Pan-London MTC guidance for patients with REBOA in situ
|
|
|
- Roland Roberts
- 5 years ago
- Views:
Transcription
1 Pan-London MTC guidance for patients with REBOA in situ Introduction REBOA (resuscitative endovascular balloon occlusion of the aorta) is currently being performed by London s air ambulance for exsanguinating noncompressible haemorrhage. Given the extremely shocked state of these patients they are likely to present to any of the London MTCs and require rapid definitive haemorrhage control and balloon deflation. A working knowledge of REBOA is required and the hospital system prepared to ensure safe, smooth and rapid transition from pre-hospital to definitive care. REBOA is a bridge to definitive haemorrhage control and should be seen as an emergency procedure to perfuse central organs and ward off cardiac arrest. It carries numerous significant risks, most notably ischaemia to the limbs, bowel, kidneys and spinal cord depending on the level of occlusion. This summary includes: 1. Background 2. Response to balloon 3. Balloon deflation and removal 4. Post procedure management 5. Appendices: checklist, ED action care, team member roles and patient destination 1. Background Non-compressible torso haemorrhage is the leading cause of preventable trauma deaths. Trauma systems have optimised access to definitive means of haemorrhage control, however a significant proportion of deaths occur before definitive haemorrhage control can be achieved. Half of shocked patients with a pelvic fracture or a torso vascular injury who ultimately die, suffer a cardiac arrest prior to, or soon after arrival in the Emergency department, before any opportunity for intervention (1). Currently, resuscitative thoracotomy with aortic compression is the only means of temporary haemorrhage control in catastrophic torso haemorrhage. This procedure is effective in patients with a thoracic source of haemorrhage that can be directly controlled, but is maximally invasive and has poor outcomes in those with sub-diaphragmatic haemorrhage. For a meaningful reduction in mortality from these injuries, novel methods of early haemorrhage control are required.
2 REBOA involves positioning an endovascular balloon in the proximal or distal aorta as a means of inflow control and afterload augmentation in patients with severe non-compressible haemorrhage, providing temporary circulatory support until haemostasis can be achieved (11-14). REBOA carries numerous potential risks, including renal, splanchnic and spinal cord ischaemia and vascular injury. It should be seen as an extreme temporizing measure to save the life of an exsanguinating patient and to avoid thoracotomy. Practically speaking, only two areas of the aorta are of interest in the context of catastrophic haemorrhage control: the supra-coeliac aorta (immediately above the coeliac trunk and diaphragm) and the terminal aorta (below the renal and mesenteric arteries). As with an aortic cross clamp, the higher the occlusion, the greater the risk of organ and life-threatening ischaemia. Procedure summary: Using a seldinger technique, a 7 French vascular sheath is inserted into the femoral artery and through this a balloon catheter is fed into the aorta. The balloon is inflated to occlude the aorta, reducing blood loss and increasing central perfusion. Current practice is to occlude the terminal aorta at its bifurcation to treat pelvic and junctional vascular (groin) haemorrhage. There may be a move in the future to occlude the supra-coeliac aorta (above the diaphragm) to treat abdominal haemorrhage. It should be noted that, until this is the case, this procedure will not control haemorrhage above the pelvis.
3 2. Response to balloon: In the majority, when the balloon is correctly sited, there will be an immediate physiological response including a rise in BP, ETCO2 and improvement in skin color. However, this may not be text book, particularly in a patient who is profoundly hypovolaemic. Such patients may show an initial response followed by a deterioration and they often require aggressive blood product resuscitation as well as immediate transfer to definitive care. A non-textbook response may be confusing to the clinical team who must decide whether this is due to balloon failure, misplacement, misdiagnosis or simply a successful procedure in a profoundly hypovolaemic patient. This will in turn rely on confidence in the initial diagnosis and confidence in the procedure. If a patient continues to deteriorate rapidly the clinician must decide whether to deflate the balloon, change position or proceed to laparotomy/thoracotomy. All will depend on the individual patient and surrounding factors, but it is well worth pre-thinking these eventualities. Conversley, a text-book response with marked improvement in haemodynamics must not distract the team from the urgency of the situation and importance of a short balloon time. Team leadership In our experience the team leader must put in a great deal of effort to expedite definitive haemorrhage control and avoid unnecessary interventions and investigations unless absolutely essential. The team are likely to become distracted given the novel nature of the procedure. It is essential that the team has a leader who is not task focused and that concurrent activity continues. It is our practice that the team leader is not the person performing the procedure or managing the balloon. Post procedure Although haemodynamics may improve dramatically following aortic occlusion, balloon inflation time correlates inversely with survival (12), therefore any delays to definitive haemorrhage control must be avoided. After REBOA, the patient must be transferred to the operating theatre or IR suite as quickly as possible. Rapid progress to definitive haemorrhage control and balloon deflation is vital. CT: Only if there is a well-defined question requires answering urgently (e.g. if you have evidence of an aortic injury or a life threatening intracranial bleed which may require simultaneous surgery), consider CT but remain mindful of
4 time. Aggressive haemostatic volume resuscitation is required if an attempt at balloon deflation in the CT scanner is to be enabled, both to facilitate a contrast CT scan and to minimise continuous balloon inflation time. If there is debate about the injury pattern or stability of the patient and whether or not REBOA was required be mindful that the balloon may give the appearance of stability in the face of extreme shock. Trust the judgment of the initial treating team. Consider very carefully before deflating the balloon and undertaking CT, if you do not have the confidence to deflate the balloon, do not delay for a CT which is not absolutely essential. Decision making The overriding aim should be definitive vascular control and balloon deflation, these should both be seen as an extreme emergency. Imaging As part of the immediate primary survey in the ED resus room, a Chest X-Ray, Pelvic X-ray and FAST scan are likely to yield important information. These patients should not go straight to CT on arrival as this is not indicated in the vast majority and will serve to prolong occlusion time and increase mortality. If the handover, response to balloon and primary survey reveals a definite indication for CT imaging it may be considered, as described above. Be acutely mindful of time and verbalise a plan B with the whole team. Interventions Filling: All patients are likely to need aggressive blood product resuscitation, do not be falsely reassured by an improvement in haemodynamics. In some cases volume resuscitation may need to be limited if blood pressures are supranormal, but be ready with large bore central access to fill rapidly once the balloon is deflated. Drugs: Calcium chloride and sodium bicarbonate are likely to help mitigate complications of aortic occlusion and reperfusion as well massive haemorrhage and transfusion. Close dialogue between team leader and senior anaesthetist is essential before and during deflation, the situation can be compared to an aortic cross-clamp. Time and team management: This should be constantly borne in mind and best practice is to have a separate team leader from the REBOA operator. Be aware of the likely distraction by this novel procedure. Consider very carefully the need for any test or intervention which delays time to vascular control and balloon deflation.
