REGIONAL ANESTHESIA RESIDENT HANDBOOK
|
|
|
- Arabella Reed
- 6 years ago
- Views:
Transcription
1 REGIONAL ANESTHESIA RESIDENT HANDBOOK Stanford University Department of Anesthesia Special thanks to previous fellow and attending who have contributed to this handbook: Meredith Kan, MD and Meghana Yajnik, MD Page 1 of 18
2 I. Preparing for Blocks a. The Night Before b. The Morning Of c. Documentation and Orders i. Ultrasound image ii. EPIC Notes iii. EPIC orders iv. Block followup note v. Call schedule Table of Contents II. III. Other Helpful Information a. OSC/SMOC b. Journal Club Consenting Patients Risks and Benefits IV. Reference: a. Upper Extremity Blocks b. Lower Extremity Blocks c. Paravertebral Blocks d. TAP Blocks e. Anticoagulation Guidelines Page 2 of 18
3 I. Preparing for Blocks a. The Night Before Look over the ed schedule from the fellow for the plan for both Stanford and OSC. When pre-oping the patients: pay particular attention to any chronic pain conditions, allergies, anticoagulation, Hct/Coags, and cardio-pulmonary comorbidities, including anything that might delay or cancel surgery. You do not need to call your attending for the plan at Stanford or OSC, though they will be happy to answer questions if it helps you to prepare better. If several 1 st case blocks, please call/consent your assigned patient the day prior and remind patients to be at registration at 5AM Tuesday thru Friday (6AM on Mondays). b. The Morning Of Arrival time for residents is usually between 5:30 and 6:00, depending on how many first case blocks. No filled syringes or drug vials are ever to be left out. It is your responsibility to keep the area clean and organized. Things to get done: o Draw up local (ask the fellow if you re not sure what you ll need) o Draw up sedation (fent/versed, from the block area pyxis) o Place the ultrasound on the correct side of the patient (opposite of block side) o Hook patient up to pulse ox, BP cuff, EKG, nasal cannula o Start patient s IV and draw any necessary labs (example- stat VBG for AV fistula patients). If the nurse is checking the patient in, briefly introduce yourself to the patient and get the IV and monitors on. o Consent patient for the block once the pre-op nurse has checked the patient in. o Collect supplies: For single shot injections, you will need: 1. Sterile gloves 2. Chloraprep 3. Local anesthetic 4. Gauze (not sterile) 5. 21G Pajunk 100mm needle 6. Sterile ultrasound cover (includes ultrasound gel) 7. 3 ml syringe of lidocaine for SQ infiltration For nerve catheters, you will need 1. Sterile gloves and gown 2. Chloraprep 10ml stick 3. Local anesthetic 4. Ultrasound probe cover (sterile) 5. Flexblock nerve block kit 6. Sterile towels (1 pack) 7. Tegaderms-2 large + 1 small 8. Dermabond (1) 9. Sterile Saline (20cc drawn up and injected into kit) 10. Biopatch (1) Page 3 of 18
4 c. Documentation and Orders i.ultrasound image on GE machines 1) Select Patient on ultrasound screen 2) Select New Patient 3) Enter patient s MRN, then select Register 4) During the block, hit the P1 button to capture an image. This image will be linked to that patient s electronic medical record. ii. EPIC note A new intraop procedure must be created, separate from the surgical intraop procedure. To do this: 1) Select the patient list button at the top of Epic: 2) Click system lists on the left, scroll down to surgery, and choose the location the patient is in (ie MOR, ASC, OSC, etc). 3) Double-click on the patient s name orselect intraop from the open chart drop-down 4) When it asks, select procedure to document on, click other and select "Nerve Block from the drop-down menu 5) Select the device to autopopulate vitals SAU10 or 11 for Stanford ASCPRE1 or 2 for ASC OPAC15 etc for OSC Note: If you have to manually enter in vitals, 2 sets are needed for an analgesic block. If the block will be used for the primary anesthetic, vital signs must be recorded q5min. 5) Assign staff as you would in the OR 6) Procedure note is done as a peripheral nerve block procedure note within the intra-op navigator. Select either the catheter or single shot macro at the upper right hand corner of the procedure note screen. 7) Local anesthetic and sedation are charted in the medications section (as if you were in the OR). 8) For catheter patients to be admitted, please press the pain button for adding a pain consult so they will be added to the Acute Pain consult list for follow-up. Note: If patients are discharged home by Acute Pain with a catheter that we placed, we are responsible for the outpatient follow-up. We need to touch base with the pain team regularly to identify these patients so they can be followed up appropriately. iii. EPIC orders 1. Inpatients and Outpatients: PACU resident will place orders but please check in with them throughout the day. 2. If the PACU resident is not present: Page 4 of 18
5 a. Click Orders b. Type in On Q c. Select the Ropivicaine 0.2% anesthetic pump 550ml variable rate 2-14ml Rate d. Choose 6 or 8ml/hr Route e. If at SMOC: select On Q PCA option. Documentation and Orders Cont iv.sign out all in-house catheters to PACU resident throughout the day Please remember to add every patient to the Acute Pain list by clicking the pain button tab in the record on EPIC! We will show you how to do this. iv. Block Follow-up Note 1. All catheter and single injection in-patients must be followed up on POD day All outpatient catheters must be continued to be followed up daily while the catheter is in. 3. If a patient is discharged home from the in-patient Pain service with an On Q, we continue to follow them (the pain service will notify us when this happens). 1. Go to "My cases" Status board and click on "Block followup" icon. 2. Click the "create note" to open the note template. Find the patient's number by clicking on the demographics tab. Also, when opened, the "follow up report" tab should have at least one phone number for the patient. Page 5 of 18
6 Documentation and Orders Cont. 3. Begin documenting the note. v. Call Schedule The regional service has a ghost pager that will be forwarded to the resident on call. The number is (which spells out block ). The OSC resident carries the call pager as they place most of our outpatient catheters. The pager call is from the first day of the rotation at OSC thru the Sunday before switching to the Stanford week. The residents will alternate weekly. Each day, please call the operator and let them know your pager so they may forward the regional pages to the correct person. Because the person who placed the catheter is calling the patients daily to check-in, most calls can be avoided with good patient education. Fellows and attendings are always available for anything you may be unsure about or questions you may have. Please coordinate with the fellows if a patient is having uncontrolled pain and needs to come back in to the hospital for a repeat procedure or to have catheter evaluated. During the day, this can be done at the OSC regional clinic, sparing the patient an ED visit. Page 6 of 18
