PROPHYLACTIC USE OF CORTICOSTEROIDS IN A SINGLE LONG BONE FRACTURE OF LOWER LIMB TO PREVENT FAT EMBOLISM SYNDROME A CLINICAL EXPERIENCE
|
|
|
- Anna Pearson
- 5 years ago
- Views:
Transcription
1 RESEARCH ARTICLE PROPHYLACTIC USE OF CORTICOSTEROIDS IN A SINGLE LONG BONE FRACTURE OF LOWER LIMB TO PREVENT FAT EMBOLISM SYNDROME A CLINICAL EXPERIENCE Prashanth N 1, Neeta PN 2, Amit RU 3, *, Shilpa K 4 1Senior Resident, Department of Anesthesiology, 2 Assistant Professor, Department of Community Medicine, VIMS, Bellary, Karnataka, India. 3Assistant Professor, Department of Microbiology, 4 Assistant Professor, Department of Community Medicine, Azeezia Institute of Medical Sciences, Kerala, India. *Corresponding Author: address: amitrun9979@gmail.com ABSTRACT Background: Fat embolism syndrome is commonly associated with long bone fractures and the mortality associated with it is due to cerebral and pulmonary involvement. Recently experimental and clinical data have suggested that the benefit of corticosteroid therapy may be maximized if the treatment is given early as a prophylaxis for the development of the fat embolism syndrome in high risk patients. The aim of our study was to test the efficacy of single dose methyl prednisolone as prophylaxis to prevent Fat embolism syndrome in patients with single long bone fracture of lower limb. Methods: We conducted a double blinded randomized control among 44 patients, who showed signs and symptoms of sub clinical fat embolism and fulfilled our inclusion and exclusion criteria over 2years period in a tertiary trauma care centre, Bangalore, Karnataka. These 44 patients were randomly selected and assigned 1 envelope and segregated to respective group. The nursing staffs who were educated about the division of groups administered the drug methyl prednisolone or normal saline accordingly. We were blinded to this allocation of groups and drug administration. The patients were followed up by us in the ICU and wards. At the end of study, the group allocation was disclosed. Among these patients were divided into Control A (21 patients), who were given placebo treatment with normal saline and Study B (23 patients), who were given a single dose of methyl prednisolone 30mg/kg over one. Results: Among the 44 patients analyzed, 33.3% of group A and 8.7% of group B patients developed clinical Fat Embolism Syndrome (FES). The mean duration of ventilator support in group A (9.25 days) was higher than in the group B (7.33days). There was significant increase in the vital parameters like heart rate and respiratory rate as well as significant fall of Spo2, in control group than the study group postoperatively. There is no change in the PaCO2, systolic and diastolic blood pressure. Conclusion: A Single prophylactic dose of Methyl Prednisolone 30 mg/kg significantly reduces the incidence of Fat Embolism Syndrome. Hence use of Methyl Prednisolone as a Prophylaxisfor Fat Embolism Syndrome in long bone fractures of lower limbs is beneficial. Key words: Fat embolism syndrome, Methyl prednisolone, long bone fracture INTRODUCTION Fat embolism is the most frequent cause of death after fracture of long bones [1].The most common clinical situation in which Fat embolism syndrome may develop is orthopedic or general trauma. A high association with multiple long bone fractures also is found. Although pulmonary fat embolization occurs in almost all patients with long bone fracture [2, 3], only 1% to 30% [4] of patients develop the full, clinical fat embolism syndrome that consists of petechial rash, diffuse pulmonary infiltrates, hypoxemia, confusion, pyrexia, tachycardia and tachypnea, 24 to 48 after trauma. Since 1966, several studies have claimed benefit from corticosteroid therapy for this syndrome [5, 6, 7]. However most of these studies have been retrospective. Recently experimental and clinical data have suggested that the benefit of corticosteroid therapy may be maximized if the treatment is given early as a prophylaxis for the development of the fat embolism syndrome in high risk patients. A study reported a series of 48 patients with uncomplicated extremity fractures who were randomized into fluid loading, hypertonic glucose, aspirin, steroids or control groups. Methyl prednisolone 30ml/kg every six s was given to steroid group. They demonstrated Indian Journal of Clinical Anaesthesia, January March 2015;2(1):
2 consistently significant improvement in PO 2 levels with apparent coagulation mechanism stabilization in steroid group as compared to control [8]. Another study conducted a prospective randomized trial of prophylactic therapy in fat embolism syndrome with three groups treated with (a) Hypertonic glucose (b) Methyl prednisolone and (c) Placebo and showed that methyl prednisolone given prophylactically may reduce the incidence of fat embolism syndrome and can reduce the degree of hypoxemia associated with long bone fractures of lower extremity. In this study the first group received 50% Dextrose; study group received three 1 gm doses of methyl prednisolone every eight s beginning on admission. Incidence was 21% in glucose group, 0% in steroid group and 29% in control groups [9]. To test the prophylactic value of corticosteroid therapy in patients with fracture, we prospectively administered methyl prednisolone sodium succinate in a randomized double blind study of 44 patient believed to be at risk for fat embolism syndrome and who had no other major injuries that might otherwise predispose them to posttraumatic respiratory failure. MATERIALS AND METHODS The present study was conducted from May 2005 to May 2007, in a tertiary care centre especially for trauma in Bangalore, Karnataka, India. In this period 210 patients with single long bone fracture of lower limb (femur or tibia) fulfilling our criteria were attended in the casualty and evaluated for subclinical fat embolism by peripheral oxygen saturation using pulse oxymeter and arterial blood gases. Inclusion criteria - a. Patients with closed fracture long bone in lower limb. b. ASA I c. Age- < 45 years Exclusion Criteriaa. Patients with polytrauma. b. Patients with head injury and sepsis. c. Patients associated with fracture ribs and lung contusion. d. Patients with ischemic heart disease, congenital heart disease, hypertension and valvular heart disease. e. Patients with blunt injury to thorax, abdomen, head and neck. f. Patients with cervical spine injury and facio-maxillary injuries. g. Patients with shock hemorrhagic, septic, cardiogenic and neurogenic. h. Patients with vascular injuries. i. Associated with respiratory system and other medical illness like chronic obstructive airway disease, pneumonia (Aspiration) or lower respiratory tract infection. Among these, total of 44 patients showed signs and symptoms of subclinical fat embolism and were selected for our study and assigned 1 envelope and segregated to respective group. Of selected patients, 21 were in A (control) and 23 were in B (study) were placed randomly. These 