Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines
|
|
|
- Lilian Bates
- 5 years ago
- Views:
Transcription
1 Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines Non-Accidental Trauma (NAT) PEDIATRIC Practice Management Guideline Contact: Trauma Center Medical Director/ Trauma Center Trauma Program Manager Effective: 04/2014 Last Reviewed: 07/ Purpose: To provide guidelines for the initial evaluation and management of all children <12 months of age or non-ambulatory with a skeletal fracture or other injury suspicious for abuse, and children months of age with an injury suspicious for abuse. Older children with injuries concerning for abuse are also evaluated on a case by case basis with recommendations included in this guideline. For the purpose of this guideline, non-ambulatory children are defined as those who are not walking independently. Cruising is not considered walking independently. 2.0 Etiology/Statistics: There were 678,932 cases of confirmed child abuse and neglect reported to the U.S. Department of Health & Human Services in o This is equal to 9.1 victims per 1,000 children in this population. o The victims of abuse were 44% white, 22.4% Hispanic, and 21.2% African- American. o The highest rate of abuse occurs in the first year of life with a rate of 23.1 per 1,000 children. There were 1,484 total deaths from child abuse or neglect reported to the U.S. Department of Health & Human Services in o This is equal to 2.04 deaths per 100,000 children. o Nearly three quarters (73.9%) of the deaths reported were younger than 3 years old. o 79% of deaths were caused by one or both parents. 3.0 Differential Diagnosis: Accidental injury and certain medical conditions may mimic abuse. 4.0 Guideline Eligibility Criteria: Page 1 of 11
2 Children from newborn through adolescence with an injury suspicious for abuse. 5.0 Guideline Exclusion Criteria: Children in motor-vehicle collision, regardless of age or ambulatory status are excluded from this guideline. 6.0 Critical Points of Evidence: 6.1 Evidence Supports Physical abuse is the cause of 12-20% of all fractures in infants and toddlers (3). Age is a strong determinant of abuse potential and a non-ambulatory child presenting with a fracture should be regarded highly suspicious of NAT (2). Children <2 years with fractures suspicious for child abuse should have a radiographic skeletal survey to look for other bone injuries or osseous abnormalities. (3). Additional fractures are identified in approximately 10% of skeletal surveys, with higher yields in infants (3). Abusive head trauma (AHT) is the leading cause of death from trauma in children younger than 2 years (6). It is vital that a diagnosis of abuse is not missed, with evidence showing that in 50-80% of fatal or near-fatal abuse cases there was evidence of prior abusive injuries (2). Infants are at the greatest risk of abusive head injury with the median age between 2-6 months, correlating with the peak age of crying (6). AHT should be considered in all children with neurological signs and symptoms, especially if there is no history of trauma, or history of minor trauma such as a short fall (17). Head CT is recommended as the initial imaging modality when there is concern for AHT (9, 18). Bruising or bleeding in a child may raise the concern for child abuse. Assessing whether the findings are the result of trauma and/or whether the child has a bleeding disorder is important (1). The patient with bruising or intracranial hemorrhage with concern for abuse should have a hematological evaluation including CBC, PT/PTT, VW panel, and Factor VIII and IX levels to rule out the most common bleeding disorders (1). 6.2 Evidence Lacking/Inconclusive Hepatic transaminases have traditionally been ordered to screen for internal injuries in patients who have sustained blunt abdominal trauma, as well as in the non-accidental trauma work-up of young children with skeletal or other injuries suspicious for abuse. There is limited data as to what threshold indicates the need for further testing such as CT abd/pelvis. While levels of IU/L are often used to trigger imaging in the patient with blunt abdominal trauma, there is recent data to suggest that children Page 2 of 11
3 evaluated for physical abuse with transaminase levels >80 IU/L should undergo definitive testing for abdominal injury (13). Providers may have concern regarding radiation exposure and the increased number of patients who will undergo CT abd/pelvis to rule out abdominal injury with the lower threshold for ALT/AST. Urinalysis has also been traditionally used to identify patients with microscopic hematuria that may indicate occult internal injury both in the setting of NAT and in the determination for imaging in blunt abdominal trauma. It is unclear which patients undergoing NAT work-up would benefit from urinalysis screening and what threshold of RBCs may indicate the need for further imaging. Since UA screening is low-cost and non-invasive, it seems prudent to obtain a urinalysis along with transaminase levels when screening for abuse. 7.0 Diagnostic Evaluation: Reasons to suspect abuse: 7.1 History: No explanation or vague explanation of an injury. An important detail of the explanation changes significantly. An explanation that is inconsistent with the pattern, age, or severity of the injury or injuries. An explanation that is inconsistent with the child s physical and/or developmental capabilities. Different caregivers provide different explanations for the injury or injuries or a single caregiver provides history that change over time. 7.2 Physical Examination: Age o Injuries in non-ambulatory children are of greatest concern for abuse. Bruising o Bruising in children<9 months of age o Bruising in non-ambulatory children o Patterned bruising o Extensive or clustered bruising o Intraoral injuries (frenulum tears) <9 months or non-ambulatory Burns o Patterned burns, i.e. suspected cigarette burns o Stocking or glove immersion burns o Burns in non-ambulatory patients Fractures (highly specific) o Classic metaphyseal lesions o Rib fractures Page 3 of 11
