Thoracic Trauma: 5/19/2010. Keihan Golshani, MD, Assistant Professor of emergency Medicine, Isfahan Medical University,
|
|
|
- Edwina Jones
- 5 years ago
- Views:
Transcription
1 Thoracic Trauma: 1
2 Thoracic trauma: A significant cause of mortality. Many patients with thoracic trauma: die after reaching the hospital Many of them can be prevented by: Prompt diagnosis and treatment. 10% of blunt chest injury require thoracotomy 15 30% of penetrating chest injury 2
3 Chest injury can induce: Hypoxia Hypercarbia Acidosis 3
4 Initial assessment and treatment: Primary survey Resuscitation of vital functions Detailed secondary survey Definitive care 4
5 Because hypoxia is the most serious feature of chest injury the goal of early intervention is to prevent or correct hypoxia. 5
6 What are the significant pathophysiologic effects of chest injury that I should identify in primary survey and when and who do I correct them? 6
7 Primary survey begins with the airway Major problems should corrected as they are identified. Listening for air movement at the patient s nose, mouth and lung fields. Inspecting the oropharynx for foreign body obstruction. Observing for intercostal and supraclavicular muscle retractions. 7
8 Acute laryngeal obstruction from laryngeal trauma. Posterior dislocation of the clavicular head causing upper airway obstruction ( stridor or marked change in the expected voice quality. Treatment with extending the shoulders or grasping the clavicle with a towel clip and reducing the fracture. 8
9 Breathing: Patient s chest and neck completely exposed for assessment of breathing and neck veins. Observing Palpating for assessment of respiratory quality Listening 9
10 Important signs of chest injury: RR Change in breathing pattern Shallow respirations Cyanosis (late) 10
11 Major thoracic injuries: Tension pneumothorax Open pneumothorax Flail chest Pulmonary contusion Massive hemothorax 11
12 Pitfalls: After intubation: common reason for loss of breath sounds in left thorax is a right mainstem intubation. 12
13 Tension pneumothorax: One way valve Also may occur after markedly displaced thoracic spine fractures. Is a clinical diagnosis. Chest pain, air hunger, respiratory distress, tachycardia, hypotension, tracheal deviation, unilateral absence of breath sounds, neck vein distension and cyanosis. Treatment: needle thoracentesis and then insertion of chest tube. 13
14 Open pneumothorax: If the opening in the chest wall is approximately two thirds the diameter of trachea air passes preferentially through the chest wall defect with each respiratory effort so ventilation is impaired. Closing the defect with a sterile occlusive dressing then typed on three sides+ a chest tube remote of the wound as soon as possible. Definitive surgical closure of the defect is frequently required. 14
15 15
16 Flail chest and pulmonary contusion: When a segment of the chest wall does not have bony continuity with the rest of the thoracic cage. Two or more ribs fractured in two or more places. Results in sever disruption of normal chest wall movement. If the injury to the lung (pulmonary contusion) is significant, serious hypoxia may results. Restricted chest wall movement associated with pain and underlying lung injury are important causes of hypoxia. 16
17 Cont. flail chest: May not be apparent initially. The patient moves air poorly. Movement of the thorax is asymmetrical and uncoordinated. Palpation of abnormal respiratory motion and crepitation of rib or cartilage fractures. CXR may suggest multiple rib fractures but may not show costochondral separation. ABG (respiratory failure with hypoxia)may aid in diagnosing a flail chest. 17
18 Cont. flail chest: Initial therapy includes: adequate ventilation administration of humidified oxygen fluid resuscitation (avoid over hydration) provide analgesia to improve ventilation A short period of intubation and ventilation may be required. 18
19 19
20 Massive hemothorax: By compressing the lung and preventing adequate ventilation. Acute accumulations of blood more dramatically present as hypotension and shock. 20
21 Circulation: The patient s pulse should be assessed for quality, rate and regularity. Blood pressure and pulse pressure is measured and the peripheral circulation assessed by observing and palpating the skin for color and temperature. Neck veins should be assessed for distention, remembering that neck veins may not be distended in patients with hypovolemia and cardiac tamponade, tension pneumothorax or traumatic diaphragmatic injury. 21
22 A cardiac monitor and pulse oximeter should be attached to the patient. Thoracic trauma are susceptible to myocardial injury, may lead to dysrhythmias. Hypoxia and acidosis enhance this possibility. PEA may be present in cardiac tamponade, tension pneumothorax, profound hypovolemia and cardiac injury. 22
23 Massive hemothorax: Rapid accumulation of more than 1500 ml of blood or one third or more of the patient s blood volume in the chest cavity. Discovered when shock is associated with the absence of breath sounds or dullness to percussion on one side of the chest. 23
24 Cont. Massive hemothorax: Large caliber intravenous and a rapid crystalloid infusion are begun and type specific blood is administered as soon as possible. restoration of blood volume and decompression of the chest cavity. A single chest tube (38 French) is inserted. Be prepare for autotransfusion. If 1500 ml is immediately evacuated it is highly likely that an early thoracotomy will be required. 24
25 Initial volume output of less than 1500 ml but continue to bleed may require a thoracotomy. This decision is based not on the rate of continuing blood loss (200 cc/hour for 2 4 hr), but on the patient s physiologic status. A persistent need for blood transfusions is an indication for thoracotomy. 25
26 Penetrating anterior chest wounds medial to the nipple line and posterior wounds medial to the scapula should alert the doctor to the possible need for thoracotomy. Thoracotomy is not indicated unless a surgeon qualified by training and experience is present. 26
27 Cardiac tamponade: Beck s triad: venous pressure elevation decline in arterial pressure muffled heart tones Diagnostic methods include: Echocardiography (5 10% false negative) FAST, pericardial window. 27