5 Destination There are a limited number of outcomes following balloon occlusion of the aorta and they will guide your destination: Successful placement and a positive haemodynamic response. - Push immediately to theatre or interventional radiology, depending on predicted injury and preparedness of each. See examples in appendix 1. No positive response to balloon occlusion. One, or all of the sites of haemorrhage may be above the balloon, there has been a complication in the procedure or the balloon is incorrectly placed. - Push immediately to theatre as there are likely too many unknowns to commit to IR (prolonged time to control and likely multiple bleeding sources). Look carefully for signs of improvement, such as pinkness of the lips, change in ETCO2, strength of pulses before deciding there is a complication or misdiagnosis, the balloon may be doing it s job but the patient extremely under-filled. Catastrophic deterioration after balloon occlusion. - Consider balloon deflation if any possibility of complication, especially IVC placement. Check balloon has not been accidentally deflated/displaced. - Consider emergency thoracotomy if deteriorating uncontrollably, the bleed may be above the balloon. Damage/complications: If an iatrogenic injury is suspected and time/stability allows, consider IR as a place to search for and repair the problem. Deflate the balloon if absolutely necessary but leave the wire, catheter and sheath in place. 3. Balloon deflation and sheath removal Treat the REBOA balloon as an aortic clamp. Ongoing requirement for REBOA is assessed frequently and balloon inflation time is kept to an absolute minimum. Prolonged balloon inflation is likely to lead to vital organ damage, permanent disability and death. The risks of aortic occlusion must be balanced carefully against the risk of death from uncontrolled haemorrhage. The REBOA operator should task a team member with alerting the team every 10 minutes after balloon inflation. There should be clear indications for balloon deflation: First and foremost is when vascular control is obtained by other means, deflation should occur as soon as possible. Deflation may be required in order to confirm haemorrhage control e.g. during laparotomy.
6 Balloon deflation may be required in order to gain arterial access in the IR suite. Be prepared to re-inflate quickly if cardiovascular collapse occurs. Deflation may be considered during CT if a scan has been deemed essential, both to facilitate a contrast CT scan and to minimise continuous balloon inflation time. Definitive deflation: As soon as definitive vascular control is achieved, you should aim to definitively deflate and remove the REBOA catheter. This still requires caution and may precipitate cardiovascular collapse due to loss of afterload, ischaemia and reperfusion. Ultimate responsibility for ensuring prompt balloon deflation rests with the trauma team leader coordinating the perioperative phase of the patient s treatment. A full resuscitation/theatre team should be present and the balloon deflated in a planned, coordinated manner, following a full team briefing. Profound haemodynamic instability is common following balloon deflation due to sudden afterload reduction, hypovolaemia, reperfusion of ischaemic tissue, washout of metabolic by-products, hyperkalaemia, hypocalcaemia and acidosis. Sodium Bicarbonate and Calcium Chloride may help to reduce these metabolic effects and close discussion with the anaesthetist in charge is vital. Blood products should be immediately available, for administration through an appropriate warming device and these sequelae prepared for. On deflation, if severe haemodynamic instability is precipitated, a period of intermittent balloon inflation and titrated deflation may be required. At this stage, care must be taken to prevent distal migration of the balloon as described above. Once REBOA is no longer deemed necessary, the REBOA operator may withdraw the balloon catheter. The sheath should be flushed with saline and the IABP monitoring line connected to the side arm of the 7Fr sheath. Sheath removal will require input from the vascular surgeon or interventional radiologist, including closure of the vessel wall defect and active exploration for thrombus.
7 4. Post Procedure Thrombus: Arterial thrombus is very likely, even in the coagulopathic patient, and clot should be actively sought in every case to avoid compounding the effects of balloon occlusion with devastating consequences. Re-vascularisation should be achieved urgently and very close attention paid to limb perfusion and compartment pressures over the coming days. As with an aortic cross clamp there is a risk of a reperfusion insult, rhabdomyolysis and vital organ dysfunction. The patient should remain closely monitored in a high dependency area following the procedure. HEMS Data collection: Accurate and complete data collection is essential. The task of data sheet completion should be the responsibility of the HEMS REBOA operator who performed the procedure. If any missing data or completed data collection forms remain in your MTC, please return to Dr Samy Sadek, ED Consultant at the Royal London Hospital, (samy.sadek@bartshealth.nhs.uk) and Frank Chege, Patient Liaison Nurse at London s Air Ambulance (f.chege@londonsairambulance.co.uk).
8 Appendix 1: Emergency Department preparation checklist. Pre-alert: ED REBOA CHECKLIST - Establish whether REBOA performed, which zone and timing Activate: - Massive haemorrhage protocol - Full Trauma Team Response - Ensure key team members informed and present or prepared: o Consultant and senior nurse in ED o Vascular + Trauma surgery o Interventional Radiology o Anaesthesia o ITU o REBOA operator Prepare: - Resus bay - Trauma team action cards distributed - Blood products ready to give warmed - Drugs: CaCl, NaBicarb, TXA, Anaesthetic - Equipment: thoracotomy pack, trauma line - Portable X ray ready - Ultrasound scanner ready - Emergency theatre open - Interventional radiology suite open - Route to theatre/ir clear
9 Appendix 2: Emergency Department actions. Emergency Department ACTION CARD On arrival in the ED, the key priorities are: - Establish pattern of injury - Establish response to balloon - Make rapid clinical diagnosis - Push to definitive control - Minimize balloon time Imaging: - CXR, PXR and FAST are useful - CT adds time and carries high risk: only consider if a specific urgent question requires answering In theatre: - Control haemorrhage urgently - Visualise/feel balloon position in aorta - Deflate balloon ASAP when haemorrhage controlled - If haemorrhage recurs, re-inflate balloon and control surgically - Brief entire team before deflation - Ensure balloon catheter does not migrate when deflated In IR: - Consider balloon catheter removal or access to contralateral side - Likely need deflation to visualize and access vessels - Rescue/repair of any complications, After definitive deflation: - Remove central balloon catheter, with guidewire - Note total balloon occlusion time - Leave arterial sheath in place until formal removal and vascular repair - Sheath has a self sealing port, side port may be used as arterial transducer - Complete data collection sheet Post procedure: - Consider full CT imaging depending on progress and clinical state - Thrombus: actively seek in all cases - Formal vessel closure as required with sheath removal - Watch carefully for limb thrombus, ischaemia and compartment syndrome
10 Appendix 3: Recommended individual roles. Individual team member Action Cards: To be developed by the MTCs, depending on individual systems, but to contain the following team members and these basic principles: Trauma team leader Role decision making and situational awareness Senior ED nurse Role coordinate monitoring, blood transfusion and equipment Trauma surgery consultant Role decision on definitive care Senior anaesthetist Role orchestrate resuscitation and anaesthesia ODP Role ensure safe anaesthesia and expedite transfer Interventional Radiologist Role definitive haemorrhage control +/- rescue or repair from procedure Theatre coordinator Role ensure swift transfer to and through theatres REBOA Operator Role manage the balloon catheter - Ensure balloon is not displaced during movement - Monitor balloon time and alert the team every 10 minutes - Stay with patient until balloon deflated - Ensure data collection completed
11 Appendix 4: Destination The immediate destination for a patient after arrival in hospital is crucial. In order to aid decision making and avoid delays it is worth pre-thinking the likely situations, in the context of your MTC s process and resources. These are not fixed or exclusive and depend on individual circumstances, hence examples are given but an algorithm is not drawn. Theatre or IR? - FAST negative with a pelvic fracture: IR if ready immediately, if not, to theatre for damage control surgery. - FAST positive with a pelvic fracture: IR if ready immediately and you are certain the pelvis is the source of bleeding, if not, to theatre damage control surgery. - Stab wound to groin: to theatre for damage control surgery. - Stab wound to buttock: Consider IR if ready and you are certain the pelvis is the source of bleeding, if not, to theatre damage control surgery. Need for an immediate CT? As mentioned, only if a well-defined question requires answering urgently consider CT but remain mindful of time. - Evidence of a skull fracture but high GCS on scene, or normal pupils at primary survey. - Possibility of aortic injury but no hard signs. - Concern re the exact pattern of injury and other associated injuries. Do not scan now, push to IR or theatre. CT should be delayed until the primary life-threatening problem is treated and the balloon is deflated. Apparent haemodynamic stability is created by the balloon and ischaemic time is building. Ensure team leader is aware that CT is required as soon as possible after haemorrhage control is achieved and balloon deflated. - Strong signs of a life threatening intracranial bleed with mass effect and neurosurgeons able to operate simultaneously with damage control surgery: consider immediate CT. - Strong evidence of aortic injury and the means to repair this concurrently are available: consider immediate CT. Think carefully about what you are scanning and why, consider deflating balloon for CT depending on injuries and response, verbalise your plan B should the patient deteriorate or scanning become prolonged.
