Per Bergman Swedish physician. Robert Tigerstedt Finnisch pyhsician
|
|
|
- Ashlyn Hines
- 5 years ago
- Views:
Transcription
1 Regulation of Cardiovascular functions Goals: Maintain normal blood pressure (heart pump + vascular resistance + blood volume) Adaptation of blood pressure to special circumstances (redistribution) Maintains the blood flow to the heart and brain (hemorrhage) Increase blood supply to active tissues Increase or decrease heat loss from the body Robert Tigerstedt Finnisch pyhsician Per Bergman Swedish physician Robert Tigerstedt and Per Bergman: Niere und Kreislauf. Arch. Physiol. 8: , The discovery of RENIN Page 1
2 Robert W. Furchgott Louis J. Ignarro Ferid Murad Discovery the role of nitric oxide in the vascular system 1998: Nobel-prize Types of regulation Local Autoregulation: flow independence from blood pressure Metabolic, humoral, mechanical, thermal factors Systemic Hormones Neural regulation by transmitters Page 2
3 Local factors Tissue pressure Myogenic mechanism Metabolic factors (Vasodilators): low level of O 2 (except lung vessels), high level of CO 2 (except lung vessels), ph decrease, high level of K +, adenosine (heart) Humoral factors: Endothel-related vasoactive factors: NO, Endothelin Kinins, Serotonin, Histamine, Eicosanoids, CO, H 2 S, Purines Vasoactive peptides (VIP, SP, CGRP, CCK, NPY, cytokines, etc,) Page 3
4 Locations of the action of metabolites Autoregulation of blood flow during blood pressure changes: myogenic theory (Bayliss effect) Page 4
5 Blood flow Reactive hyperemia in the hind limb of the dog after 15-, 30-, and 60- second occlusions of the femoral artery. Time (min) Active hyperemia during physical work in the muscle. Purine: ATP Cotransmitter with NE, GABA, Dopamine, Ach, histamine Receptors: P2Y: metabotropic P2X: ionotropic Role: vasoconstriction, vasodilation, pain, sensory transmission Page 5
6 ATP Vasoconstriction Vasodilation Adenosine Tissue cell ATP Na + A A A A Caffeine Inozin S-adenozylhomocisteine A2 camp Smooth muscle cell Vasodilation Page 6
7 Blood flow Ach, Na Calcium Histamine NITRIC OXIDE (NO) ENDOTHEL CELL NOS Serotonin Bradykinin SP, CGRP Cytokines L-ARGININE CITRULLINE Hypoxia Hypercapnia Smooth muscle GUANYLATE CYCLASE cgmp PKG Decreased Ca-level VASODILATION Action mechanism of NO in smooth muscle cells PKG decreases the permeability of calcium channels => IC calcium => relaxation Activation of potassium channels => hyperpolarisation => relaxation Activation the myosin light chain phosphatase => dephosphorilation => relaxation Increased calcium uptake into the SR Page 7
8 NOS-1 (nnos) neural Types of NOS NOS-2 (inos) induced phagocyte (cytokine-induced NOS) NOS-3 (cnos) constitutional endothel cell Page 8
9 THE MOST POTENT EDRF: NITRIC OXIDE Receptor G q α Calmodulin Arg NOS PLC IP3 Ca Citrulline + NO NO GTP PKG Ca decrease Guanylylcyclase cgmp Phosphodiesterase Inactivation Sildenafil citrate RELAXATION Endothelial cell Smooth muscle Eicosanoids Cortisol Histamine Bradykinin phsopholipides Leukotriens vasoconstriction Arachidonic acid Lypoxigenase Endoperoxidase (COX1, COX2) ASPIRIN endoperoxides TROMBOXANE A2 vasoconstriction Produced by platelets Prostacycline (PGI2) Vasodilation (produced by endothelial cells PGE2 (D) PGD (C) PGF (C) PGH (C) Page 9
