International Journal of Medical Science in Clinical Research and Review
|
|
|
- Hugo Logan
- 5 years ago
- Views:
Transcription
1 International Journal of Medical Science in Clinical Research and Review Available Online at Volume 01 Issue Not all new Left Bundle Branch Block (LBBB) requires Cardiac Catheterization 1 Ang Alene, Wong, 2 Chun Hui Sharmaine, 3* Assoc. Prof. Fatimah Lateef, 4 Assoc. Prof. Dukes, 5 Dir. Singhealth Duke 1,2 M4 Student, National University of Singapore 3* Senior Consultant/ Director of Training and Education Dept. of Emergency Medicine, Singapore General Hospital 4 NUS Graduate Medical School and Yong Loo Lin School of Medicine, National University of Singapore 5 NUS Institute of Medical Simulation Abstract: *Correspondence Author: fatimah.abd.lateef@singhealth.com.sg Presence of concomitant left bundle brunch block (LBBB) in patients presenting with possible acute myocardial infarction (AMI) showcases a unique diagnostic and therapeutic challenge. Current guidelines recommend that patients with new or presumed new LBBB undergo emergency reperfusion therapy. However, only a minority of patients prove to have occluded artery at cardiac catheterization. Alternative strategies have been proposed to triage patients to select those suitable for acute reperfusion therapy, invasive and non-invasive cardiac investigations. We report a case of a 65-year-old man with atypical chest pain and new onset left bundle branch block on his electrocardiogram (ECG), who was managed without emergency reperfusion therapy, but instead, with observation and subsequent outpatient non-invasive cardiac investigation. Key Words: left bundle branch block, acute coronary syndrome, myocardial infaction, cardiac catheterization, Sgarbossa criteria Introduction: Between 1% and 9% of patients seeking evaluation for suspected acute myocardial infarction (AMI) have left bundle branch block (LBBB) (chronicity uncertain). Patients presenting with a new or presumed new onset LBBB, with suspected AMI present as an important diagnostic and management challenge (1,2). An electrocardiographic (ECG) diagnosis of ST-segment elevation AMI (STEMI) in these patients is difficult as altered ventricular depolarization in LBBB interfere with ST segment elevation analysis, due to ST-segment discordant changes which obscure or mimic ECG manifestations of STEMI. Complex algorithms created to assist diagnosis also do not always provide diagnostic certainty (3-6). LBBB is essentially a manifestation of disruption in the electrical conduction system of the heart. It has been noted in patients with cardiomyopathy as well as those without any known cardiac disease (2,6,7). Studies show that in patients with a clinical suspicion of ongoing myocardial ischemia, LBBB may suggest higher risk for mortality, sudden deaths, ischemic heart disease and congestive heart failure, compared to patients without a LBBB. This is because the left bundle branch is an anatomically large and diffuse structure, deeper in the myocardium than the right bundle branch, hence, a large insult leading to acute ischemic injury is typically involved. A LBBB has been considered to be a STEMI equivalent, and thought to require optimal management of urgently identifying coronary occlusion and promptly providing reperfusion therapy. LBBB can also arise in healthy hearts with no myocardial infarction, secondary to ischemic, structural heart disease or fibrotic conduction system, in conditions such as chronic ischemic heart disease, left ventricular hypertrophy, or cardiomyopathy. As such, LBBB also defines a subset of patients with chronic cardiac disease at high risk of morbidity and mortality when there is concomitant AMI (6-12). There are also observations of transient LBBB in some patients. This may be a step in the progression from a normal ECG to a chronic LBBB as has been suggested (2,7,8). It has also been observed that between 6% to 51% of all patients with suspected AMI and LBBB will ultimately be diagnosed with AMI based on Page 1
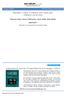
2 angiographic evidence. Although a significant proportion of patients will not have an occluded coronary artery at cardiac catheterization, previous guidelines recommended for LBBB to be an activating criterion for coronary angiography, in view of higher mortality in LBBB patients with AMI. A major disadvantage to this approach is overtreatment with a high false-positive catheterization laboratory activation rate among patients presenting with new-onset LBBB and exposure of a significant proportion of these patients to the risk of fibrinolytic therapy or invasive procedures (1,4,5,7-9). The Case Report: A 65-year-old Chinese gentleman, Mr. A, presented to the Emergency Department (ED) after routine health screening for the evaluation of his chest symptoms. He complained of a few months history of intermittent, localized left sided, sharp chest pain, radiating to left shoulder, with each episode lasting less than 10 minutes. This pain was worse with pressure over the area, but not on inspiration, and was relieved with rest. It was not progressively worsening with time, and was not associated with shortness of breath, diaphoresis, palpitations, Figure 1: The first ECG showing normal sinus rhythm syncope, nausea, or vomiting. The last episode of chest pain was four hours before arriving at the ED. He did not have any symptoms suggestive of acute decompensated heart failure, such as lower limb edema, reduced effort tolerance, orthopnea, or paroxysmal nocturnal dyspnea. Mr. A has a background of intermittent chest pain for the past 10 years, which he has never been formally evaluated for. However, this history was not consistent, as there were days when he could walk relatively long distances with no symptoms. He is a smoker of 50 pack-years, and has no other cardiovascular risk factors. He has a history of rectal cancer which had been resected more than 10 years ago. Mr. A is not on any medications, and does not have a family history of sudden cardiac deaths. The physical examination done was normal, as were his vital signs. The first ECG done is shown in Fig 1, with normal sinus rhythm. He was asymptomatic during consultation and the doctor sent off blood investigations which included, renal panel, full blood count, HbA1C, lipid panel and a chest X-ray was done. His 12 ECG was repeated 20 minutes after the first one and this is shown in Fig 2. This time a new LBBB was noted but the patient remained asymptomatic and vital signs were stable. Page 2
3 Figure 2: The second ECG which showed the new and acute onset LBBB All the initial blood investigations came back normal. A bedside 2D echocardiography noted a grade 1 left ventricular diastolic dysfunction, with ejection fraction 64% and no regional wall motion abnormalities. He was on telemetric monitoring and it was noted that he had reverted to normal sinus rhythm again. Thus, another 12 lead ECG was done. (Fig 3). Figure 3: The 12 lead ECG which was repeated when his telemetry recording was noted to have reverted back to normal sinus rhythm The cardiac catheterization laboratory was not activated in view that Mr. A remained asymptomatic. He was admitted to the inpatient Cardiology ward, where he was monitored and had another two serial cardiac enzymes done, which were also normal (not elevated) After evaluation by an electrophysiologist specialist, Mr. A was discharged with a scheduled outpatient myocardial perfusion imaging scan and Holter monitoring. Discussion: Currently, new guidelines no longer recommend treating new or presumably new LBBB as a STEMI equivalent with planned emergent reperfusion therapy. ACCF/AHA 2013 STEMI guidelines suggest not to consider a new LBBB at presentation alone diagnostic of STEMI (5). ESC 2017 STEMI guidelines recognize that the presence of a new LBBB does not predict AMI, but likely, ongoing myocardial ischemia and LBBB should be managed in a way similar to STEMI patients with early reperfusion therapy in the appropriate patients. Historically, the Sgarbossa ST-segment concordance criteria is used to assess the probability of AMI in new-onset LBBB. The initial study noted that a Sgarbossa's score >3 has a specificity of 96% for AMI but a sensitivity of only 36% (4). However, a recent meta-analysis suggested sensitivity of only 20% (6). In 2012, Smith et al. proposed a modified Sgarbossa rule replacing the third criterion with the ST/S ratio < 0.25 thus obtaining a 91% sensitivity and 90% specificity in prediction of acute coronary occlusion. (11) It was suggested that if validated in an independent study, the new criteria would provide a more sensitive tool to guide the decision for reperfusion therapy (6) Other new algorithms have also been proposed in recent years which include non-invasive test to counter the potential to overtreat Page 3