44 patients were subjected to a prospective randomized double blind study to test the efficacy of single dose of Methyl Prednisolone as a prophylactic for fat embolism syndrome development. The nursing staffs who were educated about the division of groups administered the drug methyl prednisolone or normal saline accordingly. We were blinded to this allocation of groups and drug administration. The patients were followed up by us in the ICU and wards. At the end of study, the group allocation was disclosed. Patients in Control A (21 patients), received placebo treatment with normal saline and Study B (23 patients), received a single dose of methyl prednisolone 30mg/kg over one. A. Mellor & Neil Soni 10 reviewed several Randomized Controlled Trials which reported beneficial effect of Methyl prednisolone used in doses ranging from 9 90 mg/kg. Only three trials reported significantly improved gas exchange. A tenfold decrease in Fat Embolism Syndrome was seen in one series. One fatality was reported in these trials due to sepsis in a patient receiving Methyl prednisolone. 30 mg/kg of methyl prednisolone is the Indian Journal of Clinical Anaesthesia, January March 2015;2(1):
3 recommended therapy for some life threatening conditions. 22 Institutional ethical committee clearance was obtained and written informed consent was taken from all patients or their relatives. Both groups otherwise received the same supportive treatment like oxygen supplementation, intra venous fluids, antibiotics, antacids, chest physiotherapy, incentive spirometry, etc. All the patients underwent surgical fixation of bones i.e. intramedullary nailing within 12 s. The patients were followed up and assessed for development of signs and symptoms suggestive of clinical "Fat Embolism Syndrome" using clinical monitoring and serial investigations like pulse oximetry, arterial blood gases, urine fat globules, platelet count, fibrin degradation products (D-Dimer), altered sensorium and chest x ray. Intra operatively patients were supplied oxygen at 5 lit/min through ordinary mask or FiO 2 of 0.4 maintained in general anesthesia. All the patients monitored clinically for fat embolism syndrome. Arterial blood gas analysis was done in some patients who had hypoxia intra operatively and FiO 2 increased accordingly. Post operatively also patients were monitored for 24 s in similar way. The patients who developed respiratory failure were given ventilator support. In the study Fat embolism syndrome was described on basis of Lindeque s criteria [10]. 1. A sustained PaO 2 of less than 8 k.pa (60mm of Hg) with FiO A sustained PaCo 2 of more than 7.3 k.pa (55mm of Hg) or ph of less than A sustained respiratory rate of greater than 35breath/min. even after adequate sedation. 4. Increased work of breathing judged by dyspnoea use of accessory muscles, tachycardia and anxiety. Any patient with fracture femur and/or tibia showing one or more of these criteria was judged as having Fat Embolism Syndrome. Data was analyzed and expressed in terms of rates, ratios and percentages. Statistical analysis was done using Pearson s Chi Square test. A probability value (p value) of less than 0.05 was considered as significant. RESULTS The study was conducted in HOSMAT hospital, Bangalore, a tertiary trauma care centre from May 2005 to May Ethical Clearance was obtained from the Hospital Ethics review committee. The objective was to study the efficacy of methyl prednisolone as prophylaxis for Fat Embolism Syndrome in single long bone fracture of lower limb. One fatality was reported in the series of trials due to sepsis in a patient receiving Methyl prednisolone of 9-90mg/kg. 30 mg/kg of methyl prednisolone is the recommended therapy for some life threatening conditions. 10,22 In the study period, all patients coming to the Casualty with single long bone fractures were evaluated. A total of 210 Patients with closed fracture of tibia or femur and without any other major injuries were screened for sub clinical Fat Embolism. Among them, 44 patients (20.95 %) confirmed to the inclusion criteria for Fat Embolism and were hence included for the study after obtaining informed consent. Out of 210 patients, nine developed FES, eight among fracture femur and one among fracture tibia. These 44 patients were then placed randomly into A (control), with 21 patients and B (study), with 23 patients. Mean age was years for A and years for B. Majority of patients (76.19% A & 86.96% B) were males. Most of the patients (61.9% of A & 73.91% of B) showed normal chest X- ray. On admission mean values of vital parameters (heart rate, respiratory rate, systolic and diastolic Blood Pressure as well as SPO 2) were within normal limits for both the groups. Arterial blood gas analysis (ph, Indian Journal of Clinical Anaesthesia, January March 2015;2(1):
4 PaO 2, P aco 2) of both groups was similar and within normal limits on admission. These data shows that we received both groups of patients in same condition. At start of surgery, the mean values of SPO 2 were 94.38% with s.d of ±1.72 in A and 94.74% with s.d of 1.57 in B. 24 s after the surgery the Spo 2 was 94±6.53% in A and 97.48±3.98% in B. There was significant fall in saturation in A patients 24 s after surgery. (Table 1) Table.1: Compares the Spo2 readings of patients in two groups at regular intervals. (n=21) (n=23) A B Intraop 1 st Hour Intraop 2 nd Intraop 3 rd 4 th 8 th 12 th 16 th 20 th 24 th ±1.72 ±1.40 ±2.39 ±2.77 ±3.79 ±4.81 ±5.50 ±6.22 ± ±1.57 ±1.20 ±1.94 ±2.30 ±2.69 ±2.61 ±3.56 ±3.69 ±3.98 t p-value Statistical significance N.S. N.S. N.S. N.S. N.S. N.S. N.S. S. S. The heart rate on admission was 92.90±12beats/min and 90.96±9.23beats/min in A and B patients respectively. The heart rate was significantly increased in A patients i.e ±20.93beats/min as compared to B (80.91±8.93 beats/min), 24 s after surgery. (Graph 1) A B IO-1 IO-2 IO-3 PO-4 PO-8 PO-12 Trend in Heart rate PO-16 PO-20 PO-24 Graph.1: Shows the trend in heart rate in patients of two groups. Before the surgery respiratory rate was around 18breaths/min in both the groups. Whereas 24 s after the surgery it was increased significantly in A Patients i.e. 19±6breaths/min when compared to B, i.e.16±3breaths/min. (Graph 2) Indian Journal of Clinical Anaesthesia, January March 2015;2(1):
