Management of Victims with Submersion Injury
|
|
|
- Hope Douglas
- 5 years ago
- Views:
Transcription
1 S89 Submersion Injury Management of Victims with Submersion Injury Tzong-Luen Wang, MD, PhD Abstract Submersion injury remains high mortality and morbidity in little babies and adolescents. Because most of these events are due to accidents, preventive measures are the first priority to be considered. Hypoxemia and subsequent multi-organ insults, especially for the brain, are devastating sequelae. Aggressive pulmonary support are thus encouraged and required. There is still no definite prognostic scale that accurately predicts the patients outcome. However, those presenting with clear consciousness at arrival are almost 100% survived. Traditional HYPER therapy (hypothermia, hyperventilation, steroids, dehydration, barbiturate coma, and neuromuscular blockade) has been proven not to improve the prognosis.(ann Disaster Med. 2004;2 Suppl 2:S89-S96) Key words: Submersion; Drowning; Near-Drowning; Environmental Medicine Introduction Submersion injury consists of drowning and near-drowning. 1-8 Drowning is defined as death secondary to asphyxia while immersed in a liquid, usually water, or within 24 hours of submersion, whereas near-drowning means those who eventually survive from the submersion or immersion. 1-8 Because of complicated medical conditions, near drowning suggests an immersion episode severe enough to warrant medical attention to avoid morbidity and mortality. 1-8 Epidemiological studies revealed that there are more than one thousand and fifty thousands reported deaths from drowning worldwide, but some of the densely populated countries did not have the data of near drowning incidents. 7, 8 The prevalence or incidence of submersion injury and drowning deaths can thus not be measured accurately. However, the limited data showed that there is a bimodal age distribution of drowning deaths, with an initial peak in the toddler age group and a second peak in adolescent to young adult males. 7,8 In pediatric populations, trauma remains the leading mortality and drowning also always presents as the big three. 9 Accordingly, morbidity from submersion occurs in 12-27% of survivors in this age group. 9 In America, preschool-aged boys are at greatest risk of submersion injury. Approximately 10% of children younger than 5 years had an experience judged a serious threat of near drowning. 9 Swimming pools at home are the most common submersion site in this age group. Epidemiological studies revealed that male-to-female ratios are ap- From Department of Emergency Medicine, Shin-Kong Wu Ho-Su Memorial Hospital, Taipei, Taiwan Address for reprints:dr. Tzong-Luen Wang, Department of Emergency Medicine, Shin Kong Wu Ho-Su Memorial Hospital, No 95, Wen Chang Road, Taipei, Taiwan Received: Feb Revised: Feb Accepted: Mar TEL: FAX: M002183@ms.skh.org.tw
2 Submersion Injury S90 proximately 12:1 for boat-related drowning and 5:1 for non-boat-related drowning, whereas the girls predominate only in bathing incidents. 10,11 The peak age groups are children younger than 4 years and adolescents/young people between 15 and 24 years. 1-9 Mortality is primarily due to laryngospasm and lung injury, resulting hypoxemia, and its subsequent neurological and/or other systemic damages. 8 Morbidity is always due to neurological insult and multiple organ system failure. Thirty-five percent of immersion episodes in children are fatal; one third results in some degree of neurological impairment, one tenth in severe neurological complications. 9,12 In addition, a high risk of death exists secondary to the development of adult respiratory distress syndrome (ARDS) or socalled postimmersion syndrome. 1-8 The devastating events mentioned above and the fact that these incidents always involve a toddler left unattended, an adolescent found floating in the water, or a victim diving and not resurfacing demonstrated that prevention is the most important measure Community education is the key to prevention. Every one should know his own swimming abilities and never do anything above the limitations. 13 Parents should always supervise children carefully around water. Children should be taught safe conduct around water and during water sports. Use of alcohol or other recreational drugs is contraindicated when swimming or doing water sports. Appropriate boating equipment should be used, and sufficient barriers must be used around any water-containing devices at home. Every one should seriously considers learning CPR and water safety training to provide immediate and necessary rescue and resuscitation if needed. Pathophysiology of Submersion Injury Hypoxemia is the major pathologic consequence of subimmersion injury. Airway management and good ventilation are still the first priority for those victims. That is why the ACLS algorithm assumes that one should resuscitate firstly instead of call for help, as he should do for the victims of those less than 8 years old, those with trauma or intoxication. After initial gasping, and possible aspiration, immersion stimulates hyperventilation, followed by voluntary apnea and a variable degree and duration of laryngospasm. Hypoxemia has begun since then. Furthermore, the persistent hypoxemia and subsequent acidosis, also make the patient prone to cardiac arrest and central nervous system damage. The victims in submersion are traditionally considered to have dry lungs because of the initial laryngospasm. However, there are more and more data revealing that asphyxia may lead to smooth muscle relaxation of the airway and then permits the lungs to fill with water in significant portion of the victims. There may be only 10-20% of the patients keep laryngospasm until cardiac arrest and do not aspirate any fluid. In other words, most of the patients have wet lungs may develop pulmonary edema, and a small part of them dry lungs. Past physiological studies also demonstrated that sudden immersion in cold water may induce diving reflex which is manifested as apnea, bradycardia, and peripheral vasoconstriction with resultant shunting of blood to the vital organs such as the heart and the brain. The lung is the first target organ that submersion injury attacks. Most of the damages to
