Bone Marrow Derived Progenitor Cells Modulate Vascular Reendothelialization and Neointimal Formation
|
|
|
- Junior Harrington
- 5 years ago
- Views:
Transcription
1 Bone Marrow Derived Progenitor Cells Modulate Vascular Reendothelialization and Neointimal Formation Effect of 3-Hydroxy-3-Methylglutaryl Coenzyme A Reductase Inhibition Nikos Werner,* Josef Priller,* Ulrich Laufs, Matthias Endres, Michael Böhm, Ulrich Dirnagl, Georg Nickenig Objective Atherosclerosis and restenosis after vascular injury are both characterized by endothelial dysfunction, apoptosis, inappropriate endothelialization, and neointimal formation. Bone marrow derived endothelial progenitor cells have been implicated in neovascularization, resulting in adult blood vessel formation. Despite the anticipated stem cell plasticity, the role of bone marrow derived endothelial progenitor cells has not been clarified in vascular lesion development. Methods and Results We investigated vascular lesion formation in mice after transplantation of bone marrow transfected by means of retrovirus with enhanced green fluorescent protein. Carotid artery injury was induced, resulting in neointimal formation. Fluorescence microscopy and immunohistological analysis revealed that bone marrow derived progenitor cells are involved in reendothelialization of the vascular lesions. Treatment with rosuvastatin (20 mg/kg body wt per day), a 3-hydroxy-3-methylglutaryl coenzyme A reductase inhibitor, enhanced the circulating pool of endothelial progenitor cells, propagated the advent of bone marrow derived endothelial cells in the injured vessel wall, and, thereby, accelerated reendothelialization and significantly decreased neointimal formation. Conclusions Vascular lesion development initiated by endothelial cell damage is moderated by bone marrow derived progenitor cells. 3-Hydroxy-3-methylglutaryl coenzyme A reductase inhibition promotes bone marrow dependent reendothelialization and diminishes vascular lesion development. These findings may help to establish novel pathophysiological concepts and therapeutic strategies in the treatment of various cardiovascular diseases. (Arterioscler Thromb Vasc Biol. 2002;22: ) Key Words: endothelium endothelial progenitor cells vascular injury neointima 3-hydroxy-3-methylglutaryl coenzyme A reductase inhibition Atherosclerosis leads to serious medical conditions, including coronary heart disease, the main cause of death in the Western world. 1 Atherosclerotic lesions are initiated by endothelial cell damage, followed by macrophage adhesion and invasion as well as smooth muscle cell migration and growth. 2 If stenosis due to atherosclerosis is treated by balloon angioplasty and/or stent implantation, restenosis of the target vessel is frequently observed. 3 This is caused by See cover and page 1509 endothelial cell damage and rapid neointimal formation, which is mainly composed of proliferating smooth muscle cells. 4,5 Thus, despite numerous epidemiological, cellular, and molecular differences, atherosclerosis and restenosis after vascular injury share at least 1 important pathophysiological step: endothelial cell damage followed by an impaired reendothelialization. 5,6 It is currently believed that this reendothelialization is controlled by the adjacent endothelial cells within the vessel wall. 7 Accumulating evidence indicates that bone marrow derived cells are involved in repair processes throughout the cardiovascular system Accordingly, endothelial progenitor cells (EPCs) have been implicated in neovascularization in the context of peripheral arterial disease as well as coronary heart disease. 8,12 16 In addition, bone marrow derived cells may help to reestablish myocardial tissue after myocardial infarction. 10,15,17 21 Little is known about the relevance of EPCs in the development and cure of atherosclerotic lesions. It is unclear whether bone marrow derived cells are involved in the reendothelialization and neointimal formation causing restenosis after vascular injury and whether these events can be Received July 16, 2002; revision accepted August 21, From the Medizinische Klinik und Poliklinik, Innere Medizin III (N.W., U.L., M.B., G.N.), Universität des Saarlandes, Homburg/Saar, Germany, and Experimentelle Neurologie (J.P., M.E., U.D.), Universitätsklinikum Charité, Humboldt-Universität zu Berlin, Berlin, Germany. *These authors contributed equally to the present study. Correspondence to Dr Georg Nickenig, Medizinische Klinik und Poliklinik, Innere Medizin III, Universität des Saarlandes, Homburg/Saar, Germany. nickenig@med-in.uni-sb.de 2002 American Heart Association, Inc. Arterioscler Thromb Vasc Biol. is available at DOI: /01.ATV D8 1567
2 1568 Arterioscler Thromb Vasc Biol. October 2002 modulated by 3-hydroxy-3-methylglutaryl coenzyme A (HMG CoA) reductase inhibitors, which are thought to influence the release of progenitor cells from the bone marrow. 22,23 In the present study, mice with green fluorescent protein (GFP)-marked bone marrow were subjected to carotid artery injury to elucidate the role of the bone marrow in reendothelialization and neointimal formation. Furthermore, the effect of rosuvastatin versus placebo on circulating EPCs and reendothelialization was evaluated. Methods Retroviral Gene Transfer and Bone Marrow Transplantation Reconstitution of hematopoiesis with GFP-marked bone marrow cells was performed as described previously. 24,25 Briefly, bone marrow was harvested from 8- to 10-week-old male C57/BL6 mice 2 days after treatment with 5-fluorouracil (Sigma Chemical Co). Bone marrow cells were stimulated in DMEM/15% FCS supplemented with 20 ng/ml recombinant murine interleukin-3, 50 ng/ml human interleukin-6 (PromoCell), and 50 ng/ml rat stem cell factor (generously provided by Amgen, Munich, Germany) for 48 hours. Subsequently, bone marrow cells were cocultured with irradiated (13-Gy) viral producer cells. The ecotropic packaging cell line GP E86 was used for the generation of MGirL22Y retroviral vector particles. The MGirL22Y vector was generated by cloning the enhanced GFP (Clontech) gene upstream from the internal ribosomal entry site from the encephalomyocarditis virus linked to a mutant dihydrofolate reductase gene (L22Y) in a murine stem cell virus vector. The presence of recombinant retrovirus was excluded in assays that used a mus dunni test cell line. After 48 hours of coculture, nonadherent bone marrow cells were rinsed off the producer cell monolayer. Transduced bone marrow cells ( ) were transplanted by tail vein injection into lethally irradiated 8- to 10-week-old male C57/BL6 mice (11-Gy cumulative dose). Flow cytometric analysis of GFP expression was performed in peripheral blood leukocytes of mice 8 months after transplantation of GFPexpressing bone marrow cells and in leukocytes of control mice that did not receive GFP-labeled bone marrow. Approximately 70% of white blood cells were stably expressing the fluorophore in GFP bone marrow chimeras. All myeloid and lymphocytic populations were labeled, but the levels of GFP expression varied within lineages. The highest expression was observed in monocytes/macrophages and granulocytes. Carotid Injury and Treatment Six months after bone marrow reconstitution, the mice received daily doses of rosuvastatin (Crestor, generously provided by AstraZeneca, Cheshire, UK) at 20 mg/kg body wt subcutaneously. Control animals received a corresponding amount of normal saline. Treatment was started 10 days before carotid injury and was continued until tissue harvesting. Carotid artery injury was induced as described previously. 26 Briefly, the mice were anesthetized with halothane/n 2 O. By use of a dissecting microscope (MZ6, Leica), the bifurcation of the left carotid artery was exposed via a midline incision of the ventral side of the neck. Two ligatures were placed proximally and distally around the external carotid artery. The distal ligature was then tied off. After temporary occlusion of the internal and common carotid artery with ligatures, a transverse arteriotomy was performed between the ligatures of the external carotid artery to introduce a 0.13-mm-diameter curved flexible wire. The wire was passed 3 times along the common carotid artery in a rotating manner. After removal of the wire, the proximal ligature of the external carotid artery was tied off. Restoration of normal blood flow was confirmed, and the skin was closed with single sutures with the use of 6/0 silk. Animals were allowed to recover, and carotid arteries were harvested after 14 days. All animal procedures were approved and were in accordance with the institutional guidelines. Vessel Harvesting After perfusion-fixation with 4% paraformaldehyde, carotid arteries were embedded in Tissue Tek OCT embedding medium (Miles Laboratories), snap-frozen, and stored at 80 C. Samples were sectioned on a Leica cryostat (7 m) and placed on poly-l-lysine (Sigma) coated slides for immunohistochemical analysis. Histochemistry Cryosections were assessed for endothelial cell markers (von Willebrand factor [vwf], polyclonal antibody, clone A 0082, Dako; vascular endothelial growth factor receptor 2, monoclonal antibody [mab] A-3, Santa Cruz; and vascular endothelial cadherin, F-8, Santa Cruz), smooth muscle cells (mab smooth muscle -actin, clone 1A4, Sigma), and inflammatory cell markers (mab Mac-3, clone M3/84; mab CD45.1, clone A20; Pharmingen) with a direct immunofluorescence method. For light microscopy, a peroxidaseconjugated anti-gfp antibody (mab GFP, B-2, Santa Cruz) with DAB staining (Dako) or APAAP Mouse Monoclonal IgG (F-8, Santa Cruz) with BCIP/NBT (Dako) was used. Nuclear staining was performed with the use of 4,6-diamidino-2-phenylindole (Dapi, Linaris). Isotype-specific secondary antibodies (Santa Cruz) were used for negative controls. For immunohistochemistry, tissue cryosections were postfixed in 4% formaldehyde for 2 minutes. Slides were preincubated with 0.5% Igepal (Sigma) and 5% normal goat serum (Sigma) for 30 minutes each. The primary antibody was applied for 2 to 3 hours at room temperature or at 4 C overnight, followed by application of the appropriate TRITC-conjugated secondary antibody (Sigma) for 30 minutes. Sections were washed and mounted with fluorescent mounting medium (Dako) for fluorescence microscopic analysis. For morphometric analyses, hematoxylin and eosin staining was performed according to standard protocols. All sections were examined under a Nikon E600 microscope. For morphometric analyses, Lucia Measurement Version 4.6 software (Nikon, Germany) was used to measure external elastic lamina, internal elastic lamina, and lumen circumference, as well as medial and neointimal area of 25 sections per animal. To determine reendothelialization, mice received 50 L of 5% Evans blue diluted in normal saline by tail vein injection 10 minutes before euthanization, followed by perfusion-fixation. Arteries were opened longitudinally and placed between slides with mounting medium (Dako). After transparency scanning (Nikon SMZ800), stained carotid arteries were planimetered (Lucia Measurement Version 4.6 software), and the ratio between the area stained in blue and the total carotid area was calculated. Fluorescence-Activated Cell Sorter Analysis Peripheral blood of rosuvastatin-treated or placebo (normal saline) treated mice was collected at 1, 10, 11, and 24 days after the initiation of treatment. After lysis of whole blood and Fc blockade (Fc-Block, Pharmingen), the viable lymphocyte population was analyzed for the expression of Sca-1-FITC (clone E , Pharmingen) and vascular endothelial growth factor receptor-2 (clone A3, Santa Cruz) conjugated with the corresponding phycoerythrinlabeled secondary antibody (Sigma). Isotype-identical antibodies served as controls (Becton Dickinson). Single- and 2-color flow cytometric analyses were performed by using a Becton Dickinson FACScan equipped with an argon ion laser. Data were evaluated by Cellquest software. Cell Culture Spleens were mechanically minced, and mononuclear cells were isolated by use of a Ficoll (Biochrom) gradient. Cells ( ) were seeded into fibronectin (Sigma) coated 24-well plates in 0.5 ml endothelial basal medium (CellSystems). After 7 days in culture, cells were stained for 1,1 -dioctadecyl-3,3,3,3 -tetramethylindocarbocyanine perchlorate (DiI-Ac-LDL, CellSystems) and FITClabeled lectin (UEA-1, Sigma). At least 3 high-power fields of each
