CIRCULATORY DISTURBANCES
|
|
|
- Julianna Dickerson
- 6 years ago
- Views:
Transcription
1 CIRCULATORY DISTURBANCES Shannon Martinson, January 2017 Office: 418N All lecture notes and slide shows are available online: REFERENCE TEXTS: Pathologic Basis of Veterinary Disease, Zachary (Ed): 6 th edition (2017), Chapter 2. Robbins & Cotran, Pathologic Basis of Disease, Kumar, et al (Ed); 9 th edition (2015), Chapter 4. NORMAL CIRCULATORY SYSTEM [for background information only] Important Concepts Distribution of fluid is a carefully controlled homeostatic mechanism. Deviations from normal may have profound pathological effects. Normal functions require intact blood and lymph vessels. Endothelial cells play important roles in fluid distribution, hemostasis, inflammation, and healing. Components of the Circulatory System Heart pump. Arteries distribution system. Microcirculation system nutrient / waste exchange between blood and tissue. Veins & lymphatics collection system. Endothelial cells All components of the circulatory system are lined by a single layer of endothelial cells These cells synthesize & secrete substances which effect fluid balance, hemostasis, inflammation / immunity, angiogenesis / healing. Microcirculation Called microcirculation because it is microscopic. There are 3 main components 1) Arterioles Walls contain innervated smooth muscle cells (myocytes); contract to control blood flow. 2) Postcapillary venules Similar structure to capillary, but acquire thin layer of muscle as they move away from capillary bed. 3) Capillaries Enormous volume (1300 times the cross-sectional area of the aorta), but normally contain only ~5% of the blood; ~ 95% of capillary beds are not open during normal conditions. Site where nutrients and wastes are exchanged and a critical area in fluid balance*. Mechanisms for substance transport across the capillary wall: The capillary wall is a semipermeable membrane; influences movement of fluid (water and solutes), nutrients and waste between blood and interstitial space.
2 1) Direct diffusion Most small molecules move by passive diffusion through the endothelial cell membrane (eg gas, lipid soluble molecules) or via interendothelial pores (eg water, ions, glucose, amino acids, waste). Normal interendothelial pores too small to allow escape of large proteins (eg albumin).* o During inflammation, endothelial cells contract allowing larger molecules to escape. 2) Transcytosis With some endothelial cells, fluids / macromolecules can be transported across the cell by vesicles. Regional Differences in Capillary Lining: 1) Continuous capillaries Lined by a complete simple endothelium and a basal lamina. Found in muscle, brain, thymus, skin, bone, lung and other tissues. 2) Fenestrated capillaries Have many small openings; found in tissues with abundant fluid transport. Often have a diaphragm (egs intestinal villi, kidney interstitium, choroid plexus). Can act as a filter (eg renal glomerulus). 3) Discontinuous capillaries Larger gaps than fenestrated with discontinuous basal lamina; allows large molecules or even cells to exit (eg red blood cells in the spleen). Hepatic and splenic sinusoids are lined by this type of endothelium. Fluid Distribution & Homeostasis Total Body Water (~60% of lean body weight) Extracellular fluid (20%) o Plasma (5%) o Interstitial tissue fluid (15%) Intracellular fluid (40%) Interstitium Interstitium = space between microcirculation and the cells*. Functions: o It binds cellular and structural elements into discrete organs and tissues. o Acts as a medium through which all metabolic products must pass between microcirculation and cells. Structure: o Interstitium is composed of extracellular matrix (ECM) + supporting cells (eg fibroblasts) o ECM provides structural support and has adhesive & absorptive properties: ➀ Structural molecules: collagen, reticulin & elastin fibers. ➁ Adhesive glycoproteins: fibronectin, laminin. ➂ Absorptive (hydroscopic) molecules: glycosaminoglycans, proteoglycans.
3 Movement of Fluids* Distribution of fluids, nutrients & wastes between blood interstitium cells is controlled by physical structures, pressures gradients, and ion concentration (osmotic) gradients. In most areas, the capillary allows the free passage of water and ions and opposes the passage of plasma proteins. Water distribution between plasma and interstitium is primarily determined by the differences in hydrostatic and osmotic pressure between the two compartments. Starling's equation Hydrostatic pressure in the vascular system (aided slightly by interstitial colloidal osmotic/oncotic pressure) is the force that moves fluid out of the vessels. Plasma oncotic pressure (= osmotic pressure exerted by plasma proteins - especially albumin), and to a lesser extent, tissue hydrostatic pressure around blood vessels are the forces that contain the fluid within the vascular system. ARTERIOLAR VENULAR Plasma Hydrostatic Psi 30 mm Hg 17 mm Hg Tissue Hydrostatic Psi 8 mm Hg 8 mm Hg Plasma Colloidal Osmotic Psi 25 mm Hg 25 mm Hg Tissue Colloidal Osmotic Psi 10 mm Hg 10 mm Hg (30-8)- (25-10) = 7 mm Hg (17-8)-(25-10) = 6 mm Hg Net filtration Pressure Net absorption Pressure The difference between the two pressures indicates that there is constant net movement of fluid out of the capillary bed into the interstitium this fluid is removed by the lymphatics. EDEMA* Edema = Excess accumulation of fluid in interstitial tissues or in body cavities. o Edema fluid is outside both the vascular and cellular compartments. Gross: o Organs are swollen, wet (gelatinous) and heavy; fluid weeps from cut surface. o In several species (eg horses, some cattle) fluids are slightly yellow. Histology: o Lightly staining eosinophilic ( protein) or clear/colorless ( protein) fluid. o Tissue spaces are distended by the edema (collagen bundles separated by increased clear space) and lymphatics are dilated. Four Mechanisms of Edema Production: 1. Increased intravascular hydrostatic pressure Results from an impediment to venous blood flow o Can be generalized (eg heart failure) o Can be localized (eg tightly bandaged limb resulting in venous occlusion).
4 2. Decreased plasma colloidal osmotic (oncotic) pressure Results from hypoproteinemia o Proteins are not absorbed from the diet (egs starvation, GI malabsorption). o Proteins are not produced (eg liver disease). o Proteins are lost from the body (egs glomerular disease, intestinal damage). 3. Decreased lymphatic drainage / Lymphatic obstruction Results from damage or obstruction of lymphatics (by surgery / trauma, neoplasia, or inflammation [lymphangitis]). 4. Increased vascular permeability / Endothelial damage Mostly due to the initial reaction of the microvasculature to inflammatory / immunologic stimuli release of inflammatory mediators vasodilation and increased vascular permeability inflammatory edema o This mechanism will be further discussed in your inflammation lectures. Note: The endothelium can also be damaged directly by some bacteria, viruses, toxins, and autoimmune diseases, resulting in increased vascular permeability. Mechanisms 1, 2 and 3 result in "non-inflammatory edema" - protein poor effusion referred to as transudate. o Transudate: Protein content < 30 g/l Specific gravity < Total nucleated cell count < 1.5X10 9 /L Mechanism 4 results in inflammatory edema" - protein rich effusion referred to as exudate. o Exudate Protein content > 30 g/l Specific gravity > Total nucleated cell count > 7.0X10 9 /L Localized versus Generalized Edema: 1) Local Edema a) Mechanisms ➀ Local impaired venous drainage. ➁ Local lymphatic obstruction. ➂ Local inflammation. 2) Generalized Edema a) Mechanisms ➀ Increased generalized hydrostatic pressure of blood (heart failure). ➁ Decreased colloid osmotic pressure of blood (hypoproteinemia).
5 b) Common Locations of Generalized Edema With edema is generalized, we often see a combination of ascites, hydrothorax & subcutaneous ( dependent ) edema. o Dependent edema: Subcutaneous tissues of the ventrum ("brisket edema") Subcutaneous tissues of the ventral mandibular/cervical region ("bottle jaw") Terminology of Edema: Pitting Edema = when pressure is applied to an area of subcutaneous edema a depression or dent results as excessive interstitial fluid is forced to adjacent areas. Anasarca = Severe and generalized edema with profound subcutaneous tissue swelling (fetuses). Hydrothorax = Non-inflammatory fluid (transudate) in the thoracic cavity. Hydropericardium = Non-inflammatory fluid (transudate) in the sac around the heart. Ascites (= Hydroperitoneum) = Non-inflammatory fluid (transudate) in the peritoneal cavity. Clinical Significance of Edema The clinical significance of edema is dependent upon: ➀ Extent - mild vs moderate vs marked/severe ➁ Location - site of accumulation: skin (relatively insignificant) vs lung or brain (often lethal). ➂ Duration - tissues may become more firm and distorted due to increased fibrous connective tissue after prolonged edema. Pulmonary Edema Definition = accumulation of edema fluid in the interstitium and alveoli of the lungs. This is a common cause of death in many disease processes. a) Mechanisms of pulmonary edema ➀ Circulatory failure (especially due to left-sided heart failure) Due to increased hydrostatic pressure of blood in the pulmonary veins (congestion) transudation of fluid into the alveolar spaces. It is the most common cause of pulmonary edema. ➁ Damage to pulmonary capillary endothelium (microvascular injury) Usually occurs with acute inflammation (ie inflammatory edema) or less commonly toxins. o Due to a sudden increase in vascular permeability. Often results in sudden death (when peracute); can be followed by pneumonia in survivors. b) Gross appearance of pulmonary edema The lungs are heavy and wet. Froth (edema fluid + air bubbles) may be present within the trachea and bronchi and is obvious on cut section. The interlobular septa are prominent / thickened due to the increased fluid within this space.
6 Often accompanied by congestion of the pulmonary vessels (especially when there is leftsided heart failure). c) Histopathology of pulmonary edema See edema fluid in the interstitium and alveolar spaces; eventually see dilated interlobular / pleural lymphatics. The edema fluid can be clear or pink in color (depending on the protein content: protein = pink fluid). d) Chronic Pulmonary Edema Most commonly seen with chronic cardiac failure and accompanying pulmonary congestion (discussed later). Over a long period, pleura and alveolar walls may become thickened with fibrous connective tissue. Edema of the Brain (Cerebral Edema) Can be caused by: trauma (head injury), obstruction of venous outflow, intracranial infections (eg meningitis, encephalitis). a) Gross appearance of cerebral edema Brain is heavier than normal. Gyri are swollen and become flattened and the sulci are narrow. When severe can see: ➀ Cerebellar coning - herniation of the cerebellum through the foramen magnum. ➁ Cerebral herniation - herniation of the caudal cerebral cortex beneath the tentorium cerebella. b) Histopathology of cerebral edema Expansion of perivascular (Virchow-Robin) spaces. DEHYDRATION* Definition = Deficiency of water; resulting from an imbalance between uptake and loss of water from the body. Causes include: uncontrolled diarrhea, vomiting, renal failure, heat-stroke, water deprivation. a) Mechanisms A decrease in the total body water results in water deficit, which is shared among plasma, intracellular and interstitial fluid compartments. Tissue perfusion is reduced. Severe dehydration may result in hypovolemic shock as plasma water is drawn into the interstitium. b) Gross appearance of dehydration Folds of skin pulled out from the body hesitate before returning to their normal position ("skin tenting"). Eyes are sunken, mucous membranes and subcutaneous tissues are dry and sticky.
