside diameter, inch inside diameter) was inserted through the needle, which was then removed over the catheter. The tip of the catheter was placed in the "free" left lower pulmonary vein 1.5 to 2 cm beyond its junction with the left atrium and secured in position. Before the pericardium was closed, two additional polyvinyl catheters were fixed in position in the pericardial space for measurement of intrapericardial pressure and for infusion and withdrawal of fluid. The pericardium was then closed and examined carefully for any leakage. Intrathoracic pressure was measured with either an intraesophageal balloon or a polyvinyl catheter located in the intrapleural space. All catheters were exteriorized and the chest closed. Pres- 249
2 250 LV RICHARD J. GOLINKO, NEVILLE KAPLAN, AND ABRAHAM M. RUDOLPH CONTROL LA 0 PV PERI.IE FIG. 1. THE EFFECT OF NORMAL RESPIRATION ON LEFT VENTRICULAR, LEFT ATRIAL, PULMONARY VENOUS, AND PERICARDIAL PRESSURES IN THE CONTROL ANIMAL. sures were measured by means of Statham P 23D pressure transducers and continually recorded on a Grass direct-writing polygraph. In two experiments, cardiac output was determined by indicator dilution techniques (5) using indocyanine green. In one additional experiment, phasic aortic flow was measured by a gated, sinewave, electromagnetic flowmeter of the Kolin type with the cuff flow transducer placed around the descending aorta. After the chest was closed, pressures in the various segments were recorded simultaneously and the effects of the normal respiratory pattern observed. In order to exaggerate the respiratory changes, the effect of increased negative ventilation was also studied by use of a two-way respiratory valve, which permitted graded occlusion of the inspiratory side of the valve. All observations were made during varying degrees of pericardial tamponade produced by infusion and withdrawal of normal saline. The amounts of saline infused to produce tamponade varied from 100 to 180 ml, depending on the size of the animal. In two further experiments, pulmonary venous and inferior vena caval flow rates were studied by means of cineangiography. Small droplets of iodinized oil (Lipiodol) were injected into the inferior vena cava and pulmonary vein, and the rate and direction of flow were observed during the respiratory phases with and without pericardial tamponade. RESULTS ISO The production of pulsus paradoxus by introduction of fluid into the pericardial space was demonstrated by measurement of systemic arterial or left ventricular pressure. A small respiratory fluctuation in left ventricular systolic pressure was noted with a slightly lower pressure in inspiration and a greater pressure in expiration with an average variation of 2 to 8 mm Hg in the control animal (Figure 1). During pericardial tamponade, a significant, increased, respiratory fluctuation of left ventricular systolic pressure developed averaging 15 to 22 mm Hg (Figure 2). In several instances, when the degree of pericardial tamponade was extreme and systemic pressure markedly reduced, the pulsus paradoxus disappeared. Analysis of the aortic flow tracings showed that the pressure phenomena were directly related to changes in blood flow so that any fall in left ventricular systolic pressure was accompanied by a corresponding reduction in aortic blood flow. Cardiac output in the normal animal averaged 4.7 L per minute, but was reduced during pericardial tamponade to 1.7 L per minute. Intrapericardial pressure. In the control animal, intrapericardial pressure levels were close to those of intrathoracic pressures and showed wide fluctuation with respiration (Tables I and II, Figure 1). During the period of increasing pericardial tamponade, intrapericardial pressure rose sharply after each increment of fluid. This LVA LA TAMPONADE 5V--~-JV.20 PV = Rio' PERI' 1E FIG. 2. THE EFFECT OF NORMAL RESPIRATION ON LEFT VENTRICULAR, LEFT ATRIAL, PULMONARY VENOUS, AND PERICARDIAL PRESSURES DURING PERICARDIAL TAMPONADE. loo en
3 PULSUS PARADOXUS IN ACUTE PERICARDIAL TAMPONADE 251 TABLE I Average pressures measured in 5 experiments Control Tamponade Pressure Inspiration Expiration Inspiration Expiration mm Hg mm Hg Left atrial Pulmonary venous Pericardial Intrathoracic Pulmonary venous-left atrial was followed immediately by a period of adjustment and small fall in pressure, and the intrapericardial pressure finally became stable at a level slightly greater than that of control. With increasing degrees of pericardial tamponade, intrapericardial pressure gradually reached levels averaging 11 to 14 mm Hg. The contour of the intrapericardial pressure tracing, which in the control animal closely resembled the intrathoracic pressure tracing, in the presence of pericardial tamponade showed a disapearance or marked diminution of respiratory fluctuation, and the pressure closely approximated left atrial pressure (Tables I and III, Figure 2). In one experiment in which inspiratory obstruction was used to exaggerate negative pressure ventilation, only minimal fluctuation of intrapericardial pressure was observed despite wide fluctuations of intrathoracic pressure. Pulmonary venous and left atrial pressures. In the animal with normal respiration and without pericardial tamponade, both pulmonary venous and left atrial pressures fluctuated considerably with respiration (Figure 1). Pulmonary venous pressure was consistently greater than left atrial pressure during all phases of respiration, although TABLE II Pressures (mm Hg) measured without pericardial tamponade during a single experiment Pul- mon- Pul- ary mon- Peri- venous- Breath- Left ary car- Intratho- left ing atrial venous dial racic atrial Exp Exp Exp the gradient from the pulmonary venous to left atrial pressure was maximal during expiration and minimal during inspiration (Tables I and II). This respiratory variation of the magnitude of the gradient between pulmonary venous and left atrial pressures is clearly shown when these two pressures are graphically superimposed (Figure 3). Measurements of pulmonary venous and left atrial pressure during various phases of ventricular systole and diastole indicated that respiratory fluctuation and the relationship between pulmonary venous and left atrial pressure were not altered by the phase of the cardiac cycle. During pericardial tamponade, left atrial and pericardial pressures usually fluctuated less than pulmonary venous pressure with respiration (Figure 2). In one experiment in which respiration was accentuated by inspiratory obstruction, pulmonary venous pressure showed wide fluctuation with respiration while left atrial pressure remained relatively constant (Figure 4). The gradient between pulmonary venous and left atrial pressure was markedly altered during tamponade. Although pulmonary venous pressure continued to exceed left atrial pressure during expiration, dur- TABLE III Pressures (mm Hg) measured with pericardial tamponade during a single experiment Pulmonary Pul- venous- Left monary Peri- Intratho- left atrial venous cardial racic atrial Exp Exp Exp Exp
4 = 8 E RICHARD J. GOLINKO, NEVILLE KAPLAN, AND ABRAHAM M. RUDOLPH Pv LA (- a) J 0 FIG. 3. THE EFFECT OF CONTROL - NORMAL RESPI RATION NORMAL RESPIRATION ON THE GRADIENT BETWEEN PULMONARY VENOUS AND LEFT ATRIAL PRESSURES IN THE CONTROL ANIMAL. ing inspiration it usually was- equal to or below left atrial pressure. 'This resulted in a negative or reversed gradient between pulmonary venous and left atrial pressure during inspiration (Tables I and III). These relationships are clearly shown in Figures 4 and 5, in which pulmonary venous and left atrial pressures are graphically superimposed. Figure 2 shows how pulmonary venous pressure was affected by intrapleural pressure, whereas left atrial pressure followed intrapericardial pressure during tamponade. Cineangiograms. In the control animal, when iodinated oil was injected into the inferior vena I nsp. I nsp. 12 I I Pv I 8 1 OA w 4 Go _w LA 0 TAMPONADE with INSPIRATORY OBSTRUCTION FIG. 4. THE EFFECT OF INCREASED NEGATIVE VENTILATION ON THE GRADIENT BETWEEN PULMONARY VENOUS AND LEFT ATRIAL PRESSURE DURING PERICARDIAL TAMPONADE.
