posterior pituitary extract administered
|
|
|
- Jocelyn Horn
- 5 years ago
- Views:
Transcription
1 EVIDENCE IN MAN THAT URINARY ELECTROLYTE LOSS IN- DUCED BY PITRESSIN IS A FUNCTION OF WATER RETENTION' By ALEXANDER LEAF,2 FREDERIC C. BARTTER,3 ROBERTO F. SANTOS,4 AND OLIVER WRONG (From the Department of Medicine, Massachusetts General Hospital and the Harvard Medical School, Boston, Mass., and the Clinic of General Medicine and Experimental Therapeutics, National Heart Institute, Baltimore, Md.) (Submitted for publication April 21, 1953; accepted May 15, 1953) INTRODUCTION There are many conflicting reports on the acute effects of posterior pituitary extract on the renal excretion of sodium and chloride. This subject has been recently reviewed (1). The present study was made to' determine the effects on electrolyte excretion in man of a longacting posterior pituitary extract administered over a period of several days. The results suggest that the state of hydration determines the effect of pitressin on electrolyte excretion. The relationship of the findings to the problem of volume regulation of the body fluids will be considered. METHODS Metabolic studies were conducted at the Metabolism Ward of the Massachusetts General Hospital (2) and at the U. S. Public Health Service Hospital, Baltimore, Maryland. Subjects studied included four normal adults, two patients with anterior pituitary insufficiency, one with anterior and posterior pituitary insufficiency, one with adrenal cortical insufficiency, and one with ovarian agenesis. Subjects were maintained on a constant diet, and the fluid intake was controlled at various levels. No restrictions were made on the activity or position of the subjects. Dietary sodium intake was fixed in each study and ranged in different studies from 20 to 175 meq. per day. Following an initial control period of several days, posterior pituitary extract was administered intramuscu- 1 Supported by grants from the Milton Fund of Harvard University, the American Heart Association, and the Worcester Chapter of the Massachusetts Heart Association. 2Howard R. Hughes Fellow in Medicine. B Senior Surgeon, United States Public Health Service. Present address: National Heart Institute, National Institutes of Health, United States Public Health Service, Bethesda, Maryland. 4Kellogg Fellow of the American College of Physicians. Present address: Bahia, Brazil. larly as Pitressin Tannate in Oil,5 2.0 units initially, followed by 1.0 unit every 12 hours for two to four days. This dose of pitressin was estimated to be within the physiological range of endogenous antidiuretic hormone production (3, 4). Twenty separate periods of pitressin administration were studied. In all but one instance an antidiuretic effect was maintained throughout the period of hormone administration. Urine and serum were analyzed for sodium, chloride, potassium, nitrogen, and total solutes. Two studies included calcium and phosphorus determinations and stool analyses. Analytical methods used have been described in a previous communication (5). Recently, however, the saline standard solutions used in the measurement of total solute concentrations have -been corrected for activity coefficients calculated from data obtained in the Intemational Critical Tables (6). Thus, in the studies on R. S., N. W., and 0. W. i which the new standards were used, the normal level of total solute concentration of serum was found to be approximately 290 mosm. per L. rather than the previously reported value of 310 mosm. per L. Inulin and para-aminohippurate clearances (7) were used as measures of glomerular filtration rate and renal plasma flow in one subject, M. K. H. In two subjects, R. S. and 0. W., 24 hour clearances of endogenous creatinine were used as an estimate of glomerular filtration rate's (8). Acute changes in plasma volume were calculated in subjects R. S. and 0. W. from hematocrit and hemoglobin measurements (9). RESULTS A. The effects of pitressin on electrolyte excretion Figure 1 shows a typical response of a normal subject to administration of pitressin over a period 5Lots L888G or L654C were used. The Pitressin Tannate in Oil was generously supplied by Dr. A. C. Bratton, Jr., Parke, Davis and Co., Detroit 23, Michigan. 6 Although not as valid a measure of glomerular filtration rate as is the clearance of inulin, the clearance of endogenous creatinine is a useful estimate of the filtration rate over the daily period of urine collection. This avoids the fallacy of correlating the excretion of water and solutes over twenty-four hours with the clearance of inulin over a few minutes. 868
2 WATER RETENTION AND ELECTROLYTE LOSS 869 E.L ME 35 UNITS/24fR NORMAAL FEMALE /27/5I s'lt8 160 Ii 1 3E ~~~~~~~~~~~~~~~~ Lt - -] 3o0J135S" Z CONCEN\/TR _ , KE9. EQ4H A MLEQJL li KDYL~~~~~~~~~~~~~ '@''- 0 SERUM It48 N.EO/ asoi I 6l FIG.1. in t0 964S THE EFFECTS OF PSERNONK SERUM ELECTROLYTE CONCEN- 468 KEQ mosm/l 0C alyi t_ a 32 5FLEQ[./4R r. lsoo9~ ~ ~...4.LJ24HR intravenously 4.0NETO,AD CoCrRct OYWEGTO the e...te#7/ SUAVJNRMPAL SUBECT 56.0 KG ACTUAAL WEIGHT ~4. 7 S 9 10 pays t r b n-diet REFUSALs *1300CC. 3% SALINE LV. FIG. 1. THE EFFECTS OF PITRESSIN ON SERUm ELECTROLYTE CONCENTRA- TIONS, URiNARY ELECTROLYTE EXCRETION, URINARY VOLUME AND TOTAL SOLUTE CONCENTRATION, ANqD BoDY WEIGHT OF A N'ORMAL SuBjECTr The hatched columns represent total 24 hour excretions and the broken lines urinary concentrations. Note the prompt antidiuret.ic effect of pitressin but the delay in the excretion of sodium and chloride. Sodium intake was 60 meq. per day by analysis. Because of anorexia and nausea, part of the diet and fluid intake was refused on the last two- days of pitressin administration. The day after pitressin was stopped 300 ml. of 'three per cent saline were administered intravenously to correct the extracellular fluid hypotonicity. The abnortmally high serum potassium on Day 10 was twice repeated but remains unexplained; no comparable result was seen in any other experiment.
3 870 A. LEAF, F. C. BARTTER, R. F. SANTOS, AND 0. WRONG toc o URtAR,0/M 0o 54' WEIGHT *REFUSD P ET 6 a a FIG. 2. THE EFFECTS OF PITRESSIN ON SERUM ELECTROLYTE AND TOTAL SOLUTE CONCENTRATIONS, URINARY ELECTROLYTE EXCRETION, URINARY VOLUME AND TorAL SOLUTE CONCENTRATION, AND BODY WEIGHT IN A SUBJECT WITH ANTERIOR AND POSTERIOR PITUrrARY INSUFFICIENCY The concentrations of serum sodium, chloride and total solute were abnormally high during the control period. In the left-hand section of this figure the effects of pitressin alone are presented. In the right-hand section the effects of pitressin following seven days of continuous cortisone therapy are presented. On cortisone the antidiuretic effect of pitressin was increased, as indicated by the higher urinary total solute concentration. The sodium and chloride loss and symptoms of water intoxication were also increased with cortisone. Sodium iptake was 49 meq. per day by analysis. 0 a
4 WATER RETENTION AND ELECTROLYTE LOSS 871 of three days. The antidiuretic effect of pitressin is seen in the abrupt decrease in urine volume and increase in urine total solute concentration that occurred on the first day of hormone administration. The water retention produced by this antidiuretic effect resulted in an increase in body weight and dilution of serum sodium, chloride and total solutes. On the third day of pitressin administration a large increase in urinary sodium and chloride excretion occurred. The large water diuresis following the pitressin period represented excretion of water retained during pitressin administration, and returned the weight to the control level. The urinary sodium excretion fell to low levels in the post-pitressin period. These after-effects have been constant sequelae of pitressin administration when the latter has caused fluid retention and sodium loss. The left-hand section of Figure 2 shows similar data obtained from a patient with anterior and posterior pituitary insufficiency. Again pitressin had a prompt antidiuretic effect. Only after the first 24 hours was there an increased excretion of sodium and chloride, which progressed stepwise throughout the remainder of the pitressin period. Similar, though less striking, results were obtained in a subject with adrenal cortical insufficiency (Figure 3) treated with 25 mgs. of cortisone acetate orally every eight hours throughout the study. The delay in the appearance of the increases in electrolyte excretion suggested that they could be dissociated from the prompt antidiuretic action of pitressin. The increased sodium excretion during administration of pitressin was associated with progressive retention of water. This suggested that the effects on electrolyte excretion could result from the overhydration produced by pitressin rather than from a primary action of pitressin. B. Prevention of the effects of pitressin on electrolyte excretion by dehydration To test this hypothesis pitressin was given to three normal subjects during periods of low fluid intake which would preclude fluid retention in spite of exogenous antidiuretic activity. The same dose of pitressin was repeated later in the study during periods of high fluid intake. Figures 4 5/IZiSI O * S IS W~ ~ ~wrsa aaam *fuwa. of OCT FIG. 3. THE EFFECTS OF PITRESSIN ON SERuM ELEC- TROLYTE AND TOTAL SOLUTE CONCENTRATIONS, URINARY ELECTROLYTE AND NITROGEN EXCRETION, URINARY VOL- UME AND ToTAL SOLUTE CONCENTRATION, AND BODY WEIGHT IN A SUBJECT WITH ADRENAL CORTICAL INSUF- FICIENCY The subject was maintained on 25 mg. of cortisone acetate orally every eight hours throughout the study. Urinary calcium and phosphorus excretion and salivary electrolyte concentrations are also shown. Sodium intake was 124 meq. per day by analysis. and 5 show the influence of the state of hydration on renal sodium excretion. Figure 4 shows the effects of two different levels
5 872 A. LEAF, P. C. BARTTER, R. V. SANTO, AND 0. WRONG of fluid intakes on the excretion of electrolytes during pitressin administration. The urine volume was small, and its total solute concentration high, during the control period of low fluid intake. Administration of pitressin resulted in no further increase in urine total solute concentration and no fluid retention, as indicated by the constancy of I LOW FLLUD INTAK(E - HK;H."l, INITAKE FIG. 4. THE EFFECTS OF PITRESSIN ON SERUM ELEC- TROLYTE AND TOTAL SOLUTE CONCENTRATIONS, URINARY ELECTROLYTE AND NITROGEN EXCRETION, URINARY VOL- UME AND TOTAL SOLUTE CONCENTRATION, HEMATOCRIT, ENDOGENOUS CREATININE CLEARANCE, AND BODY WEIGHT IN A NORMAL MAN ON LoW AND HIGH FLUID INTAKES Fluid restriction prevented all of the effects of pitressin (weight gain, serum dilution, sodium and chloride loss) observed during the high fluid intake. Sodium intake was 78 meq. per day by analysis. body weights and the absence of serum dilution. No change in sodium or chloride excretion resulted from pitressin in the absence of fluid retention. The fluid intake was then increased. Urine volumes increased and urine concentration dropped. When pitressin was again given, its prompt antidiuretic effect was evident. Water was now retained, as indicated by the weight curve. A definite increase in urinary sodium was present on the third day of pitressin. The increase in chloride occurred the following day. The marked dilution of the serum sodium and total solute concentrations resulted both from water retention and, to a lesser extent, from excretion of sodium. Figure 5 shows the effect of three different levels of fluid intake on the excretion of electrolytes during pitressin administration. Again with restriction of fluid intake to low levels (920 ml. of water in total fluid intake daily) no significant changes in sodium and chloride excretion were noted. When a further 1,500 ml. of water were given daily, repetition of the pitressin dosage now resulted in definite fluid retention and weight gain, accompanied by a slight increase in sodium and chloride excretion. Finally, the fluid intake was increased to a total of 4,000 ml. daily; pitressin now caused a very large increase in sodium and chloride excretion.7 Because of the rapidity of water retention and the marked dilution of serum solute concentration that occurred with the high fluid intake, the last pitressin period was shortened to two days' duration. These observations suggested that the electrolyte excretion following pitressin is determined by the state of hydration. Figure 6 shows the relationship between per cent increase in body weight and cumulative sodium loss during fifteen periods of pitressin administration. It is apparent that a rough correlation exists between fluid retention and sodium loss. The possibility existed that the late increase in sodium and chloride excretion might simply be the result of an accumulation of pitressin activity in excess of physiological amounts. The total of 7 Although the sodium and chloride excretion had not reached "base-line" control values by the time the third course of pitressin was started, the effects on salt-loss are unequivocal.