7 II. Other Helpful Info a. SMOC Review the daily regional anesthesia plan sent out by fellows to see the plan. If there are less than 5 blocks, you and the attending may be placed in OR perform blocks in between cases. If assigned to room, set up room as usual. Block area is Bay 15. However, the blocks can be performed in any of the Bays. There are 2 block carts (Code ) If you are doing a block far away - move the cart with you. The sedation medications are taken from a pyxis in the pre-op nursing station. Your Stanford access should work, however you may need to get access from the SMOC pharmacist (Ming). The codonics is located next to the physician computer area in between preop and PACU. It is very important to keep block cart locked since it contains needles and meds. The key is kept in the SMOC anesthesia work room. The pre-op nurses will usually start the IV, though they always appreciate our help. Place standard monitoring on the patient. Position the patient, ultrasound machine, and your supplies ergonomically. Perform a procedural time-out with the attending. Review any pain medications, anticoagulation status, and pre-existing neuropathies. Logistics: The OSC is located on the 3rd floor of the Stanford Medicine Outpatient Center in Redwood City (450 Broadway 94063). Parking is currently off site due to construction. You can get access to the surgery center suite from security. You will need to get the designated OSC scrubs from the surgery center front office on or before your first day. You can fill out a form to get access from your ID badge. Breakfast and snacks are available at the café on the first floor. b. Journal Club 3rd Thursday of the month: Each resident presents an article chosen by the fellow or attending. Please also give a short M&M/ rotation summary including # of blocks performed, follow-up information, complications, and interesting findings. Page 7 of 18
8 III. Consenting Patients Risks and Benefits Introduce yourself as part of the regional anesthesia team. You are here to offer and perform a nerve block, and a separate anesthesia team will be caring for the patient intraop. Explain that the numbing injection before or after surgery will supplement their pain control and that it is the standard of practice to offer nerve blocks for certain procedures. The patient should understand we ROUTINELY perform these blocks for their surgical procedure. Benefits: Patients require less narcotics/anesthesia, have improved post-op pain control, avoid GA in some cases, and have improved quality of recovery. Better pain control with less sedation means faster rehab and shorter hospital stays. Risks: All risks are rare. Benefits outweigh risks by far in every case where a block is offered. Please mention bleeding, infection, hematoma, local anesthetic toxicity, and nerve damage (extremely rare). Pneumothorax if doing a paravertebral. More than 95% of cases of nerve injury are transient with full recovery over time. So if a delay in recovery occurs, emphasize that it is almost always a matter of time for full recovery. May want to mention the theoretical risk of permanent injury. Assure the patients that they will receive sedation and oxygen for comfort and safety during the block placement. All vital signs will be monitored. If a catheter is placed, the pain service will see them while they are in-house with catheter. The regional team will see them on day 1 following surgery. Set realistic expectations for pain control: The numbing injection will last approximately 4-16 hours (depending on local anesthetic selection). If placing a catheter, describe to the patient that the local anesthetic delivered post-op will dull the pain but not numb the area as the first injection did. A small amount of leakage from the insertion site is normal backtracking of local anesthetic. Address outpatient regimen for pain control: Patients go from a numb limb to severe pain without much warning as the block wears off if a single shot. Advise your outpatients to take their PO meds approximately 6 hours after block (even if block is still working) and every 4 hrs after that to stay ahead of pain. Warn about care and protection of numb limb: Altered sensation, proprioception, and motor function of the affected limb can be dangerous. Inform the patient to take care and not to attempt any tasks with the blocked limb. Page 8 of 18
9 IV. Reference This is a brief outline of some of the blocks you will most commonly encounter on this rotation. For a more comprehensive review of sono-anatomy and block performance, please reference the anesthesia toolbox. There is a link on the regional anesthesia specialty page on ether. If you have any difficulty accessing the site, contact Meredith Kan. UPPER EXTREMITY NERVE BLOCKS BRACHIAL PLEXUS BLOCKS INTERSCALENE BLOCK Indications: Shoulder, clavicle (if supplement with superficial cervical) Distribution: Roots of brachial plexus (C4-C7 typically) Setup: Standard Positioning: Supine with face turned 45 degrees away from side of block Technique: -Bony landmarks: sternal notch, clavicle, and mastoid process -Sternal and clavicular heads of sternocleidomastoid muscle -External Jugular Ultrasound guided: Place probe in the supraclavicular fossa to identify subclavian artery and the brachial plexus (superior and lateral to the artery). Other landmarks are first rib, lung pleura. Scan the US probe proximally following the brachial plexus until it takes on the look of distinct nerve bundles often described as a traffic light. These bundles should be in between the anterior and middle scalene muscles Page 9 of 18
10 Insert needle into interscalene groove, inject LA, and look for spread in and around these nerve bundles with frequent aspiration. Local Anesthetic: 20 ml 0.25% ropivacaine Common Side Infection, puncture (carotid, local anesthetic total spinal recurrent laryngeal hoarseness, nasal nerve block (~100%) compromise, ulnar Effects/Complications: hematoma, vascular subclavian, EJV, IJV), toxicity, nerve injury, anesthesia, Horner s, nerve block (causing stuffiness), phrenic causing respiratory nerve sparing Relative Contraindications: Severe respiratory distress/copd, diaphragmatic dysfunction, anticoagulation SUPRACLAVICULAR Indications: Arm, forearm, and hand surgery Distribution: Divisions of the superior, middle and inferior trunks of brachial plexus Setup: Standard Positioning:Supine or semi-sitting position, +/-pillow turned parallel to patient under patient s opposite shoulder. Technique: Ultrasound guided: Place the probe in the supraclavicular fossa. Identify the subclavian artery which usually passes under the clavicle at its midpoint. The nerves usually appear superior and lateral to the artery enclosed in a sheath. Other important landmarks include the first rib which appears hyperechoic and the lung pleura distal to this. If you see the carotid artery and the IJ you are too medial. Inject local and first insert needle into the corner pocket, then re-directing above the plexus to surround the sheath. Local Anesthetic: 20 ml + 10 ml 0.5% ropivacaine Common Side Effects/Complications: Pneumothorax, subclavian artery puncture, Horner s syndrome, phrenic nerve block Page 10 of 18