5 A B IO- 1 IO- 2 IO- 3 PO-4 PO-8 PO-12 PO-16 PO-20 PO-24 Graph.2: Shows the trend in respiratory rate in patients of two groups. The systolic as well as diastolic blood pressure did not show any variation between two groups during pre operative, intra operative or post operative period. The incidence of FES in A was 33.3% (7 out of 21), where as in B 8.7% (2 out of 23), which is statistically significant (p value = 0.043). The mean duration of ventilator support required was higher in A (9.25 days) than in B patients (7.33days). DISCUSSION Fat embolism syndrome is fat in circulation associated with an identifiable pattern of clinical symptoms and signs [11]. The lack of definitive diagnostic criteria, the unpredictable course and frequent associated disease have made it difficult to standardize patient population [12]. Fat embolism syndrome can be diagnosed using 1) Gurd s criteria [13] 2) Lindeque s criteria [14] Gurd s criteria for diagnosis of fat embolism syndrome have been criticized for being unreliable because fat droplets can frequently be found in the blood of healthy volunteers and trauma patients, without clinical evidence of fat embolism syndrome [15]. Lindeque suggested that Gurd s criteria may under diagnose the syndrome and proposed his criteria based on respiratory parameters [14]. Lindeque s criteria involved arterial blood gas study which is gold standard for detection of hypoxia. Gurd s criteria do not use arterial blood gas analysis as criteria. In our study a total of 210 patients were randomly selected and evaluated in the casualty for hypoxemia with arterial blood gas analysis. The incidence of fat embolism in patients with fracture femur was significantly higher (p= 3.63 X ) than that with tibia. The incidence of sub clinical fat embolism was similar to previous studies with involvement of patients with single long bone fracture [16]. In one study Fat embolism occurred within 72 s in all patients who developed Fat Embolism Syndrome [16]. The syndrome developed within 24 s in the present study. The interval between the injury and the admission varied widely from one to 48 s in our study. This wide interval could be attributed to the fact that our institution is the only tertiary care referral center for trauma in Bangalore and attracts patients from both within and outside the city. The mean baseline values in all patients included in the study were: Heart rate of 96 beats/min, respiratory rate 20breaths/min, Systolic BP 115 mm of Hg and Diastolic BP of 76 mm Hg. The SpO 2 on Pulse Oximetry showed less than 94 % in all patients with Fat embolism on room air. The Arterial Blood Gas (ABG) values on room air in these patients showed mean Indian Journal of Clinical Anaesthesia, January March 2015;2(1):
6 values of PO 2 61 mm Hg, PCO 2 33 mm Hg and ph The PO2 values were similar to that obtained by Tachakra et al [17]. This overall picture of Hypoxemia following long bone fracture was suggestive of Fat embolism. These 44 patients were subjected to prospective double blind study to test efficacy of methyl prednisolone as prophylaxis to fat embolism syndrome. We used single dose of 30mg/kg of Methyl prednisolone administered over one as infusion in study group patients soon after admission after being diagnosed to have sub clinical fat embolism. All fractures were surgically stabilized within 12 hrs of admission. They were followed up for a period of 24 hrs for development of signs and symptoms of fat embolism syndrome, which was defined on basis of Lindeques criteria [14]. It is thought that steroids may act by decreasing the edema, increasing vascular integrity, and preventing the inflammatory response to the hydrolyzed products of the lodged fatty acids. Steroids are also thought to exert a general effect on stabilization of lipoid membranes [5]. Methyl prednisolone has been used in different doses from 6mg/kg to 90mg/kg both as a prophylactic and as a treatment modality for fat embolism syndrome by different authors [9, 12, 18, 19, 20, 21, 22]. Another study had used mg of methyl prednisolone every six s for 3 days primarily as treatment for Fat Embolism Syndrome [5]. Methyl prednisolone used as prophylaxis in a dose of 30mg/kg does not increase risk of infection or sepsis [23]. In the present study, the reading at 24 th after surgery showed a statistically significant fall in saturation and a rise in heart rate and respiratory rate in A (Control) patients as compared to that in B (Study) patients, which is suggestive of Fat Embolism Syndrome in these patients due to fat emboli being released into the systemic circulation secondary to fracture manipulation and reaming of marrow cavity during surgery. Four out of 21 in control group and three out of 23 patients in study group required ventilator support which was not statistically significant. Only one patient in the control group with Fat embolism syndrome who was on ventilator support died of multi organ dysfunction syndrome. The incidence of clinical Fat embolism syndrome in study group patients (8.7%) was significantly lower than that in control group patients (33.3%). Our study demonstrated that Methyl prednisolone 30 mg/kg significantly reduces the incidence of Fat Embolism Syndrome when given as a single prophylactic dose. This is in close agreement in the study, where Methyl prednisolone 30 mg/kg was given in divided doses [12]. CONCLUSION A Single prophylactic dose of Methyl Prednisolone 30 mg/kg significantly reduces the incidence of Fat Embolism Syndrome. Hence use of Methyl Prednisolone as a Prophylaxisfor Fat Embolism Syndrome in long bone fractures of lower limbs is beneficial. CONFLICTS OF INTEREST: Nil. SOURCE OF FUNDING: None. ACKNOWLEDGEMENT: We thank Dr Thomas A Chandy, Dean and Director of HOSMAT hospital, Bangalore, for giving permission to carry out research. REFERENCES: 1. Warthin AS: Traumatic lipemia and fatty embolism. IntClin 1913;4: Evarts CM: The fat embolism syndrome- a review. SurgClin North America 1970;50: Emson HE: Fat embolism studied in 100 patients dying after injury. J Clin Path 1958;11: Herndon: The syndrome of fat embolism. South J Med 1975;68; Fischer JE, Turner RH, Herndon JH, Riseborough EJ: Massive steroid therapy in severe fat embolism. SurgGynecolObstet 1971 April;24: Ashbaugh DG, Petty TL: The use of corticosteroids in the treatment of respiratory failure associated with massive fat embolism. SurgGynecolObstet 1966;123:493. Indian Journal of Clinical Anaesthesia, January March 2015;2(1):
7 6. Moylan JA, Birnbaum M, Katz A, Everson MA: Fat emboli syndrome. J Trauma 1976;16; Shier MR, Wilson RF, James RE, Riddle J, Mammen EF, Pedersen HE: Fat embolism prophylaxis - A study of four treatment modalities. J Trauma 1977;17: Stoltenberg JJ, Gustilo RB: The use of methylprednisolone and hypertonic glucose in the prophylaxis of fat embolism syndrome. Clinic OrthopRelat Res 1979 Sep;143: Gosling HR, Pellengrini VD: Fat embolism syndrome A review of the Pathology and Physiological basis of treatment. Clinic OrthopRelat Res 1982 May;165: Mellor A, Soni N. Fat Embolism : Review article. Anaesthesia 2001;56: Antti A, Kari Saikku, Pekka E, Matti K, Hamalainen M: Corticosteroids in patients with a high risk of fat embolism syndrome. SurgGynecolObstet 1978 Sept;147: Gurd AR: Fat Embolism; an aid to diagnosis. J Bone Joint Surg 1970;52B: Lindeque BG, Schoeman HS, Domisse GF, Boeyens MC, Vlok AL: Fat Embolism and Fat Embolism Syndrome A double blind therapeutic study. Br J Bone Joint Surg 1987; 69: Nolte WJ, Olofsson T, Schersten T, Lewis DH: Evaluation of the Gurd test for fat embolism. Br J Bone Joint Surg 1974; 56B: Richard B Ganong: Fat embolism syndrome in isolated