Chapter 7. Lecture Outline 7-1. Copyright (c) The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
|
|
|
- Randolph Bradford
- 6 years ago
- Views:
Transcription
1 Chapter 7 Lecture Outline 7-1 Copyright (c) The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
2 Bone Tissue tissues and organs of the skeletal system histology of osseous tissue bone development physiology of osseous tissue bone disorders 7-2
3 Bone as a Tissue osteology the study of bone skeletal system - composed of bones, cartilages, and ligaments form strong flexible framework of the body cartilage forerunner of most bones covers many joint surfaces of mature bone ligaments hold bones together at the joints tendons attach muscle to bone 7-3
4 Functions of the Skeleton support hold the body up, supports muscles, mandible and maxilla support teeth protection brain, spinal cord, heart, lungs movement limb movements, breathing, action of muscle on bone electrolyte balance calcium and phosphate ions acid-base balance buffers blood against excessive ph changes blood formation red bone marrow is the chief producer of blood cells 7-4
5 Bones and Osseous Tissue bone (osseous tissue) - connective tissue with the matrix hardened by calcium phosphate and other minerals mineralization or calcification the hardening process of bone individual bones consist of bone tissue, bone marrow, cartilage, adipose tissue, nervous tissue, and fibrous connective tissue continually remodels itself and interacts physiologically with all of the other organ systems of the body permeated with nerves and blood vessels, which attests to its sensitivity and metabolic activity 7-5
6 Shapes of Bones Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Flat bones Scapula Short bones Capitate (carpal) bone Talus Sternum Ulna Irregular bones Sphenoid bone Radius Vertebra Long bones Femur Figure 7.1 long bones longer than wide rigid levers acted upon by muscles short bones equal in length and width glide across one another in multiple directions flat bones protect soft organs curved but wide & thin irregular bones elaborate shapes that don t fit into the other categories 7-6
7 General Features of Bones compact (dense) bone outer shell of long bone diaphysis (shaft) - cylinder of compact bone to provide leverage medullary cavity (marrow cavity) - space in the diaphysis of a long bone that contains bone marrow epiphyses - enlarged ends of a long bone enlarged to strengthen joint and attach ligaments and tendons spongy (cancellous) bone covered by more durable compact bone skeleton about three-fourths compact and one-fourth spongy bone by weight spongy bone found in ends of long bones, and the middle of nearly all others articular cartilage a layer of hyaline cartilage that covers the joint surface where one bone meets another allows joint to move more freely and relatively friction free nutrient foramina minute holes in the bone surface that allows blood vessels to penetrate 7-7
8 General Features of Bones periosteum external sheath that covers bone except where there is articular cartilage outer fibrous layer of collagen some outer fibers continuous with the tendons that attach muscle to bone perforating (Sharpey s) fibers other outer fibers that penetrate into the bone matrix strong attachment and continuity from muscle to tendon to bone inner osteogenic layer of bone forming cells important to growth of bone and healing of fractures endosteum thin layer of reticular connective tissue lining marrow cavity has cells that dissolve osseous tissue and others that deposit it epiphyseal plate (growth plate) area of hyaline cartilage that separates the marrow spaces of the epiphysis and diaphysis enables growth in length epiphyseal line in adults, a bony scar that marks where growth plate used to be 7-8
9 Structure of a Long Bone Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Periosteum Nutrient foramen Site of endosteum Compact bone Spongy bone Epiphyseal line Diaphysis Epiphysis epiphyses and diaphysis compact and spongy bone marrow cavity articular cartilage periosteum Articular cartilage (a) Living (b) Dried Figure
10 Structure of a Flat Bone Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Figure 7.3 Suture Outer compact bone Spongy bone (diploe) Trabeculae Inner compact bone sandwich-like construction two layers of compact bone enclosing a middle layer of spongy bone both surfaces of flat bone covered with periosteum diploe spongy layer in the cranium absorbs shock marrow spaces lined with endosteum 7-10
11 Histology of Osseous Tissue Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Osteogenic cell Osteoblast Osteocyte Rough endoplasmic reticulum Nucleus Secretory vesicles Mitochondrion (a) Osteocyte development Figure 7.4a bone is connective tissue that consists of cells, fibers and ground substance four principal types of bone cells osteogenic (osteoprogenator) cells osteoblasts osteocytes osteoclasts osteogenic (osteoprogenator) cells - stem cells found in endosteum, periosteum, and in central canals arise from embryonic mesenchymal cells multiply continuously to produce new osteoblasts 7-11
12 Histology of Osseous Tissue osteoblasts bone forming cells line up as single layer of cells under endosteum and periosteum are nonmitotic synthesize soft organic matter of matrix which then hardens by mineral deposition stress and fractures stimulate osteogenic cells to multiply more rapidly and increase number of osteocytes to reinforce or rebuild bone secrete osteocalcin thought to be the structural protein of bone stimulates insulin secretion of pancreas increases insulin sensitivity in adipocytes which limit the growth of adipose tissue osteocytes former osteoblasts that have become trapped in the matrix they have deposited lacunae tiny cavities where osteocytes reside canaliculi little channels that connect lacunae cytoplasmic processes reach into canaliculi some osteocytes reabsorb bone matrix while others deposit it contribute to homeostatic mechanism of bone density and calcium and phosphate ions when stressed, produce biochemical signals that regulate bone remodeling 7-12
13 Cells of Osseous Tissue Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Stem cells Fusion Nuclei Osteoclast Osseous tissue Periosteum Osteoclast Osteocyte Resorption bay Lysosomes Ruffled border (b) Osteoclast development Figure 7.4b osteoclasts bone-dissolving cells found on the bone surface osteoclasts develop from same bone marrow stem cells that give rise to blood cells different origin from rest of bone cells unusually large cells formed from the fusion of several stem cells typically have 3 to 4 nuclei, may have up to 50 ruffled border side facing bone surface several deep infoldings of the plasma membrane which increases surface area and resorption efficiency resorption bays (Howship lacunae) pits on surface of bone where osteoclasts reside remodeling results from combined action of the bone-dissolving osteoclasts and the bone-depositing osteoblasts 7-13
14 The Matrix matrix of osseous tissue is, by dry weight, about one-third organic and two-thirds inorganic matter organic matter synthesized by osteoblasts collagen, carbohydrate protein complexes, such as glycosaminoglycans, proteoglycans, and glycoproteins inorganic matter 85% hydroxyapatite (crystallized calcium phosphate salt) 10% calcium carbonate other minerals (fluoride, sodium, potassium, magnesium) bone is a composite combination of two basic structural materials, a ceramic and a polymer combines optimal mechanical properties of each component bone combines the polymer, collagen, with the ceramic, hydroxyapatite and other minerals ceramic portion allows the bone to support the body weight, and protein portion gives bone some degree of flexibility rickets soft bones due to deficiency of calcium salts osteogenesis imperfecta or brittle bone disease excessively brittle bones due to lack of protein, collagen 7-14
15 Histology of Compact and Spongy Bone Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Bone marrow Trabecula Pelvic bone Head of femur Spongy bone Compact bone (a) Figure 7.5a (c) Figure 7.5c Lamella Lacunae Canaliculi Central canal (d) 20 m a,c: Dr. Don W. Fawcett/Visuals Unlimited; d: Visuals Unlimited Figure 7.5d 7-15
16 Compact Bone osteon (haversian system) the basic structural unit of compact bone formed by a central canal and its concentric lamella connected to each other by canaliculi a cylinder of tissue around a central canal perforating (Volkmann) canals are transverse or diagonal passages along the length of the osteon collagen fibers corkscrew down the matrix of the lamella giving it a helical arrangement helices coil in one direction in one lamella and in the opposite direction in the next lamella for added strength blood flow - skeleton receives about half a liter of blood per minute nutrient foramina on the surface of bone tissue that allow blood vessels and nerves to enter the bone open into the perforating canals that cross the matrix and feed into the central canals innermost osteocytes near central canal receive nutrients and pass them along through their gap junction to neighboring osteocytes they also receive wastes from their neighbors and transfer them to the central canal maintaining a two-way flow of nutrients and waste not all of the matrix is organized into osteons circumferential lamellae - inner and outer boundaries of dense bone run parallel to bone surface interstitial lamellae remains of old osteons that broke down as bone grew and remodeled itself 7-16