3 Werner et al EPCs and Vascular Injury 1569 well were analyzed. Cells positive for DiI-Ac-LDL and lectin staining were judged to be EPCs and were counted. Statistical Analysis Results are presented as mean SEM. Significance of the difference between 2 measurements was determined by unpaired Student t test, and multiple comparisons were evaluated by the Newman-Keuls multiple comparison test. Values of P 0.05 were considered significant. Results Carotid Injury Model Fourteen days after carotid injury, vessels were harvested and subjected to histological analysis. Figure 1 shows a representative example of highly reproducible neointimal formation in an artery after injury compared with an unaltered carotid artery. Retrovirus-Mediated Transfer of the GFP Gene Into Hematopoietic Cells Transduction efficiency into murine myeloid clonogenic progenitors averaged 80% to 90%. Retrovirally transduced hematopoietic colonies expressed high levels of GFP, as determined by direct visualization with phase-contrast and fluorescence microscopy. All myeloid and lymphocytic lineages displayed a 50% to 80% range of GFP labeling, and GFP expression was stable during the entire observation period. Reendothelialization From the Bone Marrow Mice with reconstituted GFP bone marrow were subjected to carotid artery injury procedures. Fourteen days after injury, harvested vessels were analyzed by direct fluorescence microscopy to visualize GFP-positive cells. Immunohistochemical localization of antigens in the arterial vasculature was complicated by the presence of complex molecules such as collagen, elastin, cholesterol, and fluorescent lipids that exhibit autofluorescence over a wide spectrum of wavelengths. Figure 2A and 2B shows the contralateral uninjured carotid artery, in which an autofluorescent signal from the elastic fibers but not from GFP-positive cells was detected. In contrast, scanning of the injured artery revealed GFP-positive cells predominantly at the endothelial monolayer (Figure 2C). Light-microscopic control stainings with a peroxidaseconjugated antibody against GFP confirmed that these cells express the GFP protein and were therefore derived from the bone marrow (data not shown). To confirm the commitment of these GFP-positive cells to the endothelial cell lineage, immunohistological analysis with monoclonal antibodies against vwf (Figure 2D) and vascular endothelial cadherin (data not shown) were used, demonstrating that luminal GFP-positive cells represent endothelial cells. Control stainings with Dapi (data not shown) show the spindle-shaped nucleus of endothelial cells. The concomitant appearance of GFP and endothelial cell lineage marker indicates that reendothelialization is influenced by bone marrow derived cells. The neointima-forming tissue is mainly composed of vascular smooth muscle cells. Direct fluorescence microscopy and additional staining with antibodies against -actin (data not shown) revealed that smooth muscle cells within the analyzed vessel segments were not GFP positive and therefore did not stem from Figure 1. Hematoxylin and eosin (HE) staining of mouse carotid artery. A, Uninjured carotid artery (control). B, Prominent neointimal formation 14 days after arterial injury. the bone marrow. Macrophages and leukocytes were immunohistologically detected with antibodies against CD45 and Mac-3. However, these cells were primarily localized in the connective tissue adjacent to the injured vessel wall and only rarely at the luminal surface (please see online Figure I, available at Effect of Rosuvastatin Treatment on EPCs Mice were treated with rosuvastatin (20 mg/kg body wt per day). Peripheral blood collected after 1, 10, 11, and 24 days was submitted to fluorescence-activated cell sorter analysis to quantify Sca-1/vascular endothelial growth factor receptor 2 positive cells. Representative fluorescence-activated cell sorter analyses of the control group and of the rosuvastatintreated group are shown in online Figure IIA and IIB (available at Statistical analysis showed an increase of EPCs in the treated group to 0.076% of counted cells (213 16% control) after 24 hours and to 0.25% of counted cells ( % control) after 10 days in the peripheral circulation compared with the placebo group (0.036% of counted cells, Figure 3A). Spleens were harvested at 1, 10, 11, and 24 days after the initiation of rosuvastatin treatment, and spleen-derived
4 1570 Arterioscler Thromb Vasc Biol. October 2002 Figure 2. Fluorescence microscopy of GFP chimeras. A, Contralateral uninjured carotid arteries were negative for GFPpositive cells. B, vwf IgG-isotype control is shown. Note that the elastic laminas show a high unspecific signal (autofluorescence). C and D, Marginal zone of endothelial lesion is shown. Panel C shows bone marrow derived cell (arrow) at the luminal side of the vessel. Panel D shows bone marrow derived cell (arrow) positive for the endothelial cell marker vwf (red). Note 2 endothelial cells (*) that are negative for GFP. mononuclear cells were seeded in each well. After an in vitro expansion period of 7 days, DiI-Ac-LDL positive and lectinpositive endothelial cells were quantified as depicted in Figure 3B. A 1-day treatment with rosuvastatin caused an increase to endothelial cells (179 34% control) compared with placebo treatment (5995 cells). Further increases were ascertained after 10 and 11 days; however, the enhancing effect of rosuvastatin was more sustained, with a maximum of cells after 24 days (454 72% control). Rosuvastatin Enhances Reendothelialization From the Bone Marrow Mice were treated with either placebo or rosuvastatin (20 mg/kg body wt per day) for 10 days before carotid injury. Vessels were harvested 14 days later and evaluated. Rosuvastatin treatment profoundly increased the reendothelialization process, as shown in Figure 4A and 4B. GFP- and vwf-positive cells were abundant at the luminal side of the lesion, indicating accelerated reendothelialization. A semiquantitative analysis of GFP- and vwf-positive cells in relation to the total number of GFP-negative endothelial cells indicated a significant increase in bone marrow derived endothelial cells committed to reendothelialization after vascular injury (Figure 5A). Thus, the rosuvastatin-induced increase in EPCs is associated with an increased arrival and attachment of bone marrow derived cells at the site of injury and accelerates endothelial repair mechanisms. Rosuvastatin Decreases Neointimal Formation Because rapid reendothelialization is thought to inhibit neointimal formation, 26 we investigated whether the observed rosuvastatin-induced increase of bone marrow derived endothelial reconstitution results in increased reendothelialization and diminished neointimal formation. Figure 5B demonstrates accelerated reendothelialization in animals after a 7-day treatment with rosuvastatin compared with placebotreated animals. Rosuvastatin therapy almost completely prevented the development of intimal hyperplasia, suggesting that the bone marrow driven rapid reendothelialization with rosuvastatin was associated with reduced neointimal formation (Figure 5C and 5D). Discussion An intact endothelial monolayer is essential for the physiological functioning of the vasculature. 27 Metabolic conditions, such as hypercholesterolemia and diabetes, cause endothelial dysfunction. Mechanical manipulations, such as angioplasty, lead to endothelial denudation. 28 Endothelial dysfunction and denudation are both associated with neointimal formation, resulting in narrowing and, ultimately, in occlusion of the diseased vessel. 5,6 Improvement of endothelial function and accelerated reendothelialization reduce neointimal formation. 5,27 This is of special interest regarding the prevention of restenosis after angioplasty. 29 In the past, repair of endothelial cell damage was thought to rely on the outspreading of cells from the adjacent intact vascular wall. 7 Recent studies have raised the possibility that bone marrow derived cells contribute to neoangiogenesis after vascular occlusion and possibly to myocardial regeneration after infarction. In addition, circulating bone marrow derived cells Figure 3. A, Statistical analysis shows an early increase in circulating EPCs in peripheral blood. B, Cell culture experiments reveal a late increase of spleen-derived EPCs after rosuvastatin treatment. Values are mean SEM. *P 0.05 (n 3 per group).
5 Werner et al EPCs and Vascular Injury 1571 Figure 4. Representative section after rosuvastatin treatment with increased number of bone marrow derived endothelial cells in the marginal zone of endothelial lesion. GFP-positive endothelial cells (arrows, A) are shown with the corresponding vwf staining (B). resembling immature vascular smooth muscle cells seem to contribute to neointimal formation after severe damage of the vessel wall. 30 Therefore, stem cell based intervention could be the basis of novel treatment methods. 8,10,12 21 Despite these intriguing findings, little is known about the role of the bone marrow in the setting of reendothelialization. Our data indicate that bone marrow derived cells are directed to vascular lesion sites to reestablish an intact endothelial layer. These cells, characterized by surface markers of immaturity, circulate in the peripheral blood and are capable of adhering to the injured vascular wall. Obviously, the physiological numbers and features of these cells are insufficient to overcome exogenously applied vessel damage, because the unwanted and deleterious neointimal formation occurs reproducibly. Therefore, it may be beneficial to increase the numbers and enhance the attachment of bone marrow derived progenitor cells to accelerate reendothelialization. Vascularly derived growth factors as well as HMG CoA reductase inhibitors (statins) have been shown to increase the number of circulating premature endothelial cells in mice and humans. 22,23,31 Interestingly, the pool of EPCs seems to be dependent on coronary risk factors and coronary heart disease, with decreasing numbers in the peripheral blood associated with an increased risk profile. 32 Statins have been shown to produce a decrease in cardiovascular event rates, an effect that is often assumed to be related to their lipidlowering properties However, there is evidence that so-called pleiotropic effects, independent of lipid lowering, could account, at least partially, for some of the beneficial clinical effects. 36 In the case of enhanced release of EPCs, the activation of phosphatidylinositol 3-kinase dependent and Akt-dependent pathways seem to be involved. 22,31 In the mouse model in the present study, rosuvastatin treatment not only enhanced the number of circulating EPCs but also profoundly enhanced reendothelialization due to attachment of circulating bone marrow derived cells. This novel finding clearly extends the presently established knowledge regarding bone marrow derived vascular cells and the reendothelialization processes. Moreover, it suggests that the known advantages of statin treatment may be partially caused by a beneficial influence on bone marrow derived progenitor cells. However, several questions remain unanswered and warrant further investigation: How are EPCs released in greater quantities by statin treatment? Is this release caused by enhanced proliferation and differentiation of committed stem cells within the bone marrow, or is it due to an increased release of a preexisting pool? What are the exact mechanisms governing these events? What makes endothelial cells attach to the injured vessel wall? Are there inducible adhesion molecules at the site of injury, or are there integrin-like Figure 5. Analyses of injured mouse carotid artery. A, Rosuvastatin increases the number of bone marrow derived endothelial cells (ECs) in areas of endothelial lesion. Cells with double staining for GFP and vwf were defined as positive and were related to the total number of ECs observed in injured sections of the vessel (control group, n 5, 45 sections; rosuvastatin group, n 4, 60 sections). Values are mean SEM. *P B, Evans blue staining is shown at 1, 7, and 24 days after carotid injury. Reendothelialization was significantly improved after a 7-day treatment with rosuvastatin. C, Neointimal area is significantly reduced after rosuvastatin treatment. Values are mean SEM. *P 0.05 vs carotid injury (n 5 per group). D, Lumen circumference is significantly increased in mice treated with rosuvastatin compared with control groups.
