TEMPORARY PACEMAKERS HINTS ( DUAL CHAMBER 5392 PACER)
|
|
|
- Sheryl Walters
- 6 years ago
- Views:
Transcription
1 TEMPORARY PACEMAKERS HINTS ( DUAL CHAMBER 5392 PACER) TYPES OF PACERS TRANSCUTANEOUS: ( VENTRICULAR pacing only) Through the skin via gel electrode pads placed on the chest and back. Disadvantage: Pain / discomfort Potential loss of capture with movement or sweating TRANSVENOUS: ( VENTRICULAR pacing only) Electrode wires placed via 6 Fr introducer through the subclavian or intrajugular vein: The wire is threaded through the R atrium into the R ventricle where it is in contact with the endocardial layer of the heart. Temporary: until a permanent pacer is placed or dysrhythmia is corrected May also be through a specialized Swanz Ganz catheter (PACING SWAN) EPICARDIAL (TRANSTHORACIC) : Wires are placed on the epicardial surface of the heart during surgery Atrial, Ventricular, and AV Sequential pacing possible. RIGHT wires are always ATRIAL LEFT wire are always VENTRICULAR PERMANENT: implanted subcutaneously : usually has 2 leads and poles. CARE OF PATIENT with NEW PERMANENT PACER 1) Restrict limb movement for hours 5) Medic alert bracelet 2) No shower or bath for 48 hours 6) Activity intolerance may still be present regardless of the new pacer 3) Teach & observe site for bleeding and infection 7) Avoid electromagnetic interference: MRI, hand wands at airports, electrolysis. 4) Monitor VS and teach accurate pulse taking 8) Avoid constrictive clothing over the pacer site. WHAT DO THE LETTERS MEAN? 1st letter: the chamber PACED 2ND letter: the chamber SENSED 3RD letter: what happens when pacer senses the beat 4TH letter : Programmability 5TH letter: Antitachycardia functions (These are not applicable to temporary pacers) A = Atrial V = Ventricle D = Dual I = INHIBIT T = TRIGGER ( both A & V are sensed but if no QRS follows the P wave within a certain time interval, then the V will be paced) Mode Paced Sensed Result AAI Atrial Atrial Inhibits AOO Asynchronous Atrial VVI Ventricular Ventricular Inhibits VOO Asynchronous Ventricular DVI A & V Ventricle Inhibits DOO Asynchronous A & V DDD mode: Atrial (Pwave) sensed = Inhibition ( pacer does not fire ) Atrial (Pwave) Not sensed = Trigger : pacer fires an atrial spike If AV conduction is normal If QRS is sensed = Inhibition ( V pacer spike does not fire ) If QRS is NOT sensed ( absent or delayed) = Trigger : pacer fires a ventricular spike An upper rate is set for the ventricular response to avoid tracking rapid atrial activity. ( Menu 2) 1
2 INDICATIONS FOR PACING * symptomatic bradycardia (low BP, low CO, syncope) * advanced heart blocks or conduction disturbances (pauses) * ventricular dysrhythmias * absence of underlying rhythm * overdrive pacing attempts to terminate malignant supraventricular and ventricular dysrhythmias If an open heart patient becomes 2 bradycardic and still has their epicardial / transthoracic.. CONNECT & START THE TEMPORARY PACER 1 ST! Don t wait! The heart has 2 separate mechanism: ELECTRICAL: deals ONLY with the stimulus and CONDUCTION system within the heart. (depolarization) MECHANICAL: is the actual CONTRACTION of the muscle (the heart beat and movement of blood!) REMEMBER: conduction can still happen even if the mechanical heart beat does not. PULSELESS ELECTRICAL ACTIVITY (the pt has no pulse) PACER CONTROLS RATE: normally *the number of impulses per minute the pulse generator may send, depending upon chosen mode. OUTPUT: The amount of energy that the pacer sends to the heart. Measured in milliamps. m A: milliamps (measurement of current) low.5-20 high CAPTURE: The heart s response to the pacer by DEPOLARIZING ( + a pulse ) the cardiac muscle responds to the electrical stimulus. Atrial output Ventricular Output 2
3 3 STIMULATION THRESHOLD: The minimal amount of energy needed to stimulate depolarization. 1) Set the ma to a low number 2) Dial up the ma until capture is obtained (spike followed by depolarization/capture + pulse ) 3) Then ADD 2 ( to make sure you keep the capture! ) or Some physicians prefer to start at ma 20 then dial down until you loose capture : but always ADD 2 LOSS OF CAPTURE WHAT S THE PROBLEM??? 1) the PACER 2) the WIRES 3) the PATIENT PROBLEM PACER Batteries Faulty generator WIRES Dislodged Disconnected Damaged Transvenous wire not touching the heart tissue PATIENT Heart tissue is refractory Electrolyte imbalance MI, ischemia, hypertrophy Severe acidosis, hypoxemia TO CORRECT THE PROBLEM Change the batteries Change the pacer Check the wires Check the connections Changing position of the patient (on to side ) For transvenous pacer INCREASE the ma Correct 02 or acid imbalance Initiate CPR if necessary. A V INTERVAL Amount of time between the atrial spike (stimulus) and the ventricular spike in AV Sequential pacing 120 to 200 msec normal measured in millisecs (like the PR interval in secs) Promote adequate ventricular filling from atrial kick 3 1) Scroll to select AV interval 2) Press ENTER AV Interval changes automatically when pacer rate is changed Rarely is this manually changed
4 SENSITIVITY The pacer's ability to "sense" or "see" the pt's intrinsic heart beat When the pacer senses the intrinsic beat it INHIBITS the pacer (It should not fire) REMEMBER the T wave is the most vulnerable wave of the cycle. A stimulus sent when the heart is repolarizing can cause V FIB (R on T phenomenon) The higher the number the lower the sensitivity The lower the number the higher the sensitivity HIGH # [20] = LOW sensitivity Problem: UNDERSENSING Pacer does not sense an intrinsic beat so it fires a stimulus. UNDERSENSING OVERPACING! DANGER: a stimulus hits the R wave = R on T lead to V fib LOW # [.5] = HIGH sensitivity Problem: OVERSENSING ; Too sensitive Pacer senses everything and thinks it is a beat: hiccups, outside electrical interference, IV pumps, electric razors OVERSENSING UNDERPACING DANGER: the pacer will NOT fire even when you need it to! DEMAND PACING Uses Sensitivity to determine when to fire and NOT to fire. Pacer delivers stimulus ONLY IF the patient's heart fails to fire as fast as the predetermined rate (the distance between R-R interval is timed) EXAMPLE: Demand pacer is set at rate of 72 The white arrow illustrates the pacing interval ( the distance from spike to spike) The pacer MUST wait this long before it fires another stimulus If the pacer senses a beat before the end of the interval: it should not fire QRS was sensed: Pacer DID NOT fire! OVERSENSING UNDERPACING Picks up Hiccups! DOES NOT FIRE WHEN YOU NEED IT TO! = ASYSTOLE 4 UNDERSENSING OVERPACING DOESN T SEE DOESN T CARE FIRES ANYWAY! R on T V fib
5 5 DEMAND MODE: DOO button works even if the controls are locked or the pacer is OFF If the pacer is OFF: the DOO button will turn the pacer ON & activate Asynchronous mode [This is a quick way in an emergent situation: to turn on the pacer / ma goes to max to get capture / press to immediately get your sensitivity back! TO SET SENSITIVITY (PHYSICIAN ONLY ) Position dial at MOST sensitive setting (1mV) Adjust pacer rate to 10 less than pt intrinsic rate Reduce ma to minimum (to prevent pacer from competing with intrinsic rhythm Turn the sensitivity dial counterclockwise (higher mv) until: VENT. SENSE (orange light) stops flashing and VENT. PACE (green light) starts flashing (This is sensitivity threshold) Adjust the sensitivity indicator to half threshold value RESET THE ma and RATE TO THEIR ORIGINAL SETTINGS! 5