10 Prostaglandin receptors Metabotropic DP (PGD) camp EP1 (PGE) IP3/DAG EP2 (PGE) camp EP3 (PGE) camp EP4 (PGE) camp FP (PGF) IP3/DAG IP (prostacycline) camp TP (tromboxane) IP3/DAG EICOSANOIDS IN CIRCULATION Eicosanoids are general inter- and intracellular signal molecules that can be produced by each cell. Circulation: 1. Endothelial PGI2: continuous vasodilator tone in arteries. It inhibits aggregation of platelets. 2. PGE2: putative mediator of metabolically induced vasodilation. 3. TXA2: vasoconstrictor released from platelets. ASPIRIN can prevent coagulation/thrombosis Page 10
11 Kinins (bradykinin bradykinin, lysyl-bradykinin bradykinin) Prekallikrein (plasma) HMW/ LMW kininogen (alfa2 globulin) (Source: plasma, tissue) Kallikrein (plasma, sweatgland, salivary glands, pancreas, prostate, intestine, kidney Bradikinin Inactive 9 aminoacids metabolite Lysyl-bradykinin (kallidin) Kininase I Kininase II (ACE) ROLE OF KININS Receptors: B1receptor: PLC (inflammation) B2 receptor: PLC/PLA2 (constitutive) 1. MEDIATORS OF INFLAMMATION Vasodilation (NO release) Increased capillary permeability Pain 2. REGULATION OF BLOOD FLOW IN EXOCRIN GLANDS 3. Contraction of visceral smooth muscle Page 11
12 Serotonin Source: platelets, enterochromaffin cells Effects: Local vasoconstriction (mainly veins: 5HT 1-2 ) Pulmonary vasoconstriction (5HT 2 ) Systemic vasodilation (NO release: 5HT 7 ) Serotonin receptors 5-HT1 camp (vasoconstriction) 5-HT2 IP3/DAG (platelet aggregation, smooth muscle contraction, endothel cell activation) Page 12
13 Histamine 1. Source: mast cell, basophil granulocyte 2. Effects (metabotropic receptors): H-1 receptor (IP3/DAG, PLA2 ): a. Indirect vasodilation (NO/PGs release) b. Direct vasoconstriction c. Increased permeability d. Pain, itching e. Visceral muscle constriction f. Bronchoconstriction H2-receptor (camp ): gascric acid secretion, (smooth muscle relaxation: lung) H3-receptor (presynaptic; camp ): : inhibition of neurotransmitter release H4 (e.g. white blood cells, CNS): camp ; IP3/DAG, : inflammation Tissue damage Immune reaction HN Histidine N Histamine NH 2 HISTAMINE Histamine H1-R (IP3/Ca) HISTAMINE IS ONE OF THE MOST IMPORTANT INFLAMMATORY MEDIATOR. H2-R (camp) INFLAMMATION: Vasodilation Increased permeability Itching/pain Page 13
14 Vasoactive peptides ENDOTHELIN Paracrine vasoconstrictor peptide (21 AA) produced by endothelial cells. ET1, ET2, ET3. Circulation: ET1. ET1 is the currently known, most potent vasoconstrictor. Receptors (metabotropic): ET-A (IP3/Ca) : vascular smooth muscle: constriction ET-B: (IP3/Ca) vascular smooth muscle: constriction (endothelial cells: NO release=> vasodilation) Stimulus: angiotensin, catecholamine, hypoxia, thrombin Page 14
15 Vasoactive peptides Locally acting vasoactive peptides originated from sensory and/or autonomic nerves Vasodilators: VIP CGRP SP CCK Vasoconstrictor: NPY Neural/hormonal factors Catecholamines (norepinephrine, epinephrine, dopamine) Acetylcholine; ATP Renin-Angiotensin Vasopressine/Antidiuretic hormone (ADH) Atrial natriuretic peptide/hormone (ANP/ANH) Glucocorticoids, Mineralocorticoids Thyroxine, Triiodothyronine Page 15
16 EFFECTS OF CATECHOLAMINES ON CIRCULATION Source: 1. Sympathetic postganglionic neurons: noradrenaline (NA) 2. Adrenal medulla: 80 % adrenaline (A), 20 % Na, dopamine Receptors: α1: NA>A α 2: NA>A β1: NA=A β2: A>NA α1 (Gq IP3/DAG Ca 2+ ): arteriolar and veins: contraction α2 (Gi camp ): (few in arteriolar smooth muscle: contraction) - autoreceptors on sympathetic terminals: inhibition of NA release - NAergic neurons in the CNS: inhibition, drop in blood pressure - Endothelial cells: NO release β1 (Gs camp ): heart: positive chronotropy, inotropy etc. β2 (Gs camp ): arteriolar smooth muscle (skeletal muscle): relaxation Effect of sympathetic activation: 1. Increase in heart function (+ effects) 2. Peripheral vasoconstriction (except liver and skeletal muscle in special cases) 3. Venoconstriction SOURCE OF CIRCULATING CATECHOLAMINES Sympathetic postganglionic fibers Adrenal cortex Adrenal medulla (nerve tissue) Steroid hormones DOPA Dopamine Noradrenaline Adrenaline Aromatic aminoacid decarboxylase Dopamineβhidroxylase (norepinephrine) (epinephrine) Phenylethanolamine N-methyltransferase 20 % 80 % Page 16