17 Blood Vessels of Bone Spicules Trabeculae Spongy bone Central canal Lacuna Collagen fibers Concentric lamellae Circumferential lamellae (b) Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Figure 7.5b Nerve Blood vessel Endosteum Periosteum Perforating fibers Perforating canal Osteon nutrient foramina on bone surface perforating (Volkmann s) canals transverse or diagonal canals central canals vertical canals circumferential lamellae interstitial lamellae 7-17
18 Spongy Bone sponge-like appearance spongy bone consists of: slivers of bone called spicules thin plates of bone called trabeculae spaces filled with red bone marrow few osteons and no central canals all osteocytes close to bone marrow provides strength with minimal weight trabeculae develop along bone s lines of stress 7-18
19 Design of Spongy Bone Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Greater trochanter Head Trabeculae of spongy bone Compact bone Lines of stress Shaft (diaphysis) Robert Calentine/Visuals Unlimited Figure
20 Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Bone Marrow bone marrow general term for soft tissue that occupies the marrow cavity of a long bone and small spaces amid the trabeculae of spongy bone red marrow (myeloid tissue) in nearly every bone in a child hemopoietic tissue - produces blood cells and is composed of multiple tissues in a delicate, but intricate arrangement that is an organ to itself in adults, found in skull, vertebrae, ribs, sternum, part of pelvic girdle, and proximal heads of humerus and femur Figure 7.7 yellow marrow found in adults most red marrow turns into fatty yellow marrow no longer produces blood 7-20
21 Bone Development ossification or osteogenesis the formation of bone in the human fetus and infant, bone develops by two methods: intramembranous ossification endochondral ossification 7-21
22 Intramembranous Ossification intramembranous ossification produce the flat bones of the skull and most of the clavicle (collar bone) these bones develop within a fibrous sheet similar to epidermis of the skin (dermal bones) mesenchyme embryonic connective tissue condenses into a layer of soft tissue with dense supply of blood capillaries mesenchymal cells differentiate into osteogenic cells regions of mesenchyme become a network of soft sheets trabeculae osteogenic cells differentiate into osteoblasts these cells deposit organic matrix osteoid tissue as trabeculae grow thicker, calcium phosphate is deposited in the matrix mesenchyme close to the surface of a trabecula remains uncalcified becomes denser and more fibrous, forming periosteum osteoblasts continue to deposit minerals producing a honeycomb of bony trabeculae some persist as permanent spongy bone osteoclasts resorb and remodel others to form a marrow cavity in the middle of bone trabeculae at the surface continue to calcify until the spaces between them are filled in, converting spongy bone to compact bone gives rise to the sandwich-like arrangement of mature flat bone 7-22
23 Intramembranous Ossification Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Mesenchymal cell Osteocyte Osteoblasts Sheet of condensing mesenchyme Blood capillary Trabecula Calcified bone Osteoid tissue Fibrous periosteum 1 Condensation of mesenchyme into soft sheet permeated with blood capillaries 2 Deposition of osteoid tissue by osteoblasts on mesenchymal surface; entrapment of first osteocytes; formation of periosteum Osteoblasts Trabeculae Osteocytes Marrow cavity Fibrous periosteum Osteoblasts Spongy bone Compact bone 3 Honeycomb of bony trabeculae formed by 4 continued mineral deposition; creation of spongy bone Surface bone filled in by bone deposition, Figure 7.8 converting spongy bone to compact bone. Persistence of spongy bone in the middle layer. produces flat bones of skull and clavicle 7-23
24 Intramembranous Ossification Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Periosteum: Fibrous layer Osteogenic layer Osteoid tissue Osseous tissue (bone) Osteoblasts Osteocytes Ken Saladin note the periosteum and osteoblasts. Figure
25 Endochondral Ossification endochondral ossification process in which bone develops from preexisting cartilage model beginning the 6 th fetal week and ending in early 20 s most bones develop by this process mesenchyme develops into a body of hyaline cartilage in location of future bone covered with fibrous perichondrium perichondrium produces chondrocytes initially, and later produces osteoblasts osteoblasts form a bony collar around middle of cartilage model former perichondrium is now considered to be periosteum primary ossification center - chondrocytes in the middle of the model enlarge matrix between lacunae are reduced to thin walls walls of this thin matrix ossify and block nutrients from reaching chondrocytes they die and their lacunae merge into a single cavity in the middle of the model blood vessels penetrate the bony collar and invade primary ossification center primary marrow cavity forms from blood and stem cells filling hollow cavity 7-25
26 Primary Ossification Center and Primary Marrow Cavity Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Secondary ossification center Enlarging chondrocytes Bony collar Primary ossification center Primary marrow cavity Periosteum 2 Formation of primary ossification center, bony collar, and periosteum Figure 7.10 (2-3) 3 Vascular invasion, formation of primary marrow cavity, and appearance of secondary ossification center 7-26
27 Endochondral Ossification blood vessels penetrate the bony collar and invade primary ossification center primary marrow cavity forms from blood and stem cells filling hollow cavity stem cells give rise to osteoblasts and osteoclasts osteoblasts line cavity and deposit osteoid tissue and calcify it forming temporary network of trabeculae wave of cartilage death progresses toward the ends osteoclasts follow the wave dissolving the cartilage remnants enlarging the marrow cavity metaphysis region of transition from cartilage to bone at each end of primary marrow cavity secondary ossification center created by chondrocyte enlargement and death in the epiphyses become hollowed out by the same process generating a secondary marrow cavity in epiphyses cavity expands outward from the center in all directions 7-27
28 Secondary Ossification Centers and Secondary Marrow Cavities Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Articular cartilage Spongy bone Epiphyseal line Secondary marrow cavity Epiphyseal plate Periosteum Epiphysis Metaphysis Nutrient foramen Marrow cavity Blood vessel Diaphysis Compact bone Secondary ossification center Metaphysis Cartilage 4 Bone at birth, with 5 Bone of child, with 6 enlarged primary epiphyseal plate at marrow cavity and distal end appearance of secondary marrow cavity in one epiphysis Adult bone with a single marrow cavity and closed epiphyseal plate Figure 7.10 (4-6) 7-28
29 Endochondral Ossification during infancy and childhood, the epiphyses fill with spongy bone cartilage limited to the articular cartilage covering each joint surface, and to the epiphyseal plate a thin wall of cartilage separating the primary and secondary marrow cavities epiphyseal plate persists through childhood and adolescence serves as a growth zone for bone elongation by late teens to early twenties, all remaining cartilage in the epiphyseal plate is generally consumed gap between epiphyses and diaphysis closes primary and secondary marrow cavities unite into a single cavity bone can no longer grow in length 7-29
30 Stages of Endochondral Ossification Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Articular cartilage Spongy bone Epiphyseal line 1 2 Perichondrium Hyaline cartilage Early cartilage model Enlarging chondrocytes Bony collar Primary ossification center Periosteum Formation of primary ossification center, bony collar, and periosteum Secondary ossification center Blood vessel Primary marrow cavity Secondary marrow cavity Epiphysis Metaphysis Diaphysis Secondary ossification center Epiphyseal plate Nutrient foramen Compact bone Metaphysis Cartilage 3 Vascular invasion, 4 Bone at birth, with 5 Bone of child, with 6 epiphyseal plate at distal end formation of primary marrow cavity, and appearance of secondary ossification center enlarged primary marrow cavity and appearance of secondary marrow cavity in one epiphysis Adult bone with a single marrow cavity and closed epiphyseal plate Figure 7.10 Periosteum Marrow cavity 7-30
31 Cartilaginous Epiphyseal Plates Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Diaphysis Epiphysis Epiphyseal plate Metacarpal bone Epiphyseal plates Courtesy of Utah Valley Regional Medical Center, Department of Radiology Figure