4 as according to ESC 2017 guidelines, and undertreat as according to ACCF/AHA 2013 guidelines. Cai et al. and Neeland et al. proposed a triage algorithm, suggesting for i) patients who present with hemodynamic instability or acute heart failure to be triaged to percutaneous coronary intervention (PCI) or fibrinolytic reperfusion; ii) hemodynamically stable patients with Sgarbossa score >3, ST/S ratio < 0.25 to be triaged to reperfusion therapy based on additional diagnostic tools including serial ECGs, serial troponin, and bedside echocardiogram; iii) patients with Sgarbossa score <3 and ST/S ratio > 0.25 to be also evaluated with the above mentioned additional investigation before deciding on whether they should receive angiography or non-invasive cardiac testing (8,9). This triage algorithm was again used in another study by Wyant et al., which concluded that its use facilitates more accurate diagnosis, fewer complications, better resource allocation, and improved risk stratification for patients (13). Our patient, Mr. A, experienced atypical chest pain, with a new-onset LBBB seen on ECG. Mr. A s Sgarbossa score was 0, ST/S ratio >0.25. Mr. A was also hemodynamically stable. The management of Mr. A took into account ACC/AHA 2013 and ESC 2017 STEMI guidelines, which suggest not to consider new-onset LBBB alone as diagnostic of AMI. In this case, the new triage algorithm by Cai et al. and Neeland et al. was applicable to evaluate Mr. A s new onset LBBB (8,9). According to the algorithm, Mr. A was not managed with perfusion therapy, but serial ECGs, troponin levels, as well as a bedside echocardiogram were done. Since results were unremarkable, Mr. A is less likely to have a NSTEMI or STEMI, and he was scheduled for outpatient noninvasive cardiac investigations. Mr. A represents a significant group of patients who presents with newonset LBBB, but do not actually have acute coronary occlusion (7). This case report is a positive validation of how a stable patient with new-onset LBBB and suspected AMI can be triaged using non-invasive investigations to conclude a low probability of STEMI, and subsequently, managed conservatively. This is as opposed to more invasive recommendations of present ESC 2017 STEMI guidelines, which do not advocate for use of other investigations to select patients for reperfusion therapy. On the other hand, the ACCF/AHA 2013 to recognize patients with chronic LBBB who actually do have STEMI, delaying reperfusion and increasing morbidity due to under-treatment. Hence, we recommend that noninvasive diagnostic tools included in the proposed triage algorithm to be used to aid in accurately determining appropriate interventions for these patients This will ensure that patients with the highest likelihood of STEMI will receive emergency perfusion therapy with little delay, whilst a more careful and judicious approach to rule out STEMI or NSTEMI and reduce overtreatment risks is taken for patients where clinical picture is less clear. Further research can be done to explore additional diagnostic and therapeutic strategies such as other cardiac biomarkers to predict AMI in the presence of new onset LBBB. A study by Wahab, M. suggests that ischemia modified albumin (IMA) can be used as an additional parameter to exclude cardiac ischemia in patients with LBBB (12). As more research is conducted on excluding AMI in new onset LBBB patients, the evaluation and ultimate management of patients with new onset LBBB can be modified and improved. More evidence can also be gathered for the proposed approach to suspected AMI with LBBB (13-18). Conclusion: Patients with suspected AMI and LBBB present as a unique diagnostic and therapeutic challenge. Current guideline recommendations do not account for the complexity and heterogeneity of this group of patients. Given the potential to reduce overtreatment (reduce rate of false positive catheterization laboratory activation, exposure to risk of fibrinolytic therapy and costs) and undertreatment (reduce mortality and morbidity), we recommend that the new triage algorithm to be taken into consideration to better evaluate new-onset LBBB with stable hemodynamics and no prominent ECG changes characteristic of STEMI (8, 9, 17-19). References: 1) Borja, I, Stefan J, Stefan et al. ESC Scientific Document Group; 2017 ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation: The Task Force for the management of acute myocardial infarction in patients presenting with ST-segment elevation of the European Society of Cardiology (ESC), European Heart Journal, 2018; 39(2): ) Chang AM, Shofer FS, Tabas JA, et al. Lack of association between left bundle-branch block and acute myocardial infarction in symptomatic STEMI guidelines lead to undertreatment by failing Page 4
5 ED patients. Am J Emerg Med. 2009; 27(8): ) Ciliberti, G. Left bundle branch block, chest pain and catheterization laboratory activation: an unavoidable cascade reaction? Journal of Electrocardiology 2016; 49 (4) ) Sgarbossa EB, Pinski SL, Barbagelata A Et al. Electrocardiographic diagnosis of evolving acute myocardial infarction in the presence of left bundle-branch block. GUSTO-1 (global utilization of streptokinase and tissue plasminogen activator for occluded coronary arteries) investigators. N Engl J Med 1996; 334 (8): ) Ghimire, G., Gupta, A., Hage, F. Guidelines in review: 2013 ACCF/AHA Guideline for the Management of ST-Elevation Myocardial Infarction. Journal of Nuclear Cardiology 2013; 21(1), doi: /s x 6) Tabas JA, Rodriguez RM, Seligman HA et al. Electrocardiographic criteria for detecting acute myocardial infarction in patients with left bundle branch block: a meta-analysis. Ann Emerg Med 2008; 52 (4): ) Jolobe, O. Timely catheterisation may still be necessary for all LBBB patients with suspected myocardial infarction. International Journal of Cardiology 2013; 170(1): p. e7. 8) Neeland, I J, Kontos MC, delemos JA. Evolving considerations in the management of patients with left bundle branch block and suspected myocardial infarction. J am Coll Cardiol 2012; 2(10): ) Cai Q, Mehta N, Sgarbossa EB et al. The left bundle-branch block puzzle in the 2013 STelevation myocardial infarction guideline: from falsely declaring emergency to denying reperfusion in a high-risk population. Are the sgarbossa criteria ready for prime time? Am Heart J 2013; 166 (3): ) McMahon R, Siow W, Bhindi R Et al. Left bundle branch block without concordant ST changes is rarely associated with acute coronary occlusion. Int J Cardiol 2013; 167: ) Smith SW, Dodd KW, Henry TD et al. Diagnosis of ST-elevation myocardial infarction in the presence of left bundle branch block with the STelevation to S-wave ratio in a modified Sgarbossa rule. Ann Emerg Med 2012; 60 (6): ) Wahab, M. Ischemia modified albumin (IMA) in acute coronary syndrome (ACS) and left bundle branch block (LBBB). Does it make the difference? The Egyptian Heart Journal 2017; 69(3), doi: /j.ehj ) Wyant, A., Chatterjee, S., Bennett, T. Managing chest pain in patients with concomitant left bundle-branch block. Journal of The American Academy of Physician Assistants 2017, 30(11): doi: /01.jaa c 14) Gabasha S, Ratajczak T. LBBB in a 29-year-old noncompetitive runner. Journal of Medical Cases 2017; 8(30: ) Kim JH, Baggish AL. ECG Right and Left BBB pattern in athletes: pathology and clinical significance. J Electrocardiol 2015; 48(3): ) Brown AS, Hoole SP, McCormick LM et al. LBBB with acute thrombotic occlusion is associated with increased myocardial jeopardy score, with poor clinical outcomes on primary percutaneous coronary intervention activation. Heart Br Card Soc 2013; 99: ) Jain S, Ting HT, Bell M Et al. Utility of LBBB as a diagnostic criterion for acute MI. Am J Cardiol 2011; 107: ) Kontos MC, Aziz AA, Chau VQ et al. Outcomes in patients with chronicity of LBBB with possible AMI. Am Heart J 2011; 161: ) Brown AJ, Malone-Lee M, McCormick LM et al. LBBB as an activation criterion for primary PCI: where is the evidence? Doi /heartjnl b.26 Page 5
Goals: Widen Your Understanding of the Wide QRS!