12 References 1. Perkins ZB, De'Ath HD, Aylwin C, Brohi K, Walsh M, Tai NRM. Epidemiology and outcome of vascular trauma at a British Major Trauma Centre. Eur J Vasc Endovasc Surg Aug.;44(2): Veith FJ, Lachat M, Mayer D, Malina M, Holst J, Mehta M, et al. Collected world and single center experience with endovascular treatment of ruptured abdominal aortic aneurysms. Ann Surg Nov.;250(5): Karkos CD, Harkin DW, Giannakou A, Gerassimidis TS. Mortality after endovascular repair of ruptured abdominal aortic aneurysms: a systematic review and meta-analysis. Arch Surg Aug.;144(8): Malina M, Veith F, Ivancev K, Sonesson B. Balloon occlusion of the aorta during endovascular repair of ruptured abdominal aortic aneurysm. J. Endovasc. Ther Oct.;12(5): Karkos CD, Bruce IA, Lambert ME. Use of the intra-aortic balloon pump to stop gastrointestinal bleeding. Ann Emerg Med Sep.;38(3): Harma M, Harma M, Kunt AS, Andac MH, Demir N. Balloon occlusion of the descending aorta in the treatment of severe post-partum haemorrhage. Aust N Z J Obstet Gynaecol Apr.;44(2): Gupta BK, Khaneja SC, Flores L, Eastlick L, Longmore W, Shaftan GW. The role of intra-aortic balloon occlusion in penetrating abdominal trauma. The Journal of Trauma: Injury, Infection, and Critical Care. 1989;29: White JM, Cannon JW, Stannard A, Markov NP, Spencer JR, Rasmussen TE. Endovascular balloon occlusion of the aorta is superior to resuscitative thoracotomy with aortic clamping in a porcine model of hemorrhagic shock. Surgery Sep.;150(3): Morrison JJ, Percival TJ, Markov NP, Villamaria C, Scott DJ, Saches KA, et al. Aortic balloon occlusion is effective in controlling pelvic hemorrhage. J Surg Res Oct.;177(2): Moore LJ, Brenner M, Kozar RA, Pasley J, Wade CE, Baraniuk MS, et al. Implementation of resuscitative endovascular balloon occlusion of the aorta as an alternative to resuscitative thoracotomy for noncompressible truncal hemorrhage. The Journal of Trauma and Acute Care Surgery Oct.;79(4): Stannard A, Eliason JL, Rasmussen TE. Resuscitative endovascular balloon occlusion of the aorta (REBOA) as an adjunct for hemorrhagic shock. The Journal of Trauma: Injury, Infection, and Critical Care Dec. 1;71(6):
13 12. Martinelli T, Thony F, Decléty P, Sengel C, Broux C, Tonetti J, et al. Intraaortic balloon occlusion to salvage patients with life-threatening hemorrhagic shocks from pelvic fractures. J Trauma Apr.;68(4): Brenner ML, Moore LJ, DuBose JJ, Tyson GH, McNutt MK, Albarado RP, et al. A clinical series of resuscitative endovascular balloon occlusion of the aorta for hemorrhage control and resuscitation. Journal of Trauma and Acute Care Surgery Sep. 1;75(3): Ogura T, Lefor AT, Nakano M, Izawa Y, Morita H. Nonoperative management of hemodynamically unstable abdominal trauma patients with angioembolization and resuscitative endovascular balloon occlusion of the aorta. The Journal of Trauma and Acute Care Surgery Jan.;78(1):132 5.
RESUSCITATIVE ENDOVASCULAR BALLOON OCCLUSION OF THE AORTA (REBOA)
 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
5/30/2013. I have no conflicts of interest to disclose. Alicia Privette, MD Trauma & Critical Care Fellow. Trauma = #1 cause of death persons <40 yo 1
 I have no conflicts of interest to disclose. Alicia Privette, MD Trauma & Critical Care Fellow Trauma = #1 cause of death persons
I have no conflicts of interest to disclose. Alicia Privette, MD Trauma & Critical Care Fellow Trauma = #1 cause of death persons
Guidelines and Protocols
 TITLE: PELVIC TRAUMA PURPOSE: Develop a protocol of care that will insure rapid identification and treatment of these patients PROCESS: I. CARE OF PATIENTS WITH PELVIC TRAUMA A. Patients in hemorrhagic
TITLE: PELVIC TRAUMA PURPOSE: Develop a protocol of care that will insure rapid identification and treatment of these patients PROCESS: I. CARE OF PATIENTS WITH PELVIC TRAUMA A. Patients in hemorrhagic
May Clinical Director, Peninsula Trauma Network (Edited for PTN)
 Network Policy Traumatic vascular injuries Guidelines Purpose Date May 2015 Version Following the national introduction of Regional Trauma Networks, Major Trauma Networks (MTN s) are required to have a
Network Policy Traumatic vascular injuries Guidelines Purpose Date May 2015 Version Following the national introduction of Regional Trauma Networks, Major Trauma Networks (MTN s) are required to have a
Latest Advances in Pre-hospital and Retrieval Medicine: what you need to know
 Latest Advances in Pre-hospital and Retrieval Medicine: what you need to know A/Prof Andrew Pearce Clinical Director Education and Training MedSTAR Senior Consultant Emergency Medicine Royal Adelaide Hospital
Latest Advances in Pre-hospital and Retrieval Medicine: what you need to know A/Prof Andrew Pearce Clinical Director Education and Training MedSTAR Senior Consultant Emergency Medicine Royal Adelaide Hospital
REBOA new snake in the grass?
