Arrhythmias_for_6_c..docx. Олена Костянтинівна Редько
|
|
|
- Brianna Bond
- 6 years ago
- Views:
Transcription
1 Arrhythmias_for_6_c..docx Олена Костянтинівна Редько 2015
2
3 Ключові терміни: 3 Зміст Ключові терміни: Arrhythmias 3 3
4 Ключові терміни: 4 Arrhythmias Ключові терміни: An irregular heart rhythm, Atrial flutter, First-degree heart block, Questions, Second degree heart block, Supraventricular tachycardia (SVT),, The management, The prolonged QT syndrome, heart block, ventricular fibrillation Arrhythmias This is a 1 month old male who presents to the emergency room with a chief complaint of fever, lethargy, and poor feeding for the past 36 hours. He was well until he developed a tactile fever. His parents began noticing increasing lethargy and tiring with feeding and decreased oral intake for about 12 hours prior to presentation. He is the product of a G2P1, full term, uncomplicated pregnancy. Delivery and stay in the nursery was uneventful. Exam: VS T 38.0, HR 240, RR 72, BP 87/64, oxygen saturation 98% in room air. He is well developed, well nourished, but pale, lethargic and tachypneic, with mild subcostal retractions. HEENT exam is normal. Neck is supple without adenopathy. Lungs are clear to auscultation with good aeration. His heart is tachycardic with a regular rhythm. No murmur, rub, or valve clicks are heard. There is a soft S3 gallop that can be head from the lower left sternal border to the cardiac apex. His abdomen is soft, nondistended, non-tender, and without masses. His liver is 2 to 3 cm below right costal margin. His feet and hands are cool. His peripheral pulses are 1+ to 2+ (out of 4+) throughout. Capillary refill time is 3 to 4 seconds. He has no rashes or other significant lesions. A chest x-ray shows mild cardiomegaly and mild pulmonary edema. A 12 lead electrocardiogram shows a narrow complex tachycardia (rate of 240 bpm) with no visible P-waves. Mild ST segment depression in the inferior-lateral leads is present. The patient is felt to be in supraventricular tachycardia and mild congestive heart failure. A peripheral IV is started and he is given a rapid IV bolus dose of adenosine. The patient immediately becomes briefly bradycardic followed by resumption of a normal sinus rhythm at a rate of 140 beats per minute. He is admitted for overnight observation and initiation of an anti-arrhythmic medication. A 12 lead electrocardiogram following conversion shows no evidence of a delta-wave, so a loading dose of digoxin is administered. An irregular heart rhythm is not an unusual finding in children with or without known cardiac disease. Some irregular rhythms are normal findings in healthy children. If the heart rate is not too slow or too fast, as to limit the cardiac output, then an arrhythmia may be well tolerated. Most children can be satisfactorily evaluated with a 12 lead electrocardiogram and rhythm strip, with possible supplementation by a chest x-ray, echocardiogram, Holter or event monitor, or an exercise study. There are several important determinants of arrhythmias, which should be considered. These include the arrhythmogenic substrate (e.g., accessory conduction pathway, automatic ectopic focus), modulating factors, and triggers of the arrhythmia. Changes in sinus rhythm (P-wave preceding each QRS complex, with a normal P-wave axis) are most commonly seen with a sinus arrhythmia, sinus bradycardia, or sinus tachycardia. In pediatrics, a sinus arrhythmia is usually secondary to a variation in vagal tone during the normal respiratory cycle. This causes an increase in heart rate during inspiration and a decrease in heart rate during exhalation. It is most pronounced when the heart rate is slower and resolves with an increase in heart rate.
5 Ключові терміни: 5 Sinus bradycardia is a sinus rhythm with a rate below the lower normal limits for age and activity level. It is most often encountered in well conditioned athletes. Pathologic states in which sinus bradycardia may occur include increased intracranial, intrathoracic, or intraabdominal pressure, and systemic hypertension. Sinus tachycardia is a sinus rhythm with a rate greater than the higher limits for age and activity level. If the child is not active then the tachycardia usually has a secondary cause such as fever, heart failure, pain, anxiety, hypovolemia, anemia, myocarditis, or thyrotoxicosis. Supraventricular tachycardia (SVT), also known as paroxysmal supraventricular tachycardia (PSVT) is a tachyarrhythmia manifesting with a narrow complex QRS duration (<0.08 sec).
6 Ключові терміни: 6 Many definitions of SVT exist, some of, which include all abnormal tachycardias originating in or around the atria (which would include PSVT, atrial fibrillation and atrial flutter). For the sake of this discussion, SVT will be defined as those narrow complex tachycardias involving the SA node and an accessory electrical pathway anywhere along the atrioventricular junction or very near the AV node itself (this definition excludes atrial fibrillation and atrial flutter). These are considered reciprocating tachycardias, as two discrete pathways are present, one with antegrade conduction and the other with retrograde conduction. One pathway is considered a "fast" pathway, with rapid conduction, and the other a "slow" pathway, with slower conduction. This creates the reentrant circuit. With orthodromic (conventional pathway) SVT, the antegrade conduction is down the "slow" pathway, usually the AV node, and the retrograde conduction is up the "fast" pathway, usually the accessory conduction tissue. Antidromic SVT is characterized by antegrade conduction down the "fast" pathway, and retrograde conduction up the "slow" pathway. Supraventricular tachycardia is the most common abnormal tachycardia in the pediatric age group. The most common types of SVT in children include atrioventricular reentrant tachycardia (AVRT), which includes Wolff-Parkinson-White syndrome (WPW), and AV nodal reentrant tachycardia (AVNRT formerly called Lown-Ganong-Levine or LGL syndrome). Supraventricular tachycardia usually has its onset at rest but may initiate during exercise. The precipitating factor(s) is often difficult to identify, but occasionally a febrile illness may precipitate an episode. The heart rate is usually in the 160 to 300 beat/min range. In general, the younger the patient the more rapid the SVT heart rate, but the longer the tachycardia is tolerated before symptoms (usually congestive heart failure) become obvious. As a rule, episodes of SVT onset and terminate abruptly, and may last anywhere from a few minutes to many hours, which is why it is called paroxysmal. In infants, symptoms of SVT may not become apparent until the patient has been in SVT for 24 hours, or longer. They will often present with symptoms of congestive heart failure such as tachypnea, pallor, poor feeding, fussiness or lethargy. In children and adolescents, symptoms may include palpitations, chest pain, shortness of breath, dizziness, syncope or near syncope, pallor, and diaphoresis. It is unusual for older patients to present in heart failure, as they will usually become symptomatic soon after the onset of SVT. They will often complain of intermittent episodes of palpitations, with mild associated symptoms. Supraventricular tachycardia may present as syncope or near syncope. This may occur in patients with WPW who develop atrial fibrillation and rapid conduction down the accessory pathway to the ventricles.
