Valgus instability as a cause for recurrent lateral patellar dislocation : A new mechanism for patellofemoral instability?
|
|
|
- Aldous Hall
- 5 years ago
- Views:
Transcription
1 Acta Orthop. Belg., 2013, 79, ASPECT OF CURRENT MANAGEMENT Valgus instability as a cause for recurrent lateral patellar dislocation : A new mechanism for patellofemoral instability? Kristof Hermans, Steven Claes, Johan Bellemans From the University Hospital Pellenberg (K.U.L.), Lubbeek, Belgium An association between lateral patellar dislocation (LPD) and medial collateral ligament injury (MCL) has recently been demonstrated on MRI. The same valgus injury that disrupts the femoral MCL insertion can also cause a simultaneous MPFL tear at its femoral insertion, due to the close anatomical relationship of both ligamentous structures. Valgus laxity due to MCL-deficiency increases the Q-angle and further adversely affects patellar stability. A knee diagnosed with a severe MCL tear, should be evaluated for patellofemoral instability, as a temporary patella dislocation could have been caused by the same injury and an acute LPD indicating a tear of the MPFL can be associated with a concomitant injury of the MCL. In case of recurrent symptoms of patellofemoral instability in a MCL-deficient knee, both the MPFL and MCL should be managed operatively. An isolated MPFL reconstruction in this knee is likely to fail due to a persistent increase of the Q-angle. Keywords : patellar instability ; risk factors ; medial patellofemoral ligament ; medial collateral ligament ; combined injury. Lateral patellar dislocation (LPD) accounts for 2% to 3% of all acute knee injuries (1) and can lead to recurrent patellar instability and knee pain. It is the second most frequent cause of knee haemarthrosis (1) and typically happens when the knee undergoes a twisting maneuver in a slightly flexed position (around 30 ). Through the range of motion of the human knee, patellar stability is mainly controlled by the patellofemoral joint geometry (9,16). Classic bony risk factors for patellofemoral instability include trochlear and patellar dysplasia and an increased Q-angle or tibial tubercle-trochlear groove distance (TT- TG). Trochlear dysplasia can be assessed by evaluating the three criteria suggested by Dejour : the depth of the trochlea, the crossing sign and the trochlear prominence or boss (7). The Q-angle is the angle formed by a line drawn from the center of the patella to the tibial tubercle and a second line drawn from the anterior superior iliac spine (ASIS) to the center of the patella. It can be influenced by tibial tuberosity lateralization as in genu valgum (31), external torsion of the tibia, generalized ligamentous laxity, excessive foot pronation (29), tightness of the INTRODUCTION n Kristof Hermans, MD, Resident. n Steven Claes, MD, Resident. n Johan Bellemans, MD, PhD, Professor and Head of the Department. Department of Orthopaedic Surgery, University Hospital Pellenberg, (K.U.L.), Lubbeek, Belgium. Correspondence : Kristof Hermans, Department of Orthopaedic surgery, University Hospital Pellenberg, Weligerveld 1, 3212 Pellenberg, Belgium. Kristof.hermans@student.kuleuven.be 2013, Acta Orthopædica Belgica. No benefits or funds were received in support of this study. The authors report no conflict of interests.
2 496 k. hermans, s. claes, j. bellemans iliotibial band (ITB), weakness of the gluteus medius muscle, hip anteversion (21) or patella alta (2). Soft-tissue restraints are important in stabilizing the patella at full extension and early knee flexion (16). Proven soft-tissue risk factors for LPD include lesions of the MPFL, medial retinacular laxity and lateral tightness (16). Biomechanical studies have identified the MPFL accounts for 53-67% of the total medial restraining force preventing lateral patellar subluxation or dislocation (5). The medial patellomeniscal ligament and associated retinacular fibres in the deep capsular layer of the knee contribute approximately 22%, whereas the patellotibial ligament and the medial parapatellar retinaculum contribute little in the prevention of lateral patellar displacement (5).These findings are confirmed by studies reporting a restoration of the excessive lateral mobility to normal values after reconstruction of the MPFL in the non-dysplastic patellofemoral joint (14). The medial collateral ligament (MCL) complex is one of the most commonly injured ligamentous structures of the knee joint (22). MCL lesions usually follow a direct valgus injury on the knee, forced tibial external rotation or a combination of both. The MCL complex consists of three closely related components : the superficial MCL (smcl), the deep MCL (dmcl) and the posterior oblique ligament (POL) (24). Warren and Marshall (38) divided the anatomy of the medial knee structures in three layers, with the smcl to be part of layer two, the dmcl part of the third and deepest layer, while the POL arises as a conjoined structure from the second and third layer. The smcl is the most important structure on the medial aspect of the knee, exerting the largest load response to both valgus and external rotation torques. The smcl, positioned between the superficial sartorial fascia and the dmcl, arises slightly proximal and posterior to the medial epicondyle (22). It has two tibial attachments ; a proximal one located just over 1 cm distal to the joint line and a strong distal attachment, located approximately 6 cm distal to the joint line and directly attached to bone. The functionally less important dmcl is a thickening of the joint capsule deep to the smcl, extending from the femur to the mid-portion of the medial meniscus and inserting just below the tibial part of the joint line. Thirdly, the POL reveals a significant static restraint to valgus and internal rotation torques, particularly in extension. It arises from the adductor tubercle of