28 t Initial administration of intravenous fluid. If surgical intervention is not available, pericardiocentesis can be diagnostic as well as therapeutic, but is not definitive treatment for cardiac tamponade. 28
29 Resuscitative thoracotomy: Patients with penetrating thoracic injuries (not blunt) with PEA may be candidates for immediate resuscitative thoracotomy ( a qualified surgeon must be present) 29
30 Secondary survey: 30
31 The secondary survey: CXR ABG Pulse oximetry ECG monitoring In this step, the injuries that usually are not obvious on physical examination and missed will be evaluated. 31
32 Simple Pneumothorax: Any pneumothorax is best treated with a chest tube. Observation and aspiration of an asymptomatic pneumothorax may be appropriate but the choice should be made by a qualified doctor. The patient with a pneumothorax should also undergo chest decompression before he/she is transported via air ambulance. 32
33 Hemothorax: Lung laceration Laceration of an intercostal vessel Laceration of internal mammary artery Thoracic spine fracture dislocation An acute hemothorax large enough to appear on a CXR film is best treated with a large caliber (36 French) chest tube. 33
34 Operative exploration should be considered: If 1500 ml of blood obtained immediately through the chest tube If drainage of more than 200 ml/hr for 2 4 hr occurs If blood transfusion is required 34
35 Pulmonary contusion: Is the most common potentially lethal chest injury. Respiratory failure can be subtle (it develops overtime). Pao2<65 mmhg or Sao2<90% on room air may require intubation and mechanical intubation. Pulse oximetry monitoring, ABG, ECG monitoring and appropriate ventilatory equipment are necessary for optimal treatment. 35
36 Any patient with the aforementioned preexisting conditions who is to be transferred should undergo intubation and ventilation. 36
37 Tracheobronchial tree injury: Unusual and potentially fetal. In blunt trauma the majority of such injuries occur within 1 in. (2.54 cm) of the carina. Most die at the scene. If tracheobronchial injury is suspected immediate surgical consultation is warranted. hemoptysis subcutaneous amphysema Tension pneumothorax pneumothorax with a persistent large air leak after tube thoracostomy 37
38 Cont. Tracheobronchial tree injury: Placement of more than one chest tube is often necessary to overcome a very large leak and expand the lung. Temporary intubation of opposite mainstem bronchus may be required for adequate oxygenation. 38
39 Blunt cardiac injury: Can result in: myocardial muscle contusion cardiac chamber rupture coronary artery dissection and/or thrombosis valvular disruption. The clinically important sequelae of myocardial contusion are hypotension, dysrhythmias or wall motion abnormality on 2D echocardiography. ECG findings: Multiple PVC, Unexplained sinus tachycardia, AF, BBB (often RBBB), St segment changes. Elevated CVP in the absent of an obvious cause may indicate RV dysfunction secondary to contusion. 39
40 Traumatic Aortic disruption: A common cause of sudden death after an automobile collision or fall from a great heigh. A history of decelarating force + Widened mediastinum Obliteration of aortic knob Deviation of the trachea to the right Depression of the left mainstem bronchus Elevation of the right mainstem bronchus CXR Obliteration of the space between pulmonary artery and aorta FINDINGS Deviation of the esophagus to the right Widened paratracheal stripe Widened paraspinalinterfaces presence of a pleural or apical cap Left hemothorax fractures of first or second ribs and scapula 40
41 Cont.Traumatic Aortic disruption: Helical contrast CT: be an accurate screening method for patients with suspected blunt aortic injury. Suspected aortic injury= transfer to a facility capable of rapid definitive diagnosis and treatment center 41
42 Blunt esophageal rupture: Should be consider in: left pneumothorax or hemothorax without a rib fx. Received a sever blow to the lower sternum or epigastrium and is on pain or shock out of proportion to the apparent injury Has particulate matter in chest tube Presence of mediastinal air 42
43 Subcutaneous emphysema Crushing injury to the chest (Traumatic Asphyxia): crush injury to the chest include upper torso, facial and arm plethora with petechiae secondary to acute, temporary compression of the superior vena cava. Rib, sternum and scapular fx. 43
44 44
45 Abdominal and Pelvic trauma: 45
46 Penetrating torso wounds between the nipple and perineum must be considered as potential causes of intraabdominal injury. Ant.Abdomen: trans nipple line, Inguinal ligaments, symphysis pubis, ant. axillary line 46
47 Blunt trauma: Organs more commonly injured include: The spleen (40 55%) The liver (35 45%) The small bowel (5 10%) Retroperitoneal hematoma (15%) 47
48 Penetrating Trauma: Most commonly involve: the liver the small bowel the abdomen vascular structures 48
49 In patients with hypotension, the doctor s goal is to rapidly determine whether an abdominal injury is present and whether it is the cause of hypotension. 49
50 History: Speed of vehicle Type of collision (frontal impact, lateral impact, side swipe, rear impact or rollover) Vehicle intrusion in to the passenger compartment. Types of restraints used Deployment of air bags Patient s position in the vehicle Status of passengers Information about VS, obvious injuries and prehospital treatment. 50
51 History in penetrating trauma: The time of injury The type of weapon (knife, handgun, rifles, shotgun) Distance from the assailant (in shotgun wounds the likelihood of major visceral injuries decrease beyond the 10 foot or 3 meter range) Number of stab or gunshot wounds sustained The amount of external bleeding The magnitude and location of abdominal pain and is it refer to shoulder or not 51
52 Physical examination: Inspection Ausculation Percussion Palpation Assessment of pelvic stability; urethral, perineal, rectal exam, vaginal exam and gluteal exam (penetrating injury to the gluteal injury are assosciated with an incidence of up to 50% of significant intaabdominal injury.) After rapid PhE the patient should covered with warm blankets to prevent hypothermia. 52