5 PULSUS PARADOXUS IN ACUTE PERICARDIAL TAMPONADE I Pv 12 * LA I n in en a) I TAMPONADE NORMAL RESPIRATION FIG. 5. THE EFFECT OF NORMAL RESPIRATION ON THE GRADIENT BETWEEN PULMONARY VENOUS AND LEFT ATRIAL PRESSURE DURING PERICARDIAL TAMPONADE. cava, the droplets moved towards the right atrium during all phases of respiration, but with maximal velocity during inspiration. During injection into the left upper pulmonary vein, the droplets moved towards the left atrium during all phases of respiration, but with maximum velocity during expiration. After production of pericardial tamponade and in the presence of pulsus paradoxus, the movement of the droplets in the inferior vena cava was reduced during all phases of respiration, but during expiration it was almost halted or actually reversed (Figure 6). The movement of the oil droplets in the pulmonary vein was also slowed during all phases of respiration. Whereas maximal forward velocity occurred with expiration, however, there was now marked decrease in forward movement of the droplets during inspiration, and actual retrograde movement was observed in some instances. In one instance, a large amount of opaque oil was injected into the left atrium during pericardial tamponade. A large globule of oil remained in the left atrium after the injection was completed, allowing the effects of respiration on pulmonary venous flow to be clearly observed. During expiration the globule was located entirely within the left atrium, but with inspiration there was a marked retrograde movement of the opaque material into the pulmonary veins, extending even into the major tributaries (Figure 7). This provided conclusive evidence of reversal of pulmonary venous flow during inspiration. DISCUSSION The results of the present study indicate that an abnormal gradient between pulmonary venous and left atrial pressure is the major underlying hemodynamic alteration responsible for pulsus paradoxus. Katz and Gauchat (3) in 1924 first suggested that the marked inspiratory fall in systemic arterial pressure observed during tamponade was related to reduced filling of the left ventricle. This was based entirely on indirect evidence resulting from observations of measured pressure gradients between superior vena cava and right atrium. These authors noted that during tamponade the pressure gradient between the superior
6 254 RICHARD J. GOLINKO, NEVILLE KAPLAN, AND ABRAHAM M. RUDOLPH vena cava and the right atrium was reduced during inspiration. This finding, coupled with the observation that during tamponade the respiratory fluctuations of intrapericardial pressure disappeared, suggested to them that intrathoracic pressure was not equally transmitted to intrapericardial and extrapericardial structures, in the presence of pericardial tamponade. They postulated that this reduction of the gradient between the filling veins and the right heart probably also occurred between the pulmonary veins and the left heart. Thus, reduced filling of the left ventricle during inspiration might occur and would then result in a lowered left ventricular stroke output and systemic arterial pressure. During a study of experimental tamponade, Isaacs, Berglund, and Sarnoff (6) measured gradients between pulmonary venous and left atrial pressures, but failed to demonstrate any significant gradient. Since their study was performed in the open-chest animal maintained on positive-pressure breathing, it does not apear to have any direct application to the present discussion. More recently, Sharp and co-workers (4) studied the hemodynamic effects of induced cardiac tamponade in man. They were able to study the relationship of pulmonary arterial wedge pressure to intrapericardial pressure during varying degrees of pericardial tamponade. Their data indicated that the filling gradient of the left ventricle was reduced during inspiration, thus corroborating the hypothesis suggested by Katz and Gauchat some years earlier. Their data, however, were based on measurements of pulmonary artery wedge and DYE P A DA WC -CATHETER "\DYE FIG. 6. THE EFFECT OF NORMAL RESPIRATION ON INFERIOR VENA CAVAL FLOW DURING PERICARDIAL TAMPONADE. A. Droplet streaming into right atrium during inspiration. B. Droplet extending retrograde in the inferior vena cava during expiration.
7 PULSUS PARADOXUS IN ACUTE PERICARDIAL TAMPONADE 255 CATHETER I N AORTA FIG. 7. THE EFFECT OF NORMAL RESPIRATION ON PULMONARY VENOUS FLOW DURING PERICARDIAL TAMPONADE. A. Left atrium and pulmonary veins during injection of opaque material into the left atrium. B. Retained globule within the left atrium during expiration. C. Retained globule extending retrograde into pulmonary veins during inspiration. LA
8 256 RICHARD J. GOLINKO, NEVILLE KAPLAN, AND ABRAHAM M. RUDOLPH intrapericardial pressures, and actual pulmonary venous and left atrial pressures were not measured. The present study offers direct evidence that the mechanism for pulsus paradoxus resides in the altered relationship between pulmonary venous and left atrial pressure during the respiratory cycle. Normally, the variations in intrathoracic pressures are well transmitted to the pericardial space. Even under normal conditions, however, the intrathoracic pressure changes do not equally affect left atrial and pulmonary venous pressures so that there is a small reduction in the gradient between pulmonary venous and left atrial pressure during inspiration. This would interfere with left atrial and left ventricular filling and would explain the lowered left ventricular ejection and systemic arterial pressure observed during inspiration under normal conditions. During pericardial tamponade, the fluid under high pressure in the pericardial space interferes markedly with transmission of the negative pressure to the left atrium during inspiration. During tamponade, left atrial pressure tends to follow intrapericardial pressure rather than intrathoracic pressure, while pulmonary venous pressure continues to show wide fluctuations with changes in intrathoracic pressure. Thus during inspiration a disproportionate fall in pulmonary venous pressure may occur as compared to left atrial pressure, resulting in a fall or actual reversal of the normal filling gradient of the left atrium. This interferes with left atrial and left ventricular filling even more than usual during inspiration, exaggerating the normal drop in left ventricular stroke volume and systemic arterial pressure. In several instances where the degree of pericardial tamponade was extreme and systemic pressure markedly reduced, the pulsus paradoxus disappeared. This might have been due to reduction of the total cardiac output. Another possible explanation, however, might be that as the pulmonary veins became more and more distended they lost their capacity to expand further in response to changes in intrathoracic pressure. An interesting concept relating to mechanics of left ventricular filling is presented in this study. In some experiments, a constant level of left atrial pressure was observed throughout the respiratory cycle during pericardial tamponade. Despite this constant filling pressure of the left ventricle, there was a marked variation in its stroke output. It is possible that very minor differences in filling pressure, not measurable by the methods used, could account for these observations. The phenomenon could also be explained on the basis of a different effective compliance of the left atrial and ventricular walls during tamponade. In the normal animal, filling of the left ventricle will depend on the filling pressure and the compliance of the wall. During tamponade, a constant external pressure is applied to the ventricle, markedly limiting its distensibility. During diastole there is direct communication between the left ventricle, left atrium, and pulmonary veins. The amount of blood flow from left atrium into left ventricle may therefore be influenced by retrograde flow into the pulmonary veins. Thus even in the face of a constant left atrial pressure, occasioned by the constant external pressure from the pericardial sac, the flow from left atrium into left ventricle, and hence left ventricular volume in diastole, may vary. During inspiration, when pulmonary venous pressure falls below left atrial and intrapericardial pressure and retrograde flow into the pulmonary veins occurs, left ventricular filling may be reduced. During expiration, when pulmonary venous pressure exceeds left atrial pressure, greater filling of the left ventricle may occur. It is interesting that the cineangiogram studies we conducted suggest that maximal filling of the right atrium during tamponade occurs during inspiration. Katz and Gauchat (3), on the other hand, from their measurements of gradients between superior vena caval and right atrial pressures, indicated that maximal filling of the right atrium would occur during expiration when the gradient is most favorable. A possible explanation for this difference seems to rest in the nature of the superior vena cava as an intrathoracic but extrapericardial vessel, subjected to respiratory fluctuations similar to those of the pulmonary veins. The inferior vena cava, on the other hand, is largely extrathoracic and during tamponade would not be subjected to the same extent to changes in intrathoracic pressure. Brecher (7) has in fact shown that inferior vena caval pressure actually increases during inspiration owing to descent of the diaphragm and the pressure exerted on it.
