Indications for Permanent Pacing Joe Gallinghouse, M.D. Texas Cardiac Arrhythmia Austin, Texas
|
|
|
- Jane Jones
- 5 years ago
- Views:
Transcription
1 Indications for Permanent Pacing Joe Gallinghouse, M.D. Texas Cardiac Arrhythmia Austin, Texas Remember the Suture!
2 Impulse Formation and Conduction Disturbances Cardiac Electrical Anatomy Sinoatrial Node
3 Cardiac Electrical Anatomy Atrioventricular Node Cardiac Electrical Anatomy Bundle of HIS
4 Cardiac Electrical Anatomy Left Bundle Branch (LBB) Posterior Fascicle of LBB Anterior Fascicle of LBB Right Bundle Branch (RBB) Symptoms- Bradyarrhythmia Syncope or pre-syncope Dizziness Congestive heart failure Mental confusion Palpitations Shortness of breath Exercise intolerance
5 Case Example 86 yo female with no prior history of cardiac disease, presents with syncope Eating lunch, fell into soup Past Med Hx: HTN, DJD Meds: ACE I Admitted to telemetry 12 lead EKG unremarkable Echo Efx 65%, moderate MR, LA 5.5 cm Telemetry Strip
6 Sinus Node Recovery Time (SNRT) Sinus Node Dysfunction Sinus bradycardia Sinus arrest SA block Brady-tachy syndrome Chronotropic incompetence
7 Sinus Node Dysfunction Sinus Bradycardia Persistent slow rate from the SA node. The parameters from this waveform include: - Rate = 45 bpm - PR interval = 180 ms (.18 seconds) Sinus Node Dysfunction Sinus Arrest 2.8-second arrest Failure of sinus node discharge resulting in the absence of atrial depolarization and periods of ventricular asystole - Rate = 75 bpm - PR interval = 180 ms (.18 seconds) second arrest
8 Sinus Node Dysfunction SA Exit Block 2.1-second pause Transient blockage of impulses from the SA node - Rate = 52 bpm - PR interval = 180 ms (.18 seconds) second pause Sinus Node Dysfunction Bradycardia-Tachycardia (Brady-Tachy) Syndrome Intermittent episodes of slow and fast rates from the SA node or atria - Rate during bradycardia = 43 bpm - Rate during tachycardia = 130 bpm
9 Chronotropic Incompetence Max Heart Rate Slow Unstable Quick Rest Start Activity Time Stop Activity ACC/AHA Classification of Indications Class I Conditions for which there is evidence and/or general agreement that a given procedure or treatment is beneficial, useful, and effective. Class II Conditions for which there is conflicting evidence and/or a divergence of opinion about the usefulness/efficacy of a procedure or treatment. - Class IIa: Weight of evidence/opinion is in favor of usefulness/efficacy. - Class IIb: Usefulness/efficacy is less well established by evidence/opinion.
10 ACC/AHA Classification of Indications Class III Conditions for which there is evidence and/or general agreement that a procedure or treatment is not useful/effective and in some cases may be harmful. ACC/AHA Classification of Clinical Evidence Evidence supporting current recommendations are ranked as levels A, B, and C: - Level A: Data derived from multiple randomized clinical trials involving a large number of individuals. - Level B: Data derived from a limited number of trials involving comparatively small numbers of patients or from well-designed data analysis of nonrandomized studies or observational data registries. - Level C: Consensus of expert opinion was the primary source of recommendation.
11 Pacing in Sinus Node Dysfunction Class I Indications 1. Sinus node dysfunction with documented symptomatic bradycardia, including frequent sinus pauses that produce symptoms. - May be a consequence of essential long-term drug therapy for which there is no alternative. 2. Symptomatic chronotropic incompetence. Pacing in Sinus Node Dysfunction Class IIa Indications 1. Sinus node dysfunction with heart rate <40 bpm, developing either spontaneously or as a result of necessary drug therapy, when a clear association between significant symptoms consistent with bradycardia and the actual presence of bradycardia has not been documented. 2. Syncope of unexplained origin when major abnormalities of sinus node function are discovered or provoked in EP studies.
12 Pacing in Sinus Node Dysfunction Class IIb Indications 1. In minimally symptomatic patients, chronic heart rates <40 bpm, while awake. Pacing in Sinus Node Dysfunction Class III Indications 1. Sinus node dysfunction in asymptomatic patients including those in whom substantial bradycardia (heart rate <40 bpm) is a result of long-term drug treatment. 2. Sinus node dysfunction in patients in whom symptoms suggestive of bradycardia are clearly documented not to be associated with a slow heart rate. 3. Sinus node dysfunction with symptomatic bradycardia due to nonessential drug therapy.
13 Case Example 67 yo male with hx HTN, moderate aortic stenosis Presents with complaint of DOE Meds: ASA, HCTZ Presenting 12 Lead EKG
14 Case Example Carotid Massage results in transient restoration of 1:1 conduction Echo unchanged from previously- Efx 60%, moderate AS AV Block First-degree AV block Second-degree AV block - Mobitz types I and II Third-degree AV block Bifascicular and trifascicular block
15 First-Degree AV Block 340 ms AV conduction is delayed, and the PR interval is prolonged (>200 ms or.2 seconds) - Rate = 79 bpm - PR interval = 340 ms (.34 seconds) Second-Degree AV Block Mobitz I (Wenckebach) ms ms ms No QRS Progressive prolongation of the PR interval until a ventricular beat is dropped - Ventricular rate = irregular - Atrial rate = 90 bpm - PR interval = progressively longer until a P-wave fails to conduct
16 Second-Degree AV Block Mobitz II P P QRS Regularly dropped ventricular beats - 2:1 block (2 P waves to 1 QRS complex) - Ventricular rate = 60 bpm - Atrial rate = 110 bpm Third-Degree AV Block No impulse conduction from the atria to the ventricles - Ventricular rate = 37 bpm - Atrial rate = 130 bpm - PR interval = variable
17 Pacing for Acquired AV Block Class I Indications 1. Third-degree and advanced second degree AV block at any anatomic level with: a) Bradycardia and symptoms (including heart failure) presumed due to AV block, b) Arrhythmias and other medical conditions requiring drugs that result in symptomatic bradycardia, c) Documented asystole >3.0 sec. or escape rate <40 bpm in awake, symptom-free patients, d) Post AV junction ablation. Pacing for Acquired AV Block Class I Indications 1. Third-degree and advanced second degree AV block at any anatomic level with (continued): e) Postoperative AV block not expected to resolve after cardiac surgery, f) Neuromuscular diseases with AV block, with or without symptoms. 2. Second-degree AV block regardless of type or site of block, with associated symptomatic bradycardia.
18 Pacing for Acquired AV Block Class IIa Indications 1. Asymptomatic third-degree AV block at any anatomic site with average, awake ventricular rate >40 bpm, especially if cardiomegaly or LV dysfunction is present. 2. Asymptomatic type II second-degree AV block with a narrow QRS. 3. Asymptomatic type I second-degree AV block at intraor infra-his levels at EP study. 4. First or second degree AV block with symptoms similar to pacemaker syndrome. Pacing for Acquired AV Block Class IIb Indications 1. Marked first-degree AV block (>0.30 sec.) in patients with LV dysfunction and CHF in whom a shorter AV interval results in hemodynamic improvement, presumably by left atrial filling pressure. 2. Neuromuscular diseases with any degree of AV block (including first degree AV block), with or without symptoms.