4 o Scapular or sternal fractures Fractures (moderately specific) o Long bone fractures in non-ambulatory children o Digit fractures o Complex skull fractures o Vertebral body fractures/subluxations o Epiphyseal separations o Fractures of varying ages o Multiple fractures, especially bilateral Abusive head trauma (AHT) Vague presenting signs and symptoms may be associated with AHT. AHT should be considered in the differential diagnoses of young children with non-specific findings such as: o Altered mental status o Fussiness o Vomiting o Lethargy o Seizures o Acute life threatening event o Apnea Principles of Clinical Management 8.0 Initial Evaluation Children < 12months or non-ambulatory children with a skeletal fracture or an injury suspicious for abuse will receive the following: Thorough history to include any history of trauma as well as circumstances leading to the discovery of injury. It is important to document the history as early as practical in the process. Head-to-toe physical assessment: This includes thorough documentation of all abnormal findings. Social services consultation Skeletal survey Transaminase Levels (ALT/AST) Urinalysis with micro Heat CT o All children less than 6 months o Children 6-12 months with neurologic abnormality and/or external evidence of head injury. See signs of abusive head trauma under section Initial Evaluation Children months with an injury suspicious for abuse will receive the following: Thorough history to include any history of trauma as well as circumstances leading to the discovery of injury. It is important to document the history as early as practical in the process. Page 4 of 11
5 Head-to-toe physical assessment: This includes thorough documentation of all abnormal findings. Social services consultation Skeletal survey Transaminase levels (ALT/AST) Urinalysis with micro Head CT o Children with a neurologic abnormality and/or external evidence of head injury. See signs of abusive head trauma under section Initial Evaluation Children >24 months with an injury suspicious for abuse will receive the following: Thorough history to include any history of trauma as well as circumstances leading to the discovery of injury. It is important to document the history as early as practical in the process. Head-to-toe physical assessment: This includes thorough documentation of all abnormal findings. Social services consultation Skeletal survey recommended only in children up to 5 years on a case-by-case basis: o i.e. unconscious patient, non-verbal patient, or inadequate exam Transaminase levels (ALT/AST) o Recommended with multiple or severe injuries or with concern for abd/pelvic trauma. o Order in conjunction with UA as indicated Urinalysis with micro o Recommended with multiple or severe injuries or with concern for abd/pelvic trauma. o Order in conjunction with ALT/AST as indicated o Order in conjunction with urine toxicology as indicated Head CT o Children with neurologic abnormality and/or external evidence of head injury. See signs of abusive head trauma under section Further laboratory evaluation specific to the injury or individual circumstances Urine and serum toxicology o Concern for ingestion o Evidence of neurologic abnormality If head CT is obtained due to concerns for abusive head trauma (fussiness, vomiting, seizures, ALTE, etc.), urine and serum toxicology is also indicated o Report or suspicion of substance abuse in caregiver, either by history or presentation. CBC, PT/PTT, VW Panel, Factor VIII and IX levels* Page 5 of 11
6 o o o Intracranial hemorrhage (ICH) concerning for abusive head trauma (i.e. diffuse intracranial hemorrhage, mixed density blood, bilateral subdural hematomas, ICH with altered mental status, ICH with no history of trauma). Bruising concerning for inflicted injury. Factors which increase the likelihood of abusive bruising include: <9 months of age Non-ambulatory child Location: buttocks, genitals, ears, hands, feet, torso Patterned bruising Extensive or clustered bruising Other injury associated with bleeding Solid organ injury concerning for inflicted trauma * Patients with clinically significant bleeding (especially if surgery may be required) will need urgent CBC, PT/PTT and Platelet Function Assay (PFA). Hematology should be consulted urgently if PFA is elevated Further Diagnostic Evaluation Abd/pelvis CT with IV contrast o Abnormal abdominal exam such as bruising, distention, tenderness, vomiting o Consider with >10 RBCs per HPF on urinalysis o ALT/AST >80 mg/dl Or admit to Trauma Service for observation and serial abdominal exams. MRI brain/spine o May be indicated with ICH to further delineate injury, per neurosurgery or CARE team Consultation Social Services Consult o In patients with a history and exam/diagnostic findings that may be concerning for abuse and warrant a comprehensive SW evaluation. Department of Human Services(DHS) o In accordance with federal and state laws, any person with concerns about the safety of a minor must initiate a referral to Iowa Department of Human Services within 24-hours. If made, the attending provider must be made aware of this referral. BCH Regional Child Protection Center (RCPC) notification/consultation o Indicated with concerns of abuse identified by social worker or attending physician such as inconsistency between pattern of injury an mechanism. Orthopedic consultation o Children < 12 months or non-ambulatory children with a long bone fracture must have orthopedic consultation prior to disposition from the ED. This may include radiologic review only, at the discretion of the orthopedic team. Page 6 of 11
7 Neurosurgical Consult o All patients with skull fractures (including convexity, base and orbits) must have a neurosurgical consultation prior to discharge from the hospital. See Management of Pediatric Skull Fractures Guideline. Ophthalmology Consult o Indicated in patients with intracranial hemorrhage. Also consider for injuries to the face/neck or eyes and/or eye findings concerning for genetic disorders. Ophthalmology may be consulted by the Trauma Service after admission if appropriate Admission/Disposition Injuries require admission for medical management: o Pediatrics will admit all patients with suspected NAT. o Consult Trauma Service for evaluation on all pts with suspected or proven NAT. o Sub-specialty consultation as indicated. o It is advisable to inform the family of the plan to involve the CARE team if applicable. o Isolated injuries with no ongoing concern for abuse may be admitted to the appropriate surgical sub-specialty as appropriate (Neurosurgery, Orthopedics, Trauma). Injuries DO NOT require admission for medical management: o Reasonable suspicion for abuse: DHS report is made Request DHS involvement for discharge. Once a safe disposition has been established by DHS, the patient may be discharged from the ED. If a safe disposition cannot be developed by DHS in the ED in a timely manner, the patient will be admitted to the Trauma Service for observation until a plan is in place. o Provider is unsure if there is reasonable suspicion for abuse: Discuss with RCPC team for further direction, if available. A DHS report at discretion of provider/sw. Discharge home at discretion of provider. o No reasonable suspicion for abuse: No CPS referral made. Documentation indicating no concerns for abuse Important considerations: Admitted for a Medical Diagnosis Page 7 of 11