11 Relative Contraindications: INR >1.5 and respiratory compromise INFRACLAVICULAR Indications: Arm, forearm, and hand surgery Position: Supine Distribution: Cords of brachial plexus Ultrasound guided technique: Position patient supine with arm abducted and externally rotated. Place the probe below the distal part of clavicle. The brachial plexus is deeper compared to the supraclavicular block so you may need a curved probe. Look for subclavian artery surrounded by the 3 cords of the brachial plexus contained within a sheath. Inject local near visible nerve bundles with 1-2 passes. AXILLARY Indications: Forearm and hand surgery Distribution: Terminal nerves of brachial plexus innervating the forearm and hand Setup: Standard Positioning: Supine, with patient s arm abducted at 90 degrees at the shoulder and externally rotated Technique: Ultrasound guided: Place the probe in the mid-axillary line to identify the axillary artery within the axillary sheath. It is usually relatively shallow. If necessary, move the probe proximally to look for the musculocutaneous nerve between the biceps and coracobrachialis muscles. Blocking the radial nerve which is usually located below the artery usually leads to a spread of local around the circumference of the artery. The positions of the nerves often vary making it challenging to get all 4 nerves in one ultrasound view. It might require a few passes of the needle to surround all 3 nerve bundles. Nerve Stimulator: Palpate the axillary artery pulse and mark the longitudinal path of the artery in the middle of the axilla. Insert your needle above the artery, pointing in a proximal direction almost parallel to the artery at a degree angle to the skin. Once twitch is obtained in the wrist, hand or forearm you can inject your LA. Place needle above (lateral) to artery to stimulate median nerve, below (medial) to artery to stimulate ulnar nerve, posterior to (behind) artery to stimulate radial nerve. Musculocutaneous n.-imbedded in coracobrachialis muscle, can stimulate or inject 5 ml local into body of coracobrachialis m Intercostobrachial n. subcutaneous fanning skin wheal extending laterally and medially from ax block needle entry site Look for current < 0.5 ma and inject LA with frequent aspiration. Page 11 of 18
12 Local Anesthetic: 15 ml (axillary) + 5 ml (musculocutaneous) 0.5% ropivacaine Common Side Effects/Complications: Musculocutaneous nerve sparing, axillary artery intravascular injection with LA toxicity. Relative Contraindications: INR >1.5. Surgery in the area of the block. LOWER EXTREMITY BLOCKS FEMORAL Indications: Knee surgery, anterior thigh surgery, LE surgery if they need femoral nerve distribution blocked as such as with ankle surgery on the medial side of the leg. Distribution: (T12-L4) anterior thigh, most of femur and knee joint, skin on the medial aspect of the leg below the knee joint Setup: Standard Positioning: Supine Technique: Ultrasound guided: Place the probe in the inguinal crease and identify the femoral artery. The femoral nerve will be lateral to the artery. At the inguinal crease, the nerve is covered by the fascia iliaca and separated from the artery and vein by the psoas muscle and the ligamentum ileopectineum. Make sure that you are above the femoral artery bifurcation. The femoral nerve is in the hyperechoic triangle. Page 12 of 18
13 Nerve Stimulator: Palpate the femoral pulse within the inguinal crease. The femoral vein is medial to the artery and nerve is lateral to the artery (V-A-N). Insert needle approx 1 cm lateral to arterial pulse and 1cm inferior. Direct the needle cephalad with a 60 degree angle to the skin. Look for quadriceps contraction and proximal patellar movement with a current of 0.5 ma or less. Local Anesthetic: 20 ml 0.5% ropivacaine Common Side Effects/Complications: Intravascular injection, quadriceps weakness Adductor Canal Block/Saphenous Block Indications: Knee surgery, Incisions in saphenous nerve distribution (ie medial leg) Distribution: medial/anterior knee, skin on the medial aspect of the leg below the knee joint, medial leg, medial maleoulus Setup: Standard Positioning: Supine Technique: Ultrasound guided: Place the probe over the anteromedial aspect of the proximal 1/3 or the thigh. Identify the superficial femoral artery, and vein under the deep to the Sartorius muscle. The saphenous and nerve to vastus medialias are often hyperechoic structures within this compartment. The needle must puncture the subsartorial fascia and local should be seen spreading right next to the vascular structures since they also run in the adductor canal. Dr. Goodman likes these catheters to be tunneled. A fellow or attending will show you how to do this. Page 13 of 18
14 Local Anesthetic: 30 ml 0.25% ropivacaine Common Side Effects/Complications: Intravascular injection, quadriceps weakness (less so then femoral) SCIATIC Indications: LE surgery: posterior thigh, below the knee cases outside of medial aspect of the leg Distribution: (L4-S3) skin of posterior thigh, hamstring and biceps muscle, part of hip and knee joint and entire part of leg below the knee except for the medical aspect of the lower leg (supplied by saphenous and the terminal branch of femoral nerve) Setup: Standard Positioning: Lateral decubitus with hip and knee flexed, supine for anterior approach; either position with ultrasound Technique: Ultrasound guidance: Prone Position: Place the probe axially, midway between the greater trochanter (lateral) and the ischial spine (medial) just below the gluteal crease. Both these landmarks are seen as curvilinear hypoechoic shadows. The sciatic nerve is seen as a Page 14 of 18
15 hyperechoic elliptical structure deep to the gluteus maximus muscle. Nerve Stimulator: (Posterior/Classic Approach) Identify the greater trochanter (GT) and the posterior superior iliac spine (PSIS) and draw a line joining the inner aspect of both landmarks. Then, draw a line from the sacral hiatus to the greater trochanter. Bisect the first line from the GT to the PSIS and then draw a line perpendicular from this point downward 4-5 cm. The insertion point of the needle is where this line intersects the 2 nd line from the GT to the sacral hiatus. Insert needle perpendicular to skin. Once gluteal twitching is observed, advance needle until gluteal twitch is gone and hamstring, calf foot, plantar flexion or dorsiflexion or toe twitching is observed. Local Anesthetic: 30 ml 0.5% ropivacaine Common Side Effects/Complications: Hematoma, nerve damage, sympathetic fibers in the nerve blocked causing slight BP drop POPLITEAL Indications: LE surgery, ankle or foot surgery.. Distribution: The entire LE below the knee except for the cutaneous sensation of the medial leg. Blocking sciatic nerve before it branches into common peroneal and tibial in popliteal fossa. Setup: Standard Positioning: Supine or prone, depending on patient comfort and ability. Technique: Ultrasound guidance: Prone position or Supine position. If patient is supine, flex the knee. Start scanning in the popliteal fossa. Identify the popliteal artery. The popliteal artery, nerve, and femur should form a triangle, with the nerve as the apex. As you move up leg proximally, the distance between the popliteal artery and nerve increases. Identify the sciatic nerve. Scan the area to identify the area of sciatic bifurcation into the common peroneal and posterior tibial branches. Page 15 of 18