6 Connection / Adapter Cables are REQUIRED: 6 Connecting the Pacer: Transthoracic pacing wires: 2 wires coming out of the Right side of the chest are connected to the ATRIA 2 wires coming out of the Left side of the chest are connected to the VENTRICLE ATRIAL PACING: [AAI mode] Can be used when conduction system of the heart beyond the SA node is normal. USES: [the pacer is only stimulating a p wave: the QRS must follow from the heart!] Sinus Bradycardia symptomatic Sick Sinus Syndrome Sinus Arrythmia Sinus Rhythm: Higher heart rate to increase cardiac output (better perfusion) Junctional Rhythm may work R L 1) Attach the 2 Right (atrial wires) to the extension cable marked ATRIAL on top of the pacer. 2) Turn the Ventricle ma to 0 this will give you atrial pacing only [You can also scroll down to the bottom of the screen / choose Mode Selection Press Scroll to AAI mode Press Rhythm: spike will be followed by P wave then normal width QRS 6
7 VENTRICULAR PACING: [VVI mode ] 7 Stimulates ONLY the ventricles only. Disadvantages: 1. No atrial kick if patient does not have their own intrinsic p waves Atrial kick is % of cardiac output decreased cardiac output 2. Thrombus -no atrial contraction => blood clot in the atrium TO VENTRICULAR PACE with Epicardial Wires 1. Place the 2 left VENTRICULAR wires into the ventricular poles 2. Set the pacer rate 3. Turn the Atrial ma to 0 (off) 4. Set the Ventriclar ma (Stimulation threshold +2) [This can also be accomplished: Scroll to bottom of screen Choose Mode Selection Ventricular Pacing Rhythm: spike will be followed by a widened QRS. (wider because the conduction through the ventricles is slower) The atrium will not be stimulated by the pacer. 7
8 AV SEQUENTIAL PACING: Stimulates the atria then the ventricles in sequence Advantage: Atrial kick for better cardiac output and perfusion. 8 TO AV SEQUENTIAL PACE 1) Place patient's right wires into the atrial ( blue ) poles Place patient's left wires into the ventricle (white) poles 2) Set the Rate 3) Check the AV interval This is preset by the dual chamber pacer and does not need to be changed. Measured in millisecs ( correlates with PR interval ) 4) Set the atrial and ventricular ma (stimulation threshold + 2) RAPID ATRIAL PACING Used to overdrive the ATRIA out of rhythms with rapid atrial rates ( A fib and A flutter ) NEVER use this with Ventricular only Pacing 1. Press to open the menu 2. Press \/ arrow to Scroll down to Rapid Atrial Pacing 3. Press to select 4. Set the rate at which you want the ATRIA to be stimulated with turn knob Example A flutter : atrial rate is usually between A- Fib : atrial rate is usually Press and HOLD the RAP button 6. The atrial pacer will continue to fire at the rapid rate until you release the button. During A-V Sequential Pacing Activating RAP disables the Ventricular Rate and Ventricular ma so only the Atrial stimulus goes through Technique of Overdrive Pacing for Atrial Flutter ( Smith and Hood 2007) When two atrial epicardial wires are in situ, each wire should be tested to confirm that it is recording only an atrial ECG and to measure the atrial rate. The pacing pulse width should be increased to 2ms and pacing begun at 20mA at 100 beats per minute to confirm the absence of ventricular capture. The pacing rate should be increased to 20 beats faster than the intrinsic atrial rate ( typical atrial rates are bpm and may be as high as 330bpm) The ECG should be observed to confirm atrial capture. After 30 seconds the pacing rate should be increased by a further 20 bpm. Atrial capture is confirmed by 1) an increase in HR as the pacing rate is increased. 2) a subsequent abrupt fall in hear rate as the AV conduction ratio increases ( 2:1 to 3:1 to 4:1 ) 3) a constant relationship between the pacing spikes and the flutter wave. Pacing is abruptly stopped after 1 2 minutes of atrial capture. Which typically results in the establishment of sinus rhythm. If sinus rhythm is not present the process should be repeated after reversal of the atrial lead polarity. If it is still unsuccessful, deliberate induction of atrial fibrillation should be attempted by burst pacing at rates of 600 per minute for 30 seconds or until Afib wnsues. Pacing induced atrial fibrillation is typically unstable and frequently reverts spontaneously to sinus rhythm, though reorganization of atrial flutter is possible. 8
9 SAFETY TIPS FOR TEMPORARY PACERS 9 CONTROLS Lock 60 seconds after last adjustment was made. when not manipulating pacer setting : to avoid patient tampering. ( lock automatically engages ) Press and hold the lock button the middle right corner of the pacer SECURE THE PACER FOR MOBILE PATIENT: Secure pacer box to the patient using the "pacer pouch" with straps securely fastened around patient neck. (Make sure you do not impede blood flow to their head!) DO NOT PUT TAPE DIRECTLY ON THE FACE OF THE PACER!!!! Use the hooks located on the back of the pacer when securing the pacer The adhesive gets into the dials making them difficult to adjust. SECURE THE WIRES Wear gloves while securing transthoracic (epicardial) pacing wires in Preservative Free test tubes Tape the tubes to the chest. Secure transvenous pacing wires with a stress loop before taping to prevent wires from being dislodged if the pacer gets tugged. DO NOT PLACE TAPE ON THE PLASTIC SHEATH / COVER: The sheath / cover is placed ONLY to keep the wire sterile and DOES NOT prevent the wire from being pulled. Torn plastic cover = contaminated Change the Battery: Medtronic Pacer (2 AA Alkaline batteries) The New Medtronic pacer will flash a red battery picture When you change the battery the pacer will continue to pace for several seconds without battery. To change the battery 1. Push the button on the bottom of the pacer (looks like a belly button) 2. When the battery drawer pops out 3. Replace the battery just like the picture inside the battery drawer 4. Slide the battery door closed PREVENT MICROSHOCK AND ELECTRICAL INTERFERENCE Wear rubber gloves when handling pacer wires Use only a grounded electrical bed Allow pt only to use rechargeable electric razor or nonelectric razor Keep other electrical equipment off of the bed if possible. OTHER CAUSES OF ELECTRICAL INTERFERENCE: Electrocautery Defibrillation current Radiation therapy MRI devices TENS units (transcutaneous electrical nerve stimulation LESS COMMON BUT VERY REAL COMPLICATIONS OF TEMPORARY PACING WIRES Endocarditis Myocardial perforation Cardiac tamponade Infection Hiccups: dislodged wire touching diaphragm 9 Refernces: Medtronic Technical Manual Dual Chamber Temporary Pacemaker Thelan,Lynne, et al. Critical Care Nursing, Diagnosis and Management, 4 th Ediction, Mosby Corporation, Lynn-McHale, D. and Carlson, K.(2001) AACN Procedure Manual for Critical Care 4 th Ed. W.B. Saunders Company Philadelphia.