17 Dopamine Source: adrenal medulla Receptors (metabotropic): D1,D5: camp ; pulmonary/kidney arteries: vasodilation D2, D3, D4: camp DOPAMINE RECEPTORS EFFECTS OF CATECHOLAMINES ON CIRCULATION NA/A β-1 Stimulation of the heart α-1 Contraction of veins Increased venous return α-1 Contraction of arteries, arterioles α-1 / β-2 Less strong contraction of arterioles in skeletal muscle Increased cardiac output x Increased TPR INCREASED BLOOD PRESSURE Page 17
18 Effect of noradrenaline on local circulation Acetylcholine Source: Postganglionic parasympathetic nerves Some postganglionic sympathetic nerves (10%) Enteric nervous system Effects: HEART: M 2 receptor camp : Heart rate conductivity Endothel cells: M 1 receptor: IP3/DAG=> Ca 2+ => NO release => vasodilation (Vascular smooth muscle: M 3 receptor: IP3/DAG=> Ca 2+ => vasoconstriction) Page 18
19 Acetylcholine effects Acetylcholine Acetylcholine Vascular smooth muscle (endothelial cells are removed) Endothelial lining is intact Contraction Relaxation Renin-angiotensin System Renin (protease) Source: juxtaglomerular apparatus A Renal corpuscle B Proximal tubule C Distal convoluted tubule D Juxtaglomerular apparatus 1. Basement membrane (Basal lamina) 2. Bowman's capsule parietal layer 3. Bowman's capsule visceral layer 3a. Pedicels (Foot processes from podocytes) 3b. Podocyte 4. Bowman's space (urinary space) 5a. Mesangium Intraglomerular cell 5b. Mesangium Extraglomerular cell 6. Granular cells (Juxtaglomerular cells: Renin secretion) 7. Macula densa 8. Myocytes (smooth muscle) 9. Afferent arteriole 10. Glomerulus Capillaries 11. Efferent arteriole Page 19
20 Renin-releasing factors Decreased blood pressure in the afferent arterioles Decreased tubular sodium concentrations Sympathetic activation (beta1-receptor) Effect: protease activity: angiotensinogen => angiotensin I (10 aminoacids) Angiotensinogen I Angiotensin I Angiotensin II (8 aminoacid) Inactivation: Angiotensin II (8 aminoacid) Angiotensin III (7 AA) Angiotensin IV (6 AA) Page 20
21 Effects of Angiotensin II Receptors (metabotropic): AT 1 : PLC (IP3/DAG ), camp blood vessels: vasoconstriction Adrenal cortex: aldosterone secretion Hypothalamus: ADH secretion Hypothalamus: thirst sensation Kidney: renin release Kidney: sodium and water reabsorption Hypothalamus: thirst sensation AT 2 : Vasodilation Antiproliferation Kidney: sodium and vater reabsorption Bradykinin release NO release Captopril Angiotensinconvertase (ACE) (Endothelial cells) Salt appetite RENIN-ANGIOTENSIN SYSTEM Losartan Drinking Increased CO Vasopressin secretion x Blood: Angiotensinogen (From liver) Angiotensin I Angiotensin II AT-R1 (IP3 Ca) Increased TPR Renin Kidney JGA Arteriolar vasoconstriction Decreased renal blood flow Stimulation of Aldosterone Na-reabsorbtion = Increased BP β1 stimulation Hyponatremia Saralasin Page 21
