Effect of varying water intake on renal function in healthy preterm babies
|
|
|
- Abraham Webb
- 6 years ago
- Views:
Transcription
1 Archives of Disease in Childhood, 1985, 6, Effect of varying water intake on renal function in healthy preterm babies M G COULTHARD AND E N HEY Department of Child Health, Princess Mary Maternity Hospital, Newcastle upon Tyne SUMMARY Renal control of water and electrolyte homeostasis was studied in 1 healthy babies (gestation 29 to 34 weeks; birthweight 1-19 to 2-19 kg) while water intake was varied. Glomerular filtration rate and urine flow were estimated daily from spot plasma and urine samples for six days using a constant inulin infusion, and simultaneous sodium, potassium, osmolar, and free water clearances were calculated. The infusion was started at an average age of 14 hours. Each baby received a total fluid intake of 96 ml/kg daily on study days 1, 2, and 5, and about 2 ml/kg on study days 3, 4, and 6. Daily sodium intake was kept constant at 3 mmollkg. At the end of the first study day the babies were undergoing a diuresis, but thereafter their estimated daily water balances remained stable regardless of intake. Glomerular filtration remained stable; alterations in urine flow reflected a change in the percentage of filtrate excreted. Plasma electrolytes and osmolality were stable throughout, and on study days 2 to 6 the urinary excretion rates of sodium, potassium, and other osmoles remained the same regardless of urine flow. The delivery of sodium to the distal tubule was estimated to be between 17 and 2% of the filtered load. Well preterm babies can cope with daily water intakes between 96 and 2 mvlkg from the third day of life. Until about 2 years ago it was standard practice to withhold virtually all fluid during the first 2 to 4 days of life. 1 In 1964 it was shown that early feeding could prevent hypoglycaemia,2 and six years later it was shown that restricting early feeds could lead to poor brain growth.3 Since then there has been a trend towards giving more fluid, especially to the smallest infants. Recently, however, it has been suggested that there may be a swing back towards older practices.4 Two factors have influenced this more cautious approach. Firstly, it has been suggested that there may be a link between a high fluid intake and the development of problems such as necrotising enterocolitis and cardiac failure associated with a patent ductus arteriosus.5 Secondly, some authors have implied that preterm babies are unable to tolerate such large fluid intakes without becoming overloaded with water6 or losing appreciable amounts of sodium in the urine.6 7We have therefore studied 1 healthy preterm infants during sustained periods of both low and high rates of fluid intake while their sodium intakes were kept constant, each baby thus acting as its own control. Patients and methods Patients. Ten healthy preterm infants (Table) were studied with fully informed parental consent and with the approval of the local ethical committee. All had birthweights above the fifth centile for their gestational age. Babies 8 and 9 were twins. Baby 4 developed clinical signs of a patent ductus arteriosus on the sixth day of life which resolved by the 1th day. Three infants received five day courses of penicillin and gentamicin because of prolonged rupture of membranes, but no other drugs were administered. All the babies were nursed in incubators at an ambient water vapour pressure of 4 to 5 kpa. Study design. The study protocol lasted six days, starting an average of 14 hours after birth. Observations on three babies were stopped early because they no longer required intravenous fluids. A low total fluid intake (mean 96 ml/kg) was given on the first two and the fifth study days, and a high total intake (mean 2 ml/kg) on the third, fourth, and sixth days. These intakes fell within the ranges 614 Arch Dis Child: first published as /adc on 1 July Downloaded from on 26 April 218 by guest. Protected by copyright.
2 Table Study details Effect of varying water intake on renal function in healthy preterm babies 615 Case Gestation Birthweight Age at onset Water intakes Sodium intakes Study days completed no (weeks) (gm) of infusion (mllkg per day) (mmollkg per day) (1, 2, 5 =low days (days) 3, 4, 6=high days) Low High Low High days days days days ) () 3-) ( ) () Means Low High Low days, fluid intake='96 mi/kg; high days, fluid intake-2 ml/kg. normally prescribed at that time for healthy preterm babies in the newborn nurseries in Newcastle. Each day the volume of oral fluid (SMA Gold Cap) was decided by the clinical staff, and it was increased gradually over the study. The balance was provided intravenously as dextrose solution with added sodium chloride, which was adjusted to provide a total daily sodium intake of about 3 mmol/kg (Table) regardless of their fluid intakes. Measurements. At the end of each study day, the glomerular filtration rate and urine flow rate were estimated from plasma and urine inulin concentrations after prolonged inulin infusion.8 A solution of inulin in water (25 mg/ml) was infused throughout the entire study period, using a syringe pump set to deliver 15 mg/kg per hour. Plasma samples were taken by heelprick before the study began and daily thereafter; small aliquots of urine were collected at the same time from a plastic nappy liner. Inulin concentrations were assayed as previously described in triplicate on 1 R1 samples of plasma, of diluted urine, or of infusate.8 Glomerular filtration rate was calculated from the inulin infusion rate divided by the plasma inulin concentration, and urine flow rate from the inulin infusion rate divided by the urine inulin concentration. If the inulin infusion was stopped during the resiting of an intravenous cannula, a period of infusion at least six times the duration of the interval was allowed before further samples were taken. Because of this restriction samples were not collected on two occasions (cases 6 and 7). Osmolality was measured on 2 RI samples of plasma and urine by depression of freezing point, and free water clearance was calculated by subtracting the osmolar clearance from the urine flow. Sodium and potassium concentrations were measured in duplicate on 1,ud samples by flame photometry. In each case the coefficient of variation of the estimation was less than one per cent. Filtered loads of substances were calculated as the product of their plasma concentrations and glomerular filtration rate, excretion rates as the product of their urine concentrations and urine flow rate, and -fractional excretion values as their excretion rates divided by their filtration rates. Clearance data were expressed per kg9 birthweight until the babies had exceeded this, and of body weight thereafter. Data from each study day were compared with those from other study days using paired t tests, and data from combinations of study days were compared with those from other days using grouped t tests. Unless stated, the P values given refer to grouped t tests. Results All the babies were in negative water balance at the end of the first study day, but not subsequently. Thus, only data from 2 to 6 are considered in the first two results sections, and the diuresis seen on the first day is considered separately in the next section. Water balance. The estimated daily water balance (excluding insensible and stool losses) averaged + 15 ml/kg on days 2 to 6, and there were no significant differences between any of these days or groups of days. Thus, allowing for unmeasured losses, the babies seemed to have achieved stable water balance by making appropriate adjustments to urine flow by the third day of life (Fig. 1). Alterations in urine flow were the result of variations in the Arch Dis Child: first published as /adc on 1 July Downloaded from on 26 April 218 by guest. Protected by copyright.