53 Adjuncts to Physical Exams: Gastric tube Urinary catheter: inability to void, unstable pelvic fracture, blood at the meatus, scrotal hematoma, perineal echymosis, high riding prostate, mandate retrograde urethrography before inserting a Foley catheter. X ray (CXR, AP pelvic) FAST: perform it again after 30 minutes. DPL CT scan: in stable patients with no apparent indication for laparotomy. Some GI, diaphragmatic, pancreatic injuries may be missed in CT. Urethrography, Cystography, IV pyelography, GI contrast study 53
54 If there is early or obvious evidence that the patient will be transferred to another facility time consuming tests such as contrast urologic and GI studies, DPL and CT scan, should not be performed. 54
55 Evaluation of penetrating Trauma: Wound exploration and serial physical exam. DPL or CT in ant.abd.stab wounds Double or Triple contrast CT in flank and back injuries Most gunshot wounds to the abdomen managed with laparotomy. 55
56 DPL: 56
57 Indications for laparotomy in penetrating abdominal wounds: Any patient with hemodynamic abnormality Gunshot wound Signs of peritoneal irritation Signs of fascial penetration 57
58 Thoracoabdominal lower chest wounds: Options in asymptomatic patients: serial PhE, CXR, Thoracoscopy, Laparoscopy, CT (for right thoracoabdominal wounds) Due to late posttraumatic left sided diaphragmatic hernias after thoracoabdominal stabwounds so early or immediate laparotomy is an option. 58
59 Indications for laparotomy in adults: Blunt abd. trauma+ hypotension+ positive FAST Blunt abd. trauma+ positive DPL Penetrating abd. Trauma+ Hypotension Gunshot wounds tracing pertoneal or retroperitoneal cavity Evisceration Penetrating trauma+ Bleeding from stomach, rectum, GU Peritonitis Free air, retroperitoneal air, rupture of hemidiaphragm Ruptured viscus 59
60 Specific diagnosis: Diaphragm injuries: L.hemidiaphragm is more commonly injured. Duodenal injuries: unrestrained drivers, bicycle handlebars: bloody gastric aspirate, retroperitoneal air Pancreatic injuries: elevated or rising Amylase, CT(recheck after 8 hours if think about it) Genitourinary injuries Small bowel injuries:sudden deceleration, corrected seat belts, early FAST and CT aren t diagnostic and DPL is better when there is abdominal wall echymosis Solid organes injuries(concomitant hollow viscus injury in less than 5% who primary think having only S.O.I) 60
61 Pelvic fractures: 61
62 Management: A sheet wrapped around the pelvis Pelvic splints Pelvis stabilizing devices Since significant resources are required to care for patients with sever pelvic fractures early consideration for transfer to a Trauma center must be considered. 62
63 63
64 64
65 Thank you 65
In ESH we usually see blunt chest trauma but penetrating injuries also treated here (usually as single injuries, like stab wound)
 Chest Trauma Dr Csaba Dioszeghy MD PhD FRCEM FFICM FERC East Surrey Hospital Emergency Department Scope Thoracic injuries are common and can be life threatening In ESH we usually see blunt chest trauma
Chest Trauma Dr Csaba Dioszeghy MD PhD FRCEM FFICM FERC East Surrey Hospital Emergency Department Scope Thoracic injuries are common and can be life threatening In ESH we usually see blunt chest trauma
CHEST TRAUMA. Dr Naeem Zia FCPS,FACS,FRCS
 CHEST TRAUMA Dr Naeem Zia FCPS,FACS,FRCS Learning objectives Anatomy of chest wall and thoracic viscera Physiology of respiration and nerve pathways for pain Enumerate different thoracic conditions requiring
CHEST TRAUMA Dr Naeem Zia FCPS,FACS,FRCS Learning objectives Anatomy of chest wall and thoracic viscera Physiology of respiration and nerve pathways for pain Enumerate different thoracic conditions requiring
The Management of Chest Trauma. Tom Scaletta, MD FAAEM Immediate Past President, AAEM
 The Management of Chest Trauma Tom Scaletta, MD FAAEM Immediate Past President, AAEM Trichotomizing Rib Fractures Upper 1-3 vascular injuries Middle 4-9 Lower 10-12 12 liver/spleen injuries Management
The Management of Chest Trauma Tom Scaletta, MD FAAEM Immediate Past President, AAEM Trichotomizing Rib Fractures Upper 1-3 vascular injuries Middle 4-9 Lower 10-12 12 liver/spleen injuries Management
9/10/2012. Chapter 49. Learning Objectives. Learning Objectives (Cont d) Thoracic Trauma
 Chapter 49 Thoracic Trauma 1 Learning Objectives Explain relevance of thoracic injuries as part of the overall mortality rate from major trauma List thoracic injuries that may result in early death if
Chapter 49 Thoracic Trauma 1 Learning Objectives Explain relevance of thoracic injuries as part of the overall mortality rate from major trauma List thoracic injuries that may result in early death if
Medical NREMT-PTE. NREMT Paramedic Trauma Exam.
 Medical NREMT-PTE NREMT Paramedic Trauma Exam https://killexams.com/pass4sure/exam-detail/nremt-pte Question: 41 Which of the following most accurately describes the finding of jugular venous distension
Medical NREMT-PTE NREMT Paramedic Trauma Exam https://killexams.com/pass4sure/exam-detail/nremt-pte Question: 41 Which of the following most accurately describes the finding of jugular venous distension
The ABC s of Chest Trauma
 The ABC s of Chest Trauma J Bradley Pickhardt MD, FACS Providence St Patrick Hospital What s the Problem? 2/3 of trauma patients have chest trauma Responsible for 25% of all trauma deaths Most injuries
The ABC s of Chest Trauma J Bradley Pickhardt MD, FACS Providence St Patrick Hospital What s the Problem? 2/3 of trauma patients have chest trauma Responsible for 25% of all trauma deaths Most injuries
Chapter 29 - Chest Injuries
 1 2 3 4 5 6 7 8 9 National EMS Education Standard Competencies (1 of 5) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
1 2 3 4 5 6 7 8 9 National EMS Education Standard Competencies (1 of 5) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
Introduction to Advanced Trauma Life Support ATLS
 Introduction to Advanced Trauma Life Support ATLS Objectives Concepts of primary & secondary survey Priorities & Life threatening conditions Clinical & Surgical skills Basic knowledge Rapid assessment
Introduction to Advanced Trauma Life Support ATLS Objectives Concepts of primary & secondary survey Priorities & Life threatening conditions Clinical & Surgical skills Basic knowledge Rapid assessment
Chest Trauma.
