Management of Tethered Cord Syndrome in Adults: Experience of 23 Cases
|
|
|
- Giles Cox
- 5 years ago
- Views:
Transcription
1 DOI: / JTN Received: / Accepted: Published Online: Original Investigation Management of Tethered Cord Syndrome in Adults: Experience of 23 Cases Ozden Erhan SOFUOGLU *, Anas ABDALLAH *, Erhan EMEL, Ali Ender OFLUOGLU, Muslum GUNES, Betul GULER Bakirköy Research and Training Hospital for Neurology Neurosurgery, and Psychiatry, Department of Neurosurgery, Istanbul, Turkey * Ozden Erhan SOFUOGLU and Anas ABDALLAH contributed equally to this work. ABSTRACT AIm: Tethered cord syndrome (TCS) is rarely diagnosed in adults. It is a complex clinicopathological entity that remains poorly understood. In this study, clinical outcomes of 23 consecutive congenital TCSs diagnosed in adults have been evaluated to establish a standard approach to treat congenital TCS diagnosed in adults. MaterIal and Methods: Medical records were retrospectively reviewed in 73 cases of TCS who were underwent surgery in our hospital, between 2005 and Cases which diagnosed and treated surgically in adults (patient age > 18 years) were included in this study. Results: Twenty-three adult cases of TCSs were treated surgically and 15 of them were female and 8 were male. The mean age was 30.3±10.7 years. The mean follow-up period was 75.6±40.5 months. The most common complaint was low back pain. The most common findings in the neurological examinations were muscular weakness and urinary. The most common co-malformations were diastematomyelia and vertebral fusion anomalies. Conus medullaris was mostly terminated at the L5 level. Detethering procedure was carried out in 87% of patients and bony septum resection without detethering was applied in 13%. Laminoplasty was performed only in 39.1%. 60.9% of patients were recovered good. 34.8% of patients were improved. The most common complication was cerebrospinal fluid leakage. ConclusIon: Despite the good results obtained in our surgical interventions for symptomatic TCS in adults, tethered cord releasing is complex procedure and has serious complications. Therefore, it is suggested to plan surgery according to symptoms emphasized with full neurological examination, craniospinal imaging and urodynamic tests. Keywords: Tethered cord syndrome, Dysraphic lesions, Scoliosis, Diastematomyelia, Laminoplasty, Intraoperative neurophysiological monitoring, Urodynamic test INTRODUCTION Tethered cord syndrome (TCS) is a deterioration involving an abnormal stretching of the tethered spinal cord, the ascent of which is limited and is disproportionate to the growth of the spinal column (9,13). TCS is not a rare pathological disorder particularly in developing countries. This congenital syndrome usually associates to other syndromes may develop in children who are born to mothers suffered from folic acid deficiency. In contrast, TCS is rarely diagnosed in adults as well as it is a complex clinicopathological entity that remains poorly understood. The incidence of neural tube defects is per 1000 live births worldwide (2). TCS is one of the common spinal dysraphic lesions which have been reduced in developed countries due to supplementation of folic acid during pregnancy and prenatal diagnosis of dysraphic malformations qr code Corresponding author: Anas ABDALLAH abdallahanas@hotmail.com Turk Neurosurg,
2 almost leading to termination of the pregnancy. Presenting symptoms due to a congenital TCS (such as; back pain, leg weakness, foot deformity, scoliosis, sensory loss, and/or bowel or bladder dysfunction) most common occur in children, but in many adult patients, the diagnosis is not established until symptoms manifest. Several pathological conditions including fatty and thickened filum terminale, lipomyelomeningocele, meningocele, split cord malformation, and post-repair myelomeningocele may be responsible for TCS (5). It has been well established that children involved with TCS, whether symptomatic or otherwise, early surgical intervention (detethering) of congenital TCS in children prevents additional neurosurgical deficits (4,9,11). With early diagnosis of these conditions, however, there is an ongoing debate of whether asymptomatic adult patients with a TCS should undergo prophylactic surgery (9). According to Rajpal et al. with advancing age of the patients who involved to congenital TCS, these patients have an increased risk of developing new neurological deteriorations (14), therefore, they suggest surgery for adult patients with TCS to protect patients from new neurological deficits which may be permanent. Despite the management of congenital TCS diagnosed in adulthood remains controversial, results of recent clinical studies of surgical intervention in adults are encouraged (7,9,12,14,19). The question here, how can neurosurgeons manage this complex entity to protect the patients from new deficits and keep their neurological functions intact? Herein, the surgical treatment outcomes of 23 consecutive congenital TCSs diagnosed in adults have been evaluated to find out the perfect (standard protocol) management for TC in adults (according to the authors here). MATERIAL and METHODS This retrospective, randomized study was approved by the medical ethics committee of our hospital. Written informed consent was obtained from all patients for publication of their cases and accompanying images. Medical records were retrospectively reviewed in 73 cases of congenital TCS who were treated surgically in our hospital at department of neurosurgery, between 2005 and TCS cases which diagnosed and treated surgically in adults (patient age > 18 years) were included in this study. The longterm clinical outcomes were evaluated retrospectively using patient complaints, the periods of first complaint and surgery, localizations, co-malformations, magnetic resonance imaging (MRI) findings, recurrence rate and complications. All patients underwent a hemilaminectomy, laminectomy or laminotomy before neurosurgical bony or fibrous septums removal then detethering filum terminale. To avoid serious complications, intraoperative neurophysiological monitoring and laminoplasty were performed especially in recent four years. Postoperative outcomes have been evaluated using neurological scoring system which presented by Klekamp and Samii in 1993 (Table I) (8). Data are expressed as mean±standard deviation (SD) values of the mean, median, and minimum-maximum. Differences among groups were assessed with one-way analysis of variance (ANOVA) using SPSS 21.0 statistical package. Differences were considered statistically significant when p < Surgical Procedure Under general anesthesia and intraoperative neurophysiological monitoring (especially in recent four years) the patients are positioned prone using supporting roll on each side. The paramedian vertical midline incision between the superior and inferior laminas that detected via MRI (e.g. If conus medullaris at L5 level the incision would be extended between L4 to S1) was performed. After dissecting the paraspinal muscles [if the aim was to perform partial or total (complete) laminectomy, the dissection was done unilaterally, but if the surgeons were planning to perform laminoplasty, the dissection done bilaterally]. Hemilaminectomy, laminectomy or laminotomy (in cases of spina bifida occulta, defective laminotomy was used) was completed. If the purpose was laminoplasty, bilateral Table I: Neurological Scoring System (8) Score Pain Intensity Sensory Disturbance, Dysesthesias Motor Weakness Gait Ataxia Sphincter Function 5 None Normal Full power Normal Normal 4 Slight, no medication Present, not significant Tolerable w/ medication Insufficient control w/ medication Severe despite medication Significant, function not restricted Some restriction of function Severe restriction of function Movement against resistance Movement against gravity Unsteady, no aid Mobile w/ aid Slight disturbance, no catheter Residual in urodynamic studies, no catheter* Movement w/o gravity Few steps w/ aid Rarely incontinent Contraction w/o movement Standing w/ aid Frequent catheter 0 Incapacitating Incapacitated function Paralysis Paralysis Permanent catheter *Modified according our protocol. W: with; w/o: without. 2 Turk Neurosurg, 2016