16 Nerve Stimulator-Classic approach: Landmarks: Identify the popliteal natural crease. Go 7 cm cephalad and 1 cm lateral. Mark the semitendonosus and semimembranosous, as well as the biceps femoris muscles. Insert the needle perpendicular to the floor and advance needle until twitches are evident. The twitches should be dorsiflexion / eversion (common peroneal) and plantar flexion/ inversion (tibial) of foot at <0.5mA. Plantar flexion is more desirable to ensure superior block. Local Anesthetic: 3 ml 0.5% ropi Common Side Effects/Complications: Block failure LUMBAR PLEXUS BLOCK Indications: Hip replacement, resections of above knee lesions Distribution: Nerves from L1-L4 travel within a fascial plane in the psoas muscle. Setup: Standard + stimuplex 4-6 inch, nerve stimulator Positioning: Sitting or lateral decubitus Technique: Draw line connecting iliac crests, place skin mark 5 cm lateral to midline and 3 cm caudad which should be at level of L4 transverse process. Insert needle perpendicular until contacts transverse process at depth of 6-8cm (can be deeper in obese patients), step off the transverse process with the needle and advance 2 cm deeper. Have an assistant feel for quadriceps contraction to less than 0.6. There is no need to stim lower than 0.6 and refrain from directing the needle medially for concern of epidural/dural spread. Local Anesthetic: 20 ml + 10 ml 0.5% ropi Common Side Effects/Complications: Inadvertent puncture of epidural space, dura, peritoneum, kidney, ureter, intravascular Contraindications: INR > 1.5, infection (consider single shot only) TRANSVERSUS ABDOMINIS PLANE (TAP) Indications: Inguinal hernia repair, abdominal hysterectomy, lower abdominal incisions, usually placed post-induction Distribution: Anterior divisions of spinal segmental nerves supplying abdominal wall run between internal oblique and transverses abdominis muscle layers Page 16 of 18
17 Setup: Sterile gloves, chlorhexidine, ultrasound, ultrasound gel, 22 gauge Tuohy, 30 cm extension tubing Positioning: Supine Technique: Place the probe near midline over the rectus abdominis muscle and follow it as it tapers laterally to a junction that leads to the three muscle layers of the lateral abdominal wall: external oblique, internal oblique, transversus abdominis. Insert the block needle in-plane with the transducer, using an anterior-posterior direction. Look for local anesthetic spread between the fascial layer separating the internal oblique and the transverses abdominis muscles. **It is important to be aware of the bowel that lies just beneath the transversus abdominis-bowel movement is evident on ultrasound Local Anesthetic: ml 0.25% ropi Common Side Effects/Complications: Block failure, puncture of peritoneum, intravascular injection Contraindications: INR > 1.5 References: 1. Nysora.com 2. Peripheral Nerve Blocks, Third Edition. Jacques E. Chelly Page 17 of 18
18 GUIDELINES FOR CONTINUOUS NERVE CATHETER PLACEMENT IN ANTICOAGULATED PATIENTS *Download the ASRA coags application for the latest in recommendations for neuraxial, deep and superficial peripheral nerve block placement/removal in anticoagulated patients *Fibrinolytics/ GIIB-IIIA inhibitors: Neuraxial Anesthesia is contraindicated **General rule-hemostasis can be achieved with at least 25-30% of normal activity of coagulation factors AND Fibrinogen levels mg/dl (in absence of Heparin or other factor antagonists) Page 18 of 18
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
inerve Guide to Nerves 2009
 inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
Ultrasound Guided Lower Extremity Blocks
 Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Lower Extremity Ultrasound-Guided Regional Anesthesia. Stephanie Duffy, CRNA Regional Anesthesia Faculty Acute Pain Service NMCSD
 Lower Extremity Ultrasound-Guided Regional Anesthesia Stephanie Duffy, CRNA Regional Anesthesia Faculty Acute Pain Service NMCSD Objectives Review anatomy of lumbosacral plexus Lumbar plexus blocks Psoas
Lower Extremity Ultrasound-Guided Regional Anesthesia Stephanie Duffy, CRNA Regional Anesthesia Faculty Acute Pain Service NMCSD Objectives Review anatomy of lumbosacral plexus Lumbar plexus blocks Psoas
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist
 Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
USRA OF THE LOWER EXTREMITY
 USRA OF THE LOWER EXTREMITY Christian R. Falyar, CRNA, DNAP Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE LOWER EXTREMITY Christian R. Falyar, CRNA, DNAP Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
Disclaimer. Why Regional anesthesia? Peripheral Nerve Blocks: Upper/Lower Extremity & TAP BLOCKS
 Peripheral Nerve Blocks: Upper/Lower Extremity & TAP BLOCKS Presented by: Nathan Merritt, MD Director of Regional Anesthesia and Acute Pain Parkhill Medical Center Fort Worth Co authored by: Mark Zimmerman,
Peripheral Nerve Blocks: Upper/Lower Extremity & TAP BLOCKS Presented by: Nathan Merritt, MD Director of Regional Anesthesia and Acute Pain Parkhill Medical Center Fort Worth Co authored by: Mark Zimmerman,
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics
 Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
ANATYOMY OF The thigh
 ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
FASCIAL PLANE BLOCKS TOM BARIBEAULT MSN, CRNA
 FASCIAL PLANE BLOCKS TOM BARIBEAULT MSN, CRNA TECHNIQUES Abdominal Wall TAP Rectus Sheath Quadratus Lumborum Erector Spinae Chest PECS I & II Erector Spinae TECHNIQUES Knee Ipack/LIA Hip Fascia Iliaca
FASCIAL PLANE BLOCKS TOM BARIBEAULT MSN, CRNA TECHNIQUES Abdominal Wall TAP Rectus Sheath Quadratus Lumborum Erector Spinae Chest PECS I & II Erector Spinae TECHNIQUES Knee Ipack/LIA Hip Fascia Iliaca
The thigh. Prof. Oluwadiya KS
 The thigh Prof. Oluwadiya KS www.oluwadiya.com The Thigh: Boundaries The thigh is the region of the lower limb that is approximately between the hip and knee joints Anteriorly, it is separated from the
The thigh Prof. Oluwadiya KS www.oluwadiya.com The Thigh: Boundaries The thigh is the region of the lower limb that is approximately between the hip and knee joints Anteriorly, it is separated from the
Lower Limb Nerves. Clinical Anatomy
 Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
ANATYOMY OF The thigh
 ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
Ultrasound Guided Regional Nerve Blocks
 Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Where should you palpate the pulse of different arteries in the lower limb?
 Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
Anterior and Medial compartments of the thigh. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Anterior and Medial compartments of the thigh Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Terms Related to Movements Movement Flexion Extension Abduction Adduction Medial (internal)
Anterior and Medial compartments of the thigh Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Terms Related to Movements Movement Flexion Extension Abduction Adduction Medial (internal)
Adductor canal (Subsartorial) or Hunter s canal
 Adductor canal (Subsartorial) or Hunter s canal John Hunter described the exposure and ligation of the femoral artery in this canal for aneurysm of the popliteal artery; this method has the advantage that
Adductor canal (Subsartorial) or Hunter s canal John Hunter described the exposure and ligation of the femoral artery in this canal for aneurysm of the popliteal artery; this method has the advantage that
rotation of the hip Flexion of the knee Iliac fossa of iliac Lesser trochanter Femoral nerve Flexion of the thigh at the hip shaft of tibia
 Anatomy of the lower limb Anterior & medial compartments of the thigh Dr. Hayder The fascia lata encloses the entire thigh like a sleeve/stocking. Three intramuscular fascial septa (lateral, medial, and
Anatomy of the lower limb Anterior & medial compartments of the thigh Dr. Hayder The fascia lata encloses the entire thigh like a sleeve/stocking. Three intramuscular fascial septa (lateral, medial, and
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
Basics of US Regional Anaesthesia. November 2008
 Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
The arm: *For images refer back to the slides
 The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
PERIPHERAL REGIONAL BLOCKS. by Mike DeBroeck, DNP, CRNA
 PERIPHERAL REGIONAL BLOCKS by Mike DeBroeck, DNP, CRNA Why am I bothering with this topic at all? Do CRNAs REALLY even do peripheral regional anesthetics? YES!!!!!!! TOPICS GENERAL INFO SUCCESS RATES
PERIPHERAL REGIONAL BLOCKS by Mike DeBroeck, DNP, CRNA Why am I bothering with this topic at all? Do CRNAs REALLY even do peripheral regional anesthetics? YES!!!!!!! TOPICS GENERAL INFO SUCCESS RATES
Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes
 Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes 1 This lab involves the second section of the exercise Spinal Cord, Spinal Nerves, and the Autonomic Nervous System,
Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes 1 This lab involves the second section of the exercise Spinal Cord, Spinal Nerves, and the Autonomic Nervous System,
Posterior compartment of the thigh. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Posterior compartment of the thigh Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Posterior compartment of the thigh 1-Muscles: Biceps femoris Semitendinosus Semimembranosus Adductor magnus
Posterior compartment of the thigh Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Posterior compartment of the thigh 1-Muscles: Biceps femoris Semitendinosus Semimembranosus Adductor magnus
Misc Anatomy. Upper Limb! 2. Lower Limb! 5. Venous Drainage! Head & neck! 8
 Misc Anatomy Upper Limb! 2 Arteries!... 2 Veins!... 2 Spaces!... 4 Lower Limb! 5 Arteries!... 5 Venous Drainage!... 6 Spaces!... 7 Head & neck! 8 Artery!... 8 Ultrasound View for IJ CVL!... 8 Arteries
Misc Anatomy Upper Limb! 2 Arteries!... 2 Veins!... 2 Spaces!... 4 Lower Limb! 5 Arteries!... 5 Venous Drainage!... 6 Spaces!... 7 Head & neck! 8 Artery!... 8 Ultrasound View for IJ CVL!... 8 Arteries
Australian and New Zealand Registry of Regional Anaesthesia (AURORA)
 Australian and New Zealand Registry of Regional Anaesthesia (AURORA) Overview of Results First 4000 procedures recorded to - www.anaesthesiaregistry.org June 1st 2011 to February 2012 Background Australian
Australian and New Zealand Registry of Regional Anaesthesia (AURORA) Overview of Results First 4000 procedures recorded to - www.anaesthesiaregistry.org June 1st 2011 to February 2012 Background Australian
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 1: Proximal bones, plexuses and patterns
 213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 1: Proximal bones, plexuses and patterns CLAVICLE Examine an isolated clavicle and compare it with a clavicle on an articulated skeleton. Viewed from above,
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 1: Proximal bones, plexuses and patterns CLAVICLE Examine an isolated clavicle and compare it with a clavicle on an articulated skeleton. Viewed from above,
The Lower Limb II. Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa
 The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Lumbar Plexus. Ventral rami L1 L4 Supplies: Major nerves.. Abdominal wall External genitalia Anteromedial thigh
 Lower Limb Nerves Lectures Objectives Describe the structure and relationships of the plexuses of the lower limb. Describe the course, relationships and structures supplied for the major nerves of the
Lower Limb Nerves Lectures Objectives Describe the structure and relationships of the plexuses of the lower limb. Describe the course, relationships and structures supplied for the major nerves of the
ULTRASOUND GUIDED NERVE BLOCKS
 2 ULTRASOUND GUIDED NERVE BLOCKS Elizabeth Kwan, MD UCSF High Risk Emergency Medicine 2014 1 Instructors Kristin Berona Reza Danesh Sally Graglia Daniel Kievlan Starr Knight Allison Mulcahy Carmen Partida
2 ULTRASOUND GUIDED NERVE BLOCKS Elizabeth Kwan, MD UCSF High Risk Emergency Medicine 2014 1 Instructors Kristin Berona Reza Danesh Sally Graglia Daniel Kievlan Starr Knight Allison Mulcahy Carmen Partida
ANATYOMY OF The thigh
 ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 1, 2 and 3 are From the lumber plexus 5- Intermediate cutaneous
ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 1, 2 and 3 are From the lumber plexus 5- Intermediate cutaneous
Regional Blocks a practical guide:
 Regional Blocks a practical guide: Author Fleur Roberts email: fleur_roberts@hotmail.com Please use this guide in conjunction with the previous tutorial (16/01/06) which describes the rules for performing
Regional Blocks a practical guide: Author Fleur Roberts email: fleur_roberts@hotmail.com Please use this guide in conjunction with the previous tutorial (16/01/06) which describes the rules for performing
The Language of Anatomy. (Anatomical Terminology)
 The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
Mohammad Ashraf. Abdulrahman Al-Hanbali. Ahmad Salman. 1 P a g e
 - 7 Mohammad Ashraf Abdulrahman Al-Hanbali Ahmad Salman 1 P a g e Structures under the cover of Gluteus Maximus: 1-Bones: Ileum, Femur (Head, greater trochanter and gluteal tuberosity), Ischium (ischial
- 7 Mohammad Ashraf Abdulrahman Al-Hanbali Ahmad Salman 1 P a g e Structures under the cover of Gluteus Maximus: 1-Bones: Ileum, Femur (Head, greater trochanter and gluteal tuberosity), Ischium (ischial
TRAINING TOOLS THE MOST ADVANCED. ULTRASOUND
 THE MOST ADVANCED ULTRASOUND TRAINING TOOLS Introducing NYSORA ULTRASOUND SIMULATORS Developed by opinion leaders and educators, NYSORA ULTRASOUND SIMULATORS are the most anatomically accurate, tissue-like
THE MOST ADVANCED ULTRASOUND TRAINING TOOLS Introducing NYSORA ULTRASOUND SIMULATORS Developed by opinion leaders and educators, NYSORA ULTRASOUND SIMULATORS are the most anatomically accurate, tissue-like