 Chest Trauma www.fisiokinesiterapia.biz Objectives Anatomy of Thorax Main Causes of Chest Injuries S/S of Chest Injuries Different Types of Chest Injuries Treatments of Chest Injuries Anatomy of the chest
Chest Trauma www.fisiokinesiterapia.biz Objectives Anatomy of Thorax Main Causes of Chest Injuries S/S of Chest Injuries Different Types of Chest Injuries Treatments of Chest Injuries Anatomy of the chest
Emergency Room Resuscitation of the Unstable Trauma Patient
 Emergency Room Resuscitation of the Unstable Trauma Patient Goals of trauma resuscitation Maintain: Systemic oxygenation Systemic perfusion Neurologic function Approach to unstable trauma patient Primary
Emergency Room Resuscitation of the Unstable Trauma Patient Goals of trauma resuscitation Maintain: Systemic oxygenation Systemic perfusion Neurologic function Approach to unstable trauma patient Primary
Chapter 29 - Chest_and_Abdominal_Trauma
 Introduction to Emergency Medical Care 1 OBJECTIVES 29.1 Define key terms introduced in this chapter. Slides 11, 15, 18, 27 29.2 Describe mechanisms of injury commonly associated with chest injuries. Slides
Introduction to Emergency Medical Care 1 OBJECTIVES 29.1 Define key terms introduced in this chapter. Slides 11, 15, 18, 27 29.2 Describe mechanisms of injury commonly associated with chest injuries. Slides
Abdomen and Genitalia Injuries. Chapter 28
 Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Trauma. Neck trauma zones. Neck Injuries 1/3/2018. Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure
 Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
The Primary Survey. C. Clay Cothren, MD FACS. Attending Surgeon, Denver Health Medical Center Assistant Professor of Surgery, University of Colorado
 The Primary Survey C. Clay Cothren, MD FACS Attending Surgeon, Denver Health Medical Center Assistant Professor of Surgery, University of Colorado Outlining the ABCs Why do we need such an approach? The
The Primary Survey C. Clay Cothren, MD FACS Attending Surgeon, Denver Health Medical Center Assistant Professor of Surgery, University of Colorado Outlining the ABCs Why do we need such an approach? The
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
INJURIES CHEST, ABDOMEN, LIMBS. FN Brno November 2011
 INJURIES CHEST, ABDOMEN, LIMBS FN Brno November 2011 Injury Chest Abdomen Limbs Injury to the rib cage Fractured one or more ribs Sharp pain at the site of fracture Pain on taking a deep breath Shallow
INJURIES CHEST, ABDOMEN, LIMBS FN Brno November 2011 Injury Chest Abdomen Limbs Injury to the rib cage Fractured one or more ribs Sharp pain at the site of fracture Pain on taking a deep breath Shallow
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D.
 1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
PRE-HOSPITAL EMERGENCY CARE COURSE.
 PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
PEDIATRIC TRAUMA: Implications for Respiratory Care
 PEDIATRIC TRAUMA: Implications for Respiratory Care 17 th Annual Rainbow Respiratory Conference - September 4, 2015 Mike Dingeldein, MD Pediatric Surgeon Pediatric Trauma Medical Director Disclosures none
PEDIATRIC TRAUMA: Implications for Respiratory Care 17 th Annual Rainbow Respiratory Conference - September 4, 2015 Mike Dingeldein, MD Pediatric Surgeon Pediatric Trauma Medical Director Disclosures none
CHEST INJURIES. Jacek Piątkowski M.D., Ph. D.
 CHEST INJURIES Jacek Piątkowski M.D., Ph. D. CHEST INJURIES 3-4% of all injuries 8% of patients hospitalized due to injuries 65% of patients who died at the accident place CLASSIFICATION OF THE CHEST INJURIES
CHEST INJURIES Jacek Piątkowski M.D., Ph. D. CHEST INJURIES 3-4% of all injuries 8% of patients hospitalized due to injuries 65% of patients who died at the accident place CLASSIFICATION OF THE CHEST INJURIES
The Primary Survey. Clay Cothren Burlew, MD FACS
 The Primary Survey Clay Cothren Burlew, MD FACS Director, Surgical Intensive Care Unit Attending Surgeon, Denver Health Medical Center Associate Professor of Surgery, University of Colorado Outlining the
The Primary Survey Clay Cothren Burlew, MD FACS Director, Surgical Intensive Care Unit Attending Surgeon, Denver Health Medical Center Associate Professor of Surgery, University of Colorado Outlining the
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Chapter 13. Injuries to the Thorax and Abdomen
 Chapter 13 Injuries to the Thorax and Abdomen Anatomy Review Thoracic cage has 12 pairs of ribs. The first 7 pairs connect directly to sternum. Pairs 8 through 10 connect via common costal cartilage. Pairs
Chapter 13 Injuries to the Thorax and Abdomen Anatomy Review Thoracic cage has 12 pairs of ribs. The first 7 pairs connect directly to sternum. Pairs 8 through 10 connect via common costal cartilage. Pairs
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Imaging of Thoracic Trauma: Tips and Traps. Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania
 Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Abdominal Trauma. Nat Krairojananan M.D., FRCST Department of Trauma and Emergency Medicine Phramongkutklao Hospital
 Abdominal Trauma Nat Krairojananan M.D., FRCST Department of Trauma and Emergency Medicine Phramongkutklao Hospital overview Quick review abdominal anatomy Review of mechanism of injury Review of investigation
Abdominal Trauma Nat Krairojananan M.D., FRCST Department of Trauma and Emergency Medicine Phramongkutklao Hospital overview Quick review abdominal anatomy Review of mechanism of injury Review of investigation
The Secondary Survey
 The Secondary Survey Clay Cothren Burlew, MD FACS Director, Surgical Intensive Care Unit Attending Surgeon, Denver Health Medical Center Associate Professor of Surgery, University of Colorado Outlining
The Secondary Survey Clay Cothren Burlew, MD FACS Director, Surgical Intensive Care Unit Attending Surgeon, Denver Health Medical Center Associate Professor of Surgery, University of Colorado Outlining
Aurora Health Care EMS Continuing Education Spring 2011 Packet THORACIC TRAUMA THE PREHOSPITAL APPROACH TO CHEST INJURY MANAGEMENT
 Aurora Health Care EMS Continuing Education Spring 2011 Packet THORACIC TRAUMA Chest injuries are significant contributors to death from major trauma and can be difficult to assess adequately in the pre-hospital
Aurora Health Care EMS Continuing Education Spring 2011 Packet THORACIC TRAUMA Chest injuries are significant contributors to death from major trauma and can be difficult to assess adequately in the pre-hospital
ATLS: Initial Assessment and Management. SAUSHEC Medical Student Lecture Series
 ATLS: Initial Assessment and Management SAUSHEC Medical Student Lecture Series Objectives Identify sequence of priorities in assessing the multiply injured patient Apply principles outlined in primary
ATLS: Initial Assessment and Management SAUSHEC Medical Student Lecture Series Objectives Identify sequence of priorities in assessing the multiply injured patient Apply principles outlined in primary
Chapter 34. Objectives. Objectives 01/09/2013. Chest Trauma
 Chapter 34 Chest Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced
Chapter 34 Chest Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced
Thoracic Trauma The Spectrum
 Thoracic Trauma The Spectrum Joseph Mathew Consultant, s & Emergency dept. 2 Thoracic Trauma Responsible for 20-25% of all deaths attributed to trauma. Contributing cause of death in an additional 25%
Thoracic Trauma The Spectrum Joseph Mathew Consultant, s & Emergency dept. 2 Thoracic Trauma Responsible for 20-25% of all deaths attributed to trauma. Contributing cause of death in an additional 25%
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
1. Which of the following organs is contained in the retroperitoneal region of the abdomen? A. Stomach B. Liver C. Kidney D.