6 WATER RETENTION AND ELECTROLYTE LOSS 873 asmal AM 260 = LOA 2000 =fll0ld INTAK 1 Or2Ht 4000 a ' O a 1 13 It7 I FIG. 5. THE Emc'rs of PImESSIN ON SERUM ELECTROLYTE AND TOTAL SOLUTE CONCENTRATIONS, URINARY ELECTROLYTE AND NITROGEN EXCRETION, URINARY VOLUME AND TOTAL SOLUTE CONCENTRATION, HEMATOCRIT, ENDOGENOUS CREATININE CLEARANCE, AND BODY WEIGHT IN A NORMAL MAN DURING THREE DIFFERENT LEVELS OF FLUID INTAKE During dehydration there was no loss of sodium in excess of intake, which by analysis was 60 meq. per day. With a moderate and a large increase in water intake, pitressin produced corresponding degrees of fluid retention and sodium and chloride loss. The severity of dehydration on the low fluid intake in this subject was indicated by the high serum sodium and total solute concentrations and the weight loss. The progressive fall in urine total solute concentration and increase in urine volume, in spite of this dehydration and in spite of pitressin is unexplained and was not observed in other studies.
7 874 PERCENT WEIGHT GAIN * * 0 0 A. LEAF, F. C. BARTTER, R. F. SANTOS, AND 0. WRONG CUMULATIVE URINARY SODIUM LOSS M.EQ. Q FIG. 6. THE RELATIONSHIP BETWEEN PITRESSIN-IN- DUCED WATER RETENTION (PER CENT INCREASE IN BoDy WEIGHT) AND CUMULATM SODIUM Loss The data include all the pitressin periods except those during ACTH and very low sodium intake, both of which prevented sodium loss. The cumulative sodium loss was calculated as that in excess of control urinary sodium excretion and per cent weight gain was calculated from the maximum weight increase achieved during pitressin. 7.0 units of pitressin had previously been administered over three days in most of the studies. Therefore, this dose was administered to one subject, O.W., all at one time in five injection sites, in order to produce hormone levels higher than any that could have occurred in the other studies. Antidiuresis was accompanied by a weight gain of only 0.5 per cent (0.4 Kg.), and no increase in sodium or chloride excretion. This indicates that the large sodium and chloride losses from pitressin in these experiments cannot be explained as effects of excessive doses of pitressin. C. Prevention of the effects of pitressin on electrolyte excretion by ACTH In two studies adrenocorticotropic hormone was administered concomitantly with pitressin to see whethet the sodium and chloride excretion could be prevented by stimulation of the adrenal cortex. Figure 7 shows the results in one subject; the other subject responded in similar fashion. Pitressin alone produced the expected fluid retention, weight gain, serum dilution and diuresis of sodium and chloride. A potent corticotropin,8 0.5 mg. administered subcutaneously every six hours for five days, completely abolished the sodium and chloride diuresis during pitressin; in fact, sodium excretion was markedly inhibited until ACTH was stopped. The maximum increase in body weight was 2.3 kilograms when pitressin alone was administered but 3.1 kilograms when pitressin and ACTH were given. In spite of the larger fluid retention that occurred during the ACTH administration the serum dilution was less because of the concomitant sodium retention. A very low sodium intake, 20 meq. per day, during another study on this subject likewise prevented the expected sodium loss during pitressin administration. Such a low sodium intake is a potent stimulus for renal conservation of sodium (10). D. Hemodynamic and renal changes during pitressin administration In none of the subjects was there a significant change in blood pressure during administration of pitressin. Expansion of plasma volume subsequent to water retention was shown in subjects 0. W. and R. S. The peak increase of plasma volume (as calculated from changes in hematocrit and hemoglobin) was 8 per cent in 0. W. and 13 per cent in R. S. In the three studies in which renal clearances were measured they were found to be increased during the fluid retention. In subject R. S. the clearance of endogenous creatinine rose from a mean control level of 171 ± 11 liters per day to a maximum of 217 liters during the second day of the last pitressin period. In 0. W. the clearance of endogenous creatinine rose from a mean control level of 189 ± 9 liters per day to a maximum of 226 liters on the day after the second pitressin period. In subject M. K. H. the inulin clearance rose from control values of 105, 102, and 85 ml. per minute per 1.73 m2 to 124 ml. per minute per 1.73 m2 during the last day of the first pitressin period in Figure 7. The simultaneous clearances of para-aminohippurate showed no significant changes. 8 Generously supplied by Dr. E. B. Astwood.
8 E. The effects of pitressin on excretion of other electrolytes and nitrogen In the two studies in which calcium and phosphorus balances were measured there occurred an increase in urinary calcium excretion similar to WATER RETENTION AND ELECTROLYTE LOSS 875 that shown in Figure 3. Changes in phosphorus excretion were equivocal. No constant pattern of potassium excretion was noted. Urinary nitrogen was not significantly affected by pitressin administration (Figures 4 and 5). KKH FEMALE AGE 42 WSiMZ4IR 64/ AGElESIS~~~~~ PWRE!;SI TAtATE IN OL NRTS/24IR 4 MG /24 H 1 1 ACTH ; I laqurv I FIG. 7. THE EFFECTS OF PITRESSIN, ALONE AND WITH ACTH, ON SERUM ELECTROLYTE AND ToTAL SOLUTE CONCENTRATIONS, URINARY ELECTROLYTE EXCRETION, URINARY VOLUME AND TOTAL SOLUTE CONCENTRATION, CIRCU- LATING EOSINOPHILS, AND BoDy WEIGHT IN A SUBJECT WrrH OVARIAN AGENESIS The natriuresis and chloruresis induced by pitressin were completely abolished by ACTH. The serum dilution was less with ACTH together with pitressin than with pitressin alone, although the weight gain was greater.