7 ALTERATIONS IN BLOOD FLOW AND PERFUSION HYPEREMIA* Definition= Active engorgement of vascular beds due to increased arteriolar inflow. Types of Hyperemia: 1. Physiologic Hyperemia examples: blood flow to the stomach and intestines during digestion blood flow in the muscles during exercise blood flow in skin to dissipate heat neurovascular hyperemia (blushing) 2. Pathologic Hyperemia Results from an underlying pathologic process (usually inflammation). Arteriolar dilation is a response to inflammatory stimuli / mediators. Red coloration is a cardinal sign of inflammation = "Hyperemia of Inflammation" Often accompanied by edema. The effect of hyperemia: Hastens movement of metabolites into an area Flushes catabolites from the area Gross Appearance of hyperemia: The affected tissue is red and warm, as arterioles and capillaries are filled with oxygenated blood. CONGESTION* Definition = Passive engorgement of a vascular bed generally caused by a decreased outflow of blood. Gross appearance: o Tissues are dark red to blue/black (cyanotic), depending on degree of stagnation (deoxygenated blood). o Cut surfaces ooze blood and tissues are often wet (due to accompanying edema). Histology: o Acute: Capillaries engorged with blood and usually some edema. o Chronic: Engorgement by poorly oxygenated venous blood chronic local hypoxia atrophy, degeneration or even necrosis of parenchymal cells. The effect of congestion: o Leads to hypoxia and accumulation of catabolites o Often edema occurs (due to increased hydrostatic pressure) o Interference with normal tissue function o May get thrombosis of congested veins o +/- Proliferation of connective tissue (if chronic)
8 Two factors are considered in defining the type of congestion: 1) Duration: Acute: Implies abrupt onset with rapid development. Chronic: Slowly developing or present for a long time. 2) Extent: Localized congestion: Confined to a discrete area (eg isolated venous obstruction). Generalized congestion: Indicates a systemic change (eg cardiac failure). Localized Congestion Local obstruction to venous drainage (eg intestinal torsion / intussusception / splenic torsion, strangulation). Blood backs up into the microvascular bed passive venous engorgement of the drainage area. Generalized Congestion Congestion associated with pathology of the heart or lung tends to be generalized and can be acute or chronic: o With left-sided heart failure Congestion of lungs (= pulmonary congestion). o With right-sided heart failure Systemic congestion (especially the liver) and generalized edema (eg ascites, dependent edema). o With certain types of primary pulmonary disease progressive loss of pulmonary vascular bed pulmonary hypertension right heart failure secondary to pulmonary disease = Cor Pulmonale. Acute generalized congestion is most commonly seen with acute heart failure or following euthanasia with barbiturates Pulmonary Congestion Most commonly caused by left heart failure. Left ventricular failure impedes forward flow of blood from the lungs congestion of the lungs alveolar capillaries become engorged with blood ( pressure in alveolar capillaries). Gross appearance of acute congestion: Diffuse red lungs (congestion) which are wet (edema) and heavy). Histology of acute congestion: The capillaries are filled with RBCs, +/- proteinaceous fluid in the alveoli (edema) Gross appearance of chronic congestion: Lungs can be lightly tan in color (due to presence of hemosiderin - see below). Histology of chronic congestion: The capillaries are filled with RBCs and there is proteinaceous fluid (edema), RBCs and hemosiderin laden macrophages (heart failure cells) in the alveolar spaces Consequences of Chronic Pulmonary Congestion: 1. Intra-alveolar hemorrhage o Small capillaries rupture focal hemorrhage into the alveolar spaces RBCs are phagocytized by alveolar macrophages the iron from the heme of RBCs is
9 stored as hemosiderin pigment within macrophages = "heart failure cells". 2. Pulmonary Edema (see previous discussion on edema) o Causes interference with gaseous exchange. 3. Fibrosis of Interstitium o Fibroblasts secrete excess collagen in response to increased pressure in alveolar capillaries and chronic edema in alveolar interstitium. 4. Pulmonary Hypertension Increased pressure in the alveolar capillaries increased pressure in pulmonary arteries pulmonary hypertension. Can result in right heart failure (cor pulmonale) Hepatic congestion Most commonly due to right heart failure Right ventricular failure impedes forward flow of blood from the body (vena cava) congestion of the liver, also ascites and dependent edema Cor pulmonale (see above) a) Gross appearance of hepatic congestion Liver is usually enlarged and dark red-brown with rounded edges. o Acutely there is an increase in liver size due to increased volume of added blood. o Chronically there is low-grade hypoxia & blood pressure atrophy & death of centrilobular hepatocytes & fibrosis (with a possible decrease in size of the liver). On cut surface has a reticular appearance (= regular dark red and tan-brown zonal pattern) = "nutmeg liver". o Dark red areas correspond to the congested zones around the central veins (zone 3) and the tan-brown areas correspond to the less affected parenchyma around the portal / midzonal areas (zone 1 & 2). b) Histology Acute congestion o Central veins and sinusoids in zone 3 are distended with erythrocytes. o Centrilobular hepatocyte (zone 3) atrophy, degeneration and/or necrosis due to hypoxia in stagnant blood. o Midzonal hepatocyte (zone 2) fatty change due to partial hypoxia. o Periportal hepatocytes (zone 1) mostly normal. Chronic congestion o As above with these additional changes in the centrilobular region (zone 3): Hemosiderin-filled macrophages (Kupffer cells) due to erythrocyte phagocytosis. Dilation of sinusoids atrophy/ loss of centrilobular hepatocytes. Low-grade hypoxia and increased pressure in zone 3 fibrous connective tissue deposition ("cardiac cirrhosis").
10 Hyperemia and Congestion vs Hemorrhage Hyperemia / congestion blood is inside a blood vessel (ie: intravascular) Hemorrhage blood is outside the vessel wall (ie: extravascular) SHOCK Shock is characterized by systemic hypotension due to either reduced cardiac output or to reduced effective circulating blood volume which results in impaired tissue perfusion and cellular hypoxia* Brain and heart are the organs most susceptible to ischemic damage from shock. Shock is the final common pathway for many potentially lethal clinical events which include microbial sepsis, severe hemorrhage, extensive trauma or burns, myocardial infarction, severe pulmonary embolism, etc. Three General Categories of Shock* 1. Cardiogenic Shock Results from failure of the heart to adequately pump blood; ie cardiac output is decreased. Can occur with a variety of heart diseases. o Eg: myocardial infarction, ventricular tachycardia, arrhythmias, cardiomyopathy, or an obstruction of the flow of blood from the heart 2. Hypovolemic Shock Results from decreased circulating blood volume. Can be due to blood loss from hemorrhage (internal or external) or fluid loss (dehydration) secondary to vomiting, diarrhea or burns. 3. Blood Maldistribution (Vasogenic shock) See a decrease in peripheral vascular resistance and resultant pooling of blood in peripheral tissues. Many causes, including neural or cytokine induced vasodilation, trauma, systemic hypersensitivity to allergens (anaphylaxis) or endotoxemia. Three main causes: o Anaphylactic Shock - vasodilation due to release of vasoactive amines. o Neurogenic Shock - vasodilation due to loss of the autonomic nervous system signals to the smooth muscle in vessel walls. o Septic Shock*- vasodilation due to release of inflammatory mediators associated with overwhelming infections (especially Gram negative bacteria) o Pathogenesis of Septic Shock o Inflammatory cells have a number of receptors (Toll-like receptors) that respond to a variety of substances (such as endotoxin = lipopolysaccharide) derived from microbes. o When microbial components (eg LPS) bind to a WBC surface receptors WBCs release cytokines activation/injury of endothelial cells vasodilation, coagulation cascade ( DIC), complement activation, etc.
11 Three Stages of Shock* 1. Nonprogressive (compensated) shock Reflex compensatory mechanisms are activated and perfusion of vital organs is maintained (eg increased heart rate, peripheral vasoconstriction, etc). 2. Progressive shock Characterized by tissue hypoperfusion and onset of worsening circulatory and metabolic imbalances, including acidosis. 3. Irreversible shock Sets in after the body has incurred cellular and tissue injury so severe that even if the hemodynamic defects are corrected, survival is not possible. Lesions of Shock Shock is characterized by failure of multiple organ systems: Pulmonary congestion and edema Liver congestion Kidneys: Acute tubular necrosis. Heart: Subendocardial hemorrhage and myocardial necrosis. Blood vessels: Endothelial damage with possible thrombosis / DIC. Brain: Neuronal cell death. Adrenal glands: Hemorrhage. Gastrointestinal tract: Mucosal congestion and necrosis. Skeletal muscle: Pallor (probably due to peripheral vasoconstriction). HEMOSTASIS Hemostasis refers to the arrest of bleeding. Normally it s a well-regulated process which maintains blood in a fluid, clot-free state within a normal vessel.* Rapid clot formation (hemostatic plug) will occur at the site of vessel injury. Thrombosis can be considered an inappropriate activation of the normal hemostatic processes. Three general components are required for hemostasis and thrombosis:* o Endothelial cells (vascular wall) o Platelets o Coagulation Cascade Normal Hemostasis = Sequence of events following vascular injury:* 1. Arteriolar vasoconstriction Transient effect mediated by the ENDOTHELIUM Due to reflex neurogenic mechanism and local secretion of endothelin. 2. Primary hemostasis Mediated by PLATELETS
12 Damage to the endothelium exposes the subendothelial ECM (extracellular matrix). Causes platelets to react: I. Adhere to the ECM (adhesion) and change shape (from round discs to flat plates) II. Secretion of granules III. Recruit other platelets to the site and aggregate forming a primary hemostatic plug Primary hemostatic plug: o Covers and seals the small area of vascular damage o If injury is minimal, the platelet plug may be adequate o If injury is more severe, secondary hemostasis occurs 3. Secondary hemostasis Mediated by the COAGULATION CASCADE Tissue factor (TF) o A membrane-bound procoagulant factor is exposed at the site of injury (damaged endothelium) which initiates the coagulation cascade (culminating in thrombin formation). Platelets o Exposed phospholipid complexes on platelets provide sites for coagulation reactions; helps localize the coagulation process. Thrombin activation o Thrombin converts fibrinogen (soluble) to fibrin monomers. Fibrin polymerization / stabilization o Fibrin monomers polymerize into an insoluble gel called fibrin which cements & anchors the primary platelet aggregate forming the 2 o hemostatic plug. 4. Antithrombotic Counter-Regulation Release of components to limit the size of hemostatic plug. ROLE OF ENDOTHELIAL CELLS IN HEMOSTASIS Injury to the endothelium is the major initiating event for thrombosis and coagulation. The endothelium modulates many aspects of normal hemostasis. o Provides a surface that promotes the smooth, laminar (non-turbulent) flow of blood ( antithrombotic property). o When required it can also enhance vasodilation and inhibit platelet adhesion, aggregation and coagulation ( antithrombotic property). o When necessary it produces and responds to substances to form a thrombus or blood clot ( prothrombotic property). Antithrombotic Properties of Endothelial Cells* 1. Antiplatelet Acts as a barrier - prevent platelets and plasma factors from being exposed to subendothelial extracellular matrix. Prostacyclin & nitric oxide (NO) - inhibit platelet adhesion / aggregation and maintains vascular relaxation. Adenosine diphosphatase (ADPase) - degrades ADP (ADP promotes platelet aggregation).