6 1572 Arterioscler Thromb Vasc Biol. October 2002 structures on the endothelial cells, or do both occur, propagating the interaction of endothelial cells with the vascular wall? How is this modulated by statins? These results provide novel insight into the biology of vascular lesion repair. In contrast to widely believed dogma, repair of endothelial cell damage is modulated not only by adjacent vessel structures but also by bone marrow derived cells. As well as adding another facet to the properties of HMG CoA reductase inhibitors, this discovery raises the possibility that treatment regimens involving bone marrow derived cells might help prevent advanced vascular lesion formation. Acknowledgments Rosuvastatin was generously provided by AstraZeneca. We thank S. Karren and S. Karl for excellent technical assistance and J. Schultze for assistance with the carotid artery injury model. References 1. Lusis AJ. Atherosclerosis. Nature. 2000; 407: Schwartz SM. Perspectives series: cell adhesion in vascular biology: smooth muscle migration in atherosclerosis and restenosis. J Clin Invest. 1997;99: Ferns GA, Avades TY. The mechanisms of coronary restenosis: insights from experimental models. Int J Exp Pathol. 2000;81: Andres V. Control of vascular smooth muscle cell growth and its implication in atherosclerosis and restenosis. Int J Mol Med. 1998;2: Bauters C, Isner JM. The biology of restenosis. Prog Cardiovasc Dis. 1997;40: Libby P, Schwartz D, Brogi E, Tanaka H, Clinton SK. A cascade model for restenosis: a special case of atherosclerosis progression. Circulation. 1992;86(suppl III):III-47 III Carmeliet P, Moons L, Stassen JM, De Mol M, Bouche A, van den Oord JJ, Kock M, Collen D. Vascular wound healing and neointima formation induced by perivascular electric injury in mice. Am J Pathol. 1997;150: Asahara T, Murohara T, Sullivan A, Silver M, van der ZR, Li T, Witzenbichler B, Schatteman G, Isner JM. Isolation of putative progenitor endothelial cells for angiogenesis. Science. 1997;275: Asahara T, Masuda H, Takahashi T, Kalka C, Pastore C, Silver M, Kearne M, Magner M, Isner JM. Bone marrow origin of endothelial progenitor cells responsible for postnatal vasculogenesis in physiological and pathological neovascularization. Circ Res. 1999;85: Orlic D, Kajstura J, Chimenti S, Bodine DM, Leri A, Anversa P. Transplanted adult bone marrow cells repair myocardial infarcts in mice. Ann N Y Acad Sci. 2001;938: Gill M, Dias S, Hattori K, Rivera ML, Hicklin D, Witte L, Girardi L, Yurt R, Himel H, Rafii S. Vascular trauma induces rapid but transient mobilization of VEGFR2( )AC133( ) endothelial precursor cells. Circ Res. 2001;88: Crosby JR, Kaminski WE, Schatteman G, Martin PJ, Raines EW, Seifert RA, Bowen-Pope DF. Endothelial cells of hematopoietic origin make a significant contribution to adult blood vessel formation. Circ Res. 2000; 87: Ikenaga S, Hamano K, Nishida M, Kobayashi T, Li TS, Kobayashi S, Matsuzaki M, Zempo N, Esato K. Autologous bone marrow implantation induced angiogenesis and improved deteriorated exercise capacity in a rat ischemic hindlimb model. J Surg Res. 2001;96: Kalka C, Masuda H, Takahashi T, Kalka-Moll WM, Silver M, Kearney M, Li T, Isner JM, Asahara T. Transplantation of ex vivo expanded endothelial progenitor cells for therapeutic neovascularization. Proc Natl Acad Sci U S A. 2000;97: Kawamoto A, Gwon HC, Iwaguro H, Yamaguchi JI, Uchida S, Masuda H, Silver M, Ma H, Kearney M, Isner JM, Asahara T. Therapeutic potential of ex vivo expanded endothelial progenitor cells for myocardial ischemia. Circulation. 2001;103: Shintani S, Murohara T, Ikeda H, Ueno T, Honma T, Katoh A, Sasaki K, Shimada T, Oike Y, Imaizumi T. Mobilization of endothelial progenitor cells in patients with acute myocardial infarction. Circulation. 2001;103: Jackson KA, Majka SM, Wang H, Pocius J, Hartley CJ, Majesky MW, Entman ML, Michael LH, Hirschi KK, Goodell MA. Regeneration of ischemic cardiac muscle and vascular endothelium by adult stem cells. J Clin Invest. 2001;107: Kamihata H, Matsubara H, Nishiue T, Fujiyama S, Tsutsumi Y, Ozono R, Masaki H, Mori Y, Iba O, Tateishi E, Kosaki A, Shintani S, Murohara T, Imaizumi T, Iwasaka T. Implantation of bone marrow mononuclear cells into ischemic myocardium enhances collateral perfusion and regional function via side supply of angioblasts, angiogenic ligands, and cytokines. Circulation. 2001;104: Kocher AA, Schuster MD, Szabolcs MJ, Takuma S, Burkhoff D, Wang J, Homma S, Edwards NM, Itescu S. Neovascularization of ischemic myocardium by human bone marrow-derived angioblasts prevents cardiomyocyte apoptosis, reduces remodeling and improves cardiac function. Nat Med. 2001;7: Orlic D, Kajstura J, Chimenti S, Limana F, Jakoniuk I, Quaini F, Nadal- Ginard B, Bodine DM, Leri A, Anversa P. Mobilized bone marrow cells repair the infarcted heart, improving function and survival. Proc Natl Acad Sci U S A. 2001;98: Tomita S, Li RK, Weisel RD, Mickle DA, Kim EJ, Sakai T, Jia ZQ. Autologous transplantation of bone marrow cells improves damaged heart function. Circulation. 1999;100(suppl II):II-247 II Llevadot J, Murasawa S, Kureishi Y, Uchida S, Masuda H, Kawamoto A, Walsh K, Isner JM, Asahara T. HMG-CoA reductase inhibitor mobilizes bone marrow-derived endothelial progenitor cells. J Clin Invest. 2001; 108: Vasa M, Fichtlscherer S, Adler K, Aicher A, Martin H, Zeiher AM, Dimmeler S. Increase in circulating endothelial progenitor cells by statin therapy in patients with stable coronary artery disease. Circulation. 2001; 103: Priller J, Flugel A, Wehner T, Boentert M, Haas CA, Prinz M, Fernandez-Klett F, Prass K, Bechmann I, de Boer BA, Frotscher M, Kreutzberg GW, Persons DA, Dirnagl U. Targeting gene-modified hematopoietic cells to the central nervous system: use of green fluorescent protein uncovers microglial engraftment. Nat Med. 2001;7: Priller J, Persons DA, Klett FF, Kempermann G, Kreutzberg GW, Dirnagl U. Neogenesis of cerebellar Purkinje neurons from gene-marked bone marrow cells in vivo. J Cell Biol. 2001;155: Lindner V, Fingerle J, Reidy MA. Mouse model of arterial injury. Circ Res. 1993;73: Kinlay S, Libby P, Ganz P. Endothelial function and coronary artery disease. Curr Opin Lipidol. 2001;12: Libby P, Aikawa M, Kinlay S, Selwyn A, Ganz P. Lipid lowering improves endothelial functions. Int J Cardiol. 2000;74:S3 S Nikol S, Huehns TY, Hofling B. Molecular biology and post-angioplasty restenosis. Atherosclerosis. 1996;123: Han CI, Campbell GR, Campbell JH. Circulating bone marrow cells can contribute to neointimal formation. J Vasc Res. 2001;38: Dimmeler S, Aicher A, Vasa M, Mildner-Rihm C, Adler K, Tiemann M, Rutten H, Fichtlscherer S, Martin H, Zeiher AM. HMG-CoA reductase inhibitors (statins) increase endothelial progenitor cells via the PI 3-kinase/Akt pathway. J Clin Invest. 2001;108: Vasa M, Fichtlscherer S, Aicher A, Adler K, Urbich C, Martin H, Zeiher AM, Dimmeler S. Number and migratory activity of circulating endothelial progenitor cells inversely correlate with risk factors for coronary artery disease. Circ Res. 2001;89:E1 E Scandinavian Simvastatin Study Group. Randomised trial of cholesterol lowering in 4444 patients with coronary heart disease: the Scandinavian Simvastatin Survival Study (4S). Lancet. 1994;344: Shepherd J, Cobbe SM, Ford I, Isles CG, Lorimer AR, MacFarlane PW, McKillop JH, Packard CJ. Prevention of coronary heart disease with pravastatin in men with hypercholesterolemia: West of Scotland Coronary Prevention Study Group. N Engl J Med. 1995;333: The Long-Term Intervention with Pravastatin in Ischaemic Disease (LIPID) Study Group. Prevention of cardiovascular events and death with pravastatin in patients with coronary heart disease and a broad range of initial cholesterol levels. N Engl J Med. 1998;339: Maron DJ, Fazio S, Linton MF. Current perspectives on statins. Circulation. 2000;101:
Basic Science Reports
 Basic Science Reports Estrogen Increases Bone Marrow Derived Endothelial Progenitor Cell Production and Diminishes Neointima Formation Kerstin Strehlow, MD*; Nikos Werner, MD*; Jan Berweiler, MS; Andreas
Basic Science Reports Estrogen Increases Bone Marrow Derived Endothelial Progenitor Cell Production and Diminishes Neointima Formation Kerstin Strehlow, MD*; Nikos Werner, MD*; Jan Berweiler, MS; Andreas
Statins and endothelium function