9 PULSUS PARADOXUS IN ACUTE PERICARDIAL TAMPONADE 257 SUMMARY The mechanism responsible for the increased respiratory variation of systemic arterial pressure during pericardial tamponade (pulsus paradoxus) was studied in the closed-chest animal. Simultaneous measurements of pulmonary venous, left atrial, left ventricular, intrapericardial, and intrathoracic pressures were made during varying degrees of pericardial tamponade, and the effects of both normal ventilation and increased negative ventilation observed. Pulmonary venous and inferior vena caval flow rates were studied by cineangiography. Results indicate that a disturbance of the gradient between pulmonary venous and left atrial pressures is the fundamental circulatory defect responsible for the exaggerated respiratory variation in pulse, characteristic of pericardial tamponade. In pericardial tamponade, pulmonary venous pressure follows intrathoracic pressure, whereas left atrial pressure follows intrapericardial pressure, resulting in a marked reduction or actual reversal of the gradient between pulmonary venous and left atrial pressure during inspiration. This interferes with left ventricular filling even more than usual during inspiration, exaggerating the decrease in left ventricular stroke volume and the fall in systemic arterial pressure. This hypothesis was further confirmed by the cineangiograms, which demonstrated reversal of flow in the pulmonary veins during inspiration in pericardial tamponade. REFERENCES 1. Wood, P. Diseases of the Heart and Circulation, 1st ed. London, J. B. Lippincott, Dornhorst, A. C., Howard, P., and Leathart, G. L. Pulsus paradoxus. Lancet, 1952, 262, Katz, L. N., and Gauchat, H. W. Observations on pulsus paradoxus (with special reference to pericardial effusions): II. Experimental. Arch. intern. Med. 1924, 33, Sharp, J. T., Bunnell, I. L., Holland, J. F., Griffith, G. T., and Greene, D. G. Hemodynamics during induced cardiac tamponade in man. Amer. J. Med. 1960, 29, Kinsman, J. M., Moore, J. W., and Hamilton, W. F. Studies on the circulation. I. Injection method: physical and mathematical considerations. Amer. J. Physiol. 1929, 89, Isaacs, J. P., Berglund, E., and Sarnoff, S. J. Ventricular function. III. The pathologic physiology of acute cardiac tamponade studied by means of ventricular function curves. Amer. Heart J. 1954, 48, Brecher, G. A. Venous Return. New York, Grune & Stratton, 1956.
Research. Relationship of Pericardial to Pleural Pressure During Quiet Respiration and Cardiac Tamponade
 Research JUNE VOL. XVI An Official Journal of the American Heart Association 19 NO. Relationship of Pericardial to Pleural Pressure During Quiet Respiration and Cardiac Tamponade M.D., Warren G. Gunrherorh,
Research JUNE VOL. XVI An Official Journal of the American Heart Association 19 NO. Relationship of Pericardial to Pleural Pressure During Quiet Respiration and Cardiac Tamponade M.D., Warren G. Gunrherorh,
stroke volume in cardiac tamponade
 British Heart journal, 1970, 32, 592-596. Effect of respiration on venous return and stroke volume in cardiac tamponade I. T. Gabe, D. T. Mason, J. H. Gault, J. Ross, Jr., R. Zelis, C. J. Mills, E. Braunwald,
British Heart journal, 1970, 32, 592-596. Effect of respiration on venous return and stroke volume in cardiac tamponade I. T. Gabe, D. T. Mason, J. H. Gault, J. Ross, Jr., R. Zelis, C. J. Mills, E. Braunwald,
Mechanism of Pulsus Paradoxus in Clinical Shock *
 The Journal of Clinical Investigatton Vol. 46, No. 11, 1967 Mechanism of Pulsus Paradoxus in Clinical Shock * JAY N. COHN,$ ALAN L. PINKERSON, AND FELIX E. TRISTANI (From the Medical Service, Veterans
The Journal of Clinical Investigatton Vol. 46, No. 11, 1967 Mechanism of Pulsus Paradoxus in Clinical Shock * JAY N. COHN,$ ALAN L. PINKERSON, AND FELIX E. TRISTANI (From the Medical Service, Veterans
Outline. Echocardiographic Assessment of Pericardial Effusion/Tamponade: The Essentials
 Echocardiographic Assessment of Pericardial Effusion/Tamponade: The Essentials John R Schairer DO FACC Henry Ford Heart and Vascular Institute No Disclosures Outline Normal Anatomy and Physiology Pathophysiology
Echocardiographic Assessment of Pericardial Effusion/Tamponade: The Essentials John R Schairer DO FACC Henry Ford Heart and Vascular Institute No Disclosures Outline Normal Anatomy and Physiology Pathophysiology
Flow patterns in cavae, pulmonary artery, pulmonary vein, and aorta in intact dogs
 Flow patterns in cavae, pulmonary artery, pulmonary vein, and aorta in intact dogs BEVERLY C. MORGAN, FRANCIS L. ABEL,2 GAY L. MULLINS, AND WARREN G. GUNTHEROTH Division of Pediatric Cardiology, University
Flow patterns in cavae, pulmonary artery, pulmonary vein, and aorta in intact dogs BEVERLY C. MORGAN, FRANCIS L. ABEL,2 GAY L. MULLINS, AND WARREN G. GUNTHEROTH Division of Pediatric Cardiology, University
Adel Hasanin Ahmed 1
 Adel Hasanin Ahmed 1 PERICARDIAL DISEASE The pericardial effusion ends anteriorly to the descending aorta and is best visualised in the PLAX. PSAX is actually very useful sometimes for looking at posterior
Adel Hasanin Ahmed 1 PERICARDIAL DISEASE The pericardial effusion ends anteriorly to the descending aorta and is best visualised in the PLAX. PSAX is actually very useful sometimes for looking at posterior
Technique. Technique. Technique. Monitoring 1. Local anesthetic? Aseptic technique Hyper-extend (if radial)
 Critical Care Monitoring Hemodynamic Monitoring Arterial Blood Pressure Cannulate artery Uses 2 Technique Sites Locate artery, prep 3 1 Technique Local anesthetic? Aseptic technique Hyper-extend (if radial)
Critical Care Monitoring Hemodynamic Monitoring Arterial Blood Pressure Cannulate artery Uses 2 Technique Sites Locate artery, prep 3 1 Technique Local anesthetic? Aseptic technique Hyper-extend (if radial)
Georgios C. Bompotis Cardiologist, Director of Cardiological Department, Papageorgiou Hospital,
 Georgios C. Bompotis Cardiologist, Director of Cardiological Department, Papageorgiou Hospital, Disclosure Statement of Financial Interest I, Georgios Bompotis DO NOT have a financial interest/arrangement
Georgios C. Bompotis Cardiologist, Director of Cardiological Department, Papageorgiou Hospital, Disclosure Statement of Financial Interest I, Georgios Bompotis DO NOT have a financial interest/arrangement
The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the Edwards PreSep oximetry catheter
 1 2 The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the Edwards PreSep oximetry catheter for continuous central venous oximetry (ScvO2) 3
1 2 The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the Edwards PreSep oximetry catheter for continuous central venous oximetry (ScvO2) 3
Citation Acta medica Nagasakiensia. 1984, 29
 NAOSITE: Nagasaki University's Ac Title Author(s) Efficacy of Coenzyme Q10 Administra Aortic Stenosis and Pacemaker Induc Igarashi, Katsuro Citation Acta medica Nagasakiensia. 1984, 29 Issue Date 1984-10-25
NAOSITE: Nagasaki University's Ac Title Author(s) Efficacy of Coenzyme Q10 Administra Aortic Stenosis and Pacemaker Induc Igarashi, Katsuro Citation Acta medica Nagasakiensia. 1984, 29 Issue Date 1984-10-25
The Cardiac Cycle Clive M. Baumgarten, Ph.D.