3 616 Coulthard and Hey fraction of filtered water that was excreted and not due to changes in glomerular filtration rate (Fig. 2). The percentage excretion of filtrate was mean (SD), 7.4 (3.5)% on days 2 and 5, which was much lower than the 13-1 (3-6)% seen on high volume days '- IuuW, 's 1~. i. E E E _9 --i2 1'/2 2V2 3P2 4/' /2 Age (days) Fig. 1 Fluid intake and estimated urine volume and water balance plottedfor each study day. Bars represent ±SD values. *P<-2 that estimated fluid balance on first study day is less than on study days 2 to 'aa *s 1- c 5- GD L OJ -W%^ II I1/2 '- m 6 3 O2 L H H L H Highorlbw vdume day /2 41/2 5V2 6/2 Age (days) Fig. 2 Percentage excretion ofglomerularfiltrate and glomerularfiltration rate (GFR) plotted as mean (SD) for each study day. 1-2 r1. (P<1). Glomerular filtration rate averaged 92 ml/kg per min overall. Although the means were slightly higher on the high volume days, and towards the end of the study, these differences were not significant. Sodium, potassium, and osmolar balance. The osmolality and sodium and potassium concentrations of plasma were stable throughout the entire study period, being unaffected by postnatal age or fluid intake (Fig. 3(a)). Similarly, from days 2 to 6 there were no differences in the urinary excretion rates of sodium, potassium or of other osmoles between the high and low intake days (Fig. 3(b)), the excretion of 'other osmoles' being calculated as the osmolar excretion rate -2 (sodium + potassium excretion rates). Thus on high volume days, with a high urine flow rate but a similar solute excretion rate, the urine was more dilute with respect to osmolality, sodium, and potassium than on low volume days (P<1 in each case) (Fig. 3(c)). Early diuresis. The estimated fluid balance at the end of the first study day (mean age 38 hours) was -42 ml/kg, significantly less than during the rest of the study (P<2) (Fig. 1). Compared with the other days on a low fluid intake, the glomerular filtration rate was similar, but the percentage excretion of filtered water was higher, at mean (SD) 1O8 (3.8)% (P<5) (Fig. 2). Sodium excretion was lowest and potassium excretion highest at the end of day 1 (for each ion, P<5 compared with days 2 to 6) (Fig. 3(b)). Thus the sodium:potassium concentration ratio in the urine was significantly lower on the first than on any other study day (P<5, paired t test). The excretion rate of the other osmoles was also higher on study day 1 than on either the other low volume days 2 and 5 (P<-2) or study days 2 to 6 (P<5) (Fig. 3(b)). Thus, at mean age 38 hours these babies were undergoing a diuresis which was associated with an excess loss of potassium and other osmoles, but not of sodium. 'Distal tubular sodium delivery'. Under conditions of maximal diuresis, when very little water is reabsorbed in the distal tubule, the delivery of sodium by the proximal tubule is approximately equal to the sum of the sodium and free water clearances multiplied by the plasma sodium concentration.1 During antidiuresis this value will be a considerable underestimate because more water will be reabsorbed in the distal segment. The logarithm of the fractional delivery of filtrate to the distal tubule (the sum of the sodium and free water Arch Dis Child: first published as /adc on 1 July Downloaded from on 26 April 218 by guest. Protected by copyright.
4 Effect of varying water intake on renal function in healthy preterm babies 617 Sodium (mmol/1) o~~~ N. o o ^~~~ I N *WW I~~~~~~~~~~( /" Ie (6)1/wsow) Aplulowso wnissdoco. E -> ND o o U on on + -, + I ^ InC V a O (1/wsow ) A6i1oiowsO WflSSDOd,/ww o ~ ~~S In C n I I UAo /OWW) /~ ~ / I > A IIO, WSO Jn4SDw n i pos w s (4/ WSOW) ig so1owso.j (mmol/o sss t + In eo CD J. 'In T (n - (6/s* 41 1w OPt lux4.n.o. Arch Dis Child: first published as /adc on 1 July Downloaded from on 26 April 218 by guest. Protected by copyright.
5 618 Coulthard and Hey - 3 IL 81 E a) c u N * lb * 8% ', *e r= 83 P < 1 y=11l 4--38x.4~~~~~~~~~~~ Urine osmololity (mosm/ kg) Fig. 4 Regression of the sum ofsodium andfree water clearances (ml/loo ml ofglomerular filtration rate (GFR)) on the urine osmolality (mosmlkg). Note that the vertical scale is logarithmic. clearances expressed per 1 ml of glomerular filtration rate) was negatively correlated with urine osmolality (Fig. 4). Discussion This is the first study of fluid homeostasis in the healthy preterm baby in which water was the only factor altered and in which babies acted as their own controls.6 7 We have shown that there is an early diuresis after birth, and that fluid balance is subsequently maintained over a wide range of water intakes. We have also shown that the glomerular filtration rate changes little between 38 hours and 7 days of age, and is not influenced by the volume of water taken; changes in urine flow reflect adjustments to the proportion of water reabsorbed in the tubules. Early diuresis. A shortcoming of our study is the lack of data in the first 38 hours, due to the method used to measure glomerular filtration rate and urine flow. Evidence, however, that the babies underwent a diuresis comes from their early weight loss (4 to 16%) and their negative water balance at 38 hours. Others have concluded7 that the early diuresis is a controlled physiological event because wide variations in fluid intake have a relatively small effect on the amount of weight lost. This even seems to apply when infants are starved,' although the small volume of concentrated urine which they then pass has been shown to relate to the osmolar excretion rate. I It is widely assumed that sodium is the main ion lost during the physiological diuresis, as the loss of body fluid is mainly from the extracellular compartment.12 We saw a relatively higher potassium excretion rate on the second postnatal day, as did McCance and Widdowson in starved infants." It may be that the babies had excreted more sodium before we began making measurements, or that they were born potassium replete, were losing intracellular water, or were catabolic. Electrolyte balances in the first two days of life need further investigation. Maintenance of water balance. The positive fluid balance of 15 ml/kg per day which the infants maintained from the third day of life is close to the insensible losses expected in healthy infants of their age and gestation nursed in high humidity.13 The maintenance of such a balance despite varying water intake was not mediated by changes in the glomerular filtration rate. Although young rats given infusions of salt and water to achieve acute volume expansion may experience an increase in glomerular filtration rate and a fall in renal vascular resistance,'4 there is no reason to believe that a maintained increase in water intake alone would have a similar effect. The only human study which claims such an effect6 measured glomerular filtration by an invalid technique8 after brief fluid infusions were administered to different babies with widely varying backgrounds of salt and water intake. The fraction of the glomerular filtrate that appears as urine is much higher than in adult life: this is an inevitable consequence of the higher fluid turnover and the lower glomerular filtration rate/kg in babies. Similar values have previously been interpreted as providing evidence of osmotic diuresis.'5 Even when the urine osmolality fell, however, to 45 mosm/kg in the present study there was no evidence that a maximal diuresis had been achieved; neither the osmolar excretion rate nor the plasma osmolality changed. When the urine osmolality was as low as 45 mosm/kg, the mean value for the sum of the sodium and free water clearances was 16-9% of the glomerular filtration rate (Fig. 4). Under conditions of maximal water diuresis this figure may be assumed to approximately equal the percentage of filtered sodium delivered to the distal tubule.1 Assuming a maximally dilute urine to have an osmolality between 35 and 45 mosm/kg, the distal sodium delivery in our infants would be between 17 and 2% of the glomerular filtrate; this is similar to that reported for older infants,'( but higher than claimed for newborns.'6 In the latter study, how- Arch Dis Child: first published as /adc on 1 July Downloaded from on 26 April 218 by guest. Protected by copyright.
