Disability Duration Guidelines
|
|
|
- Willis Horn
- 6 years ago
- Views:
Transcription
1 Updated: 11/2015
2 Table of Contents Introduction... 2 Permanent Functional Impairment ()... 2 Disclaimer... 3 s... 3 Factors Influencing Duration of Disability... 6 General Procedures... 6 Miscellaneous Soft Tissue Injuries (all body regions) :... 6 Open Wounds:... 7 Upper Extremities... 9 Upper Extremities: Fractures... 9 Upper Extremities: Dislocations Upper Extremities: Soft Tissue Injuries: Sprains and Strains Upper Extremities: Amputations Upper Extremities: Miscellaneous Upper Extremities: Surgical/Therapeutic/Diagnostic Procedures Lower Extremities...20 Lower Extremities: Fractures Pelvis Lower Extremities: Dislocation Lower Extremities: Soft Tissue Injuries: Sprains and Strains Lower Extremities: Amputations Lower Extremities: Surgical/Therapeutic/Diagnostic Procedures Error! Bookmark not defined.0 Head/Trunk/Spine Head/Trunk/Spine: Fractures Head/Trunk/Spine: Dislocations/Subluxations Head/Trunk/Spine: Soft Tissue Injuries: Sprains and Strains Head/Trunk/Spine: Surgical/Therapeutic/Diagnostic Procedures Appendix A. Glossary of Terms Appendix B. Categorization of Muscle/Tendon Strains and Joint/Ligament Sprains P age
3 Introduction The Saskatchewan WCB uses these guidelines to determine which workers might require additional case management and/or medical services to reach maximum recovery and return to work. Recovery Time Many factors influence recovery time, i.e. psychosocial considerations, age, associated medical conditions, complications, and treatment including surgery and medications. It is important that these are taken into account when using these guidelines. Refer to Factors Influencing Duration of Disability section for more information. Return to Work The guidelines give an estimate of the approximate time required for workers to return to work after various work-related injuries and treatments. It should be emphasized that: The maximum time given is not necessarily a definite RTW date, but rather the time when questions should be asked as to why the worker has not returned to work. The questions may be answered by medical reporting, discussion with the treating physician or it may be necessary to attend an independent assessment team review. These guidelines are specific to the injured part (e.g. fracture, tendon rupture, etc.) yet take into account that the worker need not lose time away from work if modified or alternate job duties are available or work duties may be safely performed using uninjured limbs, without compromising treatment. Permanent Functional Impairment () With respect to, the following terms are utilized in the Guidelines: Term Definition Not anticipated Possible Expected Complete recovery anticipated Injury may result in some assessable impairment depending on case. anticipated or scheduled This material is copyright by, and used with the permission of, The Workers' Compensation Board of Alberta (c) All rights reserved. These guidelines were prepared from the following sources: The Medical Disability Advisor - Workplace Guidelines for Disability Duration by Presley Reed, M.D., Second Edition, This resource is the industry standard, supported by occupational health and safety associations in United State and Canada. External clinical experience Alberta WCB experience. No warranty of any kind, implied, expressed or statutory, including, but not limited to, the warranties of merchantability or fitness for a particular purpose is given with respect to the contents of the Guidelines. 2 P age
4 Disclaimer These are not intended to provide strict rules for these conditions in all workers. The Guidelines have been prepared to assist case managers and care providers in medical management of claims. No warranty of any kind, implied, expressed or statutory, including, but not limited to, the warranties of merchantability or fitness for a particular purpose is given with respect to the contents of the Guidelines. Injury duration may vary from these guidelines if, in the judgment of the WCB or care provider, variance is warranted: To meet the health care needs of the workers To fall within standards generally accepted by the health care community. In determining the expected length of disability, the physical and other specific requirements of the job to which an injured worker is to return must be considered. classify all jobs into categories based on their physical requirements - sedentary, light, medium, heavy and very heavy. These categories are accepted by occupational health professionals in both the United States and Canada. These guidelines are specific to the injured part (e.g. fracture, tendon rupture, etc.) that take into account that the work need not lose time away from work if modified or alternate job duties are available or work duties may be safely performed using uninjured limbs, without compromising treatment. These Guidelines cannot be used to determine the period for which benefits are paid. s The job classifications in the tables are taken from the U.S. Department of Labor's Dictionary of Occupational Titles, and are comparable to those classifications as found in the National Occupational Classification Career Handbook (NOC-CH). - Exerting up to 10 pounds of force occasionally and/or a negligible amount of force frequently or constantly to lift, carry, push, pull or otherwise move objects, including the human body. Sedentary work involves sitting most of the time, but may involve walking or standing for brief periods of time. Jobs are sedentary if walking and standing are required only occasionally and all other sedentary criteria are met. - Exerting up to 20 pounds of force occasionally and/or up to 10 pounds of force frequently, and/or negligible amount of force constantly to move objects. Physical demand requirements are in excess of those for sedentary work. Light work usually requires walking or standing to a significant degree. However, if the use of the arm and/or leg controls require exertion of forces greater than that for sedentary work, and the worker sits most of the time, the job is rated light work. - Exerting up to 50 pounds of force occasionally, and/or up to 20 pounds of force frequently, and/or up to 10 pounds of force constantly to move objects. 3 P age
5 - Exerting up to 100 pounds of force occasionally, and/or up to 50 pounds of force frequently, and/or up to 20 pounds of force constantly to move objects. Very - Exerting in excess of 100 pounds of force occasionally, and/or in excess of 50 pounds of force frequently, and/or in excess of 20 pounds of force constantly to move objects. Factors Influencing Duration of Disability A. General Factors Some important factors that may influence duration of disability include: Psychological Factors Age Motivation to return to work Attitude of employer towards employee Availability of co-worker to help out Pre-existing psychological condition(s) Prior experience with injury/illness Age may contribute to the course/progress of recovery/healing Complications Medical complications resulting from the primary condition and/or subsequent therapeutic procedures Medication Medications can restrict the type of work an individual can safely perform Individual Variation There may be different durations of disability among workers with the same injury/illness or undergoing the same procedure because of: Severity of the condition Individual response to treatment The course of recovery Late diagnosis Whether treatment is medical or surgical Presence of pre-existing or incidental condition(s) 4 P age
6 B. Fractures Factors that may influence duration of disability: Age The specific fracture The stability of the fracture Direction and degree of displacement Degree of commination Extent of articular damage Severity of associated soft tissue injury (nerves, blood vessels, tendons and ligaments) Promptness, method and adequacy of treatment Duration of immobilization Presence of complications Surgical treatment Life style/occupational requirements Pre-existing or incidental condition(s) e.g. osteoporosis C. Dislocations Factor that may influence duration of disability: Which joint is involved Direction and degree of displacement Severity of associated damage to ligaments, tendons, or articular surfaces Neurovascular damage Type and promptness of treatment Life style/occupational requirements Pre-existing or incidental condition(s) D. Sprains and Strains Factor that may influence duration of disability: Severity of the injury Location Need for surgical repair Timing of surgical repair Promptness of treatment Life style/occupational requirements Pre-existing or incidental condition(s) E. Amputations Factors that may influence duration of disability: An underlying disease process The particular limb or digit amputated Whether dominant or non-dominant hand/arm is involved 5 P age
7 Complications Life style/occupational requirements Pre-existing or incidental condition(s) F. Procedures Factors that may influence duration of disability: The condition for which the procedure is done Whether dominant or non-dominant hand/arm is involved Complications Joint involved Lifestyle/occupational requirements Pre-existing or incidental condition(s) General Procedures Head/Trunk/Spine RTW - Minimum/Maximum 1 day - 1 week Not anticipated Very Heavy 1 day - 2 weeks 1 day - 2 weeks 1 day - 2 weeks 1 day - 2 weeks Miscellaneous Soft Tissue Injuries (all body regions): Bursitis: RTW - Minimum/Maximum 0 day - 2 week Not anticipated Very Heavy 0 day - 3 weeks 1 week - 4 weeks 1 week - 6 weeks 1 week - 8 weeks 6 P age