10 HINTS FOR FLOATING A TRANSVENOUS PACER 10 6F introducer placed via IJ or Subclav Prior to floating the pacer wire: place the plastic sheath over the pacer wire with the lock cap at the distal end. Once the wire is placed and capture is established: snap / lock the plastic sheath onto the introducer and stretch the plastic sheath several inches to maintain sterility of the pacer wire for repositioning. Do Not Put Tape over the plastic sheath! This will not secure the catheter Tearing will cause contamination Lock cap Secure transvenous pacing wires with a stress loop before taping to prevent wires from being dislodged if the pacer gets tugged. tape Transvenous Pacer Hints Sherri Welch ) Test the balloon by inflating with 1.5 cc 2) Connect the adapter cable to the Ventricular Pacer Port 3) Connect the pacer wires to adapter cable 10
11 11 Transvenous pacing use VVI Mode Only Do not use DDD mode. * Even if you only have the V wire connected the Atrial ma continues to fire * If the V connection senses the atrial ma The Ventricular ma will be inhibited [it will not fire] Floating the pacer wire (Elective) 1. Connect the Distal Negative (-) Electrode to the ECG Lead V 2. Continuously monitor the V lead on the bedside monitor 3. Pass the wire through the introducer to 20 cm. 4. Inflate the balloon 5. Advance the wire forward while observing the ECG tracing. 6. Look for ST elevation in the V lead This indicates the pacerwire is in contact with the myocardium (May see LBBB and L axis deviation) 7. Set / Check Stimulation Threshold Connect To ECG monitor Sherri Welch GWUH 2012 Ventricular Pacing Only acer wire (EMERGENT) tal to Negative ximal to positive ly monitor ECG on the nitor re through the introducer to alloon Connect To Pacer Connect Pacer 1. Pacer extension wire to Ventricular [V] pole 2. Connect Distal to Negative [Black] 3. Connect Proximal to Positive [Red] Continuous ECG Pass pacer wire through introducer to 20 cm [Maintain the catheter curve toward the heart Inflate balloon with 1.5 cc cer ensitivity to MD order E ASYNCH mode e wire forward while e ECG tracing. pacer spikes but ma 25 Sherri Welch GWUH 2012 Turn Pacer ON Set Rate per MD [must be higher than patient rate] Set Ventricular ma to 25 [Do not use ASYNCH mode] Advance pacer wire until Ventricular Capture [Spike followed by wide QRS + pulse] de QRS complex and a ing pulse. es the pacerwire is in the myocardium stimulation threshold Check the Stimulation Threshold [Minimal ma to capture then add 2mA] Secure / lock the plastic steri sleeve Document the depth of the catheter in cm 11
12 ICCUPS (if the pacer wires dislodge from the heart and rest on the diaphragm) 12 Sherri Welch MSN, RN, CCRN Temporary Pacer Hints 2018 Pacer Tips
13 13 To check sensitivity with the rhythm 1) Measure spike to spike [this is the pacing interval / timing] 2) Locate an Intrinsic [pt] beat. 3) When the pacer senses a beat; it should wait this long [pacing interval] after the beat before it fires again. 4) Failure to Sense: The pacer did not wait long enough to fire [X] if the pacer fires to soon the impulse could hit the T wave [R on T -> Vfib] 13
Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC
 Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC Pacemaker: An electric device implanted in the body to regulate the heart beat. Delivers electrical stimuli over leads with electrodes in contact
Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC Pacemaker: An electric device implanted in the body to regulate the heart beat. Delivers electrical stimuli over leads with electrodes in contact
Figure 2. Normal ECG tracing. Table 1.
 Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I
 1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 PROFESSIONAL NURSING PRACTICE CAN ONLY ADVANCE AS MUCH AS INDIVIDUAL
1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 PROFESSIONAL NURSING PRACTICE CAN ONLY ADVANCE AS MUCH AS INDIVIDUAL
SARASOTA MEMORIAL HOSPITAL
 SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE PACEMAKERS AND DETERMINING PACEMAKER DATE: REVIEWED: PAGES: 10/99 11/18 1 of 7 PS1094 ISSUED FOR: Nursing RESPONSIBILITY: *Qualified RN PURPOSE: To establish
SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE PACEMAKERS AND DETERMINING PACEMAKER DATE: REVIEWED: PAGES: 10/99 11/18 1 of 7 PS1094 ISSUED FOR: Nursing RESPONSIBILITY: *Qualified RN PURPOSE: To establish
Temporary pacemaker 삼성서울병원 심장혈관센터심장검사실 박정왜 RN, CCDS
 Temporary pacemaker 삼성서울병원 심장혈관센터심장검사실 박정왜 RN, CCDS NBG Codes 1st Letter 2nd Letter 3rd Letter A V D Chamber(s) Paced = atrium = ventricle = dual (both atrium and ventricle) Chamber(s) Sensed A = atrium
Temporary pacemaker 삼성서울병원 심장혈관센터심장검사실 박정왜 RN, CCDS NBG Codes 1st Letter 2nd Letter 3rd Letter A V D Chamber(s) Paced = atrium = ventricle = dual (both atrium and ventricle) Chamber(s) Sensed A = atrium
MODEL EPG SINGLE CHAMBER TEMPORARY EXTERNAL PACEMAKER
 MODEL 53401 EPG SINGLE CHAMBER TEMPORARY EXTERNAL PACEMAKER In-service Guide 53401 TRAINING LEARNING OBJECTIVES Identify the control knobs and be able to explain how to use them to program device. Distinguish
MODEL 53401 EPG SINGLE CHAMBER TEMPORARY EXTERNAL PACEMAKER In-service Guide 53401 TRAINING LEARNING OBJECTIVES Identify the control knobs and be able to explain how to use them to program device. Distinguish
Pediatric pacemakers & ICDs:
 Pediatric pacemakers & ICDs: perioperative management Manchula Navaratnam Clinical Assistant Professor LPCH, Stanford SPA 2016 Conflict of interest: none Objectives Indications in pediatrics Components
Pediatric pacemakers & ICDs: perioperative management Manchula Navaratnam Clinical Assistant Professor LPCH, Stanford SPA 2016 Conflict of interest: none Objectives Indications in pediatrics Components
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
Cardioversion / Defibrillation / Transcutaneous Pacer Helpful Hints [ZOLL] 2018