 Goals: Widen Your Understanding of the Wide QRS! 1. Describe an approach to diagnosis of LBBB 2. Describe the predictive value of New LBBB 3. Describe the ST segment changes that are diagnostic of AMI
Goals: Widen Your Understanding of the Wide QRS! 1. Describe an approach to diagnosis of LBBB 2. Describe the predictive value of New LBBB 3. Describe the ST segment changes that are diagnostic of AMI
Marcin Dada, MD December 03, 2013
 STEMI Imposters Marcin Dada, MD December 03, 2013 Marcin Dada, MD Associate Director, Chest Pain Center Hartford Hospital, Hartford, CT Member, AHA Mission Lifeline Steering Committee Outline of Topics
STEMI Imposters Marcin Dada, MD December 03, 2013 Marcin Dada, MD Associate Director, Chest Pain Center Hartford Hospital, Hartford, CT Member, AHA Mission Lifeline Steering Committee Outline of Topics
ECG Workshop. Nezar Amir
 ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
Παύλος Στουγιάννος. Καρδιολόγος ΓΝΑ «Η ΕΛΠΙΣ»
 Επεμβατική Καρδιολογία. STEMI. Σύγχρονη θεώρηση Παύλος Στουγιάννος Καρδιολόγος ΓΝΑ «Η ΕΛΠΙΣ» Criteria for acute myocardial infarction Thygesen K, et al. Third universal definition of myocardial infarction.
Επεμβατική Καρδιολογία. STEMI. Σύγχρονη θεώρηση Παύλος Στουγιάννος Καρδιολόγος ΓΝΑ «Η ΕΛΠΙΣ» Criteria for acute myocardial infarction Thygesen K, et al. Third universal definition of myocardial infarction.
Supplementary material 1. Definitions of study endpoints (extracted from the Endpoint Validation Committee Charter) 1.
 Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
CME Article Brugada pattern masking anterior myocardial infarction
 Electrocardiography Series Singapore Med J 2011; 52(9) : 647 CME Article Brugada pattern masking anterior myocardial infarction Seow S C, Omar A R, Hong E C T Cardiology Department, National University
Electrocardiography Series Singapore Med J 2011; 52(9) : 647 CME Article Brugada pattern masking anterior myocardial infarction Seow S C, Omar A R, Hong E C T Cardiology Department, National University
BEDSIDE ASSESSMENT OF PATIENTS WITH STEMI
 BEDSIDE ASSESSMENT OF PATIENTS WITH STEMI Prof. Maria Dorobantu, PhD, FESC, FACC Emergency Hospital of Bucharest, Romania Presenter Disclosures There are no conflicts/ grants/ disclosures for this presentation.
BEDSIDE ASSESSMENT OF PATIENTS WITH STEMI Prof. Maria Dorobantu, PhD, FESC, FACC Emergency Hospital of Bucharest, Romania Presenter Disclosures There are no conflicts/ grants/ disclosures for this presentation.
Acute Myocardial Infarction
 Acute Myocardial Infarction Hafeza Shaikh, DO, FACC, RPVI Lourdes Cardiology Services Asst.Program Director, Cardiology Fellowship Associate Professor, ROWAN-SOM Acute Myocardial Infarction Definition:
Acute Myocardial Infarction Hafeza Shaikh, DO, FACC, RPVI Lourdes Cardiology Services Asst.Program Director, Cardiology Fellowship Associate Professor, ROWAN-SOM Acute Myocardial Infarction Definition:
Acute Myocardial Infarction. Willis E. Godin D.O., FACC
 Acute Myocardial Infarction Willis E. Godin D.O., FACC Acute Myocardial Infarction Definition: Decreased delivery of oxygen and nutrients to the myocardium Myocardial tissue necrosis causing irreparable
Acute Myocardial Infarction Willis E. Godin D.O., FACC Acute Myocardial Infarction Definition: Decreased delivery of oxygen and nutrients to the myocardium Myocardial tissue necrosis causing irreparable
9/2/2016 CARDIOLOGY TESTING WHAT TO ORDER WHEN REFERENCE OBJECTIVES
 CARDIOLOGY TESTING WHAT TO ORDER WHEN A J W A D F A R A H, M S, P A - C A S S O C I A T E D I R E C T O R O F M E D I C A L O P E R A T I O N S O F A D V A N C E D P R A C T I C E P R O V I D E R S W I
CARDIOLOGY TESTING WHAT TO ORDER WHEN A J W A D F A R A H, M S, P A - C A S S O C I A T E D I R E C T O R O F M E D I C A L O P E R A T I O N S O F A D V A N C E D P R A C T I C E P R O V I D E R S W I
Particularities of Coronary Artery Disease in Hypertensive Patients with Left Bundle Branch Block Larisa ANGHEL a ; Catalina ARSENESCU GEORGESCU a,b
 MAEDICA a Journal of Clinical Medicine 2014; 9(4): 333-337 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Particularities of Coronary Artery Disease in Patients with Left Bundle Branch Block Larisa
MAEDICA a Journal of Clinical Medicine 2014; 9(4): 333-337 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Particularities of Coronary Artery Disease in Patients with Left Bundle Branch Block Larisa
Diagnosis of Myocardial Infarction/Ischemia with Bundle Branch Blocks
 Diagnosis of Myocardial Infarction/Ischemia with Bundle Branch Blocks Mark I. Langdorf, MD, MHPE, FACEP, FAAEM, RDMS Professor and Chair Associate Residency Director Department of Emergency Medicine University
Diagnosis of Myocardial Infarction/Ischemia with Bundle Branch Blocks Mark I. Langdorf, MD, MHPE, FACEP, FAAEM, RDMS Professor and Chair Associate Residency Director Department of Emergency Medicine University
Myocardial Infarction. Reading Assignment (p66-78 in Outline )
 Myocardial Infarction Reading Assignment (p66-78 in Outline ) Objectives 1. Why do ST segments go up or down in ischemia? 2. STEMI locations and culprit vessels 3. Why 15-lead ECGs? 4. What s up with avr?
Myocardial Infarction Reading Assignment (p66-78 in Outline ) Objectives 1. Why do ST segments go up or down in ischemia? 2. STEMI locations and culprit vessels 3. Why 15-lead ECGs? 4. What s up with avr?
Chest Pain. Dr Robert Huggett Consultant Cardiologist
 Chest Pain Dr Robert Huggett Consultant Cardiologist Outline Diagnosis of cardiac chest pain 2016 NICE update on stable chest pain Assessment of unstable chest pain/acs and MI definition Scope of the
Chest Pain Dr Robert Huggett Consultant Cardiologist Outline Diagnosis of cardiac chest pain 2016 NICE update on stable chest pain Assessment of unstable chest pain/acs and MI definition Scope of the
DR ALEXIA STAVRATI CARDIOLOGIST, DIRECTOR OF CARDIOLOGY DEPT, "G. PAPANIKOLAOU" GH, THESSALONIKI
 The Impact of AF on Natural History of CAD DR ALEXIA STAVRATI CARDIOLOGIST, DIRECTOR OF CARDIOLOGY DEPT, "G. PAPANIKOLAOU" GH, THESSALONIKI CAD MOST COMMON CARDIOVASCULAR DISEASE MOST COMMON CAUSE OF DEATH
The Impact of AF on Natural History of CAD DR ALEXIA STAVRATI CARDIOLOGIST, DIRECTOR OF CARDIOLOGY DEPT, "G. PAPANIKOLAOU" GH, THESSALONIKI CAD MOST COMMON CARDIOVASCULAR DISEASE MOST COMMON CAUSE OF DEATH
Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist. Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI
 Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist physician Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI Outcome objectives of the discussion: At the end of the
Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist physician Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI Outcome objectives of the discussion: At the end of the
From left bundle branch block to cardiac failure
 OF JOURNAL HYPERTENSION JH R RESEARCH Journal of HYPERTENSION RESEARCH www.hypertens.org/jhr Original Article J Hypertens Res (2017) 3(3):90 97 From left bundle branch block to cardiac failure Cătălina
OF JOURNAL HYPERTENSION JH R RESEARCH Journal of HYPERTENSION RESEARCH www.hypertens.org/jhr Original Article J Hypertens Res (2017) 3(3):90 97 From left bundle branch block to cardiac failure Cătălina
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Stress Testing:Which Study is Indicated for My Patient?