8 Open Wounds: Lacerations and Punctures: superficial I Single Fusion RTW- Minimum/Maximum 0 days - 2 weeks Not anticipated 0 days - 2 weeks 1 week - 2 week 1 week - 2 week Very 1 week - 2 week Complex: RTW - Minimum/Maximum Possible 12 Months Very Contusion: usually not disabling RTW- Minimum/Maximum 0 days - 2 weeks Not anticipated 0 days - 2 weeks 0 days - 2 weeks 0 days - 2 weeks Very Heavy 0 days - 2 weeks Crash Injury: RTW- Minimum/Maximum if return to work more than 4 weeks Possible 18 Months 7 P age
9 Complications of Trauma or Surgical Procedures 1. Deep vein thrombosis 2. Pulmonary embolus 3. Fat emboli 4. Infection Be guided s and Medical Advisor review Scapula Very Possible 18 Months 8 P age
10 Nerve Injuries of Extremities There are usually other injuries involved with major nerve injuries (i.e. crush injury). The return to work date will often depend on the severity of the combined injuries. Upper Extremities Upper Extremities: Fractures Clavicle : Shaft Very Not anticipated Humerus: Very Possible 12 Months Radius: shaft Very Not Anticipated 9 P age
11 Ulna: shaft Very Not Anticipated Radius and Ulna: shaft Very Not Anticipated Colles Fracture: Very Possible 18 Months Carpal Bones: excluding scaphoid Very Possible 18 Months 10 P age
12 Scaphoid Bone: any evidence of avascular necrosis/non-union requires Medical Advisor opinion Very Possible 24 Months Metacarpal Bones Very Not anticipated Phalanges Very Not anticipated Upper Extremities: Dislocations Acromioclavicular (AC) Joint and Sternoclavicular (SC) Joint: RTW - Minimum/Maximum 0 days- 3 weeks Possible 18 Months 0 days- 4 weeks 2 weeks- 6 weeks 3 weeks - 8 weeks Very 4 weeks- 8 weeks 11 P age
13 Includes all sprains (Grade I-III) treated non-surgically. Glenohumeral Joint: traumatic anterior and posterior and first time dislocation (different for multidirectional instability and for multiple RTW - Minimum/Maximum 0 days- 2 weeks Possible 18 Months Very 1 week - 4 weeks 1 weeks- 4 weeks 4 weeks - 6 weeks 4 weeks- 6 weeks Elbow: RTW - Minimum/Maximum 1 week - 3 weeks Expected 18 Months 2 week - 6 weeks 4 weeks- 8 weeks 6 weeks - 10 weeks Very 6 weeks- 12 weeks Wrist: includes distal radial ulnar joint RTW - Minimum/Maximum 3 days- 2 weeks Expected 24 Months 1 week - 4 weeks 2 weeks- 6 weeks Very Finger or Thumb Joints: interphalangeal joints (all) and distal interphalangeal (DIP) and proximal interphalangeal (PIP) joints of the finger RTW - Minimum/Maximum 0 days- 1 week Not anticipated Very 0 days - 2 weeks 1 weeks- 3 weeks 1 weeks - 4 weeks 1 weeks- 4 weeks 12 P age
14 Metacarpophalangeal (MCP) Joint(s): RTW - Minimum/Maximum Requires Medical Advisor opinion Possible 18 Months Glenohumeral Joint Instability: recurrent dislocation and/or subluxation RTW - Minimum/Maximum Sedentary/ 0 days - 2 week Not anticipated (where WCB not responsible for the underlying condition or surgery) Heavy/Very Heavy Work 1 week - 3 weeks 1 week - 4 weeks Upper Extremities: Soft Tissue Injuries: Sprains and Strains Shoulder/Wrist/Elbow/Fingers: RTW - Minimum/Maximum 0 days - 3 weeks Not anticipated 0 days - 3 weeks 1 weeks- 4 weeks 2 weeks - 4 weeks Very 2 weeks- 4 weeks Tendonitis, Epicondylitis: medial/lateral RTW - Minimum/Maximum 0 days- 3 weeks Not anticipated 0 days- 3 weeks 1 weeks- 4 weeks 2 weeks - 6 weeks Very 2 weeks- 8 weeks 13 P age
15 Thumb: including sprain to media/lateral ligament RTW - Minimum/Maximum Sedentary/Medium work Heavy/Very Heavy Work 0 days- 6 weeks Possible 12 Months 1 week- 8 weeks * Depends on joint injured, severity and whether dominant or non-dominant hand is involved Biceps Tendinitis: long head RTW - Minimum/Maximum Sedentary/ 0 days- 3 weeks Not anticipated Heavy/Very Heavy Work 0 days- 4 weeks 4 weeks- 12 weeks *Depends on severity of symptoms, whether dominant and extremity involved. Rotator Cuff Tendinitis/Strain: 1st to 3rd degree RTW - Minimum/Maximum 0 days- 4 days Not anticipated but possible with 3rd degree Very 0 days- 1 weeks 2 weeks- 6 weeks 4 weeks - 12 weeks 4 weeks- 12 weeks Upper Extremities: Amputations Finger: any level RTW - Minimum/Maximum 0 days- 2 weeks Expected 18 Months Very 0 days- 2 weeks 2 weeks- 4 weeks 4 weeks - 6 weeks 4 weeks- 6 weeks 14 P age
16 Thumb: Interphalangeal (IP) RTW - Minimum/Maximum 0 days- 2 weeks Expected 18 Months 2 days- 4 weeks 4 weeks- 6 weeks 6 weeks - 8 weeks Very 6 weeks- 8 weeks Thumb: TOTAL RTW - Minimum/Maximum 2 weeks - 4 weeks Expected 18 Months 3 weeks- 4 weeks 4 weeks- 6 weeks by assessment Very by assessment Upper Extremities: Miscellaneous Carpal Tunnel Syndrome: no surgery Need for layoff/return to work would be based on Doctor's reports and whether modified, non-repetitive duties are available. Not anticipated Upper Extremities: Surgical/Therapeutic/Diagnostic Procedures Tendon Repairs/Transfers RTW- Minimum/Maximum 2 weeks - 4 weeks Possible 18 Months 2 weeks - 6 weeks 4 weeks- 8 weeks 4 weeks- 8 weeks Very 6 weeks - 12 weeks 15 P age
17 Tenolysis/Tendon Releases: RTW- Minimum/Maximum 2 weeks - 4 weeks Possible 18 Months 2 weeks - 4 weeks 3 weeks- 6 weeks 3 weeks- 6 weeks Very 4 weeks - 8 weeks Repair of Rotator Cuff and/or Biceps Tendon Tear(s):arthroscopic or open arthrotomy RTW - Minimum/Maximum Sedentary / 1 weeks - 3 weeks Possible 24 Months 4 weeks - 8 weeks Heavy\Very 8 weeks- 12 weeks * Disability may be permanent if work requires arms overhead Decompression Surgery for Impingement syndrome: arthroscopic or open arthrotomy RTW - Minimum/Maximum Sedentary / 2 weeks - 4 weeks Possible 24 Months 6 weeks - 12 weeks Heavy\Very 12 weeks- 16 weeks * Disability may be permanent if work requires arms overhead Radial Head/Neck Resection: primary radial head/neck resection for fracture RTW - Minimum/Maximum 3 weeks Possible 18 Months 6 weeks 8 weeks 12 weeks Very 12 weeks 16 P age
18 Ulnar Nerve Transposition: RTW - Minimum/Maximum 4 weeks Not anticipated 4 weeks 6 weeks 6 weeks Very 6 weeks Shoulder Repair- Glenohumeral Dislocation: recurrent RTW - Minimum/Maximum 2 weeks - 4 weeks Possible 24 Months post-surgery Very 3 weeks - 6 weeks 4 weeks- 8 weeks 6 weeks - 10 weeks Unlikely to return to Very Carpal Tunnel Release: RTW -Minimum/Maximum 0 days - 3 weeks Not anticipated but possible Minimum 24 Months post-surgery Very 0 days - 3 weeks 0 days - 3 weeks 3 weeks - 6 weeks 3 weeks - 6 weeks 17 P age
19 Carpal Fusion: RTW - Minimum/Maximum 8 weeks - 12 weeks Expected 24 Months post-surgery Very 12 weeks - 16 weeks 12 weeks - 16 weeks 6 months - probably not advisable 6 months - probably not advisable Fusion of Metacarpal - Phalangeal (MP) Joint of Thumb: RTW - Minimum/Maximum 6 weeks - 10 weeks Expected 18 Months post-surgery Very 6 weeks - 10 weeks 10 weeks - 14 weeks 18 weeks 18 weeks Fusion of Interphalangeal Joints of Finger and Thumb: RTW - Minimum/Maximum 1 week - 6 weeks Expected 18 Months post-surgery Very 1 week - 6 weeks 4 weeks - 8 weeks 8 weeks - 10 weeks 8 weeks - 10 weeks Acromioclavicular (AC) Excision (Mumford): RTW - Minimum/Maximum 2 weeks - 4 weeks Expected 24 Months post-surgery Very 4 week - 6 weeks 6 weeks - 8 weeks 8 weeks - 10 weeks 10 weeks - 12 weeks 18 P age
20 Acromioclavicular (AC) Joint Surgical Reduction : (Grade IV - V ACJ Separation) RTW - Minimum/Maximum 2 weeks - 8 weeks Not anticipated Very 6 weeks - 8 weeks 8 weeks- 10 weeks 10 weeks - 12 weeks 10 weeks - 12 weeks Injured arm should be relatively immobile for 6 weeks to allow for good soft tissue healing. 19 P age
21 Lower Extremities Lower Extremities: Fractures Pelvis Minor Fracture: stable pelvic ring or avulsions not involving pelvic ring Not anticipated with single fracture Possible if symptom resolution slow 18 Months to 24 Months Very Major Fractures: unstable/serious complications expected 24 Months post-injury Acetabulum - Displaced: Very Expected 24 Months post-injury (in future due to O.A.) Acetabulum - Displaced: expected 24 Months post-injury 20 P age
22 Hip: head, neck including sub trochanter region Very Expected 24 Months post-injury Femur: shaft Very Expected 18 Months to 24 Months post-injury Intra-Articular Fractures of the knee: distal femur and proximal tibia Very Expected 24 Months post-injury Patella: Displaced: non-operative treatment Very Expected 18 Months to 24 Months post-injury 21 P age
23 Patella: Displaced: surgical reduction Very Expected 24 Months post-injury Tibia: shaft Very Possible 18 Months post-injury Fibula: shaft Very Not anticipated Ankle: Unimalleolar: Lateral or medial malleolus (excluding flake fractures): Very Lateral malleolus: Not anticipated Medial malleolus: Possible 24 Months post-injury 22 P age
24 Ankle: Bimalleolar: Medium Very Expected 24 Months post-injury Trimalleolar: Medium Very Expected 24 Months post-injury Trimalleolar fracture with diastasis of the inferior tibiofibular joint: Expected 24 Months post-injury Very Talus: Very Expected 24 Month post-injury 23 P age
25 Calcaneum: os calcis - Displaced Very Not anticipated Calcaneum: os calcis - Displaced: Very Possible 24 Months post-injury Tarsal Bones: excluding talus and os calcis Very Expected 24 Month post-injury Metatarsal: Very Not anticipated Possible- with multiple fractures 24 P age