7 Ключові терміни: 7 The onset of SVT can also cause a decrease in cardiac output with resultant hypotension, decreased cerebral perfusion pressure, and syncope. In the pediatric age group, the most common cause of syncope is neurocardiogenic syncope (also called a vasovagal faint). Syncopal episodes associated with palpitations should raise the suspicion of a possible tachyarrhythmia contributing to the patients symptoms. Nearly any type of cardiac arrhythmia can cause syncope if a sudden fall in cardiac output occurs. Cardiac dysrhythmias to consider should include SVT, ventricular tachycardia (in particular, long QT syndrome), advance degree AV block, sick sinus syndrome in patients with previous cardiac surgery, and pacemaker malfunction in those patients who are pacer dependent. Other cardiac related disease to consider in patients presenting with syncope include outflow tract obstruction (hypertrophic cardiomyopathy, aortic stenosis, pulmonic stenosis, pulmonary hypertension), coronary artery anomalies, cardiomyopathies, and mitral valve prolapse. The diagnosis can often be made with a thorough history and physical examination performed as close to the time of the syncopal episode as possible. Cases, which should arouse increased concern, include those not consistent with neurocardiogenic syncope, syncope with exercise, a family history of sudden death, and those patients with known structural cardiac disease. All patients who present with syncope should, at the minimum, have an EKG performed. In most cases of neurocardiogenic syncope, symptoms will improve or resolve with increased fluid and salt intake. Treatment for other causes of syncope should address the underlying etiology. The differential diagnosis of a pediatric patient who presents in a narrow complex tachycardia includes SVT, sinus tachycardia, atrial flutter, atrial fibrillation, junctional ectopic tachycardia, ectopic atrial tachycardia, and chaotic atrial rhythm. Some patients with SVT and a bundle branch block or antidromic WPW, may present with a wide complex tachycardia, which if often difficult to distinguish from ventricular tachycardia (VT). Most of the narrow complex tachyarrhythmias may be distinguished from their electrocardiogram findings. Supraventricular tachycardia ranges in heart rate from 160 to 300 beats per minute. The diagnosis of AVRT or AVNRT requires the presence of 1:1 A-V conduction. The heart rate usually remains in a very narrow range regardless of the patient's physiologic state. P-waves, which are oftentimes retrograde, are visible only in 50% or less of cases. Upon conversion to a sinus rhythm, patients with WPW or Mahaim fibers (an accessory pathway able to conduct only antegrade, with slow conduction, connecting the atrium directly to a portion of the right bundle branch) will demonstrate the classical delta waves as evidenced by an upsloping or slurring of the initial portion of the QRS complex. Delta waves are secondary to rapid antegrade conduction from the atrium to the ventricles through the accessory pathway, thus causing ventricular pre-excitation. With WPW the PR interval is short, but with the presence of Mahaim fibers the PR interval is normal. Forms of SVT with concealed accessory pathways (i.e., those capable of only retrograde conduction), will not show evidence of a delta wave, and therefore most will have normal PR intervals. An exception is those patients with James fibers (a form of AVNRT), who have a short PR interval. Most patients with SVT have normal cardiac anatomy. Congenital heart defects in which SVT is most commonly encountered are Ebstein's anomaly and L-transposition of the great arteries. Atrial flutter may present with a regular or regularly irregular tachycardia with an atrial rate in the range of 250 to 400 beats per minutes. The classic sawtooth flutter waves may be seen, or revealed following a dose of adenosine. The ventricular rate will depend on the degree of A-V conduction (e.g. 2:1, 3:1, etc.). Atrial flutter will most often be encountered in the setting of congenital heart disease, presence of significant mitral or tricuspid valve regurgitation with atrial dilatation, fetuses or newborns with normal hearts (i.e., it sometimes occurs in normal fetuses and newborns), or in patients with myocarditis.