fractures of the tibia and femur. Clinic OrthopRelat Res 1993 June; 291: Tachakra SS, Sevitt S: Hypoxaemia after fractures. J Bone Joint Surg 1975 May;57(2): Schonfeld AS, Yongyudh P, Ralph D, John DC, Edward M, Dale EH et al: Fat embolism prophylaxis with corticosteroids; a prospective study in high risk patients. Annals of Internal Medicine 1983; 99: Kallenbach JL, Zaltzman M, Feldman C, Orford A, Zwi S: 'Low dose' corticosteroid prophylaxis against Fat Embolism. J Trauma 1987 Oct:27(10): Babalis GA, Yiannakopoulos CK, Karliaftis K, Antonogiannakis E: Prevention of posttraumatic hypoxemia in isolated lower limb long bone fracture with a minimal prophylactic dose of corticosteroids. Injury 2004 Mar;35(3): Rokkanen PA, Avikainen AV, Karaharaju E, Kataja J, Lahdensuu M, Lepisto et al: The efficacy of corticosteroids in severe trauma. SurgGynecolObstet 1974; 138: Shier MR, Wilson RF, James RE, Riddle J, Mammen EF, Pedersen HE: Fat embolism prophylaxis - A study of four treatment modalities. J Trauma 1977; 17: Therapeutic index: Anti-inflammatory drugs :URL: Indian Journal of Clinical Anaesthesia, January March 2015;2(1):
Lutheran Medical Center Department of Surgery
 Lutheran Medical Center Department of Surgery Morbidity & Mortality Conference Case & Topic Presentation Baiju C. Gohil, M.D. April 9, 2004 FAT EMBOLISM SYNDROME INTRODUCTION Fat emboli were first noted
Lutheran Medical Center Department of Surgery Morbidity & Mortality Conference Case & Topic Presentation Baiju C. Gohil, M.D. April 9, 2004 FAT EMBOLISM SYNDROME INTRODUCTION Fat emboli were first noted
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68, Page
 The Egyptian Journal of Hospital Medicine (July 2017) Vol.68, Page 923-928 Fat Embolism Syndrome Due to Fracture Right Femur: A Case Report Khalid Al Shareef, Muhammad Asadullah, Muhammad Helal General
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68, Page 923-928 Fat Embolism Syndrome Due to Fracture Right Femur: A Case Report Khalid Al Shareef, Muhammad Asadullah, Muhammad Helal General
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Fat Embolism Syndrome Todd Nickoles, MBA, RN, BSN
 Fat Embolism Syndrome Todd Nickoles, MBA, RN, BSN Learning Objectives Identify the risk factors and causes of fat embolism syndrome Recognize the signs and symptoms of fat embolism syndrome following acute
Fat Embolism Syndrome Todd Nickoles, MBA, RN, BSN Learning Objectives Identify the risk factors and causes of fat embolism syndrome Recognize the signs and symptoms of fat embolism syndrome following acute
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS
 REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
Fat Embolism in Differential Diagnosis of Acute Cor Pulmonale: Case Report
 Fat Embolism in Differential Diagnosis of Acute Cor Pulmonale: José Luis de Castro e Silva Pretto, Andriéli Cristina de Oliveira, Daniel Spilmann, Eduardo Dal Magro Marcon, Elias Sato de Almeida, Lucas
Fat Embolism in Differential Diagnosis of Acute Cor Pulmonale: José Luis de Castro e Silva Pretto, Andriéli Cristina de Oliveira, Daniel Spilmann, Eduardo Dal Magro Marcon, Elias Sato de Almeida, Lucas
Staging Sepsis for the Emergency Department: Physician
 Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Head Trauma Protocol
 Injuries to the head may cause underlying brain tissue damage. Increased intracranial pressure from bleeding or swelling tissue is a common threat after head trauma. Common signs and symptoms of increased
Injuries to the head may cause underlying brain tissue damage. Increased intracranial pressure from bleeding or swelling tissue is a common threat after head trauma. Common signs and symptoms of increased
Trial protocol - NIVAS Study
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
Effective Date: Approved by: Laboratory Director, Jerry Barker (electronic signature)
 1 of 5 Policy #: 702 (PHL-702-05) Effective Date: 9/30/2004 Reviewed Date: 8/1/2016 Subject: TRANSFUSION GUIDELINES Approved by: Laboratory Director, Jerry Barker (electronic signature) Approved by: Laboratory
1 of 5 Policy #: 702 (PHL-702-05) Effective Date: 9/30/2004 Reviewed Date: 8/1/2016 Subject: TRANSFUSION GUIDELINES Approved by: Laboratory Director, Jerry Barker (electronic signature) Approved by: Laboratory
Exacerbations. Ronald Dahl, Aarhus University Hospital, Denmark
 1st WAO Allied Health Session - Asthma: Diagnosi Exacerbations Ronald Dahl, Aarhus University Hospital, Denmark The health professional that care for patients with asthma exacerbation must be able to Identificafy
1st WAO Allied Health Session - Asthma: Diagnosi Exacerbations Ronald Dahl, Aarhus University Hospital, Denmark The health professional that care for patients with asthma exacerbation must be able to Identificafy
Lecture Notes. Chapter 2: Introduction to Respiratory Failure
 Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
7/4/2015. diffuse lung injury resulting in noncardiogenic pulmonary edema due to increase in capillary permeability
 Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
SIMPLY Arterial Blood Gases Interpretation. Week 4 Dr William Dooley
 SIMPLY Arterial Blood Gases Interpretation Week 4 Dr William Dooley Plan Structure for interpretation 5-step approach Works for majority of cases Case scenarios Some common concerns A-a gradient BE Anion
SIMPLY Arterial Blood Gases Interpretation Week 4 Dr William Dooley Plan Structure for interpretation 5-step approach Works for majority of cases Case scenarios Some common concerns A-a gradient BE Anion
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
5. What is the cause of this patient s metabolic acidosis? LACTIC ACIDOSIS SECONDARY TO ANEMIC HYPOXIA (HIGH CO LEVEL)
 Self-Assessment RSPT 2350: Module F - ABG Analysis 1. You are called to the ER to do an ABG on a 40 year old female who is C/O dyspnea but seems confused and disoriented. The ABG on an FiO 2 of.21 show:
Self-Assessment RSPT 2350: Module F - ABG Analysis 1. You are called to the ER to do an ABG on a 40 year old female who is C/O dyspnea but seems confused and disoriented. The ABG on an FiO 2 of.21 show:
Acute Respiratory Distress Syndrome (ARDS) An Update
 Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Capnography. Capnography. Oxygenation. Pulmonary Physiology 4/15/2018. non invasive monitor for ventilation. Edward C. Adlesic, DMD.
 Capnography Edward C. Adlesic, DMD University of Pittsburgh School of Dental Medicine 2018 North Carolina Program Capnography non invasive monitor for ventilation measures end tidal CO2 early detection
Capnography Edward C. Adlesic, DMD University of Pittsburgh School of Dental Medicine 2018 North Carolina Program Capnography non invasive monitor for ventilation measures end tidal CO2 early detection
Sample Case Study. The patient was a 77-year-old female who arrived to the emergency room on
 Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
Images have been removed from the PowerPoint slides in this handout due to copyright restrictions.