 Statins and endothelium function Matthias Endres Berlin, Germany Klinik und Poliklinik für Neurologie Conflict of interest: research grant from AstraZeneca from prevention to acute therapy... Pleiotropic
Statins and endothelium function Matthias Endres Berlin, Germany Klinik und Poliklinik für Neurologie Conflict of interest: research grant from AstraZeneca from prevention to acute therapy... Pleiotropic
Mr S. is a 62-year-old restaurant owner who has had
 Brief Review: From Bench to Bedside Endothelial Progenitor Cells New Hope for a Broken Heart Paul E. Szmitko, BSc; Paul W.M. Fedak, MD; Richard D. Weisel, MD; Duncan J. Stewart, MD; Michael J.B. Kutryk,
Brief Review: From Bench to Bedside Endothelial Progenitor Cells New Hope for a Broken Heart Paul E. Szmitko, BSc; Paul W.M. Fedak, MD; Richard D. Weisel, MD; Duncan J. Stewart, MD; Michael J.B. Kutryk,
The vascular endothelium represents a dynamic border
 Brief Review Endothelial Progenitor Cells Mobilization, Differentiation, and Homing Mihail Hristov, Wolfgang Erl, Peter C. Weber Abstract Postnatal bone marrow contains a subtype of progenitor cells that
Brief Review Endothelial Progenitor Cells Mobilization, Differentiation, and Homing Mihail Hristov, Wolfgang Erl, Peter C. Weber Abstract Postnatal bone marrow contains a subtype of progenitor cells that
Progenitor cells circulate in the bloodstream, with the
 Granulocyte Colony-Stimulating Factor Mobilizes Functional Endothelial Progenitor Cells in Patients With Coronary Artery Disease Tiffany M. Powell, Jonathan D. Paul, Jonathan M. Hill, Michael Thompson,
Granulocyte Colony-Stimulating Factor Mobilizes Functional Endothelial Progenitor Cells in Patients With Coronary Artery Disease Tiffany M. Powell, Jonathan D. Paul, Jonathan M. Hill, Michael Thompson,
Vascular injury leads to pathological repair and remodeling
 Cytokine-Induced Mobilization of Circulating Endothelial Progenitor Cells Enhances Repair of Injured Arteries Deling Kong, PhD; Luis G. Melo, PhD; Massimiliano Gnecchi, MD; Lunan Zhang, MD; Gustavo Mostoslavsky,
Cytokine-Induced Mobilization of Circulating Endothelial Progenitor Cells Enhances Repair of Injured Arteries Deling Kong, PhD; Luis G. Melo, PhD; Massimiliano Gnecchi, MD; Lunan Zhang, MD; Gustavo Mostoslavsky,
Diabetes mellitus is associated with both an increased risk
 Human Endothelial Progenitor Cells From Type II Diabetics Exhibit Impaired Proliferation, Adhesion, and Incorporation Into Vascular Structures Oren M. Tepper, BA; Robert D. Galiano, MD; Jennifer M. Capla,
Human Endothelial Progenitor Cells From Type II Diabetics Exhibit Impaired Proliferation, Adhesion, and Incorporation Into Vascular Structures Oren M. Tepper, BA; Robert D. Galiano, MD; Jennifer M. Capla,
Circulating Endothelial Progenitor Cells and Cardiovascular Outcomes
 original article Circulating Endothelial Progenitor Cells and Cardiovascular Outcomes Nikos Werner, M.D., Sonja Kosiol, M.D., Tobias Schiegl, M.D., Patrick Ahlers, M.D., Katrin Walenta, M.D., Andreas Link,
original article Circulating Endothelial Progenitor Cells and Cardiovascular Outcomes Nikos Werner, M.D., Sonja Kosiol, M.D., Tobias Schiegl, M.D., Patrick Ahlers, M.D., Katrin Walenta, M.D., Andreas Link,
Statin Therapy Accelerates Reendothelialization
 Statin Therapy Accelerates Reendothelialization A Novel Effect Involving Mobilization and Incorporation of Bone Marrow Derived Endothelial Progenitor Cells Dirk H. Walter, MD; Kilian Rittig, MD; Ferdinand
Statin Therapy Accelerates Reendothelialization A Novel Effect Involving Mobilization and Incorporation of Bone Marrow Derived Endothelial Progenitor Cells Dirk H. Walter, MD; Kilian Rittig, MD; Ferdinand
Endothelial progenitor cells (EPCs) are
 Separation and identification of endothelial progenitor cells from rat peripheral blood Si-Lin Pan, Quan-Sheng Xing, Long Sun Qingdao, China 50 Background: Kawasaki disease (KD) as the most commonly acquired
Separation and identification of endothelial progenitor cells from rat peripheral blood Si-Lin Pan, Quan-Sheng Xing, Long Sun Qingdao, China 50 Background: Kawasaki disease (KD) as the most commonly acquired
Stem Cells. Keith Channon. Department of Cardiovascular Medicine University of Oxford John Radcliffe Hospital, Oxford
 Stem Cells Keith Channon Department of Cardiovascular Medicine University of Oxford John Radcliffe Hospital, Oxford Adult Stem Cells Unique cells that are capable of self-renewal Have the ability to differentiate
Stem Cells Keith Channon Department of Cardiovascular Medicine University of Oxford John Radcliffe Hospital, Oxford Adult Stem Cells Unique cells that are capable of self-renewal Have the ability to differentiate
Cardiac Myocytes are Recruited by Bone Marrow-Derived Cells in Intact Murine Heart
 Kobe J. Med. Sci., Vol. 48, No. 6, pp. 161-166, 2002 Cardiac Myocytes are Recruited by Bone Marrow-Derived Cells in Intact Murine Heart SEIMI SATOMI-KOBAYASHI 1, SEINOSUKE KAWASHIMA 1*, TSUYOSHI SAKODA
Kobe J. Med. Sci., Vol. 48, No. 6, pp. 161-166, 2002 Cardiac Myocytes are Recruited by Bone Marrow-Derived Cells in Intact Murine Heart SEIMI SATOMI-KOBAYASHI 1, SEINOSUKE KAWASHIMA 1*, TSUYOSHI SAKODA
Santulli G. et al. A microrna-based strategy to suppress restenosis while preserving endothelial function
 ONLINE DATA SUPPLEMENTS Santulli G. et al. A microrna-based strategy to suppress restenosis while preserving endothelial function Supplementary Figures Figure S1 Effect of Ad-p27-126TS on the expression
ONLINE DATA SUPPLEMENTS Santulli G. et al. A microrna-based strategy to suppress restenosis while preserving endothelial function Supplementary Figures Figure S1 Effect of Ad-p27-126TS on the expression
Endothelial progenitor cells (EPCs) have been discovered
 Smoking Cessation Rapidly Increases Circulating Progenitor Cells in Peripheral Blood in Chronic Smokers Takahisa Kondo, Mutsuharu Hayashi, Kyosuke Takeshita, Yasushi Numaguchi, Koichi Kobayashi, Shigeo
Smoking Cessation Rapidly Increases Circulating Progenitor Cells in Peripheral Blood in Chronic Smokers Takahisa Kondo, Mutsuharu Hayashi, Kyosuke Takeshita, Yasushi Numaguchi, Koichi Kobayashi, Shigeo
Suppl Video: Tumor cells (green) and monocytes (white) are seeded on a confluent endothelial
 Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
SDF-1/CXCR4 Axis on Endothelial Progenitor Cells Regulates Bone Fracture Healing
 SDF-1/CXCR4 Axis on Endothelial Progenitor Cells Regulates Bone Fracture Healing Yohei Kawakami, M.D., Ph.D. 1,2, Masaaki Ii 3, Tomoyuki Matsumoto, M.D., Ph.D. 1, Astuhiko Kawamoto, M.D., Ph.D. 2, Yutaka
SDF-1/CXCR4 Axis on Endothelial Progenitor Cells Regulates Bone Fracture Healing Yohei Kawakami, M.D., Ph.D. 1,2, Masaaki Ii 3, Tomoyuki Matsumoto, M.D., Ph.D. 1, Astuhiko Kawamoto, M.D., Ph.D. 2, Yutaka
Pathology of Coronary Artery Disease
 Pathology of Coronary Artery Disease Seth J. Kligerman, MD Pathology of Coronary Artery Disease Seth Kligerman, MD Assistant Professor Medical Director of MRI University of Maryland Department of Radiology
Pathology of Coronary Artery Disease Seth J. Kligerman, MD Pathology of Coronary Artery Disease Seth Kligerman, MD Assistant Professor Medical Director of MRI University of Maryland Department of Radiology
VEGFR2-Mediated Vascular Dilation as a Mechanism of VEGF-Induced Anemia and Bone Marrow Cell Mobilization
 Cell Reports, Volume 9 Supplemental Information VEGFR2-Mediated Vascular Dilation as a Mechanism of VEGF-Induced Anemia and Bone Marrow Cell Mobilization Sharon Lim, Yin Zhang, Danfang Zhang, Fang Chen,
Cell Reports, Volume 9 Supplemental Information VEGFR2-Mediated Vascular Dilation as a Mechanism of VEGF-Induced Anemia and Bone Marrow Cell Mobilization Sharon Lim, Yin Zhang, Danfang Zhang, Fang Chen,
Evaluation of directed and random motility in microslides Assessment of leukocyte adhesion in flow chambers
 Evaluation of directed and random motility in microslides Motility experiments in IBIDI microslides, image acquisition and processing were performed as described. PMN, which ended up in an angle < 180
Evaluation of directed and random motility in microslides Motility experiments in IBIDI microslides, image acquisition and processing were performed as described. PMN, which ended up in an angle < 180
Data Alert. Vascular Biology Working Group. Blunting the atherosclerotic process in patients with coronary artery disease.