3 laminotomy was performed using high-speed drills or kerrison rongeurs. Then, ligamentum flavum and the adipose tissue were removed. The spinal cord may continue until the S1 or S2 levels by giving some sacral rootlets, the laminectomy or laminotomy should be performed up to this level. The operative microscope is brought in over operation field. Thecal sac should be opened in the midline and tacked up bilaterally using strong sutures. After exposure of all nerve roots, filum terminale and arachnoid bands, the neurosurgeons select the filum terminale using the microscope (generally senior neurosurgeons select the filum terminale according to suspected of its structure). Filum terminale appears darker in color than nerve rootlets under the microscope. This aspect of filum terminale is related to its fibrovascular tag structure that contains a large vessel, which becomes smaller across through thecal sac (10,16,18). On the other hand, this vessel is not a reliable landmark for filum terminale (because similar vessels can be found on the rootlets or no vessel may be seen on filum terminale). Therefore, the neurosurgeons checked it with probe of neurophysiological device. The rootlets at the sacral levels are directed to both sides and may be identified by their size, passing route and location. The arachnoid bands are attached to the thecal sac and rootlets. Both of the nerve rootlets and arachnoid bands are thin and white in color. To detect the place of untethering surgeons put probe of neurophysiological device on the posterior point of the filum terminale, after the save sign (the sign of the neurophysiological device means that the indicated structure is not neural structure) is taken. The rootlets are retracted laterally, then, filum terminale is coagulated and cut after the identification. All connective tissues attached to the caudal part of the spinal cord and conus medullaris should be released. After hemostasis using serum physiologic water, duraplasty is performed using 5.0 absorbable sutures (such as vicryl). In cases of bony septum (BS) or fibrous band (FB) (can detect via study craniospinal MRI), first, resection of BS or FB should be done before untethering conus medullaris. Three cases (13%) of our series were resection of BS or FB enough to relief patients complaints. In cases of dermal sinus, the tracts may be attached to the thecal sac, therefore, these structures should also be removed and duraplasty should be done if it was necessary. In cases of lipoma, cyst or other hamartomas that press on nerve rootlets and narrowing the thecal sac, hamartomas should be removed too. To avoid the serious complications and prevent retethering; lipomas should not be removed aggressively. This decision should be taken after the intraoperative evaluation. Keep the operation field clean and preserve cerebrospinal fluid (CSF) circulation between the neural elements. Illustrative Cases Case 1: A 61-year-old male was referred to our hospital with low back and right leg pains. He was experiencing trauma (failing) before 6 years. His neurological examination was intact; expect weakness in right leg distal muscle group of 4/5, L2-5 and S1 dermatomal hypoesthesia, neurogenic claudication and Babinski: bilateral indifferent. MRI demonstrated that diastematomyelia expends between both of L2 and L4. L3 and L4 vertebral fusion anomaly (block vertebra), at L3 level split cord malformation as bony septum and dermal sinus tract are apparent. Giant cyst extends between L1 and S2; spinal cord at S1-2 level (Figure 1A-C). Urodynamic study showed normocompliance normotonic bladder function. The patient underwent bony septum resection and duraplasty using total L3 and 4 laminoplasty, then cystectomy using total S1 laminoplasty. He made good recovery and was discharged after 3 days without any complication. The patient on his postoperative 48 th month physician visit was doing well. Case 2: A 21-year-old female was referred to our hospital with low back and both legs pain for more than 5 years. In the last month her urinary developed. Her neurological examination was intact; expect rarely loss control of her urination. MRI showed that spinal cord terminates at L5 level (Figure 2). No additional malformation was detected in physical examination. The patient underwent tethered cord release using L5 laminoplasty. She made good recovery and was discharged after 2 days without any complication. The patient on her postoperative 10 th month physician visit was doing well. RESULTS Twenty-three cases of TCSs were treated surgically in fifteen female (65.2%) and eight male (34.8%) patients. Baseline clinical characteristics, co-malformations, treatment, outcomes and complications of treatment were given in Table II. The mean age was 30.3±10.7 (18-61) years. The mean follow-up period was 75.6±40.5 (10-127) months. The duration between the initial symptom and time of surgical intervention ranged between 4 months and 25 years with average of 6.3 years. The most common complaint was low back pain, which followed by legs pain and urinary±bowel (Table IV). The most common finding in the neurological examinations were urinary (seen in 12 patients) and motor weakness (seen in 12 patients), which were followed by hypoesthesia (seen in 8 patients) (Table V). Urodynamic test was performed in 19 patients which revealed on overactive detrusor muscle in 3 patients, post-void residual urine (> 100 ml) showed in 8 patients and normocompliance normotonic bladder function in 8 patients. The most associated malformations were diastematomyelia (seen in 10 patients) and vertebral fusion anomalies (seen in 10 patients), which were followed by split cord malformations (seen in 8 patients) (Table VI). The most common level of conus medullaris was L5 level which was detected 34.8% of the patients. Detethering carried out in 87% of patients and bony septum resection without detethering applied in 13%. Surgical approaches were laminoplasty (39.1%), laminectomy (43.5%) and hemilaminectomy (17.4%). Surgical outcomes were divided in three groups; recovered good group which seen in 60.9% of our patients, improved group which was seen 34.8% of our series and worsened neurological deficits which was seen in one patient (Table III). The surgical morbidity rate is 4.3%. The most common complications were CSF leakage (13%) and surgical site infections (13%). Pseudomeningocele was developed in one female patient 4 years after detethering surgery. All of these patients were successfully treated either conservatively or surgically. Turk Neurosurg,
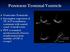
4 A B c Figure 1: A 61-yearmale patient presented with numbness, low back and leg pain; A) Sagittal MRI demonstrated cyst extends between L1 and S2. Note that L3 and L4 vertebral fusion anomaly (block vertebra) is apparent; B) Axial MRI showed that diastematomyelia expends between both of L2 and L4. Note that split cord malformation as bony septum at L3 level, and dermal sinus tract are apparent; C) Sagittal MRI demonstrated that spinal cord terminates at S1-2 level. Figure 2: A 21-yearold female was presented with low back and both legs pains for more than 5 years. Her neurological examination was intact; expect rarely loss control of her urination. MRI demonstrated that spinal cord terminates at L5 level. DISCUSSION The female preponderance in adult patients with TCS is well-established observation in all series reported before (6,7,11,14). However, some authors reported a whole series of males such as article of Akay et al. who reported nine young males of SCMs (1). In our series, the female predominance of 5:8 (65.2%) was observed in our patients. Klekamp reported in his series that the female predominance was observed in 71.8% of his patients whom underwent detethering procedure (7). The structure of filum terminale is especially important in the development of TCS. The recent studies (10, 18) such as; Tehli et al. (18) report, in their comparative study of histopathological analysis of filum terminale between TCS patients and normal human fetuses, that adipose tissue, fibrosis, hyalinization, and meningothelial proliferation were observed in filum terminale samples of TCS patients, while none of these findings were observed in normal fetal samples. Elastic fibers were present in all TCS specimens and the adult cadaver, but were not observed in fetuses (10, 18). Peripheral nerves, ganglion cells 4 Turk Neurosurg, 2016
5 Table II: Baseline Clinical Characteristics, Co-malformations, Treatment, Outcomes and Complications of Treatment No Age/ Sex Clinical Presentation Neurogenic Examination Operation Admission Period (days), PO Course and Complications MRI Findings and Comalformations Followup (months) 1 35/M Pain, weakness, and urinary-fecal Loss of anal tone and sensation, 4/5 strength on the left leg distal muscle group Vertebral fusion anomalies; DTM; SCM (FB); SM; LMM; left pes planus; and TC 12 days, his pain was relieved while weakness and compliants did not improved; None /F Pain and weakness Weakness, hypoesthesia, increased DTR, Babinski P/E, Hoffman (+) and clonus (+) Htr; DTM; SCM (BS); Lipoma and TC BS resection then 5 days, her pain was relieved while weakness had some improvement; None /F Numbness, unsteady gait and urinary-fecal Weakness, increased right DTR, hypoesthesia Equinavarus; SM; scoliosis, sacral spina bifida occulta; LM; TC 3 days, her motor deficit worsened than preoperative level /F Low back and right leg pain 4/5 strength on the right leg Htr; equinavarus; DTM; vertebral fusion anomalies; SCM (FB); SM; lipoma; TC FB resection then 7 days, she recovered good; None /F Frequent infection and pain Normal Htr; DST; TC DST resection then Deth; laminoplasty 2 days, she recovered good; SSI on POD 23 (treated using antibiotics) /F Pain, right leg atrophy, urinary, loss of walking capasity (bed-bounded) 2/5 strength on the right leg, increased DTR, right leg atrophy, hypoesthesia Lipoma; DST; SCM (BS); DTM; TC BS and DST resection then Deth; laminectomy 12 days, her pain was relieved while weakness and sphincter function had some improvement; POD 14 CSF leakage was developed (treated surgically); 4 years later pseudomeningocele developed which had been treated surgically /F Low back pain Normal DTM; SCM (BS); scoliosis; butterfly vertebrae; TC 1 st session: BS resection; 2 nd session 4 and one days, she recovered good; None /M Low back pain and fecal-urinary Increased bilateral DTR DST; lipoma; hyperpigmentation area in lumbal skin; TC 1 st session: DST resection; 2 nd session 8 days, his pain was relieved, weakness had some improvement while sphincter dysfunction did not improve; POD 15 CSF leakage was developed (treated surgically) /F Pain and numbness Atrophy, hypoesthesia Htr; L4 spina bifida occulta; TC Deth; hemilaminectomy 7 days, she recovered good; None /M Weakness, numbness, and difficulty in urination Weakness, atrophy, hypoesthesia Lipoma; TC 4 days, he recovered good; None 96 Turk Neurosurg,