6 Effect of varying water intake on renal function in healthy preterm babies 619 ever, maximum urine flow was assumed to have been reached at urine osmolalities of around 15 mosm/kg. Figure 4 illustrates the size of the error caused by this assumption. From a knowledge of the glomerular filtration rate in preterm infants9 and of the fractional distal sodium delivery, it may be estimated that the smallest subjects are likely to have an upper limit for urine flow of about 7 ml/kg per hour, whereas the larger babies may achieve double this rate. The most immature infants may therefore be expected to excrete a fluid bolus more slowly, and to be at the greatest risk from fluid overload. It has been shown, however, that the peak urine flow of mature infants given water load is the same as in adults when the results are expressed per unit of body water.'7 It should also be noted that some of the widely accepted evidence suggesting that newborns excrete only a small fraction of a water-load'8 was obtained in infants who may have been dehydrated1 because of the then standard practice of giving only minimal fluids for the first few days of life. Sodium balance at high urine flow. The sodium balance of our infants remained negative throughout their first week of life, as reported by others.'9 It was completely unaffected by urine flow, which is at variance with the findings of Leake et al.6 Problems with the experimental design of the latter study have already been discussed. In addition, recalculation of their statistics for fractional sodium excretion under high and low fluid conditions shows that the difference claimed is not significant (P> *5, t test). The immature kidney is capable of producing dilute urine, and of concentrating up to 6 mosm/ kg in the presence of a normal plasma urea. As long as urine osmolality is kept well within these limits there is no reason to expect a change in urine flow to influence sodium excretion. The widely held view that a high urine flow in a preterm infant will cause an excess loss of sodium,4 2 and the recommendation that extra salt be given to compensate for this2 are without foundation. Recommended fluid intakes. Attempts to produce guidelines for precise fluid requirements in babies are complicated by the number of factors that can influence non-renal water losses.'3 These include gestation and postnatal age, ambient humidity and the use of radiant heaters and phototherapy lamps, as well as pathology such as diarrhoea and some skin disorders. On the basis of our data we question the need for guidelines and special allowances in healthy preterm babies because we have shown that they cope with a wide range of fluid intakes without stressing either their diluting or concentrating capacities. If there were any doubt whether a particular fluid regimen was causing either over hydration or dehydration, a check that the urine osmolality lay in the range 8 to 4 mosm/kg would confirm that the kidneys were working well within the limits of their homeostatic capabilities. Because our babies coped with a daily fluid intake of 2 ml/kg (once the initial diuresis was over) in conditions that allow only minimal insensible losses, it is likely that this volume would be tolerated by healthy preterm infants under most conditions from the third postnatal day. This intake, however, may not be appropriate for babies with respiratory distress; their increased incidence of necrotising enterocolitis and of heart failure complicating patent ductus arteriosus5 may be related in part to the amount of water (or sodium) that they are given. Conclusions This study indicates that healthy preterm infants are capable of exercising close control of water homeostasis over a wide range of intakes, and that this is not mediated through a change in the glomerular filtration rate and has no effect on renal sodium handling. It is suggested that fluid intakes in well preterm babies should be guided more by the urine osmolality achieved than by fixed schedules, and that a daily intake of 2 ml/kg is likely to be well tolerated from the third day. We thank the nursing staff of the neonatal unit, Mrs Valerie Ruddock for skilled technical assistance, and Mrs Marjorie Renwick for her secretarial help. This was supported by MRC Project Grant References Cornblath M, Forbes AE, Pildes RS, Leubben G, Greengard J. A controlled study of early fluid administration on survival of low birth weight infants. Pediatrics 1966;38: Smallpiece V, Davies PA. Immediate feeding of premature infants with undiluted breast milk. Lancet 1964;ii: Davies PA, Davis JP. Very low birth-weight and subsequent head growth. Lancet 197;ii: Anonymous. Fluid therapy in the neonate-concepts in transition. J Pediatr 1982;11: Bell EF, Warburton D, Stonestreet BS, Oh W. Effect of fluid administration on the development of symptomatic patent ductus arteriosus and congestive heart failure in premature infants. N Engl J Med 198;32: Leake RD, Zakauddin S, Trygstad CW, Fu P, Oh W. The effects of large volume intravenous fluid infusion on neonatal renal function. J Pediatr 1976;89: Lorenz JM, Kleinman LI, Kotagal UR, Reller MD. Water balance in very low-birth-weight infants: relationship to water and sodium intake and effect on outcome. J Pediatr 1982;11: Coulthard MG. Comparison of methods of measuring renal function in preterm babies using inulin. J Pediatr 1983;12: Arch Dis Child: first published as /adc on 1 July Downloaded from on 26 April 218 by guest. Protected by copyright.