32 Bone Growth and Remodeling ossification continues throughout life with the growth and remodeling of bones bones grow in two directions: length and width bone elongation epiphyseal plate a region of transition from cartilage to bone functions as growth zone where the bones elongate consists of typical hyaline cartilage in the middle with a transition zone on each side where cartilage is being replaced by bone metaphysis is the zone of transition facing the marrow cavity 7-32
33 Histology of Metaphysis zone of reserve cartilage typical hyaline cartilage farthest from marrow cavity shows no sign of transforming into bone zone of proliferation chondrocytes multiply forming columns of flat lacunae zone of hypertrophy chondrocyte enlargement matrix between lacunae become very thin zone of calcification mineral deposited in the matrix between columns of lacunae temporary support for cartilage zone of bone deposition chondrocytes die, longitudinal columns fill with osteoblasts and blood vessels, osteoclasts dissolve the calcified cartilage osteons and spongy bone are created by osteoblasts 7-33
34 Zones of the Metaphysis Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Zone 1 Zone 5 Multiplying chondrocytes Enlarging chondrocytes Breakdown of lacunae Calcifying cartilage Bone marrow Osteoblasts Osteocytes Trabeculae of spongy bone Victor Eroschenko Zone of reserve cartilage Typical histology of resting hyaline cartilage Zone of cell proliferation Chondrocytes multiplying and lining up in rows of small flattened lacunae Zone of cell hypertrophy Cessation of mitosis; enlargement of chondrocytes and thinning of lacuna walls Zone of calcification Temporary calcification of cartilage matrix between columns of lacunae Zone of bone deposition Breakdown of lacuna walls, leaving open channels; death of chondrocytes; bone deposition by osteoblasts, forming trabeculae of spongy bone Figure
35 Fetal Skeleton at 12 Weeks Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cranial bones Mandible Humerus Radius Ulna Vertebrae Scapula Ribs Femur Pelvis Biophoto Associates/Photo Researchers, Inc. Figure
36 Bone Growth and Remodeling interstitial growth - bones increase in length bone elongation is really a result of cartilage growth within epiphyseal plate epiphyses close when cartilage is gone epiphyseal line length-wise growth is finished occurs at different ages in different bones appositional growth - bones increase in width throughout life the deposition of new bone at the surface osteoblasts on deep side of periosteum deposit osteoid tissue Become trapped as tissue calcifies lay down matrix in layers parallel to surface forms circumferential lamellae over surface osteoclasts of endosteum enlarge marrow cavity bone remodeling occurs throughout life - 10% per year repairs microfractures, releases minerals into blood, reshapes bones in response to use and disuse Wolff s law of bone - architecture of bone determined by mechanical stresses placed on it and bones adapt to withstand those stresses remodeling is a collaborative and precise action of osteoblasts and osteoclasts bony processes grow larger in response to mechanical stress 7-36
37 Dwarfism Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. achondroplastic dwarfism long bones stop growing in childhood normal torso, short limbs failure of cartilage growth in metaphysis spontaneous mutation produces mutant dominant allele The McGraw-Hill Companies, Inc./Joe DeGrandis, photographer Figure 7.14 pituitary dwarfism lack of growth hormone normal proportions with short stature 7-37
38 Physiology of Osseous Tissue a mature bone remains a metabolically active organ involved in its own maintenance of growth and remodeling exerts a profound influence over the rest of the body by exchanging minerals with tissue fluid disturbance of calcium homeostasis in skeleton disrupts function of other organ systems especially nervous and muscular 7-38
39 Mineral Deposition mineral deposition (mineralization) - a crystallization process in which calcium phosphate, and other ions are taken from the blood plasma and deposited in bone tissue osteoblasts produce collagen fibers that spiral the length of the osteon fibers become encrusted with minerals that harden the matrix calcium and phosphate (hydroxyapatite) from blood plasma are deposited along the fibers the calcium and phosphate ion concentration must reach a critical value called the solubility product for crystal formation to occur most tissues have inhibitors to prevent this so they do not become calcified osteoblasts neutralize these inhibitors and allow salts to precipitate in the bone matrix first few crystals (seed crystals) attract more calcium and phosphate from solution abnormal calcification (ectopic ossification) may occur in lungs, brain, eyes, muscles, tendons or arteries (arteriosclerosis) 7-39 calculus calcified mass in an otherwise soft organ such as the lung
40 Mineral Resorption mineral resorption the process of dissolving bone and releasing minerals into the blood performed by osteoclasts at the ruffled border hydrogen pumps in membrane secrete hydrogen into space between the osteoclast and bone surface chloride ions follow by electrical attraction hydrochloric acid (ph 4) dissolves bone minerals acid phosphatase enzyme digests the collagen orthodontic appliances (braces) reposition teeth tooth moves because osteoclasts dissolve bone ahead of the tooth, where the pressure on the bone is the greatest osteoblasts deposit bone more slowly in the low-pressure zone behind the tooth 7-40
41 Calcium Homeostasis calcium and phosphate are used for much more than bone structure phosphate is a component of DNA, RNA, ATP, phospholipids, and ph buffers calcium needed in neuron communication, muscle contraction, blood clotting, and exocytosis minerals are deposited in the skeleton and withdrawn when they are needed for other purposes about 1100g of calcium in adult body 99% in the skeleton as easily exchangeable calcium ions and more stable hydroxyapatite reserve 18% of adult skeleton exchanged with blood each year normal calcium concentration in blood plasma is normally 9.2 to 10.4 mg/dl 45% as Ca 2+ can diffuse across capillary walls and affect other tissues rest in reserve, bound to plasma proteins hypocalcemia - blood calcium deficiency causes excess excitability of muscle, tremors, spasms or tetany (inability to relax) Na + enters cells too easily and excites nerves and muscles hypercalcemia - blood calcium excess sodium channels less responsive and nerve and muscle less excitable than 7-41 normal (sluggish reflexes, depression)
42 Carpopedal Spasm Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Figure 7.15 hypocalcemia demonstrated by muscle spasm of hands and feet 7-42
43 hypercalcemia is rare Ion Imbalances hypocalcemia has a wide variety of causes vitamin D deficiency diarrhea thyroid tumors underactive parathyroids pregnancy and lactation accidental removal of parathyroid glands during thyroid surgery calcium homeostasis depends on a balance between dietary intake, urinary and fecal loses, and exchanges between osseous tissue calcium homeostasis is regulated by three hormones: calcitriol, calcitonin, and parathyroid hormone 7-43
44 Hormonal Control of Calcium Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Calcium Intake and Excretion Blood Bone Dietary requirement 1,000 mg/day Digestive tract Absorption by digestive tract Calcitriol Deposition by osteoblasts Calcitonin (weak effect) Ca 2+ ( mg/dl) Hydroxyapatite Ca 10 (PO 4 ) 6 (OH) 2 Kidneys Filtration by kidneys Resorption by osteoclasts Calcium carbonate CaCO 3 Reabsorption by kidneys Calcitriol PTH Calcitriol (weak effect) PTH Fecal loss 350 mg/day Urinary loss 650 mg/day Figure 7.17 calcitriol, calcitonin, and PTH maintain normal blood calcium concentration 7-44
45 Calcitriol (Activated Vitamin D) calcitriol a form of vitamin D produced by the sequential action of the skin, liver, and kidneys produced by the following process: epidermal keratinocytes use UV radiation to convert a steroid, 7-dehydrocholesterol to previtamin D 3 liver adds a hydroxyl group converting it to calcidiol kidneys adds another hydroxyl group, converting that to calcitriol (most active form of vitamin D) also from fortified milk calcitriol behaves as a hormone that raises blood calcium concentration increases calcium absorption by small intestine increases calcium resorption from the skeleton increases stem cell differentiation into osteoclasts which liberates calcium and phosphate from bone promotes kidney reabsorption of calcium ions, so less lost in urine necessary for bone deposition need adequate calcium and phosphate abnormal softness of bones (rickets) in children and (osteomalacia) in adults without adequate vitamin D 7-45
46 Calcitriol Synthesis and Action Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. 7-dehydrocholesterol HO Ultraviolet light Vitamin D 3 (cholecalciferol) CH 2 HO Bone resorption Calcidiol CH 2 OH Reduced excretion of Ca 2+ HO OH CH 2 Calcitriol Absorption of Ca 2+ and phosphate HO OH Figure