19 Pacing for Acquired AV Block Class III Indications 1. Asymptomatic first-degree AV block. 2. Asymptomatic type I second-degree AV block at the supra-his level. 3. AV block expected to resolve and unlikely to recur (e.g., drug toxicity, Lyme disease, etc), or during hypoxia in sleep apnea syndrome in absence of symptoms. No Ventricular Capture
20 Case Example 43 yo female with hx sarcoidosis Presents to ER with syncopal event while walking to mailbox Facial trauma 3 months prior: Echo Efx 55%, no significant valvular dz Presenting 12 Lead EKG
21 Finding at EPS Bifascicular Block Right bundle branch block and left posterior hemiblock
22 Bifascicular Block Right bundle branch block and left anterior hemiblock Bifascicular Block Complete left bundle branch block
23 Trifascicular Block Complete block in the right bundle branch and complete or incomplete block in both divisions of the left bundle branch Pacing for Chronic Bifascicular and Trifascicular Block Class I Indications 1. Intermittent third-degree AV block. 2. Type II second-degree AV block. 3. Alternating bundle-branch block.
24 Pacing for Chronic Bifascicular and Trifascicular Block Class IIa Indications 1. Syncope not demonstrated to be due to AV block when other likely causes have been excluded, specifically ventricular tachycardia. 2. Incidental finding at EP study of markedly prolonged HV interval (>100 ms) in asymptomatic patients. 3. Incidental finding at EP study of pacing-induced infra-his block that is not physiological. Pacing for Chronic Bifascicular and Trifascicular Block Class IIb Indications 1. Neuromuscular diseases..with any degree of fascicular block with or without symptoms, because there may be unpredictable progression of AV conduction disease.
25 Pacing for Chronic Bifascicular and Trifascicular Block Class III Indications 1. Fascicular block without AV block or symptoms. 2. Fascicular block with first-degree AV block without symptoms. Case Example 72 yo male develops recurrent near syncope Always seems to occur while dressing for church on Sundays No prior cardiac hx On no meds
26 Case Example EEG, CT/MRI head normal Echo: Efx 55%, mild AI Stress perfusion study normal Carotid Sinus Massage
27 Neurocardiogenic Syncope Carotid Sinus Syndrome (CSS/CSH) Vasovagal Syncope (VVS) Mechanisms of Neurocardiogenic Syncope Cardioinhibitory - Initiated by inappropriate drop in heart rate Vasodepressor - Symptomatic decrease in systolic blood pressure due to vasodilation Mixed - Includes components of cardioinhibitory and vasodepressor
28 Hypersensitive Carotid Sinus Syndrome (CSS) Extreme reflex response to carotid sinus stimulation Results in bradycardia and/or vasodilation Can be induced by: - Tight collar - Shaving - Head turning - Exercise - Other activities that stimulate the carotid sinus Vasovagal Syncope (VVS) Neurally mediated transient loss of consciousness Can be precipitated by: - Fear, anxiety - Physical pain or anticipation of trauma/pain - Prolonged standing Symptoms include: - Dizziness - Blurred vision - Weakness - Nausea, abdominal discomfort - Sweating
29 Vasovagal Syncope Pacing in CSS and VVS Class I Indications 1. Recurrent syncope caused by carotid sinus stimulation; minimal carotid sinus pressure induces ventricular asystole >3 sec duration in absence of any medication that depresses the sinus node or AV conduction.
30 Pacing in CSS and VVS Class IIa Indications 1. Recurrent syncope without clear, provocative events and with a hypersensitive cardioinhibitory response. 2. Significantly symptomatic and recurrent neurocardiogenic syncope associated with bradycardia documented spontaneously or at the time of tilt-table testing. NOTE: There are No Class IIb Indications. The Role of Pacing as Therapy for Vasovagal Syncope VVS with +HUT and cardioinhibitory response: Class IIa indication for pacing Three randomized, prospective trials reported benefits of pacing in select VVS patients: - VPS I 1 - VASIS 2 - SYDIT 3 Subsequent study results less clear - VPS II 4 - Synpace 5 - INVASY 6 2 Sutton R. Circulation. 2000;102: Ammirati F. Circ. 2001;104: Connolly SJ. J Am Coll Cardiol. 1999;33: Connolly S. JAMA. 2003;289: Giada F. PACE. 2003;26:1016 (abstract). 6 Occhetta E, et al. Europace. 2004;6:
31 Role of Pacing as Therapy for Vasovagal Syncope: Summary Three earlier studies single blind Bias? Pacemaker implantation may modulate reflex syncope and autonomic responses 1 Study results may differ based on pre-implant selection criteria and tilt-testing techniques Pacing therapy is effective in some but not all (cardioinhibition vs. vasodepression) In five pacing studies, syncope recurred in 33/156 (21%) of paced patients, 72/162 (44%) in non-paced patients (p<0.001) 2 1 Kapoor W. JAMA. 2003;289: Brignole M, et al.. Europace. 2004;6: Pacing for CSS and VVS Class III Indications 1. Hyperactive cardioinhibitory response to CS stimulation in absence of symptoms or in the presence of vague symptoms such as dizziness, lightheadedness, or both. 2. Recurrent syncope, lightheadedness or dizziness in absence of hyperactive cardioinhibitory response. 3. Situational vasovagal syncope in which avoidance behavior is effective.
32 Other Indications Other Indications 1. Pacing for AV Block Associated with Acute MI 2. Pacing after Cardiac Transplantation 3. Pacing in Children, Adolescents, and Patients with Congenital Heart Disease 4. Pacing for Hypertrophic Obstructive Cardiomyopathy 5. Pacing for Idiopathic Dilated Cardiomyopathy 6. Prevention and Termination of Tachyarrhythmias by Pacing 1. Pacemakers that Automatically Detect and Pace to Terminate Tachycardias 2. Pacing Recommendations to Prevent Tachycardia
33 Pacing for AV Block Associated with Acute Myocardial Infarction Class I Indications 1. Persistent second-degree AV block in the His- Purkinje system with bilateral BBB or third-degree AV block within or below the His-Purkinje system. 2. Transient, advanced (second- or third-degree) infranodal AV block and associated BBB. If the site of the block is uncertain, an EP study may be necessary. 3. Persistent and symptomatic second- or third-degree AV block. Pacing for AV Block Associated with Acute Myocardial Infarction Class IIa and IIb Indications Class IIa: None Class IIb: 1. Persistent second- or third-degree AV block at the AV node level.
34 Pacing for AV Block Associated with Acute Myocardial Infarction Class III Indications 1. Transient AV block in absence of intraventricular conduction defects. 2. Transient AV block in presence of isolated left anterior fascicular block (LAFB). 3. Acquired LAFB in absence of AV block. 4. Persistent first-degree AV block in presence of BBB that is old or age indeterminate. Pacing After Cardiac Transplantation Class I-III I III Indications Class I: 1. Symptomatic bradyarrhythmias/chronotropic incompetence not expected to resolve and other Class I indications for permanent pacing. Class IIa: None Class IIb: 1. Symptomatic bradyarrhythmias/chronotropic incompetence that, although transient, may persist for months and require intervention. Class III: 1. Postoperative asymptomatic bradyarrhythmias.