3 S91 Submersion Injury other organs are largely secondary to hypoxemia, ischemia and tissue acidosis. Aspiration of water into the lungs produces vagotonia, pulmonary vasoconstriction and hypertension. For those with fresh water aspiration, water moves rapidly across the alveolar-capillary membrane and destroys the surfactant to result in alveolar instability, atelectasis, decreased compliance and ventilation/perfusion mismatching that may be as high as 75%. In contrast, salt water can cause surfactant washout, produce protein-rich fluid exudates in the alveoli and pulmonary interstitium and alveolar-capillary basement membrane damage to result in stiff lung and shunting. All of the above phenomena contribute to severe hypoxia and possibly cerebral insult. Besides, fresh water and hypoxemia may cause lysis of red blood cells and subsequent hyperkalemia. Salt water may decrease blood volume and increase serum electrolyte concentrations. However, most of the victims do not aspirate enough fluid to cause substantial changes of blood volume and serum electrolyte concentrations. Clinical Aspects The victims of submersion injury should be always treated as those with trauma. For example, cervical spine injuries and head trauma, which result from diving into shallow water, surfing, water skiing, jet skiing or other hazards, may occur. Concomitant secondary trauma should be evaluated and managed according to the guidelines of Advanced Trauma Life Support (ATLS) or other related principles. In addition, most of the victims may be hypothermic that deserves special clinical alert and management such as rewarming. Some histories may be of beneficial in managing the patients with submersion injury. They include special environment such as cold water or hot water, past history of systemic diseases such as pulmonary, heart or seizure disorders, conscious level at presentation and during transportation, presence of vomiting, concomitant drug or alcohol use. A classification of the victims of submersion incidents attributes them into asymptomatic, symptomatic, cardiopulmonary arrest and death. Symptomatic patients may present with altered vital signs, arrhythmia, hypothermia, tachypnea, dyspnea, hypoxia, conscious change, and metabolic acidosis. More than half of the victims with cardiopulmonary arrest present with asystole, thirty percent ventricular tachycardia or fibrillation, and less than 20% bradycardia. Immersion syndrome and apnea are usually the manifestations of cardiopulmonary arrest due to submersion. However, normotheric victims with asystole, apnea, rigor mortis and dependent lividity always suggest definite death refractory to resuscitation. Some special considerations should be taken. Bathtub and pail drownings may represent child abuse. Examine the child carefully for other evidence of injury and review the details of the incident very carefully with the child s parent or guardian. Alcohol and, to a lesser extent, other recreational drugs are implicated in many cases. It is most important in older adolescents and adults who drowned in boating incidents, as determined by blood alcohol concentrations. In addition, always consider the underlying disease/illness in all age groups. They include seizure disorder, myocardial infarction or syncopal episode, malignant arrhythmia, poor neuromuscular control (such as significant
4 Submersion Injury S92 arthritis, Parkinson, or other neurological disorders), major depression/suicide, diabetes and hypoglycemia. Laboratory examination consists of arterial blood gas (ABG), complete blood cell counting, electrolytes, biochemistry, coagulation profile, and urine analysis. Arterial blood gas (ABG) analysis is probably the most reliable clinical parameter in patients who are asymptomatic or mildly symptomatic. Serial estimations of serum creatinine should be performed when there are elevated serum creatinine, marked metabolic acidosis, abnormal urinalysis, or significant lymphocytosis initially. Acute renal impairment is frequent in near drowning, ranging from mild to severe renal failure requiring dialysis. Consider a blood alcohol level and urine toxicology screen for abuse of drugs in specific situations mentioned above. First Aids and Management Prehospital care. Maintenance of the ABC is still the first priority, with particular focus on securing the airway and providing adequate oxygenation and ventilation, especially for those with altered mental status. Immediately place the patient on 100% oxygen by mask. If the patient remains dyspneic or low oxygen saturation, continuous positive airway pressure (CPAP) or consider endotracheal intubation with appropriate use of positive end-expiratory pressure (PEEP) should be indicated although there is still no such equipment in most of the ambulances in Taiwan. Cervical immobilization during resuscitation and transportation should be performed. Begin rewarming as soon as possible if hypothermia occurs. Emergency department care. Provide all victims of a submersion injury with supplemental oxygen during their evaluations. Evaluate early associated injuries such as cervical spine injury that may complicate airway management. Intubation may be required for a patient unable to maintain a po 2 of greater than mm Hg in adults or >80 mm Hg in kids with 100% oxygen by face masks. A trial of bilevel positive airway pressure (BiPAP)/CPAP can be considered to provide adequate oxygenation before intubation is performed for the alert and cooperative patients. Altered level of consciousness, inability to protect airway, high alveolar-arterial (A-a) gradient, PaO 2 of mm Hg or less on 15 L oxygen nonrebreathing mask, PaCO 2 >45 mm Hg, and worsening ABG results also indicate intubation. For these victims, PEEP has been shown to improve ventilation in the noncompliant lung. Prevention of expiratory airway collapse, shifting out interstitial pulmonary water, increasing alveolar ventilation, decreasing capillary blood flow, and bronchodilatation to improve distribution of ventilation may be the possible mechanisms. Patients with core temperatures less than 32 C after sudden and rapid immersion may display slowing of metabolism and preferential shunting of blood to the heart, brain, and lungs. However, most of the immersion victims become hypothermic gradually at a risk for ventricular fibrillation and brain insult, and need aggressive rewarming. Diving reflex that has been postulated to be reflex inhibition of the respiratory center (apnea), bradycardia, and vasoconstriction of nonessential capillary beds triggered by the sensory stimulus of the face by cold water may have protective effects after prolonged immersion in cold water. These re-