the distal femur and runs to three distal attachments forming a tibial, a capsular and an inferior arm (38). The classification of MCL injuries (22,28) includes three degrees of severity. A first-degree tear is a microscopic disruption of the fibers with localized tenderness without instability. A second-degree tear, considered as a an incomplete tear of the MCL complex, involves more fibers resulting in more generalized tenderness and instability at 30 of flexion, but still no instability at full extension. Finally a third-degree tear is defined as a complete tear of the MCL complex with a decrease in tenderness, massive valgus instability at 30 of flexion and instability at early flexion angles, indicating the concomitant tear of the POL. ILLUSTRATIVE CASE A 41-year-old male patient was seen in the outpatient clinic with a chief complaint of medial knee instability being present for about 2 years after a twisting injury. He described a sensation of giving-way at the medial side of the left knee during activities causing a valgus force on the affected knee, leading to a near-fall. Pain was definitely no major complaint. There were no complaints of locking or patellar catching. He furthermore reported recurrent, prominent effusions after each episode of medial giving-way. At subsequent clinical examination, obvious valgus instability was found, with significant opening of the medial knee joint during the valgus stress test in 30 of flexion. The patient showed clear signs of apprehension while performing this test, stating that this feeling of medial giving-way formed his chief complaint. In full extension, no medial instability was noted. Further examination revealed slight pain by palpating the region of the femoral medial epicondyle. McMurray s test for meniscal lesions was negative, as were the Lachman and anterior drawer test for ACL injury. A clearly positive apprehension for patellar instability was found as well, with the patella showing apparent lateral laxity compared to
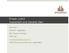
3 recurrent lateral patellar dislocation 497 Based on the clinical findings of patellofemoral instability we looked for the presence of bony and soft-tissue risk factors for patellar instability on plain radiographs and MRI (Table I). There were no signs of trochlear dysplasia, TT-TG was normal and patellar height was normal. The diagnosis of a combined valgus laxity and patellofemoral instability was recorded ensuing a chronic injury to the region of the medial femoral epicondyle. An operative approach was offered, with the goal of reconstructing the MPFL with a tendon graft and subsequently addressing chronic MCL laxity by performing an advancement of the MCL complex as proposed by Hughston (17). Fig. 1. MRI study of the left knee reveals complete rupture of the smcl and dmcl from the femur (large arrow). Bone bruise can be noted on the lateral femoral condyle, suggesting a valgus mechanism (small arrow). the contralateral knee. Although the patient recalled this sensation as a minor component of his aforementioned episodes of giving-way, he clearly delineated this feature from instability during the valgus stress test. Magnetic resonance imaging of the affected knee showed a chronic grade III femoral insertion tear of the MCL (Fig. 1). A prominent effusion and a distinct area of bone bruise in both the lateral femoral condyle and the medial patella were observed, corresponding with a recent episode of LPD. MRI poorly visualized the MPFL, and no clear rupture or avulsion of this structure could be shown. No other knee injuries were noted. Operative treatment With the patient under general anaesthesia and positioned in the supine position, a valgus stress test was performed, resulting in frank lateral patellar dislocation without applying any force to the patella itself (Fig. 2). A longitudinal anteromedial incision of the knee was made at mid distance between the medial patellar edge and the medial femoral epicondyle. A midvastus arthrotomy was performed preserving an 8 mm rim of medial retinacular tissue attached to the patella. The patella was slightly everted to confirm the absence of patellar cartilage lesions. To reconstruct the patellar MPFL insertion, two stab incisions in the medial retinacular sleeve directly adjacent to the medial patellar edge were made and a fresh frozen gracilis tendon allograft was looped through. A more medial incision of layer 1 was performed posterior to the medial epicondyle, and both the superficial and deep part of the MCL as well as Table 1. Reference values in normal knees and patient values concerning traditional risk factors for LPD Traditional risk factors Reference values in normal knees Patient values Sulcus angle (6) 137 Trochlear depth 2.4 mm-10.5 mm (27) 7.5 mm Trochlear facet asymmetry > 40% (27) 65.38% TT - TG distance < 20 mm (13,33) 17.8 mm Insall - Salvati ratio (20) 1.08 Caton - Deschamps index (4) 1.15
4 498 k. hermans, s. claes, j. bellemans Fig. 2. Valgus stress test resulting in frank lateral patellar dislocation without applying any force to the patella itself. the posterior oblique ligament (POL) were clearly identified. Although all three ligamentous structures showed continuous fibers, these ligaments seemed extremely floppy or abundant. According to Hughston (17), the complete medial ligamentous complex was detached from the femur with an L- shaped incision. The femoral end of the MPFL reconstruction was continued by creating a 6 mm bone tunnel starting at the native MPFL femoral insertion which was confirmed by fluoroscopic control according to Schöttle et al (32). The free ends of the gracilis allograft were passed between the two layers of the medial patellar retinaculum and inside the femoral tunnel. With the knee flexed at 60, the free ends were fixed in the femoral tunnel using a PEEK interference screw (Biosure PK 6 25 mm