6 Table II: Cont /F Pain and urinary Increased bilateral DTR, 4/5 strength on left leg LM; sacral spina bifida occulta; TC Deth; hemilaminectomy 3 days, her pain was relieved, weakness recovered while sphincter dysfunction did not improve; None /F Low back pain Hypoesthesia, Babinski: bilateral indifferent Equinavarus; DTM; SCM (BS); DST; TC BS resection; laminectomy 4 days, she recovered good; None /M Pain and urinary Weakness of the right leg distal muscle group of 4/5 grade Right kidney hypoplasia; Lipoma; TC Deth and lipoma removal; laminoplasty 8 days, he recovered good; None /M Unsteady gait, urinary, headache and vertigo Increased bilateral DTR, Babinski: E/E, Rhomberg test (+) Hydrocephalus; Chiari-malformation; LM; SM; TC 4 days, sphincter dysfunction did not improve; SSI on POD 20 (treated using antibiotics) /F Back pain Babinski: bilateral indifferent SM; scoliosis; TC Deth; hemilaminectomy 2 days, she recovered good; POD 9 CSF leakage was developed (treated surgically) /M Numbness, urinary, pain Weakness, hypoesthsia, neurogenic claudication and Babinski: bilateral indifferent DTM; vertebral fusion anomalies; SCM (BS); DST; cyst; TC BS resection, then cystectomy ; laminoplasty 3 days, he recovered good; None /F Unsteady gait, muscular weakness and fecalurinary Weakness, increased bilateral DTR, bilateral clonus (+), Babinski: E/E TC Deth; laminoplasty 7 days, she improved; None /F Low back and both legs pain Normal Equinavarus; vertebral fusion anomalies; horseshoe kidney; scoliosis; DTM; BS; SM; TC BS resection; laminoplasty 2 days, she recovered good; None /F Numbness, low back and both legs pain Weakness, hypoesthesia, Babinski P/indifferent DST and lipoma; TC DST resection, lipoma removal and Deth; laminoplasty 3 days, she recovered good; None /M Both legs pain Normal DTM; TC Deth; laminoplasty 4 days, he recovered good; SSI on POD 19 (treated using antibiotics) /F Low back and both legs pain Normal DTM; vertebral fusion anomalies; TC Deth; laminoplasty 4 days, she recovered good; None /M Both legs pain and urinary Weakness Right kidney hypoplasia; Lipoma; re-tc De-reteth and lipoma removal; laminoplasty 4 days, his complaints were improved; None /F Pain and urinary Urinary (Rarely) TC Deth; laminoplasty 2 days, she recovered good; None 10 M: Male, F: Female, DTM: Diastematomyelia, SCM: Split cord malformation, FB: Fibrous bands, BS: Bony septum, SM: Syringomyelia, LMM: Lipomyelomeningocele, LM: Lipomeningocele, TC: Tethered cord, DST: Dermal sinus tract, Htr: Cutaneous stigmata (hypertrichosis), Deth: Detethering, DTR: Deep tendon reflexes, P: Plantar (flexor), E: Extensor, SSI: Surgical site infection, POD: Postoperative day. 6 Turk Neurosurg, 2016
7 and ependymal cells were observed in normal human fetal filum terminale samples (18). Because these changes are not observed in fetuses, they suggest that this syndrome did not begin in intrauterine life (18). Most adult patients experience tethered cord (TC) during normal daily activity or mild static neurological deficits in childhood. As a result of the development in imaging technologies, the number of adults in whom congenital TCS is diagnosed increases. However, adults compared with pediatric population may be denial of any significant symptoms and unwilling to visit their doctors, therefore, usually diagnosis of TCS in adults done after progressive scoliosis, foot deformities, leg length discrepancy, or muscular atrophy which may increase their chances of disability. In some cases, serious traumas such as traffic accident or failing as well as dynamic and static changes occur on spinal column (such as those happen in pregnancy) that may aggravate the degenerative processes and induce back and leg pains. In our series, the most common complaint was pain that was seen in 20 patients (87% of our patients); 15 patients were experienced low back pain (65.2%) and 13 patients were experienced legs pain (56.5%). The pain was followed by bladder dysfunction and muscular weakness which were seen in 12 patients (52.2%) of each (Tables II, IV). In TCS, stretching of the conus medullaris and nerve roots may induce back pain, leg weakness, foot deformity, scoliosis, sensory loss, and/or bowel or bladder dysfunction (5,9,11,13). Untreated TCS can progress in 27.5%, 40%, and 60% of cases at 1, 2, and 5 years after diagnosis, respectively (13). In our institute, in the last 10 years 93 adult patients were diagnosed with TC after permanent or severe pain in their Table III: Clinical Outcomes according to the Neurological Scoring System No** Leg±Back Pain Intensity Preop/ Postop Sensory Disturbance, Dysesthesias Preop/ Postop Motor Weakness Preop/Postop Gait Ataxia Preop/Postop Sphincter Function Preop/Postop Surgical Outcome 1 2/4 5/5 4/4 4/4 3/4 Improved 2 3/4 4/4 3/4 4/4 5/5 Improved 3 5/5 2/3 4/2 2/3 0/1 Worsened 4 3/5 5/5 4/5 5/5 5/5 Good recovery 5 4/5 5/5 5/5 5/5 5/5 Good recovery 6 2/4 1/3 2/2 1/1 2/4 Improved 7 2/5 5/5 5/5 4/5 5/5 Good recovery 8 3/5 5/5 5/5 2/4 0/1 Improved 9 3/5 4/5 5/5 5/5 5/5 Good recovery 10 5/5 4/5 4/5 5/5 3/4 Good recovery 11 4/5 5/5 4/5 5/5 1/2 Improved 12 1/4 4/5 5/5 5/5 5/5 Good recovery 13 2/5 5/5 4/5 4/5 2/4 Good recovery 14 4/5 5/5 5/5 3/5 1/3 Improved 15 2/5 5/5 5/5 5/5 5/5 Good recovery 16 2/5 4/5 4/5 5/5 3/5 Good recovery 17 3/4 5/5 3/5 2/4 3/4 Improved 18 1/5 5/5 5/5 5/5 5/5 Good recovery 19 2/5 4/4 4/5 5/5 5/5 Good recovery 20 1/4 5/5 5/5 5/5 5/5 Good recovery 21 1/4 5/5 5/5 5/5 5/5 Good recovery 22 2/4 5/5 4/5 5/5 2/3 Improved 23 2/5 5/5 5/5 5/5 2/5 Good recovery ** Case No in this table refere to the same case No in Table II. Turk Neurosurg,
8 back and/or legs (incidentally) or in those experienced serious urological complaints. Only 23 adult patients (24.7%) that diagnosed as symptomatic TC were treated surgically, after all investigations and full evaluation to clinical status of the patients. Table IV: The Presenting Symptoms of 23 Adult TCS Patients Presenting Symptoms No of the patients Percentage Low back pain % Leg pain % Bladder dysfunction ( or retention) % Muscular weakness % Numbness % Unsteady Gait % Bowel dysfunction (fecal ) % Muscular atrophy 3 13% Lumbar swelling 2 8.7% Frequent lumbar skin infection 1 4.3% Headache 1 4.3% Vertigo 1 4.3% Table V: The Clinical Findings in Neurological Examination of 23 Adult TCS Patients Clinical Findings Bladder dysfunction ( or retention) Muscular weakness (motor deficit) No of the patients Percentage % % Hypoesthesia % Increased deep tendon reflex % Loss of anal tone and sensation (fecal ) % Extensor or indifferent Babinski 4/2 17.4%/8.7% Muscular atrophy 3 13% Lumbar local tenderness 3 13% Positive clonus 2 8.7% Positive hoffman 1 4.3% Normal clinical findings % The patients with tolerable pain which was seen in all of the adult patients with TCS in our series were treated conservatively, with close follow-up (by 3 months periods of follow-up) to avoid permanent new neurological deficits. The patients have to undergo full neurological examination especially those who experienced low back and legs pain associated with urination complaints, the most common clinical findings in our series are bladder dysfunction and muscular weakness which are seen in 12 patients of each (52.2%). The pathological Table VI: Co-Malformations that were Detected in 23 Tcs Adult Patients Malformation No of the patients Percentage Conus medullaris (Tethered cord) % At L2 level 1 4.3% At L3 level 3 13% At L4 level 3 13% At L5 level % At S1 level % At S2 level 2 8.7% Diastematomyelia % Vertebral fusion anomalies % Split cord malformation % As Bony septum % As Fibrous bands 3 13% Lipoma % Scoliosis % Syringohydromyelia % Dermal sinus tract % Foot anomalies (equinavarus, pes planus) % Hypertrichosis % Lipomeningocele 3 13% Kidney malformations (hypoplastic, horseshoe) 3 13% Lipomyelomeningocele 1 4.3% Mitral valve prolapse 1 4.3% Chiari malformation 1 4.3% Hydrocephalus 1 4.3% Skin hyperpigmentation 1 4.3% Only tethered cord without co-malformation 2 8.7% 8 Turk Neurosurg, 2016
9 (abnormal) responses of all of deep tendon reflexes, Babinski reflex, clonus, and Hoffman sign which are noticed in 11 patients of our series (47.8%) are important indicators to check-up the patient craniospinal MRI (Tables II, V). Because of the expected new neurological deficits in their age group are high, the surgical intervention rate was 100% (50 child was diagnosed with TCS) of all children and adolescents with TCS referred to us. Klekamp reported that 43 out of his 85 (50.8%) adult patients with TC underwent detethering procedure (7). Review of the literature suggests that the reversible symptoms associated with TCS are related to metabolic derangements and alterations in oxidative metabolism (20). All neuronal damages occur in TCS patients may not repair after surgical intervention, persisting of symptoms can vary depending on severity and duration between presentation and the initial treatment. If treated early, patients can recover from their neurological deficits. Chronic or excessive stretching of the spinal cord can lead to permanent disability. Although the duration between the initial symptom and time of surgery in our series ranged between 4 months and 25 years with average of 6.3 years, the early surgical intervention after increasing intensity of pain, or severity of complaints gave good results as recovered good was seen in 60.9% and improved group was seen 34.8%. only one patient had worsened neurological deficits (Table III). Our good surgical outcomes were related to the full evaluation performed in