7 62 Coulthard and Hey Coulthard MG, Hey EN. Weight as the best standard for glomerular filtration in the newborn. Arch Dis Child 1984;59: '1 Rodriguez-Soriano J, Vallo A, Castillo G, Oliveros R. Renal handling of water and sodium in infancy and childhood: a study using clearance methods during hypotonic saline diuresis. Kidney Int 1981;2:7-4. McCance RA, Widdowson EM. Normal renal function in the first two days of life. Arch Dis Child 1954;29: Friiss-Hansen B. Body water compartments in children: changes during growth and related changes in body composition Pediatri 1961;28: Thompson MH, Stothers JK, McLellan NJ. Weight and water loss in the neonate in natural and forced convection. Arch Dis Child 1984;59: Elinder G, Aperia A, Herin P, Kallskog. Effect of isotonic volume expansion on glomerular filtration rate and renal hemodynamics in the developing rat kidney. Acta Physiol Scand 198;18: '5 Stonestreet BS, Rubin L, Pollak A, Cowett RM, Oh W. Renal functions of low birth weight infants with hyperglycemia and glucosuria produced by glucose infusions. Pediatrics 198;66: Sulyok E, Varga F, Gyory E, Jobst K, Csaba IF. On the mechanisms of renal sodium handling in newborn infants. Biol Neonate 198;37: McCance RA, Naylor NJB, Widdowson EM. The response of infants to a large dose of water. Arch Dis Child 1954;29: Ames RG. Urinary water excretion and neurohypophysial function in full term and premature infants shortly after birth. Pediatrics 1952;12: Al-Dahhan J, Haycock GB, Chantler C, Stimmler L. Sodium homeostasis in term and preterm neonates: 1 Renal aspects. Arch Dis Child 1983;58: ) Leake RD. Perinatal nephrobiology: a developmental perspective. Clin Perinatol 1977;4: Correspondence (no reprints available) to Dr M G Coulthard, Department of Child Health, Royal Victoria Infirmary, Newcastle upon Tyne NEI 4LP. Received 4 February 1985 Arch Dis Child: first published as /adc on 1 July Downloaded from on 26 April 218 by guest. Protected by copyright.
INTRAVENOUS FLUID THERAPY
 INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
INTRAVENOUS FLUIDS PRINCIPLES
 INTRAVENOUS FLUIDS PRINCIPLES Postnatal physiological weight loss is approximately 5-10% Postnatal diuresis is delayed in Respiratory Distress Syndrome (RDS) Preterm babies have limited capacity to excrete
INTRAVENOUS FLUIDS PRINCIPLES Postnatal physiological weight loss is approximately 5-10% Postnatal diuresis is delayed in Respiratory Distress Syndrome (RDS) Preterm babies have limited capacity to excrete
Satellite Symposium. Sponsored by
 Satellite Symposium Sponsored by Management of fluids and electrolytes in the preterm infant in the first week of life Pam Cairns St Michaels Hospital Bristol Healthy, term, breast fed babies Limited intake
Satellite Symposium Sponsored by Management of fluids and electrolytes in the preterm infant in the first week of life Pam Cairns St Michaels Hospital Bristol Healthy, term, breast fed babies Limited intake
Renal processing of glucose in well and sick neonates
 F92 Department of Child Health Royal Victoria Infirmary Newcastle upon Tyne NE1 4LP M G Coulthard E N Hey Correspondence to: Dr M G Coulthard. Accepted 7 April 1999 Renal processing of glucose in well
F92 Department of Child Health Royal Victoria Infirmary Newcastle upon Tyne NE1 4LP M G Coulthard E N Hey Correspondence to: Dr M G Coulthard. Accepted 7 April 1999 Renal processing of glucose in well
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
Sodium homeostasis in term and preterm neonates
 Archives of Disease in Childhood, 1983, 58, 335-342 Sodium homeostasis in term and preterm neonates Renal aspects J AL-DAHHAN, G B HAYCOCK, C CHANTLER, AND L STMMLER Evelina Department ofpaediatrics, Guy's
Archives of Disease in Childhood, 1983, 58, 335-342 Sodium homeostasis in term and preterm neonates Renal aspects J AL-DAHHAN, G B HAYCOCK, C CHANTLER, AND L STMMLER Evelina Department ofpaediatrics, Guy's
Management of Acute Kidney Injury in the Neonate. Carolyn Abitbol, M.D. University of Miami Miller School of Medicine / Holtz Children s Hospital
 Management of Acute Kidney Injury in the Neonate Carolyn Abitbol, M.D. University of Miami Miller School of Medicine / Holtz Children s Hospital Objectives Summarize the dilemmas in diagnosing & recognizing
Management of Acute Kidney Injury in the Neonate Carolyn Abitbol, M.D. University of Miami Miller School of Medicine / Holtz Children s Hospital Objectives Summarize the dilemmas in diagnosing & recognizing
Fluid & Electrolyte Balances in Term & Preterm Infants. Carolyn Abitbol, M.D. University of Miami/ Holtz Children s Hospital
 Fluid & Electrolyte Balances in Term & Preterm Infants Carolyn Abitbol, M.D. University of Miami/ Holtz Children s Hospital Objectives Review maintenance fluid & electrolyte requirements in neonates Discuss
Fluid & Electrolyte Balances in Term & Preterm Infants Carolyn Abitbol, M.D. University of Miami/ Holtz Children s Hospital Objectives Review maintenance fluid & electrolyte requirements in neonates Discuss
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Neonatal Fluid Therapy Not my mother s physiology!!