9 876 A. LEAF, F. C. BARTTER, R. F. SANTOS, AND 0. WRONG DISCUSSION The confusion that exists regarding the effects of pitressin on renal excretion of electrolytes is probably the result of a diversity of experimental conditions. Species' differences, variations in dose, and the use of different extracts may have contributed to the conflicting findings. The present study indicates that the state of hydration of the experimental subject may be an important variable. Thus, dehydration prevented the large excretion of sodium and chloride produced by pitressin in hydrated subjects. This finding is in accord with the observation that endogenous antidiuretic hormone, released by dehydration (11-13), does not cause natriuresis or chloruresis (14, 15). That pitressin does not exert a direct effect on electrolyte excretion in man is suggested by the results of the present study. The increased electrolyte excretion associated with pitressin appeared to be secondary to water retention and was prevented by dehydration. The possibility, however, of a direct effect of pitressin on renal excretion of sodium and chloride has not been excluded. Mechanisms for sodium retention may come into play during dehydration and obscure a pitressin effect. Increased adrenal cortical activity was capable of inhibiting the natriuresis and chloruresis, and it is possible that dehydration stimulates the adrenal cortex. Further evidence that pitressin has no direct electrolyte effects was seen in the dissociation between its rapid antidiuretic action and the late increase in electrolyte excretion which occurred in the hydrated subjects. That this late effect was not simply the result of an accumulation of pitressin activity in excess of physiological amounts is indicated by the following: 1) no such effect was seen from the same pitressin dosage during dehydration; 2) when the total dosage was administered at one time to a hydrated subject there were no electrolyte effects. The effects of a given quantity of water retention on sodium diuresis could be prevented by 9Theoretically at least, during dehydration, administered pitressin is superimposed upon endogenous antidiuretic hormone, so that the total quantity of circulating hormone is greater than that obtaining when pitressin is administered to the hydrated subject, adrenal stimulation or salt restriction.10 This was demonstrated by studying exactly comparable pitressin periods at the same level of fluid intake, in the same subject, "on" and "off" ACTH, and on low and high salt intakes. Thus it was apparent that this degree of water retention had not served to release endogenous sodium-conserving mechanisms. In these experiments, small doses of pitressin were given over periods of several days, and it is possible that acute effects were obscured. However, several recent studies in which physiological amounts of posterior pituitary extract were given to human subjects in acute experiments reveal no effect on sodium and chloride excretion (1, 16-20). Water retention with dilution of extracellular fluid, when marked, was accompanied by symptoms of water intoxication. These were progressive mental confusion, fatigue, headache, and nausea leading to vomiting. Muscle cramps occurred in only one instance. No essential differences were observed in the response of normal subjects and those with endocrine disorders, including adrenal cortical insufficiency. In two subjects, cortisone neither diminished the antidiuretic response to pitressin nor ameliorated the symptoms of water intoxication. Adrenocorticotropic hormone, on the other hand (Figure 7) did not diminish the antidiuretic response to pitressin, but did ameliorate the symptoms of water intoxication, presumably by causing sodium retention, and hence less serum and extracellular fluid dilution. Low serum sodium concentrations have been considered to be a cause of decreased renal function. Serum sodium levels as low as 120 meq. per L. were found in this study in the absence of any evidence of diminished renal function. Inulin, para-aminohippurate, and creatinine clearances, as well as renal concentrating ability, were unimpaired. This would suggest that the cause of reduced renal function in other low sodium states is not the low serum sodium concentration per se, but rather some associated abnormality, such as a 10 Since an increase of glomerular filtration rate was found to accompany water retention, it is likely that water retention of a sufficient magnitude could produce sodium loss in spite of a maximal stimulus to tubular reabsorption of sodium.
10 WATER RETENTION AND ELECTROLYTE LOSS 877 reduced plasma volume or cardiac output commonly found in these disorders. It has been postulated that edema may result from an excess of endogenous antidiuretic hormone activity (21, 22). The assumption is made that primary water retention will cause sodium retention and the resultant isotonic over-expansion of extracellular fluid volume which characterizes the edematous state. The present studies, though of short duration, suggest that this sequence of events does not occur. Pitressin had no effect on the dehydrated subject; when the fluid intake was increased water retention occurred but sodium loss rather than retention ensued. It appears that antidiuretic hormone activity itself, in the absence of simultaneous and independent mechanisms for sodium retention, does not result in edema. No edema was noted in our subjects; indeed it is unlikely that pure water retention could cause significant clinical edema without lethal water intoxication. Some increase in glomerular filtration apparently occurred during the water retention and natriuresis. However, the demonstration that ACTH prevented such sodium and chloride loss indicates that tubular reabsorptive capacity for sodium and chloride had not been exceeded. The finding of large excretions of sodium and chloride at a time when their concentrations in the serum were falling, clearly indicates that serum concentrations of sodium and chloride were not effective stimuli for their renal conservation. It is thought that this renal loss of sodium and chloride in the presence of obligatory retention of water is a homeostatic response to over-expansion of fluid volume. It is of interest that Stewart and Rourke (23) produced an increased excretion of sodium by acutely over-loading a normal subject with water to the point of water intoxication. No posterior pituitary extract was administered to their subject. Strauss, Davis, Rosenbaum, and Rossmeisl (24) have increased renal sodium excretion by expansion of extracellular fluid volume with hypotonic saline solutions. These results appear to be manifestations of the same phenomenon: increased sodium excretion in response to over-expansion of body fluid volume. SUMMARY AND CONCLUSIONS The effects of a long-acting posterior pituitary extract on electrolyte and water excretion were studied in man. Observations were made during twenty 2 to 4 day periods of pitressin (1 unit per 12 hours) in nine subjects maintained on constant diets and fluid intakes. It was found that pitressin produced in normally hydrated subjects the following: 1) prompt water retention and resulting weight gain; 2) serum dilution; and 3) a marked increase in urinary sodium and chloride excretion manifest on the second or third day of pitressin administration. Cessation of pitressin administration was followed by: 1) a large water diuresis with fall in body weight; 2) return of serum concentration to control levels; and 3) a decrease in urinary sodium and chloride excretion to levels below the control. All the above changes were prevented by restriction of fluid intake during pitressin administration. This strongly suggests that the increased excretion of sodium and chloride was the result of water retention and not a direct effect of pitressin Ṡome increase in glomerular filtration rate apparently occurred during the water retention and natriuresis. Evidence that the tubular reabsorptive capacity for sodium and chloride had not been exceeded, however, was indicated by the prevention of such electrolyte loss by ACTH or by a low sodium diet. The renal loss of sodium and chloride resulting from obligatory retention of water is interpreted as a homeostatic response to over-expansion of fluid volume. ACKNOWLEDGMENTS The authors wish to express their gratitude to Dr. Fuller Albright in whose laboratory this study was initiated and to Miss Dorothy B. Richardson for invaluable technical assistance. REFERENCES 1. White, A. G., Rubin, G., and Leiter, L., Studies in edema. III. The effect of pitressin on the renal excretion of water and electrolytes in patients with and without liver disease. J. Clin. Invest., 1951, 30, Reifenstein, E. C., Jr., Albright, F., Wells, S. L., The accumulation, interpretation, and presentation
11 878 A. LEAF, F. C. BARTTER, R. F. SANTOS, AND 0. WRONG of data relating to metabolic balances, notably those of calcium, phosphorus, and nitrogen. J. Clin. Endocrinol., 1945, 5, Shannon, J. A., The control of the renal excretion of water. II. The rate of liberation of the posterior pituitary antidiuretic hormone in the dog. J. Exper. Med., 1942, 76, Lauson, H. D., Eder, H. A., Chinard, F. P., Cotzias, G. C., and Greif, R. L., Estimation of the rate of antidiuretic hormone secretion in normal men. Federation Proc. 1948, 7, Leaf, A., Mamby, A. R., Rasmussen, H., Marasco, J. P., Some hormonal aspects of water excretion in man. J. Clin. Invest., 1952, 31, International Critical Tables of Numerical Data, Physics, Chemistry and Technology. Vol. IV, p McGraw-Hill Book Company, Inc., New York, Goldring, W., and Chasis, H., Hypertension and hypertensive disease. The Commonwealth Fund. New York, Leaf, A., and Camara, A. A., Renal tubular secretion of potassium in man. J. Clin. Invest., 1949, 28, Elkinton, J. R., Danowski, T. S., Winkler, A., Hemodynamic changes in salt depletion and in dehydration. J. Clin. Invest., 1946, 25, Leaf, A., and Couter, W. T., Evidence that renal sodium excretion by normal human subjects is regulated by adrenal cortical activity. J. Clin. Invest., 1949, 28, Gilman, A., and Goodman, L., The secretory response of the posterior pituitary to the need for water conservation. J. Physiol., 1937, 90, Ames, R. G., Moore, D. H., and Van Dyke, H. B., The excretion of the posterior pituitary antidiuretic hormone in the urine and its detection in the blood. Endocrinol., 1950, 46, Leaf, A., and Mamby, A. R., The normal antidiuretic mechanism in man and dog; its regulation by extracellular fluid tonicity. J. Clin. Invest., 1952, 31, Elkinton, J. R., and Taffel, M., Prolonged water deprivation in the dog. J. Clin. Invest., 1942, 21, Peters, J. P., Sodium, water and edema. J. Mt. Sinai Hosp., 1950, 17, Sinclair-Smith, B. C., Sisson, J., Kattus, A. A., Genecin, A., Monge, C., McKeever, W., and Newman, E. V., The effects of posterior pituitary extract and smoking on water, sodium and chloride excretion in normal subjects and in patients with congestive cardiac failure. Bull. Johns Hopkins Hosp., 1950, 87, Chalmers, T. M., Lewis, A. A. G., and Pawan, G. L. S., The effect of posterior pituitary extracts on the renal excretion of sodium and chloride in man. J. Physiol., 1951, 112, Black, D. A. K., and Thompson, A. E., Day to day changes in sodium and water output with and without posterior pituitary extract. Clin. Sc., 1951, 10, Murphy, R. J. F., and Stead, E. A., Jr., Effects of exogenous and endogenous posterior pituitary antidiuretic hormone on water and electrolyte excretion. J. Clin. Invest., 1951, 30, Nelson, W. P., III, and Welt, L. G., The effects of pitressin on the metabolism and exoretion of water and electrolytes in normal subjects and patients with cirrhosis and ascites. J. Clin. Invest., 1952, 31, Robinson, F. H., Jr., and Farr, L. E., The relation between clinical edema and the excretion of an antidiuretic substance in the urine. Ann. Int. Med., 1940, 14, Ralli, E. P., Robson, J. S., Clarke, D., and Hoagland, C. L., Factors influencing ascites in patients with cirrhosis of the liver. J. Clin. Invest., 1945, 24, Stewart, J. D., and Rourke, G. M., The effects of large intravenous infusions on body fluid. J. Clin. Invest., 1942, 21, Strauss, M. B., Davis, R. K., Rosenbaum, J. D., and Rossmeisl, E. C., Production of increased renal sodium excretion by the hypotonic expansion of extracellular fluid volume in recumbent subjects. J. Clin. Invest., 1952, 31, 80.