all patients separately. The patients who were diagnosed with TC incidentally after moderate pain were closely followed-up and when their complaints started to be symptomatic and urological complaints were added to their clinical pictures urodynamic studies were reperformed and then a decision was made for surgical intervention. Iskandar et al. (6) reported that untethering can improve in 22 of 27 patients (81.5%) presenting with pain, 13 of 27 (48.1%) patients with motor or sensory dysfunction, and 11 of 18 patients (61.1%) with bowel and bladder disturbance. TC release and/or BS resection in our patients can improve and recover pain in 15.8% (3 out of 19 patients) and 84.6% (16 out of 19 patients), respectively. Muscular weakness recovered in 8 out of 12 our patients (66.7%), unchanged in two, worsened and improved in one patient each. However, sensory disturbance remained unchanged in 50% (4 out of 8 patients) in our series. Bladder and bowel dysfunction improved, recovered and unchanged in 50% (6 out of 12 patients), 25% and 25%, respectively. These surgical outcomes are better than those reported by Lee et al. (12) who found that surgical intervention can improve back and leg pain in 78% and 83% of patients, respectively. Motor weakness will stabilize or improve in only 27% and 64% of patients, respectively. Sensory deficits remained unchanged in 50% of patients. Urological abnormalities improved in 50% of patients undergoing detethering and remained stable in 45%. Solmaz et al. (16) reported in their results of the untethering procedure carried out in the pediatric population that neurological improvement was observed in 4 (44.4%) of 9 children, while unchanged in the others. Urological disturbances improved in 2 (20%) of 10 children (16). Back pain was improved in all patients (16). These results show that our results were better. However, the complication rate in the same study (16) was less than our complication rate. CSF leakage was seen in 3 (6.1%) of 49 their children versus 3 (13%) of adult patients in our study. Solmaz et al. (16) reported no neurological deterioration or surgical site infection was recorded. Unfortunately, in our results surgical site infections were seen in 3 (13%) patients. Pseudomeningocele was developed in one female patient 4 years after detethering surgery. Retethering was obsereved in one patient (4.3%) of us, while Solmaz et al. (16) reported high retethering rate as 24.5% among children involved with TC. The neurosurgical team here ought to use the same surgical procedure was described by Solmaz et al. (16) with some differences. In this article, laminoplasty and neurophysiological monitoring were the purpose of the surgery especially in last four years. Although a lot of approaches described for detethering procedure in adults such as; mini-open (minimal invasive), traditional open laminectomy or laminoplasty, A wide lumbosacral laminectomy is still the standard approach used to explore split cord malformation and to detether the filum terminale. In a comparison between laminoplasty (laminas were removed bilaterally using high-speed drill then after detethering or whatever the planned surgery was performed, laminas were sutured using a strong non-absorbable suture bilaterally to both lamina parts and interspinous ligaments cranially and caudally), hemilaminectomy and laminectomy in our series, the author found that laminoplasty is less than hemilaminectomy and laminectomy approaches in the length of stay at hospital with averages of 3.9±2.2 (2-8) days, against 4±2.2 (2-7) days, and 6.4 ±3.3 (3-12) days, respectively. This difference was not significantly different (P=0.57) and (P=0.29), respectively (significance level was considered when P <0.05). On the other hand, three approaches did not affect the neurological outcomes and surgery-related complications. Only 2 patients in our series were free of other malformations that associated with TC (Tables II, VI), therefore, the malformations in patients with classic symptoms of TCS have to aware the physicians to refer such patients to neurosurgeons. Split cord malformations are mainly associated with TCS in adults (1). Seven of 8 patients who had split cord malformation had been treated by bony septum (BS) or fibrous band (FB) resection, and only 4 of these seven needed to detethering procedure after this to relieve their pain or other complaints. In the rest three patients detethering procedure did not apply to avoid new neurological deficits. 2 out of 8 patients who had lipoma had been treated by removal of lipoma, and one else treated with cystectomy. 4 out of 5 patients presented with dermal sinus tract had been treated by resection it and repair the skin surgically. Compared with our pediatric TCS patients, our adult patients with TCS who presented with scoliosis and syringohydromyelia did not need to additional surgical intervention, whereas 38% of our child TCS patients who presented with the same malformations were underwent additional surgery to treat their complaints. Surgery-related complications included three cerebrospinal fluid (CSF) leakages, three surgical site infections (SSI), and Turk Neurosurg,
10 one pseudomeningocele. Pseudomeningocele was developed in one female patient 4 years after detethering surgery. All of these patients successfully treated either conservatively or surgically. One patient complained of worsening muscular weakness. Our complications remain less than those of Iskandar et al. (6) who reported that one CSF leakage, five pseudomeningocele, two patients complained of worsening bladder dysfunction, whereas four patients experienced persistent pain and one complained of worsening pain postoperatively. In the adult population, the rate of retethering has been quoted to be as high as 29% (2,3,6,7,15,16). Usually recurrent TCS can lead to the same significant complaints that seen in patients before primary surgery. In our series, the retethering rate is 4.3% which developed in a male patient 6 years later. The patient underwent detethering procedure and complete resection of his lipoma surgically and improved. In this case, the authors noticed that laminoplasty was a good barrier to protect thecal sac and nerve roots from fibrosis and granulation tissues. Standard Management of TC in Adults Almost authors generally, recommend surgery as soon as neurological symptoms were present (3,5-7,11,12). Whereas, there are bit authors recommended surgery for those with progressive neurological symptoms (7). The authors in this paper aimed to describe standard management protocol that they use to treat TC in adults. Despite the initial approach of surgical intervention is aimed at dealing with the pathological conditions that cause the symptoms in symptomatic patients with TCS, the surgical management of asymptomatic TC remains controversial. Therefore, the patients present with suspicious symptoms (back pain, legs pain and/or urinaryfecal ) (Table V) associated with any malformations or structural lesions (such as; lipomyelomeningocele, lipomeningocele, dermal sinus tract, cutaneous stigmata (hypertrichosis), scoliosis or another system malformations (e.g. congenital heart diseases, congenital kidney diseases or genetic syndromes) (Tables II, VI) have to undergo detailed neurological and physical examination, followed by craniospinal MRIs have to be performed. If there are any findings that support TC, the patients have to undergo a urodynamic test. If all investigations lead us to diagnose the patient as symptomatic TCS, the neurosurgeons have to explain the risks, complications and benefits of the surgical intervention for TCS to patients and their families which will help them to make decision about the operative option. If both physicians and patient s family plan to surgery, the neurophysiological monitoring and laminoplasty rather than laminectomy have to be applied. Intraoperative surgical strategies depend on the additional pathological entities that associated with TC. Klekamp recommended that a complete resection, including the capsules in hamartomas (i.e. lipomas, dermoid cysts, epidermoid cysts and neurenteric cysts), and using artificial materials for duraplasty (7). In our series, there were 8 adult TCS patients associated with lipomas, only 3 out of these 8 patients were lipomas resection performed, one patient had recurrence after 6 years even complete resection of lipoma with its capsule had been done. To avoid the serious complications and retethering lipoma was left without resection after the intraoperative evaluation showed that lipoma did not press on nerve roots or dural sac. However, asymptomatic patients have an increased risk of developing new neurological deteriorations. Close patient follow-up and timely treatment for local pathologies after detecting change in urodynamic or manual motor testing may protect patients from new deficits. The adult TCS patients are less likely to show any neurological deterioration because there has already been rapid spinal column growth in the setting of medulla spinalis that is tethered caudally. Three patients out of our patients did not undergo TC release, just BS resection, one of these three patients underwent cystectomy too (illustrative case 1). The guide here is the consistent all of clinical presentation, neurological examination with urodynamic study. In these three cases, the presenting symptom was pain, while the urodynamic tests showed normocompliant normotonic bladder function with less than 50 ml post-void residual urine (normal). Therefore, BS resection was adequate to resolve their