 Neonatal Fluid Therapy Not my mother s physiology!! Physiologic Approach to Neonatal Fluid Therapy General principles of fluid balance Fetal physiology of fluid balance Neonatal physiology of fluid balance
Neonatal Fluid Therapy Not my mother s physiology!! Physiologic Approach to Neonatal Fluid Therapy General principles of fluid balance Fetal physiology of fluid balance Neonatal physiology of fluid balance
Basic Fluid and Electrolytes
 Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Diuretic Use in Neonates
 Neonatal Nursing Education Brief: Diuretic Use in the Neonate http://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/ Diuretics
Neonatal Nursing Education Brief: Diuretic Use in the Neonate http://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/ Diuretics
et al., 1963; Fisher et al., 1963), only those premature University Obstetric Department, 13 premature infants
 Arch. Dis. Childh., 1965, 4, 291. THE OSMOTIC CONCENTRATING ABILITY IN HEALTHY INFANTS AND CHILDREN BY E. POLACEK, J. VOCEL, L. NEUGEBAUEROVA, M. 9EBKOVA, and E. VECHETOVA with the technical co-operation
Arch. Dis. Childh., 1965, 4, 291. THE OSMOTIC CONCENTRATING ABILITY IN HEALTHY INFANTS AND CHILDREN BY E. POLACEK, J. VOCEL, L. NEUGEBAUEROVA, M. 9EBKOVA, and E. VECHETOVA with the technical co-operation
Renal Function in Preterm Neonates
 0031-3998/94/3605-0572$03.00/0 PEDIATRIC RESEARCH Copyright O 1994 International Pediatric Research Foundation, Inc. Vol. 36, No. 5, 1994 Printed in U.S.A. Renal Function in Preterm Neonates A. BUEVA AND
0031-3998/94/3605-0572$03.00/0 PEDIATRIC RESEARCH Copyright O 1994 International Pediatric Research Foundation, Inc. Vol. 36, No. 5, 1994 Printed in U.S.A. Renal Function in Preterm Neonates A. BUEVA AND
BIOL 2402 Renal Function
 BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
Ch 17 Physiology of the Kidneys
 Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
NATURAL HISTORY AND SURVIVAL OF PATIENTS WITH ASCITES. PATIENTS WHO DO NOT DEVELOP COMPLICATIONS HAVE MARKEDLY BETTER SURVIVAL THAN THOSE WHO DEVELOP
 PROGNOSIS Mortality rates as high as 18-30% are reported for hyponatremic patients. High mortality rates reflect the severity of underlying conditions and are not influenced by treatment of hyponatremia
PROGNOSIS Mortality rates as high as 18-30% are reported for hyponatremic patients. High mortality rates reflect the severity of underlying conditions and are not influenced by treatment of hyponatremia
NUTRITIONAL REQUIREMENTS
 NUTRITION AIMS To achieve growth and nutrient accretion similar to intrauterine rates To achieve best possible neurodevelopmental outcome To prevent specific nutritional deficiencies Target population
NUTRITION AIMS To achieve growth and nutrient accretion similar to intrauterine rates To achieve best possible neurodevelopmental outcome To prevent specific nutritional deficiencies Target population
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Disorders o f of water water Detlef Bockenhauer
 Disorders of water Detlef Bockenhauer How do we measure water? How do we measure water? Not directly! Reflected best in Na concentration Water overload => Hyponatraemia Water deficiency => Hypernatraemia
Disorders of water Detlef Bockenhauer How do we measure water? How do we measure water? Not directly! Reflected best in Na concentration Water overload => Hyponatraemia Water deficiency => Hypernatraemia
For more information about how to cite these materials visit
 Author(s): Michael Heung, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Michael Heung, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Sodium intake and preterm babies
 Archives of Disease in Childhood 1993; 69: 87-91 87 CURRENT TOPIC Department of Paediatrics and Neonatal Medicine, Royal Postgraduate Medicine School, Du Cane Road, London W12 ONN Correspondence to: Dr
Archives of Disease in Childhood 1993; 69: 87-91 87 CURRENT TOPIC Department of Paediatrics and Neonatal Medicine, Royal Postgraduate Medicine School, Du Cane Road, London W12 ONN Correspondence to: Dr
Applications of Freezing Point Osmometry
 Applications of Freezing Point Osmometry Table of Contents Chapter 1 Introduction and Basic Principles 1 Chapter 2 Biological Applications 3 2.1 Range of, and reason for, abnormal serum values 5 2.2 Osmolality
Applications of Freezing Point Osmometry Table of Contents Chapter 1 Introduction and Basic Principles 1 Chapter 2 Biological Applications 3 2.1 Range of, and reason for, abnormal serum values 5 2.2 Osmolality
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick Neonatal Pharmacist
 CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
Terminology. Terminology. Terminology. Molarity number of moles of solute / Liter of solution. a) Terminology b) Body Fluid Compartments
 Integrative Sciences: Biological Systems A Fall 2011 Body Fluids Compartments, Renal Clearance and Renal Excretion of Drugs Monday, November 21, 2011 Lisa M. Harrison-Bernard, Ph.D. Department of Physiology;
Integrative Sciences: Biological Systems A Fall 2011 Body Fluids Compartments, Renal Clearance and Renal Excretion of Drugs Monday, November 21, 2011 Lisa M. Harrison-Bernard, Ph.D. Department of Physiology;
DBL MAGNESIUM SULFATE CONCENTRATED INJECTION
 DBL MAGNESIUM SULFATE CONCENTRATED INJECTION NAME OF MEDICINE Magnesium Sulfate BP DESCRIPTION DBL Magnesium Sulfate Concentrated Injection is a clear, colourless, sterile solution. Each ampoule contains
DBL MAGNESIUM SULFATE CONCENTRATED INJECTION NAME OF MEDICINE Magnesium Sulfate BP DESCRIPTION DBL Magnesium Sulfate Concentrated Injection is a clear, colourless, sterile solution. Each ampoule contains
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Randomised controlled trial of postnatal sodium supplementation on body composition in 25 to 30 week gestational age infants
 F24 Section of Paediatrics and Neonatal Medicine, Imperial College School of Medicine, Hammersmith Hospital, London W12 0NN G Hartnoll N Modi P Bétrémieux Correspondence to: Dr Neena Modi Email: nmodi@ic.ac.uk
F24 Section of Paediatrics and Neonatal Medicine, Imperial College School of Medicine, Hammersmith Hospital, London W12 0NN G Hartnoll N Modi P Bétrémieux Correspondence to: Dr Neena Modi Email: nmodi@ic.ac.uk
Functions of Proximal Convoluted Tubules
 1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
Acid Base Balance. Professor Dr. Raid M. H. Al-Salih. Clinical Chemistry Professor Dr. Raid M. H. Al-Salih
 Acid Base Balance 1 HYDROGEN ION CONCENTRATION and CONCEPT OF ph Blood hydrogen ion concentration (abbreviated [H + ]) is maintained within tight limits in health, with the normal concentration being between
Acid Base Balance 1 HYDROGEN ION CONCENTRATION and CONCEPT OF ph Blood hydrogen ion concentration (abbreviated [H + ]) is maintained within tight limits in health, with the normal concentration being between
Medicine, Cambridge, England, and Wuppertal, B.A.O.R.