 REBOA new snake in the grass? Does it have a place in South Africa and other LMICs? Tim Hardcastle Trauma Surgeon IALCH/UKZN Controversies in Surgery 2016 History nothing new under the sun (Solomon = Ecclesiates)
REBOA new snake in the grass? Does it have a place in South Africa and other LMICs? Tim Hardcastle Trauma Surgeon IALCH/UKZN Controversies in Surgery 2016 History nothing new under the sun (Solomon = Ecclesiates)
Endovascular Trauma Management. Thomas Larzon, MD, PhD Dep of Cardiothoracic and Vascular Surgery Örebro University Hospital, Sweden
 Endovascular Trauma Management Thomas Larzon, MD, PhD Dep of Cardiothoracic and Vascular Surgery Örebro University Hospital, Sweden Medtronic Symposium, LINC 2016 Disclosures I have the following potential
Endovascular Trauma Management Thomas Larzon, MD, PhD Dep of Cardiothoracic and Vascular Surgery Örebro University Hospital, Sweden Medtronic Symposium, LINC 2016 Disclosures I have the following potential
doi: /ams2.212
 Acute Medicine & Surgery 2016; 3: 345 350 doi: 10.1002/ams2.212 Original Article Outcomes of abdominal trauma patients with hemorrhagic shock requiring emergency laparotomy: efficacy of intra-aortic balloon
Acute Medicine & Surgery 2016; 3: 345 350 doi: 10.1002/ams2.212 Original Article Outcomes of abdominal trauma patients with hemorrhagic shock requiring emergency laparotomy: efficacy of intra-aortic balloon
Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
6. Endovascular aneurysm repair
 Introduction The standard treatment for aortic aneurysm, open repair, involves a large abdominal incision and cross-clamping of the aorta. In recent years, a minimally invasive technique, endovascular
Introduction The standard treatment for aortic aneurysm, open repair, involves a large abdominal incision and cross-clamping of the aorta. In recent years, a minimally invasive technique, endovascular
CDR Jacob Glaser MD 1, William Teeter MD, MS 2, LCOL Travis Gerlach MD 3 and CDR Nathanial Fernandez MD 4
 Case Report Vol. 1, No. 1; 2017; pp 58 62 DOI: 10.26676/jevtm.v1i1.16 Resuscitative Endovascular Balloon Occlusion of the Aorta (REBOA) as an Adjunct to Damage Control Surgery for Combat Trauma: A Case
Case Report Vol. 1, No. 1; 2017; pp 58 62 DOI: 10.26676/jevtm.v1i1.16 Resuscitative Endovascular Balloon Occlusion of the Aorta (REBOA) as an Adjunct to Damage Control Surgery for Combat Trauma: A Case
REBOA - Real World. Lena M. Napolitano, MD
 REBOA - Real World Lena M. Napolitano, MD Lena M. Napolitano MD, FACS Massey Foundation Professor of Surgery Acute Care Surgery [Trauma, Burn, Critical Care, Emergency Surgery] University of Michigan Ann
REBOA - Real World Lena M. Napolitano, MD Lena M. Napolitano MD, FACS Massey Foundation Professor of Surgery Acute Care Surgery [Trauma, Burn, Critical Care, Emergency Surgery] University of Michigan Ann
The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA)
 The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA) Disclosure Speaker name: Ren Wei, Li Zhui, Li Fenghe, Zhao Yu Department of Vascular Surgery, The First Affiliated Hospital of
The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA) Disclosure Speaker name: Ren Wei, Li Zhui, Li Fenghe, Zhao Yu Department of Vascular Surgery, The First Affiliated Hospital of
Hemorrhage Control. Chapter 6
 Chapter 6 The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel H. M. Gray, 1919 Stop the Bleeding!
Chapter 6 The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel H. M. Gray, 1919 Stop the Bleeding!
Resuscitation Checklist
 Resuscitation Checklist Actions if multiple responders are on scene Is resuscitation appropriate? Conditions incompatible with life Advanced decision in place Based on the information available, the senior
Resuscitation Checklist Actions if multiple responders are on scene Is resuscitation appropriate? Conditions incompatible with life Advanced decision in place Based on the information available, the senior
West Yorkshire Major Trauma Network Clinical Guidelines 2015
 WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
Endovascular Aneurysm Repair (EVAR)
 Endovascular Aneurysm Repair (EVAR) Exceptional healthcare, personally delivered You have been diagnosed with an abdominal aortic aneurysm (AAA). This means that the main artery in your abdomen (the aorta)
Endovascular Aneurysm Repair (EVAR) Exceptional healthcare, personally delivered You have been diagnosed with an abdominal aortic aneurysm (AAA). This means that the main artery in your abdomen (the aorta)
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury. Conflict of Interest. Hypotensive shock 5/5/2014. none
 EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
Section 6 Intra Aortic Balloon Pump
 Section 6 Intra Aortic Balloon Pump The Intra Aortic Balloon Pump (IABP) The balloon is synthetic and is made for single use only. It is threaded into the aorta, usually via a femoral approach. The balloon
Section 6 Intra Aortic Balloon Pump The Intra Aortic Balloon Pump (IABP) The balloon is synthetic and is made for single use only. It is threaded into the aorta, usually via a femoral approach. The balloon
Shock and Resuscitation: Part II. Patrick M Reilly MD FACS Professor of Surgery
 Shock and Resuscitation: Part II Patrick M Reilly MD FACS Professor of Surgery Trauma Patient 1823 / 18 Police Dropoff Torso GSW Lower Midline / Right Buttock Shock This Monday Trauma Patient 1823 / 18
Shock and Resuscitation: Part II Patrick M Reilly MD FACS Professor of Surgery Trauma Patient 1823 / 18 Police Dropoff Torso GSW Lower Midline / Right Buttock Shock This Monday Trauma Patient 1823 / 18
How to select ruptured AAA for EVAR or open repair?
 How to select ruptured AAA for EVAR or open repair? Dr. Skyi Pang Associate Consultant Division of Vascular Surgery Department of Surgery Pamela Youde Nethersole Eastern Hospital Hong Kong SAR, China Disclosure
How to select ruptured AAA for EVAR or open repair? Dr. Skyi Pang Associate Consultant Division of Vascular Surgery Department of Surgery Pamela Youde Nethersole Eastern Hospital Hong Kong SAR, China Disclosure
Trans-catheter aortic valve implantation (TAVI) work up
 Trans-catheter aortic valve implantation (TAVI) work up You have been referred for an assessment known as a TAVI work up because you have been diagnosed with aortic stenosis. This factsheet explains the
Trans-catheter aortic valve implantation (TAVI) work up You have been referred for an assessment known as a TAVI work up because you have been diagnosed with aortic stenosis. This factsheet explains the
Trauma CT Scanning Protocol
 Northern Trauma Network Trauma CT Scanning Protocol Background Whole body CT (WBCT) has assumed a pivotal position in trauma management. UK trauma is typically described as blunt and blind i.e. blunt trauma
Northern Trauma Network Trauma CT Scanning Protocol Background Whole body CT (WBCT) has assumed a pivotal position in trauma management. UK trauma is typically described as blunt and blind i.e. blunt trauma
2. Blunt abdominal Trauma
 Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
RESUSCITATION IN TRAUMA. Important things I have learnt
 RESUSCITATION IN TRAUMA Important things I have learnt Trauma resuscitation through the decades What was hot and now is not 1970s 1980s 1990s 2000s Now 1977 Fluids Summary Dogs subjected to arterial hemorrhage
RESUSCITATION IN TRAUMA Important things I have learnt Trauma resuscitation through the decades What was hot and now is not 1970s 1980s 1990s 2000s Now 1977 Fluids Summary Dogs subjected to arterial hemorrhage
Acute dissections of the descending thoracic aorta (Debakey
 Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Haemodynamic deterioration in lateral compression pelvic fracture after prehospital pelvic circumferential compression device application
 Haemodynamic deterioration in lateral compression pelvic fracture after prehospital pelvic circumferential compression device application Authors Alan A Garner Retrieval consultant CareFlight Northmead,
Haemodynamic deterioration in lateral compression pelvic fracture after prehospital pelvic circumferential compression device application Authors Alan A Garner Retrieval consultant CareFlight Northmead,
Severe post-partum haemorrhage (PPH) occurs
 Acta Anaesthesiol Scand 2012; : Printed in Singapore. All rights reserved 2012 The Authors Acta Anaesthesiologica Scandinavica 2012 The Acta Anaesthesiologica Scandinavica Foundation ACTA ANAESTHESIOLOGICA
Acta Anaesthesiol Scand 2012; : Printed in Singapore. All rights reserved 2012 The Authors Acta Anaesthesiologica Scandinavica 2012 The Acta Anaesthesiologica Scandinavica Foundation ACTA ANAESTHESIOLOGICA
Activity Three: Where s the Bleeding?