complaints, rather than detethering procedure that could result in new neurosurgical deficits. Thus, our management does not agree with what most authors in the literature who suggested that the TC release procedure was acceptable as a necessary intervention in adult TC patients (6,7,11,12,17). CONCLUSION Neurological deficits developed in TC adult patients are generally irreversible. Therefore, early surgery is recommended in symptomatic patients. Despite the good results obtained from our surgical interventions for symptomatic TCS in adults, the neurosurgeons have not forgotten that tethered cord releasing is complicate procedure and has serious complications. Full neurological and physical examination, craniospinal MRIs, urodynamic test are essential before planning the surgical treatment for TCS. Urodynamic test gives predicts about almost future deteriorations in adult patients with TCS, therefore it is essential before planning surgery. REFERENCES 1. Akay KM, Izci Y, Baysefer A, Timurkaynak E: Split cord malformation in adults. Neurosurg Rev 27: , Bowman RM, McLone DG, Grant JA, Tomita T, Ito JA: Spina bifida outcome: A 25-year prospective. Pediatr Neurosurg 34: , Bowman RW, Mohan A, Ito J, Seibly JM, Mcbone DG: Tethered cord release: A long-term study in 114 patients. J Neurosurg Pediatr 3: , Cochrane DD: Cord untethering for lipomyelomeningocele: Expectation after surgery. Neurosurg Focus 23(2): E9, Fehlings MG, Arvin B: Editorial. Recurrent tethered cord syndrome: A novel approach for a difficult surgical condition? J Neurosurg Spine 10: , Turk Neurosurg, 2016
11 6. Iskandar BJ, Fulmer BB, Hadley MN, Oakes WJ: Congenital tethered spinal cord syndrome in adults. Neurosurg Focus 10 (1): E7, Klekamp J: Tethered cord syndrome in dults. J Neurosurg Spine 15: , Klekamp J, Samii M: Introduction of a score system for the clinical evaluation of patients with spinal processes. Acta Neurochir (Wien) 123: , Kokubun S, Ozawa H, Aizawa T, Ly NM, Tanaka Y: Spineshortening osteotomy for patients with tethered cord syndrome caused by lipomyelomeningocele. J Neurosurg Spine 15: 21-27, Kural C, Guresci S, Simsek GG, Arslan E, Tehli O, Solmaz I, Izci Y: Histological structure of filum terminale in human fetuses: Laboratory investigation. J Neurosurg Pediatr 13(4): , Lapsiwala SB, Iskandar BJ: The tethered cord syndrome in adults with spina bifida occulta. Neurol Res 26: , Lee GY, Paradiso G, Tator CH, Gentili F, Massicotte EM, Fehlings MG: Surgical management of tethered cord syndrome in adults: Indications, techniques, and long-term outcomes in 60 patients. J Neurosurg Spine 4(2): , Phuong LK, Schoeberl KA, Raffel C: Natural history of tethered cord in patients with meningomyelocele. Neurosurgery 50: , Rajpal S, Tubbs RS, George T, Oakes WJ, Fuchs HE, Hardley MN, Iskandar BJ: Tethered cord due to spina bifida occulta presenting in adulthood: A tricenter review of 61 patients. J Neurosurg Spine 6: , Skin P, Halpin RJ, Ganju A, Liu JC: Management of recurrent adult tethered cord syndrome. Neurosurg Focus 29(1):E5, Solmaz I, Izci Y, Albayrak B, Cetinalp E, Kural C, Sengul G, Gocmez C, Pusat S, Tuzun Y: Tethered cord syndrome in childhood special emphasis in the surgical technique and review of the literature with our experience. Turk Neurosurg 21(4): , Stetler WR, Park P, Sullivan S: Pathophysiology of adult tethered cord syndrome: Review of the literature. Neurosurg Focus 29(1):E2, Tehli O, Hodaj I, Kural C, Solmaz I, Onguru O, Izci Y: A comparative study of histopathological analysis of filum terminale in patients with tethered cord syndrome and in normal human fetuses. Pediatr Neurosurg 47: , Van Leeuwen R, Notermans NC, Vandertop WP: Surgery in adults with tethered cord syndrome: Outcome study with independent clinical review. J Neurosurg 94 Suppl 2: , Yamada S, Knerium DS, Mandybur GM, Schultz RL, Yamada BS: Pathophysiology of tethered cord syndrome and other complex factors. Neurol Res 26: , 2004 Turk Neurosurg,
SPLIT NOTOCHORD SYNDROME ASSOCIATION. DR. Hasan Nugud Consultant Paediatric Surgeon
 SPLIT NOTOCHORD SYNDROME ASSOCIATION DR. Hasan Nugud Consultant Paediatric Surgeon CASE PRESENTATION :- New born baby, boy, referred to the paediatric surgical team at the age of 14 hours. Birth History
SPLIT NOTOCHORD SYNDROME ASSOCIATION DR. Hasan Nugud Consultant Paediatric Surgeon CASE PRESENTATION :- New born baby, boy, referred to the paediatric surgical team at the age of 14 hours. Birth History
Long segment composite split cord malformation with double bony spur
 Long segment composite split cord malformation with double bony spur Anand Sharma, Achal Sharma, R.S. Mittal SMS Medical College, Jaipur, India Abstract: A composite type of SCM is very rare and only a
Long segment composite split cord malformation with double bony spur Anand Sharma, Achal Sharma, R.S. Mittal SMS Medical College, Jaipur, India Abstract: A composite type of SCM is very rare and only a
Elderly-onset degenerative lumbar spondylotic myelopathy in a patient with a low-placed spinal cord successfully treated by laminotomy: a case report
 CASE REPORT Elderly-onset degenerative lumbar spondylotic myelopathy in a patient with a low-placed spinal cord successfully treated by laminotomy: a case report Ko Hashimoto 1,2, Takumi Tsubakino 1, Takeshi
CASE REPORT Elderly-onset degenerative lumbar spondylotic myelopathy in a patient with a low-placed spinal cord successfully treated by laminotomy: a case report Ko Hashimoto 1,2, Takumi Tsubakino 1, Takeshi
University Journal of Surgery and Surgical Specialties
 University Journal of Surgery and Surgical Specialties ISSN 2455-2860 Volume 2 Issue 1 2016 Profile of paediatric patients with split cord malformation MANORANJITHAKUMARI M Department of Neuro Surgery,
University Journal of Surgery and Surgical Specialties ISSN 2455-2860 Volume 2 Issue 1 2016 Profile of paediatric patients with split cord malformation MANORANJITHAKUMARI M Department of Neuro Surgery,
)93( COPYRIGHT 2014 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE
 )93( COPYRIGHT 2014 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Orthopedic Lesions in Tethered Cord Syndrome: The Importance of Early Diagnosis and Treatment on Patient Outcome Mohammad
)93( COPYRIGHT 2014 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Orthopedic Lesions in Tethered Cord Syndrome: The Importance of Early Diagnosis and Treatment on Patient Outcome Mohammad
University Journal of Surgery and Surgical Specialties
 University Journal of Surgery and Surgical Specialties ISSN 2455-2860 Volume 2 Issue 1 2016 TWO RARE CASES OF DIASTEMATOMYELIA MUTHURAMAN P Department of Neuro Surgery, THANJAVUR MEDICAL COLLEGE Abstract
University Journal of Surgery and Surgical Specialties ISSN 2455-2860 Volume 2 Issue 1 2016 TWO RARE CASES OF DIASTEMATOMYELIA MUTHURAMAN P Department of Neuro Surgery, THANJAVUR MEDICAL COLLEGE Abstract
Pediatric Spinal Anomalies
 Department of Radiology University of California San Diego Pediatric Spinal Anomalies John R. Hesselink, M.D. Spine Embryogenesis 1. Primitive streak 2. Proliferation of cells at primitive pit (Hensen's
Department of Radiology University of California San Diego Pediatric Spinal Anomalies John R. Hesselink, M.D. Spine Embryogenesis 1. Primitive streak 2. Proliferation of cells at primitive pit (Hensen's
Purpose: To discuss the fatty filum terminale which is incidentally demonstrated on MRI concerning the causes of TCS
 ISPUB.COM The Internet Journal of Spine Surgery Volume 3 Number 1 T Iizuka Citation T Iizuka.. The Internet Journal of Spine Surgery. 2006 Volume 3 Number 1. Abstract Background: Fatty filum terminale
ISPUB.COM The Internet Journal of Spine Surgery Volume 3 Number 1 T Iizuka Citation T Iizuka.. The Internet Journal of Spine Surgery. 2006 Volume 3 Number 1. Abstract Background: Fatty filum terminale
Congenital Tethered Spinal Cord Syndrome in Adults
 Page 1 of 7 http://www.medscape.com/ To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/405679 Congenital Tethered
Page 1 of 7 http://www.medscape.com/ To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/405679 Congenital Tethered
Tethered spinal cord syndrome: a developmental overview
 International Journal of Sciences & Applied Research www.ijsar.in Tethered spinal cord syndrome: a developmental overview Anushi Singh 1 *, Rekha Kumari 2 1 CHN Department, School of Nursing Science and
International Journal of Sciences & Applied Research www.ijsar.in Tethered spinal cord syndrome: a developmental overview Anushi Singh 1 *, Rekha Kumari 2 1 CHN Department, School of Nursing Science and
Tethered cord syndrome is a disorder involving an. Spine-shortening osteotomy for patients with tethered cord syndrome caused by lipomyelomeningocele
 See the corresponding editorial in this issue, pp 19 20. J Neurosurg Spine 15:21 27, 2011 Spine-shortening osteotomy for patients with tethered cord syndrome caused by lipomyelomeningocele Clinical article
See the corresponding editorial in this issue, pp 19 20. J Neurosurg Spine 15:21 27, 2011 Spine-shortening osteotomy for patients with tethered cord syndrome caused by lipomyelomeningocele Clinical article
What Every Spine Surgeon Should Know About Neurosurgical Issues
 What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
Congenital tethered spinal cord syndrome in adults
 Neurosurg Focus 10 (1):Article 7, 2001, Click here to return to Table of Contents Congenital tethered spinal cord syndrome in adults BERMANS J. ISKANDAR, M.D., BENJAMIN B. FULMER, M.D., MARK N. HADLEY,
Neurosurg Focus 10 (1):Article 7, 2001, Click here to return to Table of Contents Congenital tethered spinal cord syndrome in adults BERMANS J. ISKANDAR, M.D., BENJAMIN B. FULMER, M.D., MARK N. HADLEY,