13 2. Anticoagulant properties Heparin-like molecules o Are membrane binding sites for antithrombin III inactivates thrombin + clotting factors Thrombomodulin o Thrombomodulin binds to thrombin converting it to an anticoagulant which can activate Protein C. Active Protein C (with Protein S) cleaves / inhibits clotting factors. Tissue factor pathway inhibitor (TFPI) o Synthesized and expressed on endothelial cell membrane complexes and inactivates TF and clotting factors. 3. Fibrinolytic properties Tissue plasminogen activator (tpa) o Synthesize tpa activates plasmin (fibrinolytic cascade) removes fibrin from endothelial surfaces. Prothrombotic (Procoagulant) Properties of Endothelial Cells* Endothelial cells may be injured directly or activated by infectious agents (eg bacterial endotoxin), hemodynamic factors, plasma mediators and cytokines. When this happens, prothrombotic factors are expressed.* von Willebrand factor (vwf) o Endothelial cells synthesize, store & release vwf; essential cofactor for platelet binding to collagen and other surfaces Tissue Factor (TF = Factor III = thromboplastin) o Injured endothelial cells are induced to secrete TF which activates the extrinsic coagulation cascade. Plasminogen activator inhibitor (PAI) o Endothelial cells secrete PAI which suppresses fibrinolysis (via counteracting tpa). ROLE OF PLATELETS IN HEMOSTASIS* Derived from megakaryocytes; circulate as round, smooth discs with glycoprotein receptors. o Platelets are also referred to as thrombocytes Play a central role in normal hemostasis. o Major role is to form the initial (1 o hemostatic) plug that covers and seals a small damaged area. o Contain mostly procoagulant (& few anticoagulant) mediators in their granules or at other cell sites. Platelet Response Vascular injury exposes extracellular matrix (ECM); especially collagen, which is normally hidden by the intact endothelium. This stimulates a 3 step reaction by platelets. Platelets + ECM 3 step formation of the primary hemostatic plug:**
14 1. Adhesion and shape change Adhesion mediated via interactions with vwf acts as bridge for platelet surface receptors and ECM. 2. Secretion of granules Release of dense granules is important because Ca 2+ is required for coagulation cascade and adenosine diphosphate (ADP) is an important mediator of platelet aggregation. Leads to surface expression of phospholipid complexes (binding site for Ca 2+ & coagulation factors) 3. Recruitment and Aggregation Thromboxane A 2 (TxA 2 ) and ADP secreted by platelets; induces vasoconstriction & platelet aggregation enlarging platelet aggregation = 1 o hemostatic plug. Platelet Defects* 1. Thrombocytopenia* Definition: Circulating platelet numbers are decreased when compared to normal reference ranges (<200 x 10 9 /L is thrombocytopenia in most species; horses <100 x 109/L). Diagnosis History of bleeding and low platelet counts Mechanisms Deficient formation of platelets (eg estrogen toxicity suppresses marrow production) Excessive utilization of platelets (eg consumptive coagulopathies) Premature destruction of platelets (eg antibodies to platelets) 2. Thrombocytopathy* Definition: Defective platelet function. Diagnosis History of bleeding with normal platelet counts, but abnormal platelet function tests Mechanisms Defect in adhesion (eg von Willebrand s disease) Defect in aggregation Defect in release of granules Both thrombocytopenia and thrombocytopathy result in small foci of hemorrhage* ROLE OF THE COAGULATION CASCADE IN HEMOSTASIS The coagulation cascade is the third arm in the hemostatic process and is an amplifying series of enzymatic conversions. An enzyme (activated coagulation factor) + a substrate (non-activate coagulation factor) newly activated coagulation factor. Reactions are assembled on a phospholipid complex (platelets) which is held together by calcium ions.
15 The cascade culminates in the production of thrombin (bound to platelet surface) thrombin converts soluble fibrinogen to fibrin which stabilizes the hemostatic plug.* Generation of thrombin is the most important factor in the progression and stabilization of the clot (thrombus)*. In the classic model of coagulation, thrombin can be generated at the site of injury by either the intrinsic or extrinsic coagulation pathway, both which converge where factor X is activated common coagulation pathway. 1. Intrinsic Coagulation Pathway All factors of the intrinsic system (factors XII, XI, IX, and VIII) are present in normal plasma; the cascade is activated by contact of factor XII (Hageman factor) with the subendothelial collagen (ECM) following vascular damage. 2. Extrinsic Coagulation Pathway Tissue factor (TF = Factor III = thromboplastin) is a cell surface protein on injured endothelial cells that interacts with circulating factor VII to initiate the extrinsic pathway. 3. Common Pathway Activated factor X (Xa) is produced by proteolysis of Factor X, which occurs at the end of both the intrinsic & extrinsic coagulation pathways. Calcium and platelet surface phospholipids are necessary for factor Xa to be activated. Xa converts prothrombin to thrombin (factor II IIa). o Thrombin cleaves peptides from plasma fibrinogen (factor 1, which is soluble) to form fibrin monomers (factor 1a). Monomers self-polymerize into larger fibrin polymers (insoluble); then are cross-linked/stabilized by factor XIIIa. Contraction of fibrin-platelet thrombus reduced size of thrombus (restore blood flow) and draws damaged vessels edges closer (for healing). Cell based model of coagulation. An alternative model or coagulation breaks this process into 3 phases: Initiation, Amplification, and Propagation. The end result is the same. Coagulation Disorders* Coagulation disorders can be inherited or acquired In general, large hematomas (in the absence of trauma or other disease processes) suggest a coagulation disorder whereas petechial or ecchymotic hemorrhage on a mucosal surface may indicate a platelet deficiency or abnormality. Inherited Deficiencies of Coagulation Numerous (see PowerPoint slide - for your information only) Acquired Deficiencies of Coagulation* Can be due to decreased production of coagulation factors: o Accompany many severe diseases: As a transitory depression of factor synthesis o Many factors may be affected
16 Liver failure causes a general decrease in production (most coagulation factors are produced in the liver) o Can be more specific: Vitamin K deficiency causes a more specific decrease in production Factors II, VII, IX, X (and protein C and S) are vitamin K dependent Can be due to increased use (ie consumptive coagulopathy): o Accompany many severe diseases: Disseminated intravascular coagulation (DIC)* Severe trauma or deep burns Sepsis FIBRINOLYTIC SYSTEM / ANTICOAGULATION Coagulation must be restricted to the site of vascular injury to prevent extensive clotting away from the site. See previous discussion of "Antithrombotic Properties of Endothelial Cells". Fibrinolytic cascade limits the size and/or dissolves the thrombus (which is supposed to be a temporary patch).* o Primarily by the activation of circulating inactive precursor plasminogen* Plasminogen is activated by tissue plasminogen activator (tpa) and the coagulation pathway (XIIa-kallikrein). o Plasminogen once activated plasmin Plasmin breaks down fibrin and fibrinogen (and some clotting factors and plasma proteins) dissolving the hemostatic plug.* Fibrin degradation products (FDPs) have anticoagulant activity and can be used as a measure of thrombotic states.* HEMORRHAGE* Definition: Escape of blood from the cardiovascular system (extravasation). Can be discharge of blood from the vascular compartment to the exterior of the body or enclosed within a tissue or body cavity. Causes of Hemorrhage 1. Trauma Causes subcutaneous, body cavity, intramuscular or tissue hemorrhage. 2. Septicemia, viremia or toxic conditions widespread petechiae and ecchymoses. 3. Abdominal neoplasia rupture of masses can cause hemoperitoneum. 4. Coagulation Disorders often causes large hemorrhages. 5. Thrombocytopenia (decreased numbers of platelets) often causes small mucosal hemorrhages. 6. Severe congestion can cause capillary bleeding.
17 Outcome / Significance of Hemorrhage Depends on: 1) Location: There are two critical sites: a. Central nervous system (CNS): Subdural (or epidural) hematomas Blood accumulation beneath (or above) the dura; can compress brain b. Heart: Cardiac Tamponade due to hemopericardium Acute right heart failure due to massive blood accumulation within the pericardial sac causing restriction of diastolic cardiac filling compressive effect. 2) Rate and Volume of Blood Loss a. High rates and volumes are worse Can cause anemia and inadequate oxygenation of tissues With rapid severe blood loss (more than 1/3 of the volume lost over minutes-hours), can lead to hemorrhagic shock (hypovolemic shock). TERMINOLOGY OF HEMORRHAGE Cardiac Tamponade Acute right heart failure due to massive blood accumulation within the pericardial sac causing restriction of diastolic cardiac filling Hemorrhage by Rhexis Hemorrhage due to a substantial tear (rip / rent) in a blood vessel or heart. o Occurs with trauma, necrosis of the vessel wall, vascular invasion by neoplasia, etc o Moderate / marked flow of blood out of vascular system. Tends to result in massive or submassive hemorrhage involving all or most of the affected organ or body cavity or hematomas Hemorrhage by Diapedesis Hemorrhage due to small defect o RBCs passing through the vessel wall in inflammation or with congestion. Can also occur with hypoxia, toxic injury, and with coagulation abnormalities. o Hemorrhage is usually mild. o Tends to result in petechiae, purpura, ecchymoses, and paint brush hemorrhages (see definitions below) Hemorrhagic Diathesis = Increased tendency to hemorrhage from usually insignificant injuries. Seen in a wide variety of clinical disorders (eg coagulation deficiency / platelet disorders). Hematoma = Accumulation of blood in tissue (3 dimensional extravascular clot); may be small or very large. Hemopericardium = Blood in the pericardial sac. Hemothorax = Blood in the pleural cavity.