 182 J. Physiol. (I948) I07, i82-i86 6I2.46I.62 PHOSPHATE CLEARANCES IN INFANTS AND ADULTS BY R. F. A. DEAN AND R. A. McCANCE From the Medical Research Council, Department. of Experimental Medicine, Cambridge,
182 J. Physiol. (I948) I07, i82-i86 6I2.46I.62 PHOSPHATE CLEARANCES IN INFANTS AND ADULTS BY R. F. A. DEAN AND R. A. McCANCE From the Medical Research Council, Department. of Experimental Medicine, Cambridge,
Guidelines for the Prevention and Management of Hypoglycaemia
 ASHFORD & ST PETER S HOSPITALS NHS TRUST CHILDREN S SERVICES Guidelines for the Prevention and Management of Hypoglycaemia 1. The Care Plan for Prevention of Hypoglycaemia on Labour Ward and the Postnatal
ASHFORD & ST PETER S HOSPITALS NHS TRUST CHILDREN S SERVICES Guidelines for the Prevention and Management of Hypoglycaemia 1. The Care Plan for Prevention of Hypoglycaemia on Labour Ward and the Postnatal
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Fluid & Electrolyte Management and Early Nutritional Care of the Extremely Preterm Infant. J.M. Lorenz, M.D. April 2014
 Fluid & Electrolyte Management and Early Nutritional Care of the Extremely Preterm Infant J.M. Lorenz, M.D. April 2014 DISCLOSURES Dr. Lorenz has no relevant financial relationships to disclose or conflict
Fluid & Electrolyte Management and Early Nutritional Care of the Extremely Preterm Infant J.M. Lorenz, M.D. April 2014 DISCLOSURES Dr. Lorenz has no relevant financial relationships to disclose or conflict
simultaneously excreted. They also brought forward some evidence to
 THE EXCRETION OF CHLORIDES AND BICARBON- ATES BY THE HUMAN KIDNEY. BY H. W. DAVIES, M.B., B.S., J. B. S. HALDANE, M.A. AND G. L. PESKETT, B.A. (From the Laboratory, Cherwell, Oxford.) AM BARD and PAPI
THE EXCRETION OF CHLORIDES AND BICARBON- ATES BY THE HUMAN KIDNEY. BY H. W. DAVIES, M.B., B.S., J. B. S. HALDANE, M.A. AND G. L. PESKETT, B.A. (From the Laboratory, Cherwell, Oxford.) AM BARD and PAPI
PACKAGE LEAFLET: INFORMATION FOR THE USER. SODIPHOS 22mEq / 10ml Concentrate for solution for infusion. Disodium phosphate dihydrate
 PACKAGE LEAFLET: INFORMATION FOR THE USER SODIPHOS 22mEq / 10ml Concentrate for solution for infusion Disodium phosphate dihydrate Read all of this leaflet carefully before you start using this medicine.
PACKAGE LEAFLET: INFORMATION FOR THE USER SODIPHOS 22mEq / 10ml Concentrate for solution for infusion Disodium phosphate dihydrate Read all of this leaflet carefully before you start using this medicine.
Chapter 23. Composition and Properties of Urine
 Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
Pathogenesis of Metabolic Acidosis in Preterm Infants
 Original Article Pathogenesis of Metabolic Acidosis in Preterm Infants DOI: IJNMR/2013/5233.1976 Acid Base Balance Section Christopher Geoffrey Alexander Aiken ABSTRACT Objective: To determine how the
Original Article Pathogenesis of Metabolic Acidosis in Preterm Infants DOI: IJNMR/2013/5233.1976 Acid Base Balance Section Christopher Geoffrey Alexander Aiken ABSTRACT Objective: To determine how the
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
DIURETIC HORMONE * sky, Davidson and Eden (14) and by Schmidt- In rats fed urea, Crawford, Doyle and Probst (21)
 RENAL CONCENTRATING MECHANISMS IN NEWBORN INFANTS. EFFECT OF DIETARY PROTEIN AND WATER CONTENT, ROLE OF UREA, AND RESPONSIVENESS TO ANTI- DIURETIC HORMONE * By C. M. EDELMANN, JR.,t H. L. BARNETT AND V.
RENAL CONCENTRATING MECHANISMS IN NEWBORN INFANTS. EFFECT OF DIETARY PROTEIN AND WATER CONTENT, ROLE OF UREA, AND RESPONSIVENESS TO ANTI- DIURETIC HORMONE * By C. M. EDELMANN, JR.,t H. L. BARNETT AND V.
Fluid and electrolyte balance, imbalance
 Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
Kidney Physiology. Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed
 Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Author: Contact Name and Job Title.
 Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Author: Contact Name and Job Title of Fluid and Electrolytes in Neonates D2 (prev.d14) Version 3 : Dr. Ai May Lee,
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Author: Contact Name and Job Title of Fluid and Electrolytes in Neonates D2 (prev.d14) Version 3 : Dr. Ai May Lee,
IV Fluids. I.V. Fluid Osmolarity Composition 0.9% NaCL (Normal Saline Solution, NSS) Uses/Clinical Considerations
 IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
CONCERNING THE EFFECTS OF MAGNESIUM SULFATE ON RENAL FUNCTION, ELECTROLYTE EXCRETION, AND CLEARANCE OF MAGNESIUM
 CONCERNING THE EFFECTS OF MAGNESIUM SULFATE ON RENAL FUNCTION, ELECTROLYTE EXCRETION, AND CLEARANCE OF MAGNESIUM B. I. Heller,, J. F. Hammarsten, F. L. Stutzman J Clin Invest. 1953;32(9):858-861. https://doi.org/10.1172/jci102803.
CONCERNING THE EFFECTS OF MAGNESIUM SULFATE ON RENAL FUNCTION, ELECTROLYTE EXCRETION, AND CLEARANCE OF MAGNESIUM B. I. Heller,, J. F. Hammarsten, F. L. Stutzman J Clin Invest. 1953;32(9):858-861. https://doi.org/10.1172/jci102803.