22 PROSTAGLANDIN, KININS AND RENIN-ANGIOTENSIN Arachidonic acid PGI2, PGE2 Systemic vasoconstriction to angiotensin is associated with local vasodilation in the arterioles of the kidney. Kininogen Kallikrein Prorenin Angiotensinogen Bradykinin Renin Inactive peptides ACE Kininase II Angiotensin I Angiotensin II LOCAL VASODILATION SYSTEMIC VASOCONSTRICTION Vasopressin/ADH 1. Source: hypothalamus supraoptic and paraventricular nuclei 2. Releasing factors: hyperosmosis (osmoreceptors) hypovolaemia (baroreceptors) angiotensin II hypotension 3. Effects: increased water reabsorption in the kidney (V2 receptors) vasoconstriction: decreased filtration (V1 receptors Page 22
23 Angiotensin II Hyperosmosis VASOPRESSIN Hypothalamus Hypovolemia Hypotension Main effect Kidney: [V2 (camp )] Reabsorption of water Neurohypophysis VASOPRESSIN (ADH) Less important Arterioles: [V1 (IP3 Ca)] Vasoconstriction Increased cardiac output x Increased TPR INCREASED BLOOD PRESSURE Action of ADH in the kidney ADH is absent Collecting duct ADH is present Collecting duct AP2 V2 AP3 camp ADH H 2 O AP2 V2 AP3 H 2 O camp ADH AP2 V2 AP3 camp ADH Page 23
24 Atrial natriuretic peptide (ANP, ANH) 1. Source: heart (right atria) 2. Releasing factor: Increased stretch in the right atria (hypervolaemia) 3. Effects: a. Decreased sodium reabsorption (kidney) b. Vasodilation c. Decreased renin, aldosteron, angiotensin II secretion d. Decreased Norepinephiren release e. Suppression of thirst Summary: TPR, blood volume => MAP ANH RECEPTORS (metabotropic) cgmp ANH Guanylyl cyclase GTP cgmp PKG In smooth muscle, cgmp PKG inhibits intracellular Ca and causes relaxation. Page 24
25 ANP, BNP and CNP ANP (ANH): atrial natriuretic peptide (hormone) (heart, brain): hormone and neurotransmitter BNP: brain natriuretic peptide (heart, brain): hormone and neurotransmitter CNP: C-type natriuretic peptide (brain, hypophysis, kidney): paracrin ANP and BNP acting in the brain as neurotransmitters are decreasing blood pressure. Page 25
26 Glucocorticoid - Cortisol Receptors: intracellular: Steroid type II receptor => gene transcription Permissive effect on alfa 1 -receptors Increased binding of noradrenaline/adrenaline to their receptors Increased bindings of adrenoceptors to G-proteins Increased production of camp by adrenaline Prolongation of effects of noradrenaline/adrenaline in smooth muscles => vasoconstriction => MAP Inhibition of synthesis of prostanoids (inhibition of vasodilation) Permisszive for the synthesis of angiotensinogen in the liver Decreases the sensitivity of angiotensin receptors Permissive for renin and ANP synthesis Permissive for normal GFR Decreases the ADH secretion Ensures normal blood pressure Lack: circulation failure Mineralocorticoid - Aldosterone Receptors: intracellular: Steroid type I receptor => gene transcription Effects: Increased Na + reabsorption (and potassium+ proton secretion) = > blood volume => MAP Lack: circulation failure Page 26
27 Thyroid hormones Thyroxine, triiodothyronine Receptors: intranuclear receptor => gene transcription Effects: Heart contractility => Stroke volume β1-receptor number and sensitivity α MHC (increased ATP-ase activity) SR Ca 2+ -ATP-ase Na + -K + -ATP-ase K+-channels β MHC Na + -Ca 2+ -exchanger Heart rate β1-receptor number and sensitivity Cardiac output Peripheral resistance (release of vasodilator factors in tissues, and effect of heat) vasodilation (mainly in the skin vessels) => increased water and Na + reabsorption) => blood volume Pulse pressure Mean arterial blood pressure: No change Page 27
28 MUSCLE ET-A IP3/Ca TP 5HT2a Endothelin-1 Contraction B1 TXA2 NK2 Serotonin 5HT2a M1 α1 Bradykinin B1 H1 Neurokinin A NK2 NK1 Contraction Acetylcholine M1 α2 Noradrenaline α1 camp A1 Histamine H1 H2 Substance P NK1 CGRP?? VIP? Adenosine Relaxation? A2 camp EP1-4 IP NO PGE2 PGI2 ENDOTHEL IP3/Ca NO Page 28
Cardiovascular Physiology V.