5 S93 Submersion Injury sponses preserve the circulation to the vital organs and conserve oxygen to increase survival. Sudden drop of temperature inhibits cellular metabolism significantly and thus limits the harm of hypoxia and metabolic acidosis. Place a nasogastric tube to assist in rewarming efforts and urinary catheter to assess urine output. Core rewarming with warmed oxygen, continuous bladder lavage with fluid at 40 C, and intravenous (IV) infusion of isotonic fluids at 40 C should be initiated during resuscitation. Warm peritoneal lavage may be required for core rewarming in severely hypothermic patients. Warm inspired air is also needed. Thoracotomy with open heart massage and warm mediastinal lavage may be indicated. A hypothermic heart is refractory to pharmacological and electrical therapies. More aggressive rewarming such as extracorporeal bypass may be used in severely hypothermic patients failing the above treatment. Central venous access should be attempted very cautiously because of possible stimuli for the hypothermic atrium with resultant dysrhythmias. A submersion victim cannot be declared death until he has been warmed to a minimum of 30 C. Initiate appropriate treatment of electrolyte imbalances, seizures, bronchospasm, and cold-induced bronchorrhea, dysrhythmias, and hypotension as needed. Disposition decision depends on the history, presence of associated injuries, and degree of immersion injury. Patients able to relay a good history of minor immersion injury, without evidence of significant injury and without evidence of bronchospasm, respiratory distress, or inadequate oxygenation can be discharged from the ED after 6-8 hours of observation. Victims of mild to moderately severe submersion, who only have mild symptoms that improve during observation and have no abnormalities on blood gas or chest radiograph, can be also discharged after 6-8 hours of observation in the ED. Observe victims of severe submersion with only mild symptoms and normal laboratory findings for a more prolonged period. Admit the patients with mild to moderately severe hypoxemia. Some of them improve easily with oxygen and can be discharged after resolution of hypoxemia with no complications. Patients requiring intubation and mechanical ventilation should be admitted to the intensive care units. Admission care. The victims may suffer from varying degrees of neurologic as well as pulmonary insults. In patients with significant lung disease but a reasonable likelihood of neurologic recovery, extracorporeal membrane oxygenation has been employed successfully to treat pulmonary insufficiency. Look for evidence of acute respiratory distress syndrome (ARDS); multiple organ system failure; nosocomial infection, especially pneumonia; and/or gastric stress ulceration. Management of ARDS due to submersion is similar to that of ARDS from other causes. Use of permissive hypercapnia to decrease barotrauma in many ARDS patients may not be appropriate in this setting of hypoxic ischemic CNS injury. The extent of invasive monitoring needed (eg, arterial catheter, pulmonary artery catheter, and/or central venous pressure catheter) is determined by the degree of hemodynamic or respiratory instability and the presence of renal failure. Prognosis Survival depends upon multiple factors. The submersion time, water temperature, water
6 Submersion Injury S94 tonicity, symptoms, associated injuries (especially cervical spine and head), type of rescue, and response to initial resuscitation are all relevant factors. Patients who are alert or mildly obtunded at presentation have an excellent chance for full recovery. Patients who are comatose, receiving CPR at presentation to the ED, or have fixed and dilated pupils and no spontaneous respirations have a poor prognosis. The classic protocol for cerebral resuscitation, which included neuromuscular blockade, barbiturate coma, dehydration, hyperventilation, hypothermia, and corticosteroids (HYPER therapy) does not improve outcome. Summary Submersion injury remains high mortality and morbidity in little babies and adolescents and prevention is the best policy to reduce the incidence. Hypoxemia and subsequent multiorgan insults are devastating. Pulmonary support is the most important treatment. Concomitant trauma should also be in detail evaluated and treated. Those presenting with clear consciousness at arrival are almost 100% survived. HYPER therapy has been abandoned. References 1. Newman AB, Stewart RD. Submersion incidents. In: Wilderness Medicine: Management of Wilderness and Environmental Emergencies. Chicago: Mosby; 1995: Asher KN, Rivara FP, Felix D, et al. Water safety training as a potential means of reducing risk of young children s drowning. Inj Prev 1995;1: Olshaker JS. Near drowning. Emerg Med Clin North Am 1992;10: Bross MH, Clark JL. Near-drowning. Am Fam Physician 1995;51: Sachdeva RC. Near drowning. Critical Care Clinics 1999;15: Fiser DH. Near-drowning. Pediatr Rev 1993;14: Weinstein MD, Krieger BP. Neardrowning: epidemiology, pathophysiology, and initial treatment. J Emerg Med 1996; 14: Szpilman D. Near-drowning and drowning classification: a proposal to stratify mortality based on the analysis of 1,831 cases. Chest 1997;112: Fields AI. Near-drowning in the pediatric population. Crit Care Clin 1992; 8: Chochinov A. Alcohol on board, man overboard boating fatalities in Canada. CMAJ 1998;159: Howland J, Smith GS, Mangione T, et al. Missing the boat on drinking and boating. JAMA 1993;270: Norberg WJ, Agnew RF, Brunsvold R, et al. Successful resuscitation of a cold water submersion victim with the use of cardiopulmonary bypass. Crit Care Med 1992;20: Thompson DC, Rivara FP. Pool fencing for preventing drowning in children. Cochrane Database Syst Rev 2000;2:CD Dunagan DP, Cox JE, Chang MC, Haponik EF. Sand aspiration with neardrowning. Radiographic and bronchoscopic findings. Am J Respir Crit Care Med 1997;156: Ender PT, Dolan MJ. Pneumonia associated with near-drowning. Clinical Infectious Diseases 1997;25:
7 S95 Submersion Injury 16. Bolte RG, Black PG, Bowers RS, et al. The use of extracorporeal rewarming in a child submerged for 66 minutes. JAMA 1988;260: Causey AL, Tilelli JA, Swanson ME. Predicting discharge in uncomplicated neardrowning. Resuscitation 2000;46: Spicer ST, Quinn D, NyiNyi NN, et al. Acute renal impairment after immersion and near-drowning. Journal of the American Society of Nephrology 1999;10: Christensen DW, Jansen P, Perkin RM. Outcome and acute care hospital costs after warm water near drowning in children. Pediatrics 1997;99: Graf WD, Cummings P, Quan L, Brutocao D. Predicting outcome in pediatric submersion victims. Ann Emerg Med 1995;26: Kyriacou DN, Arcinue EL, Peek C, Kraus JF. Effect of immediate resuscitation on children with submersion injury. Pediatrics; 94(2 Pt 1): Levin DL, Morriss FC, Toro LO, et al. Drowning and near-drowning. Pediatr Clin North Am 1993;40: Shatz DV, Kirton OC, McKenney MG, et al. Personal watercraft crash injuries: an emerging problem. J Trauma 1998;44: Peake PW. Emergency management of near drowning. Aust Fam Physician 1992;21:42-6
8 Submersion Injury S96 (Ann Disaster Med. 2004;2 Suppl 2:S89-S96) HYPER ( ) 95 (02) (02) M002183@ms.skh.org.tw
Drowning is a leading cause of death and loss of years of life with over 90% of cases occurring in lower- and middle-income countries.