26 Toes: lesser Not anticipated Very Toes : great Very Possible with joint involvement (interphalangeal or metatarsalphalangael) 18 Months 25 P age
27 Lower Extremities: Dislocation Hip Joint: RTW - Minimum/Maximum 4 weeks - 12 weeks Possible 24 Months post-injury Very 8 weeks - 12 weeks 8 weeks - 12 weeks 8 weeks - 12 weeks Knee Joint: RTW - Minimum/Maximum Expected 24 Months post-injury Very Patella: RTW - Minimum/Maximum 1 weeks - 3 weeks Not anticipated 3 weeks - 6 weeks 6 weeks - 8 weeks 8 weeks - 12 weeks Very 8 weeks - 12 weeks 26 P age
28 Tarso-Metatarsal Joint: RTW - Minimum/Maximum 3 weeks - 6 weeks Possible 24 Months post-injury Very 3 weeks - 6 weeks 6 weeks - 8 weeks 8 weeks - 10 weeks Toes: RTW - Minimum/Maximum 0 weeks - 1 weeks Not anticipated 0 weeks - 3 weeks 0 weeks - 3 weeks 0 weeks - 3 weeks Very 3 weeks - 5 weeks Lower Extremities: Soft Tissue Injuries: Sprains and Strains Knee: medial and lateral collateral ligaments RTW - Minimum/Maximum 0 weeks - 1 weeks Not anticipated 0 weeks - 2 weeks 2 weeks - 8 weeks 2 weeks - 8 weeks Very 2 weeks - 12 weeks Anterior Cruciate Ligament (ACL) Tear (without surgery) and Posterior Cruciate Ligament Tear (PCL): RTW - Minimum/Maximum 3 weeks - 4 weeks Possible 24 Months 4 weeks - 6 weeks 6 weeks - 8 weeks 8 weeks - 12 weeks Very 8 weeks - 12 weeks 27 P age
29 Ankle: without chronic instability RTW - Minimum/Maximum 0 days - 3 days Not anticipated 10 days - 3 weeks 10 days - 3 weeks 3 weeks - 6 weeks Very 3 weeks - 6 weeks Lower Extremities: Amputations Hip Disarticulation: RTW - Minimum/Maximum 3 months - 1 year 3 Months after satisfactory fitting of prosthesis Very Above Knee RTW - Minimum/Maximum 12 weeks - 30 weeks 3 Months after satisfactory fitting of prosthesis 12 weeks - 30 weeks Very 28 P age
30 Below Knee: RTW - Minimum/Maximum 12 weeks - 26 weeks 3 Months after satisfactory fitting of prosthesis Very 12 weeks - 26 weeks 18 weeks - 26 weeks 18 weeks - 26 weeks 18 weeks - 26 weeks Foot - Mid-Metatarsal Amputation: RTW - Minimum/Maximum 6 weeks - 8 weeks Expected 18 Months post-amputation Very 6 weeks - 8 weeks All Toes at Metatarsophalangeal Joint: RTW - Minimum/Maximum 4 weeks - 8 weeks Expected 18 Months post-amputation Very 8 weeks - 10 weeks 10 weeks - 14 weeks 29 P age
31 Great Toe: RTW - Minimum/Maximum 2 weeks - 4 weeks Expected 18 Months post-amputation Very 4 weeks - 5 weeks 6 weeks - 8 weeks Lesser Toe: single RTW - Minimum/Maximum 1 weeks - 2 weeks Expected 18 Months post-amputation Very 3 weeks - 4 weeks 4 weeks 4 weeks 4 weeks Lower Extremities: Surgical/Therapeutic/Diagnostic Procedures Meniscectomy: partial to total meniscal removal RTW - Minimum/Maximum 1 weeks - 2 weeks Possible 18 Months 2 weeks - 4 weeks 2 weeks - 4 weeks 4 weeks - 6 weeks Very 4 weeks - 6 weeks 30 P age
32 Meniscal Repair: suture repair of meniscal tear (combined arthroscopy and arthrotomy) RTW - Minimum/Maximum 2 weeks - 3 weeks Possible 18 Months 6 weeks - 8 weeks 8 weeks - 12 weeks 12 weeks - 24 weeks Very 12 weeks - 24 weeks Lateral Retinacular Release: recurrent patellar dislocation RTW - Minimum/Maximum 3 days - 1 weeks Not anticipated 2 weeks - 3 weeks 2 weeks - 3 weeks 2 weeks - 3 weeks Very based on primary injury Patellectomy: RTW - Minimum/Maximum 2 weeks - 4 weeks Expected 24 Months post-surgery Very 2 weeks - 6 weeks 3 weeks - 8 weeks 6 weeks or 6 weeks or Anterior Cruciate Ligament (ACL) Reconstruction/Replacement: RTW - Minimum/Maximum 3 weeks - 6 weeks Possible 24 Months post-surgery Very 4 weeks - 12 weeks 12 weeks - 24 weeks 31 P age
33 Return to very heavy repetitive work may take 9-12 months. Functional brace may/will be required for heavy and very heavy work and for medium work on uneven terrain and/or rotational activity. Ankle Ligament Reconstruction (Evans Repair): RTW - Minimum/Maximum 2 weeks - 4 weeks Possible 24 Months postsurgery Very 6 weeks - 8 weeks 8 weeks - 12 weeks 8 weeks - 14 weeks 12 weeks - 16 weeks Hip Replacement: RTW - Minimum/Maximum 3 weeks - 6 weeks Expected 24 Months post-surgery Very 4 weeks - 6 weeks 4 weeks - 6 weeks Osteotomy of Tibia: requires Medical Advisor review RTW - Minimum/Maximum 4 weeks - 6 weeks PCI based on knee joint status in 24 months Very 6 weeks - 8 weeks 8 weeks - 12 weeks 12 weeks - 24 weeks 12 weeks - 24 weeks 32 P age
34 Arthroplasty of Knee / Total Knee Replacement: RTW - Minimum/Maximum 4 weeks - 6 weeks Expected 24 Months post-surgery Very 12 weeks - 16 weeks 12 weeks - 20 weeks Ankle Fusion: RTW - Minimum/Maximum 4 weeks - 6 weeks Expected 18 Months post-surgery Very 12 weeks - 16 weeks 12 weeks - 16 weeks Achilles Tendon Rupture: for surgical and nonsurgical intervention RTW - Minimum/Maximum 2 weeks - 4 weeks Possible 24 Months 8 weeks - 10 weeks 10 weeks - 12 weeks 14 weeks - 16 weeks Very 14 weeks - 16 weeks Plantar Fasciitis: RTW - Minimum/Maximum 0 days - 1 week Not anticipated 2 weeks - 3 weeks 2 weeks - 3 weeks 2 weeks - 3 weeks Very 2 weeks - 3 weeks 33 P age
35 Head/Trunk/Spine Head/Trunk/Spine: Fractures Skull: Simple fracture Very Not anticipated Skull : Compound, comminuted or depressed fracture by Medical Advisor review (Brain injury assessed separately Maxilla: Very Not anticipated If job requires verbal communication, modified duties may be required. Minimum return-to-work 1 week for all levels. Mandible: For fracture management of jaw bone go to Head/Trunk/Spine Surgical/Therapeutic/Diagnostic Procedures section. 34 P age
36 Nose: Very Not anticipated with displaced fracture Possible (displaced fracture) 12 Months Ribs: Single or Multiple Very Not anticipated Sternum: Very Not anticipated Vertebrae: non-vertebral body: e.g. spinous process, transverse processes I. Single Level Fractures Very Not anticipated 35 P age
37 Vertebrae: non-vertebral body: e.g. spinous process, transverse processes II. Multiple Level Fractures Possible 24 Months post-injury Compression Fractures: vertebral bodies (Requires Medical Advisor review) Possible 24 Months Heavy /Very Head/Trunk/Spine: Dislocations/Subluxations Temporomandibular Joint(s): TMJ RTW - Minimum/Maximum 0 days - 1 week Not anticipated 0 days - 1 week 0 days - 1 week 0 days - 1 week Very 0 days - 1 week Spondylolysis, Spondylolisthesis: Medical Advisor referral necessary if layoff exceeds 3 weeks (otherwise see lumbosacral sprain) Head/Trunk/Spine: Soft Tissue Injuries: Sprains and Strains Temporomandibular Joint Disorders (TMJD): No time loss from work usually anticipated Not anticipated 36 P age
38 Cervical: e.g. Whiplash or non-whiplash soft tissue injuries without nerve root involvement RTW - Minimum/Maximum 0 weeks - 4 weeks Not anticipated Heavy /Very Heavy Work 0 weeks - 5 weeks 0 weeks - 6 weeks Medical Advisor opinion based on medical reporting if lay off exceeds 6 weeks Head/Trunk/Spine: Surgical/Therapeutic/Diagnostic Procedures Coccyx Disorder: Coccydynia following direct trauma RTW - Maximum/Minimum Medical Advisory opinion based on medical reporting if layoff exceeds 2 weeks Not anticipated Herniated Disc: Conservative medical treatment RTW - Maximum/Minimum 0 weeks - 4 weeks Expected - Medical Advisor review /recommendation at 24 Months postinjury Very Heavy 0 weeks - 4 weeks 4 weeks - 8 weeks Nerve Root and Plexus Disorders: including arachnoiditis/scarring RTW - Maximum/Minimum Medical Advisor opinion recommended when nerve root and plexus disorders first diagnosed on medical reporting Expected -Medical Advisor review/ recommendation at 24 Months postinjury 37 P age
39 Paralytic Syndrome: Post traumatic or post procedural RTW - Maximum/Minimum Medical Advisor opinion recommended when paralytic syndrome first diagnosed on medical reporting Expected - Medical Advisor review/ recommendation at 24 Months postinjury/surgery Spinal Cord Injury: RTW - Maximum/Minimum Medical Advisor opinion based on medical reporting Possible 24 Months postinjury Spinal Osteoarthritis: Degenerative joint disease, spondylosis - post traumatic or postsurgical Job Classification RTW - Maximum/Minimum Medical Advisor opinion recommended when Spinal Osteoarthritis first diagnosed on medical reporting Possible 24 Months postinjury/surgery Mandible: wired Very Heavy Not anticipated If job requires verbal communication, modified duties may be required. 38 P age
40 Repair of Vertebral Fracture: surgical instrumental e.g. rods, screws Expected 24 Months post-surgery Lysis of Adhesions of Spinal Cord and Nerve Roots: RTW - Minimum/Maximum Medical Advisory opinion based on medical reporting if layoff exceeds 12 weeks Expected at least 24 Months postsurgery Discectomy/Excision of Interverbal Disc: RTW - Minimum/Maximum 4 weeks - 6 weeks Expected 24 Months Postsurgery Heavy /Very Heavy Work 4 weeks - 6 weeks 6 weeks - 10 weeks Microdiscetomy: RTW - Minimum/Maximum 4 weeks - 6 weeks Expected 24 Months Postsurgery Heavy/Very Heavy Work 4 weeks - 6 weeks 6 weeks - 10 weeks 39 P age
41 Spinal Fusion: requires Medical Advisor referral: I Single Fusion RTW - Minimum/Maximum 12 weeks - 16 weeks Expected 24 months surgery Heavy\Very Heavy Work 14 weeks - 16 weeks 16 weeks - 24 weeks Spinal Fusion: requires Medical Advisor referral: II Multiple Levels RTW - Minimum/Maximum 16 weeks - 20 weeks Expected 24 Months Postsurgery Heavy\Very Heavy Work 22 weeks - 26 weeks 26 weeks - 32 weeks Hernia Surgery: inguinal and femoral RTW - Minimum/Maximum 2 weeks - 4 weeks Not anticipated 6 weeks - 8 weeks 6 weeks - 8 weeks 6 weeks - 8 weeks Very Heavy 6 weeks - 8 weeks 40 P age