STUDIES ON INTRAVENOUS WATER DIURESIS AND NICOTINE
 STUDIES ON INTRAVENOUS WATER DIURESIS AND NICOTINE AND PITRESSIN ANTIDURESIS IN NORMAL SUBJECTS AND PATIENTS WITH LIVER DISEASE' By STANLEY H. BERNSTEIN,2 RAYMOND E. WESTON, GEORGE ROSS, JACOB GROSSMAN,
STUDIES ON INTRAVENOUS WATER DIURESIS AND NICOTINE AND PITRESSIN ANTIDURESIS IN NORMAL SUBJECTS AND PATIENTS WITH LIVER DISEASE' By STANLEY H. BERNSTEIN,2 RAYMOND E. WESTON, GEORGE ROSS, JACOB GROSSMAN,
SUBJECTS TO THE INGESTION OF ISOTONIC SALINE
 FACTORS INFLUENCING THE DIURETIC RESPONSE OF SEATED SUBJECTS TO THE INGESTION OF ISOTONIC SALINE SOLUTION By WILLIAM H. BIRCHARD AND MAURICE B. STRAUSS (From the Medical Service and Research Laboratory,
FACTORS INFLUENCING THE DIURETIC RESPONSE OF SEATED SUBJECTS TO THE INGESTION OF ISOTONIC SALINE SOLUTION By WILLIAM H. BIRCHARD AND MAURICE B. STRAUSS (From the Medical Service and Research Laboratory,
MIGUEL CHIAPPORI 4. Renal function. Twelve healthy Peruvian males between the ages of 20 and 28 years were studied. None
 ORAL SODIUM LOADING IN NORMAL INDIVIDUALS By KEHL MARKLEY,1 MANUEL BOCANEGRA,2 GUILLERMO MORALES,3 AND MIGUEL CHIAPPORI 4 (From the U. S. Public Health Service, U. S. Department of Health, Education, and
ORAL SODIUM LOADING IN NORMAL INDIVIDUALS By KEHL MARKLEY,1 MANUEL BOCANEGRA,2 GUILLERMO MORALES,3 AND MIGUEL CHIAPPORI 4 (From the U. S. Public Health Service, U. S. Department of Health, Education, and
ADRENALECTOMY. Potassium Chloride " 108 Total protein.. 79 g- i 7 0 g. i. The history of thirst and polyuria together with
 J. clin. Path. (1959), 12, 530. DIABETES INSIPIDUS COMPLICATING TOTAL ADRENALECTOMY Diabetes insipidus is seldom complicated by other hormonal defects. As far as we know only one patient with diabetes
J. clin. Path. (1959), 12, 530. DIABETES INSIPIDUS COMPLICATING TOTAL ADRENALECTOMY Diabetes insipidus is seldom complicated by other hormonal defects. As far as we know only one patient with diabetes
venous blood samples were drawn. The plasma was separated rapidly by centrifugation and assayed within one
 THE ANTIDIURETIC ACTIVITY OF PLASMA OF PATIENTS WITH HEPATIC CIRRHOSIS, CONGESTIVE HEART FAIL- URE, HYPERTENSION AND OTHER CLINICAL DISORDERS' By MARVIN STEIN,2 ROBERT SCHWARTZ, AND I. ARTHUR MIRSKY (From
THE ANTIDIURETIC ACTIVITY OF PLASMA OF PATIENTS WITH HEPATIC CIRRHOSIS, CONGESTIVE HEART FAIL- URE, HYPERTENSION AND OTHER CLINICAL DISORDERS' By MARVIN STEIN,2 ROBERT SCHWARTZ, AND I. ARTHUR MIRSKY (From
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
CONCERNING THE EFFECTS OF MAGNESIUM SULFATE ON RENAL FUNCTION, ELECTROLYTE EXCRETION, AND CLEARANCE OF MAGNESIUM
 CONCERNING THE EFFECTS OF MAGNESIUM SULFATE ON RENAL FUNCTION, ELECTROLYTE EXCRETION, AND CLEARANCE OF MAGNESIUM B. I. Heller,, J. F. Hammarsten, F. L. Stutzman J Clin Invest. 1953;32(9):858-861. https://doi.org/10.1172/jci102803.
CONCERNING THE EFFECTS OF MAGNESIUM SULFATE ON RENAL FUNCTION, ELECTROLYTE EXCRETION, AND CLEARANCE OF MAGNESIUM B. I. Heller,, J. F. Hammarsten, F. L. Stutzman J Clin Invest. 1953;32(9):858-861. https://doi.org/10.1172/jci102803.
clamped. At 30- or 60-minute intervals urine specimens were collected and the bladder washed out with saline
 Downloaded from http://www.jci.org on January 11, 218. https://doi.org/1.1172/jci11171 THE MECHANISM OF THE EXCRETION OF VITAMIN C BY THE HUMAN KIDNEY AT LOW AND NORMAL PLASMA LEVELS OF ASCORBIC ACID 1
Downloaded from http://www.jci.org on January 11, 218. https://doi.org/1.1172/jci11171 THE MECHANISM OF THE EXCRETION OF VITAMIN C BY THE HUMAN KIDNEY AT LOW AND NORMAL PLASMA LEVELS OF ASCORBIC ACID 1
The antihypertensive and diuretic effects of amiloride and. of its combination with hydrochlorothiazide
 The antihypertensive and diuretic effects of amiloride and of its combination with hydrochlorothiazide The hypotensive effect as well as changes in serum electrolytes and uric acid of amiloride (AM) and
The antihypertensive and diuretic effects of amiloride and of its combination with hydrochlorothiazide The hypotensive effect as well as changes in serum electrolytes and uric acid of amiloride (AM) and
Fluids and electrolytes
 Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
M6ller, McIntosh and Van Slyke (5) has been employed. The cases. changes in functional activity. Indications suggesting that such changes
 STUDIES OF UREA EXCRETION. VIII. THE EFFECTS ON THE UREA CLEARANCE OF CHANGES IN PROTEIN AND SALT CONTENTS OF THE DIET BY CUTHBERT L. COPE I (From the Hospital of the Rockefeller Institute for Medical
STUDIES OF UREA EXCRETION. VIII. THE EFFECTS ON THE UREA CLEARANCE OF CHANGES IN PROTEIN AND SALT CONTENTS OF THE DIET BY CUTHBERT L. COPE I (From the Hospital of the Rockefeller Institute for Medical
Effect of an Intravenous Sodium Chloride Load on Renal Hemodynamics and Electrolyte Excretion in Essential Hypertension
 Effect of an Intravenous Sodium Chloride Load on Renal Hemodynamics and Electrolyte Excretion in Essential Hypertension BY PAUL T. COTTIER, M.D., JOHN M. WELLER, M.D., AND SIBLEY W. HOOBLER, M.D. Excretion
Effect of an Intravenous Sodium Chloride Load on Renal Hemodynamics and Electrolyte Excretion in Essential Hypertension BY PAUL T. COTTIER, M.D., JOHN M. WELLER, M.D., AND SIBLEY W. HOOBLER, M.D. Excretion
transudation is accompanied by an increase
 THE EFFECT OF AN INFUSION OF HYPERONCOTIC ALBUMIY ON THE EXCRETION OF WATER AND SOLUTES 1'2 By R. G. PETERSDORF 3 AND L. G. WELT 4 (From the Department of Internal Medicine, Yale University School of Medscine,
THE EFFECT OF AN INFUSION OF HYPERONCOTIC ALBUMIY ON THE EXCRETION OF WATER AND SOLUTES 1'2 By R. G. PETERSDORF 3 AND L. G. WELT 4 (From the Department of Internal Medicine, Yale University School of Medscine,
had no effect on the production of aldosterone, corticosterone, or cortisol after
 INHIBITION OF THE EFFECTS OF ANGIOTENSIN II ON ADRENAL STEROID PRODUCTION BY DIETARY SODIUM BY WARREN W. DAVIS,* LAWRENCE R. BURWELL,t AND FREDERIC C. BARTTERt ENDOCRINOLOGY BRANCH, NATIONAL HEART INSTITUTE,
INHIBITION OF THE EFFECTS OF ANGIOTENSIN II ON ADRENAL STEROID PRODUCTION BY DIETARY SODIUM BY WARREN W. DAVIS,* LAWRENCE R. BURWELL,t AND FREDERIC C. BARTTERt ENDOCRINOLOGY BRANCH, NATIONAL HEART INSTITUTE,
CLINICAL PROGRESS Editor: HERRMAN L. BLUMGART, M.D.