 Chapter 145 Drowning Episode Overview: 1) List risk factors for drowning 2) List 5 variables that portend poor outcome 3) Describe the diving reflex 4) Describe the management of a drowning patient with
Chapter 145 Drowning Episode Overview: 1) List risk factors for drowning 2) List 5 variables that portend poor outcome 3) Describe the diving reflex 4) Describe the management of a drowning patient with
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
The Dangers of Summertime Important information to keep you and your patients safe. Stephanie Malchak, AEMT-P
 The Dangers of Summertime Important information to keep you and your patients safe. Stephanie Malchak, AEMT-P It s time for outdoor activities! For many, summer means fun in the sun. Kids are out of school.
The Dangers of Summertime Important information to keep you and your patients safe. Stephanie Malchak, AEMT-P It s time for outdoor activities! For many, summer means fun in the sun. Kids are out of school.
Disclaimer: All photos and/or videos included in the following presentation are permitted by subjects or are not subject to privacy laws due to lack
 Disclaimer: All photos and/or videos included in the following presentation are permitted by subjects or are not subject to privacy laws due to lack of patient information or identifying factors. Pediatric
Disclaimer: All photos and/or videos included in the following presentation are permitted by subjects or are not subject to privacy laws due to lack of patient information or identifying factors. Pediatric
Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor
 Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Resuscitation in Special Situations what s new
 Resuscitation in Special Situations what s new Asc. Prof. Dr. Serkan Şener Acıbadem University, School of Medicine Department of Emergency Medicine Acıbadem Ankara Hospital Objectives To understand the
Resuscitation in Special Situations what s new Asc. Prof. Dr. Serkan Şener Acıbadem University, School of Medicine Department of Emergency Medicine Acıbadem Ankara Hospital Objectives To understand the
Lecture Notes. Chapter 2: Introduction to Respiratory Failure
 Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
Acute Respiratory Distress Syndrome (ARDS) An Update
 Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Accidental Hypothermia
 Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
ARDS: an update 6 th March A. Hakeem Al Hashim, MD, FRCP SQUH
 ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
Prehospital Care Bundles
 Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
Hyaline membrane disease. By : Dr. Ch Sarishma Peadiatric Pg
 Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Cold Water Shock, Hypothermia and Cardiac Arrest
 Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Respiratory Failure. Causes of Acute Respiratory Failure (ARF): a- Intrapulmonary:
 Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
7/4/2015. diffuse lung injury resulting in noncardiogenic pulmonary edema due to increase in capillary permeability
 Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
11/27/2017. Stroke Management in the Neurocritical Care Unit. Conflict of interest. Karel Fuentes MD Medical Director of Neurocritical Care
 Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Conflict of interest None Introduction Reperfusion therapy remains the mainstay in the treatment
Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Conflict of interest None Introduction Reperfusion therapy remains the mainstay in the treatment
ACUTE RESPIRATORY DISTRESS SYNDROME
 ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
Outcomes From Severe ARDS Managed Without ECMO. Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016
 Outcomes From Severe ARDS Managed Without ECMO Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016 Severe ARDS Berlin Definition 2012 P:F ratio 100 mm Hg Prevalence:
Outcomes From Severe ARDS Managed Without ECMO Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016 Severe ARDS Berlin Definition 2012 P:F ratio 100 mm Hg Prevalence:
Head injuries. Severity of head injuries
 Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
UNIT VI: ACID BASE IMBALANCE
 UNIT VI: ACID BASE IMBALANCE 1 Objectives: Review the physiological mechanism responsible to regulate acid base balance in the body i.e.: Buffers (phosphate, hemoglobin, carbonate) Renal mechanism Respiratory
UNIT VI: ACID BASE IMBALANCE 1 Objectives: Review the physiological mechanism responsible to regulate acid base balance in the body i.e.: Buffers (phosphate, hemoglobin, carbonate) Renal mechanism Respiratory
Pulmonary Problems of the Neonate. Jon Palmer, VMD, DACVIM Chief, Neonatal Intensive Care Service New Bolton Center, University of Pennsylvania, USA
 Pulmonary Problems of the Neonate Jon Palmer, VMD, DACVIM Chief, Neonatal Intensive Care Service New Bolton Center, University of Pennsylvania, USA Lower Respiratory Diseases Ventilation/Perfusion Abnormalities
Pulmonary Problems of the Neonate Jon Palmer, VMD, DACVIM Chief, Neonatal Intensive Care Service New Bolton Center, University of Pennsylvania, USA Lower Respiratory Diseases Ventilation/Perfusion Abnormalities
CHEST INJURY PULMONARY CONTUSION
 CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2
 2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
UTSW/BioTel EMS TRAINING BULLETIN January EMS TB Accidental Hypothermia
 UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
Case discussion Acute severe asthma during pregnancy. J.G. van der Hoeven
 Case discussion Acute severe asthma during pregnancy J.G. van der Hoeven Case (1) 32-year-old female - gravida 3 - para 2 Previous medical history - asthma Pregnant (33 w) Acute onset fever with wheezing
Case discussion Acute severe asthma during pregnancy J.G. van der Hoeven Case (1) 32-year-old female - gravida 3 - para 2 Previous medical history - asthma Pregnant (33 w) Acute onset fever with wheezing
1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation.