Fractional excretion of uric acid in infancy and childhood
 Archives of Disease in Childhood, 1974, 49, 878. Fractional excretion of uric acid in infancy and childhood Index of tubular maturation J. H. PASSWELL, M. MODAN, M. BRISH, S. ORDA, and H. BOICHIS From
Archives of Disease in Childhood, 1974, 49, 878. Fractional excretion of uric acid in infancy and childhood Index of tubular maturation J. H. PASSWELL, M. MODAN, M. BRISH, S. ORDA, and H. BOICHIS From
Normosol -R and 5% Dextrose Injection MULTIPLE ELECTROLYTES AND 5% DEXTROSE INJECTION TYPE 1, USP For Replacing Acute Losses of Extracellular Fluid
 Normosol -R and 5% Dextrose Injection MULTIPLE ELECTROLYTES AND 5% DEXTROSE INJECTION TYPE 1, USP For Replacing Acute Losses of Extracellular Fluid R x only Flexible Plastic Container DESCRIPTION Normosol-R
Normosol -R and 5% Dextrose Injection MULTIPLE ELECTROLYTES AND 5% DEXTROSE INJECTION TYPE 1, USP For Replacing Acute Losses of Extracellular Fluid R x only Flexible Plastic Container DESCRIPTION Normosol-R
Dr Shipa Shah, Lorraine Bell Dietician
 CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Enteral feeding and use of fortification and supplements in the preterm infant Dr Shipa Shah, Lorraine Bell Dietician Neonatalogy
CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Enteral feeding and use of fortification and supplements in the preterm infant Dr Shipa Shah, Lorraine Bell Dietician Neonatalogy
Two Little Water Cravers
 Two Little Water Cravers Baby Mo (5mths/M) Chief complaint Repeated vomiting since 2 months old with poor weight gain PMH Gestation 40+6wks, BW 3.375kg Hx of fracture Rt clavicle at birth HbH disease on
Two Little Water Cravers Baby Mo (5mths/M) Chief complaint Repeated vomiting since 2 months old with poor weight gain PMH Gestation 40+6wks, BW 3.375kg Hx of fracture Rt clavicle at birth HbH disease on
Physiology questions review
 Physiology questions review 1- The consumption of O2 by the kidney: a- decrease as blood flow increases b- regulated by erythropoiten c- remains constant as blood flow increase d- direct reflects the level
Physiology questions review 1- The consumption of O2 by the kidney: a- decrease as blood flow increases b- regulated by erythropoiten c- remains constant as blood flow increase d- direct reflects the level
Fluids and electrolytes
 Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
ELECTROLYTE DISTURBANCES IN CONGESTIVE HEART FAILURE*
 ELECTROLYTE DISTURBANCES IN CONGESTIVE HEART FAILURE* DAVID P. B.AUMANN, M.D. Department of Medicine, University of Arkansas School of Medicine, Little Rock, Arkansas The retention of salt and water secondary
ELECTROLYTE DISTURBANCES IN CONGESTIVE HEART FAILURE* DAVID P. B.AUMANN, M.D. Department of Medicine, University of Arkansas School of Medicine, Little Rock, Arkansas The retention of salt and water secondary
PARENTERAL NUTRITION
 PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
Guideline scope Neonatal parenteral nutrition
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Neonatal parenteral nutrition The Department of Health in England has asked NICE to develop a new guideline on parenteral nutrition in
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Neonatal parenteral nutrition The Department of Health in England has asked NICE to develop a new guideline on parenteral nutrition in
Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are
 Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Neonatal renal function assessment
 Archives of Disease in Childhood, 1989, 64, 1264-1269 Neonatal renal function assessment P M R CLARK,* T N BRYANT,t M A HALL,* J A LOWES,t AND D J F ROWE *Special Care Baby Unit, Princess Anne Hospital,
Archives of Disease in Childhood, 1989, 64, 1264-1269 Neonatal renal function assessment P M R CLARK,* T N BRYANT,t M A HALL,* J A LOWES,t AND D J F ROWE *Special Care Baby Unit, Princess Anne Hospital,
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS
 RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (2) Dr. Attila Nagy 2017 TUBULAR FUNCTIONS (Learning objectives 54-57) 1 Tubular Transport About 99% of filtrated water and more than 90% of the filtrated
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (2) Dr. Attila Nagy 2017 TUBULAR FUNCTIONS (Learning objectives 54-57) 1 Tubular Transport About 99% of filtrated water and more than 90% of the filtrated
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
1. remove: waste products: urea, creatinine, and uric acid foreign chemicals: drugs, water soluble vitamins, and food additives, etc.
 Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
THe Story of salty Sam
 THe Story of salty Sam Understanding fluids, urea and electrolyte balance; a quantitative approach. A self-directed learning activity. Part One. meet salty sam Salty Sam is a pretty average 70 kg bloke,
THe Story of salty Sam Understanding fluids, urea and electrolyte balance; a quantitative approach. A self-directed learning activity. Part One. meet salty sam Salty Sam is a pretty average 70 kg bloke,
Last lec we have studied what controls GFR; either high or low GFR are bad and how to measure GFR. Today we will talk about the tubules.