 1. Which of the following organs is contained in the retroperitoneal region of the abdomen? A. Stomach B. Liver C. Kidney D. Uterus 2. What is Sellick's maneuver? A. A method allowing the rescuer to hold
1. Which of the following organs is contained in the retroperitoneal region of the abdomen? A. Stomach B. Liver C. Kidney D. Uterus 2. What is Sellick's maneuver? A. A method allowing the rescuer to hold
Muscle spasm Diminished bowel sounds Nausea/vomiting
 3 4 5 6 7 8 9 0 Chapter 8: Abdomen and Genitalia Injuries Abdominal Injuries Abdomen is major body cavity extending from to pelvis. Contains organs that make up digestive, urinary, and genitourinary systems.
3 4 5 6 7 8 9 0 Chapter 8: Abdomen and Genitalia Injuries Abdominal Injuries Abdomen is major body cavity extending from to pelvis. Contains organs that make up digestive, urinary, and genitourinary systems.
European Resuscitation Council
 European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
CHEST INJURY PULMONARY CONTUSION
 CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
LIVER INJURIES PROFF. S.FLORET
 LIVER INJURIES PROFF. S.FLORET Abdominal injuries For anatomical consideration: Abdomen can be divided in four areas Intra thoracic abdomen True abdomen Pelvic abdomen Retroperitoneal abdomen ETIOLOGY
LIVER INJURIES PROFF. S.FLORET Abdominal injuries For anatomical consideration: Abdomen can be divided in four areas Intra thoracic abdomen True abdomen Pelvic abdomen Retroperitoneal abdomen ETIOLOGY
Thoracic trauma. 1 The majority of deaths occur after the. FEBRUARY 2001 The Surgical Technologist
 Thoracic trauma Richard Wills, MD, MBA, ACSM, Michael Norton, DC, and Kathryn DeLaney Approximately 25% of nonmilitary trauma-related deaths are due to thoracic trauma. 1 The majority of deaths occur after
Thoracic trauma Richard Wills, MD, MBA, ACSM, Michael Norton, DC, and Kathryn DeLaney Approximately 25% of nonmilitary trauma-related deaths are due to thoracic trauma. 1 The majority of deaths occur after
Trauma Overview. Chapter 22
 Trauma Overview Chapter 22 Kinematics of Trauma Injuries are the leading cause of death among children and young adults. Kinematics introduces the basic physical concepts that dictate how injuries occur
Trauma Overview Chapter 22 Kinematics of Trauma Injuries are the leading cause of death among children and young adults. Kinematics introduces the basic physical concepts that dictate how injuries occur
Shot Through the Heart (And You re to Blame): Penetrating Cardiac Trauma
 Shot Through the Heart (And You re to Blame): Penetrating Cardiac Trauma Yalaunda M. Thomas, MD, FACS The American College of Osteopathic Emergency Physicians Spring Seminar April 5, 2018 Disclosures I
Shot Through the Heart (And You re to Blame): Penetrating Cardiac Trauma Yalaunda M. Thomas, MD, FACS The American College of Osteopathic Emergency Physicians Spring Seminar April 5, 2018 Disclosures I
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
SPECIAL DIAGNOSTIC STUDIES IN BLUNT TRAUMA OLEH : Prof.DR.Dr Abdul Rasyid SpRad (K),Ph.D Dr.Evo Elidar Sp.Rad
 SPECIAL DIAGNOSTIC STUDIES IN BLUNT TRAUMA OLEH : Prof.DR.Dr Abdul Rasyid SpRad (K),Ph.D Dr.Evo Elidar Sp.Rad Trauma Emergency Room layout Ideally the trauma emergency room is centrally located to provide
SPECIAL DIAGNOSTIC STUDIES IN BLUNT TRAUMA OLEH : Prof.DR.Dr Abdul Rasyid SpRad (K),Ph.D Dr.Evo Elidar Sp.Rad Trauma Emergency Room layout Ideally the trauma emergency room is centrally located to provide
ITLS Advanced Pre-Test Annotated Key 8 th Edition
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
Basic Assessment and Treatment of Trauma
 Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Shedding Light on Neonatal X-rays. Objectives. Indications for X-Rays 5/14/2018
 Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
Professional Development & Training MM3. Firefighter Prehospital Care Program. Maintenance Module 3 Course Mill Version
 Professional Development & Training MM3 Firefighter Prehospital Care Program F T Maintenance Module 3 Course Mill Version S Objectives Upon successful completion of the Firefighter Prehospital Care Maintenance
Professional Development & Training MM3 Firefighter Prehospital Care Program F T Maintenance Module 3 Course Mill Version S Objectives Upon successful completion of the Firefighter Prehospital Care Maintenance
Damage Control in Abdominal and Pelvic Injuries
 Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Advances in MDCT of Thoracic Trauma
 Baltic Congress of Radiology, Riga 2010 Advances in MDCT of Thoracic Trauma Robert A. Novelline, MD Professor of Radiology, Harvard Medical School Director of Emergency Radiology, Massachusetts General
Baltic Congress of Radiology, Riga 2010 Advances in MDCT of Thoracic Trauma Robert A. Novelline, MD Professor of Radiology, Harvard Medical School Director of Emergency Radiology, Massachusetts General
RCH Trauma Guideline. Management of Traumatic Pneumothorax & Haemothorax. Trauma Service, Division of Surgery
 RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
Session Number 219 A BLUNT REVIEW OF THE PENETRATING ISSUES IN CHEST TRAUMA
 Session Number 219 A BLUNT REVIEW OF THE PENETRATING ISSUES IN CHEST TRAUMA Lisa C. Laphan-Morad, MSN, APN-C Administrative Director of Surgical & Ambulatory Services Nurse Practitioner Virtua Health Marlton,