Muscles of the Thigh. 6.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group
 Muscles of the Thigh 6.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group Sartorius: This is a long strap like muscle with flattened tendons at each
Muscles of the Thigh 6.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group Sartorius: This is a long strap like muscle with flattened tendons at each
Electrode Placement. Skin Preparation. Frontalis (FRL) (Specific) Temporalis Anterior (TA) (Specific) Sternocleidomastoid (SCM) (Specific)
 Electrode Placement Skin Preparation 1) Removing the hair: Shave if necessary 2) Clean the skin: Use a towel or abrasive pad with conductive cleaning paste or alcohol to remove dead skin cells (high impedance)
Electrode Placement Skin Preparation 1) Removing the hair: Shave if necessary 2) Clean the skin: Use a towel or abrasive pad with conductive cleaning paste or alcohol to remove dead skin cells (high impedance)
lower limb Anterior Compartment: lecture 3 The deep fascia ( fascia lata) divides the thigh into 3 compartments:
 lower limb lecture 3 The deep fascia ( fascia lata) divides the thigh into 3 compartments: 1. Anterior Extensor compartment 2. Medial Adductor compartment 3. Posterior Flexor compartment Anterior Compartment:
lower limb lecture 3 The deep fascia ( fascia lata) divides the thigh into 3 compartments: 1. Anterior Extensor compartment 2. Medial Adductor compartment 3. Posterior Flexor compartment Anterior Compartment:
musculoskeletal system anatomy nerves of the lower limb 1 done by: dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy nerves of the lower limb 1 done by: dina sawadha & mohammad abukabeer What is the importance of plexuses? plexuses provides us the advantage of a phenomenon called convergence
musculoskeletal system anatomy nerves of the lower limb 1 done by: dina sawadha & mohammad abukabeer What is the importance of plexuses? plexuses provides us the advantage of a phenomenon called convergence
USRA OF THE UPPER EXTREMITY
 USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
The Hip (Iliofemoral) Joint. Presented by: Rob, Rachel, Alina and Lisa
 The Hip (Iliofemoral) Joint Presented by: Rob, Rachel, Alina and Lisa Surface Anatomy: Posterior Surface Anatomy: Anterior Bones: Os Coxae Consists of 3 Portions: Ilium Ischium Pubis Bones: Pubis Portion
The Hip (Iliofemoral) Joint Presented by: Rob, Rachel, Alina and Lisa Surface Anatomy: Posterior Surface Anatomy: Anterior Bones: Os Coxae Consists of 3 Portions: Ilium Ischium Pubis Bones: Pubis Portion
Quillen College of Medicine
 Ea s t T e n n e s s e e St a t e Un i v e r s i t y Quillen College of Medicine Failing to prepare is preparing to fail. John Wooden, UCL A Dr. Tom Kwasigroch Associate Dean Director, Medical Human Gross
Ea s t T e n n e s s e e St a t e Un i v e r s i t y Quillen College of Medicine Failing to prepare is preparing to fail. John Wooden, UCL A Dr. Tom Kwasigroch Associate Dean Director, Medical Human Gross
Contents of the Posterior Fascial Compartment of the Thigh
 Contents of the Posterior Fascial Compartment of the Thigh 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t
Contents of the Posterior Fascial Compartment of the Thigh 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t
Clinical Protocols of the Anesthesiology Department at the Dartmouth-Hitchcock Medical Center: Techniques for lower extremity nerve blocks.
 Clinical Protocols of the Anesthesiology Department at the Dartmouth-Hitchcock Medical Center: Techniques for lower extremity nerve blocks. Authors from DHMC: Brian D. Sites, MD. Assistant Professor of
Clinical Protocols of the Anesthesiology Department at the Dartmouth-Hitchcock Medical Center: Techniques for lower extremity nerve blocks. Authors from DHMC: Brian D. Sites, MD. Assistant Professor of
perivascular, sensory and motor effects, 62, side effects, 64 and subfascial hematoma, 221 axillary plexus, 6 7 axonotmesis, 221, 222
 249 Index A abscess, and continuous peripheral nerve block, 244 Achilles tendon rupture, 173 and saphenous nerve block, 208 and sural nerve block, 209 and tibial nerve block, 203, 204, 210, 211 acromion,
249 Index A abscess, and continuous peripheral nerve block, 244 Achilles tendon rupture, 173 and saphenous nerve block, 208 and sural nerve block, 209 and tibial nerve block, 203, 204, 210, 211 acromion,
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS
 HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
MUSCULOSKELETAL LOWER LIMB
 MUSCULOSKELETAL LOWER LIMB Spinal Cord Lumbar and Sacral Regions Spinal cord Dorsal root ganglion Conus medullaris Cauda equina Dorsal root ganglion of the fifth lumbar nerve End of subarachnoid space
MUSCULOSKELETAL LOWER LIMB Spinal Cord Lumbar and Sacral Regions Spinal cord Dorsal root ganglion Conus medullaris Cauda equina Dorsal root ganglion of the fifth lumbar nerve End of subarachnoid space
Ali Yaghi. Omar Eyad. Ahmad Salman. 1 P a g e
 5 Ali Yaghi Omar Eyad Ahmad Salman 1 P a g e **There are two types of groin hernia; the femoral hernia and the inguinal hernia. But how can we differentiate between the inguinal hernia and the femoral
5 Ali Yaghi Omar Eyad Ahmad Salman 1 P a g e **There are two types of groin hernia; the femoral hernia and the inguinal hernia. But how can we differentiate between the inguinal hernia and the femoral
Ultrasound-guided supraclavicular block
 THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
Regional Anaesthesia
 Regional Anaesthesia Lower limb anatomy and blocks Hip and Knee Joint Hip Joint: Nerve supply Lumbar plexus Femoral nerve through the nerve to the Rectus Femoris Ant division of the Obturator nerve The
Regional Anaesthesia Lower limb anatomy and blocks Hip and Knee Joint Hip Joint: Nerve supply Lumbar plexus Femoral nerve through the nerve to the Rectus Femoris Ant division of the Obturator nerve The
Ultrasound-guided Sciatic Nerve Blocks: Higher and Popliteal Approaches
 10.5005/jp-journals-10027-1026 K Kondov, S Fransis REVIEW ARTICLE Ultrasound-guided Sciatic Nerve Blocks: Higher and Popliteal Approaches K Kondov, S Fransis ABSTRACT Background and objective: In modern
10.5005/jp-journals-10027-1026 K Kondov, S Fransis REVIEW ARTICLE Ultrasound-guided Sciatic Nerve Blocks: Higher and Popliteal Approaches K Kondov, S Fransis ABSTRACT Background and objective: In modern
Chapter 1: Introduction to the Human Body Test Bank
 Chapter 1: Introduction to the Human Body Test Bank MULTIPLE CHOICE 1. What is the branch of science that studies how the body functions? a. Anatomy b. Histology c. Pathology d. Physiology 2. Which word
Chapter 1: Introduction to the Human Body Test Bank MULTIPLE CHOICE 1. What is the branch of science that studies how the body functions? a. Anatomy b. Histology c. Pathology d. Physiology 2. Which word
Lecture 08 THIGH MUSCLES ANTERIOR COMPARTMENT. Dr Farooq Khan Aurakzai. Dated:
 Lecture 08 THIGH MUSCLES ANTERIOR COMPARTMENT BY Dr Farooq Khan Aurakzai Dated: 11.02.2017 INTRODUCTION to the thigh Muscles. The musculature of the thigh can be split into three sections by intermuscular
Lecture 08 THIGH MUSCLES ANTERIOR COMPARTMENT BY Dr Farooq Khan Aurakzai Dated: 11.02.2017 INTRODUCTION to the thigh Muscles. The musculature of the thigh can be split into three sections by intermuscular
Identify the muscles associated with the medial compartment of the thigh. Identify the attachment points of the medial thigh muscles.