18 Hemoperitoneum = Blood in the peritoneal cavity. Hemarthrosis = Blood in a joint space. Hemoptysis = Coughing up of blood from the lungs or airways. Epistaxis = Bleeding from the nose. Hematemesis = Vomiting up blood. Hematochezia = Presence of (fresh) blood in the stool. Melena = Presence of tarry (digested) blood in the stool. Petechia (pl. petechiae) = Small, up to 1-2 mm, hemorrhages; most often occur on skin, mucosal / serosal surfaces. Often caused by platelet disorders Purpura = Hemorrhages measuring 3 mm to 1 cm; most often occur on skin, mucosal / serosal surfaces. Often seen with diseases that cause petechiae (platelet disorders) but also with vasculitis / blood vessel damage. Ecchymosis (pl. ecchymoses) = Hemorrhages larger than petechiae & purpura (>1 cm). Often blotchy or irregular, as seen in bruises (contusions). Occur with vasculitis / moderate blood vessel damage. Paint Brush Hemorrhages = Hemorrhages which look as though red paint was hastily applied with a paint brush; most commonly found on serosal or mucosal surfaces. Suffusive Hemorrhage = Affected areas of hemorrhage are larger than ecchymosis and are contiguous. Agonal Hemorrhages = Small hemorrhages (petechiae and ecchymoses) associated with the death struggle (ie terminal hypoxia). RESOLUTION OF HEMORRHAGE Arrest of hemorrhage occurs as a result of hemostasis (covered in the next lecture) Resolution depends on amount of hemorrhage: Resorption Small amount of hemorrhage can be resorbed. Organization Larger amounts of hemorrhage require phagocytosis and degradation by macrophages. Pigments from degraded hemoglobin form sequentially:
19 Hemoglobin Bilirubin Hemosiderin (red-blue) (blue-green) (yellow-brown) Organizing hematoma: Central mass of fibrin and RBCs surrounded by vascularized connective tissue (supplies nutrients and support) Macrophages phagocytize and degrade the fibrin and RBCs (see pigment from degraded hemoglobin) THROMBOSIS* Terminology Thrombosis o Inappropriate activation (occurring in uninjured or mildly injured vessels) of the hemostatic process resulting in the formation or presence of a solid mass (thrombus) within the blood vessels or heart. Thrombus (pl. thrombi) o Aggregate of blood factors, primarily platelets & fibrin, with entrapment of cellular elements (RBCs/WBCs) causing partial or complete vascular obstruction. o Often adherent to the vessel wall (differentiates it from a post-mortem blood clot). Pathogenesis of Thrombosis: Three primary influences favour thrombosis = Virchow's triad. 1. Endothelial injury Dominant influence = can lead to thrombosis by itself. Eg Inflammation of heart valves (endocarditis) exposure of the subendothelial ECM platelet adherence / release of tissue factor primary and secondary hemostatic plug formation thrombosis. 2. Alterations in normal blood flow Normal blood flow is laminar with the cellular elements in the middle of the vessel lumen and surrounded by plasma. With turbulence or stasis disruption of normal laminar flow allows platelets to contact endothelium: o Turbulence also promotes endothelial cell injury / activation o Stasis also prevents dilution of activated clotting factors by fresh-flowing blood and allows the build-up of thrombi (causes hypercoagulability). 3. Hypercoagulability Definition = any alteration of the coagulation pathways that predisposes to thrombosis. Due to: o Increased prothrombotic factors (eg with sepsis) o Decreased inhibitory factors (eg loss of antithrombin III with glomerular disease).
20 Locations for thrombi Thrombi may develop anywhere in cardiovascular system: on the valves, in the cardiac chambers or within the lumina of arteries, veins and capillaries. Thrombi grow towards the heart (ie, arterial thrombi grow against blood flow, while venous thrombi grow with blood flow). Pieces of a thrombus can break off and travel downstream forming emboli. Arterial thrombi o Arterial thrombi usually form at sites of endothelial injury or turbulence. o Grow towards the heart (according to most sources). o Often paler & "meatier" than venous thrombi. Composed mainly of platelets & fibrin, because rapid blood flow tends to exclude RBCs. o Can have alternating dark and pale laminations called lines of Zahn: Reflects continued waves of thrombosis: pale layers (mostly fibrin / platelets) alternating with dark red layers (more entrapped RBCs). Venous thrombi o Grow towards the heart. o Usually form in static (slow flow) environment. o Contain more entrapped RBCs and therefore are more uniformly dark red. o Attachment to wall is often focal and loose which can make it difficult to differentiate from a postmortem blood clot. Blood Clot = Clotted blood within a blood vessel (blood clot can refer to thrombus or postmortem blood clot, so be specific). Post-mortem blood clots are not associated with a pathological condition and are not attached to the vessel wall. A thrombus and a post-mortem blood clot can look very similar. Chicken-Fat Clot = Common gelatinous, yellow, post-mortem blood clot seen at necropsy (especially horses). Plasma clot that develops because of rapid erythrocyte sedimentation in animals with high fibrinogen. Yellow areas represent fibrin and plasma and dark red areas at the margins represent sedimented RBCs. Morphological Differentiation of Thrombi and Post-Mortem Clots Arterial Thrombus Venous Thrombus Postmortem Clot Colour Pale to dark red Red Yellow or red Lamination Yes Not frequent No Attachment Yes Focal / loose (can be difficult to detect) No Size Often small Often fill lumen Fill lumen
21 Outcome of Thrombi 1. Lysis (dissolution) Especially when thrombi are small and in the early phases due to potent thrombolytic / fibrinolytic activity of blood. 2. Propagation An increase in size of the thrombus may eventually occlude the vessel. 3. Embolization Can occur if pieces (thromboemboli) break off the thrombus and travel downstream. 4. Organization and recanalization The presence of a thrombus induces inflammation and fibrosis (organization); the latter reduces the size of the thrombus. New small blood vessels can penetrate / grow within the organizing thrombus (recanalization). Both of the above aid in the restoration of blood flow. EMBOLISM* Terminology of Embolism* Embolism = Passage through the venous or arterial circulation of any material capable of lodging in a blood vessel and thereby obstructing the lumen. o Most common form of embolism is thromboembolism: piece(s) broken off of a thrombus. Embolus (pl. emboli) = Detached intravascular material (solid, liquid, or gaseous) carried via the blood to a site distant from its origin. Thromboembolism = Occlusion of a blood vessel by an embolus that has broken away from a thrombus. o Localizes at point where it can no longer "fit" through. Thromboembolus (pl. thromboemboli) o The piece of thrombotic material transported in the bloodstream to another site. Composition of Emboli Remember that most emboli are thromboemboli, however many other types exist: o Parasites Nematodes - Dirofilaria immitis (heartworm) Nematode larvae - Ascarid or Strongyle larvae o Fibrocartilaginous emboli Originate from intervertebral disk material (traumatic implantation into spinal vessels)
22 Causes necrotizing myelopathy (spinal cord infarction) o Fat (or bone marrow) Can originate from several sources: Eg bone fractures, surgery, osteomyelitis, hyperlipidemia. o Other Foreign material (air bubbles, hair, etc), tumour cell clusters ("tumor emboli"), amniotic fluid Infectious causes of thrombosis or thromboembolism* Infectious agents can damage endothelium, thereby causing thrombosis and/or thromboembolism: o Many bacteria can cause valvular endocarditis with resultant thrombosis and thromboembolism. o Several viral agents can damage endothelium leading to thrombosis. DISSEMINATED INTRAVASCULAR COAGULATION (DIC)* DIC = The sudden or insidious onset of widespread fibrin thrombi in the microcirculation. o These thrombi are not visible on gross inspection but are readily apparent microscopically. o Can cause diffuse circulatory insufficiency, particularly in the brain, lungs, heart, and kidneys. o With the development of the multiple thrombi, there is a rapid consumption of platelets and coagulation proteins o In addition fibrinolytic mechanisms are activated, thus an initial thrombotic disorder can evolve into a serious bleeding disorder (hence the term consumptive coagulopathy). o Note: DIC is not a primary disease but rather a potential complication of any condition associated with widespread activation of thrombin. o Some causes of DIC include: severe burns, heatstroke, systemic viral disease, shock, toxemia, sepsis, neoplasia, pancreatitis, heartworm disease (dogs), etc. INFARCTION* Infarct = an area of ischemic necrosis caused by occlusion of either the arterial supply or the venous drainage. Most infarcts result from thrombotic or embolic events or vascular occlusion due to compression of a vessel (eg intestinal volvulus, testicular torsion, etc). 40% of all human deaths in N. Am. are due to cardiovascular disease, mostly from myocardial or cerebral infarction; whereas pulmonary, intestinal and renal infarction are more common in domestic animals.
23 Factors that Influence the Development / Characteristics of an Infarct 1. Nature of the vascular supply. Tissues with a single blood supply (egs kidney, brain, heart, spleen) are more prone to infarction than those with dual or collateral blood supply (egs lung, liver, intestine, skeletal muscle). 2. Rate of development of occlusion of the vessel. If slow, allows time for the collateral supply to fully open. 3. Vulnerability to hypoxia. Certain cell/tissue types are more vulnerable to ischemic damage (especially the brain and heart). 4. Oxygen content of blood at time of infarct. Underlying anemia would increase the likelihood of ischemia resulting in infarction. Gross appearance of an infarct Often wedge-shaped, with the base at the periphery and the occluded vessel at the apex. Early they are ill defined (+/- irregular margins) and often hyperemic. Later (by 48 hours) most become pale. 1. Red Infarct Due to the presence of blood in the infarcted region (also called hemorrhagic infarct). o Occurs in some acute infarcts due to RBCs leaking in from adjacent arteries and veins (eventually the RBCs lyse pale). o In venous occlusions, where blood is prevented from draining from the organ (eg volvulus, strangulations); called a venous infarct. o Also occurs in organs with dual blood supply (eg lung, liver) or where blood collects in loose tissue. 2. White Infarct Lack of blood in the infarct (also called pale or anemic infarct). o Mostly occurs with arterial occlusions in solid organs with end arterial circulation (eg heart, kidney). Usually has a red zone at periphery because the capillaries at the border of infarct undergo dissolution and blood seeps into this marginal area. Histopathology of an Infarct Ischemic necrosis of affected parenchyma: o Discrete areas of coagulative necrosis (+/- hemorrhage) in all tissues except brain where liquefactive necrosis will occur o Peripheral rim of inflammation and hemorrhage. o Infarcts arising from septic (bacterially infected) emboli may be converted to an abscess with time. Repair of Infarcts Fibrous connective tissue (scar tissue) replaces necrotic parenchyma. As fibrous tissue matures and condenses (contracts), it forms a depression / indentation on the organ surface.
24 Septic Infarct Develop from a bacterially infected thromboembolus or when the necrotic tissue of an infarct is seeded by bacteria (necrotic tissue is a good growth medium for these pathogenic organisms). Venous Infarct Severe venous obstruction can cause venous infarction. Mostly due to twisting of vessels (eg intestinal volvulus / torsion / strangulation) shock / death. Also seen with obstruction (eg thrombosis or tumor invasion) of the cranial or caudal vena cava o Often obstruction is incomplete causing slowly developing stasis with engorgement of the tributary veins. Important examples of venous obstruction/infarction Acute Blockage of the Portal Venous System o Mostly with twists in portions of GI tract / portal venous system venous infarction of stomach or intestine; twisted vessels are compressed, but because arterial pressure > venous pressure blood enters the tissue but cannot leave. Sequelae: shock and death unless corrected with surgery. Eg: gastric torsion (dogs) obstruction of gastric portion of portal vein severe venous congestion vascular stasis ischemic necrosis (infarction) loss of endothelial integrity hemorrhage shock. Blockage of the posterior vena cava o Possible etiologies: Severe dirofilariasis (heartworm) or adrenal tumors in dogs Hepatic abscesses in ruminants. o Possible result: Acute and complete occlusion death. Chronic occlusion possibility of collateral circulation developing from azygous vein. Important example of arterial blockage / infarction Pulmonary Artery Thrombosis / Thromboembolism o Thrombosis / thromboembolism of the pulmonary artery can be due to a variety of causes, eg pneumonia, parasite infestations (eg heartworm), hypercoagulability (eg hyperadrenocorticism, nephrotic syndrome), liver abscess rupture into the vena cava with subsequent thromboembolism to the lungs, etc o Possible result: If acute and involves large branch of artery death. If incomplete and smaller branches variably altered circulation or possibly pulmonary infarcts.