 1994--4 Vascular Biology Working Group www.vbwg.org c/o Medical Education Consultants, LLC 25 Sylvan Road South, Westport, CT 688 Chairman: Carl J. Pepine, MD Eminent Scholar American Heart Association
1994--4 Vascular Biology Working Group www.vbwg.org c/o Medical Education Consultants, LLC 25 Sylvan Road South, Westport, CT 688 Chairman: Carl J. Pepine, MD Eminent Scholar American Heart Association
Paracrine Mechanisms in Adult Stem Cell Signaling and Therapy
 Paracrine Mechanisms in Adult Stem Cell Signaling and Therapy Massimiliano Gnecchi, Zhiping Zhang, Aiguo Ni, Victor J. Dzau Circulation Research 2008 Nov 21;103(11):1204-19 Introduction(1) After AMI all
Paracrine Mechanisms in Adult Stem Cell Signaling and Therapy Massimiliano Gnecchi, Zhiping Zhang, Aiguo Ni, Victor J. Dzau Circulation Research 2008 Nov 21;103(11):1204-19 Introduction(1) After AMI all
Pretargeting and Bioorthogonal Click Chemistry-Mediated Endogenous Stem Cell Homing for Heart Repair
 Pretargeting and Bioorthogonal Click Chemistry-Mediated Endogenous Stem Cell Homing for Heart Repair Mouse Model of Myocardial Infarction (MI) All animal work was compliant with the Institutional Animal
Pretargeting and Bioorthogonal Click Chemistry-Mediated Endogenous Stem Cell Homing for Heart Repair Mouse Model of Myocardial Infarction (MI) All animal work was compliant with the Institutional Animal
ENDOGENOUS CARDIAC STEM CELLS IN THE REGENERATION OF ACUTE AND CHRONIC ISCHEMIC MYOCARDIUM
 ENDOGENOUS CARDIAC STEM CELLS IN THE REGENERATION OF ACUTE AND CHRONIC ISCHEMIC MYOCARDIUM Bernardo Nadal-Ginard, M.D., Ph.D. New York Medical College Angioplasty Summit 2004, Seoul 04/29/04 MYOCARDIAL
ENDOGENOUS CARDIAC STEM CELLS IN THE REGENERATION OF ACUTE AND CHRONIC ISCHEMIC MYOCARDIUM Bernardo Nadal-Ginard, M.D., Ph.D. New York Medical College Angioplasty Summit 2004, Seoul 04/29/04 MYOCARDIAL
Postnatal neovascularization comprises angiogenesis and vasculogenesis
 Angiogenesis and Vasculogenesis Are Impaired in the Precocious-Aging klotho Mouse Toshifumi Shimada, MD; Yoshiaki Takeshita, MD; Toyoaki Murohara, MD; Ken-ichiro Sasaki, MD; Kimiyasu Egami, MD; Satoshi
Angiogenesis and Vasculogenesis Are Impaired in the Precocious-Aging klotho Mouse Toshifumi Shimada, MD; Yoshiaki Takeshita, MD; Toyoaki Murohara, MD; Ken-ichiro Sasaki, MD; Kimiyasu Egami, MD; Satoshi
Supplementary Materials for
 www.sciencetranslationalmedicine.org/cgi/content/full/4/117/117ra8/dc1 Supplementary Materials for Notch4 Normalization Reduces Blood Vessel Size in Arteriovenous Malformations Patrick A. Murphy, Tyson
www.sciencetranslationalmedicine.org/cgi/content/full/4/117/117ra8/dc1 Supplementary Materials for Notch4 Normalization Reduces Blood Vessel Size in Arteriovenous Malformations Patrick A. Murphy, Tyson
Restenosis after coronary angioplasty occurs in 20% to
 Bolus Endovascular PDGFR- Antisense Treatment Suppressed Intimal Hyperplasia in a Rat Carotid Injury Model Nicolas Noiseux, MD, MSc; Caroline H. Boucher, BSc; Raymond Cartier, MD; Martin G. Sirois, PhD
Bolus Endovascular PDGFR- Antisense Treatment Suppressed Intimal Hyperplasia in a Rat Carotid Injury Model Nicolas Noiseux, MD, MSc; Caroline H. Boucher, BSc; Raymond Cartier, MD; Martin G. Sirois, PhD
Pathology of Cardiovascular Interventions. Body and Disease 2011
 Pathology of Cardiovascular Interventions Body and Disease 2011 Coronary Artery Atherosclerosis Intervention Goals: Acute Coronary Syndromes: Treat plaque rupture and thrombosis Significant Disease: Prevent
Pathology of Cardiovascular Interventions Body and Disease 2011 Coronary Artery Atherosclerosis Intervention Goals: Acute Coronary Syndromes: Treat plaque rupture and thrombosis Significant Disease: Prevent
Distribution of type IV collagen, laminin, nidogen and fibronectin in the haemodynamically stressed vascular wall
 Histol Histopath (1 990) 5: 161-1 67 Histology and Histopathology Distribution of type IV collagen, laminin, nidogen and fibronectin in the haemodynamically stressed vascular wall Reinhold Kittelberger,
Histol Histopath (1 990) 5: 161-1 67 Histology and Histopathology Distribution of type IV collagen, laminin, nidogen and fibronectin in the haemodynamically stressed vascular wall Reinhold Kittelberger,
Understanding the Role of Endothelial Progenitor Cells in Percutaneous Coronary Intervention
 Journal of the American College of Cardiology Vol. 55, No. 15, 2010 2010 by the American College of Cardiology Foundation ISSN 0735-1097/10/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2009.10.070
Journal of the American College of Cardiology Vol. 55, No. 15, 2010 2010 by the American College of Cardiology Foundation ISSN 0735-1097/10/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2009.10.070
Supplementary Materials. for Garmy-Susini, et al, Integrin 4 1 signaling is required for lymphangiogenesis and tumor metastasis
 Supplementary Materials for Garmy-Susini, et al, Integrin 4 1 signaling is required for lymphangiogenesis and tumor metastasis 1 Supplementary Figure Legends Supplementary Figure 1: Integrin expression
Supplementary Materials for Garmy-Susini, et al, Integrin 4 1 signaling is required for lymphangiogenesis and tumor metastasis 1 Supplementary Figure Legends Supplementary Figure 1: Integrin expression
CD34 + VEGFR-3 + progenitor cells have a potential to differentiate towards lymphatic endothelial cells
 CD34 + VEGFR-3 + progenitor cells have a potential to differentiate towards lymphatic endothelial cells Tan YZ et al. J Cell Mol Med. (2014 Mar;18(3):422-33) Denise Traxler-Weidenauer April 2014 Introduction
CD34 + VEGFR-3 + progenitor cells have a potential to differentiate towards lymphatic endothelial cells Tan YZ et al. J Cell Mol Med. (2014 Mar;18(3):422-33) Denise Traxler-Weidenauer April 2014 Introduction
Supplementary Figure 1
 Supplementary Figure 1 The average sigmoid parametric curves of capillary dilation time courses and average time to 50% peak capillary diameter dilation computed from individual capillary responses averaged
Supplementary Figure 1 The average sigmoid parametric curves of capillary dilation time courses and average time to 50% peak capillary diameter dilation computed from individual capillary responses averaged
Invited Review. Vascular smooth muscle cell proliferation in the pathogenesis of atherosclerotic cardiovascular diseases
 Histol Histopathol (2000) 15: 557-571 Histology and Histopathology Cellular and Molecular Biology Invited Review Vascular smooth muscle cell proliferation in the pathogenesis of atherosclerotic cardiovascular
Histol Histopathol (2000) 15: 557-571 Histology and Histopathology Cellular and Molecular Biology Invited Review Vascular smooth muscle cell proliferation in the pathogenesis of atherosclerotic cardiovascular
Since endothelial progenitor cells (EPCs) were identified. Molecular Cardiology
 Molecular Cardiology CD34-Positive Cells Exhibit Increased Potency and Safety for Therapeutic Neovascularization After Myocardial Infarction Compared With Total Mononuclear Cells Atsuhiko Kawamoto, MD,
Molecular Cardiology CD34-Positive Cells Exhibit Increased Potency and Safety for Therapeutic Neovascularization After Myocardial Infarction Compared With Total Mononuclear Cells Atsuhiko Kawamoto, MD,
Vascular smooth muscle cell phenotypes in primary pulmonary hypertension
 Eur Respir J 2001; 17: 316 320 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 CASE STUDY Vascular smooth muscle cell phenotypes in primary
Eur Respir J 2001; 17: 316 320 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 CASE STUDY Vascular smooth muscle cell phenotypes in primary
Catheter and stent-based brachytherapy have shown promise
 Late Arterial Responses (6 and 12 Months) After 32 -Emitting Stent lacement Sustained Intimal Suppression With Incomplete Healing Andrew Farb, MD; Sweta Shroff, MS; Michael John, BA; William Sweet, MD;
Late Arterial Responses (6 and 12 Months) After 32 -Emitting Stent lacement Sustained Intimal Suppression With Incomplete Healing Andrew Farb, MD; Sweta Shroff, MS; Michael John, BA; William Sweet, MD;
Basic Science Reports. Rosiglitazone Facilitates Angiogenic Progenitor Cell Differentiation Toward Endothelial Lineage
 Basic Science Reports Rosiglitazone Facilitates Angiogenic Progenitor Cell Differentiation Toward Endothelial Lineage A New Paradigm in Glitazone Pleiotropy Chao-Hung Wang, MD; Nadia Ciliberti, BSc; Shu-Hong
Basic Science Reports Rosiglitazone Facilitates Angiogenic Progenitor Cell Differentiation Toward Endothelial Lineage A New Paradigm in Glitazone Pleiotropy Chao-Hung Wang, MD; Nadia Ciliberti, BSc; Shu-Hong
(A) RT-PCR for components of the Shh/Gli pathway in normal fetus cell (MRC-5) and a
 Supplementary figure legends Supplementary Figure 1. Expression of Shh signaling components in a panel of gastric cancer. (A) RT-PCR for components of the Shh/Gli pathway in normal fetus cell (MRC-5) and
Supplementary figure legends Supplementary Figure 1. Expression of Shh signaling components in a panel of gastric cancer. (A) RT-PCR for components of the Shh/Gli pathway in normal fetus cell (MRC-5) and
Effective activity of cytokine-induced killer cells against autologous metastatic melanoma including cells with stemness features
 Effective activity of cytokine-induced killer cells against autologous metastatic melanoma including cells with stemness features Loretta Gammaitoni, Lidia Giraudo, Valeria Leuci, et al. Clin Cancer Res
Effective activity of cytokine-induced killer cells against autologous metastatic melanoma including cells with stemness features Loretta Gammaitoni, Lidia Giraudo, Valeria Leuci, et al. Clin Cancer Res
Mesenchymal Stem Cells and Cancer: Their Interplay
 Mesenchymal Stem Cells and Cancer: Their Interplay Gang Li, MBBS, DPhil (Oxon) Stem Cell and Regeneration Program School of Biomedical Sciences Li Ka Shing Institute of Health Sciences Department of Orthopaedics
Mesenchymal Stem Cells and Cancer: Their Interplay Gang Li, MBBS, DPhil (Oxon) Stem Cell and Regeneration Program School of Biomedical Sciences Li Ka Shing Institute of Health Sciences Department of Orthopaedics
Mesenchymal Stem Cells to Repair Vascular Damage after Chemotherapy: Past, Present and Future