Session Number 219 A BLUNT REVIEW OF THE PENETRATING ISSUES IN CHEST TRAUMA Lisa C. Laphan-Morad, MSN, APN-C Administrative Director of Surgical & Ambulatory Services Nurse Practitioner Virtua Health Marlton,
Initial Assessment and Management of the Trauma Patient
 Initial Assessment and Management of the Trauma Patient 1 Epidemiology Road Traffic Accidents are major cause of long term morbidity and mortality in developing nations WHO predicts that by 2020, Road
Initial Assessment and Management of the Trauma Patient 1 Epidemiology Road Traffic Accidents are major cause of long term morbidity and mortality in developing nations WHO predicts that by 2020, Road
Purpose This Operating Procedure provides guidance on the management of blunt thoracic traumatic injury
 Blunt Thoracic Trauma HELI.CLI.09 Purpose This Operating Procedure provides guidance on the management of blunt thoracic traumatic injury Procedure Management of Blunt Thoracic Traumatic Injury For Review
Blunt Thoracic Trauma HELI.CLI.09 Purpose This Operating Procedure provides guidance on the management of blunt thoracic traumatic injury Procedure Management of Blunt Thoracic Traumatic Injury For Review
: TORSO & PELVIC TRAUMA
 INTRODUCTION Torso injuries include those involving the chest, back, flanks, and abdomen. This guideline also includes assessment and management of pelvic injuries. Neurological Trauma guideline and Management
INTRODUCTION Torso injuries include those involving the chest, back, flanks, and abdomen. This guideline also includes assessment and management of pelvic injuries. Neurological Trauma guideline and Management
Focused History and Physical Examination of the
 Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
PARA107 Summary. Page 1-3: Page 4-6: Page 7-10: Page 11-13: Page 14-17: Page 18-21: Page 22-25: Page 26-28: Page 29-33: Page 34-36: Page 37-38:
 PARA107 Summary Page 1-3: Page 4-6: Page 7-10: Page 11-13: Page 14-17: Page 18-21: Page 22-25: Page 26-28: Page 29-33: Page 34-36: Page 37-38: Injury, Mechanisms of Injury, Time Critical Guidelines Musculoskeletal
PARA107 Summary Page 1-3: Page 4-6: Page 7-10: Page 11-13: Page 14-17: Page 18-21: Page 22-25: Page 26-28: Page 29-33: Page 34-36: Page 37-38: Injury, Mechanisms of Injury, Time Critical Guidelines Musculoskeletal
2. Blunt abdominal Trauma
 Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
APPROACH TO TRAUMA. Dr E.Memary Anesthesiologist Assistant Professor of SBMU
 APPROACH TO TRAUMA Dr E.Memary Anesthesiologist Assistant Professor of SBMU Objectives Describe the initial approach to the injured patient, including the primary and secondary surveys. Identify the types
APPROACH TO TRAUMA Dr E.Memary Anesthesiologist Assistant Professor of SBMU Objectives Describe the initial approach to the injured patient, including the primary and secondary surveys. Identify the types
Kinetic Energy Energy in Motion KE = Mass (weight) X Velocity (speed)² 2 Double Weight = Energy Double Speed = Energy IS THE GREATEST DETERMINANT
 1 Chapter 17 Blunt Trauma 2 Introduction to Blunt Trauma Most common cause of trauma death and disability exchange between an object and the human body, without intrusion through the skin 3 Blunt trauma
1 Chapter 17 Blunt Trauma 2 Introduction to Blunt Trauma Most common cause of trauma death and disability exchange between an object and the human body, without intrusion through the skin 3 Blunt trauma
ABDOMINAL TRAUMA. Aurora Health Care EMS Continuing Education 2 nd Quarter 2011 Packet
 Aurora Health Care EMS Continuing Education 2 nd Quarter 2011 Packet ABDOMINAL TRAUMA Blunt and penetrating abdominal trauma are major causes of morbidity and mortality in the United States, particularly
Aurora Health Care EMS Continuing Education 2 nd Quarter 2011 Packet ABDOMINAL TRAUMA Blunt and penetrating abdominal trauma are major causes of morbidity and mortality in the United States, particularly
TNP Teaching Station E Focus: Intubated Patient, Interpersonal Violence
 TNP Teaching Station E Focus: Intubated Patient, Interpersonal Violence Objective Upon completion of this teaching station the learner will be able to: 1. demonstrate appropriate assessment for a hemodynamically
TNP Teaching Station E Focus: Intubated Patient, Interpersonal Violence Objective Upon completion of this teaching station the learner will be able to: 1. demonstrate appropriate assessment for a hemodynamically
2 Blunt Abdominal Trauma
 2 Blunt Abdominal Trauma Ricardo Ferrada, Diego Rivera, and Paula Ferrada Pearls and Pitfalls Patients suffering a high-energy trauma have solid viscera rupture in the abdomen and/or aortic rupture in
2 Blunt Abdominal Trauma Ricardo Ferrada, Diego Rivera, and Paula Ferrada Pearls and Pitfalls Patients suffering a high-energy trauma have solid viscera rupture in the abdomen and/or aortic rupture in
Pneumothorax. Defined as air in the pleural space which can occur through a number of mechanisms
 Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Algorithms for managing the common trauma patient
 ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
Aggressive Management of Chest Trauma. James Moore Cardiothoracic Anaesthetist & Intensive Care Specialist CCDHB