42 Neurostimulator Implants: insertion RTW - Minimum/Maximum 0 weeks - 2 weeks For primary surgical procedure or condition Heavy/Very Heavy Work 0 weeks - 2 weeks 0 weeks - 2 weeks Coccygectomy: RTW - Minimum/Maximum 2 weeks - 4 weeks Not anticipated 3 weeks - 5 weeks 3 weeks - 5 weeks Heavy/Very Heavy Work 4 weeks - 6 weeks 41 P age
43 Appendix A Glossary of Terms Glossary of Terms Term endotrans- -ectomy -ology -lysis -plasty -rrhaphy -ostomy -otomy -itis -lysthesis -desis -osis diastasis duration of disability sprain strain Meaning Inside, within Across, through, over Excision Study of Breakdown Plastic repair/reconstruction/replacement To suture, sew Creation of an opening Incision into Inflammation Slippage Fusion Degeneration Separation beyond normal between associated bones Refers to the approximate time required to return the worker to pre-accident or modified work. It does not denote how long the worker should be away from work or when they should absolutely return to work. A sprain is an injury to the ligaments (bands of tough fibrous tissue) that bind bones together at a joint. Sprains result from overstretching of ligaments, usually due to twisting of a joint. A strain is an injury to a muscle or tendon (fibrous attachment of a muscle to a bone). Strains result from overstretching or overuse of a muscle. 42 P age
44 Appendix B Categorization of Muscle/Tendon Strains and Joint/Ligament Sprains Categorization of Muscle/Tendon Strains and Joint/Ligament Sprains Grades of Severity First Degree (mild) Second Degree (moderate) Third Degree (severe) Structural Damage Loss of Function Joint Stability (Sprains Only) Minimal - structure mostly intact Minimal - early resolution Minimal - No instability Partial tear; large spectrum of injury; few to most fibers torn Complete tear; rupture Significant early loss, especially when more fibers torn Severe/complete loss of function of involved structure Mild to moderate instability Significant instability 43 P age
Promoting Safe Workplaces... Protecting Employers and Workers. Disability Duration Guidelines and Expected Healing Times
 Promoting Safe Workplaces... Protecting Employers and Workers Disability Duration Guidelines and Expected Healing Times Volume 1 September, 2003 Disability Duration Guidelines Acknowledgement The Workers
Promoting Safe Workplaces... Protecting Employers and Workers Disability Duration Guidelines and Expected Healing Times Volume 1 September, 2003 Disability Duration Guidelines Acknowledgement The Workers
WorkSafeNB. Disability Duration Guidelines
 WorkSafeNB Edition: July 2009 NB Table of Contents Introduction and Use...Page 7 Disclaimer...Page 8 Acknowledgement...Page 8 s...page 8 Factors Influencing Disability Duration...Page 9 General Miscellaneous
WorkSafeNB Edition: July 2009 NB Table of Contents Introduction and Use...Page 7 Disclaimer...Page 8 Acknowledgement...Page 8 s...page 8 Factors Influencing Disability Duration...Page 9 General Miscellaneous
10/12/2010. Upper Extremity. Pectoral (Shoulder) Girdle. Clavicle (collarbone) Skeletal System: Appendicular Skeleton
 Skeletal System: Appendicular Skeleton Pectoral girdle Pelvic girdle Upper limbs Lower limbs 8-1 Pectoral (Shoulder) Girdle Consists of scapula and clavicle Clavicle articulates with sternum (Sternoclavicular
Skeletal System: Appendicular Skeleton Pectoral girdle Pelvic girdle Upper limbs Lower limbs 8-1 Pectoral (Shoulder) Girdle Consists of scapula and clavicle Clavicle articulates with sternum (Sternoclavicular
DART Diagnosis and Related Treatments
 DART Diagnosis and Related Treatments The DART Tool allows a user to obtain Treatment recommendations based on the disorder/condition. These recommendations are provided by ACOEM (American College of Occupational
DART Diagnosis and Related Treatments The DART Tool allows a user to obtain Treatment recommendations based on the disorder/condition. These recommendations are provided by ACOEM (American College of Occupational
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abscess, epidural, 822 824 Achilles tendon rupture, 894 895, 981 982 Acromioclavicular separations, shoulder pain in, 751 753 Adhesive capsulitis,
Note: Page numbers of article titles are in boldface type. A Abscess, epidural, 822 824 Achilles tendon rupture, 894 895, 981 982 Acromioclavicular separations, shoulder pain in, 751 753 Adhesive capsulitis,
Trauma & Orthopaedic Undergraduate Syllabus
 Trauma & Orthopaedic Undergraduate Syllabus Introduction The purpose of this document is to provide a recommended syllabus for medical students in Trauma & Orthopaedics (T&0). It should help students on
Trauma & Orthopaedic Undergraduate Syllabus Introduction The purpose of this document is to provide a recommended syllabus for medical students in Trauma & Orthopaedics (T&0). It should help students on
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Pectoral (Shoulder) Girdle
 Chapter 8 Skeletal System: Appendicular Skeleton Pectoral girdle Pelvic girdle Upper limbs Lower limbs 8-1 Pectoral (Shoulder) Girdle Consists of scapula and clavicle Clavicle articulates with sternum
Chapter 8 Skeletal System: Appendicular Skeleton Pectoral girdle Pelvic girdle Upper limbs Lower limbs 8-1 Pectoral (Shoulder) Girdle Consists of scapula and clavicle Clavicle articulates with sternum
Musculoskeletal System
 Musculoskeletal System CPT CPT copyright 2011 American Medical Association. All rights reserved. Fee schedules, relative value units, conversion factors and/or related components are not assigned by the
Musculoskeletal System CPT CPT copyright 2011 American Medical Association. All rights reserved. Fee schedules, relative value units, conversion factors and/or related components are not assigned by the
Musculoskeletal and Orthopaedic Conditions Treated
 General category Sub-categories Often used diagnosis/common terms Muscle and tendon pain and injuries Strains, tears/ruptures, contusions, lacerations, muscle pain, myofascial pain Tendinopathy, tendinitis,
General category Sub-categories Often used diagnosis/common terms Muscle and tendon pain and injuries Strains, tears/ruptures, contusions, lacerations, muscle pain, myofascial pain Tendinopathy, tendinitis,
NHS Training for Physiotherapy Support Workers. Workbook 11 The articular system
 NHS Training for Physiotherapy Support Workers Workbook 11 The articular system Contents Workbook 11 The articular system 1 11.1 Aim 3 11.2 Learning outcomes 3 11.3 The articular system 4 11.4 Individual
NHS Training for Physiotherapy Support Workers Workbook 11 The articular system Contents Workbook 11 The articular system 1 11.1 Aim 3 11.2 Learning outcomes 3 11.3 The articular system 4 11.4 Individual
MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM. What Are Musculoskeletal Disorders
 MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM What Are Musculoskeletal Disorders Every year more than 1.8 million workers in the United States suffer painful back and repetitive strain injuries,
MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM What Are Musculoskeletal Disorders Every year more than 1.8 million workers in the United States suffer painful back and repetitive strain injuries,
Anatomy of the Musculoskeletal System
 Anatomy of the Musculoskeletal System Kyle E. Rarey, Ph.D. Department of Anatomy & Cell Biology and Otolaryngology University of Florida College of Medicine Outline of Presentation Vertebral Column Upper
Anatomy of the Musculoskeletal System Kyle E. Rarey, Ph.D. Department of Anatomy & Cell Biology and Otolaryngology University of Florida College of Medicine Outline of Presentation Vertebral Column Upper
Chapter 8B. The Skeletal System: Appendicular Skeleton. The Appendicular Skeleton. Clavicle. Pectoral (Shoulder) Girdle
 The Appendicular Skeleton Chapter 8B The Skeletal System: Appendicular Skeleton 126 bones Pectoral (shoulder) girdle Pelvic (hip) girdle Upper limbs Lower limbs Functions primarily to facilitate movement
The Appendicular Skeleton Chapter 8B The Skeletal System: Appendicular Skeleton 126 bones Pectoral (shoulder) girdle Pelvic (hip) girdle Upper limbs Lower limbs Functions primarily to facilitate movement
Table of Compensation for Injury 1/2015
 Table of Compensation for 1/2015 Valid from 01.04.2015 1. CRANIAL INJURIES 1.1 Cranial bone fractures: a) fracture of cranial dome 10 b) fracture of cranial base 15 c) fracture of cranial dome and base
Table of Compensation for 1/2015 Valid from 01.04.2015 1. CRANIAL INJURIES 1.1 Cranial bone fractures: a) fracture of cranial dome 10 b) fracture of cranial base 15 c) fracture of cranial dome and base
Bone Composition. Bone is very strong for its relatively light weight The major components of bone are:
 Human Bones Bone Composition Bone is very strong for its relatively light weight The major components of bone are: Calcium carbonate Calcium phosphate Collagen Water Cortical Bone Spongy Bone Medullary
Human Bones Bone Composition Bone is very strong for its relatively light weight The major components of bone are: Calcium carbonate Calcium phosphate Collagen Water Cortical Bone Spongy Bone Medullary