 Mesenchymal Stem Cells to Repair Vascular Damage after Chemotherapy: Past, Present and Future Cell Therapy 2014 Las Vegas, NV, USA Sulaiman Al-Hashmi, PhD Sultan Qaboos University Oman What are MSCs? Stem
Mesenchymal Stem Cells to Repair Vascular Damage after Chemotherapy: Past, Present and Future Cell Therapy 2014 Las Vegas, NV, USA Sulaiman Al-Hashmi, PhD Sultan Qaboos University Oman What are MSCs? Stem
Previous studies from our laboratory 1 6 and others 7 13 have
 Basic Science Reports Endothelial Progenitor Cell Vascular Endothelial Growth Factor Gene Transfer for Vascular Regeneration Hideki Iwaguro, MD; Jun-ichi Yamaguchi, MD, PhD; Christoph Kalka, MD; Satoshi
Basic Science Reports Endothelial Progenitor Cell Vascular Endothelial Growth Factor Gene Transfer for Vascular Regeneration Hideki Iwaguro, MD; Jun-ichi Yamaguchi, MD, PhD; Christoph Kalka, MD; Satoshi
Endothelial Injury and Repair as a Working Paradigm
 Endothelial Injury and Repair as a Working Paradigm A. Linke ESC Meeting 2010 UNIVERSITÄTLEIPZIG H ERZZEN TRUM Physiology of Endothelial Function: Regulation of Vascular Tone L-Arg. L-Arg. Agonists Shear
Endothelial Injury and Repair as a Working Paradigm A. Linke ESC Meeting 2010 UNIVERSITÄTLEIPZIG H ERZZEN TRUM Physiology of Endothelial Function: Regulation of Vascular Tone L-Arg. L-Arg. Agonists Shear
Improvement of Collateral Perfusion and Regional Function by Implantation of Peripheral Blood Mononuclear Cells Into Ischemic Hibernating Myocardium
 Improvement of Collateral Perfusion and Regional Function by Implantation of Peripheral Blood Mononuclear Cells Into Ischemic Hibernating Myocardium Hiroshi Kamihata,* Hiroaki Matsubara, Takashi Nishiue,*
Improvement of Collateral Perfusion and Regional Function by Implantation of Peripheral Blood Mononuclear Cells Into Ischemic Hibernating Myocardium Hiroshi Kamihata,* Hiroaki Matsubara, Takashi Nishiue,*
Diminished Circulating Monocytes after Peripheral Bypass Surgery for Critical Limb Ischemia
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 5-6-2009 Diminished Circulating Monocytes after Peripheral Bypass
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 5-6-2009 Diminished Circulating Monocytes after Peripheral Bypass
Supplementary Figure 1. EC-specific Deletion of Snail1 Does Not Affect EC Apoptosis. (a,b) Cryo-sections of WT (a) and Snail1 LOF (b) embryos at
 Supplementary Figure 1. EC-specific Deletion of Snail1 Does Not Affect EC Apoptosis. (a,b) Cryo-sections of WT (a) and Snail1 LOF (b) embryos at E10.5 were double-stained for TUNEL (red) and PECAM-1 (green).
Supplementary Figure 1. EC-specific Deletion of Snail1 Does Not Affect EC Apoptosis. (a,b) Cryo-sections of WT (a) and Snail1 LOF (b) embryos at E10.5 were double-stained for TUNEL (red) and PECAM-1 (green).
REVIEW Hematopoietic, vascular and cardiac fates of bone marrow-derived stem cells
 (2002) 9, 648 652 2002 Nature Publishing Group All rights reserved 0969-7128/02 $25.00 www.nature.com/gt REVIEW Hematopoietic, vascular and cardiac fates of bone marrow-derived stem cells KK Hirschi 1
(2002) 9, 648 652 2002 Nature Publishing Group All rights reserved 0969-7128/02 $25.00 www.nature.com/gt REVIEW Hematopoietic, vascular and cardiac fates of bone marrow-derived stem cells KK Hirschi 1
Supplemental Information. Tissue Myeloid Progenitors Differentiate. into Pericytes through TGF-b Signaling. in Developing Skin Vasculature
 Cell Reports, Volume 18 Supplemental Information Tissue Myeloid Progenitors Differentiate into Pericytes through TGF-b Signaling in Developing Skin Vasculature Tomoko Yamazaki, Ani Nalbandian, Yutaka Uchida,
Cell Reports, Volume 18 Supplemental Information Tissue Myeloid Progenitors Differentiate into Pericytes through TGF-b Signaling in Developing Skin Vasculature Tomoko Yamazaki, Ani Nalbandian, Yutaka Uchida,
The Number of Endothelial Progenitor Cell Colonies in the Blood Is Increased in Patients With Angiographically Significant Coronary Artery Disease
 Journal of the American College of Cardiology Vol. 48, No. 8, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.04.101
Journal of the American College of Cardiology Vol. 48, No. 8, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.04.101
Statins and control of MHC2TA gene transcription
 Statins and CIITA 4 4 Statins and control of MHC2TA gene transcription 4 Hedwich F. Kuipers and Peter J. van den Elsen Nature Medicine, 2005, 11: 365-366 Statins and control of MHC2TA gene transcription
Statins and CIITA 4 4 Statins and control of MHC2TA gene transcription 4 Hedwich F. Kuipers and Peter J. van den Elsen Nature Medicine, 2005, 11: 365-366 Statins and control of MHC2TA gene transcription
Effects of Treatment for Diabetes Mellitus on Circulating Vascular Progenitor Cells
 J Pharmacol Sci 102, 96 102 (2006) Journal of Pharmacological Sciences 2006 The Japanese Pharmacological Society Full Paper Effects of Treatment for Diabetes Mellitus on Circulating Vascular Progenitor
J Pharmacol Sci 102, 96 102 (2006) Journal of Pharmacological Sciences 2006 The Japanese Pharmacological Society Full Paper Effects of Treatment for Diabetes Mellitus on Circulating Vascular Progenitor
DECLARATION OF CONFLICT OF INTEREST. No conflicts of interest
 DECLARATION OF CONFLICT OF INTEREST No conflicts of interest University Heart Centre Tübingen Angiogenic actions of platelets Meinrad Gawaz, MD, FESC Tübingen, Germany ESC 2011 Paris GPIb GPIb GPVI TxA2
DECLARATION OF CONFLICT OF INTEREST No conflicts of interest University Heart Centre Tübingen Angiogenic actions of platelets Meinrad Gawaz, MD, FESC Tübingen, Germany ESC 2011 Paris GPIb GPIb GPVI TxA2
Hybrid Cell Gene Therapy for Pulmonary Hypertension Based on Phagocytosing Action of Endothelial Progenitor Cells
 Hybrid Cell Gene Therapy for Pulmonary Hypertension Based on Phagocytosing Action of Endothelial Progenitor Cells Noritoshi Nagaya, MD; Kenji Kangawa, PhD; Munetake Kanda, MD; Masaaki Uematsu, MD; Takeshi
Hybrid Cell Gene Therapy for Pulmonary Hypertension Based on Phagocytosing Action of Endothelial Progenitor Cells Noritoshi Nagaya, MD; Kenji Kangawa, PhD; Munetake Kanda, MD; Masaaki Uematsu, MD; Takeshi
Endogenous TNFα orchestrates the trafficking of neutrophils into and within lymphatic vessels during acute inflammation
 SUPPLEMENTARY INFORMATION Endogenous TNFα orchestrates the trafficking of neutrophils into and within lymphatic vessels during acute inflammation Samantha Arokiasamy 1,2, Christian Zakian 1, Jessica Dilliway
SUPPLEMENTARY INFORMATION Endogenous TNFα orchestrates the trafficking of neutrophils into and within lymphatic vessels during acute inflammation Samantha Arokiasamy 1,2, Christian Zakian 1, Jessica Dilliway
New Features of the National Cholesterol Education Program Adult Treatment Panel III Lipid-Lowering Guidelines
 Clin. Cardiol. Vol. 26 (Suppl. III), III-19 III-24 (2003) New Features of the National Cholesterol Education Program Adult Treatment Panel III Lipid-Lowering Guidelines H. BRYAN BREWER, JR, M.D. Molecular
Clin. Cardiol. Vol. 26 (Suppl. III), III-19 III-24 (2003) New Features of the National Cholesterol Education Program Adult Treatment Panel III Lipid-Lowering Guidelines H. BRYAN BREWER, JR, M.D. Molecular
Journal Club Semmler Lorenz
 Beer et al. 2015 - Analysis of the Secretome of Apoptotic Peripheral Blood Mononuclear Cells: Impact of Released Proteins and Exosomes for Tissue Regeneration Journal Club 13.11.2017 1 Introduction to
Beer et al. 2015 - Analysis of the Secretome of Apoptotic Peripheral Blood Mononuclear Cells: Impact of Released Proteins and Exosomes for Tissue Regeneration Journal Club 13.11.2017 1 Introduction to
and Restenosis Yangsoo Jang, MD, PhD. Yonsei University College of Medicine
 PPAR- Agonist and In-Stent Restenosis Yangsoo Jang, MD, PhD. Yonsei University College of Medicine Peroxisome Proliferator- activated Receptors (PPAR) Lipid-activated transcription factors : => regulating
PPAR- Agonist and In-Stent Restenosis Yangsoo Jang, MD, PhD. Yonsei University College of Medicine Peroxisome Proliferator- activated Receptors (PPAR) Lipid-activated transcription factors : => regulating
Endothelial Progenitor Cell Dysfunction: a Novel Concept in the Pathogenesis of Vascular Complications of Type 1 Diabetes
 Chapter3 Endothelial Progenitor Cell Dysfunction: a Novel Concept in the Pathogenesis of Vascular Complications of Type 1 Diabetes Cindy J.M. Loomans 1, Eelco J.P. de Koning 1, Frank J.T. Staal 2, Maarten
Chapter3 Endothelial Progenitor Cell Dysfunction: a Novel Concept in the Pathogenesis of Vascular Complications of Type 1 Diabetes Cindy J.M. Loomans 1, Eelco J.P. de Koning 1, Frank J.T. Staal 2, Maarten
Several bone marrow subpopulations, such as endothelial
 Local Delivery of Marrow-Derived Stromal Cells Augments Collateral Perfusion Through Paracrine Mechanisms T. Kinnaird, MBBCh; E. Stabile, MD; M.S. Burnett, PhD; M. Shou, MD; C.W. Lee, MD; S. Barr, MBBCh;
Local Delivery of Marrow-Derived Stromal Cells Augments Collateral Perfusion Through Paracrine Mechanisms T. Kinnaird, MBBCh; E. Stabile, MD; M.S. Burnett, PhD; M. Shou, MD; C.W. Lee, MD; S. Barr, MBBCh;
(A) PCR primers (arrows) designed to distinguish wild type (P1+P2), targeted (P1+P2) and excised (P1+P3)14-
 1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION Supplementary Figure 1. Long-term protection studies. 45 minutes of ischemia was induced in wild type (S1pr2 +/+ ) and S1pr2 -/- by MCAO. A) 5 days later brains were harvested
SUPPLEMENTARY INFORMATION Supplementary Figure 1. Long-term protection studies. 45 minutes of ischemia was induced in wild type (S1pr2 +/+ ) and S1pr2 -/- by MCAO. A) 5 days later brains were harvested
HMG-CoA reductase inhibitor mobilizes bone marrow derived endothelial progenitor cells
 HMG-CoA reductase inhibitor mobilizes bone marrow derived endothelial progenitor cells See related Commentary on pages 365 366. Joan Llevadot, 1 Satoshi Murasawa, 1 Yasuko Kureishi, 1 Shigeki Uchida, 1
HMG-CoA reductase inhibitor mobilizes bone marrow derived endothelial progenitor cells See related Commentary on pages 365 366. Joan Llevadot, 1 Satoshi Murasawa, 1 Yasuko Kureishi, 1 Shigeki Uchida, 1
Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/-
 Supplemental Material Results. Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/- and Slc2a7 -/- mice. The expression of AE1 in the kidney was examined in Slc26a7 KO mice.