 Arterial Blood Gas Interpretation Routine Assessment Inspection Palpation Auscultation Labs Na 135-145 K 3.5-5.3 Chloride 95-105 CO2 22-31 BUN 10-26 Creat.5-1.2 Glu 80-120 Arterial Blood Gases WBC 5-10K
Arterial Blood Gas Interpretation Routine Assessment Inspection Palpation Auscultation Labs Na 135-145 K 3.5-5.3 Chloride 95-105 CO2 22-31 BUN 10-26 Creat.5-1.2 Glu 80-120 Arterial Blood Gases WBC 5-10K
NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP)
 Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
BREAK 11:10-11:
 1. Sepsis Tom Heaps 09:30-10:20 2. Oncological Emergencies Clare Pollard 10:20-11:10 ------------------------ BREAK 11:10-11:30 ------------------------ 3. Diabetic Ketoacidosis Tom Heaps 11:30-12:20 4.
1. Sepsis Tom Heaps 09:30-10:20 2. Oncological Emergencies Clare Pollard 10:20-11:10 ------------------------ BREAK 11:10-11:30 ------------------------ 3. Diabetic Ketoacidosis Tom Heaps 11:30-12:20 4.
Pediatric Code Blue. Goals of Resuscitation. Focus Conference November Ensure organ perfusion
 Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy
 Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Prone ventilation revisited in H1N1 patients
 International Journal of Advanced Multidisciplinary Research ISSN: 2393-8870 www.ijarm.com DOI: 10.22192/ijamr Volume 5, Issue 10-2018 Case Report DOI: http://dx.doi.org/10.22192/ijamr.2018.05.10.005 Prone
International Journal of Advanced Multidisciplinary Research ISSN: 2393-8870 www.ijarm.com DOI: 10.22192/ijamr Volume 5, Issue 10-2018 Case Report DOI: http://dx.doi.org/10.22192/ijamr.2018.05.10.005 Prone
2. To provide an ethical, moral and practical framework for decision-making during a public health emergency.
 November 2010 TABLE TOP EXERCISE PARTICIPANT GUIDE When Routine Critical Care Resources Are Not Available Time expectations for each session: SECTION ACTIVITY TIME I Introduction 5 minutes II Exercise
November 2010 TABLE TOP EXERCISE PARTICIPANT GUIDE When Routine Critical Care Resources Are Not Available Time expectations for each session: SECTION ACTIVITY TIME I Introduction 5 minutes II Exercise
Initial Resuscitation of Sepsis & Septic Shock
 Initial Resuscitation of Sepsis & Septic Shock Dr. Fatema Ahmed MD (Critical Care Medicine) FCPS (Medicine) Associate professor Dept. of Critical Care Medicine BIRDEM General Hospital Is Sepsis a known
Initial Resuscitation of Sepsis & Septic Shock Dr. Fatema Ahmed MD (Critical Care Medicine) FCPS (Medicine) Associate professor Dept. of Critical Care Medicine BIRDEM General Hospital Is Sepsis a known
Head injuries. Severity of head injuries
 Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
The Septic Patient. Dr Arunraj Navaratnarajah. Renal SpR Imperial College NHS Healthcare Trust
 The Septic Patient Dr Arunraj Navaratnarajah Renal SpR Imperial College NHS Healthcare Trust Objectives of this session Define SIRS / sepsis / severe sepsis / septic shock Early recognition of Sepsis The
The Septic Patient Dr Arunraj Navaratnarajah Renal SpR Imperial College NHS Healthcare Trust Objectives of this session Define SIRS / sepsis / severe sepsis / septic shock Early recognition of Sepsis The
Michael Avant, M.D. The Children s Hospital of GHS
 Michael Avant, M.D. The Children s Hospital of GHS OVERVIEW ER to ICU Transition Early Management Priorities the First 48 hours Organ System Support Complications THE FIRST 48 HOURS Communication Damage
Michael Avant, M.D. The Children s Hospital of GHS OVERVIEW ER to ICU Transition Early Management Priorities the First 48 hours Organ System Support Complications THE FIRST 48 HOURS Communication Damage
Outcomes From Severe ARDS Managed Without ECMO. Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016
 Outcomes From Severe ARDS Managed Without ECMO Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016 Severe ARDS Berlin Definition 2012 P:F ratio 100 mm Hg Prevalence:
Outcomes From Severe ARDS Managed Without ECMO Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016 Severe ARDS Berlin Definition 2012 P:F ratio 100 mm Hg Prevalence:
Sleep Apnea and ifficulty in Extubation. Jean Louis BOURGAIN May 15, 2016
 Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit
 Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
-Cardiogenic: shock state resulting from impairment or failure of myocardium
 Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Standardize comprehensive care of the patient with severe traumatic brain injury
 Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
MANAGEMENT OF THORACIC TRAUMA. Luis H. Tello MV, MS DVM, COS Portland Hospital Classic Banfield Pet Hospital - USA
 MANAGEMENT OF THORACIC TRAUMA Luis H. Tello MV, MS DVM, COS Portland Hospital Classic Banfield Pet Hospital - USA luis.tello@banfield.com Chest Trauma: Big threat!!!! CAUSES OF THORACIC TRAUMA Blunt Trauma
MANAGEMENT OF THORACIC TRAUMA Luis H. Tello MV, MS DVM, COS Portland Hospital Classic Banfield Pet Hospital - USA luis.tello@banfield.com Chest Trauma: Big threat!!!! CAUSES OF THORACIC TRAUMA Blunt Trauma
Intravenous Methylprednisolone, a Possible Cause of the Atrial Fibrillation
 R Iranian Journal of Pharmaceutical Sciences Winter 2010: 6(1): 13-18 ijps.sums.ac.ir Original Article Intravenous Methylprednisolone, a Possible Cause of the Atrial Fibrillation Afsaneh Vazin a,*, Gholamreza
R Iranian Journal of Pharmaceutical Sciences Winter 2010: 6(1): 13-18 ijps.sums.ac.ir Original Article Intravenous Methylprednisolone, a Possible Cause of the Atrial Fibrillation Afsaneh Vazin a,*, Gholamreza
Bronchospasm & SOB. Kim Kilmurray Senior Clinical Teaching Fellow
 Bronchospasm & SOB Kim Kilmurray Senior Clinical Teaching Fellow LEARNING OBJECTIVES Perform a comprehensive respiratory examination & link clinical signs to underlying pathology Identify the spectrum
Bronchospasm & SOB Kim Kilmurray Senior Clinical Teaching Fellow LEARNING OBJECTIVES Perform a comprehensive respiratory examination & link clinical signs to underlying pathology Identify the spectrum
Analgesia for chest trauma - RVI
 Analgesia for chest trauma - RVI Northern Network Initial Management Patients with blunt chest trauma will be managed in a standard fashion within the context of the well established trauma systems at
Analgesia for chest trauma - RVI Northern Network Initial Management Patients with blunt chest trauma will be managed in a standard fashion within the context of the well established trauma systems at
Rounds in the ICU. Eran Segal, MD Director General ICU Sheba Medical Center
 Rounds in the ICU Eran Segal, MD Director General ICU Sheba Medical Center Real Clinical cases (including our mistakes) Emphasis on hemodynamic monitoring Usually no single correct answer We will conduct
Rounds in the ICU Eran Segal, MD Director General ICU Sheba Medical Center Real Clinical cases (including our mistakes) Emphasis on hemodynamic monitoring Usually no single correct answer We will conduct
Landmark articles on ventilation
 Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
INDICATIONS FOR RESPIRATORY ASSISTANCE A C U T E M E D I C I N E U N I T P - Y E A R M B B S 4