![Cardioversion / Defibrillation / Transcutaneous Pacer Helpful Hints [ZOLL] 2018 Cardioversion / Defibrillation / Transcutaneous Pacer Helpful Hints [ZOLL] 2018](/thumbs/81/84173335.jpg) Cardioversion / Defibrillation / Transcutaneous Pacer Helpful Hints [ZOLL] 08 4 Universal cable may be inserted to the side Defib Short Block to perform 0 J check Universal Cable must be connected to APEX
Cardioversion / Defibrillation / Transcutaneous Pacer Helpful Hints [ZOLL] 08 4 Universal cable may be inserted to the side Defib Short Block to perform 0 J check Universal Cable must be connected to APEX
TIP CARD. Model Temporary External Pacemaker
 TIP CARD Model 5392 Temporary External Pacemaker PRE-USE What to do... What NOT to do... Battery Replace the battery for each new patient. Do NOT reuse battery. Physical Check case for cracks/damage.**
TIP CARD Model 5392 Temporary External Pacemaker PRE-USE What to do... What NOT to do... Battery Replace the battery for each new patient. Do NOT reuse battery. Physical Check case for cracks/damage.**
Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO
 Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Follow me on Twitter! CEE Med Updates@BarbaraFurryRN Like me on Facebook! What is a
Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Follow me on Twitter! CEE Med Updates@BarbaraFurryRN Like me on Facebook! What is a
MONITORING PATIENTS WITH A TEMPORARY EXTERNAL EPICARDIAL PACEMAKER PURPOSE POLICY STATEMENTS SITE APPLICABILITY PRACTICE LEVEL/COMPETENCIES
 PURPOSE Guidelines for caring for and monitoring patients with a temporary external epicardial pacemaker. Epicardial pacemaker monitoring is performed on a continuous basis by a nurse to evaluate the effectiveness
PURPOSE Guidelines for caring for and monitoring patients with a temporary external epicardial pacemaker. Epicardial pacemaker monitoring is performed on a continuous basis by a nurse to evaluate the effectiveness
ΤΟ ΗΚΓ ΣΤΟΝ ΒΗΜΑΤΟΔΟΤΟΥΜΕΝΟ ΑΣΘΕΝΗ
 ΤΟ ΗΚΓ ΣΤΟΝ ΒΗΜΑΤΟΔΟΤΟΥΜΕΝΟ ΑΣΘΕΝΗ ΤΖΩΡΤΖ ΔΑΔΟΥΣ ΕΠΙΚΟΥΡΟΣ ΚΑΘΗΓΗΤΗΣ Α.Π.Θ. ΜΑΡΙΑ ΚΑΡΑΛΙΟΛΙΟΥ ΕΙΔΙΚΕΥΟΜΕΝΗ ΙΑΤΡΟΣ ΚΑΡΔΙΟΛΟΓΟΣ Β ΚΑΡΔΙΟΛΟΓΙΚΗ ΚΛΙΝΙΚΗ Α.Π.Θ. ΙΠΠΟΚΡΑΤΕΙΟ Γ.Ν.Θ. 5 Why a Pacemaker is Implanted
ΤΟ ΗΚΓ ΣΤΟΝ ΒΗΜΑΤΟΔΟΤΟΥΜΕΝΟ ΑΣΘΕΝΗ ΤΖΩΡΤΖ ΔΑΔΟΥΣ ΕΠΙΚΟΥΡΟΣ ΚΑΘΗΓΗΤΗΣ Α.Π.Θ. ΜΑΡΙΑ ΚΑΡΑΛΙΟΛΙΟΥ ΕΙΔΙΚΕΥΟΜΕΝΗ ΙΑΤΡΟΣ ΚΑΡΔΙΟΛΟΓΟΣ Β ΚΑΡΔΙΟΛΟΓΙΚΗ ΚΛΙΝΙΚΗ Α.Π.Θ. ΙΠΠΟΚΡΑΤΕΙΟ Γ.Ν.Θ. 5 Why a Pacemaker is Implanted
RN-BC, MS, CCRN, FAHA
 Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Follow me on Twitter! CEE Med Updates@BarbaraFurryRN Like me on Facebook! 1 A. Atropine
Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Follow me on Twitter! CEE Med Updates@BarbaraFurryRN Like me on Facebook! 1 A. Atropine
BEDSIDE ECG INTERPRETATION
 BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
Ass. Prof. Tomon Thongsri, MD Buddhachinaraj Phitsanuloke Hospital
 Treatment Bradyarrhythmia Ass. Prof. Tomon Thongsri, MD Buddhachinaraj Phitsanuloke Hospital 1 What is the rhythm? Sinus Bradycardia What s rhythm Sinus Bradycardia Treatment Asymptomatic No treatment
Treatment Bradyarrhythmia Ass. Prof. Tomon Thongsri, MD Buddhachinaraj Phitsanuloke Hospital 1 What is the rhythm? Sinus Bradycardia What s rhythm Sinus Bradycardia Treatment Asymptomatic No treatment
Title and contents page 1 Who should read this document 2 Scope of the Guideline 2 Background 2 What is new in this version 2
 Temporary Transvenous Pacing Guideline Classification: Clinical Guideline Lead Author: Dr Peter Woolfson Additional author(s): Dr Alan Fitchet Sister Joanne Hughes, Matron Julie Winstanley Authors Division:
Temporary Transvenous Pacing Guideline Classification: Clinical Guideline Lead Author: Dr Peter Woolfson Additional author(s): Dr Alan Fitchet Sister Joanne Hughes, Matron Julie Winstanley Authors Division:
The heart's "natural" pacemaker is called the sinoatrial (SA) node or sinus node.
 PACEMAKER Natural pacemaker: The heart's "natural" pacemaker is called the sinoatrial (SA) node or sinus node. Artificial pacemaker: It is a small, battery-operated device that helps the heart beat in
PACEMAKER Natural pacemaker: The heart's "natural" pacemaker is called the sinoatrial (SA) node or sinus node. Artificial pacemaker: It is a small, battery-operated device that helps the heart beat in
CORONARY ARTERIES HEART
 CARDIAC/ECG MODULE THE HEART CORONARY ARTERIES FIBRILLATING HEART CORONARY ARTERIES HEART PRACTICE RHYTHMS PRACTICE RHYTHMS ELECTRICAL CONDUCTION SA Node (60 100) Primary pacemaker AV Node (40 60) ***Creates
CARDIAC/ECG MODULE THE HEART CORONARY ARTERIES FIBRILLATING HEART CORONARY ARTERIES HEART PRACTICE RHYTHMS PRACTICE RHYTHMS ELECTRICAL CONDUCTION SA Node (60 100) Primary pacemaker AV Node (40 60) ***Creates
CRC 431 ECG Basics. Bill Pruitt, MBA, RRT, CPFT, AE-C
 CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
Dual Chamber Temporary External Pacemaker
 5392 Dual Chamber Temporary External Pacemaker Technical Manual Caution: Federal law (USA) restricts this device to sale by or on the order of a physician. The following list includes trademarks or registered
5392 Dual Chamber Temporary External Pacemaker Technical Manual Caution: Federal law (USA) restricts this device to sale by or on the order of a physician. The following list includes trademarks or registered
Reviewed Date: Supersedes (Policy #/description & date): Prepared by: Jacque Callis, RN Approved by: D.R. Johnson, MD
 External Pacemaker Set-up and Revised Date: 11/13/2014 Page 1 of 5 POLICY: The transcutaneous external pacemaker will be used as a noninvasive method of delivering electrical stimuli to the myocardium
External Pacemaker Set-up and Revised Date: 11/13/2014 Page 1 of 5 POLICY: The transcutaneous external pacemaker will be used as a noninvasive method of delivering electrical stimuli to the myocardium
Is This Thing Working?