36.3 The Integumentary System The Skin. KEY CONCEPT The integumentary system has many tissues that protect the body.
 36.3 The Integumentary System The Skin KEY CONCEPT The integumentary system has many tissues that protect the body. 36.3 The Integumentary System The Skin The integument is the body system that surrounds
36.3 The Integumentary System The Skin KEY CONCEPT The integumentary system has many tissues that protect the body. 36.3 The Integumentary System The Skin The integument is the body system that surrounds
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Adductor strain, 625 Agility-training lateral hurdles, 689 Ankle sprain, and lateral ligament reconstruction, complications of, 704 705
Index Note: Page numbers of article titles are in boldface type. A Adductor strain, 625 Agility-training lateral hurdles, 689 Ankle sprain, and lateral ligament reconstruction, complications of, 704 705
Dr.Israa H. Mohsen. Lecture 5. The vertebral column
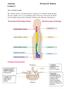 Anatomy Lecture 5 Dr.Israa H. Mohsen The vertebral column The vertebral column a flexible structure consisting of 33 vertebrae holds the head and torso upright, serves as an attachment point for the legs,
Anatomy Lecture 5 Dr.Israa H. Mohsen The vertebral column The vertebral column a flexible structure consisting of 33 vertebrae holds the head and torso upright, serves as an attachment point for the legs,
Human Anatomy, First Edition McKinley & O'Loughlin
 Human Anatomy, First Edition McKinley & O'Loughlin Chapter 8 : Appendicular Skeleton 8-1 Appendicular Skeleton Includes the bones of the upper and lower limbs. The girdles of bones that attach the upper
Human Anatomy, First Edition McKinley & O'Loughlin Chapter 8 : Appendicular Skeleton 8-1 Appendicular Skeleton Includes the bones of the upper and lower limbs. The girdles of bones that attach the upper
The Skeletal System THE APPENDICULAR SKELETON
 The Skeletal System THE APPENDICULAR SKELETON The appendicular skeleton consists of the girdles and the skeleton of the limbs. The upper (anterior) limbs are attached to the pectoral (shoulder) girdle
The Skeletal System THE APPENDICULAR SKELETON The appendicular skeleton consists of the girdles and the skeleton of the limbs. The upper (anterior) limbs are attached to the pectoral (shoulder) girdle
Chiropractic ICD-10 Common Codes List
 Chiropractic ICD-10 Common Codes List This is a preliminary list of Common ICD-10 Codes for chiropractic diagnoses. This is a common code list to be used as a guide for coding and is not intended to represent
Chiropractic ICD-10 Common Codes List This is a preliminary list of Common ICD-10 Codes for chiropractic diagnoses. This is a common code list to be used as a guide for coding and is not intended to represent
Post test for O&P 2 Hrs CE. The Exam
 Post test for O&P 2 Hrs CE The Exam This examination is taken in "open book" format. That means you are free to answer the questions after research or discussion with your fellow workers. We feel this
Post test for O&P 2 Hrs CE The Exam This examination is taken in "open book" format. That means you are free to answer the questions after research or discussion with your fellow workers. We feel this
COURSE OUTLINE-IB 128: SPORTS MEDICINE INTRODUCTION
 COURSE OUTLINE-IB 128: SPORTS MEDICINE INTRODUCTION Definition of sports medicine Pre-participation physical exam Epidemiology of sports injuries injury rates for various sports sports risks relative to
COURSE OUTLINE-IB 128: SPORTS MEDICINE INTRODUCTION Definition of sports medicine Pre-participation physical exam Epidemiology of sports injuries injury rates for various sports sports risks relative to
Contents SECTION 1: GENERAL TRAUMA AND RECONSTRUCTIVE HIP SURGERY
 SECTION 1: GENERAL TRAUMA AND RECONSTRUCTIVE HIP SURGERY 1. Acetabular and Pelvic Fractures...3 2. Acetabular Orientation (Total Hips)...6 3. Acetabular Osteotomy...7 4. Achilles Tendon Ruptures...9 5.
SECTION 1: GENERAL TRAUMA AND RECONSTRUCTIVE HIP SURGERY 1. Acetabular and Pelvic Fractures...3 2. Acetabular Orientation (Total Hips)...6 3. Acetabular Osteotomy...7 4. Achilles Tendon Ruptures...9 5.
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Achilles tendonitis, criteria for full competition in, 164 165 description of, 164 patient education in, 165 prophylactic support in,
Index Note: Page numbers of article titles are in boldface type. A Achilles tendonitis, criteria for full competition in, 164 165 description of, 164 patient education in, 165 prophylactic support in,
Phase II Health Sciences as Applied to Coaching.
 Phase II Health Sciences as Applied to Coaching www.topform.us Overview What is going to be covered today is.. Skeletal System Muscular System Most common injuries to know about in your sport Part One:
Phase II Health Sciences as Applied to Coaching www.topform.us Overview What is going to be covered today is.. Skeletal System Muscular System Most common injuries to know about in your sport Part One:
Exercise Science Section 4: Joint Mechanics and Joint Injuries
 Exercise Science Section 4: Joint Mechanics and Joint Injuries An Introduction to Health and Physical Education Ted Temertzoglou Paul Challen ISBN 1-55077-132-9 Types of Joints Fibrous joint Cartilaginous
Exercise Science Section 4: Joint Mechanics and Joint Injuries An Introduction to Health and Physical Education Ted Temertzoglou Paul Challen ISBN 1-55077-132-9 Types of Joints Fibrous joint Cartilaginous
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
11/25/2012. Chapter 7 Part 2: Bones! Skeletal Organization. The Skull. Skull Bones to Know Cranium
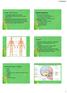 Chapter 7 Part 2: Bones! 5) Distinguish between the axial and appendicular skeletons and name the major parts of each 6) Locate and identify the bones and the major features of the bones that compose the
Chapter 7 Part 2: Bones! 5) Distinguish between the axial and appendicular skeletons and name the major parts of each 6) Locate and identify the bones and the major features of the bones that compose the
The scapula is located on the back side of the ribcage and helps provide part of the shoulder joint and movement for the arms.
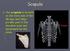 The scapula is located on the back side of the ribcage and helps provide part of the shoulder joint and movement for the arms. Scapula Humerus (Upper Arm Bone) Radius and Ulna Radius on Top Ulna on Bottom
The scapula is located on the back side of the ribcage and helps provide part of the shoulder joint and movement for the arms. Scapula Humerus (Upper Arm Bone) Radius and Ulna Radius on Top Ulna on Bottom
CLINICAL CONCEPTS FOR ORTHOPEDICS. CMS Clinical Concepts
 CLINICAL CONCEPTS FOR ORTHOPEDICS CMS Clinical Concepts ICD 10 LESSONS FROM OFFICE DOCUMENTATION Presented by Dr. Frankeny OUR CHALLENGE: CHANGING OUR DOCUMENTATION ICD 10 Learn the nomenclature Documenting
CLINICAL CONCEPTS FOR ORTHOPEDICS CMS Clinical Concepts ICD 10 LESSONS FROM OFFICE DOCUMENTATION Presented by Dr. Frankeny OUR CHALLENGE: CHANGING OUR DOCUMENTATION ICD 10 Learn the nomenclature Documenting
Country Health SA Medical Imaging
 Country Health SA Medical Imaging REMOTE OPERATORS POSITIONING GUIDE Contents Image Evaluation Page 4 Positioning Guides Section 1 - THORAX 1.1 Chest Page 5 1.2 Bedside Chest Page 7 1.3 Ribs Page 8 Section
Country Health SA Medical Imaging REMOTE OPERATORS POSITIONING GUIDE Contents Image Evaluation Page 4 Positioning Guides Section 1 - THORAX 1.1 Chest Page 5 1.2 Bedside Chest Page 7 1.3 Ribs Page 8 Section
Radiographic Positioning Summary (Basic Projections RAD 222)
 Lower Extremity Radiographic Positioning Summary (Basic Projections RAD 222) AP Pelvis AP Hip (Unilateral) (L or R) AP Femur Mid and distal AP Knee Lateral Knee Pt lies supine on table Align MSP to Center
Lower Extremity Radiographic Positioning Summary (Basic Projections RAD 222) AP Pelvis AP Hip (Unilateral) (L or R) AP Femur Mid and distal AP Knee Lateral Knee Pt lies supine on table Align MSP to Center
AMERICAN RED CROSS FIRST AID RESPONDING TO EMERGENCIES FOURTH EDITION Copyright 2006 by The American National Red Cross All rights reserved.
 Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
The Shoulder Complex. Anatomy. Articulations 12/11/2017. Oak Ridge High School Conroe, Texas. Clavicle Collar Bone Scapula Shoulder Blade Humerus
 The Shoulder Complex Oak Ridge High School Conroe, Texas Anatomy Clavicle Collar Bone Scapula Shoulder Blade Humerus Articulations Sternoclavicular SC joint. Sternum and Clavicle. Acromioclavicular AC
The Shoulder Complex Oak Ridge High School Conroe, Texas Anatomy Clavicle Collar Bone Scapula Shoulder Blade Humerus Articulations Sternoclavicular SC joint. Sternum and Clavicle. Acromioclavicular AC
Important Parts of Bones
 Important Parts of Bones For 2015 Know: Humerus (posterior) Clavical Femur (Anterior) Foot Hand Mandible Os Coxa Scapula Skull (Anterior, Inferior, Lateral) Sternum Humerus (posterior) A. olecranon fossa
Important Parts of Bones For 2015 Know: Humerus (posterior) Clavical Femur (Anterior) Foot Hand Mandible Os Coxa Scapula Skull (Anterior, Inferior, Lateral) Sternum Humerus (posterior) A. olecranon fossa
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatry. Procedure List. As Of. 01 April Government of Alberta
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
The Appendicular Skeleton
 8 The Appendicular Skeleton PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris 8-1 The Pectoral Girdle The Pectoral Girdle Also called shoulder girdle Connects the
8 The Appendicular Skeleton PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris 8-1 The Pectoral Girdle The Pectoral Girdle Also called shoulder girdle Connects the
The Skeletal System in Action!! The Skeletal System in Action!
 Skeletal System The Skeletal System in Action!! The Skeletal System in Action! 5 Functions of the Skeletal System 1. Movement: Skeletal system provides points of attachment for muscles. Your legs and arms
Skeletal System The Skeletal System in Action!! The Skeletal System in Action! 5 Functions of the Skeletal System 1. Movement: Skeletal system provides points of attachment for muscles. Your legs and arms
TRAINING LAB SKELETAL REMAINS: IDENTIFYING BONES NAME
 TRAINING LAB SKELETAL REMAINS: IDENTIFYING BONES NAME Background: Skeletal remains are important pieces of evidence. The flesh, muscle, and organs of a victim rapidly decompose; however, the victim s skeleton
TRAINING LAB SKELETAL REMAINS: IDENTIFYING BONES NAME Background: Skeletal remains are important pieces of evidence. The flesh, muscle, and organs of a victim rapidly decompose; however, the victim s skeleton
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatric Surgery. Procedure List. As Of.
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2016 Alberta Health Care Insurance Plan Page i Generated 2016/03/22 TABLE OF CONTENTS As of 2016/04/01 07 PHYSICAL MEDICINE, REHABILITATION,
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2016 Alberta Health Care Insurance Plan Page i Generated 2016/03/22 TABLE OF CONTENTS As of 2016/04/01 07 PHYSICAL MEDICINE, REHABILITATION,
EPIPHYSEAL PLATE IN FEMUR
 Reviewing: Epiphyseal Plates (younger skeletons) eventually will disappear. Bones grow lengthwise up and down from each plate, and in a circular collar like fashion around the diaphysis. These plates will
Reviewing: Epiphyseal Plates (younger skeletons) eventually will disappear. Bones grow lengthwise up and down from each plate, and in a circular collar like fashion around the diaphysis. These plates will
Cluster - 26 ORTHOPEDICS. X Ray of Affected Limb, MIR of Shoulder
 Sr.No Package no 1708 26.1 Orthopeidc 1709 26.2 Orthopeidc Sub speciality Procedure name Pre-Operative Investigation AC joint reconstruction/ Stabilization/ Acromionplasty (Nonoperative management is recommended
Sr.No Package no 1708 26.1 Orthopeidc 1709 26.2 Orthopeidc Sub speciality Procedure name Pre-Operative Investigation AC joint reconstruction/ Stabilization/ Acromionplasty (Nonoperative management is recommended
Chapter 8 The Skeletal System: The Appendicular Skeleton. Copyright 2009 John Wiley & Sons, Inc.
 Chapter 8 The Skeletal System: The Appendicular Skeleton Appendicular Skeleton It includes bones of the upper and lower limbs Girdles attach the limbs to the axial skeleton The pectoral girdle consists
Chapter 8 The Skeletal System: The Appendicular Skeleton Appendicular Skeleton It includes bones of the upper and lower limbs Girdles attach the limbs to the axial skeleton The pectoral girdle consists
Human Anatomy - Problem Drill 06: The Skeletal System Axial Skeleton & Articualtions
 Human Anatomy - Problem Drill 06: The Skeletal System Axial Skeleton & Articualtions Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper
Human Anatomy - Problem Drill 06: The Skeletal System Axial Skeleton & Articualtions Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper
UPPER EXTREMITY INJURIES. Recognizing common injuries to the upper extremity
 UPPER EXTREMITY INJURIES Recognizing common injuries to the upper extremity ANATOMY BONES Clavicle Scapula Spine of the scapula Acromion process Glenoid fossa/cavity Humerus Epicondyles ANATOMY BONES Ulna
UPPER EXTREMITY INJURIES Recognizing common injuries to the upper extremity ANATOMY BONES Clavicle Scapula Spine of the scapula Acromion process Glenoid fossa/cavity Humerus Epicondyles ANATOMY BONES Ulna
Joints Dr. Ali Ebneshahidi
 Joints Dr. Ali Ebneshahidi Function of Joints 1. Serve as functional junctions between bones. 2. Bind bones, strokes, and other related tissues together. 3. Allow bone growth to occur. 4. Permit certain
Joints Dr. Ali Ebneshahidi Function of Joints 1. Serve as functional junctions between bones. 2. Bind bones, strokes, and other related tissues together. 3. Allow bone growth to occur. 4. Permit certain
PRESENTED BY: JOHN STIMLER, DO, CPC, CHC, FACEP BSA HEALTHCARE AND BSA HEALTHCARE ADVISORY GROUP
 PRESENTED BY: JOHN STIMLER, DO, CPC, CHC, FACEP BSA HEALTHCARE AND BSA HEALTHCARE ADVISORY GROUP TOPICS (1) Fracture types ICD-10-CM diagnostic coding CPT procedure coding Fracture care treatments: Manipulated
PRESENTED BY: JOHN STIMLER, DO, CPC, CHC, FACEP BSA HEALTHCARE AND BSA HEALTHCARE ADVISORY GROUP TOPICS (1) Fracture types ICD-10-CM diagnostic coding CPT procedure coding Fracture care treatments: Manipulated
NOTES SKELETAL SYSTEM
 NOTES for the SKELETAL SYSTEM Anatomy & Physiology 2016 Johnson The Skeletal System I. System includes 4 basic parts: A. Bones (206 of em) B. Joints C. Cartilages D. Ligaments II. Bones have 5 basic functions:
NOTES for the SKELETAL SYSTEM Anatomy & Physiology 2016 Johnson The Skeletal System I. System includes 4 basic parts: A. Bones (206 of em) B. Joints C. Cartilages D. Ligaments II. Bones have 5 basic functions:
Functions of Skeletal System
 Skeletal System Skeletal System Adult Human has 206 Bones This slideshow will offer fun ways to remember the names of some of the bones, and you can come up with your own tricks! Functions of Skeletal
Skeletal System Skeletal System Adult Human has 206 Bones This slideshow will offer fun ways to remember the names of some of the bones, and you can come up with your own tricks! Functions of Skeletal
LANGUAGE OF ANATOMY PART 1
 1 LANGUAGE OF ANATOMY PART 1 Courtesy of Dr. Susan Maskel Western Connecticut State University 2 ANATOMICAL POSITION In the anatomical position, the human body is erect, with the feet only slightly apart,
1 LANGUAGE OF ANATOMY PART 1 Courtesy of Dr. Susan Maskel Western Connecticut State University 2 ANATOMICAL POSITION In the anatomical position, the human body is erect, with the feet only slightly apart,
CASE ONE CASE ONE. RADIAL HEAD FRACTURE Mason Classification. RADIAL HEAD FRACTURE Mechanism of Injury. RADIAL HEAD FRACTURE Imaging
 CASE ONE An eighteen year old female falls during a basketball game, striking her elbow on the court. She presents to your office that day with a painful, swollen elbow that she is unable to flex or extend
CASE ONE An eighteen year old female falls during a basketball game, striking her elbow on the court. She presents to your office that day with a painful, swollen elbow that she is unable to flex or extend
The Lower Limb II. Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa
 The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination
 SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
New Authorization Requirements for Outpatient Physical, Occupational, and Speech Therapy (Eff. 1/1/18)
 New Authorization Requirements for Outpatient Physical, Occupational, and Speech Therapy (Eff. 1/1/18) Effective January 1, 2018, Martin s Point Health Care will require providers to submit initial and
New Authorization Requirements for Outpatient Physical, Occupational, and Speech Therapy (Eff. 1/1/18) Effective January 1, 2018, Martin s Point Health Care will require providers to submit initial and
Ch. 5 - Skeletal System
 Ch. 5 - Skeletal System Bones are living, ever-changing structures. This allows them grow and adapt to new situations that the body encounters. The functions of the skeletal system: 1) support bones are
Ch. 5 - Skeletal System Bones are living, ever-changing structures. This allows them grow and adapt to new situations that the body encounters. The functions of the skeletal system: 1) support bones are
Contents. copyrighted material by PRO-ED, Inc. Chapter 1. Chapter 2. Chapter 3. Chapter 4. Chapter 5. Conditions in Athletic Injuries
 Acknowledgments xiii Introduction to the First Edition xv Introduction to the Second Edition xvii Chapter 1 Conditions in Athletic Injuries Anterior Cruciate Ligament (ACL) Tear 2 Biceps Tendon Strain
Acknowledgments xiii Introduction to the First Edition xv Introduction to the Second Edition xvii Chapter 1 Conditions in Athletic Injuries Anterior Cruciate Ligament (ACL) Tear 2 Biceps Tendon Strain
Exercise 11. The Appendicular Skeleton
 Exercise 11 The Appendicular Skeleton The Appendicular Skeleton The appendicular skeleton contains 126 bones. Consists of the upper and lower limbs, the pectoral girdles, and the pelvic girdles. The pectoral
Exercise 11 The Appendicular Skeleton The Appendicular Skeleton The appendicular skeleton contains 126 bones. Consists of the upper and lower limbs, the pectoral girdles, and the pelvic girdles. The pectoral
The skeletal system is the framework for the muscular system to attach to so we can move.