Circulatory Disturbances 5: Thrombosis, Embolism, Infarction, Shock
 Circulatory Disturbances 5: Thrombosis, Embolism, Infarction, Shock Shannon Martinson, Feb 2016 http://people.upei.ca/smartinson/ VPM 152 General Pathology Thrombosis, Embolism, Infarction, Shock Learning
Circulatory Disturbances 5: Thrombosis, Embolism, Infarction, Shock Shannon Martinson, Feb 2016 http://people.upei.ca/smartinson/ VPM 152 General Pathology Thrombosis, Embolism, Infarction, Shock Learning
HYPEREMIA AND CONGESTION
 HYPEREMIA AND CONGESTION Learning Objectives Define congestion and hyperemia Differentiate between the two with regard to: Mechanisms / underlying causes Appearance (gross and histologic) Effects Differentiate
HYPEREMIA AND CONGESTION Learning Objectives Define congestion and hyperemia Differentiate between the two with regard to: Mechanisms / underlying causes Appearance (gross and histologic) Effects Differentiate
EDEMA. Learning Objectives
 EDEMA Learning Objectives Define edema Recognize and be able to describe the gross and microscopic appearance of edema Know the four pathophysiological mechanisms by which edema develops Understand the
EDEMA Learning Objectives Define edema Recognize and be able to describe the gross and microscopic appearance of edema Know the four pathophysiological mechanisms by which edema develops Understand the
Circulatory Disturbances 1: Introduction and Edema
 Circulatory Disturbances 1: Introduction and Edema Shannon Martinson, January 2016 http://people.upei.ca/smartinson/ VPM 152 General Pathology INTRODUCTION NORMAL CIRCULATORY SYSTEM Important concepts
Circulatory Disturbances 1: Introduction and Edema Shannon Martinson, January 2016 http://people.upei.ca/smartinson/ VPM 152 General Pathology INTRODUCTION NORMAL CIRCULATORY SYSTEM Important concepts
HEMODYNAMIC DISORDERS
 HEMODYNAMIC DISORDERS Normal fluid homeostasis requires vessel wall integrity as well as maintenance of intravascular pressure and osmolarity within certain physiologic ranges. Increases in vascular volume
HEMODYNAMIC DISORDERS Normal fluid homeostasis requires vessel wall integrity as well as maintenance of intravascular pressure and osmolarity within certain physiologic ranges. Increases in vascular volume
Hemodynamic Disorders, Thrombosis, and Shock. Richard A. McPherson, M.D.
 Hemodynamic Disorders, Thrombosis, and Shock Richard A. McPherson, M.D. Edema The accumulation of abnormal amounts of fluid in intercellular spaces of body cavities. Inflammation and release of mediators
Hemodynamic Disorders, Thrombosis, and Shock Richard A. McPherson, M.D. Edema The accumulation of abnormal amounts of fluid in intercellular spaces of body cavities. Inflammation and release of mediators
General Pathology. Hemorrhage (Web)
 General Pathology Hemorrhage (Web) Paul Hanna Feb 2015 Hemorrhage escape of blood from the cardiovascular system may be external or internal Hemorrhage Causes Trauma Sepsis, viruses or toxins Coagulation
General Pathology Hemorrhage (Web) Paul Hanna Feb 2015 Hemorrhage escape of blood from the cardiovascular system may be external or internal Hemorrhage Causes Trauma Sepsis, viruses or toxins Coagulation
Hemodynamic Disorders Thrombosis and Shock. 1. Interstitial, between the cells, but outside of the vascular system. - water making up the blood and
 Hemodynamic Disorders Thrombosis and Shock I. Body water, where is it and what keeps it there? A. Intracellular B. Extracellular (intercellular) 1. Interstitial, between the cells, but outside of the vascular
Hemodynamic Disorders Thrombosis and Shock I. Body water, where is it and what keeps it there? A. Intracellular B. Extracellular (intercellular) 1. Interstitial, between the cells, but outside of the vascular
Disturbance of Circulation Hemodynamic Disorder
 Disturbance of Circulation Hemodynamic Disorder 2/17/2017 By Dr. Hemn Hassan Othman PhD, Pathology Fall 2016 1 Thrombosis Definition: Thrombosis is the formation of solid or semisolid blood clot within
Disturbance of Circulation Hemodynamic Disorder 2/17/2017 By Dr. Hemn Hassan Othman PhD, Pathology Fall 2016 1 Thrombosis Definition: Thrombosis is the formation of solid or semisolid blood clot within
Hemodynamic Disorders, Thromboembolic Disease, and Shock
 Hemodynamic Disorders, Thromboembolic Disease, and Shock Kumar et al: Robbins & Cotran Pathologic Basis of Disease 7E Figure 4-1 Factors affecting fluid balance across capillary walls. Capillary hydrostatic
Hemodynamic Disorders, Thromboembolic Disease, and Shock Kumar et al: Robbins & Cotran Pathologic Basis of Disease 7E Figure 4-1 Factors affecting fluid balance across capillary walls. Capillary hydrostatic
Shock, Hemorrhage and Thrombosis
 Shock, Hemorrhage and Thrombosis 1 Shock Systemic hypoperfusion due to: Reduction in cardiac output Reduction in effective circulating blood volume Hypotension Impaired tissue perfusion Cellular hypoxia
Shock, Hemorrhage and Thrombosis 1 Shock Systemic hypoperfusion due to: Reduction in cardiac output Reduction in effective circulating blood volume Hypotension Impaired tissue perfusion Cellular hypoxia
5 DISTURBANCES IN CIRCULATION. Congestion / Hyperemia Haemorrhage Thrombosis Embolism Ischemia Infarction Oedema Shock Sludged blood Model Questions
 5 DISTURBANCES IN CIRCULATION Congestion / Hyperemia Haemorrhage Thrombosis Embolism Ischemia Infarction Oedema Shock Sludged blood Model Questions CONGESTION/ HYPEREMIA Hyperemia is increased amount of
5 DISTURBANCES IN CIRCULATION Congestion / Hyperemia Haemorrhage Thrombosis Embolism Ischemia Infarction Oedema Shock Sludged blood Model Questions CONGESTION/ HYPEREMIA Hyperemia is increased amount of
CIRCULATORY DISTURBANCES
 CIRCULATORY DISTURBANCES Shannon Martinson, January 2016 Email: smartinson@upei.ca All lecture notes and slide shows are available online: http://people.upei.ca/smartinson Office: 418N REFERENCE TEXTS:
CIRCULATORY DISTURBANCES Shannon Martinson, January 2016 Email: smartinson@upei.ca All lecture notes and slide shows are available online: http://people.upei.ca/smartinson Office: 418N REFERENCE TEXTS:
Disturbances of Circulation, Lab 1: Edema and Congestion/Hyperemia. Shannon Martinson, Feb
 Disturbances of Circulation, Lab 1: Edema and Congestion/Hyperemia Shannon Martinson, Feb 2017 http://people.upei.ca/smartinson/ Case #1 Signalment and History: 6-month old feeder lamb found dead on pasture
Disturbances of Circulation, Lab 1: Edema and Congestion/Hyperemia Shannon Martinson, Feb 2017 http://people.upei.ca/smartinson/ Case #1 Signalment and History: 6-month old feeder lamb found dead on pasture
Hemodynamic derangement. Komson Wannasai, M.D.,FRCPath. Department of Pathology Faculty of Medicine Chiang Mai University
 Hemodynamic derangement Komson Wannasai, M.D.,FRCPath. Department of Pathology Faculty of Medicine Chiang Mai University Objective The students should be able to Explain normal body fluid homeostasis Explain
Hemodynamic derangement Komson Wannasai, M.D.,FRCPath. Department of Pathology Faculty of Medicine Chiang Mai University Objective The students should be able to Explain normal body fluid homeostasis Explain
Hemodynamic Disorders Thrombosis and Shock
 Hemodynamic Disorders Thrombosis and Shock SCPA 202 Basic Pathology Somphong Narkpinit, M.D. Department of Pathobiology, Faculty of Science, Mahidol University Email : somphong.nar@mahidol.ac.th Hemodynamic
Hemodynamic Disorders Thrombosis and Shock SCPA 202 Basic Pathology Somphong Narkpinit, M.D. Department of Pathobiology, Faculty of Science, Mahidol University Email : somphong.nar@mahidol.ac.th Hemodynamic
According to the etiology, edema may be:
 What is edema? Edema : It refers to the accumulation of excess liquid in the interstitial (extracellular) spaces of a tissue or in pre-existing cavities. It may affect any organ, but most often it appears
What is edema? Edema : It refers to the accumulation of excess liquid in the interstitial (extracellular) spaces of a tissue or in pre-existing cavities. It may affect any organ, but most often it appears
This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion
 This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms
This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms
Hyperemia, Congestion, and Edema
 Hyperemia, Congestion, and Edema Hyperemia Acute, actively increased blood flow Tissues look red (erythema) Congestion Chronic, passively reduced outflow Tissues look pale or blue (cyanosis) Edema Water
Hyperemia, Congestion, and Edema Hyperemia Acute, actively increased blood flow Tissues look red (erythema) Congestion Chronic, passively reduced outflow Tissues look pale or blue (cyanosis) Edema Water
UNIT VI. Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav. Copyright 2011 by Saunders, an imprint of Elsevier Inc.
 UNIT VI Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav Hemostasis: Prevention of Blood Loss Vascular constriction Formation of a platelet plug Formation of a blood
UNIT VI Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav Hemostasis: Prevention of Blood Loss Vascular constriction Formation of a platelet plug Formation of a blood
Bachelor of Chinese Medicine Shock
 BCM Year 2 Dr. Irene Ng Jan 28, 2003 9:30 am 1:00 pm Rm 004 UPB Bachelor of Chinese Medicine 2002 2003 Shock Learning objectives Be able to: know the definition of shock know the classification and causes
BCM Year 2 Dr. Irene Ng Jan 28, 2003 9:30 am 1:00 pm Rm 004 UPB Bachelor of Chinese Medicine 2002 2003 Shock Learning objectives Be able to: know the definition of shock know the classification and causes
Part IV Antithrombotics, Anticoagulants and Fibrinolytics
 Part IV Antithrombotics, Anticoagulants and Fibrinolytics "The meaning of good and bad, of better and worse, is simply helping or hurting" Emerson Chapter 16: Blood Coagulation and Fibrinolytic System
Part IV Antithrombotics, Anticoagulants and Fibrinolytics "The meaning of good and bad, of better and worse, is simply helping or hurting" Emerson Chapter 16: Blood Coagulation and Fibrinolytic System
Ischaemia It means local anemia, it is characterized by a decrease amount of blood in an organ or region. Causes of Ischemia: *1.