8 Ключові терміни: 8 Atrial fibrillation demonstrates a rapid atrial rate ( beats per minute) with a very chaotic pattern, and an irregularly irregular ventricular rhythm. Atrial fibrillation is most often seen in older children following palliative surgery for congenital heart defects, especially those involving intra-atrial surgery (e.g., Fontan, Mustard, or Senning procedures), and those children with significant atrioventricular valve disease. Ectopic atrial tachycardia and chaotic atrial rhythm are rare tachyarrhythmias in the pediatric age group. On EKG, ectopic atrial tachycardia will show the presence of a variable atrial rate with an abnormal P-wave axis indicating a single atrial focus. Chaotic atrial rhythm, also referred to as multifocal atrial tachycardia, typically demonstrates at least 3 non-sinus P-wave morphologies, an irregular ventricular response, and variable PR, PP, and RR intervals. Both types of dysrhythmias occur most often in patients with structurally normal hearts, at times with concomitant myocarditis. Junctional ectopic tachycardia is most commonly encountered in children less than 2 years of age, in the immediate post-operative period following corrective surgery for a congenital heart defect involving the region around the AV node (e.g., a VSD or tetralogy of Fallot repair). This is one of the most common post-operative arrhythmias encountered. The EKG typically demonstrates a narrow complex tachycardia with a regular atrial and ventricular rhythm, and a ventricular rate, which is more rapid than the atrial rate. This dysrhythmia originates from a focus of enhanced automaticity in the peri-av nodal region. The heart rate typically rises and decreases gradually (warms up and cools down). This feature helps differentiate it from a reentrant type of tachyarrhythmia. Significant ventricular arrhythmias, such at ventricular tachycardia (VT) and ventricular fibrillation (VF), are rarely encountered in the pediatric age group. Benign premature ventricular contractions (PVC) are not uncommon in infants, older children, and adolescents. Patients with ventricular arrhythmias may be asymptomatic or they may present with symptoms of palpitations, chest pain, dizziness, and/or syncope. Ventricular tachycardia is defined at 3 or more consecutive abnormal QRS complexes at a rate greater than 120 beats per minute. As mentioned previously, SVT may occasionally present as a wide complex tachycardia, which may be difficult to distinguish from ventricular tachycardia. In these cases, the definitive diagnosis may not be known until the patient is converted to a sinus rhythm. In these situations the patient should be presumptively treated as having ventricular tachycardia (VT) until proven otherwise. It should be remembered that VT does not always present as a wide QRS complex tachycardia, especially in infants. Ventricular fibrillation displays unidentifiable QRS complexes due to an uncoordinated state of ventricular depolarization, resulting in a state of poor cardiac output. Significant ventricular dysrhythmias in the pediatric age range are most commonly encountered in the setting of congenital heart disease, myocarditis, cardiomyopathies, myocardial trauma, hypoxia, acidosis, and electrolyte abnormalities (most notably hypokalemia and hyperkalemia). The prolonged QT syndrome causes a distinct type of VT called Torsades de Pointes characterized by a polymorphic VT, which oftentimes causes syncope or sudden death. Recent genetic linkage analyses have isolated a number of genetic foci associated with defects in cardiac ion channels (namely sodium
9 Ключові терміни: 9 and potassium channels). Prior to the advent of genetic analysis, patients with long QT syndrome were classified into two groups: Jervell-Lange-Nielsen (autosomal recessive, associated with congenital deafness) and Romano-Ward (autosomal dominant, without deafness). Prolongation of the QT interval may also develop secondary to drugs (anti-arrhythmic agents, antihistamines, antidepressants, antipsychotics, some antibiotics), CNS trauma, cardiomegaly, hypokalemia, and hypocalcemia.
10 Ключові терміни: 10 Various forms of heart block are usually encountered in children with congenital heart defects, heart failure, or with congenitally acquired heart block. Congenital complete heart block is most commonly seen in the setting of a maternal collagen vascular disorder, namely systemic lupus erythematosus or Sjogren's syndrome. In nearly all cases, maternal SS-A/Ro and SS-B/La autoantibodies can be isolated. Conversely, not all fetuses whose mother is positive for these antibodies will develop heart block. The most common congenital heart defect associated with complete heart block is L-transposition of the great arteries. If the ventricular rate is too slow to maintain adequate cardiac output, heart failure may develop in utero or postnatally. Treatment involves permanent pacing. The decision to treat depends on the baseline ventricular rate and the likelihood of sudden death. First-degree heart block is diagnosed by an ECG. First-degree heart block is a condition characterized by a slowing down of the electrical impulse that controls the heartbeat, according to the American Heart Association. This condition is diagnosed after a delay in the heart's electrical impulse is seen on an electrocardiogram (ECG). First-degree heart block can be caused by a number of conditions. Usually this condition does not need treatment. Skipped heart beats indicate second degree heart block. Second degree heart block describes a disorder of the conduction pathways in the heart. Normally, an electrical impulse initiates at the sinus node located in the right atrium. Cells carry the impulse to the
11 Ключові терміни: 11 atrioventricular node or AV node located in the center of the heart between the atria and ventricles. The electrical impulse is delayed at the AV node. Once the atrium contracts, the electrical impulse passes to the ventricles. With second degree heart block, some electrical impulses are not conducted from the atria to the ventricle and skipped heart beats occur. The causes are acquired, congenital or unknown. The management approach for SVT depends upon the age and condition of the patient on presentation. If the patient is clinically stable, vagal maneuvers may be initially attempted to convert the tachycardia. Such vagal maneuvers may include bearing down (as though having a bowel movement, i.e., Valsalva maneuver), or inducing the diving reflex using an ice bag to the face or submerging the patient's face into a container of ice water. Other vagal maneuvers such as eyeball pressure and unilateral carotid massage are less effective and may be harmful. If the patient appears clinically unstable, then an intravenous line should be immediately started in a centrally located peripheral vein (antecubital preferred over a hand vein) through which an IV bolus of adenosine may be given. It must be remembered that this medication has a very short half life of approximately 10 seconds, therefore it should be administered via bolus injection followed by an immediate bolus of saline utilizing either a 3 way stopcock or simultaneous needles within the same IV hub (the IV push and immediate flush technique). A 12 lead electrocardiogram