screw, Smith&Nephew, Andover, USA), thus finishing the MPFL reconstruction. The sleeve containing the medial ligamentous complex was advanced proximally and anteriorly on the femur, following the technique described by Hughston (17). In this position, the sleeve was fixed to the medial femoral condyle using two suture loaded bone anchors (Twinfix 5.0 anchor, Smith&Nephew, Andover, USA), thus restoring proper tension in the medial ligamentary complex. The MCL plication was finalized by suturing the advanced POL fibers by 4 stitches (Ethibond Excel 2.0, Ethicon, Somerville, USA) to the smcl, The redundant tissue proximal to the femoral fixation was sutured to the lower fibers of the vastus medialis obliquus (VMO). Finally, both patellar and valgus laxity were carefully tested and judged as adequate without remaining instability. After closure of the subcutaneous layers and skin, an immobilizing hinged brace was applied with the knee fixed in 10 degrees of flexion during the first two weeks. The hinged brace was gradually allowed into more flexion the following 4 weeks, after which a cage-type brace was applied for the next 3 months. Full weight bearing was only allowed after 4 weeks. Rehabilitation was uneventful, with the patient reporting to feel well at 3 months after surgery, showing full ROM without residual pain. At final follow-up 1 year after surgery, he had never again experienced either patellar or medial knee instability and was fully functional. Clinically, a slight residual valgus laxity of 2 mm in 30 of flexion was found, when compared to the contralateral side. However, apprehension or effusion were completely absent. DISCUSSION The clinical picture of valgus laxity associated with patellar dislocation as demonstrated by examination under anaesthesia, led to the assumption of a strong correlation between the two types of instability. We believe that a tear of the MCL complex can adversely affect patellar stability by both a direct and an indirect mechanism (Fig. 3). The direct mechanism is responsible when the femoral MPFL insertion site is injured simultaneously by the same valgus injury affecting the femoral MCL complex insertion due to the close anatomical proximity of both ligamentous structures (Fig. 4). It has been shown that the anatomy of the medial knee structures can be divided in three layers, with both the medial patellofemoral ligament (MPFL) and the superficial medial collateral ligament (MCL) to be part of layer two (38). The MPFL is said to arise from the medial femoral epicondyle (14,38) or the
5 recurrent lateral patellar dislocation 499 Fig. 4. The femoral MPFL insertion site can be directly injured by a valgus injury sustained in the area of the femoral MCL complex insertion due to the close anatomical proximity of both ligamentous structures. Fig. 3. Traditional risk factors for LPD completed with the new risk factor : a serious MCL lesion at its femoral insertion. adductor tubercle (5,36) and extends anteriorly to the superomedial two-thirds of the patella. Disruption of the MPFL most commonly occurs in the fibers attached to the medial femoral epicondyle (35). As the MPFL courses anteriorly, its fibers fuse with the undersurface of the VMO tendon (26). The superficial MCL arises slightly proximal and posterior to the medial epicondyle, almost at the same place as the distal femoral attachment of the VMO. The most common location for MCL injury is the femoral insertion, accounting for 65% of the MCL tears. In the era before the first description of the MPFL as a distinct ligamentous structure, some reports not only mentioned injury to the medial retinaculum after an acute LPD but also the co-existence of lesions to the VMO insertion in these cases. Hunter et al (18) noted a femoral lesion of the MCL in 61% of the patients diagnosed with a disruption of the VMO from the adductor tubercle. Since the identification of the MPFL refined the knowledge of the precise anatomy of the medial retinaculum, it can be assumed that these authors noticed the same injury mechanism as is demonstrated in this case. More recently, Quinlan et al (30) evaluated the integrity of the MCL by MRI in a series of 80 patients who were diagnosed with a transient lateral patellar dislocation. Forty patients (50%) were diagnosed with coexistent MCL injuries, adding to the evidence of an existent relationship between patellar instability and MCL lesions. Based on the common insertion of the smcl and MPFL, we believe an injury causing a femoral lesion of the smcl can vice versa cause a disruption of the MPFL at its femoral insertion. The dynamic increase of the Q-angle in the chronic MCL deficient setting, causing valgus laxity constitutes the indirect mechanism and acts as an adjunctive patellar destabilizer. This hypothesis is supported by the results of a 7-year follow-up study, reporting that the MPFL injury location has to be taken into account when planning treatment : whereas MPFL avulsion at the femoral attachment in primary traumatic patellar dislocations predicts patellar instability, a disruption at the mid-substance or at the patella results significantly less often into patellar instability (34). Initial management of a first time patella dislocation is usually non-operative (3). However recurrence