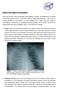 Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
11/1/2014. Just The. Pearls. Everything I do is Off-Label! This is the ultimate lecture for the ADHD emergency physician.
 Just The Everything I do is Off-Label! Pearls This is the ultimate lecture for the ADHD emergency physician. 1 >20 Tips in 60 Minutes You re repeatin yourself ½ Trauma ½ Medical Arrest Crit Care in The
Just The Everything I do is Off-Label! Pearls This is the ultimate lecture for the ADHD emergency physician. 1 >20 Tips in 60 Minutes You re repeatin yourself ½ Trauma ½ Medical Arrest Crit Care in The
J O I N T T R A U M A S Y S T E M C L I N I C A L P R A C T I C E G U I D E L I N E ( J T S C P G ) Contributors T A B L E O F C O N T E N T S
 J O I N T T R A U M A S Y S T E M C L I N I C A L P R A C T I C E G U I D E L I N E ( J T S C P G ) Resuscitative Endovascular Balloon Occlusion of the Aorta (REBOA) for Hemorrhagic Shock (CPG ID: 38)
J O I N T T R A U M A S Y S T E M C L I N I C A L P R A C T I C E G U I D E L I N E ( J T S C P G ) Resuscitative Endovascular Balloon Occlusion of the Aorta (REBOA) for Hemorrhagic Shock (CPG ID: 38)
Competency Title: Caring for a patient with an arterial line
 Appendix 2 Competency Title: Caring for a patient with an arterial line Aims and objectives Following completion of this competency document the practitioner will be able to: Discuss the indications for
Appendix 2 Competency Title: Caring for a patient with an arterial line Aims and objectives Following completion of this competency document the practitioner will be able to: Discuss the indications for
Chapter 2 Triage. Introduction. The Trauma Team
 Chapter 2 Triage Chapter 2 Triage Introduction Existing trauma courses focus on a vertical or horizontal approach to the ABCDE assessment of an injured patient: A - Airway B - Breathing C - Circulation
Chapter 2 Triage Chapter 2 Triage Introduction Existing trauma courses focus on a vertical or horizontal approach to the ABCDE assessment of an injured patient: A - Airway B - Breathing C - Circulation
Ryota Sato 1,2*, Akira Kuriyama 3, Rei Takaesu 4, Nobuhiro Miyamae 5, Wataru Iwanaga 1, Hayato Tokuda 6 and Takehiro Umemura 4
 Sato et al. Critical Care (2018) 22:103 https://doi.org/10.1186/s13054-018-2032-y RESEARCH Open Access Resuscitative endovascular balloon occlusion of the aorta performed by emergency physicians for traumatic
Sato et al. Critical Care (2018) 22:103 https://doi.org/10.1186/s13054-018-2032-y RESEARCH Open Access Resuscitative endovascular balloon occlusion of the aorta performed by emergency physicians for traumatic
Sussex Trauma Network Guidelines for: The Management of Compartment Syndrome
 Sussex Trauma Network Guidelines for: The Management of Compartment Syndrome Management of Compartment Syndrome Control Page Version: 1 Category number: Approved by: Date approved: Name of author: and
Sussex Trauma Network Guidelines for: The Management of Compartment Syndrome Management of Compartment Syndrome Control Page Version: 1 Category number: Approved by: Date approved: Name of author: and
Management of Bleeding Pelvic Fractures
 Management of Bleeding Pelvic Fractures Clay Cothren Burlew, MD FACS Professor of Surgery Program Director, SCC and TACS Fellowships Director, Surgical Intensive Care Unit Denver Health Medical Center/University
Management of Bleeding Pelvic Fractures Clay Cothren Burlew, MD FACS Professor of Surgery Program Director, SCC and TACS Fellowships Director, Surgical Intensive Care Unit Denver Health Medical Center/University
Algorithms for managing the common trauma patient
 ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
Patient Information Booklet
 Patient Information Booklet Endovascular Stent Grafts: A Treatment for Thoracic Aortic Aneurysms Table of Contents Table of Contents Introduction 1 Anatomy of the Thoracic Aorta 2 What Is an Aneurysm?
Patient Information Booklet Endovascular Stent Grafts: A Treatment for Thoracic Aortic Aneurysms Table of Contents Table of Contents Introduction 1 Anatomy of the Thoracic Aorta 2 What Is an Aneurysm?
Sussex Trauma Network Guidelines for: Interventional Radiology in Trauma
 Sussex Trauma Network Guidelines for: Interventional Radiology in Trauma Interventional Radiology in trauma Control Page Version: 1 Category number: Approved by: Date approved: Name of author: and Name
Sussex Trauma Network Guidelines for: Interventional Radiology in Trauma Interventional Radiology in trauma Control Page Version: 1 Category number: Approved by: Date approved: Name of author: and Name
Acutely Ischaemic Arm Spoke Sites (RWHT + WMH)
 Ward In patients/medical ward Acutely Ischaemic Arm Spoke Sites (RWHT + WMH) Sudden onset of painful, pale and cold arm. Worrying features: -loss of sensation In patients/medical ward On call surgical
Ward In patients/medical ward Acutely Ischaemic Arm Spoke Sites (RWHT + WMH) Sudden onset of painful, pale and cold arm. Worrying features: -loss of sensation In patients/medical ward On call surgical
Intro: Slide 1. Slide 2. Slide 3. Basic understanding of interventional radiology. Gain knowledge of key terms and phrases
 Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
National Hospital for Neurology and Neurosurgery
 National Hospital for Neurology and Neurosurgery Venous sinus stents (for the treatment of venous sinus stenosis and idiopathic intracranial hypertension) Lysholm Department of Neuroradiology If you would
National Hospital for Neurology and Neurosurgery Venous sinus stents (for the treatment of venous sinus stenosis and idiopathic intracranial hypertension) Lysholm Department of Neuroradiology If you would
Damage Control in Abdominal and Pelvic Injuries
 Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
RCH Trauma Guideline. Management of Traumatic Pneumothorax & Haemothorax. Trauma Service, Division of Surgery
 RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
Emergency endovascular repair of ruptured abdominal aortic aneurysms - our experience
 Emergency endovascular repair of ruptured abdominal aortic aneurysms - our experience Poster No.: C-0837 Congress: ECR 2011 Type: Scientific Paper Authors: D. Kuhelj, M. Baraga, P. Popovi#, T. Klju#evšek,
Emergency endovascular repair of ruptured abdominal aortic aneurysms - our experience Poster No.: C-0837 Congress: ECR 2011 Type: Scientific Paper Authors: D. Kuhelj, M. Baraga, P. Popovi#, T. Klju#evšek,
Joint Working Group to produce guidance on delivering an Endovascular Aneurysm Repair (EVAR) Service.