should be obtained before and after conversion, if possible, and a rhythm strip should be continuously run during attempted conversion. External pacing equipment should be available since some patients go into sinus arrest following administration of adenosine. Adenosine causes a transient AV block and sinus bradycardia thus interrupting the reentrant circuit involving the AV node and accessory pathway. Potential side effects with adenosine include hypotension, bronchospasm, and flushing. In rare cases, a patient will present in very unstable condition. Immediate electrical cardioversion may be required in such cases, especially if an IV cannot be started in an expedient manner or the patient fails to convert with IV adenosine. Other modes of acute treatment include use of digoxin, verapamil, propranolol, transesophageal or transvenous pacing. Conversion to a sinus rhythm with these medications will usually be slower, therefore most are utilized for chronic control once the SVT has been converted by other means. If adenosine fails to convert the SVT, but the patient is hemodynamically stable, they may be started on one, or more, of these medications (with the exception of verapamil which should be avoided in infants) and monitored for conversion. It is important to remember not to use digoxin on patients with ventricular pre-excitation (e.g., WPW), as it may increase antegrade conduction down the accessory pathway. Patients with WPW are more prone to develop atrial flutter or fibrillation, and are therefore at risk for 1:1 conduction to the ventricles while on digoxin, potentially sending the patient into ventricular tachycardia or fibrillation. Long term management of SVT depends on the severity and frequency of episodes. In those patients with no ventricular pre-excitation and infrequent, mild episodes that can be converted with vagal maneuvers, no treatment is required. Patients with frequent episodes, or severe symptoms, and those with ventricular pre-excitation, medical management should be started with a beta-blocker, digoxin, or calcium channel blocker. Patients diagnosed in infancy often will not require continued treatment beyond 1 year of age, but may have recurrent episodes later in life. With the presence of severe symptoms, syncope, difficult to control SVT, or other situations, e.g., patient preference, an electrophysiology study and radiofrequency ablation can be performed with a high success rate for cure. The majority of fetuses and infants who present in SVT will have no recurrences off medication after 6 to 12 months of age. Patients who present in later childhood or during adolescence will likely have recurrent episodes of SVT throughout their lifetime. Many of these patients will require medical treatment and will eventually seek curative treatment with radiofrequency ablation. Radiofrequency ablation involves mapping out accessory conduction pathways in the heart with the use of electrodes placed in the atria, coronary sinus, and ventricles through central venous access. Upon localization of the pathway a specialized ablation catheter (tip is heated using radiofrequency energy) is used to burn and cause irreversible tissue injury to the accessory conduction tissue. With the recent advancements in pediatric electrophysiology, the prognosis for patients with SVT is
12 Ключові терміни: 12 very good. The success rate with radiofrequency ablation continues to improve, especially when performed at centers with experienced specialists. Death or significant morbidity is rare with the present state of medical management. Most patients can be expected to live a normal life expectancy with little or no lifestyle alteration due to this condition. Questions What are the two most common forms of SVT in the pediatric population? What are the two most common types of congenital heart defects associated with SVT? Name two instances in which SVT may present as a wide complex QRS tachycardia In a hemodynamically stable patient who presents with SVT, what are the two most commonly used methods for attempted conversion to a sinus rhythm? True/False: Supraventricular tachycardia is the most common cause of syncope in the pediatric age group. Answers 1. Atrioventricular reentrant tachycardia (AVRT) and AV nodal reentrant tachycardia (AVNRT). 2. Ebstein anomaly and L-transposition of the great vessels. 3. With the presence of a bundle branch block or with antidromic conduction. 4. Vagal maneuvers and intravenous adenosine. 5. False.
Supraventricular Tachycardia: From Fetus to Adult. Mohamed Hamdan, MD
 Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Pediatrics. Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment. Overview
 Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Case-Based Practical ECG Interpretation for the Generalist
 Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
PEDIATRIC SVT MANAGEMENT
 PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
Case #1. 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136
 Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Step by step approach to EKG rhythm interpretation:
 Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif
 2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
Anti arrhythmic drugs. Hilal Al Saffar College of medicine Baghdad University
 Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
Cardiac Arrhythmias. Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company
 Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
Paramedic Rounds. Tachyarrhythmia's. Sean Sutton Dallas Wood
 Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Sudden cardiac death: Primary and secondary prevention
 Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
Emergency treatment to SVT Evidence-based Approach. Tran Thao Giang
 Emergency treatment to SVT Evidence-based Approach Tran Thao Giang Description ECG manifestations: HR is extremely rapid and regular (240bpm ± 40) P wave is: usually invisible When visible: anormal P axis,
Emergency treatment to SVT Evidence-based Approach Tran Thao Giang Description ECG manifestations: HR is extremely rapid and regular (240bpm ± 40) P wave is: usually invisible When visible: anormal P axis,
CRC 431 ECG Basics. Bill Pruitt, MBA, RRT, CPFT, AE-C
 CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
EKG Abnormalities. Adapted from:
 EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
CSI Skills Lab #5: Arrhythmia Interpretation and Treatment
 CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
Arrhythmic Complications of MI. Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine
 Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD
 Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
physiology 6 Mohammed Jaafer Turquoise team
 15 physiology 6 Mohammed Jaafer 22-3-2016 Turquoise team Cardiac Arrhythmias and Their Electrocardiographic Interpretation Today, we are going to talk about the abnormal excitation. As we said before,
15 physiology 6 Mohammed Jaafer 22-3-2016 Turquoise team Cardiac Arrhythmias and Their Electrocardiographic Interpretation Today, we are going to talk about the abnormal excitation. As we said before,
Review Packet EKG Competency This packet is a review of the information you will need to know for the proctored EKG competency test.
 Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
ECGs and Arrhythmias: Family Medicine Board Review 2009
 Rate Rhythm Intervals Hypertrophy ECGs and Arrhythmias: Family Medicine Board Review 2009 Axis Jess (Fogler) Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Ischemia Overview
Rate Rhythm Intervals Hypertrophy ECGs and Arrhythmias: Family Medicine Board Review 2009 Axis Jess (Fogler) Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Ischemia Overview
Huseng Vefali MD St. Luke s University Health Network Department of Cardiology
 Huseng Vefali MD St. Luke s University Health Network Department of Cardiology Learning Objectives Establish Consistent Approach to Interpreting ECGs Review Essential Cases for Paramedics and first responders
Huseng Vefali MD St. Luke s University Health Network Department of Cardiology Learning Objectives Establish Consistent Approach to Interpreting ECGs Review Essential Cases for Paramedics and first responders
Cardiac arrhythmias. Janusz Witowski. Department of Pathophysiology Poznan University of Medical Sciences. J. Witowski
 Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT
 Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Ventricular Preexcitation (Wolff-Parkinson-White Syndrome and Its Variants) 柯文欽醫師 國泰綜合醫院心臟內科主治醫師 臺北醫學大學講師
 Ventricular Preexcitation (Wolff-Parkinson-White Syndrome and Its Variants) 柯文欽醫師 國泰綜合醫院心臟內科主治醫師 臺北醫學大學講師 The Nobel Prize in Physiology or Medicine 1924 "for his discovery of the mechanism of the electrocardiogram"
Ventricular Preexcitation (Wolff-Parkinson-White Syndrome and Its Variants) 柯文欽醫師 國泰綜合醫院心臟內科主治醫師 臺北醫學大學講師 The Nobel Prize in Physiology or Medicine 1924 "for his discovery of the mechanism of the electrocardiogram"
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
Patient Resources: Arrhythmias and Congenital Heart Disease
 Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
PhD FRCP MESC MEAPCI. Consultant Cardiologist SVT - Supra Ventricular Tachycardia. Coronary Arteries
 SVT - Supra Ventricular Tachycardia Coronary Arteries Overview LMS Supraventricular tachycardia is defined as an abnormally fast heartbeat. It's a describes a group of arrhythmias which all originate from
SVT - Supra Ventricular Tachycardia Coronary Arteries Overview LMS Supraventricular tachycardia is defined as an abnormally fast heartbeat. It's a describes a group of arrhythmias which all originate from
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
The ABCs of EKGs/ECGs for HCPs. Al Heuer, PhD, MBA, RRT, RPFT Professor, Rutgers School of Health Related Professions
 The ABCs of EKGs/ECGs for HCPs Al Heuer, PhD, MBA, RRT, RPFT Professor, Rutgers School of Health Related Professions Learning Objectives Review the basic anatomy of the heart Describe the cardiac conducting
The ABCs of EKGs/ECGs for HCPs Al Heuer, PhD, MBA, RRT, RPFT Professor, Rutgers School of Health Related Professions Learning Objectives Review the basic anatomy of the heart Describe the cardiac conducting
The most common. hospitalized patients. hypotension due to. filling time Rate control in ICU patients may be difficult as many drugs cause hypotension
 Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
TACHYARRHYTHMIAs. Pawel Balsam, MD, PhD
 TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
Problems in Pediatrics: Pediatric Cardiology Cases
 Problems in Pediatrics: Pediatric Cardiology Cases Kristin C. Lombardi, M.D. Assistant Professor of Pediatrics, Clinical Educator The Warren Alpert Medical School of Brown University Pediatric Cardiologist,
Problems in Pediatrics: Pediatric Cardiology Cases Kristin C. Lombardi, M.D. Assistant Professor of Pediatrics, Clinical Educator The Warren Alpert Medical School of Brown University Pediatric Cardiologist,
EKG Competency for Agency
 EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
ECG Interpretation Made Easy
 ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
a lecture series by SWESEMJR
 Arrhythmias Automaticity- the ability to depolarize spontaneously. Pacemakers: Sinoatrial node: 70 bpm AV-nodal area: 40 bpm His-Purkinje: 20-40 bpm it Mechanisms of arrhythmias 1. Increased automaticity
Arrhythmias Automaticity- the ability to depolarize spontaneously. Pacemakers: Sinoatrial node: 70 bpm AV-nodal area: 40 bpm His-Purkinje: 20-40 bpm it Mechanisms of arrhythmias 1. Increased automaticity
Core Content In Urgent Care Medicine
 Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Cardiology Flash Cards
 Cardiology Flash Cards EKG in a nut shell www.brain101.info Conduction System www.brain101.info 2 Analyzing EKG Step by step Steps in Analyzing ECG'S 1. Rhythm: - Regular _ Sinus, Junctional or Ventricular.
Cardiology Flash Cards EKG in a nut shell www.brain101.info Conduction System www.brain101.info 2 Analyzing EKG Step by step Steps in Analyzing ECG'S 1. Rhythm: - Regular _ Sinus, Junctional or Ventricular.