 CLINICAL PROGRESS Editor: HERRMAN L. BLUMGART, M.D. Associate Editor: A. STONE FREEDBERG, M.D. Downloaded from http://ahajournals.org by on November 11, 2018 Renal Factor in Congestive Heart Failure P
CLINICAL PROGRESS Editor: HERRMAN L. BLUMGART, M.D. Associate Editor: A. STONE FREEDBERG, M.D. Downloaded from http://ahajournals.org by on November 11, 2018 Renal Factor in Congestive Heart Failure P
Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are
 Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
ance of the sugar, until at plasma levels of 140 mgm. per cent the creatinine/sugar clearance ratio
 THE RENAL EXCRETION OF CREATININE IN MAN BY JAMES A. SHANNON 1 (From The Department of Physiology, New York University College of Medicine, New York City) In a previous paper the evidence on the excretion
THE RENAL EXCRETION OF CREATININE IN MAN BY JAMES A. SHANNON 1 (From The Department of Physiology, New York University College of Medicine, New York City) In a previous paper the evidence on the excretion
THE CONTROL OF THE RENAL EXCRETION OF WATER* II. TB~ RATE OF LIBERATION OF THE POSTERIOR PITUITARY ANTIDIURETIC HORMONE IN THE DOG
 Published Online: 1 October, 1942 Supp Info: http://doi.org/10.1084/jem.76.4.387 Downloaded from jem.rupress.org on July 3, 2018 THE CONTROL OF THE RENAL EXCRETION OF WATER* II. TB~ RATE OF LIBERATION
Published Online: 1 October, 1942 Supp Info: http://doi.org/10.1084/jem.76.4.387 Downloaded from jem.rupress.org on July 3, 2018 THE CONTROL OF THE RENAL EXCRETION OF WATER* II. TB~ RATE OF LIBERATION
Treating the syndrome of inappropriate ADH secretion with isotonic saline
 Q J Med 1998; 91:749 753 Treating the syndrome of inappropriate ADH secretion with isotonic saline W. MUSCH and G. DECAUX1 From the Department of Internal Medicine, Bracops Hospital, Brussels, and 1Department
Q J Med 1998; 91:749 753 Treating the syndrome of inappropriate ADH secretion with isotonic saline W. MUSCH and G. DECAUX1 From the Department of Internal Medicine, Bracops Hospital, Brussels, and 1Department
ELECTROLYTE DISTURBANCES IN CONGESTIVE HEART FAILURE*
 ELECTROLYTE DISTURBANCES IN CONGESTIVE HEART FAILURE* DAVID P. B.AUMANN, M.D. Department of Medicine, University of Arkansas School of Medicine, Little Rock, Arkansas The retention of salt and water secondary
ELECTROLYTE DISTURBANCES IN CONGESTIVE HEART FAILURE* DAVID P. B.AUMANN, M.D. Department of Medicine, University of Arkansas School of Medicine, Little Rock, Arkansas The retention of salt and water secondary
The technique of multiple clearance was chosen. because it supplied us with the filtration rate, the
 RENAL REABSORPTION OF CHLORIDE AND PHOSPHATE IN NORMAL SUBJECTS AND IN PATIENTS WITH ESSENTIAL ARTERIAL HYPERTENSION' By EDITH B. FARNSWORTH (From the Department of Medicine, Northwestern University Medical
RENAL REABSORPTION OF CHLORIDE AND PHOSPHATE IN NORMAL SUBJECTS AND IN PATIENTS WITH ESSENTIAL ARTERIAL HYPERTENSION' By EDITH B. FARNSWORTH (From the Department of Medicine, Northwestern University Medical
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
dynamic action of ingested amino acids effected
 THE.EFFECT OF GLYCINE ON THE PRODUCTION AND EXCRETION OF URIC ACID1 BY MEYER FRIEDMAN (Fromn the Harold Brunn Institute for Cardiovascular Research, San Francisco, California) Mt. Zion Hospital, (Received
THE.EFFECT OF GLYCINE ON THE PRODUCTION AND EXCRETION OF URIC ACID1 BY MEYER FRIEDMAN (Fromn the Harold Brunn Institute for Cardiovascular Research, San Francisco, California) Mt. Zion Hospital, (Received
was limited to the arm and was presumably due to recurrent breast cancer involving the chest wall and axilla.
 SODIUM DEPLETION IN ADRENALECTOMIZED HUMANS' By MORTIMER B. LIPSETT2 AND OLOF H. PEARSON (From the Division of Clinical Investigation, Sloan-Kettering Institute for Cancer Research; and the Department
SODIUM DEPLETION IN ADRENALECTOMIZED HUMANS' By MORTIMER B. LIPSETT2 AND OLOF H. PEARSON (From the Division of Clinical Investigation, Sloan-Kettering Institute for Cancer Research; and the Department
hormone. Until recently, evidence that the
 THE EXPERIMENTAL PRODUCTION OF ASCITES IN THE DOG WITH DIABETES INSIPIDUS1 By JOHN H. LARAGH, H. B. VAN DYKE, JULIUS JACOBSON,2 KARLIS ADAM- SONS, JR.,3 AND STAMFORD L. ENGEL4 (From the Departments of
THE EXPERIMENTAL PRODUCTION OF ASCITES IN THE DOG WITH DIABETES INSIPIDUS1 By JOHN H. LARAGH, H. B. VAN DYKE, JULIUS JACOBSON,2 KARLIS ADAM- SONS, JR.,3 AND STAMFORD L. ENGEL4 (From the Departments of
has been noted in particular in patients with mercury
 BIOCHEMICAL AND HEMODYNAMIC CHANGES FOLLOWING THE SUBCUTANEOUS INJECTION OF GLUCOSE SOLUTION 1 By T. S. DANOWSKI, A. W. WINKLER,2 AND J. R. ELKINTON (From the Department of Internal Medicine, Yale University
BIOCHEMICAL AND HEMODYNAMIC CHANGES FOLLOWING THE SUBCUTANEOUS INJECTION OF GLUCOSE SOLUTION 1 By T. S. DANOWSKI, A. W. WINKLER,2 AND J. R. ELKINTON (From the Department of Internal Medicine, Yale University
EFFECT OF 9-a-FLUOROHYDROCORTISONE ON THE ILEAL EXCRETA OF ILEOSTOMIZED SUBJECTS
 GASTROENTEROLOGY Copyright @ 1972 by The Williams & Wilkins Co. Vol. 62, No. 2 Printed in U. S. A. EFFECT OF 9-a-FLUOROHYDROCORTISONE ON THE ILEAL EXCRETA OF ILEOSTOMIZED SUBJECTS PHIT.IP KRAMER, M.D.,
GASTROENTEROLOGY Copyright @ 1972 by The Williams & Wilkins Co. Vol. 62, No. 2 Printed in U. S. A. EFFECT OF 9-a-FLUOROHYDROCORTISONE ON THE ILEAL EXCRETA OF ILEOSTOMIZED SUBJECTS PHIT.IP KRAMER, M.D.,
function. Likewise it was hoped to determine whether a reduction in filtration rate would reduce
 STUDIES ON DIURETICS. II. THE RELATIONSHIP BETWEEN GLOMERULAR FILTRATION RATE, PROXIMAL TUBULAR ABSORPTION OF SODIUM AND DIURETIC EFFICACY OF MERCURIALS 1 By ROBERT F. PITTS AND JOHN J. DUGGAN WITH THE
STUDIES ON DIURETICS. II. THE RELATIONSHIP BETWEEN GLOMERULAR FILTRATION RATE, PROXIMAL TUBULAR ABSORPTION OF SODIUM AND DIURETIC EFFICACY OF MERCURIALS 1 By ROBERT F. PITTS AND JOHN J. DUGGAN WITH THE
New Haven, Conn.) laboratory, having abstained from food and fluids for the preceding 12 hours. In order to assure a constant and
 THE INFLUENCE OF BODILY HYDRATION ON THE RENAL CONCENTRATING PROCESS 1 By FRANKLIN H. EPSTEIN,2 CHARLES R. KLEEMAN, AND ACHIEL HENDRIKX (From the Department of Internal Medicine, Yale University School
THE INFLUENCE OF BODILY HYDRATION ON THE RENAL CONCENTRATING PROCESS 1 By FRANKLIN H. EPSTEIN,2 CHARLES R. KLEEMAN, AND ACHIEL HENDRIKX (From the Department of Internal Medicine, Yale University School
NORMOSOL -R MULTIPLE ELECTROLYTES INJECTION TYPE 1, USP For Replacing Acute Losses of Extracellular Fluid Flexible Plastic Container
 NORMOSOL -R MULTIPLE ELECTROLYTES INJECTION TYPE 1, USP For Replacing Acute Losses of Extracellular Fluid Flexible Plastic Container R x only DESCRIPTION Normosol-R is a sterile, nonpyrogenic isotonic
NORMOSOL -R MULTIPLE ELECTROLYTES INJECTION TYPE 1, USP For Replacing Acute Losses of Extracellular Fluid Flexible Plastic Container R x only DESCRIPTION Normosol-R is a sterile, nonpyrogenic isotonic
(ethanol) suggests that it is similar to the diuresis following ingestion of water.
 435 J. Physiol. (I946) I04, 435-442 6I2.464.I THE EFFECT OF ETHYL ALCOHOL AND SOME OTHER DIURETICS ON CHLORIDE EXCRETION IN MAN BY M. GRACE EGGLETON AND ISABEL G. SMITH, From the Physiology Department,
435 J. Physiol. (I946) I04, 435-442 6I2.464.I THE EFFECT OF ETHYL ALCOHOL AND SOME OTHER DIURETICS ON CHLORIDE EXCRETION IN MAN BY M. GRACE EGGLETON AND ISABEL G. SMITH, From the Physiology Department,
Disclaimer. Chapter 3 Disorder of Water, Electrolyte and Acid-base Professor A. S. Alhomida. Disorder of Water and Electrolyte
 Disclaimer King Saud University College of Science Department of Biochemistry The texts, tables, figures and images contained in this course presentation (BCH 376) are not my own, they can be found on:
Disclaimer King Saud University College of Science Department of Biochemistry The texts, tables, figures and images contained in this course presentation (BCH 376) are not my own, they can be found on:
during the 8 days prior to the first intraperitoneal
 EXPERIMENTAL HYPERTONICITY: ALTERATIONS IN THE DISTRIBUTION OF BODY WATER, AND THE CAUSE OF DEATH 1 By ALEXANDER W. WINKLER, J. RUSSELL ELKINTON,2 JAMES HOPPER, JR.,8 AND HEBBEL E. HOFF (From the Department
EXPERIMENTAL HYPERTONICITY: ALTERATIONS IN THE DISTRIBUTION OF BODY WATER, AND THE CAUSE OF DEATH 1 By ALEXANDER W. WINKLER, J. RUSSELL ELKINTON,2 JAMES HOPPER, JR.,8 AND HEBBEL E. HOFF (From the Department
man of the effects of diabetes and of insulin on the maximum ability of the tubules to reabsorb glucose.