 INDICATIONS FOR RESPIRATORY ASSISTANCE A C U T E M E D I C I N E U N I T P - Y E A R M B B S 4 RESPIRATORY FAILURE Acute respiratory failure is defined by hypoxemia with or without hypercapnia. It is one
INDICATIONS FOR RESPIRATORY ASSISTANCE A C U T E M E D I C I N E U N I T P - Y E A R M B B S 4 RESPIRATORY FAILURE Acute respiratory failure is defined by hypoxemia with or without hypercapnia. It is one
LeMone & Burke Ch 30-32
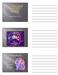 LeMone & Burke Ch 30-32 2 Right side- Low oxygenation Low pressure Light workload Goes toward the lungs Left side High oxygenation Thick walled high pressure Heavier workload Carries oxygenation blood
LeMone & Burke Ch 30-32 2 Right side- Low oxygenation Low pressure Light workload Goes toward the lungs Left side High oxygenation Thick walled high pressure Heavier workload Carries oxygenation blood
SEPSIS SYNDROME
 INTRODUCTION Sepsis has been defined as a life threatening condition that arises when the body s response to an infection injures its own tissues and organs. Sepsis may lead to shock, multiple organ failure
INTRODUCTION Sepsis has been defined as a life threatening condition that arises when the body s response to an infection injures its own tissues and organs. Sepsis may lead to shock, multiple organ failure
Physiological Causes of Abnormal ABG s
 Physiological Causes of Abnormal ABG s Major Student Performance Objective 1 1. The student will be able to discuss causes for various types of blood gas results. 2. They will also be required to discuss
Physiological Causes of Abnormal ABG s Major Student Performance Objective 1 1. The student will be able to discuss causes for various types of blood gas results. 2. They will also be required to discuss
Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye
 Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye Steroids in ARDS: conclusion Give low-dose steroids if indicated for another problem
Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye Steroids in ARDS: conclusion Give low-dose steroids if indicated for another problem
NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity
 NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Use of NIV 1998-2010 50 45 40 35 30 25 20 15 10 5 0 1998
NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Use of NIV 1998-2010 50 45 40 35 30 25 20 15 10 5 0 1998
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sprung CL, Annane D, Keh D, et al. Hydrocortisone therapy for
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sprung CL, Annane D, Keh D, et al. Hydrocortisone therapy for
Fat Embolism Syndrome
 Fat Embolism Syndrome Dr Jaideep Ravi DA, MD, FRCA, Senior Consultant in Anaesthesiology, Ananthapuri Hospitals and Research Institute, Trivandrum FA Zenker in 1861 first described fat embolism in a rail
Fat Embolism Syndrome Dr Jaideep Ravi DA, MD, FRCA, Senior Consultant in Anaesthesiology, Ananthapuri Hospitals and Research Institute, Trivandrum FA Zenker in 1861 first described fat embolism in a rail
Traumatic Brain Injury
 Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
A Clinico-pharmacological Study on Effect of Methylprednisolone in Acute Respiratory Distress Syndrome Patients
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/135 A Clinico-pharmacological Study on Effect of Methylprednisolone in Acute Respiratory Distress Syndrome Patients
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/135 A Clinico-pharmacological Study on Effect of Methylprednisolone in Acute Respiratory Distress Syndrome Patients
EMT. Chapter 10 Review
 EMT Chapter 10 Review 1. The term shock is MOST accurately defined as: A. a decreased supply of oxygen to the brain. B. cardiovascular collapse leading to inadequate perfusion. C. decreased circulation
EMT Chapter 10 Review 1. The term shock is MOST accurately defined as: A. a decreased supply of oxygen to the brain. B. cardiovascular collapse leading to inadequate perfusion. C. decreased circulation
Objectives. Health care significance of ARF 9/10/15 TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION
 TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION Louisa Chika Ikpeama, DNP, CCRN, ACNP-BC Objectives Identify health care significance of acute respiratory
TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION Louisa Chika Ikpeama, DNP, CCRN, ACNP-BC Objectives Identify health care significance of acute respiratory
ACUTE RESPIRATORY DISTRESS SYNDROME
 ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
Oxygen: Is there a problem? Tom Heaps Acute Physician
 Oxygen: Is there a problem? Tom Heaps Acute Physician Case 1 79-year-old female, diabetic, morbidly obese Admitted with LVF Overnight Reduced GCS?cause 15l NRB in situ ABG showed ph 6.9, pco 2 15.9kPa
Oxygen: Is there a problem? Tom Heaps Acute Physician Case 1 79-year-old female, diabetic, morbidly obese Admitted with LVF Overnight Reduced GCS?cause 15l NRB in situ ABG showed ph 6.9, pco 2 15.9kPa
a. Will not suppress respiratory drive in acute asthma
 Status Asthmaticus & COPD with Respiratory Failure - Key Points M.J. Betzner MD FRCPc - NYEMU Toronto 2018 Overview This talk is about the sickest of the sick patients presenting with severe or near death
Status Asthmaticus & COPD with Respiratory Failure - Key Points M.J. Betzner MD FRCPc - NYEMU Toronto 2018 Overview This talk is about the sickest of the sick patients presenting with severe or near death
Oxygen and ABG. Dr Will Dooley
 Oxygen and ABG G Dr Will Dooley Oxygen and ABGs Simply in 10 cases Recap of: ABG interpretation Oxygen management Some common concerns A-a gradient Base Excess Anion Gap COPD patients CPAP/BiPAP First
Oxygen and ABG G Dr Will Dooley Oxygen and ABGs Simply in 10 cases Recap of: ABG interpretation Oxygen management Some common concerns A-a gradient Base Excess Anion Gap COPD patients CPAP/BiPAP First
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Written Guidelines for Laboratory Testing in Intensive Care - Still Effective After 3 Years
 Written Guidelines for Laboratory Testing in Intensive Care - Still Effective After 3 Years S. M. MEHARI, J. H. HAVILL Intensive Care Unit, Waikato Hospital, Hamilton, NEW ZEALAND ABSTRACT Objective: The
Written Guidelines for Laboratory Testing in Intensive Care - Still Effective After 3 Years S. M. MEHARI, J. H. HAVILL Intensive Care Unit, Waikato Hospital, Hamilton, NEW ZEALAND ABSTRACT Objective: The
Advanced Monitoring of Cardiovascular and Respiratory Systems in Infants Kuwait 2018 Dr. Yasser Elsayed, MD, PhD Director of the Targeted Neonatal
 Advanced Monitoring of Cardiovascular and Respiratory Systems in Infants Kuwait 2018 Dr. Yasser Elsayed, MD, PhD Director of the Targeted Neonatal Echocardiography, Point of Care and Hemodynamics Program
Advanced Monitoring of Cardiovascular and Respiratory Systems in Infants Kuwait 2018 Dr. Yasser Elsayed, MD, PhD Director of the Targeted Neonatal Echocardiography, Point of Care and Hemodynamics Program
Contraindications to time critical surgery; when not to proceed from the perspective of: The Physician A/Prof Peter Morley
 Contraindications to time critical surgery; when not to proceed from the perspective of: The Physician A/Prof Peter Morley British Journal of Surgery 2013; 100: 1045 1049 The risk of 30 day mortality