Dr. Schroeder has no financial relationships to disclose
 Valerie A Schroeder MD MS Assistant Professor University of Kansas Medical Center READING THE WAVES- THE HEART S ELECTRICAL MESSAGE FINANCIAL DISCLOSURE Dr. Schroeder has no financial relationships to
Valerie A Schroeder MD MS Assistant Professor University of Kansas Medical Center READING THE WAVES- THE HEART S ELECTRICAL MESSAGE FINANCIAL DISCLOSURE Dr. Schroeder has no financial relationships to
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 5: Rhythm Strip Interpretation and Sinus Rhythms Learning Outcomes 5.1 Explain the process of evaluating ECG tracings
Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 5: Rhythm Strip Interpretation and Sinus Rhythms Learning Outcomes 5.1 Explain the process of evaluating ECG tracings
Rhythm ECG Characteristics Example. Normal Sinus Rhythm (NSR)
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Substances
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Substances
Sustained tachycardia with wide QRS
 Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
BEDSIDE ECG INTERPRETATION
 BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
Clinical Cardiac Electrophysiology
 Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Electrocardiography Abnormalities (Arrhythmias) 7. Faisal I. Mohammed, MD, PhD
 Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
ECG Basics Sonia Samtani 7/2017 UCI Resident Lecture Series
 ECG Basics Sonia Samtani 7/2017 UCI Resident Lecture Series Agenda I. Introduction II.The Conduction System III.ECG Basics IV.Cardiac Emergencies V.Summary The Conduction System Lead Placement avf Precordial
ECG Basics Sonia Samtani 7/2017 UCI Resident Lecture Series Agenda I. Introduction II.The Conduction System III.ECG Basics IV.Cardiac Emergencies V.Summary The Conduction System Lead Placement avf Precordial
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology
 EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
Dysrhythmias: Diagnosis and management
 15 Dysrhythmias: Diagnosis and management Wanda C. Miller-Hance Kathryn K. Collins Introduction The practice of pediatric cardiac anesthesia has evolved significantly over the years, expanding beyond the
15 Dysrhythmias: Diagnosis and management Wanda C. Miller-Hance Kathryn K. Collins Introduction The practice of pediatric cardiac anesthesia has evolved significantly over the years, expanding beyond the
APPROACH TO TACHYARRYTHMIAS
 APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
Dr.Binoy Skaria 13/07/15
 Dr.Binoy Skaria binoyskaria@hotmail.com binoy.skaria@heartofengland.nhs.uk 13/07/15 Acknowledgement Medtronic, Google images & Elsevier for slides Natalie Ryan, Events Manager, HEFT- for organising the
Dr.Binoy Skaria binoyskaria@hotmail.com binoy.skaria@heartofengland.nhs.uk 13/07/15 Acknowledgement Medtronic, Google images & Elsevier for slides Natalie Ryan, Events Manager, HEFT- for organising the
Ventricular Tachycardia Basics
 Ventricular Tachycardia Basics OVERVIEW Ventricular refers to the ventricles of the heart; tachycardia is the medical term for rapid heart rate The heart of the dog or cat is composed of four chambers;
Ventricular Tachycardia Basics OVERVIEW Ventricular refers to the ventricles of the heart; tachycardia is the medical term for rapid heart rate The heart of the dog or cat is composed of four chambers;
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES
 UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
Arrhythmia 341. Ahmad Hersi Professor of Cardiology KSU
 Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
Wolff-Parkinson-White Syndrome
 Wolff-Parkinson-White Syndrome www.consultant360.com /articles/wolff-parkinson-white-syndrome A 37-year-old woman presented to the office with intermittent dizziness, palpitations, and multiple syncopal
Wolff-Parkinson-White Syndrome www.consultant360.com /articles/wolff-parkinson-white-syndrome A 37-year-old woman presented to the office with intermittent dizziness, palpitations, and multiple syncopal
Rate: The atrial and ventricular rates are equal; heart rate is greater than 100 bpm (usually between bpm).
 Sinus Bradycardia Regularity: The R-R intervals are constant; the rhythm is regular. Rate: The atrial and ventricular rates are equal; heart rate is less than 60 bpm. P wave: There is a uniform P wave
Sinus Bradycardia Regularity: The R-R intervals are constant; the rhythm is regular. Rate: The atrial and ventricular rates are equal; heart rate is less than 60 bpm. P wave: There is a uniform P wave
SIMPLY ECGs. Dr William Dooley
 SIMPLY ECGs Dr William Dooley Content Basic ECG interpretation pattern Some common (examined) abnormalities Presenting ECGs in context Setting up an ECG Setting up an ECG 1 V1-4 th Right intercostal space
SIMPLY ECGs Dr William Dooley Content Basic ECG interpretation pattern Some common (examined) abnormalities Presenting ECGs in context Setting up an ECG Setting up an ECG 1 V1-4 th Right intercostal space
Practical Approach to Arrhythmias
 Outline Practical Approach to Arrhythmias Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Conduction System ECG Acquisition ECG Interpretation Heart rate Rhythm Arrhythmias Tachyarrhythmias Supraventricular
Outline Practical Approach to Arrhythmias Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Conduction System ECG Acquisition ECG Interpretation Heart rate Rhythm Arrhythmias Tachyarrhythmias Supraventricular
Introduction. Pediatric Cardiology. General Appearance. Tools of Assessment. Auscultation. Vital Signs
 Introduction Pediatric Cardiology An introduction to the pediatric patient with heart disease: M-III Lecture Douglas R. Allen, M.D. Assistant Professor and Director of Community Pediatric Cardiology at
Introduction Pediatric Cardiology An introduction to the pediatric patient with heart disease: M-III Lecture Douglas R. Allen, M.D. Assistant Professor and Director of Community Pediatric Cardiology at