 Stress Testing:Which Study is Indicated for My Patient? Cardiology-Primary Care Conference 7/14/17 Peter Casterella, MD Co-Executive Director Swedish Heart and Vascular Institute 1 Stress Testing Options
Stress Testing:Which Study is Indicated for My Patient? Cardiology-Primary Care Conference 7/14/17 Peter Casterella, MD Co-Executive Director Swedish Heart and Vascular Institute 1 Stress Testing Options
Acute Coronary Syndrome
 ACUTE CORONOARY SYNDROME, ANGINA & ACUTE MYOCARDIAL INFARCTION Administrative Consultant Service 3/17 Acute Coronary Syndrome Acute Coronary Syndrome has evolved as a useful operational term to refer to
ACUTE CORONOARY SYNDROME, ANGINA & ACUTE MYOCARDIAL INFARCTION Administrative Consultant Service 3/17 Acute Coronary Syndrome Acute Coronary Syndrome has evolved as a useful operational term to refer to
Acute Coronary Syndrome. Emergency Department Updated Jan. 2017
 Acute Coronary Syndrome Emergency Department Updated Jan. 2017 Goals and Objectives To reduce mortality and morbidity for people who have cardiovascular disease, with a focus on those who experience an
Acute Coronary Syndrome Emergency Department Updated Jan. 2017 Goals and Objectives To reduce mortality and morbidity for people who have cardiovascular disease, with a focus on those who experience an
The Fundamentals of 12 Lead EKG. ECG Recording. J Point. Reviewing the Cardiac Conductive System. Dr. E. Joe Sasin, MD Rusty Powers, NRP
 The Fundamentals of 12 Lead EKG Dr. E. Joe Sasin, MD Rusty Powers, NRP SA Node Intranodal Pathways AV Junction AV Fibers Bundle of His Septum Bundle Branches Purkinje System Reviewing the Cardiac Conductive
The Fundamentals of 12 Lead EKG Dr. E. Joe Sasin, MD Rusty Powers, NRP SA Node Intranodal Pathways AV Junction AV Fibers Bundle of His Septum Bundle Branches Purkinje System Reviewing the Cardiac Conductive
Cardiac Ischemia ECG Workshop
 Cardiac Ischemia ECG Workshop Classic, Confusing, and Confounding Patterns Amal Mattu, MD, NE Professor and Vice Chair Department of Emergency Medicine University of Maryland School of Medicine amalmattu@comcast.net
Cardiac Ischemia ECG Workshop Classic, Confusing, and Confounding Patterns Amal Mattu, MD, NE Professor and Vice Chair Department of Emergency Medicine University of Maryland School of Medicine amalmattu@comcast.net
VCU HEALTH SYSTEM EMERGENCY DEPARTMENT GUIDELINE
 VCU HEALTH SYSTEM EMERGENCY DEPARTMENT GUIDELINE SUBJECT: Care of the Chest Pain Patient in the Emergency Department FILE SECTION: VCUHS/ED Section: Please note: Clinical Practice Guideline Evidence-based
VCU HEALTH SYSTEM EMERGENCY DEPARTMENT GUIDELINE SUBJECT: Care of the Chest Pain Patient in the Emergency Department FILE SECTION: VCUHS/ED Section: Please note: Clinical Practice Guideline Evidence-based
Pre Hospital and Initial Management of Acute Coronary Syndrome
 Pre Hospital and Initial Management of Acute Coronary Syndrome Dr. Muhammad Fadil, SpJP 3rd SymCARD 2013 Classification of ACS ESC Guidelines for the management of Acute Coronary Syndrome in patients without
Pre Hospital and Initial Management of Acute Coronary Syndrome Dr. Muhammad Fadil, SpJP 3rd SymCARD 2013 Classification of ACS ESC Guidelines for the management of Acute Coronary Syndrome in patients without
Improving the Outcomes of
 Improving the Outcomes of STEMI Shelley Valaire, ACP; and Robert Welsh, MD, FRCPC Presented at the University of Alberta s 6th Annual Cardiology Update for General Practitioners and Internists, Edmonton,
Improving the Outcomes of STEMI Shelley Valaire, ACP; and Robert Welsh, MD, FRCPC Presented at the University of Alberta s 6th Annual Cardiology Update for General Practitioners and Internists, Edmonton,
HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM
 REVIEW DATE REVIEWER'S ID HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM : DISCHARGE DATE: RECORDS FROM: Hospitalization ER Please check all that may apply: Myocardial Infarction Pages 2, 3,
REVIEW DATE REVIEWER'S ID HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM : DISCHARGE DATE: RECORDS FROM: Hospitalization ER Please check all that may apply: Myocardial Infarction Pages 2, 3,
INTERPRETAZIONE ECG NEL PAZIENTE CON SOSPETTO STEMI
 INTERPRETAZIONE ECG NEL PAZIENTE CON SOSPETTO STEMI Giacomo Veronese Scuola di Specializzazione Medicina d Emergenza e Urgenza Università Milano-Bicocca Siete d accordo se vi propongo per una relazione..
INTERPRETAZIONE ECG NEL PAZIENTE CON SOSPETTO STEMI Giacomo Veronese Scuola di Specializzazione Medicina d Emergenza e Urgenza Università Milano-Bicocca Siete d accordo se vi propongo per una relazione..
10/22/16. Lay of the land. Definition of ACS. Why do we worry about ST elevations?
 Lay of the land Update on Acute Coronary Syndrome: Five Things Hospitalists Must Know Dhruv S. Kazi, MD, MSc, MS Assistant Professor Department of Medicine (Cardiology), Department of Epidemiology and
Lay of the land Update on Acute Coronary Syndrome: Five Things Hospitalists Must Know Dhruv S. Kazi, MD, MSc, MS Assistant Professor Department of Medicine (Cardiology), Department of Epidemiology and
TOPICS IN EMERGENCY MEDICINE SEMI-FINAL
 RISK ASSESSMENT IN PATIENTS WITH CHEST PAIN Nora Goldschlager, M.D. FACP, FACC, FAHA, FHRS Cardiology - San Francisco General Hospital UCSF Disclosures: None 1 CHEST PAIN NOT DUE TO MYOCARDIAL ISCHEMIA
RISK ASSESSMENT IN PATIENTS WITH CHEST PAIN Nora Goldschlager, M.D. FACP, FACC, FAHA, FHRS Cardiology - San Francisco General Hospital UCSF Disclosures: None 1 CHEST PAIN NOT DUE TO MYOCARDIAL ISCHEMIA
presenters 2010 Sameh Sabet Ain Shams University
 Guidelines for PCI in late STEMI presenters 2010 Sameh Sabet Assistant Professor of Cardiology Ain Shams University 29% of MI patients have STEMI. NRMI 4 (Fourth National Registry of Myocardial Infarction),
Guidelines for PCI in late STEMI presenters 2010 Sameh Sabet Assistant Professor of Cardiology Ain Shams University 29% of MI patients have STEMI. NRMI 4 (Fourth National Registry of Myocardial Infarction),
Acute Coronary Syndrome. Sonny Achtchi, DO
 Acute Coronary Syndrome Sonny Achtchi, DO Objectives Understand evidence based and practice based treatments for stabilization and initial management of ACS Become familiar with ACS risk stratification