 L 8 A B O R A T O R Y Thigh MEDIAL THIGH Identify the muscles associated with the medial compartment of the thigh. Identify the attachment points of the medial thigh muscles. Identify the actions of these
L 8 A B O R A T O R Y Thigh MEDIAL THIGH Identify the muscles associated with the medial compartment of the thigh. Identify the attachment points of the medial thigh muscles. Identify the actions of these
The Lower Limb. Anatomy RHS 241 Lecture 2 Dr. Einas Al-Eisa
 The Lower Limb Anatomy RHS 241 Lecture 2 Dr. Einas Al-Eisa The bony pelvis Protective osseofibrous ring for the pelvic viscera Transfer of forces to: acetabulum & head of femur (when standing) ischial
The Lower Limb Anatomy RHS 241 Lecture 2 Dr. Einas Al-Eisa The bony pelvis Protective osseofibrous ring for the pelvic viscera Transfer of forces to: acetabulum & head of femur (when standing) ischial
Human Anatomy Biology 255
 Human Anatomy Biology 255 Exam #4 Please place your name and I.D. number on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
Human Anatomy Biology 255 Exam #4 Please place your name and I.D. number on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
Lecture 09. Popliteal Fossa. BY Dr Farooq Khan Aurakzai
 Lecture 09 Popliteal Fossa BY Dr Farooq Khan Aurakzai Dated: 14.02.2018 What is popliteus? Introduction Anything relating to, or near the part of the leg behind the knee. From New Latin popliteus the muscle
Lecture 09 Popliteal Fossa BY Dr Farooq Khan Aurakzai Dated: 14.02.2018 What is popliteus? Introduction Anything relating to, or near the part of the leg behind the knee. From New Latin popliteus the muscle
Muscles of the lower extremities. Dr. Nabil khouri MD, MSc, Ph.D
 Muscles of the lower extremities Dr. Nabil khouri MD, MSc, Ph.D Posterior leg Popliteal fossa Boundaries Biceps femoris (superior-lateral) Semitendinosis and semimembranosis (superior-medial) Gastrocnemius
Muscles of the lower extremities Dr. Nabil khouri MD, MSc, Ph.D Posterior leg Popliteal fossa Boundaries Biceps femoris (superior-lateral) Semitendinosis and semimembranosis (superior-medial) Gastrocnemius
Baraa Ayed حسام أبو عوض. Ahmad Salman. 1 P a g e
 4 Baraa Ayed حسام أبو عوض Ahmad Salman 1 P a g e Today we are going to cover these concepts: Iliotibial tract Anterior compartment of the thigh and the hip Medial compartment of the thigh Femoral triangle
4 Baraa Ayed حسام أبو عوض Ahmad Salman 1 P a g e Today we are going to cover these concepts: Iliotibial tract Anterior compartment of the thigh and the hip Medial compartment of the thigh Femoral triangle
The Muscular System. Chapter 10 Part D. PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College
 Chapter 10 Part D The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.14: Muscles Crossing the Hip and
Chapter 10 Part D The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.14: Muscles Crossing the Hip and
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve
 Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve 2. Gluteus Maximus O: ilium I: femur Action: abduct the thigh Nerve:
Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve 2. Gluteus Maximus O: ilium I: femur Action: abduct the thigh Nerve:
Lab no 1 Structural organization of the human body
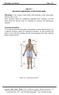 Physiology Lab Manual Page 1 of 6 Lab no 1 Structural organization of the human body Physiology is the science which deals with functions of the body parts, and how they work. Since function cannot be
Physiology Lab Manual Page 1 of 6 Lab no 1 Structural organization of the human body Physiology is the science which deals with functions of the body parts, and how they work. Since function cannot be
Peripheral Nerve Blocks
 Peripheral Nerve Blocks N U R S I N G E D U C A T I O N JPS Acute Pain Service Peripheral nerve blocks are used as part of a multimodal analgesic program which provides the patient with safe and effective
Peripheral Nerve Blocks N U R S I N G E D U C A T I O N JPS Acute Pain Service Peripheral nerve blocks are used as part of a multimodal analgesic program which provides the patient with safe and effective
First BHMS Anatomy Question Papers Calicut University
 First BHMS Anatomy Question Papers Calicut University 1996-2000 FIRST B.H.M.S. DEGREE EXAMINATION, DECEMBER 1996 Time: Three Hours Maximum: 100 Marks Answer any five questions. Draw diagrams wherever needed.
First BHMS Anatomy Question Papers Calicut University 1996-2000 FIRST B.H.M.S. DEGREE EXAMINATION, DECEMBER 1996 Time: Three Hours Maximum: 100 Marks Answer any five questions. Draw diagrams wherever needed.
Diana Mathioudakis DEAA EDIC AFRCA. consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d)
 & Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
& Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
TRAINING TOOLS THE MOST ADVANCED. ULTRASOUND
 THE MOST ADVANCED ULTRASOUND TRAINING TOOLS Introducing NYSORA ULTRASOUND SIMULATORS -the most time efficient ultrasound TISSUE SIMULATORS on the market. Developed by opinion leaders and workshop instructors,
THE MOST ADVANCED ULTRASOUND TRAINING TOOLS Introducing NYSORA ULTRASOUND SIMULATORS -the most time efficient ultrasound TISSUE SIMULATORS on the market. Developed by opinion leaders and workshop instructors,
Gateway to the upper limb. An area of transition between the neck and the arm.
 Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
MODULE 9 ARTERIAL AND VENOUS CATHETERIZATION. Robert B. McLafferty M.D. Southern Illinois University
 MODULE 9 ARTERIAL AND VENOUS CATHETERIZATION Robert B. McLafferty M.D. Southern Illinois University I. OBJECTIVES By the end of this laboratory session the residents should be able to A. Identify the anatomic
MODULE 9 ARTERIAL AND VENOUS CATHETERIZATION Robert B. McLafferty M.D. Southern Illinois University I. OBJECTIVES By the end of this laboratory session the residents should be able to A. Identify the anatomic
DISSECTION SCHEDULE. Session I - Hip (Front) & Thigh (Superficial)
 DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
Acute Peri-Operative Pain Management Strategies
 Slide 1 Acute Peri-Operative Pain Management Strategies Phillip Gallegos, MD USAP Pinnacle Anesthesiologist Director of Anesthesia and Peri-Operative Medicine BOSHA Slide 2 ERAS Enhanced Recovery After
Slide 1 Acute Peri-Operative Pain Management Strategies Phillip Gallegos, MD USAP Pinnacle Anesthesiologist Director of Anesthesia and Peri-Operative Medicine BOSHA Slide 2 ERAS Enhanced Recovery After
Fascial Compartments of the Upper Arm
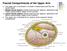 Fascial Compartments of the Upper Arm The upper arm is enclosed in a sheath of deep fascia and has two fascial septa: 1- Medial fascial septum (medial intermuscular septum): attached to the medial supracondylar
Fascial Compartments of the Upper Arm The upper arm is enclosed in a sheath of deep fascia and has two fascial septa: 1- Medial fascial septum (medial intermuscular septum): attached to the medial supracondylar
Prime movers provide the major force for producing a specific movement Antagonists oppose or reverse a particular movement Synergists
 Dr. Gary Mumaugh Prime movers provide the major force for producing a specific movement Antagonists oppose or reverse a particular movement Synergists Add force to a movement Reduce undesirable or unnecessary
Dr. Gary Mumaugh Prime movers provide the major force for producing a specific movement Antagonists oppose or reverse a particular movement Synergists Add force to a movement Reduce undesirable or unnecessary
In which arm muscle are intramuscular injections most often given? (not in text)
 AP1 Lab 9 - Muscles of the Arms and Legs Locate the following muscles on the models and on yourself. Recall anatomical position. Directional terms such as anterior, posterior, lateral, etc. all assume
AP1 Lab 9 - Muscles of the Arms and Legs Locate the following muscles on the models and on yourself. Recall anatomical position. Directional terms such as anterior, posterior, lateral, etc. all assume
Gluteal region DR. GITANJALI KHORWAL
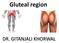 Gluteal region DR. GITANJALI KHORWAL Gluteal region The transitional area between the trunk and the lower extremity. The gluteal region includes the rounded, posterior buttocks and the laterally placed
Gluteal region DR. GITANJALI KHORWAL Gluteal region The transitional area between the trunk and the lower extremity. The gluteal region includes the rounded, posterior buttocks and the laterally placed
1-Muscles: 2-Blood supply: Branches of the profunda femoris artery. 3-Nerve supply: Sciatic nerve
 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t r i n g p a r t o r i s c h i a l p a r t ) 2-Blood supply:
1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t r i n g p a r t o r i s c h i a l p a r t ) 2-Blood supply:
Upper limb Arm & Cubital region 黃敏銓
 Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
Femoral Triangle and Adductor Canal. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Femoral Triangle and Adductor Canal Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Femoral Triangle and Adductor Canal Femoral triangle Is a triangular depressed area located in the upper
Femoral Triangle and Adductor Canal Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Femoral Triangle and Adductor Canal Femoral triangle Is a triangular depressed area located in the upper
Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block
 Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
Ultrasound Use in Anaesthesia
 Trainee Name: 1 Ultrasound Use in Anaesthesia Assessments to accompany Workbook for anaesthetic trainees in North Queensland 2010 Authors: Mark Fairley, Emile Kurukchi, Andrew Potter 2 Trainee Name: Ultrasound
Trainee Name: 1 Ultrasound Use in Anaesthesia Assessments to accompany Workbook for anaesthetic trainees in North Queensland 2010 Authors: Mark Fairley, Emile Kurukchi, Andrew Potter 2 Trainee Name: Ultrasound
57b Deep Tissue: Technique Demo and Practice - Anterior Lower Body!
 57b Deep Tissue: Technique Demo and Practice - Anterior Lower Body! 57b Deep Tissue: Technique Demo and Practice - Anterior Lower Body! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
57b Deep Tissue: Technique Demo and Practice - Anterior Lower Body! 57b Deep Tissue: Technique Demo and Practice - Anterior Lower Body! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
Sign up to receive ATOTW weekly -
 ULTRASOUND GUIDED ADDUCTOR CANAL BLOCK (SAPHENOUS NERVE BLOCK) ANAESTHESIA TUTORIAL OF THE WEEK 301 13 TH JANUARY 2014 Dr Daniel Quemby, Specialist Trainee Anaesthesia Dr Andrew McEwen, Consultant Anaesthetist
ULTRASOUND GUIDED ADDUCTOR CANAL BLOCK (SAPHENOUS NERVE BLOCK) ANAESTHESIA TUTORIAL OF THE WEEK 301 13 TH JANUARY 2014 Dr Daniel Quemby, Specialist Trainee Anaesthesia Dr Andrew McEwen, Consultant Anaesthetist
GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR
 GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR INTRODUCTION Regional block provides superior pain relief, compared
GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR INTRODUCTION Regional block provides superior pain relief, compared
Location Terms. Anterior and posterior. Proximal and Distal The term proximal (Latin proximus; nearest) describes where the appendage joins the body.
 HUMAN ANAT OMY Location Terms Anterior and posterior In human anatomical usage, anterior refers to the front of the individual. Similarly, posterior refers to the back of the subject. In standard anatomical
HUMAN ANAT OMY Location Terms Anterior and posterior In human anatomical usage, anterior refers to the front of the individual. Similarly, posterior refers to the back of the subject. In standard anatomical
Abdominal muscles. Subinguinal hiatus and ingiunal canal. Femoral and adductor canals. Neurovascular system of the lower limb. Sándor Katz M.D.,Ph.D.
 Abdominal muscles. Subinguinal hiatus and ingiunal canal. Femoral and adductor canals. Neurovascular system of the lower limb. Sándor Katz M.D.,Ph.D. External oblique muscle Origin: outer surface of the
Abdominal muscles. Subinguinal hiatus and ingiunal canal. Femoral and adductor canals. Neurovascular system of the lower limb. Sándor Katz M.D.,Ph.D. External oblique muscle Origin: outer surface of the
*the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone
 *the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone - muscles in the arm : *brachialis muscle *Biceps brachii
*the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone - muscles in the arm : *brachialis muscle *Biceps brachii
Lecture 14: The Spinal Cord
 Lecture 14: The Spinal Cord M/O Chapters 16 69. Describe the relationship(s) between the following structures: root, nerve, ramus, plexus, tract, nucleus, and ganglion. 70. Trace the path of information
Lecture 14: The Spinal Cord M/O Chapters 16 69. Describe the relationship(s) between the following structures: root, nerve, ramus, plexus, tract, nucleus, and ganglion. 70. Trace the path of information
Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore
 CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E
 Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
The posterior abdominal wall. Prof. Oluwadiya KS
 The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
3 Mohammad Al-Mohtasib Areej Mosleh
 3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
ULTRASOUND GUIDED TECHNIQUES FOR PERIOPERATIVE PAIN MANAGEMENT IN TOTAL KNEE ARTHOPLASTY
 No. 11 28 July 2017 ULTRASOUND GUIDED TECHNIQUES FOR PERIOPERATIVE PAIN MANAGEMENT IN TOTAL KNEE ARTHOPLASTY S Bobaker Moderator: Dr Y Hookamchand School of Clinical Medicine Discipline of Anaesthesiology
No. 11 28 July 2017 ULTRASOUND GUIDED TECHNIQUES FOR PERIOPERATIVE PAIN MANAGEMENT IN TOTAL KNEE ARTHOPLASTY S Bobaker Moderator: Dr Y Hookamchand School of Clinical Medicine Discipline of Anaesthesiology