35 Pacing in Children, Adolescents, and Patients with Congenital Heart Disease Class I Indications 1. Advanced second- or third-degree AV block associated with symptomatic bradycardia, ventricular dysfunction or low cardiac output. 2. Sinus node dysfunction with correlation of symptoms during age-inappropriate bradycardia. 3. Postoperative advanced second- or third-degree AV block not expected to resolve, or persists >7 days after cardiac surgery. Pacing in Children, Adolescents, and Patients with Congenital Heart Disease Class I Indications 4. Congenital third-degree AV block with a wide QRS escape rhythm, complex ventricular ectopy, or ventricular dysfunction. 5. Congenital third-degree AV block in the infant with a ventricular rate <50-55 bpm or with congenital heart disease and a ventricular rate <70 bpm. 6. Sustained pause-dependent VT, with or without prolonged QT, in which the efficacy of pacing is thoroughly documented.
36 Pacing in Children, Adolescents, and Patients with Congenital Heart Disease Class IIa Indications 1. Brady-tachy syndrome with the need for chronic antiarrhythmic treatment other than digitalis. 2. Congenital third-degree AV block, beyond the first year of life, with an average heart rate <50 bpm, or abrupt pauses in the ventricular rate which are 2x or 3x the basic cycle length or associated with symptoms due to chronotropic incompetence. Pacing in Children, Adolescents, and Patients with Congenital Heart Disease Class IIa Indications 3. Long QT syndrome with 2:1 AV or third-degree AV block. 4. Asymptomatic sinus bradycardia in child with complex congenital heart disease where the resting heart rate is <40 bpm or >3 sec. pauses occur in the ventricular rate. 5. Patients with congenital heart disease and impaired hemodynamics due to sinus bradycardia or loss of AV synchrony.
37 Pacing in Children, Adolescents, and Patients with Congenital Heart Disease Class IIb Indications 1. Transient postoperative third-degree AV block that reverts to sinus rhythm with residual bifascicular block. 2. Congenital third-degree AV block in asymptomatic infant, child, adolescent or young adult with an acceptable rate, narrow QRS complex, and normal ventricular function. Pacing in Children, Adolescents, and Patients with Congenital Heart Disease Class IIb Indications 3. Asymptomatic sinus bradycardia in adolescents with congenital heart disease with resting heart rate <40 bpm or >3 second pauses in the ventricular rate. 4. Neuromuscular diseases with any degree of AV block (including first-degree AV block), with or without symptoms, because there may be unpredictable progression of AV conduction disease.
38 Pacing in Children, Adolescents, and Patients with Congenital Heart Disease Class III Indications 1. Transient postoperative AV block with return of normal AV conduction. 2. Asymptomatic postoperative bifascicular block with or without first-degree AV block. 3. Asymptomatic type I second-degree AV block. 4. Asymptomatic sinus bradycardia in adolescent where the longest RR interval is <3 sec and the minimum heart rate is >40 bpm. Pacing for Hypertrophic Obstructive Cardiomyopathy Class I, IIa and IIb Indications Class I: 1. Class I indications for sinus node dysfunction or AV block as previously described. Class IIa: None Class IIb: 1. Medically refractory, symptomatic hypertrophic cardiomyopathy with significant resting or provoked LV outflow obstruction..
39 Pacing for Hypertrophic Obstructive Cardiomyopathy Class III Indications 1. Patients who are asymptomatic or medically controlled. 2. Symptomatic patients without evidence of LV outflow obstruction. Pacing for Idiopathic Dilated Cardiomyopathy Class I, IIa and IIb Indications Class I: 1. Class I indications for sinus node dysfunction or AV block as previously described. Class IIa: 1. Biventricular pacing in medically refractory, symptomatic NYHA Class III/IV patients with idiopathic dilated or ischemic cardiomyopathy, prolonged QRS interval (>130 msec), LV enddiastolic diameter >55mm, and LVEF <35%. Class IIb: None
40 Pacing for Idiopathic Dilated Cardiomyopathy Class III Indications 1. Asymptomatic dilated cardiomyopathy. 2. Symptomatic dilated cardiomyopathy when patients are rendered asymptomatic by drug therapy. 3. Symptomatic ischemic cardiomyopathy when the ischemia is amenable to intervention.
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc.
 Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
Sincopi ricorrenti: diagnosi differenziale e management. Alessandro Proclemer SOC Cardiologia Az. Osp.-Univ. Udine
 Sincopi ricorrenti: diagnosi differenziale e management Alessandro Proclemer SOC Cardiologia Az. Osp.-Univ. Udine DISCLOSURE INFORMATION Dr. Alessandro Proclemer negli ultimi due anni ho avuto i seguenti
Sincopi ricorrenti: diagnosi differenziale e management Alessandro Proclemer SOC Cardiologia Az. Osp.-Univ. Udine DISCLOSURE INFORMATION Dr. Alessandro Proclemer negli ultimi due anni ho avuto i seguenti
Death after Syncope: Can we predict it? Daniel Zamarripa, MD Senior Medical Director December 2013
 Death after Syncope: Can we predict it? Daniel Zamarripa, MD Senior Medical Director December 2013 Death after Syncope: Can we predict it? Those who suffer from frequent and severe fainting often die suddenly
Death after Syncope: Can we predict it? Daniel Zamarripa, MD Senior Medical Director December 2013 Death after Syncope: Can we predict it? Those who suffer from frequent and severe fainting often die suddenly
Use of Cardiac Pacemakers and Antiarrythmia Devices: ACC/AHA Guidelines Summary
 A/AHA ardiology Guideline Summaries Volume 101 Number 101 raunwald: Heart Disease: A Textbook of ardiovascular Medicine, 6e. Use of ardiac Pacemakers and Antiarrythmia Devices: A/AHA Guidelines Summary
A/AHA ardiology Guideline Summaries Volume 101 Number 101 raunwald: Heart Disease: A Textbook of ardiovascular Medicine, 6e. Use of ardiac Pacemakers and Antiarrythmia Devices: A/AHA Guidelines Summary
Vasovagal Syncope and Bradyarrhythmias Mechanisms, distinguishing cause and effect
 Vasovagal Syncope and Bradyarrhythmias Mechanisms, distinguishing cause and effect Walid Saliba, MD, FHRS, FACC Director EP lab Director Atrial Fibrillation Center Department of Cardiovascular Medicine
Vasovagal Syncope and Bradyarrhythmias Mechanisms, distinguishing cause and effect Walid Saliba, MD, FHRS, FACC Director EP lab Director Atrial Fibrillation Center Department of Cardiovascular Medicine
National Coverage Determination (NCD) for Cardiac Pacemakers (20.8)
 Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
The ECG Course. Boone County Fire Protection District EMS Education
 The ECG Course Level I G rated material AV Blocks What Causes AV Block? Long list of bad things that includes ischemia and.. Old age / disease Medications or drugs Electrolyte imbalances Physiologic Blocks
The ECG Course Level I G rated material AV Blocks What Causes AV Block? Long list of bad things that includes ischemia and.. Old age / disease Medications or drugs Electrolyte imbalances Physiologic Blocks