 EFFECT OF DIABETES AND INSULIN ON THE MAXIMUM CA- PACITY OF THE RENAL TUBULES TO REABSORB GLUCOSE t By SAUL J. FARBER, EUGENE Y. BERGER, AND DAVID P. EARLE (From the Department of Medicine, New York University
EFFECT OF DIABETES AND INSULIN ON THE MAXIMUM CA- PACITY OF THE RENAL TUBULES TO REABSORB GLUCOSE t By SAUL J. FARBER, EUGENE Y. BERGER, AND DAVID P. EARLE (From the Department of Medicine, New York University
The Induction of Metabolic Alkalosis by Correction of Potassium Deficiency *
 lournal of Clinical Investigation Vol. 45, No. 4, 1966 The Induction of Metabolic Alkalosis by Correction of Potassium Deficiency * HOWARD L. BLEICH,t RICHARD L. TANNEN,t AND WILLIAM B. SCHWARTZ t (From
lournal of Clinical Investigation Vol. 45, No. 4, 1966 The Induction of Metabolic Alkalosis by Correction of Potassium Deficiency * HOWARD L. BLEICH,t RICHARD L. TANNEN,t AND WILLIAM B. SCHWARTZ t (From
Hypoparathyroid Patients *
 Journal of Clinical Investigation Vol. 44, No. 6, 1965 Effects of Serum Calcium Level and Parathyroid Extracts on Phosphate and Calcium Excretion in Hypoparathyroid Patients * EUGENE EISENBERG t (From
Journal of Clinical Investigation Vol. 44, No. 6, 1965 Effects of Serum Calcium Level and Parathyroid Extracts on Phosphate and Calcium Excretion in Hypoparathyroid Patients * EUGENE EISENBERG t (From
Comparison of Sodium and Potassium Intake with Excretion JOSEPH SCHACHTER, M.D., PH.D., PATRICIA H. HARPER, R.D., MARY E. RADIN, M.A.
 Comparison of Sodium and Potassium Intake with Excretion JOSEPH SCHACHTER, M.D., PH.D., PATRICIA H. HARPER, R.D., MARY E. RADIN, M.A., ARLENE W. CAGGIULA, PH.D., ROBERT H. MCDONALD, M.D., AND WARREN F.
Comparison of Sodium and Potassium Intake with Excretion JOSEPH SCHACHTER, M.D., PH.D., PATRICIA H. HARPER, R.D., MARY E. RADIN, M.A., ARLENE W. CAGGIULA, PH.D., ROBERT H. MCDONALD, M.D., AND WARREN F.
BIOL 2402 Renal Function
 BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
norepinephrinee." 2 PNMT activity is stimulated by certain adrenocortical markedly,3' 4 but can be restored to normal by the administration of
 IMPAIRED SECRETION OF EPINEPHRINE IN RESPONSE TO INSULIN AMONG HYPOPHYSECTOMIZED DOGS* BY RICHARD J. WURTMAN, ALFRED CASPER, LARISSA A. POHORECKY, AND FREDERIC C. BARTTER DEPARTMENT OF NUTRITION AND FOOD
IMPAIRED SECRETION OF EPINEPHRINE IN RESPONSE TO INSULIN AMONG HYPOPHYSECTOMIZED DOGS* BY RICHARD J. WURTMAN, ALFRED CASPER, LARISSA A. POHORECKY, AND FREDERIC C. BARTTER DEPARTMENT OF NUTRITION AND FOOD
Cutler, Power & Wilder, 1938; Hall & Langley, 1940), in the dog (Winkler &
 8 J. Physiol. (I948) I07, 8-I3 6I2.46I.6 RENAL EXCRETION OF SODIUM AND POTASSIUM IN RATS BY S. E. DICKER (Beit Memorial Fellow) From the Department of Pharmacology, University of Bristol (Received 30 December
8 J. Physiol. (I948) I07, 8-I3 6I2.46I.6 RENAL EXCRETION OF SODIUM AND POTASSIUM IN RATS BY S. E. DICKER (Beit Memorial Fellow) From the Department of Pharmacology, University of Bristol (Received 30 December
HUMAN SUBJECT 1. Syracuse, N. Y.) the urine of increasing quantities of these buffers, it has been found in man as in the dog that (1)
 THE RENAL REGULATION OF ACID-BASE BALANCE IN MAN. II. FACTORS AFFECTING THE EXCRETION OF TITRATABLE ACID BY THE NORMAL HUMAN SUBJECT 1 By W. A. SCHIESS, J. L. AYER, W. D. LOTSPEICH AND R. F. PITTS WITH
THE RENAL REGULATION OF ACID-BASE BALANCE IN MAN. II. FACTORS AFFECTING THE EXCRETION OF TITRATABLE ACID BY THE NORMAL HUMAN SUBJECT 1 By W. A. SCHIESS, J. L. AYER, W. D. LOTSPEICH AND R. F. PITTS WITH
ADRENALECTOMIZED rats drink less than normal rats when 2 per cent saline. daily by stomach tube and water to drink freely, died quickly but such
 THE EFFECT OF PROLONGED INTRAGASTRIC INFUSIONS OF ISOTONIC AND HYPERTONIC SALINE ON WATER AND SODIUM EXCRETION AND ON EXCHANGEABLE BODY SODIUM IN NORMAL AND ADRENALECTOMIZED RATS. By C. J. EDMONDS. From
THE EFFECT OF PROLONGED INTRAGASTRIC INFUSIONS OF ISOTONIC AND HYPERTONIC SALINE ON WATER AND SODIUM EXCRETION AND ON EXCHANGEABLE BODY SODIUM IN NORMAL AND ADRENALECTOMIZED RATS. By C. J. EDMONDS. From
Clinical interpretation of the plasma sodium concentration: a volume-tonicity chart
 IFCC/EWGISE Proceedings (ISBN 87 88138-) 1986; 7: 285-91 Clinical interpretation of the plasma sodium concentration: a volume-tonicity chart OLE SIGGAARD-ANDERSEN, NIELS FOGH-ANDERSEN AND PETER D. WIMBERLEY
IFCC/EWGISE Proceedings (ISBN 87 88138-) 1986; 7: 285-91 Clinical interpretation of the plasma sodium concentration: a volume-tonicity chart OLE SIGGAARD-ANDERSEN, NIELS FOGH-ANDERSEN AND PETER D. WIMBERLEY
that, in a dog maintained on moderate doses of
 OBSERVATIONS ON ADRENAL INSUFFICIENCY By JULES STAHL,' DANA W. ATCHLEY AND ROBERT F. LOEB (From the Department of Medicine, College of Physicians and Surgeons, Columnibia University, and the Presbyterian
OBSERVATIONS ON ADRENAL INSUFFICIENCY By JULES STAHL,' DANA W. ATCHLEY AND ROBERT F. LOEB (From the Department of Medicine, College of Physicians and Surgeons, Columnibia University, and the Presbyterian
Monday, 17 April 2017 BODY FLUID HOMEOSTASIS
 Monday, 17 April 2017 BODY FLUID HOMEOSTASIS Phenomenon: shipwrecked sailor on raft in ocean ("water, water everywhere but not a drop to drink") Why are the sailors thirsty? (What stimulated thirst?) Why
Monday, 17 April 2017 BODY FLUID HOMEOSTASIS Phenomenon: shipwrecked sailor on raft in ocean ("water, water everywhere but not a drop to drink") Why are the sailors thirsty? (What stimulated thirst?) Why
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
hold for the human kidney.2 Shannon and Smith (4) have rightfully stressed
 THE RENAL EXCRETION OF INULIN AT LOW PLASMA CONCEN- TRATIONS OF THIS COMPOUND, AND ITS RELATIONSHIP TO THE GLOMERULAR FILTRATION RATE IN NORMAL, NEPHRITIC AND HYPERTENSIVE INDIVIDUALS' By BENJAMIN F. MILLER,
THE RENAL EXCRETION OF INULIN AT LOW PLASMA CONCEN- TRATIONS OF THIS COMPOUND, AND ITS RELATIONSHIP TO THE GLOMERULAR FILTRATION RATE IN NORMAL, NEPHRITIC AND HYPERTENSIVE INDIVIDUALS' By BENJAMIN F. MILLER,
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Hospital, Boston, Mass.)