 Cardiovascular Physiology V. 46. The regulation of local blood flow. 47. Factors determining cardiac output, the Guyton diagram. Ferenc Domoki, November 20 2017. Control of circulation Systemic control
Cardiovascular Physiology V. 46. The regulation of local blood flow. 47. Factors determining cardiac output, the Guyton diagram. Ferenc Domoki, November 20 2017. Control of circulation Systemic control
Cardiovascular System B L O O D V E S S E L S 2
 Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
REGULATION OF CARDIOVASCULAR SYSTEM
 REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Pharmacology - Problem Drill 11: Vasoactive Agents
 Pharmacology - Problem Drill 11: Vasoactive Agents Question No. 1 of 10 1. Vascular smooth muscle contraction is triggered by a rise in. Question #01 (A) Luminal calcium (B) Extracellular calcium (C) Intracellular
Pharmacology - Problem Drill 11: Vasoactive Agents Question No. 1 of 10 1. Vascular smooth muscle contraction is triggered by a rise in. Question #01 (A) Luminal calcium (B) Extracellular calcium (C) Intracellular
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
 Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Vasodilation. Autoregulation ป จจ ยท ควบค มขนาดของหลอดเล อด. CO 2, H +, K +, lactate, adenosine osmolarity, temperature O 2
 Regulation in cardiovascular system Local control/autoregulation of organs (brain and heart have higher priority) To provide adequate blood flow to tissue Central regulation To provide optimal blood pressure
Regulation in cardiovascular system Local control/autoregulation of organs (brain and heart have higher priority) To provide adequate blood flow to tissue Central regulation To provide optimal blood pressure
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY
 RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Otto Loewi (88) German pharmacologist. Page 1. Sir Henry Hallett Dale
 Regulation of Cardiovascular functions Goals: Maintain normal blood pressure (heart pump + vascular resistance + blood volume) Adaptation of blood pressure to special circumstances (redistribution) Maintains
Regulation of Cardiovascular functions Goals: Maintain normal blood pressure (heart pump + vascular resistance + blood volume) Adaptation of blood pressure to special circumstances (redistribution) Maintains
Blood Pressure Fox Chapter 14 part 2
 Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
BIOH122 Session 6 Vascular Regulation
 BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
CASE 13. What neural and humoral pathways regulate arterial pressure? What are two effects of angiotensin II?
 CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
Blood Pressure Regulation. Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure
 Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias
 1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
Blood Pressure Regulation -1
 CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
Mechanism: 1- waterretention from the last part of the nephron which increases blood volume, venous return EDV, stroke volume and cardiac output.
 Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Chapter 26 The Urinary System
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Functions of the kidney
 Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D.
 Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
NROSCI/BIOSC 1070 and MSNBIO 2070 September 25, 2017 Cardiovascular 5 Control of Vascular Resistance
 NROSCI/BIOSC 1070 and MSNBIO 2070 September 25, 2017 Cardiovascular 5 Control of Vascular Resistance Baroreceptors and Baroreceptor Reflexes In order to maintain stable blood pressure, it is necessary
NROSCI/BIOSC 1070 and MSNBIO 2070 September 25, 2017 Cardiovascular 5 Control of Vascular Resistance Baroreceptors and Baroreceptor Reflexes In order to maintain stable blood pressure, it is necessary
Adrenal gland And Pancreas
 Adrenal gland And Pancreas Structure Cortex Glucocorticoids Effects Control of secretion Mineralocorticoids Effects Control of secretion Sex steroids Medulla Catecholamines Adrenal cortex 80% of an adrenal
Adrenal gland And Pancreas Structure Cortex Glucocorticoids Effects Control of secretion Mineralocorticoids Effects Control of secretion Sex steroids Medulla Catecholamines Adrenal cortex 80% of an adrenal
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D.
 Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
BIOL 2458 A&P II CHAPTER 18 SI Both the system and the endocrine system affect all body cells.
 BIOL 2458 A&P II CHAPTER 18 SI 1 1. Both the system and the endocrine system affect all body cells. 2. Affect on target cells by the system is slow. Affect on target cells by the system is fast. INTERCELLULAR
BIOL 2458 A&P II CHAPTER 18 SI 1 1. Both the system and the endocrine system affect all body cells. 2. Affect on target cells by the system is slow. Affect on target cells by the system is fast. INTERCELLULAR
Blood Pressure Regulation. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Cardiovascular regulation. Neural and hormonal Regulation Dr Badri Paudel GMC. 1-Local factors (autoregulation) Control of Blood Flow
 Neural and hormonal Regulation Dr Badri Paudel GMC 1 Cardiovascular regulation Fa c t o r s i nvo l v e d i n t h e regulation of cardiovascular function include: 1- Autoregulation 2- Neural regulation
Neural and hormonal Regulation Dr Badri Paudel GMC 1 Cardiovascular regulation Fa c t o r s i nvo l v e d i n t h e regulation of cardiovascular function include: 1- Autoregulation 2- Neural regulation
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
2- Maintain the proper balance between water and. 3- Maintain the proper acid base balance. glucose by gluconeogenesis. pressure
 Filter ~180 liters of blood plasma daily, allowing toxins, metabolic wastes, and excess ions to leave the body in urine 1 Regulate volume and chemical composition of the blood 2 Maintain the proper balance
Filter ~180 liters of blood plasma daily, allowing toxins, metabolic wastes, and excess ions to leave the body in urine 1 Regulate volume and chemical composition of the blood 2 Maintain the proper balance
Cell-Derived Inflammatory Mediators
 Cell-Derived Inflammatory Mediators Introduction about chemical mediators in inflammation Mediators may be Cellular mediators cell-produced or cell-secreted derived from circulating inactive precursors,
Cell-Derived Inflammatory Mediators Introduction about chemical mediators in inflammation Mediators may be Cellular mediators cell-produced or cell-secreted derived from circulating inactive precursors,
Cardiovascular system: Blood vessels, blood flow. Latha Rajendra Kumar, MD
 Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 17 Urinary System 2 Glomerular Filtration Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Overview of Renal Physiology
BIOH122 Human Biological Science 2 Session 17 Urinary System 2 Glomerular Filtration Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Overview of Renal Physiology
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Mineralocorticoids. Introduction
 Mineralocorticoids Introduction concepts to remember: a) water, glucose, mineral metabolism; b) adrenal in stress and blood pressure 15 Renin - angiotensin (RAS) and kallikrein kinin (KKS) systems: synthesis,