 Aggressive Management of Chest Trauma James Moore Cardiothoracic Anaesthetist & Intensive Care Specialist CCDHB Outline Why is chest trauma important? Risk Assessment Which patients can go home? Management
Aggressive Management of Chest Trauma James Moore Cardiothoracic Anaesthetist & Intensive Care Specialist CCDHB Outline Why is chest trauma important? Risk Assessment Which patients can go home? Management
We have reviewed this material in accordance with U.S. Copyright Law and have tried to maximize your ability to
 Author(s): Patrick Carter, Daniel Wachter, Rockefeller Oteng, Carl Seger, 2009-2010. License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Author(s): Patrick Carter, Daniel Wachter, Rockefeller Oteng, Carl Seger, 2009-2010. License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma Penetrating neck injury (PNI) comprises 5 to 10 percent of traumatic injuries
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma Penetrating neck injury (PNI) comprises 5 to 10 percent of traumatic injuries
Northwest Community EMS System September 2017: Head and Chest Trauma Credit Questions
 NWC EMSS Sept 2017 CE: Head & Chest Trauma. Credit Questions - page 1 Northwest Community EMS System September 2017: Head and Chest Trauma Credit Questions Name: EMS Agency EMSC/Educator reviewer: Date
NWC EMSS Sept 2017 CE: Head & Chest Trauma. Credit Questions - page 1 Northwest Community EMS System September 2017: Head and Chest Trauma Credit Questions Name: EMS Agency EMSC/Educator reviewer: Date
Evaluation & Management of Penetrating Wounds to the NECK
 Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Penetrating Neck Injuries. Jason Levine MD Lutheran Medical Center July 22, 2010
 Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
Lines and tubes. 1 Nasogastric tubes Endotracheal tubes Central lines Permanent pacemakers Chest drains...
 Lines and tubes 1 Nasogastric tubes... 15 2 Endotracheal tubes.... 19 3 Central lines... 21 4 Permanent pacemakers.... 25 5 Chest drains... 30 This page intentionally left blank 1 Nasogastric tubes Background
Lines and tubes 1 Nasogastric tubes... 15 2 Endotracheal tubes.... 19 3 Central lines... 21 4 Permanent pacemakers.... 25 5 Chest drains... 30 This page intentionally left blank 1 Nasogastric tubes Background
Trauma Activation 7/18/17
 Blunt Rupture of the Thoracic Duct after Severe Thoracic Trauma Samuel Brown, MD Trauma Activation 7/18/17 53 year old male, rear end MVC, exited vehicle and was struck by a semi truck. Denies LOC, complaints
Blunt Rupture of the Thoracic Duct after Severe Thoracic Trauma Samuel Brown, MD Trauma Activation 7/18/17 53 year old male, rear end MVC, exited vehicle and was struck by a semi truck. Denies LOC, complaints
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #2 Blunt Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #2 Blunt Trauma Blunt trauma is the most common cause of traumatic death and disability. The definition
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #2 Blunt Trauma Blunt trauma is the most common cause of traumatic death and disability. The definition
Penetrating Trauma in Pediatric Patients. Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017
 Penetrating Trauma in Pediatric Patients Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017 Introduction Trauma is the leading cause of death between ages of 1-18 years Penetrating injury accounts
Penetrating Trauma in Pediatric Patients Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017 Introduction Trauma is the leading cause of death between ages of 1-18 years Penetrating injury accounts
Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC
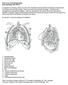 Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC An approach to reviewing a chest x-ray will create a foundation that will facilitate the detection of abnormalities. You should create your own
Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC An approach to reviewing a chest x-ray will create a foundation that will facilitate the detection of abnormalities. You should create your own
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Gunshot Wounds to the Abdomen: From Bullet to Incision. Patrick M Reilly MD FACS
 Gunshot Wounds to the Abdomen: From Bullet to Incision Patrick M Reilly MD FACS Master? I Do Get The Chance to Practice What Are We Not Discussing? Stab Wounds Prehospital Care Management of Specific Injuries
Gunshot Wounds to the Abdomen: From Bullet to Incision Patrick M Reilly MD FACS Master? I Do Get The Chance to Practice What Are We Not Discussing? Stab Wounds Prehospital Care Management of Specific Injuries
Major Trauma Scenarios. Ballarat Health Services Emergency Medicine Training Hub
 Major Trauma Scenarios Ballarat Health Services Emergency Medicine Training Hub Trauma Scenario 1 You receive a phone call from the ambulance service. They have a 27 yr old male involved in a MCA, he is
Major Trauma Scenarios Ballarat Health Services Emergency Medicine Training Hub Trauma Scenario 1 You receive a phone call from the ambulance service. They have a 27 yr old male involved in a MCA, he is
Trauma Workshop! Skills Centre, St George Hospital! Saturday 15 March 2014!