47 Calcitonin calcitonin - secreted by C cells (clear cells) of the thyroid gland when calcium concentration rises too high lowers blood calcium concentration in two ways: osteoclast inhibition reduces osteoclast activity as much as 70% less calcium liberated from bones osteoblast stimulation increases the number and activity of osteoblasts deposits calcium into the skeleton important in children, weak effect in adults osteoclasts more active in children due to faster remodeling deficiency does not cause disease in adults reduces bone loss in women during pregnancy & lactation 7-47
48 Correction for Hypercalcemia Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Blood Ca 2+ excess Blood Ca 2+ returns to normal Calcitonin secretion Reduced osteoclast activity Less bone resorption (a) Correction for hypercalcemia Increased osteoblast activity More bone deposition Figure 7.18a 7-48
49 Parathyroid Hormone parathyroid hormone (PTH) secreted by the parathyroid glands which adhere to the posterior surface of thyroid gland PTH released with low calcium blood levels PTH raises calcium blood level by four mechanisms binds to receptors on osteoblasts stimulating them to secrete RANKL which raises the osteoclast population promotes calcium reabsorption by the kidneys, less lost in urine promotes the final step of calcitriol synthesis in the kidneys, enhancing calcium raising effect of calcitriol inhibits collagen synthesis by osteoblasts, inhibiting bone deposition sporadic injection or secretion of low levels of PTH causes bone deposition, and can increase bone mass 7-49
50 Correction for Hypocalcemia Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Blood Ca 2+ deficiency Blood Ca 2+ returns to normal Parathyroid hormone secretion Increased osteoclast activity More bone resorption Reduced osteoblast activity Less bone deposition More urinary phosphate excretion Prevention of hydroxyapatite formation Less urinary calcium excretion (b) Correction for hypocalcemia Conservation of calcium Figure 7.18b 7-50
51 Phosphate Homeostasis average adult has g of phosphorus 85-90% of phosphate is in the bones normal plasma concentration is mg/dl occurs in two principal forms: HPO 4 2- and H 2 PO 4- (monohydrogen & dihydrogen phosphate ions) phosphate levels are not regulated as tightly as calcium levels no immediate functional disorders calcitriol promotes its absorption by small intestine & promotes bone deposition PTH lowers blood phosphate level by promoting its urinary excretion 7-51
52 Other Factors Affecting Bone at least 20 or more hormones, vitamins, and growth factors affect osseous tissue bone growth especially rapid in puberty & adolescence surges of growth hormone, estrogen, and testosterone occur and promote ossification these hormones stimulate multiplication of osteogenic cells, matrix deposition by osteoblasts, and chondrocyte multiplication and hypertrophy in metaphyses girls grow faster than boys and reach full height earlier estrogen stronger effect than testosterone on bone growth males grow for a longer time and taller anabolic steroids cause growth to stop epiphyseal plate closes prematurely results in abnormally short adult stature 7-52
53 Fractures and Their Repair stress fracture break caused by abnormal trauma to a bone falls, athletics, and military combat pathological fracture break in a bone weakened by some other disease bone cancer or osteoporosis usually caused by stress that would not break a healthy bone fractures classified by structural characteristics direction of fracture line break in the skin multiple pieces 7-53
54 Types of Bone Fractures Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. (a) Nondisplaced (c) Comminuted (d) Greenstick a: Custom Medical Stock Photo, Inc.; c: Lester V. Bergman/Corbis; d: Custom Medical Stock Photo, Inc. Figure
55 Healing of Fractures uncomplicated fractures normally 8-12 weeks longer in elderly stages of healing bone fractures fracture hematoma and granulation tissue bleeding of a broken bone forms a clot fracture hematoma blood capillaries, fibroblasts, macrophages, osteoclasts, and osteogenic cells invade clot granulation tissue soft fibrous mass produced by capillary and cellular invasion after about 48 hours after injury soft callus formation formed by fibroblasts and chondroblasts depositing collagen and fibrocartilage into granulation tissue conversion to hard callus osteoblasts produce a bony collar in 6 weeks called a hard callus hard callus is cemented to dead bone around the injury site and acts as a temporary splint to join broken ends together 4-6 weeks for hard callus to form and immobilization is necessary remodeling hard callus persists for 3 4 months osteoclasts dissolve fragments of broken bone osteoblasts deposit spongy bone to bridge to gap between the broken ends, transformed gradually into compact bone that is thicker in fracture area 7-55
56 Healing of Fractures Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Marrow cavity Hematoma Compact bone Fibrocartilage Soft callus New blood vessels Hard callus Spongy bone 1 Hematoma formation 2 Soft callus formation 3 Hard callus formation 4 The hematoma is converted Deposition of collagen and to granulation tissue by invasion fibrocartilage converts granulation of cells and blood capillaries. tissue to a soft callus. Osteoblasts deposit a temporary bony collar around the fracture to unite the broken pieces while ossification occurs. Bone remodeling Small bone fragments are removed by osteoclasts, while osteoblasts deposit spongy bone and then convert it to compact bone. Figure
57 Treatment of Fractures closed reduction procedure in which the bone fragments are manipulated into their normal positions without surgery open reduction involves surgical exposure of the bone and the use of plates, screws, or pins to realign the fragments cast normally used to stabilize and immobilize healing bone traction used to treat fractures of the femur in children aligns bone fragments by overriding force of the strong thigh muscles risks long-term confinement to bed rarely used for the elderly hip fractures are usually pinned in elderly and early ambulation (walking) is encouraged to promote blood circulation and healing electrical stimulation accelerates repair suppresses the effects of parathyroid hormone orthopedics the branch of medicine that deals with prevention and correction of injuries and disorders of the bones, joints, and muscles 7-57
58 Fractures and Their Repairs Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. SIU/Visuals Unlimited; 7.22a: Michael Klein/Peter Arnold, Inc. Figure
59 Osteoporosis osteoporosis the most common bone disease severe loss of bone density bones lose mass and become brittle due to loss of organic matrix and minerals affects spongy bone the most since it is the most metabolically active subject to pathological fractures of hip, wrist and vertebral column kyphosis (widow s hump) deformity of spine due to vertebral bone loss complications of loss of mobility are pneumonia and thrombosis postmenopausal white women at greatest risk begin to lose bone mass as early as 35 yoa by age 70, average loss is 30% of bone mass risk factors - race, age, gender, smoking, diabetes mellitus, diets poor in calcium, protein, vitamins C and D 7-59
60 Osteoporosis estrogen maintains density in both sexes inhibits resorption by osteoclasts testes and adrenals produce estrogen in men in women, rapid bone loss after menopause since estrogen blood level drops below 30 ng/ml osteoporosis is common in young female athletes with low body fat causing them to stop ovulating and ovarian estrogen secretion is low treatments estrogen replacement therapy (ERT) slows bone resorption, but increases risk of breast cancer, stroke and heart disease drugs Fosamax/Actonel destroys osteoclasts PTH slows bone loss if given as daily injection Forteo (PTH derivative) increases density by 10% in 1 year may promote bone cancer so use is limited to 2 years best treatment is prevention - exercise and calcium intake (1000 mg/day) between ages 25 and
61 Spinal Osteoporosis Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. (a) a: Michael Klein/Peter Arnold, Inc.; b: Dr. P. Marzzi/Photo Researchers, Inc. (b) Figure 7.22 a-b 7-61
Fig Articular cartilage. Epiphysis. Red bone marrow Epiphyseal line. Marrow cavity. Yellow bone marrow. Periosteum. Nutrient foramen Diaphysis
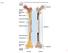 Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Chapter 6. Bone Tissue
 Chapter 6 Bone Tissue Functions of the Skeleton support hold the body up, supports muscles, mandible and maxilla support teeth protection brain, spinal cord, heart, lungs movement limb movements, breathing,
Chapter 6 Bone Tissue Functions of the Skeleton support hold the body up, supports muscles, mandible and maxilla support teeth protection brain, spinal cord, heart, lungs movement limb movements, breathing,
Functions of the Skeletal System. Chapter 6: Osseous Tissue and Bone Structure. Classification of Bones. Bone Shapes
 Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over 3 Weeks. A SEPARATE WORKSHEET WILL BE PROVIDED.
 BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
Chapter 07 Lecture Outline
 Chapter 07 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright McGraw-Hill Education. Permission required for reproduction or
Chapter 07 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright McGraw-Hill Education. Permission required for reproduction or
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS
 OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues
 An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
The Skeletal System:Bone Tissue
 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
Chapter 6: Osseous Tissue and Bone Structure
 Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
CHAPTER 6 LECTURE OUTLINE
 CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
SKELETAL SYSTEM CHAPTER 07. Bone Function BIO 211: ANATOMY & PHYSIOLOGY I. Body Movement interacts with muscles bones act as rigid bar of a lever
 Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
SKELETAL SYSTEM CHAPTER 07 BIO 211: ANATOMY & PHYSIOLOGY I
 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
The Skeletal System:Bone Tissue
 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
ANATOMY & PHYSIOLOGY - CLUTCH CH. 8 - BONE AND CARTILAGE.
 !! www.clutchprep.com CONCEPT: BONE CLASSIFICATIONS There are four classifications of bones based on their 1. Long bones are greater in length than in width - Found in the upper and lower limbs (ex: arm,
!! www.clutchprep.com CONCEPT: BONE CLASSIFICATIONS There are four classifications of bones based on their 1. Long bones are greater in length than in width - Found in the upper and lower limbs (ex: arm,
Chapter 6: Skeletal System: Bones and Bone Tissue
 Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
BIOH111. o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system
 BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
Osseous Tissue and Bone Structure
 C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
BONE TISSUE. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
Skeletal System. The skeletal System... Components
 Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM
 ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
Chapter 6 Bones and Bone Tissue Chapter Outline
 Chapter 6 Bones and Bone Tissue Chapter Outline Module 6.1: Introduction to Bones as Organs (Figures 6.1, 6.2, 6.3, 6.4) A. The skeletal system includes the bones, joints, and their associated supporting
Chapter 6 Bones and Bone Tissue Chapter Outline Module 6.1: Introduction to Bones as Organs (Figures 6.1, 6.2, 6.3, 6.4) A. The skeletal system includes the bones, joints, and their associated supporting
Skeletal Tissues. Skeletal tissues. Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs.
 Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
Due in Lab. Due next week in lab - Scientific America Article Select one article to read and complete article summary
 Due in Lab 1. Skeletal System 33-34 2. Skeletal System 26 3. PreLab 6 Due next week in lab - Scientific America Article Select one article to read and complete article summary Cell Defenses and the Sunshine
Due in Lab 1. Skeletal System 33-34 2. Skeletal System 26 3. PreLab 6 Due next week in lab - Scientific America Article Select one article to read and complete article summary Cell Defenses and the Sunshine
SKELETAL SYSTEM. Introduction Notes (pt 1)
 SKELETAL SYSTEM Introduction Notes (pt 1) I. INTRODUCTION 1. Bones include active, living tissues: bone tissue, cartilage, dense connective tissue, blood, and nervous tissue. 2. Bones: support and protect
SKELETAL SYSTEM Introduction Notes (pt 1) I. INTRODUCTION 1. Bones include active, living tissues: bone tissue, cartilage, dense connective tissue, blood, and nervous tissue. 2. Bones: support and protect
What are the parts of the skeletal system? Chapter 6- Part I Bones and Skeletal Tissues. Growth of Cartilage. Bones come in many shapes
 Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
Biology. Dr. Khalida Ibrahim
 Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
SKELETAL TISSUES CHAPTER 7 INTRODUCTION TO THE SKELETAL SYSTEM TYPES OF BONES
 SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
BIOL 2457 CHAPTER 6 SI 1. irregular ectopic: sutural (Wormian) The is between the shaft and end. It contains cartilage that is
 BIOL 2457 CHAPTER 6 SI 1 1. List 5 functions of bones: 2. Classify bones according to shape: give descriptions and examples: long short flat irregular ectopic: sutural (Wormian) ectopic: sesamoid 3. The
BIOL 2457 CHAPTER 6 SI 1 1. List 5 functions of bones: 2. Classify bones according to shape: give descriptions and examples: long short flat irregular ectopic: sutural (Wormian) ectopic: sesamoid 3. The
Osteology. Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College
 Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
2 PROCESSES OF BONE OSSIFICATION
 2 PROCESSES OF BONE OSSIFICATION ENDOCHONDRAL OSSIFICATION 6 STEPS 1. CARTILAGE ENLARGES, BY APPOSITIONAL GROWTH; CHONDROCYTES AT CENTER OF CARTILAGE GROW IN SIZE; MATRIX REDUCES IN SIZE & SPICULES CALCIFY;
2 PROCESSES OF BONE OSSIFICATION ENDOCHONDRAL OSSIFICATION 6 STEPS 1. CARTILAGE ENLARGES, BY APPOSITIONAL GROWTH; CHONDROCYTES AT CENTER OF CARTILAGE GROW IN SIZE; MATRIX REDUCES IN SIZE & SPICULES CALCIFY;
b. Adult bones produce 2.5 million RBCs each second.
 Ch 6 Skeletal System I. Functions of the Skeletal System A. The skeletal system consists of: 1. bones, cartilage, tendons and ligaments B. Living bone is not Gr. dried up 1. It is dynamic and adaptable
Ch 6 Skeletal System I. Functions of the Skeletal System A. The skeletal system consists of: 1. bones, cartilage, tendons and ligaments B. Living bone is not Gr. dried up 1. It is dynamic and adaptable
Chapter 7. Skeletal System
 Chapter 7 Skeletal System 1 Introduction: A. Bones are very active, living tissues B. Each bone is made up of several types of tissues and so is an organ. C. Bone functions include: muscle attachment,
Chapter 7 Skeletal System 1 Introduction: A. Bones are very active, living tissues B. Each bone is made up of several types of tissues and so is an organ. C. Bone functions include: muscle attachment,
Skeletal System. Chapter 6.1 Human Anatomy & Physiology
 Skeletal System Chapter 6.1 Human Anatomy & Physiology Overview of Skeletal System Bones Joints Skeletal System Cartilage Tendons (bone to muscle) Ligaments (bone to bone) Function of the Skeletal System
Skeletal System Chapter 6.1 Human Anatomy & Physiology Overview of Skeletal System Bones Joints Skeletal System Cartilage Tendons (bone to muscle) Ligaments (bone to bone) Function of the Skeletal System
Osseous Tissue and Bone Structure
 6 Osseous Tissue and Bone Structure PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Skeletal System Learning Outcomes 6-1 Describe the primary
6 Osseous Tissue and Bone Structure PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Skeletal System Learning Outcomes 6-1 Describe the primary
Chapter 6: SKELETAL SYSTEM
 Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
PowerPoint Lecture Slides. Prepared by Patty Bostwick-Taylor, Florence-Darlington Technical College. The Skeletal System Pearson Education, Inc.
 PowerPoint Lecture Slides Prepared by Patty Bostwick-Taylor, Florence-Darlington Technical College CHAPTER 5 The Skeletal System 2012 Pearson Education, Inc. Title Classification of Bones and Gross Anatomy
PowerPoint Lecture Slides Prepared by Patty Bostwick-Taylor, Florence-Darlington Technical College CHAPTER 5 The Skeletal System 2012 Pearson Education, Inc. Title Classification of Bones and Gross Anatomy
The Skeletal System PART A. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Skeletal System 5 PART A The Skeletal System Parts of the skeletal system Bones (skeleton) Joints
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Skeletal System 5 PART A The Skeletal System Parts of the skeletal system Bones (skeleton) Joints
The Skeletal System Vertebral column Sacrum. Osseous tissue For the body and soft organs. Magnesium, sodium, fluoride Levers for muscle action
 10/1/2016 Cranium Facial s Skull Clavicle Scapula Sternum Rib Humerus Vertebra Radius Ulna Carpals Thoracic cage (ribs and sternum) The Skeletal System Vertebral column Sacrum Phalanges Metacarpals Femur
10/1/2016 Cranium Facial s Skull Clavicle Scapula Sternum Rib Humerus Vertebra Radius Ulna Carpals Thoracic cage (ribs and sternum) The Skeletal System Vertebral column Sacrum Phalanges Metacarpals Femur
Skeletal Tissues Dr. Ali Ebneshahidi
 Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection: Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection: Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Module 2:! Functional Musculoskeletal Anatomy A! Semester 1! !!! !!!! Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb!
 Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
-the emphasis on this section is the structure and function of bone tissue and on the dynamics of its formation and remodeling throughout life.
 Biology 325 Fall 2004 BONES AND SKELETAL TISSUES Introduction -skeleton contains cartilage and bones -the emphasis on this section is the structure and function of bone tissue and on the dynamics of its
Biology 325 Fall 2004 BONES AND SKELETAL TISSUES Introduction -skeleton contains cartilage and bones -the emphasis on this section is the structure and function of bone tissue and on the dynamics of its
The Skeletal System PART A
 5 The Skeletal System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Skeletal System
5 The Skeletal System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Skeletal System
Chapter 6 Skeletal System
 Chapter 6 Skeletal System Functions of the skeletal system/bone 1. Support skeletal system is the internal framework of the body 2. Protection protects internal organs 3. Movement muscles & bones work
Chapter 6 Skeletal System Functions of the skeletal system/bone 1. Support skeletal system is the internal framework of the body 2. Protection protects internal organs 3. Movement muscles & bones work
The Skeletal System. Chapter 7a. Skeletal System Introduction Functions of the skeleton Framework of bones The skeleton through life
 The Skeletal System Skeletal System Introduction Functions of the skeleton Framework of bones The skeleton through life Chapter 7a Support Protection Movement Storage areas Minerals Lipids Hemopoiesis
The Skeletal System Skeletal System Introduction Functions of the skeleton Framework of bones The skeleton through life Chapter 7a Support Protection Movement Storage areas Minerals Lipids Hemopoiesis
Skeletal Tissues. Dr. Ali Ebneshahidi
 Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection : Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection : Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Chapter 5 The Skeletal System
 Chapter 5 The Skeletal System The Skeletal System Parts of the skeletal system Bones (skeleton) Joints Cartilages Ligaments (bone to bone)(tendon=bone to muscle) Divided into two divisions Axial skeleton:
Chapter 5 The Skeletal System The Skeletal System Parts of the skeletal system Bones (skeleton) Joints Cartilages Ligaments (bone to bone)(tendon=bone to muscle) Divided into two divisions Axial skeleton:
Ossification and Bone Remodeling
 Ossification and Bone Remodeling Pre-natal Ossification Embryonic skeleton: fashioned from fibrous membranes or cartilage to accommodate mitosis. 2 types of pre-natal ossification (bone formation) 1.
Ossification and Bone Remodeling Pre-natal Ossification Embryonic skeleton: fashioned from fibrous membranes or cartilage to accommodate mitosis. 2 types of pre-natal ossification (bone formation) 1.
Skeletal System worksheet
 Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
The formation of blood cells is called. hemopoiesis. What does our bone store? Where do our bones store fat? yellow marrow.
 What are the 5/6 functions of the skeletal system? support, protection, movement, blood cell formation, storage, homeostasis The formation of blood cells is called hemopoiesis What does our bone store?
What are the 5/6 functions of the skeletal system? support, protection, movement, blood cell formation, storage, homeostasis The formation of blood cells is called hemopoiesis What does our bone store?
Outline. Skeletal System. Functions of Bone. Bio 105: Skeletal System 3/17/2016. The material from this lecture packet will be on the lecture exam
 Bio 105: Skeletal System Lecture 8 Chapter 5 The material from this lecture packet will be on the lecture exam The identification that you do after this lecture will be on the lab exam Outline I. Overview
Bio 105: Skeletal System Lecture 8 Chapter 5 The material from this lecture packet will be on the lecture exam The identification that you do after this lecture will be on the lab exam Outline I. Overview
Skeletal Tissue Study Slides. Chapter 6
 Skeletal Tissue Study Slides Chapter 6 Functions of the skeletal system include all of the following, except A. support. B. storage. C. protection. D. blood cell production. E. movement. ANSWER Functions
Skeletal Tissue Study Slides Chapter 6 Functions of the skeletal system include all of the following, except A. support. B. storage. C. protection. D. blood cell production. E. movement. ANSWER Functions
Copy and Return to Teacher. The Skeletal System
 Copy and Return to Teacher The Skeletal System The Skeletal System Parts of the skeletal system o Bones (skeleton) o Joints o Cartilages o Ligaments Divided into two divisions o Axial skeleton o Appendicular
Copy and Return to Teacher The Skeletal System The Skeletal System Parts of the skeletal system o Bones (skeleton) o Joints o Cartilages o Ligaments Divided into two divisions o Axial skeleton o Appendicular
Anatomy & Physiology
 Anatomy & Physiology 101-805 Unit 6 The Skeletal System Paul Anderson 2011 Skeletal System: Components Bones major organs of system, have all functions of system. Cartilages connect & protect bones at
Anatomy & Physiology 101-805 Unit 6 The Skeletal System Paul Anderson 2011 Skeletal System: Components Bones major organs of system, have all functions of system. Cartilages connect & protect bones at
Types of Bones. 5 basic types of bones: Sutural bones - in joint between skull bones
 The Skeletal System The Skeletal System Bone and their cartilage, ligaments & tendons. Dynamic and ever changing throughout life Skeleton contains all 4 tissue types; Epithelial, connective, muscle and
The Skeletal System The Skeletal System Bone and their cartilage, ligaments & tendons. Dynamic and ever changing throughout life Skeleton contains all 4 tissue types; Epithelial, connective, muscle and
Parts of the skeletal system. Bones (skeleton) Joints Cartilages Ligaments (bone to bone)(tendon=bone to muscle)
 The Skeletal System The Skeletal System Parts of the skeletal system Bones (skeleton) Joints Cartilages Ligaments (bone to bone)(tendon=bone to muscle) Divided into two divisions Axial skeleton Appendicular
The Skeletal System The Skeletal System Parts of the skeletal system Bones (skeleton) Joints Cartilages Ligaments (bone to bone)(tendon=bone to muscle) Divided into two divisions Axial skeleton Appendicular
General osteology. General anatomy of the human skeleton. Development and classification of bones. The bone as a multifunctional organ.
 General osteology. General anatomy of the human skeleton. Development and classification of bones. The bone as a multifunctional organ. Composed by Natalia Leonidovna Svintsitskaya, Associate professor
General osteology. General anatomy of the human skeleton. Development and classification of bones. The bone as a multifunctional organ. Composed by Natalia Leonidovna Svintsitskaya, Associate professor
Osseous Tissue and Bone Structure
 6 Osseous Tissue and Bone Structure PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Skeletal System Learning Outcomes 6-1 Describe the primary
6 Osseous Tissue and Bone Structure PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Skeletal System Learning Outcomes 6-1 Describe the primary
FORMATION OF BONE. Intramembranous Ossification. Bone-Lec-10-Prof.Dr.Adnan Albideri
 FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
Bone Tissue- Chapter 5 5-1
 Bone Tissue- Chapter 5 5-1 Bone Functions Support Protection Assistance in movement Mineral storage and release Blood cell production Triglyceride storage 5-2 Bone Chemistry Water (25%) Organic Constituent
Bone Tissue- Chapter 5 5-1 Bone Functions Support Protection Assistance in movement Mineral storage and release Blood cell production Triglyceride storage 5-2 Bone Chemistry Water (25%) Organic Constituent
Unit 5 Skeletal System
 Unit 5 Skeletal System Nov 21 10:24 PM I. Functions A. Support: > internal framework, structure, anchors & supports soft tissue organs B. Protection: > protects vital organs C. Movement: > provides attach
Unit 5 Skeletal System Nov 21 10:24 PM I. Functions A. Support: > internal framework, structure, anchors & supports soft tissue organs B. Protection: > protects vital organs C. Movement: > provides attach
Skeletal System. Bio 105
 Skeletal System Bio 105 Outline I. Overview of the skeletal system II. Function of bones III. Bone structure IV. Bone cells V. Cartilage VI. Tendons and Ligaments VII. Joints VIII. Bone development IX.