 المرحلة الثالثة م. هالة عباس ناجي Ischaemia It means local anemia, it is characterized by a decrease amount of blood in an organ or region. Causes of Ischemia: *1.External pressure upon an artery e.g:
المرحلة الثالثة م. هالة عباس ناجي Ischaemia It means local anemia, it is characterized by a decrease amount of blood in an organ or region. Causes of Ischemia: *1.External pressure upon an artery e.g:
Thrombosis and emboli. Peter Nagy
 Thrombosis and emboli Peter Nagy A thrombus is any solid object developing from the blood in vivo within the vascular system or heart. Thrombosis is hemostasis in the wrong place. Major components, forms:
Thrombosis and emboli Peter Nagy A thrombus is any solid object developing from the blood in vivo within the vascular system or heart. Thrombosis is hemostasis in the wrong place. Major components, forms:
Pathophysiology. Tutorial 3 Hemodynamic Disorders
 Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
Hemostasis and Thrombosis
 Hemostasis Hemostasis and Thrombosis Normal hemostasis is a consequence of tightly regulated processes that maintain blood in a fluid state in normal vessels, yet also permit the rapid formation of a hemostatic
Hemostasis Hemostasis and Thrombosis Normal hemostasis is a consequence of tightly regulated processes that maintain blood in a fluid state in normal vessels, yet also permit the rapid formation of a hemostatic
ATHEROSCLEROSIS. Secondary changes are found in other coats of the vessel wall.
 ATHEROSCLEROSIS Atherosclerosis Atherosclerosis is a disease process affecting the intima of the aorta and large and medium arteries, taking the form of focal thickening or plaques of fibrous tissue and
ATHEROSCLEROSIS Atherosclerosis Atherosclerosis is a disease process affecting the intima of the aorta and large and medium arteries, taking the form of focal thickening or plaques of fibrous tissue and
Chapter 19. Hemostasis
 Chapter 19 Hemostasis Hemostasis Hemostasis is the cessation of bleeding stopping potentially fatal leaks important in small blood vessels not effective in hemorrhage excessive bleeding from large blood
Chapter 19 Hemostasis Hemostasis Hemostasis is the cessation of bleeding stopping potentially fatal leaks important in small blood vessels not effective in hemorrhage excessive bleeding from large blood
Branch of medicine that deals with blood, its formation and disorders is called. Three main functions of cardiovascular system are,, and.
 Chapter 19 The Blood Human body must maintain a balance called. Body fluid inside the cells is called fluid; that outside is called or fluid. Two major fluid networks that help in connecting cells are
Chapter 19 The Blood Human body must maintain a balance called. Body fluid inside the cells is called fluid; that outside is called or fluid. Two major fluid networks that help in connecting cells are
Topics of today lectures: Hemostasis
 Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms of hemostasis - Vascular contraction - Platelets plug - Blood coagulation (clotting) - Structure and functions of platelets - Blood
Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms of hemostasis - Vascular contraction - Platelets plug - Blood coagulation (clotting) - Structure and functions of platelets - Blood
What are blood clots?
 What are blood clots? Dr Matthew Fay GP Principal The Willows Medical Practice- Queensbury GPwSI and Co-Founder Westcliffe Cardiology Service GP Partner Westcliffe Medical Group Created 5/31/18 Dr. Matthew
What are blood clots? Dr Matthew Fay GP Principal The Willows Medical Practice- Queensbury GPwSI and Co-Founder Westcliffe Cardiology Service GP Partner Westcliffe Medical Group Created 5/31/18 Dr. Matthew
Physiology of. The Blood hemostasis. By prof. Israa f. jaafar
 Physiology of The Blood hemostasis By prof. Israa f. jaafar Learning objectives Understand the Platelet structure and function Explane the Platelet production Understand the phases of hemostasis: vascular
Physiology of The Blood hemostasis By prof. Israa f. jaafar Learning objectives Understand the Platelet structure and function Explane the Platelet production Understand the phases of hemostasis: vascular
Hemostasis and. Blood Coagulation
 Hemostasis and Blood Coagulation Events in Hemostasis The term hemostasis means prevention of blood loss. Whenever a vessel is severed or ruptured, hemostasis is achieved by several mechanisms: (1) vascular
Hemostasis and Blood Coagulation Events in Hemostasis The term hemostasis means prevention of blood loss. Whenever a vessel is severed or ruptured, hemostasis is achieved by several mechanisms: (1) vascular
Chapter 3 Disorder of Local Blood Circulation
 Chapter 3 Disorder of Local Blood Circulation Disorder of Circulation Disorder of vascular flow may be divided into general and local categories. The local disorders contain: 1Derangement of local blood
Chapter 3 Disorder of Local Blood Circulation Disorder of Circulation Disorder of vascular flow may be divided into general and local categories. The local disorders contain: 1Derangement of local blood
Blood Vessels. Chapter 20
 Blood Vessels Chapter 20 Summary of the Characteristics of Arteries and Veins Characteristic Artery Vein Wall thickness thick thin Shape in cross section round flattened Thickest tunic media externa Collagen
Blood Vessels Chapter 20 Summary of the Characteristics of Arteries and Veins Characteristic Artery Vein Wall thickness thick thin Shape in cross section round flattened Thickest tunic media externa Collagen
THROMBOSIS. Dr. Nisreen Abu Shahin Assistant Professor of Pathology Pathology Department University of Jordan
 THROMBOSIS Dr. Nisreen Abu Shahin Assistant Professor of Pathology Pathology Department University of Jordan NORMAL BLOOD VESSEL HISTOLOGY THROMBOSIS Pathogenesis (called Virchow's triad): 1. Endothelial*
THROMBOSIS Dr. Nisreen Abu Shahin Assistant Professor of Pathology Pathology Department University of Jordan NORMAL BLOOD VESSEL HISTOLOGY THROMBOSIS Pathogenesis (called Virchow's triad): 1. Endothelial*
Chapter 4: Haemodynamic disorders, shock
 Chapter 4: Haemodynamic disorders, shock 1. Regarding platelets (2006) (a) They are the main source of thrombin (b) they number 150-300 x10 3 per microlitre (c) They contain a nucleus (d) They are biconcave
Chapter 4: Haemodynamic disorders, shock 1. Regarding platelets (2006) (a) They are the main source of thrombin (b) they number 150-300 x10 3 per microlitre (c) They contain a nucleus (d) They are biconcave
Anatomy and Physiology
 Anatomy and Physiology For The First Class 2 nd Semester Thrombocytes = Platelets Thrombocytes = Platelets Blood platelets are non-nucleated disc like cell fragments 2-4 µm in diameter. Platelets are not
Anatomy and Physiology For The First Class 2 nd Semester Thrombocytes = Platelets Thrombocytes = Platelets Blood platelets are non-nucleated disc like cell fragments 2-4 µm in diameter. Platelets are not
Ch. 45 Blood Plasma proteins, Coagulation and Fibrinolysis Student Learning Outcomes: Describe basic components of plasma
 Chapt. 45 Ch. 45 Blood Plasma proteins, Coagulation and Fibrinolysis Student Learning Outcomes: Describe basic components of plasma Inheritance of X-linked gene for Factor VIII hemophilia A Explain the
Chapt. 45 Ch. 45 Blood Plasma proteins, Coagulation and Fibrinolysis Student Learning Outcomes: Describe basic components of plasma Inheritance of X-linked gene for Factor VIII hemophilia A Explain the
Chapter 11. Lecture and Animation Outline
 Chapter 11 Lecture and Animation Outline To run the animations you must be in Slideshow View. Use the buttons on the animation to play, pause, and turn audio/text on or off. Please Note: Once you have
Chapter 11 Lecture and Animation Outline To run the animations you must be in Slideshow View. Use the buttons on the animation to play, pause, and turn audio/text on or off. Please Note: Once you have
Disorder of Local Blood Circulation. Pathology Department, Zhejiang University School of Medicine,
 Disorder of Local Blood Circulation Pathology Department, Zhejiang University School of Medicine, maliqin198@zju.edu.cn Hyperemia Hemorrhage Thrombosis Embolism Infarction Edema Conception: Disorder of
Disorder of Local Blood Circulation Pathology Department, Zhejiang University School of Medicine, maliqin198@zju.edu.cn Hyperemia Hemorrhage Thrombosis Embolism Infarction Edema Conception: Disorder of
Moath Darweesh. Omar Sami. Saleem Khreisha. 1 P a g e
 7 Moath Darweesh Omar Sami Saleem Khreisha 1 P a g e -First of all, I want to give a quick revision to simplify the whole hemostasis mechanism, it will be much easier here with me. Enjoy (you can skip
7 Moath Darweesh Omar Sami Saleem Khreisha 1 P a g e -First of all, I want to give a quick revision to simplify the whole hemostasis mechanism, it will be much easier here with me. Enjoy (you can skip
Microcirculation. Lecture Block 11 (contributions from Brett Burton)
 Lecture Block 11 (contributions from Brett Burton) Elements of Arterioles, capillaries, venules Structure and function: transport Fluid balance Lymph system Vessels of the Circulatory System Diameter Aorta
Lecture Block 11 (contributions from Brett Burton) Elements of Arterioles, capillaries, venules Structure and function: transport Fluid balance Lymph system Vessels of the Circulatory System Diameter Aorta
Hematology. The Study of blood
 Hematology The Study of blood Average adult = 8-10 pints of blood Composition: PLASMA liquid portion of blood without cellular components Serum plasma after a blood clot is formed Cellular elements are
Hematology The Study of blood Average adult = 8-10 pints of blood Composition: PLASMA liquid portion of blood without cellular components Serum plasma after a blood clot is formed Cellular elements are
Average adult = 8-10 pints of blood. Functions:
 Average adult = 8-10 pints of blood Functions: Transports nutrients, oxygen, cellular waste products, and hormones Aids in distribution of heat Regulates acid-base balance Helps protect against infection
Average adult = 8-10 pints of blood Functions: Transports nutrients, oxygen, cellular waste products, and hormones Aids in distribution of heat Regulates acid-base balance Helps protect against infection
Any of these questions could be asked as open question or lab question, thus study them well
 Any of these questions could be asked as open question or lab question, thus study them well describe the factors which regulate cardiac output describe the sympathetic and parasympathetic control of heart
Any of these questions could be asked as open question or lab question, thus study them well describe the factors which regulate cardiac output describe the sympathetic and parasympathetic control of heart
Pathology of pulmonary vascular disease. Dr.Ashraf Abdelfatah Deyab. Assistant Professor of Pathology Faculty of Medicine Almajma ah University
 Pathology of pulmonary vascular disease Dr.Ashraf Abdelfatah Deyab Assistant Professor of Pathology Faculty of Medicine Almajma ah University Pulmonary vascular disease Type of pulmonary circulation: Types
Pathology of pulmonary vascular disease Dr.Ashraf Abdelfatah Deyab Assistant Professor of Pathology Faculty of Medicine Almajma ah University Pulmonary vascular disease Type of pulmonary circulation: Types
Disturbances of Circulation. Histopathology Lab #2 (Web)
 Disturbances of Circulation Histopathology Lab #2 (Web) Paul Hanna Winter 2015 Slide #96 History: pig was fine in the morning & found dead in the afternoon there was ~100 mls of clear fluid in the pericardial
Disturbances of Circulation Histopathology Lab #2 (Web) Paul Hanna Winter 2015 Slide #96 History: pig was fine in the morning & found dead in the afternoon there was ~100 mls of clear fluid in the pericardial
12/1/2009. Chapter 19: Hemorrhage. Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system Internal hemorrhage
 Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
HEME 10 Bleeding Disorders
 HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
Thromboembolismand Shock 血管栓塞和休克
 Thromboembolismand Shock 血管栓塞和休克 Major Hemodynamic Disorders Edema Hypermia and Congestion 充血 Haemorrhage Hemostasis 止血 and Blood Coagulation 血液凝固 Thrombosis 血栓形成 Embolism 栓塞 Infarction 梗死 Disseminated
Thromboembolismand Shock 血管栓塞和休克 Major Hemodynamic Disorders Edema Hypermia and Congestion 充血 Haemorrhage Hemostasis 止血 and Blood Coagulation 血液凝固 Thrombosis 血栓形成 Embolism 栓塞 Infarction 梗死 Disseminated
HEMODYNAMIC DISORDERS. J v = ([Pc Pi] σ[πc πi])
![HEMODYNAMIC DISORDERS. J v = ([Pc Pi] σ[πc πi]) HEMODYNAMIC DISORDERS. J v = ([Pc Pi] σ[πc πi])](/thumbs/89/98227455.jpg) HEMODYNAMIC DISORDERS J v = ([Pc Pi] σ[πc πi]) Hemodynamic Disorders Thromboembolic Disease Shock Overview Edema Hyperemia Congestion Hemorrhage Hemostasis Thrombosis Embolism Infarction Shock EDEMA ONLY
HEMODYNAMIC DISORDERS J v = ([Pc Pi] σ[πc πi]) Hemodynamic Disorders Thromboembolic Disease Shock Overview Edema Hyperemia Congestion Hemorrhage Hemostasis Thrombosis Embolism Infarction Shock EDEMA ONLY
DISTURBANCES OF CIRCULATION Lisa Miller VPM 152 General Pathology
 DISTURBANCES OF CIRCULATION Lisa Miller VPM 152 PREFACE: In this portion of normal hemostasis will be reviewed. The pathological processes which may be associated with abnormal hemostasis will be discussed.