Supplemental Material Results. Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/- and Slc2a7 -/- mice. The expression of AE1 in the kidney was examined in Slc26a7 KO mice.
Stem Cell Therapy for Ischemic Heart Disease : A Status Report
 Stem Cell Therapy for Ischemic Heart Disease : A Status Report Do Sun Lim, M.D. Department of Internal Medicine Korea University College of Medicine Anam Hospital E mail : dslmd@kumc.or.kr Abstract Myocardial
Stem Cell Therapy for Ischemic Heart Disease : A Status Report Do Sun Lim, M.D. Department of Internal Medicine Korea University College of Medicine Anam Hospital E mail : dslmd@kumc.or.kr Abstract Myocardial
Kristina Strutt, MBBS; Richard Caplan, PhD*; Howard Hutchison, MD*; Aaron Dane, MSc; James Blasetto, MD* Circ J 2004; 68:
 Circ J 2004; 68: 107 113 More Western Hypercholesterolemic Patients Achieve Japan Atherosclerosis Society LDL-C Goals With Rosuvastatin Therapy Than With Atorvastatin, Pravastatin, or Simvastatin Therapy
Circ J 2004; 68: 107 113 More Western Hypercholesterolemic Patients Achieve Japan Atherosclerosis Society LDL-C Goals With Rosuvastatin Therapy Than With Atorvastatin, Pravastatin, or Simvastatin Therapy
DECLARATION OF CONFLICT OF INTEREST. No disclosures
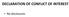 DECLARATION OF CONFLICT OF INTEREST No disclosures micrornas: Role in progression of atherosclerosis Christian Weber Institute for Cardiovascular Prevention (IPEK) Ludwig-Maximilians-University Munich
DECLARATION OF CONFLICT OF INTEREST No disclosures micrornas: Role in progression of atherosclerosis Christian Weber Institute for Cardiovascular Prevention (IPEK) Ludwig-Maximilians-University Munich
Vitamin C Reversed Malfunction of Peripheral Blood-Derived Mononuclear Cells in Smokers Through Antioxidant Properties
 Circ J 2008; 72: 654 659 Vitamin C Reversed Malfunction of Peripheral Blood-Derived Mononuclear Cells in Smokers Through Antioxidant Properties Yoshiaki Takeshita, MD; Yoshio Katsuki, MD; Yousuke Katsuda,
Circ J 2008; 72: 654 659 Vitamin C Reversed Malfunction of Peripheral Blood-Derived Mononuclear Cells in Smokers Through Antioxidant Properties Yoshiaki Takeshita, MD; Yoshio Katsuki, MD; Yousuke Katsuda,
Autologous Peripheral Blood Mononuclear Cell Implantation for Patients With Peripheral Arterial Disease Improves Limb Ischemia
 Circ J 2005; 69: 1260 1265 Autologous Peripheral Blood Mononuclear Cell Implantation for Patients With Peripheral Arterial Disease Improves Limb Ischemia Akio Ishida, MD; Yusuke Ohya, MD; Hitoshi Sakuda,
Circ J 2005; 69: 1260 1265 Autologous Peripheral Blood Mononuclear Cell Implantation for Patients With Peripheral Arterial Disease Improves Limb Ischemia Akio Ishida, MD; Yusuke Ohya, MD; Hitoshi Sakuda,
Journal of the American College of Cardiology Vol. 48, No. 2, by the American College of Cardiology Foundation ISSN /06/$32.
 Journal of the American College of Cardiology Vol. 48, No. 2, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.12.080
Journal of the American College of Cardiology Vol. 48, No. 2, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.12.080
Anti-ceramide Antibody Prevents the Radiation GI Syndrome in Mice
 Anti-ceramide Antibody Prevents the Radiation GI Syndrome in Mice Jimmy A. Rotolo 1, Branka Stancevic 1, Jianjun Zhang 1, Guoqiang Hua 1, John Fuller 1, Xianglei Yin 1, Adriana Haimovitz-Friedman 2, Kisu
Anti-ceramide Antibody Prevents the Radiation GI Syndrome in Mice Jimmy A. Rotolo 1, Branka Stancevic 1, Jianjun Zhang 1, Guoqiang Hua 1, John Fuller 1, Xianglei Yin 1, Adriana Haimovitz-Friedman 2, Kisu
Supplemental Table 1. Primer sequences for transcript analysis
 Supplemental Table 1. Primer sequences for transcript analysis Primer Sequence (5 3 ) Primer Sequence (5 3 ) Mmp2 Forward CCCGTGTGGCCCTC Mmp15 Forward CGGGGCTGGCT Reverse GCTCTCCCGGTTTC Reverse CCTGGTGTGCCTGCTC
Supplemental Table 1. Primer sequences for transcript analysis Primer Sequence (5 3 ) Primer Sequence (5 3 ) Mmp2 Forward CCCGTGTGGCCCTC Mmp15 Forward CGGGGCTGGCT Reverse GCTCTCCCGGTTTC Reverse CCTGGTGTGCCTGCTC
Title: Smooth muscle cell-specific Tgfbr1 deficiency promotes aortic aneurysm formation by stimulating multiple signaling events
 Title: Smooth muscle cell-specific Tgfbr1 deficiency promotes aortic aneurysm formation by stimulating multiple signaling events Pu Yang 1, 3, radley M. Schmit 1, Chunhua Fu 1, Kenneth DeSart 1, S. Paul
Title: Smooth muscle cell-specific Tgfbr1 deficiency promotes aortic aneurysm formation by stimulating multiple signaling events Pu Yang 1, 3, radley M. Schmit 1, Chunhua Fu 1, Kenneth DeSart 1, S. Paul
No option-patients : Is angiogenesis with gene or cell therapy still an option?