 Is This *#@!* Thing Working? Pacemaker (and ICD) ECG and Telemetry Pitfalls Wayne O. Adkisson, MD adki0004@umn.edu Disclosures I currently receive research support from Medtronic, Inc. I have been compensated
Is This *#@!* Thing Working? Pacemaker (and ICD) ECG and Telemetry Pitfalls Wayne O. Adkisson, MD adki0004@umn.edu Disclosures I currently receive research support from Medtronic, Inc. I have been compensated
EKG Competency for Agency
 EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
Pacemakers 12/04. Pacemakers. 1. What is a pacemaker?
 Pacemakers 12/04 1-What is a pacemaker? 2- What does intrinsic mean? 3- How exactly do pacemakers work on the heart? 4- What are the parts of a pacemaker? 5- Are there different kinds of pacemakers? 6-
Pacemakers 12/04 1-What is a pacemaker? 2- What does intrinsic mean? 3- How exactly do pacemakers work on the heart? 4- What are the parts of a pacemaker? 5- Are there different kinds of pacemakers? 6-
INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS
 INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS BEFORE INTERPRETING THE ECG: Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS. Cardiology San Francisco General Hospital UCSF Disclosures: None 1 2 QUESTIONS
INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS BEFORE INTERPRETING THE ECG: Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS. Cardiology San Francisco General Hospital UCSF Disclosures: None 1 2 QUESTIONS
Cardiac Resynchronisation Therapy Patient Information
 Melbourne Heart Rhythm Cardiac Resynchronisation Therapy Patient Information Normal Heart Function The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two
Melbourne Heart Rhythm Cardiac Resynchronisation Therapy Patient Information Normal Heart Function The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two
Review Packet EKG Competency This packet is a review of the information you will need to know for the proctored EKG competency test.
 Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
Pacing Codes and Modes Concepts
 Pacing Codes and Modes Concepts Pacing codes and modes concepts Objectives Upon completion of this program the participant will be able to: State what the first four positions of the NBG code represent.
Pacing Codes and Modes Concepts Pacing codes and modes concepts Objectives Upon completion of this program the participant will be able to: State what the first four positions of the NBG code represent.
You have a what, inside you?
 Costal Emergency Medicine Conference You have a what, inside you? Less than mainstream medical devices encountered in the ED. Eric Ossmann, MD, FACEP Associate Professor Duke University Medical Center
Costal Emergency Medicine Conference You have a what, inside you? Less than mainstream medical devices encountered in the ED. Eric Ossmann, MD, FACEP Associate Professor Duke University Medical Center
You have a what, inside you?
 Costal Emergency Medicine Conference You have a what, inside you? Less than mainstream medical devices encountered in the ED. Eric Ossmann, MD, FACEP Associate Professor Duke University Medical Center
Costal Emergency Medicine Conference You have a what, inside you? Less than mainstream medical devices encountered in the ED. Eric Ossmann, MD, FACEP Associate Professor Duke University Medical Center
Model 5392 EPG Temporary Pacer
 Model 5392 EPG Temporary Pacer Compatible Components Reference Card 5392 Surgical Cables 5487 Disposable, short 5487L Disposable, long 5832S Reusable, small clip 5833S 5833SL Disposable, small clip, short
Model 5392 EPG Temporary Pacer Compatible Components Reference Card 5392 Surgical Cables 5487 Disposable, short 5487L Disposable, long 5832S Reusable, small clip 5833S 5833SL Disposable, small clip, short
Temporary pacemaker : Programming &Trouble shooting
 2015 춘계심장학회 Temporary pacemaker : Programming &Trouble shooting 서울아산병원 한두영 Temporary Pacemaker Overview Indication of Temporary Pacemaker Programming ; NBG Code, Pacing/Sensing Device Trouble shooting
2015 춘계심장학회 Temporary pacemaker : Programming &Trouble shooting 서울아산병원 한두영 Temporary Pacemaker Overview Indication of Temporary Pacemaker Programming ; NBG Code, Pacing/Sensing Device Trouble shooting
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
Cardiac Telemetry Self Study: Part One Cardiovascular Review 2017 THINGS TO REMEMBER
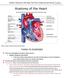 Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
Cardiac Rhythm Device Management. PBL STOP Your acronym for a standardized follow-up
 Cardiac Rhythm Device Management PBL STOP Your acronym for a standardized follow-up What s in it for you? What do you need to feel comfortable with a pacemaker/icd follow-up? 2 CORE OBJECTIVE Provide a
Cardiac Rhythm Device Management PBL STOP Your acronym for a standardized follow-up What s in it for you? What do you need to feel comfortable with a pacemaker/icd follow-up? 2 CORE OBJECTIVE Provide a
Cardiac Pacing. Learning outcomes. Introduction. The cardiac impulse - its formation and its failure CHAPTER. To understand:
 Cardiac Pacing CHAPTER 10 Learning outcomes To understand: The indications for cardiac pacing in the peri-arrest setting How to perform percussion pacing How to apply non-invasive, transcutaneous electrical
Cardiac Pacing CHAPTER 10 Learning outcomes To understand: The indications for cardiac pacing in the peri-arrest setting How to perform percussion pacing How to apply non-invasive, transcutaneous electrical
Chapter 80 Implantable Cardiac Devices
 Chapter 80 Implantable Cardiac Devices Episode Overview: 1. List 5 Indications for permanent pacing 2. Pacemaker nomenclature - what do the 5 letters mean a. What are common Pacemaker types? 3. List the
Chapter 80 Implantable Cardiac Devices Episode Overview: 1. List 5 Indications for permanent pacing 2. Pacemaker nomenclature - what do the 5 letters mean a. What are common Pacemaker types? 3. List the
Project Title Temporary Pacemaker Training Simulator
 Project Title Temporary Pacemaker Training Simulator Project Description Problem: There is no available training device for temporary pacemakers (pacemakers). A training device will have to essentially
Project Title Temporary Pacemaker Training Simulator Project Description Problem: There is no available training device for temporary pacemakers (pacemakers). A training device will have to essentially
ICD Implantation Patient Information
 Melbourne Heart Rhythm ICD Implantation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers (the right atrium
Melbourne Heart Rhythm ICD Implantation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers (the right atrium
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs
 EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale
 Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale Jason Collinson & Stuart Tan Essex Cardiothoracic Centre, Basildon and Thurrock University Hospital. Contact: jason.collinson@nhs.net
Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale Jason Collinson & Stuart Tan Essex Cardiothoracic Centre, Basildon and Thurrock University Hospital. Contact: jason.collinson@nhs.net
3/26/15 HTEC 91. EKG Sign-in Book. The Cardiac Cycle. Parts of the ECG. Waves. Waves. Review of protocol Review of placement of chest leads (V1, V2)