Contraindications to time critical surgery; when not to proceed from the perspective of: The Physician A/Prof Peter Morley British Journal of Surgery 2013; 100: 1045 1049 The risk of 30 day mortality
CURRICULUM FOR FELLOWSHIP IN CRITICAL CARE MEDICINE
 CURRICULUM FOR FELLOWSHIP IN CRITICAL CARE MEDICINE AIM: The course has been designed to train candidates by the anesthesiologists in the principles and practice of intensive care & artificial ventilation
CURRICULUM FOR FELLOWSHIP IN CRITICAL CARE MEDICINE AIM: The course has been designed to train candidates by the anesthesiologists in the principles and practice of intensive care & artificial ventilation
Unit 4 Problems of Cardiac Output and Tissue Perfusion
 Unit 4 Problems of Cardiac Output and Tissue Perfusion Lemone and Burke Ch 30-32 Objectives Review the anatomy and physiology of the cardiovascular system. Identify normal heart sounds and relate them
Unit 4 Problems of Cardiac Output and Tissue Perfusion Lemone and Burke Ch 30-32 Objectives Review the anatomy and physiology of the cardiovascular system. Identify normal heart sounds and relate them
UPDATE IN HOSPITAL MEDICINE
 UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
Author: Thomas Sisson, MD, 2009
 Author: Thomas Sisson, MD, 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author: Thomas Sisson, MD, 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Resuscitation Patient Management Tool May 2015 MET Event
 OPTIONAL: Local Event ID: Date/Time MET was activated: Time Not Documented MET 2.1 Pre-Event Pre-Event Tab Was patient discharged from an Intensive Care Unit (ICU) at any point during this admission and
OPTIONAL: Local Event ID: Date/Time MET was activated: Time Not Documented MET 2.1 Pre-Event Pre-Event Tab Was patient discharged from an Intensive Care Unit (ICU) at any point during this admission and
Oxygen prescription and administration at the Emergency Department and medical wards in Mater Dei Hospital
 Original Article Oxygen prescription and administration at the Emergency Department and medical wards in Mater Dei Hospital Rachelle Asciak, Valerie Anne Fenech, Jurgen Gatt, Stephen Montefort Abstract
Original Article Oxygen prescription and administration at the Emergency Department and medical wards in Mater Dei Hospital Rachelle Asciak, Valerie Anne Fenech, Jurgen Gatt, Stephen Montefort Abstract
ASTHMA. Epidemiology. Pathophysiology. Diagnosis. IAP UG Teaching slides
 BRONCHIAL ASTHMA ASTHMA Epidemiology Pathophysiology Diagnosis 2 CHILDHOOD ASTHMA Childhood bronchial asthma is characterized by Airway obstruction which is reversible Airway inflammation Airway hyper
BRONCHIAL ASTHMA ASTHMA Epidemiology Pathophysiology Diagnosis 2 CHILDHOOD ASTHMA Childhood bronchial asthma is characterized by Airway obstruction which is reversible Airway inflammation Airway hyper
Respiratory Failure. Causes of Acute Respiratory Failure (ARF): a- Intrapulmonary:
 Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: The National Heart, Lung, and Blood Institute Acute Respiratory
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: The National Heart, Lung, and Blood Institute Acute Respiratory
TACO CASE STUDIES RTC JUNE Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner
 TACO CASE STUDIES RTC JUNE 2017 Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner RISK FACTORS - TACO Age over 70 years although also seen in younger
TACO CASE STUDIES RTC JUNE 2017 Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner RISK FACTORS - TACO Age over 70 years although also seen in younger
Anaesthetic considerations for laparoscopic surgery in canines
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Anaesthetic considerations for laparoscopic surgery in canines Author : Chris Miller Categories : Canine, Companion animal,
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Anaesthetic considerations for laparoscopic surgery in canines Author : Chris Miller Categories : Canine, Companion animal,
Acid Base Balance by: Susan Mberenga RN, BSN, MSN
 Acid Base Balance by: Susan Mberenga RN, BSN, MSN Acid Base Balance Refers to hydrogen ions as measured by ph Normal range: 7.35-7.45 Acidosis/acidemia: ph is less than 7.35 Alkalosis/alkalemia: ph is
Acid Base Balance by: Susan Mberenga RN, BSN, MSN Acid Base Balance Refers to hydrogen ions as measured by ph Normal range: 7.35-7.45 Acidosis/acidemia: ph is less than 7.35 Alkalosis/alkalemia: ph is
Management of acute asthma in children in emergency department. Moderate asthma
 152 Moderate asthma SpO2 92% No clinical features of severe asthma NB: If a patient has signs and symptoms across categories, always treat according to their most severe features agonist 2-10 puffs via
152 Moderate asthma SpO2 92% No clinical features of severe asthma NB: If a patient has signs and symptoms across categories, always treat according to their most severe features agonist 2-10 puffs via
Pulmonary Pearls. Medical Pearls. Case 1: Case 1 (cont.): Case 1: What is the Most Likely Diagnosis? Case 1 (cont.):
 Pulmonary Pearls Christopher H. Fanta, MD Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Medical Pearls Definition: Medical fact that is
Pulmonary Pearls Christopher H. Fanta, MD Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Medical Pearls Definition: Medical fact that is
Incidence of deep vein thrombosis after major spine surgeries with no mechanical or chemical prophylaxis
 29 29 33 Incidence of deep vein thrombosis after major spine surgeries with no mechanical or chemical prophylaxis Author Institution Sreedharan Namboothiri Kovai Medical Center and Hospitals, Coimbatore,
29 29 33 Incidence of deep vein thrombosis after major spine surgeries with no mechanical or chemical prophylaxis Author Institution Sreedharan Namboothiri Kovai Medical Center and Hospitals, Coimbatore,
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Course Handouts & Disclosure
 COPD: Disease Trajectory and Hospice Eligibility Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Hospice Education Network Course Handouts & Disclosure To download presentation
COPD: Disease Trajectory and Hospice Eligibility Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Hospice Education Network Course Handouts & Disclosure To download presentation
Case Scenario 3: Shock and Sepsis
 Name: Molly Boyle 1. Define the term shock (Lewis textbook): Shock is a syndrome characterized by decreased perfusion and impaired metabolism. Shock can have a number of causes that result in damage to
Name: Molly Boyle 1. Define the term shock (Lewis textbook): Shock is a syndrome characterized by decreased perfusion and impaired metabolism. Shock can have a number of causes that result in damage to
ARDS: an update 6 th March A. Hakeem Al Hashim, MD, FRCP SQUH
 ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
ISF criteria (International sepsis forum consensus conference of infection in the ICU) Secondary peritonitis
 Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
3. Which of the following would be inconsistent with respiratory alkalosis? A. ph = 7.57 B. PaCO = 30 mm Hg C. ph = 7.63 D.