 Joint Working Group to produce guidance on delivering an Endovascular Aneurysm Repair (EVAR) Service. Royal College of Radiologists British Society of Interventional Radiology The Vascular Society of Great
Joint Working Group to produce guidance on delivering an Endovascular Aneurysm Repair (EVAR) Service. Royal College of Radiologists British Society of Interventional Radiology The Vascular Society of Great
The complications associated with Resuscitative Endovascular Balloon Occlusion of the Aorta (REBOA)
 Ribeiro Junior et al. World Journal of Emergency Surgery (2018) 13:20 https://doi.org/10.1186/s13017-018-0181-6 REVIEW The complications associated with Resuscitative Endovascular Balloon Occlusion of
Ribeiro Junior et al. World Journal of Emergency Surgery (2018) 13:20 https://doi.org/10.1186/s13017-018-0181-6 REVIEW The complications associated with Resuscitative Endovascular Balloon Occlusion of
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Flow-diverting stents (in the Treatment of intracranial aneurysms)
 National Hospital for Neurology and Neurosurgery Flow-diverting stents (in the Treatment of intracranial aneurysms) Lysholm Department of Neuroradiology If you would like this document in another language
National Hospital for Neurology and Neurosurgery Flow-diverting stents (in the Treatment of intracranial aneurysms) Lysholm Department of Neuroradiology If you would like this document in another language
What is an aneurysm? Arteries carry blood away from your heart to the rest of your body. An aneurysm occurs when the walls of an artery weaken.
 Endovascular aneurysm repair (EVAR) This leaflet aims to answer some of the questions you may have about having an endovascular aneurysm repair. It explains the benefits, risks and alternatives of the
Endovascular aneurysm repair (EVAR) This leaflet aims to answer some of the questions you may have about having an endovascular aneurysm repair. It explains the benefits, risks and alternatives of the
Angiogram, angioplasty and stenting
 Angiogram, angioplasty and stenting Who is this leaflet for? This leaflet is for people who are having: an angiogram angioplasty (with or without a stent) An angiogram (also called an arteriogram or angiography)
Angiogram, angioplasty and stenting Who is this leaflet for? This leaflet is for people who are having: an angiogram angioplasty (with or without a stent) An angiogram (also called an arteriogram or angiography)
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Percutaneous coronary intervention (angioplasty) +/- rotablation
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Why do I need this procedure? If you are coming into hospital for a cardiac procedure
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Why do I need this procedure? If you are coming into hospital for a cardiac procedure
Endovascular Control of Pelvic Hemorrhage: Concomitant use of REBOA. and Endovascular Intervention ACCEPTED
 Journal of Trauma and Acute Care Surgery, Publish Ahead of Print DOI: 10.1097/TA.0000000000002079 Endovascular Control of Pelvic Hemorrhage: Concomitant use of REBOA and Endovascular Intervention Sakib
Journal of Trauma and Acute Care Surgery, Publish Ahead of Print DOI: 10.1097/TA.0000000000002079 Endovascular Control of Pelvic Hemorrhage: Concomitant use of REBOA and Endovascular Intervention Sakib
Transcatheter Aortic Valve Implantation Procedure (TAVI)
 Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Maternal Collapse Guideline
 Maternal Collapse Guideline Guideline Number: 664 Supersedes: Classification Clinical Version No: Date of EqIA: Approved by: Date Approved: Date made active: Review Date: 1 Obstetric Written Documentation
Maternal Collapse Guideline Guideline Number: 664 Supersedes: Classification Clinical Version No: Date of EqIA: Approved by: Date Approved: Date made active: Review Date: 1 Obstetric Written Documentation
INL No. A0075 Project Medtronic Patient Information Leaflet Description 16 page booklet
 INL No. A0075 Project Medtronic Patient Information Leaflet Description 16 page booklet www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular stent grafts: A treatment for Abdominal Aortic Aneurysms
INL No. A0075 Project Medtronic Patient Information Leaflet Description 16 page booklet www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular stent grafts: A treatment for Abdominal Aortic Aneurysms
Your Angiogram/ Angioplasty and Stenting
 Your Angiogram/ Angioplasty and Stenting Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Your Angiogram/ Angioplasty and Stenting Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
The SPIDER-Graft for Thoracoabdominal Aortic Repair a feasability study in pigs
 The SPIDER-Graft for Thoracoabdominal Aortic Repair a feasability study in pigs Wipper S, Kölbel T, Manzoni D, Duprée A, Sandhu H, Nelis V, Debus ES University Heart Center Hamburg University Heart Center
The SPIDER-Graft for Thoracoabdominal Aortic Repair a feasability study in pigs Wipper S, Kölbel T, Manzoni D, Duprée A, Sandhu H, Nelis V, Debus ES University Heart Center Hamburg University Heart Center
Thoracic aortic trauma A.T.O.ABDOOL-CARRIM ACADEMIC HEAD VASCULAR SURGERY DEPARTMENT OF SURGERY UNIVERSITY OF WITWATERSRAND
 Thoracic aortic trauma A.T.O.ABDOOL-CARRIM ACADEMIC HEAD VASCULAR SURGERY DEPARTMENT OF SURGERY UNIVERSITY OF WITWATERSRAND Thoracic Aortic Trauma In USA and CANADA 7500-8000 die of blunt thoracic aortic
Thoracic aortic trauma A.T.O.ABDOOL-CARRIM ACADEMIC HEAD VASCULAR SURGERY DEPARTMENT OF SURGERY UNIVERSITY OF WITWATERSRAND Thoracic Aortic Trauma In USA and CANADA 7500-8000 die of blunt thoracic aortic
ER-REBOA Patient Selection, the Procedure, and Outcomes Joseph Ibrahim, MD FACS Trauma Medical Director Orlando Regional Medical Center
 ER-REBOA Patient Selection, the Procedure, and Outcomes Joseph Ibrahim, MD FACS Trauma Medical Director Orlando Regional Medical Center Disclosures Speaking Consultant with Prytime Medical Outline Mechanism
ER-REBOA Patient Selection, the Procedure, and Outcomes Joseph Ibrahim, MD FACS Trauma Medical Director Orlando Regional Medical Center Disclosures Speaking Consultant with Prytime Medical Outline Mechanism
account for 10% to 15% of all traffic fatalities majority fatal at the scene 50% who survive the initial injury die in the first 24 hours 90% die
 account for 10% to 15% of all traffic fatalities majority fatal at the scene 50% who survive the initial injury die in the first 24 hours 90% die within the first month if aorta not repaired 30-90% overall