Acute Coronary Syndrome Sonny Achtchi, DO Objectives Understand evidence based and practice based treatments for stabilization and initial management of ACS Become familiar with ACS risk stratification
High Value Evaluation of Chest Pain. Zoom Tips
 High Value Evaluation of Chest Pain California Quality Collaborative s Cardiology Webinar Series Webinar 1 December 7, 2017 Zoom Tips Attendees are automatically MUTED upon entry Refrain from using the
High Value Evaluation of Chest Pain California Quality Collaborative s Cardiology Webinar Series Webinar 1 December 7, 2017 Zoom Tips Attendees are automatically MUTED upon entry Refrain from using the
2018 HPN Provider Summary Guide. Adult Cardiology Patients (18 Years and Older) Referral Guidelines
 12.2 CARDIOLOGY REFERRAL GUIDELINES Contracted Group: Southwest Medical Associates For Appointments: 888 S. Rancho Las Vegas, NV 89109 Phone: (702) 877-8654 Fax: (702) 242-7998 Adult Cardiology Patients
12.2 CARDIOLOGY REFERRAL GUIDELINES Contracted Group: Southwest Medical Associates For Appointments: 888 S. Rancho Las Vegas, NV 89109 Phone: (702) 877-8654 Fax: (702) 242-7998 Adult Cardiology Patients
I have no financial disclosures
 Manpreet Singh MD I have no financial disclosures Exercise Treadmill Bicycle Functional capacity assessment Well validated prognostic value Ischemic assessment ECG changes ST segments Arrhythmias Hemodynamic
Manpreet Singh MD I have no financial disclosures Exercise Treadmill Bicycle Functional capacity assessment Well validated prognostic value Ischemic assessment ECG changes ST segments Arrhythmias Hemodynamic
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases
 Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Imaging ischemic heart disease: role of SPECT and PET. Focus on Patients with Known CAD
 Imaging ischemic heart disease: role of SPECT and PET. Focus on Patients with Known CAD Hein J. Verberne Academic Medical Center, University of Amsterdam, Amsterdam, Netherlands International Conference
Imaging ischemic heart disease: role of SPECT and PET. Focus on Patients with Known CAD Hein J. Verberne Academic Medical Center, University of Amsterdam, Amsterdam, Netherlands International Conference
2010 ACLS Guidelines. Primary goals of therapy for patients
 2010 ACLS Guidelines Part 10: Acute Coronary Syndrome Present : 內科 R1 鍾伯欣 Supervisor: F1 吳亮廷 991110 Primary goals of therapy for patients of ACS Reduce the amount of myocardial necrosis that occurs in
2010 ACLS Guidelines Part 10: Acute Coronary Syndrome Present : 內科 R1 鍾伯欣 Supervisor: F1 吳亮廷 991110 Primary goals of therapy for patients of ACS Reduce the amount of myocardial necrosis that occurs in
Name Authentication Date (Position or Committee) Quality & Patient Safety Steering. Meeting Minutes & 08/14 Committee
 Title: Document Number: Document Type: Affected Departments: Review Bodies: Revision/(Review) Dates: (Dates that included only a review, but no content 07/14 revision, are in parentheses) Effective Date:
Title: Document Number: Document Type: Affected Departments: Review Bodies: Revision/(Review) Dates: (Dates that included only a review, but no content 07/14 revision, are in parentheses) Effective Date:
Chest pain affects 20% to 40% of the general population during their lifetime.
 Chest pain affects 20% to 40% of the general population during their lifetime. More than 5% of visits in the emergency department, and up to 40% of admissions are because of chest pain. Chest pain is a
Chest pain affects 20% to 40% of the general population during their lifetime. More than 5% of visits in the emergency department, and up to 40% of admissions are because of chest pain. Chest pain is a
OUTCOME OF THROMBOLYTIC AND NON- THROMBOLYTIC THERAPY IN ACUTE MYOCARDIAL INFARCTION
 OUTCOME OF THROMBOLYTIC AND NON- THROMBOLYTIC THERAPY IN ACUTE MYOCARDIAL INFARCTION FEROZ MEMON*, LIAQUAT CHEEMA**, NAND LAL RATHI***, RAJ KUMAR***, NAZIR AHMED MEMON**** OBJECTIVE: To compare morbidity,
OUTCOME OF THROMBOLYTIC AND NON- THROMBOLYTIC THERAPY IN ACUTE MYOCARDIAL INFARCTION FEROZ MEMON*, LIAQUAT CHEEMA**, NAND LAL RATHI***, RAJ KUMAR***, NAZIR AHMED MEMON**** OBJECTIVE: To compare morbidity,
UPDATE ON THE MANAGEMENTACUTE CORONARY SYNDROME. DR JULES KABAHIZI, Psc (Rwa) Lt Col CHIEF CONSULTANT RMH/KFH 28 JUNE18
 UPDATE ON THE MANAGEMENTACUTE CORONARY SYNDROME DR JULES KABAHIZI, Psc (Rwa) Lt Col CHIEF CONSULTANT RMH/KFH 28 JUNE18 INTRODUCTION The clinical entities that comprise acute coronary syndromes (ACS)-ST-segment
UPDATE ON THE MANAGEMENTACUTE CORONARY SYNDROME DR JULES KABAHIZI, Psc (Rwa) Lt Col CHIEF CONSULTANT RMH/KFH 28 JUNE18 INTRODUCTION The clinical entities that comprise acute coronary syndromes (ACS)-ST-segment
Guideline Number: NIA_CG_024 Last Review Date: January 2011 Responsible Department: Last Revised Date: May 2, 2011 Clinical Operations
 National Imaging Associates, Inc. Clinical guidelines NUCLEAR CARDIAC IMAGING (MYOCARDIAL PERFUSION STUDY) CPT Codes: 78451, 78452, 78453, 78454, 78466, 78468, 78469, 78481, 78483, 78494, 78499 Original
National Imaging Associates, Inc. Clinical guidelines NUCLEAR CARDIAC IMAGING (MYOCARDIAL PERFUSION STUDY) CPT Codes: 78451, 78452, 78453, 78454, 78466, 78468, 78469, 78481, 78483, 78494, 78499 Original
Optimal testing for coronary artery disease in symptomatic and asymptomatic patients
 Optimal testing for coronary artery disease in symptomatic and asymptomatic patients Alexandre C Ferreira, MD Clinical Chief of Cardiology Jackson Health System Director, Interventional Cardiology Training
Optimal testing for coronary artery disease in symptomatic and asymptomatic patients Alexandre C Ferreira, MD Clinical Chief of Cardiology Jackson Health System Director, Interventional Cardiology Training
FFR-CT Not Ready for Primetime
 FFR-CT Not Ready for Primetime Leslee J. Shaw, PhD, MASNC, FACC, FAHA, FSCCT R. Bruce Logue Professor of Medicine Co-Director, Emory Clinical CV Research Institute Emory University School of Medicine Atlanta,
FFR-CT Not Ready for Primetime Leslee J. Shaw, PhD, MASNC, FACC, FAHA, FSCCT R. Bruce Logue Professor of Medicine Co-Director, Emory Clinical CV Research Institute Emory University School of Medicine Atlanta,
Acute chest pain and ECG need for immediate coronary angiography?