 EKG Sign-in Book HTEC 91 Review of protocol Review of placement of chest leads (V1, V2) Medical Office Diagnostic Tests Week 2 http://www.cvphysiology.com/arrhythmias/a013c.htm The Cardiac Cycle Represents
EKG Sign-in Book HTEC 91 Review of protocol Review of placement of chest leads (V1, V2) Medical Office Diagnostic Tests Week 2 http://www.cvphysiology.com/arrhythmias/a013c.htm The Cardiac Cycle Represents
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists
 PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
Cardiac Assist Devices. Wayne E. Ellis, Ph.D., CRNA
 Cardiac Assist Devices Wayne E. Ellis, Ph.D., CRNA Types Pacemakers AICDs VADs 2 History First pacemaker implanted in 1958 First ICD implanted in 1980 Greater than 500,000 patients in the US population
Cardiac Assist Devices Wayne E. Ellis, Ph.D., CRNA Types Pacemakers AICDs VADs 2 History First pacemaker implanted in 1958 First ICD implanted in 1980 Greater than 500,000 patients in the US population
Essentials of Pacemakers and ICD s. Rajesh Banker, MD, MPH
 Essentials of Pacemakers and ICD s Rajesh Banker, MD, MPH Pacemakers have 4 basic functions: Stimulate cardiac depolarization Sense intrinsic cardiac function Respond to increased metabolic demand by providing
Essentials of Pacemakers and ICD s Rajesh Banker, MD, MPH Pacemakers have 4 basic functions: Stimulate cardiac depolarization Sense intrinsic cardiac function Respond to increased metabolic demand by providing
Full file at
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
The Electrocardiogram
 The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
Pacemaker Concepts and Terminology*
 Pacemaker Concepts and Terminology* BAROUH V BERKOVITS, E.E., Ing. Associate in Surgery, Harvard Medical School, Boston, Mass., Associate in Electrophysiology, Miami University, Miami, Fla., Senior Research
Pacemaker Concepts and Terminology* BAROUH V BERKOVITS, E.E., Ing. Associate in Surgery, Harvard Medical School, Boston, Mass., Associate in Electrophysiology, Miami University, Miami, Fla., Senior Research
Pacemaker and AV Node Ablation Patient Information
 Melbourne Heart Rhythm Pacemaker and AV Node Ablation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers
Melbourne Heart Rhythm Pacemaker and AV Node Ablation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Chapter 9: Ventricular Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 9.1 Describe the various ventricular dysrhythmias 9.2
Electrocardiography for Healthcare Professionals Chapter 9: Ventricular Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 9.1 Describe the various ventricular dysrhythmias 9.2
SJM MRI ACTIVATOR HANDHELD DEVICE WORKFLOW Model: EX4000. SJM-EDTR Item approved for U.S. use only.
 SJM MRI ACTIVATOR HANDHELD DEVICE WORKFLOW Model: EX4000 1 APPROVED MRI SCAN CONDITIONS 1.5 TESLA FULL BODY 2 SETUP SJM MRI ACTIVATOR HANDHELD DEVICE The SJM MRI Activator handheld device must be enabled
SJM MRI ACTIVATOR HANDHELD DEVICE WORKFLOW Model: EX4000 1 APPROVED MRI SCAN CONDITIONS 1.5 TESLA FULL BODY 2 SETUP SJM MRI ACTIVATOR HANDHELD DEVICE The SJM MRI Activator handheld device must be enabled
Temporary Pacemakers
 07 Part I Anaesthesia Refresher Course 2018 University of Cape Town Dr Owen Porrill Private Practice Honorary lecturer- University of Cape Town Temporary pacemakers are usually inserted as part of the
07 Part I Anaesthesia Refresher Course 2018 University of Cape Town Dr Owen Porrill Private Practice Honorary lecturer- University of Cape Town Temporary pacemakers are usually inserted as part of the
ECG Interpretation. Introduction to Cardiac Telemetry. Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services
 ECG Interpretation Introduction to Cardiac Telemetry Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services Disclosures Nothing to disclose Objectives Describe the electrical conduction pathway in
ECG Interpretation Introduction to Cardiac Telemetry Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services Disclosures Nothing to disclose Objectives Describe the electrical conduction pathway in
Review of Pacemakers and ICD Therapy: Overview and Patient Management
 Review of Pacemakers and ICD Therapy: Overview and Patient Management Pacing Systems Charles J. Love, MD FACC FAHA FHRS CCDS Professor of Medicine Director, Cardiac Rhythm Device Services OSU Division
Review of Pacemakers and ICD Therapy: Overview and Patient Management Pacing Systems Charles J. Love, MD FACC FAHA FHRS CCDS Professor of Medicine Director, Cardiac Rhythm Device Services OSU Division
MEDTRONIC CARELINK NETWORK FOR PACEMAKERS. Comparison between the Medtronic CareLink Network for Pacemakers and Transtelephonic Monitoring
 MEDTRONIC CARELINK NETWORK FOR PACEMAKERS Comparison between the Medtronic CareLink Network for Pacemakers and Transtelephonic Monitoring Transtelephonic Monitoring Transmission What can you determine
MEDTRONIC CARELINK NETWORK FOR PACEMAKERS Comparison between the Medtronic CareLink Network for Pacemakers and Transtelephonic Monitoring Transtelephonic Monitoring Transmission What can you determine
There are different types of ICDs:
 Guidelines for Patients with Implantable Devices o Implantable Cardioverter Defibrillator (ICD) Your ICD is approximately the size of a pager and includes the following parts: The ICD: A battery powered
Guidelines for Patients with Implantable Devices o Implantable Cardioverter Defibrillator (ICD) Your ICD is approximately the size of a pager and includes the following parts: The ICD: A battery powered
TELEMETRY BASICS FOR NURSING STUDENTS
 TELEMETRY BASICS FOR NURSING STUDENTS Accuracy of cardiac monitoring is an important component of patient safety in hospitalized patients who meet the criteria for dysrhythmia monitoring. (AACN, 2016,
TELEMETRY BASICS FOR NURSING STUDENTS Accuracy of cardiac monitoring is an important component of patient safety in hospitalized patients who meet the criteria for dysrhythmia monitoring. (AACN, 2016,
Pacing Lead Implant Testing. Document Identifier
 Pacing Lead Implant Testing 1 Objectives Upon completion of this presentation, the participant should be able to: Name the two primary surgical options for implanting pacing leads Describe three significant
Pacing Lead Implant Testing 1 Objectives Upon completion of this presentation, the participant should be able to: Name the two primary surgical options for implanting pacing leads Describe three significant
Q & A: How to Safely Scan Patients with a SureScan MRI Pacemaker
 Q & A: How to Safely Scan Patients with a SureScan MRI Pacemaker Patient Scheduling and Screening Q: Is there any special (other than regular MRI consent) consent form that should be signed by the patient?
Q & A: How to Safely Scan Patients with a SureScan MRI Pacemaker Patient Scheduling and Screening Q: Is there any special (other than regular MRI consent) consent form that should be signed by the patient?
Basic Dysrhythmia Interpretation
 Basic Dysrhythmia Interpretation Objectives 2 To understand the Basic ECG To understand the meaning of Dysrhythmia To describe the normal heart conduction system. To describe the normal impulse pathways.