 The Cardiac Cycle Clive M. Baumgarten, Ph.D. OBJECTIVES: 1. Describe periods comprising cardiac cycle and events within each period 2. Describe the temporal relationships between pressure, blood flow,
The Cardiac Cycle Clive M. Baumgarten, Ph.D. OBJECTIVES: 1. Describe periods comprising cardiac cycle and events within each period 2. Describe the temporal relationships between pressure, blood flow,
by Starling [1914] and Daly [1925].
![by Starling [1914] and Daly [1925]. by Starling [1914] and Daly [1925].](/thumbs/83/88889966.jpg) 612.13 PROPERTIES OF THE PERIPHERAL VASCULAR SYSTEM AND THEIR RELATION TO THE SYSTEMIC OUTPUT. BY HENRY BARCROFT. Harmsworth Scholar, St Mary's Hospital, London. (Experiments performed in the Physiological
612.13 PROPERTIES OF THE PERIPHERAL VASCULAR SYSTEM AND THEIR RELATION TO THE SYSTEMIC OUTPUT. BY HENRY BARCROFT. Harmsworth Scholar, St Mary's Hospital, London. (Experiments performed in the Physiological
WHILE it is generally agreed that elevation
 The Derivation of Coronary Sinus Flow During Elevation of Right Ventricular Pressure By HERMAN M. GELLER, B.S., M.D., MARTIN BRANDFONBRENEU, M.D., AND CARL J. WIGGERS, M.D., The derivation of coronary
The Derivation of Coronary Sinus Flow During Elevation of Right Ventricular Pressure By HERMAN M. GELLER, B.S., M.D., MARTIN BRANDFONBRENEU, M.D., AND CARL J. WIGGERS, M.D., The derivation of coronary
Hemodynamic Monitoring
 Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
UNILATERAL ELEVATION OF THE INTERNAL JUGULAR PULSE
 BY PETER SLEIGHT From St. George's Hospital Received September 8, 1961 This paper describes a group of patients in whom the venous pressure, as shown by a distended and pulsating internal jugular vein,
BY PETER SLEIGHT From St. George's Hospital Received September 8, 1961 This paper describes a group of patients in whom the venous pressure, as shown by a distended and pulsating internal jugular vein,
Normal Pericardial Physiology
 Normal Pericardial Physiology Normal pericardium contains 20-30 ml of lymphoid fluid lubricating function that facilitates normal myocardial rotation and translation during each cardiac cycle in that the
Normal Pericardial Physiology Normal pericardium contains 20-30 ml of lymphoid fluid lubricating function that facilitates normal myocardial rotation and translation during each cardiac cycle in that the
Review Article. Interactive Physiology in Critical Illness : Pulmonary and Cardiovascular Systems. Introduction
 310 Indian Deepak J Physiol Shrivastava Pharmacol 2016; 60(4) : 310 314 Indian J Physiol Pharmacol 2016; 60(4) Review Article Interactive Physiology in Critical Illness : Pulmonary and Cardiovascular Systems
310 Indian Deepak J Physiol Shrivastava Pharmacol 2016; 60(4) : 310 314 Indian J Physiol Pharmacol 2016; 60(4) Review Article Interactive Physiology in Critical Illness : Pulmonary and Cardiovascular Systems
PERICARDIAL DIAESE. Kaijun Cui Associated professor Sichuan University
 PERICARDIAL DIAESE Kaijun Cui Associated professor Sichuan University CLASSIFICATION acute pericarditis pericardial effusion cardiac tamponade constrictive pericarditis congenitally absent pericardium
PERICARDIAL DIAESE Kaijun Cui Associated professor Sichuan University CLASSIFICATION acute pericarditis pericardial effusion cardiac tamponade constrictive pericarditis congenitally absent pericardium
-12. -Ensherah Mokheemer - ABDULLAH ZREQAT. -Faisal Mohammad. 1 P a g e
 -12 -Ensherah Mokheemer - ABDULLAH ZREQAT -Faisal Mohammad 1 P a g e In the previous lecture we talked about: - cardiac index: we use the cardiac index to compare the cardiac output between different individuals,
-12 -Ensherah Mokheemer - ABDULLAH ZREQAT -Faisal Mohammad 1 P a g e In the previous lecture we talked about: - cardiac index: we use the cardiac index to compare the cardiac output between different individuals,
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Physiology - 8 Hemodynamics - 1 M.jafar 24/3/2016 Turquoise Team
 21 Physiology - 8 Hemodynamics - 1 M.jafar 24/3/2016 Turquoise Team Hemodynamics Today we will take about hemodynamics which is the study of the movement of blood and of the forces concerned. Now how the
21 Physiology - 8 Hemodynamics - 1 M.jafar 24/3/2016 Turquoise Team Hemodynamics Today we will take about hemodynamics which is the study of the movement of blood and of the forces concerned. Now how the
PHYSIOLOGY MeQ'S (Morgan) All the following statements related to blood volume are correct except for: 5 A. Blood volume is about 5 litres. B.
 PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
BOTH ATEOPINE and isoproterenol
 Effects of tropine and Isoproterenol on Cardiac Output, Central Venous Pressure, and Transit Time of Indicators Placed at Three Different Sites in the Venous System y KLPH RTEX, M.D., J. CULIE GUNXELLS,
Effects of tropine and Isoproterenol on Cardiac Output, Central Venous Pressure, and Transit Time of Indicators Placed at Three Different Sites in the Venous System y KLPH RTEX, M.D., J. CULIE GUNXELLS,
CATCH A WAVE.. INTRODUCTION NONINVASIVE HEMODYNAMIC MONITORING 4/12/2018
 WAVES CATCH A WAVE.. W I S C O N S I N P A R A M E D I C S E M I N A R A P R I L 2 0 1 8 K E R I W Y D N E R K R A U S E R N, C C R N, E M T - P Have you considered that if you don't make waves, nobody
WAVES CATCH A WAVE.. W I S C O N S I N P A R A M E D I C S E M I N A R A P R I L 2 0 1 8 K E R I W Y D N E R K R A U S E R N, C C R N, E M T - P Have you considered that if you don't make waves, nobody
Large Arteries of Heart
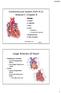 Cardiovascular System (Part A-2) Module 5 -Chapter 8 Overview Arteries Capillaries Veins Heart Anatomy Conduction System Blood pressure Fetal circulation Susie Turner, M.D. 1/5/13 Large Arteries of Heart
Cardiovascular System (Part A-2) Module 5 -Chapter 8 Overview Arteries Capillaries Veins Heart Anatomy Conduction System Blood pressure Fetal circulation Susie Turner, M.D. 1/5/13 Large Arteries of Heart
Cardiovascular system
 Cardiovascular system L-4 Blood pressure & special circulation Dr Than Kyaw 27 February 2012 Blood Pressure (BP) Pressure generation and flow Blood is under pressure within its closed system. Pressure
Cardiovascular system L-4 Blood pressure & special circulation Dr Than Kyaw 27 February 2012 Blood Pressure (BP) Pressure generation and flow Blood is under pressure within its closed system. Pressure
CVS Hemodynamics. Faisal I. Mohammed, MD,PhD.