Skeletal System Bio 105 Outline I. Overview of the skeletal system II. Function of bones III. Bone structure IV. Bone cells V. Cartilage VI. Tendons and Ligaments VII. Joints VIII. Bone development IX.
Outline. Skeletal System. Tendons link the skeletal and the muscular systems.
 Outline Skeletal System Bio 105 I. Overview of the skeletal system II. Function of bones III. Bone structure IV. Bone cells V. Cartilage VI. Tendons and Ligaments VII. Joints VIII. Bone development IX.
Outline Skeletal System Bio 105 I. Overview of the skeletal system II. Function of bones III. Bone structure IV. Bone cells V. Cartilage VI. Tendons and Ligaments VII. Joints VIII. Bone development IX.
Chapter 5 The Skeletal System:Bone Tissue. Functions of Bone. Bones
 Chapter 5 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose,
Chapter 5 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose,
Spongy Bone. Spongelike appearance formed by plates of bone called trabeculae. spaces filled with red bone marrow
 Spongy Bone Spongelike appearance formed by plates of bone called trabeculae spaces filled with red bone marrow Trabeculae have few osteons or central canals no osteocyte is far from blood of bone marrow
Spongy Bone Spongelike appearance formed by plates of bone called trabeculae spaces filled with red bone marrow Trabeculae have few osteons or central canals no osteocyte is far from blood of bone marrow
Skeletal System Functions
 Chapter 6 Skeletal System: Bones and Bone Tissue 6-1 Skeletal System Functions Support. Bone is hard and rigid; cartilage is flexible yet strong. Cartilage in nose, external ear, thoracic cage and trachea.
Chapter 6 Skeletal System: Bones and Bone Tissue 6-1 Skeletal System Functions Support. Bone is hard and rigid; cartilage is flexible yet strong. Cartilage in nose, external ear, thoracic cage and trachea.
Skeletal System worksheet
 Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
OpenStax-CNX module: m Bone Structure * Ildar Yakhin. Based on Bone Structure by OpenStax. Abstract
 OpenStax-CNX module: m63474 1 Bone Structure * Ildar Yakhin Based on Bone Structure by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
OpenStax-CNX module: m63474 1 Bone Structure * Ildar Yakhin Based on Bone Structure by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
Chapter 6. Osseous Tissue and Bone Structure. Lecture Presentation by Lee Ann Frederick University of Texas at Arlington Pearson Education, Inc.
 Chapter 6 Osseous Tissue and Bone Structure Lecture Presentation by Lee Ann Frederick University of Texas at Arlington An Introduction to the Skeletal System The Skeletal System Includes: Bones of the
Chapter 6 Osseous Tissue and Bone Structure Lecture Presentation by Lee Ann Frederick University of Texas at Arlington An Introduction to the Skeletal System The Skeletal System Includes: Bones of the
Chapter 5. The Skeletal System. Osseous Tissue and Skeletal Structure. Lecture Presentation by Steven Bassett Southeast Community College
 Chapter 5 The Skeletal System Osseous Tissue and Skeletal Structure Lecture Presentation by Steven Bassett Southeast Community College Introduction The skeletal system is made of: Skeletal bones Cartilage
Chapter 5 The Skeletal System Osseous Tissue and Skeletal Structure Lecture Presentation by Steven Bassett Southeast Community College Introduction The skeletal system is made of: Skeletal bones Cartilage
Figure ) The area that causes the lengthwise growth of a long bone is indicated by letter. Diff: 2 Page Ref:
 Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 5 The Skeletal System Short Answer Figure 5.1 Using Figure 5.1, identify the following: 1) Spongy bone is indicated by letter. Diff: 1 Page Ref:
Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 5 The Skeletal System Short Answer Figure 5.1 Using Figure 5.1, identify the following: 1) Spongy bone is indicated by letter. Diff: 1 Page Ref:
Bones. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
 Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
Anatomy & Physiology Skeletal System
 I. Functions of the Skeletal System A. the body Anatomy & Physiology Skeletal System B. of vital organs C. Provide for movement D. storage (calcium & phosphate) E. cell formation II. Bone Structure A.
I. Functions of the Skeletal System A. the body Anatomy & Physiology Skeletal System B. of vital organs C. Provide for movement D. storage (calcium & phosphate) E. cell formation II. Bone Structure A.
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 6 The Skeletal System: Bone Tissue Introduction The skeletal system has 6 important functions: Provides support Protects the internal organs (brain,
Principles of Anatomy and Physiology 14 th Edition CHAPTER 6 The Skeletal System: Bone Tissue Introduction The skeletal system has 6 important functions: Provides support Protects the internal organs (brain,
Copyright 2004 Lippincott Williams & Wilkins. 2. Bone Structure. Copyright 2004 Lippincott Williams & Wilkins
 Chapter 7 The Skeleton: Bones and Joints The Skeleton Skeletal system is made up of bones and joints and supporting connective tissue. 1. Bone Functions 1. To store calcium salts 2. To protect delicate
Chapter 7 The Skeleton: Bones and Joints The Skeleton Skeletal system is made up of bones and joints and supporting connective tissue. 1. Bone Functions 1. To store calcium salts 2. To protect delicate
The Skeletal System ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY PART A ELAINE N. MARIEB EIGHTH EDITION
 5 The Skeletal System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Skeletal System
5 The Skeletal System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Skeletal System
NOTES: Skeletal System (Ch 5, part 1)
 NOTES: Skeletal System (Ch 5, part 1) Individual bones are the organs of the skeletal system. A bone contains very active tissues. BONE STRUCTURE: *Bone structure reflects its function. Parts of a long
NOTES: Skeletal System (Ch 5, part 1) Individual bones are the organs of the skeletal system. A bone contains very active tissues. BONE STRUCTURE: *Bone structure reflects its function. Parts of a long
Skeletal System. Skeletal System 12/15/15. Bone Classification
 Skeletal System Composed of the body s bones and associated ligaments, tendons, and cartilages. Functions: 1. Support The bones of the legs, pelvic girdle, and vertebral column support the weight of the
Skeletal System Composed of the body s bones and associated ligaments, tendons, and cartilages. Functions: 1. Support The bones of the legs, pelvic girdle, and vertebral column support the weight of the
Unit 5 Skeletal System
 Unit 5 Skeletal System I. Functions A. Support: > Internal framework, structure, anchors & supports soft tissue organs B. Protection: > Protects vital organs C. Movement: > Provides attach point for muscles
Unit 5 Skeletal System I. Functions A. Support: > Internal framework, structure, anchors & supports soft tissue organs B. Protection: > Protects vital organs C. Movement: > Provides attach point for muscles
Unit 5: SKELETAL SYSTEM
 Unit 5: SKELETAL SYSTEM (a) NRSG231 Dr. Moattar Raza Rizvi Skeletal System: Contents Functions of the Skeletal System Fracture Structure of Bone Tissue Articulations & Joint Bone Development and Growth
Unit 5: SKELETAL SYSTEM (a) NRSG231 Dr. Moattar Raza Rizvi Skeletal System: Contents Functions of the Skeletal System Fracture Structure of Bone Tissue Articulations & Joint Bone Development and Growth
Chapter 4. Cartilage and Bone. Li Shu-Lei instructor. Dept. Histology and Embryology, School of Basic Medical Sciences, Jilin University
 Chapter 4 Cartilage and Bone Li Shu-Lei instructor Dept. Histology and Embryology, School of Basic Medical Sciences, Jilin University I Cartilage a specialized connective tissue Characterizers: Cartilage
Chapter 4 Cartilage and Bone Li Shu-Lei instructor Dept. Histology and Embryology, School of Basic Medical Sciences, Jilin University I Cartilage a specialized connective tissue Characterizers: Cartilage
Bone Development. Two Types of OssificaDon 10/18/14. Osteogenesis ( ) bone Dssue formadon Stages. Bones and Skeletal Tissues: Part B
 Bone Development 6 Bones and Skeletal Tissues: Part B Osteogenesis ( ) bone Dssue formadon Stages Bone formadon begins in the 2nd month of development Postnatal bone growth undl early adulthood Bone remodeling
Bone Development 6 Bones and Skeletal Tissues: Part B Osteogenesis ( ) bone Dssue formadon Stages Bone formadon begins in the 2nd month of development Postnatal bone growth undl early adulthood Bone remodeling
For more information about how to cite these materials visit
 Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 6 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 6 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
Blood. Hematopoietic Tissue
 Blood Hematopoietic Tissue Is a type of connective tissue in which its cells are suspended in a circulating fluid. Erythrocytes+ leukocytes + platelets (thrombocytes) =formed elements of blood. These formed
Blood Hematopoietic Tissue Is a type of connective tissue in which its cells are suspended in a circulating fluid. Erythrocytes+ leukocytes + platelets (thrombocytes) =formed elements of blood. These formed
The bones of the legs, pelvic girdle, and vertebral column support the weight of the erect body. The mandible (jawbone) supports the teeth.