account for 10% to 15% of all traffic fatalities majority fatal at the scene 50% who survive the initial injury die in the first 24 hours 90% die within the first month if aorta not repaired 30-90% overall
Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP)
 Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
Oral and Maxillofacial Surgeons and the seriously injured patient. Barts and The London NHS Trust
 Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Stuck dialysis catheters. ANZSIN 2013 Michael Lam & Kendal Redmond
 Stuck dialysis catheters ANZSIN 2013 Michael Lam & Kendal Redmond NT 39 yr old CI Maori - ESKD 2 o to cortical necrosis HD August 2002 R IJ tunneled Tesio catheter Oct 2002 Failed L RC AVF Feb 2004 Failed
Stuck dialysis catheters ANZSIN 2013 Michael Lam & Kendal Redmond NT 39 yr old CI Maori - ESKD 2 o to cortical necrosis HD August 2002 R IJ tunneled Tesio catheter Oct 2002 Failed L RC AVF Feb 2004 Failed
Abdominal Aortic Aneurysm - Part 1. Learning Objectives. Disclosure. University of Toronto Division of Vascular Surgery
 University of Toronto Division of Vascular Surgery Abdominal Aortic Aneurysm - Part 1 Dr Mark Wheatcroft & Dr Elisa Greco Vascular Surgeon, St Michael s Hospital, Toronto & University of Toronto Disclosure
University of Toronto Division of Vascular Surgery Abdominal Aortic Aneurysm - Part 1 Dr Mark Wheatcroft & Dr Elisa Greco Vascular Surgeon, St Michael s Hospital, Toronto & University of Toronto Disclosure
10. Severe traumatic brain injury also see flow chart Appendix 5
 10. Severe traumatic brain injury also see flow chart Appendix 5 Introduction Severe traumatic brain injury (TBI) is the leading cause of death in children in the UK, accounting for 15% of deaths in 1-15
10. Severe traumatic brain injury also see flow chart Appendix 5 Introduction Severe traumatic brain injury (TBI) is the leading cause of death in children in the UK, accounting for 15% of deaths in 1-15
TEVAR for trauma is here to stay: Advances in the Treatment of Blunt Thoracic Aortic Injury
 TEVAR for trauma is here to stay: Advances in the Treatment of Blunt Thoracic Aortic Injury Megan Brenner MD MS RPVI FACS Associate Professor of Surgery Division of Trauma/Surgical Critical Care, RA Cowley
TEVAR for trauma is here to stay: Advances in the Treatment of Blunt Thoracic Aortic Injury Megan Brenner MD MS RPVI FACS Associate Professor of Surgery Division of Trauma/Surgical Critical Care, RA Cowley
10/2/2018. Acute Management of Pelvic Injuries. Learning Objectives. 17 yo male ped struck by truck
 17 yo male ped struck by truck Acute Management of Pelvic Injuries David Volgas, MD CoxHealth University of Missouri HD unstable Open pelvic wound superior gluteal fold through rectum to scrotum Open rami
17 yo male ped struck by truck Acute Management of Pelvic Injuries David Volgas, MD CoxHealth University of Missouri HD unstable Open pelvic wound superior gluteal fold through rectum to scrotum Open rami
Gunshot Wounds to the Abdomen: From Bullet to Incision. Patrick M Reilly MD FACS
 Gunshot Wounds to the Abdomen: From Bullet to Incision Patrick M Reilly MD FACS Master? I Do Get The Chance to Practice What Are We Not Discussing? Stab Wounds Prehospital Care Management of Specific Injuries
Gunshot Wounds to the Abdomen: From Bullet to Incision Patrick M Reilly MD FACS Master? I Do Get The Chance to Practice What Are We Not Discussing? Stab Wounds Prehospital Care Management of Specific Injuries
GUIDELINE FOR RECOVERY ROOM MANAGEMENT OF PATIENTS AFTER CAROTID ENDARTERECTOMY
 GUIDELINE FOR RECOVERY ROOM MANAGEMENT OF PATIENTS AFTER CAROTID ENDARTERECTOMY Full Title of Guideline: Author (include email and role): Guideline for Recovery Room Management of Patients after Carotid
GUIDELINE FOR RECOVERY ROOM MANAGEMENT OF PATIENTS AFTER CAROTID ENDARTERECTOMY Full Title of Guideline: Author (include email and role): Guideline for Recovery Room Management of Patients after Carotid
National Vascular Registry
 National Vascular Registry AAA Repair Patient Details Patient Consent* 0 No 1 Yes 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s)
National Vascular Registry AAA Repair Patient Details Patient Consent* 0 No 1 Yes 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s)
Trauma. Neck trauma zones. Neck Injuries 1/3/2018. Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure
 Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Clinical Module. Pelvic Injury Trauma. Princess Alexandra Hospital Emergency Department. 1 Introduction
 Princess Alexandra Hospital Emergency Department Clinical Module Trauma Review Officers: Katherine Isoardi / Glenn Ryan Version no: 2 Review date: Aug 2015 Key Words: Pelvic Trauma, Pelvic Injury, Pelvic
Princess Alexandra Hospital Emergency Department Clinical Module Trauma Review Officers: Katherine Isoardi / Glenn Ryan Version no: 2 Review date: Aug 2015 Key Words: Pelvic Trauma, Pelvic Injury, Pelvic
National Emergency Laparotomy Audit. Help Box Text
 National Emergency Laparotomy Audit Help Box Text Version Control Version 1.1 06/12/13 1.2 13/12/13 1.3 20/12/13 1.4 20/01/14 1.5 30/01/14 1.6 13/03/14 1.7 07/04/14 1.8 01/12/14 1.9 05/05/15 1.10 02/07/15
National Emergency Laparotomy Audit Help Box Text Version Control Version 1.1 06/12/13 1.2 13/12/13 1.3 20/12/13 1.4 20/01/14 1.5 30/01/14 1.6 13/03/14 1.7 07/04/14 1.8 01/12/14 1.9 05/05/15 1.10 02/07/15
Neurological Complications of TEVAR. Frank J Criado, MD. Union Memorial-MedStar Health Baltimore, MD USA
 ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
Acute arterial embolism
 Acute arterial embolism Definition Thrombus come from heart or blood vessel or other embolus such as tumor,air gas or fat flow with blood stream and occlude distal limb or visceral arteries which causes
Acute arterial embolism Definition Thrombus come from heart or blood vessel or other embolus such as tumor,air gas or fat flow with blood stream and occlude distal limb or visceral arteries which causes
Paravertebral policy. The Acute pain Management Dept, UCLH
 UCLH PARAVERTEBRAL BLOCK (ADULTS) POLICY Paravertebral policy. The Acute pain Management Dept, UCLH DEFINITION A Paravertebral block is a method of providing effective analgesia using a local anaesthetic.
UCLH PARAVERTEBRAL BLOCK (ADULTS) POLICY Paravertebral policy. The Acute pain Management Dept, UCLH DEFINITION A Paravertebral block is a method of providing effective analgesia using a local anaesthetic.