 CVS Hemodynamics Faisal I. Mohammed, MD,PhD. Objectives point out the physical characteristics of the circulation: distribution of blood volume total cross sectional area velocity blood pressure List the
CVS Hemodynamics Faisal I. Mohammed, MD,PhD. Objectives point out the physical characteristics of the circulation: distribution of blood volume total cross sectional area velocity blood pressure List the
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
ANCE ON THE LEFT ATRIAL PRESSURE PULSE: A
 THE EFFECTS OF ACUTELY INCREASED SYSTEMIC RESIST- ANCE ON THE LEFT ATRIAL PRESSURE PULSE: A METHOD FOR THE CLINICAL DETECTION OF MITRAL INSUFFICIENCY By EUGENE BRAUNWALD, G. H. WELCH, JR., AND ANDREW G.
THE EFFECTS OF ACUTELY INCREASED SYSTEMIC RESIST- ANCE ON THE LEFT ATRIAL PRESSURE PULSE: A METHOD FOR THE CLINICAL DETECTION OF MITRAL INSUFFICIENCY By EUGENE BRAUNWALD, G. H. WELCH, JR., AND ANDREW G.
PROBLEM SET 2. Assigned: February 10, 2004 Due: February 19, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
PULMONARY CAPILLARY ARTERIAL PRESSURE PULSE IN MAN
 PULMONARY CAPILLARY ARTERIAL PRESSURE PULSE IN MAN BY W. WEISSEL, F. SALZMANN, AND H. VETTER From the II Medical University Clinic, Received June 11, 1951 Vienna In 1948, Hellems, Haynes, Dexter, and Kinney,
PULMONARY CAPILLARY ARTERIAL PRESSURE PULSE IN MAN BY W. WEISSEL, F. SALZMANN, AND H. VETTER From the II Medical University Clinic, Received June 11, 1951 Vienna In 1948, Hellems, Haynes, Dexter, and Kinney,
Biology Unit 3 The Human Heart P
 Biology 2201 Unit 3 The Human Heart P 314-321 Structure and Function of the Human Heart Structure of the Human Heart Has four Chambers (2 Atria and 2 Ventricles) Made of Cardiac Muscle Found in Chest Cavity
Biology 2201 Unit 3 The Human Heart P 314-321 Structure and Function of the Human Heart Structure of the Human Heart Has four Chambers (2 Atria and 2 Ventricles) Made of Cardiac Muscle Found in Chest Cavity
A Simplified Method for Calculation of the Left to-right Shunt from a Single Earpiece Dye-dilution Curve
 Tohoku J. exp. Med., 1969, 97, 337-346 A Simplified Method for Calculation of the Left to-right Shunt from a Single Earpiece Dye-dilution Curve Tetsuo Sato, Hiroshi Onoki, Norio Yamauchi and Ichiki Kano
Tohoku J. exp. Med., 1969, 97, 337-346 A Simplified Method for Calculation of the Left to-right Shunt from a Single Earpiece Dye-dilution Curve Tetsuo Sato, Hiroshi Onoki, Norio Yamauchi and Ichiki Kano
FOWLER AND COWORKERS have
 Effect of 1Arterenol Infusion on "Central Blood Volume" in the Dog By OSCAR W. SHADLB, M.D., JAMES C. MOORE, M.D. AND DOAL M. BILLIG, A.B. Infusion of 1arterenol into anesthetized dogs increased the volume
Effect of 1Arterenol Infusion on "Central Blood Volume" in the Dog By OSCAR W. SHADLB, M.D., JAMES C. MOORE, M.D. AND DOAL M. BILLIG, A.B. Infusion of 1arterenol into anesthetized dogs increased the volume
(From the Physiological Laboratory, Japanese Medioal School, Mukden.)
 THE MECHANICAL EFFECT OF FLUID IN THE PERI- CARDIUM ON THE FUNCTION OF THE HEART. BY YAS KUNO. (From the Physiological Laboratory, Japanese Medioal School, Mukden.) THE fact that a rise of pressure in
THE MECHANICAL EFFECT OF FLUID IN THE PERI- CARDIUM ON THE FUNCTION OF THE HEART. BY YAS KUNO. (From the Physiological Laboratory, Japanese Medioal School, Mukden.) THE fact that a rise of pressure in
End of chapter exercises
 End of chapter exercises Problem 1: The following diagrams show the heart during the cardiac cycle. The arrows represent the flow of blood. Study the diagrams and answer the questions that follow: Figure
End of chapter exercises Problem 1: The following diagrams show the heart during the cardiac cycle. The arrows represent the flow of blood. Study the diagrams and answer the questions that follow: Figure
Major Function of the Cardiovascular System. Transportation. Structures of the Cardiovascular System. Heart - muscular pump
 Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
Cardiovascular System
 Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
Heart Dissection. 5. Locate the tip of the heart or the apex. Only the left ventricle extends all the way to the apex.
 Heart Dissection Page 1 of 6 Background: The heart is a four-chambered, hollow organ composed primarily of cardiac muscle tissue. It is located in the center of the chest in between the lungs. It is the
Heart Dissection Page 1 of 6 Background: The heart is a four-chambered, hollow organ composed primarily of cardiac muscle tissue. It is located in the center of the chest in between the lungs. It is the
Medical NREMT-PTE. NREMT Paramedic Trauma Exam.