 Pilbeam: Mechanical Ventilation, 4 th Edition Test Bank Chapter 1: Oxygenation and Acid-Base Evaluation MULTIPLE CHOICE 1. The diffusion of carbon dioxide across the alveolar capillary membrane is. A.
Pilbeam: Mechanical Ventilation, 4 th Edition Test Bank Chapter 1: Oxygenation and Acid-Base Evaluation MULTIPLE CHOICE 1. The diffusion of carbon dioxide across the alveolar capillary membrane is. A.
Postoperative Respiratory failure( PRF) Dr.Ahmad farooq
 Postoperative Respiratory failure( PRF) Dr.Ahmad farooq Is it really or/only a postoperative issue Multi hit theory first hits second hits Definition Pulmonary gas exchange impairment that presents after
Postoperative Respiratory failure( PRF) Dr.Ahmad farooq Is it really or/only a postoperative issue Multi hit theory first hits second hits Definition Pulmonary gas exchange impairment that presents after
Assistant Professor, Anaesthesia Department, Govt. General Hospital / Guntur Medical College, Guntur, Andhra Pradesh, India.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. I (August. 2016), PP 87-91 www.iosrjournals.org A Comparative Study of 0.25% Ropivacaine
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. I (August. 2016), PP 87-91 www.iosrjournals.org A Comparative Study of 0.25% Ropivacaine
HEMODYNAMIC DISORDERS
 HEMODYNAMIC DISORDERS Normal fluid homeostasis requires vessel wall integrity as well as maintenance of intravascular pressure and osmolarity within certain physiologic ranges. Increases in vascular volume
HEMODYNAMIC DISORDERS Normal fluid homeostasis requires vessel wall integrity as well as maintenance of intravascular pressure and osmolarity within certain physiologic ranges. Increases in vascular volume
DAILY SCREENING FORM
 DAILY SCREENING FORM Patient s initials: Date of admission: Time of admission: Gender: M F Year of Birth: Type of admission: Medical/Surgical/Postoperative (elective) Days Date Mechanical ventilation Lung
DAILY SCREENING FORM Patient s initials: Date of admission: Time of admission: Gender: M F Year of Birth: Type of admission: Medical/Surgical/Postoperative (elective) Days Date Mechanical ventilation Lung
CHEST INJURY PULMONARY CONTUSION
 CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
Case 1. Case 5/30/2013. Traumatic Brain Injury : Review, Update, and Controversies
 Case 1 Traumatic Brain Injury : Review, Update, and Controversies Shirley I. Stiver MD, PhD 32 year old male s/p high speed MVA Difficult extrication Intubated at scene Case BP 75 systolic / palp GCS 3
Case 1 Traumatic Brain Injury : Review, Update, and Controversies Shirley I. Stiver MD, PhD 32 year old male s/p high speed MVA Difficult extrication Intubated at scene Case BP 75 systolic / palp GCS 3
Neuroprotective Effects for TBI. Craig Williamson, MD
 Neuroprotective Effects for TBI Craig Williamson, MD Neuroprotection in Traumatic Brain Injury Craig Williamson Clinical Assistant Professor Neurocritical Care Fellowship Director Disclosures I will discuss
Neuroprotective Effects for TBI Craig Williamson, MD Neuroprotection in Traumatic Brain Injury Craig Williamson Clinical Assistant Professor Neurocritical Care Fellowship Director Disclosures I will discuss
Objectives. Case Presentation. Respiratory Emergencies
 Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Acute Respiratory Distress
 Acute Respiratory Distress Respiratory Distress: Amos Charles, MD Clinical Associate Professor of Medicine Warren Alpert School of Medicine of the Brown University Providence Rhode Island. Waleed Ibrahim-Ali
Acute Respiratory Distress Respiratory Distress: Amos Charles, MD Clinical Associate Professor of Medicine Warren Alpert School of Medicine of the Brown University Providence Rhode Island. Waleed Ibrahim-Ali
Is ARDS Important to Recognize?
 Is ARDS Important to Recognize? Lorraine B. Ware MD Vanderbilt University Financial Disclosures: research funding from Boehringer Ingelheim, Global Blood Therapeutics Why diagnose ARDS? -initiate specific
Is ARDS Important to Recognize? Lorraine B. Ware MD Vanderbilt University Financial Disclosures: research funding from Boehringer Ingelheim, Global Blood Therapeutics Why diagnose ARDS? -initiate specific
Maternal Collapse Guideline
 Maternal Collapse Guideline Guideline Number: 664 Supersedes: Classification Clinical Version No: Date of EqIA: Approved by: Date Approved: Date made active: Review Date: 1 Obstetric Written Documentation
Maternal Collapse Guideline Guideline Number: 664 Supersedes: Classification Clinical Version No: Date of EqIA: Approved by: Date Approved: Date made active: Review Date: 1 Obstetric Written Documentation
Non-invasive Ventilation protocol For COPD
 NHS LANARKSHIRE MONKLANDS HOSPITAL Non-invasive Ventilation protocol For COPD April 2017 S Baird Review Date: Oct 2019 Approved by Medical Directorate Indications for Non-Invasive Ventilation (NIV) NIV
NHS LANARKSHIRE MONKLANDS HOSPITAL Non-invasive Ventilation protocol For COPD April 2017 S Baird Review Date: Oct 2019 Approved by Medical Directorate Indications for Non-Invasive Ventilation (NIV) NIV
Pneumonia in the Hospitalized
 Pneumonia in the Hospitalized Patient: Use of Steroids Nicolette Myers, MD Pulmonary/Sleep/Critical Care November 9, 2018 Park Nicollet Clinic Facts About Pneumonia CAP is the 8 th most common cause of
Pneumonia in the Hospitalized Patient: Use of Steroids Nicolette Myers, MD Pulmonary/Sleep/Critical Care November 9, 2018 Park Nicollet Clinic Facts About Pneumonia CAP is the 8 th most common cause of
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