 Chapter 1: Principles of Mechanical Ventilation TRUE/FALSE 1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation. F
Chapter 1: Principles of Mechanical Ventilation TRUE/FALSE 1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation. F
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
5. What is the cause of this patient s metabolic acidosis? LACTIC ACIDOSIS SECONDARY TO ANEMIC HYPOXIA (HIGH CO LEVEL)
 Self-Assessment RSPT 2350: Module F - ABG Analysis 1. You are called to the ER to do an ABG on a 40 year old female who is C/O dyspnea but seems confused and disoriented. The ABG on an FiO 2 of.21 show:
Self-Assessment RSPT 2350: Module F - ABG Analysis 1. You are called to the ER to do an ABG on a 40 year old female who is C/O dyspnea but seems confused and disoriented. The ABG on an FiO 2 of.21 show:
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
ENVIRONMENTAL EMERGENCIES
 Joanna Jakubaszko-Jabłońska ENVIRONMENTAL EMERGENCIES Chair of Emergency Medicine Wroclaw Medical University Emergency treatment of near-drowning victims Clinical findings: The victim may present with
Joanna Jakubaszko-Jabłońska ENVIRONMENTAL EMERGENCIES Chair of Emergency Medicine Wroclaw Medical University Emergency treatment of near-drowning victims Clinical findings: The victim may present with
Post Cardiac Arrest Care 2015 American Heart Association Guideline Update for CPR and Emergency Cardiovascular Care
 Post Cardiac Arrest Care 2015 American Heart Association Guideline Update for CPR and Emergency Cardiovascular Care รศ.ดร.พญ.ต นหยง พ พานเมฆาภรณ ภาคว ชาว ส ญญ ว ทยา คณะแพทยศาสตร มหาว ทยาล ยเช ยงใหม System
Post Cardiac Arrest Care 2015 American Heart Association Guideline Update for CPR and Emergency Cardiovascular Care รศ.ดร.พญ.ต นหยง พ พานเมฆาภรณ ภาคว ชาว ส ญญ ว ทยา คณะแพทยศาสตร มหาว ทยาล ยเช ยงใหม System
Objectives. Health care significance of ARF 9/10/15 TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION
 TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION Louisa Chika Ikpeama, DNP, CCRN, ACNP-BC Objectives Identify health care significance of acute respiratory
TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION Louisa Chika Ikpeama, DNP, CCRN, ACNP-BC Objectives Identify health care significance of acute respiratory
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 PS1070 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: CARDIOVASCULAR INTENSIVE Job Title of Reviewer: Director, CVICU EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY
PS1070 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: CARDIOVASCULAR INTENSIVE Job Title of Reviewer: Director, CVICU EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Capnography Connections Guide
 Capnography Connections Guide Patient Monitoring Contents I Section 1: Capnography Introduction...1 I Section 2: Capnography & PCA...3 I Section 3: Capnography & Critical Care...7 I Section 4: Capnography
Capnography Connections Guide Patient Monitoring Contents I Section 1: Capnography Introduction...1 I Section 2: Capnography & PCA...3 I Section 3: Capnography & Critical Care...7 I Section 4: Capnography
Pediatric advanced life support. Management of decreased conscious level in children. Virgi ija Žili skaitė 2017
 Pediatric advanced life support. Management of decreased conscious level in children Virgi ija Žili skaitė 2017 Life threatening conditions: primary assessment, differential diagnostics and emergency care.
Pediatric advanced life support. Management of decreased conscious level in children Virgi ija Žili skaitė 2017 Life threatening conditions: primary assessment, differential diagnostics and emergency care.