 Skeletal System The skeletal system is the framework for the muscular system to attach to so we can move. BONE: A rigid connective tissue Helps to move & support the body Protect the organs (skull, ribs)
Skeletal System The skeletal system is the framework for the muscular system to attach to so we can move. BONE: A rigid connective tissue Helps to move & support the body Protect the organs (skull, ribs)
Dupuytrens contracture
 OA Wrist Ganglion/Cysts Dupuytrens contracture Carpal Tunnel Syndrome Carpal Tunnel pathway For advice on management of CTS please follow link to Map of Medicine Trigger Finger Trigger finger pathway For
OA Wrist Ganglion/Cysts Dupuytrens contracture Carpal Tunnel Syndrome Carpal Tunnel pathway For advice on management of CTS please follow link to Map of Medicine Trigger Finger Trigger finger pathway For
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acetabular fractures, 462 464 Achilles tendon rupture, 389 Acromioclavicular dislocations, 302 Acromion fractures, 301 Ankle, anatomy of, 376
Note: Page numbers of article titles are in boldface type. A Acetabular fractures, 462 464 Achilles tendon rupture, 389 Acromioclavicular dislocations, 302 Acromion fractures, 301 Ankle, anatomy of, 376
Guide to Prevention of Sports Injuries
 Guide to Prevention of Sports Injuries Maintaining an active lifestyle offers a number of benefits for your physical and mental health. While exercise and sports-related activities often have a positive
Guide to Prevention of Sports Injuries Maintaining an active lifestyle offers a number of benefits for your physical and mental health. While exercise and sports-related activities often have a positive
SKELETAL STRUCTURES Objectives for Exam #1: Objective for Portfolio #1: Part I: Skeletal Stations Station A: Bones of the Body
 SKELETAL STRUCTURES Objectives for Exam #1: 1. Provide information on the various structures and functions of the skeletal system. 2. Describe various skeletal system disorders, including imaging techniques
SKELETAL STRUCTURES Objectives for Exam #1: 1. Provide information on the various structures and functions of the skeletal system. 2. Describe various skeletal system disorders, including imaging techniques
Surgery-Ortho. Fractures of the tibia and fibula. Management. Treatment of low energy fractures. Fifth stage. Lec-6 د.
 Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
A. Incorrect! The appendicular skeleton includes bones of the shoulder, arm, hand, pelvis, leg and foot.
 Anatomy and Physiology - Problem Drill 08: The Skeletal System III No. 1 of 10 1. Which of the following statements about the appendicular skeleton is correct? A. The appendicular skeleton includes bones
Anatomy and Physiology - Problem Drill 08: The Skeletal System III No. 1 of 10 1. Which of the following statements about the appendicular skeleton is correct? A. The appendicular skeleton includes bones
Skeletal System Practice Quiz and Exercises ANSWERS
 Skeletal System Practice Quiz and Exercises ANSWERS 1) Give the meaning of the following terms (4 marks) a) Prone b) Medial c) Posterior d) Ipsilateral a) Lying face down b) Nearer the midline c) Nearer
Skeletal System Practice Quiz and Exercises ANSWERS 1) Give the meaning of the following terms (4 marks) a) Prone b) Medial c) Posterior d) Ipsilateral a) Lying face down b) Nearer the midline c) Nearer
Anatomy. Anatomy deals with the structure of the human body, and includes a precise language on body positions and relationships between body parts.
 Anatomy deals with the structure of the human body, and includes a precise language on body positions and relationships between body parts. Proper instruction on safe and efficient exercise technique requires
Anatomy deals with the structure of the human body, and includes a precise language on body positions and relationships between body parts. Proper instruction on safe and efficient exercise technique requires
The Skeletal System. Support Systems Unit 2
 The Skeletal System Support Systems Unit 2 Vocabulary- combining forms Arthr/o joint Sacr/o Sacrum Cervic/o neck Spondyl/o vertebrae Chondr/o cartilage Stern/o Sternum Cost/o rib Ten/o, Tend/o, Tendon
The Skeletal System Support Systems Unit 2 Vocabulary- combining forms Arthr/o joint Sacr/o Sacrum Cervic/o neck Spondyl/o vertebrae Chondr/o cartilage Stern/o Sternum Cost/o rib Ten/o, Tend/o, Tendon
Human Anatomy Laboratory Manual with Cat Dissections Marieb Mitchell Smith Seventh Edition
 Human Anatomy Laboratory Manual with Cat Dissections Marieb Mitchell Smith Seventh Edition Pearson Education Limited Edinburgh Gate Harlow Essex CM20 2JE England and Associated Companies throughout the
Human Anatomy Laboratory Manual with Cat Dissections Marieb Mitchell Smith Seventh Edition Pearson Education Limited Edinburgh Gate Harlow Essex CM20 2JE England and Associated Companies throughout the
Chapter 5 The Skeletal System
 Chapter 5 The Skeletal System The Skeletal System Parts of the skeletal system Bones (skeleton) Joints Cartilages Ligaments (bone to bone)(tendon=bone to muscle) Divided into two divisions Axial skeleton:
Chapter 5 The Skeletal System The Skeletal System Parts of the skeletal system Bones (skeleton) Joints Cartilages Ligaments (bone to bone)(tendon=bone to muscle) Divided into two divisions Axial skeleton:
CHAPTER 7, PART II (BONES)
 Anatomy Name: CHAPTER 7, PART II (BONES) Entry #: INSTRUCTIONS: 1) READ Chapter 7, pg. 140-161. 2) Using the outline, make a note card for each underlined bone name or phrase. 3) On each note card, put
Anatomy Name: CHAPTER 7, PART II (BONES) Entry #: INSTRUCTIONS: 1) READ Chapter 7, pg. 140-161. 2) Using the outline, make a note card for each underlined bone name or phrase. 3) On each note card, put
ASPEN MEDICAL SURGERY REGINA
 It is hereby certified that ASPEN MEDICAL SURGERY REGINA Has successfully completed an inspection as is required under the College s Bylaw 26.1 and is therefore approved as a Non Hospital Treatment Facility
It is hereby certified that ASPEN MEDICAL SURGERY REGINA Has successfully completed an inspection as is required under the College s Bylaw 26.1 and is therefore approved as a Non Hospital Treatment Facility
8 Recovering From HAND FRACTURE SURGERY
 8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
Human Skeletal System Glossary
 Acromegaly Apatite Acromegaly - is a condition which involves excessive growth of the jaw, hands, and feet. It results from overproduction of somatotropin in adults (after fusion of the ossification centres
Acromegaly Apatite Acromegaly - is a condition which involves excessive growth of the jaw, hands, and feet. It results from overproduction of somatotropin in adults (after fusion of the ossification centres
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 8 The Skeletal System: The Appendicular Skeleton The Appendicular Skeleton The 126 bones of the appendicular skeleton are primarily concerned
Principles of Anatomy and Physiology 14 th Edition CHAPTER 8 The Skeletal System: The Appendicular Skeleton The Appendicular Skeleton The 126 bones of the appendicular skeleton are primarily concerned
Lab Exercise #04 The Skeletal System Student Performance Objectives
 Lab Exercise #04 The Skeletal System Student Performance Objectives The material that you are required to learn in this exercise can be found in either the lecture text or the supplemental materials provided
Lab Exercise #04 The Skeletal System Student Performance Objectives The material that you are required to learn in this exercise can be found in either the lecture text or the supplemental materials provided
Bones of Thorax (Rib Cage)
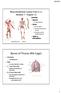 Musculoskeletal System (Part A-2) Module 7 -Chapter 10 Overview Muscles Attachments Bones Bone types Surface features of bones Divisions of the skeletal system Joints or Articulations Susie Turner, M.D.
Musculoskeletal System (Part A-2) Module 7 -Chapter 10 Overview Muscles Attachments Bones Bone types Surface features of bones Divisions of the skeletal system Joints or Articulations Susie Turner, M.D.
Bone Flashcards for 10a
 Bone Flashcards for 0a CLAVICLE (collar bone). Sternal extremity (end) flat end. Acromial extremity (end) rounded end. SCAPULA (shoulder blade). Right or left scapula?. Superior border (superior margin).