 Acute chest pain and ECG need for immediate coronary angiography? Kjell Nikus, MD, PhD Heart Center, Tampere University Hospital, Finland and Samuel Sclarovsky, MD, PhD Tel Aviv University, Israel There
Acute chest pain and ECG need for immediate coronary angiography? Kjell Nikus, MD, PhD Heart Center, Tampere University Hospital, Finland and Samuel Sclarovsky, MD, PhD Tel Aviv University, Israel There
Continuing Medical Education Post-Test
 Continuing Medical Education Post-Test Based on the information presented in this monograph, please choose one correct response for each of the following questions or statements. Record your answers on
Continuing Medical Education Post-Test Based on the information presented in this monograph, please choose one correct response for each of the following questions or statements. Record your answers on
Acute Coronary Syndromes Unstable Angina Non ST segment Elevation MI (NSTEMI) ST segment Elevation MI (STEMI)
 Leanna R. Miller, RN, MN, CCRN-CSC, PCCN-CMC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Evaluate common abnormalities that mimic myocardial infarction. Identify
Leanna R. Miller, RN, MN, CCRN-CSC, PCCN-CMC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Evaluate common abnormalities that mimic myocardial infarction. Identify
Simon A. Mahler MD, MS, FACEP Associate Professor Department of Emergency Medicine Wake Forest School of Medicine
 Simon A. Mahler MD, MS, FACEP Associate Professor Department of Emergency Medicine Wake Forest School of Medicine Research funding: American Heart Association Donaghue Foundation/ Association of American
Simon A. Mahler MD, MS, FACEP Associate Professor Department of Emergency Medicine Wake Forest School of Medicine Research funding: American Heart Association Donaghue Foundation/ Association of American
Biphasic T-wave in patient with chest pain (Wellens syndrome)
 www.edoriumjournals.com CLINICAL IMAGES PEER REVIEWED OPEN ACCESS Biphasic T-wave in patient with chest pain (Wellens syndrome) Ahmed Zedan, Osama Mukarram, Umer Malik, Raja Naidu ABSTRACT Abstract is
www.edoriumjournals.com CLINICAL IMAGES PEER REVIEWED OPEN ACCESS Biphasic T-wave in patient with chest pain (Wellens syndrome) Ahmed Zedan, Osama Mukarram, Umer Malik, Raja Naidu ABSTRACT Abstract is
Objectives. Identify early signs and symptoms of Acute Coronary Syndrome Initiate proper protocol for ACS patient 10/2013 2
 10/2013 1 Objectives Identify early signs and symptoms of Acute Coronary Syndrome Initiate proper protocol for ACS patient 10/2013 2 Purpose of this Education Module: Chest Pain Center Accreditation involves
10/2013 1 Objectives Identify early signs and symptoms of Acute Coronary Syndrome Initiate proper protocol for ACS patient 10/2013 2 Purpose of this Education Module: Chest Pain Center Accreditation involves
CLINICIAN INTERVIEW RECOGNIZING ACS AND STRATIFYING RISK IN PRIMARY CARE. An interview with A. Michael Lincoff, MD, and Eric R. Bates, MD, FACC, FAHA
 RECOGNIZING ACS AND STRATIFYING RISK IN PRIMARY CARE An interview with A. Michael Lincoff, MD, and Eric R. Bates, MD, FACC, FAHA Dr Lincoff is an interventional cardiologist and the Vice Chairman for Research
RECOGNIZING ACS AND STRATIFYING RISK IN PRIMARY CARE An interview with A. Michael Lincoff, MD, and Eric R. Bates, MD, FACC, FAHA Dr Lincoff is an interventional cardiologist and the Vice Chairman for Research
Evolving Considerations in the Management of Patients With Left Bundle Branch Block and Suspected Myocardial Infarction
 Journal of the American College of Cardiology Vol. 60, No. 2, 2012 2012 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. http://dx.doi.org/10.1016/j.jacc.2012.02.054
Journal of the American College of Cardiology Vol. 60, No. 2, 2012 2012 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. http://dx.doi.org/10.1016/j.jacc.2012.02.054
CMS Limitations Guide - Cardiovascular Services
 CMS Limitations Guide - Cardiovascular Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Cardiovascular Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
Choosing the Appropriate Stress Test: Brett C. Stoll, MD, FACC February 24, 2018
 Choosing the Appropriate Stress Test: Brett C. Stoll, MD, FACC February 24, 2018 Choosing the Appropriate Stress Test: Does it Really Matter? Brett C. Stoll, MD, FACC February 24, 2018 Conflicts of Interest
Choosing the Appropriate Stress Test: Brett C. Stoll, MD, FACC February 24, 2018 Choosing the Appropriate Stress Test: Does it Really Matter? Brett C. Stoll, MD, FACC February 24, 2018 Conflicts of Interest
Stress ECG is still Viable in Suleiman M Kharabsheh, MD, FACC Consultant Invasive Cardiologist KFHI KFSHRC-Riyadh
 Stress ECG is still Viable in 2016 Suleiman M Kharabsheh, MD, FACC Consultant Invasive Cardiologist KFHI KFSHRC-Riyadh Stress ECG Do we still need stress ECG with all the advances we have in the CV field?
Stress ECG is still Viable in 2016 Suleiman M Kharabsheh, MD, FACC Consultant Invasive Cardiologist KFHI KFSHRC-Riyadh Stress ECG Do we still need stress ECG with all the advances we have in the CV field?
Cardiovascular Images
 Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
12 Lead ECG Interpretation
 12 Lead ECG Interpretation Julie Zimmerman, MSN, RN, CNS, CCRN Significant increase in mortality for every 15 minutes of delay! N Engl J Med 2007;357:1631-1638 Who should get a 12-lead ECG? Also include
12 Lead ECG Interpretation Julie Zimmerman, MSN, RN, CNS, CCRN Significant increase in mortality for every 15 minutes of delay! N Engl J Med 2007;357:1631-1638 Who should get a 12-lead ECG? Also include
Common Codes for ICD-10
 Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
12 Lead EKG Chapter 4 Worksheet
 Match the following using the word bank. 1. A form of arteriosclerosis in which the thickening and hardening of the vessels walls are caused by an accumulation of fatty deposits in the innermost lining
Match the following using the word bank. 1. A form of arteriosclerosis in which the thickening and hardening of the vessels walls are caused by an accumulation of fatty deposits in the innermost lining
DISCUSSION QUESTION - 1
 CASE PRESENTATION 87 year old male No past history of diabetes, HTN, dyslipidemia or smoking Very active Medications: omeprazole for heart burn Admitted because of increasing retrosternal chest pressure
CASE PRESENTATION 87 year old male No past history of diabetes, HTN, dyslipidemia or smoking Very active Medications: omeprazole for heart burn Admitted because of increasing retrosternal chest pressure
The PAIN Pathway for the Management of Acute Coronary Syndrome
 2 The PAIN Pathway for the Management of Acute Coronary Syndrome Eyal Herzog, Emad Aziz, and Mun K. Hong Acute coronary syndrome (ACS) subsumes a spectrum of clinical entities, ranging from unstable angina
2 The PAIN Pathway for the Management of Acute Coronary Syndrome Eyal Herzog, Emad Aziz, and Mun K. Hong Acute coronary syndrome (ACS) subsumes a spectrum of clinical entities, ranging from unstable angina
7. Echocardiography Appropriate Use Criteria (by Indication)
 Criteria for Echocardiography 1133 7. Echocardiography Criteria (by ) Table 1. TTE for General Evaluation of Cardiac Structure and Function Suspected Cardiac Etiology General With TTE 1. Symptoms or conditions
Criteria for Echocardiography 1133 7. Echocardiography Criteria (by ) Table 1. TTE for General Evaluation of Cardiac Structure and Function Suspected Cardiac Etiology General With TTE 1. Symptoms or conditions
ST-elevation myocardial infarctions (STEMIs)
 Guidelines for Treating STEMI: Case-Based Questions As many as 25% of eligible patients presenting with STEMI do not receive any form of reperfusion therapy. The ACC/AHA guidelines highlight steps to improve
Guidelines for Treating STEMI: Case-Based Questions As many as 25% of eligible patients presenting with STEMI do not receive any form of reperfusion therapy. The ACC/AHA guidelines highlight steps to improve
OVERVIEW ACUTE CORONARY SYNDROME SYMPTOMS 9/30/14 TYPICAL WHAT IS ACUTE CORONARY SYNDROME? SYMPTOMS, IDENTIFICATION, MANAGEMENT
 OVERVIEW ACUTE CORONARY SYNDROME SYMPTOMS, IDENTIFICATION, MANAGEMENT OCTOBER 7, 2014 PETE PERAUD, MD SYMPTOMS TYPICAL ATYPICAL IDENTIFICATION EKG CARDIAC BIOMARKERS STEMI VS NON-STEMI VS USA MANAGEMENT
OVERVIEW ACUTE CORONARY SYNDROME SYMPTOMS, IDENTIFICATION, MANAGEMENT OCTOBER 7, 2014 PETE PERAUD, MD SYMPTOMS TYPICAL ATYPICAL IDENTIFICATION EKG CARDIAC BIOMARKERS STEMI VS NON-STEMI VS USA MANAGEMENT
2008, American Heart Association. All rights reserved.
 AHA 2008 Cocaine-Associated Chest Pain and Myocardial Infarction Slide Set Based on the AHA 2008 Scientific Statement for Management of Cocaine-Associated Chest Pain and Myocardial Infarction George J.