A Retrospective Analysis of Clinical Profile and Surgical Outcome in Patients with Spinal Dysraphism at Tertiary Care Center
 Original Research Article A Retrospective Analysis of Clinical Profile and Surgical Outcome in Patients with Spinal Dysraphism at Tertiary Care Center Premlal KV * Assistant Professor, Department of Neurosurgery,
Original Research Article A Retrospective Analysis of Clinical Profile and Surgical Outcome in Patients with Spinal Dysraphism at Tertiary Care Center Premlal KV * Assistant Professor, Department of Neurosurgery,
Wound healing in trophic ulcers in spina bifida patients
 J Neurosurg 82:000 000, 1995 Wound healing in trophic ulcers in spina bifida patients VINOD KUMAR SRIVASTAVA, M.B.B.S, M.CH. Neurosurgical Unit, J. N. Medical College, Aligarh Muslim University, Aligarh,
J Neurosurg 82:000 000, 1995 Wound healing in trophic ulcers in spina bifida patients VINOD KUMAR SRIVASTAVA, M.B.B.S, M.CH. Neurosurgical Unit, J. N. Medical College, Aligarh Muslim University, Aligarh,
disclosure Pediatric Tethered cord Syndrome Learning Objectives overview definiton Hoffman 1976 Pediatrics Grand Rounds 26 June 2015
 disclosure Pediatric Tethered cord Syndrome None Izabela, Tarasiewicz, MD,FRCS(C), has no relationships with commercial companies to disclose. Izabela Tarasiewicz MD. FRCS(C) Pediatric Neurosurgery overview
disclosure Pediatric Tethered cord Syndrome None Izabela, Tarasiewicz, MD,FRCS(C), has no relationships with commercial companies to disclose. Izabela Tarasiewicz MD. FRCS(C) Pediatric Neurosurgery overview
Case Report An Unusual Presentation of Adult Tethered Cord Syndrome Associated with Severe Chest and Upper Back Pain
 Case Reports in Orthopedics Volume 2015, Article ID 926185, 5 pages http://dx.doi.org/10.1155/2015/926185 Case Report An Unusual Presentation of Adult Tethered Cord Syndrome Associated with Severe Chest
Case Reports in Orthopedics Volume 2015, Article ID 926185, 5 pages http://dx.doi.org/10.1155/2015/926185 Case Report An Unusual Presentation of Adult Tethered Cord Syndrome Associated with Severe Chest
Surgical Outcome of Tethered Cord Syndrome Nazar Hussain, Wakeel Ahmad Haral, Muhammad Akmal Hussain, Inam Ullah Asghar, Tariq Ahmad
 Original Article Surgical Outcome of Tethered Cord Syndrome Nazar Hussain, Wakeel Ahmad Haral, Muhammad Akmal Hussain, Inam Ullah Asghar, Tariq Ahmad ABSTRACT Objective: Surgical Outcome of tethered cord
Original Article Surgical Outcome of Tethered Cord Syndrome Nazar Hussain, Wakeel Ahmad Haral, Muhammad Akmal Hussain, Inam Ullah Asghar, Tariq Ahmad ABSTRACT Objective: Surgical Outcome of tethered cord
ORIGINAL PAPER. Mehmet Selçuki & Ahmet Şükrü Umur & Yusuf Kurtulus Duransoy & Seymen Ozdemir & Deniz Selcuki
 DOI 10.1007/s00381-012-1713-0 ORIGINAL PAPER Inappropriate surgical interventions for midline fusion defects cause secondary tethered cord symptoms: implications for natural history report of four cases
DOI 10.1007/s00381-012-1713-0 ORIGINAL PAPER Inappropriate surgical interventions for midline fusion defects cause secondary tethered cord symptoms: implications for natural history report of four cases
Comparison of Electrophysiological Outcomes of Tethered Cord Syndrome and Spinal Intradural Tumors: A Retrospective Clinical Study
 DOI: 10.5137/1019-5149.JTN.17043-16.0 Received: 14.1.2016 / Accepted: 05.02.2016 Published Online: 24.02.2016 Original Investigation Comparison of Electrophysiological Outcomes of Tethered Cord Syndrome
DOI: 10.5137/1019-5149.JTN.17043-16.0 Received: 14.1.2016 / Accepted: 05.02.2016 Published Online: 24.02.2016 Original Investigation Comparison of Electrophysiological Outcomes of Tethered Cord Syndrome
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Spinal canal stenosis Degenerative diseases F 06
 What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
Asymptomatic posterior cervical myelomeningocele with tethered cord in an adolescent: a rare form of spinal dysraphism with rare presentation
 Romanian Neurosurgery (2016) XXX 1: 113-117 113 Asymptomatic posterior cervical myelomeningocele with tethered cord in an adolescent: a rare form of spinal dysraphism with rare presentation Gangesh Gunjan,
Romanian Neurosurgery (2016) XXX 1: 113-117 113 Asymptomatic posterior cervical myelomeningocele with tethered cord in an adolescent: a rare form of spinal dysraphism with rare presentation Gangesh Gunjan,
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
University of Groningen
 University of Groningen Long-term evaluation of intraoperative neurophysiological monitoring-assisted tethered cord surgery Dulfer, S E; Drost, Gerrie; Lange, F; Journee, H L; Wapstra, F H; Hoving, E W
University of Groningen Long-term evaluation of intraoperative neurophysiological monitoring-assisted tethered cord surgery Dulfer, S E; Drost, Gerrie; Lange, F; Journee, H L; Wapstra, F H; Hoving, E W
Disclosure. Thoracolumbar Tumors. Intraspinal Tumor Removal Options 6/4/2011. Minimally Invasive Approaches for Spinal Tumors
 Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
Role of helical CT and MRI in the evaluation of spinal dysraphism
 International Journal of Advances in Medicine Kumaran SK et al. Int J Adv Med. 2017 Feb;4(1):124-132 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20170095
International Journal of Advances in Medicine Kumaran SK et al. Int J Adv Med. 2017 Feb;4(1):124-132 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20170095
Neuropathic bladder and spinal dysraphism
 Archives of Disease in Childhood, 1981, 56, 176-180 Neuropathic bladder and spinal dysraphism MALGORZATA BORZYSKOWSKI AND B G R NEVILLE Evelina Children's Department, Guy's Hospital, London SUMMARY The
Archives of Disease in Childhood, 1981, 56, 176-180 Neuropathic bladder and spinal dysraphism MALGORZATA BORZYSKOWSKI AND B G R NEVILLE Evelina Children's Department, Guy's Hospital, London SUMMARY The
All children born with a myelomeningocele have a. Tethered cord release: a long-term study in 114 patients. Clinical article
 J Neurosurg Pediatrics 3:000 000, 3:181 187, 2009 Tethered cord release: a long-term study in 114 patients Clinical article Ro b i n M. Bo w m a n, M.D., 1 Av i n a s h Mo h a n, M.D., 1 Jo y It o, R.N.,
J Neurosurg Pediatrics 3:000 000, 3:181 187, 2009 Tethered cord release: a long-term study in 114 patients Clinical article Ro b i n M. Bo w m a n, M.D., 1 Av i n a s h Mo h a n, M.D., 1 Jo y It o, R.N.,
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Fully Endoscopic Interlaminar Detethering of Spinal Cord in Tethered Cord Syndrome: A Case Report and Technical Description
 TECHNICAL NOTE Korean J Spine 12(4):287-291, 2015 pissn 1738-2262/eISSN 2093-6729 http://dx.doi.org/10.14245/kjs.2015.12.4.287 www.e-kjs.org Fully Endoscopic Interlaminar Detethering of Spinal Cord in
TECHNICAL NOTE Korean J Spine 12(4):287-291, 2015 pissn 1738-2262/eISSN 2093-6729 http://dx.doi.org/10.14245/kjs.2015.12.4.287 www.e-kjs.org Fully Endoscopic Interlaminar Detethering of Spinal Cord in
Neurosurgery. Neurosurgery
 Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Case Report Ipsilateral Hip Dysplasia in Patients with Sacral Hemiagenesis: A Report of Two Cases
 Case Reports in Orthopedics Volume 2015, Article ID 854151, 4 pages http://dx.doi.org/10.1155/2015/854151 Case Report Ipsilateral Hip Dysplasia in Patients with Sacral Hemiagenesis: A Report of Two Cases
Case Reports in Orthopedics Volume 2015, Article ID 854151, 4 pages http://dx.doi.org/10.1155/2015/854151 Case Report Ipsilateral Hip Dysplasia in Patients with Sacral Hemiagenesis: A Report of Two Cases
Does patient history and physical examination predict MRI proven cauda equina syndrome?
 27 27 33 Does patient history and physical examination predict MRI proven cauda equina syndrome? Authors Jeremy Fairbank¹, Robin Hashimoto², Andrew Dailey ³, Alpesh A Patel³, Joseph R Dettori² Institutions
27 27 33 Does patient history and physical examination predict MRI proven cauda equina syndrome? Authors Jeremy Fairbank¹, Robin Hashimoto², Andrew Dailey ³, Alpesh A Patel³, Joseph R Dettori² Institutions
Surgery for Spinal Cord Lipomas
 39 Original Article Surgery for Spinal Cord Lipomas Manish K. Kasliwal and Ashok K. Mahapatra Department of Neurosurgery, Neurosciences Centre, All India Institute of Medical Sciences, New Delhi, India
39 Original Article Surgery for Spinal Cord Lipomas Manish K. Kasliwal and Ashok K. Mahapatra Department of Neurosurgery, Neurosciences Centre, All India Institute of Medical Sciences, New Delhi, India
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
Tethered cord syndrome: a review of the literature from embryology to adult presentation
 Neurosurg Focus 29 (1):E1, 2010 Tethered cord syndrome: a review of the literature from embryology to adult presentation De a n A. He rt z l e r II, M.D., Jo h n J. DePo w e l l, M.D., Ch a r l e s B.
Neurosurg Focus 29 (1):E1, 2010 Tethered cord syndrome: a review of the literature from embryology to adult presentation De a n A. He rt z l e r II, M.D., Jo h n J. DePo w e l l, M.D., Ch a r l e s B.
Lipomyelomeningocele (LMM) is a closed neural
 Surgical treatment for lipomyelomeningocele in children Sheng-Li Huang, Wei Shi, Li-Gen Zhang Xi'an, China Background: Lipomyelomeningocele (LMM) is a common and severe closed neural tube defect in children.
Surgical treatment for lipomyelomeningocele in children Sheng-Li Huang, Wei Shi, Li-Gen Zhang Xi'an, China Background: Lipomyelomeningocele (LMM) is a common and severe closed neural tube defect in children.