Course Objectives. Proper Lead Placements. Review the ECG print paper. Review the mechanics of the Myocardium. Review basics of ECG Rhythms
 ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
ECGs and Arrhythmias: Family Medicine Board Review 2012
 Overview ECGs and Arrhythmias: Family Medicine Board Review 2012 Jess Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Bundle branch blocks Quick review of ischemia Arrhythmias
Overview ECGs and Arrhythmias: Family Medicine Board Review 2012 Jess Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Bundle branch blocks Quick review of ischemia Arrhythmias
Conduction Problems / Arrhythmias. Conduction
 Conduction Problems / Arrhythmias Conduction Wolf-Parkinson White Syndrome (WPW) and Lown-Ganong-Levine (LGL): Atrial impulses bypass the AV node through an accessory pathway or bypass tract (bundle of
Conduction Problems / Arrhythmias Conduction Wolf-Parkinson White Syndrome (WPW) and Lown-Ganong-Levine (LGL): Atrial impulses bypass the AV node through an accessory pathway or bypass tract (bundle of
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Evaluation and Initial Treatment of Supraventricular Tachycardia
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e clinical practice Evaluation and Initial Treatment of Supraventricular Tachycardia Mark S. Link, M.D. This Journal feature begins with a case vignette
T h e n e w e ngl a nd j o u r na l o f m e dic i n e clinical practice Evaluation and Initial Treatment of Supraventricular Tachycardia Mark S. Link, M.D. This Journal feature begins with a case vignette
WOLFF PARKINSON WHITE SYNDROME. Katarzyna Bigaj PGY-1
 WOLFF PARKINSON WHITE SYNDROME Katarzyna Bigaj PGY-1 Preexcitation is defined as a premature activation of the ventricular myocardium by an impulse that travels by an anomalous path and avoids physiologic
WOLFF PARKINSON WHITE SYNDROME Katarzyna Bigaj PGY-1 Preexcitation is defined as a premature activation of the ventricular myocardium by an impulse that travels by an anomalous path and avoids physiologic
Chapter 26. Media Directory. Dysrhythmias. Diagnosis/Treatment of Dysrhythmias. Frequency in Population Difficult to Predict
 Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Electrical System Overview Electrocardiograms Action Potentials 12-Lead Positioning Values To Memorize Calculating Rates
 Electrocardiograms Electrical System Overview James Lamberg 2/ 74 Action Potentials 12-Lead Positioning 3/ 74 4/ 74 Values To Memorize Inherent Rates SA: 60 to 100 AV: 40 to 60 Ventricles: 20 to 40 Normal
Electrocardiograms Electrical System Overview James Lamberg 2/ 74 Action Potentials 12-Lead Positioning 3/ 74 4/ 74 Values To Memorize Inherent Rates SA: 60 to 100 AV: 40 to 60 Ventricles: 20 to 40 Normal
Please check your answers with correct statements in answer pages after the ECG cases.
 ECG Cases ECG Case 1 Springer International Publishing AG, part of Springer Nature 2018 S. Okutucu, A. Oto, Interpreting ECGs in Clinical Practice, In Clinical Practice, https://doi.org/10.1007/978-3-319-90557-0
ECG Cases ECG Case 1 Springer International Publishing AG, part of Springer Nature 2018 S. Okutucu, A. Oto, Interpreting ECGs in Clinical Practice, In Clinical Practice, https://doi.org/10.1007/978-3-319-90557-0
Patient Examination. Objectives for Presentation RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS 9/8/2016
 RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS Ryan Fries, DVM, DACVIM (Cardiology) Clinical Assistant Professor University of Illinois Department of Clinical Veterinary Medicine
RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS Ryan Fries, DVM, DACVIM (Cardiology) Clinical Assistant Professor University of Illinois Department of Clinical Veterinary Medicine
WPW syndrome and AVRT
 WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
3. AV Block 1. First-degree AV block 1. Delay in AV node 2. Long PR interval 3. QRS complex follows each P wave 4. Benign, no tx
 1. Rhythms & arrhythmias SA nodal rhythms Sinus rhythm Sinus tachycardia Sinus bradycardia Sinus arrhythmia Sick sinus syndrome SA block Sinus arrest AV blocks First-degree Second-degree Mobitz Type I
1. Rhythms & arrhythmias SA nodal rhythms Sinus rhythm Sinus tachycardia Sinus bradycardia Sinus arrhythmia Sick sinus syndrome SA block Sinus arrest AV blocks First-degree Second-degree Mobitz Type I
CORONARY ARTERIES. LAD Anterior wall of the left vent Lateral wall of left vent Anterior 2/3 of interventricluar septum R & L bundle branches
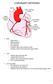 CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
the ECG, 6 mg of intravenous adenosine was administered as a fast bolus through a large bore intravenous cannula in
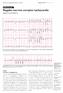 (arrows). Electrocardiography Series Singapore Med.1 2011, 52(3) 146 CME Article Regular narrow complex tachycardia Singh D, Teo S G, Poh K K V Hr JL1 11 VL VF WA, Fig. I ECG shows regular narrow complex
(arrows). Electrocardiography Series Singapore Med.1 2011, 52(3) 146 CME Article Regular narrow complex tachycardia Singh D, Teo S G, Poh K K V Hr JL1 11 VL VF WA, Fig. I ECG shows regular narrow complex
ECGs: Everything a finalist needs to know. Dr Amy Coulden As part of the Simply Finals series
 ECGs: Everything a finalist needs to know Dr Amy Coulden As part of the Simply Finals series Aims and objectives To be able to interpret basic ECG abnormalities To be able to recognise commonly tested
ECGs: Everything a finalist needs to know Dr Amy Coulden As part of the Simply Finals series Aims and objectives To be able to interpret basic ECG abnormalities To be able to recognise commonly tested
HTEC 91. Performing ECGs: Procedure. Normal Sinus Rhythm (NSR) Topic for Today: Sinus Rhythms. Characteristics of NSR. Conduction Pathway
 HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