8 o Patients admitted for a non-traumatic diagnosis (i.e. seizures, FTT) and later suspected to have an injury should have a Trauma Consultation as soon as the injury is discovered. Trauma team consultation should not be delayed for a sub-specialty surgical consult Concern for abuse outside BCH ED Outside hospitals: o Children <12 months or non-ambulatory with a skeletal fracture or other injury suspicious for abuse should be transferred to BCH ED for evaluation. o Children > 12months with an injury suspicious for abuse should also be transferred to BCH ED prior to referral for orthopedic or other sub-specialty follow-up. It is prudent to maintain a high index of suspicion for abuse in children under 24 months of age with a fracture or other injury. Reference 1. Anderst, J.D. et al. Evaluation for Bleeding Disorders in Suspected Child Abuse. Pediatrics 2014; 131 (4), e1314-e Clark, N.M.P. et al. The incidence of fractures in children under the age of 24 months In relation to non-accidental injury. Injury (2011). Doi:10.106/j.injury Flaherty, E.G. et al. Evaluating Children with Fractures for Child Physical Abuse. 2014; 133(2): e477-e Haney S.B., Starling, S.P., Heisler, K.W., Okwara, L. Characteristics of falls and risk of injury in children younger than 2 years. Pediatric Emergency Care. 2010; 26 (12), Harris, T.S. Bruises in Children: Normal or Child Abuse? Journal of Pediatric Health Care. 2009; 24 (4): Herman, B.E. et al. Abuse Head Trauma. Pediatric Emerg Care. (2011); 72 (1): Kellog, N.D. Evaluation of suspected physical abuse. Pediatrics. 2007; 119 (6), Kemp, A.M. et al. What are the clinical and radiological characteristics of spinal injuries from physical abuse: a systematic review. Arch Dis Child. 2010; 95: Kemp, A.M., Dunstand, F., Harrison, S., Morris, S., Mann, M., Rolfe, K., Datta, S., Thomas, D.P., Sibert, J.R., Maguire, S. Patterns of skeletal fractures in child abuse: systematic review. British Medical Journal. 2008; 337, Kemp, A.m. Abusive head trauma: recognition and the essential investigation. Arch Dis Child Educ Pract Ed. 2011; 96: Laskey, A.L.L., et al. Yield of Skeletal Survey in Children < 18 Months of Age Presenting with Isolated Skull Fractures. Journal of Pediatrics. 2013; 162 (1), Levin, A.V. Retinal Hemorrhage in Abuse Head Trauma. Pediatrics. 2010; 126 (5): Lindberg, R.A. et al. Utility of Hepatic Transaminases in Children with Concern for Abuse. Pediatrics. 2014; 131(2, Page 8 of 11
9 14. Loder, R.T., Feinburg, J.R. Orthopedic injuries in children with non-accidental trauma. Journal of Pediatric Orthopedics. 2007; 27(4), Pandya, N.K., Baldwin, K., Wolfgruber, H., Christian, C., Drummond, D., Hosalkar, H.S. Child abuse and orthopedic injury patterns: analysis at a level I pediatric trauma center. Journal of Pediatric Orthopedics. 2009; 29 (6), Rubin, D., Christian, C., Bilaniuk, L., Zazyczny, K., & Durbin, D. Occult head injury in high-risk abused children. Pediatrics 2003; 111(6), Sieswerda-Hoogendoom, T. et al. Abusive Head Trauma Part I. Clinical aspects. Eur J Pediatr Doi /s U.S. Department of Health and Human Services, Administration for Children and Families, Administration on Children, Youth and Families, Children s Bureau. (2015). Child maltreatment Available from Wilson, M.S. et al. Utility of Head Computer Tomography in Children with a Single Extremity Fracture. Journal of Pediatrics; Page 9 of 11
10 A. Evaluation of children < 12 months or non-ambulatory with a skeletal fracture or other injury suspicious for abuse: Thorough history Head-to-toe physical assessment Social Services consultation Skeletal survey ALT/AST UA with micro Head CT o All children less than 6 months o Children with neurologic abnormality (see section 7.2) and/or external evidence of head injury B. Blood and urine (additional evaluation) as indicated: Urine & serum toxicology Concern for ingestion Evidence of neurologic abnormality (if head CT is obtained) Report or suspicion of substance abuse in caregiver by history or presentation CBC, PT/PTT, VW Panel, Factor VIII & IX levels Intracranial hemorrhage (ICH) concerning for abusive head trauma o Diffuse ICH o ICH with mixed density blood o Bilateral SDH o ICH with altered mental status o ICH with no history of trauma Bruising concerning for inflicted injury o < 9 months of age o Non-ambulatory child o Location: buttocks, genitals, ears, hands, feet, torso o Patterned bruising o Extensive or clustered bruising Other injury associated with bleeding such as solid organ injury Bone abnormality evaluation Vit D 25, PTH, Alkaline Phosphatase, Calcium, Phosphorus levels Skeletal fracture concern for abuse Radiographic concern for osteopenia or metabolic bone disease C. Consultation as indicated: Neurosurgical Consultation All patients with skull fractures (including convexity, base and orbits) must have a neurosurgical consultation prior to discharge from the hospital. Orthopedic Consultation Children < 12 months or non-ambulatory children with a long bone fracture must have orthopedic consultation prior to disposition from the ED. Ophthalmology Consultation Patients with ICH; also consider for injuries to the face/neck or eyes and eye findings concerning for genetic disorders. Ophtho may be consulted after Page 10 of 11
11 D. Diagnostic imaging (additional) as indicated: CT Abd/Pelvis with IV contrast Abnormal chest or abdominal exam Consider with >10 RBCs per HPF on urinalysis ALT/AST >80 mg/dl imaging (additional) as indicated: Neurosurgical Consultation All patients with skull fractures (including convexity, base and orbits) must have a neurosurgical consultation prior to discharge from the hospital. Page 11 of 11
CHILD MALTREATMENT- GUIDELINES FOR SUSPICION and INITIAL MEDICAL EVALUATION DRAFT May Leslie M. Quinn M.D.
 CHILD MALTREATMENT- GUIDELINES FOR SUSPICION and INITIAL MEDICAL EVALUATION DRAFT May 2012 - Leslie M. Quinn M.D. PHYSICAL ABUSE: For any child presenting with signs and or symptoms of an injury consider
CHILD MALTREATMENT- GUIDELINES FOR SUSPICION and INITIAL MEDICAL EVALUATION DRAFT May 2012 - Leslie M. Quinn M.D. PHYSICAL ABUSE: For any child presenting with signs and or symptoms of an injury consider
Suspected Physical Abuse Clinical Practice Guideline
 Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
Abuse or Accident? Suzanne B. Haney, MD, FAAP Child Abuse Pediatrics
 Abuse or Accident? Suzanne B. Haney, MD, FAAP Child Abuse Pediatrics Disclosure I have nothing to disclose Objectives Describe common accidental injuries which can be confused with child abuse Describe
Abuse or Accident? Suzanne B. Haney, MD, FAAP Child Abuse Pediatrics Disclosure I have nothing to disclose Objectives Describe common accidental injuries which can be confused with child abuse Describe
Overview of Abusive Head Trauma: What Everyone Needs to Know. 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012
 Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Disclosure. Physical Abuse. Objectives. What is the Mechanism of the Injury?