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE. Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology
 PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
Arrhythmic Complications of MI. Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine
 Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
13/09/2018. The ISSUE Studies. International (Italy & Spain) Study of Syncope of Uncertain Etiology. ISSUE study Pre-defined inclusion cathegories
 The Studies Jean-Claude Deharo Aix-Marseille Université, France In Cardiac Electrophysiology Methods and Models Editors: Daniel C. Sigg, Paul A. Iaizzo, Yong-Fu Xiao, Bin He Springer 2010 study Pre-defined
The Studies Jean-Claude Deharo Aix-Marseille Université, France In Cardiac Electrophysiology Methods and Models Editors: Daniel C. Sigg, Paul A. Iaizzo, Yong-Fu Xiao, Bin He Springer 2010 study Pre-defined
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC
 Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
Syncope: Evaluation of the Weak and Dizzy
 Syncope: Evaluation of the Weak and Dizzy William M. Miles, MD, FACC, FHRS Professor of Medicine Silverstein Chair for Cardiovascular Education University of Florida College of Medicine Disclosures Medtronic,
Syncope: Evaluation of the Weak and Dizzy William M. Miles, MD, FACC, FHRS Professor of Medicine Silverstein Chair for Cardiovascular Education University of Florida College of Medicine Disclosures Medtronic,
Syncope: Evaluation of the Weak and Dizzy
 Syncope: Evaluation of the Weak and Dizzy William M. Miles, MD, FACC, FHRS Professor of Medicine Silverstein Chair for Cardiovascular Education University of Florida College of Medicine Disclosures Medtronic,
Syncope: Evaluation of the Weak and Dizzy William M. Miles, MD, FACC, FHRS Professor of Medicine Silverstein Chair for Cardiovascular Education University of Florida College of Medicine Disclosures Medtronic,
Conduction disorders
 Conduction disorders L.V. Bogun, N.I. Yabluchansky, F.M. Abdueva, O.Y. Bichkova, A.N. Fomich, P.A. Garkavyi, A.L. Kulik, N.V. Lysenko, N.V. Makienko, L.A. Martimyanova, I.V. Soldatenko, E.E. Tomina Department
Conduction disorders L.V. Bogun, N.I. Yabluchansky, F.M. Abdueva, O.Y. Bichkova, A.N. Fomich, P.A. Garkavyi, A.L. Kulik, N.V. Lysenko, N.V. Makienko, L.A. Martimyanova, I.V. Soldatenko, E.E. Tomina Department
Step by step approach to EKG rhythm interpretation:
 Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Bundle Branch & Fascicular Blocks. Reading Assignment (p53-58 in Outline )
 Bundle Branch & Fascicular Blocks Reading Assignment (p53-58 in Outline ) Objectives 1. QRS analysis of Right and Left BBB 2. Uncomplicated vs complicated BBB 3. Diagnosis of RBBB with LAFB and LPFB 4.
Bundle Branch & Fascicular Blocks Reading Assignment (p53-58 in Outline ) Objectives 1. QRS analysis of Right and Left BBB 2. Uncomplicated vs complicated BBB 3. Diagnosis of RBBB with LAFB and LPFB 4.
Syncope By Remus Popa
 Syncope By Remus Popa A 66 years old male is brought to the ED from a restaurant where he fainted while dining out with his family. He complained of nausea and stood up to go to the restroom but immediately
Syncope By Remus Popa A 66 years old male is brought to the ED from a restaurant where he fainted while dining out with his family. He complained of nausea and stood up to go to the restroom but immediately
ECG Interpretation Cat Williams, DVM DACVIM (Cardiology)
 ECG Interpretation Cat Williams, DVM DACVIM (Cardiology) Providing the best quality care and service for the patient, the client, and the referring veterinarian. GOAL: Reduce Anxiety about ECGs Back to
ECG Interpretation Cat Williams, DVM DACVIM (Cardiology) Providing the best quality care and service for the patient, the client, and the referring veterinarian. GOAL: Reduce Anxiety about ECGs Back to
Syncope Update Dr Matthew Lovell, Consultant in Cardiology
 Syncope Update Dr Matthew Lovell, Consultant in Cardiology Definition of Syncope Syncope is defined as TLOC due to cerebral hypoperfusion Characterized by a rapid onset, short duration, and spontaneous
Syncope Update Dr Matthew Lovell, Consultant in Cardiology Definition of Syncope Syncope is defined as TLOC due to cerebral hypoperfusion Characterized by a rapid onset, short duration, and spontaneous
La strategia diagnostica: il monitoraggio ecg prolungato. Michele Brignole
 La strategia diagnostica: il monitoraggio ecg prolungato Michele Brignole ECG monitoring and syncope In-hospital monitoring Holter Monitoring External loop recorder Remote (at home) telemetry Implantable
La strategia diagnostica: il monitoraggio ecg prolungato Michele Brignole ECG monitoring and syncope In-hospital monitoring Holter Monitoring External loop recorder Remote (at home) telemetry Implantable
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
Conduction Problems / Arrhythmias. Conduction
 Conduction Problems / Arrhythmias Conduction Wolf-Parkinson White Syndrome (WPW) and Lown-Ganong-Levine (LGL): Atrial impulses bypass the AV node through an accessory pathway or bypass tract (bundle of
Conduction Problems / Arrhythmias Conduction Wolf-Parkinson White Syndrome (WPW) and Lown-Ganong-Levine (LGL): Atrial impulses bypass the AV node through an accessory pathway or bypass tract (bundle of
Dr. Schroeder has no financial relationships to disclose
 Valerie A Schroeder MD MS Assistant Professor University of Kansas Medical Center READING THE WAVES- THE HEART S ELECTRICAL MESSAGE FINANCIAL DISCLOSURE Dr. Schroeder has no financial relationships to
Valerie A Schroeder MD MS Assistant Professor University of Kansas Medical Center READING THE WAVES- THE HEART S ELECTRICAL MESSAGE FINANCIAL DISCLOSURE Dr. Schroeder has no financial relationships to
Pennsylvania Academy of Family Physicians Foundation & UPMC 43rd Refresher Course in Family Medicine CME Conference March 10-13, 2016
 Pennsylvania Academy of Family Physicians Foundation & UPMC 43rd Refresher Course in Family Medicine CME Conference March 10-13, 2016 Disclosures: EKG Workshop Louis Mancano, MD Speaker has no disclosures
Pennsylvania Academy of Family Physicians Foundation & UPMC 43rd Refresher Course in Family Medicine CME Conference March 10-13, 2016 Disclosures: EKG Workshop Louis Mancano, MD Speaker has no disclosures
Electrocardiography Abnormalities (Arrhythmias) 7. Faisal I. Mohammed, MD, PhD
 Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
MANAGEMENT OF ASYMPTOMATIC BRADYCARDIA. Pr. HABIB HAOUALA Service de Cardiologie Hôpital militaire de Tunis
 MANAGEMENT OF ASYMPTOMATIC BRADYCARDIA Pr. HABIB HAOUALA Service de Cardiologie Hôpital militaire de Tunis DISCLOSURE STATEMENT OF FINANCIAL INTEREST Grant/research: Medtronic;Sanofi; Novartis Consulting
MANAGEMENT OF ASYMPTOMATIC BRADYCARDIA Pr. HABIB HAOUALA Service de Cardiologie Hôpital militaire de Tunis DISCLOSURE STATEMENT OF FINANCIAL INTEREST Grant/research: Medtronic;Sanofi; Novartis Consulting
Junctional Premature Contraction (JPC)
 Where s the PAC? Junctional Premature Contraction (JPC) A junctional premature contraction (JPC) is a beat that originates prematurely in the AV node. It can occur sporadically or in a grouped pattern.