DISTURBANCES OF CIRCULATION Lisa Miller VPM 152 PREFACE: In this portion of normal hemostasis will be reviewed. The pathological processes which may be associated with abnormal hemostasis will be discussed.
Chapter 14. Blood. Blood Volume. Blood Composition. Blood
 Blood connective tissue transports vital substances maintains stability of interstitial fluid distributes heat Chapter 14 Blood Blood Cells form mostly in red bone marrow red blood cells white blood cells
Blood connective tissue transports vital substances maintains stability of interstitial fluid distributes heat Chapter 14 Blood Blood Cells form mostly in red bone marrow red blood cells white blood cells
Coagulation Disorders. Dr. Muhammad Shamim Assistant Professor, BMU
 Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
General Pathology. Disturbances of Circulation Edema. (Web)
 General Pathology Disturbances of Circulation Edema (Web) Paul Hanna Jan 2015 The health of cells and organs critically depends on an unbroken circulation to deliver oxygen and nutrients and to remove
General Pathology Disturbances of Circulation Edema (Web) Paul Hanna Jan 2015 The health of cells and organs critically depends on an unbroken circulation to deliver oxygen and nutrients and to remove
-Hashim ahmed is the one who wrote this sheet. I just edited it according to our record.
 * Subjects of this lecture : - Hemostasis - Platelets, general information, their ultrastructure and role in hemostasis. - Definitions: Thrombus, Embolus, Arteriosclerosis and Atherosclerosis. *NOTE: Prof
* Subjects of this lecture : - Hemostasis - Platelets, general information, their ultrastructure and role in hemostasis. - Definitions: Thrombus, Embolus, Arteriosclerosis and Atherosclerosis. *NOTE: Prof
Wheater: Part 1: Thrombosis, embolism and infarction. Laboratory assignment: C601/C602 Histopathology manual, hemodynamic unit.
 Pathology C 601 Hemodynamic Derangements Assignment page. Reading: Robbins: Chapter 4 Clinical Lab Source: - Protime (PT) Know about INR - Activated partial thrmboplastin time (APTT) - Activated coagulation
Pathology C 601 Hemodynamic Derangements Assignment page. Reading: Robbins: Chapter 4 Clinical Lab Source: - Protime (PT) Know about INR - Activated partial thrmboplastin time (APTT) - Activated coagulation
Blood and Defense. Chapter 11
 Blood and Defense Chapter 11 Functions of Blood 1. Carry nutrients from the small intestine and oxygen from the lung to tissues in the body 2. Transport wastes from tissues to the kidneys and carbon dioxide
Blood and Defense Chapter 11 Functions of Blood 1. Carry nutrients from the small intestine and oxygen from the lung to tissues in the body 2. Transport wastes from tissues to the kidneys and carbon dioxide
Cardiovascular System B L O O D V E S S E L S 3
 Cardiovascular System B L O O D V E S S E L S 3 Fluid Shifts Between Capillaries and Tissue Permeable capillaries allow plasma and solutes to pass into interstitial space interstitial or extracellular
Cardiovascular System B L O O D V E S S E L S 3 Fluid Shifts Between Capillaries and Tissue Permeable capillaries allow plasma and solutes to pass into interstitial space interstitial or extracellular
Physiology of Circulation
 Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
Hemostasis. Learning objectives Dr. Mária Dux. Components: blood vessel wall thrombocytes (platelets) plasma proteins
 Hemostasis Learning objectives 14-16 Dr. Mária Dux Components: blood vessel wall thrombocytes (platelets) plasma proteins Hemostatic balance! procoagulating activity anticoagulating activity 1 Thrombocytes
Hemostasis Learning objectives 14-16 Dr. Mária Dux Components: blood vessel wall thrombocytes (platelets) plasma proteins Hemostatic balance! procoagulating activity anticoagulating activity 1 Thrombocytes
1- Thromboembolism. 2- fat embolism. 3- air embolism. 4- amniotic fluid embolism.
 Embolism Definition:- An embolus is a detached intravascular solid, liquid or gaseous mass that is carried by blood to sites distant from its point of origin. After traveling via the blood, the embolus
Embolism Definition:- An embolus is a detached intravascular solid, liquid or gaseous mass that is carried by blood to sites distant from its point of origin. After traveling via the blood, the embolus
Thrombosis. Dr. László Terézia
 Thrombosis Dr. László Terézia HYPERCOAGULABILITY THROMBOSIS BLOODFLOW ENDOTHEL VIRCHOW ENDOTHEL INJURY L. ventricle: Arteries: surgery infection prosthetic valve hypertension irradiation chemical: cigarette
Thrombosis Dr. László Terézia HYPERCOAGULABILITY THROMBOSIS BLOODFLOW ENDOTHEL VIRCHOW ENDOTHEL INJURY L. ventricle: Arteries: surgery infection prosthetic valve hypertension irradiation chemical: cigarette
Blood consists of red and white blood cells suspended in plasma Blood is about 55% plasma and 45% cellular elements Plasma 90% water 10% dissolved
 Bio 100 Guide 21 Blood consists of red and white blood cells suspended in plasma Blood is about 55% plasma and 45% cellular elements Plasma 90% water 10% dissolved inorganic ions, proteins, nutrients,
Bio 100 Guide 21 Blood consists of red and white blood cells suspended in plasma Blood is about 55% plasma and 45% cellular elements Plasma 90% water 10% dissolved inorganic ions, proteins, nutrients,
Blood. Biol 105 Lecture 14 Chapter 11
 Blood Biol 105 Lecture 14 Chapter 11 Outline I. Overview of blood II. Functions of blood III. Composition of blood IV. Composition of plasma V. Composition of formed elements VI. Platelets VII. White blood
Blood Biol 105 Lecture 14 Chapter 11 Outline I. Overview of blood II. Functions of blood III. Composition of blood IV. Composition of plasma V. Composition of formed elements VI. Platelets VII. White blood
Ischemic heart disease
 Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Disseminated Intravascular Coagulation. M.Bahmanpour MD Assistant professor IUMS
 به نام خدا Disseminated Intravascular Coagulation M.Bahmanpour MD Assistant professor IUMS Algorithm for Diagnosis of DIC DIC Score factor score Presence of known underlying disorder No= 0 yes=2 Coagolation
به نام خدا Disseminated Intravascular Coagulation M.Bahmanpour MD Assistant professor IUMS Algorithm for Diagnosis of DIC DIC Score factor score Presence of known underlying disorder No= 0 yes=2 Coagolation
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
Chapter 19 Cardiovascular System Blood: Functions. Plasma
 Chapter 19 Cardiovascular System Blood: Functions 19-1 Plasma Liquid part of blood. Colloid: liquid containing suspended substances that don t settle out of solution 91% water. Remainder proteins, ions,
Chapter 19 Cardiovascular System Blood: Functions 19-1 Plasma Liquid part of blood. Colloid: liquid containing suspended substances that don t settle out of solution 91% water. Remainder proteins, ions,
Levels of Organization. Chapter 19 6/11/2012. Homeostasis & Organization of the animal body. 4 Primary Tissues
 Levels of Organization Chapter 19 Homeostasis & Organization of the animal body Chemical Cellular Tissue Organs System Level Organismic 1-2 4 Primary Tissues 1. Epithelial Tissue: covers surfaces lines
Levels of Organization Chapter 19 Homeostasis & Organization of the animal body Chemical Cellular Tissue Organs System Level Organismic 1-2 4 Primary Tissues 1. Epithelial Tissue: covers surfaces lines
HEART HEALTH WEEK 2 SUPPLEMENT. A Beginner s Guide to Cardiovascular Disease ATHEROSCLEROSIS. Fatty deposits can narrow and harden the artery
 WEEK 2 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease ATHEROSCLEROSIS FIGURE 1 Atherosclerosis is an inflammatory process where cholesterol is deposited in the wall of arteries and
WEEK 2 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease ATHEROSCLEROSIS FIGURE 1 Atherosclerosis is an inflammatory process where cholesterol is deposited in the wall of arteries and
Hemostasis Haemostasis means prevention of blood loss from blood vessels.