AHA 2008 Cocaine-Associated Chest Pain and Myocardial Infarction Slide Set Based on the AHA 2008 Scientific Statement for Management of Cocaine-Associated Chest Pain and Myocardial Infarction George J.
HEART CONDITIONS IN SPORT
 HEART CONDITIONS IN SPORT Dr. Anita Green CHD Risk Factors Smoking Hyperlipidaemia Hypertension Obesity Physical Inactivity Diabetes Risks are cumulative (multiplicative) Lifestyles predispose to RF One
HEART CONDITIONS IN SPORT Dr. Anita Green CHD Risk Factors Smoking Hyperlipidaemia Hypertension Obesity Physical Inactivity Diabetes Risks are cumulative (multiplicative) Lifestyles predispose to RF One
New universal definition of myocardial infarction
 New universal definition of myocardial infarction L. K. Michalis, ΜRCP, FESC Professor of Cardiology, University of Ioannina Changing Criteria for definition of MI Primarily clinical & ECG approach First
New universal definition of myocardial infarction L. K. Michalis, ΜRCP, FESC Professor of Cardiology, University of Ioannina Changing Criteria for definition of MI Primarily clinical & ECG approach First
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice Review consultation document Review of Clinical Guideline (CG95) Chest pain of recent onset: Assessment and diagnosis
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice Review consultation document Review of Clinical Guideline (CG95) Chest pain of recent onset: Assessment and diagnosis
A. BISOC 1,2 A.M. PASCU 1 M. RĂDOI 1,2
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 THE ctntg4 PLASMA LEVELS IN RELATION TO ELECTROCARDIOGRAPHIC AND ECHOCARDIOGRAPHIC ABNORMALITIES IN
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 THE ctntg4 PLASMA LEVELS IN RELATION TO ELECTROCARDIOGRAPHIC AND ECHOCARDIOGRAPHIC ABNORMALITIES IN
Significance of QRS duration in non-st elevation myocardial infarction.
 Thomas Jefferson University Jefferson Digital Commons Cardiology Faculty Papers Department of Cardiology 5-6-2015 Significance of QRS duration in non-st elevation myocardial infarction. Chinualumogu Nwakile
Thomas Jefferson University Jefferson Digital Commons Cardiology Faculty Papers Department of Cardiology 5-6-2015 Significance of QRS duration in non-st elevation myocardial infarction. Chinualumogu Nwakile
Original Policy Date
 MP 2.02.18 Electrocardiographic Body Surface Mapping Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature review/12:2013 Return to
MP 2.02.18 Electrocardiographic Body Surface Mapping Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature review/12:2013 Return to
Listing Form: Heart or Cardiovascular Impairments. Medical Provider:
 Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
Supplementary Table 1. Details of the components of the primary composite endpoint
 Supplementary Table 1. Details of the components of the primary composite endpoint 1. Death The cause of death will be defined by the underlying cause, not the immediate mode of death. Death will be classified
Supplementary Table 1. Details of the components of the primary composite endpoint 1. Death The cause of death will be defined by the underlying cause, not the immediate mode of death. Death will be classified
My Patient Needs a Stress Test
 My Patient Needs a Stress Test Amy S. Burhanna,, MD, FACC Coastal Cardiology Cape May Court House, New Jersey Absolute and relative contraindications to exercise testing Absolute Acute myocardial infarction
My Patient Needs a Stress Test Amy S. Burhanna,, MD, FACC Coastal Cardiology Cape May Court House, New Jersey Absolute and relative contraindications to exercise testing Absolute Acute myocardial infarction
P F = R. Disorder of the Breast. Approach to the Patient with Chest Pain. Typical Characteristics of Angina Pectoris. Myocardial Ischemia
 Disorder of the Breast Approach to the Patient with Chest Pain Anthony J. Minisi, MD Department of Internal Medicine, Division of Cardiology Virginia Commonwealth University School of Medicine William
Disorder of the Breast Approach to the Patient with Chest Pain Anthony J. Minisi, MD Department of Internal Medicine, Division of Cardiology Virginia Commonwealth University School of Medicine William
Observation Medicine ECG Instructor Workshop session 2 Serial 12 Lead ECG Interpretation
 American College of Cardiology 20 th Congress 2017 Observation Medicine ECG Instructor Workshop session 2 Serial 12 Lead ECG Interpretation Part 1 By: Wayne W Ruppert, CVT, CCCC, NREMT-P This curriculum
American College of Cardiology 20 th Congress 2017 Observation Medicine ECG Instructor Workshop session 2 Serial 12 Lead ECG Interpretation Part 1 By: Wayne W Ruppert, CVT, CCCC, NREMT-P This curriculum
The Value of Stress MRI in Evaluation of Myocardial Ischemia
 The Value of Stress MRI in Evaluation of Myocardial Ischemia Dr. Saeed Al Sayari, MBBS, EBCR, MBA Department of Radiology and Nuclear Medicine Mafraq Hospital, Abu Dhabi United Arab Emirates Introduction
The Value of Stress MRI in Evaluation of Myocardial Ischemia Dr. Saeed Al Sayari, MBBS, EBCR, MBA Department of Radiology and Nuclear Medicine Mafraq Hospital, Abu Dhabi United Arab Emirates Introduction
Use of Nuclear Cardiology in Myocardial Viability Assessment and Introduction to PET and PET/CT for Advanced Users
 Use of Nuclear Cardiology in Myocardial Viability Assessment and Introduction to PET and PET/CT for Advanced Users February 1 5, 2011 University of Santo Tomas Hospital Angelo King A-V Auditorium Manila,
Use of Nuclear Cardiology in Myocardial Viability Assessment and Introduction to PET and PET/CT for Advanced Users February 1 5, 2011 University of Santo Tomas Hospital Angelo King A-V Auditorium Manila,
Cardiac evaluation for the noncardiac. Nathaen Weitzel MD University of Colorado Denver Dept of Anesthesiology
 Cardiac evaluation for the noncardiac patient Nathaen Weitzel MD University of Colorado Denver Dept of Anesthesiology Objectives! Review ACC / AHA guidelines as updated for 2009! Discuss new recommendations
Cardiac evaluation for the noncardiac patient Nathaen Weitzel MD University of Colorado Denver Dept of Anesthesiology Objectives! Review ACC / AHA guidelines as updated for 2009! Discuss new recommendations
Cardiovascular Health Nova Scotia Update to Antiplatelet Sections of the Nova Scotia Guidelines for Acute Coronary Syndromes, 2008.
 Cardiovascular Health Nova Scotia Update to Antiplatelet Sections of the Nova Scotia Guidelines for Acute Coronary Syndromes, 2008. ST Elevation Myocardial Infarction (STEMI)-Acute Coronary Syndrome Guidelines:
Cardiovascular Health Nova Scotia Update to Antiplatelet Sections of the Nova Scotia Guidelines for Acute Coronary Syndromes, 2008. ST Elevation Myocardial Infarction (STEMI)-Acute Coronary Syndrome Guidelines:
Unnecessary hospitalisation and investigation of low risk patients presenting to hospital with chest pain
 Unnecessary hospitalisation and investigation of low risk patients presenting to hospital with chest pain Michael Perera Advanced Trainee in General and Acute Medicine Leena Aggarwal Director, Medical
Unnecessary hospitalisation and investigation of low risk patients presenting to hospital with chest pain Michael Perera Advanced Trainee in General and Acute Medicine Leena Aggarwal Director, Medical
Acute coronary syndrome (ACS) is a potentially
 DIAGNOSING ACUTE CORONARY SYNDROME AND DETERMINING PATIENT RISK Edith A. Nutescu, PharmD* ABSTRACT Acute coronary syndrome is a form of coronary artery disease and has a broad range of clinical presentations.
DIAGNOSING ACUTE CORONARY SYNDROME AND DETERMINING PATIENT RISK Edith A. Nutescu, PharmD* ABSTRACT Acute coronary syndrome is a form of coronary artery disease and has a broad range of clinical presentations.
IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT JANUARY 24, 2012
 IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT201203 JANUARY 24, 2012 The IHCP to reimburse implantable cardioverter defibrillators separately from outpatient implantation Effective March 1, 2012, the
IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT201203 JANUARY 24, 2012 The IHCP to reimburse implantable cardioverter defibrillators separately from outpatient implantation Effective March 1, 2012, the
Assessment and Diagnosis of Heart Failure
 Assessment and Diagnosis of Heart Failure Heart failure (HF) is a complex clinical syndrome resulting from any structural or functional impairment of ventricular filling or ejection of blood and is characterized
Assessment and Diagnosis of Heart Failure Heart failure (HF) is a complex clinical syndrome resulting from any structural or functional impairment of ventricular filling or ejection of blood and is characterized
General Cardiovascular Magnetic Resonance Imaging
 2 General Cardiovascular Magnetic Resonance Imaging 19 Peter G. Danias, Cardiovascular MRI: 150 Multiple-Choice Questions and Answers Humana Press 2008 20 Cardiovascular MRI: 150 Multiple-Choice Questions
2 General Cardiovascular Magnetic Resonance Imaging 19 Peter G. Danias, Cardiovascular MRI: 150 Multiple-Choice Questions and Answers Humana Press 2008 20 Cardiovascular MRI: 150 Multiple-Choice Questions
An update on the management of UA / NSTEMI. Michael H. Crawford, MD
 An update on the management of UA / NSTEMI Michael H. Crawford, MD New ACC/AHA Guidelines 2007 What s s new in the last 5 years CT imaging advances Ascendancy of troponin and BNP Clarification of ACEI/ARB
An update on the management of UA / NSTEMI Michael H. Crawford, MD New ACC/AHA Guidelines 2007 What s s new in the last 5 years CT imaging advances Ascendancy of troponin and BNP Clarification of ACEI/ARB
Severe Hypertension. Pre-referral considerations: 1. BP of arm and Leg 2. Ambulatory BP 3. Renal causes
 Severe Hypertension *Prior to making a referral, call office or Doc Halo, to speak with a Cardiologist or APP to discuss patient and possible treatment options. Please only contact the patient's cardiologist.
Severe Hypertension *Prior to making a referral, call office or Doc Halo, to speak with a Cardiologist or APP to discuss patient and possible treatment options. Please only contact the patient's cardiologist.
Ticagrelor compared with clopidogrel in patients with acute coronary syndromes the PLATO trial
 compared with clopidogrel in patients with acute coronary syndromes the PLATO trial August 30, 2009 at 08.00 CET PLATO background In NSTE-ACS and STEMI, current guidelines recommend 12 months aspirin and
compared with clopidogrel in patients with acute coronary syndromes the PLATO trial August 30, 2009 at 08.00 CET PLATO background In NSTE-ACS and STEMI, current guidelines recommend 12 months aspirin and
Previous MI with no intervention
 Previous MI with no intervention F. Mut, M. Beretta Nuclear Medicine Service, Asociacion Española Montevideo, Uruguay Clinical history Woman 68 y.o. Recent acute MI (3 weeks) with no intervention. Discharged
Previous MI with no intervention F. Mut, M. Beretta Nuclear Medicine Service, Asociacion Española Montevideo, Uruguay Clinical history Woman 68 y.o. Recent acute MI (3 weeks) with no intervention. Discharged
Horizon Scanning Technology Summary. Magnetic resonance angiography (MRA) imaging for the detection of coronary artery disease
 Horizon Scanning Technology Summary National Horizon Scanning Centre Magnetic resonance angiography (MRA) imaging for the detection of coronary artery disease April 2007 This technology summary is based
Horizon Scanning Technology Summary National Horizon Scanning Centre Magnetic resonance angiography (MRA) imaging for the detection of coronary artery disease April 2007 This technology summary is based
All About STEMIs. Presented By: Brittney Urvand, RN, BSN, CCCC. Essentia Health Fargo Cardiovascular Program Manager.
 All About STEMIs Presented By: Brittney Urvand, RN, BSN, CCCC Essentia Health Fargo Cardiovascular Program Manager Updated 10/2/2018 None Disclosures Objectives Identify signs and symptoms of a heart attack
All About STEMIs Presented By: Brittney Urvand, RN, BSN, CCCC Essentia Health Fargo Cardiovascular Program Manager Updated 10/2/2018 None Disclosures Objectives Identify signs and symptoms of a heart attack
Brugada Syndrome: Age is just a number
 Brugada Syndrome: Age is just a number 1 Deepthi Kagolanu, MD, 2 Cynthia Pacas, 1 Usman Jilani, DO, 1 Ebisa Bekele, MD, 3 Christopher Henessey, 4 Kent Stephenson MD 1 Nassau University Medical Center,
Brugada Syndrome: Age is just a number 1 Deepthi Kagolanu, MD, 2 Cynthia Pacas, 1 Usman Jilani, DO, 1 Ebisa Bekele, MD, 3 Christopher Henessey, 4 Kent Stephenson MD 1 Nassau University Medical Center,
Corporate Medical Policy Electrocardiographic Body Surface Mapping
 Corporate Medical Policy Electrocardiographic Body Surface Mapping File Name: Origination: Last CAP Review: Next CAP Review: Last Review: eletrocardiographic_body_surface_mapping 6/2009 10/2016 10/2017
Corporate Medical Policy Electrocardiographic Body Surface Mapping File Name: Origination: Last CAP Review: Next CAP Review: Last Review: eletrocardiographic_body_surface_mapping 6/2009 10/2016 10/2017
Managing Quality of ACS Care in VHA The IDH Guideline Key Points and Metrics
 Managing Quality of ACS Care in VHA The IDH Guideline Key Points and Metrics Robert L. Jesse, MD, PhD National Program Director for Cardiology Veterans Health Administration Washington, DC Chief, Cardiology
Managing Quality of ACS Care in VHA The IDH Guideline Key Points and Metrics Robert L. Jesse, MD, PhD National Program Director for Cardiology Veterans Health Administration Washington, DC Chief, Cardiology
Coding an Acute Myocardial Infarction: Unravelling the Mystery
 Coding an Acute Myocardial Infarction: Unravelling the Mystery by Karen Carr, MS, BSN, RN, CCDS, CDIP, and Lisa Romanello, MSHI, BSN, RN, CCDS, CDIP WHITE PAPER Summary: The following white paper offers
Coding an Acute Myocardial Infarction: Unravelling the Mystery by Karen Carr, MS, BSN, RN, CCDS, CDIP, and Lisa Romanello, MSHI, BSN, RN, CCDS, CDIP WHITE PAPER Summary: The following white paper offers
Management of Acute Myocardial Infarction
 Management of Acute Myocardial Infarction Prof. Hossam Kandil Professor of Cardiology Cairo University ST Elevation Acute Myocardial Infarction Aims Of Management Emergency care (Pre-hospital) Early care
Management of Acute Myocardial Infarction Prof. Hossam Kandil Professor of Cardiology Cairo University ST Elevation Acute Myocardial Infarction Aims Of Management Emergency care (Pre-hospital) Early care
Diagnosis and Management of Acute Myocardial Infarction
 Diagnosis and Management of Acute Myocardial Infarction Acute Myocardial Infarction (AMI) occurs as a result of prolonged myocardial ischemia Atherosclerosis leads to endothelial rupture or erosion that
Diagnosis and Management of Acute Myocardial Infarction Acute Myocardial Infarction (AMI) occurs as a result of prolonged myocardial ischemia Atherosclerosis leads to endothelial rupture or erosion that
DIFFERENTIATING THE PATIENT WITH UNDIFFERENTIATED CHEST PAIN
 DIFFERENTIATING THE PATIENT WITH UNDIFFERENTIATED CHEST PAIN Objectives Gain competence in evaluating chest pain Recognize features of moderate risk unstable angina Review initial management of UA and
DIFFERENTIATING THE PATIENT WITH UNDIFFERENTIATED CHEST PAIN Objectives Gain competence in evaluating chest pain Recognize features of moderate risk unstable angina Review initial management of UA and