Where s the PAC? Junctional Premature Contraction (JPC) A junctional premature contraction (JPC) is a beat that originates prematurely in the AV node. It can occur sporadically or in a grouped pattern.
CRC 431 ECG Basics. Bill Pruitt, MBA, RRT, CPFT, AE-C
 CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
Practice Guideline: Executive Summary
 Practice Guideline: Executive Summary Practice Guideline: Executive Summary ACC/AHA/HRS 2008 Guidelines for Device-Based Therapy of Cardiac Rhythm Abnormalities: Executive Summary A Report of the American
Practice Guideline: Executive Summary Practice Guideline: Executive Summary ACC/AHA/HRS 2008 Guidelines for Device-Based Therapy of Cardiac Rhythm Abnormalities: Executive Summary A Report of the American
Value of the implantable loop recorder for the management of patients with unexplained syncope
 Europace (2004) 6, 70e76 Value of the implantable loop recorder for the management of patients with unexplained syncope Lucas Boersma a, ), Lluís Mont b, Alessandro Sionis b, Emilio García b, Josep Brugada
Europace (2004) 6, 70e76 Value of the implantable loop recorder for the management of patients with unexplained syncope Lucas Boersma a, ), Lluís Mont b, Alessandro Sionis b, Emilio García b, Josep Brugada
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
Revisions to the BC Guide for Physicians in Determining Fitness to Drive a Motor Vehicle
 Revisions to the BC Guide for Physicians in Determining Fitness to Drive a Motor Vehicle Thank you for taking the time to review the draft Cardiovascular Diseases and Disorders chapter. Please provide
Revisions to the BC Guide for Physicians in Determining Fitness to Drive a Motor Vehicle Thank you for taking the time to review the draft Cardiovascular Diseases and Disorders chapter. Please provide
Bradydysrhythmias and Atrioventricular Conduction Blocks
 Emerg Med Clin N Am 24 (2006) 1 9 Bradydysrhythmias and Atrioventricular Conduction Blocks Jacob W. Ufberg, MD*, Jennifer S. Clark, MD Department of Emergency Medicine, Temple University School of Medicine,
Emerg Med Clin N Am 24 (2006) 1 9 Bradydysrhythmias and Atrioventricular Conduction Blocks Jacob W. Ufberg, MD*, Jennifer S. Clark, MD Department of Emergency Medicine, Temple University School of Medicine,
Cardiac arrhythmias. Janusz Witowski. Department of Pathophysiology Poznan University of Medical Sciences. J. Witowski
 Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
The current update of the ACC/AHA/NASPE Guidelines
 ACC/AHA/NASPE Practice Guidelines ACC/AHA/NASPE 2002 Guideline Update for Implantation of Cardiac Pacemakers and Antiarrhythmia Devices: Summary Article A Report of the American College of Cardiology/American
ACC/AHA/NASPE Practice Guidelines ACC/AHA/NASPE 2002 Guideline Update for Implantation of Cardiac Pacemakers and Antiarrhythmia Devices: Summary Article A Report of the American College of Cardiology/American
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs
 EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Ασυμπτωματικός ασθενής με διαταραχές αγωγής. Πρόγνωση θεραπεία
 Ασυμπτωματικός ασθενής με διαταραχές αγωγής. Πρόγνωση θεραπεία Dr Ηλίας Θ. Ζάρβαλης Καρδιολόγος Επιμελητής Α Καρδιολογική Κλινική Γ. Ν. Παπαγεωργίου Θεσσαλονίκη 1899 he provided a description of irregular
Ασυμπτωματικός ασθενής με διαταραχές αγωγής. Πρόγνωση θεραπεία Dr Ηλίας Θ. Ζάρβαλης Καρδιολόγος Επιμελητής Α Καρδιολογική Κλινική Γ. Ν. Παπαγεωργίου Θεσσαλονίκη 1899 he provided a description of irregular
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists
 PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
CORONARY ARTERIES. LAD Anterior wall of the left vent Lateral wall of left vent Anterior 2/3 of interventricluar septum R & L bundle branches
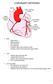 CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
HTEC 91. Performing ECGs: Procedure. Normal Sinus Rhythm (NSR) Topic for Today: Sinus Rhythms. Characteristics of NSR. Conduction Pathway
 HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
EKG Competency for Agency
 EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
ECG S: A CASE-BASED APPROACH December 6,
 ECG S: A CASE-BASED APPROACH December 6, 2018 1 Faculty Disclosure Faculty: Lorne Gula MD, FRCPC Professor, Western University Cardiologist, Hearth Rhythm Specialist Director, Electrophysiology Laboratory,
ECG S: A CASE-BASED APPROACH December 6, 2018 1 Faculty Disclosure Faculty: Lorne Gula MD, FRCPC Professor, Western University Cardiologist, Hearth Rhythm Specialist Director, Electrophysiology Laboratory,
Sequoia Heart Symposium 2018: Syncope. Gregory Engel, MD
 Sequoia Heart Symposium 2018: Syncope Gregory Engel, MD Silicon Valley Cardiology Palo Alto Medical Foundation Sutter Health Palo Alto, Redwood City, and San Carlos, CA Chief, Cardiovascular Division Sequoia
Sequoia Heart Symposium 2018: Syncope Gregory Engel, MD Silicon Valley Cardiology Palo Alto Medical Foundation Sutter Health Palo Alto, Redwood City, and San Carlos, CA Chief, Cardiovascular Division Sequoia
ACC/AHA Guidelines for Ambulatory Electrocardiography: Executive Summary and Recommendations
 (Circulation. 1999;100:886-893.) 1999 American Heart Association, Inc. ACC/AHA Practice Guidelines ACC/AHA Guidelines for Ambulatory Electrocardiography: Executive Summary and Recommendations A Report
(Circulation. 1999;100:886-893.) 1999 American Heart Association, Inc. ACC/AHA Practice Guidelines ACC/AHA Guidelines for Ambulatory Electrocardiography: Executive Summary and Recommendations A Report
How To Think About Rhythms and Conduction
 How To Think About Rhythms and Conduction Frank Yanowitz, MD Professor of Medicine (Cardiology) University of Utah School of Medicine Medical Director, IHC ECG Services Intermountain Healthcare http://ecg.utah.edu
How To Think About Rhythms and Conduction Frank Yanowitz, MD Professor of Medicine (Cardiology) University of Utah School of Medicine Medical Director, IHC ECG Services Intermountain Healthcare http://ecg.utah.edu
Bradyarrhythmias are frequently
 Bradyarrhythmias, temporary and permanent pacing Vineet Kaushik, MD; Angel R. Leon, MD; James S. Forrester Jr, MD; Richard G. Trohman, MD Bradycardia is common in critical care units. It may be transient,