Mineralocorticoids Introduction concepts to remember: a) water, glucose, mineral metabolism; b) adrenal in stress and blood pressure 15 Renin - angiotensin (RAS) and kallikrein kinin (KKS) systems: synthesis,
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
8. URINE CONCENTRATION
 8. URINE CONCENTRATION The final concentration of the urine is very dependent on the amount of liquid ingested, the losses through respiration, faeces and skin, including sweating. When the intake far
8. URINE CONCENTRATION The final concentration of the urine is very dependent on the amount of liquid ingested, the losses through respiration, faeces and skin, including sweating. When the intake far
Blood pressure. Formation of the blood pressure: Blood pressure. Formation of the blood pressure 5/1/12
 Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
MAJOR FUNCTIONS OF THE KIDNEY
 MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
3/10/2009 VESSELS PHYSIOLOGY D.HAMMOUDI.MD. Palpated Pulse. Figure 19.11
 VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Cardiovascular System. Blood Vessel anatomy Physiology & regulation
 Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
Urine Formation. Urinary Physiology Urinary Section pages Urine Formation. Glomerular Filtration 4/24/2016
 Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
The Endocrine System. I. Overview of the Endocrine System. II. Three Families of Hormones. III. Hormone Receptors. IV. Classes of Hormone Receptor
 The Endocrine System I. Overview of the Endocrine System A. Regulates long term metabolic processes B. Releases hormones from endocrine cells 1. Hormones are chemicals 2. Alter metabolism of cells 3. Release
The Endocrine System I. Overview of the Endocrine System A. Regulates long term metabolic processes B. Releases hormones from endocrine cells 1. Hormones are chemicals 2. Alter metabolism of cells 3. Release
Endocrine System Hormones
 Endocrine System Hormones 2007-2008 Regulation Why are hormones needed? chemical messages from one body part to another communication needed to coordinate whole body homeostasis & regulation metabolism
Endocrine System Hormones 2007-2008 Regulation Why are hormones needed? chemical messages from one body part to another communication needed to coordinate whole body homeostasis & regulation metabolism
Chapter 16: Endocrine System 1
 Ch 16 Endocrine System Bi 233 Endocrine system Endocrine System: Overview Body s second great controlling system Influences metabolic activities of cells by means of hormones Slow signaling Endocrine glands
Ch 16 Endocrine System Bi 233 Endocrine system Endocrine System: Overview Body s second great controlling system Influences metabolic activities of cells by means of hormones Slow signaling Endocrine glands
Cardiovascular Physiology IV.
 Cardiovascular Physiology IV. 48. Short-term control mechanisms of arterial blood pressure. 49. Long-term control of arterial blood pressure. Ferenc Domoki, November 14 2017. Challenges/expectations Blood
Cardiovascular Physiology IV. 48. Short-term control mechanisms of arterial blood pressure. 49. Long-term control of arterial blood pressure. Ferenc Domoki, November 14 2017. Challenges/expectations Blood
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Urinary System kidneys, ureters, bladder & urethra
 Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Cardiovascular System. Heart
 Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Lecture 16: The Nephron
 Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Therefore MAP=CO x TPR = HR x SV x TPR
 Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
P215 Spring 2018: Renal Physiology Chapter 18: pp , Chapter 19: pp ,
 P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
Heart. Large lymphatic vessels Lymph node. Lymphatic. system Arteriovenous anastomosis. (exchange vessels)
 Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Kidney Structure. Renal Lobe = renal pyramid & overlying cortex. Renal Lobule = medullary ray & surrounding cortical labryinth.