Surgery. Conus medullaris and Cauda Equina Syndromes. Anatomy. See online here
 Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Persistent Terminal Ventricle
 Persistent Terminal Ventricle Ventriculus Terminalis Incomplete regression of TV of 2 neurulation, continuity with central canal small cavity PTV vs terminal myelocystocele (?severe manifestation from
Persistent Terminal Ventricle Ventriculus Terminalis Incomplete regression of TV of 2 neurulation, continuity with central canal small cavity PTV vs terminal myelocystocele (?severe manifestation from
CAUDAL REGRESSION SYNDROME
 CAUDAL REGRESSION SYNDROME *Prateek Gehlot 1 and Jagdish Mandliya 2 1 Department of Radio-Diagnosis, R.D.Gardi Medical College,, Ujjain (MP). 2 Department of Pediatrics, R.D.Gardi Medical College, Ujjain
CAUDAL REGRESSION SYNDROME *Prateek Gehlot 1 and Jagdish Mandliya 2 1 Department of Radio-Diagnosis, R.D.Gardi Medical College,, Ujjain (MP). 2 Department of Pediatrics, R.D.Gardi Medical College, Ujjain
Laterally positioned hemivertebrae and the resultant. Dorsal midline hemivertebra at the lumbosacral junction: report of 2 cases.
 spine case report J Neurosurg Spine 22:84 89, 2015 Dorsal midline hemivertebra at the lumbosacral junction: report of 2 cases Shaheryar F. Ansari, MD, 1 Richard B. Rodgers, MD, 2 and Daniel H. Fulkerson,
spine case report J Neurosurg Spine 22:84 89, 2015 Dorsal midline hemivertebra at the lumbosacral junction: report of 2 cases Shaheryar F. Ansari, MD, 1 Richard B. Rodgers, MD, 2 and Daniel H. Fulkerson,
Tethered cord syndrome is a rare intraspinal anomaly, Pediatric tethered cord syndrome: response of scoliosis to untethering procedures
 J Neurosurg Pediatrics 4:000 000, 4:270 274, 2009 Pediatric tethered cord syndrome: response of scoliosis to untethering procedures Clinical article Ma t t h e w J. McGi r t, M.D., 1 Vi v e k Me h ta,
J Neurosurg Pediatrics 4:000 000, 4:270 274, 2009 Pediatric tethered cord syndrome: response of scoliosis to untethering procedures Clinical article Ma t t h e w J. McGi r t, M.D., 1 Vi v e k Me h ta,
Spinal congenital dermal sinus with dual ostia
 J Neurosurg Pediatrics 3:000 000, 3:407 411, 2009 Spinal congenital dermal sinus with dual ostia Clinical article Ch a n g Su b Le e, M.D., 1 Ji Ho o n Ph i, M.D., 2 Se u n g -Ki Kim, M.D., Ph.D., 2 By
J Neurosurg Pediatrics 3:000 000, 3:407 411, 2009 Spinal congenital dermal sinus with dual ostia Clinical article Ch a n g Su b Le e, M.D., 1 Ji Ho o n Ph i, M.D., 2 Se u n g -Ki Kim, M.D., Ph.D., 2 By
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
The Chiari malformation I (CM I) is a disorder that has been
 DOI: 10.5137/1019-5149.JTN.18349-16.1 Received: 31.05.2016 / Accepted: 01.07.2016 Published Online: 22.08.2016 Original Investigation Are Herniated Cerebellar Tonsils the Main Culprit of Chiari Malformation
DOI: 10.5137/1019-5149.JTN.18349-16.1 Received: 31.05.2016 / Accepted: 01.07.2016 Published Online: 22.08.2016 Original Investigation Are Herniated Cerebellar Tonsils the Main Culprit of Chiari Malformation
Corporate Medical Policy
 Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Spinal Stenosis Surgical
 Spinal Stenosis Surgical Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Spinal Stenosis Surgical Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Congenital Spinal Lipoma: analyzing the perplexed nomenclature and our management
 Congenital Spinal Lipoma: analyzing the perplexed nomenclature and our management Nidal Khasawneh MD *, Rami Alqroom MD *, Firas Sha'ban MD *, Rafeed Al Drous MD *, Rima Nserat **, Amer Al Shurbaji MD
Congenital Spinal Lipoma: analyzing the perplexed nomenclature and our management Nidal Khasawneh MD *, Rami Alqroom MD *, Firas Sha'ban MD *, Rafeed Al Drous MD *, Rima Nserat **, Amer Al Shurbaji MD
Simultaneous Surgical Treatment in Congenital Scoliosis and/or Kyphosis Associated With Intraspinal Abnormalities
 Simultaneous Surgical Treatment in Congenital Scoliosis and/or Kyphosis Associated With Intraspinal Abnormalities SPINE Volume 32, Number 25, pp 2880 2884 2007, Lippincott Williams & Wilkins, Inc. Azmi
Simultaneous Surgical Treatment in Congenital Scoliosis and/or Kyphosis Associated With Intraspinal Abnormalities SPINE Volume 32, Number 25, pp 2880 2884 2007, Lippincott Williams & Wilkins, Inc. Azmi
Guillermo Aldave, MD, PhD, 1 Daniel Hansen, MD, 1 Steven W. Hwang, MD, 2 Amee Moreno, NP, 1 Valentina Briceño, RN, 1 and Andrew Jea, MD 1,3
 CLINICAL ARTICLE J Neurosurg Pediatr 19:703 710, 2017 Spinal column shortening for tethered cord syndrome associated with myelomeningocele, lumbosacral lipoma, and lipomyelomeningocele in children and
CLINICAL ARTICLE J Neurosurg Pediatr 19:703 710, 2017 Spinal column shortening for tethered cord syndrome associated with myelomeningocele, lumbosacral lipoma, and lipomyelomeningocele in children and
Guidelines in the management of neural tube defects and hydrocephalus
 Guidelines in the management of neural tube defects and hydrocephalus Dominic Venne, MD, MSc, FRCSC, Division of Neurosurgery Sheikh Khalifa Medical City Abu Dhabi, UAE 1. Introduction: Neural tube defects
Guidelines in the management of neural tube defects and hydrocephalus Dominic Venne, MD, MSc, FRCSC, Division of Neurosurgery Sheikh Khalifa Medical City Abu Dhabi, UAE 1. Introduction: Neural tube defects
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
Managing life with neurological symptoms
 Managing life with neurological symptoms Petra M Klinge Professor of Neurosurgery Director, Division of Pediatric Neurosurgery Director, CSF center of the brain and Spine Rhode Island Hospital and Hasbro
Managing life with neurological symptoms Petra M Klinge Professor of Neurosurgery Director, Division of Pediatric Neurosurgery Director, CSF center of the brain and Spine Rhode Island Hospital and Hasbro
Diastematomyelia: A Case with Familial Aggregation of Neural Tube Defects
 Case Study TheScientificWorldJOURNAL (2004) 4, 847 852 ISSN 1537-744X; DOI 10.1100/tsw.2004.140 Diastematomyelia: A Case with Familial Aggregation of Neural Tube Defects Nuray Öksüz Kanbur 1, *, Pınar
Case Study TheScientificWorldJOURNAL (2004) 4, 847 852 ISSN 1537-744X; DOI 10.1100/tsw.2004.140 Diastematomyelia: A Case with Familial Aggregation of Neural Tube Defects Nuray Öksüz Kanbur 1, *, Pınar
Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for
 Chapter 13 Outline Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for what you need to know from Exhibits 13.1 13.4 I. INTRODUCTION A. The spinal cord and spinal nerves
Chapter 13 Outline Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for what you need to know from Exhibits 13.1 13.4 I. INTRODUCTION A. The spinal cord and spinal nerves
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Split cord malformation in children undergoing neurosurgical intervetion in India: a descriptive study
 ORIGINAL ARTICLE Journal of Pediatric Neurology 2004; 2(1): 21-27 www.jpneurology.org in children undergoing neurosurgical intervetion in India: a descriptive study Raj Kumar 1, Vinita Singh 2, Satya Narayan
ORIGINAL ARTICLE Journal of Pediatric Neurology 2004; 2(1): 21-27 www.jpneurology.org in children undergoing neurosurgical intervetion in India: a descriptive study Raj Kumar 1, Vinita Singh 2, Satya Narayan
Lipomyelomeningocele for the Urologist: should we view it the same as myelomeningocele?
 Lipomyelomeningocele for the Urologist: should we view it the same as myelomeningocele? Grace Yoshiba BS Chris Halline, BA Earl Y. Cheng MD Theresa A. Meyer RN Ilina Rosoklija MPH Robin Bowman MD Elizabeth
Lipomyelomeningocele for the Urologist: should we view it the same as myelomeningocele? Grace Yoshiba BS Chris Halline, BA Earl Y. Cheng MD Theresa A. Meyer RN Ilina Rosoklija MPH Robin Bowman MD Elizabeth
Management of Bone and Spinal Cord in Spinal Surgery.
 Management of Bone and Spinal Cord in Spinal Surgery. G. Saló, PhD, MD. Senior Consultant Spine Unit. Hospital del Mar. Barcelona. Ass. Prof. Universitat Autònoma de Barcelona. Introduction The management
Management of Bone and Spinal Cord in Spinal Surgery. G. Saló, PhD, MD. Senior Consultant Spine Unit. Hospital del Mar. Barcelona. Ass. Prof. Universitat Autònoma de Barcelona. Introduction The management
Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment
 Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
Disclosures None. Common Neurosurgical Problems Seen in Office Encounters. Macrocephaly Low Back Pain Sacral Dimple Concussion Chiari Malformation
 Common Neurosurgical Problems Seen in Office Encounters When to Manage, When to Refer Andrew Jea MD FAAP Professor and Chief of Pediatric Neurosurgery Riley Hospital for Children Indiana University School
Common Neurosurgical Problems Seen in Office Encounters When to Manage, When to Refer Andrew Jea MD FAAP Professor and Chief of Pediatric Neurosurgery Riley Hospital for Children Indiana University School
Sonography of the Neonatal Spine: Part 2, Spinal Disorders
 Neonatal Spine Sonography Pediatric Imaging Pictorial Essay Downloaded from www.ajronline.org by 148.251.232.83 on 04/11/18 from IP address 148.251.232.83. Copyright RRS. For personal use only; all rights
Neonatal Spine Sonography Pediatric Imaging Pictorial Essay Downloaded from www.ajronline.org by 148.251.232.83 on 04/11/18 from IP address 148.251.232.83. Copyright RRS. For personal use only; all rights
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Chiari malformations. A fact sheet for patients and carers
 A fact sheet for patients and carers Chiari malformations This fact sheet provides information on Chiari malformations. It focuses on Chiari malformations in adults. Our fact sheets are designed as general
A fact sheet for patients and carers Chiari malformations This fact sheet provides information on Chiari malformations. It focuses on Chiari malformations in adults. Our fact sheets are designed as general
S YRINGOMYELIA and syringobulbia are
 Syringomyelia: A Look at Surgical Therapy J. GRAFTON LOVE, M.D. AND RICHARD A. OLAFSON, M.D. Mayo Clinic and Mayo Foundation, Section of Neurologic Surgery, and Mayo Graduate School of Medicine, University
Syringomyelia: A Look at Surgical Therapy J. GRAFTON LOVE, M.D. AND RICHARD A. OLAFSON, M.D. Mayo Clinic and Mayo Foundation, Section of Neurologic Surgery, and Mayo Graduate School of Medicine, University
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Chiari FAQ's. 1. What is a Chiari Malformation?