Bradyarrhythmias, temporary and permanent pacing Vineet Kaushik, MD; Angel R. Leon, MD; James S. Forrester Jr, MD; Richard G. Trohman, MD Bradycardia is common in critical care units. It may be transient,
Blocks & Dissociations. Reading Assignment (p47-52 in Outline )
 Blocks & Dissociations Reading Assignment (p47-52 in Outline ) Objectives Who are Wenckebach and Mobitz? Review SA and AV Blocks AV Dissociations: learning who s the boss and why 2 nd degree SA Block:
Blocks & Dissociations Reading Assignment (p47-52 in Outline ) Objectives Who are Wenckebach and Mobitz? Review SA and AV Blocks AV Dissociations: learning who s the boss and why 2 nd degree SA Block:
TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT
 Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Remote Monitoring & the Smart Home of the 21 Century
 Cardiostim EHRA Europace 2016, Nice - June 8-11, 2016 Remote Monitoring & the Smart Home of the 21 Century Antonio Raviele, MD, FESC, FHRS President ALFA -Alliance to Fight Atrial fibrillation- Venezia
Cardiostim EHRA Europace 2016, Nice - June 8-11, 2016 Remote Monitoring & the Smart Home of the 21 Century Antonio Raviele, MD, FESC, FHRS President ALFA -Alliance to Fight Atrial fibrillation- Venezia
Recurrent Implantable Defibrillator Discharges (ICD) Discharges ICD Storm
 Recurrent Implantable Defibrillator Discharges (ICD) Discharges ICD Storm Guy Amit, MD, MPH Soroka University Medical Center Ben-Gurion University of the Negev Beer-Sheva, Israel Disclosures Consultant:
Recurrent Implantable Defibrillator Discharges (ICD) Discharges ICD Storm Guy Amit, MD, MPH Soroka University Medical Center Ben-Gurion University of the Negev Beer-Sheva, Israel Disclosures Consultant:
Practice Questions.
 IBHRE Prep Practice Questions Question 1 The relative refractory yperiod of the ventricular myocardium corresponds to which of the following phases of the action potential? A. (0) B. (1) C. (2) D. (3)
IBHRE Prep Practice Questions Question 1 The relative refractory yperiod of the ventricular myocardium corresponds to which of the following phases of the action potential? A. (0) B. (1) C. (2) D. (3)
Syncope Guidelines Update. Bernard Harbieh, FHRS AUBMC-KMC Beirut-Lebanon
 Syncope Guidelines Update Bernard Harbieh, FHRS AUBMC-KMC Beirut-Lebanon New Syncope Guidelines Increase the volume of information on diagnosis and management Incorporation of emergency specialists, neurologists,
Syncope Guidelines Update Bernard Harbieh, FHRS AUBMC-KMC Beirut-Lebanon New Syncope Guidelines Increase the volume of information on diagnosis and management Incorporation of emergency specialists, neurologists,
Valutazione iniziale e stratificazione del rischio
 Valutazione iniziale e stratificazione del rischio Paolo Alboni Sezione di Cardiologia Ospedale Privato Quisisana Ferrara DEFINITION OF SYNCOPE Syncope is a transient loss of consciousness due to global
Valutazione iniziale e stratificazione del rischio Paolo Alboni Sezione di Cardiologia Ospedale Privato Quisisana Ferrara DEFINITION OF SYNCOPE Syncope is a transient loss of consciousness due to global
Northwest Community Healthcare Paramedic Education Program AV Conduction Defects/AV Blocks Connie J. Mattera, M.S., R.N., EMT-P
 Northwest Community Healthcare Paramedic Education Program AV Conduction Defects/ Connie J. Mattera, M.S., R.N., EMT-P Reading assignments: Bledsoe Vol. 3: pp. 88-93; 120-121 (atropine, norepinephrine,
Northwest Community Healthcare Paramedic Education Program AV Conduction Defects/ Connie J. Mattera, M.S., R.N., EMT-P Reading assignments: Bledsoe Vol. 3: pp. 88-93; 120-121 (atropine, norepinephrine,
Clinical Case 1 A patient with a syncope Panos E. Vardas President Elect of the ESC, Prof of Cardiology, University Hospital of Crete
 Clinical Case 1 A patient with a syncope Panos E. Vardas President Elect of the ESC, Prof. of Cardiology, University Hospital of Crete Case presentation A 64-year-old male smoker, with arterial hypertension
Clinical Case 1 A patient with a syncope Panos E. Vardas President Elect of the ESC, Prof. of Cardiology, University Hospital of Crete Case presentation A 64-year-old male smoker, with arterial hypertension
KNOW YOUR ECG. G. Somasekhar MD DM FEp Consultant Electro physiologist, Aayush Hospital, Vijayawada
 KNOW YOUR ECG G. Somasekhar MD DM FEp Consultant Electro physiologist, Aayush Hospital, Vijayawada CASE DETAILS A 48-year-old female non hypertensive, non diabetic presented with history of shortness of
KNOW YOUR ECG G. Somasekhar MD DM FEp Consultant Electro physiologist, Aayush Hospital, Vijayawada CASE DETAILS A 48-year-old female non hypertensive, non diabetic presented with history of shortness of
InterQual Care Planning SIM plus Criteria 2014 Clinical Revisions
 InterQual Care Planning SIM plus Criteria 2014 Clinical Revisions The Clinical Revisions provide details of changes to InterQual Clinical Criteria. They do not provide information on changes made to CareEnhance
InterQual Care Planning SIM plus Criteria 2014 Clinical Revisions The Clinical Revisions provide details of changes to InterQual Clinical Criteria. They do not provide information on changes made to CareEnhance
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Adenosine in idiopathic AV block, 445 446 Adolescent(s) syncope in, 397 409. See also Syncope, in children and adolescents AECG monitoring.
Index Note: Page numbers of article titles are in boldface type. A Adenosine in idiopathic AV block, 445 446 Adolescent(s) syncope in, 397 409. See also Syncope, in children and adolescents AECG monitoring.
REtrive. REpeat. RElearn Design by. Test-Enhanced Learning based ECG practice E-book
 Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
December 2018 Tracings
 Tracings Tracing 1 Tracing 4 Tracing 1 Answer Tracing 4 Answer Tracing 2 Tracing 5 Tracing 2 Answer Tracing 5 Answer Tracing 3 Tracing 6 Tracing 3 Answer Tracing 6 Answer Questions? Contact Dr. Nelson
Tracings Tracing 1 Tracing 4 Tracing 1 Answer Tracing 4 Answer Tracing 2 Tracing 5 Tracing 2 Answer Tracing 5 Answer Tracing 3 Tracing 6 Tracing 3 Answer Tracing 6 Answer Questions? Contact Dr. Nelson
Supplementary Online Content
 Supplementary Online Content Tseng ZH, Hayward RM, Clark NM, et al. Sudden death in patients with cardiac implantable electronic devices. JAMA Intern Med. Published online June 22, 2015. doi:10.1001/jamainternmed.2015.2641.