Renal angioplasty (including transplant kidneys) and stent insertion
 Renal angioplasty (including transplant kidneys) and stent insertion UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Renal angioplasty (including transplant kidneys) and stent insertion UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Overview
 Overview Tutorial Script 1 Script for the Virtual Stroke Lab Tutorial Overview http://www.ilstu.edu Background and Vocabulary This podcast provides an overview of The Virtual Stroke Lab, a free virtual
Overview Tutorial Script 1 Script for the Virtual Stroke Lab Tutorial Overview http://www.ilstu.edu Background and Vocabulary This podcast provides an overview of The Virtual Stroke Lab, a free virtual
General Imaging. Imaging modalities. Incremental CT. Multislice CT Multislice CT [ MDCT ]
![General Imaging. Imaging modalities. Incremental CT. Multislice CT Multislice CT [ MDCT ] General Imaging. Imaging modalities. Incremental CT. Multislice CT Multislice CT [ MDCT ]](/thumbs/76/74079340.jpg) General Imaging Imaging modalities Conventional X-rays Ultrasonography [ US ] Computed tomography [ CT ] Radionuclide imaging Magnetic resonance imaging [ MRI ] Angiography conventional, CT,MRI Interventional
General Imaging Imaging modalities Conventional X-rays Ultrasonography [ US ] Computed tomography [ CT ] Radionuclide imaging Magnetic resonance imaging [ MRI ] Angiography conventional, CT,MRI Interventional
ACUTE CLINICAL MANAGEMENT OF TRAUMA Tina Gaarder, MD, PhD
 ACUTE CLINICAL MANAGEMENT OF TRAUMA Tina Gaarder, MD, PhD Trauma represents a leading cause of disability and preventable death and is mainly affecting people between 15 and 40 years of age, accounting
ACUTE CLINICAL MANAGEMENT OF TRAUMA Tina Gaarder, MD, PhD Trauma represents a leading cause of disability and preventable death and is mainly affecting people between 15 and 40 years of age, accounting
CLINICAL GUIDELINES ID TAG
 Title: Author: Speciality/ Division: Directorate: Date Uploaded: Review Date: September 2019 CG ID TAG CG0423 CLINICAL GUIDELINES ID TAG Clinical Guideline for Alteplase in intra-arterial thrombolysis
Title: Author: Speciality/ Division: Directorate: Date Uploaded: Review Date: September 2019 CG ID TAG CG0423 CLINICAL GUIDELINES ID TAG Clinical Guideline for Alteplase in intra-arterial thrombolysis
Major Haemorrhage Transfusion Pathway
 Major Haemorrhage Transfusion Pathway SENIOR CLINICIAN ASSESSMENT: DECLARES MAJOR HAEMORRHAGE ( Call for help ( Telephone via switchboard: Consultant or Senior Clinician Duty Anaesthetist Porters (if will
Major Haemorrhage Transfusion Pathway SENIOR CLINICIAN ASSESSMENT: DECLARES MAJOR HAEMORRHAGE ( Call for help ( Telephone via switchboard: Consultant or Senior Clinician Duty Anaesthetist Porters (if will
Abdominal Aortic Aneurysm 가천대길병원 이상준
 Abdominal Aortic Aneurysm 가천대길병원 이상준 1 Definition Diameter of the aorta 1.5 times greater than normal. Most are infrarenal, and a significant number extend down into one or both iliac arteries Abdominal
Abdominal Aortic Aneurysm 가천대길병원 이상준 1 Definition Diameter of the aorta 1.5 times greater than normal. Most are infrarenal, and a significant number extend down into one or both iliac arteries Abdominal
Open Repair of RAAA is always possible -is it always better? No disclosures!! Lazar B. Davidovic MD, PhD, FETCS
 Open Repair of RAAA is always possible -is it always better? Lazar B. Davidovic MD, PhD, FETCS Professor of Surgery School of Medicine, University of Belgrade Head of the Clinic for Vascular and Endovascular
Open Repair of RAAA is always possible -is it always better? Lazar B. Davidovic MD, PhD, FETCS Professor of Surgery School of Medicine, University of Belgrade Head of the Clinic for Vascular and Endovascular
Open repair of Abdominal Aortic Aneurysms (AAA)
 Open repair of Abdominal Aortic Aneurysms (AAA) Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us
Open repair of Abdominal Aortic Aneurysms (AAA) Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us
Ancillary Components with Z-Trak Introduction System
 Ancillary Components with Z-Trak Introduction System Zenith Flex AAA Endovascular Graft Ancillary Components Converter Converters can be used to convert a bifurcated graft into an aortouniiliac graft if
Ancillary Components with Z-Trak Introduction System Zenith Flex AAA Endovascular Graft Ancillary Components Converter Converters can be used to convert a bifurcated graft into an aortouniiliac graft if
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies. Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018
 Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
ANGIOPLASTY AND STENTING
 ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection
 Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Introduction What Causes Peripheral Vascular Disease? How Do Doctors Treat Peripheral Vascular Disease?... 9
 Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
CPT 2018 Radiology Code Changes
 CPT 2018 Radiology Code Changes CPT 2018 Radiology Code Changes The following is a listing of new Current Procedural Terminology (CPT ) codes and their descriptors as described in the CPT 2018 codebook.
CPT 2018 Radiology Code Changes CPT 2018 Radiology Code Changes The following is a listing of new Current Procedural Terminology (CPT ) codes and their descriptors as described in the CPT 2018 codebook.
Interventional Options in Management of Placenta Abnormalities
 Interventional Options in Management of Placenta Abnormalities Caroline Clausen and Lars Lönn Department of Cardiovascular Radiology Faculty of Health Sciences Copenhagen University Rigshospitalet, Denmark.
Interventional Options in Management of Placenta Abnormalities Caroline Clausen and Lars Lönn Department of Cardiovascular Radiology Faculty of Health Sciences Copenhagen University Rigshospitalet, Denmark.
THE CARE AND MAINTENANCE OF TOTALLY IMPLANTED VENOUS ACCESS DEVICES (PORTS)
 Children s Hospital for Wales Department of Paediatric Respiratory Medicine and Cystic Fibrosis THE CARE AND MAINTENANCE OF TOTALLY IMPLANTED VENOUS ACCESS DEVICES (PORTS) This protocol applies to the
Children s Hospital for Wales Department of Paediatric Respiratory Medicine and Cystic Fibrosis THE CARE AND MAINTENANCE OF TOTALLY IMPLANTED VENOUS ACCESS DEVICES (PORTS) This protocol applies to the
ER REBOA Catheter. Instructions for Use
 ER REBOA Catheter Instructions for Use Prytime Medical Devices, Inc. 229 N. Main Street Boerne, TX 78006, USA feedback@prytimemedical.com www.prytimemedical.com US 1 210 340 0116 U.S. and Foreign Patents
ER REBOA Catheter Instructions for Use Prytime Medical Devices, Inc. 229 N. Main Street Boerne, TX 78006, USA feedback@prytimemedical.com www.prytimemedical.com US 1 210 340 0116 U.S. and Foreign Patents
Traumatic Cardiac Arrest Protocol
 Traumatic Cardiac Arrest Protocol Background: Major Trauma continues to be the leading worldwide cause of death in young adults. Mortality remains high but there are reports of good neurological outcomes
Traumatic Cardiac Arrest Protocol Background: Major Trauma continues to be the leading worldwide cause of death in young adults. Mortality remains high but there are reports of good neurological outcomes
The Leeds Teaching Hospitals NHS Trust Catheter directed thrombolysis and pelvic venous stenting for ilio-femoral DVT
 n The Leeds Teaching Hospitals NHS Trust Catheter directed thrombolysis and pelvic venous stenting for ilio-femoral DVT Information for patients Catheter directed thrombolysis and pelvic venous stenting
n The Leeds Teaching Hospitals NHS Trust Catheter directed thrombolysis and pelvic venous stenting for ilio-femoral DVT Information for patients Catheter directed thrombolysis and pelvic venous stenting
Cheltenham General Hospital
 Page 1 of 5 Coronary angioplasty Introduction This leaflet provides information for patients undergoing coronary angioplasty also known as PCI (Percutaneous Coronary Intervention). What is coronary artery
Page 1 of 5 Coronary angioplasty Introduction This leaflet provides information for patients undergoing coronary angioplasty also known as PCI (Percutaneous Coronary Intervention). What is coronary artery
Diagnosis & Management of Kidney Trauma. LAU - Urology Residency Program LOP Urology Residents Meeting
 Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