 Chiari FAQ's These FAQ's are for informational purposes only and in no way represent an attempt to provide medical advice. This information may or may not apply to your case and anyone with a question
Chiari FAQ's These FAQ's are for informational purposes only and in no way represent an attempt to provide medical advice. This information may or may not apply to your case and anyone with a question
Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management
 THIEME Original Article 15 Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management Vernon Velho 1 Sachin Guthe 1 Pravin Survashe 1 Poonam
THIEME Original Article 15 Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management Vernon Velho 1 Sachin Guthe 1 Pravin Survashe 1 Poonam
Orthopedic Issues in Children with Special Healthcare Needs
 Orthopedic Issues in Children with Special Healthcare Needs Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department
Orthopedic Issues in Children with Special Healthcare Needs Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department
Spinal Cord Protection. Chapter 13 The Spinal Cord & Spinal Nerves. External Anatomy of Spinal Cord. Structures Covering the Spinal Cord
 Spinal Cord Protection Chapter 13 The Spinal Cord & Spinal Nerves We are only going to cover Pages 420-434 and 447 Together with brain forms the CNS Functions spinal cord reflexes integration (summation
Spinal Cord Protection Chapter 13 The Spinal Cord & Spinal Nerves We are only going to cover Pages 420-434 and 447 Together with brain forms the CNS Functions spinal cord reflexes integration (summation
The spinal dermal-sinus-like stalk
 Childs Nerv Syst (2009) 25:191 197 DOI 10.1007/s00381-008-0669-6 ORIGINAL PAPER The spinal dermal-sinus-like stalk J. van Aalst & E. A. M. Beuls & E. M. J. Cornips & H. W. M. van Straaten & A. F. M. Boselie
Childs Nerv Syst (2009) 25:191 197 DOI 10.1007/s00381-008-0669-6 ORIGINAL PAPER The spinal dermal-sinus-like stalk J. van Aalst & E. A. M. Beuls & E. M. J. Cornips & H. W. M. van Straaten & A. F. M. Boselie
Johnson Rogers and colleagues- used Term LMM
 LIPOMENINGOMYELOCELE: CLASSIFICATION, MANAGEMENT AND CONTROVERSIES Definition : Lipomyelomeningocele is a form of OSD in which a subcutaneous fibrofatty mass traverses the lumbodorsal fascia, causes a
LIPOMENINGOMYELOCELE: CLASSIFICATION, MANAGEMENT AND CONTROVERSIES Definition : Lipomyelomeningocele is a form of OSD in which a subcutaneous fibrofatty mass traverses the lumbodorsal fascia, causes a
Corporate Medical Policy
 Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Filum terminale lipomas (FTLs) are a type of lumbosacral. Filum terminale lipomas: imaging prevalence, natural history, and conus position
 J Neurosurg Pediatrics 13:559 567, 2014 AANS, 2014 Filum terminale lipomas: imaging prevalence, natural history, and conus position Clinical article Michael J. Cools, M.D., 1 Wajd N. Al-Holou, M.D., 1
J Neurosurg Pediatrics 13:559 567, 2014 AANS, 2014 Filum terminale lipomas: imaging prevalence, natural history, and conus position Clinical article Michael J. Cools, M.D., 1 Wajd N. Al-Holou, M.D., 1
Human Anatomy. Spinal Cord and Spinal Nerves
 Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
The Spinal Cord & Spinal Nerves
 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward and downward travel
The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward and downward travel
Review date: February Lumbar Discectomy
 Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Introduction to the Tethered Cord Syndrome
 1 Introduction to the Tethered Cord Syndrome Shokei Yamada The word tether means to restrain, an example of which is an animal held to the maximal range of motion by a rope. This definition leads to the
1 Introduction to the Tethered Cord Syndrome Shokei Yamada The word tether means to restrain, an example of which is an animal held to the maximal range of motion by a rope. This definition leads to the
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Anatomy of the Nervous System. Brain Components
 Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
Surgical treatments on adult tethered cord syndrome: A retrospective study
 Surgical treatments on adult tethered cord syndrome: A retrospective study The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation
Surgical treatments on adult tethered cord syndrome: A retrospective study The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation
Chiari Malformations. Google. Objectives Seventh Annual NKY TBI Conference 3/22/13. Kerry R. Crone, M.D.
 Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Iatrogenic lumbar Pseudomeningocele: A case report and review of literature
 Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Minimally Invasive Discectomy/ Decompression
 Minimally Invasive Discectomy/ Decompression What Is A Minimally Invasive Lumbar Discectomy? A lumbar discectomy is a surgical procedure that involves relieving the pressure placed on nerve roots and/or
Minimally Invasive Discectomy/ Decompression What Is A Minimally Invasive Lumbar Discectomy? A lumbar discectomy is a surgical procedure that involves relieving the pressure placed on nerve roots and/or
Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms.
 RHEUMATOID SPINE Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms. When neurology is present it may manifest
RHEUMATOID SPINE Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms. When neurology is present it may manifest
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
ASJ. Myxopapillary Ependymoma of the Cauda Equina in a 5-Year-Old Boy. Asian Spine Journal. Introduction
 Asian Spine Journal 846 Masashi Case Uehara Report et al. Asian Spine J 2014;8(6):846-851 http://dx.doi.org/10.4184/asj.2014.8.6.846 Asian Spine J 2014;8(6):846-851 Myxopapillary Ependymoma of the Cauda
Asian Spine Journal 846 Masashi Case Uehara Report et al. Asian Spine J 2014;8(6):846-851 http://dx.doi.org/10.4184/asj.2014.8.6.846 Asian Spine J 2014;8(6):846-851 Myxopapillary Ependymoma of the Cauda
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES
 A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
LUMPS, TUFTS AND DIMPLES IT S THE PITS!! Session Information. Faculty Disclosure Information
 Session Information Session Title: Lumps, Tufts and Dimples Session Number: F3056, F2130 Faculty Name: Mark S. Dias, MD, FAAP Faculty Institution: Penn State Children s Hospital, Penn State University
Session Information Session Title: Lumps, Tufts and Dimples Session Number: F3056, F2130 Faculty Name: Mark S. Dias, MD, FAAP Faculty Institution: Penn State Children s Hospital, Penn State University
PATIENT: DOB: TODAY S DATE:
 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
MRI of chronic spinal cord injury
 The British Journal of Radiology, 76 (2003), 347 352 DOI: 10.1259/bjr/11881183 E 2003 The British Institute of Radiology Pictorial review MRI of chronic spinal cord injury 1 K POTTER, FRCR and 1 A SAIFUDDIN,
The British Journal of Radiology, 76 (2003), 347 352 DOI: 10.1259/bjr/11881183 E 2003 The British Institute of Radiology Pictorial review MRI of chronic spinal cord injury 1 K POTTER, FRCR and 1 A SAIFUDDIN,
Chapter 13. The Spinal Cord & Spinal Nerves. Spinal Cord. Spinal Cord Protection. Meninges. Together with brain forms the CNS Functions
 Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
Neonatal Spinal Ultrasound Imaging - A Pictorial Review from The Royal Liverpool Children Hospital, Alder Hey, Liverpool
 Neonatal Spinal Ultrasound Imaging - A Pictorial Review from The Royal Liverpool Children Hospital, Alder Hey, Liverpool Poster No.: C-0081 Congress: ECR 2012 Type: Educational Exhibit Authors: K. Chetcuti,
Neonatal Spinal Ultrasound Imaging - A Pictorial Review from The Royal Liverpool Children Hospital, Alder Hey, Liverpool Poster No.: C-0081 Congress: ECR 2012 Type: Educational Exhibit Authors: K. Chetcuti,
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
The ABC s of LUMBAR SPINE DISEASE
 The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery Diagnosis/Imaging/Surgery of Lumbar Spine Disorders Objectives Identify the most common
The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery Diagnosis/Imaging/Surgery of Lumbar Spine Disorders Objectives Identify the most common
Nursing review section of Surgical Neurology International: Part 1 lumbar disc disease
 SNI: Neurosurgical Nursing OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein, MD Winthrop Hospital, Mineola, NY, USA Review Article Nursing review
SNI: Neurosurgical Nursing OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein, MD Winthrop Hospital, Mineola, NY, USA Review Article Nursing review