 Medical NREMT-PTE NREMT Paramedic Trauma Exam https://killexams.com/pass4sure/exam-detail/nremt-pte Question: 41 Which of the following most accurately describes the finding of jugular venous distension
Medical NREMT-PTE NREMT Paramedic Trauma Exam https://killexams.com/pass4sure/exam-detail/nremt-pte Question: 41 Which of the following most accurately describes the finding of jugular venous distension
The Cardiovascular System (Heart)
 The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
PART I: HEART ANATOMY
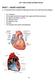 Lab 7: Heart Sounds and Blood Pressure PART I: HEART ANATOMY a) You should be able to identify the following structures on an adult human heart diagram. the 4 chambers the bicuspid (mitral) and tricuspid
Lab 7: Heart Sounds and Blood Pressure PART I: HEART ANATOMY a) You should be able to identify the following structures on an adult human heart diagram. the 4 chambers the bicuspid (mitral) and tricuspid
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Heart transplantation is the gold standard treatment for
 Organ Care System for Heart Procurement and Strategies to Reduce Primary Graft Failure After Heart Transplant Masaki Tsukashita, MD, PhD, and Yoshifumi Naka, MD, PhD Primary graft failure is a rare, but
Organ Care System for Heart Procurement and Strategies to Reduce Primary Graft Failure After Heart Transplant Masaki Tsukashita, MD, PhD, and Yoshifumi Naka, MD, PhD Primary graft failure is a rare, but
Performance Enhancement. Cardiovascular/Respiratory Systems and Athletic Performance
 Performance Enhancement Cardiovascular/Respiratory Systems and Athletic Performance Functions of the Cardiovascular System Deliver oxygen & nutrients to body tissues Carry wastes from the cells Anatomy
Performance Enhancement Cardiovascular/Respiratory Systems and Athletic Performance Functions of the Cardiovascular System Deliver oxygen & nutrients to body tissues Carry wastes from the cells Anatomy
The Cardiovascular System
 The Cardiovascular System The Manila Times College of Subic Prepared by: Stevens B. Badar, RN, MANc THE HEART Anatomy of the Heart Location and Size approx. the size of a person s fist, hollow and cone-shaped,
The Cardiovascular System The Manila Times College of Subic Prepared by: Stevens B. Badar, RN, MANc THE HEART Anatomy of the Heart Location and Size approx. the size of a person s fist, hollow and cone-shaped,
The Doppler Examination. Katie Twomley, MD Wake Forest Baptist Health - Lexington
 The Doppler Examination Katie Twomley, MD Wake Forest Baptist Health - Lexington OUTLINE Principles/Physics Use in valvular assessment Aortic stenosis (continuity equation) Aortic regurgitation (pressure
The Doppler Examination Katie Twomley, MD Wake Forest Baptist Health - Lexington OUTLINE Principles/Physics Use in valvular assessment Aortic stenosis (continuity equation) Aortic regurgitation (pressure
Pericardial Diseases. Smonporn Boonyaratavej, MD. Division of Cardiology, Department of Medicine Chulalongkorn University
 Pericardial Diseases Smonporn Boonyaratavej, MD Division of Cardiology, Department of Medicine Chulalongkorn University Cardiac Center, King Chulalongkorn Memorial Hospital 21 AUGUST 2016 Pericardial
Pericardial Diseases Smonporn Boonyaratavej, MD Division of Cardiology, Department of Medicine Chulalongkorn University Cardiac Center, King Chulalongkorn Memorial Hospital 21 AUGUST 2016 Pericardial
The Cardiovascular System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Slides 11.1 11.19 Seventh Edition Chapter 11 The Cardiovascular System Functions of the Cardiovascular system Function of the heart: to pump blood
Essentials of Human Anatomy & Physiology Elaine N. Marieb Slides 11.1 11.19 Seventh Edition Chapter 11 The Cardiovascular System Functions of the Cardiovascular system Function of the heart: to pump blood
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
PEEP, and Interrupted PEEP
 Comparative Hemodynamic Consequences of Inflation Hold, PEEP, and Interrupted PEEP An Experimental Study in Normal Dogs Kenneth F. MacDonnell, M.D., Armand A. Lefemine, M.D., Hyung S. Moon, M.D., Daniel
Comparative Hemodynamic Consequences of Inflation Hold, PEEP, and Interrupted PEEP An Experimental Study in Normal Dogs Kenneth F. MacDonnell, M.D., Armand A. Lefemine, M.D., Hyung S. Moon, M.D., Daniel
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Cath Lab Essentials: Pericardial effusion & tamponade
 Cath Lab Essentials: Pericardial effusion & tamponade Pranav M. Patel, MD, FACC, FSCAI Chief, Division of Cardiology Director, Cardiac Cath Lab & CCU University of California, Irvine Division of Cardiology
Cath Lab Essentials: Pericardial effusion & tamponade Pranav M. Patel, MD, FACC, FSCAI Chief, Division of Cardiology Director, Cardiac Cath Lab & CCU University of California, Irvine Division of Cardiology
CVS Hemodynamics. Change in blood pressure:
 CVS Hemodynamics -The distribution of blood inside the circulation: The major part of blood volume is found in the venous system 60% (2/3), that s why veins are called the capacitance vessels. -Arteries
CVS Hemodynamics -The distribution of blood inside the circulation: The major part of blood volume is found in the venous system 60% (2/3), that s why veins are called the capacitance vessels. -Arteries
Comparison of Flow Differences amoiig Venous Cannulas
 Comparison of Flow Differences amoiig Venous Cannulas Edward V. Bennett, Jr., MD., John G. Fewel, M.S., Jose Ybarra, B.S., Frederick L. Grover, M.D., and J. Kent Trinkle, M.D. ABSTRACT The efficiency of
Comparison of Flow Differences amoiig Venous Cannulas Edward V. Bennett, Jr., MD., John G. Fewel, M.S., Jose Ybarra, B.S., Frederick L. Grover, M.D., and J. Kent Trinkle, M.D. ABSTRACT The efficiency of
Point-of-Care Ultrasound Closer look at the Inferior Vena Cavae &
 Point-of-Care Ultrasound Closer look at the Inferior Vena Cavae & Brief Introduction to Gross Systolic Function Omar S. Darwish, MS, DO Certified in Point-of-Care Ultrasound Hospitalist University of California,
Point-of-Care Ultrasound Closer look at the Inferior Vena Cavae & Brief Introduction to Gross Systolic Function Omar S. Darwish, MS, DO Certified in Point-of-Care Ultrasound Hospitalist University of California,
The Mammalian Circulatory System
 The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
CIRCULATION & GAS EXCHANGE
 AP BIOLOGY ACTIVITY2.13 Text:Campbell,v.8,chapter42 NAME DATE HOUR CIRCULATION & GAS EXCHANGE 1. In general, what is the function of transport systems? 2. What method/structure do most invertebrates use
AP BIOLOGY ACTIVITY2.13 Text:Campbell,v.8,chapter42 NAME DATE HOUR CIRCULATION & GAS EXCHANGE 1. In general, what is the function of transport systems? 2. What method/structure do most invertebrates use
612.I73:6I2.I3. mammary and mediastinal vessels tied off. The thoracic wall on the left
 612.I73:6I2.I3 CARDIAC OUTPUT AND BLOOD DISTRIBUTION. By H. BAR CROFT (Harmsworth Scholar, St Mary's Hospital, London). (From the Physiological Laboratory, Cambridge.) THE methods for the measurement of
612.I73:6I2.I3 CARDIAC OUTPUT AND BLOOD DISTRIBUTION. By H. BAR CROFT (Harmsworth Scholar, St Mary's Hospital, London). (From the Physiological Laboratory, Cambridge.) THE methods for the measurement of
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies
 Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Hemodynamic effects of isoproterenol and norepinephrine in acute cardiac tamponade
 Hemodynamic effects of isoproterenol and norepinephrine in acute cardiac tamponade Noble O. Fowler, John C. Holmes J Clin Invest. 1969;48(3):502-507. https://doi.org/10.1172/jci106007. Research Article
Hemodynamic effects of isoproterenol and norepinephrine in acute cardiac tamponade Noble O. Fowler, John C. Holmes J Clin Invest. 1969;48(3):502-507. https://doi.org/10.1172/jci106007. Research Article
Portal vein catheterization and selective angiography in diagnosis of total anomalous pulmonary venous connexion
 British Heart journal, 974, 36, 155-59. Portal vein catheterization and selective angiography in diagnosis of total anomalous pulmonary venous connexion Michael Tynan, D. Behrendt, W. Urquhart, and G.
British Heart journal, 974, 36, 155-59. Portal vein catheterization and selective angiography in diagnosis of total anomalous pulmonary venous connexion Michael Tynan, D. Behrendt, W. Urquhart, and G.
This is not a required assignment but it is recommended.