 Disclosure Abuse or Not Abuse: What is the Answer? Natalie Kissoon, MD Assistant Professor Division of Child Abuse Pediatrics University of Texas Health Science Natalie Kissoon, MD has no relationships
Disclosure Abuse or Not Abuse: What is the Answer? Natalie Kissoon, MD Assistant Professor Division of Child Abuse Pediatrics University of Texas Health Science Natalie Kissoon, MD has no relationships
The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast
 The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast September 27, 2018 Introduction: Hello everyone, my name is Dominique Piché
The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast September 27, 2018 Introduction: Hello everyone, my name is Dominique Piché
PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation **
 PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation ** I. RECOGNITION A. History 1. Unexplained or un-witnessed injury 2.
PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation ** I. RECOGNITION A. History 1. Unexplained or un-witnessed injury 2.
Evaluation of a Pediatric Patient
 September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
2/13/13. Ann S. Botash, MD SUNY Upstate Medical University
 Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
Bilateral rib fractures 2 on right and 1 on left In different stages of healing, with left fracture older than right fractures
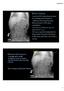 More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
OVERVIEW OF CHILD PHYSICAL ABUSE
 2011 MFMER slide-1 OVERVIEW OF CHILD PHYSICAL ABUSE Mark S. Mannenbach, MD Mayo Medical Center Rochester, MN 2011 MFMER slide-2 Objectives At the conclusion of this session, the participant will be able
2011 MFMER slide-1 OVERVIEW OF CHILD PHYSICAL ABUSE Mark S. Mannenbach, MD Mayo Medical Center Rochester, MN 2011 MFMER slide-2 Objectives At the conclusion of this session, the participant will be able
of Trauma Assembly 27 th Page 1
 Eastern Association for the Surgery of Trauma 27 th Annual Scientific Assembly Sunrise Session 08 To Scan or Not To Scan Thatt is the Question January 16, 2014 Waldorf Astoria Naples Naples, Floridaa Page
Eastern Association for the Surgery of Trauma 27 th Annual Scientific Assembly Sunrise Session 08 To Scan or Not To Scan Thatt is the Question January 16, 2014 Waldorf Astoria Naples Naples, Floridaa Page
Pediatric Abusive Head Trauma
 Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
Subtle Signs of Child Abuse Child s Protection Office MOH Presented by Dr.Fatoumah Alabdulrazzaq M.D,FRCPC,FAAP,PEM(C)
 Subtle Signs of Child Abuse Child s Protection Office MOH Presented by Dr.Fatoumah Alabdulrazzaq M.D,FRCPC,FAAP,PEM(C) Cutaneous Injuries Bruise : injury to soft tissues in which skin is not broken, characterized
Subtle Signs of Child Abuse Child s Protection Office MOH Presented by Dr.Fatoumah Alabdulrazzaq M.D,FRCPC,FAAP,PEM(C) Cutaneous Injuries Bruise : injury to soft tissues in which skin is not broken, characterized
Radiological investigations
 Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Guide to the Medical Evaluation in Suspected Physical Abuse
 Guide to the Medical Evaluation in Suspected Physical Abuse Introduction Every year more than 3 million referrals are made to child protective services for concerns of child abuse and neglect with almost
Guide to the Medical Evaluation in Suspected Physical Abuse Introduction Every year more than 3 million referrals are made to child protective services for concerns of child abuse and neglect with almost
Non-Accidental Trauma (NAT) Protocol
 Non-Accidental Trauma (NAT) Protocol All children suspected of non-accidental trauma will have a complete work-up including a complete history and physical exam with a focus on injuries and explanation
Non-Accidental Trauma (NAT) Protocol All children suspected of non-accidental trauma will have a complete work-up including a complete history and physical exam with a focus on injuries and explanation
Analysis of pediatric head injury from falls
 Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Children diagnosed with skull fractures are often. Transfer of children with isolated linear skull fractures: is it worth the cost?
 clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
Reviewing the recent literature to answer clinical questions: Should I change my practice?
 Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age. DRAFT REVIEW May 2008
 Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age DRAFT REVIEW May 2008 Responsibility for monitoring Review and update CPU Dr. Jean Herbison Current
Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age DRAFT REVIEW May 2008 Responsibility for monitoring Review and update CPU Dr. Jean Herbison Current
Index. Note: Page numbers of article titles are in bold face type.
 Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
I have no financial disclosures.
 In the Belly of the Whale: Surviving Thoracoabdominal Trauma Debra Esernio Jenssen, MD, FAAP I have no financial disclosures. Objectives Review epidemiology of abusive chest and abdominal trauma. Identify
In the Belly of the Whale: Surviving Thoracoabdominal Trauma Debra Esernio Jenssen, MD, FAAP I have no financial disclosures. Objectives Review epidemiology of abusive chest and abdominal trauma. Identify
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines
 Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Blunt Abdominal Trauma Evaluation and Management Guideline PEDIATRIC Practice Management Guideline Contact: Trauma Center
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Blunt Abdominal Trauma Evaluation and Management Guideline PEDIATRIC Practice Management Guideline Contact: Trauma Center
Use of CT in minor traumatic brain injury. Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD
 Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Recognising and Managing Child Abuse in General Practice. Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital
 Recognising and Managing Child Abuse in General Practice Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital Definition Outline Importance of Child Abuse Common
Recognising and Managing Child Abuse in General Practice Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital Definition Outline Importance of Child Abuse Common
The Viewing Study Guide for Physical Abuse Slides
 The Viewing Study Guide for Physical Abuse Slides Adapted From The Visual Diagnosis of Non-Accidental Trauma and Failure to Thrive A Study Guide By Barton D. Schmitt, M.D. in Cooperation with The American
The Viewing Study Guide for Physical Abuse Slides Adapted From The Visual Diagnosis of Non-Accidental Trauma and Failure to Thrive A Study Guide By Barton D. Schmitt, M.D. in Cooperation with The American
Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision
 Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision Support Using the Canadian CT Head Rule to Reduce Unnecessary
Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision Support Using the Canadian CT Head Rule to Reduce Unnecessary
Pediatric head trauma: the evidence regarding indications for emergent neuroimaging
 DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
The Evaluation of Suspected Child Physical Abuse
 CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care The Evaluation of Suspected Child Physical Abuse Cindy W. Christian, MD, FAAP, COMMITTEE ON CHILD ABUSE AND NEGLECT Child physical
CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care The Evaluation of Suspected Child Physical Abuse Cindy W. Christian, MD, FAAP, COMMITTEE ON CHILD ABUSE AND NEGLECT Child physical
PEM GUIDE CHILDHOOD FRACTURES
 PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
Common Abusive Skeletal Injuries
 Common Abusive Skeletal Injuries Paul Kleinman, M.D. Children s Hospital Harvard Medical School Boston, Ma. Rib fractures, especially posteromedial Rib fractures, especially posteromedial Kemp AM et. Al.