6 500 k. hermans, s. claes, j. bellemans rates of 15% to 44% have been reported after conservative treatment (25). Operative treatment of both acute and chronic patellar instability through reconstruction of the medial patellofemoral ligament showed significantly less pain and recurrence compared to non-operative treatment (3,12). Initial management of most MCL lesions, including high-grade tears also is conservative. Chronic cases or multiligament injuries are considered for surgical approach (24). In conclusion we believe that the possible simultaneous occurrence of both valgus and patellar instability implicates reconsideration of the diagnostic and therapeutic approach of these injuries : 1. In case of a high-grade femoral tear of the MCL complex, a concomitant MPFL lesion should be excluded. In some cases, MRI can be useful as patellar dislocations can be clinically missed. 2. When confronted with an acute patellar dislocation, a simultaneous injury to the femoral MCL insertion site should be excluded. It is important to be aware of the fact that patellar apprehension can make the valgus stress test unclear. 3. When a femoral lesion of the MPFL combined with a high-grade MCL injury is diagnosed, conservative treatment is advisable if both pathologic conditions and their mutual relationship are recognized and treated accordingly. In cases of recurrent instability not responding to conservative treatment, both ligaments should be treated surgically by either MCL reconstruction or advancement combined with MPFL reconstruction. REFERENCES 1. Arendt EA, Fithian DC, Cohen E. Current concepts of lateral patella dislocation. Clin Sports Med 2002 ; 21 : Balcarek P, Jung K, Ammon J et al. Anatomy of lateral patellar instability. Am J Sports Med 2010 ; 38 : Bitar AC, Demange MK, D Elia CO, Camanho GL. Traumatic patellar dislocation : nonoperative treatment compared with MPFL reconstruction using patellar tendon. Am J Sports Med 2012 ; 40 : Caton J, Deschamps G, Chambat P, Lerat JL, Dejour H. [Patella infera : a study of 128 cases.] (in French). Rev Chir Orthop Répar Appar Mot ; 68 : Conlan T, Garth WP, Lemons JE. Evaluation of the medial soft-tissue restraints of the extensor mechanism of the knee. J Bone Joint Surg 1993 ; 75-A : Davies AP, Costa ML, Donnell ST, Glasgow MM, Shepstone L. The sulcus angle and malalignment of the extensor mechanism of the knee. J Bone Joint Surg 2000 ; 82-B : Dejour H, Walch G, Nove-Josserand L, Guier C. Factors of patellar instability : An anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc 1994 ; 2 : Elias DA, White LM, Fithian DC. Acute lateral patellar dislocation at MR imaging. Radiology 2002 ; 225 : Farahmand F, Tahmasbi MN, Amis AA. Lateral forcedisplacement behaviour of the human patella and its variation with knee flexion : A biomechanical study in vitro. J Biomech 1998 ; 31 : Fithian DC, Paxton EW, Stone ML et al. Epidemiology and natural history of acute patellar dislocation. Am J Sports Med 2004 ; 32 : Gardiner JC, Weiss JA, Rosenberg TD. Strain in the human medial collateral ligament during valgus loading of the knee. Clin Orthop Relat Res 2001 ; 391 : Gomes JLE, Marczyk LRS, Cesar de Cesar SP, Jungblut CF. Medial patellofemoral ligament reconstruction with semitendinosus autograft for chronic patellar instability : A follow-up study. Arthroscopy 2004 ; 20 : Goutallier D, Bernageau J, Lecudonnec B. Measurement of the tibial tubercle-trochlear groove distance (TT-TG).] (in French). Rev Chir Orthop Réparatrice Appar Mot, 1978 ; 64 : Hautamaa PV, Fithian DC, Kaufman KR et al. Medial soft-tissue restraints in lateral patellar instability and repair. Clin Orthop Relat Res 1998 ; 349 : Hawkins RJ, Bell RH, Garth A. Acute patellar dislocations : The natural history. Am J Sports Med 1986 ; 14 : Heegaard J, Leyvraz PF, Van Kampen A et al. Influence of soft structures on patellar three-dimensional tracking. Clin Orthop Relat Res 1994 ; 299 : Hughston JC. The importance of the posterior oblique ligament in repairs of acute tears of the medial ligaments in knees with and without an associated rupture of the anterior cruciate ligament. Results of long-term follow-up. J Bone Joint Surg 1994 ; 76-A : Hunter SC, Marascalco R, Hughston JC. Disruption of the vastus medialis obliquus with medial knee ligament injuries. Am J Sports Med 1983 ; 11 : Insall J, Goldberg V, Salvat E. Recurrent dislocation and the high-riding patella. Clin Orthop Relat Res 1972 ; 88 : Insall J, Salvati E. Patella position in the normal knee joint. Radiology 1971 ; 101 : Kijowski R, Plagens D, Shaeh SJ et al. The effects of rotational deformities of the femur on contact pressure and
7 recurrent lateral patellar dislocation 501 contact area in the patellofemoral joint and on strain in the medial patellofemoral ligament. Annuel Meeting of the International Patellofemoral Study Group 1999 Napa Valley, San Francisco. 22. LaPrade RF, Wijdicks CA. The management of injuries to the medial side of the knee. J Orthop Sports Phys Ther 2012 ; 42 : Maldague B, Malghem J. Significance of the radiograph of the knee profile on the detection of knee patellar instability : Preliminary report. Rev Chir Orthop Réparatrice Appar Mot 1985 ; 71 (Suppl 2) : Marchant MH, Jr, Tibor LM, Sekiya JK et al. Management of medial-sided knee injuries, Part 1 : Medial collateral ligament. Am J Sports Med 2011 ; 39 : Mehta VM, Inoue M, Nomura E, Fithian DC. An algorithm guiding the evaluation and treatment of acute primary patellar dislocations. Sports Med Arthrosc 2007 ; 15 : Nomura E, Fujikawa T, Takeda et al. Anatomical study of the medial patellofemoral ligament. Orthop Surg Suppl 1992 ; 22 : Pfirrmann CW, Zanetti M, Romero J, Hodler J. Femoral trochlear dysplasia : MR findings. Radiology 2000 ; 216 : Phisitkul P., James SL, Wolf BR, Amendola A. MCL injuries of the knee : current concepts review. Iowa Orthop J 2006 ; 26 : Post WR. Clinical evaluation of patients with patellofemoral disorders. Arthroscopy 1999 ; 15 : Quinlan JF, Farrekky C, Kelly G, Eustace S. Co-existent medial collateral ligament injury seen following transient patellar disloaction : observations at magnetic resonance imaging. Br J Sports Med 2010 ; 44 : Sanchis-Alfonso V, Avila-Carrasco C, Prat-Pastor J, Atienza-Vicente C, Cunat E. Biomechanical bases for anterior knee pain and patellar instability. Anterior Knee Pain and Patellar Instability. 