Supplementary Online Content Tseng ZH, Hayward RM, Clark NM, et al. Sudden death in patients with cardiac implantable electronic devices. JAMA Intern Med. Published online June 22, 2015. doi:10.1001/jamainternmed.2015.2641.
SIMPLY ECGs. Dr William Dooley
 SIMPLY ECGs Dr William Dooley Content Basic ECG interpretation pattern Some common (examined) abnormalities Presenting ECGs in context Setting up an ECG Setting up an ECG 1 V1-4 th Right intercostal space
SIMPLY ECGs Dr William Dooley Content Basic ECG interpretation pattern Some common (examined) abnormalities Presenting ECGs in context Setting up an ECG Setting up an ECG 1 V1-4 th Right intercostal space
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif
 2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
ECG Basics Sonia Samtani 7/2017 UCI Resident Lecture Series
 ECG Basics Sonia Samtani 7/2017 UCI Resident Lecture Series Agenda I. Introduction II.The Conduction System III.ECG Basics IV.Cardiac Emergencies V.Summary The Conduction System Lead Placement avf Precordial
ECG Basics Sonia Samtani 7/2017 UCI Resident Lecture Series Agenda I. Introduction II.The Conduction System III.ECG Basics IV.Cardiac Emergencies V.Summary The Conduction System Lead Placement avf Precordial
Cardiac Telemetry Self Study: Part One Cardiovascular Review 2017 THINGS TO REMEMBER
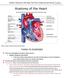 Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
2018 ESC SYNCOPE GUIDELINES SUMMARY
 208 ESC SYNCOPE GUIDELINES SUMMARY NEW GUIDELINES OVERVIEW OF UPDATED RECOMMENDATIONS SINCE 2009 208 EUROPEAN SOCIETY OF CARDIOLOGY SYNCOPE GUIDELINES Goals of 208 Task Force Reducing Cost & Admissions:
208 ESC SYNCOPE GUIDELINES SUMMARY NEW GUIDELINES OVERVIEW OF UPDATED RECOMMENDATIONS SINCE 2009 208 EUROPEAN SOCIETY OF CARDIOLOGY SYNCOPE GUIDELINES Goals of 208 Task Force Reducing Cost & Admissions:
Improving Patient Outcomes with a Syncope Center. Suneet Mittal, MD
 Improving Patient Outcomes with a Syncope Center Suneet Mittal, MD Improving Patient Outcomes with a Syncope Center: Early Risk Stratification of Patients who Require Device Therapy Suneet Mittal, MD Director,
Improving Patient Outcomes with a Syncope Center Suneet Mittal, MD Improving Patient Outcomes with a Syncope Center: Early Risk Stratification of Patients who Require Device Therapy Suneet Mittal, MD Director,
Appendix D Output Code and Interpretation of Analysis
 Appendix D Output Code and Interpretation of Analysis 8 Arrhythmia Code No. Description 8002 Marked rhythm irregularity 8110 Sinus rhythm 8102 Sinus arrhythmia 8108 Marked sinus arrhythmia 8120 Sinus tachycardia
Appendix D Output Code and Interpretation of Analysis 8 Arrhythmia Code No. Description 8002 Marked rhythm irregularity 8110 Sinus rhythm 8102 Sinus arrhythmia 8108 Marked sinus arrhythmia 8120 Sinus tachycardia
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 5: Rhythm Strip Interpretation and Sinus Rhythms Learning Outcomes 5.1 Explain the process of evaluating ECG tracings
Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 5: Rhythm Strip Interpretation and Sinus Rhythms Learning Outcomes 5.1 Explain the process of evaluating ECG tracings
Diploma in Electrocardiography
 The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
Cardiac Event Monitors
 Last Review Date: July 14, 2017 Number: MG.MM.DM.18aCv2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: July 14, 2017 Number: MG.MM.DM.18aCv2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
12-Lead ECG Interpretation. Kathy Kuznar, RN, ANP
 12-Lead ECG Interpretation Kathy Kuznar, RN, ANP The 12-Lead ECG Objectives Identify the normal morphology and features of the 12- lead ECG. Perform systematic analysis of the 12-lead ECG. Recognize abnormalities
12-Lead ECG Interpretation Kathy Kuznar, RN, ANP The 12-Lead ECG Objectives Identify the normal morphology and features of the 12- lead ECG. Perform systematic analysis of the 12-lead ECG. Recognize abnormalities
Figure 2. Normal ECG tracing. Table 1.
 Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
SIMPLY ECGs. Dr William Dooley
 SIMPLY ECGs Dr William Dooley 1 No anatomy just interpretation 2 Setting up an ECG 3 Setting up an ECG 1 V1-4 th Right intercostal space at sternal border 2 V2-4 th Left intercostal space at sternal border
SIMPLY ECGs Dr William Dooley 1 No anatomy just interpretation 2 Setting up an ECG 3 Setting up an ECG 1 V1-4 th Right intercostal space at sternal border 2 V2-4 th Left intercostal space at sternal border
Return to Basics. ECG Rate and Rhythm. Management of the Hospitalized Patient October 4, 2007
 Management of the Hospitalized Patient October 4, 2007 ECG Refresher for the Hospitalists Return to Basics Determine rate and rhythm Determine intervals and axes Define morphology of P-QRS-T-U Compare
Management of the Hospitalized Patient October 4, 2007 ECG Refresher for the Hospitalists Return to Basics Determine rate and rhythm Determine intervals and axes Define morphology of P-QRS-T-U Compare
Bradyarrhythmias: How SSSSSLOW is Too Slow?
 Bradyarrhythmias: How SSSSSLOW is Too Slow? Daniel H. Cooper, MD Assistant Professor, Division of Cardiology, Department of Medicine, Washington University School of Medicine Clinical Cardiac Electrophysiologist
Bradyarrhythmias: How SSSSSLOW is Too Slow? Daniel H. Cooper, MD Assistant Professor, Division of Cardiology, Department of Medicine, Washington University School of Medicine Clinical Cardiac Electrophysiologist
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation
 The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Return to Basics. ECG Rate and Rhythm. Management of the Hospitalized Patient September 25, 2009
 Management of the Hospitalized Patient September 25, 2009 ECG Refresher and Update 2009 Return to Basics Determine rate and rhythm Determine intervals and axes Define morphology of P-QRS-T-U Compare with
Management of the Hospitalized Patient September 25, 2009 ECG Refresher and Update 2009 Return to Basics Determine rate and rhythm Determine intervals and axes Define morphology of P-QRS-T-U Compare with
Return to Basics. Normal Intervals & Axes. ECG Rate and Rhythm
 Return to Basics Management of the Hospitalized Patient October 15, 2010 ECG Refresher and Update 2010 Determine rate and rhythm Determine intervals and axes Define morphology of P-QRS-T-U Compare with
Return to Basics Management of the Hospitalized Patient October 15, 2010 ECG Refresher and Update 2010 Determine rate and rhythm Determine intervals and axes Define morphology of P-QRS-T-U Compare with
Reading Assignment (p1-91 in Outline ) Objectives What s in an ECG?