RESPIRATORY COMPLICATIONS AFTER SCI
 SHEPHERD.ORG RESPIRATORY COMPLICATIONS AFTER SCI NORMA I RIVERA, RRT, RCP RESPIRATORY EDUCATOR SHEPHERD CENTER 2020 Peachtree Road, NW, Atlanta, GA 30309-1465 404-352-2020 DISCLOSURE STATEMENT I have no
SHEPHERD.ORG RESPIRATORY COMPLICATIONS AFTER SCI NORMA I RIVERA, RRT, RCP RESPIRATORY EDUCATOR SHEPHERD CENTER 2020 Peachtree Road, NW, Atlanta, GA 30309-1465 404-352-2020 DISCLOSURE STATEMENT I have no
Accidental Hypothermia
 Accidental Hypothermia Doug Brown, MD, FRCPC Emergency Physician Royal Columbian & Eagle Ridge Hospital October, 2013 Objectives 45min lecture, 15min discussion & questions: Inspirational case & overview
Accidental Hypothermia Doug Brown, MD, FRCPC Emergency Physician Royal Columbian & Eagle Ridge Hospital October, 2013 Objectives 45min lecture, 15min discussion & questions: Inspirational case & overview
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit
 Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Lesson 4-3: Cardiac Emergencies. CARDIAC EMERGENCIES Angina, AMI, CHF and AED
 Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
Restrictive Pulmonary Diseases
 Restrictive Pulmonary Diseases Causes: Acute alveolo-capillary sysfunction Interstitial disease Pleural disorders Chest wall disorders Neuromuscular disease Resistance Pathophysiology Reduced compliance
Restrictive Pulmonary Diseases Causes: Acute alveolo-capillary sysfunction Interstitial disease Pleural disorders Chest wall disorders Neuromuscular disease Resistance Pathophysiology Reduced compliance
Epilepsy CASE 1 Localization Differential Diagnosis
 2 Epilepsy CASE 1 A 32-year-old man was observed to suddenly become unresponsive followed by four episodes of generalized tonic-clonic convulsions of the upper and lower extremities while at work. Each
2 Epilepsy CASE 1 A 32-year-old man was observed to suddenly become unresponsive followed by four episodes of generalized tonic-clonic convulsions of the upper and lower extremities while at work. Each
Post-Anesthesia Care In the ICU
 Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Surviving Sepsis Campaign. Guidelines for Management of Severe Sepsis/Septic Shock. An Overview
 Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
HealthCare Training Service
 HealthCare Training Service Advanced Life Support Exam Time: Perusal Time: 20 minutes 5 minutes Total Marks: 25 Instructions: Read each question carefully. Using a pencil, record your response to each
HealthCare Training Service Advanced Life Support Exam Time: Perusal Time: 20 minutes 5 minutes Total Marks: 25 Instructions: Read each question carefully. Using a pencil, record your response to each
Management of refractory ARDS. Saurabh maji
 Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
Breathing life into new therapies: Updates on treatment for severe respiratory failure. Whitney Gannon, MSN ACNP-BC
 Breathing life into new therapies: Updates on treatment for severe respiratory failure Whitney Gannon, MSN ACNP-BC Overview Definition of ARDS Clinical signs and symptoms Causes Pathophysiology Management
Breathing life into new therapies: Updates on treatment for severe respiratory failure Whitney Gannon, MSN ACNP-BC Overview Definition of ARDS Clinical signs and symptoms Causes Pathophysiology Management
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen
 Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
NON INVASIVE LIFE SAVERS. Non Invasive Ventilation (NIV)
 Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Outcomes of Therapeutic Hypothermia in Cardiac Arrest. Saad Mohammed Shariff, MBBS Aravind Herle, MD, FACC
 Outcomes of Therapeutic Hypothermia in Cardiac Arrest Saad Mohammed Shariff, MBBS Aravind Herle, MD, FACC https://my.americanheart.org/idc/groups/ahamah-public/@wcm/@sop/@scon/documents/downloadable/ucm_427331.pdf
Outcomes of Therapeutic Hypothermia in Cardiac Arrest Saad Mohammed Shariff, MBBS Aravind Herle, MD, FACC https://my.americanheart.org/idc/groups/ahamah-public/@wcm/@sop/@scon/documents/downloadable/ucm_427331.pdf
Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical]
![Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical] Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical]](/thumbs/87/96512765.jpg) Children s Acute Transport Service Clinical Guidelines Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical] Document Control Information Author D Lutman Author Position Head of Clinical
Children s Acute Transport Service Clinical Guidelines Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical] Document Control Information Author D Lutman Author Position Head of Clinical
PALS NEW GUIDELINES 2010
 PALS NEW GUIDELINES 2010 DR WALEED ALAMRI PEDIATRIC EMERGENCY CONSULTANT FEB 24, 2011 Pediatric Basic Life Support Change in CPR Sequence (C-A-B Rather Than A-B-C) 2010 (New): Initiate CPR for infants
PALS NEW GUIDELINES 2010 DR WALEED ALAMRI PEDIATRIC EMERGENCY CONSULTANT FEB 24, 2011 Pediatric Basic Life Support Change in CPR Sequence (C-A-B Rather Than A-B-C) 2010 (New): Initiate CPR for infants
CRACKCast Episode Hydrocarbons (Ch th )
 CRACKCast Episode Hydrocarbons (Ch. 152 9 th ) Episode Overview Key Concepts: Aspiration is the major toxic risk of hydrocarbon poisoning. Hydrocarbons may cause systemic toxicity, burns, seizures, cardiac
CRACKCast Episode Hydrocarbons (Ch. 152 9 th ) Episode Overview Key Concepts: Aspiration is the major toxic risk of hydrocarbon poisoning. Hydrocarbons may cause systemic toxicity, burns, seizures, cardiac
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
FOR REPRESENTATIVE EDUCATION
 Neuromuscular Blockade in the ICU NIMBEX Indication 1 NIMBEX (cisatracurium besylate) is indicated as an adjunct to general anesthesia to facilitate tracheal intubation in adults and in pediatric patients
Neuromuscular Blockade in the ICU NIMBEX Indication 1 NIMBEX (cisatracurium besylate) is indicated as an adjunct to general anesthesia to facilitate tracheal intubation in adults and in pediatric patients
Oxygen and ABG. Dr Will Dooley
 Oxygen and ABG G Dr Will Dooley Oxygen and ABGs Simply in 10 cases Recap of: ABG interpretation Oxygen management Some common concerns A-a gradient Base Excess Anion Gap COPD patients CPAP/BiPAP First