 Last lec we have studied what controls GFR; either high or low GFR are bad and how to measure GFR. Today we will talk about the tubules. In the tubules first thing we have urine formation; which is the
Last lec we have studied what controls GFR; either high or low GFR are bad and how to measure GFR. Today we will talk about the tubules. In the tubules first thing we have urine formation; which is the
Renal Excretion of Drugs
 Renal Excretion of Drugs 3 1 Objectives : 1 Identify main and minor routes of Excretion including renal elimination and biliary excretion 2 Describe its consequences on duration of drugs. For better understanding:
Renal Excretion of Drugs 3 1 Objectives : 1 Identify main and minor routes of Excretion including renal elimination and biliary excretion 2 Describe its consequences on duration of drugs. For better understanding:
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
Fal Fal P h y s i o l o g y 6 1 1, S a n F r a n c i s c o S t a t e U n i v e r s i t y
 Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
Renal Physiology II Tubular functions
 Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
You should know the T max for any substance that you use and for PAH ; T max = mg / min
 Tubular function - What is clearance? o clearance referred to the theoretical volume of plasma from which a substance is cleared ( cleaned ) over a period of time and so its unit would be ((ml/min)) -
Tubular function - What is clearance? o clearance referred to the theoretical volume of plasma from which a substance is cleared ( cleaned ) over a period of time and so its unit would be ((ml/min)) -
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Ch 19: The Kidneys. Functional unit of kidneys:?? Developed by John Gallagher, MS, DVM
 Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines
 Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines Author: Richard Pugh June 2015 Guideline for management of hyponatraemia in intensive care Background
Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines Author: Richard Pugh June 2015 Guideline for management of hyponatraemia in intensive care Background
The kidney. (Pseudo) Practical questions. The kidneys are all about keeping the body s homeostasis. for questions Ella
 The kidney (Pseudo) Practical questions for questions Ella (striemit@gmail.com) The kidneys are all about keeping the body s homeostasis Ingestion Product of metabolism H 2 O Ca ++ Cl - K + Na + H 2 O
The kidney (Pseudo) Practical questions for questions Ella (striemit@gmail.com) The kidneys are all about keeping the body s homeostasis Ingestion Product of metabolism H 2 O Ca ++ Cl - K + Na + H 2 O
The kidneys are excretory and regulatory organs. By
 exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
Osmoregulation and Excretion
 Animal Life and Excretion Harder for multicellular organisms Internal circulation Coordination, information transfer Structural maintenance Movement Maintenance of homeostatic internal environment 15 July
Animal Life and Excretion Harder for multicellular organisms Internal circulation Coordination, information transfer Structural maintenance Movement Maintenance of homeostatic internal environment 15 July
Functional morphology of kidneys Clearance
 Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Physiology Lecture 2. What controls GFR?
 Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
After studying this lecture, you should be able to...
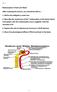 Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
Pediatric Sodium Disorders
 Pediatric Sodium Disorders Guideline developed by Ron Sanders, Jr., MD, MS, in collaboration with the ANGELS team. Last reviewed by Ron Sanders, Jr., MD, MS on May 20, 2016. Definitions, Physiology, Assessment,
Pediatric Sodium Disorders Guideline developed by Ron Sanders, Jr., MD, MS, in collaboration with the ANGELS team. Last reviewed by Ron Sanders, Jr., MD, MS on May 20, 2016. Definitions, Physiology, Assessment,
Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009
 www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers HOW
www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers HOW
Neonatal Hypoglycaemia Guidelines
 N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed versions of the document. The Intranet should be referred to for the current version of the
N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed versions of the document. The Intranet should be referred to for the current version of the
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Hyponatraemia. Detlef Bockenhauer
 Hyponatraemia Detlef Bockenhauer Key message Plasma sodium can be low due to either excess water or deficiency of salt In clinical practice, dysnatraemias almost always reflect an abnormality of water
Hyponatraemia Detlef Bockenhauer Key message Plasma sodium can be low due to either excess water or deficiency of salt In clinical practice, dysnatraemias almost always reflect an abnormality of water
Glucosuria: Diabetes Mellitus
 172 PHYSIOLOGY CASES AND PROBLEMS Case 30 Glucosuria: Diabetes Mellitus David Mandel was diagnosed with type I (insulin-dependent) diabetes mellitus when he was 12 years old, right after he started middle
172 PHYSIOLOGY CASES AND PROBLEMS Case 30 Glucosuria: Diabetes Mellitus David Mandel was diagnosed with type I (insulin-dependent) diabetes mellitus when he was 12 years old, right after he started middle
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
Dr.Nahid Osman Ahmed 1
 1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
Diuretics having the quality of exciting excessive excretion of urine. OED. Inhibitors of Sodium Reabsorption Saluretics not Aquaretics
 Diuretics having the quality of exciting excessive excretion of urine. OED Inhibitors of Sodium Reabsorption Saluretics not Aquaretics 1 Sodium Absorption Na Entry into the Cell down an electrochemical
Diuretics having the quality of exciting excessive excretion of urine. OED Inhibitors of Sodium Reabsorption Saluretics not Aquaretics 1 Sodium Absorption Na Entry into the Cell down an electrochemical
clamped. At 30- or 60-minute intervals urine specimens were collected and the bladder washed out with saline
 Downloaded from http://www.jci.org on January 11, 218. https://doi.org/1.1172/jci11171 THE MECHANISM OF THE EXCRETION OF VITAMIN C BY THE HUMAN KIDNEY AT LOW AND NORMAL PLASMA LEVELS OF ASCORBIC ACID 1
Downloaded from http://www.jci.org on January 11, 218. https://doi.org/1.1172/jci11171 THE MECHANISM OF THE EXCRETION OF VITAMIN C BY THE HUMAN KIDNEY AT LOW AND NORMAL PLASMA LEVELS OF ASCORBIC ACID 1
Filtration and Reabsorption Amount Filter/d
 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD Contact me at lharris@lsuhsc.edu Renal Physiology Lecture 3 Renal Clearance and Glomerular Filtration Filtration and Reabsorption Amount Filter/d Amount
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD Contact me at lharris@lsuhsc.edu Renal Physiology Lecture 3 Renal Clearance and Glomerular Filtration Filtration and Reabsorption Amount Filter/d Amount
URINARY NET CHARGE IN HYPERCHLOREMIC METABOLIC ACIDOSIS. Seema Kumar, Meera Vaswani*, R.N. Srivastava and Arvind Bagga
 INDIAN PEDIATRICS VOLUME 35-JANUARY 1998 Original Articles URINARY NET CHARGE IN HYPERCHLOREMIC METABOLIC ACIDOSIS Seema Kumar, Meera Vaswani*, R.N. Srivastava and Arvind Bagga From the Departments of
INDIAN PEDIATRICS VOLUME 35-JANUARY 1998 Original Articles URINARY NET CHARGE IN HYPERCHLOREMIC METABOLIC ACIDOSIS Seema Kumar, Meera Vaswani*, R.N. Srivastava and Arvind Bagga From the Departments of
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance
 Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Renal Functions: Renal Functions: Renal Function: Produce Urine
 Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Renal Reabsorption & Secretion
 Renal Reabsorption & Secretion Topics for today: Nephron processing of filtrate Control of glomerular filtration Reabsorption and secretion Examples of solute clearance rates Hormones affecting kidney
Renal Reabsorption & Secretion Topics for today: Nephron processing of filtrate Control of glomerular filtration Reabsorption and secretion Examples of solute clearance rates Hormones affecting kidney