 Skeletal System Composed of the body s bones and associated ligaments, tendons, and cartilages. Functions: 1. Support EXAMPLES: The bones of the legs, pelvic girdle, and vertebral column support the weight
Skeletal System Composed of the body s bones and associated ligaments, tendons, and cartilages. Functions: 1. Support EXAMPLES: The bones of the legs, pelvic girdle, and vertebral column support the weight
Human Anatomy and Physiology I Laboratory
 Human Anatomy and Physiology I Laboratory Skeletal Tissue: Cartilage and Bone This lab involves study of the laboratory exercise Overview of the Skeleton, Classification and Structure of Bones and Cartilages,
Human Anatomy and Physiology I Laboratory Skeletal Tissue: Cartilage and Bone This lab involves study of the laboratory exercise Overview of the Skeleton, Classification and Structure of Bones and Cartilages,
SKELETAL SYSTEM. Bone Shapes Long longer than they are wide; have a shaft plus two ends Ex. bones of limbs except wrist and ankle
 SKELETAL SYSTEM FUNCTIONS 1. Support Bones form the internal framework that supports and anchors all soft organs. 2. Protection Bones protect soft body organs. 3. Movement Skeletal muscles, which attach
SKELETAL SYSTEM FUNCTIONS 1. Support Bones form the internal framework that supports and anchors all soft organs. 2. Protection Bones protect soft body organs. 3. Movement Skeletal muscles, which attach
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name 1) An open or fracture projects through the skin. 1) 2) The humerus is an example of a(n) bone. 2) A) flat B) sesamoid C) long D) short E) irregular 3) Accelerated closure of the epiphyseal plates
Exam Name 1) An open or fracture projects through the skin. 1) 2) The humerus is an example of a(n) bone. 2) A) flat B) sesamoid C) long D) short E) irregular 3) Accelerated closure of the epiphyseal plates
Human Biology Chapter 15.3: Bone Structure *
 OpenStax-CNX module: m58082 1 Human Biology Chapter 15.3: Bone Structure * Willy Cushwa Based on Bone Structure by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons
OpenStax-CNX module: m58082 1 Human Biology Chapter 15.3: Bone Structure * Willy Cushwa Based on Bone Structure by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons
The Skeletal S 1Jstem
 . / : /~ 4,.',ifṾI : /'i I,"~ ~". ~ /', - 1"';-- '"i-:~.~ I!.,J'" The Skeletal S 1Jstem ". P 'J : ~lj:::' ~,- The skeleton is constructed of two of the most supportive tissues found in the human body-cartilage
. / : /~ 4,.',ifṾI : /'i I,"~ ~". ~ /', - 1"';-- '"i-:~.~ I!.,J'" The Skeletal S 1Jstem ". P 'J : ~lj:::' ~,- The skeleton is constructed of two of the most supportive tissues found in the human body-cartilage
What is bone? Specialized form of connective tissue: mineralized collagen matrix, therefore very rigid and strong while still retaining some degree of
 Bone What is bone? Specialized form of connective tissue: mineralized collagen matrix, therefore very rigid and strong while still retaining some degree of flexibility Other types of connective tissue:
Bone What is bone? Specialized form of connective tissue: mineralized collagen matrix, therefore very rigid and strong while still retaining some degree of flexibility Other types of connective tissue:
The Skeletal System. Mosby items and derived items 2010, 2006, 2002, 1997, 1992 by Mosby, Inc., an affiliate of Elsevier Inc.
 The Skeletal System Functions of Skeletal System Provides internal framework that supports the body Protects internal organs Helps fight disease by producing white blood cells 2 Functions of Skeletal System
The Skeletal System Functions of Skeletal System Provides internal framework that supports the body Protects internal organs Helps fight disease by producing white blood cells 2 Functions of Skeletal System
in compact bone, large vertical canals carrying blood vessels and nerves. in compact bone, large horizontal canals carrying blood vessels and nerves.
 Carl Christensen, PhD Skeletal System (Bones`) Bio. 2304 Human Anatomy 1. Identify a term for each of the following: shaft of a long bone ends of a long bone ossified remnant of the "growth plate" connective
Carl Christensen, PhD Skeletal System (Bones`) Bio. 2304 Human Anatomy 1. Identify a term for each of the following: shaft of a long bone ends of a long bone ossified remnant of the "growth plate" connective
Lecture 2: Skeletogenesis
 Jilin University School of Stomatology Skeletogenesis Lecture 2: Skeletogenesis Aug. 18, 2015 Yuji Mishina, Ph.D. mishina@umich.edu Student will describe Development of Bone - the general anatomy of bone
Jilin University School of Stomatology Skeletogenesis Lecture 2: Skeletogenesis Aug. 18, 2015 Yuji Mishina, Ph.D. mishina@umich.edu Student will describe Development of Bone - the general anatomy of bone
Bone Formation, Growth, and Remodeling
 Bone Formation, Growth, and Remodeling Pre-natal Ossification Embryonic skeleton: fashioned from fibrous membranes or cartilage to accommodate mitosis. 2 types of pre-natal ossification (bone formation)
Bone Formation, Growth, and Remodeling Pre-natal Ossification Embryonic skeleton: fashioned from fibrous membranes or cartilage to accommodate mitosis. 2 types of pre-natal ossification (bone formation)
UNIT 5 THE SKELETAL SYSTEM
 UNIT 5 THE SKELETAL SYSTEM Nov 20 12:02 PM I. Functions A. Support: Internal framework, Structure, Anchors & Supports soft tissue/organs B. Protection: Protects vital organs C. Movement: Provide attach
UNIT 5 THE SKELETAL SYSTEM Nov 20 12:02 PM I. Functions A. Support: Internal framework, Structure, Anchors & Supports soft tissue/organs B. Protection: Protects vital organs C. Movement: Provide attach
Skeletal System. Chapter 7.1. Objective- Read 7.1 and understand that bones are alive and multifunctional. Introduction:
 Chapter 7.1 Skeletal System Objective- Read 7.1 and understand that bones are alive and multifunctional. Introduction: A. Bones are very active tissues B. Each bone is made up of several types of tissues
Chapter 7.1 Skeletal System Objective- Read 7.1 and understand that bones are alive and multifunctional. Introduction: A. Bones are very active tissues B. Each bone is made up of several types of tissues
Chapter 6 Part B Bones and Skeletal Tissue
 Chapter 6 Part B Bones and Skeletal Tissue 6.5 Bone Development Ossification (osteogenesis) is the process of bone tissue formation Formation of bony skeleton begins in month 2 of development Postnatal
Chapter 6 Part B Bones and Skeletal Tissue 6.5 Bone Development Ossification (osteogenesis) is the process of bone tissue formation Formation of bony skeleton begins in month 2 of development Postnatal
Regulation of the skeletal mass through the life span
 Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