 No option-patients : Is angiogenesis with gene or cell therapy still an option? Professor Sigrid Nikol Clinical and Interventional Angiology Asklepios-Klinik St. Georg Hamburg, Germany Angiogenic gene
No option-patients : Is angiogenesis with gene or cell therapy still an option? Professor Sigrid Nikol Clinical and Interventional Angiology Asklepios-Klinik St. Georg Hamburg, Germany Angiogenic gene
Synergistic Effect of Bone Marrow Mobilization and Vascular Endothelial Growth Factor-2 Gene Therapy in Myocardial Ischemia
 Synergistic Effect of Bone Marrow Mobilization and Vascular Endothelial Growth Factor-2 Gene Therapy in Myocardial Ischemia Atsuhiko Kawamoto, MD, PhD*; Toshinori Murayama, MD, PhD*; Kengo Kusano, MD,
Synergistic Effect of Bone Marrow Mobilization and Vascular Endothelial Growth Factor-2 Gene Therapy in Myocardial Ischemia Atsuhiko Kawamoto, MD, PhD*; Toshinori Murayama, MD, PhD*; Kengo Kusano, MD,
Previous studies have suggested that bone marrow
 Essential Role of ICAM-1/CD18 in Mediating EPC Recruitment, Angiogenesis, and Repair to the Infarcted Myocardium Yaojiong Wu, James E. Ip, Jing Huang, Lunan Zhang, Kenichi Matsushita, Choong-Chin Liew,
Essential Role of ICAM-1/CD18 in Mediating EPC Recruitment, Angiogenesis, and Repair to the Infarcted Myocardium Yaojiong Wu, James E. Ip, Jing Huang, Lunan Zhang, Kenichi Matsushita, Choong-Chin Liew,
Supplementary Table 1. Characterization of HNSCC PDX models established at MSKCC
 Supplementary Table 1. Characterization of HNSCC PDX models established at MSKCC Supplementary Table 2. Drug content and loading efficiency estimated with F-NMR and UV- Vis Supplementary Table 3. Complete
Supplementary Table 1. Characterization of HNSCC PDX models established at MSKCC Supplementary Table 2. Drug content and loading efficiency estimated with F-NMR and UV- Vis Supplementary Table 3. Complete
IKK-dependent activation of NF-κB contributes to myeloid and lymphoid leukemogenesis by BCR-ABL1
 Supplemental Figures BLOOD/2014/547943 IKK-dependent activation of NF-κB contributes to myeloid and lymphoid leukemogenesis by BCR-ABL1 Hsieh M-Y and Van Etten RA Supplemental Figure S1. Titers of retroviral
Supplemental Figures BLOOD/2014/547943 IKK-dependent activation of NF-κB contributes to myeloid and lymphoid leukemogenesis by BCR-ABL1 Hsieh M-Y and Van Etten RA Supplemental Figure S1. Titers of retroviral
Tissue repair. (3&4 of 4)
 Tissue repair (3&4 of 4) What will we discuss today: Regeneration in tissue repair Scar formation Cutaneous wound healing Pathologic aspects of repair Regeneration in tissue repair Labile tissues rapid
Tissue repair (3&4 of 4) What will we discuss today: Regeneration in tissue repair Scar formation Cutaneous wound healing Pathologic aspects of repair Regeneration in tissue repair Labile tissues rapid
Promoting Fracture Healing Through Systemic or Local Administration of Allogeneic Mesenchymal Stem Cells
 Promoting Fracture Healing Through Systemic or Local Administration of Allogeneic Mesenchymal Stem Cells Gang Li Dept. of Orthopaedics and Traumatology School of Biomedical Sciences, The Chinese University
Promoting Fracture Healing Through Systemic or Local Administration of Allogeneic Mesenchymal Stem Cells Gang Li Dept. of Orthopaedics and Traumatology School of Biomedical Sciences, The Chinese University
Therapeutic Potential of Human Umbilical Cord Derived Stem Cells in a Rat Myocardial Infarction Model
 Therapeutic Potential of Human Umbilical Cord Derived Stem Cells in a Rat Myocardial Infarction Model Kai Hong Wu, MD, PhD,* Bin Zhou, PhD,* Cun Tao Yu, MD, Bin Cui, MD, Shi Hong Lu, BS, Zhong Chao Han,
Therapeutic Potential of Human Umbilical Cord Derived Stem Cells in a Rat Myocardial Infarction Model Kai Hong Wu, MD, PhD,* Bin Zhou, PhD,* Cun Tao Yu, MD, Bin Cui, MD, Shi Hong Lu, BS, Zhong Chao Han,
Shanghai Institute of Cardiovascular Diseases, Zhongshan Hospital, Fudan University, Shanghai , China 2
 Biomedicine and Biotechnology Volume 22, Article ID 65296, 7 pages doi:.55/22/65296 Research Article Transfer of Bone-Marrow-Derived Mesenchymal Stem Cells Influences Vascular Remodeling and Calcification
Biomedicine and Biotechnology Volume 22, Article ID 65296, 7 pages doi:.55/22/65296 Research Article Transfer of Bone-Marrow-Derived Mesenchymal Stem Cells Influences Vascular Remodeling and Calcification
III. Results and Discussion
 III. Results and Discussion 1. Histological findings in the coronary artery Twenty-four swine had surgical treatments performed in two of the coronary arteries, LAD as well as either the LCX or RCA. A
III. Results and Discussion 1. Histological findings in the coronary artery Twenty-four swine had surgical treatments performed in two of the coronary arteries, LAD as well as either the LCX or RCA. A
(a) Significant biological processes (upper panel) and disease biomarkers (lower panel)
 Supplementary Figure 1. Functional enrichment analyses of secretomic proteins. (a) Significant biological processes (upper panel) and disease biomarkers (lower panel) 2 involved by hrab37-mediated secretory
Supplementary Figure 1. Functional enrichment analyses of secretomic proteins. (a) Significant biological processes (upper panel) and disease biomarkers (lower panel) 2 involved by hrab37-mediated secretory
Chapter 2 Drug therapy or coronary angioplasty for the treatment of coronary artery disease: new insights
 D RUG THERAPY VS CORONARY ANGIOPLASTY R EFERENCES Chapter 2 Drug therapy or coronary angioplasty for the treatment of coronary artery disease: new insights Giovanni Amoroso Ad J. Van Boven Harry J.G.M.
D RUG THERAPY VS CORONARY ANGIOPLASTY R EFERENCES Chapter 2 Drug therapy or coronary angioplasty for the treatment of coronary artery disease: new insights Giovanni Amoroso Ad J. Van Boven Harry J.G.M.
Journal Club WS 2012/13 Stefanie Nickl
 Journal Club WS 2012/13 Stefanie Nickl Background Mesenchymal Stem Cells First isolation from bone marrow 30 ys ago Isolation from: spleen, heart, skeletal muscle, synovium, amniotic fluid, dental pulp,
Journal Club WS 2012/13 Stefanie Nickl Background Mesenchymal Stem Cells First isolation from bone marrow 30 ys ago Isolation from: spleen, heart, skeletal muscle, synovium, amniotic fluid, dental pulp,
Supplemental Methods: Histopathology scoring of individual components of Valentino
 Supplementary Materials Online: Supplemental Methods: Histopathology scoring of individual components of Valentino synovitis grade and Mankin cartilage pathology scale Hemophilic synovitis was graded 0-10
Supplementary Materials Online: Supplemental Methods: Histopathology scoring of individual components of Valentino synovitis grade and Mankin cartilage pathology scale Hemophilic synovitis was graded 0-10
Lessons & Perspectives: What is the role of Cryoplasty in SFA Intervention?
 Lessons & Perspectives: What is the role of Cryoplasty in SFA Intervention? Michael Wholey, MD, MBA San Antonio, TX USA 19/06/2009 at 09:35 during 4mn as a Speaker Session: Improving Femoral Artery Recanalization
Lessons & Perspectives: What is the role of Cryoplasty in SFA Intervention? Michael Wholey, MD, MBA San Antonio, TX USA 19/06/2009 at 09:35 during 4mn as a Speaker Session: Improving Femoral Artery Recanalization
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Stem cell therapy of cardiac disease: an update
 Nephrol Dial Transplant (2004) 19: Editorial Comments 1673 PS analyses, the authors found that the results between these two techniques were not materially different in most of these studies. Even if the
Nephrol Dial Transplant (2004) 19: Editorial Comments 1673 PS analyses, the authors found that the results between these two techniques were not materially different in most of these studies. Even if the
Innovation Interlude: Molecular Imaging in Cardiology. Celestial Doppelgangers and Relativity
 Innovation Interlude: Molecular Imaging in Cardiology Jonathan R. Lindner, M.D. M. Lowell Edwards Professor of Cardiology Knight Cardiovascular Institute Oregon National Primate Research Center Oregon
Innovation Interlude: Molecular Imaging in Cardiology Jonathan R. Lindner, M.D. M. Lowell Edwards Professor of Cardiology Knight Cardiovascular Institute Oregon National Primate Research Center Oregon
Nature Immunology: doi: /ni Supplementary Figure 1. Huwe1 has high expression in HSCs and is necessary for quiescence.
 Supplementary Figure 1 Huwe1 has high expression in HSCs and is necessary for quiescence. (a) Heat map visualizing expression of genes with a known function in ubiquitin-mediated proteolysis (KEGG: Ubiquitin
Supplementary Figure 1 Huwe1 has high expression in HSCs and is necessary for quiescence. (a) Heat map visualizing expression of genes with a known function in ubiquitin-mediated proteolysis (KEGG: Ubiquitin
Supplemental Experimental Procedures
 Cell Stem Cell, Volume 2 Supplemental Data A Temporal Switch from Notch to Wnt Signaling in Muscle Stem Cells Is Necessary for Normal Adult Myogenesis Andrew S. Brack, Irina M. Conboy, Michael J. Conboy,
Cell Stem Cell, Volume 2 Supplemental Data A Temporal Switch from Notch to Wnt Signaling in Muscle Stem Cells Is Necessary for Normal Adult Myogenesis Andrew S. Brack, Irina M. Conboy, Michael J. Conboy,
Haematopoietic stem cells
 Haematopoietic stem cells Neil P. Rodrigues, DPhil NIH Centre for Biomedical Research Excellence in Stem Cell Biology Boston University School of Medicine neil.rodrigues@imm.ox.ac.uk Haematopoiesis: An
Haematopoietic stem cells Neil P. Rodrigues, DPhil NIH Centre for Biomedical Research Excellence in Stem Cell Biology Boston University School of Medicine neil.rodrigues@imm.ox.ac.uk Haematopoiesis: An
Endothelial PGC 1 - α 1 mediates vascular dysfunction in diabetes
 Endothelial PGC-1α mediates vascular dysfunction in diabetes Reporter: Yaqi Zhou Date: 04/14/2014 Outline I. Introduction II. Research route & Results III. Summary Diabetes the Epidemic of the 21st Century
Endothelial PGC-1α mediates vascular dysfunction in diabetes Reporter: Yaqi Zhou Date: 04/14/2014 Outline I. Introduction II. Research route & Results III. Summary Diabetes the Epidemic of the 21st Century
Supplementary Figure (OH) 22 nanoparticles did not affect cell viability and apoposis. MDA-MB-231, MCF-7, MCF-10A and BT549 cells were
 Supplementary Figure 1. Gd@C 82 (OH) 22 nanoparticles did not affect cell viability and apoposis. MDA-MB-231, MCF-7, MCF-10A and BT549 cells were treated with PBS, Gd@C 82 (OH) 22, C 60 (OH) 22 or GdCl
Supplementary Figure 1. Gd@C 82 (OH) 22 nanoparticles did not affect cell viability and apoposis. MDA-MB-231, MCF-7, MCF-10A and BT549 cells were treated with PBS, Gd@C 82 (OH) 22, C 60 (OH) 22 or GdCl
Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury
 Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury Bastian OW, Koenderman L, Alblas J, Leenen LPH, Blokhuis TJ. Neutrophils contribute to
Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury Bastian OW, Koenderman L, Alblas J, Leenen LPH, Blokhuis TJ. Neutrophils contribute to
LDL Uptake Cell-Based Assay Kit
 LDL Uptake Cell-Based Assay Kit Catalog Number KA1327 100 assays Version: 07 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 Principle of the Assay...
LDL Uptake Cell-Based Assay Kit Catalog Number KA1327 100 assays Version: 07 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 Principle of the Assay...
SUPPLEMENTARY INFORMATION
 b 350 300 250 200 150 100 50 0 E0 E10 E50 E0 E10 E50 E0 E10 E50 E0 E10 E50 Number of organoids per well 350 300 250 200 150 100 50 0 R0 R50 R100 R500 1st 2nd 3rd Noggin 100 ng/ml Noggin 10 ng/ml Noggin
b 350 300 250 200 150 100 50 0 E0 E10 E50 E0 E10 E50 E0 E10 E50 E0 E10 E50 Number of organoids per well 350 300 250 200 150 100 50 0 R0 R50 R100 R500 1st 2nd 3rd Noggin 100 ng/ml Noggin 10 ng/ml Noggin