Common Abusive Skeletal Injuries Paul Kleinman, M.D. Children s Hospital Harvard Medical School Boston, Ma. Rib fractures, especially posteromedial Rib fractures, especially posteromedial Kemp AM et. Al.
PEDIATRIC MILD TRAUMATIC HEAD INJURY
 PEDIATRIC MILD TRAUMATIC HEAD INJURY October 2011 Quality Improvement Resources Illinois Emergency Medical Services for Children is a collaborative program between the Illinois Department of Public Health
PEDIATRIC MILD TRAUMATIC HEAD INJURY October 2011 Quality Improvement Resources Illinois Emergency Medical Services for Children is a collaborative program between the Illinois Department of Public Health
Injuries in Non Mobile Infants Protocol
 Injuries in Non Mobile Infants Protocol Contents 1. Introduction 2. Definition 3. Recommended Action 4. Specific considerations for disabled children 5. Accidental / non-accidental / inconclusive categories
Injuries in Non Mobile Infants Protocol Contents 1. Introduction 2. Definition 3. Recommended Action 4. Specific considerations for disabled children 5. Accidental / non-accidental / inconclusive categories
Validity of Caregivers Reports on Head Trauma Due to Falls in Young Children Aged Less than 2 Years
 Clinical Medicine Insights: Pediatrics Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Validity of Caregivers Reports on Head Trauma Due
Clinical Medicine Insights: Pediatrics Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Validity of Caregivers Reports on Head Trauma Due
5 B s of Child Physical Abuse: Bruises, Burns, Bones, Bellies, and Brains
 5 B s of Child Physical Abuse: Bruises, Burns, Bones, Bellies, and Brains Kristen Reeder, MD Child Abuse Pediatrician, REACH Program Children s Health SM Children s Medical Center Dallas Assistant Professor
5 B s of Child Physical Abuse: Bruises, Burns, Bones, Bellies, and Brains Kristen Reeder, MD Child Abuse Pediatrician, REACH Program Children s Health SM Children s Medical Center Dallas Assistant Professor
Overview. Overview. Chapter 30. Injuries to the Head and Spine 9/11/2012. Review of the Nervous and Skeletal Systems. Devices for Immobilization
 Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Abuse Or Not? Interactive Visual Clues in Child Abuse
 Abuse Or Not? Interactive Visual Clues in Child Abuse Amy Baxter MD FAAP FACEP Associate Clinical Professor Medical College of Georgia 4 month old sleepy vomiting Mom works nights Wouldn t feed well Shivering
Abuse Or Not? Interactive Visual Clues in Child Abuse Amy Baxter MD FAAP FACEP Associate Clinical Professor Medical College of Georgia 4 month old sleepy vomiting Mom works nights Wouldn t feed well Shivering
Evidence Base for Child Abuse Fractures
 Evidence Base for Child Abuse Fractures SPR Sunrise Session May 17, 2018 Megan B. Marine, MD, FAAP Assistant Professor of Clinical Radiology, Pediatric Division Co-Director, Pediatric Radiology Fellowship
Evidence Base for Child Abuse Fractures SPR Sunrise Session May 17, 2018 Megan B. Marine, MD, FAAP Assistant Professor of Clinical Radiology, Pediatric Division Co-Director, Pediatric Radiology Fellowship
Instructional Course #34. Review of Neuropharmacology in Pediatric Brain Injury. John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD
 Instructional Course #34 Review of Neuropharmacology in Pediatric Brain Injury John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD Outline of Course 1. Introduction John Pelegano MD 2. Neuropharmocologic
Instructional Course #34 Review of Neuropharmacology in Pediatric Brain Injury John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD Outline of Course 1. Introduction John Pelegano MD 2. Neuropharmocologic
Annotation. Outcomes of infants and children with inflicted traumatic brain injury
 Outcomes of infants and children with inflicted traumatic brain injury Kathi L Makaroff* MD, Research Instructor of Pediatrics; Frank W Putnam MD, Director, Mayerson Center for Safe and Healthy Children,
Outcomes of infants and children with inflicted traumatic brain injury Kathi L Makaroff* MD, Research Instructor of Pediatrics; Frank W Putnam MD, Director, Mayerson Center for Safe and Healthy Children,
Shenandoah Co. Fire & Rescue. Injuries to. and Spine. December EMS Training Bill Streett Training Section Chief
 Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
2. Blunt abdominal Trauma
 Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
Imaging in the Trauma Patient
 Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
USASOC Neurocognitive Testing and Post Injury Evaluation and Treatment Clinical Practice Guideline (CPG)
 USASOC Neurocognitive Testing and Post Injury Evaluation and Treatment Clinical Practice Guideline (CPG) Note: The intent of this CPG is to serve as general guidance for medics and medical officers. It
USASOC Neurocognitive Testing and Post Injury Evaluation and Treatment Clinical Practice Guideline (CPG) Note: The intent of this CPG is to serve as general guidance for medics and medical officers. It
Brain and Cervico-Medullary Injury : Patterns and Mechanisms
 Brain and Cervico-Medullary Injury : Patterns and Mechanisms P. Ellen Grant MD Associate Professor of Radiology, HMS Director, Center for Fetal-Neonatal Neuroimaging & Developmental Science Children s
Brain and Cervico-Medullary Injury : Patterns and Mechanisms P. Ellen Grant MD Associate Professor of Radiology, HMS Director, Center for Fetal-Neonatal Neuroimaging & Developmental Science Children s
Non-accidental Trauma: An unresponsive infant with bilateral retinal hemorrhages.