Oxygen and ABG G Dr Will Dooley Oxygen and ABGs Simply in 10 cases Recap of: ABG interpretation Oxygen management Some common concerns A-a gradient Base Excess Anion Gap COPD patients CPAP/BiPAP First
Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist
 Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist Introduction. Basic Life Support (BLS). Advanced Cardiac Life Support (ACLS). Cardiovascular diseases (CVDs) are the number one cause of death
Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist Introduction. Basic Life Support (BLS). Advanced Cardiac Life Support (ACLS). Cardiovascular diseases (CVDs) are the number one cause of death
Key Points. Angus DC: Crit Care Med 29:1303, 2001
 Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Evolution of the Hospital Capacity for SARS in Taipei
 HRC for SARS 26 Evolution of the Hospital Capacity for SARS in Taipei Tzong-Luen Wang, MD, PhD; Kuo-Chih Chen, MD; I-Yin Lin, MD; Chien-Chih Chen, MD; Chun-Chieh Chao, MD; Hang Chang, MD, PhD Abstract
HRC for SARS 26 Evolution of the Hospital Capacity for SARS in Taipei Tzong-Luen Wang, MD, PhD; Kuo-Chih Chen, MD; I-Yin Lin, MD; Chien-Chih Chen, MD; Chun-Chieh Chao, MD; Hang Chang, MD, PhD Abstract
Pediatric Advanced Life Support
 Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
In-hospital Care of the Post-Cardiac Arrest Patient. David A. Pearson, MD, FACEP, FAAEM Associate Program Director Department of Emergency Medicine
 In-hospital Care of the Post-Cardiac Arrest Patient David A. Pearson, MD, FACEP, FAAEM Associate Program Director Department of Emergency Medicine Disclosures I have no financial interest, arrangement,
In-hospital Care of the Post-Cardiac Arrest Patient David A. Pearson, MD, FACEP, FAAEM Associate Program Director Department of Emergency Medicine Disclosures I have no financial interest, arrangement,
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
ACLS Prep. Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep.
 November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
The use of proning in the management of Acute Respiratory Distress Syndrome
 Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION
 SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date Gender Female Male Date of surgery INCLUSION & EXCLUSION CRITERIA YES
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date Gender Female Male Date of surgery INCLUSION & EXCLUSION CRITERIA YES
Handling Common Problems & Pitfalls During. Oxygen desaturation in patients receiving mechanical ventilation ACUTE SEVERE RESPIRATORY FAILURE
 Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
9/5/2018. Conflicts of Interests. Pediatric Acute Respiratory Distress Syndrome. Objectives ARDS ARDS. Definitions. None
 Pediatric Acute Respiratory Distress Syndrome Conflicts of Interests Diane C Lipscomb, MD Director Inpatient Pediatric Medical Director Mercy Springfield Associate Clerkship Clinical Director University
Pediatric Acute Respiratory Distress Syndrome Conflicts of Interests Diane C Lipscomb, MD Director Inpatient Pediatric Medical Director Mercy Springfield Associate Clerkship Clinical Director University
2. To provide an ethical, moral and practical framework for decision-making during a public health emergency.
 November 2010 TABLE TOP EXERCISE PARTICIPANT GUIDE When Routine Critical Care Resources Are Not Available Time expectations for each session: SECTION ACTIVITY TIME I Introduction 5 minutes II Exercise
November 2010 TABLE TOP EXERCISE PARTICIPANT GUIDE When Routine Critical Care Resources Are Not Available Time expectations for each session: SECTION ACTIVITY TIME I Introduction 5 minutes II Exercise
Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo
 Instant dowload and all chapters Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo https://testbanklab.com/download/test-bank-pilbeams-mechanical-ventilation-physiologicalclinical-applications-6th-edition-cairo/
Instant dowload and all chapters Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo https://testbanklab.com/download/test-bank-pilbeams-mechanical-ventilation-physiologicalclinical-applications-6th-edition-cairo/
Hypothermia: The Science and Recommendations (In-hospital and Out)
 Hypothermia: The Science and Recommendations (In-hospital and Out) L. Kristin Newby, MD, MHS Professor of Medicine Duke University Medical Center Chair, Council on Clinical Cardiology, AHA President, Society
Hypothermia: The Science and Recommendations (In-hospital and Out) L. Kristin Newby, MD, MHS Professor of Medicine Duke University Medical Center Chair, Council on Clinical Cardiology, AHA President, Society
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Therapeutic hypothermia
 INDUCED HYPOTHERMIA Dr. Attilla Kiss M.D. Acting Medical Director Emergency Services EMS Medical Director St. John Medical Center OBJECTIVES Define and explain Induced Hypothermia Discuss both pre-hospital
INDUCED HYPOTHERMIA Dr. Attilla Kiss M.D. Acting Medical Director Emergency Services EMS Medical Director St. John Medical Center OBJECTIVES Define and explain Induced Hypothermia Discuss both pre-hospital
11/23/2015. Disclosures. Stroke Management in the Neurocritical Care Unit. Karel Fuentes MD Medical Director of Neurocritical Care.
 Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Disclosures I have no relevant commercial relationships to disclose, and my presentations will not
Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Disclosures I have no relevant commercial relationships to disclose, and my presentations will not
NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP)
 Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Z19.2 Cross Reference to Patient Care Maps & Clinical Care Procedures
 2017-04-07 Old version G1 Code of Ethics G2 Scope and Function G3 Scene Assessment G4 Triage G5 Primary Survey G6 Shock G7 Load and Go G8 Secondary Survey G9 Unconscious Patient G10A Obstructed Airway
2017-04-07 Old version G1 Code of Ethics G2 Scope and Function G3 Scene Assessment G4 Triage G5 Primary Survey G6 Shock G7 Load and Go G8 Secondary Survey G9 Unconscious Patient G10A Obstructed Airway
Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off.