2nd ed, Springer, London, New York,2011, pp Schöttle PB, Schmeling A, Rosenstiel N, Weiler A. Radiographic landmarks for femoral tunnel placement in medial patellofemoral ligament reconstruction. Am J Sports Med 2007 ; 35 : Schöttle PB, Zanetti M, Seifert B et al. The tibial tuberosity-trochlear groove distance ; a comparative study between CT and MRI scanning. Knee 2006 ; 13 : Sillanpää PJ, Peltola E, Mattila VM, Kiuru M. Femoral avulsion of the medial patellofemoral ligament after primary traumatic patellar dislocation predicts subsequently instability in men. Am J Sports Med 2009 ; 37 : Stefancin KK, Parker RD. First-time traumatic patellar dislocation : a systematic review. Clin Orthop Relat Res 2007 ; 455 : Terry GC. The anatomy of the extensor mechanism. Clin Sports Med 1989 ; 8 : Van Huyssteen AL, Hendrix MR, Barnett AJ, Wakeley CJ, Eldridge JD. Cartilage-bone mismatch in the dysplastic trochlea : an MRI study. J Bone Joint Surg 2006 ; 88-B : Warren LF, Marshall JL. The supporting structures and layers on the medial side of the knee : Anatomical analysis. J Bone Joint Surg 1979 ; 61-A :
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
10/30/18. Disclosures. Recurrent Patellar Instability. Management of Recurrent Patellar Instability
 Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
Peggers Super Summaries: PFJ
 Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Medial Patellofemoral Ligament (MPFL) Surgical Technique
 Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
MCL Injuries: When and How to Repair Scott D. Mair, MD
 MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
Jacques Menetrey, MD, PD. Uniklinik Balgrist. Unité d Orthopédie et Traumatologie du Sport (UOTS)
 Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
8/9/2017. Case Based: Beyond Medial Patellofemoral Ligament. Editorial Board AJSM Social Media. Consultant. Not talking about PF pain/chondrosis Rehab
 Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Medial Patellofemoral Ligament Reconstruction
 53 Medial Patellofemoral Ligament Reconstruction Hany Elrashidy, Joseph Carney, Najeeb Khan, and Donald C. Fithian CHAPTER DEFINITION Stability of the patellofemoral joint (PFJ) is multifactorial as it
53 Medial Patellofemoral Ligament Reconstruction Hany Elrashidy, Joseph Carney, Najeeb Khan, and Donald C. Fithian CHAPTER DEFINITION Stability of the patellofemoral joint (PFJ) is multifactorial as it
Please differentiate an internal derangement from an external knee injury.
 Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Financial Disclosure. Medial Collateral Ligament
 Matthew Murray, M.D. UTHSCSA Sports Medicine Financial Disclosure Dr. Matthew Murray has no relevant financial relationships with commercial interests to disclose. Medial Collateral Ligament Most commonly
Matthew Murray, M.D. UTHSCSA Sports Medicine Financial Disclosure Dr. Matthew Murray has no relevant financial relationships with commercial interests to disclose. Medial Collateral Ligament Most commonly
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction
 In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
What s your diagnosis?
 Case Study 58 A 61-year-old truck driver man presented with a valgus injury to the left knee joint when involved in a truck accident. What s your diagnosis? Diagnosis : Avulsion of Deep MCL The medial
Case Study 58 A 61-year-old truck driver man presented with a valgus injury to the left knee joint when involved in a truck accident. What s your diagnosis? Diagnosis : Avulsion of Deep MCL The medial
Ligamentous and Meniscal Injuries: Diagnosis and Management
 Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Abstract. Introduction. Michele Vasso 1 Katia Corona 2 Giuseppe Toro 1 Marco Rossini 1 Alfredo Schiavone Panni 1
 256 Technical Note THIEME Anatomic Double-Bundle Medial Patellofemoral Ligament Reconstruction with Autologous Semitendinosus: Aperture Fixation Both at the Femur and the Patella Michele Vasso 1 Katia
256 Technical Note THIEME Anatomic Double-Bundle Medial Patellofemoral Ligament Reconstruction with Autologous Semitendinosus: Aperture Fixation Both at the Femur and the Patella Michele Vasso 1 Katia
Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no
 Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Medial patellofemoral ligament reconstruction using dual patella docking technique
 2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
Jia Li 1, Yongqian Li 1, Jingchao Wei 2, Jianzhao Wang 1, Shijun Gao 1 and Yong Shen 1*
 Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff),
 Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
SLARD Symposium: MCL s Injuries
 SLARD Symposium: MCL s Injuries ISAKOS 11 th Biennial Congress Tue June 6 th 2017 13:30 14:15 Shanghai, China Gustavo A. Rincón, MD Chairman Department Orthopedic Surgery Hospital de San José Bogotá -
SLARD Symposium: MCL s Injuries ISAKOS 11 th Biennial Congress Tue June 6 th 2017 13:30 14:15 Shanghai, China Gustavo A. Rincón, MD Chairman Department Orthopedic Surgery Hospital de San José Bogotá -
Doron Sher. 160 Belmore Rd, Randwick Burwood Rd, Concord. MBBS, MBiomedE, FRACS FAOrthA
 Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Computational Evaluation of Predisposing Factors to Patellar Dislocation
 Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Acute patellar dislocation in adults
 CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
Medial collateral ligament (MCL) injury, is one
 )3( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY EDITORIAL Medial Collateral Ligament Injury; A New Classification Based on MRI and Clinical Findings. A Guide for Patient Selection and Early
)3( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY EDITORIAL Medial Collateral Ligament Injury; A New Classification Based on MRI and Clinical Findings. A Guide for Patient Selection and Early
Reconstruction of the medial patellofemoral ligament for treatment of patellar instability
 354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force.
 Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis Autograft without Bone Tunnel
 Original Article Clinics in Orthopedic Surgery 2015;7:457-464 http://dx.doi.org/10.4055/cios.2015.7.4.457 Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis
Original Article Clinics in Orthopedic Surgery 2015;7:457-464 http://dx.doi.org/10.4055/cios.2015.7.4.457 Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis
Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery. Restore patella stability.
 Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco
 Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability
 Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
Surgical treatments of patellar instability have been
 Reconstruction of the Medial Patellofemoral Ligament With Gracilis Tendon Autograft in Transverse Patellar Drill Holes Svend Erik Christiansen, M.D., Bent W. Jacobsen, M.D., Bent Lund, M.D., and Martin
Reconstruction of the Medial Patellofemoral Ligament With Gracilis Tendon Autograft in Transverse Patellar Drill Holes Svend Erik Christiansen, M.D., Bent W. Jacobsen, M.D., Bent Lund, M.D., and Martin
The Knee. Tibio-Femoral
 The Knee Tibio-Femoral Osteology Distal Femur with Proximal Tibia Largest Joint Cavity in the Body A modified hinge joint with significant passive rotation Technically, one degree of freedom (Flexion/Extension)
The Knee Tibio-Femoral Osteology Distal Femur with Proximal Tibia Largest Joint Cavity in the Body A modified hinge joint with significant passive rotation Technically, one degree of freedom (Flexion/Extension)
Tibial tubercle osteotomy in patello-femoral instability and in patellar height abnormality
 International Orthopaedics (SICOT) (2010) 34:305 309 DOI 10.1007/s00264-009-0929-4 ORIGINAL PAPER Tibial tubercle osteotomy in patello-femoral instability and in patellar height abnormality Jacques H.
International Orthopaedics (SICOT) (2010) 34:305 309 DOI 10.1007/s00264-009-0929-4 ORIGINAL PAPER Tibial tubercle osteotomy in patello-femoral instability and in patellar height abnormality Jacques H.
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
5/14/2013. Acute vs Chronic Mechanism of Injury:
 Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
The medial side of the knee has been relatively overlooked
 REVIEW ARTICLE Medial and Posteromedial Instability of the Knee: Evaluation, Treatment, and Results James P. Stannard, MD Abstract: Medial-sided knee ligament injuries are complex and require a thorough
REVIEW ARTICLE Medial and Posteromedial Instability of the Knee: Evaluation, Treatment, and Results James P. Stannard, MD Abstract: Medial-sided knee ligament injuries are complex and require a thorough
Imaging the Athlete s Knee. Peter Lowry, MD Musculoskeletal Radiology University of Colorado
 Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
ACL AND PCL INJURIES OF THE KNEE JOINT
 ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
Knee Joint Assessment and General View
 Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
DISCLOSURES. Overview 09/24/2015. Patellofemoral Instability and Treatment Options. I do not have anything to disclose
 Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
On Field Assessment and Management of Acute Knee Injuries: A Physiotherapist s Perspective
 On Field Assessment and Management of Acute Knee Injuries: A Physiotherapist s Perspective Jessica Condliffe Physiotherapist / Clinic Manager TBI Health Wellington Presentation Outline Knee anatomy review
On Field Assessment and Management of Acute Knee Injuries: A Physiotherapist s Perspective Jessica Condliffe Physiotherapist / Clinic Manager TBI Health Wellington Presentation Outline Knee anatomy review
First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability
 Special Focus Section 303 First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability Laura Lewallen, MD 1 Amy McIntosh, MD 1 Diane Dahm, MD 1 1 Department of Orthopedic Surgery, Mayo
Special Focus Section 303 First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability Laura Lewallen, MD 1 Amy McIntosh, MD 1 Diane Dahm, MD 1 1 Department of Orthopedic Surgery, Mayo
Knee Injury Assessment
 Knee Injury Assessment Clinical Anatomy p. 186 Femur Medial condyle Lateral condyle Femoral trochlea Tibia Intercondylar notch Tibial tuberosity Tibial plateau Fibula Fibular head Patella Clinical Anatomy
Knee Injury Assessment Clinical Anatomy p. 186 Femur Medial condyle Lateral condyle Femoral trochlea Tibia Intercondylar notch Tibial tuberosity Tibial plateau Fibula Fibular head Patella Clinical Anatomy
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD
 Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
SURGICAL TECHNIQUE PREPARED BY MEDSHAPE, INC. IN CONJUNCTION WITH JACK FARR, M.D. MPFL RECONSTRUCTION
 ! SURGICAL TECHNIQUE PREPARED BY MEDSHAPE, INC. IN CONJUNCTION WITH JACK FARR, M.D. LATERAL PATELLOFEMORAL INSTABILITY AND THE MEDIAL PATELLOFEMORAL COMPLEX Lateral patellofemoral instability is characterized
! SURGICAL TECHNIQUE PREPARED BY MEDSHAPE, INC. IN CONJUNCTION WITH JACK FARR, M.D. LATERAL PATELLOFEMORAL INSTABILITY AND THE MEDIAL PATELLOFEMORAL COMPLEX Lateral patellofemoral instability is characterized
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
Radiological evaluation of the causes of patellar instability.
 Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
The Role of Medial Patellofemoral Ligament Repair and Imbrication
 A Review Paper The Role of Medial Patellofemoral Ligament Repair and Imbrication Kyle R. Duchman, MD, and Matthew J. Bollier, MD Abstract Repair, reefing, and advancement of the medial patellofemoral ligament
A Review Paper The Role of Medial Patellofemoral Ligament Repair and Imbrication Kyle R. Duchman, MD, and Matthew J. Bollier, MD Abstract Repair, reefing, and advancement of the medial patellofemoral ligament
Assessment of Patellar Laxity in the in vitro Native Knee
 Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
Personal use only. MRI of the extensor mechanism of the knee. 5 th Musculoskeletal MRI meeting. Falkowski, MD, MHBA
 MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
HISTORY AND INDICATIONS OF LATERAL TENODESIS IN ATHLETES
 HISTORY AND INDICATIONS OF LATERAL TENODESIS IN ATHLETES Written by Philippe Landreau, Qatar The treatment of anterior cruciate ligament injuries remains challenging in young athletic populations. A residual
HISTORY AND INDICATIONS OF LATERAL TENODESIS IN ATHLETES Written by Philippe Landreau, Qatar The treatment of anterior cruciate ligament injuries remains challenging in young athletic populations. A residual
1 st Time Patella Dislocation When is it best to intervene? The Dilemma. Patellar Dislocation The Issues 3/9/2018. Is there a difference?
 1 st Time Patella Dislocation When is it best to intervene? Jim Bradley MD Clinical Professor UPMC Head Team Physician, Pittsburgh Steelers Consultant Miami Marlins Michael Nickoli MD Orthopaedic Surgery
1 st Time Patella Dislocation When is it best to intervene? Jim Bradley MD Clinical Professor UPMC Head Team Physician, Pittsburgh Steelers Consultant Miami Marlins Michael Nickoli MD Orthopaedic Surgery
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management
 SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
ORIGINAL STUDY INTRODUCTION
 Acta Orthop. Belg., 2006, 72, 65-71 ORIGINAL STUDY Clinical results of isolated reconstruction of the medial patellofemoral ligament for recurrent dislocation and subluxation of the patella Yoshinori MIKASHIMA,
Acta Orthop. Belg., 2006, 72, 65-71 ORIGINAL STUDY Clinical results of isolated reconstruction of the medial patellofemoral ligament for recurrent dislocation and subluxation of the patella Yoshinori MIKASHIMA,
Anterolateral Ligament. Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine
 Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Retinacular tear knee
 P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
Disclosures. Outline. The Posterior Cruciate Ligament 5/3/2016
 The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
The Lower Limb II. Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa
 The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
The Knee 20 S1 (2013) S3 S15. Contents lists available at SciVerse ScienceDirect. The Knee
 The Knee 20 S1 (2013) S3 S15 Contents lists available at SciVerse ScienceDirect The Knee Review The contemporary management of anterior knee pain and patellofemoral instability Toby O. Smith, Iain McNamara,
The Knee 20 S1 (2013) S3 S15 Contents lists available at SciVerse ScienceDirect The Knee Review The contemporary management of anterior knee pain and patellofemoral instability Toby O. Smith, Iain McNamara,
Iliotibial Band Tension Reduces Patellar Lateral Stability
 Iliotibial Band Tension Reduces Patellar Lateral Stability Azhar M. Merican, 1,2 Farhad Iranpour, 2 Andrew A. Amis 2,3 1 Department of Orthopaedic Surgery, University Malaya Medical Centre, 50603 Kuala
Iliotibial Band Tension Reduces Patellar Lateral Stability Azhar M. Merican, 1,2 Farhad Iranpour, 2 Andrew A. Amis 2,3 1 Department of Orthopaedic Surgery, University Malaya Medical Centre, 50603 Kuala
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Surgical treatment of patellar instability can be
 Medial Patellofemoral Ligament Reconstruction Using a Modified Reverse-Loop Technique Nels E. Sampatacos, M.D., and Mark H. Getelman, M.D. Abstract: Medial patellofemoral ligament reconstruction is a commonly
Medial Patellofemoral Ligament Reconstruction Using a Modified Reverse-Loop Technique Nels E. Sampatacos, M.D., and Mark H. Getelman, M.D. Abstract: Medial patellofemoral ligament reconstruction is a commonly
Medial Patellofemoral Ligament Reconstruction
 Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
9/24/2012. Greg Bennett, PT, DSc Excel Physical Therapy Marymount University
 Greg Bennett, PT, DSc Excel Physical Therapy Marymount University Hx often diagnostic Least to most threatening Sx trump exam Develop consistent routine Don t inflame inflamed tissue 1 1. ESTABLISH OR
Greg Bennett, PT, DSc Excel Physical Therapy Marymount University Hx often diagnostic Least to most threatening Sx trump exam Develop consistent routine Don t inflame inflamed tissue 1 1. ESTABLISH OR
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player
 UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
Lower Extremity Sports Injuries
 Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Patellar instability
 Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
The Knee. Two Joints: Tibiofemoral. Patellofemoral
 Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Patellar malalignment: a new method on knee MRI
 DOI 10.1186/s40064-016-3195-0 RESEARCH Open Access Patellar malalignment: a new method on knee MRI Hülya Kurtul Yildiz * and Elif Evrim Ekin Abstract Purpose: The medial patellofemoral ligament (MPFLL)/lateral
DOI 10.1186/s40064-016-3195-0 RESEARCH Open Access Patellar malalignment: a new method on knee MRI Hülya Kurtul Yildiz * and Elif Evrim Ekin Abstract Purpose: The medial patellofemoral ligament (MPFLL)/lateral
CHRONIC PATELLOFEMORAL INSTABILITY
 INSTRUCTIONAL COURSE LECTURE DAVID J. DANDY From Addenbrooke s Hospital, Cambridge, England This article aims to discuss the many causes of patellofemoral instability so that an appropriate stabilisation
INSTRUCTIONAL COURSE LECTURE DAVID J. DANDY From Addenbrooke s Hospital, Cambridge, England This article aims to discuss the many causes of patellofemoral instability so that an appropriate stabilisation
MPFL positioning on the femoral side
 MPFL positioning on the femoral side Stephen et al AJSM 2012 Prof Dr med Jacques Menetrey, MD, PhD Dr med Philippe Tscholl, MD Centre de médecine de l appareil moteur et du sport - HUG Swiss Olympic medical
MPFL positioning on the femoral side Stephen et al AJSM 2012 Prof Dr med Jacques Menetrey, MD, PhD Dr med Philippe Tscholl, MD Centre de médecine de l appareil moteur et du sport - HUG Swiss Olympic medical
Chapter 20 The knee and related structures
 Chapter 20 The knee and related structures Athletic Training Spring 2014 Jihong Park Bones & joints Femur, tibia, fibula, & patella Femur & tibia Weight bearing & muscle attachment Patella functions Anterior
Chapter 20 The knee and related structures Athletic Training Spring 2014 Jihong Park Bones & joints Femur, tibia, fibula, & patella Femur & tibia Weight bearing & muscle attachment Patella functions Anterior
Diagnosis and Management of Knee Conditions. Jenny Love / Lynn Robertson AFLAR Oct 2009
 Diagnosis and Management of Knee Conditions Jenny Love / Lynn Robertson AFLAR Oct 2009 AIMS Review 4 common Knee Conditions: Anterior knee pain Meniscal Injuries Ligament injuries ACL Osteoarthritis Discuss
Diagnosis and Management of Knee Conditions Jenny Love / Lynn Robertson AFLAR Oct 2009 AIMS Review 4 common Knee Conditions: Anterior knee pain Meniscal Injuries Ligament injuries ACL Osteoarthritis Discuss
Prevention and Treatment of Injuries. Anatomy. Anatomy. Chapter 20 The Knee Westfield High School Houston, Texas
 Prevention and Treatment of Injuries Chapter 20 The Knee Westfield High School Houston, Texas Anatomy MCL, Medial Collateral Ligament LCL, Lateral Collateral Ligament PCL, Posterior Cruciate Ligament ACL,
Prevention and Treatment of Injuries Chapter 20 The Knee Westfield High School Houston, Texas Anatomy MCL, Medial Collateral Ligament LCL, Lateral Collateral Ligament PCL, Posterior Cruciate Ligament ACL,
Medical Diagnosis for Michael s Knee
 Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
Department of Orthopedic Surgery, Ewha Womans University Mokdong Hospital, Seoul, Korea
 Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Fibular collateral ligament reconstruction of knee using titanium button: a new fixation technique and an outcome of 35 cases
 International Journal of Research in Orthopaedics Rai SK et al. Int J Res Orthop. 2017 May;3(3):573-577 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20171904
International Journal of Research in Orthopaedics Rai SK et al. Int J Res Orthop. 2017 May;3(3):573-577 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20171904
Knee Injuries. PSK 4U Mr. S. Kelly North Grenville DHS. Medial Collateral Ligament Sprain
 Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
SOFT TISSUE KNEE INJURIES
 SOFT TISSUE KNEE INJURIES Soft tissue injuries of the knee commonly occur in all sports or in any activity that requires sudden changes in activity or movement. The knee is a complex joint and any injury
SOFT TISSUE KNEE INJURIES Soft tissue injuries of the knee commonly occur in all sports or in any activity that requires sudden changes in activity or movement. The knee is a complex joint and any injury
THE LOWER EXTREMITY EXAM FOR THE FAMILY PRACTITIONER
 THE LOWER EXTREMITY EXAM FOR THE FAMILY PRACTITIONER Melinda A. Scott, D.O. Orthopedic Associates of Dayton Board Certified in Primary Care Sports Medicine GOALS Identify landmarks necessary for exam of
THE LOWER EXTREMITY EXAM FOR THE FAMILY PRACTITIONER Melinda A. Scott, D.O. Orthopedic Associates of Dayton Board Certified in Primary Care Sports Medicine GOALS Identify landmarks necessary for exam of
World Medical & Health Games
 Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
40 th Annual Symposium on Sports Medicine. Knee Injuries In The Pediatric Athlete. Disclosure
 40 th Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio Knee Injuries In The Pediatric Athlete Disclosure Dr. Travis Murray
40 th Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio Knee Injuries In The Pediatric Athlete Disclosure Dr. Travis Murray