 Non-accidental Trauma: An unresponsive infant with bilateral retinal hemorrhages. Lucas J. A. Wendel, MD, Susannah Q. Longmuir, MD, and Nasreen A. Syed, MD February 12, 2009 Chief Complaint: 7 month old
Non-accidental Trauma: An unresponsive infant with bilateral retinal hemorrhages. Lucas J. A. Wendel, MD, Susannah Q. Longmuir, MD, and Nasreen A. Syed, MD February 12, 2009 Chief Complaint: 7 month old
10/8/17. I have no disclosures. What are they? Upper extremity fractures Lower extremity fractures Non accidental trauma
 I have no disclosures Upper extremity fractures Lower extremity fractures Non accidental trauma What are they? Fractures of the radius, ulna and/or humerus Who gets them? Active children usually after
I have no disclosures Upper extremity fractures Lower extremity fractures Non accidental trauma What are they? Fractures of the radius, ulna and/or humerus Who gets them? Active children usually after
CLINICAL PRACTICE RESOURCE FOR HOSPITALS AND EMERGENCY DEPARTMENTS: Evaluation and Management of Suspected Child Abuse or Neglect
 CLINICAL PRACTICE RESOURCE FOR HOSPITALS AND EMERGENCY DEPARTMENTS: Evaluation and Management of Suspected Child Abuse or Neglect I. IDENTIFY THE CHILD WHO MAY BE A VICTIM OF ABUSE OR NEGLECT. A. Injuries
CLINICAL PRACTICE RESOURCE FOR HOSPITALS AND EMERGENCY DEPARTMENTS: Evaluation and Management of Suspected Child Abuse or Neglect I. IDENTIFY THE CHILD WHO MAY BE A VICTIM OF ABUSE OR NEGLECT. A. Injuries
Subdural haematoma and effusion in children aged < 2 years
 Subdural haematoma and effusion in children aged < 2 years Zurynski YA 1,2, Marks S 3, Chaseling R 3 on behalf of the Subdural Haematoma study group 1. Australian Paediatric Surveillance Unit 2. The University
Subdural haematoma and effusion in children aged < 2 years Zurynski YA 1,2, Marks S 3, Chaseling R 3 on behalf of the Subdural Haematoma study group 1. Australian Paediatric Surveillance Unit 2. The University
ORTHOPEDIC ASPECTS CHILD ABUSE. A summary of the physical, metaphysical, psychological, and sociological aspects of Non-
 ORTHOPEDIC ASPECTS OF CHILD ABUSE A summary of the physical, metaphysical, psychological, and sociological aspects of Non- Accidental Injury with specific references to both the perpetrator and victim
ORTHOPEDIC ASPECTS OF CHILD ABUSE A summary of the physical, metaphysical, psychological, and sociological aspects of Non- Accidental Injury with specific references to both the perpetrator and victim
Recognizing and Responding to Child Abuse & Neglect
 Recognizing and Responding to Child Abuse & Neglect Maria D. McColgan, MD Associate Professor Drexel University College of Medicine Director, Child Protection Program St. Christopher s Hospital for Children
Recognizing and Responding to Child Abuse & Neglect Maria D. McColgan, MD Associate Professor Drexel University College of Medicine Director, Child Protection Program St. Christopher s Hospital for Children
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Medical Aspects of Child Physical Abuse the approach to physically abused kids. Objectives
 Center for Safe & Healthy Children Medical Aspects of Child Physical Abuse the approach to physically abused kids Nancy S. Harper, MD FAAP Child Abuse Pediatrics Associate Professor of Pediatrics, University
Center for Safe & Healthy Children Medical Aspects of Child Physical Abuse the approach to physically abused kids Nancy S. Harper, MD FAAP Child Abuse Pediatrics Associate Professor of Pediatrics, University
ARTICLE. Intracranial Hemorrhage in Children Younger Than 3 Years
 Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
Can we abolish skull x-rays for head injury?
 ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
Goals. Geriatric Trauma. What s the impact Erlanger Trauma Symposium
 Geriatric Trauma William S. Havron III MD Assistant Professor of Surgery University of Oklahoma Goals Realize the impact of injuries in the ageing population Identify the pitfalls associated with geriatric
Geriatric Trauma William S. Havron III MD Assistant Professor of Surgery University of Oklahoma Goals Realize the impact of injuries in the ageing population Identify the pitfalls associated with geriatric
Pan Scan Instead of Clinical Exam? David A. Spain, MD
 Pan Scan Instead of Clinical Exam? David A. Spain, MD Granted, some patients don t t need CT scan Platinum Package Stanford Special CT Scan Head Neck Chest Abdomen Pelvis Takes about 20 minutes to do
Pan Scan Instead of Clinical Exam? David A. Spain, MD Granted, some patients don t t need CT scan Platinum Package Stanford Special CT Scan Head Neck Chest Abdomen Pelvis Takes about 20 minutes to do
CHILD PHYSICAL ABUSE
 CHILD PHYSICAL ABUSE Kansas Association of Osteopathic Medicine April 13 th, 2018 Jami Jackson DO, FAAP, MPH Children s Mercy Hospitals and Clinics Department of Emergency Medicine Assistant Professor
CHILD PHYSICAL ABUSE Kansas Association of Osteopathic Medicine April 13 th, 2018 Jami Jackson DO, FAAP, MPH Children s Mercy Hospitals and Clinics Department of Emergency Medicine Assistant Professor
ACR Appropriateness Criteria Suspected Physical Abuse Child EVIDENCE TABLE
 6. Merten DF, Carpenter BL. Radiologic imaging of inflicted injury in the child abuse syndrome. Pediatr Clin North Am. 1990;7():815-87. 7. Servaes S, Brown SD, Choudhary AK, et al. The etiology and significance
6. Merten DF, Carpenter BL. Radiologic imaging of inflicted injury in the child abuse syndrome. Pediatr Clin North Am. 1990;7():815-87. 7. Servaes S, Brown SD, Choudhary AK, et al. The etiology and significance
Emergency Department Management of Acute Ischemic Stroke
 Emergency Department Management of Acute Ischemic Stroke R. Jason Thurman, MD Associate Professor of Emergency Medicine and Neurosurgery Associate Director, Vanderbilt Stroke Center Vanderbilt University,
Emergency Department Management of Acute Ischemic Stroke R. Jason Thurman, MD Associate Professor of Emergency Medicine and Neurosurgery Associate Director, Vanderbilt Stroke Center Vanderbilt University,
Just Clear Them The Approach to Medical Clearance
 Just Clear Them The Approach to Medical Clearance Dr. Nalin Ahluwalia MD CCFP(EM) Associate Chief of Staff Emergency Physician Oakville Trafalgar Memorial Hospital My Disclosures None! Exemplary patient