Bone Flashcards for 0a CLAVICLE (collar bone). Sternal extremity (end) flat end. Acromial extremity (end) rounded end. SCAPULA (shoulder blade). Right or left scapula?. Superior border (superior margin).
Anatomy & Physiology Skeletal System Worksheet
 1. Name the five functions of the skeleton. c) d) e) Anatomy & Physiology Skeletal System Worksheet 2. The term for the shaft of a bone is:. 3. The bony struts found in spongy bone are called. 4. In ossification,
1. Name the five functions of the skeleton. c) d) e) Anatomy & Physiology Skeletal System Worksheet 2. The term for the shaft of a bone is:. 3. The bony struts found in spongy bone are called. 4. In ossification,
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles. Striated Skeletal. Smooth
 1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
Lab-1. Miss. Lina Al-Onazy & samar Al-Wgeet =)
 Lab-1 Introduction The human skeleton is composed of 300 bones at birth and by the time adulthood is reached, some bones have fused together to give a total of 206 bones in the body. The human skeleton
Lab-1 Introduction The human skeleton is composed of 300 bones at birth and by the time adulthood is reached, some bones have fused together to give a total of 206 bones in the body. The human skeleton
CHAPTER 8 LECTURE OUTLINE
 CHAPTER 8 LECTURE OUTLINE I. INTRODUCTION A. The appendicular skeleton includes the bones of the upper and lower extremities and the shoulder and hip girdles. B. The appendicular skeleton functions primarily
CHAPTER 8 LECTURE OUTLINE I. INTRODUCTION A. The appendicular skeleton includes the bones of the upper and lower extremities and the shoulder and hip girdles. B. The appendicular skeleton functions primarily
Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles
 1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
TOP RYDE CHIROPRACTIC
 1. Ankle Pain Conditions Helped by Chiropractic The ankle joint is made up of ligaments, tendons, nerves, and a disc to cushion motion. Distortions of motion of the ankle can strain the ligaments and muscles
1. Ankle Pain Conditions Helped by Chiropractic The ankle joint is made up of ligaments, tendons, nerves, and a disc to cushion motion. Distortions of motion of the ankle can strain the ligaments and muscles
Adult Reconstruction Hip Education Tracks
 Adult Reconstruction Hip Education Tracks Adult Reconstruction Hip Track for the Specialist - HIP1 ICL 281 A Case-based Approach to High Risk Total Hip - When Do I Do Something Differently? ICL 241 The
Adult Reconstruction Hip Education Tracks Adult Reconstruction Hip Track for the Specialist - HIP1 ICL 281 A Case-based Approach to High Risk Total Hip - When Do I Do Something Differently? ICL 241 The
ERI Safety Videos Videos for Safety Meetings. ERGONOMICS EMPLOYEE TRAINING: Preventing Musculoskeletal Disorders. Leader s Guide 2001, ERI PRODUCTIONS
 ERI Safety Videos Videos for Safety Meetings 2120 ERGONOMICS EMPLOYEE TRAINING: Preventing Musculoskeletal Disorders Leader s Guide 2001, ERI PRODUCTIONS ERGONOMICS EMPLOYEE TRAINING: Preventing Musculoskeletal
ERI Safety Videos Videos for Safety Meetings 2120 ERGONOMICS EMPLOYEE TRAINING: Preventing Musculoskeletal Disorders Leader s Guide 2001, ERI PRODUCTIONS ERGONOMICS EMPLOYEE TRAINING: Preventing Musculoskeletal
/ ~ HAND.AND WRIST:. Carpal Tunnel Syndrome (354.0).ORTHO-6 Ganglion (727.4).ORTIfO-7 JOINTS Joint Replacement, Prosthesis (81)...
 ORTHOPEDICS. :::::./ J. ) / MUSCULOSKELETAL, ARTHRITIS AND RELATED DISORDERS TABLE OF CONTENTS I. LETTER II. CONDITIONS " II.A GENERAL CONDITIONS............................................. ORTHO-1 II.S
ORTHOPEDICS. :::::./ J. ) / MUSCULOSKELETAL, ARTHRITIS AND RELATED DISORDERS TABLE OF CONTENTS I. LETTER II. CONDITIONS " II.A GENERAL CONDITIONS............................................. ORTHO-1 II.S
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Achilles tendinopathy in dancers, 831 832 treatment of PRP in, 871 872 Achilles tendinopathy/tendonitis in ultramarathon athletes, 847
Index Note: Page numbers of article titles are in boldface type. A Achilles tendinopathy in dancers, 831 832 treatment of PRP in, 871 872 Achilles tendinopathy/tendonitis in ultramarathon athletes, 847
Montreal Children s Hospital McGill University Health Center Emergency Department Fracture Guideline
 Montreal Children s Hospital McGill University Health Center Emergency Department Guideline Disclaimers This document is designed to assist physicians working in our emergency department in caring for
Montreal Children s Hospital McGill University Health Center Emergency Department Guideline Disclaimers This document is designed to assist physicians working in our emergency department in caring for
QUICK ASSESSMENT: CONCEPT MAP
 FUNCTIONS OF THE SKELETAL SYSTEM 7th Grade THE SKELETAL SYSTEM Provides shape, strength, and support (3S s) Internal framework of the body Support and anchor for soft organs Protects soft internal organs
FUNCTIONS OF THE SKELETAL SYSTEM 7th Grade THE SKELETAL SYSTEM Provides shape, strength, and support (3S s) Internal framework of the body Support and anchor for soft organs Protects soft internal organs
Biology 218 Human Anatomy
 Chapter 8 Adapted from Tortora 10 th ed. LECTURE OUTLINE A. Introduction (p. 203) 1. The appendicular skeleton contains 126 bones that form: i. two pectoral (shoulder) girdles two upper limbs i one pelvic
Chapter 8 Adapted from Tortora 10 th ed. LECTURE OUTLINE A. Introduction (p. 203) 1. The appendicular skeleton contains 126 bones that form: i. two pectoral (shoulder) girdles two upper limbs i one pelvic
For more information call , or visit
 Target Coding ICD-10 List for Chiropractic HEADACHE G43: Migraine G43.0: Migraine without aura (common migraine) G43.009: Migraine without aura, not intractable, without status migrainosus (migraine without
Target Coding ICD-10 List for Chiropractic HEADACHE G43: Migraine G43.0: Migraine without aura (common migraine) G43.009: Migraine without aura, not intractable, without status migrainosus (migraine without
The Musculoskeletal System
 The Musculoskeletal System Introduction The skeletal system and muscular system are often considered together because they are close in terms of structure and function. The two systems are referred to
The Musculoskeletal System Introduction The skeletal system and muscular system are often considered together because they are close in terms of structure and function. The two systems are referred to
Anatomy and Physiology 2016
 Anatomy and Physiology 2016 O = Temporal line I = coronoid process (Mandible) A = elevates mandible (chewing) O = galea aponeurotica (layer of dense fibrous tissue which covers the upper part of the cranium)
Anatomy and Physiology 2016 O = Temporal line I = coronoid process (Mandible) A = elevates mandible (chewing) O = galea aponeurotica (layer of dense fibrous tissue which covers the upper part of the cranium)
PowerPoint Lecture Slides. Prepared by Patty Bostwick-Taylor, Florence-Darlington Technical College. The Skeletal System Pearson Education, Inc.
 PowerPoint Lecture Slides Prepared by Patty Bostwick-Taylor, Florence-Darlington Technical College CHAPTER 5 The Skeletal System 2012 Pearson Education, Inc. Title Classification of Bones and Gross Anatomy
PowerPoint Lecture Slides Prepared by Patty Bostwick-Taylor, Florence-Darlington Technical College CHAPTER 5 The Skeletal System 2012 Pearson Education, Inc. Title Classification of Bones and Gross Anatomy
Amy Warenda Czura, Ph.D. 1 SCCC BIO130 Lab 7 Appendicular Skeleton & Articulations
 The Skeletal System II: Appendicular Skeleton and Articulations Exercises 11, 13 (begins: page 145 in 9 th and 10 th editions) Exercises 10, 11 (begins: page 147 in 11 th edition, page 149 in 12 th edition)
The Skeletal System II: Appendicular Skeleton and Articulations Exercises 11, 13 (begins: page 145 in 9 th and 10 th editions) Exercises 10, 11 (begins: page 147 in 11 th edition, page 149 in 12 th edition)
Types of Body Movements
 Types of Body Movements Bởi: OpenStaxCollege Synovial joints allow the body a tremendous range of movements. Each movement at a synovial joint results from the contraction or relaxation of the muscles
Types of Body Movements Bởi: OpenStaxCollege Synovial joints allow the body a tremendous range of movements. Each movement at a synovial joint results from the contraction or relaxation of the muscles
Prior authorization will not be required for outpatient speech therapy.*
 POLICY CHANGE: Authorization for All Outpatient Speech Therapy and Pediatric Outpatient Physical and Occupational Therapy NOT REQUIRED by Martin s Point Health Care Effective June 25, 2018 Thank you for
POLICY CHANGE: Authorization for All Outpatient Speech Therapy and Pediatric Outpatient Physical and Occupational Therapy NOT REQUIRED by Martin s Point Health Care Effective June 25, 2018 Thank you for
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK. Musculoskeletal Anatomy & Kinesiology I TERMINOLOGY, STRUCTURES, & SKELETAL OVERVIEW
 BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology I TERMINOLOGY, STRUCTURES, & SKELETAL OVERVIEW MSAK101-I Session 1 Learning Objectives: 1. Define
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology I TERMINOLOGY, STRUCTURES, & SKELETAL OVERVIEW MSAK101-I Session 1 Learning Objectives: 1. Define