 ١ Hemostasis Haemostasis means prevention of blood loss from blood vessels. Bleeding is stopped by several mechanisms, which are: 1. Local vasoconstriction 2. Formation of platelet plug 3. Blood coagulation
١ Hemostasis Haemostasis means prevention of blood loss from blood vessels. Bleeding is stopped by several mechanisms, which are: 1. Local vasoconstriction 2. Formation of platelet plug 3. Blood coagulation
The Cardiovascular and Lymphatic Systems Cardiovascular System Blood Vessels Blood Vessels Arteries Arteries Arteries
 CH 12 The Cardiovascular and s The Cardiovascular and s OUTLINE: Cardiovascular System Blood Vessels Blood Pressure Cardiovascular System The cardiovascular system is composed of Blood vessels This system
CH 12 The Cardiovascular and s The Cardiovascular and s OUTLINE: Cardiovascular System Blood Vessels Blood Pressure Cardiovascular System The cardiovascular system is composed of Blood vessels This system
Blood flows away from the heart in arteries, to the capillaries and back to the heart in the veins
 Cardiovascular System Summary Notes The cardiovascular system includes: The heart, a muscular pump The blood, a fluid connective tissue The blood vessels, arteries, veins and capillaries Blood flows away
Cardiovascular System Summary Notes The cardiovascular system includes: The heart, a muscular pump The blood, a fluid connective tissue The blood vessels, arteries, veins and capillaries Blood flows away
1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary.
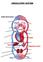 CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
What is the composition of blood, including blood cells? What organs and structures control the flow of blood throughout the body?
 3 Chapter 10: Circulatory System and Lymphatic System In this chapter, you will learn about the structure and function of the circulatory system and lymphatic system. What is the composition of blood,
3 Chapter 10: Circulatory System and Lymphatic System In this chapter, you will learn about the structure and function of the circulatory system and lymphatic system. What is the composition of blood,
Introduction to Lesson 4 - The Lymphatic System
 Introduction to Lesson 4 - The Lymphatic System Your circulatory system is not your body s only vascular transport system. Closely associated with the blood vessels of the circulatory system is the lymphatic
Introduction to Lesson 4 - The Lymphatic System Your circulatory system is not your body s only vascular transport system. Closely associated with the blood vessels of the circulatory system is the lymphatic
Bleeding and Haemostasis. Saman W.Boskani HDD, FIBMS Maxillofacial Surgeon
 Bleeding and Haemostasis Saman W.Boskani HDD, FIBMS Maxillofacial Surgeon 1 Beeding Its escaping or extravasation of blood contents from blood vessels Types: - Arterial - Venous - Capillary Differences
Bleeding and Haemostasis Saman W.Boskani HDD, FIBMS Maxillofacial Surgeon 1 Beeding Its escaping or extravasation of blood contents from blood vessels Types: - Arterial - Venous - Capillary Differences
Blood clotting. Subsequent covalent cross-linking of fibrin by a transglutaminase (factor XIII) further stabilizes the thrombus.
 Blood clotting It is the conversion, catalyzed by thrombin, of the soluble plasma protein fibrinogen (factor I) into polymeric fibrin, which is deposited as a fibrous network in the primary thrombus. Thrombin
Blood clotting It is the conversion, catalyzed by thrombin, of the soluble plasma protein fibrinogen (factor I) into polymeric fibrin, which is deposited as a fibrous network in the primary thrombus. Thrombin
Blood coagulation and fibrinolysis. Blood clotting (HAP unit 5 th )
 Blood coagulation and fibrinolysis Blood clotting (HAP unit 5 th ) Vessel injury Antithrombogenic (Favors fluid blood) Thrombogenic (Favors clotting) 3 Major systems involved Vessel wall Endothelium ECM
Blood coagulation and fibrinolysis Blood clotting (HAP unit 5 th ) Vessel injury Antithrombogenic (Favors fluid blood) Thrombogenic (Favors clotting) 3 Major systems involved Vessel wall Endothelium ECM
Thrombosis. Jeffrey Jhang, M.D.
 Thrombosis Jeffrey Jhang, M.D. Introduction The human hemostatic system has evolved to maintain blood flow under normal physiologic conditions while remaining primed to rapidly respond to vascular injury
Thrombosis Jeffrey Jhang, M.D. Introduction The human hemostatic system has evolved to maintain blood flow under normal physiologic conditions while remaining primed to rapidly respond to vascular injury
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp , , , I. Major Functions of the Circulatory System
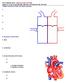 P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
Blood and the Lymphatic System. Lesson Overview. Lesson Overview Blood and the Lymphatic System
 Lesson Overview 33.2 Blood and the Lymphatic System THINK ABOUT IT When you think about body tissues, you probably picture something with a definite shape, like muscle or skin. But blood is a tissue too
Lesson Overview 33.2 Blood and the Lymphatic System THINK ABOUT IT When you think about body tissues, you probably picture something with a definite shape, like muscle or skin. But blood is a tissue too
The Cardiovascular System: Blood
 C h a p t e r 11 The Cardiovascular System: Blood PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Introduction to the Cardiovascular System A circulating transport system
C h a p t e r 11 The Cardiovascular System: Blood PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Introduction to the Cardiovascular System A circulating transport system
Circulatory disorders
 Circulatory disorders Edema = fluid in interstitium transudate s.w.1.012, exudate 1.020) generalized x local prominent cavities hydrothorax, hydropericardium, ascites subcutaneous tissue (pitting edema)
Circulatory disorders Edema = fluid in interstitium transudate s.w.1.012, exudate 1.020) generalized x local prominent cavities hydrothorax, hydropericardium, ascites subcutaneous tissue (pitting edema)
Hemostasis Haemostasis means prevention of blood loss from blood vessels.
 1 Hemostasis Haemostasis means prevention of blood loss from blood vessels. Bleeding is stopped by several mechanisms, which are: 1. Local vasoconstriction 2. Formation of platelet plug 3. Blood coagulation
1 Hemostasis Haemostasis means prevention of blood loss from blood vessels. Bleeding is stopped by several mechanisms, which are: 1. Local vasoconstriction 2. Formation of platelet plug 3. Blood coagulation
CH 11 Blood OUTLINE: Functions of Blood Composition of Blood Blood Cell Disorders Blood Types Blood Clotting Functions of Blood Transportation
 1 CH 11 Blood OUTLINE: Functions of Blood Composition of Blood Blood Cell Disorders Blood Types Functions of Blood Transportation Protection Regulation ph Temperature Composition of Blood Plasma: liquid
1 CH 11 Blood OUTLINE: Functions of Blood Composition of Blood Blood Cell Disorders Blood Types Functions of Blood Transportation Protection Regulation ph Temperature Composition of Blood Plasma: liquid
Chapter 19 Blood Lecture Outline
 Chapter 19 Blood Lecture Outline Cardiovascular system Circulatory system Blood 1. distribution 2. regulation 3. protection Characteristics: ph 7.4 38 C 4-6 L Composition: Plasma Formed elements Erythrocytes
Chapter 19 Blood Lecture Outline Cardiovascular system Circulatory system Blood 1. distribution 2. regulation 3. protection Characteristics: ph 7.4 38 C 4-6 L Composition: Plasma Formed elements Erythrocytes
CEREBROVASCULAR DISEASES. By: Shifaa AlQa qa
 CEREBROVASCULAR DISEASES By: Shifaa AlQa qa Cerebrovascular diseases Brain disorders caused by pathologic processes involving blood vessels 3 pathogenic mechanisms (1) thrombotic occlusion, (2) embolic
CEREBROVASCULAR DISEASES By: Shifaa AlQa qa Cerebrovascular diseases Brain disorders caused by pathologic processes involving blood vessels 3 pathogenic mechanisms (1) thrombotic occlusion, (2) embolic
4/5/17. Blood. Blood. Outline. Blood: An Overview. Functions of Blood
 Outline Blood Biol 105 Chapter 11 I. Overview of blood II. Functions of blood III. Composition of blood IV. Composition of plasma V. Composition of formed elements VI. Platelets VII. White blood cells
Outline Blood Biol 105 Chapter 11 I. Overview of blood II. Functions of blood III. Composition of blood IV. Composition of plasma V. Composition of formed elements VI. Platelets VII. White blood cells
PHM142 Lecture 4: Platelets + Endothelial Cells
 PHM142 Lecture 4: Platelets + Endothelial Cells 1 Hematopoiesis 2 Platelets Critical in clotting - activated by subendothelial matrix proteins (e.g. collagen, fibronectin, von Willebrand factor) and thrombin
PHM142 Lecture 4: Platelets + Endothelial Cells 1 Hematopoiesis 2 Platelets Critical in clotting - activated by subendothelial matrix proteins (e.g. collagen, fibronectin, von Willebrand factor) and thrombin
Sinusoids and venous sinuses
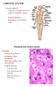 LYMPHOID SYSTEM General aspects Consists of organs that are made of lymphoid tissue; Immune defense Breakdown of red blood cells. 1 Sinusoids In place of capillaries Endothelium; often fenestrated More
LYMPHOID SYSTEM General aspects Consists of organs that are made of lymphoid tissue; Immune defense Breakdown of red blood cells. 1 Sinusoids In place of capillaries Endothelium; often fenestrated More
INFLAMMATION & REPAIR
 INFLAMMATION & REPAIR Lecture 7 Chemical Mediators of Inflammation Winter 2013 Chelsea Martin Special thanks to Drs. Hanna and Forzan Course Outline i. Inflammation: Introduction and generalities (lecture
INFLAMMATION & REPAIR Lecture 7 Chemical Mediators of Inflammation Winter 2013 Chelsea Martin Special thanks to Drs. Hanna and Forzan Course Outline i. Inflammation: Introduction and generalities (lecture
Copyright 2010 Pearson Education, Inc. Blood Vessel Structure
 Blood Vessel Structure Structure of Blood Vessel Walls Arteries and veins Tunica intima, tunica media, and tunica externa Lumen Central blood-containing space Capillaries Endothelium with sparse basal
Blood Vessel Structure Structure of Blood Vessel Walls Arteries and veins Tunica intima, tunica media, and tunica externa Lumen Central blood-containing space Capillaries Endothelium with sparse basal
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 11 THE LYMPHATIC SYSTEM AND IMMUNITY
 ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 11 THE LYMPHATIC SYSTEM AND IMMUNITY Functions of the Lymphatic System The lymphatic system has three primary functions. First of all, it returns excess interstitial
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 11 THE LYMPHATIC SYSTEM AND IMMUNITY Functions of the Lymphatic System The lymphatic system has three primary functions. First of all, it returns excess interstitial
Fourth Practical Pathology. Circulatory disturbances
 Fourth Practical Pathology Circulatory disturbances 12.12.2018 1 Organ: Lung (40X, low power) 1) The blood capillaries within the alveolar septa are engorged with blood 2) Pinkish proteinaceous fluid,
Fourth Practical Pathology Circulatory disturbances 12.12.2018 1 Organ: Lung (40X, low power) 1) The blood capillaries within the alveolar septa are engorged with blood 2) Pinkish proteinaceous fluid,
Study of different tissues Abnormal cells and tissues can be compared to normal tissues to identify disease, such as cancer Being able to know and
 CHAPTER 4 Study of different tissues Abnormal cells and tissues can be compared to normal tissues to identify disease, such as cancer Being able to know and recognize normal tissues under the microscope
CHAPTER 4 Study of different tissues Abnormal cells and tissues can be compared to normal tissues to identify disease, such as cancer Being able to know and recognize normal tissues under the microscope