Just Clear Them The Approach to Medical Clearance Dr. Nalin Ahluwalia MD CCFP(EM) Associate Chief of Staff Emergency Physician Oakville Trafalgar Memorial Hospital My Disclosures None! Exemplary patient
Brief Clinical Report: Recognizing Subdural Hemorrhage in Older Adults
 Research Brief Clinical Report: Recognizing Subdural Hemorrhage in Older Adults Mark T. Pfefer, RN, MS, DC *1 ; Richard Strunk MS, DC 2 Address: 1 Professor and Director of Research, Cleveland Chiropractic
Research Brief Clinical Report: Recognizing Subdural Hemorrhage in Older Adults Mark T. Pfefer, RN, MS, DC *1 ; Richard Strunk MS, DC 2 Address: 1 Professor and Director of Research, Cleveland Chiropractic
Kristin s Head Trauma Board Questions 11/07/14
 Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Evaluation of Children with Blunt Abdominal Trauma. James F. Holmes, MD, MPH UC Davis School of Medicine
 Evaluation of Children with Blunt Abdominal Trauma James F. Holmes, MD, MPH UC Davis School of Medicine Objectives Epidemiology of intra-abdominal injury (IAI) Physical examination findings with IAI Laboratory
Evaluation of Children with Blunt Abdominal Trauma James F. Holmes, MD, MPH UC Davis School of Medicine Objectives Epidemiology of intra-abdominal injury (IAI) Physical examination findings with IAI Laboratory
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY
 Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
recommendations of the Royal College of
 Archives of Emergency Medicine, 1993, 10, 138-144 Skull X-ray after head injury: the recommendations of the Royal College of Surgeons Working Party Report in practice R. E. MACLAREN, H. I. GHOORAHOO &
Archives of Emergency Medicine, 1993, 10, 138-144 Skull X-ray after head injury: the recommendations of the Royal College of Surgeons Working Party Report in practice R. E. MACLAREN, H. I. GHOORAHOO &
NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOLS. ACUTE CEREBROVASCULAR ACCIDENT TPA (ACTIVASE /alteplase) FOR THROMBOLYSIS
 NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOLS ACUTE CEREBROVASCULAR ACCIDENT TPA (ACTIVASE /alteplase) FOR THROMBOLYSIS I. Purpose : A. To reduce morbidity and mortality associated
NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOLS ACUTE CEREBROVASCULAR ACCIDENT TPA (ACTIVASE /alteplase) FOR THROMBOLYSIS I. Purpose : A. To reduce morbidity and mortality associated
Med 536 Communicating About Prognosis Workshop. Case 1
 Med 536 Communicating About Prognosis Workshop Case 1 ID / CC: 39 year-old woman status-post motor-vehicle collision History of the Presenting Illness Previously healthy 39 year-old woman was found in
Med 536 Communicating About Prognosis Workshop Case 1 ID / CC: 39 year-old woman status-post motor-vehicle collision History of the Presenting Illness Previously healthy 39 year-old woman was found in
Traumatic Brain Injuries
 Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services OBJECTIVES DEFINITION 11/8/2017. Identify SCIWORA.
 SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
6/23/2017. What do you see? skull fracture
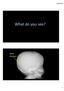 What do you see? skull fracture 1 Head CT On soft tissue windows, posterior soft tissues swelling and hemorrhage, no definite evidence of fracture Head CT On bone windows, fracture now seen subjacent to
What do you see? skull fracture 1 Head CT On soft tissue windows, posterior soft tissues swelling and hemorrhage, no definite evidence of fracture Head CT On bone windows, fracture now seen subjacent to
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Cuyahoga County Division of Children and Family Services (CCDCFS) Policy Statement
 Cuyahoga County Division of Children and Family Services (CCDCFS) Policy Statement Policy Chapter: Case Requirements Policy Number: 5.01.03 Policy Name: Family Cases Involving Substance Use Original Effective
Cuyahoga County Division of Children and Family Services (CCDCFS) Policy Statement Policy Chapter: Case Requirements Policy Number: 5.01.03 Policy Name: Family Cases Involving Substance Use Original Effective
Pediatric metabolic bone diseases
 Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
CONTENT OUTLINE. Child Abuse Pediatrics
 THE AMERICAN BOARD OF PEDIATRICS CONTENT OUTLINE Child Abuse Pediatrics Subspecialty In-Training, Certification, and Maintenance of Certification (MOC) Examinations INTRODUCTION This document was prepared
THE AMERICAN BOARD OF PEDIATRICS CONTENT OUTLINE Child Abuse Pediatrics Subspecialty In-Training, Certification, and Maintenance of Certification (MOC) Examinations INTRODUCTION This document was prepared
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Date of Admission: [DATE]. Date of Discharge:
![Date of Admission: [DATE]. Date of Discharge: Date of Admission: [DATE]. Date of Discharge:](/thumbs/74/71277118.jpg) Date of Admission: [DATE]. Date of Discharge: History of Present Illness: Mr. [NAME] AKA [NAME] is a 31-year-old male who presents to the [PLACE] Trauma Surgery Service as a moderate trauma on [DATE] following
Date of Admission: [DATE]. Date of Discharge: History of Present Illness: Mr. [NAME] AKA [NAME] is a 31-year-old male who presents to the [PLACE] Trauma Surgery Service as a moderate trauma on [DATE] following
O ne million patients are treated annually in United
 859 ORIGIAL ARTICLE Can we abolish skull x rays for head injury? M J Reed, J G Browning, A G Wilkinson, T Beattie... See end of article for authors affiliations... Correspondence to: Matthew J Reed, Accident
859 ORIGIAL ARTICLE Can we abolish skull x rays for head injury? M J Reed, J G Browning, A G Wilkinson, T Beattie... See end of article for authors affiliations... Correspondence to: Matthew J Reed, Accident
CLINICAL MANAGEMENT GUIDELINE PAGE 1 NO REVISION NO. 1 EFFECTIVE DATE: 03/01/2015 SUPERSEDES: 9/26/12
 CLINICAL MANAGEMENT GUIDELINE PAGE 1 REVISION NO. 1 EFFECTIVE DATE: 03/01/2015 SUPERSEDES: 9/26/12 DEPARTMENT (DIVISION): Trauma TITLE: Management of Abdominal Solid Organ Injuries PURPOSE The vast majority
CLINICAL MANAGEMENT GUIDELINE PAGE 1 REVISION NO. 1 EFFECTIVE DATE: 03/01/2015 SUPERSEDES: 9/26/12 DEPARTMENT (DIVISION): Trauma TITLE: Management of Abdominal Solid Organ Injuries PURPOSE The vast majority
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease.
 Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Listen Observe Evaluate Test Refer Guide for primary care providers includes: Surveillance Aid: Assessing Weakness
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Listen Observe Evaluate Test Refer Guide for primary care providers includes: Surveillance Aid: Assessing Weakness
Radiologic Assessment of Child Abuse in Infants: A Focus on Plain Film Analysis of Highly Specific Fractures
 July 2006 Radiologic Assessment of Child Abuse in Infants: A Focus on Plain Film Analysis of Highly Specific Fractures Denise De Las Nueces, Harvard Medical School Year IV General Overview Introduction
July 2006 Radiologic Assessment of Child Abuse in Infants: A Focus on Plain Film Analysis of Highly Specific Fractures Denise De Las Nueces, Harvard Medical School Year IV General Overview Introduction
Pediatric Abdomen Trauma
 Pediatric Abdomen Trauma Susan D. John, MD, FACR Pediatric Trauma Trauma is leading cause of death and disability in children and adolescents Causes and effects vary between age groups Blunt trauma predominates
Pediatric Abdomen Trauma Susan D. John, MD, FACR Pediatric Trauma Trauma is leading cause of death and disability in children and adolescents Causes and effects vary between age groups Blunt trauma predominates
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES
 TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
Neuropathology Of Head Trauma. Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center
 Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
EMS System for Metropolitan Oklahoma City and Tulsa 2019 Medical Control Board Treatment Protocols
 EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 14G PATIENT PRIORITIZATION While each patient will receive the best possible EMS care in a humane and ethical manner, proper patient
EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 14G PATIENT PRIORITIZATION While each patient will receive the best possible EMS care in a humane and ethical manner, proper patient
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 Through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 Through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Abdomen and Genitalia Injuries. Chapter 28
 Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Care for Children Exposed to Illicit Drugs
 Volume 17 l Number 1 l Winter 2009 Care for Children Exposed to Illicit Drugs Resmiye Oral, MD, Assistant Professor of Clinical Pediatrics Director, Child Protection Program, University of Iowa Hospitals
Volume 17 l Number 1 l Winter 2009 Care for Children Exposed to Illicit Drugs Resmiye Oral, MD, Assistant Professor of Clinical Pediatrics Director, Child Protection Program, University of Iowa Hospitals
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Little Kids in Big Crashes The Bio-mechanics of Kids in Car Crashes. Lisa Schwing, RN Trauma Program Manager Dayton Children s
 Little Kids in Big Crashes The Bio-mechanics of Kids in Car Crashes Lisa Schwing, RN Trauma Program Manager Dayton Children s Very Little Research There has been very little research on the forces a crash
Little Kids in Big Crashes The Bio-mechanics of Kids in Car Crashes Lisa Schwing, RN Trauma Program Manager Dayton Children s Very Little Research There has been very little research on the forces a crash
17. Imaging and interventional radiology
 17. Imaging and interventional radiology These guidelines have been adapted from the Leeds Major Trauma Centre Imaging in Paediatric Major Trauma guidelines Written by Dr Annmarie Jeanes (Consultant Paediatric
17. Imaging and interventional radiology These guidelines have been adapted from the Leeds Major Trauma Centre Imaging in Paediatric Major Trauma guidelines Written by Dr Annmarie Jeanes (Consultant Paediatric
Med 536 Communicating About Prognosis Workshop. Case 2
 Med 536 Communicating About Prognosis Workshop Case 2 ID / CC: 33 year-old man with intracranial hemorrhage History of the Presenting Illness 33 year-old man with a prior history of melanoma of the neck
Med 536 Communicating About Prognosis Workshop Case 2 ID / CC: 33 year-old man with intracranial hemorrhage History of the Presenting Illness 33 year-old man with a prior history of melanoma of the neck
PEDIATRIC EMERGENCY DEPARTMENT CLINICAL GUIDELINE: GI SURGICAL EMERGENCIES: VOMITING
 GI SURGICAL EMERGENCIES: VOMITING PYLORIC STENOSIS Population: Infants: onset between 2-5 weeks of age 1 in 250 births Male: female ratio 4:1 Familial incidence History: No vomiting in the first few weeks
GI SURGICAL EMERGENCIES: VOMITING PYLORIC STENOSIS Population: Infants: onset between 2-5 weeks of age 1 in 250 births Male: female ratio 4:1 Familial incidence History: No vomiting in the first few weeks
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Neurology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
RADIOLOGIC TECHNOLOGY PROGRAM COURSE DESCRIPTIONS
 RADIOLOGIC TECHNOLOGY PROGRAM COURSE DESCRIPTIONS Term I: Radiographic Procedures I (3 credits) This course is the first in a series of courses dealing with principals, techniques and radiographic procedures
RADIOLOGIC TECHNOLOGY PROGRAM COURSE DESCRIPTIONS Term I: Radiographic Procedures I (3 credits) This course is the first in a series of courses dealing with principals, techniques and radiographic procedures
Guideline for the Management of Blunt Liver and Spleen Injuries
 Pediatric Trauma Practice Guideline Management of Blunt Liver and Spleen Guideline for the Management of Blunt Liver and Spleen Background: Children are more vulnerable to blunt abdominal injury than adults.
Pediatric Trauma Practice Guideline Management of Blunt Liver and Spleen Guideline for the Management of Blunt Liver and Spleen Background: Children are more vulnerable to blunt abdominal injury than adults.