 SU 12 Name: This is not a required assignment but it is recommended. BIO 116 - Anatomy & Physiology II Practice Assignment 2 - The Respiratory and Cardiovascular Systems 1. The exchange of oxygen and carbon
SU 12 Name: This is not a required assignment but it is recommended. BIO 116 - Anatomy & Physiology II Practice Assignment 2 - The Respiratory and Cardiovascular Systems 1. The exchange of oxygen and carbon
We are now going to review the diagnosis and management of pericardial collections and tamponade
 We are now going to review the diagnosis and management of pericardial collections and tamponade FEEL COURSE PAGE 1 Paying particular attention to the difference between a collection and cardiac tamponade
We are now going to review the diagnosis and management of pericardial collections and tamponade FEEL COURSE PAGE 1 Paying particular attention to the difference between a collection and cardiac tamponade
Smith, Miller and Grab er(4) state that the maintenance of an efficient
 THE SIGNIFICANCE OF THE DIASTOLIC AND SYSTOLIC BLOOD-PRESSURES FOR THE MAINTENANCE OF THE CORONARY CIRCULATION. BY G. V. ANREP AND B. KING. (From the Physiological Laboratory, Cambridge.) IT is generally
THE SIGNIFICANCE OF THE DIASTOLIC AND SYSTOLIC BLOOD-PRESSURES FOR THE MAINTENANCE OF THE CORONARY CIRCULATION. BY G. V. ANREP AND B. KING. (From the Physiological Laboratory, Cambridge.) IT is generally
Cardiovascular System. Heart Anatomy
 Cardiovascular System Heart Anatomy 1 The Heart Location & general description: Atria vs. ventricles Pulmonary vs. systemic circulation Coverings Walls The heart is found in the mediastinum, the medial
Cardiovascular System Heart Anatomy 1 The Heart Location & general description: Atria vs. ventricles Pulmonary vs. systemic circulation Coverings Walls The heart is found in the mediastinum, the medial
THE HEART. Unit 3: Transportation and Respiration
 THE HEART Unit 3: Transportation and Respiration The Circulatory System Also called the Cardiovascular System Circulates blood in the body Transports nutrients, oxygen, carbon dioxide, hormones, and blood
THE HEART Unit 3: Transportation and Respiration The Circulatory System Also called the Cardiovascular System Circulates blood in the body Transports nutrients, oxygen, carbon dioxide, hormones, and blood
CARDIOVASCULAR PHYSIOLOGY
 CARDIOVASCULAR PHYSIOLOGY LECTURE 4 Cardiac cycle Polygram - analysis of cardiac activity Ana-Maria Zagrean MD, PhD The Cardiac Cycle - definitions: the sequence of electrical and mechanical events that
CARDIOVASCULAR PHYSIOLOGY LECTURE 4 Cardiac cycle Polygram - analysis of cardiac activity Ana-Maria Zagrean MD, PhD The Cardiac Cycle - definitions: the sequence of electrical and mechanical events that
Prof. Dr. Iman Riad Mohamed Abdel Aal
 The Use of New Ultrasound Indices to Evaluate Volume Status and Fluid Responsiveness in Septic Shock Patients Thesis Submitted for partial fulfillment of MD degree in Anesthesiology, Surgical Intensive
The Use of New Ultrasound Indices to Evaluate Volume Status and Fluid Responsiveness in Septic Shock Patients Thesis Submitted for partial fulfillment of MD degree in Anesthesiology, Surgical Intensive
Level 2 Anatomy and Physiology Bite size revision. Respiratory System. The order of the passage of oxygen into the body (inhalation/inspiration) is: -
 Respiratory System Function of the respiratory system The lungs are located in the chest cavity and their function is to intake oxygen and remove carbon dioxide from the body. Structure of the respiratory
Respiratory System Function of the respiratory system The lungs are located in the chest cavity and their function is to intake oxygen and remove carbon dioxide from the body. Structure of the respiratory
PIAF study: Placental insufficiency and aortic isthmus flow Jean-Claude Fouron, MD
 Dear colleagues, I would like to thank you very sincerely for agreeing to participate in our multicentre study on the clinical significance of recording fetal aortic isthmus flow during placental circulatory
Dear colleagues, I would like to thank you very sincerely for agreeing to participate in our multicentre study on the clinical significance of recording fetal aortic isthmus flow during placental circulatory
Heart. Structure Physiology of blood pressure and heartbeat
 Heart Structure Physiology of blood pressure and heartbeat Location and Anatomy Location and Anatomy Pericardial cavity: surrounds, isolates, and anchors heart Parietal pericardium lined with serous membrane
Heart Structure Physiology of blood pressure and heartbeat Location and Anatomy Location and Anatomy Pericardial cavity: surrounds, isolates, and anchors heart Parietal pericardium lined with serous membrane
HISTORY. Question: What category of heart disease is suggested by this history? CHIEF COMPLAINT: Heart murmur present since early infancy.
 HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
Cardiac Cycle MCQ. Professor of Cardiovascular Physiology. Cairo University 2007
 Cardiac Cycle MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Regarding the length of systole and diastole: a- At heart rate 75 b/min, the duration of
Cardiac Cycle MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Regarding the length of systole and diastole: a- At heart rate 75 b/min, the duration of
Chapter 9, Part 2. Cardiocirculatory Adjustments to Exercise
 Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Cath Lab Essentials: Basic Hemodynamics for the Cath Lab and ICU
 Cath Lab Essentials: Basic Hemodynamics for the Cath Lab and ICU Ailin Barseghian El-Farra, MD, FACC Assistant Professor, Interventional Cardiology University of California, Irvine Department of Cardiology
Cath Lab Essentials: Basic Hemodynamics for the Cath Lab and ICU Ailin Barseghian El-Farra, MD, FACC Assistant Professor, Interventional Cardiology University of California, Irvine Department of Cardiology
CARDIAC CATHETERIZATION IN DOGS
 CARDIAC CATHETERIZATION IN DOGS WILLIAM H. NOBLE, B.A., IVLD., DIP.ANAES., F.R.C.P.(C) AND J. COLIN KAY, A.I.IX~.L.T. (ENG.) INTRODUCTION MANY INVESTIGATORS require cardiac catheterization data as a part
CARDIAC CATHETERIZATION IN DOGS WILLIAM H. NOBLE, B.A., IVLD., DIP.ANAES., F.R.C.P.(C) AND J. COLIN KAY, A.I.IX~.L.T. (ENG.) INTRODUCTION MANY INVESTIGATORS require cardiac catheterization data as a part
CARDIAC OUTPUT,VENOUS RETURN AND THEIR REGULATION. DR.HAROON RASHID. OBJECTIVES
 CARDIAC OUTPUT,VENOUS RETURN AND THEIR REGULATION. DR.HAROON RASHID. OBJECTIVES Define Stroke volume, Cardiac output Venous return,& identity their normal values. Describe control (intrinsic & extrinsic)
CARDIAC OUTPUT,VENOUS RETURN AND THEIR REGULATION. DR.HAROON RASHID. OBJECTIVES Define Stroke volume, Cardiac output Venous return,& identity their normal values. Describe control (intrinsic & extrinsic)
The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to:
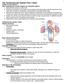 The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Describe the functions of the heart 2. Describe the location of the heart,
The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Describe the functions of the heart 2. Describe the location of the heart,
Effect of Atrial and Ventricular Tachycardia on Cardiac Oxygen Consumption
 Effect of Atrial and Ventricular Tachycardia on Cardiac Oxygen Consumption fly Henry S. Badeer, M.D., and Kholil A. Feisol, M.D. Clinical experience has shown that ventricular is a more serious arrhythmia
Effect of Atrial and Ventricular Tachycardia on Cardiac Oxygen Consumption fly Henry S. Badeer, M.D., and Kholil A. Feisol, M.D. Clinical experience has shown that ventricular is a more serious arrhythmia