Chapter 03: Sinus Mechanisms Test Bank MULTIPLE CHOICE
 Instant download and all chapters Tesst Bank ECGs Made Easy 5th Edition Barbara J Aehlert https://testbanklab.com/download/tesst-bank-ecgs-made-easy-5th-edition-barbara-jaehlert/ Chapter 03: Sinus Mechanisms
Instant download and all chapters Tesst Bank ECGs Made Easy 5th Edition Barbara J Aehlert https://testbanklab.com/download/tesst-bank-ecgs-made-easy-5th-edition-barbara-jaehlert/ Chapter 03: Sinus Mechanisms
Catheter Ablation for Supraventricular Tachycardias
 Catheter Ablation for Supraventricular Tachycardias - A Patient's Guide - Westby G. Fisher, MD, FACC Director, Cardiac Electrophysiology Evanston Northwesten Healthcare Evanston, IL, USA (Last Updated
Catheter Ablation for Supraventricular Tachycardias - A Patient's Guide - Westby G. Fisher, MD, FACC Director, Cardiac Electrophysiology Evanston Northwesten Healthcare Evanston, IL, USA (Last Updated
HR: 50 bpm (Sinus) PR: 280 ms QRS: 120 ms QT: 490 ms Axis: -70. Sinus bradycardia with one ventricular escape (*)
 1? HR: 50 bpm (Sinus) PR: 280 ms QRS: 120 ms QT: 490 ms Axis: -70 1 Sinus P waves? 2 sinus cycles The pause (2 sinus cycles) suggests that the sinus fired (?) but did not conduct to the atria (i.e., missing
1? HR: 50 bpm (Sinus) PR: 280 ms QRS: 120 ms QT: 490 ms Axis: -70 1 Sinus P waves? 2 sinus cycles The pause (2 sinus cycles) suggests that the sinus fired (?) but did not conduct to the atria (i.e., missing
ECG Interpretation Cat Williams, DVM DACVIM (Cardiology)
 ECG Interpretation Cat Williams, DVM DACVIM (Cardiology) Providing the best quality care and service for the patient, the client, and the referring veterinarian. GOAL: Reduce Anxiety about ECGs Back to
ECG Interpretation Cat Williams, DVM DACVIM (Cardiology) Providing the best quality care and service for the patient, the client, and the referring veterinarian. GOAL: Reduce Anxiety about ECGs Back to
SIMPLY ECGs. Dr William Dooley
 SIMPLY ECGs Dr William Dooley 1 No anatomy just interpretation 2 Setting up an ECG 3 Setting up an ECG 1 V1-4 th Right intercostal space at sternal border 2 V2-4 th Left intercostal space at sternal border
SIMPLY ECGs Dr William Dooley 1 No anatomy just interpretation 2 Setting up an ECG 3 Setting up an ECG 1 V1-4 th Right intercostal space at sternal border 2 V2-4 th Left intercostal space at sternal border
Cardiac Telemetry Self Study: Part One Cardiovascular Review 2017 THINGS TO REMEMBER
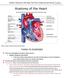 Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
I have nothing to disclose.
 I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
Catheter Ablation. Patient Education
 Catheter Ablation Patient Education Allina Health System Your heart has four chambers. Two upper chambers (atria) pump blood to the two lower chambers (ventricles). In order for the heart to pump, it requires
Catheter Ablation Patient Education Allina Health System Your heart has four chambers. Two upper chambers (atria) pump blood to the two lower chambers (ventricles). In order for the heart to pump, it requires
REtrive. REpeat. RElearn Design by. Test-Enhanced Learning based ECG practice E-book
 Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Atrial Fibrillation 10/2/2018. Depolarization & ECG. Atrial Fibrillation. Hemodynamic Consequences
 Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Chest Pain. Dr. Amitesh Aggarwal. Department of Medicine
 Chest Pain Dr. Amitesh Aggarwal Department of Medicine BACKGROUND Approx 5% of all ED visits 15 % - AMI 25-30 % - Unstable angina 50-55 % - Other conditions Atypical presentations common 2% of patients
Chest Pain Dr. Amitesh Aggarwal Department of Medicine BACKGROUND Approx 5% of all ED visits 15 % - AMI 25-30 % - Unstable angina 50-55 % - Other conditions Atypical presentations common 2% of patients
Lecture outline. Electrical properties of the heart. Automaticity. Excitability. Refractoriness. The ABCs of ECGs Back to Basics Part I
 Lecture outline The ABCs of ECGs Back to Basics Part I Meg Sleeper VMD, DACVIM (cardiology) University of Florida Veterinary School Electrical properties of the heart Action potentials Normal intracardiac
Lecture outline The ABCs of ECGs Back to Basics Part I Meg Sleeper VMD, DACVIM (cardiology) University of Florida Veterinary School Electrical properties of the heart Action potentials Normal intracardiac
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University. OBHG Education Subcommittee
 -RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
Pathological Arrhythmias/ Tachyarrhythmias
 Pathological Arrhythmias/ Tachyarrhythmias caused by: 1.Ectopic focus: Extrasystole or premature beat. If discharge is occasional. Can be: Atrial Extrasystole Vevtricular Extrasystole 2.Cardiac Arrhythmia
Pathological Arrhythmias/ Tachyarrhythmias caused by: 1.Ectopic focus: Extrasystole or premature beat. If discharge is occasional. Can be: Atrial Extrasystole Vevtricular Extrasystole 2.Cardiac Arrhythmia
EKG Rhythm Interpretation Exam
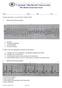 as EKG Rhythm Interpretation Exam Name: Date: ID# Unit Assume each strip is a 6 second strip. Passing is 80%. 1. Identify the following rhythm: a. Asystole b. Ventricular fibrillation c. Atrial fibrillation
as EKG Rhythm Interpretation Exam Name: Date: ID# Unit Assume each strip is a 6 second strip. Passing is 80%. 1. Identify the following rhythm: a. Asystole b. Ventricular fibrillation c. Atrial fibrillation
Chad Morsch B.S., ACSM CEP
 What Is Cardiac Stress Testing? Chad Morsch B.S., ACSM CEP A Cardiac Stress Test is a test used to measure the heart's ability to respond to external stress in a controlled clinical environment. Cardiac
What Is Cardiac Stress Testing? Chad Morsch B.S., ACSM CEP A Cardiac Stress Test is a test used to measure the heart's ability to respond to external stress in a controlled clinical environment. Cardiac