 THE NORMAL ANTDURETC MECHANSM N MAN AND DOG; TS REGULATON BY EXTRACELLULAR FLUD TONCTY 1, 2 By ALEXANDER LEAF 8 AND AUDLEY R. MAMBY (From the Departments of Medicine of Harvard Medical School and the Massachusetts
THE NORMAL ANTDURETC MECHANSM N MAN AND DOG; TS REGULATON BY EXTRACELLULAR FLUD TONCTY 1, 2 By ALEXANDER LEAF 8 AND AUDLEY R. MAMBY (From the Departments of Medicine of Harvard Medical School and the Massachusetts
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
BODY FLUID. Outline. Functions of body fluid Water distribution in the body Maintenance of body fluid. Regulation of fluid homeostasis
 BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
Plasma 17-Ketosteroids of Full-Term and Premature Infants
 Plasma 17-Ketosteroids of Full-Term and Premature Infants Lytt I. Gardner, R. Lee Walton J Clin Invest. 1954;33(12):1642-1645. https://doi.org/10.1172/jci103045. Research Article Find the latest version:
Plasma 17-Ketosteroids of Full-Term and Premature Infants Lytt I. Gardner, R. Lee Walton J Clin Invest. 1954;33(12):1642-1645. https://doi.org/10.1172/jci103045. Research Article Find the latest version:
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
NATURAL HISTORY AND SURVIVAL OF PATIENTS WITH ASCITES. PATIENTS WHO DO NOT DEVELOP COMPLICATIONS HAVE MARKEDLY BETTER SURVIVAL THAN THOSE WHO DEVELOP
 PROGNOSIS Mortality rates as high as 18-30% are reported for hyponatremic patients. High mortality rates reflect the severity of underlying conditions and are not influenced by treatment of hyponatremia
PROGNOSIS Mortality rates as high as 18-30% are reported for hyponatremic patients. High mortality rates reflect the severity of underlying conditions and are not influenced by treatment of hyponatremia
Use the following diagram to answer the next question. 1. In the diagram above, pressure filtration occurs in a. W b. X c. Y d. Z
 Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
of tubular reabsorption, was measured by inulin instead of creatinine clearances, and the quantity, of infusion fluid, expressed in relation to body
 THE RENAL EXCRETON OF CHLORDE AND WATER N DABETES NSPDUS By ROBERT C. HCKEY AND KENDRCK HARE (From the Departments of Surgery and Anatomy, State University of owa, otva City) (Received for publication
THE RENAL EXCRETON OF CHLORDE AND WATER N DABETES NSPDUS By ROBERT C. HCKEY AND KENDRCK HARE (From the Departments of Surgery and Anatomy, State University of owa, otva City) (Received for publication
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines
 Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines Author: Richard Pugh June 2015 Guideline for management of hyponatraemia in intensive care Background
Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines Author: Richard Pugh June 2015 Guideline for management of hyponatraemia in intensive care Background
All patients were well hydrated in order to obtain a. good urine flow.2 They were given a liter of water to
 URIC ACID CLEARANCE IN NORMAL PREGNANCY AND PRE-ECLAMPSIA1 By N. K SCHAFFER, L. V. DILL, AND J. F. CADDEN (From the Department of Obstetrics and Gynecology, Cornell University Medical College, and the
URIC ACID CLEARANCE IN NORMAL PREGNANCY AND PRE-ECLAMPSIA1 By N. K SCHAFFER, L. V. DILL, AND J. F. CADDEN (From the Department of Obstetrics and Gynecology, Cornell University Medical College, and the
14). Heparin (1 per cent) was used as an anticoagulant;
 THE MECHANISM OF THE EXCRETION OF VITAMIN C BY THE HUMAN KIDNEY 1 BY ELAINE P. RALLI, GERALD J. FRIEDMAN AND SAUL H. RUBIN (From the Department of Medicine, New York University College of Medicine, and
THE MECHANISM OF THE EXCRETION OF VITAMIN C BY THE HUMAN KIDNEY 1 BY ELAINE P. RALLI, GERALD J. FRIEDMAN AND SAUL H. RUBIN (From the Department of Medicine, New York University College of Medicine, and
Sodium Bicarbonate Injection, USP
 Sodium Bicarbonate Injection, USP FOR THE CORRECTION OF METABOLIC ACIDOSIS AND OTHER CONDITIONS REQUIRING SYSTEMIC ALKALINIZATION. Plastic Ansyr II Syringe R x only DESCRIPTION Sodium Bicarbonate Injection,
Sodium Bicarbonate Injection, USP FOR THE CORRECTION OF METABOLIC ACIDOSIS AND OTHER CONDITIONS REQUIRING SYSTEMIC ALKALINIZATION. Plastic Ansyr II Syringe R x only DESCRIPTION Sodium Bicarbonate Injection,
DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI Page 1 Page 2 syndrome of inappropriate secretion of antidiuretic hormone in malignancy
DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI Page 1 Page 2 syndrome of inappropriate secretion of antidiuretic hormone in malignancy
Mechanisms of Fluid and Electrolyte Retention in Experimental Preparations in Dogs
 Mechanisms of Fluid and Electrolyte Retention in Experimental Preparations in Dogs III. Effect of Adrenalectomy and Subsequent Desoxycorticosterone Acetate Administration on Ascites Formation By JAMES.
Mechanisms of Fluid and Electrolyte Retention in Experimental Preparations in Dogs III. Effect of Adrenalectomy and Subsequent Desoxycorticosterone Acetate Administration on Ascites Formation By JAMES.
INDICATORS OF POLYURIA AND POLYDIPSIA
 Horses rarely drink more than 5% of their bodyweight daily (25 litres per 500 kg) Horses rarely urinate more than 3% of their bodyweight daily (15 litres per 500 kg) The only common causes of PUPD are
Horses rarely drink more than 5% of their bodyweight daily (25 litres per 500 kg) Horses rarely urinate more than 3% of their bodyweight daily (15 litres per 500 kg) The only common causes of PUPD are
Major intra and extracellular ions Lec: 1
 Major intra and extracellular ions Lec: 1 The body fluids are solutions of inorganic and organic solutes. The concentration balance of the various components is maintained in order for the cell and tissue
Major intra and extracellular ions Lec: 1 The body fluids are solutions of inorganic and organic solutes. The concentration balance of the various components is maintained in order for the cell and tissue
1.2 Synonyms There are several synonyms e.g. diaminomethanal, but in a medical context, this substance is always referred to as urea.
 Urea (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Urea 1.2 Synonyms There are several synonyms e.g. diaminomethanal, but in a medical context, this substance is always referred
Urea (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Urea 1.2 Synonyms There are several synonyms e.g. diaminomethanal, but in a medical context, this substance is always referred
OF SERUM SODIUM CONCENTRATION
 Journal of Clinical Investigation Vol. 42, No. 5, 1963 STUDIES ON TASTE THRESHOLDS IN NORMAL MAN AND IN PATIENTS WITH ADRENAL CORTICAL INSUFFICIENCY: THE ROLE OF ADRENAL CORTICAL STEROIDS.AND OF SERUM
Journal of Clinical Investigation Vol. 42, No. 5, 1963 STUDIES ON TASTE THRESHOLDS IN NORMAL MAN AND IN PATIENTS WITH ADRENAL CORTICAL INSUFFICIENCY: THE ROLE OF ADRENAL CORTICAL STEROIDS.AND OF SERUM
to assess the renal reabsorptive capacity after restoration of normal carbon dioxide tension in
 Journal of Clinical nvestigation Vol. 41, No. 12, 1962 EFFECTS OF CHRONC HYPERCAPNA ON ELECTROLYTE AND ACD-BASE EQULBRUM.. CHARACTERSTCS OF THE ADAPTVE AND RECOVERY PROCESS AS EVALUATED BY PROVSON OF ALKAL
Journal of Clinical nvestigation Vol. 41, No. 12, 1962 EFFECTS OF CHRONC HYPERCAPNA ON ELECTROLYTE AND ACD-BASE EQULBRUM.. CHARACTERSTCS OF THE ADAPTVE AND RECOVERY PROCESS AS EVALUATED BY PROVSON OF ALKAL
LESSON ASSIGNMENT. Diuretic and Antidiuretic Agents. After you finish this lesson you should be able to:
 LESSON ASSIGNMENT SUBCOURSE MD0806 LESSON 8 Therapeutics III. Diuretic and Antidiuretic Agents. LESSON ASSIGNMENT Paragraphs 8-1--8-7. LESSON OBJECTIVES After you finish this lesson you should be able
LESSON ASSIGNMENT SUBCOURSE MD0806 LESSON 8 Therapeutics III. Diuretic and Antidiuretic Agents. LESSON ASSIGNMENT Paragraphs 8-1--8-7. LESSON OBJECTIVES After you finish this lesson you should be able
nephron alone does not account for the antidiuretic antidiuresis is enhanced by a low sodium intake.
 Journal of Clinical Investigation Vol. 41, No. 11, 1962 THE MECHANISM OF ANTIDIURESIS ASSOCIATED WITH THE ADMINISTRATION OF HYDROCHLOROTHIAZIDE TO PA- TIENTS WITH VASOPRESSIN-RESISTANT DIABETES INSIPIDUS
Journal of Clinical Investigation Vol. 41, No. 11, 1962 THE MECHANISM OF ANTIDIURESIS ASSOCIATED WITH THE ADMINISTRATION OF HYDROCHLOROTHIAZIDE TO PA- TIENTS WITH VASOPRESSIN-RESISTANT DIABETES INSIPIDUS
HYPOTHALAMIC ELECTRICAL ACTIVITIES PRODUCED BY FACTORS CAUSING DISCHARGE OF PITUITARY HORMONES
 HYPOTHALAMIC ELECTRICAL ACTIVITIES PRODUCED BY FACTORS CAUSING DISCHARGE OF PITUITARY HORMONES TERUO NAKAYAMA* Institute of Physiology, School of Medicine, University of Nagoya It is known that electrical
HYPOTHALAMIC ELECTRICAL ACTIVITIES PRODUCED BY FACTORS CAUSING DISCHARGE OF PITUITARY HORMONES TERUO NAKAYAMA* Institute of Physiology, School of Medicine, University of Nagoya It is known that electrical
DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE. Jules B. Puschett, M.D.
 DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE Jules B. Puschett, M.D. Diuretic Resistance A clinical circumstance in which patients do not respond to a combination of salt restriction and even large
DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE Jules B. Puschett, M.D. Diuretic Resistance A clinical circumstance in which patients do not respond to a combination of salt restriction and even large
1.7) (21, 22, 23); (2) this ratio is depressed towards
 DEPRESSION OF THE EXOGENOUS CREATININE/INULIN OR THIOSULFATE CLEARANCE RATIOS IN MAN BY DIODRAST AND p-aminohippuric ACID1 By BETTY CRAWFORD (From the Department of Physiology, New York University College
DEPRESSION OF THE EXOGENOUS CREATININE/INULIN OR THIOSULFATE CLEARANCE RATIOS IN MAN BY DIODRAST AND p-aminohippuric ACID1 By BETTY CRAWFORD (From the Department of Physiology, New York University College
(5), the presumed site of potassium secretion. RENAL EXCRETION OF POTASSIUM IN NORMAL AND SODIUM
 RENAL EXCRETION OF POTASSIUM IN NORMAL AND SODIUM DEPLETED DOGS' By HELEN M. ANDERSON AND JOHN H. LARAGH WITH THE TECHNICAL ASSISTANCE OF CLARA W. HALL, SALLY MOORE, AND JOSEPH HARTOG (From the Department
RENAL EXCRETION OF POTASSIUM IN NORMAL AND SODIUM DEPLETED DOGS' By HELEN M. ANDERSON AND JOHN H. LARAGH WITH THE TECHNICAL ASSISTANCE OF CLARA W. HALL, SALLY MOORE, AND JOSEPH HARTOG (From the Department
test. Urine was collected every 10 to 30 minutes over a period of approximately 3 hours. Typhoid vaccine (75,-
 THE URINARY EXCRETION OF SODIUM AND POTASSIUM DURING THE PYROGENIC REACTION IN MAN 1, 2 By WILLOUGHBY LATHEM 8 (From the Veterans Administration Hospital, West Haven, Connecticut, and The Department of
THE URINARY EXCRETION OF SODIUM AND POTASSIUM DURING THE PYROGENIC REACTION IN MAN 1, 2 By WILLOUGHBY LATHEM 8 (From the Veterans Administration Hospital, West Haven, Connecticut, and The Department of
potassium ratio and response to diuretics in
 Postgraduate Medical Journal (March 1977) 53, 117-121. Nineteen patients The urinary sodium : potassium ratio and response to diuretics in resistant oedema WILLIAM D. ALEXANDER* D. F. LEVINE R. A. BRANCHt
Postgraduate Medical Journal (March 1977) 53, 117-121. Nineteen patients The urinary sodium : potassium ratio and response to diuretics in resistant oedema WILLIAM D. ALEXANDER* D. F. LEVINE R. A. BRANCHt
Normosol -R and 5% Dextrose Injection MULTIPLE ELECTROLYTES AND 5% DEXTROSE INJECTION TYPE 1, USP For Replacing Acute Losses of Extracellular Fluid
 Normosol -R and 5% Dextrose Injection MULTIPLE ELECTROLYTES AND 5% DEXTROSE INJECTION TYPE 1, USP For Replacing Acute Losses of Extracellular Fluid R x only Flexible Plastic Container DESCRIPTION Normosol-R
Normosol -R and 5% Dextrose Injection MULTIPLE ELECTROLYTES AND 5% DEXTROSE INJECTION TYPE 1, USP For Replacing Acute Losses of Extracellular Fluid R x only Flexible Plastic Container DESCRIPTION Normosol-R
DISEASE. Bethesda, Md.) sistently correlated with the level of calcium or phosphate in the diet.
 RENAL REABSORPTION OF PHOSPHATE IN NORMAL HUMAN SUBJECTS AND IN PATIENTS WITH PARATHYROID DISEASE By DAVID D. THOMPSON 1 AND HOWARD H. HIATT 2 (From the National Institute of Arthritis and Metabolic Diseases,
RENAL REABSORPTION OF PHOSPHATE IN NORMAL HUMAN SUBJECTS AND IN PATIENTS WITH PARATHYROID DISEASE By DAVID D. THOMPSON 1 AND HOWARD H. HIATT 2 (From the National Institute of Arthritis and Metabolic Diseases,
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
THE PRESENT STUDY is concerned
 Mechanisms of Fluid and Electrolyte Retention in Experimental Preparations in Dogs II. With Thoracic Inferior Vena Cava Constriction By JAMES 0. DAVIS, PH.D., M.D., AND DAVID S. HOWELL, M.D. Cardiovascular
Mechanisms of Fluid and Electrolyte Retention in Experimental Preparations in Dogs II. With Thoracic Inferior Vena Cava Constriction By JAMES 0. DAVIS, PH.D., M.D., AND DAVID S. HOWELL, M.D. Cardiovascular
Basic Fluid and Electrolytes
 Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua
 Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua Assistant Professor Nephrology Unit, Department of Medicine College of Medicine,
Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua Assistant Professor Nephrology Unit, Department of Medicine College of Medicine,
J. Physiol. (I944) I02; :6I2.0I4.46I.2
 415 J. Physiol. (I944) I02; 45-428 612.463:6I2.0I4.46I.2 THE SECRETION OF URINE DURING DEHYDRATION AND REHYDRATION BY R. A. McCANCE AND W. F. YOUNG WITH THE ASSISTANCE OF D. A. K. BLACK From the Department
415 J. Physiol. (I944) I02; 45-428 612.463:6I2.0I4.46I.2 THE SECRETION OF URINE DURING DEHYDRATION AND REHYDRATION BY R. A. McCANCE AND W. F. YOUNG WITH THE ASSISTANCE OF D. A. K. BLACK From the Department
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Interrelationship between Angiotensin Catecholamines. Tatsuo SATO, M.D., Masaru MAEBASHI, M.D., Koji GOTO, M.D., and Kaoru YOSHINAGA, M.D.
 Interrelationship between Angiotensin and Catecholamines Tatsuo SATO, M.D., Masaru MAEBASHI, M.D., Koji GOTO, M.D., and Kaoru YOSHINAGA, M.D. SUMMARY Urinary catecholamines were measured with an attempt
Interrelationship between Angiotensin and Catecholamines Tatsuo SATO, M.D., Masaru MAEBASHI, M.D., Koji GOTO, M.D., and Kaoru YOSHINAGA, M.D. SUMMARY Urinary catecholamines were measured with an attempt
The Urinary System. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Patients studied and experimental procedures followed The patients studied in our experiments were 3 nephrotic
 THE RELATION OF HIGH AND LOW UREA CLEARANCES TO THE INULIN AND CREATININE CLEARANCES IN CHIL- DREN WITH THE NEPHROTIC SYNDROME BY KENDALL EMERSON, JR., PALMER H. FUTCHER, AND LEE E. FARR (From the Hospital
THE RELATION OF HIGH AND LOW UREA CLEARANCES TO THE INULIN AND CREATININE CLEARANCES IN CHIL- DREN WITH THE NEPHROTIC SYNDROME BY KENDALL EMERSON, JR., PALMER H. FUTCHER, AND LEE E. FARR (From the Hospital
Body water content. Fluid compartments. Regulation of water output. Water balance and ECF osmolallty. Regulation of water intake
 Body water content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; females 50% This difference reflects
Body water content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; females 50% This difference reflects
undertaken, (1) to determine the responses of a group of cirrhotics to administration of hypertonic salt solution under conditions of hydropenia when
 SALT RETENTION IN CIRRHOSIS OF THE LIVER' By ALLAN V. N. GOODYER, ARNOLD S. RELMAN, F. DOUGLAS LAWRASON,2 AND FRANKLIN H. EPSTEIN (From the Department of Inzternzal Medicinie, Yale Unizecrsity School of
SALT RETENTION IN CIRRHOSIS OF THE LIVER' By ALLAN V. N. GOODYER, ARNOLD S. RELMAN, F. DOUGLAS LAWRASON,2 AND FRANKLIN H. EPSTEIN (From the Department of Inzternzal Medicinie, Yale Unizecrsity School of
INTRAVENOUS FLUIDS PRINCIPLES
 INTRAVENOUS FLUIDS PRINCIPLES Postnatal physiological weight loss is approximately 5-10% Postnatal diuresis is delayed in Respiratory Distress Syndrome (RDS) Preterm babies have limited capacity to excrete
INTRAVENOUS FLUIDS PRINCIPLES Postnatal physiological weight loss is approximately 5-10% Postnatal diuresis is delayed in Respiratory Distress Syndrome (RDS) Preterm babies have limited capacity to excrete
Patterns of Sodium Excretion During Sympathetic Nervous System Arousal. Gregory A. Harshfield, Derrick A. Pulliam, and Bruce S.
 1156 Patterns of Sodium Excretion During Sympathetic Nervous System Arousal Gregory A. Harshfield, Derrick A. Pulliam, and Bruce S. Alpert The purpose of this study was to examine Na + handling and regulation
1156 Patterns of Sodium Excretion During Sympathetic Nervous System Arousal Gregory A. Harshfield, Derrick A. Pulliam, and Bruce S. Alpert The purpose of this study was to examine Na + handling and regulation
INTRAVENOUS FLUID THERAPY
 INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
45779C/Revised: April 2008 MANNITOL INJECTION, USP
 45779C/Revised: April 2008 MANNITOL INJECTION, USP 25% For Intravenous Use and Urologic Irrigation DESCRIPTION: Mannitol is a 6-carbon sugar alcohol and has the following structure: C 6 H 14 O 6 182.17
45779C/Revised: April 2008 MANNITOL INJECTION, USP 25% For Intravenous Use and Urologic Irrigation DESCRIPTION: Mannitol is a 6-carbon sugar alcohol and has the following structure: C 6 H 14 O 6 182.17
The Art and Science of Diuretic therapy
 The Art and Science of Diuretic therapy Dr. Fayez EL Shaer Associate Professour of cardiology Consultant cardiologist MD, MSc, PhD, CBNC, NBE FESC, ACCP, FASNC,HFA KKUH, KFCC Heart failure: fluid overload
The Art and Science of Diuretic therapy Dr. Fayez EL Shaer Associate Professour of cardiology Consultant cardiologist MD, MSc, PhD, CBNC, NBE FESC, ACCP, FASNC,HFA KKUH, KFCC Heart failure: fluid overload
After studying this lecture, you should be able to...
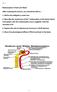 Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
The Urinary System 15PART B. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
Medicine, Cambridge, England, and Wuppertal, B.A.O.R.
 182 J. Physiol. (I948) I07, i82-i86 6I2.46I.62 PHOSPHATE CLEARANCES IN INFANTS AND ADULTS BY R. F. A. DEAN AND R. A. McCANCE From the Medical Research Council, Department. of Experimental Medicine, Cambridge,
182 J. Physiol. (I948) I07, i82-i86 6I2.46I.62 PHOSPHATE CLEARANCES IN INFANTS AND ADULTS BY R. F. A. DEAN AND R. A. McCANCE From the Medical Research Council, Department. of Experimental Medicine, Cambridge,