Basic Dysrhythmia Interpretation Objectives 2 To understand the Basic ECG To understand the meaning of Dysrhythmia To describe the normal heart conduction system. To describe the normal impulse pathways.
Anesthesia Assistants Review Course
 American Association of Oral and Maxillofacial Surgeons Anesthesia Assistants Review Course Four Seasons Las Vegas February 24-25, 2018 Las Vegas, Nevada Anesthesia Assistants Review Course EKG Lecture
American Association of Oral and Maxillofacial Surgeons Anesthesia Assistants Review Course Four Seasons Las Vegas February 24-25, 2018 Las Vegas, Nevada Anesthesia Assistants Review Course EKG Lecture
Transcutaneous Pacing on Zoll Defibrillator Version 4 Related Documents SOP-Zoll defibrillator ; Phillips MRX SOP Dr Randal McRoberts
 Emergency Medical Retrieval Service (EMRS) www.emrs.scot.nhs.uk Standard Operating Procedure Public Distribution Title Transcutaneous Pacing on Zoll Defibrillator Version 4 Related Documents SOP-Zoll defibrillator
Emergency Medical Retrieval Service (EMRS) www.emrs.scot.nhs.uk Standard Operating Procedure Public Distribution Title Transcutaneous Pacing on Zoll Defibrillator Version 4 Related Documents SOP-Zoll defibrillator
Patient Resources: Arrhythmias and Congenital Heart Disease
 Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
11/21/18. EKG Pop Quiz. Michael Giocondo, MD Cardiac Electrophysiology Saint Luke s Cardiovascular Consultants
 EKG Pop Quiz Michael Giocondo, MD Cardiac Electrophysiology Saint Luke s Cardiovascular Consultants 1 Disclosures No financial relationships to disclose. EKG #1 75 y/o woman with a dual-chamber pacemaker
EKG Pop Quiz Michael Giocondo, MD Cardiac Electrophysiology Saint Luke s Cardiovascular Consultants 1 Disclosures No financial relationships to disclose. EKG #1 75 y/o woman with a dual-chamber pacemaker
About atrial fibrillation (AFib) Atrial Fibrillation (AFib) What is AFib? What s the danger? Who gets AFib?
 Understanding AFib Atrial Fibrillation (AFib) About AFib 3 How Your Heart Works 4 Types of AFib 5 Symptoms 5 Risk Factors 5 How is AFib Diagnosed? 6 Treatment 6 What to Ask Your Doctor 7 A normal heartbeat
Understanding AFib Atrial Fibrillation (AFib) About AFib 3 How Your Heart Works 4 Types of AFib 5 Symptoms 5 Risk Factors 5 How is AFib Diagnosed? 6 Treatment 6 What to Ask Your Doctor 7 A normal heartbeat
Sinus rhythm with premature atrial beats 2 and 6 (see Lead II).
 Cardiac Pacemaker Premature Beats When one of ectopic foci becomes irritable, it may spontaneously fire, leading to one or more premature beats. Atrial and junctional foci may become irritable from excess
Cardiac Pacemaker Premature Beats When one of ectopic foci becomes irritable, it may spontaneously fire, leading to one or more premature beats. Atrial and junctional foci may become irritable from excess
OBJECTIVE. 1. Define defibrillation. 2. Describe Need and history of defibrillation. 3. Describe the principle and mechanism of defibrillation.
 Defibrillators OBJECTIVE 1. Define defibrillation. 2. Describe Need and history of defibrillation. 3. Describe the principle and mechanism of defibrillation. 4. Types and classes of defibrillator 5. Describe
Defibrillators OBJECTIVE 1. Define defibrillation. 2. Describe Need and history of defibrillation. 3. Describe the principle and mechanism of defibrillation. 4. Types and classes of defibrillator 5. Describe
WHAT S THAT RHYTHM I AM HEARING? GUIDE TO AUSCULTATION OF ARRHYTHMIAS IN HORSES
 WHAT S THAT RHYTHM I AM HEARING? GUIDE TO AUSCULTATION OF ARRHYTHMIAS IN HORSES Michelle Henry Barton DVM, PhD, DACVIM University of Georgia, Athens, GA INTRODUCTION The purpose of this talk is to review
WHAT S THAT RHYTHM I AM HEARING? GUIDE TO AUSCULTATION OF ARRHYTHMIAS IN HORSES Michelle Henry Barton DVM, PhD, DACVIM University of Georgia, Athens, GA INTRODUCTION The purpose of this talk is to review
Intermittent episodes of paced tachycardia: what is the cause?
 Intermittent episodes of paced tachycardia: what is the cause? Lindsey Parkinson and Lucy Broadhurst, Rotherham NHS Foundation Trust Contact: Lindsey.Parkinson@rothgen.nhs.uk Introduction A hospital in-patient
Intermittent episodes of paced tachycardia: what is the cause? Lindsey Parkinson and Lucy Broadhurst, Rotherham NHS Foundation Trust Contact: Lindsey.Parkinson@rothgen.nhs.uk Introduction A hospital in-patient
Course Objectives. Proper Lead Placements. Review the ECG print paper. Review the mechanics of the Myocardium. Review basics of ECG Rhythms
 ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
CORONARY ARTERIES. LAD Anterior wall of the left vent Lateral wall of left vent Anterior 2/3 of interventricluar septum R & L bundle branches
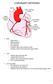 CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
Cardiac muscle is different from other types of muscle in that cardiac muscle
 6 E X E R C I S E Cardiovascular Physiology O B J E C T I V E S 1. To define autorhythmicity, sinoatrial node, pacemaker cells, and vagus nerves 2. To understand the effects of the sympathetic and parasympathetic
6 E X E R C I S E Cardiovascular Physiology O B J E C T I V E S 1. To define autorhythmicity, sinoatrial node, pacemaker cells, and vagus nerves 2. To understand the effects of the sympathetic and parasympathetic
Specified Tolerance (ms)
 SigmaPace TM 1000: Medtronic Temporary External Pacemaker Model 5388 Checkout Procedure 1. PRELIMINARY SET UP a. Connect the pacemaker output to the analyzer s ATRIAL and VENTRICULAR 4 mm interface jacks
SigmaPace TM 1000: Medtronic Temporary External Pacemaker Model 5388 Checkout Procedure 1. PRELIMINARY SET UP a. Connect the pacemaker output to the analyzer s ATRIAL and VENTRICULAR 4 mm interface jacks
Implant Procedure Concepts
 1 4 7 2 5 LV Lead 8 3 6 Implant Procedure Concepts 9 ICD and CRT LV Lead This presentation is provided with the understanding that the slide content must not be altered in any manner as the content is
1 4 7 2 5 LV Lead 8 3 6 Implant Procedure Concepts 9 ICD and CRT LV Lead This presentation is provided with the understanding that the slide content must not be altered in any manner as the content is
Pacing and Device Jargon Made Simple. Dr Jonathan Timperley MB ChB MD FRCP Consultant Cardiologist Northampton General Hospital
 Pacing and Device Jargon Made Simple Dr Jonathan Timperley MB ChB MD FRCP Consultant Cardiologist Northampton General Hospital Disclosure Dr Jonathan Timperley Honorarium from Bayer Arne Larson (1915
Pacing and Device Jargon Made Simple Dr Jonathan Timperley MB ChB MD FRCP Consultant Cardiologist Northampton General Hospital Disclosure Dr Jonathan Timperley Honorarium from Bayer Arne Larson (1915
Lab #3: Electrocardiogram (ECG / EKG)
 Lab #3: Electrocardiogram (ECG / EKG) An introduction to the recording and analysis of cardiac activity Introduction The beating of the heart is triggered by an electrical signal from the pacemaker. The
Lab #3: Electrocardiogram (ECG / EKG) An introduction to the recording and analysis of cardiac activity Introduction The beating of the heart is triggered by an electrical signal from the pacemaker. The
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University. OBHG Education Subcommittee
 -RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
DEFIBRILLATORS ATRIAL AND VENTRICULAR FIBRILLATION
 1 DEFIBRILLATORS The two atria contract together and pump blood through the valves into the two ventricles, when the action potentials spread rapidly across the atria surface. After a critical time delay,
1 DEFIBRILLATORS The two atria contract together and pump blood through the valves into the two ventricles, when the action potentials spread rapidly across the atria surface. After a critical time delay,
Arrhythmia Study Guide 3 Junctional and Ventricular Rhythms
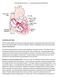 Arrhythmia Study Guide 3 Junctional and Ventricular Rhythms JUNCTIONAL RHYTHMS The AV Junction (Bundle of His and surrounding cells) only acts as pacemaker of the heart when the SA Node is not firing normally
Arrhythmia Study Guide 3 Junctional and Ventricular Rhythms JUNCTIONAL RHYTHMS The AV Junction (Bundle of His and surrounding cells) only acts as pacemaker of the heart when the SA Node is not firing normally
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH
 ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc.
 Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS
 PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS DR SUSAN CORCORAN CARDIOLOGIST ONCE UPON A TIME.. Single chamber pacemakers Programmed at 70/min VVI 70 UNIPOLAR SYSTEMS A Unipolar Pacing
PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS DR SUSAN CORCORAN CARDIOLOGIST ONCE UPON A TIME.. Single chamber pacemakers Programmed at 70/min VVI 70 UNIPOLAR SYSTEMS A Unipolar Pacing
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES
 UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
Aortic Dissection Causes of Death
 Aortic Dissection Causes of Death Rupture aorta 33.3% Unspecified 33.3% Neurological l deficit it 13.9% Visceral ischemia/kidney failure 11.5% Cardiac tamponade 7.9% (Circulation 2002;105:200-6) Medical
Aortic Dissection Causes of Death Rupture aorta 33.3% Unspecified 33.3% Neurological l deficit it 13.9% Visceral ischemia/kidney failure 11.5% Cardiac tamponade 7.9% (Circulation 2002;105:200-6) Medical
EXTERNAL TEMPORARY PACEMAKERS
 Czech Republic EXTERNAL TEMPORARY PACEMAKERS Lukas Peter Engineering and Business Coordinator Pavel Taborsky Chief Executive Officer MEDIATRADE s.r.o. PRAGUE Valasske Mezirici MEDIATRADE s.r.o. More than
Czech Republic EXTERNAL TEMPORARY PACEMAKERS Lukas Peter Engineering and Business Coordinator Pavel Taborsky Chief Executive Officer MEDIATRADE s.r.o. PRAGUE Valasske Mezirici MEDIATRADE s.r.o. More than
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
PART I. Disorders of the Heart Rhythm: Basic Principles
 PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
The Nuts and Bolts of ICD Therapy
 Electrical Management of Cardiac Rhythm Disorders For Cardiology Fellows December 5-8 Austin, Texas The Nuts and Bolts of ICD Therapy 1 2 Action Potential Localized Differences in Conduction Conduction
Electrical Management of Cardiac Rhythm Disorders For Cardiology Fellows December 5-8 Austin, Texas The Nuts and Bolts of ICD Therapy 1 2 Action Potential Localized Differences in Conduction Conduction
Catheter Ablation. Patient Education
 Catheter Ablation Patient Education Allina Health System Your heart has four chambers. Two upper chambers (atria) pump blood to the two lower chambers (ventricles). In order for the heart to pump, it requires
Catheter Ablation Patient Education Allina Health System Your heart has four chambers. Two upper chambers (atria) pump blood to the two lower chambers (ventricles). In order for the heart to pump, it requires
UNDERSTANDING PACEMAKERS
 UNDERSTANDING PACEMAKERS Living Well with a Pacemaker Why You Need a Pacemaker Your heart has an electrical system that keeps it beating at the right speed. Problems with this system can make your heart
UNDERSTANDING PACEMAKERS Living Well with a Pacemaker Why You Need a Pacemaker Your heart has an electrical system that keeps it beating at the right speed. Problems with this system can make your heart
AWAY Model # RTLAGF-900 REV
 AWAY Model # RTLAGF-900 REV2.4.9.15 Contents User manual English 2 General Description 2 Intended Use 3 Included in this Package 4 Instructions for Use 7 Application Duration 7 Electrode Placement 8 Tips
AWAY Model # RTLAGF-900 REV2.4.9.15 Contents User manual English 2 General Description 2 Intended Use 3 Included in this Package 4 Instructions for Use 7 Application Duration 7 Electrode Placement 8 Tips
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2
Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2
8/20/2012. Learning Outcomes (Cont d)
 1 2 3 4 Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2 Identify premature junctional complexes
1 2 3 4 Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2 Identify premature junctional complexes
National Coverage Determination (NCD) for Cardiac Pacemakers (20.8)
 Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
Manual Defibrillators, Automatic External Defibrillators, Cardioversion, and External Pacing. D. J. McMahon cewood rev
 Manual Defibrillators, Automatic External Defibrillators, Cardioversion, and External Pacing D. J. McMahon 141001 cewood rev 2017-10-04 Key Points Defibrillators: - know the definition & electrical value
Manual Defibrillators, Automatic External Defibrillators, Cardioversion, and External Pacing D. J. McMahon 141001 cewood rev 2017-10-04 Key Points Defibrillators: - know the definition & electrical value
Electrocardiography Abnormalities (Arrhythmias) 7. Faisal I. Mohammed, MD, PhD
 Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
EKG Abnormalities. Adapted from:
 EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
Cardiovascular Physiology
 Cardiovascular Physiology The mammalian heart is a pump that pushes blood around the body and is made of four chambers: right and left atria and right and left ventricles. The two atria act as collecting
Cardiovascular Physiology The mammalian heart is a pump that pushes blood around the body and is made of four chambers: right and left atria and right and left ventricles. The two atria act as collecting
ICD: Basics, Programming and Trouble-shooting
 ICD: Basics, Programming and Trouble-shooting Amir AbdelWahab, MD Electrophysiology and Pacing Service Cardiology Department Cairo University Feb 2013 Evolution of ICD Technology ICD Evolution Indications
ICD: Basics, Programming and Trouble-shooting Amir AbdelWahab, MD Electrophysiology and Pacing Service Cardiology Department Cairo University Feb 2013 Evolution of ICD Technology ICD Evolution Indications