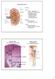 Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
RENAL PHYSIOLOGY. Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM
 RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte, H
RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte, H
Neuron types and Neurotransmitters
 Neuron types and Neurotransmitters Faisal I. Mohammed. PhD, MD University of Jordan 1 Transmission of Receptor Information to the Brain the larger the nerve fiber diameter the faster the rate of transmission
Neuron types and Neurotransmitters Faisal I. Mohammed. PhD, MD University of Jordan 1 Transmission of Receptor Information to the Brain the larger the nerve fiber diameter the faster the rate of transmission
Cell Signaling (part 1)
 15 Cell Signaling (part 1) Introduction Bacteria and unicellular eukaryotes respond to environmental signals and to signaling molecules secreted by other cells for mating and other communication. In multicellular
15 Cell Signaling (part 1) Introduction Bacteria and unicellular eukaryotes respond to environmental signals and to signaling molecules secreted by other cells for mating and other communication. In multicellular
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX
 One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
Lujain Hamdan. Ayman Musleh & Yahya Salem. Mohammed khatatbeh
 12 Lujain Hamdan Ayman Musleh & Yahya Salem Mohammed khatatbeh the last lecture, we have studied the differences between the two divisions of the ANS: sympathetic and parasympathetic pathways which work
12 Lujain Hamdan Ayman Musleh & Yahya Salem Mohammed khatatbeh the last lecture, we have studied the differences between the two divisions of the ANS: sympathetic and parasympathetic pathways which work
Structure and organization of blood vessels
 The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
Hormonal Control of Osmoregulatory Functions *
 OpenStax-CNX module: m44828 1 Hormonal Control of Osmoregulatory Functions * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of
OpenStax-CNX module: m44828 1 Hormonal Control of Osmoregulatory Functions * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of
RENAL PHYSIOLOGY. Zekeriyya ALANOGLU, MD, DESA. Ahmet Onat Bermede, MD. Ankara University School of Medicine Dept. Anesthesiology and ICM
 RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA. Ahmet Onat Bermede, MD. Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte,
RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA. Ahmet Onat Bermede, MD. Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte,
Control of blood tissue blood flow. Faisal I. Mohammed, MD,PhD
 Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
Chapter 15 Fluid and Acid-Base Balance
 Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Endocrine System Hormones. AP Biology
 Endocrine System Hormones 2007-2008 Regulation Why are hormones needed? u chemical messages from one body part to another u communication needed to coordinate whole body u daily homeostasis & regulation
Endocrine System Hormones 2007-2008 Regulation Why are hormones needed? u chemical messages from one body part to another u communication needed to coordinate whole body u daily homeostasis & regulation
Glomerular filtration rate (GFR)
 LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
Urinary System kidneys, ureters, bladder & urethra
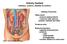 Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
Receptors Functions and Signal Transduction L1- L2
 Receptors Functions and Signal Transduction L1- L2 Faisal I. Mohammed, MD, PhD University of Jordan 1 Introduction to Physiology (0501110) Summer 2012 Subject Lecture No. Lecturer Pages in the 11 th edition.
Receptors Functions and Signal Transduction L1- L2 Faisal I. Mohammed, MD, PhD University of Jordan 1 Introduction to Physiology (0501110) Summer 2012 Subject Lecture No. Lecturer Pages in the 11 th edition.
GENERAL CHARACTERISTICS OF THE ENDOCRINE SYSTEM FIGURE 17.1
 GENERAL CHARACTERISTICS OF THE ENDOCRINE SYSTEM FIGURE 17.1 1. The endocrine system consists of glands that secrete chemical signals, called hormones, into the blood. In addition, other organs and cells
GENERAL CHARACTERISTICS OF THE ENDOCRINE SYSTEM FIGURE 17.1 1. The endocrine system consists of glands that secrete chemical signals, called hormones, into the blood. In addition, other organs and cells
Urinary System and Fluid Balance. Urine Production
 Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Introduction to Autonomic
 Part 2 Autonomic Pharmacology 3 Introduction to Autonomic Pharmacology FUNCTIONS OF THE AUTONOMIC NERVOUS SYSTEM The autonomic nervous system (Figure 3 1) is composed of the sympathetic and parasympathetic
Part 2 Autonomic Pharmacology 3 Introduction to Autonomic Pharmacology FUNCTIONS OF THE AUTONOMIC NERVOUS SYSTEM The autonomic nervous system (Figure 3 1) is composed of the sympathetic and parasympathetic
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Renal physiology II. Basic renal processes. Dr Alida Koorts BMS
 Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Biology 2100 Human Physiology C. Iltis SLCC March 8, Midterm Examination #2
 Biology 2100 Human Physiology Name: KEY C. Iltis SLCC March 8, 2000 Midterm Examination #2 Multiple Choice Questions (2 POINTS EACH) 1. When glucose levels are above 100 mg/dl, which of the following is
Biology 2100 Human Physiology Name: KEY C. Iltis SLCC March 8, 2000 Midterm Examination #2 Multiple Choice Questions (2 POINTS EACH) 1. When glucose levels are above 100 mg/dl, which of the following is