 Reading Assignment (p1-91 in Outline ) Objectives What s in an ECG? The 5-Step Method ECG #: Mearurements: Rhythm (s): Conduction: Waveform: Interpretation: A= V= PR= QRS= QT= Axis= 1. Compute the 5 basic
Reading Assignment (p1-91 in Outline ) Objectives What s in an ECG? The 5-Step Method ECG #: Mearurements: Rhythm (s): Conduction: Waveform: Interpretation: A= V= PR= QRS= QT= Axis= 1. Compute the 5 basic
HR: 50 bpm (Sinus) PR: 280 ms QRS: 120 ms QT: 490 ms Axis: -70. Sinus bradycardia with one ventricular escape (*)
 1? HR: 50 bpm (Sinus) PR: 280 ms QRS: 120 ms QT: 490 ms Axis: -70 1 Sinus P waves? 2 sinus cycles The pause (2 sinus cycles) suggests that the sinus fired (?) but did not conduct to the atria (i.e., missing
1? HR: 50 bpm (Sinus) PR: 280 ms QRS: 120 ms QT: 490 ms Axis: -70 1 Sinus P waves? 2 sinus cycles The pause (2 sinus cycles) suggests that the sinus fired (?) but did not conduct to the atria (i.e., missing
An Approach to the Patient with Syncope. Guy Amit MD, MPH Soroka University Medical Center Beer-Sheva
 An Approach to the Patient with Syncope Guy Amit MD, MPH Soroka University Medical Center Beer-Sheva Case presentation A 23 y.o. man presented with 2 episodes of syncope One during exercise,one at rest
An Approach to the Patient with Syncope Guy Amit MD, MPH Soroka University Medical Center Beer-Sheva Case presentation A 23 y.o. man presented with 2 episodes of syncope One during exercise,one at rest
Cardiac Pacemakers» 2013 HOSPITAL REIMBURSEMENT GUIDE
 Cardiac Pacemakers» 2013 HOSPITAL REIMBURSEMENT GUIDE 2 Contents Page Introduction Medicare Coding and Payment Overview Hospital Inpatient Hospital Outpatient HCPCS Device Category C-Codes Coverage for
Cardiac Pacemakers» 2013 HOSPITAL REIMBURSEMENT GUIDE 2 Contents Page Introduction Medicare Coding and Payment Overview Hospital Inpatient Hospital Outpatient HCPCS Device Category C-Codes Coverage for
ESC Guidelines. ESC Guidelines Update For internal training purpose. European Heart Journal, doi: /eurheart/ehn309
 ESC Guidelines Update 2008 ESC Guidelines Heart failure update 2008 For internal training purpose. 0 Agenda Introduction Classes of recommendations Level of evidence Treatment algorithm Changes to ESC
ESC Guidelines Update 2008 ESC Guidelines Heart failure update 2008 For internal training purpose. 0 Agenda Introduction Classes of recommendations Level of evidence Treatment algorithm Changes to ESC
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
General Introduction to ECG. Reading Assignment (p2-16 in PDF Outline )
 General Introduction to ECG Reading Assignment (p2-16 in PDF Outline ) Objectives 1. Practice the 5-step Method 2. Differential Diagnosis: R & L axis deviation 3. Differential Diagnosis: Poor R-wave progression
General Introduction to ECG Reading Assignment (p2-16 in PDF Outline ) Objectives 1. Practice the 5-step Method 2. Differential Diagnosis: R & L axis deviation 3. Differential Diagnosis: Poor R-wave progression
Cardiac Arrhythmias in Sleep
 Cardiac Arrhythmias in Sleep Only 53 Slides! Gauresh H Kashyap, MD, FACP, FCCP, FAASM 1 2 Cardiac Arrhythmias in Sleep Out of 400 Patients with OSA, 48% had some Arrhythmias 20% - 2 PVCs/min 7% - Bradycardia
Cardiac Arrhythmias in Sleep Only 53 Slides! Gauresh H Kashyap, MD, FACP, FCCP, FAASM 1 2 Cardiac Arrhythmias in Sleep Out of 400 Patients with OSA, 48% had some Arrhythmias 20% - 2 PVCs/min 7% - Bradycardia
Diagnostic and therapeutic management of the patient with syncope M. Brignole Arrhythmologic Centre and Syncope Unit Lavagna, Italy
 Diagnostic and therapeutic management of the patient with syncope M. Brignole Arrhythmologic Centre and Syncope Unit Lavagna, Italy Eur Heart J. 2009 Nov;30(21):2631-71 Available on www.escardio.org/guidelines
Diagnostic and therapeutic management of the patient with syncope M. Brignole Arrhythmologic Centre and Syncope Unit Lavagna, Italy Eur Heart J. 2009 Nov;30(21):2631-71 Available on www.escardio.org/guidelines
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
2016 NIA Clinical Guidelines for Medical Necessity Review HORIZON NJ CARDIAC MANAGEMENT
 2016 for Medical Necessity Review HORIZON NJ CARDIAC MANAGEMENT 2016 Magellan Health, Inc. Proprietary Page 1 of 58 Guidelines for Clinical Review Determination Preamble NIA is committed to the philosophy
2016 for Medical Necessity Review HORIZON NJ CARDIAC MANAGEMENT 2016 Magellan Health, Inc. Proprietary Page 1 of 58 Guidelines for Clinical Review Determination Preamble NIA is committed to the philosophy
ECG interpretation basics
 ECG interpretation basics Michał Walczewski, MD Krzysztof Ozierański, MD 21.03.18 Electrical conduction system of the heart Limb leads Precordial leads 21.03.18 Precordial leads Precordial leads 21.03.18
ECG interpretation basics Michał Walczewski, MD Krzysztof Ozierański, MD 21.03.18 Electrical conduction system of the heart Limb leads Precordial leads 21.03.18 Precordial leads Precordial leads 21.03.18
Clinical Policy: Holter Monitors Reference Number: CP.MP.113
 Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
ECG Interpretation. Introduction to Cardiac Telemetry. Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services
 ECG Interpretation Introduction to Cardiac Telemetry Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services Disclosures Nothing to disclose Objectives Describe the electrical conduction pathway in
ECG Interpretation Introduction to Cardiac Telemetry Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services Disclosures Nothing to disclose Objectives Describe the electrical conduction pathway in
EKG Abnormalities. Adapted from:
 EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
Hatim Al Lawati. MD, FRCPC, DABIM(CV), FACC
 Hatim Al Lawati. MD, FRCPC, DABIM(CV), FACC Consultant Interventional Cardiology & Structural Heart Disease Department of Medicine Sultan Qaboos University Hospital hatim.al.lawati@gmail.com April 2017
Hatim Al Lawati. MD, FRCPC, DABIM(CV), FACC Consultant Interventional Cardiology & Structural Heart Disease Department of Medicine Sultan Qaboos University Hospital hatim.al.lawati@gmail.com April 2017