Simultaneous Pressure, Flow and Diameter of the Vena Cava with Fright and Exercise
 Simultaneous Pressure, Flow and Diameter of the Vena Cava with Fright and Exercise By Emilio Tafur, M.D., and Warren G. Guntheroth, M.D. With the technical assistance of Donald G. Breozea/e and George
Simultaneous Pressure, Flow and Diameter of the Vena Cava with Fright and Exercise By Emilio Tafur, M.D., and Warren G. Guntheroth, M.D. With the technical assistance of Donald G. Breozea/e and George
2. Langendorff Heart
 2. Langendorff Heart 2.1. Principle Langendorff heart is one type of isolated perfused heart which is widely used for biochemical, physiological, morphological and pharmacological researches. It provides
2. Langendorff Heart 2.1. Principle Langendorff heart is one type of isolated perfused heart which is widely used for biochemical, physiological, morphological and pharmacological researches. It provides
Definition- study of blood flow Haemodynamic monitoring refers to monitoring of blood in the cardiovascular system Uses Is NB in the critically ill
 By Craig Definition- study of blood flow Haemodynamic monitoring refers to monitoring of blood in the cardiovascular system Uses Is NB in the critically ill pt Can assist diagnosis and decision making
By Craig Definition- study of blood flow Haemodynamic monitoring refers to monitoring of blood in the cardiovascular system Uses Is NB in the critically ill pt Can assist diagnosis and decision making
echocardiographic study
 LABORATORY INVESTIGATION ECHOCARDIOGRAPHY The relative merits of pulsus paradoxus and right ventricular diastolic collapse in the early detection of cardiac tamponade: an experimental echocardiographic
LABORATORY INVESTIGATION ECHOCARDIOGRAPHY The relative merits of pulsus paradoxus and right ventricular diastolic collapse in the early detection of cardiac tamponade: an experimental echocardiographic
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
Cardiovascular Structure & Function
 Cardiovascular Structure & Function Cardiovascular system: The heart Arteries Veins Capillaries Lymphatic vessels Weighting of the heart ceremony: Ancient Egyptians William Harvey and Blood Flow April
Cardiovascular Structure & Function Cardiovascular system: The heart Arteries Veins Capillaries Lymphatic vessels Weighting of the heart ceremony: Ancient Egyptians William Harvey and Blood Flow April
The Role of the Right Heart in Acute Cardiac Tamponade in Dogs
 The Role of the Right Heart in Acute Cardiac Tamponade in Dogs 71 ROY DITCHEY, ROBERT ENGLER, MARTIN LEWINTER, RICHARD PAVELEC, VALMIK BHARGAVA, JAMES COVELL, WILLIAM MOORES, AND RALPH SHABETAI SUMMARY
The Role of the Right Heart in Acute Cardiac Tamponade in Dogs 71 ROY DITCHEY, ROBERT ENGLER, MARTIN LEWINTER, RICHARD PAVELEC, VALMIK BHARGAVA, JAMES COVELL, WILLIAM MOORES, AND RALPH SHABETAI SUMMARY
Cardiac output and Venous Return. Faisal I. Mohammed, MD, PhD
 Cardiac output and Venous Return Faisal I. Mohammed, MD, PhD 1 Objectives Define cardiac output and venous return Describe the methods of measurement of CO Outline the factors that regulate cardiac output
Cardiac output and Venous Return Faisal I. Mohammed, MD, PhD 1 Objectives Define cardiac output and venous return Describe the methods of measurement of CO Outline the factors that regulate cardiac output
JACC Vol. 18, No. I July 1991 :243-52
 JACC Vol. 18, No. I July 1991 :243-52 243 Experimental Cardiac Tamponade: A Hemodynamic and Doppler Echocardiographic Reexamination of the Rlation of Right and Left Heart Ejection Dynamics to the Phase
JACC Vol. 18, No. I July 1991 :243-52 243 Experimental Cardiac Tamponade: A Hemodynamic and Doppler Echocardiographic Reexamination of the Rlation of Right and Left Heart Ejection Dynamics to the Phase
Identify and describe the circulation system that is missing from the organizer above.
 Lesson 15.1 NOTES: The Circulatory System (Unlock) Essential Question: -What are the structures and functions of the circulatory system? Learning Target(s): -I can identify structures and explain functions
Lesson 15.1 NOTES: The Circulatory System (Unlock) Essential Question: -What are the structures and functions of the circulatory system? Learning Target(s): -I can identify structures and explain functions
Distribution and Responses of the Cardiac Sympathetic Receptors to Mechanically Induced Circulatory Changes
 Distribution and Responses of the Cardiac Sympathetic Receptors to Mechanically Induced Circulatory Changes Hideo UEDA, M.D., Yasumi UCHIDA, M.D., and Kazuaki KAMISAKA, M.D. SUMMARY Distribution and mode
Distribution and Responses of the Cardiac Sympathetic Receptors to Mechanically Induced Circulatory Changes Hideo UEDA, M.D., Yasumi UCHIDA, M.D., and Kazuaki KAMISAKA, M.D. SUMMARY Distribution and mode
Chapter 20 (1) The Heart
 Chapter 20 (1) The Heart Learning Objectives Describe the location and structure of the heart Describe the path of a drop of blood from the superior vena cava or inferior vena cava through the heart out
Chapter 20 (1) The Heart Learning Objectives Describe the location and structure of the heart Describe the path of a drop of blood from the superior vena cava or inferior vena cava through the heart out
THE HEART. A. The Pericardium - a double sac of serous membrane surrounding the heart
 THE HEART I. Size and Location: A. Fist-size weighing less than a pound (250 to 350 grams). B. Located in the mediastinum between the 2 nd rib and the 5 th intercostal space. 1. Tipped to the left, resting
THE HEART I. Size and Location: A. Fist-size weighing less than a pound (250 to 350 grams). B. Located in the mediastinum between the 2 nd rib and the 5 th intercostal space. 1. Tipped to the left, resting
Index of subjects. effect on ventricular tachycardia 30 treatment with 101, 116 boosterpump 80 Brockenbrough phenomenon 55, 125
 145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
The Heart. Made up of 3 different tissue: cardiac muscle tissue, nerve tissue, and connective tissue.
 The Heart The Heart Made up of 3 different tissue: cardiac muscle tissue, nerve tissue, and connective tissue. Your heart pumps with a regular beat (Heart Rate) Your heart rate can change depending on
The Heart The Heart Made up of 3 different tissue: cardiac muscle tissue, nerve tissue, and connective tissue. Your heart pumps with a regular beat (Heart Rate) Your heart rate can change depending on
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
Packet #6 Cells: Internal Environment, part 2 (organ systems) Summer This Activity Packet belongs to:
 Packet #6 Cells: Internal Environment, part 2 (organ systems) Summer 2014 This Activity Packet belongs to: You should expect a variety of quizzes: announced, unannounced, open-notes and closed-notes. Packet
Packet #6 Cells: Internal Environment, part 2 (organ systems) Summer 2014 This Activity Packet belongs to: You should expect a variety of quizzes: announced, unannounced, open-notes and closed-notes. Packet
Heart and Lung Dissection
 Heart and Lung Dissection Name(s) Before you begin any work or dissection of your specimen, please try to identify the following. You will need to illustrate what you see, so make sure to note size, texture
Heart and Lung Dissection Name(s) Before you begin any work or dissection of your specimen, please try to identify the following. You will need to illustrate what you see, so make sure to note size, texture
Impedance Cardiography (ICG) Method, Technology and Validity
 Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