 1 2 EMT OPTIONAL SKILL Naloxone Intranasal Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. 3 4 5 6 Course Outline Introduction
1 2 EMT OPTIONAL SKILL Naloxone Intranasal Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. 3 4 5 6 Course Outline Introduction
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms. Introduction to the Algorithms
 Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
THE ACUTE RESPIRATORY DISTRESS SYNDROME. Daniel Brockman, DO
 THE ACUTE RESPIRATORY DISTRESS SYNDROME Daniel Brockman, DO Objectives Describe the history and evolution of the diagnosis of ARDS Review the diagnostic criteria for ARDS Discuss the primary interventions
THE ACUTE RESPIRATORY DISTRESS SYNDROME Daniel Brockman, DO Objectives Describe the history and evolution of the diagnosis of ARDS Review the diagnostic criteria for ARDS Discuss the primary interventions
Critical Care Treatment Guidelines
 Critical Care Treatment Guidelines West Virginia Office of Emergency Medical Services CCT Guidelines CCT Guidelines TABLE OF CONTENTS Preface Acknowledgments Using the Guidelines INITIAL TREATMENT / UNIVERSAL
Critical Care Treatment Guidelines West Virginia Office of Emergency Medical Services CCT Guidelines CCT Guidelines TABLE OF CONTENTS Preface Acknowledgments Using the Guidelines INITIAL TREATMENT / UNIVERSAL
Respiratory Failure in the Pediatric Patient
 Respiratory Failure in the Pediatric Patient Ndidi Musa M.D. Associate Professor of Pediatrics Medical College of Wisconsin Pediatric Cardiac Intensivist Children s Hospital of Wisconsin Objectives Recognize
Respiratory Failure in the Pediatric Patient Ndidi Musa M.D. Associate Professor of Pediatrics Medical College of Wisconsin Pediatric Cardiac Intensivist Children s Hospital of Wisconsin Objectives Recognize
TTC Catalog - Respiratory Care (RES)
 2018-2019 TTC Catalog - Respiratory Care (RES) RES 110 - Cardiopulmonary Science I This course focuses on assessment, treatment evaluation of patients with cardiopulmonary disease. RES 121 Restrictions:
2018-2019 TTC Catalog - Respiratory Care (RES) RES 110 - Cardiopulmonary Science I This course focuses on assessment, treatment evaluation of patients with cardiopulmonary disease. RES 121 Restrictions:
Hospital Resource and Clinical Management Guidelines for Hospital Healthcare Providers When Routine Critical Care Resources Are Not Available
 Hospital Resource and Clinical Management Guidelines for Hospital Healthcare Providers When Routine Critical Care Resources Are Not Available Medical College of Wisconsin Center for Medical Incident Management
Hospital Resource and Clinical Management Guidelines for Hospital Healthcare Providers When Routine Critical Care Resources Are Not Available Medical College of Wisconsin Center for Medical Incident Management
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION
 SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date (DD/MMM/YYYY) (DD/MMM/YYYY) Gender Female Male Date of surgery (DD/MMM/YYYY)
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date (DD/MMM/YYYY) (DD/MMM/YYYY) Gender Female Male Date of surgery (DD/MMM/YYYY)
HEAVY METALS : Review
 HEAVY METALS : Review INHALED TOXINS Dr. Tawfiq Almezeiny MBBS FRCPC (CCM) Introduction Airborne toxins typically produce local noxious effects on the airways and lungs. Examples of Inhalational exposure:
HEAVY METALS : Review INHALED TOXINS Dr. Tawfiq Almezeiny MBBS FRCPC (CCM) Introduction Airborne toxins typically produce local noxious effects on the airways and lungs. Examples of Inhalational exposure:
Patient Case. Post cardiac arrest pathophysiology 10/19/2017. Disclosure. Objectives. Patient Case-TM
 Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Ac#ve, ECMO or locally available alterna#ves. invasive warming. Ini#ally: Ac#ve noninvasive or minimally
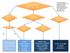 Suspected Hypothermia Temp
Suspected Hypothermia Temp
Management of Cardiac Arrest Based on : 2010 American Heart Association Guidelines
 Management of Cardiac Arrest Based on : 2010 American Heart Association Guidelines www.circ.ahajournals.org Elham Pishbin. M.D Assistant Professor of Emergency Medicine MUMS C H E S Advanced Life Support
Management of Cardiac Arrest Based on : 2010 American Heart Association Guidelines www.circ.ahajournals.org Elham Pishbin. M.D Assistant Professor of Emergency Medicine MUMS C H E S Advanced Life Support
NON-INVASIVE VENTILATION. Lijun Ding 23 Jan 2018
 NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Post-Cardiac Arrest Syndrome. MICU Lecture Series
 Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
Naloxone Intranasal EMT OPTIONAL SKILL. Cell Phones and Pagers. Course Outline 09/2017
 EMT OPTIONAL SKILL Naloxone Intranasal Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and Overview
EMT OPTIONAL SKILL Naloxone Intranasal Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and Overview
Landmark articles on ventilation
 Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Drowning induced acute respiratory failure: A case report
 CASE REPORT Touzani et al. 1 PEER REVIEWED OPEN ACCESS Drowning induced acute respiratory failure: A case report Soumaya Touzani, Nawfal Houari, Abderrahim Elbouazzaoui, Brahim Boukatta, Nabil Kanjaa ABSTRACT
CASE REPORT Touzani et al. 1 PEER REVIEWED OPEN ACCESS Drowning induced acute respiratory failure: A case report Soumaya Touzani, Nawfal Houari, Abderrahim Elbouazzaoui, Brahim Boukatta, Nabil Kanjaa ABSTRACT