 Trauma Workshop Skills Centre, St George Hospital Saturday 15 March 2014 VMO facilitators: Dr Ricardo Hamilton (Campbelltown Hospital) Dr Mary Langcake (St George Hospital) Dr Anthony Chambers (St George
Trauma Workshop Skills Centre, St George Hospital Saturday 15 March 2014 VMO facilitators: Dr Ricardo Hamilton (Campbelltown Hospital) Dr Mary Langcake (St George Hospital) Dr Anthony Chambers (St George
UBC Department of Urologic Sciences Lecture Series. Urological Trauma
 UBC Department of Urologic Sciences Lecture Series Urological Trauma Disclaimer: This is a lot of information to cover and we are unlikely to cover it all today These slides are to be utilized for your
UBC Department of Urologic Sciences Lecture Series Urological Trauma Disclaimer: This is a lot of information to cover and we are unlikely to cover it all today These slides are to be utilized for your
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
CAE Healthcare istan. Neurological Features Anatomy, Physiology and Clinical signs
 CAE Healthcare istan NYSIM has two wireless istans available for your sessions. We also have them preprogrammed with the NLN Nursing These are available for you to review at the NYSIM Center. They can
CAE Healthcare istan NYSIM has two wireless istans available for your sessions. We also have them preprogrammed with the NLN Nursing These are available for you to review at the NYSIM Center. They can
CAE Healthcare Human Patient Simulator (HPS)
 CAE Healthcare Human Patient Simulator (HPS) The Human Patient Simulator, HPS, is a tethered simulator that is capable of patient assessment and treatment including mechanical ventilation and anesthesia.
CAE Healthcare Human Patient Simulator (HPS) The Human Patient Simulator, HPS, is a tethered simulator that is capable of patient assessment and treatment including mechanical ventilation and anesthesia.
9/10/2012. Chapter 44. Learning Objectives. Learning Objectives (Cont d) Bleeding
 Chapter 44 Bleeding 1 Learning Objectives Describe the etiology, history, and physical findings of external bleeding Predict hemorrhage on the basis of the patient s mechanism of injury Distinguish between
Chapter 44 Bleeding 1 Learning Objectives Describe the etiology, history, and physical findings of external bleeding Predict hemorrhage on the basis of the patient s mechanism of injury Distinguish between
Trauma is a Disease Lets Get it Right A Good Trauma Examination Gives Your Patient Increased Odds for a Good Outcome
 A Good Trauma Examination Gives Your Patient Increased Odds for a Good Outcome druffol@lumc.edu 708.216.4541 Lets Get it Right Trauma is a Disease Importance of Trauma Care and the trauma provider role
A Good Trauma Examination Gives Your Patient Increased Odds for a Good Outcome druffol@lumc.edu 708.216.4541 Lets Get it Right Trauma is a Disease Importance of Trauma Care and the trauma provider role
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT NC ITLS Rev. 2/18 STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT What to wear ITLS is a practical course that stresses hands-on teaching. You should wear comfortable
INTERNATIONAL TRAUMA LIFE SUPPORT NC ITLS Rev. 2/18 STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT What to wear ITLS is a practical course that stresses hands-on teaching. You should wear comfortable
Management of Pelvic Fracture
 Management of Pelvis Fracture with Hemodynamic Instability James W. Davis MD Professor of Clinical Surgery, UCSF/Fresno Chief of Trauma Management of Pelvic Fracture How NOT to do it The basics Evaluation
Management of Pelvis Fracture with Hemodynamic Instability James W. Davis MD Professor of Clinical Surgery, UCSF/Fresno Chief of Trauma Management of Pelvic Fracture How NOT to do it The basics Evaluation
Imaging in the Trauma Patient
 Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
Pediatric Trauma Practice. Guideline for Management of the Child in Shock. Background
 Pediatric Trauma Practice Guideline for Management of the Child in Shock Background Guideline for Management Trauma is the leading cause of death in children and adolescents in the United States. Although
Pediatric Trauma Practice Guideline for Management of the Child in Shock Background Guideline for Management Trauma is the leading cause of death in children and adolescents in the United States. Although
Procedure: Chest Tube Placement (Tube Thoracostomy)
 Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
H. Mitchell Shulman MDCM FRCPC CSPQ Assistant Professor, Dept. of Surgery, McGill Medical School Attending Physician, Royal Victoria Hospital,
 H. Mitchell Shulman MDCM FRCPC CSPQ Assistant Professor, Dept. of Surgery, McGill Medical School Attending Physician, Royal Victoria Hospital, Montreal General Hospital, McGill University Health Center
H. Mitchell Shulman MDCM FRCPC CSPQ Assistant Professor, Dept. of Surgery, McGill Medical School Attending Physician, Royal Victoria Hospital, Montreal General Hospital, McGill University Health Center
Hypotension / Shock. Adult Medical Section Protocols. Protocol 30
 Hypotension / Shock History Blood loss - vaginal or gastrointestinal bleeding, AAA, ectopic Fluid loss - vomiting, diarrhea, fever nfection Cardiac ischemia (M, CHF) Medications Allergic reaction regnancy
Hypotension / Shock History Blood loss - vaginal or gastrointestinal bleeding, AAA, ectopic Fluid loss - vomiting, diarrhea, fever nfection Cardiac ischemia (M, CHF) Medications Allergic reaction regnancy
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Handling Common Problems & Pitfalls During. Oxygen desaturation in patients receiving mechanical ventilation ACUTE SEVERE RESPIRATORY FAILURE
 Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
Assessment of the Trauma Patient
 CHAPTER 10 Assessment of the Trauma Patient Overall Assessment Scheme Scene Size-Up Initial Assessment Trauma Physical Exam Vital Signs & SAMPLE History Medical SAMPLE History Physical Exam & Vital Signs
CHAPTER 10 Assessment of the Trauma Patient Overall Assessment Scheme Scene Size-Up Initial Assessment Trauma Physical Exam Vital Signs & SAMPLE History Medical SAMPLE History Physical Exam & Vital Signs
INTRA-THORACIC AND INTRA-ABDO-MINAL PERFORATION OF THE COLON IN TRAUMATIC DIAPHRAGMATIC
 INTRA-THORACIC AND INTRA-ABDO-MINAL PERFORATION OF THE COLON IN TRAUMATIC DIAPHRAGMATIC Pages with reference to book, From 14 To 16 S. Amjad Hussain, Chinda Suriyapa, Karl Grubaugh ( Depts. of Surger and
INTRA-THORACIC AND INTRA-ABDO-MINAL PERFORATION OF THE COLON IN TRAUMATIC DIAPHRAGMATIC Pages with reference to book, From 14 To 16 S. Amjad Hussain, Chinda Suriyapa, Karl Grubaugh ( Depts. of Surger and
 55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
